Key Points
Question
Does maternal diabetes, a strong risk factor for very preterm birth, have an association with risks of in-hospital mortality or severe neonatal morbidity in very preterm infants?
Findings
In this international cohort study of singleton infants born very preterm, the risk of in-hospital mortality or severe neonatal morbidity for infants who were born to mothers with diabetes was not significantly different from the risk of infants who were born to mothers without diabetes.
Meaning
Maternal diabetes is not associated with an excess risk of in-hospital mortality or severe morbidity in infants born very preterm in high-income countries.
Abstract
Importance
Diabetes in pregnancy is associated with a 2-times to 3-times higher rate of very preterm birth than in women without diabetes. Very preterm infants are at high risk of death and severe morbidity. The association of maternal diabetes with these risks is unclear.
Objective
To determine the associations between maternal diabetes and in-hospital mortality, as well as neonatal morbidity in very preterm infants with a birth weight of less than 1500 g.
Design, Setting, Participants
This retrospective cohort study was conducted at 7 national networks in high-income countries that are part of the International Neonatal Network for Evaluating Outcomes in Neonates and used prospectively collected data on 76 360 very preterm, singleton infants without malformations born between January 1, 2007, and December 31, 2015, at 24 to 31 weeks’ gestation with birth weights of less than 1500 g, 3280 (4.3%) of whom were born to diabetic mothers.
Exposures
Any type of diabetes during pregnancy.
Main Outcomes and Measures
The primary outcome was in-hospital mortality. The secondary outcomes were severe neonatal morbidities, including intraventricular hemorrhages of grade 3 to 4, cystic periventricular leukomalacia, retinopathy of prematurity needing treatment and bronchopulmonary dysplasia, and other morbidities, including respiratory distress, treated patent ductus arteriosus, and necrotizing enterocolitis. Odds ratios (ORs) with 95% confidence intervals were estimated, adjusted for potential confounders, and stratified by gestational age (GA), sex, and network.
Results
The mean (SD) birth weight of offspring born to mothers with diabetes was significantly higher at 1081 (262) g than in offspring born to mothers without diabetes (mean [SD] birth weight, 1027 [270] g). Mothers with diabetes were older and had more hypertensive disorders, antenatal steroid treatments, and deliveries by cesarean delivery than mothers without diabetes. Infants of mothers with diabetes were born at a later GA than infants of mothers without diabetes. In-hospital mortality (6.6% vs 8.3%) and the composite of mortality and severe morbidity (31.6% vs 40.6%) were lower in infants of mothers with diabetes. However, in adjusted analyses, no significant differences in in-hospital mortality (adjusted OR, 1.16 (95% CI, 0.97-1.39) or the composite of mortality and severe morbidity (adjusted OR, 0.99 (95% CI, 0.88-1.10) were observed. With few exceptions, outcomes of infants born to mothers with and without diabetes were similar regardless of infant sex, GA, or country of birth.
Conclusions and Relevance
In high-resource settings, maternal diabetes is not associated with an increased risk of in-hospital mortality or severe morbidity in very preterm infants with a birth weight of fewer than 1500 g.
This cohort study explored the association between maternal diabetes and the risk of in-hospital mortality or severe neonatal morbidity for infants born very preterm across 7 national networks in high-income countries.
Introduction
Diabetes affects hundreds of millions of people. The incidence is compounded by obesity and is increasing in many parts of the world, including in women of reproductive age.1,2 Diabetes and obesity are significant risk factors for spontaneous and indicated preterm delivery (<37 weeks’ gestation).2,3,4 Despite advances in the care of women with pregestational diabetes (types 1 and 2), rates of preterm delivery remain 3- to 5-fold higher in women with diabetes than in the general obstetric population without diabetes.5,6,7 Furthermore, the risk of preterm delivery is significantly increased in pregnancies with gestational diabetes.8
Worldwide, approximately 11% of births are preterm and the incidence is rising.9 Preterm birth is a major contributor to the global burden of disease.10,11 Infants born with very low birth weights (<1500 g) or who are very preterm (<32 weeks’ gestation) constitute 1% to 2% of all births but account for up to half of all neonatal and infant deaths,12 a significant proportion of childhood disability13 and high health care costs.12 In offspring of women with diabetes, preterm birth is the most important contributor to neonatal morbidity.14
While the obstetric risks that are associated with diabetes in pregnancy are fairly well established, as is knowledge of the increased risks of malformations, fetal death, fetal macrosomia, and neonatal hypoglycemia, less is known about other neonatal outcomes.5,6,7,15 In particular, it is unclear how maternal diabetes affects infants who are born very preterm. The few studies that address this question describe conflicting results. One article indicated a higher risk of respiratory distress syndrome (RDS) in preterm infants born to mothers with diabetes vs infants born to mothers without diabetes,16 while other studies did not detect a difference in the risk of RDS.17 Preterm infants born to mothers with diabetes have even been reported to have a lower risk of bronchopulmonary dysplasia than infants born to mothers without diabets.18 However, an increased risk of necrotizing enterocolitis (NEC), neonatal sepsis, and small head circumference at follow-up were recently reported for extremely preterm infants born to mothers with type 1 diabetes.19,20
The overall research question was to fill the previously mentioned gap in knowledge and to provide solid estimates for neonatal outcomes in very preterm infants born to mothers with diabetes. Given the comparatively low prevalence of maternal diabetes and the low incidence of very preterm birth, large sample sizes are required to accurately estimate neonatal risks that are associated with maternal diabetes. The International Network for Evaluating Outcomes in Neonates (iNeo) is a collaboration between neonatal networks from high-income countries with the goal of improving outcomes for children born very preterm and with a very low birth weight.21 With detailed information on more than 100 000 infants, the iNeo database offers an opportunity to assess the associations of maternal diabetes with neonatal outcomes. We hypothesized that any maternal diabetes would increase the risk of in-hospital mortality and morbidity in very preterm infants with birth weights of fewer than 1500 g.
