Abstract
Background. The magnitude of the 2013–2016 Ebola virus disease outbreak in West Africa was unprecedented, with >28 500 reported cases and >11 000 deaths. Understanding the key elements of Ebola virus transmission is necessary to implement adequate infection prevention and control measures to protect healthcare workers and halt transmission in the community.
Methods. We performed an extensive PubMed literature review encompassing the period from discovery of Ebola virus, in 1976, until 1 June 2016 to evaluate the evidence on modes of Ebola virus shedding and transmission.
Findings. Ebola virus has been isolated by cell culture from blood, saliva, urine, aqueous humor, semen, and breast milk from infected or convalescent patients. Ebola virus RNA has been noted in the following body fluids days or months after onset of illness: saliva (22 days), conjunctiva/tears (28 days), stool (29 days), vaginal fluid (33 days), sweat (44 days), urine (64 days), amniotic fluid (38 days), aqueous humor (101 days), cerebrospinal fluid (9 months), breast milk (16 months [preliminary data]), and semen (18 months). Nevertheless, the only documented cases of secondary transmission from recovered patients have been through sexual transmission. We did not find strong evidence supporting respiratory or fomite-associated transmission.
Keywords: Ebola virus, shedding, transmission
Ebola virus is a 19-kb, single-strand, negative-sense RNA virus that belongs to the family Filoviridae, order Mononegavirales. Among the 5 species of the genus, 4 are known to cause Ebola virus disease (EVD) in humans: Zaire ebolavirus (EBOV), Sudan ebolavirus (SUDV), Bundibugyo ebolavirus, and Taï Forest ebolavirus. Reston ebolavirus seems to cause only asymptomatic infection in humans [1]. The main reservoir for this virus genus is considered to be bats [2]. Viral entry into humans is thought to occur at mucosal surfaces or through breached skin [3]. Ebola viruses primarily target dendritic cells, monocytes, and macrophages before reaching the lymph nodes and eventually the general circulation through the lymphatics, after which they infect and replicate in a wide range cells and organs, especially the liver, spleen, and adrenal glands [3]. The combined viral cytopathic effect and the host response result in a strong and potentially deleterious inflammatory reaction that can lead to severe coagulopathy, shock, and fatal end organ damage [4]. Outside the body, Ebola virus has been shown to survive up to 3 days on a Tyvek coverall in conditions reproducing a tropical climate [5], up to 8 days in wastewater [6], and up to 46 days in blood-based liquid media at room temperature [7].
As of March 2016, >28 500 symptomatic cases and >11 000 deaths attributed to EVD have been reported during the 2013–2016 outbreak in West Africa [8]. Nearly 900 healthcare workers (HCWs) working on the frontlines of the outbreak has contracted EVD, with 513 deaths [8, 9]. Twenty-seven patients with EVD, mostly working for humanitarian aid agencies, have been medically evacuated and treated in the United States or Europe [10] since the beginning of the 2013–2016 outbreak, leading to 3 cases of nosocomial transmission [11, 12]. Accumulating evidence from the massive outbreak in West Africa demonstrate EBOV persistence in various immune-privileged sites after recovery from acute disease, with the potential for reactivation of replication, virus shedding, and secondary transmission [13, 14], especially sexual transmission from persistent virus in male survivors [15, 16]. A thorough understanding of the dynamics of Ebola virus persistence and shedding in the diverse body compartments and fluids is essential to estimating and mitigating risk of transmission from EVD survivors. We review here the present evidence on the subject and discuss the potential risk of transmission from persistent Ebola virus infection.
METHODS
We performed a comprehensive PubMed literature review encompassing the period from discovery of Ebola virus, in 1976, until 1 June 2016, using the search terms “Ebolavirus”, “Ebola virus disease”, “transmission”, and “shedding” in various combinations without any language restrictions. Articles were included if considered relevant to the review.
SHEDDING
The Need for Standardization
In patients with acute EVD, there is evidence that the virus is shed in a broad range of body compartments and fluids, including blood, stool, urine, sweat, vaginal secretions, amniotic fluid, saliva, tears, aqueous humor, cerebrospinal fluid (CSF), breast milk, and semen [3, 17–20]. The preponderance of the data come from RNA detection assays, primarily real-time reverse transcription–polymerase chain reaction (rRT-PCR), which appears to presently be the most sensitive diagnostic tool available. Data are derived from testing of convenience samples, with the largest data collection on RNA shedding in humans coming from the 2013–2016 epidemic in West Africa. Most recent investigations have not included confirmatory cell culture to demonstrate the presence of infectious virus, making interpretation of infectivity difficult, since nucleic acid detection may simply reflect the presence of remnant viral RNA or even defective infectious particles [21]. Furthermore, no standardized assay or international units exist to allow reliable comparison of viral loads between rRT-PCR assays. Although the Makona variant of EBOV that caused the outbreak in West Africa is genetically similar to EBOV variants from Central Africa, functional or “phenotypic” data are lacking to assess whether different variants or species may have different dynamics of virus persistence and shedding. Factors that may influence results from cell culture include the size of the inoculum, the type of specimen, and the cell line used.
Blood
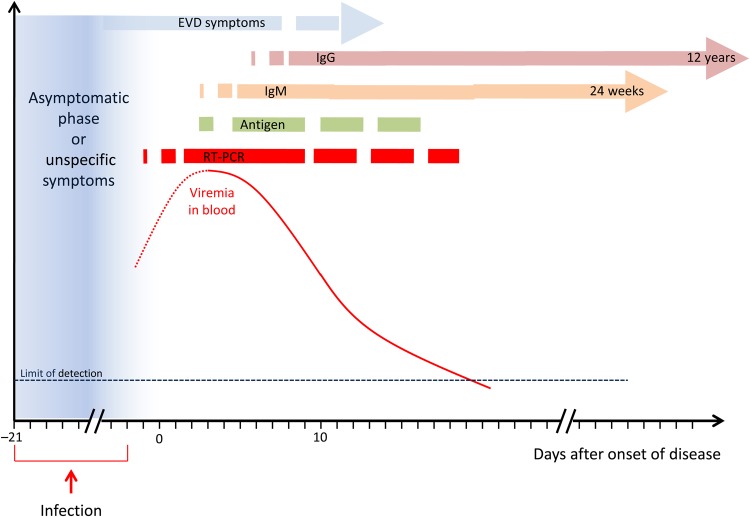
Soon after initial dissemination to and infection of the organs, explosive replication of Ebola virus in the liver, spleen, and adrenal glands results in an exponential rise in viral titers in blood [3] (Figure 1). Blood is among the most infectious body fluids because of its high viral load. Viral RNA has been detected as early as 3 days before appearance of fever, in a pregnant woman [22], and viral load in blood has been described as high as 107 RNA copies/mL as early as day 2 of disease [23–25]. The peak viremia level is higher and occurs an average of 2 days later in patients who die, compared with the level in survivors, with high viral load maintained until death [25, 26]. In patients who survive, the viral load in plasma usually starts to decrease 5 days after symptoms onset [25].
