Editor’s Note
Every whiff you take not only brings a cloud of chemicals swirling up your nose, but matters to your experience of taste as well as smell. Scientists studying smell have not only provided compelling evidence that it’s more sophisticated than previously thought, but believe that the sense of smell impacts our mood and behavior and has the potential to detect and treat some neurological disorders. Compared to other senses, smell has long been underappreciated, writes our author, but that is now beginning to change.
In many ways, the sense of smell—also known as olfaction (from the Latin word for smell or odor, olfactorius)—is our most complex sensory system, capable of distinguishing thousands, if not millions, of different odors, often at concentrations below those detectable by sophisticated instruments. The biological machinery required for such a feat is remarkable, involving six to ten million odorant receptor cells embedded within a thin layer of tissue (epithelium) high in the nasal chambers. Each receptor cell projects 10 to 30 thread-like cilia into the mucus covering the epithelium (see figure 1 below).
Figure 1.
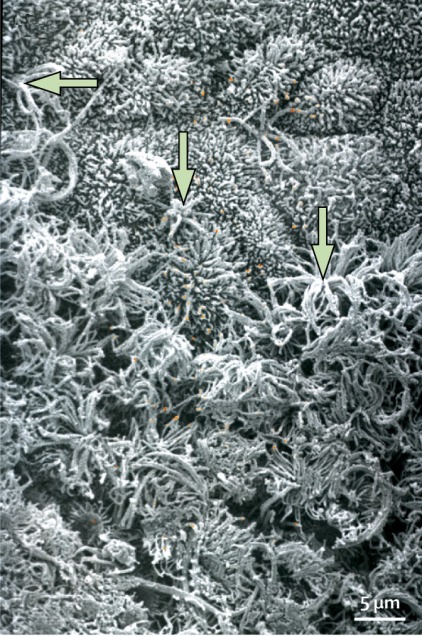
A transition region between the human olfactory neuroepithelium (bottom) and the respiratory epithelium (top). Arrows identify olfactory receptor cell dendritic endings with cilia, some of which are cut off. (From Menco and Morrison.49 Copyright © 2003 Richard L Doty.)
These cilia carry receptors—protein structures specialized to respond to odor-carrying molecules, termed odorants. There are nearly 400 types of receptors, different subsets of which are triggered by different odorants. Each of the olfactory receptor cells contains only one type of receptor. When enough odorant molecules get through the mucus layer and bind to the receptors located on the receptor cell cilia, they stimulate a neural impulse. The pattern of activated receptors is specific to a given odorant, and the neural impulses that are generated are decoded by higher brain regions. Memory processes also become involved, allowing us to recognize odor sensations of which we are familiar.
The major breakthrough for understanding the first phase of olfactory transduction came in 1991 when Linda Buck and Richard Axel at Columbia University published their seminal paper identifying the gene family responsible for the expression of the olfactory receptors.1 Their work, which led to the 2004 Nobel Prize in Medicine or Physiology, put to rest questions as to the nature of initial olfactory transduction that had puzzled scientists for hundreds of years.
Since then the situation has become much more complex, with ever more types of receptors being found on some olfactory receptor cells,2 and the realization that olfactory receptors are present in tissues throughout the body. These include the skin,3 skeletal muscle,4 thyroid,5 heart,6 lungs,7 pancreas,8 thymus,9 prostate,10 kidney,11 bladder,9 testes,5 intestine,12 blood vessels,13 and ganglia of the autonomic nervous system.13 Their widespread distribution raises the question of whether these receptors should, indeed, be called “olfactory.” Depending upon their location, they are involved in many biological and physiological processes, including glucose homeostasis, lung ventilation, regulation of blood pressure, mitigation of tumor progression, promotion of angiogenesis, facilitation of sperm motility, induction of wound healing, and alteration of gut motility and secretion.14 Understanding the role of such receptors in these diverse processes is opening new vistas for novel pharmacological approaches to disease management and treatment.
The Underrated Sense
Although most of us take our sense of smell for granted, it is critical for our well-being. We use olfaction to verify the cleanliness of our clothes and homes, and to fully enjoy foods, beverages, personal care products, flowers, and other aspects of our environment. Without a sense of smell, we are exposed to the dangers of spoiled food, leaking natural gas, burning electrical wires, smoke, and other environmental hazards. The sense of smell is so important that those who can’t smell (anosmics) are disqualified for “appointment, enlistment, and induction” into the US Armed Forces. Indeed, the lack of smell ability can be the basis for retirement or discharge.15
Multiple factors influence our ability to smell. These include occupation (e.g., perfumers and master sommeliers perform better than most of us on olfactory tests), sex, age, exercise, smoking, nutrition, head trauma, disease, and exposures to viruses, bacteria, and xenobiotics.16 The influence of age on smell function is particularly salient. More than three-quarters of individuals over the age of 80 have a demonstrable smell problem, usually reduced sensitivity.17 This decrease is illustrated below (see Figure 2 below), where a major drop occurs in later life in scores on the University of Pennsylvania Smell Identification Test (UPSIT), a 40-odor smell test developed at our center in the early 1980s (Figure 3).18 (Note in Figure 2 that women, on average, outperform men on this test and maintain their superiority into later life.) Over the age of 85 years, 40 percent of men and 26 percent of women are anosmic, i.e., have no sense of smell at all.19
Figure 2.