Methods
Setting
The study used data from national neonatal networks in 7 high-resource countries in 3 continents: Canada, Finland, Israel, Italy, Japan, Sweden, and the United Kingdom. The participating networks and the iNeo Coordinating Centre at the Maternal-Infant Research Centre, Mount Sinai Hospital in Toronto, Ontario, Canada, obtained data sharing agreements and research ethics approval for data collection and transfer. The rules and regulations of each country were followed and ethics approval was obtained by each individual country. All participants were informed about the collection of the data in the register with the purpose of quality assessment of care and research.
Data Sources
Prospectively collected individual-level data from the following neonatal networks were included: Canadian Neonatal Network,22 Finnish Medical Birth Register, Neonatal Research Network of Japan,23 Israel Neonatal Network,24 Tuscany Neonatal Network (TIN-Toscane online), the Swedish Neonatal Quality Register, and UK Neonatal Collaborative (UKNC).25 Previous reports provide details of the proportion of neonates in this data set out of the total number of neonates born in each country.25 Based on a consensus between all iNeo networks, data collection was standardized and included information on maternal age, maternal diabetes and hypertensive disorders in pregnancy, mode of delivery, neonatal characteristics, and outcomes. All variables were classified according to the tenth version of the International Statistical Classification of Diseases and Related Health Problems, Tenth Revision (ICD-10).
Study Population
The study population included all singleton infants born alive in high-income countries who were very preterm (24-31 weeks’ gestation) and with a birth weight of less than 1500 g. The database did not hold information on stillbirths. Multiple pregnancies and major congenital malformations were excluded. The study period covered 9 years from January 1, 2007, to December 31, 2015.
Main Exposure
A diagnosis of any type of pregestational diabetes or gestational diabetes, recorded in tick boxes (pregestational or gestational diabetes were ticked if “yes”) or defined according to ICD 10 codes, was recorded as a dichotomous variable in the iNeo database. Differentiating between pregestational and gestational diabetes was not possible, and information on the duration of diabetes or the type of treatment (insulin or oral antidiabetic agents) was not available. The definitions and screening protocols for diabetes in pregnancy used in the participating countries are provided in eTable 1 in the Supplement.
Outcomes
The main outcome was in-hospital infant mortality. Secondary outcomes included a composite of mortality and severe neonatal morbidity. In addition, severe and major morbidities were analyzed as separate outcomes. Severe neonatal morbidity was defined as 1 or more of the following diagnoses: intraventricular hemorrhage (IVH) grade of 3 to 4,26 cystic periventricular leukomalacia (cPVL),27 treated severe retinopathy of prematurity (ROP),28 and bronchopulmonary dysplasia (BPD, defined as oxygen requirement, with or without mechanical respiratory support, at 36 weeks of postmenstrual age or at time of transfer to level 2 units).29 Additional morbidities studied were RDS, severe brain injury (IVH grade 3-4 or cPVL), pharmacologically or surgically treated patent ductus arteriosus, and NEC.30 Necrotizing enterocolitis was analyzed in a subgroup of the cohort because data from the UKNC were not available for stage 2 or 3 NEC.
Covariates
Covariates and potential confounders included advanced (≥35 years) maternal age at delivery, hypertensive disorder of pregnancy (chronic hypertension, gestational hypertension, preeclampsia, eclampsia, or HELLP syndrome), any treatment with antenatal corticosteroids, mode of delivery, delivery outside of a tertiary center (outborn; for all networks but UKNC), gestational age (GA) at delivery, sex, birth weight z score, and neonatal network.
Statistical Analysis
Maternal and infant characteristics and outcomes were compared between neonates born to mothers with and without diabetes. Frequency (percentage) or means with standard deviations were reported. Differences were assessed with Pearson χ2 and the t test for categorical variables and continuous variables, respectively. Univariate and multivariable logistic analyses were applied for primary and secondary outcomes. Odds ratios (ORs) with 95% confidence intervals were estimated. In the adjusted analyses, covariates were included as confounders based on the literature or statistical significance. Maternal age was introduced as a dichotomous variable (ie, age ≥35 years, yes or no) and GA was analyzed by week and birth weight as z scores. Two regression models were used: model 1 included the following possible confounders: a maternal age of 35 years or older, maternal hypertensive disorder in pregnancy, GA, sex, birth weight z score, and network. Model 2 included the variables in model 1 as well as antenatal treatment with corticosteroids, mode of delivery, and outborn status. Stratified analyses by GA, sex, and network were also performed.
Finally, propensity score (PS) matching was used, stratified by networks. The PS represented a single-index variable summarizing the maternal and perinatal covariates known or hypothesized to be either related to the exposure (maternal diabetes) or the neonatal outcomes. Matching the PS among infants born to mothers with diabetes to that of infants born to mothers without diabetes was performed using the SAS macro “match.sas” (SAS Institute) and was based on a caliper width of 0.2 times the standard deviation of the logit-transformed PS. Within each matched sample (n = 2914 pairs), covariates were tested for balance using paired t tests for continuous variables, and the McNemar tests for categorical covariates. The association between maternal diabetes and neonatal outcomes in each matched sample was examined using logistic regression analyses as described previously, using generalized estimating equations with an unstructured correlation. All analyses were conducted using SAS, version 9.4 (SAS Institute) with a 2-sided significance level of P = .05. The statistic package R (R Foundation) was applied to generate the plot.
Results
Between January 1, 2007, and December 31, 2015, there were 78 126 singleton eligible infants, 76 360 (95.7%) of whom had information on maternal diabetes; 3280 (4.3%) infants were born to mothers with diabetes. Compared with mothers without diabetes, women with diabetes were older, had more hypertensive complications, were administered antenatal corticosteroids more often, and had cesarean deliveries more frequently (Table 1). Infants of mothers with diabetes had a higher GA and higher birth weight but lower mean birth weight z score than infants of mothers without diabetes. The rate of small for GA was similar between infants with mothers with and without diabetes; infants born to mothers without diabetes were born outside a tertiary unit more often than infants of mothers with diabetes (Table 1).
