ABSTRACT
Breastfeeding initiation and duration are decreased in adolescent mothers compared to older mothers. A prospective descriptive cohort design was used to explore personal, social, cultural, and infant factors that explain and predict breastfeeding initiation and maintenance at 4 weeks postpartum. Adolescent mothers (N = 120) were recruited at prenatal clinics in Thailand. Data were collected at enrollment, during birth hospitalization (N = 102), and at 4 weeks postpartum (N = 96). Findings revealed breastfeeding attitudes, social support, and cultural beliefs about “being a good mother” were positively correlated with breastfeeding initiation. Furthermore, breastfeeding attitudes and social support were significant positive predictors of exclusive breastfeeding (both p ≥ .01) continuation through 4 weeks, whereas infant temperament was a significant negative predictor (p ≥ .04). Maternal competence at 4 weeks postpartum was also positively correlated with exclusive breastfeeding continuation.
Keywords: exclusive breastfeeding, breastfeeding attitude, maternal competence infant temperament, adolescent mothers
Globally, the number of adolescent mothers continues to increase (World Health Organization, 2008), yet adolescent mothers have the lowest rate of breastfeeding worldwide (Centers for Disease Control and Prevention, 2015). Similarly in Thailand, breastfeeding performance in adolescent mothers is considered poor. There are efforts to increase the incidence and duration of breastfeeding in Thailand, including national programs to increase awareness as well as initiation of educational interventions. According to the Breastfeeding Friendly Hospital Initiative in Thailand, specific guidelines to promote continued breastfeeding exist. However, in a Thai national survey (2003–2008), only 17% of adolescent mothers continued breastfeeding at 6 months, compared to 45% of mothers aged 20–29 years and 51% of women aged 30 and older (Bureau of Health Promotion, 2006; Laisiriruangrai, Wiriyasirivaj, Phaloprakarn, & Manusirivithaya, 2008).
In a Thai national survey (2003–2008), only 17% of adolescent mothers continued breastfeeding at 6 months, compared to 45% of mothers aged 20–29 years and 51% of women aged 30 and older.
Spear (2006) found that, although more than 39% of adolescent mothers intended to breastfeed for at least 6 months after birth, only 6% actually continued breastfeeding until 6 months. Likewise, Misra and James (2000) found that in the United States, although some adolescent mothers might begin with exclusive breastfeeding at birth, 95% of those mothers provided some infant formula feedings before the infant was 2 weeks of age, further reducing the number of infants receiving breastmilk for the first 6 months.
There are several factors that may contribute to the initiation and continuation of breastfeeding in adolescent mothers. Research indicates that, when compared to older mothers, adolescent mothers interact with their babies with a more controlling style (Hanna, 2001), which has consistently been linked to less positive parenting and feeding choices (Crnic, Gaze, & Hoffman, 2005). Adolescent motherhood not only has negative consequences related to the teenage mother’s social and educational well-being but her child is also more likely to have problems with physical health and cognitive development compared to a child born to an older mother (Moore & Brooks-Gunn, 2002).
Moreover, research has indicated that a mother’s psychosocial developmental level influences her ability to parent and that adolescent mothers do not maintain the same psychosocial developmental trajectory as adolescents who are not mothers (Shapiro-Mendoza, Selwyn, Smith, & Sanderson, 2007). Adolescents have not reached adult developmental maturity in a variety of different social and cognitive dimensions. For example, during adolescence, individual progress from concrete to formal operational thinking often occurs, providing a foundation for better problem solving (Borkowski et al., 2002). This developmental process adversely affects a young woman’s ability to parent because many mothering tasks draw from an adult woman’s social and cognitive abilities to respond, guide, and make choices that benefit the child even though the mother herself may not benefit in the same ways. Consequently, it is important to gain a deeper understanding of motherhood within the context of adolescent psychosocial development.
Breastfeeding as a specific task of motherhood is correlated with a wide range of beneficial outcomes that could be particularly applicable to adolescent mothers and their children (Bartok, 2011; Dewey, 2003). Infants who are breastfed have a reduced rate of respiratory infections, ear infections, diarrhea, childhood obesity, asthma, and lower rates of infant morbidity and hospitalization (Gartner et al., 2005). Although breastfeeding is beneficial for both the mother and infant, the breastfeeding rates remain low in this age group, and the needs of adolescent mothers around infant feeding choices also remain poorly understood (Dykes, Moran, Burt, & Edwards, 2003). Various explanations for the low rates of breastfeeding among adolescent mothers have been considered. First, adolescent mothers are more likely than older mothers to be single and to have lower levels of education and income—characteristics that are often negatively associated with breastfeeding (Park, Meier, & Song, 2003). The personal factor of attitude is also viewed as associating intentions for breastfeeding in the prenatal period with initiation and continuation of breastfeeding in the postpartum period. Wambach and Koehn (2004) explained that adolescent mothers have both positive and negative attitudes toward decision making about infant feeding methods and breastfeeding continuation. Furthermore, numerous studies have revealed that the factors associated with initiation and continuation of breastfeeding in mothers may not only depend on personal perspectives about breastfeeding but also are related to infant responses and social expectations, as well as types of support provided by family and friends (Kong & Lee, 2004). The early postpartum period is an important transitional period for the mother and her infant. Breastfeeding initiation occurs during this critical period, and particularly for adolescent mothers who are also experiencing the new and sometimes ambiguous role of mothering, breastfeeding performance can seem very demanding and difficult to achieve (Mossman, Heaman, Dennis, & Morris, 2008).