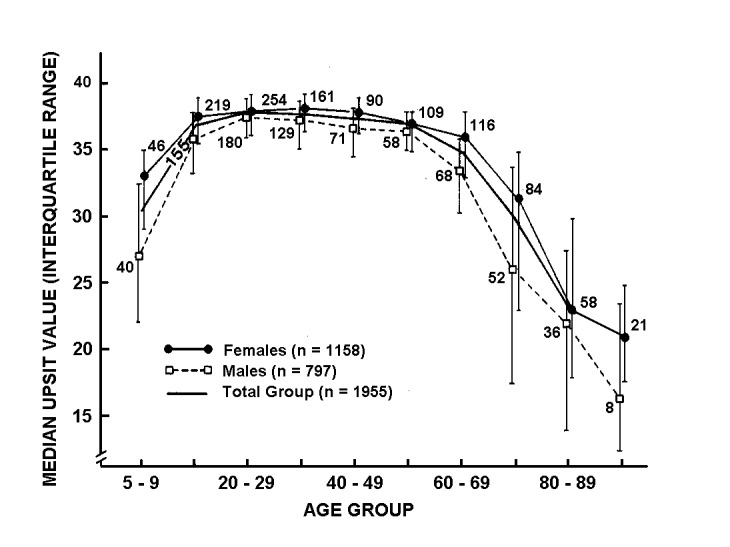
University of Pennsylvania Smell Identification (UPSIT) scores as a function of age and sex. Note that women identify odorants better than men at all ages although significant overlap occurs. Numbers by data points indicate sample sizes. (From Doty and colleagues.17 Copyright 1984 American Association for the Advancement of Science.)
Figure 3.

The University of Pennsylvania Smell Identification Test can be self-administered and is comprised of four booklets, each of which contains 10 ‘scratch and sniff’ odorants. The subject’s task is to identify the smell of each odorant based upon cued alternatives. Norms based upon 4,000 subjects are available for this test which has been translated into 30 different languages and administered to over one million people. (Photo courtesy of Sensonics, International. Copyright © 2004, Sensonics International, Haddon Heights, NJ.)
Taste versus Smell
It is noteworthy that many patients who come to our center’s clinic for evaluation and treatment do not recognize that they have a smell problem, complaining only of a “taste” problem. However, when we formally test them, their ability to smell proves to be the culprit. Why? Because the taste buds, located throughout the oral cavity but primarily on the tongue, sense only sweet, sour, bitter, salty, and savory (“umami) sensations. Everything else we think of as taste, such as strawberry, apple, chocolate, coffee, butterscotch, meat sauce, and apple pie, are really flavors that depend upon the sense of smell.
This is easily demonstrated. The next time you sip your coffee, pinch your nose closed while swishing the coffee around in your mouth. You will notice the bitterness of the coffee, its warmth and smoothness, but not the distinctive coffee flavor. Indeed, the sensation is much like swishing bitter hot water. The reason why the coffee “taste” disappears is that, by holding your nose shut, you block the flow of coffee flavor molecules from the rear of the oral cavity to the olfactory receptors via the nasopharyx, the opening from the mouth into the nose.
I was once asked to visit a large retirement home to better understand why there was concern about bad tasting food. The situation was quite dire, since some residents had largely refused to eat the food and a few were wasting away. Such turmoil arose around this issue that many of the residents were on a campaign to have the chef fired. The chef eventually quit, but the problem continued even after a new chef had come on board. I had the opportunity to give a lecture to 100 or so of the residents on nutrition and the chemical senses, and passed out the UPSIT for them to take immediately after my talk. It was at this time that most of the residents discovered they could not smell very well, with most exhibiting hyposmia (decreased smell function), and that the problem with the institution’s food was largely in their noses, not in the kitchen!
