In the 200 years since the New England Journal of Medicine was founded, cancer has gone from a black box to a blueprint. During the first century of the Journal’s publication, medical practitioners could observe tumors, weigh them, and measure them but had few tools to examine the workings within the cancer cell. A few astute observers were ahead of their time, including Rudolf Virchow, who with the benefit of a microscope deduced the cellular origin of cancer in 1863,1 and Stephen Paget, who in 1889 wisely mused about the seed-and-soil hypothesis of metastatic disease,2 a theory that is coming into its own today (Table 1). Other key advances were the discovery of a viral cause of avian cancer by Peyton Rous in 19113 and the proposal by Theodor Boveri in 1914 that cancer can be triggered by chromosomal mutations.4
Table 1.
Singular Discoveries and Major Events in the Cancer Field and Changing Relative Survival Rates for Patients with Cancer in the United States, 1863–2006.*
| Year | Discovery or Event | Relative Survival Rate |
|---|---|---|
| 1863 | Cellular origin of cancer (Virchow) | |
| 1889 | Seed-and-soil hypothesis (Paget) | |
| 1914 | Chromosomal mutations in cancer (Boveri) | |
| 1937 | Founding of NCI | |
| 1944 | Transmission of cellular information by DNA (Avery) | |
| 1950 | Availability of cancer drugs through Cancer Chemotherapy National Service Center | |
| 1953 | Report on structure of DNA | 35% |
| 1961 | Breaking of the genetic code | |
| 1970 | Reverse transcriptase | |
| 1971 | Restriction enzymes Passage of National Cancer Act | |
| 1975 | Hybridomas and monoclonal antibodies Tracking of cancer statistics by SEER program | 50% |
| 1976 | Cellular origin of retroviral oncogenes | |
| 1979 | Epidermal growth factor and receptor | |
| 1981 | Suppression of tumor growth by p53 | |
| 1984 | G proteins and cell signaling | |
| 1986 | Retinoblastoma gene | |
| 1990 | First decrease in cancer incidence and mortality | |
| 1991 | Association between mutation in APC gene and colorectal cancer | |
| 1994 | Genetic cancer syndromes Association between BRCA1 and breast cancer | |
| 2000 | Sequencing of the human genome | |
| 2002 | Epigenetics in cancer MicroRNAs in cancer | |
| 2005 | First decrease in total number of deaths from cancer | 68% |
| 2006 | Tumor stromal interaction |
Data are from the National Cancer Institute (NCI) Survival, Epidemiology, and End Results (SEER) program. APC denotes adenomatous polyposis coli.
But the lid of the black box was not seriously pried open until 1944, when a retired scientist at Rockefeller University, Oswald Avery, reported the results of his beautifully clear experiments with the pneumococcal bacillus, which showed that cellular information was transmitted not by proteins but by DNA.5 His work led directly to the important discovery of the structure of DNA by Watson and Crick in 1953.6 Eight years later, the genetic code was broken by Nirenberg and colleagues,7 and the central dogma of biology was established; that information was transmitted from DNA to RNA and resulted in the synthesis of proteins. Then, the first of a series of totally unexpected discoveries disrupted this thinking, and we were reminded that things are not always what they seem in dealing with Mother Nature. The discovery of reverse transcriptase by Temin and Mizutani8 and Baltimore9, which showed that information could be transmitted the other way, from RNA to DNA, had a profound influence on medicine but most particularly on cancer medicine.
Early investigators discovered that DNA is a very large molecule that was difficult to study in the laboratory. In 1970, Smith and Wilcox solved this problem by identifying enzymes that bacteria used defensively to cleave DNA at specific restriction sites.10 These discoveries gave birth to the molecular revolution and the biotechnology industry. They also paved the way for the sequencing of the genome.
This kind of science was expensive. The U.S. Congress partially addressed the problem by passing the National Cancer Act, which expanded the role of the National Cancer Institute (NCI), the first disease-oriented agency at the National Institutes of Health (NIH). The act, which was signed into law on December 23, 1971, by President Richard Nixon, created a new mandate for an NIH institute: “to support research and the application of the results of research to reduce the incidence, morbidity and mortality from cancer.” The emphasis on the application of the results of research was new; it had not been in the mission statement of the NIH. The act would quintuple the budget of the NCI by the end of the decade and provide the fuel for the revolution in molecular biology.
