Abstract
Background
We conducted a systematic review and meta-analysis of double-blind, randomized, placebo-controlled trials of anti-dementia drugs plus antipsychotics for schizophrenia.
Methods
Primary outcomes of efficacy and safety included improving overall symptoms (Positive and Negative Syndrome Scale and Brief Psychiatric Rating Scale scores) and all-cause discontinuation, respectively. Other outcomes included psychopathology subscales (positive, negative, general, and anxiety/depressive symptoms), cognitive function (attention/vigilance, reasoning/problem solving, social cognition, speed of processing, verbal learning, visual learning, working memory, and cognitive control/executive function), Mini-Mental State Examination scores, treatment discontinuation due to adverse events and inefficacy, and individual adverse events. We evaluated the effect size using a random effects model.
Results
We identified 37 studies (n=1574): 14 donepezil-based (n=568), 10 galantamine-based (n=371), 4 rivastigmine-based (n=146), and 9 memantine-based (n=489) studies. Pooled anti-dementia drugs plus antipsychotics treatments were superior to placebo plus antipsychotics in improving the overall symptoms (24 studies, 1069 patients: standardized mean difference=−0.34, 95% CI=−0.61 to −0.08, P=.01), negative symptoms (24 studies, 1077 patients: standardized mean difference =−0.62, 95% CI=−0.92 to −0.32, Pcorrected=.00018), and Mini-Mental State Examination scores (7 studies, 225 patients: standardized mean difference=−0.79, 95% CI=−1.23 to −0.34, P=.0006). No significant differences were found between anti-dementia drugs plus antipsychotics and placebo plus antipsychotics regarding other outcomes.
Conclusions
Although the results suggest that anti-dementia drugs plus antipsychotics treatment improves negative symptoms and Mini-Mental State Examination scores in schizophrenia patients, they possibly were influenced by a small-study effect and some bias. However, it was not superior to placebo plus antipsychotics in improving composite cognitive test score, which more systematically evaluates cognitive impairment than the Mini-Mental State Examination score. Overall, the anti-dementia drugs plus antipsychotics treatment was well tolerated.
Keywords: anti-dementia drugs, cognitive impairment, psychopathology, schizophrenia, systematic review, meta-analysis
Significance Statement
We conducted a systematic review and meta-analysis of double-blind, randomized, placebo-controlled trials of anti-dementia drugs plus antipsychotics (ADD+AP) for treating schizophrenia (37 studies, n = 1574). The meta-analysis evaluated the effect size based on a random effects model. Pooled ADD+AP treatments were superior to placebo+AP in terms of improving overall symptoms (24 studies, 1069 patients: standardized mean difference [SMD] = −0.34, 95% CI = −0.61 to −0.08, P = .01), negative symptoms (24 studies, 1077 patients: SMD = −0.62, 95% CI = −0.92 to −0.32, Pcorrected = .00018), and MMSE scores (7 studies, 225 patients: SMD = −0.79, 95% CI = −1.23 to −0.34, P = .0006). However, we consider that the results were influenced by a small-study effect and some bias. Notably, no significant differences were observed between ADD+AP and placebo+AP in terms of other outcomes of efficacy and safety.
Introduction
Although cognitive impairment is the major feature of schizophrenia (van Os and Kapur, 2009), antipsychotic pharmacotherapy remains the conventional treatment for schizophrenia. Antipsychotics fail to effectively treat cognitive impairments (Nielsen et al., 2015), although their efficacy in treating psychopathologies is relatively well established (Leucht et al., 2013), particularly regarding positive symptoms (Miyamoto et al., 2012). In patients with schizophrenia, cognitive impairment is commonly considered stable throughout their lifespan (Heilbronner et al., 2016). Because most patients tend to have a chronic course due to various residual schizophrenia symptoms, particularly negative and cognitive symptoms (Lang et al., 2013), antipsychotic treatments are often considered insufficient to improve the patients’ quality of life.
In schizophrenia, cognitive impairment and negative symptoms share some common features with those of dementia (van Os and Kapur, 2009), although the deficits are more prominent in prefrontal functions (Kumar et al., 2017). For instance, early-onset frontotemporal dementia and schizophrenia show similar characteristics such as psychotic symptoms (Velakoulis et al., 2009). Moreover, attentional deficits in schizophrenia and dementia possibly share a common neuronal mechanism (Sarter, 1994), and cognitive impairment in schizophrenia may not be histopathologically distinguishable from that in dementia (Arnold and Trojanowski, 1996), supporting the potential of anti-dementia drugs in effectively treating schizophrenia symptoms, including cognitive impairment (Singh et al., 2012; Choi et al., 2013; Correll et al., 2017; Kishi et al., 2017).
Although anti-dementia drugs are relevant in treating schizophrenia symptoms (including cognitive symptoms), their efficacy and safety remain inconclusive, with only weak evidence available limited to only 2 subtypes of anti-dementia treatments: cholinesterase inhibitors and glutaminergic antagonists (Scheltens et al., 2016). Several randomized, placebo-controlled trials have attempted to investigate the efficacy and safety of anti-dementia drugs in treating schizophrenia (supplementary Table 1a). In schizophrenia patients treated with antipsychotics, a recent meta-analysis showed that augmentation with pooled cholinesterase inhibitors (donepezil, galantamine, and rivastigmine) was comparatively more effective than placebo in terms of improving overall and negative symptoms but not in terms of improving cognitive impairment (Choi et al., 2013). Additionally, co-treatment with memantine, a N-methyl-d-aspartate receptor antagonist, was effective in treating negative symptoms (Kishi et al., 2017). However, the meta-analysis did not include the outcomes of specific cognitive impairment domains, as insufficient data was available on these outcomes (Kishi et al., 2017). A meta-analysis can increase the statistical power for group comparisons, thus overcoming the limitation of statistically inadequate sample size in underpowered studies (Higgins and Green, 2011). On the other hand, a low statistical power implies that small meta-analyses may not accurately estimate the efficacy of anti-dementia drugs (i.e., insufficient sample size). However, a number of randomized trials involving the use of cholinesterase inhibitors for the treatment of schizophrenia have been published since the meta-analysis was conducted (Choi et al., 2013), suggesting a potentially higher statistical power. Our previous meta-analysis regarding memantine (Kishi et al., 2017) was also updated to include the psychopathological data from a recent study (Omranifard et al., 2017), thus filling the literature gap regarding the efficacy and safety of anti-dementia drugs added onto antipsychotics (ADD+AP) for the treatment of patients with schizophrenia (supplementary Table 1a,b). This current comprehensive systematic review and meta-analysis were performed to update the available evidence regarding the efficacy (psychopathology and cognitive impairment) and safety (discontinuation rate and the incidence of individual adverse events) of ADD+AP treatment in patients with schizophrenia.
