Abstract
Objective
Dialectical Behavior Therapy (DBT) with the DBT Prolonged Exposure (DBT PE) protocol is an integrated treatment for suicidal and self-injuring individuals with PTSD and borderline personality disorder (BPD) that occurs in three stages: Stage 1 targets behavioral dyscontrol, Stage 2 targets PTSD via the DBT PE protocol, and Stage 3 addresses remaining problems. We evaluated the course of change in multiple outcomes across these three stages and compared them to changes found in DBT alone.
Method
Participants were 38 women with BPD, PTSD and recent suicidal and/or non-suicidal self-injury. Data were collected weekly or bi-weekly to assess PTSD, BPD, global well-being, state dissociation, and urges to engage in problem behaviors.
Results
In DBT + DBT PE, there was a significant improvement in PTSD in Stage 2 and in PTSD, BPD, and state dissociation in Stage 3. Compared to DBT, DBT + DBT PE led to significantly higher global well-being and moderately, but non-significantly, lower PTSD and BPD in Stages 2 and/or 3.
Conclusions
PTSD does not improve until it is directly targeted and changes in other comorbid problems occur after PTSD is treated. Adding the DBT PE protocol to DBT was associated with improvement rather than worsening of outcomes.
Keywords: PTSD, borderline personality disorder, intentional self-injury, Dialectical Behavior Therapy, Prolonged Exposure
Individuals meeting criteria for posttraumatic stress disorder (PTSD) typically exhibit multiple comorbid problems and diagnoses (Pietrzak, Goldstein, Southwick, & Grant, 2011). However, PTSD treatments often focus solely on treating PTSD and exclude many individuals with serious comorbidities (Ronconi, Shiner & Watts, 2014). In addition, although evidence-based PTSD treatments improve some comorbid problems, their effect on more severe comorbidities appears to be limited (van Minnen, Zoellner, Harned, & Mills, 2015). Integrated treatments that allow for concurrent targeting of multiple problems in the same treatment are increasingly recommended as the optimal approach for individuals with PTSD and severe comorbidities (e.g., Najavits et al., 2009; Rizvi & Harned, 2013; van Minnen et al., 2015).
Individuals who meet criteria for borderline personality disorder (BPD) and PTSD are a particularly high-risk and comorbid client population. In clinical samples of BPD clients, approximately half meet criteria for PTSD (Harned, Rizvi, & Linehan, 2010; Zanarini, Frankenburg, Hennen, Reich, & Silk, 2004) and those with PTSD are generally more impaired than those without PTSD across multiple domains of functioning (e.g., Harned et al., 2010; Pagura et al., 2010; Rüsch et al., 2007). Some of the most common co-occurring problems among individuals with BPD and PTSD are suicide attempts, non-suicidal self-injury (NSSI), dissociation, and substance use. Among individuals with BPD, the presence of PTSD more than doubles the frequency of NSSI (Harned et al., 2010; Rüsch et al., 2007) and nearly doubles the risk of suicide attempts (Pagura et al., 2010; Wedig et al., 2012). In addition, more than two-thirds of clients with BPD report moderate to high levels of dissociation (Zanarini, Ruser, Frankenburg, & Hennen, 2000), and those with high levels of dissociation have more PTSD symptoms and traumatic experiences (Sar, Akyuz, Kugu, Ozturk, & Ertem-Vehid, 2006). Approximately 50% of clients with BPD also meet criteria for a substance use disorder (SUD; Grant et al., 2008), and individuals with both BPD and PTSD are more likely to meet criteria for a lifetime SUD than those with BPD alone (Pagura et al., 2010).
The increased risk of these co-occurring problems among individuals with BPD and PTSD is likely due to the use of these behaviors to cope with the intense negative affect and cognitions associated with PTSD and trauma exposure. For example, BPD clients with PTSD are more likely than those without PTSD to report self-injuring and attempting suicide in response to flashbacks, nightmares, and thoughts about sexual abuse or rape (Harned et al., 2010). Similarly, individuals with BPD are particularly likely to dissociate in response to thoughts about aversive personal experiences, and this dissociation functions to reduce emotional distress (Barnow et al., 2012). Individuals with BPD are also more likely than those without BPD to report using illicit drugs or misusing prescribed medications to control PTSD symptoms (Leeies, Pagura, Sareen, & Bolton, 2010). Moreover, both dissociation and substance use increase the risk of suicide attempts and NSSI among individuals with BPD (Wedig et al., 2012; Zanarini, Laudate, Frankenburg, Reich, & Fitzmaurice, 2011).
Faced with a client with BPD and PTSD who reports multiple high-risk and severe problems, many of which are functionally related to PTSD, it can be difficult for clinicians to decide how and in what order these many problems should be targeted. This is further complicated by the fact that many clinicians believe that trauma-focused treatments such as exposure therapy are likely to cause increases in suicidality, self-injury, dissociation, substance use, and treatment dropout, particularly among more complex clients (Becker et al., 2004; van Minnen, Hendriks, & Olff, 2010). Dialectical Behavior Therapy (DBT) with the DBT Prolonged Exposure protocol (DBT + DBT PE) is an integrated treatment that has been shown to be safe and more effective than DBT alone in reducing suicide attempts, NSSI, PTSD, and multiple additional problems (e.g., dissociation, global impairment) among suicidal and self-injuring individuals with BPD and PTSD (Harned, Korslund, Foa, & Linehan, 2012; Harned, Korslund, & Linehan, 2014). This one-year treatment combines standard DBT (Linehan, 1993) with adapted Prolonged Exposure therapy for PTSD (Foa, Hembree, & Rothbaum, 2007) and occurs in three stages. Stage 1 focuses on stabilizing life-threatening behaviors and other types of severe behavioral dyscontrol. Once sufficient behavioral stability has been achieved, clients progress to Stage 2 that involves integrating the DBT PE protocol into ongoing DBT to allow for direct targeting of PTSD while continuing to address comorbid problems. Stage 3 occurs after PTSD treatment is complete and involves using DBT to address any remaining problems that interfere with having a positive quality of life. The treatment is principle-driven and idiographic, with clients progressing through stages at different times based on their progress and treatment goals.
The primary aim of the present study was to evaluate the timing and course of changes in multiple areas of functioning relevant to individuals with BPD and PTSD across the three stages of DBT + DBT PE. The secondary aim was to compare these changes to those found in DBT when PTSD was not directly targeted either because clients were randomized to receive DBT alone (DBT) or they did not initiate the DBT PE protocol during DBT (DBT-No DBT PE). To that end, we conducted secondary analyses of data from two treatment outcome studies of DBT with and without the DBT PE protocol (Harned et al., 2012; Harned et al., 2014). In contrast to the primary outcome studies that used data collected at quarterly or bi-annual outcome assessments to evaluate change over treatment as a whole, the present analyses used data collected at weekly individual therapy sessions to evaluate the weekly or bi-weekly course of change during the three stages of treatment. In addition, outcomes and measures reflect those recommended for routine monitoring by clinicians during delivery of DBT + DBT PE, including PTSD severity, BPD severity, global well-being, state dissociation, and urges to commit suicide, self-injure, use substances, and drop out of therapy. Consistent with the targets of each stage of DBT + DBT PE, as well as prior research demonstrating the superiority of DBT + DBT PE over DBT, we made the following apriori hypotheses:
In DBT + DBT PE, urges to commit suicide and self-harm would decrease in Stage 1, PTSD severity would decrease in Stage 2, no outcomes would significantly worsen in Stage 2, and other outcomes would improve in Stage 3.
Improvements in all outcomes would be greater by Stage 3 of DBT + DBT PE compared to time-matched legs of DBT and DBT-No DBT PE.
Methods
Participants
Eligibility criteria
Participants were 38 women with BPD and PTSD who participated in an open trial of DBT + DBT PE (n = 13; Harned et al., 2012) or a randomized controlled trial comparing DBT with and without the DBT PE protocol (n = 25; Harned et al., 2014). Inclusion criteria were: (1) BPD, (2) PTSD, (3) 18–60 years of age, (4) female, and (5) recent (past 3 months (Harned et al., 2012) or past 2 months (Harned et al., 2014)) suicidal behavior or serious NSSI. Given that DBT + DBT PE is intended for individuals who would typically be excluded from standard PTSD treatments, NSSI was required to be serious (defined as behavior that had more than a mild effect on the person’s physical condition) to reflect the exclusion criteria specified in the PE manual (Foa et al., 2007). Participants were excluded if they met criteria for a lifetime psychotic or bipolar disorder, had an IQ less than 70, or were mandated to treatment.
Sample characteristics
The sample ranged in age from 19 to 57 years (M = 35.0, SD = 12.2). Participants were White (76.3%), biracial (18.4%), and Asian-American (5.2%). In addition, 5.3% were of Hispanic ethnicity. Nearly all participants had graduated from high school (94.7%) and 28.9% had graduated from college. The majority were non-married (78.9%) and earned less than $20,000 in the past year (82.4%). Index (i.e., most distressing) traumas included: childhood sexual abuse (55.3%), adult rape (15.8%), childhood physical abuse (10.5%), physical assault by an intimate partner (5.3%), threats of death or serious harm (5.3%), sudden death of a friend or loved one (5.3%), and witnessing domestic violence as a child (2.6%). The sample was highly comorbid (current Axis I diagnoses: M = 4.7, SD = 2.0; Axis II diagnoses: M = 2.1, SD = 1.1) and seriously impaired (GAF score: M = 43.1, SD = 3.7). In the past year, participants had engaged in an average of 54.9 NSSI acts (SD = 91.3) and 1.7 suicide attempts (SD = 4.6). There were no significant differences between the three treatment groups on any baseline demographic or clinical characteristic.