Although the enthusiasm in Congress for eradicating cancer was largely derived from excitement over a few clinical advances, about 85% of these new funds went to support basic research. At its peak in the early 1980s, the NCI accounted for 23% of the budget of the NIH, yet it supported 53% of the research in molecular biology in the United States. And the results have been explosive.
The discovery of genes that drive or suppress cellular growth and the complex regulation of signaling systems used by both normal cells and cancer cells to communicate with each other and their environment have brought the blueprint of cancer-cell machinery into bold relief (Table 1). The association of specific abnormalities with specific cancers has allowed scientists to identify persons who are at increased risk for common cancers, such as breast and colon cancer.
MILESTONES IN CANCER TREATMENT
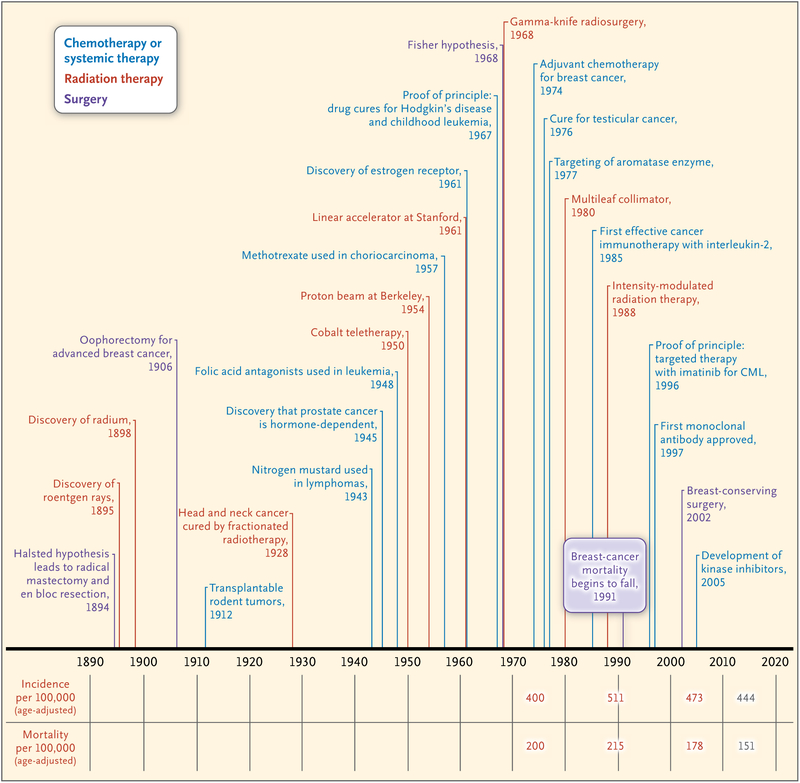
Experiments that can be done in hours in the laboratory take months and years to replicate in the clinic, so clinical advances, though plentiful, develop slowly. Figures 1 and 2 depict the pace of change for the past two centuries in four areas: cancer treatment, chemoprevention, viruses and cancer-vaccine development, and tobacco control.
Figure 1. Timeline of Pivotal Events in Cancer Treatment.
CML denotes chronic myeloid leukemia.
