Abstract
Background.
Our previous articles showed that suppressive or preventive treatment with the herbal Gene-Eden-VIR/Novirin reduced the number and duration of genital herpes outbreaks with no adverse effects. These studies also revealed that the herbal Gene-Eden-VIR/Novirin is mostly superior to acyclovir, valacyclovir, and famciclovir drugs in genital herpes. This study tested the effect of Gene-Eden-VIR/Novirin in oral herpes (also called cold sores and fever blisters).
Methods.
The framework of the study was a retrospective chart review. The study included 68 participants. The participants took 1 to 4 capsules per day over a period of 2 to 36 months. The study included 2 Food and Drug Administration–recommended controls: baseline and a no-treatment.
Results.
Gene-Eden-VIR/Novirin was effective in 89.3% of participants. The treatment reduced the mean number of outbreaks per year from 6.0 and 3.6 in the control groups to 2.0 in the treatment group (P < .0001 and P = .07, respectively). Gene-Eden-VIR/Novirin reduced the mean duration of outbreaks from 9.8 and 5.8 days in the control groups to 3.2 days in the treatment group (P < .0001 and P = .02, respectively). There were no reports of adverse experiences. Gene-Eden-VIR/Novirin was compared to acyclovir and valacyclovir in 6 tests. In all tests, Gene-Eden-VIR/Novirin showed higher efficacy. Gene-Eden-VIR/Novirin also showed superior safety.
Conclusions.
This clinical study showed that suppressive or preventive treatment with the herbal Gene-Eden-VIR/Novirin reduced the number and duration of outbreaks in oral herpes without any adverse effects. The study also showed that the herbal Gene-Eden-VIR/Novirin had better clinical effects than acyclovir and valacyclovir, the leading drugs in the category. Based on these results, we recommend using the herbal Gene-Eden-VIR/Novirin as preventive treatment for oral herpes and, specifically, as an alternative to the acyclovir and valacyclovir drugs.
Keywords: HSV1, HSV2, acyclovir, valacyclovir, famciclovir, natural treatment, herbal treatment, oral herpes, cold sores, fever blisters, outbreaks, gene-Eden-VIR, Novirin
Oral herpes, also known as recurrent herpes simplex labialis (HSL), cold sores, and fever blisters, is mostly caused by the herpes simplex virus type 1 (HSV-1).1 HSL affects the lips, manifesting on the skin as vesicular lesions, which follow prodromal symptoms between 6 and 53 hours prior to the appearance of the first vesicles.2 The frequency of recurrence among adults with HSL varies from 1 to 12 episodes or more per year.3 Approximately 35% of patients experience more than 5 episodes per year.4 Furthermore, in healthy individuals, the duration of an episode is 7 to 14 days.5
Three drugs are currently used in the treatment of recurrent HSL: acyclovir (ACV), valacyclovir (VACV), and famciclovir (FCV).6 The Food and Drug Administration (FDA) approved ACV in 1984, VACV in 1995, and FCV in 1994. The 3 drugs use modified nucleosides, or their prodrugs. Their mechanism of action is inhibition of the viral DNA polymerase, which is the main replication enzyme of the virus.7 All 3 drugs are used in episodic treatment. ACV and VACV are also used in suppressive treatment of recurrent HSL.8 In episodic treatment, the drug is administered during outbreaks. The main objective of episodic treatment is to decrease the duration of the outbreak.9 Clinical studies have shown that episodic treatment with ACV, VACV, and FCV decreased the time to healing of lesions by 1 to 2 days.10–13 In suppressive treatment, the drug is administered irrespective of the timing of outbreaks, that is, before, during, and after outbreaks. The most common objective of suppressive treatment is to decrease the number of outbreaks.14 Clinical studies have shown that a 4-month suppressive treatment with ACV and VACV decreased the mean number of outbreaks by more than 50%, and increased the number of recurrence-free patients by more than 20%.3,15,16 Furthermore, suppressive treatment resulted in a longer time (24-72 days) to first recurrence.
Gene-Eden-VIR/Novirin is a patented herbal treatment. The Gene-Eden-VIR/Novirin formula includes 5 ingredients: a 100 mg extract of quercetin, a 150 mg extract of green tea, a 50 mg extract of cinnamon, a 25 mg extract of licorice, and 100 μg of selenium. According to microcompetition theory, latent viruses cause most major diseases.17–19 To reverse the effect of latent viruses on the host, a team of scientists developed the herbal Gene-Eden-VIR/Novirin. The treatment was introduced to the public at the end of 2009. Previous clinical studies conducted at the Center for the Biology of Chronic Disease tested the effect of Gene-Eden-VIR/Novirin on viruses. The studies showed that the herbal treatment has an antiviral effect.20–22 Since viruses are linked to fatigue, another clinical study tested the effect of Gene-Eden-VIR/Novirin on fatigue. The study reported that Gene-Eden-VIR/Novirin safely reduced the feeling of fatigue in individuals infected with a latent virus.23 In 2016, Polansky et al reported that Gene-Eden-VIR/Novirin safely decreased the number and duration of outbreaks in individuals suffering from genital herpes.21,22 The study also compared the clinical effects of the herbal Gene-Eden-VIR/Novirin to the leading drugs ACV, VACV, an FCV. The comparison showed that Gene-Eden-VIR/Novirin was better than these drugs.21
This article reports the effects of suppressive or preventive treatment with Gene-Eden-VIR/Novirin on the number and duration of oral herpes outbreaks. The article also compares the effects of the herbal Gene-Eden-VIR/Novirin to those of ACV and VACV, the 2 leading drugs in the category.