Procedures
Recruitment and screening
All procedures were approved by the University of Washington Institutional Review Board. Participants were recruited via advertisements and outreach to area treatment providers. After an initial phone screen, participants completed an in-person assessment to evaluate study inclusion/exclusion criteria and gather more detailed diagnostic and pre-treatment information. The current analyses include data from 38 of the 39 participants in the intent-to-treat (ITT) samples. (One ITT participant in the DBT condition of the RCT could not be included due to an administrative error in obtaining consent to use weekly treatment data.)
Assessments
Outcome data analyzed in the present study were collected before and after weekly individual therapy sessions. Clients completed these self-report measures independently using a computer in the clinic waiting area. Client responses on these measures were not shared with their therapists with the exception of the PTSD Checklist (which was used clinically to monitor progress).
Subject Flow and Retention
Participants in the open trial (n = 13) were assigned to receive one year of DBT with the DBT PE protocol. Participants in the RCT were randomized to receive DBT (n = 8) or DBT + DBT PE (n = 17). Consistent with prior studies of PE (Foa et al., 2005), completing the DBT PE protocol was defined as completing 8 sessions, at least 6 of which included imaginal exposure, or achieving diagnostic remission from PTSD, whichever came first. Of the 30 participants assigned to DBT + DBT PE from both studies, 18 (60.0%; n’s = 10 from the open trial and 8 from the RCT) started the DBT PE protocol; of these, 13 (72.2%; n’s = 7 from the open trial and 6 from the RCT) completed it. The remaining 12 participants (40.0%; n’s = 3 from the open trial and 9 from the RCT) did not start the DBT PE protocol. For the present analyses, participants were separated into three groups. The DBT group included participants assigned to DBT in the RCT (n = 8). The DBT + DBT PE group included participants from both studies who received at least one session of the DBT PE protocol (n = 18). The DBT-No DBT PE group included participants assigned to DBT + DBT PE in both studies who never started the DBT PE protocol (n = 12). The rate of treatment dropout was significantly lower in the DBT + DBT PE group (n = 1, 5.6%) than in the DBT-No DBT PE group (n = 8, 66.7%) and the DBT group (n = 4, 50.0%; χ2 (2) = 13.1, p = .001). Participants who dropped out of treatment were less likely to have current major depression (60%) than those who completed treatment (96%; Fisher’s exact test, p < .02). There were no other differences between dropouts and completers on baseline Axis I and II diagnoses, global functioning, or frequency of suicidal and self-injurious behavior.
Treatment Groups
DBT (n=8)
Treatment consisted of one year of standard DBT (Linehan, 1993), including individual therapy (1 hour/week), group skills training (2.5 hours/week), phone consultation (as needed) and weekly therapist consultation team (1 hour/week). DBT targets, in hierarchical order: life-threatening behaviors (e.g., suicide attempts and NSSI), behaviors that interfere with treatment delivery (e.g., noncompliance), and severe quality of life interfering behaviors (e.g., severe Axis I disorders, relationship and employment problems). Consistent with standard clinical practice of DBT, direct or structured targeting of PTSD via trauma processing did not occur. Instead, therapists addressed PTSD using a present-centered approach that focused on teaching clients skills to manage PTSD symptoms as needed.
DBT + DBT PE (n=18)
In addition to receiving one year of standard DBT, these participants also received at least one session of the DBT PE protocol. Treatment occurred in 3 stages: Stage 1 (DBT targeting behavioral dyscontrol), Stage 2 (DBT with DBT PE for PTSD), and Stage 3 (DBT targeting any remaining problems). To progress from Stage 1 to 2, clients had to meet specified readiness criteria (i.e., not at imminent risk of suicide, no suicidal or self-injurious behavior for at least 2 months, no serious therapy-interfering behavior, PTSD is the client’s highest priority treatment goal, and ability to experience intense emotions without escaping). Once these criteria were met, the DBT PE protocol was implemented concurrently with DBT such that patients received either one combined individual therapy session per week (90 min of DBT PE and 30 min of DBT) or two individual therapy sessions per week (one DBT PE session (90 min) and one DBT session (1 hour)) as well as group DBT skills training and as needed phone consultation. The DBT PE protocol is based on PE (Foa et al., 2007) and uses the same primary components of in vivo exposure and imaginal exposure followed by emotional processing of the exposure experience. The DBT PE protocol includes adaptations designed to address the specific characteristics of this client population, as well as to maximize compatibility with DBT (Harned, 2013). The duration of the DBT PE protocol was based on continuous assessment of the client’s PTSD.
DBT-No DBT PE (n=12)
In addition to receiving one year of standard DBT, these participants had the option of receiving the DBT PE protocol, but did not initiate it. Reasons for not starting the DBT PE protocol included: premature dropout from DBT (n = 7), PTSD remitted without targeted treatment (n = 3), and inability to stabilize higher priority behaviors (n = 2).
Measures
Screening measures
BPD and other Axis II disorders were diagnosed using the International Personality Disorder Examination (Loranger, 1995), PTSD was diagnosed using the DSM-IV version of the PTSD Symptom Scale – Interview (Foa, Riggs, Dancu, & Rothbaum, 1993), and other Axis I disorders were diagnosed using the Structured Clinical Interview for DSM-IV (First, Spitzer, Gibbon & Williams, 1995). The Suicide Attempt Self-Injury Interview (Linehan, Comtois, Brown, Heard, & Wagner, 2006) was used to assess the frequency, intent, and severity of suicide attempts and NSSI.
PTSD Checklist – Civilian Version (PCL-C)
The 17-item PCL-C (Weathers et al., 1993) was administered every other week to assess the severity of the 17 DSM-IV PTSD symptoms over the past two weeks. Items were rated on a Likert scale from 1 (not at all) to 5 (extremely). A total score is created by summing the items (range = 17 to 85). The PCL-C has been shown to have acceptable internal consistency (α > .75) and test-retest reliability (r = .75–.88) (Wilkins, Lang, & Norman, 2012). Internal consistency in the present sample was excellent (α = .94).
Borderline Symptom List (BSL)
An adapted 15-item version of the BSL (Bohus et al., 2007) was administered on alternate weeks as the PCL-C. Items assess problems common in BPD in the past week such as “I was overwhelmed by my feelings” and “I was longing for death” and are rated on a Likert scale from 0 (not at all) to 4 (very strong). The BSL has been shown to have excellent internal consistency (α = .97) and good test-rest reliability (r = .84). Items were averaged for analyses and internal consistency in the present sample was excellent (α = .94). The BSL also includes a visual analog scale to assess global well-being that ranges from 0% (very bad) to 100% (excellent). This item asks about the “quality of your overall personal state” in the last week and has been found to be highly correlated with the BSL total score (Bohus et al., 2007).
Dissociative State Scale (DSS)
The 4-item DSS (Stiglmayr et al., 2009) was administered before and after every individual therapy session to assess the level of current state dissociation. Example items include: “I have the impression that my body does not belong to me” and “I have the impression other people or things around me are unreal.” Items are rated on a Likert scale ranging from 0 (not present) to 9 (very strong). The DSS has been shown to have good internal consistency (α =.87) and excellent split-half reliability (r = .91). A total score is computed by averaging the items. The average of the pre- and post-session DSS total scores was used in the present analyses and showed excellent internal consistency (α = .94).
Urges to engage in problem behaviors
Urges to commit suicide, self-harm, use substances (alcohol and/or drugs), and drop out of therapy were assessed before and after individual therapy sessions. These urges are routinely assessed during DBT + DBT PE sessions to enable clinicians to monitor clients’ current level of risk and intervene when urges are high to reduce the likelihood of an escalation to actual behaviors. As is done in routine clinical practice, each urge was assessed using a single item that was rated on a Likert scale ranging from 0 to 5. Each type of urge was analyzed separately using the average of the pre- and post-session ratings.
Data Analysis
A multiphase mixed-effects model (MPMEM; Cudeck & Klebe, 2002) was calculated for each outcome to analyze within-group changes by stage of treatment in DBT + DBT PE, and between-group comparisons by time-matched legs of treatment in DBT + DBT PE versus DBT and DBT-No DBT PE. MPMEMs are designed to evaluate behaviors that develop in phases and may exhibit distinctively different rates of change in one phase than in others and have been found to be robust with small sample sizes (Institute of Medicine, 2001; Mass & Hox, 2004). MPMEM models the within-patient correlation of the repeated measures using spatial covariance structures, where the correlation between repeated measures is dependent on the amount of time between the respective pair of points, which may be quite distinct across participants (Moser & Macchiavelli, 1996). For participants who received DBT + DBT PE, three indicator variables were created that indicated the stage of treatment within which each data point was collected. In addition, three time variables were calculated that represented the actual number of weeks within each of the three stages of treatment: Stage 1 (M = 19.3, SD = 9.4), Stage 2 (M = 13.4, SD = 7.5), and Stage 3 (M = 16.5, SD = 11.5). To enable time-matched comparisons between groups, three indicator variables were created for participants in the non-staged treatments (DBT and DBT-No DBT PE) that indicated the “leg” of treatment within which the data were collected. Treatment legs were calculated to match the median number of weeks of each stage of DBT + DBT PE for a given outcome measure. In addition, three time variables were calculated that represented the actual number of weeks within each of the three treatment legs.