Table 1. Characteristics of Very Preterm Infants With a Very Low Birth Weight and Their Mothers.
| Characteristic | No. (%) | P Value | |
|---|---|---|---|
| Infants of Mothers With Diabetes (n = 3280) |
Infants of Mothers Without Diabetes (n = 73 080) |
||
| Maternal Characteristics | |||
| Maternal age ≥35 y | 1107 (36.7) | 15 616 (22.5) | <.01 |
| Hypertensive disorders of pregnancya | 1106 (34.1) | 15 214 (20.9) | <.01 |
| Antenatal corticosteroids | 2674 (83.5) | 54 307 (76.6) | <.01 |
| Cesarean delivery | 2365 (72.4) | 46 359 (65.3) | <.01 |
| Neonatal Characteristics | |||
| Apgar score <7 at 5 minb | 710 (27.1) | 12 723 (28.1) | .28 |
| Gestational age, No. (%) | |||
| 28-31 wk | 2145 (65.4) | 40 662 (55.6) | <.01 |
| <28 wk | 1135 (34.6) | 32 418 (44.4) | |
| Males | 1707 (52.1) | 38 434 (52.6) | .53 |
| Birth weight, mean (SD) | |||
| Grams | 1081 (262) | 1027 (270) | <.01 |
| z Score | −0.31 (0.91) | −0.28 (0.93) | .04 |
| Small for gestational age | 498 (15.2) | 10 759 (14.7) | .47 |
| Outborn,b,c No./total No. (%) | 196/2634 (7.4) | 4239/46 106 (9.2) | <.01 |
Hypertension in pregnancy includes gestational hypertension, preeclampsia, eclampsia, and HELLP syndrome.
UK Neonatal Collaborative info unavailable.
No. is number in the group and total No. is the total number in the category.
Infants of mothers with diabetes had lower crude risks of in-hospital mortality and the composite of in-hospital mortality or severe neonatal morbidity (IVH grade 3-4, cPVL, treated ROP, or BPD) than infants of mothers without diabetes (Table 2). Similarly, infants of mothers with diabetes had lower rates of IVH grade of 3 to 4, treated ROP, treated patent ductus arteriosus, and BPD than infants of mothers without diabetes. In contrast, the crude risks of RDS and NEC were higher in infants of mothers with diabetes than in infants of mothers without diabetes. After adjusting for confounders (model 1), infants of mothers with diabetes had a lower risk of IVH. This difference disappeared after further adjustment for antenatal steroid treatment, mode of delivery, and outborn status (eTable 2 in the Supplement). In the final step using PS matched analyses, the risk estimates for adverse neonatal outcomes remained similar between the 2 groups (Table 2, Figure).
Table 2. In-Hospital Mortality and Morbidity of Very Preterm Infants of Mothers With Diabetes.
| Characteristic | No. (%) | OR (95% CI) | ||||
|---|---|---|---|---|---|---|
| Infants of Mothers With Diabetes (n = 3280) |
Infants of Mothers Without Diabetes (n = 73 080) |
Crude | Model 1 Adjusteda |
Model 2 Adjustedb |
Model 3 PS-Matchedc |
|
| In-hospital mortality | 215 (6.6) | 6043 (8.3) | 0.78 (0.68-0.90) | 1.06 (0.90-1.24) | 1.16 (0.97-1.39) | 1.08 (0.88-1.32) |
| In-hospital mortality or severe neonatal morbidityd | 984 (31.6) | 28 803 (40.6) | 0.67 (0.62-0.73) | 0.94 (0.86-1.03) | 0.99 (0.88-1.10) | 0.94 (0.85-1.04) |
| RDS | 2165 (67.0) | 45 237 (62.4) | 1.22 (1.13-1.32) | 1.04 (0.96-1.13) | 1.01 (0.91-1.11) | 1.05 (0.95-1.17) |
| IVH grade 3-4 or cPVL | 218 (6.9) | 6187 (8.7) | 0.78 (0.68-0.90) | 0.84 (0.72-0.98) | 0.91 (0.77-1.08) | 0.91 (0.75-1.12) |
| Treated PDA | 766 (23.4) | 18 536 (25.4) | 0.90 (0.83-0.97) | 1.00 (0.91-1.10) | 0.98 (0.89-1.09) | 1.01 (0.91-1.13) |
| Severe ROP (treated) | 157 (4.8) | 5259 (7.2) | 0.82 (0.70-0.96) | 0.93 (0.77-1.11) | 0.85 (0.69-1.03) | 1.01 (0.81-1.26) |
| BPD | 611 (20.3) | 18 544 (27.9) | 0.66 (0.60-0.72) | 0.96 (0.87-1.07) | 1.01 (0.89-1.14) | 0.94 (0.83-1.06) |
| NECe | 137 (5.2) | 1940 (4.2) | 1.25 (1.04-1.49) | 1.18 (0.97-1.43) | 1.18 (0.97-1.44) | 1.10 (0.84-1.43) |
Abbreviations: BPD, bronchopulmonary dysplasia; cPVL, cystic periventricular leukomalacia; IVH, intraventricular hemorrhage; N, total number in category; n, number in group; NEC, necrotizing enterocolitis; OR, odds ratio; PDA, patent ductus arteriosus; PS, propensity score; RDS, respiratory distress syndrome; ROP, retinopathy of prematurity.
Model 1 adjusted for maternal age of 35 years or older, maternal hypertensive disease in pregnancy, gestational age, sex, birth weight z score, and network.
Model 2 adjusted for the same covariates as in model 1 and antenatal corticosteroids, mode of delivery, and outborn.
Model 3: PS-matched ORs, stratified by network.
Severe neonatal morbidity defined as IVH grade 3-4, cPVL, treated ROP, or BPD.
