Abstract
BACKGROUND AND OBJECTIVES
β-thalassemia results from a deficiency of β-globin chains leading to an excess in α globin chains resulting in hypochromic microcytic red cells, ineffective erythropoiesis and hemolytic anemia. It is a result of a decline of HbF synthesis during the first year of life. F-cell levels are influenced by a sequence variant (C → T) at position −158 upstream of the -globin gene, so the frequency of the Xmnl Gγ polymorphism in Egyptian patients with β-thalassemia major needed evaluation to decide on the value of HbF augmentation drugs in treating Egyptian β-thalessemia.
DESIGN AND SETTING
A cross-sectional study including 30 β-thalassemia major patients diagnosed and attending the Pediatric Hematology Unit, Children’s University Hospital, Ain Shams University, Cairo, Egypt, in the period from October 2008 to October 2009.
PATIENTS AND METHODS
The 17 males and 13 females underwent a medical history and physical examination. Tests included a complete blood count, hemoglobin electrophoresis, serum ferritin, and detection of Xmnl Gγ polymorphism by PCR.
RESULTS
The mean (SD) age was [2]10.2 (6.9) years. The most frequent genotype observed was homozygosity for the absence of the site XmnI (−/−) in 96% of cases. Heterozygosity (+/−) genotype was detected in 4% of cases, while homozygosity for the site XmnI (+/+) genotype was absent. Genotype was not related to age at first transfusion, fetal hemoglobin level or transfusion frequency.
CONCLUSION
Despite the small sample size, the study demonstrated that Egyptian β-thalessemia patients have low frequency of positivity for the XmnI polymorphism whether in heterozygous (+/−) or homozygous (+/+) state.
Thalassemia syndromes are the most common hereditary chronic hemolytic anemia due to impaired globin chain synthesis.1 β-thalassemia results from a deficiency of β-globin chains which leads to an excess in α globin chains, resulting in hypochromic microcytic red cells, ineffective erythropoiesis and hemolyticanemia.2 Heterogeneity in the clinical manifestation of β-thalassemia diseases may occur from the nature of β-globin gene mutations, α-thalassemia gene interaction or differences in the amount of fetal hemoglobin (HbF) production.3 This condition is characterized by transfusion-dependent anemia, massive splenomegaly, bone deformities, growth retardation, and peculiar facies in untreated individuals.4 In Egypt, β-thalassemia is the most common form of chronic hemolytic anemia with a carrier rate varying from 5.3% to ≥ 9% and a gene frequency of 0.03. Thus, it has been estimated that 1000/1.5 million per year live births suffer from thalassemia disease in Egypt.5
Patients with homozygous β-thalassemia usually present during infancy between the age of 6 to 24 months. It becomes manifest as a result of decline of HbF synthesis during the first year of life.6 Increased levels of HbF (alpha 2 gamma 2), are of no consequence in healthy adults, but confer clinical benefits in patients with sickle cell anemia and in thalassemia patients7 who are mildly affected despite having minimal or no HbA.3 Inter-individual HbF variation is genetically controlled, caused by mutations involving the beta globin gene complex, historically referred to as pancellular hereditary persistence of fetal hemoglobin (HPFH)7 associated with large cluster deletions removing silencer elements from γ- to δ-globin gene regions or juxtaposing enhancer elements in proximity of γ-globin. These Mendelian forms of HPFH are rare and do not explain the common form of heterocellular HPFH which represents the upper tail of normal HbF variation, and is clearly inherited as a quantitative genetic trait.7 In nondeletional forms of HbF, a group of single point mutations in the γ-globin gene promoters are associated with increased γ-globin gene transcription, probably through mechanisms of increased competition for the locus control region (LCR) sequences respect to the adult globin genes or as a consequence of reduced binding of repressor factors. The switch from fetal to adult hemoglobin is incomplete; the residual HbF in adults is restricted to a subset of erythrocytes called F cells.8
Studies have shown F cells to be influenced by age, sex and a DNA sequence variant (C→T) at position −158 upstream of the Gγ-globin gene, referred to as the Xmnl Gγ polymorphism8–10 accounting for approximately 13% of the total F cells variance which has been strongly correlated with increased expression of the Gγ-globin gene and higher production of HbF.11 Epidemiologic studies have shown that the Xmnl Gγ polymorphism is common in several populations. The frequency of the Xmnl Gγ restriction site is approximately 0.33 in Europeans, and the genotype accounts for 13% to 32% of the total phenotypic variance.8 The Gγ-158 T variant predisposes toward increased HbF production in adult life, particularly in conditions of erythroid stress, such as β-thalassemia and sickle cell anemia.2,12
To date, there have been no reported studies on the molecular characterization and frequency of the Xmnl Gγ polymorphism in Egyptian β-thalassemia major patients, so this study aimed to assess the prevalence of Xmnl Gγ polymorphism in a cohort of Egyptian transfusion dependent β-thalassemia major patients and to study its impact on the clinical and laboratory presentations and transfusion requirements.