METHODS
This study was performed according to the Preferred Reporting Items for Systematic Reviews and Meta-Analyses guidelines (supplementary Appendix, PRISMA Checklist) (Moher et al., 2009), and it was registered with PROSPERO (http://www.crd.york.ac.uk/PROSPERO/. CRD42017068991).
Search Strategy and Inclusion Criteria
We performed a systematic literature review based on the PICO (participants/population, interventions, comparator/control, outcomes) strategy as follows. Participants/population: schizophrenia or/and schizophrenia spectrum disorder patients who were receiving antipsychotics (exclusion: schizophrenia or/and schizophrenia spectrum disorder patients who were not receiving antipsychotics); interventions: anti-dementia drugs (donepezil, galantamine, rivastigmine, and memantine); comparator/control: placebo; and outcomes: efficacy and safety (detailed information is shown in the following section). In this study, only double-blind, randomized, placebo-controlled trials of >1 day-lasting ADD+AP treatment in patients with schizophrenia were exclusively included.
Accordingly, to identify relevant studies, 2 of the authors (T.K. and Y.M.) independently searched Scopus, MEDLINE, the Cochrane library, and PsycINFO without language restrictions from inception to January 6, 2018. The search terms included “schizophrenia” AND “donepezil” OR “galantamine” OR “rivastigmine” OR “memantine.” Additionally, the authors searched ClinicalTrials.gov (http://clinicaltrials.gov/) and the International Clinical Trials Registry Platform (http://www.who.int/ictrp/en /), thus ensuring a comprehensive search and minimizing publication bias. The selected studies were categorized into an inpatients or outpatients group based on whether they included >50% of inpatients or >50% of outpatients, respectively (supplementary Table 1a). Moreover, the studies that included >50% of patients who were receiving second-generation antipsychotics (SGA) were categorized into an SGA group (supplementary Table 1a). Three authors (T.K., Y.M., and S.M.) independently assessed the selected studies based on the inclusion/exclusion criteria. Additionally, the reference lists of the selected articles and reviews were searched for additional relevant published and unpublished studies, including conference abstracts.
Data Synthesis and Outcome Measures
Primary outcomes comprised the improvement of overall symptoms (efficacy) and all-cause discontinuation (safety). The overall symptoms were evaluated based on the total scores for the Positive and Negative Syndrome Scale (PANSS) (Kay et al., 1989) and the Brief Psychiatric Rating Scale (Overall and Gorham, 1962). These scores have previously been used as outcome measures in many studies on treatment efficacy and are also increasingly used in clinical practice (Fleischhacker and Kemmler, 2007). Other outcomes included psychopathology subscales (positive, negative, general, and anxiety/depressive symptoms), cognitive impairment (attention/vigilance, reasoning/problem solving, social cognition, speed of processing, verbal learning, visual learning, working memory, cognitive control/executive function, and composite cognitive test score), Mini-Mental State Examination (MMSE) scores (Folstein et al., 1975), Clinical Global Impression Severity (CGI-S) scores (Guy and Bonato, 1970), discontinuation due to adverse events or inefficacy, and individual adverse events. The assessment of cognitive impairment was based on previous studies (Choi et al., 2013; Iwata et al., 2015) that used the Measurement and Treatment Research to Improve Cognition in Schizophrenia domains (Green et al., 2004). Supplementary Tables 2a and 2b list the detailed distribution of the outcomes included in this meta-analysis.
Data Extraction
Three authors (T.K., S.M., and K.O.) independently extracted the data from the selected studies. Where possible, intention-to-treat (ITT) or modified ITT (mITT) analyses were used. In the absence of such data, the results from observed case analysis were extracted from each study (supplementary Table 1a). For crossover studies, period 1 data (before crossover) were used for the meta-analysis, if available (supplementary Table 1a). Missing data essential for the meta-analysis were obtained by contacting the authors (or industries) of that particular study or by requesting for unpublished data.
Meta-Analysis Methods
To obtain a higher statistical power than that obtained by previous meta-analyses (Choi et al., 2013; Kishi et al., 2017), we pooled the studies that used cholinesterase inhibitors and memantine as anti-dementia drugs. The current meta-analysis was conducted using the Review Manager software (Collaboration, 2014), and a random effects model was used to account for potential heterogeneity across studies. Dichotomous outcomes are presented as risk ratios with a 95% CI. Further, continuous outcomes were analyzed using standardized mean difference (SMD), allowing the combination of the data generated by the use of the different scales. In cases of unavailability of the SD values, the SD values from similar studies (using the same drug) were used (Higgins and Green, 2011). SMD corresponded to the difference between the 2 means, divided by the pooled SD, with a correction for small sample bias. Because lower scores (e.g., MMSE) indicate a higher impairment or symptom severity, we reversed the algebraic sign of the numerical scores for these scales. Regarding cognitive impairment, the meta-analysis method was followed as that described in previous studies (Choi et al., 2013; Iwata et al., 2015). Briefly, the overall cognitive function outcome was derived from the composite scores of cognitive batteries or from the average SMD of the cognitive domains on condition that ≥6 of the 8 cognitive domains were measured. When one cognitive domain had ≥2 cognitive tests, the average SMD values were used (supplementary Table 2a).
