Abstract
Oral papilloma is a benign proliferation of the stratified epithelium, which results in a papillary or verrucous exophytic mass, which can be induced by human papillomavirus. These oral mucosa lesions are most often asymptomatic and have small progression. Laser-assisted surgery is common nowadays with several advantages including successful hemostasis, devoid of sutures, wound sterilization and minimal postoperative pain, and edema. The aim of this report is to present the oral papilloma in a 40-year-old female patient and its treatment with soft-tissue laser. The lesion was excised with diode laser, and the healing was uneventful in a follow-up visit after 1 month. Oral papillomas can be found in young adult patient's oral cavity, and laser dentistry can be used by dental clinicians to treat these kinds of oral lesions and should be considered as an alternative to conventional surgery.
Keywords: Benign tumor, diode laser, low-level laser therapy, oral papilloma
Introduction
Papilloma is a benign neoplasia of the stratified squamous epithelium, which is relatively common in children.[1,2] The findings of a study that reviewed data from 2356 biopsies of young patients (birth to 14 years) received over 15 years in an oral pathology service in Brazil revealed that papillomas were the most frequently observed benign tumors of nonodontogenic origin, corresponding to 29.5% of these lesions.[3] Al Khateeb et al.,[4] in a 10-year retrospective analysis of the types and distribution of oral and maxillofacial tumors in North Jordanian children and adolescents, reported that the papilloma was the most commonly found benign epithelial tumor in this population. Das et al., after reviewing the results from 2370 biopsies of patients up to 20 years of age collected over 11 years in the biopsy service at the University of Illinois, USA, reported that the papilloma was the most prevalent oral neoplasia in this population. Although its exact etiology is still unknown, it is believed that the origin of papillomas is related to traumatisms or human papillomavirus (HPV), especially HPV-6, 11, and 16, which have already been identified in these lesions.[5] The theory that associates papillomas to the HPV advocates that this virus is capable of invading the nuclei of the cells in the spinous layer, inducing a series of proliferative alterations that result in tumoral growth.[6,7]
The use of laser in oral and maxillofacial surgery has been widespread over the last decades with favorable experiences, and most of the oral soft-tissue surgical procedures are done using lasers. Among the commonly available lasers today, the diode laser is frequently used in dentistry. Bleeding control, visibility, and better tissue manipulation are some of the advantages of it. We aim to present a case of oral papilloma located on the lingual mucosa treated with diode laser and the successful postoperational follow-up with no sign of recurrence.[8]
Case Report
A 40-year-old female patient was referred with a complaint of soft-tissue mass in her dorsal side of the tongue. According to the history, this lesion occurred 2 months ago; however, she neglected it until the patient recognized the expansion of the lesion size. Clinical examination showed that there was a pink-colored lesion located on the dorsal side of the tongue and was approximately 0.5 cm in length [Figure 1]. There was nothing abnormal in her systemic review. The lesion was completely excised, from its connection to the tongue under local anesthesia [Figures 2–5], with diode laser. Immediately after laser therapy, the patient described a remarkable pain comfort [Figure 6]. One week later, the patient had no more pain, early healing, and reduction in the lesion size [Figure 7]. Two weeks later, the lesion was approximatively healed with no pain or discomfort [Figure 8]. One month later, we noted a complete tissue healing with no sign of recurrence [Figure 9].
Figure 1.

Preoperative view showing the lingual oral papilloma lesion
Figure 2.

Application of local anesthesia around the oral papilloma lesion
Figure 5.

The surgical specimen which was removed from the oral cavity
Figure 6.
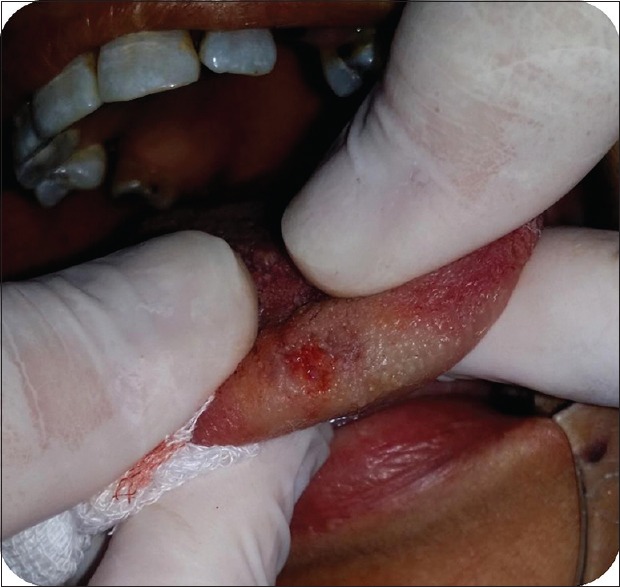
Postoperative view after excision of the lesion with low-level laser therapy
Figure 7.