UK info unavailable.
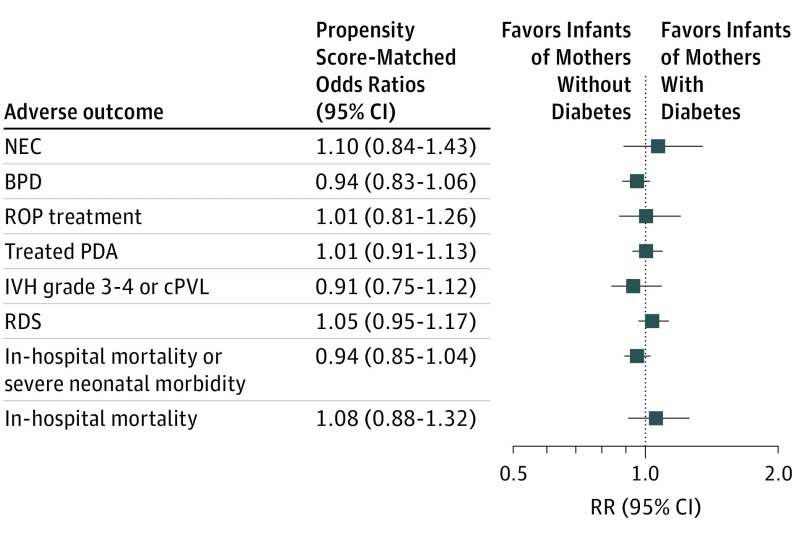
Figure. Association of Maternal Diabetes and Adverse Neonatal Outcomes After Very Preterm Birth.
Severe neonatal morbidity was indicated by an intraventricular hemorrhage (IVH) grade of 3 to 4, cystic periventricular leukomalacia (cPVL), and severe retinopathy of prematurity (ROP) that needed treatment or bronchopulmonary dysplasia (BPD). Propensity score–matched odds ratios were stratified by network. The infants were very preterm infants (<32 weeks of gestation) and were considered very low birth weight (<1500 g). NEC indicates necrotizing enterocolitis; PDA, patent ductus arteriosus; RDS, respiratory distress syndrome.
A stratified analysis by GA week was conducted to identify GA-related risks of maternal diabetes. Infants of mothers with diabetes had a significantly higher risk of mortality at 26 weeks’ gestation and mortality or severe morbidity at 31 weeks’ gestation than infants of mothers without diabetes, while no difference in risk was found in other GA strata (test for an interaction between maternal diabetes and GA on in-hospital mortality: GA [SE], −0.02 [0.03]; P = .58) (Table 3). The rate of in-hospital mortality or severe neonatal morbidity in very preterm infants of mothers with diabetes varied from 23% to 39% across the 7 networks, but the adjusted odds of adverse outcomes in infants of mothers with diabetes did not differ significantly from that in infants of mothers without diabetes (test for interaction between maternal diabetes and network on in-hospital mortality: Canadian Neonatal Network [SE], −0.05 [0.30]; Israel Neonatal Network [SE], −0.18 [0.33]; Neonatal Research Network of Japan [SE], 0.14 [0.31]; Swedish Neonatal Quality Register [SE], 0.34 [0.42]; Finnish Medical Birth Register [SE], 0.22 [0.35]; P = .30) (Table 4).
Table 3. Mortality and Composite Outcome of Infants Born to Mothers With or Without Diabetes by Gestational Age.
| Gestational Age, wk | No. (%) | OR (95% CI) | ||
|---|---|---|---|---|
| Infants of Mothers With Diabetes | Infants of Mothers Without Diabetes | Crude | Adjusteda | |
| In-hospital mortality | ||||
| 24 | 42/162 (25.9) | 1760/6171 (28.5) | 0.88 (0.61-1.25) | 1.10 (0.70-1.71) |
| 25 | 35/209 (16.8) | 1294/7347 (17.6) | 0.94 (0.65-1.36) | 1.07 (0.69-1.68) |
| 26 | 47/336 (14.0) | 984/8817 (11.2) | 1.29 (0.94-1.77) | 1.65 (1.13-2.40) |
| 27 | 31/428 (7.2) | 799/10 083 (7.9) | 0.91 (0.63-1.32) | 0.87 (0.54-1.40) |
| 28 | 29/528 (5.5) | 556/11 684 (4.8) | 1.16 (0.79-1.71) | 1.52 (0.92-2.50) |
| 29 | 14/614 (2.3) | 353/11 605 (3.0) | 0.74 (0.43-1.28) | 1.05 (0.55-1.98) |
| 30 | 9/578 (1.6) | 190/10 072 (1.9) | 0.82 (0.42-1.61) | 0.51 (0.16-1.66) |
| 31 | 8/425 (1.9) | 107/7301 (1.5) | 1.29 (0.62-2.66) | 1.92 (0.79-4.67) |
| Composite outcome, in-hospital mortality or severe neonatal morbidityb | ||||
| 24 | 130/159 (81.8) | 5103/6090 (83.8) | 0.87 (0.58-1.30) | 1.13 (0.68-1.88) |
| 25 | 141/203 (69.5) | 5235/7165 (73.1) | 0.84 (0.62-1.14) | 0.85 (0.61-1.19) |
| 26 | 185/325 (56.9) | 5170/8575 (60.3) | 0.87 (0.70-1.09) | 1.08 (0.83-1.41) |
| 27 | 171/413 (41.4) | 4550/9815 (46.4) | 0.82 (0.67-1.00) | 1.03 (0.80-1.33) |
| 28 | 149/503 (29.6) | 3905/11 364 (34.4) | 0.80 (0.66-0.98) | 0.99 (0.77-1.26) |
| 29 | 107/581 (18.4) | 2670/11 208 (23.8) | 0.72 (0.58-0.89) | 0.89 (0.68-1.18) |
| 30 | 61/541 (11.3) | 1434/9704 (14.8) | 0.73 (0.56-0.96) | 0.75 (0.51-1.09) |
| 31 | 40/394 (10.2) | 736/7024 (10.5) | 0.97 (0.69-1.35) | 1.59 (1.05-2.42) |
Abbreviation: OR, odds ratio.