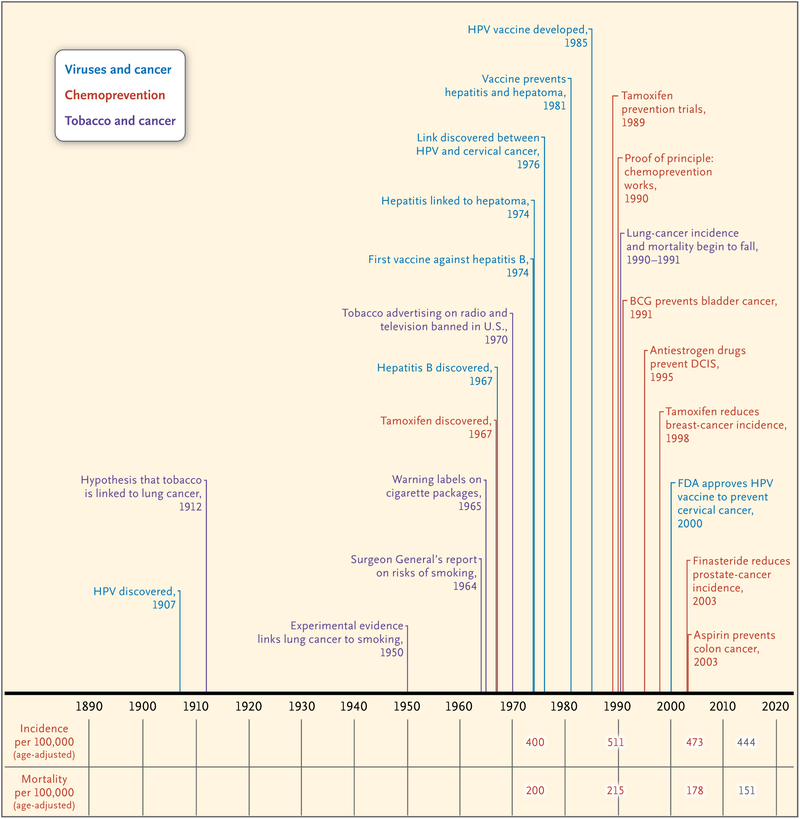
Figure 2. Timeline of Pivotal Events in Cancer Prevention.
BCG denotes bacille Calmette–Guérin, DCIS ductal carcinoma in situ, FDA Food and Drug Administration, and HPV human papillomavirus.
In the treatment of cancer, surgery was the first tool available. In 1809, Ephraim McDowell removed an ovarian tumor without the use of anesthesia, the first abdominal surgery performed in the United States, and provided evidence that tumor masses could be cured by surgery. The first public use of anesthesia, as reported by John Collins Warren in the Journal in 1846,11 and the introduction of antisepsis by Joseph Lister in 186712 paved the way for a cascade of surgical firsts in cancer treatment in the 19th and early 20th centuries. These innovative surgeons showed that any organ that was affected by cancer could be dealt with surgically.13
The most profound influence on cancer surgery occurred in 1894, when William Halsted14 introduced radical mastectomy for breast cancer. Halsted based his operation on the supposition that breast cancer spread in a centrifugal fashion from the primary tumor to adjacent structures. He recommended en bloc resection of all surrounding tissue to remove all cancer cells, even the head of the humerus if it was involved. En bloc resection became known as “the cancer operation,” and it was applied to the removal of all other cancers, despite scant evidence supporting its use. It would be 74 years before the use of radical mastectomy and en bloc resection was questioned by another surgeon, Dr. Bernard Fisher. On the basis of experiments in rodent tumors, Fisher proposed that breast cancer had early access to the bloodstream and lymphatic tissues. Lymph-node involvement, he hypothesized, was merely an indication of generalized spread of disease. Radical mastectomy was both too much and too little: too much for small tumors and too little for large tumors that had already metastasized. In a series of clinical trials conducted by what is now called the National Surgical Adjuvant Breast and Bowel Project (NSABP), which Fisher led, he clearly showed that radical en bloc removal of tissue did nothing more than could be accomplished by removing the tumor mass itself, if surgery was supplemented by chemotherapy, radiation therapy, or both. Fisher also showed that less radical surgery plus chemo-therapy or radiation therapy accomplished the goal with much less morbidity. These studies15–25 revolutionized the treatment of breast cancer. Since then, most other surgical procedures have been tailored to the availability of other treatments, and cancer surgery has become more effective, with less morbidity. In the first half of the 20th century, however, surgery was the only option, and a minority of patients could be cured by surgical removal of their tumors alone.