Methods
Objective
The objective of the study was to measure the effects of suppressive or preventive treatment with the herbal Gene-Eden-VIR/Novirin on the frequency and duration of oral herpes outbreaks and to compare these effects to those of the leading drugs in the category.
Framework
The framework of the study was a retrospective chart review. Lilac Corp, the company that sells Gene-Eden-VIR/Novirin to the public, assists its customers in tracking the effects of the treatment on their health. To track these effects, Lilac Corp uses the Natural Origin Treatment Clinical Questionnaire (NotCiq). Professional interviewers collect the answers to the questionnaire over the phone in single sessions. The answers are considered patient-reported outcomes (PROs). The output of the sessions are the charts that we analyzed in this study. For more information on the NotCiq questionnaire, see our previous study.20 The raw data included all the charts that mentioned oral herpes, which were collected during the months of October and November 2015. The 2 months were randomly selected. To avoid a selection bias commonly associated with retrospective chart reviews, charts of both current, past, and noncustomers were analyzed. The framework followed the Good Research Practices for retrospective chart reviews described in Cox et al,24 and the methodological suggestions found in Vassar and Holzmann.25
Ethical Consideration
The institutional review board that approved the study was Salus Institutional Review Board. Since the study was a retrospective chart review, the institutional review board approved a waiver of the requirement to obtain an informed consent from the participants under the exemption status of the federal regulations 45 CFR 46.101(b)(4).
Treatment
The participants took 1, 2, 3, or 4 capsules per day over a period of 2 to 36 months. The mean duration of treatment was 10.4 months. The study included 68 participants.
Controls
The study included 2 FDA-recommended controls. The first control was a baseline control. This group consisted of 56 participants, out of which 38 were current users, and 18 were past users. The second control group was a no-treatment control. This group consisted of 12 participants. The participants in the baseline control were the “before” treatment, or pretreatment participants. The participants in the no-treatment control were those who have not used Gene-Eden-VIR/Novirin at all.
Measures
The NotCiq questionnaire has several sections: a section on age, gender, and ethnicity; a section on dosage used by the participants, the duration of treatment; a section on adverse experiences; a section on diagnosis; a section on type of symptoms; a section on the duration of symptoms; and a section on the frequency of symptoms. The questionnaire used both open- and closed-ended questions. To answer the closed-ended questions, the participants used a scale of 1 to 7. The NotCiq questionnaire was administered by 4 independent interviewers specializing in outbound calls. The answers were collected over the phone. To preserve objectivity, the interviewers were blinded to the objective of the study.
Efficacy
The primary end points were the frequency, or number of outbreaks per period, and the duration of outbreaks, or the number of days passed between initiation of symptoms and signs and complete resolution of the symptoms. There were several secondary end points. Those included the number of participants who had over a 50% reduction in their recurrence rate, the percentage of patients who were recurrence-free, the time to a first recurrence in all participants, and the percentage of patients with prevented or delayed recurrences.
Safety
We analyzed all reports of adverse events.
Population
We excluded all participants who used Gene-Eden-VIR/Novirin for other purposes, including those who used it as treatment for other diseases. We also excluded participants who were concurrently using antiviral drugs a suppressive treatment, specifically ACV or VACV. In the duration of outbreaks analysis, 2 additional participants were excluded due to concurrent episodic treatment with ACV. The final list of participants included 68 participants. All participants had at least one oral herpes outbreak per year.
Statistical Analysis
The analysis of the data in the study was based on the intent-to-treat population. We used the Kaplan-Meier product-limit method to calculate the time to first recurrence of an oral herpes outbreak. We evaluated the differences between the curves using the log-rank, Wilcoxon, and Tarone-Ware tests. We also calculated the difference between pretreatment and treatment (Δ), and calculated the statistical difference between the deltas. We performed the statistical analysis using a one-tail t test assuming unequal variances, or a single-factor analysis of variance. We considered a P ≤ .05 as statistically significant.
Results
Patient Demographic and Baseline Characteristics
The study included 68 participants. We divided the participants into 2 groups: a treatment group, which included 56 participants, and a no-treatment control group, which included 12 participants. Note that the 56 individuals in the treatment group also comprise the 56 individuals in the baseline or pretreatment control group (see Table 2). Table 1 summarizes the demographic and clinical characteristics of the pretreatment/treatment and no-treatment groups.
Table 2.
Summary of the Efficacy Endpoints in the Current Study. All Participants Had at Least One Outbreak per Year.
| Treatment | N | Mean Number of Outbreaks per Year | Time to First Recurrence (Days)a | % Recurrence-Free | % With Decrease in Recurrence | % With >50% Decrease | Mean Duration of Outbreak (Days) |
|---|---|---|---|---|---|---|---|
| No-Tx control | 12 | 3.58 | 175.9 | 0.0% | — | — | 5.83 |
| Pre-Tx control | 56 | 5.96 | 106.5 | 0.0% | 89.3% | 80.4% | 9.78 |
| Tx | 56 | 2.02 (P = .07, no-Tx) (P < .0001, pre-Tx) | 364.6 (P < .0001, pre-Tx) (P = .01, no-Tx) | 46.4% (P < .0001, both controls) | 3.2 (P = .02, no-Tx) (P < .0001, pre-Tx) |
Abbreviation: Tx, treatment.
a Using Kaplan-Meier test.