Adjusted for the following: a maternal age of 35 years or older, maternal hypertensive disease in pregnancy, antenatal corticosteroids, mode of delivery, gestational age, sex, outborn-birth weight z score, and network.
Severe neonatal morbidity defined as intraventricular hemorrhage grade 3-4, cystic periventricular leukomalacia, retinopathy of prematurity stage ≥3, or bronchopulmonary dysplasia.
Table 4. Composite Outcome of Very Preterm Infants Born to Mothers With Diabetes by Neonatal Network.
| Neonatal Network | No./Total No. (%) | OR (95% CI) | ||
|---|---|---|---|---|
| Infants of Mothers With Diabetes | Infants of Mothers Without Diabetes | Crude | Adjustedb | |
| CNN | 316/1130 (28.0) | 4203/11 305 (37.2) | 0.66 (0.57-0.75) | 0.96 (0.80-1.14) |
| FinMBR | 66/190 (34.7) | 493/1385 (35.6) | 0.96 (0.70-1.32) | 1.17 (0.79-1.74) |
| INN | 70/295 (23.7) | 1855/5452 (34.0) | 0.60 (0.46-0.79) | 0.82 (0.60-1.14) |
| NRNJ | 269/697 (38.6) | 8245/21 512 (38.3) | 1.01 (0.87-1.18) | 1.07 (0.89-1.29) |
| SNQ | 21/65 (32.3) | 1247/3525 (35.4) | 0.87 (0.52-1.47) | 1.31 (0.72-2.38) |
| TuscanNN | 23/101 (22.8) | 240/831 (28.9) | 0.73 (0.45-1.18) | 0.94 (0.52-1.71) |
| UKNC | 219/641 (34.2) | 12 520/26 935 (46.5) | 0.60 (0.51-0.70) | 0.85 (0.70-1.04) |
| All networks | 984/3280 (31.6) | 28 803/73 080 (40.6) | 0.67 (0.62-0.73) | 0.99 (0.88-1.10) |
Abbreviations: BPD, bronchopulmonary dysplasia; CNN, Canadian Neonatal Network; FinMBR, Finnish Medical Birth Registry; INN, Israel Neonatal Network; NRNJ, Neonatal Research Network of Japan; OR, odds ratio; SNQ, Swedish Neonatal Quality Register; TuscanNN, Tuscany Neonatal Network (Italy); UKNC, UK Neonatal Collaborative.
In-hospital mortality or severe neonatal morbidity defined as intraventricular hemorrhage grade 3-4, cystic periventricular leukomalacia, -retinopathy of prematurity stage ≥3, or BPD.
Adjusted for a maternal age of 35 years or older, maternal hypertensive disease in pregnancy, antenatal corticosteroids, mode of delivery, gestational age, sex, outborn, and birth weight z score.
An analysis of adverse outcomes in girls and boys of mothers with diabetes did not reveal any significant difference between the sexes (test for interaction between maternal diabetes and infant sex on in-hospital mortality [SE]: −0.18 [0.11]; P = .10) (eTable 2 in the Supplement). Girls of mothers with diabetes had a significantly higher risk of in-hospital mortality (adjusted OR, 1.37; 95% CI, 1.06, 1.77) than girls of mothers without diabetes (eTable 3 in the Supplement).
Discussion
This study has 3 clinically important findings: (1) very preterm infants born to mothers with diabetes are not at a higher risk of in-hospital mortality or morbidity than the population without diabetes, (2) the odds for adverse neonatal outcomes in very preterm infants born to mothers with diabetes did not vary between countries despite different screening and diagnostic protocols for gestational diabetes, and (3) the results are consistent for most GAs, both sexes, and all national populations assessed.
Strength and Limitations
To our knowledge, this study is the largest with adequate power to detect clinically important associations of maternal diabetes with neonatal outcomes of very preterm infants. The number of infants was sufficient to assess outcomes by week of GA and for boys and girls independently. Data on diabetes exposure and outcomes were collected according a standardized protocol, limiting information bias. With data on very preterm births from 7 countries on 4 different continents, we believe that our results have high external validity because of the various diabetes protocols used and populations.
Our study also has limitations. The most important is that although individual databases, such as that from the UKNC and the Swedish Neonatal Quality Register, contain details on all admissions to neonatal care, the iNeo database, like some international databases, such as the Vermont Oxford Network, only includes information on infants with birth weights of 1500 g or less. Maternal diabetes may lead to either restricted or enhanced fetal growth. By including only infants with a birth weight of less than 1500 g we have excluded a significant portion of very preterm infants with birth weights above the mean, particularly those born at 29 to 31 weeks’ gestation. However, the risk of neonatal mortality and morbidity in infants of mothers with diabetes born at 28 to 31 weeks’ gestation was not significantly different than that of infants born before 28 weeks (including large-for-GA infants), suggesting that this limitation may not have introduced a significant selection bias.
Our study was restricted to live births and we did not have information on abortions or fetal deaths before 24 weeks of gestation. The risks of fetal death due to factors like major malformations and placental insufficiency are higher in pregnancies with maternal diabetes. Thus, it is possible that the offspring included in the study reflect a selection of healthier pregnancies, which may have led to an underestimation of the risks associated with maternal diabetes and preterm birth.
Moreover, the data did not enable us to differentiate the type of maternal diabetes (ie, type 1, type 2, or gestational diabetes), and we had no information on the level of glycemic control before or during pregnancy or on diabetes-related complications (except for hypertensive disorders in pregnancy). Despite accounting for many important confounders, we cannot exclude residual confounding by unmeasured or unknown confounders. Neonatal outcomes differed slightly between networks, which may reflect differences in definitions, screening programs, and obstetric interventions. However, the lack of difference in the risk of infants of mothers with or without diabetes was consistent through all networks.