Smelling Danger
Aside from altered perception of the flavor of foods and attendant nutritional issues, the loss of smell function that most of us experience in our later years has potentially lethal consequences. This is evidenced by the disproportionate number of elderly people who have died in accidental gas poisonings, in part because of their inability to detect the odor added as a safety factor to natural gas.20 Most of us have, at some time in our lives, used this sense to avert a danger from something burning on the stove, a smoldering wire in an electrical outlet, or gas from a stove that was not completely turned off. In a study of over 1,000 persons conducted by the Medical College of Virginia, anosmics were three times more likely than those with a normal sense of smell to report having experienced a potentially life-threatening event such as the ingestion of spoiled food or a failure to detect smoke or leaking natural gas.21
Recent studies suggest that smell loss is an extremely strong risk factor for death in healthy older persons, increasing the odds of dying by more than 300 percent over a four-to five-year period.22 Although the reasons behind the association have yet to be determined, smell loss is a stronger predictor of death than cognitive deficits, cancer, stroke, lung disease, or hypertension, even after controlling for sex, age, race, education, socioeconomic status, smoking behavior, cardiovascular disease, diabetes, and liver damage.22, 23
Independent of age, we now know that smell dysfunction heralds the onset of a number of neurological diseases, including Alzheimer’s and Parkinson’s diseases.24 In some cases, such dysfunction occurs years, even decades, before the appearance of the classic disease symptoms. The olfactory bulb—a structure at the base of the brain that receives information from the olfactory receptor neurons—is among the two brain regions that first show disease-related pathology in Parkinson’s disease.25 Although damage to the olfactory bulb also occurs in early Alzheimer’s disease, some studies suggest that disrupted connections between the olfactory cortex and the hippocampus, which is involved in memory, predate it.25 Factors including damage to neurotransmitter systems critical for olfactory function may precede the development of the neuropathology of such diseases, possibly even catalyzing disease development itself.26
Impact on Memory
We and others have observed a close relationship between the ability to smell and memory: older persons with olfactory loss are more likely to report difficulties in memory.27 In a study of 1,092 non-demented elderly persons (average age 80 years) from a multi-ethnic community in New York, UPSIT scores varied with the degree of memory impairment and with performance on a number of cognitive tests.28 Importantly, such scores were weakly correlated with the MRI-determined volume of the hippocampus, a brain structure intimately associated with memory.
Numerous longitudinal studies have demonstrated that olfactory deficits are associated with future cognitive decline and Alzheimer’s disease in older populations.29 Moreover, interactions with genetics have also been demonstrated. In 1999, Amy Bornstein Graves and her associates at the University of South Florida published a pioneering study in which a 12-odor version of the UPSIT was administered to 1,604 community-dwelling senior citizens. None initially showed any signs of dementia.30 The smell test scores were found to be a better predictor of cognitive decline over the study’s two-year period than scores on a global cognitive test. Persons with normal smell function who carried one or two APOE-4 alleles (a risk factor for Alzheimer’s disease) had only a slight elevation in risk of developing cognitive decline. However, anosmic carriers of such alleles had a five-fold risk in developing cognitive decline during this time period. While this risk was approximately three-fold in men, it was nearly 10-fold in women.
Close relatives of patients with Alzheimer’s disease appear to have poorer smell function than non-relatives of the same sex and age, implying that genetic factors may be at play.31 However, the potential influences of interactions between environmental factors and genes, including the APOE-4 allele, cannot be overlooked. Using the UPSIT, Calderon-Garciduenas and her colleagues in Mexico City found olfactory dysfunction in 35.5 percent of 62 young persons (average age 21 years) living in a highly polluted area of that city, as compared to only 12 percent of those living in a much less polluted city.32 Interestingly, APOE-4 carriers from the polluted areas failed to identify 24 percent on the 10 items reported to be particularly sensitive to Alzheimer’s disease,33 whereas carriers of the APOE 2/3 and 3/3 alleles, which are not risk factors for Alzheimer’s disease, failed only 13.6 percent of such items, suggesting that AOE-4 gene carriers are more susceptible to adverse influences of pollution on their olfactory pathways.
Association with Parkinson’s
In the 1990s, G. Webster Ross and his collaborators at the University of Hawaii administered the 12-item version of the UPSIT to 2,276 non-symptomatic elderly men (average age: 80) of Japanese ancestry.34 Over the next four years, 35 were clinically diagnosed with Parkinson’s disease, a disorder whose motor dysfunction is due to damage to areas of the brain that employ the neurotransmitter dopamine for motor control. After adjusting for age, smoking behavior, and other confounders, those persons whose initial olfactory test scores fell within the bottom 25 percent of the group were five times more likely to develop Parkinson’s disease than those whose test scores fell within the top 25 percent.
Additional support for early olfactory involvement in Parkinson’s disease came from a 2004 study performed at the Vrije Universiteit (VU University) in Amsterdam. In this study, olfactory tests were administered to 361 asymptomatic first-degree relatives of Parkinson’s disease patients.35 The health of regions of the brain involved in motor control also was determined using single photon emission tomography (SPECT) imaging. This procedure measures the concentration of dopamine transporter, the protein responsible for returning the neurotransmitter into cells after its release into the synaptic cleft (see Figure 4). Those with the best (top 10 percent) and worse (bottom 10 percent) olfactory test scores were followed over time to determine who developed Parkinson’s disease.
Figure 4.
