Abstract
Background
Few studies have longitudinally explored the experience and needs of family caregivers of ICU survivors after patients’ home discharge.
Methods
Qualitative content analysis of interviews drawn from a parent study that followed family caregivers of adults ICU survivors for 4 months post-ICU discharge.
Results
Family caregivers (n=20, all white, 80% woman) viewed home discharge as positive progress, but reported having insufficient time to transition from family visitor to the active caregiver role. Caregivers expressed feelings of relief during the steady recovery of family members’ physical and cognitive function. However, the slow pace of improvement conflicted with their expectations. Even after patients achieved independent physical function, emotional needs persisted and these issues contributed to caregivers’ anxiety, worry, and view that recovery was incomplete.
Conclusion
Family caregivers of ICU survivors need information and skills to help managing patients’ care needs, pacing expectations with actual patients’ progress, and caregivers’ health needs.
Keywords: Critical care, survivorship, family caregivers, adult, psychosocial, qualitative research
Introduction
Each year in the United States, more than 5 million individuals experience critical illness that results in admission to an intensive care unit (ICU).1 Because of improved therapeutics, the majority of critically ill patients survive and many are ultimately discharged home.2 For patients and family caregivers, home discharge represents positive progress, but also a new challenge. Support from professional care providers is highly variable after home discharge3 and family caregivers often assume responsibility for needed support.
Improving understanding of—and providing support to—family caregivers of the critically ill has received growing attention. Researchers have begun to examine family caregivers’ physical and psychological needs across the continuum from ICU admission.4,5 to recovery.6–15 Psychosocial symptoms are most prevalent during the acute phase of patients’ illness. According to studies with a one-year follow-up, caregivers of ICU survivors experience depressive symptoms comparable to rates reported by caregivers of patients with dementia.16–18 High levels of anxiety are correlated with high levels of caregiver strain in the post-discharge period.19 Prevalence of Post-traumatic Stress increases over time after ICU discharge.19–21 In a study by Fumis et al. that followed dyads of family caregivers and ICU survivors, depression, anxiety and PTSD symptoms in family caregivers persisted for 3 months post-discharge and were worse than the symptoms reported in ICU survivors.22
To date, a limited number of qualitative studies interviewed patients, family members or both to describe their response to long-term recovery following critical illness.23–25 Cox et al. interviewed 24 family caregivers and 23 patients at varied time points after patients’ home discharge (from one to 12 months).19 These caregivers reported feeling distressed by patients’ fluctuating emotions and limited support during transition from hospital to home.23 In a study by Young et al., 20 family caregivers of ICU survivors and 15 family caregivers of elective cardiac surgery survivors were interviewed at 3 months after home discharge25 and concluded that family caregivers of ICU survivors were more troubled than caregivers of post-cardiac surgery patients because recovery was less predictable. In another longitudinal study, Czerwonka et al., interviewed 7 family caregivers and 5 patients at varied time points which range from 7 days to 24 months post ICU discharge.24 The study by Czerwonka et al.24 highlighted following three major points: (1) there is constant and evolving informational needs in this population across the timeline; (2) when informational needs are not met, transition from one care setting to another provokes anxiety and uncertainty in family caregivers; and (3) supporting survivors making transition from dependence to independence needs efforts and negotiation from both ICU survivors and family caregivers. In their findings, home discharge was described as a particularly challenging transition because supports from formal health service gradually decrease and family caregivers begin taking more responsibilities.
Despite importance of supporting needs of family caregivers at varied time points after patients’ home discharge, few studies have examined how caregivers’ needs and perceptions change over time following home discharge. The purpose of this study was to longitudinally describe the varying challenges and needs of family caregivers of ICU survivors related to patients’ home discharge.
Methods
This descriptive qualitative study involved a content analysis of semi-structured interview data drawn from a parent study that longitudinally examined stress responses in family caregivers of adult ICU patients from patients’ ICU hospitalization to 4 months post-ICU discharge26. Additional details of the parent study are available elsewhere.5,8–10,27,28 For this secondary analysis, we included a subsample of interviews with family caregivers who experienced home discharge of patients during 4 months follow-up period. The protocol was reviewed and approved by the Institutional Review Board. All family caregiver participants provided written informed consent.
In the parent study, family caregivers were recruited in the medical ICU of a tertiary university hospital in Western Pennsylvania and followed for 4 months after their respective patient was discharged from the ICU. All baseline interviews were taken place at the ICU. Interviews after ICU discharge were took place at various post-ICU settings (e.g., long-term acute care hospital) and patients’ home.
Sample
A family caregiver was defined as an individual who provided the majority of emotional, financial, and physical support to a given patient. Neither legal relation nor cohabitation with the patient was required for participation in the study. Eligibility criteria for caregivers were: (1) non-professional, non-paid caregiver; (2) 21years or age or older; (3) has reliable telephone access; (4) able to read and speak English. Eligibility criteria for patients were: (1) 21 years of age or older; (2) residing at home prior to ICU admission; (3) on mechanical ventilation for 4 or more consecutive days in a medical ICU; (4) not dependent on mechanical ventilation prior to this ICU admission. In this secondary analysis, we used data from 20 family caregivers (1) of patients who were discharged to home during 4 months follow-up period and (2) participated in qualitative interview.