For each outcome, a MPMEM was conducted that included effects for each time variable (3 variables per group as defined above) as well as interactions between each stage/leg variable and its associated time variable (i.e., the slope within each stage). The effects of specific interest for the purposes of this study were the slope effects within each stage of DBT + DBT PE. In addition, statistical contrast statements were used to examine: (1) within-group differences in average scores between each stage of DBT + DBT PE, and (2) between-group differences in average scores for each time-matched stage/leg of treatment across the three groups. Given the small sample sizes, emphasis was placed on evaluating the magnitude of differences for the statistical constrasts. Specifically, Cohen’s d effect sizes with 95% confidence intervals were calculated for within- and between-group MPMEM contrasts of average scores using the formula specified by Feingold (2009) (equation 7) with the SD term estimated by Wackerly, Mendenhall, and Scheaffer (2008). Cohen’s d is interpreted as .20 = small, .50 = medium, and .80 = large (Cohen, 1988). Consistent with the primary outcome studies, we interpret effect sizes that are medium or large.
Although MPMEM is flexible in handling missing data, pattern-mixture models were used to assess whether the rate of change within phases was dependent on missing data patterns (Hedeker & Gibbons, 1997). Given the difference in treatment dropout rates between groups, we used the pattern mixture approach to examine the impact of missing data due to treatment dropout for each outcome. If the estimate of interest (i.e., the rate of change within phase) is dependent on missing data patterns, then the missing data are informative.
Results
Preliminary Analyses
Descriptive data for the start and average values for each outcome by group and stage or leg of treatment are presented in Table 1. Statistical contrasts from the MPMEM analyses indicated there were no significant differences in baseline start values on any outcome between the three groups (p’s = .06 – .94). The pattern mixture models indicated no significant effect of missing data due to dropout on any outcome.
Table 1.
Descriptive Data for Start Values and Average Values
| DBT + DBT PE (n=18) | DBT-No DBT PE (n=12) | DBT (n=8) | |||||||
|---|---|---|---|---|---|---|---|---|---|
|
|
|
|
|||||||
| Stage 1 | Stage 2 | Stage 3 | Leg 1 | Leg 2 | Leg 3 | Leg 1 | Leg 2 | Leg 3 | |
| PTSD severity, n | 18 | 18 | 17 | 11 | 9 | 5 | 7 | 7 | 5 |
| Start value, M (SE) | 54.19 (3.46) | 57.90 (3.59) | 50.49 (3.77) | 59.42 (4.84) | 66.62 (5.76) | 58.44 (5.83) | 56.96 (6.04) | 62.66 (7.09) | 62.43 (6.45) |
| Average value, M (SE) | 55.11 (3.24) | 54.78 (3.28) | 46.75 (3.34) | 56.13 (5.69) | 52.68 (6.10) | 58.00 (5.15) | 56.73 (6.22) | 62.84 (8.03) | 57.11 (5.86) |
| BPD severity, n | 18 | 17 | 18 | 12 | 9 | 6 | 8 | 5 | 5 |
| Start value, M (SE) | 1.88 (0.20) | 1.73 (0.21) | 1.78 (0.22) | 2.53 (0.27) | 1.74 (0.35) | 2.21 (0.32) | 1.99 (0.33) | 2.23 (0.45) | 2.47 (0.41) |
| Average value, M (SE) | 1.83 (0.18) | 1.76 (0.19) | 1.56 (0.19) | 1.54 (0.34) | 2.52 (0.39) | 2.21 (0.28) | 2.22 (0.39) | 2.45 (0.45) | 2.21 (0.35) |
| Global well-being, n | 18 | 17 | 18 | 12 | 9 | 6 | 8 | 5 | 5 |
| Start value, M (SE) | 41.26 (3.97) | 44.18 (4.57) | 45.70 (4.76) | 27.94 (6.81) | 57.81 (10.06) | 26.78 (7.58) | 31.28 (8.01) | 19.01 (13.39) | 19.27 (10.11) |
| Average value, M (SE) | 42.91 (2.73) | 48.54 (3.08) | 47.59 (3.31) | 41.85 (9.79) | 15.68 (11.76) | 28.97 (5.42) | 44.84 (10.46) | 25.45 (13.02) | 25.36 (7.09) |
| State dissociation, n | 12 | 15 | 18 | 10 | 8 | 6 | 8 | 7 | 5 |
| Start value, M (SE) | 1.51 (0.55) | 2.32 (0.54) | 1.95 (0.54) | 2.71 (0.74) | 2.77 (0.82) | 2.39 (0.83) | 2.85 (0.82) | 2.80 (0.88) | 3.51 (0.91) |
| Average value, M (SE) | 1.59 (0.52) | 1.99 (0.50) | 1.55 (0.48) | 1.86 (0.78) | 2.22 (0.87) | 2.35 (0.75) | 2.35 (0.86) | 3.04 (0.95) | 3.02 (0.82) |
| Urges to suicide, n | 12 | 14 | 18 | 10 | 7 | 6 | 8 | 7 | 5 |
| Start value, M (SE) | 1.14 (0.34) | 0.95 (0.34) | 1.33 (0.33) | 1.36 (0.47) | 1.18 (0.57) | 1.04 (0.55) | 1.08 (0.52) | 1.36 (0.59) | 1.79 (0.60) |
| Average value, M (SE) | 1.06 (0.30) | 1.16 (0.29) | 1.08 (0.28) | 1.02 (0.52) | 1.18 (0.61) | 1.02 (0.47) | 1.50 (0.56) | 2.11 (0.65) | 1.71 (0.50) |
| Urges to self-harm, n | 12 | 14 | 18 | 10 | 7 | 6 | 8 | 7 | 5 |
| Start value, M (SE) | 1.41 (0.35) | 1.56 (0.35) | 1.30 (0.34) | 1.53 (0.47) | 0.95 (0.55) | 1.07 (0.53) | 1.23 (0.52) | 1.06 (0.58) | 1.89 (0.58) |
| Average value, M (SE) | 1.39 (0.33) | 1.43 (0.31) | 1.08 (0.30) | 0.85 (0.51) | 1.06 (0.59) | 1.01 (0.48) | 1.45 (0.56) | 2.31 (0.64) | 1.77 (0.52) |
| Urges to use substances, n | 12 | 14 | 18 | 10 | 7 | 6 | 8 | 7 | 5 |
| Start value, M (SE) | 1.20 (0.40) | 1.41 (0.39) | 1.24 (0.38) | 2.09 (0.53) | 2.10 (0.60) | 1.47 (0.60) | 1.26 (0.59) | 1.38 (0.64) | 1.77 (0.66) |
| Average value, M (SE) | 1.10 (0.37) | 1.34 (0.36) | 1.23 (0.34) | 1.84 (0.57) | 1.35 (0.64) | 1.60 (0.54) | 1.53 (0.62) | 2.21 (0.69) | 1.80 (0.59) |
| Urges to quit therapy, n | 12 | 14 | 18 | 10 | 7 | 6 | 8 | 7 | 5 |
| Start value, M (SE) | 1.10 (0.35) | 1.64 (0.34) | 1.22 (0.34) | 1.64 (0.49) | 0.86 (0.61) | 2.52 (0.58) | 1.53 (0.54) | 1.65 (0.62) | 1.94 (0.62) |
| Average value, M (SE) | 1.13 (0.29) | 1.44 (0.27) | 1.05 (0.27) | 2.19 (0.55) | 2.70 (0.65) | 2.21 (0.46) | 1.42 (0.59) | 2.38 (0.69) | 1.60 (0.50) |
Note. Descriptive data are estimates from the multi-phase mixed effects models. In DBT-No DBT PE and DBT, Legs 1–3 were calculated to match the median weeks of treatment for Stages 1–3 in DBT + DBT PE. The lower n’s for DBT + DBT PE and DBT-No DBT PE on state dissociation and urges are due to the fact that these measures were added to the assessment battery after the open trial had started.
Hypothesis 1: Within-Group Change in DBT + DBT PE
Our first hypothesis was that the pattern of change in outcomes during DBT + DBT PE would be consistent with the targets for each stage of treatment and that there would be no evidence of significant worsening of any outcome during Stage 2. This hypothesis was evaluated by examining the slope effects from the MPMEM analyses for each outcome during each stage of DBT + DBT PE (Table 2) and the within-group contrasts and effect sizes of differences in average values between stages of DBT + DBT PE (Table 3). Figure 1 displays the average start and end values for each stage of treatment.
Table 2.
