ABSTRACT
It is possible to unify three-dimensional customized orthodontic techniques and three-dimensional surgical technology. In this case report, it is introduced a treatment scheme consisting of passive self-ligation customized brackets and virtual surgical planning combined with the orthognathic surgery-first approach in a Class III malocclusion patient. Excellent facial and occlusal outcomes were obtained in a reduced treatment time of five months.
Keywords: Angle Class III malocclusion, Orthodontic surgery, Orthodontics, Three-dimensional image
RESUMO
É possível unificar técnicas ortodônticas personalizadas e tecnologia de planejamento cirúrgico 3D. No presente relato de caso, apresenta-se um plano de tratamento envolvendo o uso de braquetes autoligáveis passivos personalizados e planejamento cirúrgico virtual, combinado com cirurgia ortognática de benefício antecipado, em um paciente com má oclusão de Classe III. Foram obtidos excelentes resultados faciais e oclusais em um tempo reduzido de tratamento, de 5 meses.
INTRODUCTION
Accurate surgical treatment starts with precise diagnosis, by evaluating all dimensions and determining the nature of deformity, because it might be a combination of hard and soft tissue components. 1
The main limitation of conventional surgical planning is its two-dimensional approach that involves clinical examination, extraoral and intraoral photographs, lateral and posteroanterior cephalograms, and plaster dental models. 2 , 3 To overcome these deficiencies, cone-beam computed tomography (CBCT) for imaging the craniofacial region brought a true paradigm shift from a two-dimensional to a three-dimensional (3D) approach. 4
Computer-aided surgical simulation (CASS) utilizing three-dimensional images obtained from multislice computed tomography (MSCT)/cone beam computer tomography (CBCT) has been successfully performed previously to plan craniofacial surgery.5-8 Also, CASS has been combined with the surgery-first approach (SFA) to demonstrate two useful and practical methods for planning these cases. 9
Furthermore, the patient can be virtually visualized by generating a fusion model with digital dental casts, a CBCT reconstructed bony volume and textured facial soft tissue image. 10 , 11 Additionally, with this fusion model the clinicians can accurately create surgical splints using the computer-aided design/computer-aided manufacturing (CAD/CAM) system for successful surgical treatments. 11 , 12
Recently, significant technological advancements have been made in computer-aided orthodontic treatment. In the Insignia system (Ormco Corporation, Orange County, CA), polyvinyl siloxane (PVS) impressions are digitized with computed tomography to produce highly detailed digital models, or an intraoral dental scanner is used to generate 3D digital models. The orthodontist adjusts the digital setup using a real-time 3D interface, while referring to the patient’s intra and extraoral photographs and radiographs for consideration of esthetic treatment goals. After the clinician approves the final setup, the customized brackets, tubes, and arch-wires are fabricated and bracket-positioning jigs are provided, for accurate indirect transfer. 13
In the present case report, 3D virtual customized bracket design (Insignia, Ormco Corporation, Orange County, CA) was integrated with 3D virtual surgical planning along with fabrication of digital surgical splints using a CAD/CAM technique. This article aims to report how the use of 3D digital technology, self-ligating brackets and the SFA can drastically reduce treatment time.
CASE REPORT
A 21-year-old Hispanic male reported to the orthodontist office with the primary complaint of not feeling comfortable with the bite and chin projection (Fig 1). A subsequent clinical examination showed that the profile had worsened since a previous orthodontic treatment.
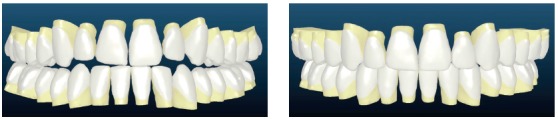
Figure 1. Pre-treatment photographs showing skeletal and dental Class III malocclusion.