Interviews and Data Collection
In the parent study, family caregivers were interviewed by one research team member (JC) at three time points: within 2 weeks, 2 months and 4 months post-ICU discharge. All family caregivers were interviewed face-to-face in places where patients are staying at each time point, except one interview that took place over the telephone. We used a semi-structured interview to ask about the general caregiving experience and its impact on the caregiver’s life and relationships with others at each corresponding time point. Each interview started with a question asking about family caregivers’ typical day at the time of interview followed by questions asking about caregiving experience and perceived challenges (e.g., “What has been the most difficult thing you have had to help with?”). All interviews were audiotaped for transcription prior to analysis.
Data Analysis
Content analysis was used to determine predominant concepts or text to identify recurring themes consistent with standard qualitative methods.29 Three research team members (JC, JAT, JHL) independently reviewed first one third of the interview texts. Each conducted line by line coding of their subset of transcripts and identified initial sets of codes for categories that described experiences conveyed by interviewees. The group then met to share and compare coding schemes and category labels using constant comparative analysis to organize the data. Each team member presented illustrative quotes from assigned transcripts, discussed defining properties of each category/theme, reviewed divergent ideas, and finalized themes via group collaboration. Final analysis was conducted independently using stepwise replication. Finally, all transcripts were reviewed to ensure dependability of the analysis.
The team established trustworthiness of these results using standard qualitative strategies.30 Credibility of the data was secured by prolonged engagement with informants. The group used reflexivity to decrease the likelihood of biased interpretation of the data based on preconceived ideas or experiences. Dependability was obtained by stepwise replication and by maintaining an audit trail. Confirmability was enhanced by using a team of three researchers rather than a single researcher.
Because family caregivers were interviewed at multiple time points following home discharge, emerging themes were organized along three sequences following home discharge: (1) within 2 weeks post– home discharge; (2) within 2 months post– home discharge; and (3) greater than 2 months post – home discharge. Descriptive results are reported with representative quotes.
Results
Sample Characteristics
In the parent study, we enrolled 47 patient-family caregiver dyads and completed baseline assessment during patients’ ICU hospitalization. Among them, 40 patients survived and were discharged from the ICU. Among those 40 ICU survivors, 26 were discharged to home within the 4-month follow-up period. In 26 family caregivers of these survivors, 20 participated in qualitative interview while 6 elected to skip the qualitative interview portion due to time constraints. Detailed information regarding recruitment and retention of sample was illustrated in Figure 1. Only one case was discharge directly from the ICU to home. Transitions to home from post-ICU care settings occurred at varying time points and along different trajectories. Sixty percent of the caregivers (n = 12) participated in interviews at more than two time points.
Figure 1.
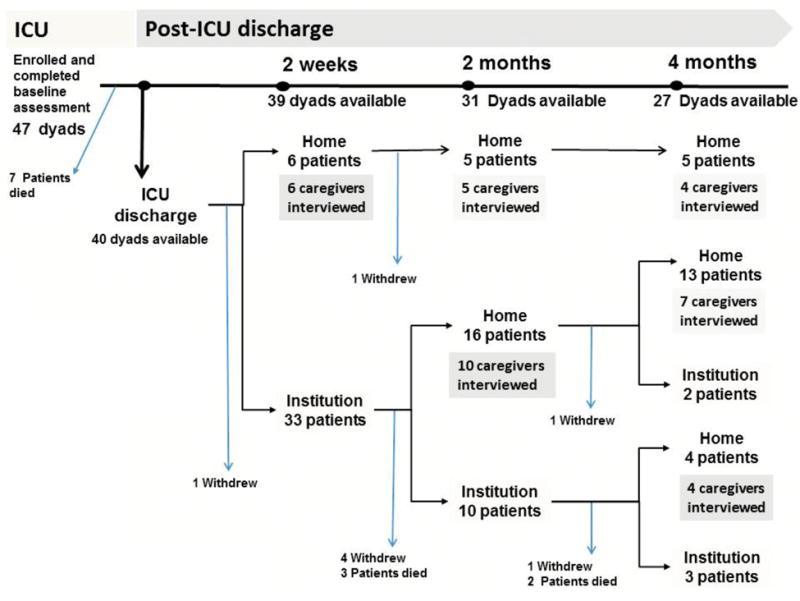
Sample enrollment, follow-up by home discharge status at each time point and number of caregivers interviewed at each time point.
Sample characteristics are summarized in Table 1. Family caregivers were predominantly woman (80%), middle-aged (52 ± 12 years), and the spouse (n = 12), parent (n = 5) or an adult child (n = 3) of the patient. Patients were predominantly men (65%), middle-aged (51 ± 19 years), and independent (75%) prior to their ICU admission. During their ICU stay (23 ± 10 days), patients were on mechanical ventilation for 20 ± 10 days.
Table 1.
