Abstract
Background: Fifth metacarpal neck fractures (commonly named “boxer’s fractures”) are the most common metacarpal injuries and usually affect young active people. These lesions are mainly treated conservatively. Their surgical management, if indicated, is still a matter of debate. Different procedures have been described. The aim of this study was to evaluate the outcomes of 18 boxer’s fractures which were synthesized with antegrade locked flexible intramedullary nailing. Materials and methods: All patients, at a mean follow-up of 45 months, were clinically evaluated using the Disabilities of the Arm, Shoulder and Hand (DASH) score and the Patient Rated Wrist/Hand Evaluation (PRWHE). Active and passive range of motion (ROM) of metacarpo-phalangeal (MP), proximal and distal interphalangeal (PIP and DIP) joints and Total Active Motion (TAM), and grip strength were also analyzed. Apex dorsal angulation and axial shortening were radiologically measured preoperatively and at final follow-up. Results: Clinical and radiological results which were observed were satisfactory. No TAM and grip strength differences were recorded between the operated and healthy contralateral hand. Conclusions: According to the positive outcomes and the low rate of complications of this study, antegrade locked flexible intramedullary nailing can be considered a valid treatment option in boxer’s fractures. (www.actabiomedica.it)
Keywords: boxer’s fracture, metacarpal, neck, osteosynthesis, intramedullary nailing
Introduction
Metacarpal fractures are one of the most common injuries and account for 36 % of all hand fractures (13). Among these, localizations at the neck of the fifth metacarpal bone, also called “boxer’s fractures”, are the commonest, with an incidence ranging from 9.7 to 50 %, and are mainly observed in the dominant hand of young active men (1, 4, 5). Boxer’s fractures are generally associated with aggressive behaviors and are typically caused by a longitudinal compression force to the knuckles when the hand is in a clenched fist posture (6, 7). Based on the severity of the trauma, the metacarpal head displaces in the direction of flexion and tends to heal poorly due to the destruction of the volar cortex and deforming force of intrinsic muscles (8, 9). Cosmetic and functional losses may occur in cases of inappropriate reduction and fixation (8-10). The management of these fractures is still a matter of debate (11-13). The majority of these lesions are isolated injuries, simple, closed, and stable and, for this reason, they are usually recommended for conservative treatment (3, 6, 14).
Surgery is usually indicated when clinical malrotation of the fifth finger upon flexion and a longitudinal shortening of more than 3 mm are present, and when the amount of volar angulation of the metacarpal head is judged important. However, in the literature, the degree of acceptable volar angulation varies widely (3, 13, 15). Many surgical techniques have been described to treat the unstable neck fractures of the fifth metacarpal; such procedures include antegrade intramedullary nailing (AIMN), antegrade and retrograde intramedullary K-wiring, retrograde cross pinning with K-wiring, transverse K-wire pinning, external and plate fixation (16-22). In the last decade, the AIMN has gained popularity among surgeons. Many authors have reported good clinical outcomes using this method because it is minimally invasive (no need to expose the fracture site and to pass through the extensor mechanism of the MP joint), relatively simple and it provides a valid stabilization of the bone fragments (l7-19, 23-27).
The purpose of this study was to clinically and radiologically assess 18 patients affected with displaced or unstable fifth metacarpal neck fracture and surgically treated with antegrade locked flexible intramedullary nailing.
Methods
This study is the result of a collaboration between the Parma University Orthopaedic Clinic and Vaio-Fidenza Hospital Orthopaedic Unit.
Between January 2010 and December 2015, 18 patients, affected by Boxer’s fracture underwent surgical treatment with antegrade locked flexible intramedullary nailing.
Inclusion criteria were the following: presence of malrotation of the 5th finger upon flexion, shortening of >3 mm and an angulation of the metacarpal neck of ≥30°. Multi-fragmentary fractures, complex injuries or uncooperative patients were not included for this treatment.
Informed consent relating to the surgical and anestesiological procedures were always obtained. Patients also gave their signed consent for the use of their personal data and clinical/instrumental outcomes for future scientific researches.