Table 1.
Demographic and Clinical Characteristics of the Participants.
| Pretreatment and Treatment Groups | No-Treatment Group | |
|---|---|---|
| Age, average (years) | 49 | 46 |
| Age, n (%) | ||
| 20-40 | 15 (26.8%) | 2 (16.7%) |
| 41-50 | 14 (25.0%) | 5 (41.7%) |
| 51-60 | 16 (28.6%) | 4 (33.3%) |
| 61-80 | 11 (19.6%) | 1 (8.3%) |
| Gender, n (%) | ||
| Male | 33 (58.9%) | 3 (25%) |
| Female | 23 (41.1%) | 9 (75%) |
| Race, n (%) | ||
| African American | 8 (14.3%) | 4 (33.3%) |
| Caucasian | 36 (64.3%) | 8 (66.7%) |
| Hispanic | 6 (10.7%) | 0 (0%) |
| Other | 6 (10.7%) | 0 (0%) |
| Years since diagnosis by physician | 0.5-50 (range), 9.0 (mean), 4.5 (median) | 1-40 (range), 8.5 (mean), 2.5 (median) |
| Years since initial episode | 1-40 (range), 18.7 (mean), 19 (median) | 1-40 (range), 13.5 (mean), 12 (median) |
| Percentage diagnosed by physician | 67.9% | 58.3% |
| Percentage that had a laboratory test to confirm diagnosis (out of those diagnosed by a physician) | 65.8% | 57.1% |
| Symptoms of infection, n (%) | ||
| Oral blisters/ulcers | 49 (87.5%) | 9 (75.0%) |
| Local pain | 38 (67.9%) | 9 (75.0%) |
| General discomfort | 25 (44.6%) | 6 (50.0%) |
| Light sensitivity | 13 (23.2%) | 2 (16.7%) |
| Flu-like symptoms | 20 (35.7%) | 7 (58.3%) |
| Duration of treatment (months), n (%) | ||
| 2-5 | 21 (37.5%) | N/A |
| 6-18 | 24 (42.9%) | N/A |
| >18 | 11 (19.6%) | N/A |
Efficacy
Primary Efficacy Endpoints
Out of the 56 participants in the pretreatment group, 89.3% reported a decrease, and 80.4% a greater than 50% decrease in the number (frequency) of outbreaks per year (Table 2). The mean number of outbreaks per year decreased from 3.58 and 5.96, in the no-treatment and pretreatment controls, respectively, to 2.02 in the treatment group (44% and 66%, P = .07 and P < .0001, respectively; Table 2).
Out of 56 participants in the pretreatment group, 91% reported a decrease in the duration of outbreaks. The mean duration of outbreaks decreased from 5.83 days and 9.78 days, in the no-treatment and pre-treatment control groups, respectively, to 3.21 days in the treatment group (P = .02 and P < .0001, respectively; Table 2).
We tested the internal consistency of the participants’ answers using a second set of questions. On frequency of symptoms, the participants were asked, “How often did the symptoms appear before (after) taking Gene-Eden-VIR/Novirin?” using a scale from 1 to 7, where 1 is “very often” and 7 is “not at all.” The mean scores were 3.05 and 5.57 for the “before” and “after” taking Gene-Eden-VIR/Novirin questions, respectively (P < .0001). On duration of symptoms, the participants were asked, “How long did your symptoms last, before (after) taking Gene-Eden-VIR/Novirin?” using a scale from 1 to 7, where 1 is “very long time” and 7 is “didn’t have symptoms.” The mean scores were 3.00 and 5.73 for the “before” and “after” taking Gene-Eden-VIR/Novirin questions, respectively (P < .0001). These results show that the participants provide consistent answers.
To test for a possible difference between current and past users of Gene-Eden-VIR/Novirin, we compared the answers of these groups. The decrease in number of days per episode in current and past users was 6.71 and 6.28, respectively (P = .36). The decrease in number of episodes per year in current and past users was 4.32 and 3.17, respectively (P = .15). No statistical difference was found between the answers provided by participants in the 2 groups.
We also tested the effect of duration of treatment. We divided the treatment group into 3 subgroups according to their duration of treatment: 2 to 5 months (N = 21), 6 to 18 months (N = 24), >18 months (N = 11). The number of outbreaks per year for the 3 subgroups before treatment were 5.77, 4.57, and 8.27, for the 2 to 7 months, 8 to 18 months, and over 18 months, respectively. There was no statistically significant difference between these values (P = .15). The results showed that there is a statistically significant difference in the delta values between the 3 subgroups (3.05, 3.25, and 7.18, respectively, F[2, 53] = 5.43, P = .007; Table 3). Longer duration of treatment was associated with a larger decrease in the frequency of symptoms. These results show a duration of treatment effect.
Table 3.