Characteristics of Caregivers and Patients (n = 20)
| Characteristicsa | Mean ± SD (Range) | n (%) |
|---|---|---|
| Caregiver | ||
| Age (years) | 52 ± 12 (24–71) | |
| Sex: female | 16 (80) | |
| Race: white | 20 (100) | |
| Relationship to patient | ||
| Spouse or significant other | 13 (65) | |
| Adult child | 3 (15) | |
| Parent or sibling | 4 (20) | |
| Education (years) | 14 ± 3 (10–21) | |
| Working full or part time (yes) | 11 (55) | |
| Having religious belief or preference (yes) | 17 (85) | |
| Difficulty in paying for needs Extremely or somewhat difficult Not at all difficult |
9 (45) 11 (55) |
|
| Patient | ||
| Age (years) | 51 ± 19 (21–84) | |
| Sex: male | 13 (65) | |
| Race: white | 20 (100) | |
| Primary diagnosis | ||
| Respiratory | 14 (70) | |
| Gastrointestinal, Hepatic | 2 (10) | |
| Cardiovascular | 3 (15) | |
| Endocrine | 1 (5) | |
| Charlson Comorbidity Score | 3.2 ± 3.3 (0–10) | |
| APACHE II score | 18.8 ± 5.9 (12–36) | |
| ICU length of stay (days) | 23 ± 10 (5–39) | |
| Days on mechanical ventilation (days) | 20 ± 10 (4–38) | |
| Care needs prior to ICU admissionb No needs Moderate needs High needs |
15 (75) 2 (10) 3 (15) |
Continuous variables are presented as mean ± SD (range), and categorical variables are presented as number (%).
No needs = no impairment in ADL or IADL; Moderate needs = more than one impairment in IADL, but no impairment in ADL; High needs = at least one impairment in ADL
ICU = Intensive Care Unit; APACHE = Acute Physiology and Chronic Health Evaluation; ADL = Activities in Daily Living; IADL = Instrumental Activities in Daily Living
Main Themes
We identified 6 themes that described caregivers’ responses varying by timeline. Figure 2 depicts a summary of these themes by timeline. Family caregivers’ perceptions of “care needs of patients” changed over time. The remaining five themes illustrate emerging responses and needs of family caregivers and reflect assimilation to the caregiver role at home over time. The remaining themes include: (1) feeling overwhelmed and unprepared, (2) feeling relieved and hopeful in the beginning but uncertain over time, (3) staying vigilant, (4) pacing expectations and negotiation, and (5) negative impact on caregivers’ health. These family caregivers described their attention to the ICU survivor’s needs, commitment to care, changes in expectations, and returning to or recalibrating definitions of normal.
Figure 2.
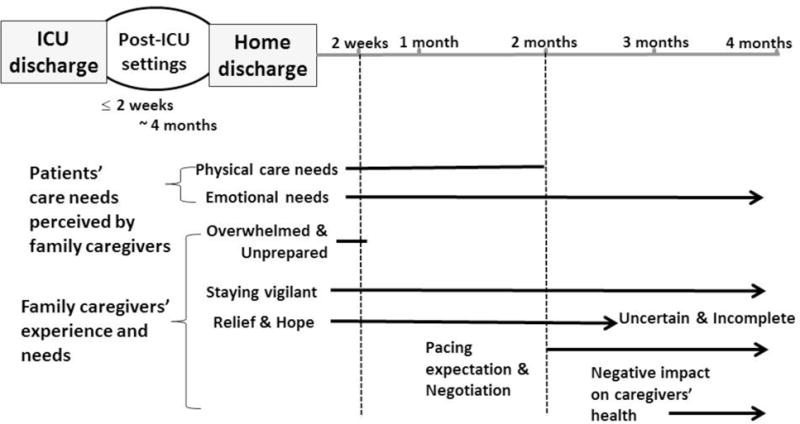
Conceptual summary of the main themes by timeline.
1. Patients’ care needs perceived by family caregivers
Patients’ care needs contain two dimensions, physical and emotional needs. For most of the family caregivers (10 of 20), providing hands-on care to assist in activities in daily living (e.g., personal care) was common, especially during the initial months after home discharge. Family caregivers described how they witnessed improvement in patients’ physical function over time.
“He can make it walking from our house to the car pretty well. And he’s pretty stable with that as long as he has his walker and everything.” (Interviewed between 2 weeks and 2 months after home discharge)
While physical care needs was a main concern in the earlier period, family caregivers no longer mentioned physical care needs in later period. However, emotional needs continued to be a challenge during the latter months. Many family caregivers (9 of 20) reported seeing patients being worried, anxious, and dealing with occasional outbursts, experiences they described as stressful.
“when he would be confused and he would like say some things, that were hurtful. He did not mean them hurtful to me.” (Interviewed < 2 weeks post-home discharge)
“They recommended that she see a therapist and we thought that was dumb. But now I wished she would have done it earlier…. I think she is even more depressed.” (Interviewed > 2 months after home discharge discharge)
Family caregivers perceived patients’ emotional distress was likely due to discordance between patients’ expectations and the actual pace of recovery. While they expressed empathy toward the patient, providing support was difficult at times for these family caregivers.
“The most difficult thing is seeing him not being able to deal with it. He just breaks down, and he just sits there and cries because he does not know what to do. And it is sort of hard to see him when I know he is such a strong guy.” (Interviewed between 2 weeks – 2 months post-home discharge)
2. Feeling overwhelmed and unprepared
Most family caregivers (11 of 20) mentioned their feelings when they either anticipated or underwent home discharge. In these family caregivers, patients were at post-ICU settings prior to home discharge (3 from long-term acute care hospital [LTACH], 3 from an inpatient rehabilitation unit, 3 from general hospital floor, and 2 from a skilled nursing facility). Despite variability in patients’ post-ICU courses prior to home discharge, almost universally, family caregivers described their reaction to patients’ home discharge as “feeling overwhelmed and unprepared.” Even in cases in which support and resources from other family members were available and identifiable, family caregivers expressed concerns that the majority of care would likely to be their responsibility. One spouse caregiver described her feeling:
“Coming home is a little scary to me. I worry about taking care of him … what it’s gonna involve. I have support from my children, but, of course, they have jobs.” (Interviewed < 2 weeks post-home discharge)
Physical environment in each household was highly variable, and family caregivers described the need to rearrange their home environment, for example, moving a patient’s bedroom to the first floor and preparing access to a bathroom, etc.