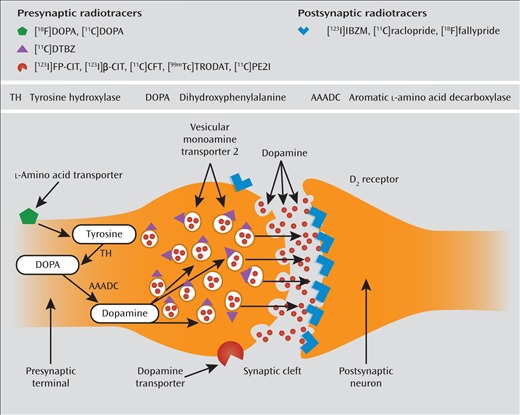
Illustration of the location of the dopamine transporter on the pre-synaptic membrane of a dopaminergic cell. The dopamine transporter removes dopamine from the synaptic cleft and returns it to the terminal of the presynaptic nerve cell. From Fusar-Poli and colleaguesl.50 Copyright © 2012 American Psychiatric Association.
Two years into the study, four of the 40 relatives (10 percent) with the worst olfactory test scores developed clinical Parkinson’s disease, whereas none of the 38 relatives with the best test scores did. By five years, the incidence among relatives rose to 12.5 percent. Only those from the poor-smelling group evidenced decreased imaging of the dopamine transporter and, in some cases, such decreases were evident at baseline, suggesting that subclinical disease had already begun. These data suggested that the risk of developing Parkinson’s disease in the presence of hyposmia may be as high as 22 percent in first-degree relatives.35
Numerous other studies support the view that olfactory testing may be helpful in predicting the development of cognitive and motor disorders.24 Indeed, olfactory dysfunction rivals and even exceeds the sensitivity of a number of other biomarkers in such prediction, including SPECT imaging of the dopamine transporter,36 as described above. Currently, novel methods are being developed to enhance the predictive power of olfactory tests. For example, spraying the inside of the nose with atropine, a drug that accentuates cognitive dysfunction in patients with Alzheimer’s disease via its anticholinergic effects, may induce a greater degree of smell loss in individuals who are at risk for future dementia, in effect “unmasking” the disease.37
Although quantitative smell testing is rarely performed by most physicians, it has been found to be useful in not only detecting, but also discriminating among, a number of neurodegenerative diseases. For example, a disorder called progressive supranuclear palsy (PSP) is often misdiagnosed as Parkinson’s disease. Unlike Parkinson’s, however, patients with PSP have a relatively normal sense of smell.38 Thus, a neurologist whose evaluation of such a person is inconclusive can use smell testing to aid in making the correct diagnosis. The same is true for distinguishing between depression and Alzheimer’s disease, with depressed patients showing little evidence of smell loss.39 In a position paper, the quality standards committee of the American Academy of Neurology has in fact recommended that olfactory testing be considered to differentiate Parkinson’s disease from PSP and corticobasal degeneration, another neurological disorder.40
Keeping Your Sense of Smell Sharp
How can each of us maintain a healthy sense of smell? All through life, viruses, air pollutants, and other environmental toxins cumulatively damage receptor cells In the uppermost regions of our noses. Such cumulative damage is not manifested until later in life, when few cells are left to provide a normal sense of smell. Hence, the degree to which we can minimize exposure to such agents, such as having good air filters in our homes and washing our hands regularly, can go a long way in preventing damage.
Maintaining good sleep patterns also protects smell function. Obstructive sleep apnea, in particular, has been associated with smell loss,41 which may be attenuated by the use of a CPAP (continuous positive airway pressure) machine at night.42 Importantly, daily exercise has been shown to help avert age-related decrements in the ability to smell.43 It may even help preserve olfaction in persons with Parkinson’s disease.44
Aside from maintaining good health via exercise, sleep, and avoidance of pathogens, a healthy diet and certain dietary interventions may also help. Gopinath and associates at the University of Sydney compared the odor identification ability of 1331 persons who differed in terms of their dietary intake of nuts, fish, butter, and margarine.45 Those with the most nut and fish consumption had a reduced likelihood of olfactory loss, possibly because of the anti-inflammatory properties of these foods’ constituents. Similarly, Richard Stevenson and his colleagues at Macquarie University in Sydney found that persons who ate a Western style diet high in saturated fat and sugar exhibited poorer odor identification test scores than those whose diets were low in these nutrients.46
Conversely, an impaired sense of smell may lead to dietary changes that ultimately impact health, as evidenced by a study at Yale University that assessed dietary habits in 80 elderly women, 37 of whom had olfactory dysfunction.47 The latter exhibited a nutrient intake profile that increases the chances for cardiac disease, including a higher intake of sweets and a lower preference for citrus fruits.
A Tie to Coffee
My own colleagues and I showed, in 2007, that the lifetime history of coffee drinking was positively associated with UPSIT scores in relatives of patients with Parkinson’s disease.48 Thus, after correcting for age, gender, and tobacco use, the mean UPSIT score for those who drank less than one cup a day was 30.4 (out of a possible 40); for those who drank one cup a day it was 32.6, while for those who drank two to three cups a day or four or more cups a day the mean scores were 33.1 and 34.1, respectively. This pattern was statistically significant (p < 0.009) and was stronger in men than in women. Whether the same relationship may be found in the general population has yet to be determined.