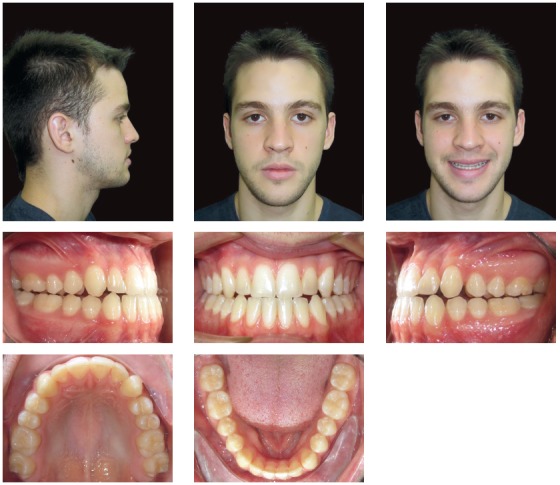
Systemically, he referred controlled Diabetes Mellitus Type I. The extraoral examination showed concave facial profile, with a slight maxillary hypoplasia, significant chin projection, upper lip retrusion and adequate nasolabial angle (Fig 1). Dentally, the patient presented a Class III malocclusion with proclined upper incisors and retroclined lower incisors, edge to edge bite, lower proper alignment and spacing of 2mm in the upper arch (Figs 1, 2, and 3A).The panoramic radiograph showed mild different ramus lengths (Fig 3B). Skeletally, Class III pattern with mandibular prognathism and macrognathism was observed (Fig 3A, 3C).
Figure 3. A) Pre-treatment lateral cephalometric radiograph. B) Pre-treatment panoramic radiograph. C) Pre-treatment lateral cephalometric tracing.
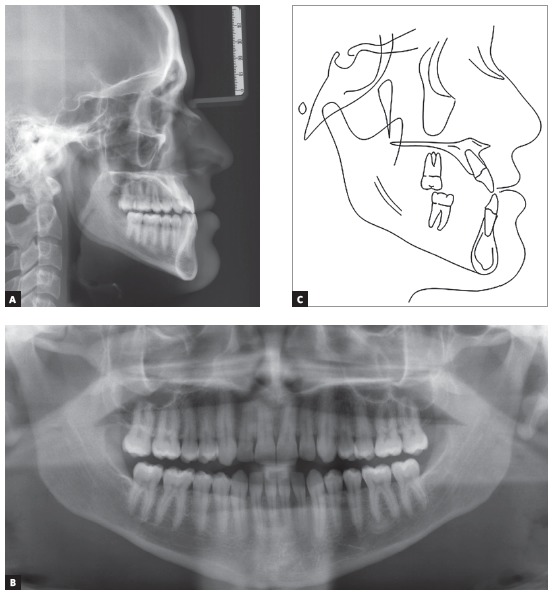
Figure 2. Pre-treatment dental casts.
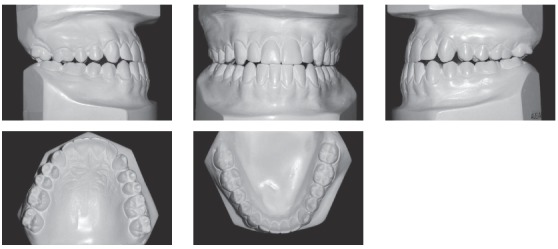
The treatment objectives were to correct the Class III skeletal pattern, to improve profile, to increase overjet and to improve facial aesthetics. The treatment options presented were presurgical orthodontic treatment followed by mandibular setback surgery and SFA with mandibular setback followed by fixed appliances to align, level and stabilize the occlusion. Considering that the patient’s chief concern was his facial esthetics, it was decided to proceed with SFA, because the patient wanted immediate facial change. This approach would avoid deterioration in his profile and malocclusion during presurgical orthodontics, and would also take advantage of the biological potential of the regional acceleratory phenomenon (RAP).