Duration of Treatment Effect in Those Taking Gene-Eden-VIR/Novirin for 2 to 5 Months Versus Those Taking Gene-Eden-VIR/Novirin for 6 to 18 Months and More Than 18 Months.
| Duration of Treatment | Delta (Change in Number of Outbreaks) | P Value | F Value |
|---|---|---|---|
| 2-5 months (n = 21) | 3.05 | P < .01 | F(2, 53) = 5.43 |
| 6-18 months (n = 24) | 3.25 | ||
| >18 months (n = 11) | 7.18 |
Diagnosis
Thirty-eight participants were diagnosed by a physician and 18 used self-diagnosis. We tested the differences between these groups. Table 4 presents the results. All participants in the 2 groups reported a statistically significant improvement in the number, duration, severity, interference in daily life, and the level of pain. However, those diagnosed by a physician were younger, had more episodes, experienced more severe and painful symptoms, and reported a greater interference in their daily life (borderline significance) during the pretreatment period. In contrast, the participants in the 2 groups report similar duration of episodes during this period. The results also showed that there is no statistically significant difference in the treatment period between the 2 groups in all aspects except the interference in daily life (borderline significance). These results are consistent with those reported in the literature on help-seeking behavior, which shows a positive relationship between the level of pain and disability and the likelihood of seeking professional help.26,27
Table 4.
Diagnosis by a Physician Versus Self-Diagnosis.
| Self-Diagnosis | Diagnosis by Physician | Statistics (Between Groups) | |
|---|---|---|---|
| Mean age at diagnosis (years) | 42 | 25 | P < .0001 |
| Mean number of episodes | 4.28 (pretreatment) | 6.76 (pretreatment) | P = .01 |
| 1.33 (treatment) | 2.34 (treatment) | P = .12 | |
| (P = .0001) | (P = .0001) | ||
| Mean duration of episodes | 9.83 (pretreatment) | 9.75 (pretreatment) | P = .48 |
| 4.28 (treatment) | 2.70 (treatment) | P = .11 | |
| (P = .0008) | (P < .0001) | ||
| Severity of symptoms; 1 is “very bad” and 7 is “not bad at all” | 3.89 (pretreatment) | 2.89 (pretreatment) | P = .02 |
| 6.17 (treatment) | 5.89 (treatment) | P = .93 | |
| (P < .0001) | (P < .0001) | ||
| Interference in daily life; 1 is “interfered all the time” and 7 is “did not interfere | 3.70 (pretreatment) | 2.84 (pretreatment) | P = .09 |
| 6.50 (treatment) | 5.80 (treatment) | P = .06 | |
| (P = .0001) | (P < .0001) | ||
| Pain level; 1 is “very painful” and 7 is “not at all” | 3.56 (pretreatment) | 2.75 (pretreatment) | P = .03 |
| 5.89 (treatment) | 6.03 (treatment) | P = .35 | |
| (P < .0001) | (P < .0001) |
Secondary Efficacy Endpoints
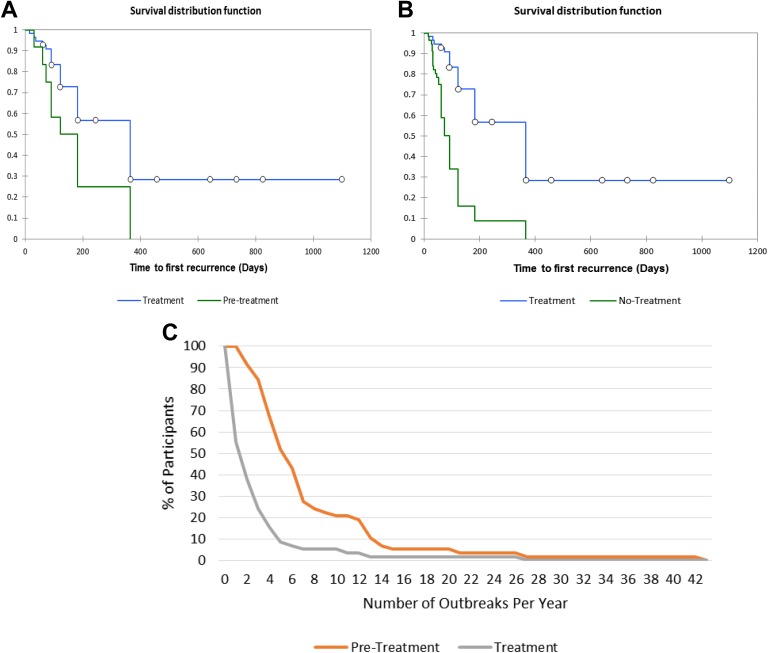
We used the Kaplan-Meier product-limit method to calculate the time to first recurrence. The number of days to a first recurrence, or mean survival time, was 106.5 and 175.91 during the pretreatment and no-treatment periods, respectively, and 364.6 days during the treatment period (P < .0001 and P = .01 for the pretreatment and no-treatment controls, respectively; Figure 1). These results show that treatment with the herbal Gene-Eden-VIR/Novirin increased the time to a first recurrence.
Figure 1.
Kaplan-Meier plots of time to first oral herpes recurrence in the current study from participants with a history of at least 1 recurrence per year compared to (A) treatment versus pretreatment groups, (B) treatment versus no-treatment groups, (C) percentage of participants who have a certain number of outbreaks per year, treatment versus pretreatment groups.