Results of Multi-Phase Mixed Effects Models with Cohen’s d Effect Sizes for the Slopes
| DBT + DBT PE (n=18) | DBT-No DBT PE (n=12) | DBT (n=8) | |||||||
|---|---|---|---|---|---|---|---|---|---|
|
|
|
|
|||||||
| Stage 1 | Stage 2 | Stage 3 | Leg 1 | Leg 2 | Leg 3 | Leg 1 | Leg 2 | Leg 3 | |
| PTSD severity, n | 18 | 18 | 17 | 11 | 9 | 5 | 7 | 7 | 5 |
| Slope, B (SE) | 0.08 (0.12) | −0.40* (0.19) | −0.49* (0.20) | −0.30 (0.45) | −1.81* (0.85) | −0.06 (0.26) | −0.02 (0.47) | 0.02 (1.21) | −0.69** (0.25) |
| Effect size, d (CI) | 0.33 (−0.57, 1.23) | −0.98 (−1.88, −0.08) | −1.13 (−2.03, −0.23) | −0.30 (−1.21, 0.60) | −0.97 (−1.87, −0.07) | −0.10 (−1.00, 0.80) | −0.02 (−0.92, 0.88) | 0.01 (−0.89, 0.91) | −1.25 (−2.15, −0.35) |
| BPD severity, n | 18 | 17 | 18 | 12 | 9 | 6 | 8 | 5 | 5 |
| Slope, B (SE) | −0.004 (0.007) | 0.004 (0.01) | −0.03* (0.02) | −0.09* (0.03) | 0.10 (0.06) | −0.001 (0.01) | 0.02 (0.03) | 0.03 (0.07) | −0.03* (0.02) |
| Effect size, d (CI) | −0.27 (−1.17, 0.63) | 0.15 (−0.75, 1.06) | −1.06 (−1.97, −0.16) | −1.32 (−2.22, −0.42) | 0.74 (−0.16, 1.64) | −0.02 (−0.92, 0.88) | 0.27 (−0.63, 1.17) | 0.18 (−0.72, 1.08) | −0.91 (−1.81, −0.01) |
| Global well-being, n | 18 | 17 | 18 | 12 | 9 | 6 | 8 | 5 | 5 |
| Slope, B (SE) | 0.15 (0.22) | 0.57 (0.42) | 0.25 (0.44) | 1.26 (1.20) | −5.47* (2.32) | 0.28 (0.41) | 1.23 (1.30) | 0.84 (2.74) | 0.79 (0.51) |
| Effect size, d (CI) | 0.31 (−0.59, 1.21) | 0.61 (−0.29, 1.51) | 0.35 (−0.55, 1.25) | 0.48 (−0.42, 1.38) | −1.08 (−1.98, −0.18) | 0.32 (−0.58, 1.22) | 0.43 (−0.47, 1.33) | 0.14 (−0.76, 1.04) | 0.71 (−0.19, 1.61) |
| State dissociation, n | 12 | 15 | 18 | 10 | 8 | 6 | 8 | 7 | 5 |
| Slope, B (SE) | 0.01 (0.01) | −0.04 (0.02) | −0.05* (0.03) | −0.08 (0.06) | −0.07 (0.11) | −0.005 (0.03) | −0.05 (0.06) | 0.03 (0.10) | −0.06 (0.03) |
| Effect size, d (CI) | 0.20 (−0.69, 1.10) | −0.81 (−1.71, 0.09) | −0.92 (−1.82, −0.02) | −0.62 (−1.52, 0.28) | −0.31 (−1.21, 0.59) | −0.06 (−0.96, 0.84) | −0.35 (−1.25, 0.55) | 0.14 (−0.76, 1.04) | −0.86 (−1.76, 0.04) |
| Urges to suicide, n | 12 | 14 | 18 | 10 | 7 | 6 | 8 | 7 | 5 |
| Slope, B (SE) | −0.01 (0.01) | 0.03 (0.02) | −0.03 (0.02) | −0.03 (0.05) | <0.001 (0.09) | −0.003 (0.03) | 0.04 (0.05) | 0.10 (0.09) | −0.01 (0.03) |
| Effect size, d (CI) | −0.24 (−1.14, 0.66) | 0.59 (−0.31, 1.49) | −0.75 (−1.65, 0.15) | −0.29 (−1.19, 0.61) | 0.0004 (−0.90, 0.90) | −0.05 (−0.95, 0.85) | 0.34 (−0.56, 1.24) | 0.49 (−0.41, 1.39) | −0.16 (−1.06, 0.74) |
| Urges to self-harm, n | 12 | 14 | 18 | 10 | 7 | 6 | 8 | 7 | 5 |
| Slope, B (SE) | −0.001 (0.01) | −0.02 (0.02) | −0.03 (0.02) | −0.06 (0.04) | 0.01 (0.08) | −0.01 (0.02) | 0.02 (0.04) | 0.16 (0.08) | −0.02 (0.02) |
| Effect size, d (CI) | −0.07 (−0.97, 0.83) | −0.44 (−1.34, 0.46) | −0.74 (−1.64, 0.16) | −0.67 (−1.57, 0.23) | 0.08 (−0.82, 0.98) | −0.16 (−1.06, 0.74) | 0.21 (−0.69, 1.11) | 0.89 (−0.01, 1.80) | −0.32 (−1.23, 0.57) |
| Urges to use substances, n | 12 | 14 | 18 | 10 | 7 | 6 | 8 | 7 | 5 |
| Slope, B (SE) | −0.01 (0.01) | −0.01 (0.02) | −0.001 (0.02) | −0.02 (0.04) | −0.10 (0.08) | 0.02 (0.03) | 0.02 (0.05) | 0.11 (0.08) | 0.004 (0.02) |
| Effect size, d (CI) | −0.36 (−1.26, 0.53) | −0.23 (−1.13, 0.67) | −0.02 (−0.92, 0.88) | −0.25 (−1.15, 0.65) | −0.54 (−1.44, 0.36) | 0.30 (−0.60, 1.20) | 0.25 (−0.65, 1.15) | 0.60 (−0.30, 1.50) | 0.07 (−0.83, 1.00) |
| Urges to quit therapy, n | 12 | 14 | 18 | 10 | 7 | 6 | 8 | 7 | 5 |
| Slope, B (SE) | 0.003 (0.01) | −0.03 (0.02) | −0.02 (0.02) | 0.05 (0.06) | 0.24* (0.11) | −0.04 (0.03) | −0.01 (0.06) | 0.09 (0.10) | −0.04 (0.03) |
| Effect size, d (CI) | 0.09 (−0.81, 0.99) | −0.51 (−1.41, 0.39) | −0.47 (−1.37, 0.42) | 0.39 (−0.51, 1.29) | 1.04 (0.14, 1.94) | −0.64 (−1.54, 0.26) | −0.08 (−0.98, 0.82) | 0.41 (−0.49, 1.31) | −0.69 (−1.59, 0.21) |
Note. CI = 95% Confidence interval.
p < .05,
p < .01,
p < .001.
Table 3.
Cohen’s d Within and Between-Group Effect Sizes of Differences in Average Values
| Within-Group Effect Sizes | Between-Group Effect Sizes | ||||||||
|---|---|---|---|---|---|---|---|---|---|
|
|
|
||||||||
| DBT + DBT PE | DBT + DBT PE vs. DBT-No DBT PE | DBT + DBT PE vs. DBT | |||||||
|
|
|
|
|||||||
| Stage 1 vs. 2 |
Stage 2 vs. 3 |
Stage 1 vs. 3 |
Stage 1 vs. Leg 1 |
Stage 2 vs. Leg 2 |
Stage 3 vs. Leg 3 |
Stage 1 vs. Leg 1 |
Stage 2 vs. Leg 2 |
Stage 3 vs. Leg 3 |
|
|
|
|
|
|
|
|
|
|
|
|
| d (CI) | d (CI) | d (CI) | d (CI) | d (CI) | d (CI) | d (CI) | d (CI) | d (CI) | |
| PTSD severity | 0.08 (−0.82, 0.98) | 1.72*** (0.82, 2.62) | 1.37** (0.47, 2.27) | 0.05 (−0.59, 0.69) | −0.10 (−0.74, 0.54) | 0.59 (−0.04, 1.23) | 0.07 (−0.56, 0.71) | 0.30 (−0.34, 0.94) | 0.50 (−0.14, 1.13) |
| BPD severity | 0.28 (−0.62, 1.18) | 0.69 (−0.21, 1.59) | 0.74 (−0.16, 1.64) | −0.25 (−0.88, 0.39) | 0.57 (−0.07, 1.21) | 0.61 (−0.03, 1.25) | 0.29 (−0.35, 0.93) | 0.46 (−0.18, 1.09) | 0.52 (−0.11, 1.16) |
| Global well-being | −0.69 (−1.59, 0.21) | 0.11 (−0.79, 1.01) | −0.50 (−1.41, 0.40) | −0.03 (−0.67, 0.60) | −0.88** (−1.51, −0.24) | −0.95** (−1.59, −0.31) | 0.06 (−0.58, 0.69) | −0.56 (−1.20, 0.08) | −0.92** (−1.56, −0.28) |
| State dissociation | −0.71 (−1.61, 0.19) | 0.70 (−0.20, 1.60) | 0.04 (−0.86, 0.94) | 0.09 (−0.54, 0.73) | 0.07 (−0.56, 0.71) | 0.29 (−0.35, 0.93) | 0.24 (−0.39, 0.88) | 0.32 (−0.32, 0.95) | 0.50 (−0.14, 1.13) |
| Urges to suicide | −0.20 (−1.10, 0.70) | 0.17 (−0.73, 1.06) | −0.02 (−0.92, 0.88) | −0.03 (−0.66, 0.61) | 0.01 (−0.63, 0.65) | −0.03 (−0.67, 0.60) | 0.22 (−0.41, 0.86) | 0.43 (−0.20, 1.07) | 0.36 (−0.28, 0.99) |
| Urges to self-harm | −0.10 (−1.00, 0.80) | 0.79 (−0.11, 1.69) | 0.51 (−0.38, 1.41) | −0.29 (−0.93, 0.35) | −0.18 (−0.82, 0.46) | −0.04 (−0.68, 0.60) | 0.03 (−0.60, 0.67) | 0.40 (−0.23, 1.04) | 0.37 (−0.27, 1.00) |
| Urges to use substances | −0.54 (−1.44, 0.36) | −0.23 (−0.67, 1.13) | −0.20 (−1.10, 0.70) | 0.35 (−0.29, 1.00) | 0.004 (−0.63, 0.64) | 0.18 (−0.45, 0.82) | 0.19 (−0.44, 0.83) | 0.36 (−0.27, 1.00) | 0.27 (−0.37, 0.90) |
| Urges to quit therapy | −0.58 (−1.48, 0.32) | 0.72 (−0.18, 1.62) | 0.11 (−0.79, 1.01) | 0.55 (−0.09, 1.19) | 0.58 (−0.06, 1.21) | 0.71* (0.07, 1.34) | 0.14 (−0.49, 0.78) | 0.41 (−0.22, 1.05) | 0.32 (−0.32, 0.96) |
Note. CI = 95% Confidence interval. Effect sizes with an asterisk represent statistically significant differences in the multi-phase mixed effect models. Positive within-group effect sizes indicate decreases in scores in the later stage of treatment.