The era of radiation treatment began in 1895, when Roentgen reported on his discovery of x-rays,26 and accelerated in 1898 with the discovery of radium by Pierre and Marie Curie.27 In 1928, it was shown that head it was shown that and neck cancers could be cured by fractionated radiation treatments, a milestone in the field.28 The modern era of radiation therapy began in 1950 with the introduction of cobalt teletherapy. Since then, aided by advances in computing, the field has been driven by advances in technology that have allowed the therapeutic radiologist to deliver beam energy precisely to the tumor and to spare the normal tissue in the path of the radiation beam. Like surgery, radiation therapy has become more effective, with less morbidity, and can be used in combination with other treatments.
By the 1950s, it had become apparent that no matter how complete the resection or how good the radiation therapy or how high the dose delivered, cure rates after surgery, radiation therapy, or the two combined had flattened out. Only about a third of all cancers could be cured by the use of these two treatment approaches, alone or together.
It was Paul Ehrlich at the turn of the 20th century who first made a concerted effort to develop chemicals to cure cancer. He coined the word “chemotherapy.” After animal models of transplantable tumors were developed in the early 20th century,29 researchers devoted the first half of the century to establishing screening systems that would reliably predict antitumor activity in humans on the basis of data from murine models. However, these efforts were largely unsuccessful. Part of the problem was the limited capability for testing new agents in humans. Two events provided optimism about the future of anticancer drugs: the use of nitrogen mustard in lymphomas at Yale in 194330 and Farber’s report in 1948 that folic acid antagonists could induce temporary remission in childhood leukemia.31 In 1955, these discoveries led to a national screening effort to develop and test anticancer drugs. Then the use of cancer chemotherapy, although shrouded in controversy, began in earnest. Missing was proof of principle, already established for surgery and radiation therapy, that drugs could cure any cancer. Major advances came in the mid-1960s with firm evidence that childhood leukemia32 and advanced Hodgkin’s disease in adults33,34 could be cured by combination chemotherapy.
Proof of cure by chemotherapy had a permissive effect on the use of drugs as an adjuvant to surgery and radiation therapy. Doctors started to be willing to consider using chemotherapy. In the mid-1970s, two landmark studies of adjuvant chemotherapy in breast cancer were published: one from the NSABP, which tested a single drug and was reported by Fisher and colleagues in 1975,15 and one from Italy, which tested a drug combination and was reported by Bonadonna et al. in 1976.35 The latter study evaluated a combination regimen (cyclophosphamide, methotrexate, and fluorouracil) developed by the NCI but was performed under contract with the Milan Cancer Institute, despite large populations of patients with operable breast cancer in the United States, because no major U.S. center was willing to test combination chemotherapy as an adjuvant. The results of both studies were positive, and the race was on. By 1991, thanks to the availability of multiple effective chemotherapeutic agents and hormone treatments, improved diagnostic tools for early diagnosis, and intelligently designed clinical trials, the rate of death from breast cancer began to fall, a trend that has continued.36 Early diagnosis and lumpectomy coupled with systemic therapy have greatly reduced the morbidity associated with breast-cancer treatment, with good cosmetic effects. Such advances have fulfilled the mandate of the war on cancer “to support research … to reduce the incidence, morbidity and mortality from cancer.”
The success of adjuvant treatment of breast cancer, in turn, had a permissive effect on the use of drugs in the postoperative treatment of other major cancers, such as colorectal cancer. As a consequence of early diagnosis, prevention, and adjuvant treatment, the rate of death from colorectal cancer has fallen by 40% during the past four decades.36
Another paradigmatic change in cancer treatment occurred in 2006, when Druker et al.37 showed the efficacy of a drug (imatinib) that targeted the unique molecular abnormality in chronic myeloid leukemia. This work provided proof of principle that treatments targeting specific molecular abnormalities that are unique to certain cancers could convert them into manageable chronic illnesses. Since then, chemotherapy has become targeted therapy, and the literature has been dominated by the search for drugs to inhibit unique molecular targets, with recent success in the treatment of some very difficult-to-treat tumors, such as melanoma38 and lung cancer.39
Until recently, cancer treatment was a three-legged stool sitting on a base of surgery, radiation therapy, and chemotherapy. In the past 25 years, immunotherapy has been added as an important component of cancer treatment.