“I have to wait until he gets home to find out he can’t get somewhere safely or can’t fit through a doorway.” (Interviewed < 2 weeks post-home discharge)
One family caregiver shared his experience on the day of home discharge. In this case, the patient and family caregiver lived in a rural area located approximately 100 miles away from the major city hospital and accessibility to resources was relatively limited. Several critical home care therapies were not ready when they arrived, which created a stressful transition to home:
“I would have actually asked the doctors to give me a chance to get home and get things ready for her …. We got home that night and things that were supposed to be ready weren’t ready, that other people were supposed to have taken care of.” (Interviewed < 2 weeks post-home discharge)
3. Feeling relieved and hopeful in the beginning but uncertain over time
All family caregivers framed home discharge as positive progress. Family caregivers described how small steps of patient improvement enabled them to be hopeful. They expressed excitement and appreciation of patients’ recovery, regardless of the magnitude of improvement:
“It’s been hard to see him not as he was before. But then it’s not difficult because he’s getting better every day.” (Interviewed < 2 weeks post-home discharge)
However, for some family caregivers, as time progressed, hope was also accompanied by tension, worry, and uncertainty. In 12 family caregivers whose interviews took place 2 months or longer following home discharge, five observed that patients’ recovery was slower than expected and expressed concern that recovery seemed incomplete. Even as patients needed less physical assistance, family caregivers expressed worries about the lingering effects of critical illness. Family caregivers did not view symptoms, such as fatigue and pain as life threatening but considered them an indicator of incomplete recovery.
“No one seems to know how long his condition is going to be the way it is or if it is ever going to be any different, if he’s ever going to get better, or if he’s just going to stay the same.” (Interviewed > 2 months post-home discharge)
4. Staying vigilant
At all time points, all family caregivers embraced their personal responsibility for maintaining good care and vigilance in detecting changes that might warrant medical attention for patients. Even in cases which patients had progressed to independence in self-care and/or medication management, family caregivers were reluctant to leave their patients alone:
“My main job right now is to help him pace himself appropriately and to help him when he doesn’t.” (Interviewed between 2 weeks – 2 months post-home discharge)
Family caregivers expressed contrasting views toward sharing details of the ICU experience with the patient. One family caregiver chose not to share details of the ICU experience with the patient, as a means of protection:
“I don’t want to remind him how bad he was…. I find it hard for him to talk about it sometimes. I don’t know if it makes things worse when we talk about it because it reminds him of how weak he was.” (Interviewed between > 2 months post-home discharge)
In contrast, other caregivers described sharing details was difficult but ultimately helpful:
“That was probably the hardest thing for me though; just explaining to her like having tubes down her throat, and being in a coma for like three weeks. But, to be honest, I was surprised how much she wanted to know.” (Interviewed between > 2 months post-home discharge)
5. Pacing expectation and negotiation
Despite descriptions of improvement in patients’ ability to handle daily activities over time by their family caregivers, only five patients achieved pre-critical illness level of function and routine at 4 months post-ICU discharge (e.g., return to work full time, live independently in his/her residence). Remaining patients had to modify their routines (e.g., taking more frequent breaks during daytime, returning to work part time or decreasing the number of tasks). Family caregivers expressed difficulty reconciling their initial expectations with more realistic expectations of the patient’s capabilities over time:
“I don’t want to be a nag, but I want to try to give him a realistic picture of where he is at and where he is going… I am glad he listens and hopefully that will help prevent him from having unrealistic expectations and getting frustrated as he goes along over the next few months.” (Interviewed between 2 weeks to 2 months post-home discharge)
“This has been really hard because there’s no one to one correlation with what he does and how he feels. Like he can go out and do something one day, feel pretty good, but then 2 days later he’ll be really tired. No one can tell us how to increase that activity level appropriately; it’s really just trial and error, so it’s a little frustrating.” (Interviewed at > 2 months post-home discharge)
6. Negative impact on caregivers’ health
After > 2 months post-home discharge, some family caregivers (4 of 20) described how caregiving negatively affected their own physical health over time despite advice from the ICU staff to take steps to maintain health.
“It seems I’m worse tired now than I was when she was sick and right out the hospital. I don’t know whether it’s just catching up with me or not, but I’m mentally and emotionally exhausted…. Everything just seems like a struggle lately.” (Interviewed at > 2 months post-home discharge)
“I would do what the doctors told me to do in the first place and go home and rest while he was in the hospital. I think I drained myself a lot. I think my health went downhill a lot when he was sick…. But I think looking back, in retrospect, I should have.” (Interviewed at > 2 months post-home discharge)
Discussion
In this qualitative content analysis, we explored the challenges and needs in family caregivers of ICU survivors after patients’ home discharge. Our study adds new dimensions to previous qualitative studies as one of few studies that involved repeated interviews with family caregivers following patients’ home discharge. Our findings depicts how family caregivers’ experience mirrors changes in patients’ care needs. In our sample, family caregivers became less concerned about patients’ physical deficits over time, yet their concerns regarding patients’ emotions continued. Initially after home discharge, family caregivers felt overwhelmed and unprepared, but also relieved and hopeful. As time progressed, the feelings of being overwhelmed lessened and family caregivers remained hopeful about progress toward recovery, regardless of the magnitude of improvement in patients’ physical ability. As time progressed, family caregivers expressed difficulty balancing their initial expectations about how recovery would progress with the reality of the slow pace of recovery. Feelings of uncertainty about patients’ recovery and concern for caregivers’ own health became more prominent concerns in the later follow-up period.