The fixation devices that were implanted are made of flexible, blunt, and pre-bent nails measuring 1.1 or 1.6 mm in diameter, which are positioned through a percutaneous approach, under manual power with the aid of a specially designed prefabricated awl (Small Bone Fixation System, Hand Innovations, LLC, Miami, FL). The procedure is performed under fluoroscopic guidance and peripheral anesthesia, thus allowing the reduction by closed manipulation. A small stab incision is placed over the proximal base of the 5th fractured metacarpal. Blunt soft tissue dissection is carried down to the dorsal cortex that cortex is perforated manually using the awl. The nail is then progressed along the diaphyseal canal beyond the fracture until the subchondral bone of the head. Once obtained a satisfactory reduction the nail handle is cut off, and the proximal end of the nail is bent approximately 90 degrees with the assistance of a custom device. A proximal locking sleeve is introduced over the cut end of the nail and is gently driven palmarward through the entrance portal into the proximal metaphysis, thus greatly enhancing rotational and longitudinal stability. Next, the prominent ends of the locking pin and nail are cut below the skin, and a radiopaque plastic cap is applied in order to prevent soft tissue irritation. For the majority of metacarpal fractures a single intramedullary nail is sufficient. This nail is usually removed after 45 days under local anesthesia and after fracture healing.
The rehabilitation plan is individualized and is based on each patient’s circumstances. In general postoperative management consisted in the application of a circumferential hand-based safe position orthosis in order to immobilize the 4th and 5th MP joints in a flexed position (roughly 70°), but with the interphalangeal (IP) joints free to move. Edema management is begun immediately after surgery using self-adhesive compressive bandaging and Game Ready® compressive cryotherapy (GRPro 2.1, CoolSystems Inc., Concord, California, USA) on a daily basis. The patient is instructed to begin immediate active and passive IP joint motion within 5-7 days from surgery and within pain tolerance. In stable fractures, the orthosis was removed after two weeks, the injured finger was buddy-taped with the adjacent finger and rehabilitation continued with active range-of motion exercises to the MP joints and edema management. In unstable fractures this process began three weeks after surgery and the resting orthosis was used during night and during high risk activity of daily livings or at work.
All patients were clinically assessed, at a minimum follow-up of 12 months, with the DASH (28) and PRWHE (29) questionnaires. Bilateral active and passive ROM (AROM and PROM) of MP, PIP and DIP joints were recorded using a 5.5 inch long flat stainless steel finger goniometer (Baseline®, Fabrication Enterprise Inc., White Plains, NY, USA), from which the TAM of both affected (AH) and unaffected hand (UH) and TAM ratio, expressed as a percentage [(TAM AH/TAM UH) * 100], were calculated. Hand grip strength were also analyzed using an hydraulic hand held dynamometer (Sammons Preston, Bolingbrook, IL, USA) according the the standardize procedure (16, 30, 31). Grip strength measurement were recorded three times and results were averaged.
Dorsal apex angle (DAA) and axial shortening were radiologically measured preoperatively and at final follow-up.
Furthermore, postoperative complications were registered as well as the amount of satisfaction of the patients regarding this surgical procedure.
Statistical analysis
Results were statistically analyzed using SPSS 20.0 software (IBM Corp, Armonk, NY, USA). Univariate analysis with the Mann-Whitney test (23) compared clinical results of the affected versus unaffected hand at follow-up regarding TAM and grip strength. The differences were considered significant when the p value was <0.05.
Results
The mean follow-up of the study was 45 months (range 12-84).
Demographic data of the 18 patients are reported in Table 1. All fractures involved the dominant hand (16 right and 2 left).
Table 1.
Demographic data of the patients
| Age (years) | 34 (18-48) |
| Gender (M/F) | 18/0 |
| Dominant hand | 18/0 |
| Right/left side | 16/2 |
DASH and PRWHE scores of the affected side are summarized in Table 2. The optional PRWHE question on aesthetic appearance, was also analyzed with a mean of 1.5 on the separate numerical scale of the questionnaire.
Table 2.
Results of DASH and PRWHE questionnaires of the affected hand at follow-up
| DASH | 2.4 (0-10) |
| PRWHE | 4.7 (1-12) |
AROM and PROM of bilateral 5th MP, PIP and DIP joints are listed in Tables 3 and 4.
Table 3.
Mean values of AROM of AH and hand at follow-up
| AROM (°) | |||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| MP | PIP | DIP | |||||||||
| AH | UH | AH | UH | AH | UH | ||||||
| Extension | Flexion | Extension | Flexion | Extension | Flexion | Extension | Flexion | Extension | Flexion | Extension | Flexion |
| -2.2° | 89.5° | -4.7° | 93.1 | 0.6° | 91.7° | 0.6° | 92.8° | 0° | 88.3° | 0° | 90° |
Table 4.