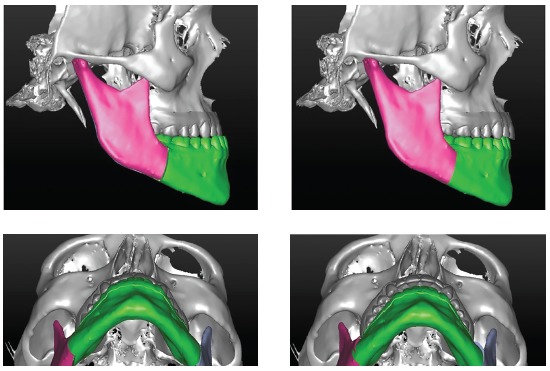
A computed tomography (CT) (Bright Speed Elite, General Electric, and Fairfield, Connecticut, USA) was taken for the construction of a model of the skull 8 with Proplan CMF (Materialise, Plymouth, MIs). The surgical plan was mandibular setback (Fig 4). The virtual design was transferred to the CAD/CAM software for production of surgical splints. The intermediate splint was physically generated by a 3D printer (Fortus 250mc, Stratasys, Eden Prairie, MN, USA) with hybrid epoxy-acrylate polymer.
Figure 4. Surgical planning of mandibular setback.
The first step in the Insignia system (Ormco Corporation, Orange, CA) for custom-designed orthodontics is to send precise polyvinyl siloxane impressions as well as photographic and radiographic information to the manufacturer. The brackets chosen were Insignia self-ligating (SL) brackets, which are the customized version of Damon Q SL brackets (Ormco Corporation, Orange, CA). 14 The final set-up for the patient was approved with an overcorrection of lower incisors positive torque, ensuring optimal expression of the lower incisors decompensation exploiting the massive RAP after orthognathic surgery (Fig 5). The selected sequence of wires was CuNiTi 0.014-in, CuNiTi 0.014 x 0.025-in, CuNiTi 0.018 x 0.025-in, TMA 0.019 x 0.025-in and stainless steel 0.019 x 0.025-in (Ormco Corporation, Orange, CA). The brackets were bonded three days before surgery and no archwire was placed.
Figure 5. Custom designed orthodontics, with Insignia.
In the day of the surgery, immediately before intubation assisted by a fiber optic probe, CuNiTi 0.014-in (Ormco Corporation, Orange, CA) archwires were placed (Fig 6). After mandibular setback surgery by sagittal osteotomy, under brain activity monitoring, and once a suitable rigid fixation and postoperative occlusion were established, ¼ 3.5 oz intermaxillary elastics were applied with Class III vector.
Figure 6. First archwire placed during the surgery.
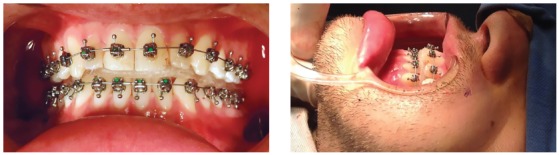
After 15 days, 1/8 3.5 oz intermaxillary elastics were used (Fig 7) and the archwires were changed to 0.014 x 0.025-in CuNiTi (Ormco Corporation, Orange, CA). One month after surgery 0.018 x 0.025-in CuNiTi archwires (Ormco Corporation, Orange, CA) were placed and Class III intermaxillary elastics were continued. Then, 0.019 x 0.025-in TMA arches (Ormco Corporation, Orange, CA) were placed six weeks later. The orthodontic treatment was completed five months after mandibular setback, showing great improvements in facial profile, Class I occlusion with ideal overjet and overbite (Figs 8, 9, and 10). The 24-month posttreatment photographs show excellent stability of the treatment results (Fig 11).
Figure 7. Class III intermaxillary elastics.