Figure 1.
Evolution of viral load in blood and appearance of immune response during the course of Ebola virus disease (EVD). Abbreviations: IgG, immunoglobulin G; IgM, immunoglobulin M; RT-PCR, reverse transcription–polymerase chain reaction.
Body Fluids
Evidence from the West African and prior outbreaks suggests that virus persists in various body compartments and fluids in addition to blood (Table 1). The viral RNA load in stool has been found to peak at high levels during the course of the disease [23, 27]. Studies in nonhuman primates (NHPs) suggest that the clinical course following infection with the Makona variant differs from that seen with previous isolated EBOV variants, with Makona being associated with more-frequent diarrhea and delayed disease progression [28, 29]. If extrapolatable to humans, these features may lead to increased transmission opportunities through the prolonged shedding of infectious virus, perhaps explaining the high incidence of EVD in West Africa. While viral RNA has been found in stool after clearance of viremia, attempts in prior outbreaks to recover virus from stool in cell culture have failed to date, although this may also simply reflect the usual technical challenges of bacterial and fungal overgrowth when attempting to isolate virus from stool [17, 18].
Table 1.
Maximum Interval Between Onset of Ebola Virus Disease (EVD) and Last Detection of Ebolavirus RNA by Reverse Transcription–Polymerase Chain Reaction (RT-PCR) and Last Detection of Ebolavirus by Culture, by Human Body Fluid Specimen
| Specimen(s) | Last Positive RT-PCR Result, d | Last Positive Culture Result, d |
|---|---|---|
| Saliva | 22 | 4 |
| Tears/conjunctival swab | 28 | …a |
| Rectal swab/stool | 29 | …b |
| Vaginal swab | 33 | …c |
| Amniotic fluid/placenta | 38 | NA |
| Skin swab/sweat | 44 | NA |
| Urine | 64 | 26 |
| Aqueous humor | 101 | 101 |
| Cerebrospinal fluid | 283 | NA |
| Breast milk | 486d | 15 |
| Semen | 488 | 82 |
Abbreviation: NA, no report available in the literature.
a No data on final positive results are available. Culture results were negative 6 days after EVD onset.
b No data on final positive results are available. Culture results were negative 4–12 days after EVD onset.
c No data on final positive results are available. Culture results were negative 22, 25, and 33 days after EVD onset.
d The time was specified as 16 months in the literature but is converted here to days for parallelism with units specified elsewhere in the column. This sample was Ebolavirus RNA positive at low levels, making interpretation difficult. Further testing is necessary to confirm these results.
In a patient requiring mechanical ventilation, a high number of viral RNA copies were found in bronchoalveolar lavage 20 days after onset of disease [30], suggesting viral replication in the lungs. It was not specified whether the virus could be isolated in cell culture.
Ebola virus has been cultured from saliva, urine, aqueous humor of the eye, semen, and breast milk from infected or convalescent patients [17, 18, 31, 32]. While EBOV RNA and viable virus are typically detected in saliva early in the course of disease, viral shedding does not seem to persist after resolution of symptoms [18, 23, 33]. From urine specimens, EBOV was isolated up to 9 days after clearance of viral RNA from blood in a male patient with severe disease [31], and RNA was recovered up to 36 days (64 days after disease onset) after blood tested negative by RT-PCR from a young woman who presented with EVD complicated by severe encephalopathy [34]. In a severely ill patient who needed renal replacement therapy, EBOV could not be detected in effluent waste [35]. In breast milk from a lactating woman, infectious Ebola virus was recovered by cell culture both during the acute and convalescent phases of disease up to day 15 after onset of symptoms [18]. Detection of viral RNA up to 16 months after disease onset has been described, although at low levels, making interpretation difficult [20]. EBOV has been isolated in aqueous humor from a patient presenting with uveitis up to 14 weeks after onset of disease, 9 weeks after clearance of viremia [32]. The maximal reported duration of virus shedding detected in a conjunctival swab in humans is 10 days after clearance of viremia [33].
Virus has been detected by RT-PCR in semen up to 16 months (488 days) after symptom onset [36] and isolated in cell culture up to 82 days after symptom onset [17]. EBOV RNA was detected in semen from half of participants at least once during follow-up in a pilot study involving 93 EVD survivors in Sierra Leone, with 26% of survivors still shedding viral RNA 7–9 months after acute disease [13]. The viral load in semen decreased over time in patients who underwent serial testing [13, 37, 38]. Whether virus can be cultured that long after remission remains to be determined. Sexual transmission during the ongoing EVD outbreak is now quite well documented [15, 16] and has likely been the cause of sporadic EVD resurgence in West Africa in late 2015 and early 2016 [39].
Viral RNA has been detected in amniotic fluid 34 days after clearance of viremia [40], but no attempts at cell culture of this sample have been published to date. A pregnant survivor delivered an EVD-positive stillborn baby 32 days after she tested negative for EBOV [40]. EBOV RNA has been detected in a skin swab up to 23 days after clearance of viremia [31], but results of cell culture performed at the same time were negative. The maximal reported duration of EBOV RNA detection in an axillary swab was 44 days after onset of symptoms, in a patient who experienced a prolonged course of disease [34]. Whether this reflects the presence of infectious virus, remnant RNA, or external contamination from other body fluids remains unknown.