Mean values of PROM of AH and hand at follow-up
| PROM (°) | |||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| MP | PIP | DIP | |||||||||
| AH | UH | AH | UH | AH | UH | ||||||
| Extension | Flexion | Extension | Flexion | Extension | Flexion | Extension | Flexion | Extension | Flexion | Extension | Flexion |
| -6.4° | 94.2° | -9.7° | 98.6 | 0.6° | 95.3° | 0.3° | 97.2° | -1.4° | 81.7° | -1.7° | 92.8° |
TAM and TAM ratio are outlined in Table 5. The comparison of operated arm vs. the healthy contralateral did not show significant statistical differences (p=0.431).
Table 5.
TAM of AH and UH and percentage of recovery
| Pt | TAM (°) | ||
|---|---|---|---|
| AH | UH | AH/UH (%) | |
| 1 | 260 | 275 | 94.5% |
| 2 | 280 | 305 | 91.8% |
| 3 | 290 | 290 | 100.0% |
| 4 | 240 | 255 | 94.1% |
| 5 | 300 | 305 | 98.4% |
| 6 | 275 | 280 | 98.2% |
| 7 | 270 | 280 | 96.4% |
| 8 | 280 | 290 | 96.6% |
| 9 | 270 | 285 | 94.7% |
| 10 | 265 | 280 | 94.6% |
| 11 | 270 | 280 | 96.4% |
| 12 | 260 | 265 | 98.1% |
| 13 | 265 | 270 | 98.1% |
| 14 | 260 | 270 | 96.3% |
| 15 | 270 | 275 | 98.2% |
| 16 | 285 | 285 | 100.0% |
| 17 | 275 | 285 | 96.5% |
| 18 | 266 | 265 | 100.4% |
| Mean | 271.2 (260-300) | 280 (255-305) | 96.9% (91.8-100%) |
| p value | 0.431 | ||
Grip strength results are shown in Table 6. Statistical analysis also failed to demonstrated differences for this outcome between operated and healthy hands (p=0.783).
Table 6.
Grip strength of AH and UH at different time of measurements and percentage of recovery.
| Grip strength (Kg) | |||||||||
|---|---|---|---|---|---|---|---|---|---|
| Pt | AH | UH | Mean | Recovery (%) AH/UH (%) | |||||
| I | II | II | I | II | II | AH | UH | ||
| 1 | 47 | 45 | 46 | 48 | 48 | 42 | 46.0 | 46.0 | 100 |
| 2 | 38 | 42 | 42 | 40 | 40 | 38 | 40.7 | 39.3 | 103.4 |
| 3 | 55 | 52 | 58 | 60 | 52 | 60 | 55.0 | 57.3 | 95.9 |
| 4 | 46 | 52 | 52 | 44 | 46 | 42 | 50.0 | 44.0 | 113.6 |
| 5 | 60 | 60 | 62 | 62 | 60 | 60 | 60.7 | 60.7 | 100 |
| 6 | 50 | 52 | 52 | 50 | 48 | 50 | 51.3 | 49.3 | 104.1 |
| 7 | 52 | 56 | 54 | 50 | 56 | 52 | 54.0 | 52.7 | 102.5 |
| 8 | 48 | 52 | 52 | 50 | 52 | 50 | 50.7 | 50.7 | 100 |
| 9 | 50 | 48 | 54 | 50 | 50 | 52 | 50.7 | 50.7 | 100 |
| 10 | 44 | 44 | 48 | 46 | 48 | 46 | 45.3 | 46.7 | 97.1 |
| 11 | 50 | 52 | 50 | 52 | 52 | 50 | 50.7 | 51.3 | 98.7 |
| 12 | 58 | 56 | 56 | 52 | 56 | 58 | 56.7 | 55.3 | 102.4 |
| 13 | 40 | 44 | 44 | 44 | 42 | 44 | 42.7 | 43.3 | 98.5 |
| 14 | 60 | 58 | 58 | 58 | 56 | 56 | 58.7 | 56.7 | 103.5 |
| 15 | 54 | 56 | 52 | 52 | 54 | 54 | 54.0 | 53.3 | 101.3 |
| 16 | 50 | 52 | 48 | 50 | 48 | 50 | 50.0 | 49.3 | 101.4 |
| 17 | 48 | 48 | 50 | 50 | 52 | 50 | 48.7 | 50.7 | 96.1 |
| 18 | 42 | 44 | 44 | 46 | 48 | 44 | 43.3 | 46.0 | 94.2 |
| Mean | 49.6 | 50.7 | 51.2 | 50.2 | 50.4 | 49.9 | 50.5 | 50.2 | 100.71 |
| p value | 0.783 | ||||||||
DAA was measured using the lateral radiograph views and its mean value was 50° preoperatively (range: 35-80°) and 8° postoperatively (range: 3-15°).