Looking Forward
What does the future hold? In Japan, a major pharmaceutical company has begun an initiative to educate physicians about the importance of this primary sensory system and to distribute olfactory tests via pharmacies to promote better understanding of the health of the Japanese elderly population. In light of recent discoveries, it is inevitable that more and more physicians will begin to pay attention to the smell ability of their patients, and to routinely test this faculty.
Given that olfactory receptors are not just confined to the nose, future research will establish whether smell testing can provide information on the distribution of olfactory receptors elsewhere in the body and indicate whether such information may aid in the detection and treatment of some genetic-related diseases. More research on how odors influence mood and behavior is underway, and novel devices for adding odors to the environment are in development.
Just as we largely control our auditory environment, we may soon be able to engineer our olfactory environment in a much more sophisticated way, to alter our states of mind and improve our mental health. The future of olfactory research seems on target to fulfill the prescient assessment of Alexander Graham Bell in a 1927 Scientific Monthly article: “Odors are becoming more and more important in the world of scientific experiments and in medicine—and the need for more knowledge of odors will bring more knowledge, as surely as the sun shines.”
Figure 5.
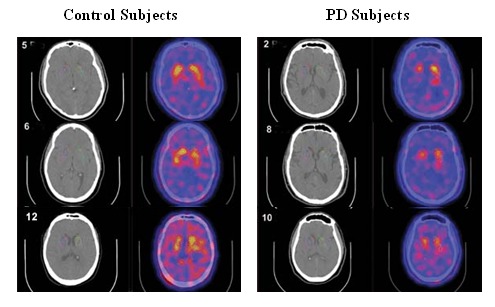
Imaging of the dopamine receptor in patients with Parkinson’s disease (PD) (Right) and age-and sex matched normal controls (Left). Note the depletion of the radioactively labelled ligand sensitive to the dopamine transporter in the PD subjects relative to the controls. Photograph courtesy of Jacob Dubroff, Smell and Taste Center and Department of Neuroradiology, University of Pennsylvania.
Footnotes
Richard L. Doty, Ph.D. is the director of the University of Pennsylvania’s Smell and Taste Center and the inventor of the University of Pennsylvania Smell Identification Test (UPSIT), a standardized olfactory test heralded as the olfactory equivalent to the eye chart. Dr. Doty is editor of the Handbook of Olfaction and Gustation (Marcel Dekker, 1995, 2003, 2015), the largest collection of basic, clinical, and applied knowledge on the chemical senses ever compiled in one volume. He is an author or co-author of over 400 professional publications (including 10 books and contributions to such publications as Science, Nature, and the Encyclopedia Britannica). His most recent books are The Neurology of Olfaction, co-authored by Christopher Hawkes (Cambridge University Press) and The Great Pheromone Myth (Johns Hopkins University Press). Among his numerous awards are the James A. Shannon Award from the National Institutes of Health (1996), the Olfactory Research Fund’s Scientific Sense of Smell Award (2000), the William Osler Patient-Oriented Research Award from the University of Pennsylvania (2003), and the Association for Chemoreception Science’s Max Mozell Award for Outstanding Achievement in the Chemical Senses (2005).
Financial Disclosure
Richard Doty is president and major shareholder of Sensonics International, the manufacturer and distributor of the commercial version of the University of Pennsylvania Smell Identification Test.
References
- 1.Buck L, Axel R. A novel multigene family may encode odorant receptors: a molecular basis for odor recognition. Cell. 1991;65(1):175–187. doi: 10.1016/0092-8674(91)90418-x. [DOI] [PubMed] [Google Scholar]
- 2.Greer PL, Bear DM, Lassance JM, Bloom ML, Tsukahara T, Pashkovski SL, Masuda FK, Nowlan AC, Kirchner R, Hoekstra HE, Datta SR. A Family of non-GPCR chemosensors defines an alternative logic for mammalian olfaction. Cell. 2016;165(7):1734–1748. doi: 10.1016/j.cell.2016.05.001. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Busse D, Kudella P, Gruning NM, Gisselmann G, Stander S, Luger T, Jacobsen F, Steinstrasser L, Paus R, Gkogkolou P, Bohm M, Hatt H, Benecke H. A synthetic sandalwood odorant induces wound-healing processes in human keratinocytes via the olfactory receptor OR2AT4. J Invest Dermatol. 2014;134(11):2823–2832. doi: 10.1038/jid.2014.273. [DOI] [PubMed] [Google Scholar]