For a 3-arm study (donepezil, 5 mg/d; donepezil, 10 mg/d; and placebo) (Friedman et al., 2002), we combined the data of 2 donepezil arms. The methodological quality of the included trials was assessed based on the Cochrane risk-of-bias criteria (Higgins and Green, 2011). Further, heterogeneity was tested using the I2 statistic, where I2≥50% indicated considerable heterogeneity (Higgins and Green, 2011). The following subgroup/sensitivity analyses were performed to detect the confounding factors for the primary and other efficacy outcomes (negative symptoms and MMSE scores), showing the superiority of ADD+AP to placebo+AP: anti-dementia drug class (cholinesterase inhibitor vs memantine), individual anti-dementia drug (donepezil, galantamine, rivastigmine, and memantine), antipsychotic class (SGA vs first-generation antipsychotic [FGA]), clozapine (clozapine vs other antipsychotic), sponsorship (industry vs non-industry), patient status (inpatient vs outpatient), the scale of psychiatric symptoms (Brief Psychiatric Rating Scale and PANSS vs Scale for the Assessment of Negative Symptoms [SANS, for negative symptoms] (Andreasen, 1982), we did not include this subgroup/sensitivity analysis of MMSE scores), geographical region (Asia vs other regions), and population analysis (ITT/mITT vs non-ITT/mITT). The other subgroup/sensitivity analyses of the negative symptoms were performed in terms of the PANSS negative subscale (original vs other versions) and the negative symptoms of patients (studies that included only patients with defined negative symptoms vs other studies) (supplementary Table 2b). Subgroup/sensitivity analysis was preformed even if there was only one study included in a subgroup. However, we did not discuss results for subgroup that included only one study.
A meta-regression analysis was performed to evaluate the association between the meta-analysis results for overall symptoms, negative symptoms, MMSE scores, and certain modulators (PANSS total scores at baseline, CGI-S scores at baseline, the age of a patient, the duration of illness, the total number of patients, the percentage of males, the percentage of smokers, and study duration) using the Comprehensive Meta-Analysis software version 2 (Biostat Inc.). Further, a second meta-regression analysis was performed to examine whether the effect size of the anti-dementia drugs, in terms of negative symptoms, was associated with baseline PANSS negative subscale scores using the data from studies that exclusively used the original version of the PANSS negative subscale (supplementary Table 2b). In cases of multiple comparisons, Bonferroni corrections were performed. Cognitive impairment is considered a symptom of schizophrenia; however, since the scales differ from psychopathology scales, cognitive impairment and psychopathology were set as independent outcomes. Lastly, funnel plots were used to explore potential publication bias, and Egger’s regression was used to detect publication bias in the meta-analyses. The methodological quality of the included articles was assessed according to the Cochrane Risk of Bias criteria (Cochrane Collaboration, http://www.cochrane.org/).
RESULTS
Study Characteristics
Our literature search identified a total of 1649 studies; of these, we excluded 895 duplicate studies, 647 after reviewing their title/abstract, and 72 after full-text review (60 review articles, 1 single-arm study, 1 case study, and 10 duplicated studies; supplementary Figure 1). Additionally, 2 studies were retrieved by searching review articles (Ribeiz et al., 2010; Singh et al., 2012) (supplementary Figure 1).
Following exclusions, 37 studies were selected for inclusion, comprising a total of 1574 patients. Among the 37 studies, there were 14 donepezil-based (n=568), 10 galantamine-based (n=371), 4 rivastigmine-based (n=146), and 9 memantine-based (n=489) studies. A summary of the included studies is presented in supplementary Table 1a.
All included studies were double-blind, placebo-controlled trials published in English (supplementary Table 1a). However, most of the included studies were small (supplementary Table 1a) and had inconsistent results (supplementary Table 1b). Thirteen studies were sponsored by pharmaceutical companies (supplementary Table 1a). The mean study duration, mean duration of illness, and mean patient age were 13.5 weeks, 17.2 years, and 40.1 years, respectively, and 68.3% of the patients were males. Out of the 37 studies, 15 were conducted in Asia. The data from 31 studies were used for the meta-analysis, as the remaining 6 studies (Allen et al., 2003; Hussain and Chaudhry, 2003; Erickson et al., 2005; Mazeh et al., 2006; Sacco et al., 2008; Swerdlow et al., 2016) did not report the data required to perform a meta-analysis. Notably, although 10 of the 31 studies included in the meta-analysis did not use ITT/mITT populations in their analyses (supplementary Table 1a), they were included to maximize the sample size. Additionally, most included studies did not provide sufficient information about selection, performance, and detection biases. The results of the evaluation of the methodological quality based on the Cochrane risk-of-bias criteria is shown in supplementary Figure 2.
Efficacy Outcomes
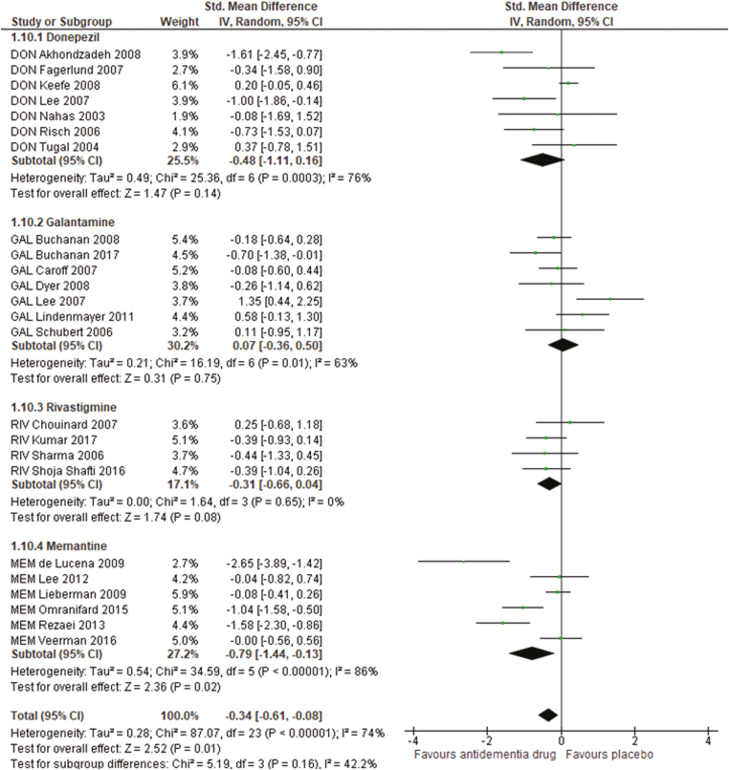
Compared with the placebo+AP treatment, the pooled treatments with ADD+AP (24 studies, 1069 patients) significantly improved the overall symptoms (SMD=−0.34, 95% CI=−0.61 to −0.08, P=.01, I2=74%; Figure 1; Table 1). Notably, no publication bias was detected within each treatment group (Funnel plot: supplementary Figure 3a, Egger’s test P =.100).