Shortening >3 mm was never encountered on antero-posterior projections performed after consolidation.
Complications related to the surgical technique were observed in 3 cases (3 penetrations of the nail through the metacarpal head) that did not influence the final outcomes.
All fractures healed, and nonunions related to excessive distraction, as well as malunions characterized by finger malrotation, were never recorded (Figures 1 and 2).
Figure 1.
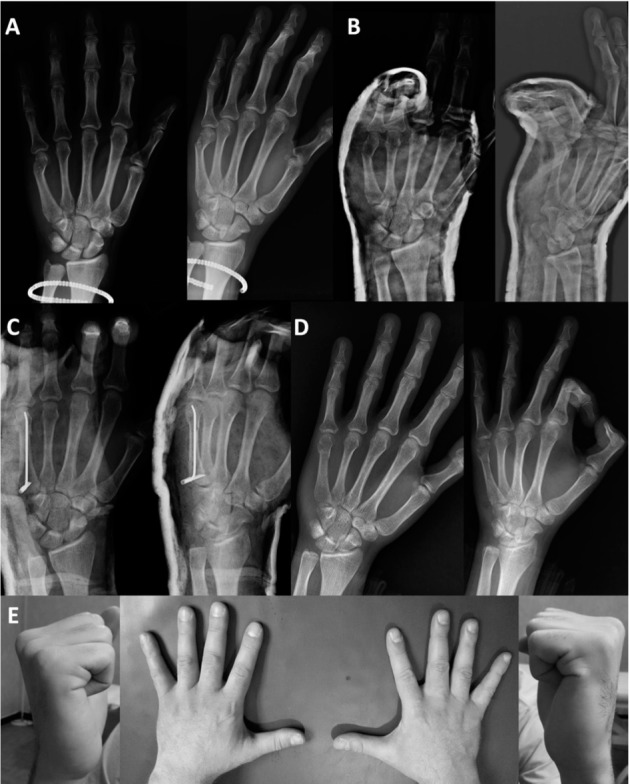
Fifth metacarpal neck fracture of the left hand. Preoperative radiographs (A) and x-rays after closed reduction and application of a splint (unsatisfactory result) (B). Postoperative views (C) and after removal of the nail (D). Satisfactory clinical outcome (E)
Figure 2.
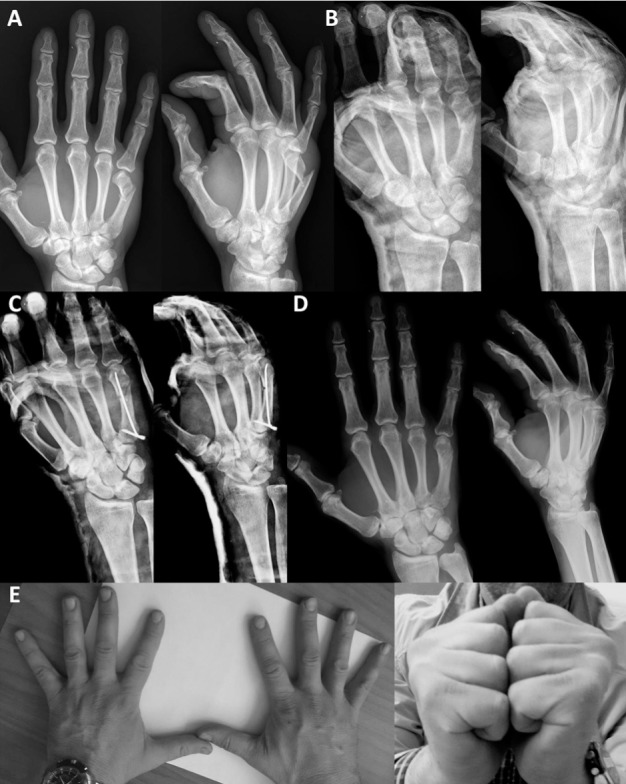
Fifth metacarpal neck fracture of the right hand with fragmentation of the volar cortex. Preoperative radiographs (A) and x-rays after closed reduction and application of a splint (unsatisfactory result) (B). Postoperative views (C) and after removal of the nail (D). Satisfactory clinical outcome (E).