No participants in both the pretreatment and no-treatment controls were recurrence-free (Table 2). Following treatment with the herbal Gene-Eden-VIR/Novirin, 46.4% were recurrence-free (P < .0001). Also, the herbal Gene-Eden-VIR/Novirin treatment prevented or delayed 89% of the recurrences, and 45 of 56 (80%) participants had a greater than 50% decrease in the recurrence rate.
Safety
There were no reports of adverse experiences following treatment with the herbal Gene-Eden-VIR/Novirin.
Gene-Eden-VIR/Novirin Versus Leading Drugs
The next section compares the herbal Gene-Eden-VIR/Novirin with ACV and VACV, the 2 leading drugs in the category. This study did not include what the FDA calls “concurrent”28 groups of ACV or VACV. According to the FDA guidelines, concurrent groups are test or control groups that “are chosen from the same population and treated concurrently.”28 Instead, we compared the effect of Gene-Eden-VIR/Novirin to “external” ACV and VACV groups.
We started creating the external ACV and VACV groups by searching PubMed (MEDLINE) for articles that reported the results of clinical studies that tested suppressive treatment with ACV and VACV in oral herpes. We used the following keywords: “herpes,” “labialis,” “acyclovir,” “valacyclovir,” and “valaciclovir.” We limited the search by the article type “randomized controlled trial,” and the English language. There were no date restrictions. We included all articles that tested the effect of oral treatment on the frequency of oral herpes outbreaks in immunocompetent adult men and nonpregnant women. The final list included 2 articles,3,16 a crossover study that tested the efficacy of a 4-month use of oral ACV in preventing HSL,16 and a placebo-controlled study that tested the effects of VACV 500 mg once daily for 16 weeks in preventing HSL.3
Efficacy
Table 5 present a comparison of the effects of the herbal Gene-Eden-VIR/Novirin and 400 mg of the ACV drug on time to first recurrence, percent reduction in mean number of recurrences, percent reduction in the number of individuals with recurrences, and the mean duration of outbreaks. Table 6 presents a comparison of the effect of Gene-Eden-VIR/Novirin and VACV 500 mg on time to first recurrence, number of recurrences per month, and percent of participants who are recurrence-free. All 7 measures showed that the herbal Gene-Eden-VIR/Novirin is superior to the ACV and VACV drugs in decreasing the number and duration of oral herpes outbreaks (Table 7).
Table 5.
Summary of Efficacy Endpoints in Rooney et al16 and Current Study. In Both Studies, the Participants Had at Least 6 Oral Outbreaks per Year.
| Study | Treatment | N | Time to First Recurrence (Days)a | Reduction in Mean Number of Recurrences (%) | Reduction in Number of Individuals With Recurrences (%)b | Mean Duration of Outbreak (Days) |
|---|---|---|---|---|---|---|
| Rooney et al16 | Pre-Tx | 9 | 59 | 53% | 7% | — |
| Placebo | 11 | 46 | 7.9 ± 1.6 | |||
| ACV 400 mg 2× | 9 | 118 (P = .05, Δ = 66) | 4.3 ± 0.9 (P = .11, Δ = 3.6) | |||
| Current study | GEV/NV pre-Tx | 23 | 44 | 63% | 43% | 9.9 |
| GEV/NV Tx | 23 | 201 (P < .0001, Δ = 157) | 3.4 (P < .0001, Δ = 6.5) |
Abbreviations: Tx, treatment; ACV, acyclovir; GEV/NV, herbal Gene-Eden-VIR/Novirin.
a Using Kaplan-Meier test.
b Adjusted from 4 months to a full year for the Rooney et al study. The P values are taken from the original study.
Table 6.
Summary of Efficacy Endpoints in 2 Clinical Studies. In All Studies, the Participants Had at Least 4 Oral Outbreaks per Year.
| Study | Treatment | N | Time to First Recurrence (Days)a | Number of Recurrences per Month | Recurrence-Free Participants (%)b |
|---|---|---|---|---|---|
| Baker et al3 | Placebo | 49 | 67 | 0.21 | 5.3% |
| VACV 500 mg 1× | 49 | 92 (P = .016, Δ = 25) | 0.12 (P = .042, Δ = 0.09) | 20.4% (P = .041, Δ = 15.1) | |
| Current study | GEV/NV pre-Txc | 37 | 59 | 0.66 | 0.0% |
| GEV/NV Tx | 37 | 351 (P < .0001, Δ = 292) | 0.23 (P < .0001, Δ = 0.43) | 43.2% (P < .0001, Δ = 43.2) |
Abbreviations: Tx, treatment; VACV, valacyclovir; GEV/NV, herbal Gene-Eden-VIR/Novirin.
a Using Kaplan-Meier test.
b Adjusted from 4 months to a full year for the Baker et al study. The P values are taken from the original study.
Table 7.
Efficacy of GEV/N Versus ACV and VACV.
| End Point | Superiority of Efficacy | Source |
|---|---|---|
| Mean number of recurrences per month | GEV/N > VACV | Baker et al3 |
| Percentage recurrence-free | GEV/N > VACV | Baker et al3 |
| Time to first recurrence | GEV/N > ACV | Rooney et al16 |
| Time to first recurrence | GEV/N > VACV | Baker et al3 |
| Percent reduction in recurrence | GEV/N > ACV | Rooney et al16 |
| Percent reduction in those with recurrences | GEV/N > ACV | Rooney et al16 |
| Mean duration of lesion | GEV/N > ACV | Rooney et al16 |
Abbreviations: GEV/NV, herbal Gene-Eden-VIR/Novirin; ACV, acyclovir; VACV, valacyclovir.