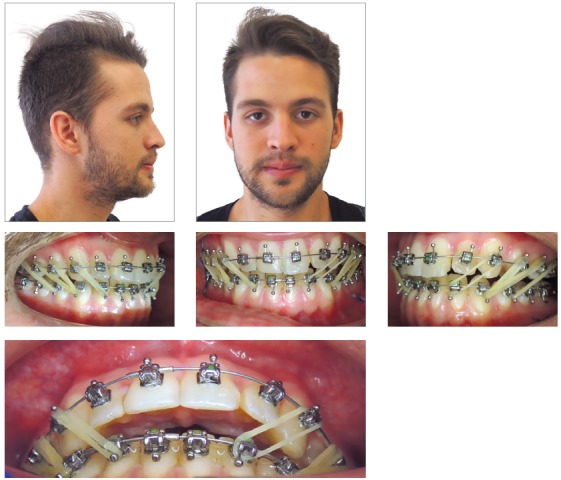
Figure 11. Follow-up photographs (24 months).
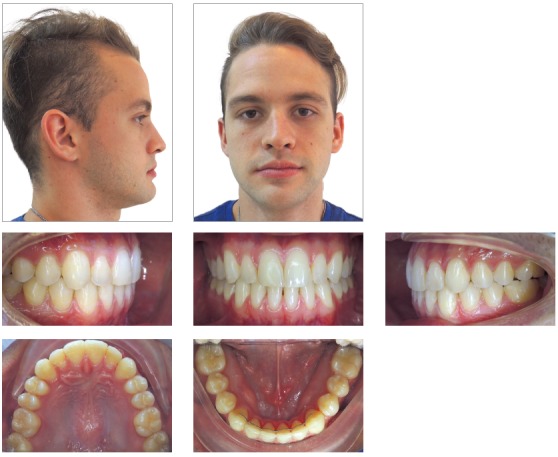
Figure 8. Post-treatment photographs.
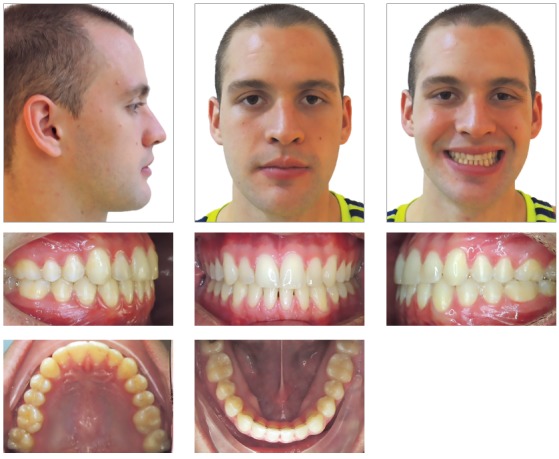
Figure 9. Post-treatment dental casts.
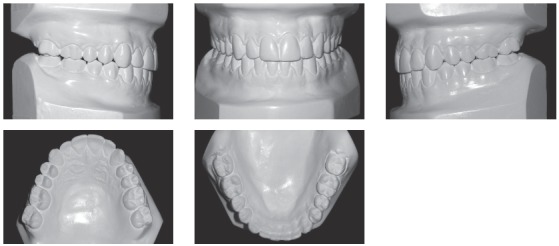
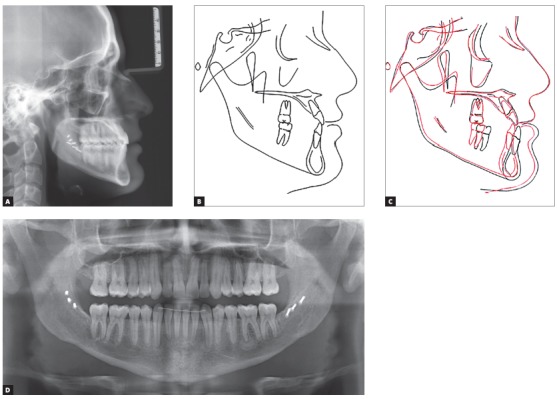
Figure 10. A) Post-treatment lateral cephalometric radiograph. B) Post-treatment cephalometric tracing. C) Superimposition of pre and post-treatment cephalometric tracings. D) Post-treatment panoramic radiograph.