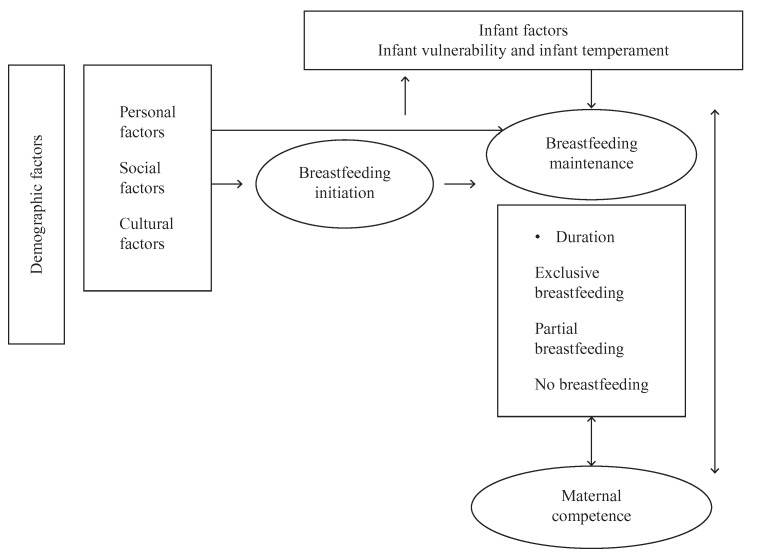
Thus, the purpose of this study was to obtain a better understanding of factors associated with breastfeeding practices, especially initiation and continuation among adolescent mothers in Thailand. Specific aims were to (a) evaluate relationships among breastfeeding initiation and personal, social, and cultural factors during pregnancy; (b) define predictive factors associated with breastfeeding initiation; (c) explore relationships among breastfeeding continuation and personal, social, cultural, and infant factors in the postpartum period; (d) define predictive factors associated with breastfeeding continuation; and (e) evaluate the relationship between breastfeeding continuation and maternal competence in Thai adolescent mothers. The study was based on conceptual framework of breastfeeding in adolescent mothers as shown in Figure 1.
Figure 1.
Conceptual framework of breastfeeding in adolescent mothers.
METHOD
Study Design and Setting
This research was a prospective descriptive cohort study. Thai adolescent mothers were recruited from prenatal clinics in one of two large, Baby Friendly Hospitals in Saraburi and Lopburi provinces in the central region of Thailand. There were three time points for data collection. First, mothers were enrolled during the prenatal period between 34 and 40 weeks’ gestation in the prenatal care clinic. During enrollment, adolescent mothers who voluntarily agreed to participate in the study and completed informed consent were asked to complete questionnaires related to breastfeeding (first data point). Then, within 48 hours from birth during the early postpartum period in the hospital, mothers again were asked to complete questionnaires related to breastfeeding initiation (second data point). Finally at 4–5 weeks postpartum, mothers once more completed the questionnaires during their postpartum visits (third data point). Each time, questionnaires took approximately 30 minutes to complete.
Ethical issues for study participation were a major consideration for this population because of the participant’s vulnerability in term of age and maturity. We were very careful in designing the study to “do no harm,” “carefully explain informed consent,” and “maintain confidentiality for the participants.” The study was approved by the Virginia Commonwealth University Institutional Review Board. Also in each Thai setting, the study was approved by the Ethical Committee of Phraputtabath and King Narai Hospital, Thailand.
Participants
Thai pregnant women 14–19 years of age participated in the study. Inclusion criteria were (a) pregnant between 34 and 40 weeks’ gestation at enrollment; (b) able to read, write, and understand Thai; and (c) primigravida. Exclusion criteria were pregnancy complicated by multiples or comorbidities. Participants were administratively withdrawn if their infants were born preterm, with an abnormality, or admitted to the neonatal intensive care unit (NICU).
Measurement
Predictive variables included in the study design were personal, social, cultural, and infant factors. Outcome variables consisted of breastfeeding initiation, exclusive breastfeeding continuation, and degree of maternal competence at 4 weeks. Instruments used to measure these variables are described in the following texts.
