Summary
A 50-year-old male patient with a secundum-type atrial septal defect (ASD) suffering from respiratory distress for 7 days was referred to our hospital. Transthoracic echocardiography demonstrated the defects of 9 mm and 4 mm in the middle atrial septum in the parasternal four-chamber view. However, we found not 2, but 6 atrial defects by using real time 3-dimensional transesophageal echocardiography. Open heart surgery was not indicated, because his pulmonary function was poor. After fully informed consent, we decided to treat ASD with Amplatzer septal occluders.
Keywords: Real time 3-dimensional transoesophageal echocardiography, Atrial septal defect, Amplatzar septal occluder
Introduction
The closure of atrial septal defect (ASD) is now routinely performed by using a percutaneous approach under echocardiographic guidance. Centrally located secundum defects are ideal for device closure, but there is considerable morphological variation in size and location of the defects 1, 2, 3. A small proportion of ASDs may have multiple fenestrations and these are often considered unsuitable for device closure [4]. We report the case of a 50-year-old male patient with multiple ASDs and poor pulmonary function. He had 6 defects in the atrial septum and two Amplatzer septal occluders (ASOs; AGA Medical Corporation, Golden Valley, MN, USA) were implanted successfully.
Case report
A 50-year-old male patient with a secundum-type ASD suffering from respiratory distress for 7 days was referred to our hospital for further treatment. He was diagnosed with asymptomatic ASD for many years. He did not have palpitations, sweating, or chest pain. Furosemide and digoxin were used but his symptoms did not improve.
Physical examination on admission revealed a pale, middle-aged man in mild respiratory distress, with a heart rate of 105 beats/min, a blood pressure of 130/80 mmHg, a body temperature of 36.5 °C, and a respiratory rate of 19 beats/min. A grade 4/6 systolic murmur was audible in pulmonary valve auscultation area. The spleen and liver were not palpable. There was no lower extremity edema. The remainder of his physical examination was unremarkable. The surface 12-lead electrocardiogram showed sinus arrhythmia, increased magnitude anterior of first portion of P, mild depression of ST segment in V1–V2, and incomplete right bundle branch block. The chest X-ray found increased lung markings and pulmonary artery segment bulging.
Transthoracic echocardiography (TTE) demonstrated the defects of 9 mm and 4 mm in the middle atrial septum in the parasternal four-chamber view. The right atrium and right ventricle were enlarged. There was mild mitral, tricuspid, and pulmonary regurgitation. Notably, TTE also showed that the pulmonary valves were thickened and calcified, and that the peak systolic pulmonary velocity was 287 cm/s. His pulmonary function test showed severe pulmonary obstruction from his 30-year smoking (forced expiratory volume in 1 s 0.68 L, forced vital capacity 1.36 L). Arterial blood gas analysis showed type two respiratory failure (pH 7.39, PCO2 65 mmHg, PO2 55 mmHg). The patient was subsequently treated with dieresis, reducing sputum, anticoagulation, and lipid-lowering therapy for improving pulmonary function.
Ten days after admission, the arterial blood pH was 7.44, PCO2 was 49 mmHg, and PO2 was 64 mmHg. The decision for transcatheter intervention therapy was made on the basis of TTE findings and his poor pulmonary function. During operation, real time 3-dimensional transesophageal echocardiography (RT-3D-TEE, Philips iE33, Eindhoven, The Netherlands) and fluoroscopy guidance were used simultaneously during all placements of the occluder device. Right catheterization showed the pressure gradient through the pulmonary valve was less than 20 mmHg, so there was no need to repair the pulmonary valve. During the operation, we found not 2, but 6 atrial septal defects by using RT-3D-TEE. The biggest hole was about 18 mm in the inferoposterior of the interatrial septum, the other 5 defects were around the biggest hole (Fig. 1). Open heart surgery was not indicated, because his pulmonary function was poor. After fully informed consent, we decided to use ASO. Under the guidance of RT-3D-TEE, we occluded the biggest defects with 28 mm occluder, at first. The remaining defects were smaller, but there was still a 7 mm residual shunt (Fig. 2), then, we chose a 12 mm occluder. We found no residual shunt (Fig. 3), and pulling and pushing of the delivery cable ensured that the devices were in a secure and stable position. One week later, follow-up TTE showed no residual shunt. We successfully completed the closure.