p < .05,
p < .01,
p < .001.
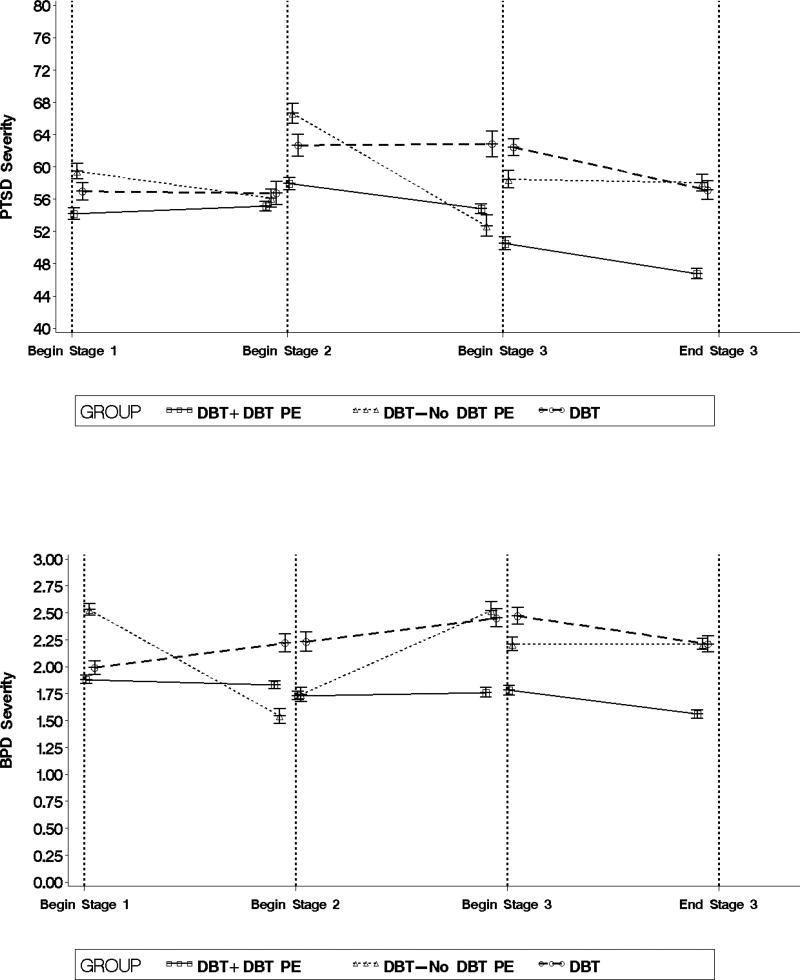
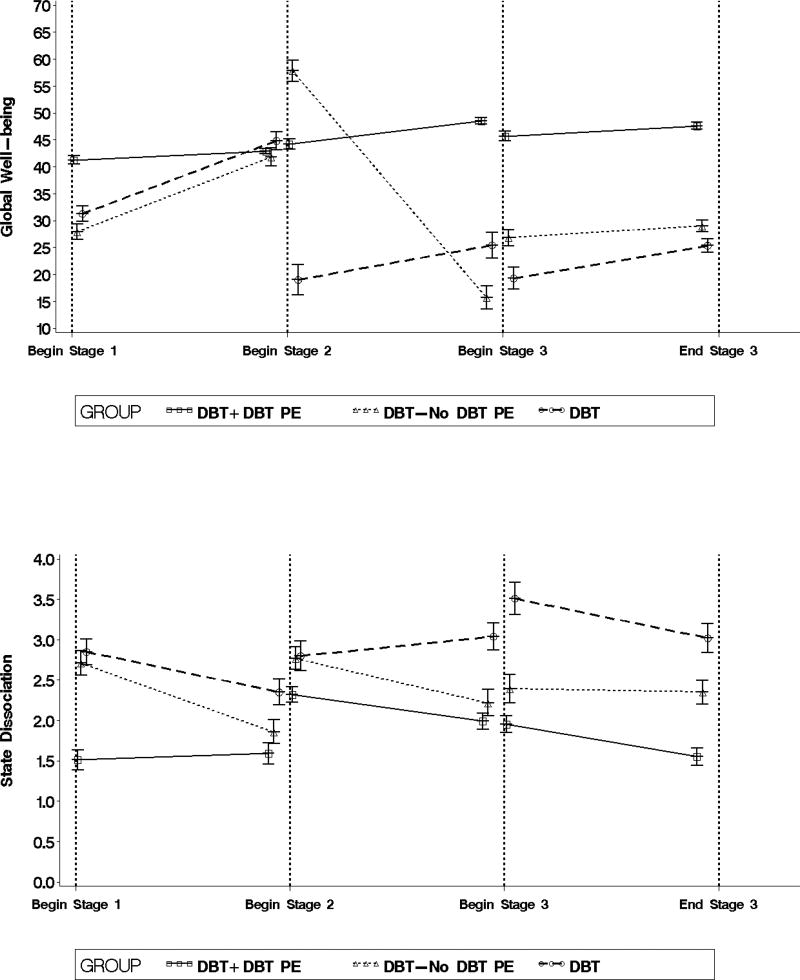
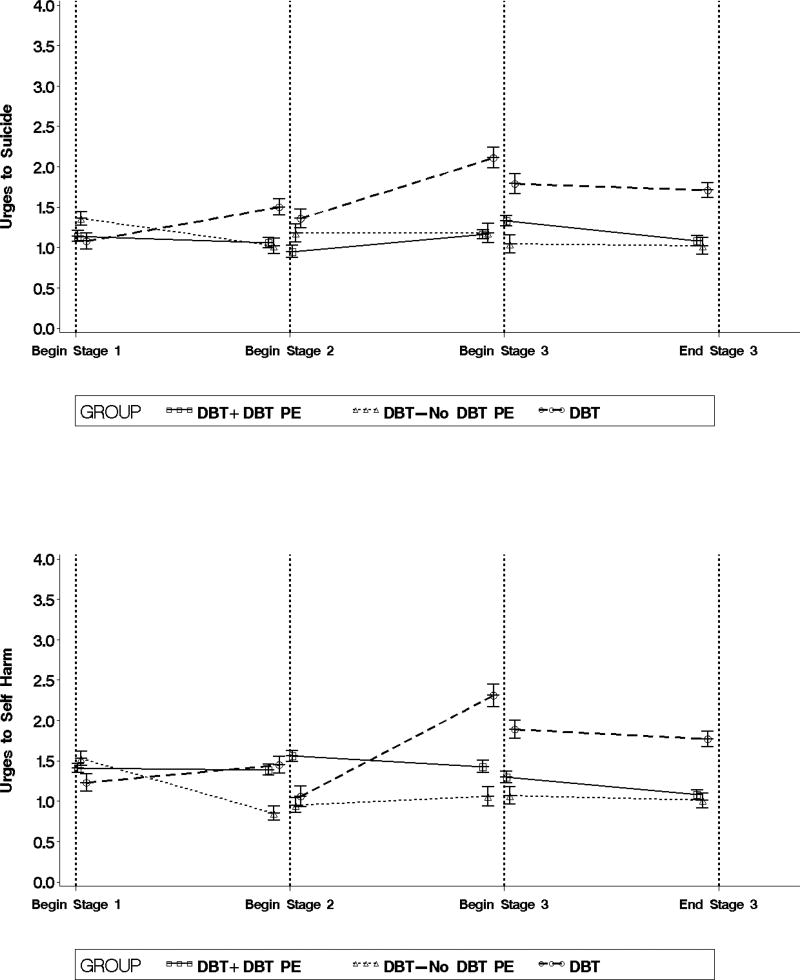
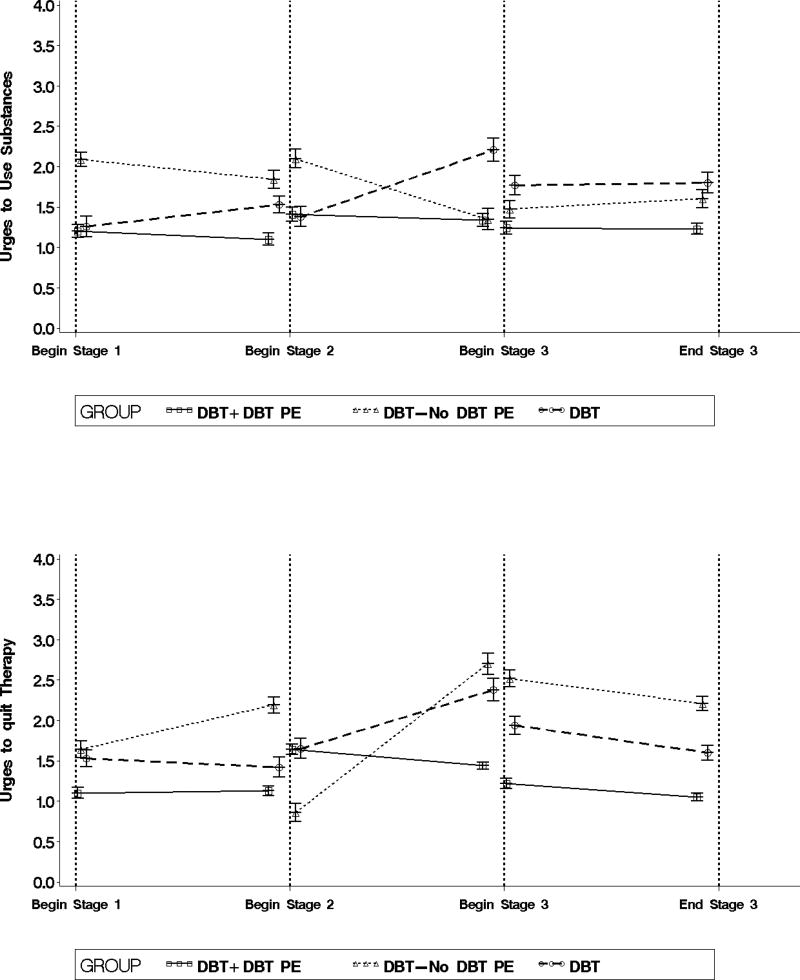
Figure 1.
Average start and end values for each outcome by stage of treatment and treatment group.
PTSD severity
During Stage 1, PTSD severity did not significantly change (F (1, 537) = 0.52, p = .47, d = 0.33). In contrast, there were large and significant reductions in PTSD severity during Stage 2 (F (1, 537) = 4.59, p < .04, d = −0.98) and Stage 3 (F (1, 537) = 6.07, p < .02, d = −1.13). In addition, average PTSD severity was significantly lower in Stage 3 compared to Stage 1 (t (537) = 2.99, p < .01, d = 1.37) and Stage 2 (t (537) = 3.74, p < .001, d = 1.72).
BPD severity
BPD severity did not significantly change during Stage 1 (F (1, 551) = 0.34, p = .56, d = −0.27) or Stage 2 (F (1, 551) = 0.11, p = .74, d = 0.15). A large and significant reduction in BPD severity occurred during Stage 3 (F (1, 551) = 5.38, p < .03, d = −1.14). There were medium but non-significant effects indicating average BPD severity was lower in Stage 3 than in Stage 1 (t (551) = 1.62, p = .11, d = 0.74) and Stage 2 (t (551) = 1.51, p = .13, d = 0.69).
Global well-being
Global well-being did not significantly change during Stage 1 (F (1, 551) = 0.45, p = .50, d = 0.31) or Stage 3 (F (1, 551) = 0.59, p = .44, d = 0.35). There was a medium but non-significant improvement in global well-being during Stage 2 (F (1, 551) = 1.78, p = .18, d = 0.61). Average global well-being was moderately but non-significantly lower in Stage 1 compared to Stage 2 (t (551) = −1.50, p =.13, d = −0.69) and Stage 3 (t (551) = −1.10, p =.27, d = −0.50).
State dissociation
During Stage 1, state dissociation did not significantly change (F (1, 961) = 0.19, p = .66, d = 0.20). There was a large but non-significant reduction in state dissociation during Stage 2 (F (1, 961) = 3.12, p = .08, d = −0.81) and these improvements became significant in Stage 3 (F (1, 961) = 4.04, p < .05, d = −0.92). Average state dissociation was moderately but non-significantly higher during Stage 2 than Stage 1 (t (961) = −1.55, p = .12, d = −0.71) and Stage 3 (t (961) = 1.53, p = .13, d = 0.70).
Urges to commit suicide
Urges to commit suicide did not significantly change during Stage 1 (F (1, 976) = 0.26, p = .61, d = −0.24), showed a medium, non-significant increase during Stage 2 (F (1, 976) = 1.63, p = .20, d = 0.59), and a medium, non-significant decrease during Stage 3 (F (1, 976) = 2.65, p = .10, d = −0.75). Average urges to commit suicide did not significantly differ between any of the stages of DBT + DBT PE and all effect sizes were small.
Urges to self-harm
Urges to self-harm did not significantly change during Stage 1 (F (1, 977) = 0.03, p = .87, d = −0.07) or Stage 2 (F (1, 977) = 0.93, p = .34, d = −0.44). There was a medium but non-significant reduction in urges to self-harm during Stage 3 (F (1, 977) = 2.62, p = .11, d = −0.74). Average urges to self-harm were moderately, but non-significantly lower in Stage 3 than in Stage 1 (t (977) = 1.12, p = .26, d = 0.51) and Stage 2 (t (977) = 1.73, p = .08, d = 0.79).