The Iowa Infant Feeding Attitude Scale (IIFAS; de la Mora, Russell, Dungy, Losch, & Dusdieker, 1999) consists of 17 items and has been used to predict infant feeding choices, as reflected by behavioral intentions and actual feeding behavior (duration). A high scale indicated high intention to breastfeed. In this study, the IIFAS was measured during late pregnancy and at 4 weeks postpartum with good internal consistency (Cronbach’s α = .87 and .89, respectively).
The Iowa Infant Feeding Attitude Scale consists of 17 items and has been used to predict infant feeding choices, as reflected by behavioral intentions and actual feeding behavior (duration).
The Breastfeeding Influencing Factor Assessment (BIFA) consists of 39 items modified from a tool, which to our knowledge had only been used once in a study in Hong Kong with adult mothers (Kong & Lee, 2004). Although its original psychometric properties were poorly reported, the unnamed, original instrument contained most but not all the factors we intended to measure in the context of breastfeeding. Thus, we modified the instrument by adding two cultural items. The modified BIFA was used to reflect breastfeeding behaviors of intention, initiation, and continuation, along with 15 items of personal (BIFAp), 11 items of social (BIFAs), and 13 items of cultural (BIFAc) categories. A high score of BIFA indicated high breastfeeding behaviors. The BIFA was used during late pregnancy and at 4 weeks postpartum with good internal consistency (α = .84 and .87, respectively).
The Hughes Breastfeeding Support Scale (HBSS; Hughes, 1984) is a 30-item instrument designed to measure a breastfeeding mother’s perception of support. The HBSS was previously translated from English to Thai (Ratananugool, 2001). High scores on the HBSS indicate high perception of support. The HBSS was used during late pregnancy and 4 weeks postpartum visit with good internal consistency (α = .89 and .91, respectively).
The Pictorial Assessment of Temperament (PAT; Clarke-Stewart, Fitzpatrick, Allhusen, & Goldberg, 2000) includes 10 vignettes, each demonstrating different infant temperaments in response to events. High scores on the PAT indicate low infant temperament. The Vulnerable Baby Scale (VBS; Kerruish, Settle, Campbell-Stokes, & Taylor, 2005) has 10 items designed to measure parents’ perceptions of baby vulnerability. Questions addressed current concerns of mothers regarding their babies. High scores indicate more maternal concerns about their infants. Both the PAT and VBS were used at the 4 weeks postpartum visit. The PAT had strong internal consistency (α = .87), whereas the VBS had acceptable internal consistency (α = .74). The Parenting Sense of Competence Scale (PSOC; Johnston & Mash, 1989) is a 17-item scale designed to measure parents’ self-efficacy and parenting role satisfaction. High scores on the PSOC indicate high maternal self-efficacy and maternal role satisfaction. The PSOC was used at the 4 weeks postpartum visit; the internal consistency was good (α = .88).
Exclusive breastfeeding continuation was defined as the total number of only exclusive breastfeeding days from birth to 4 weeks postpartum as reported by the mother. Feeding methods were classified as exclusive breastfeeding (receiving all breastmilk either at breast or in bottles), partial breastfeeding (receiving some breastmilk and some infant formula), and all infant formula feeding by maternal report.
Translation Process
The IIFAS, BIFA, PAT, VBS, and PSOC were not available in the Thai language, thus requiring translation. Beaton, Bombardier, Guillemin, and Ferraz (2007) recommend a systematic approach for translation to ensure semantic and content equivalence—the two major dimensions of cross-culture translations. Each item in the original and back-translated versions was ranked in terms of comparability of language and similarity of interpretability. Using this well-delineated process, we identified potentially problematic items and re-translated them until the items were deemed appropriate. Translated instruments were reviewed by three maternal and child health nursing experts: two were faculty from schools of nursing and one was a postpartum care nurse. The instruments were pretested with 20 Thai adolescent mothers to ensure clarity in meaning and understanding. The Cronbach’s alpha for the Thai versions of the instruments used in this study was between .64 and .77, demonstrating good internal consistency.
Data Analysis
Descriptive statistics were used to summarize demographic characteristics, personal, social, cultural, and infant factors, with study outcomes of breastfeeding initiation and continuation through 4 weeks as well as maternal competence. Pearson correlation coefficients were used to examine relationships among the variables. Variables with p values less than 0.2 were included in multivariate analyses to determine relationships when controlling for other explanatory variables. Univariate and multiple linear regression analyses were used to analyze relationships between the predictive factors and breastfeeding duration. Confounders and effect modifiers were evaluated in the multivariate analyses. An independent t test was used to evaluate the difference within maternal competence scores between exclusive and partial breastfeeding. The Cronbach’s alpha was used to identify internal consistency of the instruments. All tests were considered to be significant at p values less than 0.05.