PATIENTS AND METHODS
Thirty patients with β-thalassemia major were diagnosed in the Pediatric Hematology Clinic of the Children’s Hospital by having hematological evidence of β-thalassemia: profound hypochromic anemia, morphologic red cell abnormalities, mean erythrocyte volume less than 75 fL and characteristic Hb electrophoresis. All patients underwent a complete medical history including recording of age, sex, consanguinity, age of first blood transfusion, frequency of blood transfusion and thorough clinical examination. Laboratory investigations included a complete blood count (Coulter Counter GEM-S, Beckman Coulter Inc., Miami, Florida, United States), Hb electrophoresis (using high performance liquid chromatography (HPLC) (VARIANT; Bio-Rad Laboratories, Hercules, California, United States), serum ferritin using enzyme linked immunosorbant assay (ELISA), serum transaminases, bilirubin (total and direct) and creatinine were done by Autoanalyser Hitachi 917. Detection of Xmnl Gγ polymorphism by PCR was performed as follows: DNA was extracted by using a spin column QIA amp blood kit (Qiagen, Hilden, Germany). PCR amplification and enzymatic digestion of the products was done. Genomic DNA of 0.5 to 2 mg was amplified with each forward primer 5′-AAC TGT TGC TTT ATA GGA TTTT-3′ and reverse primer 5′-AGG AGC TT A TT G ATA ACT CAG AC-3′ at a final concentration 20 pmol each (Biosynthesism Lewisville, Texas, United States). PCR was performed with a Biometra Thermoblock, Göttingen, Germany)under conditions of initial denaturation at 95°C for 5 min, followed by 30 cycles of denaturation at 95°C for 1min, annealing at 60°C for 1 minute and elongation at 72°C for 1.5 min with a final extension at 72°C for 3 minutes. After amplification the PCR product was digested with a restriction endonuclease Xmnl and electrophoresed in a 2% agarose gel. The study was performed with the understanding and consent of each patient and/or parent, and after the approval of the ethical committee of the Pediatric department, Faculty of Medicine, Ain Shams University.
The data were coded, entered and processed on a computer using SPSS (version 15, IBM Corp, Armonk, New York, United States). The level P<.05 was considered the cutoff value for significance. The t test was used to assess the statistical significance difference between two population means in a study involving independent samples.
RESULTS
The results are shown in Tables 1 to 3 and Figure 1. The age of the study group ranged from 6 months to 19 years with a mean age of 10.2 (6.9) years. The age of first blood transfusion ranged from 6 months to 1 year of age. The mean HbF level, pretransfusion Hb, platelet count, serum ferritin and alanine transaminase level are shown in Table 1.
Table 1.