Comparison With Other Studies
Overall, we did not identify increased odds of mortality or severe morbidity in infants born very preterm to mothers with diabetes when compared with infants of mothers without diabetes. This is largely in keeping with data from previous studies,17,19,20,31 even though some studies report an increased adjusted risk of NEC in infants of mothers with diabetes.19,20 We also identified higher crude risks of NEC and RDS in infants of mothers with diabetes than infants of mothers without diabetes, but after adjusting for potential confounders there were no significant differences. Notably, women with diabetes had significantly more risk factors than women without diabetes. On the other hand, antenatal treatment with corticosteroids, cesarean delivery, and delivery at a tertiary unit were more common in pregnancies with diabetes. This is likely a reflection of a more intense monitoring of these high-risk pregnancies. Similar to our study, Grandi et al20 reported that women with diabetes delivering very preterm were more likely to have received antenatal care compared with controls without diabetes, and a study from Israel reported a higher proportion of antenatal corticosteroid treatment in pregnancies with maternal diabetes than nondiabetic pregnancies.17
Importantly, in our study infants of mothers with diabetes were born at a later GA than infants of mothers without diabetes. Our results align with several other studies,17,20 while others found opposite results19 or no significant difference in GA (or birth weight) between infants of mothers with or without diabetes.31 In our study, the higher mean GA at delivery of infants of mothers with diabetes is likely to have attenuated the crude neonatal risks associated with diabetes. Indeed, GA has been demonstrated to be the most important predictor of morbidity in infants of mothers with diabetes14 as well as mothers without diabetes.
The outlook for women with diabetes and their infants has improved significantly over the last decade following the use of a more active diabetes management strategy before and during pregnancy.5,8,32,33 However, the rates of both spontaneous and indicated preterm birth increased several-fold over the same period.3 Risk factors for preterm birth in pregnancies with diabetes include a history of preterm birth, unsatisfactory metabolic control, a premature rupture of membranes that is associated with urogenital infections, diabetes-related complications (such as chronic hypertension), preeclampsia, and, in particular, overt nephropathy.3,34,35,36,37 Even incipient nephropathy (ie, microalbuminuria) was demonstrated to increase the risk of preterm birth in pregnancies with maternal diabetes.38 However, maternal hyperglycemia in diabetes, assessed as elevated hemoglobin A1c levels throughout pregnancy, is an independent risk factor for adverse pregnancy outcomes also in women without signs of microvascular or macrovascular diabetes-related complications.34 We could not address this concern in this study as we did not have information on either the level of glycemic control or on the type of diabetes.
The 2-hour glucose cutoff for diagnosis of gestational diabetes after oral glucose tolerance test varied between countries, spanning from 140 mg/dL (to convert to micromoles per liter, multiply by 0.0555) (United Kingdom) to 180 mg/dL (Sweden). These differences most likely contributed to some of the network variation in prevalence of maternal diabetes among very preterm births, spanning from 1.8% in Sweden to 12% in Finland. Sweden has, next to Finland, the highest incidence of type 1 diabetes in the world.39 Even so, only about 0.4% of pregnancies in Sweden are complicated by type 1 diabetes5 and gestational diabetes is much more common than pregestational diabetes. Therefore, in this study, the higher prevalence of diabetes in pregnant Finnish women than pregnant Swedish women is likely a reflection of different screening protocols and diagnostic criteria for gestational diabetes in the 2 countries (eTable 1 in the Supplement). However, despite the varying prevalence of the different types of diabetes, all networks reported similar odds for adverse neonatal outcomes for very preterm infants of mothers with diabetes compared with mothers without diabetes. Thus, very preterm birth is a strong risk factor for neonatal mortality and morbidity, irrespective of maternal diabetes.
Our study found similar risks of mortality and morbidity in boys and girls born to mothers with diabetes. This is in accordance with previous findings in pregnancies with diabetes,40 but in contrast to reports from the general obstetric population, in which boys face an excess risk of mortality and morbidity.41
Conclusions
Diabetes in pregnancy is a significant risk factor for very preterm birth. However, in high-resource settings, diabetes in pregnancy is not associated with an increased risk of in-hospital neonatal mortality or severe morbidity in infants born before 32 weeks and with a birth weight of less than 1500 g.