EBOV RNA was detected in CSF 7 days after onset of symptoms in a patient who presented with acute encephalopathy [19] and up to day 41 days (13 days after blood tested negative) in a patient who experienced a biphasic course of disease characterized by the development of encephalitis after a period of improvement [34]. Recently, viral RNA and infectious virus were detected in CSF from an EVD survivor with recrudescent meningoencephalitis 9 months after resolution of disease [41].
The infectivity of the virus identified in the different body fluids during acute EVD requires further evaluation. For example, we found only 1 attempt in the literature—which failed—to recover virus from a sample of human vomitus [18]. Ebola virus is known to be inactivated by acidic pH [42], bringing into question whether the virus can survive in the gastric environment. Ebola virus may well reach the intestine by means of viremia. Its passage into the intestinal lumen may be facilitated by increased capillary permeability in the mucosa, as suggested by the presence of viral antigens in mononuclear cells within the lamina propria of the enteric mucosa in autopsies of deceased patients with EVD [43]. While it is very plausible that large quantities of viable Ebola virus are present in stool, Ebola virus stool culture data are missing. Moreover, there is only one mention of RT-PCR of intra-articular fluid, results of which were negative [34].
TRANSMISSION
Fruit bats of the Pteropodidae family are considered as the most likely natural reservoir of Ebola virus [44], and humans can become infected by close contact or by manipulating contaminated wildlife. Ebola virus is then transmitted from human to human via direct contact with body fluids of an infected person or, potentially, from contaminated surfaces and materials.
In animal models, Ebola virus transmission has been demonstrated through direct virus inoculation in mucosa (via the oral or conjunctival route); subcutaneous, intraperitoneal, or intramuscular injection; and via the respiratory tract, through respiratory droplets and aerosols. Small viral inocula of <1 plaque-forming unit can be infectious [45]. Inoculation of the conjunctiva or oropharyngeal mucosa, as well as transcutaneous infection via tiny skin breaches, are considered the main routes of natural transmission in humans.
Contact With Body Fluids and Cadavers
The major risk for human-to-human transmission is direct contact with infected body fluids from symptomatic patients with EVD [46–53]. The mean household secondary attack rate for individuals with direct contact during previous outbreaks has been calculated to be 22.9% (95% confidence interval [CI], 11.6%–34.2%) [54]. Patients often have severe diarrhea and vomiting, sometimes with bleeding in the late stages, increasing the risk of contact with infectious body fluids. Viral load increases with disease severity, and the highest levels of virus are found around the time of death [24–26, 55]. Cadavers are thus a potent source of infectious virus at high concentration and must be handled with the same precautions as body fluids. In carcasses of NHPs experimentally infected by EBOV and stored in conditions reproducing tropical climates, viral RNA was detectable for up to 10 weeks after death in oral, nasal, urogenital, rectal, conjunctival, skin, and blood swab and various tissue samples; infectious virus could be isolated up to 9 days after death in blood specimens, 7 days in oral swabs, and 2 to 4 days for other body fluids and tissue samples [27]. Touching dead bodies doubled the risk of infection (risk ratio, 2.1; 95% CI, 1.1–4.2) in household members who had direct physical contact with a patient with EVD during illness [47].
Only a few EVD cases after needle sticks have been reported [46, 53, 56–65]. However, parenteral inoculation is clearly established as a potent means of transmission and was associated with a shorter incubation period (6.3 days vs 9.5 days) and a higher overall mortality level (100% vs 88%) during the initial outbreak of EVD, in Yambuku during 1976 [66]. Recently, some HCWs with sharps exposures have been treated with postexposure prophylactic administration of rVSV-ZEBOV vaccine [61, 62, 65], monoclonal antibodies and/or favipiravir [64], and TKM-100802 [65]; none of the reported cases developed EVD, and no sign of EBOV viremia was detectable, but it is not possible to know whether infection actually occurred.
HCWs are particularly vulnerable to nosocomial infection, with associated high mortality rates, probably reflecting high viral inocula. This is dramatically illustrated by the death of 10% of Sierra Leone HCWs during the early phase of the West Africa outbreak [53, 67].
EVD as a Sexually Transmitted Disease
Asymptomatic sexual transmission was suspected in a spouse of a convalescent patient with EVD after the 1995 Kikwit EBOV outbreak in the Democratic Republic of the Congo [68]. The most convincing evidence of EVD sexual transmission comes from the West Africa EBOV epidemic, in which a woman became infected 30 days after the last reported case in Liberia. Her only identified risk factor was sexual contact with a survivor who was shedding EBOV RNA in his semen, with a sequence match with the virus obtained from the blood of the infected woman [15, 16]. Moreover, none of the mutations found in the seminal isolate sequence were observed in 22 isolates from systematic analyses conducted since January 2015 in Liberia. As a result, new recommendations have been formulated concerning sexual behaviors of EVD survivors, including avoidance of contact with semen for at least 12 months or until the semen has twice tested negative for EBOV RNA [20]. However, sexual transmissions from survivors seem rare and only anecdotally reported, despite the fact that up to 26% of the male survivors may still shed EBOV RNA in their semen 7–9 months after resolution of acute illness [13]. EBOV does not survive in acidic environments [42], and the acidic pH of normal vaginal mucosa may act as a natural barrier. The minimal inoculum, and whether the different phases of the menstrual cycle or concomitant sexually transmitted diseases can facilitate sexual transmission remain to be determined.
Although viral RNA has been detected in the convalescent phase in vaginal fluid of a survivor [18], no female-to-male sexual transmission has been documented to date.
Mother-to-Child Transmission
We found no reports of any attempt to culture virus from amniotic fluid. However, the detection of high levels of viral RNA in amniotic fluid from pregnant women with EVD and on the placenta and fetus just after delivery [69–71], combined with extremely high in utero fetal and neonatal mortality rates, strongly suggest Ebola virus vertical transmission.