DISCUSSION
Surgery-first approach (SFA) was first proposed by Nagasaka et al, 15 in 2009. With the orthognathic surgery performed before the orthodontic correction, total treatment time could be reduced to even less than the average period for presurgical orthodontics. 16 - 19 Considering the number of patients who want orthognathic surgery mainly for esthetic reasons and would appreciate a shorter treatment time, SFA offers an attractive alternative for managing skeletal malocclusions while improving patients’ self-esteem and function at the beginning of treatment. 20 , 21
The authors described several advantages offered by the surgery-first approach: (1) Improvement in patient’s facial esthetics and dental function in early treatment, rather than following a possible period of years, (2) improvement in patient’s swallowing and speech functions after surgery, (3) the proceeding of orthodontic tooth movement at a much faster pace following surgery, thus reducing the overall treatment time, (4) improved cooperation of the patient during orthodontic treatment, (5) easier orthodontic tooth movement following restoration of the normal functional and anatomic relationships of the bony skeleton and surrounding soft tissues; and (6) stability of results equal to, or in some cases superior to, those achieved using the traditional orthodontics-first approach. 22
Most articles recommended that orthodontic appliances should be placed prior to surgery, even when using a surgery-first approach. Studies reported bonding the orthodontic brackets immediately before, 15 , 23 1 week before,24-26 1 month before 27 - 29 or 1-2 months before30 surgery. Only one of the papers reported the total elimination of preoperative orthodontic treatment and the fitting of orthodontic brackets 10-14 days after surgery 20 Studies described that active orthodontic force can be applied before 26 - 29 or shortly after 15 , 23 - 25 , 30 surgery. Preoperative orthodontic preparation can, therefore, be started immediately before or approximately 1-2 months before surgery. Occasionally, it might be completely eliminated.
The shortest reported treatment time for postoperative orthodontic treatment was 4 months for correction of a skeletal Class III malocclusion with anterior open bite and dental crowding 26 and 4.5 months in the management of unilateral condylar hyperplasia, 11 similar to this case report, with total treatment time of 5 months. Most studies described completing postoperative orthodontic treatment within approximately 1 year 15 , 27 , 28 , 30 or in 6-9 months. 20 , 23 , 25 Treatment time was approximately 6-12 months shorter using the SFA, compared to using a conventional orthodontics-first approach. Only one study described similar treatment time (approximately 1.5 years) for both approaches. 29
There is no doubt that SFA requires precise and accurate diagnosis and planning. Post-surgical orthodontic movements must be carefully executed according to the surgical plan, which implies constant communication between orthodontist and oral surgeon.
To expedite post-surgical orthodontics, Insignia System (Ormco Corporation, Orange, CA) is an important tool for offering customized brackets and archwires, also diminishing errors from appliance positioning. Customized devices in orthodontics have been reported before. Subjects treated with SureSmile (OraMetrix, Richardson, Tex) were compared with those undergoing conventional orthodontic treatment, concluding that treatment time was 7 months shorter in patients treated with SureSmile. 31 Saxe et al 32 obtained comparable results. However, SureSmile technology (OraMetrix, Richardson, Tex) customizes only the archwires, using robotically-assisted archwire bending technology. 32 , 33 Insignia (Ormco Corporation, Orange County, CA) customizes bracket prescription, bonding and archwires. 14 Besides, the light forces produced by the passive self-ligating system with high-tech archwires will control the transverse dimension in coordination with post-surgical sagittal changes. 19
With two-dimensional (2D) imaging, the most usual problems are landmark identification, image distortion and magnification. 34 , 35 However 2D imaging remains as the gold standard for the craniofacial region. The 3D computer-assisted surgical planning benefits the specialists because it can predict surgical movements including translations in anteroposterior, lateral, and vertical directions, and rotations around the x-, y-, and z-axes, the so-called pitch, roll, and yaw rotations 36 and this is an undisputed advantage in determining the best treatment option.
CONCLUSIONS
» The 3D diagnostics, digital surgical planning and CAD/CAM customized bracket systems with passive self-ligation offer a more accurate alternative to improve the efficiency of orthodontic-surgical treatment.