Demographic and laboratory data of the patients.
| Variable | Mean | Standard deviation | Range | |
|---|---|---|---|---|
|
| ||||
| Age (years) | 10.2 | 6.9 | 0.5 | 19.0 |
| Age of 1st transfusion (months) | 15.2 | 14.3 | 6.0 | 12.0 |
| Hemoglobin (Hb) F level % | 40.4 | 26.2 | 1.0 | 95.3 |
| Pretransfusion Hb (gm/dl) | 7.8 | 1.1 | 6.0 | 8.5 |
| Mean corpuscular volume (fL) | 62.2 | 8.0 | 52.0 | 65.8 |
| Platelets (×1000/mm3) | 316.6 | 195.2 | 301 | 834.0 |
| Serum ferritin (ng/mL) | 1394.1 | 1217.0 | 550 | 5282.0 |
| Alanine aminotransferase (U/L) | 72.6 | 90.5 | 8.4 | 313.0 |
| Aspartate aminotransferase (U/L) | 51.7 | 61.1 | 7.8 | 230.0 |
Table 3.
Comparison between patients with XmnI polymorphism (−/−) and (+/−) (n=25).
| XmnI Gγ −/− (24) patients | XmnI Gγ −/+ (1) patient | P | |||
|---|---|---|---|---|---|
|
| |||||
| Mean | SD | Mean | SD | ||
| HbF level (%) | 41.9 | 26.5 | 71.0 | - | .2 |
| Mean corpuscular volume (fL) | 52.0 | 8.2 | 65.8 | - | .2 |
| Age at 1st transfusion (months) | 15.6 | 14.9 | 5.0 | - | .1 |
| Transfusion indexa | 12.5 | 29 | 135 | - | .12 |
Transfusion requirements in mL/kg/year of packed red cells
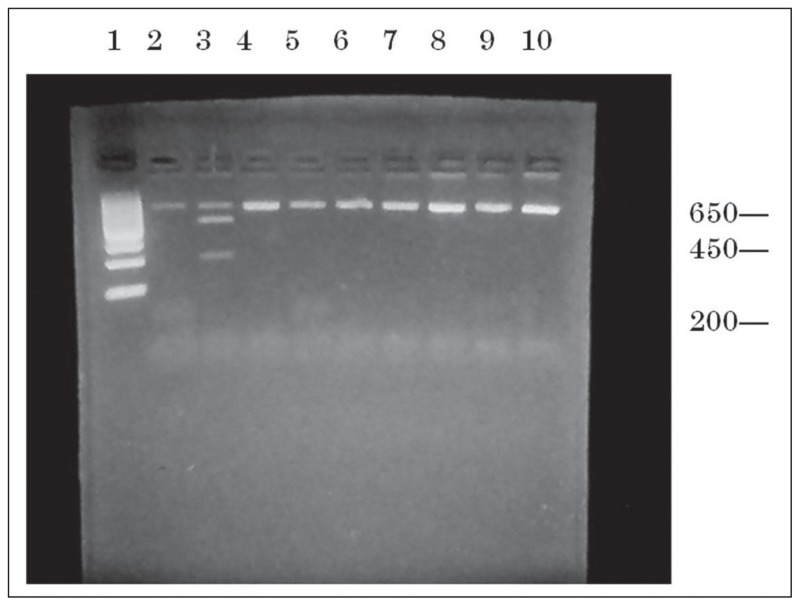
Figure 1.
Electrophoresis of amplified DNA after digestion with XmnI for the detection of Gγ XmnI polymorphism genotypes. Lane 1: 100 bp DNA ladder. Lane2 and 4–0: 650 bp fragment from patients with XmnI (−/−) genotype. Lane 3: 650 bp, 450 bp and 200 bp fragment from a patient heterozygous for the XmnI (+/−) genotype.
DNA amplification of the 650-bp sequence from the promoter region in the Gγ-globin gene using the PCR protocol developed products with an absence of non-specific bands in 25 patients while amplification failed in 5 samples (most probably the failed samples were contaminated with DNases; DNase can clip a desired DNA template molecule into fragments which would be unsuitable for PCR). Digestion of PCR products with Xmnl produced bands of 450 bp and 200 bp when both chromosomes possessed the Xmnl polymorphic site (+/+); absence of the Xmnl site in both chromosomes (−/−) showed only the original undigested 650- bp fragment. Bands of 650 bp, 450 bp and 200 bp were observed when only one chromosome possessed the site (+/−) (Figure 1, Table 2).