Metallic devices were always removed under local anesthesia after a mean period of 60 days (range: 4575) in order to avoid the progression of skin irritation at the entry point of the nails.
All patients were satisfied of the surgical procedure to which they were submitted.
Discussion
The majority of boxer’s fractures are isolated injuries, simple, closed, stable and are treated conservatively (1, 3, 6, 8). Cosmetic and functional losses may occur in cases where appropriate reduction and orthotic stabilization are not achieved (8, 10). The management of these limited cases is still a matter of debate (1, 3, 6, 8, 12). Indications for operative treatment include malrotation, longitudinal shortening and excessive angulation of the head. Although the majority of surgeons agree that a shortening of the metacarpus by more than 3 mm and any rotation deformity is poorly tolerated and needs correction, it remains controversial how much angulation can be tolerated without loss of hand function or hand pain (16, 20). Older literature quotes higher degrees of acceptable fracture angulation. This has now been challenged. Some cadaveric studies showing decreased hand function with metacarpal head angulation beyond 30 degrees concluded that this is the upper limit for acceptable final angulation (1, 32). Others biomechanical studies showed that a fracture angle up to 30° is compatible with near-normal mechanics, but a fracture angle greater than 45° produces significant muscle shortening that can limit motion of the 5th digit (16, 33). In this study all patients had DAA beyond 30° and this was the superior limit that was accepted for conservative treatment.
In recent years, the operative management choice and metalwork products for fifth metacarpal neck fractures were increased as the surgical technology and fixation products developed. Several surgical techniques have been described and all are characterized by a common target: restoration of anatomy without residual deformities and stable fixation, thus allowing a rapid recovery of joint mobility and function. These procedures, without considering external fixation, which is used in presence of open fractures and soft tissues disruption, can be divided in two groups: open or percutaneous osteosynthesis. Open and internal fixation, which is performed with plate and screws, allows a more precise reduction of the fracture’s fragments but is associated to a higher disruption of soft tissues. On the other hand, percutaneous techniques, that do not expose the fracture’s site, are characterized by a lower surgical invasiveness, thus diminishing the biological bone and muscular distress (1, 3, 6, 8). These latter includes AIMN, antegrade and retrograde intramedullary K-wiring, retrograde cross pinning with K-wire and transverse pinning with K-wires (16). Various studies describe the long-term satisfactory outcomes of antegrade and retrograde intramedullary fixation, as well as for transverse pinning (8, 22). However, Wong et al. (22) stated that percutaneous transverse wiring could lead to possible soft tissue complications and emphasized the importance of prior twisting of the K-wires to avoid their migration, and use of a hammer or forcing should be refrained.
Since Foucher et al. (23, 34) described the antegrade intramedullary K-wiring technique, the AIMN has gained popularity among surgeons because it is minimally invasive and relatively simple. Additionally, many authors have reported good clinical outcomes using this method with superior results to any other surgical techniques. Kim (16) found that antegrade pinning of 5th metacarpal neck fractures, when compared with retrograde pinning, provided better ROM, VAS, grip strength, and DASH scores at 3 months but not at 6 months. Similarly, Fujitani et al. (18), in a randomized study, compared the outcomes of antegrade intramedullary pinning with those of a low profile miniplate for boxer’s fractures and found that 5th finger ROM was better for antegrade pinning at 3 months but not at 6 months. Winter et al. (21), in a non-randomized study, compared the outcomes of antegrade intramedullary pinning and percutaneous transverse pinning for fifth metacarpal neck fractures and found that antegrade pinning provided better finger ROM at 3 months postoperatively. However, Schadel-Hofner et al. (19), in a randomized study, compared the outcomes of antegrade intramedullary pinning and percutaneous retrograde crossed pinning for displaced fifth metacarpal neck fractures and found that antegrade intramedullary pinning produced better ROM, pain scores, and Steel scores (a score comprised of pain, ROM, grip strength, and radiographic deformity) in the fifth metacarpophalangeal joint after a mean patient followup of 17 months. Finally, Yammine & Harvey (3), in a meta-analysis, concluded that patients treated with antegrade intramedullary pinning showed better grip strength, fifth digit ROM, lower pain scores, and fewer complications than patients treated with percutaneous transverse pinning or miniplate.