From the narratives of our family caregivers, patients’ emotional needs outlasted physical care needs. This is an important finding. Psychiatric illnesses, such as depression, anxiety, and post-traumatic stress disorder (PTSD), are commonly reported in studies of survivors of critical illness.31–34 For example, according to a report from Wunsch et al., which analyzed data from 24,000 ICU survivors who underwent mechanical ventilation, 1% of patients were diagnosed with new psychiatric conditions (mostly anxiety and mood disorders) by a psychiatrist, and 19% were prescribed to take one or more psychoactive medications during the first year following ICU discharge.34 According to systematic reviews, reported rates of depressive and PTSD symptoms in critical illness survivors are 28% and 22%, respectively.35,36 These findings highlight the need to assess ICU survivors for psychological symptoms over the recovery continuum and initiate appropriate treatment, if present. A relationship between psychological symptoms and motivation to engage in physical rehabilitation has been demonstrated in other populations.37,38 Helping ICU survivors managing their psychological symptoms may be a way to improve their motivation to engage in rehabilitation activities following critical illness and may improve family caregiver outcomes.
As one of unique highlights from our findings, family caregivers acknowledged that their physical health had been negatively affected since patients’ ICU admission. Adverse effects of long-term caregiving on family caregivers’ physical health has been reported in studies on caregivers of cancer or Alzheimer’s disease.39 The topic is still in its infancy in family caregivers of the critically ill. Evidence from other studies have described potential physical health problems encountered by family caregivers such as health risk behaviors (e.g., inadequate rest, skipping meals, missing doctor appointment) during patients’ ICU hospitalization,5 sleep problems,9,40,41 and fatigue.10 Quantitative studies reported such problems in family caregivers begin in the ICU settings when patients are acutely ill. But, in the present study, family caregivers did not express concerns about their own physical health in the immediate post-ICU period. Caregivers described physical problems they were experiencing in interviews 2 months or longer after patients’ home discharge. Family caregivers recalled unheeded advice from the ICU staff about maintaining their own health during the acute phase of patient’s ICU stay. Findings indicate family caregivers tend to put self-care on the back burner despite their awareness of its importance and advice from health care providers.
Patients and their family caregivers may experience symptoms reciprocally. A recent cross-sectional survey of patient-spouse caregiving dyads reported that both physical and psychological symptoms are interrelated between patients and spousal caregivers following intensive care of severe sepsis.35 Moreover, this study further highlighted an association between patients’ posttraumatic stress symptoms and spouses’ mental health related quality of life.35 In our sample, caregivers expressed concerns regarding whether caregiving was negatively impacting their own physical health. It is unclear whether caregivers’ physical and mental health is primarily influenced by ICU survivors’ recovery or sustained engagement in caregiving activities, regardless of the level of recovery. Interventions targeted to the dyad, rather than the individual caregiver, appear more likely to optimize support and should be tested in future trials.36
Our study has a few limitations. First, this study involved secondary analysis of qualitative interview data from a subsample of family caregivers from a small pilot study. Our sample lacks diversity in ethnic and socioeconomic background: all participants were white, recruited from a single medical ICU in a tertiary academic medical center. Our participants were predominantly well-educated, a group assumed to have better personal and social resources for caregiving. Notwithstanding, family caregivers in our sample expressed profound and troubling personal difficulties during the post-discharge period. In our sample, patients were largely independent prior to ICU admission, but required an extended ICU stay. We were able to capture a portion of cases which patients were discharged home within 4 months post-ICU discharge, a follow-up period pre-set by the parent study. Therefore, our findings may not be typical of other family caregivers in the situations which these characteristics are not present. For example, patients may be in need of further extended institutional care lasting longer than 4 months post-ICU discharge and then discharged to home. Second, we enrolled only one family caregiver per patient. The contributions of other family members in caregiving would likely contribute to caregivers’ experiences in ways that we have not captured. Finally, in a larger study, we would sample purposively for maximum variation and collect data until saturation was achieved.
This study has several implications to clinical practice and research. First, family caregivers have needs that are longitudinal, extending well beyond the acute phase of the patient’s illness. Helping caregivers prepare for common challenges and needs after home discharge needs to be introduced from early stage of patients’ critical illness and iterative communication and education in post-ICU settings are necessary. Nurses working in the ICU need to be able to help family caregivers understand and prepare for the uncertain and complex nature of patients’ post-ICU recovery while supporting caregivers’ immediate needs during acute phase of patients’ illness. Strategies to support family caregivers to maintain their own self-care behaviors during the acute phase of the illness such as stress reduction strategies, promoting sleep and healthy eating should be offered. Providing resources, demonstrating how to engage external support, resources and respite using various communicating tools, such as written materials, educational video clips, and websites can be part of the overall plan to assist family caregivers. For nurses working in post-ICU or home care settings, knowledge of patients’ and family caregivers’ ICU experience might enable them to better deliver patient and family-centered care. Other models of care such as post-ICU follow-up clinics are being developed to provide a more comprehensive, patient and family-centered approach to post-ICU care. Providers can make supporting caregiver needs as a part of follow-up care for ICU survivors and routinely assess caregivers’ well-being, confidence in caregiving, and their ongoing needs for other support.