RESULTS
A sample of 120 adolescents at 34–40 weeks’ gestation was recruited; 102 participants provided data in the early postpartum period in the hospital, and 96 participants were followed through 4 weeks postpartum. Of the 24 participants who did not provide data in the postpartum period, 9 had infants admitted to NICU, and 9 did not birth at the study hospital. Of the remaining 102 participants, 6 participants were lost to follow-up at 4 weeks postpartum, yielding an overall attrition rate of 20%. There were no differences in the demographic variables between those who did and did not remain in the study.
The sample’s ages ranged between 14 and 19 years, with a mean of 16.75 years (SD = 1.5). The partner’s average age was 20.3 years (SD = 4.1). Half of partners (51.1%) had completed middle school, and most of the mothers were still in high school. Many of the adolescent mothers (73.5%) were unemployed. On average, the adolescent mothers were 35 weeks pregnant at recruitment. All adolescent mothers reported that breastfeeding was the best choice for infant feeding. Most of the mothers (60.8%) reported making the decision about infant feeding methods during the early prenatal period. The vast majority of adolescent mothers (91.2%) who reported making a decision about an infant feeding method during pregnancy intended to breastfeed. Additional demographic data are presented in Table 1.
TABLE 1. Demographic Data at Enrollment.
| Characteristics (N = 102) | n | % |
|---|---|---|
| Marital status | ||
| Single or separate | 12 | 11.8 |
| Living with partner | 56 | 54.9 |
| Married | 34 | 33.3 |
| Maternal education | ||
| Elementary school | 13 | 12.7 |
| Middle school | 64 | 62.7 |
| High school | 12 | 11.8 |
| College | 13 | 12.8 |
| When feeding decision made during pregnancy | ||
| At 1–3 months | 62 | 60.8 |
| At 4–6 months | 22 | 21.6 |
| At 5–9 months | 9 | 8.8 |
| Not decided during pregnancy | 9 | 8.8 |
Infant birth weight averaged 2,959.1 g (SD = 0.9) and mean birth gestation was 38.8 weeks (SD = 0.9), with 93.1% of the infants birthed vaginally. Most of the adolescent mothers in this study (93.1%) initiated breastfeeding within 48 hours during their initial hospital stay; only 6.9% did not initiate breastfeeding. At 4 weeks postpartum, overall average continuation of exclusive breastfeeding was reported to be 24.4 days (SD = 9.9). Half of the sample (53.1%) continued exclusive breastfeeding at 4 weeks, 42.7% of the mothers were providing partial breastfeeding, and 4.2% of the mothers were infant formula feeding their infants. In addition, the partial breastfeeding group reported the mean exclusive breastfeeding days as 13.3, whereas mothers who were infant formula feeding continued exclusive breastfeeding for an average of only 2.7 days as shown in Table 2.
TABLE 2. Breastfeeding (BF) at Four Weeks Postpartum.
| Feeding Method (N = 96) | n | % | Exclusive BF Days M (SD) |
|---|---|---|---|
| Exclusive breastfeeding | 51 | 53.1 | 28.25 (2.85) |
| Partially breastfeeding | 41 | 42.7 | 13.26 (6.60) |
| No breastfeeding | 4 | 4.2 | 2.75 (0.95) |
Significant correlations existed among associated factors and breastfeeding initiation during the early postpartum period (Table 3). For example, we found that personal, social support, and cultural factors had significant relationships with breastfeeding initiation. Adolescent mothers with higher scores in personal, social, and cultural factors were noted to have higher rates of breastfeeding initiation. For univariate regression analysis (Table 4), the significant correlation of exclusive breastfeeding continuation consisted of personal factors, social factors, infant temperament, and prenatal visits. Multiple regression analysis (Table 5) was used to understand which variables predicted exclusive breastfeeding continuation. Personal, social, cultural, and infant factors, with demographic variables, explained 59.3% of the variance in exclusive breastfeeding continuation. However, after controlling confounders and interactions, the demographic variables were not significantly predictive of exclusive breastfeeding continuation. The standard coefficient (β) indicated that feeding attitudes and social influence were significant positive predictors, and infant temperament was a significant negative predictor of exclusive breastfeeding continuation. Thus, greater feeding attitudes, social influences, and lower infant temperament scores predicted longer continuation of exclusive breastfeeding.
TABLE 3. Factors Associated With BF Initiation During the First 48 Hours PP.
| Influencing Factors for Mothers Who Initiated BF (N = 102) | Instrument M (SD) | r | p |
|---|---|---|---|
| Personal factors | |||
| IIFAS | 4.13 (0.32) | 0.55 | 0.01 |
| BIFA personal attitude | 4.21 (0.34) | 0.46 | 0.01 |
| Social factors | |||
| BIFA social influence | 3.63 (0.34) | 0.08 | 0.58 |
| HBSS | 3.21 (0.45) | 0.21 | 0.05 |
| Cultural factors | |||
| BIFA cultural norm | 3.87 (0.36) | 0.46 | 0.01 |
Note. BF = breastfeeding; PP = postpartum; IIFAS = Iowa Infant Feeding Attitude Scale; BIFA = Breastfeeding Influencing Factor Assessment; HBSS = Hughes Breastfeeding Support Scale.