Transmission through breastfeeding, even if highly suspected, has never been formally confirmed [39, 72]. By use of next-generation sequencing, a case of transmission through breastfeeding from an asymptomatic mother, whose plasma tested negative and breast milk tested positive, to her 13-month-old baby has been described [39]. However, other modes of contamination could not be excluded. In a small cohort in Sierra Leone, the risk of infection in children was higher if their mother died of EVD, but it did not seem to be increased by breastfeeding [73]. As a precaution and because of confirmed isolation of virus from breast milk [18], current recommendations are for mothers with EVD to refrain from breastfeeding [74]. EVD survivors who are lactating should stop breastfeeding only if their breast milk has been tested positive until 2 negative results are obtained 48 hours apart, according to World Health Organization recommendations [20].
Droplet and Airborne Transmission
There has been much discussion about the potential for airborne transmission of Ebola virus because of the implications for infection control measures [75, 76]. Animal experiments, including those involving NHPs, have raised concerns about the possibility of Ebola virus transmission through aerosol or droplets, resulting in the development of interstitial pneumonia [77–85]. EBOV inclusions have been demonstrated within macrophages in lungs and free particles within alveolar spaces, further supporting the possibility of this route of transmission [43]. A high viral load has been detected in bronchoalveolar lavage of a patient presenting with interstitial pneumonia during the acute phase of the disease [30]. Experimentally, the EBOV half-life in aerosol has been calculated to be 15 minutes, with a decay rate of 3.06% per minute. In other words, at 50%–55% relative humidity and at a temperature of 19°C–24°C, it takes 104 minutes for 99% of aerosolized EBOV to disappear [7]. EBOV RNA could not be detected in open tubes placed inside isolation wards for up to 24 hours, arguing against airborne dissemination [18] (Kaiser, unpublished data). On the other hand, EBOV RNA has been found on the outer surface of N95 masks in Western Africa that were not visibly soiled [75]; whether this reflects infectious virus and aerosol or droplets versus contamination from hands touching the mask remains unclear. In prior outbreaks, infection prevention and control measures using surgical masks that protect against direct contamination of the oral mucosa but not aerosol transmission appeared sufficient to prevent nosocomial transmission [48, 66, 86, 87]. While theoretically possible, epidemiological data do not support airborne transmission as a mode of human-to-human EVD transmission [47, 50, 51]. However, aerosol-generating medical procedures, such as endotracheal intubation, may pose an enhanced risk, necessitating appropriate respiratory protection against aerosol spread.
Transmission via Fomites
Transmission via fomites is plausible, given the evidence of viable virus on soiled surfaces and liquids for several days to several weeks [5, 7, 18, 88–91]. Three retrospective studies assessed the risk of contracting EVD among household contacts not having direct contact with a primary case [47, 50, 51]; only 1 patient reported no direct contact and presumably became ill after sleeping with a blanket used by an infected patient [51]. In medical settings, EBOV RNA has been detected on many environmental samples collected before cleaning in an Ebola treatment center in Sierra Leone [75]. In contrast, 26 samples collected inside or outside of the isolation wards after appropriate disinfection during a SUDV outbreak in Gulu in 2000 [18], 16 samples in Madrid, Spain [33], and 14 samples collected in Geneva, Switzerland (Kaiser, unpublished data), that were associated with the West African outbreak all tested negative for Ebola virus. The preponderance of data do not suggest that fomites present a major public health problem in dedicated Ebola treatment centers. However, data are still lacking regarding this mode of contamination in overcrowded environments and households lacking sanitation, in which various routes of transmission may occur simultaneously. Indeed, Bower et al showed that nearly half of the household members of EVD survivors contracted the disease, with the risk of infection varying by age and level of exposure, dropping from 83% for people touching a dead corpse to 8% for people with only minimal contact with the infected initial case [92].
Role of Asymptomatic or Pauci-symptomatic Infections
Asymptomatic or mild infections with Ebola virus have been reported on the basis of noted immune responses (IgM/IgG seropositivity) and RNA detection in contacts of infected patients [44, 66, 68]. Preliminary results of the PREVAIL III study being conducted in Liberia revealed that 49% of 97 close contacts of survivors were IgG seropositive [36]. It is commonly accepted that, given the lack of symptoms, these people seem unlikely to contribute significantly to human-to-human transmission [44, 47]. One report relates a case of transmission of SUDV from an asymptomatic person 2 days before development of symptoms [46]. The case describe above of breastfeeding transmission from an asymptomatic mother raises new concerns about possibility of transmission from exposure to select body fluids of EVD survivors from which virus clearance is delayed [39].
Other Risks of Transmission From Survivors
Virus shedding in the anterior chamber of the eye has been shown to persist up to 14 weeks after onset of symptoms in a survivor presenting with uveitis [32]. The presence of 5 mutations in the viral sequence derived from the anterior chamber as compared to the sequences obtained from the blood at the time of viremia indicates viral replication and evolution through multiple cycles and, thus, persistence of potentially infectious virus. A concomitant conjunctival swab remained negative for both EBOV RNA detection and virus isolation by cell culture, suggesting that tears of survivors do not pose a transmission risk. The infectious risk related to eye surgery in EVD survivors remains to be determined.
Howlett et al reported having discharged a patient who was still shedding viral RNA at low level in urine [34]. No secondary transmission occurred within her contacts. Of note, her caregivers were aware of the test result and protected themselves while handling her body fluids. Whether a positive RT-PCR result in urine collected >1 month after a blood specimen tests negative represents infectious virus or remnant viral RNA is still unknown. Transmission through urinary contact of survivors, however, seems unlikely and has not been reported, especially if the survivor is ambulant and continent and can therefore manage their own body fluids and secretions.
Recently, recrudescent EVD has been described [41], with EBOV detected in the CSF of a survivor with EBOV meningoencephalitis 9 months after onset of disease. This report raises new concerns about necessary infection control measures while caring for survivors experiencing unexpected symptoms. However, noninvasive contact with Ebola survivors without fever after remission seems to pose a negligible risk of infection for HCWs; indeed, all specimens other than semen (including blood, saliva, tears, sweat and skin swabs, urine, vaginal secretions, and rectal swabs) tested negative in 2 follow-up studies of survivors, conducted in 1995 in the Democratic Republic of the Congo and in 2015 in Sierra Leone [68, 93].