» SFA helps to reduce treatment time, delivering aesthetic results from the beginning, which generates greater acceptance in surgical patients.
Footnotes
Patients displayed in this article previously approved the use of their facial and intraoral photographs.
REFERENCES
- 1.Cheong YW, Lo LJ. Facial asymmetry: etiology, evaluation, and management. Chang Gung Med J. 2011;34(4):341–351. [PubMed] [Google Scholar]
- 2.Schwartz HC. Efficient surgical management of mandibular asymmetry. J Oral MaxillofacSurg. 2011;69:645–654. doi: 10.1016/j.joms.2009.03.009. [DOI] [PubMed] [Google Scholar]
- 3.Baek SH, Cho IS, Chang YI, Kim MJ. Skeletodental factors affecting chin point deviation in female patients with Class III malocclusion and facial asymmetry a three-dimensional analysis using computed tomography. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2007;104(5):628–639. doi: 10.1016/j.tripleo.2007.03.002. [DOI] [PubMed] [Google Scholar]
- 4.Uribe F, Janakiraman N, Shafer D, Nanda R. Three-dimensional cone-beam computed tomography-based virtual treatment planning and fabrication of a surgical splint for asymmetric patients surgery first approach. Am J Orthod Dentofacial Orthop. 2013;144(5):748–758. doi: 10.1016/j.ajodo.2012.10.029. [DOI] [PubMed] [Google Scholar]
- 5.Gateno J, Xia JJ, Teichgraeber JF. Clinical feasibility of computer-aided surgical simulation (CASS) in the treatment of complex cranio- maxillofacial deformities. J Oral MaxillofacSurg. 2007;65:728–734. doi: 10.1016/j.joms.2006.04.001. [DOI] [PubMed] [Google Scholar]
- 6.Xia JJ, Gateno J, Teichgraeber JF, Christensen AM, Lasky RE, Lemoine JJ. Accuracy of the computer-aided surgical simulation (CASS) system in the treatment of patients with complex craniomaxillofacial deformity a pilot study. J Oral Maxillofac Surg. 2007;65(2):248–254. doi: 10.1016/j.joms.2006.10.005. [DOI] [PubMed] [Google Scholar]
- 7.Xia JJ, Shevchenko L, Gateno J, Teichgraeber JF, Taylor TD, Lasky RE, et al. Outcome study of computer-aided surgical simulation in the treatment of patients with craniomaxillofacial deformities. J Oral Maxillofac Surg. 2011;69(7):2014–2024. doi: 10.1016/j.joms.2011.02.018. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Xia JJ, McGrory JK, Gateno J, Teichgraeber JF, Dawson BC, Kennedy KA. A new method to orient 3-dimensional computed tomography models to the natural head position a clinical feasibility study. J Oral Maxillofac Surg. 2011;69(3):584–591. doi: 10.1016/j.joms.2010.10.034. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Hsu SS, Singhal D, Xia JJ, Gateno J, Lin C-H, Huang C-S. Planning the Surgery-first approach in Surgical- orthodontic treatment with a computer aided Surgical Simulation (CASS) Planning Protocol. J Taiwan Assoc Orthod. 2012;24(2):24–37. [Google Scholar]
- 10.Plooij JM, Maal TJ, Haers P, Borstlap WA, Kuijpers-Jagtman AM, Berge SJ. Digital three-dimensional image fusion processes for planning and evaluating orthodontics and orthognathic surgery. Int J Oral Maxillofac Surg. 2011;40(4):341–352. doi: 10.1016/j.ijom.2010.10.013. [DOI] [PubMed] [Google Scholar]