Table 2.
Xmnl Gγ polymorphism of the patients.
| Number of patients (30) | Percentage | |
|---|---|---|
|
| ||
| Failed DNA amplification | 5 | 16.7% |
| XmnI Gγ −/− | 24 | 80.0% |
| XmnI Gγ −/+ | 1 | 3.3% |
The Xmnl Gγ polymorphism in patients (n=25) showed that the most frequent genotype was absence of an Xmnl cleavage site in both chromosomes (−/−) in 80%, while the presence of Xmnl site in one chromosome (−/+) was observed in only one female patient (4%). This patient was 13 years old, and had developed early hepatosplenomegaly and transfusion dependency since the age of 6 months and had a mean HbF of 71%. She had negative screening tests for co-inheritance of G6PD deficiency or other hemoglobinopathies (Table 3).
DISCUSSION
In Egypt, β-thalassemia is the most common genetically determined chronic hemolytic anemia.6 The severity of β-thalassemia is remarkable for its variability in different populations, even in different patients.13 The 158(C-T) polymorphism of the Gγ-globin gene (Xmnl polymorphism) is known to ameliorate the severity of the disease because of its strong association with an increased production of HbF.2,3 HbF production can partially compensate for the lack of adult hemoglobin (HbA) in patients with β-thalassemia major or intermedia. 11,12 In the present study, the most frequent genotype observed was homozygosity for the absence of the Xmnl site (−/−) in 96% of cases; heterozygosity (+/−) was detected in 4% of cases, while the homozygosity (+/+) genotype was absent. Similarly, in India, Sharma et al 201014 reported the Xmnl Gγ status in β-thalassemia major patients to be −/− in 66.9%, +/− in 26.1% and +/+ in 6.9% patients, with the −/− genotype being most common. However, marked ethnic variations have been reported in Malaysia by Wong et al, 2006;12 they reported homozygosity for Xmnl genotype (−/−) in 89.7% of Chinese β-thalassemia patients, heterozygosity for (+/−) genotype in 10.3% of patients and homozygosity for (+/+) genotype in 0% of Chinese patients. In Malays β-thalassemia patients, the homozygosity (−/−) genotype was present in 28.6%, heterozygosity in (+/−) in 63.3% and homozygosity (+/+) in 3.7% of patients. In Iranians, Kosaryan et al15 found that 76% of β-thalassemia patients had either (+/−) or (+/+) for Xmnl limiting enzyme polymorphism. A previous study by Kaddah et al16 reported positivity for 158 Xmnl polymorphism only in 2 of 22 (9%) Egyptian thalassemia intermedia patients, a value which is not significantly higher than the 4% heterozygous positivity in our β-thalassemia patients. This finding coincides with the conclusion of Neishabury et al17 that the frequency of positive Xmnl Gγ polymorphism did not show a statistically significant difference between thalassemia major and intermedia cases in an Iranian study. The present study found that one patient with Xmnl Gγ (−/+) showed a high HbF level (71%), but she started transfusion dependency very early at the age of five months. Kosaryan et al15 postulated that the presence of the Xmnl polymorphism under the condition of hematopoietic stress might contribute to overproduction of HbF, causing mild features of the hemolytic β-thalassemia, but this was not true for our patient who despite having high HbF level had an early and severe hemolytic disease. The early age at first transfusion of this patient does not coincide with the results of Sharma et al,14 who reported that Xmn-1(G) gamma −/− patients presented before 1 year of age and the mean age of presentation of +/+ patients was 18.3 months.
HU therapy has been successfully used in thalassemia intermedia patients and was associated with a significant improvement in hematological parameters and quality of life.18,19 Hydroxyurea efficacy in β-thalassemia major has been variable in different studies.20–22 Although Kosaryan et al15 suggested that β-thalassemia major or intermedia with Xmnl polymorphism of (+/−) show better response to hydroxyurea therapy than (−/−) genotype, this finding was not proved by other studies. Italia et al22 and Ehsani et al19 demonstrated that Xmnl polymorphism was not the only predictor of good hematological response to hydroxyurea in thalassemia patients.
