Highlights
-
•
Ileosigmoid knotting is rare.
-
•
Presents as intestinal obstruction.
-
•
It has a high mortality and morbidity.
-
•
Viable small and large bowel.
Keywords: Ileosigmoid knotting, Intestinal obstruction, Case report
Abstract
Introduction
Ileosigmoid knot is an uncommon cause of acute intestinal obstruction where the ileum wraps around the base of a redundant sigmoid colon.
Case presentation
We present an unusual case of a 45-year-old male patient who presented with signs and symptoms of intestinal obstruction. Exploratory laparotomy revealed an ileosigmoid knot. Both the small and large bowels were viable. The sigmoid colon was resected an end to end anastomosis was done. His post-operative period was uneventful.
Discussion
Preoperative diagnosis of the condition is difficult. Diagnostic delays coupled with the infrequent occurrence of the condition often results in patients commonly presenting with gangrene of the ileum, sigmoid loop or both. There is considerable controversy regarding the optimal management of this rare condition. Management involves preoperative resuscitation, empirical antibiotics and prompt relief of the obstruction. The anatomical and pathological changes of the involved loops of bowel dictate the definitive surgical procedure. The vast majority of cases present with gangrenous loops of ileum, the sigmoid colon or both. To identify the presence of the ileum and sigmoid colon being viable on exploration is a rarity.
Conclusion
The management of a patient who has both viable loops of bowel on exploration is a contentious issue. Traditional teaching dictates that untying of the knot should be coupled with resection of the sigmoid colon to negate the risk of a recurrence. Some case reports suggest that resection may not be necessary as the risk of recurrence is believed to be low.
1. Introduction
This work is reported in line with the Surgical Case Report Guidelines (SCARE) criteria [1]. Ileosigmoid knot is an uncommon cause of acute intestinal obstruction where the ileum wraps around the base of a redundant sigmoid colon. The condition was first described by Parker in 1845 [2] and popularised by Shepherd [3]. This condition has a varied geographical distribution being more common in areas where sigmoid volvulus is common, some African, Asian and Middle Eastern countries [4,5]. Cases of Ileosigmoid knotting are reported mainly in the middle aged male patient although no age is immune [[6], [7], [8]]. Preoperative diagnosis of the condition is difficult as the clinical signs are difficult to define and the radiological signs are often inconsistent [[5], [6], [7]]. The management of a patient who has both viable loops of bowel on exploration is a contentious issue.
We present an unusual case of a 45-year-old male patient who presented with signs and symptoms of intestinal obstruction. Exploratory laparotomy revealed an ileosigmoid knot. Both the small and large bowels were viable. The sigmoid colon was resected an end to end anastomosis was done. His post-operative period was uneventful.
2. Case presentation
We present an unusual case of a 45-year-old male patient who presented at teaching central hospital, with a day’s history of signs and symptoms of intestinal obstruction. He had a sudden onset of a sharp, colicky peri umbilical pain which was not radiating and had no relieving factors. He concurrently had abdominal distension and obstipation but was not vomiting. He had no prior surgical admissions. The patient did not have any contributory family, drug or psychosocial history.
On examination his mucous membranes were pink but dry. He was tachypnoeic with a respiratory rate of 24 bpm, a pulse rate of 88 bpm, a blood pressure of 115/80 mmHg and a body temperature of 36.9 °C. The patient had a globally distended abdomen and negative cough impulse on all potential hernia orifices. The abdomen was soft and non-tender and no palpable masses were felt. There was a uniform tympanic resonant note on percussion on all 4 quadrants and bowel sounds were not audible with a stethoscope. A digital rectal examination revealed an empty rectum.
Full blood count results showed a mild leukocytosis of 12.86 × 103/μL with a left shift, haemoglobin level of 16.9 g/dL, platelet count of 217 × 103/μL and a mean corpuscular volume of 85.9 Fl. His biochemistry results showed sodium of 135 mmol/l, potassium of 5.1 mmol/L chloride 102 mmol/ L and a mild uremia of 7.7 mmol/L and a creatinine of 85 μmol/L. An abdominal series of X-rays showed gaseous distension of large bowel with no pneumo peritoneum. A computed tomography (CT) scan was not available. A clinical diagnosis of large bowel obstruction secondary to sigmoid volvulus with dehydration was made. A decision to explore the abdominal cavity was made after a brief 12-hour period of judicious fluid replacement with Ringers lactate.