- 11.Janakiraman N, Feinberg M, Vishwanath M, NalakaJayaratne YS, Steinbacher DM. Integration of 3-dimensional surgical and orthodontic technologies with orthognathic "surgery-first" approach in the management of unilateral condylar hyperplasia. Am J Orthod Dentofacial Orthop. 2015;148(6):1054–1066. doi: 10.1016/j.ajodo.2015.08.012. [DOI] [PubMed] [Google Scholar]
- 12.Gateno J, Xia J, Teichgraeber JF, Rosen A, Hultgren B, Vadnais T. The precision of computer-generated surgical splints. J Oral Maxillofac Surg. 2003;61(7):814–817. doi: 10.1016/s0278-2391(03)00240-4. [DOI] [PubMed] [Google Scholar]
- 13.Breuning KH. Efficient tooth movement with new technologies for customized treatment. J Clin Orthod. 2011;45(5):257–262. [PubMed] [Google Scholar]
- 14.Gracco A, Stellini E, Parenti SI, Bonetti GA. Individualized orthodontic treatment the Insignia system. Orthod (Chic.) 2013;14(1):e88–e94. doi: 10.11607/ortho.929. [DOI] [PubMed] [Google Scholar]
- 15.Nagasaka H, Sugawara J, Kawamura H, Nanda R. "Surgery first" skeletal Class III correction using the Skeletal Anchorage System. J Clin Orthod. 2009;43(2):97–105. [PubMed] [Google Scholar]
- 16.Luther F, Morris DO, Hart C. Orthodontic preparation for orthognathic surgery how long does it take and why? A retrospective study. Br J Oral Maxillofac Surg. 2003;41(6):401–406. doi: 10.1016/s0266-4356(03)00163-3. [DOI] [PubMed] [Google Scholar]
- 17.Dowling PA, Espeland L, Kroonstad O, Stenvik A, Kelly A. Duration of orthodontic treatment involving orthognathic surgery. Int J Adult Orthod Orthog Surg. 1999;14(2):146–152. [PubMed] [Google Scholar]
- 18.Luther F, Morris DO, Karnezi K. Orthodontic treatment following orthognathic surgery How long does it take and why? A retrospective study J Oral Maxillofac Surg. 2007;65(10):1969–1976. doi: 10.1016/j.joms.2007.05.026. [DOI] [PubMed] [Google Scholar]
- 19.Aristizábal JF, Martínez Smit R, Villegas C. The "surgery first" approach with passive self-ligating brackets for expedited treatment of skeletal Class III malocclusion. J Clin Orthod. 2015;49(6):361–370. [PubMed] [Google Scholar]
- 20.Hernández-Alfaro F, Guijarro-Martínez R, Molina-Coral A, Badía-Escriche C. "Surgery first" in bimaxillary orthognathic surgery. J Oral Maxillofac Surg. 2011;69(6):e201–e207. doi: 10.1016/j.joms.2011.01.010. [DOI] [PubMed] [Google Scholar]
- 21.Peiró-Guijarro MA, Guijarro-Martínez R, Hernández-Alfaro F. Surgery first in orthognathicsurgery a systematicreview of theliterature. Am J Orthod Dentofacial Orthop. 2016;149(4):448–462. doi: 10.1016/j.ajodo.2015.09.022. [DOI] [PubMed] [Google Scholar]
- 22.Huang CS, Hsu SS, Chen YR. Systematic review of the surgery-first approach in orthognathic surgery. Biomed J. 2014;37(4):184–190. doi: 10.4103/2319-4170.126863. [DOI] [PubMed] [Google Scholar]
- 23.Sugawara J, Aymach Z, Nagasaka DH, Kawamura H, Nanda R. "Surgery first" orthognathics to correct a skeletal class II malocclusion with an impinging bite. J Clin Orthod. 2010;44(7):429–438. [PubMed] [Google Scholar]
- 24.Liou EJ, Chen PH, Wang YC, Yu CC, Huang CS, Chen YR. Surgery-first accelerated orthognathic surgery Orthodontic guidelines and setup for model surgery. J Oral Maxillofac Surg. 2011;69(3):771–780. doi: 10.1016/j.joms.2010.11.011. [DOI] [PubMed] [Google Scholar]