- 4.Pavlath GK. A new function for odorant receptors: MOR23 is necessary for normal tissue repair in skeletal muscle. Cell Adh Migr. 2010;4(4):502–506. doi: 10.4161/cam.4.4.12291. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Kang N, Kim H, Jae Y, Lee N, Ku CR, Margolis F, Lee EJ, Bahk YY, Kim MS, Koo J. Olfactory marker protein expression is an indicator of olfactory receptor-associated events in non-olfactory tissues. PLoS One. 2015;10(1):e0116097. doi: 10.1371/journal.pone.0116097. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Foster SR, Roura E, Molenaar P, Thomas WG. G protein-coupled receptors in cardiac biology: old and new receptors. Biophys Rev. 2015;7(1):77–89. doi: 10.1007/s12551-014-0154-2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Trotier D, Bensimon JL, Herman P, Tran Ba HP, Doving KB, Eloit C. Inflammatory obstruction of the olfactory clefts and olfactory loss in humans: a new syndrome? Chem Senses. 2007;32(3):285–292. doi: 10.1093/chemse/bjl057. [DOI] [PubMed] [Google Scholar]
- 8.Kang N, Bahk YY, Lee N, Jae Y, Cho YH, Ku CR, Byun Y, Lee EJ, Kim MS, Koo J. Olfactory receptor Olfr544 responding to azelaic acid regulates glucagon secretion in alpha-cells of mouse pancreatic islets. Biochem Biophys Res Commun. 2015;460(3):616–621. doi: 10.1016/j.bbrc.2015.03.078. [DOI] [PubMed] [Google Scholar]
- 9.Kudyakova TI, Sarycheva NY, Kamenskii AA. Orientation and exploratory behavior and anxiety of CBA mice with anosmia induced by N-trimethylindole (skatole) Bull Exp Biol Med. 2007;143(1):1–4. doi: 10.1007/s10517-007-0001-6. [DOI] [PubMed] [Google Scholar]
- 10.Massberg D, Jovancevic N, Offermann A, Simon A, Baniahmad A, Perner S, Pungsrinont T, Luko K, Philippou S, Ubrig B, Heiland M, Weber L, Altmuller J, Becker C, Gisselmann G, Gelis L, Hatt H. The activation of OR51E1 causes growth suppression of human prostate cancer cells. Oncotarget. 2016;7(30):48231–48249. doi: 10.18632/oncotarget.10197. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Shepard BD, Cheval L, Peterlin Z, Firestein S, Koepsell H, Doucet A, Pluznick JL. A Renal Olfactory Receptor Aids in Kidney Glucose Handling. Sci Rep. 2016;6:35215. doi: 10.1038/srep35215. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Braun T, Voland P, Kunz L, Prinz C, Gratzl M. Enterochromaffin cells of the human gut: sensors for spices and odorants. Gastroenterology. 2007;132(5):1890–1901. doi: 10.1053/j.gastro.2007.02.036. [DOI] [PubMed] [Google Scholar]
- 13.Weber M, Pehl U, Breer H, Strotmann J. Olfactory receptor expressed in ganglia of the autonomic nervous system. J Neurosci Res. 2002;68(2):176–184. doi: 10.1002/jnr.10164. [DOI] [PubMed] [Google Scholar]
- 14.Chen Z, Zhao H, Fu N, Chen L. The diversified function and potential therapy of ectopic olfactory receptors in non-olfactory tissues. J Cell Physiol. 2017 doi: 10.1002/jcp.25929. [DOI] [PubMed] [Google Scholar]
- 15.Air Force Instructions 48-123. Accession, Retention and Administration. Medical Examination and Standards. 2006 Jun 5;2 [Google Scholar]
- 16.Doty RL. Handbook of Olfaction and Gustation. 3rd. Hoboken, N.J.: John Wiley & Sons, Inc; 2015. pp. 1–1217. [Google Scholar]
- 17.Doty RL, Shaman P, Applebaum SL, Giberson R, Siksorski L, Rosenberg L. Smell identification ability: changes with age. Science. 1984;226:1441–1443. doi: 10.1126/science.6505700. [DOI] [PubMed] [Google Scholar]
- 18.Doty RL, Shaman P, Dann M. Development of the University of Pennsylvania Smell Identification Test: a standardized microencapsulated test of olfactory function. Physiology & Behavior. 1984;32:489–502. doi: 10.1016/0031-9384(84)90269-5. [DOI] [PubMed] [Google Scholar]
- 19.Doty RL. The Smell Identification TestTM Administration Manual. 3rd Edition. Sensonics, Inc.; Haddon Hts., NJ: 1995. [Google Scholar]
- 20.Stevens JC, Cain WS. Aging Impairs the Ability to Perceive Gas Odor. Chemical Senses. 1986;11(4):668. [Google Scholar]