Figure 1.
Forest plot for overall symptoms. 95% CI, 95% confidence interval; DON, donepezil; GAL, galantamine; IV, inverse variance, MEM, memantine; RIV, rivastigmine; Std. Mean Difference, standardized mean difference.
Table 1.
Results of Efficacy Outcomes
| N | n | SMD | 95% CI | P | Corrected P | I2 | |
|---|---|---|---|---|---|---|---|
| Overall symptoms a | 24 | 1069 | -0.34 | -0.61, -0.08 | .01 | 74% | |
| Positive symptoms | 21 | 805 | -0.21 | -0.45, 0.04 | .10 | 60% | |
| Negative symptoms | 24 | 1077 | -0.62 | -0.92, -0.32 | .000045 | .00018 b | 80% |
| Anxiety/depressive symptoms | 12 | 483 | -0.20 | -0.39, -0.02 | .03 | .12 b | 4% |
| PANSS general subscale scores | 12 | 367 | -0.23 | -0.62, 0.16 | .24 | 68% | |
| CGI-S score | 8 | 356 | -0.03 | -0.38, 0.32 | .87 | 53% | |
| Composite cognitive test scores | 6 | 532 | -0.02 | -0.22, 0.18 | .83 | 37% | |
| Working memory scores | 15 | 501 | 0.08 | -0.18, 0.34 | .53 | 65% | |
| Verbal learning scores | 14 | 487 | -0.23 | -0.44, -0.01 | .04 | .32 c | 57% |
| Speed of processing scores | 12 | 417 | 0.16 | -0.08, 0.40 | .19 | 33% | |
| Attention/vigilance scores | 9 | 330 | -0.13 | -0.38, 0.13 | .34 | 28% | |
| Reasoning/problem solving scores | 4 | 130 | -0.10 | -0.45, 0.24 | .56 | 0% | |
| Cognitive control/executive function scores | 10 | 279 | 0.02 | -0.27, 0.31 | .90 | 45% | |
| Social cognition scores | 2 | 64 | 0.06 | -0.43, 0.55 | .82 | 0% | |
| Visual learning scores | 5 | 181 | -0.03 | -0.26, 0.21 | .82 | 0% | |
| MMSE scores | 7 | 225 | -0.79 | -1.23, -0.34 | .0006 | 60% |
95% CI, 95% confidence interval; CGI-S, Clinical Global Impression Severity; MMSE, Mini-Mental Status Examination; N, number of comparisons; n, number of patients; PANSS, Positive and Negative Syndrome Scale; SMD, standardized mean difference.
a Primary outcome for efficacy.
b Bonferroni correction was performed for multiple comparisons: 4 tests (4 psychopathology subscales).
c Bonferroni correction was performed for multiple comparisons: 8 tests (8 cognitive domains).
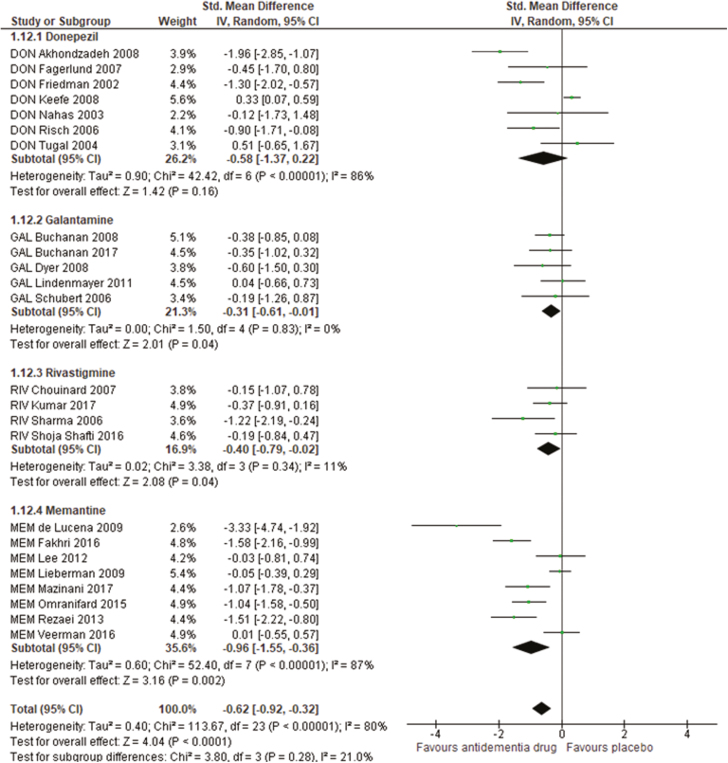
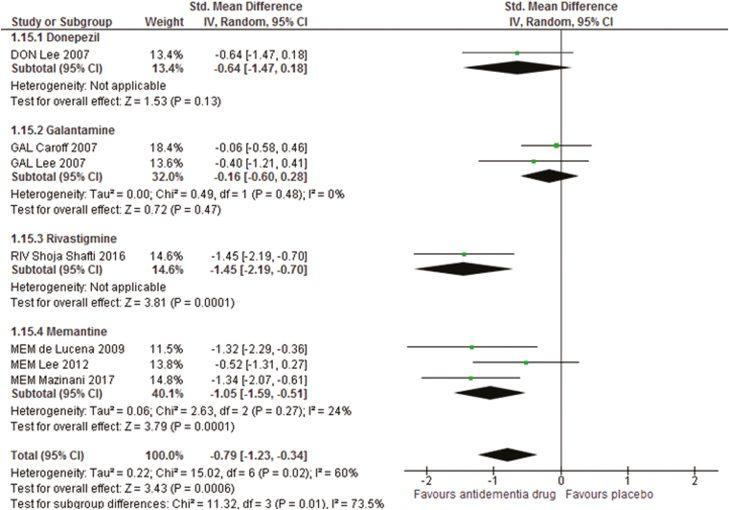
The pooled ADD+AP treatments were also superior to placebo+AP in terms of improving the negative symptoms (24 studies, 1077 patients: SMD=−0.62, 95% CI=−0.92 to −0.32, corrected P=.00018, I2=80%; Figure 2; Table 1) and MMSE scores (7 studies, 225 patients: SMD=−0.79, 95% CI=−1.23 to −0.34, P=.0006, I2=60%; Figure 3; Table 1). However, publication bias was detected for the negative symptoms (Egger’s test P =.00588; Funnel plot: supplementary Figure 3b) but not for the MMSE scores (Egger’s test P=.139; Funnel plot: supplementary Figure 3c).