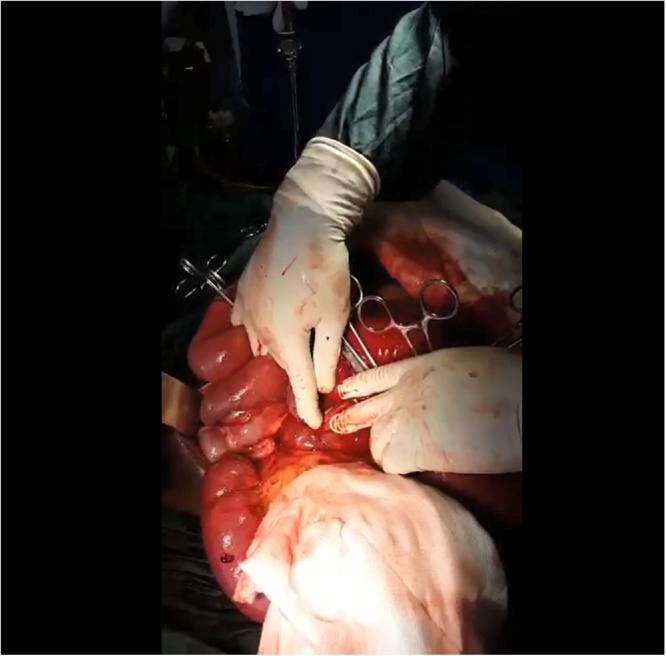
Exploratory laparotomy revealed an ileosigmoid knot with a loop of distal small bowel wrapped around the base of the sigmoid colon (Fig. 1). Both the small and large bowels were viable with a few patchy areas of hyperaemia on the anti-mesenteric side of the small bowel. The sigmoid colon was resected to remove the redundant colon and an end to end anastomosis was done. The operation was done by two general surgeons. The patient was admitted in the High care unit post operatively and his post-operative period was uneventful. Post-operative consideration was of an anastomotic leak. The patient tolerated the post-operative medications. He was discharged from the hospital on day 6 post operation and was subsequently seen in the outpatient department twice. No post-operative complications were reported on both visits. The patient expressed much appreciation to the surgical team.
Fig. 1.
Ileosigmoid knot with a loop of distal small bowel wrapped around the base of the sigmoid colon. Both small and large bowel are viable.
3. Discussion
The exact predisposing factors are not known but a long mesentery of small bowel, freely mobile small bowel and a long sigmoid colon on a narrow pedicle are believed to predispose to the condition. Dietary factors, late pregnancy trans mesenteric herniation, ileocolic intussusception and a floating caecum are possible predisposing factors [[6], [7], [8]].
Preoperative diagnosis of the condition is difficult as the clinical signs are difficult to define and the radiological signs are often inconsistent [[5], [6], [7]]. Diagnostic delays coupled with the infrequent occurrence of the condition often results in patients commonly presenting with gangrene of the ileum, sigmoid loop or both [6]. The triad of a clinical picture of small bowel obstruction, radiographic evidence of large bowel obstruction and failure to insert an endoscope has been described as a possible diagnostic aid but the yield is unfortunately low [6,7,10]. X-rays may show double loop obstruction, with the sigmoid colon in the right upper quadrant and small bowels loops in the left although this is an occasional finding. A characteristic whirl sign on CT scan has improved the pick up rate but the investigation tool is not readily available in countries where the condition is common [4]. The general consensus is that an exact preoperative diagnosis is not essential, exploration of the abdomen is recommended when patients present with intestinal obstruction and peritonitis, shock or a pneumoperitoneum [11].
Ileosigmoid knotting is classified into four types; type I, type II, type III and undetermined [12]. In type I the ileum revolves around a passive sigmoid colon, type II the colon revolves around the ileum, type III the ileocaecal segment is part of the knot and when it is impossible to identify the active segment it is undetermined. When the direction of rotation is known a suffix of a or b is added depending on whether it is clockwise or anticlockwise respectively. This classification is mainly anatomical and does not influence outcome, a new criteria that makes use of preoperative and intra operative processes has been described that is more useful in predicting mortality and morbidity (Table 1) [12].