Future research is warranted to guide evidence-based knowledge to better support family caregivers of ICU survivors. Well-designed prospective descriptive studies, particularly studies using a mixed-methods approach with a larger caregiver sample are necessary to continue improve our understanding on diverse challenges and needs in family caregivers which may vary by ethnic, socioeconomic and cultural backgrounds. Interventions to support this family caregiver population are still lacking. Studies have introduced strategies to support family caregivers at the early stage of patients’ critical illness42,43 or early post-ICU period,44 but these approaches still need more evidence through randomized controlled trials. Interventions to support family caregivers to better manage their physical health needs are another important but under researched area.
Conclusion
Family caregivers are integral care partners to ICU survivors especially after their discharge to home, but interventions are lacking to this caregiver population. Our findings support that family caregivers need information and skills to help deal with patients’ care needs, pace between expectations and reality, and practice better self-care. Future studies should include dyads of ICU survivors and family caregivers to address (1) discharge preparation specific to individual needs and (2) testing strategies to communicate and support physical and emotional needs in both ICU survivors and family caregivers.
Acknowledgments
Source of Support: This work was supported by the National Institute of Nursing Research (F32 NR 011271 and T32 NR 008857) and by Fellow Research Award from Rehabilitation Nursing Foundation (FEL-0905).
Footnotes
Publisher's Disclaimer: This is a PDF file of an unedited manuscript that has been accepted for publication. As a service to our customers we are providing this early version of the manuscript. The manuscript will undergo copyediting, typesetting, and review of the resulting proof before it is published in its final citable form. Please note that during the production process errors may be discovered which could affect the content, and all legal disclaimers that apply to the journal pertain.
Conflict of Interest Disclosure: None
Contributor Information
JiYeon Choi, Assistant Professor, Department of Acute and Tertiary Care, University of Pittsburgh, School of Nursing, Pittsburgh, PA, USA; Adjunct Professor, Yonsei University College of Nursing, Seoul, Korea.
Jennifer H. Lingler, Associate Professor, Department of Health and Community Systems, University of Pittsburg, School of Nursing, Pittsburgh, PA, USA.
Michael P. Donahoe, Professor, Executive Vice Chair of Clinical Affairs, Division of Pulmonary, Allergy, and Critical Care Medicine, Department of Medicine, University of Pittsburgh, School of Medicine, Pittsburgh, PA, USA.
Mary Beth Happ, Associate Dean of Research and Innovation, Distinguished Professor of Critical Care Research, Director, Center of Excellence in Critical and Complex Care, The Ohio State University College of Nursing, Columbus, OH, USA.
Leslie A. Hoffman, Professor Emeritus, Department of Acute and Tertiary Care, University of Pittsburgh, School of Nursing, Pittsburgh, PA, USA.
Judith A. Tate, Assistant Professor, The Ohio State University College of Nursing, Columbus, OH, USA.
References
- 1.Society of Critical Care Medicine. Critical Care Statistics. http://www.sccm.org/Communications/Pages/CriticalCareStats.aspx. Accessed April 30, 2018.
- 2.Spragg RG, Bernard GR, Checkley W, et al. Beyond mortality: future clinical research in acute lung injury. Am J Respir Crit Care Med. 2010;181(10):1121–1127. doi: 10.1164/rccm.201001-0024WS. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Elliott D, Davidson JE, Harvey MA, et al. Exploring the scope of post-intensive care syndrome therapy and care: engagement of non-critical care providers and survivors in a second stakeholders meeting. Crit Care Med. 2014;42(12):2518–2526. doi: 10.1097/CCM.0000000000000525. [DOI] [PubMed] [Google Scholar]
- 4.Azoulay E, Pochard F, Kentish-Barnes N, et al. Risk of post-traumatic stress symptoms in family members of intensive care unit patients. Am J Respir Crit Care Med. 2005;171(9):987–994. doi: 10.1164/rccm.200409-1295OC. [DOI] [PubMed] [Google Scholar]
- 5.Choi J, Hoffman LA, Schulz R, et al. Health Risk Behaviors in Family Caregivers During Patients’ Stay in Intensive Care Units: A Pilot Analysis. Am J Crit Care. 2013;22(1):41–45. doi: 10.4037/ajcc2013830. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Cameron JI, Herridge MS, Tansey CM, McAndrews MP, Cheung AM. Well-being in informal caregivers of survivors of acute respiratory distress syndrome. Crit Care Med. 2006;34(1):81–86. doi: 10.1097/01.ccm.0000190428.71765.31. [DOI] [PubMed] [Google Scholar]