Implications on Discharge Policy
Incomplete knowledge concerning virus shedding patterns in different body fluids also influences patient discharge strategies. During the ongoing 2013–2016 EVD outbreak, a negative RT-PCR result in blood was widely required to discharge a convalescent patient [94]. Clinically recovered patients who are ambulatory and continent and who can manage their own body fluids and secretions probably present a very low risk of virus transmission, irrespective of the RT-PCR results. In historical outbreaks, RT-PCR was not widely available, and yet transmission from discharged patients has not been reported to be an important source of disease.
CONCLUSION
Contact with body fluids from patients with EVD and cadavers remains the major risk for transmission of Ebola virus, and appropriate infection prevention and control measures are an absolute necessity to protect HCWs in an EVD outbreak setting. However, the relative infectivity of the various body fluids of patients with EVD remains to be established. While stools seem to represent a major source of infection during acute disease, the respective roles in Ebola virus transmission of saliva, vomitus, and urine are not clear. Sexual transmission has been well documented, but the risk seems to remain low. The necessary infection prevention and control measures while caring for survivors continue to be debated, especially regarding ophthalmologic or urological procedures. Whether and how EBOV can persist in protected body compartments other than semen, such as the eye, CSF, or intra-articular fluid, and whether it can lead to virus transmission remains unknown. Systematic data collection and thorough laboratory investigations are still missing to fully understand Ebola virus shedding and transmission.
Notes
Acknowledgments. P. V. and W. A. F. conducted the literature research and wrote the first draft. All authors critically reviewed and revised the manuscript. P. V. had final responsibility for the decision to submit for publication.
Disclaimer. The funders had no role in the preparation of the manuscript.
Financial support. This work was supported by Geneva University Hospitals, the Swiss Agency for Development and Cooperation, and the Tulane University.
Potential conflicts of interest. All authors: No reported conflicts. All authors have submitted the ICMJE Form for Disclosure of Potential Conflicts of Interest. Conflicts that the editors consider relevant to the content of the manuscript have been disclosed.
References
- 1. Miranda ME, Miranda NL. Reston ebolavirus in humans and animals in the Philippines: a review. J Infect Dis 2011; 204(suppl 3):S757–60. [DOI] [PubMed] [Google Scholar]
- 2. Leroy EM, Kumulungui B, Pourrut X et al. Fruit bats as reservoirs of Ebola virus. Nature 2005; 438:575–6. [DOI] [PubMed] [Google Scholar]
- 3. Feldmann H, Geisbert TW. Ebola haemorrhagic fever. Lancet 2011; 377:849–62. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4. Fletcher TE, Fowler RA, Beeching NJ. Understanding organ dysfunction in Ebola virus disease. Intensive Care Med 2014; 40:1936–9. [DOI] [PubMed] [Google Scholar]
- 5. Fischer R, Judson S, Miazgowicz K, Bushmaker T, Prescott J, Munster VJ. Ebola virus stability on surfaces and in fluids in simulated outbreak environments. Emerg Infect Dis 2015; 21:1243–6. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6. Bibby K, Fischer RJ, Casson LW, Stachler E, Haas CN, Munster VJ. Persistence of Ebola virus in sterilized wastewater. Environ Sci Technol Lett 2015; 2:245–9. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7. Piercy TJ, Smither SJ, Steward JA, Eastaugh L, Lever MS. The survival of filoviruses in liquids, on solid substrates and in a dynamic aerosol. J Appl Microbiol 2010; 109:1531–9. [DOI] [PubMed] [Google Scholar]
- 8. World Health Organization (WHO). Ebola response roadmap situation report. Geneva: WHO, 2016. http://apps.who.int/ebola/current-situation/ebola-situation-report-30-march-2016 Accessed 3 April 2016. [Google Scholar]
- 9. Ebola protection of health workers on the front line. Lancet 2014; 384:470. [DOI] [PubMed] [Google Scholar]
- 10. Uyeki TM, Mehta AK, Davey RT Jr et al. Clinical management of Ebola virus disease in the united states and europe. N Engl J Med 2016; 374:636–46. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11. Parra JM, Salmeron OJ, Velasco M. The first case of Ebola virus disease acquired outside Africa. N Engl J Med 2014; 371:2439–40. [DOI] [PubMed] [Google Scholar]
- 12. Chevalier MS, Chung W, Smith J et al. Ebola virus disease cluster in the United States--Dallas County, Texas, 2014. MMWR Morb Mortal Wkly Rep 2014; 63:1087–8. [PMC free article] [PubMed] [Google Scholar]
- 13. Deen GF, Knust B, Broutet N et al. Ebola RNA persistence in semen of Ebola virus disease survivors - preliminary report. N Engl J Med 2015; 10.1056/NEJMoa1511410. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14. Vetter P, Kaiser L, Schibler M, Ciglenecki I, Bausch DG. Sequelae of Ebola virus disease: the emergency within the emergency. Lancet Infect Dis 2016; 16:e82–91. [DOI] [PubMed] [Google Scholar]
- 15. Christie A, Davies-Wayne GJ, Cordier-Lasalle T et al. Possible sexual transmission of Ebola virus—Liberia, 2015. MMWR Morb Mortal Wkly Rep 2015; 64:479–81. [PMC free article] [PubMed] [Google Scholar]
- 16. Mate SE, Kugelman JR, Nyenswah TG et al. Molecular evidence of sexual transmission of Ebola virus. N Engl J Med 2015; 373:2448–54. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17. Rodriguez LL, De Roo A, Guimard Y et al. Persistence and genetic stability of Ebola virus during the outbreak in Kikwit, Democratic Republic of the Congo, 1995. J Infect Dis 1999; 179(suppl 1):S170–6. [DOI] [PubMed] [Google Scholar]
- 18. Bausch DG, Towner JS, Dowell SF et al. Assessment of the risk of Ebola virus transmission from bodily fluids and fomites. J Infect Dis 2007; 196(suppl 2):S142–7. [DOI] [PubMed] [Google Scholar]
- 19. Sagui E, Janvier F, Baize S et al. Severe Ebola virus infection with encephalopathy: evidence for direct virus involvement. Clin Infect Dis 2015; 61:1627–8. [DOI] [PubMed] [Google Scholar]
- 20. World Health Organization (WHO). Clinical care for survivors of Ebola virus disease. Geneva: WHO, 2016. http://apps.who.int/csr/resources/publications/ebola/guidance-survivors/en/index.html. Accessed 1 June 2016.