TABLE 4. Univariate Regression of EBF Continuation Through Four Weeks With Associated Factors.
| Covariate | β | SE | p |
|---|---|---|---|
| Personal factors | |||
| IIFAS | 19.09 | 2.71 | .01 |
| BIFA personal attitude | 13.82 | 2.40 | .01 |
| Social factors | |||
| BIFA social influences | 14.75 | 1.69 | .01 |
| HBSS | 15.85 | 2.51 | .01 |
| Cultural factors | |||
| BIFA cultural norm | 3.68 | 2.38 | .12 |
| Infant factors | |||
| Infant vulnerability (VBS) | 3.18 | 2.45 | .19 |
| Infant temperament (PAT) | −7.69 | 1.94 | .01 |
| Age | 0.93 | 0.65 | .15 |
| Education | 0.40 | 0.12 | .74 |
| Times of prenatal visits | 0.77 | 0.37 | .03 |
Note. EBF = exclusive breastfeeding; IIFAS = Iowa Infant Feeding Attitude Scale; BIFA = Breastfeeding Influencing Factor Assessment; HBSS = Hughes Breastfeeding Support Scale; VBS = Vulnerable Baby Scale; PAT = Pictorial Assessment of Temperament.
TABLE 5. Multivariate Regression of EBF Continuation Through Four Weeks With Associated Predictors.
| Covariate | β | SE | p |
|---|---|---|---|
| Step 1—Influencing factors | |||
| Personal factors | |||
| IIFAS | 8.42 | 2.84 | .004 |
| BIFA personal attitude | 3.25 | 2.37 | .17 |
| Social factors | |||
| BIFA social influences | 9.25 | 2.18 | .001 |
| HBSS | 1.17 | 2.86 | .68 |
| Cultural factors | |||
| BIFA cultural norm | 1.03 | 1.72 | .55 |
| Infant factors | |||
| Infant vulnerability (VBS) | 0.50 | 1.71 | .76 |
| Infant temperament (PAT) | −3.18 | 1.58 | .04 |
| Step 2—Addition of demographic variables | |||
| Personal factors | |||
| IIFAS | 8.42 | 2.84 | .01* |
| BIFA personal attitude | 3.25 | 2.38 | .15 |
| Social factors | |||
| BIFA social influences | 9.26 | 2.18 | .01* |
| HBSS | 1.16 | 2.86 | .48 |
| Cultural factors | |||
| BIFA cultural norm | 1.03 | 1.73 | .55 |
| Infant factors | |||
| Infant vulnerability (VBS) | 0.51 | 1.71 | .76 |
| Infant temperament (PAT) | −3.18 | 1.58 | .04* |
| Age | 0.72 | 0.46 | .11 |
| Education | 1.29 | 0.87 | .13 |
| Time of prenatal visits | 0.20 | 0.27 | .43 |
Note. For step 1, R2 change = 0.568, p < .001; Step 2, R2 change = 0.593, p < .001. EBF = exclusive breastfeeding; IIFAS = Iowa Infant feeding Attitude Scale; BIFA = Breastfeeding Influencing Factor Assessment; HBSS = Hughes Breastfeeding Support Scale; VBS = Vulnerable Baby Scale; PAT = Pictorial Assessment of Temperament.
*p < .05.
Greater feeding attitudes, social influences, and lower infant temperament scores predicted longer continuation of exclusive breastfeeding.
Maternal competence was found to have a significant relationship with infant feeding methods. Adolescent mothers who continued exclusively breastfeeding their infants at 4 weeks were more likely to report higher levels of maternal competence than adolescent mothers who were only partially breastfeeding or infant formula feeding their infants. Moreover, higher maternal competence scores were associated with a greater number of exclusive breastfeeding days in adolescent mothers. In addition, there was a significant negative correlation between maternal competence and infant temperament. Higher maternal competence scores were associated with lower scores in infant temperament, indicating that adolescent mothers who perceived higher satisfaction with the maternal role tended to perceive their infants as being less irritable.
DISCUSSION
Breastfeeding attitudes, social support, and cultural factors about “being a good mother” were found to be significantly positive correlations with breastfeeding initiation in adolescent mothers. As found in our study and previous studies, personal factors including perceived benefit of breastfeeding and attitudes about breastfeeding are associated with breastfeeding initiation. Similar to the findings of Hannon, Willis, Bishop-Townsend, Martinez, and Scrimshaw (2000) and Nelson and Sethi (2005), our study determined that the major reasons provided for initiating breastfeeding were related to infant benefits. Thus, information provided about breastfeeding benefits during pregnancy may assist the adolescent mother in making decisions about breastfeeding initiation. Also, these findings are congruent with previous findings that adolescent mothers with more positive prenatal attitudes about breastfeeding are more likely to initiate breastfeeding (Mossman et al., 2008).