- 7.Choi J, Donahoe MP, Zullo TG, Hoffman LA. Caregivers of the chronically critically ill after discharge from the intensive care unit: six months’ experience. Am J Crit Care. 2011;20(1):12–22. doi: 10.4037/ajcc2011243. quiz 23. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Choi J, Sherwood PR, Schulz R, et al. Patterns of depressive symptoms in caregivers of mechanically ventilated critically ill adults from intensive care unit admission to 2 months postintensive care unit discharge: a pilot study. Crit Care Med. 2012;40(5):1546–1553. doi: 10.1097/CCM.0b013e3182451c58. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Choi J, Tate JA, Donahoe MP, Ren D, Hoffman LA, Chasens ER. Sleep in family caregivers of ICU survivors for two months post-ICU discharge. Intensive Crit Care Nurs. 2016;37:11–18. doi: 10.1016/j.iccn.2016.07.003. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Choi J, Tate JA, Hoffman LA, et al. Fatigue in Family Caregivers of Adult Intensive Care Unit Survivors. Journal of Pain and Symptom Management. 2014;48(3):353–363. doi: 10.1016/j.jpainsymman.2013.09.018. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Cox CE, Martinu T, Sathy SJ, et al. Expectations and outcomes of prolonged mechanical ventilation. Crit Care Med. 2009;37(11):2888–2894. doi: 10.1097/CCM.0b013e3181ab86ed. quiz 2904. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Douglas SL, Daly BJ. Caregivers of long-term ventilator patients: physical and psychological outcomes. Chest. 2003;123(4):1073–1081. doi: 10.1378/chest.123.4.1073. [DOI] [PubMed] [Google Scholar]
- 13.Im K, Belle SH, Schulz R, Mendelsohn AB, Chelluri L. Prevalence and outcomes of caregiving after prolonged (> or =48 hours) mechanical ventilation in the ICU. Chest. 2004;125(2):597–606. doi: 10.1378/chest.125.2.597. [DOI] [PubMed] [Google Scholar]
- 14.Swoboda SM, Lipsett PA. Impact of a prolonged surgical critical illness on patients’ families. Am J Crit Care. 2002;11(5):459–466. [PubMed] [Google Scholar]
- 15.Van Pelt DC, Milbrandt EB, Qin L, et al. Informal caregiver burden among survivors of prolonged mechanical ventilation. Am J Respir Crit Care Med. 2007;175(2):167–173. doi: 10.1164/rccm.200604-493OC. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Cameron JI, Chu LM, Matte A, et al. One-Year Outcomes in Caregivers of Critically Ill Patients. N Engl J Med. 2016;374(19):1831–1841. doi: 10.1056/NEJMoa1511160. [DOI] [PubMed] [Google Scholar]
- 17.Haines KJ, Denehy L, Skinner EH, Warrillow S, Berney S. Psychosocial outcomes in informal caregivers of the critically ill: a systematic review. Crit Care Med. 2015;43(5):1112–1120. doi: 10.1097/CCM.0000000000000865. [DOI] [PubMed] [Google Scholar]
- 18.Matt B, Schwarzkopf D, Reinhart K, Konig C, Hartog CS. Relatives’ perception of stressors and psychological outcomes - Results from a survey study. J Crit Care. 2017;39:172–177. doi: 10.1016/j.jcrc.2017.02.036. [DOI] [PubMed] [Google Scholar]
- 19.McPeake J, Devine H, MacTavish P, et al. Caregiver strain following critical care discharge: An exploratory evaluation. J Crit Care. 2016;35:180–184. doi: 10.1016/j.jcrc.2016.05.023. [DOI] [PubMed] [Google Scholar]
- 20.van Beusekom I, Bakhshi-Raiez F, de Keizer NF, Dongelmans DA, van der Schaaf M. Reported burden on informal caregivers of ICU survivors: a literature review. Crit Care. 2016;20:16. doi: 10.1186/s13054-016-1185-9. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.van den Born-van Zanten SA, Dongelmans DA, Dettling-Ihnenfeldt D, Vink R, van der Schaaf M. Caregiver strain and posttraumatic stress symptoms of informal caregivers of intensive care unit survivors. Rehabilitation psychology. 2016;61(2):173–178. doi: 10.1037/rep0000081. [DOI] [PubMed] [Google Scholar]
- 22.Fumis RR, Ranzani OT, Martins PS, Schettino G. Emotional disorders in pairs of patients and their family members during and after ICU stay. PLoS One. 2015;10(1):e0115332. doi: 10.1371/journal.pone.0115332. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.Cox CE, Docherty SL, Brandon DH, et al. Surviving critical illness: acute respiratory distress syndrome as experienced by patients and their caregivers. Crit Care Med. 2009;37(10):2702–2708. doi: 10.1097/CCM.0b013e3181b6f64a. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.Czerwonka AI, Herridge MS, Chan L, Chu LM, Matte A, Cameron JI. Changing support needs of survivors of complex critical illness and their family caregivers across the care continuum: a qualitative pilot study of Towards RECOVER. J Crit Care. 2015;30(2):242–249. doi: 10.1016/j.jcrc.2014.10.017. [DOI] [PubMed] [Google Scholar]
- 25.Young E, Eddleston J, Ingleby S, et al. Returning home after intensive care: a comparison of symptoms of anxiety and depression in ICU and elective cardiac surgery patients and their relatives. Intensive Care Med. 2005;31(1):86–91. doi: 10.1007/s00134-004-2495-y. [DOI] [PubMed] [Google Scholar]
- 26.Choi J. Caregivers of Prolonged Mechanical Ventilation: Mind-Body Interaction Model. 2009 http://projectreporter.nih.gov/project_info_description.cfm?aid=7673131&icde=24939781&ddparam=&ddvalue=&ddsub=&cr=5&csb=default&cs=ASC. Accessed Nov 1, 2015.