Safety
Rooney et al reported adverse events in one patient who dropped out of the study due to headache and nausea. Baker et al observed 22 events (33% of patients) in the VACV group. The most common adverse event was headache, reported 5 times among 3 patients taking VACV.
In addition, several articles reported noncommon adverse events associated with these 2 drugs. Yavuz et al, as an example, describes a cased of a 78-year-old woman, who had a normal baseline renal function, and no contributing possible nephrotoxic factors. This woman developed irreversible renal dysfunction after oral treatment with ACV.29 Becker et al describes another case of a patient who developed rapidly progressive acute renal failure with concomitant changes in mental status after treatment with high-dose parenteral ACV.30 Another serious, yet uncommon side effect of treatment with ACV is neurotoxicity that may lead to hallucinations, confusion, seizures, and obtundation.31
Le Cleach et al tested the effectiveness and safety of the 3 oral antiviral drugs, acyclovir, famciclovir, and valacyclovir, using a meta-analysis of 26 clinical studies.32 They found that the number of withdrawals due to harms was mentioned in only 8 studies, that is, 31% of the studies. In these studies, there were 14 withdrawals due to harms in the placebo or no-treatment groups, and 31 in the antiviral groups. In addition, only 4 studies, that is, 16% of the studies, mentioned safety data in the form of the total number of adverse events. In total, the 4 studies reported 331 adverse events in 561 (59%) participants in the antiviral treatment groups compared with 115 adverse events in 291 (40%) participants in the placebo or no-treatment groups. Lam et al analyzed a cohort of 76 269 patients who were treated with acyclovir, or valacyclovir, and 84 646 who were treated with famciclovir.33 The results showed that 0.27% of the patients treated with ACV or VACV were hospitalized with acute kidney injury.
In our study, the participants reported no adverse events following treatment with the herbal Gene-Eden-VIR/Novirin.
Discussion
This study showed that suppressive or preventive treatment with the herbal Gene-Eden-VIR/Novirin reduced the frequency and duration of oral herpes outbreaks. The study also showed the existence of a duration of treatment effect, that is, longer treatment was associated with fewer outbreaks. Finally, the results showed that Gene-Eden-VIR/Novirin is safe.
In addition, the study showed that preventive treatment with Gene-Eden-VIR/Novirin is more effective in decreasing the number and duration of oral herpes outbreaks, and is safer than ACV and VACV. In other words, Gene-Eden-VIR/Novirin produced better clinical results than ACV and VACV, the 2 leading drugs in the category.
Our study has some methodological advantages. The reviewed ACV and VACV clinical studies had a single duration of treatment. Specifically, both Rooney et al and Baker et al tested their patients after 4 months of treatment. In contrast, our study included a wide range of durations, from 2 months to 36 months, with an average of 10.3 months. Moreover, 42.9% of the participants in our study used the Gene-Eden-VIR/Novirin between 6 and 18 months, and 19.6% for 18 months and over, which is a much longer duration of treatment. Moreover, since we used a range of durations, rather than a single duration, we were able to test for a duration of treatment effect.
Another methodological advantage is using 2 types of questions in gathering information about the outbreaks. The first type of questions asked the participants to count the number of outbreaks per year, and to count the number of days an outbreak lasted. The second type asked the participants to rate the frequency and duration of their outbreaks on a scale from 1 to 7. By comparing the answers to these questions, we were able to test for consistency in the participants’ reports.
Placebo controls are regarded as the gold standard in medical research. However, this is a retrospective chart review, and therefore does not include a placebo control. Instead, this study included 2 other controls recommended by the FDA: a no-treatment concurrent control and a baseline control, a type of external control.28
The scientific method argues in favor of randomization, large sample sizes, independent verification by different laboratories, and so on, to even out unique characteristics found in any specific study, that is, to minimize the effect of cofounding factors. This method considers the same result, observed under dissimilar settings, as reliable. This study showed that the effect of Gene-Eden-VIR/Novirin is significant when compared with a variety of untreated groups with dissimilar characteristics created by independent scientists. Therefore, we conclude that the observed effect is, most likely, real, that is, not an artifact of our specific treatment population, or its matching specific controls, and, therefore, with a strong external validity.
This study uses as data PROs. See a discussion on PROs in our previous study.21 A possible limitation of PROs is the subjective report of symptoms. To address this issue, we compared the participants’ reports of their symptoms with those reported in the literature. The comparison clearly showed that the symptoms reported by the participants, and those reported in the literature, overlap.
One possible cofounding factor in this study is the possible relationship between current use of the product and positive results. To test for this cofounding factor, we compared the results reported by current and past users. We found no statistically significant difference between the 2 groups. Therefore, we can conclude that this possible cofounding factor did not bias the results in this study.