Social factors were found to be important to adolescent mothers. Most adolescent mothers agreed that encouragement and support from their partner or husband were important. Cultural factors related to the belief that “being a good mother” is important and this belief was found to be generally supportive of exclusive breastfeeding. We found that cultural factors were important to the initiation of breastfeeding. In the Thai culture, breastfeeding is considered an important aspect of the maternal role. A significant number (n = 89 [87.2%]) of the adolescent mothers agreed that “breastfeeding makes me feel I am a good mother.” We also found high intercorrelations among personal, social, and cultural factors that make separating these issues difficult. Although the identified associating factors were indeed correlated with breastfeeding initiation in these adolescent mothers, hospital guidelines also played a key role in breastfeeding initiation. However, the small number of participants (n = 4) who did not initiate breastfeeding in the hospital setting limits full evaluation of the effects of influencing factors in the early postpartum period.
We theoretically considered personal, social, and cultural factors as well as infant factors to be predictors of exclusive breastfeeding continuation, and we found empirical support for many of these predictors. Similar to Spear’s findings (2006), we found breastfeeding duration in adolescent mothers was related to perceived breastfeeding benefits and support from family and friends. The important support role of the adolescent’s mother is crucial to consider when providing information to pregnant adolescent women. Furthermore, when infant temperament was perceived as easier, continuation of exclusive breastfeeding was longer. Similarly, de Lauzon-Guillain et al. (2012) found that perceptions of a more difficult infant were associated with lower breastfeeding rates in adult mothers. In another study, more irritable infant temperament was associated with earlier introduction of solid foods (Wasser et al., 2011).
In our study, exclusive breastfeeding continuation decreased quickly, with almost half of those who initiated exclusive breastfeeding providing some partial or all infant formula feeding within the first 2 weeks postpartum. Glass, Tucker, Stewart, Baker, and Kauffman (2010) also reported that with adolescent mothers who initiated breastfeeding in the hospital, exclusive breastfeeding duration dropped to half by 6 weeks postpartum. We found that the main reasons mothers provided for cessation of exclusive breastfeeding included returning to work or school, insufficient breastmilk supply, and pain. Our findings correspond with the results of previous research (Tucker, Wilson, & Samandari, 2011). Although cultural norms encourage mothers to breastfeed, more than half of adolescent mothers (60.5%) agreed with the statement, “I would feel embarrassed if someone saw me breastfeeding.” Similar to Wambach and Koehn (2004), concern about embarrassment, self-consciousness, and fear related to breastfeeding in public was a concern in our study as well.
We also grew to understand the correlation between breastfeeding and maternal competence in adolescent mothers. Acquiring maternal competence is considered maturational within the maternal role attainment. Gaining this maturity while also being an adolescent mother has been questioned, largely because these young women have other developmental tasks to be attained. Adolescent mothers in this study, with longer durations of exclusive breastfeeding, also had higher maternal competence. New mothers need positive experiences related to infant caregiving to enhance maternal competency, thus highlighting the importance of understanding Thai cultural attitudes about breastfeeding and the maternal role. As mothers, adolescents who continue breastfeeding exclusively may attain increased maternal skills and satisfaction with the maternal role. Most adolescent mothers reported that they were satisfied and felt very good when they were breastfeeding their infants.
Study Limitations
Several limitations need to be considered. As noted, hospital policies tended to enforce breastfeeding initiation, and the group of mothers who did not initiate breastfeeding in the hospital was very small, limiting insights into relationships among associating factors and breastfeeding initiation. Participants were enrolled through a hospital clinic and thus represent only Thai adolescents who sought prenatal care. In addition, all the instruments used were self-reporting and limited by personal perceptions. In addition, the number of days of exclusive breastfeeding was also by self-report at 4 weeks postpartum and could have been easily misreported.
Implications for Practice
Many factors are related to exclusive breastfeeding continuation in adolescent mothers. However, our findings with Thai mothers indicated that the key factors contributing to breastfeeding maintenance were personal attitude and belief, social support, and social influence from their mothers and their husbands/partners. Moreover, fussy infant temperament was a negative predictor. We recommend that interventions be aimed at creating a more positive attitude about breastfeeding during pregnancy and the early postpartum period. Health providers need to encourage adolescent mothers to be successful through interventions that enhance or create positive breastfeeding experiences in the early postpartum period. Adolescent mothers need information about how to best handle common difficulties faced when maintaining exclusive breastfeeding. Based on our high correlations between maternal competence and influencing factors with breastfeeding duration, we recommend that interventions promoting maternal competence begin during pregnancy and be reinforced in the early postpartum period.
Health providers need to encourage adolescent mothers to be successful through interventions that enhance or create positive breastfeeding experiences in the early postpartum period.
Perceiving one’s infant as difficult was a negative factor affecting both breastfeeding duration and maternal competence. Thus, helping adolescent mothers in understanding their infant’s characteristics and learning to work with them is also important to exclusive breastfeeding success.