- 25.Villegas C, Uribe F, Sugawara J, Nanda R. Expedited correction of significant dentofacial asymmetry using a "surgery first" approach. J Clin Orthod. 2010;44(2):97–103. [PubMed] [Google Scholar]
- 26.Yu CC, Chen PH, Liou EJ, Huang CS, Chen YR. A Surgery-first approach in surgical-orthodontic treatment of mandibular prognathism- a case report. Chang Gung Med J. 2010;33(6):699–705. [PubMed] [Google Scholar]
- 27.Wang YC, Ko EW, Huang CS, Chen YR, Takano-Yamamoto T. Comparison of transverse dimensional changes in surgical skeletal Class III patients with and without presurgical orthodontics. J Oral Maxillofac Surg. 2010;68(8):1807–1812. doi: 10.1016/j.joms.2009.09.089. [DOI] [PubMed] [Google Scholar]
- 28.Liao YF, Chiu YT, Huang CS, Ko EW, Chen YR. Presurgical orthodontics versus no presurgical orthodontics Treatment outcome of surgical-orthodontic correction for skeletal class III open bite. Plast Reconstr Surg. 2010;126(6):2074–2083. doi: 10.1097/PRS.0b013e3181f52710. [DOI] [PubMed] [Google Scholar]
- 29.Ko EW, Hsu SS, Hsieh HY, Wang YC, Huang CS, Chen YR. Comparison of progressive cephalometric changes and postsurgical stability of skeletal Class III correction with and without presurgical orthodontic treatment. J Oral Maxillofac Surg. 2011;69(5):1469–1477. doi: 10.1016/j.joms.2010.07.022. [DOI] [PubMed] [Google Scholar]
- 30.Baek SH, Ahn HW, Kwon YH, Choi JY. Surgery-first approach in skeletal class III malocclusion treated with 2-jaw surgery evaluation of surgical movement and postoperative orthodontic treatment. J Craniofac Surg. 2010;21(2):332–338. doi: 10.1097/SCS.0b013e3181cf5fd4. [DOI] [PubMed] [Google Scholar]
- 31.Alford TJ, Roberts WE, Hartsfield JK, Jr, Eckert GJ, Snyder RJ. Clinical outcomes for patients finished with the SureSmile Method compared with conventional fixed orthodontic therapy. Angle Orthod. 2011;81(3):383–388. doi: 10.2319/071810-413.1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 32.Saxe AK, Louie LJ, Mah J. Efficiency and effectiveness of SureSmile. World J Orthod. 2010;11(1):16–22. [PubMed] [Google Scholar]
- 33.Mah J, Sachdeva R. Computer-assisted orthodontic treatment: the SureSmile process. Am J Orthod Dentofacial Orthop. 2001;120(1):85–87. doi: 10.1067/mod.2001.117686. [DOI] [PubMed] [Google Scholar]
- 34.Trpkova B, Major P, Prasad N, Nebbe B. Cephalometric landmarks identification and reproducibility a meta-analysis. Am J Orthod Dentofacial Orthop. 1997;112(2):165–170. doi: 10.1016/s0889-5406(97)70242-7. [DOI] [PubMed] [Google Scholar]
- 35.Timock AM, Cook V, McDonald T, Leo MC, Crowe J, Benninger BL. Accuracy and reliability of buccal bone height and thickness measurements from cone-beam computed tomography imaging. Am J Orthod Dentofacial Orthop. 2011;140(5):734–744. doi: 10.1016/j.ajodo.2011.06.021. [DOI] [PubMed] [Google Scholar]
- 36.Dorafshar AH, Brazio PS, Mundinger GS, Mohan R, Brown EN, Rodriguez ED. Found in space: computer-assisted orthognathic alignment of a total face allograft in six degrees of freedom. J Oral Maxillofac Surg. 2014;72(9):1788–1800. doi: 10.1016/j.joms.2014.01.016. [DOI] [PubMed] [Google Scholar]