- 21. Calain P, Monroe MC, Nichol ST. Ebola virus defective interfering particles and persistent infection. Virology 1999; 262:114–28. [DOI] [PubMed] [Google Scholar]
- 22. Akerlund E, Prescott J, Tampellini L. Shedding of Ebola virus in an asymptomatic pregnant woman. N Engl J Med 2015; 372:2467–9. [DOI] [PubMed] [Google Scholar]
- 23. Schibler M, Vetter P, Cherpillod P et al. Clinical features and viral kinetics in a rapidly cured patient with Ebola virus disease: a case report. Lancet Infect Dis 2015; 15:1034–40. [DOI] [PubMed] [Google Scholar]
- 24. de La Vega MA, Caleo G, Audet J et al. Ebola viral load at diagnosis associates with patient outcome and outbreak evolution. J Clin Invest 2015; 125:4421–8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25. Lanini S, Portella G, Vairo F et al. Blood kinetics of Ebola virus in survivors and nonsurvivors. J Clin Invest 2015; 125:4692–8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26. Towner JS, Rollin PE, Bausch DG et al. Rapid diagnosis of Ebola hemorrhagic fever by reverse transcription-PCR in an outbreak setting and assessment of patient viral load as a predictor of outcome. J Virol 2004; 78:4330–41. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 27. Prescott J, Bushmaker T, Fischer R, Miazgowicz K, Judson S, Munster VJ. Postmortem stability of Ebola virus. Emerg Infect Dis 2015; 21:856–9. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 28. Thi EP, Mire CE, Lee AC et al. Lipid nanoparticle siRNA treatment of Ebola-virus-Makona-infected nonhuman primates. Nature 2015; 521:362–5. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 29. Marzi A, Feldmann F, Hanley PW, Scott DP, Gunther S, Feldmann H. Delayed disease progression in cynomolgus macaques infected with Ebola virus Makona strain. Emerg Infect Dis 2015; 21:1777–83. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 30. Petrosillo N, Nicastri E, Lanini S et al. Ebola virus disease complicated with viral interstitial pneumonia: a case report. BMC Infect Dis 2015; 15:432. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 31. Kreuels B, Wichmann D, Emmerich P et al. A case of severe Ebola virus infection complicated by gram-negative septicemia. N Engl J Med 2014; 371:2394–401. [DOI] [PubMed] [Google Scholar]
- 32. Varkey JB, Shantha JG, Crozier I et al. Persistence of Ebola virus in ocular fluid during convalescence. N Engl J Med 2015; 372:2423–7. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 33. Mora-Rillo M, Arsuaga M, Ramirez-Olivencia G et al. Acute respiratory distress syndrome after convalescent plasma use: treatment of a patient with Ebola virus disease contracted in Madrid, Spain. Lancet Respir Med 2015; 3:554–62. [DOI] [PubMed] [Google Scholar]
- 34. Howlett P, Brown C, Helderman T et al. Ebola virus disease complicated by late-onset encephalitis and polyarthritis, Sierra Leone. Emerg Infect Dis 2016; 22:150–2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 35. Connor MJ Jr, Kraft C, Mehta AK et al. Successful delivery of RRT in Ebola virus disease. J Am Soc Nephrol 2015; 26:31–7. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 36. Fallah M. A cohort study of survivors of Ebola virus infection in Liberia (PREVAIL III) [abstract 74LB]. In: Program and abstracts of the 2016 Conference on Retroviruses and Opportunistic Infections, Boston, Massachusetts, 22–25 February 2016 http://www.croiconference.org/sessions/cohort-study-survivors-ebola-virus-infection-liberia-prevail-iii. Accessed 2 April 2016. [Google Scholar]
- 37. Sissoko D, Duraffour S, Kolie J et al. Dynamics of Ebola virus clearance in semen in Guinea [abstract 75LB]. In: Program and abstracts of the Conference on Retroviruses and Opportunistic Infections, Boston, Massachusetts, 22–25 February 2016 http://www.croiconference.org/sessions/dynamics-ebola-virus-clearance-semen-guinea. Accessed 2 April 2016. [Google Scholar]
- 38. Sow MS, Etard JF, Baize S et al. New evidence of Long-lasting persistence of Ebola virus genetic material in semen of survivors. J Infect Dis 2016; 10.1093/infdis/jiw078. [DOI] [PubMed] [Google Scholar]
- 39. Arias A, Watson SJ, Asogun D et al. Rapid outbreak sequencing of Ebola virus in SL identifies transmission chains linked to sporadic cases. Virus Evol 2016; 10.1093/ve/vew016. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 40. Caluwaerts S, Fautsch T, Lagrou D et al. Dilemmas in managing pregnant women with Ebola: 2 case reports. Clin Infect Dis 2016; 62:903–5. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 41. Jacobs M, Rodger A, Bell DJ et al. Late Ebola virus relapse causing meningoencephalitis: a case report. Lancet 2016; 10.1016/S0140-6736(16)30386-5. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 42. Mitchell SW, McCormick JB. Physicochemical inactivation of Lassa, Ebola, and Marburg viruses and effect on clinical laboratory analyses. J Clin Microbiol 1984; 20:486–9. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 43. Martines RB, Ng DL, Greer PW, Rollin PE, Zaki SR. Tissue and cellular tropism, pathology and pathogenesis of Ebola and Marburg viruses. J Pathol 2015; 235:153–74. [DOI] [PubMed] [Google Scholar]
- 44. Leroy EM, Baize S, Volchkov VE et al. Human asymptomatic Ebola infection and strong inflammatory response. Lancet 2000; 355:2210–5. [DOI] [PubMed] [Google Scholar]