eTable 1. Screening protocols, diagnostic criteria and registry data for diabetes in pregnancy by participant network or country
eTable 2. Adverse neonatal outcomes of very preterm boys compared to girls of diabetic mothers
eTable 3. Adverse neonatal outcomes in very preterm infants of diabetic mothers versus non-diabetic mothers, stratified by sex
References
- 1.Stumvoll M, Goldstein BJ, van Haeften TW. Type 2 diabetes: principles of pathogenesis and therapy. Lancet. 2005;365(9467):1333-1346. doi: 10.1016/S0140-6736(05)61032-X [DOI] [PubMed] [Google Scholar]
- 2.McCance DR. Pregnancy and diabetes. Best Pract Res Clin Endocrinol Metab. 2011;25(6):945-958. doi: 10.1016/j.beem.2011.07.009 [DOI] [PubMed] [Google Scholar]
- 3.Lepercq J, Coste J, Theau A, Dubois-Laforgue D, Timsit J. Factors associated with preterm delivery in women with type 1 diabetes: a cohort study. Diabetes Care. 2004;27(12):2824-2828. doi: 10.2337/diacare.27.12.2824 [DOI] [PubMed] [Google Scholar]
- 4.Cnattingius S, Villamor E, Johansson S, et al. . Maternal obesity and risk of preterm delivery. JAMA. 2013;309(22):2362-2370. doi: 10.1001/jama.2013.6295 [DOI] [PubMed] [Google Scholar]
- 5.Persson M, Norman M, Hanson U. Obstetric and perinatal outcomes in type 1 diabetic pregnancies: a large, population-based study. Diabetes Care. 2009;32(11):2005-2009. doi: 10.2337/dc09-0656 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Balsells M, García-Patterson A, Gich I, Corcoy R. Maternal and fetal outcome in women with type 2 versus type 1 diabetes mellitus: a systematic review and metaanalysis. J Clin Endocrinol Metab. 2009;94(11):4284-4291. doi: 10.1210/jc.2009-1231 [DOI] [PubMed] [Google Scholar]
- 7.Farrar D, Simmonds M, Bryant M, et al. . Hyperglycaemia and risk of adverse perinatal outcomes: systematic review and meta-analysis. BMJ. 2016;354:i4694. doi: 10.1136/bmj.i4694 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Fadl HE, Ostlund IK, Magnuson AF, Hanson US. Maternal and neonatal outcomes and time trends of gestational diabetes mellitus in Sweden from 1991 to 2003. Diabet Med. 2010;27(4):436-441. doi: 10.1111/j.1464-5491.2010.02978.x [DOI] [PubMed] [Google Scholar]
- 9.Blencowe H, Cousens S, Oestergaard MZ, et al. . National, regional, and worldwide estimates of preterm birth rates in the year 2010 with time trends since 1990 for selected countries: a systematic analysis and implications. Lancet. 2012;379(9832):2162-2172. doi: 10.1016/S0140-6736(12)60820-4 [DOI] [PubMed] [Google Scholar]
- 10.Murray CJ, Vos T, Lozano R, et al. . Disability-adjusted life years (DALYs) for 291 diseases and injuries in 21 regions, 1990-2010: a systematic analysis for the Global Burden of Disease Study 2010. Lancet. 2012;380(9859):2197-2223. doi: 10.1016/S0140-6736(12)61689-4 [DOI] [PubMed] [Google Scholar]
- 11.GBD 2016 Causes of Death Collaborators Global, regional, and national age-sex specific mortality for 264 causes of death, 1980-2016: a systematic analysis for the Global Burden of Disease Study 2016. Lancet. 2017;390(10100):1151-1210. doi: 10.1016/S0140-6736(17)32152-9 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Thanh NX, Toye J, Savu A, Kumar M, Kaul P. Health service use and costs associated with low birth weight—a population level analysis. J Pediatr. 2015;167(3):551-556.e1, 3. doi: 10.1016/j.jpeds.2015.06.007 [DOI] [PubMed] [Google Scholar]
- 13.Blencowe H, Vos T, Lee AC, et al. . Estimates of neonatal morbidities and disabilities at regional and global levels for 2010: introduction, methods overview, and relevant findings from the Global Burden of Disease study. Pediatr Res. 2013;74(suppl 1):4-16. doi: 10.1038/pr.2013.203 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Hanson U, Persson B, Stangenberg M. Factors influencing neonatal morbidity in diabetic pregnancy. Diabetes Res. 1986;3(2):71-76. [PubMed] [Google Scholar]
- 15.Murphy HR, Steel SA, Roland JM, et al. ; East Anglia Study Group for Improving Pregnancy Outcomes in Women with Diabetes (EASIPOD) . Obstetric and perinatal outcomes in pregnancies complicated by type 1 and type 2 diabetes: influences of glycaemic control, obesity and social disadvantage. Diabet Med. 2011;28(9):1060-1067. doi: 10.1111/j.1464-5491.2011.03333.x [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Azad MB, Moyce BL, Guillemette L, et al. . Diabetes in pregnancy and lung health in offspring: developmental origins of respiratory disease. Paediatr Respir Rev. 2017;21:19-26. [DOI] [PubMed] [Google Scholar]
- 17.Bental Y, Reichman B, Shiff Y, et al. ; Collaboration With the Israel Neonatal Network . Impact of maternal diabetes mellitus on mortality and morbidity of preterm infants (24-33 weeks’ gestation). Pediatrics. 2011;128(4):e848-e855. doi: 10.1542/peds.2010-3443 [DOI] [PubMed] [Google Scholar]
- 18.Eriksson L, Haglund B, Odlind V, Altman M, Ewald U, Kieler H. Perinatal conditions related to growth restriction and inflammation are associated with an increased risk of bronchopulmonary dysplasia. Acta Paediatr. 2015;104(3):259-263. doi: 10.1111/apa.12888 [DOI] [PubMed] [Google Scholar]
- 19.Boghossian NS, Hansen NI, Bell EF, et al. ; Eunice Kennedy Shriver National Institute of Child Health and Human Development Neonatal Research Network . Outcomes of cxtremely preterm infants born to insulin-dependent diabetic mothers. Pediatrics. 2016;137(6):e20153424. doi: 10.1542/peds.2015-3424 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.Grandi C, Tapia JL, Cardoso VC. Impact of maternal diabetes mellitus on mortality and morbidity of very low birth weight infants: a multicenter Latin America study. J Pediatr (Rio J). 2015;91(3):234-241. doi: 10.1016/j.jped.2014.08.007 [DOI] [PubMed] [Google Scholar]