The results of the present case series, in which flexible, blunt and pre-bent antegrade nails were implanted (SBFS system), were similar to those previously described. DASH and PRWHE questionnaire scores showed at follow-up absence of disability. With the PRWHE was also possible to assess patient satisfaction about the aesthetic appearance. The rating scale ranged from a maximum degree of dissatisfaction (10 points) to a high degree of satisfaction (0 point). The feedback of the patients resulted in a positive rating of 1.5 point. Also PROM and AROM, which were registered also in the contralateral healthy arm, showed a complete recovery of the AH. This assumption was confirmed by TAM statistical analysis, which demonstrated the optimal ROM of MP, PIP and DIP joints.
The last parameter that was evaluated was the grip strength, that allowed to analyze the global static strength of contraction in flexion of the hand. The eventual damage of extensor tendons related to nail positioning could result is an imbalance between the flexor and extensor strength apparatus, thus determining a deficit of global static contraction strength of the operated hand, which is detectable with hydraulic hand dynamometer grip. In this study the comparison of the grip strength between the AH and UH did not show a statistically significant difference, thus confirming the validity of this surgical approach.
One limitation of this study is the small sample size but because outcomes are in accordance to other similar studies (1, 3, 6, 8, 10), authors feel findings to be of help for the hand surgery community.
The need of a second intervention to remove the nails and the high cost of the device in comparison to k-wires might limit the use of SBFS system. The efficacy of AIMN performed with this particular system is demonstrated by the low rate of complications in the 18 patients operated. This fixation device provides optimal stability of the fracture’s site. This observation is proven by the optimal radiographic results registered (DAA and metacarpal length at follow-up were similar to immediate postoperative x-rays) as well as by the absence of malrotation of the fifth finger. Furthermore, authors stress the importance of antegrade insertion of the device which prevents interfering with the extensor apparatus and MP joint. In addition, authors consider the postoperative care to be another important aspect for positive outcomes, which should preferably be managed by specialized hand and upper extremity therapists.
Conclusion
Despite the need to remove the SBFS nails with a second surgery and the high costs of this metallic device, the design of this system and its antegrade insertion justify its utilization in those cases of fifth metacarpal neck fractures in which surgery is indicated.
On the basis of the results and low complication rate observed, among the different fixation techniques for this type of injuries, AIMN with SBFS system can be considered a valid option of treatment.
References
- 1.Mohammed R, Farook MZ, Newman K. Percutaneous elastic intramedullary nailing of metacarpal fractures: surgical technique and clinical results study. J Orthop Surg Res. 2011 Jul 19;6:37. doi: 10.1186/1749-799X-6-37. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Hove LM. Fractures of the hand. Distribution and relative incidence. Scand J Plast Reconstr Surg Hand Surg. 1993;27:317–19. [PubMed] [Google Scholar]
- 3.Yammine K, Harvey A. Antegrade intramedullary nailing for fifth metacarpal neck fractures: a systematic review and meta-analysis. Eur J Orthop Surg Traumatol. 2014 Apr;24(3):273–8. doi: 10.1007/s00590-013-1344-5. [DOI] [PubMed] [Google Scholar]