- 45. Alfson KJ, Avena LE, Beadles MW et al. Particle-to-PFU ratio of Ebola virus influences disease course and survival in cynomolgus macaques. J Virol 2015; 89:6773–81. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 46. WHO. Ebola haemorrhagic fever in Zaire, 1976. Report of an International Commission. Bull World Health Organ 1978; 56:271–93. [PMC free article] [PubMed] [Google Scholar]
- 47. Dowell SF, Mukunu R, Ksiazek TG, Khan AS, Rollin PE, Peters CJ. Transmission of Ebola hemorrhagic fever: a study of risk factors in family members, Kikwit, Democratic Republic of the Congo, 1995. Commission de Lutte contre les Epidemies a Kikwit. J Infect Dis 1999; 179(suppl 1):S87–91. [DOI] [PubMed] [Google Scholar]
- 48. Khan AS, Tshioko FK, Heymann DL et al. The reemergence of Ebola hemorrhagic fever, Democratic Republic of the Congo, 1995. Commission de Lutte contre les Epidemies a Kikwit. J Infect Dis 1999; 179(suppl 1):S76–86. [DOI] [PubMed] [Google Scholar]
- 49. Richards GA, Murphy S, Jobson R et al. Unexpected Ebola virus in a tertiary setting: clinical and epidemiologic aspects. Crit Care Med 2000; 28:240–4. [DOI] [PubMed] [Google Scholar]
- 50. Baron RC, McCormick JB, Zubeir OA. Ebola virus disease in southern Sudan: hospital dissemination and intrafamilial spread. Bull World Health Organ 1983; 61:997–1003. [PMC free article] [PubMed] [Google Scholar]
- 51. Francesconi P, Yoti Z, Declich S et al. Ebola hemorrhagic fever transmission and risk factors of contacts, Uganda. Emerg Infect Dis 2003; 9:1430–7. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 52. Dietz PM, Jambai A, Paweska JT, Yoti Z, Ksaizek TG. Epidemiology and risk factors for Ebola virus disease in Sierra Leone-23 May 2014 to 31 January 2015. Clin Infect Dis 2015; 61:1648–54. [DOI] [PubMed] [Google Scholar]
- 53. Olu O, Kargbo B, Kamara S et al. Epidemiology of Ebola virus disease transmission among health care workers in Sierra Leone, May to December 2014: a retrospective descriptive study. BMC Infect Dis 2015; 15:416. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 54. Dean NE, Halloran ME, Yang Y, Longini IM. Transmissibility and pathogenicity of Ebola virus: a systematic review and meta-analysis of household secondary attack rate and asymptomatic infection. Clin Infect Dis 2016; 62:1277–86. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 55. Schieffelin JS, Shaffer JG, Goba A et al. Clinical illness and outcomes in patients with Ebola in Sierra Leone. N Engl J Med 2014; 371:2092–100. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 56. Emond RT, Evans B, Bowen ET, Lloyd G. A case of Ebola virus infection. Br Med J 1977; 2:541–4. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 57. Promed. Ebola, lab accident death—Russia (Siberia). Archive no. 20040522.1377 Promed 22 May 2004. [Google Scholar]
- 58. Pokrovsky V, Allakhverdov A. Climate change: Russia prepares to ratify Kyoto. Science 2004; 304:1225. [DOI] [PubMed] [Google Scholar]
- 59. Kortepeter MG, Martin JW, Rusnak JM et al. Managing potential laboratory exposure to ebola virus by using a patient biocontainment care unit. Emerg Infect Dis 2008; 14:881–7. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 60. Gunther S, Feldmann H, Geisbert TW et al. Management of accidental exposure to Ebola virus in the biosafety level 4 laboratory, Hamburg, Germany. J Infect Dis 2011; 204(suppl 3):S785–90. [DOI] [PubMed] [Google Scholar]
- 61. Lai L, Davey R, Beck A et al. Emergency postexposure vaccination with vesicular stomatitis virus-vectored Ebola vaccine after needlestick. JAMA 2015; 313:1249–55. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 62. Cnops L, Gerard M, Vandenberg O et al. Risk of misinterpretation of Ebola virus PCR results after rVSV ZEBOV-GP vaccination. Clin Infect Dis 2015; 60:1725–6. [DOI] [PubMed] [Google Scholar]
- 63. Guimard Y, Bwaka MA, Colebunders R et al. Organization of patient care during the Ebola hemorrhagic fever epidemic in Kikwit, Democratic Republic of the Congo, 1995. J Infect Dis 1999; 179(suppl 1):S268–73. [DOI] [PubMed] [Google Scholar]
- 64. Jacobs M, Aarons E, Bhagani S et al. Post-exposure prophylaxis against Ebola virus disease with experimental antiviral agents: a case-series of health-care workers. Lancet Infect Dis 2015; 15:1300–4. [DOI] [PubMed] [Google Scholar]
- 65. Wong KK, Davey RT Jr, Hewlett AL et al. Use of postexposure prophylaxis after occupational exposure to Zaire ebolavirus. Clin Infect Dis 2016; 10.1093/cid/ciw256. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 66. WHO. Ebola haemorrhagic fever in Sudan, 1976. Report of a WHO/International Study Team. Bull World Health Organ 1978; 56:247–70. [PMC free article] [PubMed] [Google Scholar]
- 67. Dunn AC, Walker TA, Redd J et al. Nosocomial transmission of Ebola virus disease on pediatric and maternity wards: Bombali and Tonkolili, Sierra Leone, 2014. Am J Infect Control 2016; 44:269–72. [DOI] [PubMed] [Google Scholar]
- 68. Rowe AK, Bertolli J, Khan AS et al. Clinical, virologic, and immunologic follow-up of convalescent Ebola hemorrhagic fever patients and their household contacts, Kikwit, Democratic Republic of the Congo. Commission de Lutte contre les Epidemies a Kikwit. J Infect Dis 1999; 179(suppl 1):S28–35. [DOI] [PubMed] [Google Scholar]
- 69. Baggi FM, Taybi A, Kurth A et al. Management of pregnant women infected with Ebola virus in a treatment centre in Guinea, June 2014. Euro Surveill 2014; 19:pii:20983. [DOI] [PubMed] [Google Scholar]