Figure 2.
Forest plot for negative symptoms. Although the overall P value in this figure was<.0001, the more detailed overall P value was .000045. 95% CI, 95% confidence interval; DON, donepezil; GAL, galantamine; IV, inverse variance; MEM, memantine; RIV, rivastigmine; Std. Mean Difference, standardized mean difference.
Figure 3.
Forest plot for Mini-Mental State Examination (MMSE) scores. 95% CI, 95% confidence interval; DON, donepezil; GAL, galantamine; IV, inverse variance; MEM, memantine; RIV, rivastigmine; Std. Mean Difference, standardized mean difference.
No significant differences were found between the ADD+AP and placebo+AP treatments in terms of other efficacy outcomes.
Sensitivity/Subgroup Analysis
Overall Symptoms
Regarding the overall symptoms, a considerable heterogeneity was found (I2=74%; Table 1), which disappeared in the sensitivity analyses using the data from the rivastigmine-based, industry-sponsored, and non-ITT/mITT studies (supplementary Table 3a). Following Bonferroni corrections, there were remarkably no subgroups wherein ADD+AP treatment was superior to placebo+AP in terms of improving the overall symptoms (supplementary Table 3a).
Negative Symptoms
Regarding the negative symptoms score, considerable heterogeneity was found (I2=80%; Table 1), which disappeared in the sensitivity analyses using the data from the galantamine-based, rivastigmine-based, FGA, SANS, and non-ITT/mITT studies (supplementary Table 3b). Following Bonferroni corrections, the subgroups with superior ADD+AP outcomes than placebo+AP in terms of the negative symptom improvements included the SGA studies, the studies using antipsychotics other than clozapine, non-industry-sponsored studies, the studies other than those including only patients with defined negative symptoms, Asia-based studies, and non-ITT/mITT studies (supplementary Table 3b).
MMSE Score
Regarding the MMSE scores, there was considerable heterogeneity (I2=60%; Table 1), which disappeared in the sensitivity analyses using the data from the memantine-based, galantamine-based, FGA, non-industry-sponsored, inpatient, Asia-based, and ITT/mITT studies (supplementary Table 3c). Following Bonferroni corrections, the subgroups wherein the ADD+AP treatment was superior to placebo+AP in terms of improving the MMSE scores included the memantine-based, FGA, non-industry-sponsored, inpatient, Asia-based, and ITT/mITT studies (supplementary Table 3c).
Meta-Regression Analysis
Overall Symptoms
In terms of the overall symptoms, the effect size of the ADD+AP treatment was associated with the CGI-S scores at baseline (supplementary Table S4a; supplementary Figure 4a).
Negative Symptoms
In terms of the negative symptoms, the effect size of the ADD+AP treatment was associated with the CGI-S scores at baseline and with the total number of patients (supplementary Table 4b; supplementary Figure 4b,c).
MMSE Score
In terms of MMSE score, the effect size of the ADD+AP treatment was associated with the age of a patient (supplementary Table 4c; supplementary Figure 4d).
Safety Outcomes
Notably, no significant difference was found between the ADD+AP and placebo+AP treatment groups in terms of all-cause discontinuation (28 studies, 1328 patients: risk ratio=1.16, 95% CI=0.90–1.49, P=.26, I2=0%; supplementary Table 5; supplementary Figure 5). No publication bias was found within each treatment group in terms of all-cause discontinuation (Funnel plot: supplementary Figure 3d, Egger’s test P=.155). Additionally, there were no significant differences between the treatment groups in terms of the occurrence of other adverse events (supplementary Table 5).
Discussion
This updated and comprehensive systematic review and meta-analysis investigated the use of anti-dementia drugs (donepezil, galantamine, rivastigmine, and memantine) in schizophrenia patients, and it was observed that the pooled ADD+AP treatment group experienced superior efficacy than the placebo+AP treatment group in terms of safety, without significant differences. In particular, anti-dementia drugs effectively treated overall and negative symptoms.
Although there was considerable heterogeneity, the drugs improved the overall symptoms, negative symptoms, and MMSE scores in schizophrenia patients. To date, a meta-regression and several sensitivity/subgroup analyses have been performed to study these outcomes, particularly to identify the causes of heterogeneity. For the overall symptoms, the subgroups that did not present considerable heterogeneity included the rivastigmine-based, industry-sponsored, and non-ITT/mITT studies. Markedly, the anti-dementia drugs were not superior to placebo in any of these subgroups. Therefore, although we could not identify an apparent cause for heterogeneity, sponsor and attrition biases (non-ITT/mITT studies) possibly influenced the meta-analytic results of the overall symptoms. The association found in the meta-regression analysis between the effect size of the anti-dementia drugs for the overall symptoms and CGI-S scores at baseline suggests that the baseline illness severity influences this positive result. Moreover, the small effect size of the anti-dementia drugs in terms of the overall symptoms was remarkably small.