Urges to use substances
Urges to use substances did not significantly change during any stage of treatment: Stage 1 (F (1, 977) = 0.63, p = .43, d = −0.36), Stage 2 (F (1, 977) = 0.25, p = .61, d= −0.23), and Stage 3 (F (1, 977) = 0.00, p = .97, d = −0.02). Average urges to use substances were moderately but non-significantly higher during Stage 2 than Stage 1 (t (977) = −1.17, p = .24, d = −0.54).
Urges to quit therapy
Urges to quit therapy did not significantly change during Stage 1 (F (1, 977) = 0.04, p = .84, d = 0.09) or Stage 3 (F (1, 977) = 1.07, p = .30, d = −0.47). There was a medium but non-significant decrease in urges to quit therapy during Stage 2 (F (1, 977) = 1.23, p = .27, d= −0.51). Average urges to quit therapy were moderately but non-significantly higher in Stage 2 compared to Stage 1 (t (977) = −1.26, p = .21, d = −0.58) and Stage 3 (t (977) = 1.56, p = .12, p = 0.72).
Hypothesis 2: Between-Group Comparisons
We hypothesized that improvements in all outcomes would be greater by Stage 3 of DBT + DBT PE compared to time-matched legs of DBT and DBT-No DBT PE (Hypothesis 2). The results of the between-group contrasts and effect sizes from the MPMEM analyses are reported in Table 3. Figure 1 displays the average start and end values for each stage/leg of treatment by treatment group.
PTSD severity
Between-group comparisons yielded medium, trend-level effects indicating average PTSD severity was moderately lower in Stage 3 of DBT + DBT PE than in Leg 3 of DBT-No DBT PE (t (537) = 1.83, p = .07, d = 0.59) and Leg 3 of DBT (t (537) = 1.54, p = .12, d = 0.50).
BPD severity
Between-group comparisons yielded medium, trend-level effects indicating average BPD severity was moderately lower in Stage 3 of DBT + DBT PE than in Leg 3 of DBT-No DBT PE (t (551) = 1.88, p = .06, d = 0.61) and Leg 3 of DBT (t (551) = 1.62, p = .11, d = 0.52). In addition, a medium, trend-level effect indicated average BPD severity was moderately lower in Stage 2 of DBT + DBT PE than in Leg 2 of DBT-No DBT PE (t (551) = 1.76, p = .08, d = 0.57).
Global well-being
Between-group comparisons indicated average global well-being was significantly higher in Stage 2 of DBT + DBT PE than in Leg 2 of DBT-No DBT PE (t (551) = −2.70, p < .01, d = −0.88). In addition, average global well-being was significantly higher in Stage 3 of DBT + DBT PE than in Leg 3 of DBT-No DBT PE (t (551) = −2.93, p < .01, d = −0.95) and Leg 3 of DBT (t (551) = −2.84, p < .01, d = −0.92).
State dissociation
Between-group comparisons indicated that average state dissociation was moderately but non-significantly lower in Stage 3 of DBT + DBT PE than in Leg 3 of DBT (t (978) = 1.30, p = .19, d = 0.50). All other between-group differences in average state dissociation were small and non-significant.