- 27.Choi J, Hoffman LA, Schulz R, et al. Self-reported physical symptoms in intensive care unit (ICU) survivors: pilot exploration over four months post-ICU discharge. J Pain Symptom Manage. 2014;47(2):257–270. doi: 10.1016/j.jpainsymman.2013.03.019. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 28.Choi J, Tate JA, Rogers MA, Donahoe MP, Hoffman LA. Depressive symptoms and anxiety in intensive care unit (ICU) survivors after ICU discharge. Heart Lung. 2016;45(2):140–146. doi: 10.1016/j.hrtlng.2015.12.002. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 29.Patton MQ. Qualitative Research and Evaluation Methods. Third. Thousand Oak, CA: SAGE Publications, Inc; 2001. [Google Scholar]
- 30.Guba EG. Criteria for Assessing the Trustworthiness of Naturalistic INquiries. Educational Communication and Technology. 1981;29(2):75–91. [Google Scholar]
- 31.Bienvenu OJ, Colantuoni E, Mendez-Tellez PA, et al. Depressive symptoms and impaired physical function after acute lung injury: a 2-year longitudinal study. Am J Respir Crit Care Med. 2012;185(5):517–524. doi: 10.1164/rccm.201103-0503OC. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 32.Desai SV, Law TJ, Needham DM. Long-term complications of critical care. Crit Care Med. 2011;39(2):371–379. doi: 10.1097/CCM.0b013e3181fd66e5. [DOI] [PubMed] [Google Scholar]
- 33.Mikkelsen ME, Shull WH, Biester RC, et al. Cognitive, mood and quality of life impairments in a select population of ARDS survivors. Respirology. 2009;14(1):76–82. doi: 10.1111/j.1440-1843.2008.01419.x. [DOI] [PubMed] [Google Scholar]
- 34.Wunsch H, Christiansen CF, Johansen MB, et al. Psychiatric diagnoses and psychoactive medication use among nonsurgical critically ill patients receiving mechanical ventilation. JAMA. 2014;311(11):1133–1142. doi: 10.1001/jama.2014.2137. [DOI] [PubMed] [Google Scholar]
- 35.Davydow DS, Gifford JM, Desai SV, Bienvenu OJ, Needham DM. Depression in general intensive care unit survivors: a systematic review. Intensive Care Med. 2009;35(5):796–809. doi: 10.1007/s00134-009-1396-5. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 36.Davydow DS, Gifford JM, Desai SV, Needham DM, Bienvenu OJ. Posttraumatic stress disorder in general intensive care unit survivors: a systematic review. Gen Hosp Psychiatry. 2008;30(5):421–434. doi: 10.1016/j.genhosppsych.2008.05.006. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 37.Hornikx M, Van Remoortel H, Demeyer H, et al. The influence of comorbidities on outcomes of pulmonary rehabilitation programs in patients with COPD: a systematic review. Biomed Res Int. 2013;2013:146148. doi: 10.1155/2013/146148. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 38.McGrady A, McGinnis R, Badenhop D, Bentle M, Rajput M. Effects of depression and anxiety on adherence to cardiac rehabilitation. J Cardiopulm Rehabil Prev. 2009;29(6):358–364. doi: 10.1097/HCR.0b013e3181be7a8f. [DOI] [PubMed] [Google Scholar]
- 39.Pinquart M, Sorensen S. Correlates of physical health of informal caregivers: a meta-analysis. J Gerontol B Psychol Sci Soc Sci. 2007;62(2):P126–137. doi: 10.1093/geronb/62.2.p126. [DOI] [PubMed] [Google Scholar]
- 40.Day A, Haj-Bakri S, Lubchansky S, Mehta S. Sleep, anxiety, and fatigue in family members of patients admitted to the intensive care unit: a questionnaire study. Crit Care. 2013;17(3):R91. doi: 10.1186/cc12736. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 41.Verceles AC, Corwin DS, Afshar M, et al. Half of the family members of critically ill patients experience excessive daytime sleepiness. Intensive Care Med. 2014;40(8):1124–1131. doi: 10.1007/s00134-014-3347-z. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 42.Davidson JE, Daly BJ, Agan D, Brady NR, Higgins PA. Facilitated sensemaking: a feasibility study for the provision of a family support program in the intensive care unit. Crit Care Nurs Q. 2010;33(2):177–189. doi: 10.1097/CNQ.0b013e3181d91369. [DOI] [PubMed] [Google Scholar]
- 43.Jones C, Backman C, Capuzzo M, et al. Intensive care diaries reduce new onset post traumatic stress disorder following critical illness: a randomised, controlled trial. Crit Care. 2010;14(5):R168. doi: 10.1186/cc9260. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 44.Cox CE, Porter LS, Hough CL, et al. Development and preliminary evaluation of a telephone-based coping skills training intervention for survivors of acute lung injury and their informal caregivers. Intensive Care Med. 2012;38(8):1289–1297. doi: 10.1007/s00134-012-2567-3. [DOI] [PMC free article] [PubMed] [Google Scholar]