Table 1.
Classification of patients with ileosigmoid knotting.
| Class | Patient factors |
|---|---|
| I | No risk factors (advanced age or co morbidities) |
| II | No shock or gangrene but presence of risk factors |
| III | Presence of shock |
| IV | Gangrene of ileum or sigmoid colon, no shock |
| V | Shock plus gangrene of either ileum or sigmoid colon |
| VI | Both ileum and sigmoid colon gangrenous |
There is considerable controversy regarding the optimal management of this rare condition. Management involves preoperative resuscitation, empirical administration of antibiotics and prompt relief of the obstruction. The anatomical and pathological changes of the involved loops of bowel dictate the definitive surgical procedure. The vast majority of cases present with gangrenous loops of ileum, the sigmoid colon or both [8,9,11]. To identify the presence of the ileum and sigmoid colon being viable on exploration is a rarity [8]. In the presence of gangrene untwisting of the loops of bowel is not recommended because the risk of reperfusion syndrome and the potential of perforating the gangrenous and often friable bowel. Enbloc resection of the involved loops of bowel including the knot is the preferred approach [13]. When there is concern about leaving too little residual small bowel untwisting of small bowel alone maybe be considered with an option of a relook laparotomy to inspect suspicious bowel. In the haemodynamically stable patient, intestinal continuity is re-established with an end to end anastomosis of the ileum and end to end anastomosis of the sigmoid ends. Special consideration has to be made when the distal ileal stump is less than 10 cm from the ileocaecal valve and when the caecum or ascending colon has gangrenous areas [11,13]. An end to side ileocaecostomy may be formed for the former situation and a right hemi colectomy for the latter scenario. Colostomy should be strongly considered in the elderly patient, patients with associated medical conditions, presence of shock or when the viability of the distal bowel edges is in doubt. Recent data suggest that primary anastomosis is safe as long as a tension free anastomosis can be undertaken avoiding the risk of increased morbidity and mortality associated with a two stage procedure [8,14].
The management of a patient who has both viable loops of bowel on exploration is a contentious issue. Traditional teaching dictates that untying of the knot should be coupled with resection of the sigmoid colon to negate the risk of a recurrence. Some case reports suggest that resection may not be necessary as the risk of recurrence is believed to be low [11,14,15]. The landmark case series report by Shepherd noted no cases of recurrence in patients that were not resected [3,11]. In nongangrenous cases, careful untying of the knot may be performed as a sole surgical procedure in unstable patients, or a volvulus-preventing procedure such as mesopexy, mesoplasty or resection with primary anastomosis may be added [16]. A resection and primary anastomosis was done in our case. Management ultimately should be determined by the local expertise available and decided on a patient to patient basis.
4. Conclusion
Ileosigmoid knot is an uncommon cause of acute intestinal obstruction. Preoperative diagnosis of the condition is difficult. The vast majority of cases present with gangrenous loops of ileum, the sigmoid colon or both. To identify the presence of the ileum and sigmoid colon being viable on exploration is a rarity. The management of a patient who has both viable loops of bowel on exploration is a contentious issue. Traditionally the untying of the knot is coupled with resection of the sigmoid colon to negate the risk of a recurrence. Some case reports suggest that resection may not be necessary as the risk of recurrence is believed to be low.
Conflicts of interest
There is no conflict of interest.
Sources of funding
There is no funding for the case report.
Ethical approval
Consent obtained from the patient.
Ethical approval was exempted by the institution.
Consent
Signed consent obtained from the patient.
Author contribution
Simbarashe Gift Mungazi – case report design, subject research and writing.
Brightson Mutseyekwa – case report design, subject research, consent and writing.
Mordecai Sachikonye – case report design, subject research and writing.
Registration of research studies
Not applicable. This is a case report with no recruitment of patients.
Guarantor
B. Mutseyekwa.
M. Sachikonye.
Acknowledgments
To Professor G I Muguti for his guidance, wisdom and mentorship.
This is to certify that this publication is not submitted to any other journal and there are no conflicts of interests. As the co-author, I submit this case report for peer review and positive criticism, and for possible acceptance for publication. There were no financial requirements for writing this case study.