In terms of the negative symptoms, considerable heterogeneity and a publication bias were detected. The subgroups lacking considerable heterogeneity included the galantamine-based, rivastigmine-based, FGA, SANS, and non-ITT/mITT studies; among these, we detected that the anti-dementia drugs were superior to placebo only in the non-ITT/mITT study subgroup. The meta-regression analysis also showed an association between the effect sizes of anti-dementia drugs in terms of the negative symptoms and the studies with small sample size. The studies included in the meta-analysis comprised small sample size (the median number of patients=34). In fact, the studies with a high-quality study design and large sample size (>100 patients) reported that anti-dementia drugs were not superior to placebo (Keefe et al., 2008; Lieberman et al., 2009), possibly attributable to the lack of power and type 1 errors in the included studies. A previously published article concluded that 35% of the published meta-analyses failed to accurately predict the outcomes of subsequently conducted large RCTs regarding the same topics (LeLorier et al., 1997). Therefore, the possibility that the result of meta-analysis in terms of negative symptoms is influenced by an attrition bias and a small-study effect cannot be denied (Sterne et al., 2000). Furthermore, this result possibly was a type I error owing to its small sample size. The meta-regression analysis demonstrated that the effect sizes of anti-dementia drugs for negative symptoms might be associated with disease severity (the CGI-S scores at baseline). However, the second meta-regression analysis showed no association between the effect size of anti-dementia drugs and the original version of the PANSS negative subscale score at baseline. Although only 2 studies included only patients with defined negative symptoms (de Lucena et al., 2009; Buchanan et al., 2017), the subgroup analysis did not show the superiority of anti-dementia drugs over placebo. Therefore, further studies involving a large number of patients with defined negative schizophrenia symptoms are warranted to examine whether anti-dementia drugs actually improve the negative symptoms of schizophrenia.
We found that the pooled ADD+AP treatment was superior to the placebo+AP treatment based on the MMSE score. The subgroups with the anti-dementia drugs superior to placebo in terms of the MMSE score without considerable heterogeneity included the memantine-based, FGA, non-industry-sponsored, inpatient, Asia-based, and ITT/mITT studies. All 3 memantine studies were non-industry-sponsored studies. Among these, the memantine studies have the largest effect size for anti-dementia drugs.
Although memantine is marketed to treat moderate to severe Alzheimer’s disease (i.e., mostly older adult patients) (Scheltens et al., 2016), it was noteworthy that the effect size of anti-dementia drugs for improving the MMSE score increased in younger adult patients with schizophrenia. Considering the fact that anti-dementia drugs possess a neuroprotective effect (Villarroya et al., 2007; Parsons et al., 2013), they may recover the scores in younger adult schizophrenia patients without severe neuron impairment further than in older adult patients. However, the number of studies and patients in the MMSE score meta-analysis was statistically small. Moreover, the pooled ADD+AP treatment was not superior to placebo+AP in terms of the composite cognitive test score, which evaluates cognitive impairment more comprehensively than the MMSE score. In addition, it was unclear whether the negative symptoms were actually corrected for the MMSE scores.
There were several limitations to this study that need to be addressed. First, the sample size of the included studies was small. Although our study had a larger sample size than some previous studies (Singh et al., 2012; Choi et al., 2013; Kishi et al., 2017), there might be a small-study effect in the results for the overall and negative symptoms (Sterne et al., 2000). Accordingly, a future study using a larger sample size should be conducted to obtain more robust results. Second, the patient characteristics among the examined studies differed in terms of the symptom severity, inclusion criteria, the scales for evaluating the schizophrenia symptoms, geographical region, race, ethnicity, drug dose, and study duration; these differences may have generated heterogeneity while combining the data for the systematic review and meta-analysis. Additionally, there were considerable heterogeneities in terms of the overall symptoms, negative symptoms, and MMSE scores. We also detected some bias (sponsor, publication, and attrition biases) associated with the effect size of the anti-dementia drugs in the treatment of these outcomes. Of the 37 studies, 15 were conducted in Asia. However, we failed to find the reason for the results of Asia-based studies influencing those of our meta-analysis. Because there was no standard calculation method with respect to equivalent doses of anti-dementia drugs, we did not examine whether anti-dementia drug doses had an impact on the meta-analytic results. Lastly, most included studies were industry-sponsored studies. Therefore, the impact of sponsorship bias (Naci et al., 2014) needs to be considered while interpreting our results.
In conclusion, the current meta-analysis suggests that the ADD+AP treatment influences psychopathology, particularly the negative symptoms of schizophrenia. However, the effect size of ADD+AP treatment for the overall and negative symptoms was small to medium. Moreover, since we cannot discard the possibility that a small-study effect and some bias (attrition, publication, and sponsorship biases) influenced the results, further studies using larger sample sizes with defined negative symptoms should be conducted to investigate whether the ADD+AP treatment improves the schizophrenia symptoms (particularly the negative symptoms) in patients with schizophrenia.
Statement of Interest
Drs Kishi, Ikuta, Oya, Matsunaga, Matsuda, and Iwata declare that they have no direct conflicts of interest relevant to this study. No grant support or other sources of funding were used to conduct this study or prepare this manuscript. Dr Kishi has received speaker’s honoraria from Daiichi Sankyo, Dainippon Sumitomo, Eisai, Janssen, Otsuka, Meiji, MSD, and Tanabe-Mitsubishi (Yoshitomi) and has received a Health Labour Sciences research grant and a Fujita Health University School of Medicine research grant. Dr Ikuta has received speaker’s honoraria from Eli Lilly, Daiichi Sankyo, and Dainippon Sumitomo. Dr Oya has received speaker’s honoraria from Eisai, Eli Lilly, Janssen, Meiji, Otsuka, and Tanabe-Mitsubishi and has received a Fujita Health University School of Medicine research grant. Dr Matsunaga has received speaker’s honoraria from Daiichi Sankyo, Dainippon Sumitomo, Eisai, Janssen, Meiji, MSD, Novartis, Otsuka, and Tanabe-Mitsubishi and has received a Fujita Health University School of Medicine research grant and a grant-in-aid for young scientists (B). Dr Matsuda has received speaker’s honoraria from Dainippon Sumitomo, Eisai, Eli Lilly, GlaxoSmithKline, Otsuka, Tanabe-Mitsubishi, and Pfizer and has received a grant-in-aid for young scientists (B). Dr Ikuta has received speaker’s honoraria from Eli Lilly, Daiichi Sankyo, and Dainippon Sumitomo. Dr Iwata has received speaker’s honoraria from Astellas, Dainippon Sumitomo, Eli Lilly, GlaxoSmithKline, Janssen, Yoshitomi, Otsuka, Meiji, Shionogi, Novartis, and Pfizer and has had research grants from GlaxoSmithKline, Meiji, and Otsuka.