The participants in this study were either diagnosed by a physician or self-diagnosed. First, studies showed that self-reports in conditions such as herpes zoster, oral opportunistic infections among HIV patients, fractures, cataract, and macular degeneration and physical capacity produced accurate diagnostic information.34,35 Second, the differences we observed between the 2 groups are consistent with those reported in the literature on help-seeking behavior. For instance, a study showed that health care–seeking men, with genital ulcer disease, were older, had more ulceration episodes in the past year, and were more likely to test seropositive for HSV-2.36 Another study reported that patients who delayed seeking health care assistance were younger, came from a lower socioeconomic state, had milder symptoms, and experienced less interference with their daily activities.37 Other studies showed that an increase in pain and disability increased the likelihood of seeking professional help.26,27 These findings are consistent with those reported in our study.
Conclusion
In summary, this study showed that suppressive or preventative treatment with the herbal Gene-Eden-VIR/Novirin safely reduced the frequency and duration of oral herpes outbreaks. The study also showed that the herbal Gene-Eden-VIR/Novirin is more effective and safer than ACV and VACV, the leading drugs in the category. Finally, as far as we know, this study is the first clinical study that shows that a natural treatment is better than the leading drugs in a major drug category.
Footnotes
Author Contributions: All authors contributed equally to this article.
Declaration of Conflicting Interests: The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding: The authors received no financial support for the research, authorship, and/or publication of this article.
Ethical Approval: The institutional review board that approved the study was Salus Institutional Review Board. Since the study was a retrospective chart review, the institutional review board approved a waiver of the requirement to obtain an informed consent from the participants under the exemption status of the federal regulations 45 CFR 46.101(b)(4).
References
- 1. Chi CC, Wang SH, Delamere FM, Wojnarowska F, Peters MC, Kanjirath PP. Interventions for prevention of herpes simplex labialis (cold sores on the lips). Cochrane Database Syst Rev. 2015;(8):CD010095. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2. Spruance SL, Overall JC, Jr, Kern ER, Krueger GG, Pliam V, Miller W. The natural history of recurrent herpes simplex labialis: implications for antiviral therapy. N Engl J Med. 1977;297:69–75. [DOI] [PubMed] [Google Scholar]
- 3. Baker D, Eisen D. Valacyclovir for prevention of recurrent herpes labialis: 2 double-blind, placebo-controlled studies. Cutis. 2003;71:239–242. [PubMed] [Google Scholar]
- 4. Hull CM, Levin MJ, Tyring SK, Spruance SL. Novel composite efficacy measure to demonstrate the rationale and efficacy of combination antiviral-anti-inflammatory treatment for recurrent herpes simplex labialis. Antimicrob Agents Chemother. 2014;58:1273–1278. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5. Sciubba JJ. Herpes simplex and aphthous ulcerations: presentation, diagnosis and management—an update. Gen Dent. 2003;51:510–516. [PubMed] [Google Scholar]
- 6. Whitley RJ, Gnann JW., Jr Acyclovir: a decade later. N Engl J Med. 1992;327:782. [DOI] [PubMed] [Google Scholar]
- 7. Kukhanova MK, Korovina AN, Kochetkov SN. Human herpes simplex virus: life cycle and development of inhibitors. Biochemistry (Mosc). 2014;79:1635–1652. [DOI] [PubMed] [Google Scholar]
- 8. Gilbert SC. Suppressive therapy versus episodic therapy with oral valacyclovir for recurrent herpes labialis: efficacy and tolerability in an open-label, crossover study. J Drugs Dermatol. 2007;6:400–405. [PubMed] [Google Scholar]
- 9. Mattison HR, Reichman RC, Benedetti J, et al. Double-blind, placebo-controlled trial comparing long-term suppressive with short-term oral acyclovir therapy for management of recurrent genital herpes. Am J Med. 1988;85:20–25. [PubMed] [Google Scholar]
- 10. Spruance SL, Stewart JC, Rowe NH, McKeough MB, Wenerstrom G, Freeman DJ. Treatment of recurrent herpes simplex labialis with oral acyclovir. J Infect Dis. 1990;161:185–190. [DOI] [PubMed] [Google Scholar]
- 11. Spruance SL, Bodsworth N, Resnick H, et al. Single-dose, patient-initiated famciclovir: a randomized, double-blind, placebo-controlled trial for episodic treatment of herpes labialis. J Am Acad Dermatol. 2006;55:47–53. [DOI] [PubMed] [Google Scholar]
- 12. Spruance SL, Jones TM, Blatter MM, et al. High-dose, short-duration, early valacyclovir therapy for episodic treatment of cold sores: results of two randomized, placebo-controlled, multicenter studies. Antimicrob Agents Chemother. 2003;47:1072–1080. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13. Valacyclovir (Valtrex) for herpes labialis. Med Lett Drugs Ther. 2002;44:95–96. [PubMed] [Google Scholar]
- 14. Corey L, Wald A, Patel R, et al. ; Valacyclovir HSV Transmission Study Group. Once-daily valacyclovir to reduce the risk of transmission of genital herpes. N Engl J Med. 2004;350:11–20. [DOI] [PubMed] [Google Scholar]