Urges to engage in problem behaviors
Between-group differences in average urges to commit suicide, self-harm, and use substances were small and non-significant. Average urges to quit therapy were significantly lower in Stage 3 of DBT + DBT PE than in Leg 3 of DBT-No DBT PE (t (977) = 2.18, p < .03, d = 0.71). In addition, average urges to quit therapy were moderately but non-significantly lower in Stages 1 and 2 of DBT + DBT PE compared to Legs 1 and 2 of DBT-No DBT PE (t (977) = 1.70, p = .09, d = 0.55 and t (977) = 1.78, p = .07, d= 0.58, respectively).
Discussion
The present study evaluated the timing and course of change in multiple areas of functioning across the three stages of DBT + DBT PE, an integrated treatment designed to flexibly target the full range of problems exhibited by suicidal and self-injuring individuals with BPD and PTSD. These changes were compared to those found in DBT when PTSD was not directly or formally targeted either because clients were randomized to receive DBT alone or they did not initiate the DBT PE protocol during DBT.
Our first hypothesis predicted that the pattern of change during DBT + DBT PE would be consistent with the primary targets of each stage of treatment. Contrary to this hypothesis, there were no significant changes in urges to commit suicide or self-harm during Stage 1 despite the focus of treatment being on reducing life-threatening behaviors. This is likely due to the fact that urges and behaviors are quite different phenomena. Whereas large and significant reductions in suicide attempts and NSSI acts occurred during the initial months of DBT + DBT PE (Harned et al., 2012; Harned et al., 2014), the present results suggest that urges to engage in these behaviors are likely to persist beyond Stage 1. As hypothesized, PTSD did not change until Stage 2 when it was directly targeted via the DBT PE protocol, which led to a large and significant improvement in PTSD severity. This is consistent with research on other stage-based PTSD treatments that begin with a skills training phase prior to trauma-focused treatment (e.g., Cloitre, Koenen, Cohen & Han, 2002). In Stage 3, PTSD severity continued to significantly improve and reached an average level that was significantly lower than both Stages 1 and 2. In addition, there were significant reductions in BPD severity and state dissociation during Stage 3, suggesting that improvements in these areas may be contingent on the successful treatment of PTSD.
Our first hypothesis also predicted that, in contrast to common clinician concerns (e.g., Becker et al., 2004; van Minnen et al., 2010), there would be no evidence of significant worsening in any area of functioning during the trauma-focused portion of the treatment (Stage 2). This hypothesis was supported; namely, during Stage 2 no comorbid problems significantly increased and average levels of these problems were low and did not significantly differ from those reported in Stage 1. However, several clinically relevant trends emerged from the effect size data, suggesting there were medium increases in state dissociation and urges to engage in some problem behaviors (suicide, substance use, and quitting therapy) at the beginning of Stage 2 followed by medium to large decreases in these problems during Stages 2 and/or 3. This is consistent with prior research indicating a quadratic pattern of change in PTSD during trauma-focused treatment (Nishith, Resick & Griffin, 2002), and suggests that comorbid problems that function to cope with PTSD and painful emotions may show similar moderate increases at the onset of the DBT PE protocol. Clinically, this highlights the importance of ensuring that both clients and clinicians have the skills necessary to manage moderate increases in state dissociation and urges to engage in problem behaviors that may occur at the beginning of the DBT PE protocol, while also stressing that any increases can be expected to improve if the treatment is continued. Importantly, the primary outcome studies found no evidence of worsening in suicide attempts, treatment dropout, or trait dissociation during DBT + DBT PE (Harned et al., 2012; Harned et al., 2014), suggesting that clients and clinicians were well-equipped to manage any temporary increases in urges and state-levels of these problems that may have occurred.
Our second hypothesis was that the changes in DBT + DBT PE would be larger than those found during DBT when it is delivered without the DBT PE protocol. Comparisons between each stage of DBT + DBT PE and time-matched legs of DBT and DBT-No DBT PE found that outcomes were highly similar across treatments during Stage 1 and differences only emerged in Stages 2 and 3. Specifically, clients in DBT + DBT PE reported significantly higher global well-being than those in DBT-No DBT PE in Stages 2 and 3 and than those in DBT in Stage 3. In addition, medium but non-significant effects indicated lower PTSD and BPD severity in Stages 2 and/or 3 of DBT + DBT PE compared to DBT and DBT-No DBT PE, and lower state dissociation in Stage 3 compared to DBT. These findings suggest that the addition of the DBT PE protocol to DBT may improve outcomes in PTSD and other comorbid problems, and the timing of these differences suggests that changes in comorbid problems may be due to directly targeting PTSD. Of note, there was no evidence of significant worsening in any outcome in DBT + DBT PE compared to either DBT only group.
This study had several strengths, most notably the evaluation of a novel integrated treatment for PTSD in a sample with multiple, serious comorbid problems. The main limitation of the study was the relatively small sample size. Given the low power, we also evaluated effect sizes and observed medium to large effects for many measures that did not have sufficient power to produce statistically significant effects. Additionally, we recognize the potential for an increase in Type I error due to the multiple comparisons that were conducted. However, given the small sample size, the study was intended to be exploratory and to detect any evidence of differences within and between groups. Future fully powered studies are needed to confirm these results when adjusting for multiple comparisons. Further, the groups were only partially randomly assigned, which contributed to a significantly higher rate of treatment dropout in the DBT-No DBT PE group as this group included clients originally assigned to DBT + DBT PE who never started the DBT PE protocol (primarily due to dropping out of treatment during Stage 1). However, pattern mixture models evaluating the impact of missing data due to treatment dropout did not find any significant effects. Also, single item measures were used to assess urges to engage in problem behaviors and global well-being, and these findings should be interpreted with caution. Finally, weekly measurements of actual problem behaviors were not obtained and would be useful to consider in future research.
Overall, the present findings indicate that integrated, stage-based treatments such as DBT + DBT PE provide a safe and effective approach for targeting PTSD and multiple serious comorbid problems in one comprehensive treatment. The pattern of change across stages of treatment suggests that PTSD improves only when it is directly targeted, whereas comorbid problems that may be maintained or exacerbated by PTSD improve only after PTSD has been treated. Taken together, these findings highlight the importance of providing effective PTSD treatment to this highly comorbid and severely impaired client population.
Acknowledgments
This work was supported by grant R34MH082143 from the National Institute of Mental Health to the first author. We would like to thank the clients, therapists, assessors, and staff at the Behavioral Research and Therapy Clinics for their contributions to this research. Dr. Harned is a trainer and consultant for Behavioral Tech, LLC.
Footnotes
Portions of this data were presented at the 2012 Annual Convention of the Association for Behavioral and Cognitive Therapies, National Harbor, MD.