Follow-up after 1 week
Figure 8.

Follow-up after 2 weeks
Figure 9.
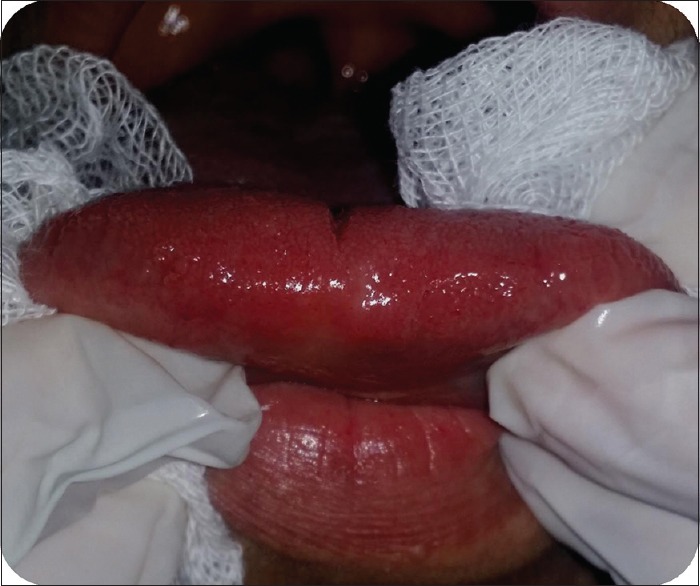
Follow-up after 1 month
Figure 3.

Application of low-level laser therapy on the oral papilloma lesion in a contact mode
Figure 4.