- 15. Worrall G. Acyclovir in recurrent herpes labialis. BMJ. 1996;312:6. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16. Rooney JF, Straus SE, Mannix ML, et al. Oral acyclovir to suppress frequently recurrent herpes labialis: a double-blind, placebo-controlled trial. Ann Intern Med. 1993;118:268–272. [DOI] [PubMed] [Google Scholar]
- 17. Polansky H, Javaherian A. 3-Econsystems: microRNAs, receptors, and latent viruses: some insights biology can gain from economic theory. Front Microbiol. 2016;7:369. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18. Polansky H, Javaherian A. Commentary: the unliganded glucocorticoid receptor positively regulates the tumor suppressor gene BRCA1 through GABP beta. Front Cell Infect Microbiol. 2015;5:66. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19. Polansky H. Microcompetition With Foreign DNA and the Origin of Chronic Disease. Rochester, NY: Center for the Biology of Chronic Disease Publishing; 2003. [Google Scholar]
- 20. Polansky H, Itzkovitz E. Gene-Eden-VIR is antiviral: results of a post marketing clinical study. Pharmacol Pharm. 2013;4:1–8. [Google Scholar]
- 21. Polansky H, Javaherian A, Itzkovitz E. Clinical study in genital herpes: natural Gene-Eden-VIR/Novirin versus acyclovir, valacyclovir, and famciclovir. Drug Des Devel Ther. 2016;10:2713–2722. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 22. Polansky H, Javaherian A, Itzkovitz E. Clinical study of Gene-Eden-VIR/Novirin in genital herpes: suppressive treatment safely decreases the duration of outbreaks in both severe and mild cases. Clin Transl Med. 2016;5:40. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23. Polansky H, Itzkovitz E. Gene-Eden-VIR decreased physical and mental fatigue in a post marketing clinical study that followed FDA guidelines; results support microcompetition theory. Pharmacol Pharm. 2014;5:280–290. [Google Scholar]
- 24. Cox E, Martin BC, Van Staa T, Garbe E, Siebert U, Johnson ML. Good research practices for comparative effectiveness research: approaches to mitigate bias and confounding in the design of nonrandomized studies of treatment effects using secondary data sources: the International Society for Pharmacoeconomics and Outcomes Research Good Research Practices for Retrospective Database Analysis Task Force Report—Part II. Value Health. 2009;12:1053–1061. [DOI] [PubMed] [Google Scholar]
- 25. Vassar M, Holzmann M. The retrospective chart review: important methodological considerations. J Educ Eval Health Prof. 2013;10:12. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26. Cornally N, McCarthy G. Help-seeking behaviour for the treatment of chronic pain. Br J Community Nurs. 2011;16:90–98. [DOI] [PubMed] [Google Scholar]
- 27. Thorstensson CA, Gooberman-Hill R, Adamson J, Williams A, Dieppe P. Help-seeking behaviour among people living with chronic hip or knee pain in the community. BMC Musculoskeletal Disorders. 2009;10:153. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 28. US Department of Health and Human Services; Food and Drug Administration; Center for Drug Evaluation and Research (CDER); Center for Biologics Evaluation and Research (CBER). Guidance for industry. E 10 choice of control group and related issues in clinical trials. https://permanent.access.gpo.gov/LPS113943/LPS113943/www.fda.gov/downloads/RegulatoryInformation/Guidances/ucm129460.pdf. Published May 2001. Accessed September 25, 2018.
- 29. Yavuz BB, Cankurtaran M, Halil M, Dagli N, Kirkpantur A. Renal dysfunction after oral acyclovir treatment in a geriatric woman: a case report. Scand J Infect Dis. 2005;37:611–613. [PubMed] [Google Scholar]
- 30. Becker BN, Fall P, Hall C, et al. Rapidly progressive acute renal failure due to acyclovir: case report and review of the literature. Am J Kidney Dis. 1993;22:611–615. [DOI] [PubMed] [Google Scholar]
- 31. Berry L, Venkatesan P. Aciclovir-induced neurotoxicity: utility of CSF and serum CMMG levels in diagnosis. J Clin Virol. 2014;61:608–610. [DOI] [PubMed] [Google Scholar]
- 32. Le Cleach L, Trinquart L, Do G, et al. Oral antiviral therapy for prevention of genital herpes outbreaks in immunocompetent and nonpregnant patients. Cochrane Database Syst Rev. 2014;(8):CD009036. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 33. Lam NN, Weir MA, Yao Z, et al. Risk of acute kidney injury from oral acyclovir: a population-based study. Am J Kidney Dis. 2013;61:723–729. [DOI] [PubMed] [Google Scholar]
- 34. Patton LL. Ability of HIV/AIDS patients to self-diagnose oral opportunistic infections. Community Dent Oral Epidemiol. 2001;29:23–29. [PubMed] [Google Scholar]
- 35. Schmader K, George LK, Newton R, Hamilton JD. The accuracy of self-report of herpes zoster. J Clin Epidemiol. 1994;47:1271–1276. [DOI] [PubMed] [Google Scholar]
- 36. Leichliter JS, Lewis DA, Sternberg M, Habel MA, Paz-Bailey G. Health care seeking among men with genital ulcer disease in South Africa: correlates and relationship to human immunodeficiency virus-1 and herpes simplex virus type 2 detection and shedding. Sex Transm Dis. 2011;38:865–870. [DOI] [PubMed] [Google Scholar]
- 37. Agambire R, Clerk C. Healthcare seeking and sexual behaviour of clients attending the Suntreso STI clinic. J Biol Agric Healthcare. 2014;3:92–100. [Google Scholar]