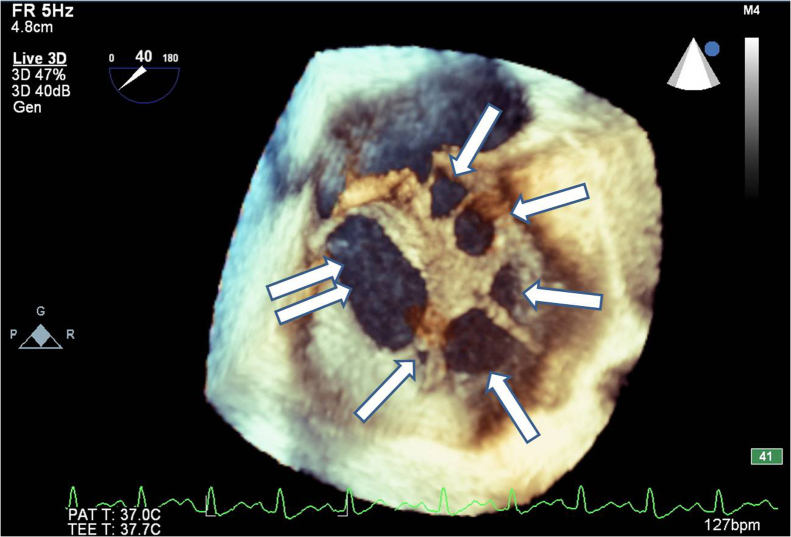
Figure 1.
Real time 3-dimensional transesophageal echocardiography showed 6 holes in the interatrial septum, the biggest one was in the inferoposterior of the interatrial septum (double arrow), the other 5 were around the biggest hole (single arrow).
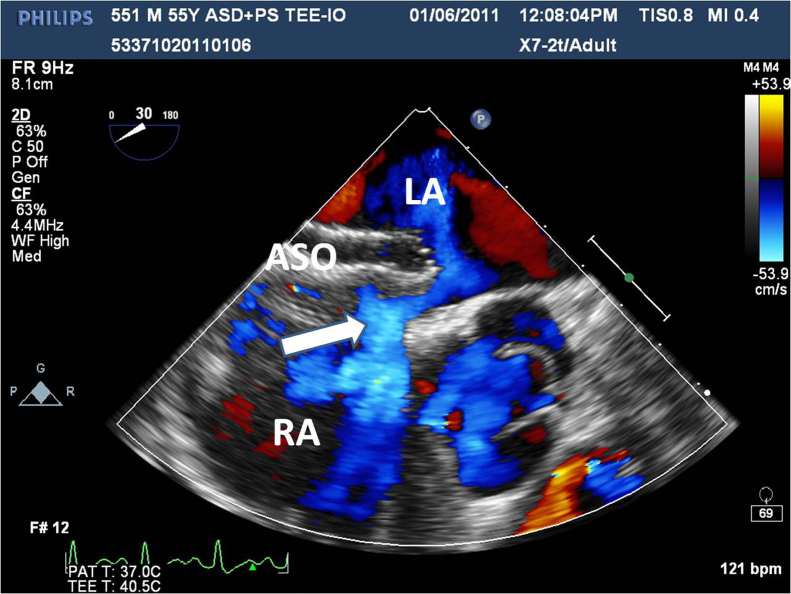
Figure 2.
After occlusion of the biggest defects with a 28 mm occluder, there was still 7 mm residual shunt. ASO, Amplatzer septal occluder; LA, left atrium; RA, right atrium.
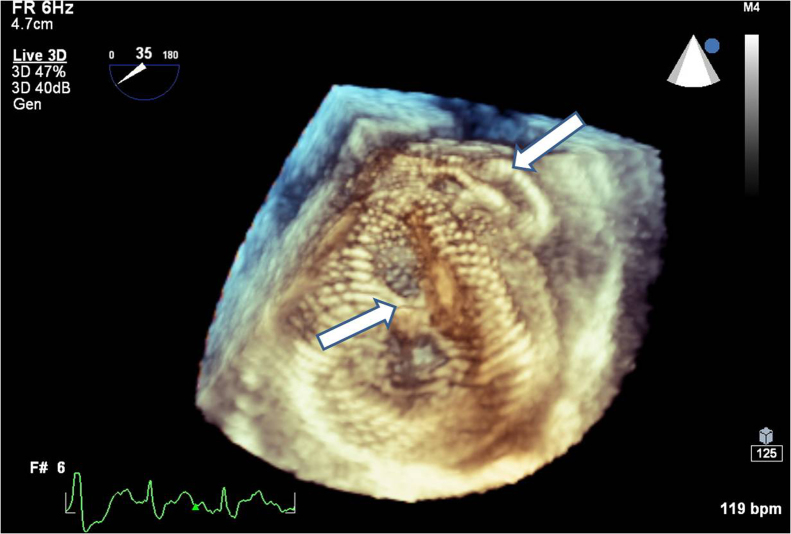
Figure 3.