- 70. Bower H, Grass JE, Veltus E et al. Delivery of an Ebola virus-positive stillborn infant in a rural community health center, sierra leone, january 2015. Am J Trop Med Hyg 2015; 94:417–9. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 71. Oduyebo T, Pineda D, Lamin M, Leung A, Corbett C, Jamieson DJ. A Pregnant patient with ebola virus disease. Obstet Gynecol 2015; 126:1273–5. [DOI] [PubMed] [Google Scholar]
- 72. Moreau M, Spencer C, Gozalbes JG et al. Lactating mothers infected with Ebola virus: EBOV RT-PCR of blood only may be insufficient. Euro Surveill 2015; 20:pii:21017. [DOI] [PubMed] [Google Scholar]
- 73. Bower H, Johnson S, Bangura MS et al. Effects of mother's illness and breastfeeding on risk of Ebola virus disease in a cohort of very young children. PLoS Negl Trop Dis 2016; 10:e0004622. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 74. World Health Organization (WHO). Ebola virus disease in pregnancy: screening and management of Ebola cases, contacts and survivors. Geneva: WHO, 2015. http://www.who.int/csr/resources/publications/ebola/pregnancy-guidance/en/ Accessed 18 September 2015. [Google Scholar]
- 75. Osterholm MT, Moore KA, Kelley NS et al. Transmission of ebola viruses: what we know and what we do not know. MBio 2015; 6:e01154. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 76. Judson S, Prescott J, Munster V. Understanding ebola virus transmission. Viruses 2015; 7:511–21. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 77. Jaax N, Jahrling P, Geisbert T et al. Transmission of Ebola virus (Zaire strain) to uninfected control monkeys in a biocontainment laboratory. Lancet 1995; 346:1669–71. [DOI] [PubMed] [Google Scholar]
- 78. Jaax NK, Davis KJ, Geisbert TJ et al. Lethal experimental infection of rhesus monkeys with Ebola-Zaire (Mayinga) virus by the oral and conjunctival route of exposure. Arch Pathol Lab Med 1996; 120:140–55. [PubMed] [Google Scholar]
- 79. Johnson E, Jaax N, White J, Jahrling P. Lethal experimental infections of rhesus monkeys by aerosolized Ebola virus. Int J Exp Pathol 1995; 76:227–36. [PMC free article] [PubMed] [Google Scholar]
- 80. Wong G, Qiu X, Richardson JS et al. Ebola virus transmission in guinea pigs. J Virol 2015; 89:1314–23. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 81. Reed DS, Lackemeyer MG, Garza NL, Sullivan LJ, Nichols DK. Aerosol exposure to Zaire ebolavirus in three nonhuman primate species: differences in disease course and clinical pathology. Microbes Infect 2011; 13:930–6. [DOI] [PubMed] [Google Scholar]
- 82. Kobinger GP, Leung A, Neufeld J et al. Replication, pathogenicity, shedding, and transmission of Zaire ebolavirus in pigs. J Infect Dis 2011; 204:200–8. [DOI] [PubMed] [Google Scholar]
- 83. Weingartl HM, Embury-Hyatt C, Nfon C, Leung A, Smith G, Kobinger G. Transmission of Ebola virus from pigs to non-human primates. Sci Rep 2012; 2:811. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 84. Alimonti J, Leung A, Jones S et al. Evaluation of transmission risks associated with in vivo replication of several high containment pathogens in a biosafety level 4 laboratory. Sci Rep 2014; 4:5824. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 85. Twenhafel NA, Mattix ME, Johnson JC et al. Pathology of experimental aerosol Zaire ebolavirus infection in rhesus macaques. Vet Pathol 2013; 50:514–29. [DOI] [PubMed] [Google Scholar]
- 86. Wamala JF, Lukwago L, Malimbo M et al. Ebola hemorrhagic fever associated with novel virus strain, Uganda, 2007–2008. Emerg Infect Dis 2010; 16:1087–92. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 87. Kerstiens B, Matthys F. Interventions to control virus transmission during an outbreak of Ebola hemorrhagic fever: experience from Kikwit, Democratic Republic of the Congo, 1995. J Infect Dis 1999; 179(suppl 1):S263–7. [DOI] [PubMed] [Google Scholar]
- 88. Sagripanti JL, Rom AM, Holland LE. Persistence in darkness of virulent alphaviruses, Ebola virus, and Lassa virus deposited on solid surfaces. Arch Virol 2010; 155:2035–9. [DOI] [PubMed] [Google Scholar]
- 89. Sagripanti JL, Lytle CD. Sensitivity to ultraviolet radiation of Lassa, vaccinia, and Ebola viruses dried on surfaces. Arch Virol 2011; 156:489–94. [DOI] [PubMed] [Google Scholar]
- 90. Sinclair R, Boone SA, Greenberg D, Keim P, Gerba CP. Persistence of category A select agents in the environment. Appl Environ Microbiol 2008; 74:555–63. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 91. Westhoff Smith D, Hill-Batorski L, N'Jai A et al. Ebola virus stability under hospital and environmental conditions. J Infect Dis 2016; 214(suppl 3):S142–4. [DOI] [PubMed] [Google Scholar]
- 92. Bower H, Johnson S, Bangura MS et al. Exposure-specific and age-specific attack rates for Ebola virus disease in Ebola-affected households, Sierra Leone. Emerg Infect Dis 2016; 10.3201/eid2208.160163. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 93. Green E, Hunt L, Ross JC et al. Viraemia and Ebola virus secretion in survivors of Ebola virus disease in Sierra Leone: a cross-sectional cohort study. Lancet Infect Dis 2016; 10.1016/S1473-3099(16)30060-3. [DOI] [PubMed] [Google Scholar]
- 94. World Health Organization. Clinical management of patients with viral hemorrhagic fever. Geneva: World Health Organization, 2014. [Google Scholar]