- 4.Feehan LM, Sheps SB. Incidence and demographics of hand fractures in British Columbia, Canada: a population-based study. J Hand Surg. 2006;31:1068–74. doi: 10.1016/j.jhsa.2006.06.006. [DOI] [PubMed] [Google Scholar]
- 5.Gudmundsen TE, Borgen L. Fractures of the fifth metacarpal. Acta Radiol. 2009;50(3):296–300. doi: 10.1080/02841850802709201. [DOI] [PubMed] [Google Scholar]
- 6.Zong SL, Zhao G, Su LX, Liang WD, Li LG, Cheng G, Wang AJ, Cao XQ, Zheng QT, Li LD, Kan SL. Treatments for the Fifth Metacarpal Neck Fractures: A Network Metaanalysis of Randomized Controlled Trials. Medicine (Baltimore) 2016 Mar;95(11):e3059. doi: 10.1097/MD.0000000000003059. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Soong M, Got C, Katarincic J. Ring and little finger metacarpal fractures: mechanisms, locations, and radiographic parameters. J Hand Surg Am. 2010;35:1256–9. doi: 10.1016/j.jhsa.2010.05.013. [DOI] [PubMed] [Google Scholar]
- 8.Cepni SK, Aykut S, Bekmezci T, Kilic A. A minimally invasive fixation technique for selected patients with fifth metacarpal neck fracture. Injury. 2016 Jun;47(6):1270–5. doi: 10.1016/j.injury.2016.01.034. [DOI] [PubMed] [Google Scholar]
- 9.Diaz-Garcia R, Waljee JF. Current management of metacarpal fractures. Hand Clin. 2013;29:507–18. doi: 10.1016/j.hcl.2013.09.004. [DOI] [PubMed] [Google Scholar]
- 10.Ozturk I, Erturer E, Sahin F, Seckin F, Toker S, Uzun M, Sahin S. Effects of fusion angle on functional results following non-operative treatment for fracture of the neck of the fifth metacarpal. Injury. 2008;39:1464–6. doi: 10.1016/j.injury.2008.03.016. [DOI] [PubMed] [Google Scholar]
- 11.Corkum JP, Davison PG, Lalonde DH. Systematic review of the best evidence in intramedullary fixation for metacarpal fractures. Hand (N Y) 2013;8:253–60. doi: 10.1007/s11552-013-9531-8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Soni A, Gulati A, Bassi JL, Singh D, Saini VC. Outcome of closed ipsilateral metacarpal fractures treated with mini fragment plates and screws: a prospective study. J Orthop Traumatol. 2012;13:29–33. doi: 10.1007/s10195-011-0166-7. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Ford DJ, Ali MS, Steel WM. Fractures of the fifth metacarpal neck: is reduction or immobilisation necessary? J Hand Surg Br. 1989;14:165–7. doi: 10.1016/0266-7681_89_90119-8. [DOI] [PubMed] [Google Scholar]
- 14.Harris AR, Beckenbaugh RD, Nettrour JF, Rizzo M. Metacarpal neck fractures: results of treatment with traction reduction and cast immobilization. Hand. 2009;4(2):161–4. doi: 10.1007/s11552-008-9150-y. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Freeland AE, Geissler WB, Weiss A-PC. Operative treatment of common displaced and unstable fractures of the hand. J Bone Joint Surg Am. 2001;83:928–45. [Google Scholar]
- 16.Kim JK, Kim DJ. Antegrade intramedullary pinning versus retrograde intramedullary pinning for displaced fifth metacarpal neck fractures. Clin Orthop Relat Res. 2015 May;473(5):1747–54. doi: 10.1007/s11999-014-4079-7. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.Facca S, Ramdhian R, Pelissier A, Diaconu M, Liverneaux P. Fifth metacarpal neck fracture fixation: locking plate versus K-wire? Orthop Traumatol Surg Res. 2010;96:506–12. doi: 10.1016/j.otsr.2010.02.009. [DOI] [PubMed] [Google Scholar]
- 18.Fujitani R, Omokawa S, Shigematsu K, Tanaka Y. Comparison of the intramedullary nail and low-profile plate for unstable metacarpal neck fractures. J Orthop Sci. 2012;17:450–6. doi: 10.1007/s00776-012-0223-y. [DOI] [PubMed] [Google Scholar]
- 19.Schadel-Hopfner M, Wild M, Windolf J, Linhart W. Antegrade intramedullary splinting or percutaneous retrograde crossed pinning for displaced neck fractures of the fifth metacarpal? Arch Orthop Trauma Surg. 2007;127:435–40. doi: 10.1007/s00402-006-0254-y. [DOI] [PubMed] [Google Scholar]