Supplementary Material
Acknowledgments
We thank Dr. S. R. T. Veerman (Mental Health Service Organization North Holland North, Community Mental Health Division, Flexible Assertive Community Treatment, Alkmaar, The Netherlands), Dr. David de Lucena (rograma de Pós-Graduação, em Medicina: Psiquiatria, Universidade Federal do Rio Grande do Sul, Porto Alegre, Brazil), Dr. Paul B. Hicks (Psychiatry and Behavioral Science, College of Medicine, Texas A&M University), Dr. Jean-Pierre Lindenmayer (Research Department, Manhattan Psychiatric Center), and Dr. Anzalee Khan (Manhattan Psychiatric Center, Office of Mental Health) for providing information for this study.
References
- Allen T, McEvoy J, Keefe R(2003)Galantamine as an adjunctive therapy in the treatment of schizophrenia. Paper presented at: 11th Congress of the International Psychogeriatric Association (IPA); August 17–22, 2003; Chicago, IL. [Google Scholar]
- Andreasen NC.(1982)Negative symptoms in schizophrenia. Definition and reliability. Arch Gen Psychiatry 39:784–788. [DOI] [PubMed] [Google Scholar]
- Arnold SE, Trojanowski JQ(1996)Cognitive impairment in elderly schizophrenia: a dementia (still) lacking distinctive histopathology. Schizophr Bull 22:5–9. [DOI] [PubMed] [Google Scholar]
- Buchanan RW, Kelly DL, Weiner E, Gold JM, Strauss GP, Koola MM, McMahon RP, Carpenter WT(2017)A randomized clinical trial of oxytocin or galantamine for the treatment of negative symptoms and cognitive impairments in people with schizophrenia. J Clin Psychopharmacol 37:394–400. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Choi KH, Wykes T, Kurtz MM(2013)Adjunctive pharmacotherapy for cognitive deficits in schizophrenia: meta-analytical investigation of efficacy. Br J Psychiatry 203:172–178. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Collaboration TC (2014)Review Manager (RevMan) [computer program]. Version 5.3. Copenhagen: The Nordic Cochrane Centre. [Google Scholar]
- Correll CU, Rubio JM, Inczedy-Farkas G, Birnbaum ML, Kane JM, Leucht S(2017)Efficacy of 42 pharmacologic cotreatment strategies added to antipsychotic monotherapy in schizophrenia: systematic overview and quality appraisal of the meta-analytic evidence. JAMA Psychiatry 74:675–684. [DOI] [PMC free article] [PubMed] [Google Scholar]
- de Lucena D, Fernandes BS, Berk M, Dodd S, Medeiros DW, Pedrini M, Kunz M, Gomes FA, Giglio LF, Lobato MI, Belmonte-de-Abreu PS, Gama CS(2009)Improvement of negative and positive symptoms in treatment-refractory schizophrenia: a double-blind, randomized, placebo-controlled trial with memantine as add-on therapy to clozapine. J Clin Psychiatry 70:1416–1423. [DOI] [PubMed] [Google Scholar]
- Erickson SK, Schwarzkopf SB, Palumbo D, Badgley-Fleeman J, Smirnow AM, Light GA(2005)Efficacy and tolerability of low-dose donepezil in schizophrenia. Clin Neuropharmacol 28:179–184. [DOI] [PubMed] [Google Scholar]
- Fleischhacker WW, Kemmler G(2007)The clinical relevance of percentage improvements on the PANSS score. Neuropsychopharmacology 32:2435–2436. [DOI] [PubMed] [Google Scholar]
- Folstein MF, Folstein SE, McHugh PR(1975)“Mini-mental state”. A practical method for grading the cognitive state of patients for the clinician. Psychiatry Res 12:189–198. [DOI] [PubMed] [Google Scholar]
- Friedman JI, Adler DN, Howanitz E, Harvey PD, Brenner G, Temporini H, White L, Parrella M, Davis KL(2002)A double blind placebo controlled trial of donepezil adjunctive treatment to risperidone for the cognitive impairment of schizophrenia. Biol Psychiatry 51:349–357. [DOI] [PubMed] [Google Scholar]
- Green MF, Nuechterlein KH, Gold JM, Barch DM, Cohen J, Essock S, Fenton WS, Frese F, Goldberg TE, Heaton RK, Keefe RS, Kern RS, Kraemer H, Stover E, Weinberger DR, Zalcman S, Marder SR(2004)Approaching a consensus cognitive battery for clinical trials in schizophrenia: the NIMH-MATRICS conference to select cognitive domains and test criteria. Biol Psychiatry 56:301–307. [DOI] [PubMed] [Google Scholar]
- Guy W, Bonato RR(1970)Manual for the ECDEU assessment battery, 2nd ed Chevy Chase, MD: National Institute of Mental Health. [Google Scholar]
- Heilbronner U, Samara M, Leucht S, Falkai P, Schulze TG(2016)The longitudinal course of schizophrenia across the lifespan: clinical, cognitive, and neurobiological aspects. Harv Rev Psychiatry 24:118–128. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Higgins J, Green S(2011)Cochrane handbook for systematic reviews of interventions version 5.1.0 (updated March 2011) Available at: http://handbook.cochrane.org.