The complete excision of the lesion
Discussion
In the oral cavity, papillomas most commonly occur on the palate (34%) [Figure 1] and jugal mucosa but may also affect the uvula, tongue, lips, and gingiva.[1,2] These tumors are characterized by an exophytic, painless, and well-delimited growths, and the numerous small digitiform projections on their surface give them a clinical “cauliflower-like” appearance. Papillomas usually manifest as single, whitish lesions but may have the color of the surrounding mucosa. Although papillomas are typically small, generally measuring only few millimeters in diameter, there are reports of lesions measuring several centimeters.[8,9] In general, the clinical appearance of oral papillomas is hardly distinguishable from that of common warts (verrucae vulgaris). For accurate differential diagnosis, it is necessary that any HPV that is normally found in skin lesions also be identified in the intraoral lesion. The papillomaviruses present in skin lesions that have been associated to intraoral common warts are HPV-2 and -575. A logical association for clinical diagnosis would be to establish a connection between the presence of common warts in the child's hands and fingers, habits such as thumb or finger-sucking and onychophagia, and the oral papilloma lesion.[10,11] The histological examination of these lesions reveals the proliferation of the spinous layer cells, following a digitiform pattern with a delicate core of fibrous connective tissue constituting the supporting stroma.[12,13] Variable degrees of inflammatory reaction can be observed in this stroma, depending on the existence of epithelial ulcerations.[14] The treatment consists of complete excision of the base of the lesion and a small area of surrounding normal tissue using a number 15 stainless steel scalpel blade12. The specimen should be sent for histopathologic examination to confirm the clinical diagnosis of papilloma and to assure that the surgical intervention and treatment management of the pathology were adequately performed.
Surgical removal is the treatment of choice for these lesions and can be performed with electrocautery, cold-steel excision, laser ablation, cryosurgery, or intralesional injections of interferon.[15,16] In the present case, surgical excision was applied with diode laser. The laser-assisted surgery has several advantages such as excellent hemostasis, high precision in tissue destruction, devoid of sutures, wound sterilization and minimal postoperative pain, and edema.[17] Considering these advantages, the diode laser was chosen as an alternative for the removal of the oral papilloma lesion in the present case. No pain medication was required after excision operation, and wound healing was notable and rapidly achievable. Minimal postoperative pain and rapid wound-healing advantages of the laser-assisted surgery may provide a tolerable procedure for the patients to remove the masses such as oral papilloma.[16,17]
Declaration of Patient Consent
The authors certify that they have obtained all appropriate patient consent forms. In the form the patient(s) has/have given his/her/their consent for his/her/their images and other clinical information to be reported in the journal. The patients understand that their names and initials will not be published and due efforts will be made to conceal their identity, but anonymity cannot be guaranteed.
Conclusion
Oral papillomas can be found in patients' oral cavity, and the clinical diagnosis of these lesions is important. Low-level laser therapy can be used by dental clinicians to treat these kinds of oral lesions and should be considered as an effective alternative to conventional surgery.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
References
- 1.Kerr AR, Phelan JA. Benign Lesions of the Oral Cavity. In: Greenberg MS, Glick, Ship, editors. Burket's Oral Medicine. Ontario, Canada: BC. Decker Inc.; 2007. pp. 132–7. [Google Scholar]
- 2.Jaju PP, Suvarna PV, Desai RS. Oral papilloma: Case report and review of literature. Int J Oral Sci. 2017;2:222–5. doi: 10.4248/IJOS10065. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Babaji P, Singh V, Chaurasia V, Masamatti V, Manmohan A. Oral papilloma of the hard palate. Indian J Dent. 2014;5:211–3. doi: 10.4103/0975-962X.144731. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Devi RS, Rajsekhar B, Srinivas GV, Moon NJ. Unusual length of pedicle: Pedunculated oral papilloma of uvula causing unusual dysphagia of long duration in a child of 10 years. Case Rep Dent. 2014 doi: 10.1155/2014/313506. [Epub ahead of print] [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Harries ML, Juman S, Bailey CM. Recurrent respiratory papillomatosis in the larynx: Re-emergence of clinical disease following surgery. Int J Pediatr Otorhinolaryngol. 1995;31:259–62. doi: 10.1016/0165-5876(94)01092-c. [DOI] [PubMed] [Google Scholar]
- 6.Carneiro TE, Marinho SA, Verli FD, Mesquita AT, Lima NL, Miranda JL, et al. Oral squamous papilloma: Clinical, histologic and immunohistochemical analyses. J Oral Sci. 2009;51:367–72. doi: 10.2334/josnusd.51.367. [DOI] [PubMed] [Google Scholar]
- 7.Anselmi AL, Premoli de Percoco G. Epidemiologic study of 147 cases of oral papilloma (Venezuela).1. Acta Odontol Venez. 1989;27:27–32. [PubMed] [Google Scholar]
- 8.Abbey LM, Page DG, Sawyer DR. The clinical and histopathologic features of a series of 464 oral squamous cell papillomas. Oral Surg Oral Med Oral Pathol. 1980;49:419–28. doi: 10.1016/0030-4220(80)90286-8. [DOI] [PubMed] [Google Scholar]
- 9.Shimoda M, Kameyama K, Morinaga S, Tanaka Y, Hashiguchi K, Shimada M, et al. Malignant transformation of sialadenoma papilliferum of the palate: A case report. Virchows Arch. 2004;445:641–6. doi: 10.1007/s00428-004-1091-4. [DOI] [PubMed] [Google Scholar]
- 10.MacDonald-Jankowski DS. A squamous cell papilloma as a cause of dysphagia and vomiting. Br Dent J. 1990;168:480–1. doi: 10.1038/sj.bdj.4807246. [DOI] [PubMed] [Google Scholar]
- 11.Goodstein LA, Khan A, Pinczewski J, Young VN. Symptomatic squamous papilloma of the uvula: Report of a case and review of the literature. Case Rep Otolaryngol. 2012;2012:1–2. doi: 10.1155/2012/329289. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Carneiro TE, Marinho SA, Verli FD, Mesquita AT, Lima NL, Miranda JL, et al. Oral squamous papilloma: Clinical, histologic and immunohistochemical analyses. J Oral Sci. 2015;51:367–72. doi: 10.2334/josnusd.51.367. [DOI] [PubMed] [Google Scholar]
- 13.Khalighi HR, Hamian M, Abbas FM, Farhadi S. Simultaneous existence of giant cell fibroma and oral papilloma in the oral cavity. IJMS. 2016;2:153–6. [Google Scholar]
- 14.Jaju PP, Suvarna PV, Desai RS. Squamous papilloma: Case report and review of literature. Int J Oral Sci. 2010;2:222–5. doi: 10.4248/IJOS10065. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Monteiro LS, Mouzinho J, Azevedo A, Câmara MI, Martins MA, La Fuente JM, et al. Treatment of epulis fissuratum with carbon dioxide laser in a patient with antithrombotic medication. Braz Dent J. 2012;23:77–81. doi: 10.1590/s0103-64402012000100014. [DOI] [PubMed] [Google Scholar]
- 16.Elanchezhiyan S, Renukadevi R, Vennila K. Comparison of diode laser-assisted surgery and conventional surgery in the management of hereditary ankyloglossia in siblings: A case report with scientific review. Lasers Med Sci. 2013;28:7–12. doi: 10.1007/s10103-011-1047-2. [DOI] [PubMed] [Google Scholar]
- 17.Goodstein LA, Khan A, Pinczewski J, Young VN. Symptomatic squamous papilloma of the uvula: Report of a case and review of the literature. Case Rep Otolaryngol. 2012;2012:329289. doi: 10.1155/2012/329289. [DOI] [PMC free article] [PubMed] [Google Scholar]