Contributor Information
Simbarashe Gift Mungazi, Email: simbarashe.mungazi@nust.ac.zw.
Brightson Mutseyekwa, Email: mutseyekwaf@africau.edu.
Mordecai Sachikonye, Email: sachikonyem@gmail.com.
References
- 1.Agha R.A., Fowler A.J., Saeta, Barai I., Rajmohan S., Orgill D.P., SCARE Group The SCARE statement: consesus-based surgical case report guidelines. Int. J. Surg. 2016;6(September (34)):180–186. doi: 10.1016/j.ijsu.2016.08.014. [DOI] [PubMed] [Google Scholar]
- 2.Parker E. Case of intestinal obstruction: sigmoid flexure strangulated by the ileum. Edinb. Med. Surg. J. 1845;64:306–308. [Google Scholar]
- 3.Shepherd J.J. Ninety two cases of ileosigmoid knotting in Uganda. Br. J. Surg. 1967;54:561–566. doi: 10.1002/bjs.1800540615. [DOI] [PubMed] [Google Scholar]
- 4.Baheti A., Patel D., Hira P., Babu D. Ileosigmoid knot: a case report. Indian J. Radiol. Imaging. 2011;21(April (2)):147–149. doi: 10.4103/0971-3026.82301. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Alver O., Oren D., Tireli M., Kayabasi B., Akedemir D. Ileosigmoid knotting in Turkey: a review of 68 cases. Dis. Colon Rectum. 1993;36(December (12)):1139–1147. doi: 10.1007/BF02052263. [DOI] [PubMed] [Google Scholar]
- 6.Atamanlap S. Ileosigmoid knotting: a clinical appearance of 73 cases over 45.5 years. ANZ J. Surg. 2013;83(January (1–2)):70–73. doi: 10.1111/j.1445-2197.2012.06146.x. [DOI] [PubMed] [Google Scholar]
- 7.Berhanu K., Abede B. Ileosigmoid knotting in Addis Ababa: a three year comprehensive retrospective analysis. Ethiop. Med. J. 2006;44(October (4)):377–383. [PubMed] [Google Scholar]
- 8.Ooko P.B., Sarun S., Oloo M., Topazian H.M., White R. Ileosigmoid knotting: a review of 61 cases in Kenya. Pan Afr. Med. J. 2016;23:198. doi: 10.11604/pamj.2016.23.198.6255. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Alver O., Oren D., Tireli M. Ileosigmoid knotting in Turkey: review of 68 cases. Dis. Colon Rectum. 1993;36:1139–1147. doi: 10.1007/BF02052263. [DOI] [PubMed] [Google Scholar]
- 10.Kedir M., Kotisso B., Messele G. Ileosigmoid knotting in Gondar teaching hospital north west Ethiopia. Ethiop. Med. J. 1998;36(October (4)):255–260. [PubMed] [Google Scholar]
- 11.Adili W., Mutua J.M., Nanabhai B.M. The ileosigmoid knot: a case report. Ann. Afr. Surg. 2014;11(July (2)):44–46. [Google Scholar]
- 12.Atamanlap S.S., Oztork G., Aydinli B. A new classification of ileosigmoid knotting. Turk. J. Med. Sci. 2009;39 [PubMed] [Google Scholar]
- 13.Atamalap S.S. Ileosigmoid knotting. Eurasian J. Med. 2009;41:116–119. [PMC free article] [PubMed] [Google Scholar]
- 14.Atamanalp S.S., Oren D., Basoglu M. Ileosigmoid knotting: outcome in 63 patients. Dis. Colon Rectum. 2004;47:906–910. doi: 10.1007/s10350-004-0528-9. [DOI] [PubMed] [Google Scholar]
- 15.Kakar A., Bhatnagar B.N.S. Ileosigmoid knotting: a clinical study in 11 cases. Aust. N. Z. J. Surg. 1981;51:456–458. doi: 10.1111/j.1445-2197.1981.tb05984.x. [DOI] [PubMed] [Google Scholar]
- 16.Atamanalp S.S. Ileosigmoid knotting. Eurasian J. Med. 2009;41(2):116–119. [PMC free article] [PubMed] [Google Scholar]