- 20.Strub B, Schindele S, Sonderegger J, Sproedt J, von Campe A, Gruenert JG. Intramedullary splinting or conservative treatment for displaced fractures of the little finger metacarpal neck? A prospective study. J Hand Surg Eur. 2010;35:725–9. doi: 10.1177/1753193410377845. [DOI] [PubMed] [Google Scholar]
- 21.Winter M, Balaguer T, Bessiere C, Carles M, Lebreton E. Surgical treatment of the boxer’s fracture: transverse pinning versus intramedullary pinning. J Hand Surg Eur. 2007;32:709–13. doi: 10.1016/J.JHSE.2007.07.011. [DOI] [PubMed] [Google Scholar]
- 22.Wong TC, Ip FK, Yeung SH. Comparison between percutaneous transverse fixation and intramedullary K-wires in treating closed fractures of the metacarpal neck of the little finger. J Hand Surg Br. 2006;31:61–5. doi: 10.1016/j.jhsb.2005.06.022. [DOI] [PubMed] [Google Scholar]
- 23.Foucher G. Bouquet’’ osteosynthesis in metacarpal neck fractures: a series of 66 patients. J Hand Surg Am. 1995;20:S86–S90. doi: 10.1016/s0363-5023(95)80176-6. [DOI] [PubMed] [Google Scholar]
- 24.Gonzalez MH, Igram CM, Hall RF Jr. Flexible intramedullary nailing for metacarpal fractures. J Hand Surg Am. 1995;20:382–87. doi: 10.1016/S0363-5023(05)80091-7. [DOI] [PubMed] [Google Scholar]
- 25.Orbay JL, Touhami A. The treatment of unstable metacarpal and phalangeal shaft fractures with flexible non locking and locking intramedullary nails. Hand Clin. 2006;22:279–86. doi: 10.1016/j.hcl.2006.02.017. [DOI] [PubMed] [Google Scholar]
- 26.Westbrook AP, Davis TR, Armstrong D, Burke FD. The clinical significance of malunion of fractures of the neck and shaft of the little finger metacarpal. J Hand Surg Eur. 2008;33:732–9. doi: 10.1177/1753193408092497. [DOI] [PubMed] [Google Scholar]
- 27.Sletten NI, Nordsletten L, Husby T, Ødegaard RA, Hellund JC, Kvernmo HD. Isolated, extra-articular neck and shaft fractures of the 4th and 5th metacarpals: a comparison of transverse and bouquet (intra-medullary) pinning in 67 patients. J Hand Surg Eur. 2012;37(5):387–95. doi: 10.1177/1753193411431048. [DOI] [PubMed] [Google Scholar]
- 28.Hudak PL, Amadio PC, Bombardier C. Development of an upper extremity outcome measure: the DASH (disabilities of the arm, shoulder and hand) [corrected]. The Upper Extremity Collaborative Group (UECG) Am J Ind Med. 1996;29(6):602–8. doi: 10.1002/(SICI)1097-0274(199606)29:6<602::AID-AJIM4>3.0.CO;2-L. [DOI] [PubMed] [Google Scholar]
- 29.Fairplay T, Atzei A, Corradi M, Luchetti R, Cozzolino R, Schoenhuber R. Cross-cultural adaptation and validation of the Italian version of the patient-rated wrist/hand evaluation questionnaire. J Hand Surg Eur. 2012;37(9):863–70. doi: 10.1177/1753193412445160. [DOI] [PubMed] [Google Scholar]
- 30.Balogun JA, Akomolafe CT, Amusa LO. Grip strength: effects of testing posture and elbow position. Arch Phys Med Rehabil. 1991;72:280–3. [PubMed] [Google Scholar]
- 31.Kadzielski J, Malhotra LR, Zurakowski D, Lee SG, Jupiter JB, Ring D. Evaluation of preoperative expectations and patient satisfaction after carpal tunnel release. J Hand Surg Am. 2008;33:1783–8. doi: 10.1016/j.jhsa.2008.06.019. [DOI] [PubMed] [Google Scholar]
- 32.Birndorf MS, Daley R, Greenwald DP. Metacarpal fracture angulation decreases flexor mechanical efficiency in human hands. Plast Reconstr Surg. 1997;99(4):1079–83. doi: 10.1097/00006534-199704000-00024. [DOI] [PubMed] [Google Scholar]
- 33.Ali A, Hamman J, Mass DP. The biomechanical effects of angulated boxer’s fractures. J Hand Surg Am. 1999;24(4):835–44. doi: 10.1053/jhsu.1999.0835. [DOI] [PubMed] [Google Scholar]
- 34.Foucher G, Chemorin C, Sibilly A. A new technic of osteosynthesis in fractures of the distal 3rd of the 5th metacarpus. Nouv Presse Med. 1976;5:1139–40. [PubMed] [Google Scholar]