CONCLUSION
Breastfeeding initiation in adolescent mothers was correlated with personal, social, and cultural factors, whereas breastfeeding maintenance at 4 weeks postpartum was predicted by personal, social, and infant factors. Exclusive breastfeeding continuation was highly correlated with maternal competence. Our findings reinforce the strategies we need to continue to encourage in practice. The interventions that support positive attitudes about breastfeeding during pregnancy and the early postpartum period, engaging both the adolescent mother and her partner/husband in supporting breastfeeding, are directions for further research. Moreover, the maternal competence in adolescent mothers should be explored in greater detail, which might be best accomplished in a qualitative study.
Biographies
SUPANNEE KANHADILOK is a member of the faculty at Boromrajonani College of Nursing, Phraputtabath, Saraburi, Thailand.
NANCY L. MCCAIN is a professor at School of Nursing, Virginia Commonwealth University.
JACQUELINE M. MCGRATH is a professor at School of Nursing, University of Connecticut.
NANCY JALLO is an assistant professor at School of Nursing, Virginia Commonwealth University.
SARAH K. PRICE is an associate professor at school of Social Work, Virginia Commonwealth University.
CHANTIRA CHIARANAI is an assistant professor at Institute of Nursing Suranaree University of Technology, Thailand.
REFERENCES
- Bartok C. J. (2011). Babies fed breastmilk by breast versus by bottle: A pilot study evaluating early growth patterns. Breastfeeding Medicine, 6, 117–124. [DOI] [PubMed] [Google Scholar]
- Beaton D., Bombardier C., Guillemin F., & Ferraz M. B. (2007). Recommendations for the cross-cultural adaptation of health status measures. Toronto, Canada: Institute for Work and Health; Retrieved from http://www.dash.iwh.on.ca/sites/dash/files/downloads/cross_cultural_adaptation_2007.pdf [Google Scholar]
- Borkowski J. G., Bisconti T., Weed K., Willard C., Keogh D. A., & Whitman T. L. (2002). The adolescent as parent: Influences on children’s intellectual, academic, and socioemotional development In Borkowski J. G., Ramey S. L., Bristol-Power M. (Eds.), Parenting and the child’s world: Influences on academic, intellectual, and social-emotional development (pp. 161–186). Mahwah, NJ: Lawrence Erlbaum Associates. [Google Scholar]
- Bureau of Health Promotion. (2006). Report of health promotion evaluation in the 9th National Economic and Social Development Plan. Nonthaburi, Thailand: Department of Health, Ministry of Public Health. [Google Scholar]
- Centers for Disease Control and Prevention. (2015). Breastfeeding among U.S. children were born 2002–2012, CDC National Immunization Survey. Retrieved from http://www.cdc.gov/BREASTFEEDING/data/NIS_data/index.htm
- Clarke-Stewart K. A., Fitzpatrick M. J., Allhusen V. D., & Goldberg W. A. (2000). Measuring difficult temperament the easy way. Journal of Developmental and Behavioral Pediatrics, 21, 207–220. [PubMed] [Google Scholar]
- Crnic K. A., Gaze C., & Hoffman C. (2005). Cumulative parenting stress across the preschool period: Relations to maternal parenting and child behaviour at age 5. Infant and Child Development, 14, 117–132. [Google Scholar]
- de la Mora A., Russell D. W., Dungy C. I., Losch M., & Dusdieker L. (1999). The Iowa Infant Feeding Attitude Scale: Analysis of reliability and validity. Journal of Applied Social Psychology, 2, 2362–2380. [Google Scholar]
- de Lauzon-Guillain B., Wijndaele K., Clark M., Acerini L. C., Hughes A. I., Dunger D. B., . . . Ong K. K. (2012). Breastfeeding and infant temperament at age three months. PloS One, 7, e29326. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Dewey K. G. (2003). Is breastfeeding protective against child obesity? Journal of Human Lactation, 19, 9–18. [DOI] [PubMed] [Google Scholar]
- Dykes F., Moran V. H., Burt S., & Edwards J. (2003). Adolescent mothers and breastfeeding: Experiences and support needs—An exploratory study. Journal of Human Lactation, 19, 391–401. [DOI] [PubMed] [Google Scholar]
- Gartner L. M., Morton J., Lawrence R. A., Naylor A. J., O’Hare D., Schanler R. J., & Eidelman A. I. (2005). Breastfeeding and the use of human milk. Pediatrics, 115, 496–506. [DOI] [PubMed] [Google Scholar]
- Glass T. L., Tucker K., Stewart R., Baker T. E., & Kauffman R. P. (2010). Infant feeding and contraceptive practices among adolescents with a high teen pregnancy rate: A 3-year retrospective study. Journal of Women’s Health, 19, 1659–1663. [DOI] [PubMed] [Google Scholar]