- 21.Pence TS, Reiter ER, DiNardo LJ, Costanzo RM. Risk factors for hazardous events in olfactory-impaired patients. JAMA Otolaryngol Head Neck Surg. 2014;140(10):951–955. doi: 10.1001/jamaoto.2014.1675. [DOI] [PubMed] [Google Scholar]
- 22.Devanand DP, Lee S, Manly J, Andrews H, Schupf N, Masurkar A, Stern Y, Mayeux R, Doty RL. Olfactory identification deficits and increased mortality in the community. Ann Neurol. 2015;78(3):401–411. doi: 10.1002/ana.24447. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.Pinto JM, Wroblewski KE, Kern DW, Schumm LP, McClintock MK. Olfactory dysfunction predicts 5-year mortality in older adults. PLoS One. 2014;9(10):e107541. doi: 10.1371/journal.pone.0107541. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.Doty RL, Hawkes CH, Good KP, Duda JE. Odor perception and neuropathology in neurodegenerative diseases and schizophrenia. In: Doty RL, editor. Handbook of Olfaction and Gustation. John Wiley & Sons; Hoboken: 2015. pp. 403–452. [Google Scholar]
- 25.Braak H, Braak E, Yilmazer D, de Vos RAI, Jansen ENH, Bohl J. Pattern of brain destruction in Parkinson’s and Alzheimer’s diseases. J Neural Trans. 1996;103:455–490. doi: 10.1007/BF01276421. [DOI] [PubMed] [Google Scholar]
- 26.Doty RL. Olfactory dysfunction in neurodegenerative diseases: is there a common pathological substrate? Lancet neurol. 2017;16(6):478–488. doi: 10.1016/S1474-4422(17)30123-0. [DOI] [PubMed] [Google Scholar]
- 27.Sohrabi HR, Bates KA, Rodrigues M, Taddei K, Laws SM, Lautenschlager NT, Dhaliwal SS, Johnston AN, Mackay-Sim A, Gandy S, Foster JK, Martins RN. Olfactory dysfunction is associated with subjective memory complaints in community-dwelling elderly individuals. J Alzheimers Dis. 2009;17(1):135–142. doi: 10.3233/JAD-2009-1020. [DOI] [PubMed] [Google Scholar]
- 28.Devanand DP, Tabert MH, Cuasay K, Manly JJ, Schupf N, Brickman AM, Andrews H, Brown TR, DeCarli C, Mayeux R. Olfactory identification deficits and MCI in a multi-ethnic elderly community sample. Neurobiol Aging. 2010;31(9):1593–1600. doi: 10.1016/j.neurobiolaging.2008.09.008. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 29.Devanand DP, Lee S, Manly J, Andrews H, Schupf N, Doty RL, Stern Y, Zahodne LB, Louis ED, Mayeux R. Olfactory deficits predict cognitive decline and Alzheimer dementia in an urban community. Neurology. 2015;84(2):182–189. doi: 10.1212/WNL.0000000000001132. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 30.Graves AB, Bowen JD, Rajaram L, McCormick WC, McCurry SM, Schellenberg GD, Larson EB. Impaired olfaction as a marker for cognitive decline: interaction with apolipoprotein E epsilon4 status. Neurology. 1999;53(7):1480–1487. doi: 10.1212/wnl.53.7.1480. [DOI] [PubMed] [Google Scholar]
- 31.Serby M, Mohan C, Aryan M, Williams L, Mohs RC, Davis KL. Olfactory identification deficits in relatives of Alzheimer’s disease patients. Biol Psychiat. 1996;39(5):375–377. doi: 10.1016/0006-3223(95)00472-6. [DOI] [PubMed] [Google Scholar]
- 32.Calderon-Garciduenas L, Franco-Lira M, Henriquez-Roldan C, Osnaya N, Gonzalez-Maciel A, Reynoso-Robles R, Villarreal-Calderon R, Herritt L, Brooks D, Keefe S, Palacios-Moreno J, Villarreal-Calderon R, Torres-Jardon R, Medina-Cortina H, Delgado-Chavez R, Aiello-Mora M, Maronpot RR, Doty RL. Urban air pollution: Influences on olfactory function and pathology in exposed children and young adults. Experimental and Toxicological Pathology. 2010;62:91–102. doi: 10.1016/j.etp.2009.02.117. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 33.Tabert MH, Liu X, Doty RL, Serby M, Zamora D, Pelton GH, Marder K, Albers MW, Stern Y, Devanand DP. A 10-item smell identification scale related to risk for Alzheimer’s disease. Ann Neurol. 2005;58(1):155–160. doi: 10.1002/ana.20533. [DOI] [PubMed] [Google Scholar]
- 34.Ross GW, Petrovitch H, Abbott RD, Tanner CM, Popper J, Masaki K, Launer L, White LR. Association of olfactory dysfunction with risk for future Parkinson’s disease. Ann Neurol. 2008;63(2):167–173. doi: 10.1002/ana.21291. [DOI] [PubMed] [Google Scholar]
- 35.Ponsen MM, Stoffers D, Wolters EC, Booij J, Berendse HW. Olfactory testing combined with dopamine transporter imaging as a method to detect prodromal Parkinson’s disease. J Neurol Neurosurg Psychiatry. 2010;81(4):396–399. doi: 10.1136/jnnp.2009.183715. [DOI] [PubMed] [Google Scholar]