Real time 3-dimensional transesophageal echocardiography showed the two occluders.
Discussion
ASD closure is now routinely performed using a percutaneous approach under echocardiographic guidance. Centrally located, secundum defects are ideal for device closure but there is considerable morphological variation in size and location of the defects. A small proportion of ASDs may have multiple fenestrations and these are often considered unsuitable for device closure [5].
The selection of patients for transcatheter or surgical closure of a secundum ASD requires accurate information regarding the anatomy of the defect such as its maximal diameter and the amount of circumferential tissue rim [2]. RT-3D-TEE is the only means to get the exact morphology of the ASD in the beating heart for pediatric interventional cardiologists, such as the size, position in the interatrial septum, proximity to surrounding structures, and adequacy of septal rim [1]. The image by TTE, which is noninvasive for children, is limited 2, 3. RT-3D-TEE is a technology allowing on-line guidance of atrial septal occlusion device deployment; such imaging should increase delivery safety and decrease fluoroscopy time [4].
RT-3D-TEE was also used to guide the measurement of the stretched diameter of ASD, which is the diameter of the ASD after the balloon sizing to ensure no residual color flow through the balloon (Amplatzer sizing balloon). The ASO was released only when TEE showed no or only trivial residual color flow through the connecting stent; otherwise, repositioning of the stent would be required. The final assessment of the position of the device was performed by TEE after its release. Many previous studies showed the usefulness of RT-3D-TEE in visualizing the morphological characteristics of ASD and its potential as a new method for selecting the size of the Amplatzer septal occluder 2, 3.
Awad et al. [6] studied 33 patients with multiple ASDs. The mean diameters of the larger and smaller defects were 12.9 and 7.7 mm, the mean larger and smaller device diameters were 19.0 and 13.4 mm, respectively. After 34.8 ± 25.7 months of follow-up, the device closure of multiple ASDs using multiple ASOs is safe and effective. The use of RT-3D-TEE provided useful information for transcatheter closure of multiple ASDs using two devices. RT-3D-TEE enhanced our ability to image and understand the spatial relationship of the ASD anatomy [7].
This case of multiple ASDs had 6 holes in the atrial septum, the largest defect diameter was 18 mm, the smaller one was 8 mm. We used 28 and 12 mm ASOs to close the defects, respectively. Despite a trivial shunt after the occlusion, TTE immediately after the operation and at 3 months follow-up showed that device closure of multiple ASDs using multiple ASOs was safe and effective.
References
- 1.Lin S.M., Tsai S.K., Wang J.K., Han Y.Y., Jean W.H., Yeh Y.C. Supplementing transesophageal echocardiography with transthoracic echocardiography for monitoring transcatheter closure of atrial septal defects with attenuated anterior rim: a case series. Anesth Analg. 2003;96:1584–1588. doi: 10.1213/01.ANE.0000062651.59656.B4. [DOI] [PubMed] [Google Scholar]
- 2.Acar P. Three-dimensional echocardiography in children with atrial septal defect. Minerva Pediatr. 2004;56:29–40. [PubMed] [Google Scholar]
- 3.Acar P., Roux D., Dulac Y., Rougé P., Aggoun Y. Transthoracic three-dimensional echocardiography prior to closure of atrial septal defects in children. Cardiol Young. 2003;13:58–63. doi: 10.1017/s1047951103000118. [DOI] [PubMed] [Google Scholar]
- 4.Mitchell A.R., Roberts P., Eichhöfer J., Timperley J., Ormerod O.J. Echocardiographic assessment and percutaneous closure of multiple atrial septal defects. Cardiovasc Ultrasound. 2004;2:9. doi: 10.1186/1476-7120-2-9. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Acar P., Massavuau P., Elbaz M. Real-time 3D transoesophageal echocardiography for guiding Amplatzer septal occlude device deployment in an adult patient with atrial septal defect. Eur J Echocardiogr. 2008;9:822–823. doi: 10.1093/ejechocard/jen178. [DOI] [PubMed] [Google Scholar]
- 6.Awad S.M., Garay F.F., Cao Q.L., Hijazi Z.M. Multiple Amplatzer septal occlude devices for multiple atrial communications: immediate and long-term follow-up results. Catheter Cardiovasc Interv. 2007;70:265–273. doi: 10.1002/ccd.21145. [DOI] [PubMed] [Google Scholar]
- 7.Cao Q., Radtke W., Berger F., Zhu W., Hijazi Z.M. Transcatheter closure of multiple atrial septal defects, initial results and value of two-and three-dimensional transoesophageal echocardiography. Eur Heart J. 2000;21:941–947. doi: 10.1053/euhj.1999.1909. [DOI] [PubMed] [Google Scholar]