- Hussain M, Chaudhry Z(2003)Rivastigmine and galantamine treatment for schizophrenic cognitive impairment. Paper presented at: The 156th Annual Meeting of the American Psychiatric Association; May 17–22, 2003; San Francisco, CA. [Google Scholar]
- Iwata Y, Nakajima S, Suzuki T, Keefe RS, Plitman E, Chung JK, Caravaggio F, Mimura M, Graff-Guerrero A, Uchida H(2015)Effects of glutamate positive modulators on cognitive deficits in schizophrenia: a systematic review and meta-analysis of double-blind randomized controlled trials. Mol Psychiatry 20:1151–1160. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Kay SR, Opler LA, Lindenmayer JP(1989)The Positive and negative syndrome scale (PANSS): rationale and standardisation. Br J Psychiatry 59–67. [PubMed] [Google Scholar]
- Keefe RS, Malhotra AK, Meltzer HY, Kane JM, Buchanan RW, Murthy A, Sovel M, Li C, Goldman R(2008)Efficacy and safety of donepezil in patients with schizophrenia or schizoaffective disorder: significant placebo/practice effects in a 12-week, randomized, double-blind, placebo-controlled trial. Neuropsychopharmacology 33:1217–1228. [DOI] [PubMed] [Google Scholar]
- Kishi T, Matsuda Y, Iwata N(2017)Memantine add-on to antipsychotic treatment for residual negative and cognitive symptoms of schizophrenia: a meta-analysis. Psychopharmacology (Berl) 234:2113–2125. [DOI] [PubMed] [Google Scholar]
- Kumar V, Shivakumar V, Chhabra H, Bose A, Venkatasubramanian G, Gangadhar BN(2017)Functional near infra-red spectroscopy (fNIRS) in schizophrenia: a review. Asian J Psychiatr 27:18–31. [DOI] [PubMed] [Google Scholar]
- Lang FU, Kösters M, Lang S, Becker T, Jäger M(2013)Psychopathological long-term outcome of schizophrenia – a review. Acta Psychiatr Scand 127:173–182. [DOI] [PubMed] [Google Scholar]
- LeLorier J, Grégoire G, Benhaddad A, Lapierre J, Derderian F(1997)Discrepancies between meta-analyses and subsequent large randomized, controlled trials. N Engl J Med 337:536–542. [DOI] [PubMed] [Google Scholar]
- Leucht S, Cipriani A, Spineli L, Mavridis D, Orey D, Richter F, Samara M, Barbui C, Engel RR, Geddes JR, Kissling W, Stapf MP, Lässig B, Salanti G, Davis JM(2013)Comparative efficacy and tolerability of 15 antipsychotic drugs in schizophrenia: a multiple-treatments meta-analysis. Lancet 382:951–962. [DOI] [PubMed] [Google Scholar]
- Lieberman JA, Papadakis K, Csernansky J, Litman R, Volavka J, Jia XD, Gage A, MEM-MD-29 Study Group (2009)A randomized, placebo-controlled study of memantine as adjunctive treatment in patients with schizophrenia. Neuropsychopharmacology 34:1322–1329. [DOI] [PubMed] [Google Scholar]
- Mazeh D, Zemishlani H, Barak Y, Mirecki I, Paleacu D(2006)Donepezil for negative signs in elderly patients with schizophrenia: an add-on, double-blind, crossover, placebo-controlled study. Int Psychogeriatr 18:429–436. [DOI] [PubMed] [Google Scholar]
- Miyamoto S, Miyake N, Jarskog LF, Fleischhacker WW, Lieberman JA(2012)Pharmacological treatment of schizophrenia: a critical review of the pharmacology and clinical effects of current and future therapeutic agents. Mol Psychiatry 17:1206–1227. [DOI] [PubMed] [Google Scholar]
- Moher D, Liberati A, Tetzlaff J, Altman DG, PRISMA Group (2009)Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. Bmj 339:b2535. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Naci H, Dias S, Ades AE(2014)Industry sponsorship bias in research findings: a network meta-analysis of LDL cholesterol reduction in randomised trials of statins. Bmj 349:g5741. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Nielsen RE, Levander S, Kjaersdam Telléus G, Jensen SO, Østergaard Christensen T, Leucht S(2015)Second-generation antipsychotic effect on cognition in patients with schizophrenia–a meta-analysis of randomized clinical trials. Acta Psychiatr Scand 131:185–196. [DOI] [PubMed] [Google Scholar]
- Omranifard V, Rajabi F, Mohammadian-Sichani M, Maracy MR(2017)The effect of add-on memantine on positive, negative and depressive symptoms of schizophrenia: a doubleblind, randomized, controlled trial. Actas Esp Psiquiatr 45:108–115. [PubMed] [Google Scholar]
- Overall JE, Gorham DR(1962)The brief psychiatric rating scale. Psychol Rep 10:799–812. [Google Scholar]
- Parsons CG, Danysz W, Dekundy A, Pulte I(2013)Memantine and cholinesterase inhibitors: complementary mechanisms in the treatment of Alzheimer’s disease. Neurotox Res 24:358–369. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Ribeiz SR, Bassitt DP, Arrais JA, Avila R, Steffens DC, Bottino CM(2010)Cholinesterase inhibitors as adjunctive therapy in patients with schizophrenia and schizoaffective disorder: a review and meta-analysis of the literature. CNS Drugs 24:303–317. [DOI] [PubMed] [Google Scholar]
- Sacco KA, Creeden C, Reutenauer EL, George TP(2008)Effects of galantamine on cognitive deficits in smokers and non-smokers with schizophrenia. Schizophr Res 103:326–327. [DOI] [PubMed] [Google Scholar]
- Sarter M.(1994)Neuronal mechanisms of the attentional dysfunctions in senile dementia and schizophrenia: two sides of the same coin?Psychopharmacology (Berl) 114:539–550. [DOI] [PubMed] [Google Scholar]
- Scheltens P, Blennow K, Breteler MM, de Strooper B, Frisoni GB, Salloway S, Van der Flier WM(2016)Alzheimer’s disease. Lancet 388:505–517. [DOI] [PubMed] [Google Scholar]
- Singh J, Kour K, Jayaram MB(2012)Acetylcholinesterase inhibitors for schizophrenia. Cochrane Database Syst Rev 1:CD007967. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Sterne JA, Gavaghan D, Egger M(2000)Publication and related bias in meta-analysis: power of statistical tests and prevalence in the literature. J Clin Epidemiol 53:1119–1129. [DOI] [PubMed] [Google Scholar]
- Swerdlow NR, Bhakta S, Chou HH, Talledo JA, Balvaneda B, Light GA(2016)Memantine effects on sensorimotor gating and mismatch negativity in patients with chronic psychosis. Neuropsychopharmacology 41:419–430. [DOI] [PMC free article] [PubMed] [Google Scholar]
- van Os J, Kapur S(2009)Schizophrenia. Lancet 374:635–645. [DOI] [PubMed] [Google Scholar]
- Velakoulis D, Walterfang M, Mocellin R, Pantelis C, McLean C(2009)Frontotemporal dementia presenting as schizophrenia-like psychosis in young people: clinicopathological series and review of cases. Br J Psychiatry 194:298–305. [DOI] [PubMed] [Google Scholar]
- Villarroya M, García AG, Marco-Contelles J, López MG(2007)An update on the pharmacology of galantamine. Expert Opin Investig Drugs 16:1987–1998. [DOI] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.