- 36.Deeb J, Shah M, Muhammed N, Gunasekera R, Gannon K, Findley LJ, Hawkes CH. A basic smell test is as sensitive as a dopamine transporter scan: comparison of olfaction, taste and DaTSCAN in the diagnosis of Parkinson’s disease. Quarterly Journal of Medicine. 2010;103(12):941–952. doi: 10.1093/qjmed/hcq142. [DOI] [PubMed] [Google Scholar]
- 37.Schofield PW, Ebrahimi H, Jones AL, Bateman GA, Murray SR. An olfactory ‘stress test’ may detect preclinical Alzheimer’s disease. BMC Neurol. 2012;12:24. doi: 10.1186/1471-2377-12-24. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 38.Doty RL, Golbe LI, McKeown DA, Stern MB, Lehrach CM, Crawford D. Olfactory testing differentiates between progressive supranuclear palsy and idiopathic Parkinson’s disease. Neurology. 1993;43(5):962–965. doi: 10.1212/wnl.43.5.962. [DOI] [PubMed] [Google Scholar]
- 39.Solomon GS, Petrie WM, Hart JR, Brackin HB., Jr Olfactory dysfunction discriminates Alzheimer’s dementia from major depression. Journal of Neuropsychiatry & Clinical Neurosciences. 1998 Winter;10(1):64–67. doi: 10.1176/jnp.10.1.64. 1998. [DOI] [PubMed] [Google Scholar]
- 40.Suchowersky O, Reich S, Perlmutter J, Zesiewicz T, Gronseth G, Weiner WJ. Practice Parameter: Diagnosis and prognosis of new onset Parkinson disease (an evidence-based review) Report of the Quality Standards Subcommittee of the American Academy of Neurology. Neurology. 2006;66(7):968–975. doi: 10.1212/01.wnl.0000215437.80053.d0. [DOI] [PubMed] [Google Scholar]
- 41.Salihoglu M, Kendirli MT, Altundag A, Tekeli H, Saglam M, Cayonu M, Senol MG, Ozdag F. The effect of obstructive sleep apnea on olfactory functions. Laryngoscope. 2014;124(9):2190–2194. doi: 10.1002/lary.24565. [DOI] [PubMed] [Google Scholar]
- 42.Walliczek-Dworschak U, Cassel W, Mittendorf L, Pellegrino R, Koehler U, Guldner C, Dworschak POG, Hildebrandt O, Daniel H, Gunzel T, Teymoortash A, Hummel T. Continuous positive air pressure improves orthonasal olfactory function of patients with obstructive sleep apnea. Sleep Med. 2017;34:24–29. doi: 10.1016/j.sleep.2017.02.018. [DOI] [PubMed] [Google Scholar]
- 43.Schubert CR, Fischer ME, Pinto AA, Klein BEK, Klein R, Cruickshanks KJ. Odor detection thresholds in a population of older adults. Laryngoscope. 2017;127(6):1257–1262. doi: 10.1002/lary.26457. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 44.Rosenfeldt AB, Dey T, Alberts JL. Aerobic Exercise Preserves Olfaction Function in Individuals with Parkinson’s Disease. Parkinsons Dis. 20162016 doi: 10.1155/2016/9725089. 9725089. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 45.Gopinath B, Sue CM, Flood VM, Burlutsky G, Mitchell P. Dietary intakes of fats, fish and nuts and olfactory impairment in older adults. Br J Nutr. 2015;114(2):240–247. doi: 10.1017/S0007114515001257. [DOI] [PubMed] [Google Scholar]
- 46.Stevenson RJ, Boakes RA, Oaten MJ, Yeomans MR, Mahmut M, Francis HM. Chemosensory Abilities in Consumers of a Western-Style Diet. Chem Senses. 2016;41(6):505–513. doi: 10.1093/chemse/bjw053. [DOI] [PubMed] [Google Scholar]
- 47.Duffy VB, Backstrand JR, Ferris AM. Olfactory dysfunction and related nutritional risk in free-living, elderly women. J Am Diet Assoc. 1995;95(8):879–884. doi: 10.1016/S0002-8223(95)00244-8. [DOI] [PubMed] [Google Scholar]
- 48.Siderowf A, Jennings D, Connolly J, Doty RL, Marek K, Stern MB. Risk factors for Parkinson’s disease and impaired olfaction in relatives of patients with Parkinson’s disease. Mov Disord. 2007;22(15):2249–2255. doi: 10.1002/mds.21707. [DOI] [PubMed] [Google Scholar]
- 49.Menco BPM, Morrison EE. Morphology of the mammalian olfactory epithelium: form, fine structure, function, and pathology. In: Doty RL, editor. Handbook of olfaction and gustation. Marcel Dekker; New York: 2003. pp. 17–49. [Google Scholar]
- 50.Fusar-Poli P, Rubia K, Rossi G, Sartori G, Balottin U. Striatal dopamine transporter alterations in ADHD: pathophysiology or adaptation to psychostimulants? A meta-analysis. Am J Psychiatry. 2012;169(3):264–272. doi: 10.1176/appi.ajp.2011.11060940. [DOI] [PubMed] [Google Scholar]