Despite the small sample size, the study demonstrates that Egyptian b-thalassemia major patients have low frequency for the positivity of the Xmnl polymorphism whether in the heterozygous (+/−) or homozygous (+/+) state. Molecular determination of genetic markers in early childhood (eg, Xmnl) is recommended to identify the prognostic value of such mutations in determining the spectrum and severity of clinical disease and variability in management. A large clinical trial using hydroxyurea in Egyptian patients with β-thalassemia with and without the Xmnl mutation, is required to evaluate the efficacy of hydroxyurea in this population of thalassemics. The authors declare that there is no conflict of interest.
REFERENCES
- 1.Rund D, Rachmilewitz E. β-thalassemia. N Engl J Med. 2005;353(11):1135–1146. doi: 10.1056/NEJMra050436. [DOI] [PubMed] [Google Scholar]
- 2.Agouti I, Badens C, Abouyoub A, Khattab M, Sayah F, Barakat A, Bennani M. Genotypic correlation between six common moroccan mutations of beta-thalassemia and XMN-I polymorphism. Hemoglobin. 2007;31(2):141–149. doi: 10.1080/03630260701285050. [DOI] [PubMed] [Google Scholar]
- 3.Winichagoon P, Fucharoen S, Chen P, Wasi P. Genetic factors affecting clinical severity in betathalassemia syndromes. 2007;22(6):573–580. doi: 10.1097/00043426-200011000-00026. [DOI] [PubMed] [Google Scholar]
- 4.Christoforidis A, Haritandi A, Tsatra I, Tsitourides I, Karyd S, Athanassiou-Metaxa M. Four- year evaluation of myocardial and liver iron assessed prospectively with serial MRI scans in young patients with β-thalassemia major: comparison between different chelation regimens. Eur J of Haemat. 2007;78(1):52–57. doi: 10.1111/j.0902-4441.2006.t01-1-EJH3013.x. [DOI] [PubMed] [Google Scholar]
- 5.El-Beshlawy A, Youssry I. Prevention of hemoglobinopathies in Egypt. Hemoglobin. 2009;33(1):S14–20. doi: 10.3109/03630260903346395. [DOI] [PubMed] [Google Scholar]
- 6.Beutler E, Hoffbrand AV, Cook JD. Iron deficiency and overload. Hematology Am Soc Hematol Educ Program. 2003:40–61. doi: 10.1182/asheducation-2003.1.40. [DOI] [PubMed] [Google Scholar]
- 7.Thein SL, Menzel S, Lathrop M, Garner C. Control of fetal hemoglobin: new insights emerging from genomics and clinical implications. Hum Mol Genet. 2009;18(R2):R216–223. doi: 10.1093/hmg/ddp401. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Sampietro M, Thein SL, Contreras M, Pazmany L. Variation of HbF and F-cell number with the G-gamma X mnI (C-T) polymorphism in normal individuals. Blood. 1992;79(3):832–833. [PubMed] [Google Scholar]
- 9.Shimmoto MM, Vicari P, Fernandes AC, Guimarães GS, Figueiredo MS. XmnI polymorphism is associated with fetal hemoglobin levels in hypoplastic syndromes. Sao Paulo Med J. 2006;124(2):110–111. doi: 10.1590/S1516-31802006000200012. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Nemati H, Rahimi Z, Bahrami G. The Xmn1 polymorphic site 5′ to the (G)gamma gene and its correlation to the (G)gamma:(A)gamma ratio, age at first blood transfusion and clinical features in beta-thalassemia patients from Western Iran. Mol Biol Rep. 2010;37(1):159–164. doi: 10.1007/s11033-009-9566-7. [DOI] [PubMed] [Google Scholar]