References
- Barnow S, Limberg A, Stopsack M, Spitzer C, Grabe HJ, Freyberger HJ, Hamm A. Dissociation and emotion regulation in borderline personality disorder. Psychological Medicine. 2012;42:783–794. doi: 10.1017/S0033291711001917. [DOI] [PubMed] [Google Scholar]
- Becker CB, Zayfert C, Anderson E. A survey of psychologists’ attitudes towards and utilization of exposure therapy for PTSD. Behaviour Research and Therapy. 2004;42:277–292. doi: 10.1016/S0005-7967(03)00138-4. [DOI] [PubMed] [Google Scholar]
- Bohus M, Limberger MF, Frank U, Chapman AL, Kühler T, Stieglitz RD. Psychometric properties of the borderline symptom list (BSL) Psychopathology. 2007;40:126–132. doi: 10.1159/000098493. [DOI] [PubMed] [Google Scholar]
- Cloitre M, Koenen KC, Cohen LR, Han H. Skills training in affective and interpersonal regulation followed by exposure: A phase-based treatment for PTSD related to childhood abuse. Journal of Consulting and Clinical Psychology. 2002;70:1067–1074. doi: 10.1037//0022-006x.70.5.1067. [DOI] [PubMed] [Google Scholar]
- Cohen J. Statistical power analysis for the behavioral sciences. 2. Hillsdale, NJ: Lawrence Erlbaum Associates; 1988. [Google Scholar]
- Cudeck R, Klebe KJ. Multiphase mixed-effects models for repeated measures data. Psychological Methods. 2002;7:41–63. doi: 10.1037/1082-989x.7.1.41. [DOI] [PubMed] [Google Scholar]
- Feingold A. Effect sizes for growth-modeling analysis for controlled clinical trials in the same metric as for classical analysis. Psychological Methods. 2009;14:43–53. doi: 10.1037/a0014699. [DOI] [PMC free article] [PubMed] [Google Scholar]
- First MB, Spitzer RL, Gibbon M, Williams JBW. Structured clinical interview for axis I DSM-IV disorders - patient edition (SCID-I/P) New York: Biometrics Research Department, NY State Psychiatric Institute; 1995. [Google Scholar]
- Foa EB, Hembree EA, Cahill SP, Rauch SA, Riggs DS, Feeny NC, Yadin E. Randomized trial of prolonged exposure for posttraumatic stress disorder with and without cognitive restructuring: outcome at academic and community clinics. Journal of Consulting and Clinical Psychology. 2005;73:953–964. doi: 10.1037/0022-006X.73.5.953. [DOI] [PubMed] [Google Scholar]
- Foa E, Hembree E, Rothbaum BO. Prolonged exposure therapy for PTSD: Emotional processing of traumatic experiences therapist guide. New York: Oxford Press; 2007. [Google Scholar]
- Foa EB, Riggs DS, Dancu CV, Rothbaum BO. Reliability and validity of a brief instrument for assessing post-traumatic stress disorder. Journal of Traumatic Stress. 1993;6:459–473. [Google Scholar]
- Grant BF, Chou SP, Goldstein RB, Huang B, Stinson FS, Saha TD, Ruan WJ. Prevalence, correlates, disability, and comorbidity of DSM-IV borderline personality disorder: Results from the Wave 2 National Epidemiologic Survey on Alcohol and Related Conditions. Journal of Clinical Psychiatry. 2008;69:533–545. doi: 10.4088/jcp.v69n0404. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Harned MS. Treatment of posttraumatic stress disorder with comorbid borderline personality disorder. In: McKay D, Storch E, editors. Handbook of Treating Variants and Complications in Anxiety Disorders. New York, NY: Springer Press; 2013. pp. 203–221. [Google Scholar]
- Harned MS, Korslund KE, Foa EB, Linehan MM. Treating PTSD in suicidal and self-injuring women with borderline personality disorder: Development and preliminary evaluation of a Dialectical Behavior Therapy Prolonged Exposure Protocol. Behaviour Research and Therapy. 2012;50:381–386. doi: 10.1016/j.brat.2012.02.011. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Harned MS, Korslund KE, Linehan MM. A pilot randomized controlled trial of Dialectical Behavior Therapy with and without the Dialectical Behavior Therapy Prolonged Exposure protocol for suicidal and self-injuring women with borderline personality disorder and PTSD. Behaviour Research and Therapy. 2014;55:7–17. doi: 10.1016/j.brat.2014.01.008. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Harned MS, Rizvi SL, Linehan MM. Impact of co-occurring posttraumatic stress disorder on suicidal women with borderline personality disorder. American Journal of Psychiatry. 2010;167:1210–1217. doi: 10.1176/appi.ajp.2010.09081213. [DOI] [PubMed] [Google Scholar]
- Hedeker D, Gibbons RD. Application of random-effects pattern-mixture models for missing data in longitudinal studies. Psychological Methods. 1997;2:64–78. [Google Scholar]
- Institute of Medicine. Small clinical trials: Issues and challenges. Washington, D.C: National Academy Press; 2001. [Google Scholar]
- Leeies M, Pagura J, Sareen J, Bolton JM. The use of alcohol and drugs to self-medicate symptoms of posttraumatic stress disorder. Depression and Anxiety. 2010;27:731–736. doi: 10.1002/da.20677. [DOI] [PubMed] [Google Scholar]
- Linehan M. Cognitive-behavioral treatment of borderline personality disorder. New York: Guilford Press; 1993. [Google Scholar]
- Linehan MM, Comtois KA, Brown MZ, Heard HL, Wagner A. Suicide Attempt Self-Injury Interview (SASII): Development, reliability, and validity of a scale to assess suicide attempts and intentional self-injury. Psychological Assessment. 2006;18:303–312. doi: 10.1037/1040-3590.18.3.303. [DOI] [PubMed] [Google Scholar]
- Loranger AW. International Personality Disorder Examination (IPDE) Manual. White Plains, NY: Cornell Medical Center; 1995. [Google Scholar]
- Maas CJM, Hox JJ. Robustness issues in multilevel regression analysis. Statistica Neerlandica. 2004;58:127–137. [Google Scholar]
- Moser EB, Macchiavelli RE. Methods for spatial analysis. In: Singh VP, Fiorentino M, editors. Geographical Information Systems in Hydrology. Vol. 26. The Netherlands: Kluwer Academic Publishers; 1996. pp. 91–113. [Google Scholar]
- Najavits LM, Ryngala D, Back SE, Bolton E, Mueser KT, Brady KT. Treatment for PTSD and comorbid disorders. In: Foa EB, Keane TM, Friedman MJ, Cohen JA, editors. Effective treatments for PTSD: Practice guidelines from the International Society for Traumatic Stress Studies. 2. New York, NY: Guilford Press; 2009. pp. 508–535. [Google Scholar]
- Nishith P, Resick PA, Griffin MG. Pattern of change in prolonged exposure and cognitive-processing therapy for female rape victims with posttraumatic stress disorder. Journal of Consulting and Clinical Psychology. 2002;70:880–886. doi: 10.1037//0022-006x.70.4.880. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Pietrzak RH, Goldstein RB, Southwick SM, Grant BF. Prevalence and Axis I comorbidity of full and partial posttraumatic stress disorder in the United States: Results from Wave 2 of the National Epidemiologic Survey on Alcohol and Related Conditions. Journal of Anxiety Disorders. 2011;25:456–465. doi: 10.1016/j.janxdis.2010.11.010. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Pagura J, Stein MB, Bolton LM, Cox BJ, Grant B, Sareen J. Comorbidity of borderline personality disorder and posttraumatic stress disorder in the U.S. population. Journal of Psychiatric Research. 2010;44:1190–1198. doi: 10.1016/j.jpsychires.2010.04.016. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Rizvi SL, Harned MS. Increasing treatment efficiency and effectiveness: Rethinking approaches to assessing and treating comorbid disorders. Clinical Psychology: Science and Practice. 2013;20:285–290. [Google Scholar]
- Ronconi JM, Shiner B, Watts BV. Inclusion and exclusion criteria in randomized controlled trials of psychotherapy for PTSD. Journal of Psychiatric Practice. 2014;20:25–37. doi: 10.1097/01.pra.0000442936.23457.5b. [DOI] [PubMed] [Google Scholar]
- Rüsch N, Corrigan PW, Bohus M, Kuhler T, Jacob GA, Lieb K. The impact of posttraumatic stress disorder on dysfunctional implicit and explicit emotions among women with borderline personality disorder. J Nerv Ment Dis 2007. 195:537–539. doi: 10.1097/NMD.0b013e318064e7fc. [DOI] [PubMed] [Google Scholar]
- Sar V, Akyuz G, Kugu N, Ozturk E, Ertem-Vehid H. Axis I dissociative disorder comorbidity in borderline personality disorder and reports of childhood trauma. Journal of Clinical Psychiatry. 2006;67(10):1583–1590. doi: 10.4088/jcp.v67n1014. [DOI] [PubMed] [Google Scholar]
- Stiglmayr C, Schmahl C, Bremner JD, Bohus M, Ebner-Priemer U. Development and psychometric characteristics of the DSS-4 as a short instrument to assess dissociative experience during neuropsychological experiments. Psychopathology. 2009;42:370–374. doi: 10.1159/000236908. [DOI] [PubMed] [Google Scholar]
- van Minnen A, Hendriks L, Olff M. When do trauma experts choose exposure therapy for PTSD patients? A controlled study of therapists and patient factors. Behaviour Research and Therapy. 2010;48:312–320. doi: 10.1016/j.brat.2009.12.003. [DOI] [PubMed] [Google Scholar]
- van Minnen A, Zoellner LA, Harned MS, Mills K. Changes in comorbid conditions after prolonged exposure for PTSD: A literature review. Current Psychiatry Reports. 2015;17:1–16. doi: 10.1007/s11920-015-0549-1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Wackerly D, Mendenhall W, Scheaffer RL. Mathematical Statistics with Applications. 7. Belmont, CA: Thomson Brooks/Cole; 2008. [Google Scholar]
- Weathers FW, Litz BT, Herman DS, Huska JA, Keane TM. Annual Convention of the International Society for Traumatic Stress Studies. San Antonio: International Society for Traumatic Stress Studies; 1993. Oct, The PTSD Checklist (PCL): Reliability, validity, and diagnostic utility. [Google Scholar]
- Wedig MM, Silverman MH, Frankenburg FR, Reich DB, Fitzmaurice G, Zanarini MC. Predictors of suicide attempts in patients with borderline personality disorder over 16 years of prospective follow-up. Psychological medicine. 2012;42:2395–2404. doi: 10.1017/S0033291712000517. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Wilkins KC, Lang AJ, Norman SB. Synthesis of the psychometric properties of the PTSD checklist (PCL) military, civilian, and specific versions. Depression and Anxiety. 2012;28:596–606. doi: 10.1002/da.20837. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Zanarini MC, Frankenburg FR, Hennen J, Reich DB, Silk KR. Prediction of the 10-year course of borderline personality disorder. American Journal of Psychiatry. 2006;163:827–832. doi: 10.1176/ajp.2006.163.5.827. [DOI] [PubMed] [Google Scholar]
- Zanarini MC, Laudate CS, Frankenburg FR, Reich DB, Fitzmaurice G. Predictors of self-mutilation in patients with borderline personality disorder: A 10-year follow-up study. Journal of Psychiatric Research. 2011;45:823–828. doi: 10.1016/j.jpsychires.2010.10.015. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Zanarini MC, Ruser T, Frankenburg FR, Hennen J. The dissociative experiences of borderline patients. Comprehensive Psychiatry. 2000;41:223–227. doi: 10.1016/S0010-440X(00)90051-8. [DOI] [PubMed] [Google Scholar]