- 21.Shah PS, Lee SK, Lui K, et al. ; International Network for Evaluating Outcomes of Neonates (iNeo) . The International Network for Evaluating Outcomes of very low birth weight, very preterm neonates (iNeo): a protocol for collaborative comparisons of international health services for quality improvement in neonatal care. BMC Pediatr. 2014;14:110. doi: 10.1186/1471-2431-14-110 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 22.Lee SK, McMillan DD, Ohlsson A, et al. . Variations in practice and outcomes in the Canadian NICU network: 1996-1997. Pediatrics. 2000;106(5):1070-1079. doi: 10.1542/peds.106.5.1070 [DOI] [PubMed] [Google Scholar]
- 23.Kusuda S, Fujimura M, Sakuma I, et al. ; Neonatal Research Network, Japan . Morbidity and mortality of infants with very low birth weight in Japan: center variation. Pediatrics. 2006;118(4):e1130-e1138. doi: 10.1542/peds.2005-2724 [DOI] [PubMed] [Google Scholar]
- 24.Bader D, Kugelman A, Boyko V, et al. ; Israel Neonatal Network . Risk factors and estimation tool for death among extremely premature infants: a national study. Pediatrics. 2010;125(4):696-703. doi: 10.1542/peds.2009-1607 [DOI] [PubMed] [Google Scholar]
- 25.Kelly LE, Shah PS, Håkansson S, et al. . Perinatal health services organization for preterm births: a multinational comparison. J Perinatol. 2017;37(7):762-768. doi: 10.1038/jp.2017.45 [DOI] [PubMed] [Google Scholar]
- 26.Papile LA, Burstein J, Burstein R, Koffler H. Incidence and evolution of subependymal and intraventricular hemorrhage: a study of infants with birth weights less than 1,500 gm. J Pediatr. 1978;92(4):529-534. doi: 10.1016/S0022-3476(78)80282-0 [DOI] [PubMed] [Google Scholar]
- 27.de Vries LS, Eken P, Dubowitz LM. The spectrum of leukomalacia using cranial ultrasound. Behav Brain Res. 1992;49(1):1-6. doi: 10.1016/S0166-4328(05)80189-5 [DOI] [PubMed] [Google Scholar]
- 28.International Committee for the Classification of Retinopathy of Prematurity The International Classification of Retinopathy of Prematurity revisited. Arch Ophthalmol. 2005;123(7):991-999. doi: 10.1001/archopht.123.7.991 [DOI] [PubMed] [Google Scholar]
- 29.Shennan AT, Dunn MS, Ohlsson A, Lennox K, Hoskins EM. Abnormal pulmonary outcomes in premature infants: prediction from oxygen requirement in the neonatal period. Pediatrics. 1988;82(4):527-532. [PubMed] [Google Scholar]
- 30.Bell MJ, Ternberg JL, Feigin RD, et al. . Neonatal necrotizing enterocolitis. Therapeutic decisions based upon clinical staging. Ann Surg. 1978;187(1):1-7. doi: 10.1097/00000658-197801000-00001 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 31.Rehan VKMD, Moddemann D, Casiro OG. Outcome of very-low-birth-weight (< 1,500 grams) infants born to mothers with diabetes. Clin Pediatr (Phila). 2002;41(7):481-491. doi: 10.1177/000992280204100705 [DOI] [PubMed] [Google Scholar]
- 32.Cnattingius S, Berne C, Nordström ML. Pregnancy outcome and infant mortality in diabetic patients in Sweden. Diabet Med. 1994;11(7):696-700. doi: 10.1111/j.1464-5491.1994.tb00335.x [DOI] [PubMed] [Google Scholar]
- 33.Hanson U, Persson B. Outcome of pregnancies complicated by type 1 insulin-dependent diabetes in Sweden: acute pregnancy complications, neonatal mortality and morbidity. Am J Perinatol. 1993;10(4):330-333. doi: 10.1055/s-2007-994754 [DOI] [PubMed] [Google Scholar]
- 34.Lauszus FF, Fuglsang J, Flyvbjerg A, Klebe JG. Preterm delivery in normoalbuminuric, diabetic women without preeclampsia: the role of metabolic control. Eur J Obstet Gynecol Reprod Biol. 2006;124(2):144-149. doi: 10.1016/j.ejogrb.2005.05.015 [DOI] [PubMed] [Google Scholar]
- 35.Kitzmiller JL, Combs CA. Diabetic nephropathy and pregnancy. Obstet Gynecol Clin North Am. 1996;23(1):173-203. doi: 10.1016/S0889-8545(05)70251-5 [DOI] [PubMed] [Google Scholar]
- 36.Jensen DM, Damm P, Ovesen P, et al. . Microalbuminuria, preeclampsia, and preterm delivery in pregnant women with type 1 diabetes: results from a nationwide Danish study. Diabetes Care. 2010;33(1):90-94. doi: 10.2337/dc09-1219 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 37.Mimouni F, Miodovnik M, Siddiqi TA, Berk MA, Wittekind C, Tsang RC. High spontaneous premature labor rate in insulin-dependent diabetic pregnant women: an association with poor glycemic control and urogenital infection. Obstet Gynecol. 1988;72(2):175-180. [PubMed] [Google Scholar]
- 38.Ekbom P, Damm P, Feldt-Rasmussen B, Feldt-Rasmussen U, Mølvig J, Mathiesen ER. Pregnancy outcome in type 1 diabetic women with microalbuminuria. Diabetes Care. 2001;24(10):1739-1744. doi: 10.2337/diacare.24.10.1739 [DOI] [PubMed] [Google Scholar]
- 39.Patterson CC, Dahlquist GG, Gyürüs E, Green A, Soltész G; EURODIAB Study Group . Incidence trends for childhood type 1 diabetes in Europe during 1989-2003 and predicted new cases 2005-20: a multicentre prospective registration study. Lancet. 2009;373(9680):2027-2033. doi: 10.1016/S0140-6736(09)60568-7 [DOI] [PubMed] [Google Scholar]
- 40.Persson M, Fadl H. Perinatal outcome in relation to fetal sex in offspring to mothers with pre-gestational and gestational diabetes—a population-based study. Diabet Med. 2014;31(9):1047-1054. doi: 10.1111/dme.12479 [DOI] [PubMed] [Google Scholar]
- 41.Kraemer S. The fragile male. BMJ. 2000;321(7276):1609-1612. doi: 10.1136/bmj.321.7276.1609 [DOI] [PMC free article] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Supplementary Materials
eTable 1. Screening protocols, diagnostic criteria and registry data for diabetes in pregnancy by participant network or country
eTable 2. Adverse neonatal outcomes of very preterm boys compared to girls of diabetic mothers
eTable 3. Adverse neonatal outcomes in very preterm infants of diabetic mothers versus non-diabetic mothers, stratified by sex