- 11.Garner C, Silver N, Best S, Menzel S, Martin C, Spector TD, Thein SL. Quantitative trait locus on chromosome 8q influences the switch from fetal to adult hemoglobin. Blood. 2004;104(7):2184–2186. doi: 10.1182/blood-2004-02-0527. [DOI] [PubMed] [Google Scholar]
- 12.Wong YC, George E, Tan KL, Yap SF, Chan LL, Tan MA. Molecular characterisation and frequency of Gγ Xmn I polymorphism in Chinese and Malay β-thalassaemia patients in Malaysia. Malaysian J Pathol. 2006;28(1):17–21. [PubMed] [Google Scholar]
- 13.Haghi M, Feizi AA, Harteveld CL, Pouladi N, Feizi MA. Homozygosity for a rare beta 0-thalassemia mutation [frameshift codons 25/26 (+T)] causes beta-thalassemia intermedia in an Iranian family. Hemoglobin. 2009;33(1):75–80. doi: 10.1080/03630260802683377. [DOI] [PubMed] [Google Scholar]
- 14.Sharma N, Das R, Kaur J, Ahluwalia J, Trehan A, Bansal D, Panigrahi I, Marwaha RK. Evaluation of the genetic basis of phenotypic heterogeneity in north Indian patients with thalassemia major. Eur J Haematol. 2010;84(6):531–537. doi: 10.1111/j.1600-0609.2010.01422.x. [DOI] [PubMed] [Google Scholar]
- 15.Kosaryan M, Vahidshahi K, Karami H, Ehteshami S. Effect of Hydroxyurea on Thalassemia Major and Thalassemia Intermedia in Iranian Patients. Pak J Med Sci. 2009;25(1):74–78. [Google Scholar]
- 16.Kaddah N, Rizk S, Kaddah AM, Salama K, Lotfy H. Study of possible genetic factors determining the clinical picture of Thalassemia Intermedia. J Med Sci. 2009;9:151–155. [Google Scholar]
- 17.Neishabury M, Azarkeivan A, Najmabadi H. Frequency of positive Xmnl Ggamma polymorphism and coinheritance of common alpha thalassemia mutations do not show statistically significant difference between thalassemia major and intermedia cases with homozygous IVSII -1 mutation. Blood Cells Mol Dis. 2010;44(2):95–99. doi: 10.1016/j.bcmd.2009.10.007. [DOI] [PubMed] [Google Scholar]
- 18.Mokhtar GM, Tantawy AA, Adly AA, Ismail EA. Clinicopathological and Radiological Study of Egyptian β-Thalassemia Intermedia and β-Thalassemia Major Patients: Relation to Complications and Response to Therapy. Hemoglobin. 2011;35(4):382–405. doi: 10.3109/03630269.2011.598985. [DOI] [PubMed] [Google Scholar]
- 19.Ehsani MA, Hedayati-Asl AA, Bagheri A, Zeinali S, Rashidi A. Hydroxyurea-induced hematological response in transfusion-independent beta-thalassemia intermedia: case series and review of literature. Pediatr Hematol Oncol. 2009;26(8):560–565. doi: 10.3109/08880010903271671. [DOI] [PubMed] [Google Scholar]
- 20.Ansari SH, Shamsi TS, Ashraf M, Perveen K, Farzana T, Bohray M, Erum S, Mehboob T. Efficacy of hydroxyurea in providing transfusion independence in β-thalassemia. J Pediatr Hematol Oncol. 2011;33(5):339–343. doi: 10.1097/MPH.0b013e31821b0770. [DOI] [PubMed] [Google Scholar]
- 21.Zamani F, Shakeri R, Eslami SM, Razavi SM, Basi A. Hydroxyurea therapy in 49 patients with major beta-thalassemia. Arch Iran Med. 2009;12(3):295–297. [PubMed] [Google Scholar]
- 22.Italia KY, Jijina FJ, Merchant R, Panjwani S, Nadkarni AH, Sawant PM, Nair SB, Ghosh K, Colah RB. Response to hydroxyurea in beta thalassemia major and intermedia: experience in western India. Clin Chim Acta. 2009 Sep;407(1–2):10–15. doi: 10.1016/j.cca.2009.06.019. [DOI] [PubMed] [Google Scholar]