- Hanna B. (2001). Negotiating motherhood: The struggles of teenage mothers. Journal of Advanced Nursing, 34, 456–464. [DOI] [PubMed] [Google Scholar]
- Hannon P. R., Willis S. K., Bishop-Townsend V., Martinez I. M., & Scrimshaw S. C. (2000). African-American and Latina adolescent mothers’ infant feeding decisions and breastfeeding practices: A qualitative study. Journal of Adolescent Health, 26, 399–407. [DOI] [PubMed] [Google Scholar]
- Hughes R. B. (1984). The development of an instrument to measure perceived emotional, instrumental, and informational support in breastfeeding mothers. Issues in Comprehensive Pediatric Nursing, 7, 357–362. [DOI] [PubMed] [Google Scholar]
- Johnston C., & Mash E. J. (1989). A measure of parenting satisfaction and efficacy. Journal of Clinical Child Psychology, 18, 167–175. [Google Scholar]
- Kerruish N. J., Settle K., Campbell-Stokes P., & Taylor B. J. (2005). Vulnerable Baby Scale: Development and piloting of a questionnaire to measure maternal perceptions of their baby’s vulnerability. Journal of Paediatrics and Child Health, 41, 419–423. [DOI] [PubMed] [Google Scholar]
- Kong S. K., & Lee D. T. (2004). Factors influencing decision to breastfeed. Journal of Advanced Nursing, 46, 367–379. [DOI] [PubMed] [Google Scholar]
- Laisiriruangrai P., Wiriyasirivaj B., Phaloprakarn C., & Manusirivithaya S. (2008). Prevalence of exclusive breastfeeding at 3, 4 and 6 months in Bangkok Metropolitan Administration Medical College and Vajira Hospital. Journal of the Medical Association of Thailand, 91, 962–967. [PubMed] [Google Scholar]
- Misra R., & James D. C. S. (2000). Breast-feeding practices among adolescents and adult mothers in the Missouri WIC population. Journal of the American Dietetic Association, 100, 1071–1073. [DOI] [PubMed] [Google Scholar]
- Moore M., & Brooks-Gunn J. (2002). Adolescent parenthood In Bornstein M. (Ed.), Handbook of parenting (Vol. 3, pp. 173–214). Mahwah, NJ: Lawrence Erlbaum Associates. [Google Scholar]
- Mossman M., Heaman M., Dennis C. L., & Morris M. (2008). The influence of adolescent mothers’ breastfeeding confidence and attitudes on breastfeeding initiation and duration. Journal of Human Lactation, 24, 268–277. [DOI] [PubMed] [Google Scholar]
- Nelson A., & Sethi S. (2005). The breastfeeding experiences of Canadian teenage mothers. Journal of Obstetric, Gynecologic, and Neonatal Nursing, 34, 615–624. [DOI] [PubMed] [Google Scholar]
- Park Y. K., Meier E. R., & Song W. O. (2003). Characteristics of teenage mothers and predictors of breastfeeding initiation in the Michigan WIC Program in 1995. Women, infants, and children. Journal of Human Lactation, 19, 50–56. [DOI] [PubMed] [Google Scholar]
- Ratananugool N. (2001). Factors influencing breastfeeding behavior among Thai adolescent mothers: A nursing predictive model (Doctoral dissertation). Retrieved from ProQuest Dissertations and Theses database. (UMI No. 3049252)
- Shapiro-Mendoza C. K., Selwyn B. J., Smith D. P., & Sanderson M. (2007). The impact of pregnancy intention on breastfeeding duration in Bolivia and Paraguay. Study in Family Planning, 38, 198–205. [DOI] [PubMed] [Google Scholar]
- Spear H. J. (2006). Breastfeeding behaviors and experiences of adolescent mothers. The American Journal of Maternal Child Nursing, 31, 106–113. [DOI] [PubMed] [Google Scholar]
- Tucker C. M., Wilson E. K., & Samandari G. (2011). Infant feeding experiences among teen mothers in North Carolina: Findings from a mixed-methods study. International Breastfeeding Journal, 6, 14. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Wambach K. A., & Koehn M. (2004). Experiences of infant-feeding decision-making among urban economically disadvantaged pregnant adolescents. Journal of Advanced Nursing, 48, 361–370. [DOI] [PubMed] [Google Scholar]
- Wasser H., Bentley M., Borja J., Goldman B. D., Thompson A., . . . Adair L. (2011). Infants perceived as “fussy” are more likely to receive complementary foods before 4 months. Pediatrics, 127, 229–237. [DOI] [PMC free article] [PubMed] [Google Scholar]
- World Health Organization. (2008). Indicators for assessing infant and young child feeding practices: Conclusions of a consensus meeting held 6–8 November 2007 in Washington, DC, USA. Geneva, Switzerland: Author; Retrieved from http://whqlibdoc.who.int/publications/2008/9789241596664_eng.pdf [Google Scholar]