Antibodies were first described in the 1880s and dominated studies of immunology for almost 100 years but had little effect on cancer treatment. In 1975, Köhler and Milstein developed methods for producing antibodies by fusing cultured myeloma cells with normal B cells from immunized mice.40 The availability of large amounts of an tibodies with a single specificity led to the successful development of therapeutic antibodies for cancer, starting with approval by the Food and Drug Administration (FDA) of rituximab for the treatment of B-cell lymphomas in 199741 and followed by the approval of many other antibodies, most of which act by inhibiting growth factor receptors on the surface of cancer cells.
In the early 1960s, it became clear that cellular rather than humoral immunity played a major role in the immune destruction of experimental cancers, although the inability to manipulate T cells outside the body severely hampered studies of tumor immunity. The description of T-cell growth factor (subsequently called interleukin-2) in 1976 was a seminal discovery that stimulated extensive studies of the cellular immune reaction to experimental and human cancers.42 The durable regression of metastatic melanoma and renal cancers in humans after the administration of interleukin-2, described in 1985, represented the first clear demonstration that immune manipulations could cause the regression of invasive metastatic disease.43 Interleukin-2 was approved for the treatment of metastatic renal cancer in 1992 and for meta-static melanoma in 1998. The subsequent development of immunomodulatory agents such as ipilimu mab,44 the development of cell-transfer therapies,45,46 and the use of genetically engineered lymphocytes to treat cancer47 have provided additional evidence of the ability of immuno-therapy to mediate cancer regression. With the increasing use of these agents, the cancer-treatment platform sits firmly on four legs.
CANCER PREVENTION
No matter how easy cancer treatment may become, it is preferable to prevent cancer. But prevention has been an elusive goal. Figure 2 illustrates three notable pathways to success, with discoveries of the connection between viruses and cancer, methods of chemoprevention, and the role of tobacco in cancer. When the cause of cancer is known, its prevention becomes a problem in modifying human behavior. Nicotine is one of the most addicting substances known, and exposure to tobacco smoke is by far the best known and most frequent cause of cancer, causing an estimated 40% of all deaths from cancer. It was suggested as early as 1912 that smoking might be related to lung cancer,48 with the epidemiologic evidence becoming solid in the 1950s. These findings led to the Surgeon General’s report on smoking and cancer that was issued in 1964,49 the use of warning labels on cigarette packages in 1965, and a ban on tobacco advertising in 1970. These and other aggressive, well-publicized public health measures, which were strongly pursued by the American Cancer Society with support from the NCI, have led to a steady reduction in the rate of smoking, which has decreased to half the 1950 level in the United States. It takes time for the deleterious effects of the thousands of carcinogenic chemicals in tobacco to dissipate, and it was not until 1990 that the incidence of lung cancer in men began to decline, followed by a decline in lung-cancer mortality beginning in 1991.
To date, the historic goal of creating a cancer vaccine has been realized only for cancers that are caused by viral infections. Even when the causal virus has been identified, the elapsed time from discovery to prevention has been long. The human papillomavirus was discovered in 1907, but it was not linked to cervical cancer until 1976,50 and a vaccine to prevent infection by the virus in young girls was not approved by the FDA until 2000. Hepatitis B virus was discovered in 1967 and was linked to liver cancer in 1974. In 1984, it was shown that both hepatitis B and liver cancer could be prevented by vaccination against hepatitis B.51 Since then, in some parts of the world, vaccination of newborns against the hepatitis B virus has become routine. Since it is estimated that 20% of all cancers are caused in some way by viruses, further development of vaccines holds much promise.
The use of chemicals to prevent cancer (chemoprevention) can be effective.52 Antiestrogens can prevent ductal carcinoma in situ and reduce the incidence of breast cancer, finasteride can prevent prostate cancer, and plain old aspirin can prevent colorectal cancer. However, this approach is not widely used because large numbers of otherwise normal persons would need to be exposed to potentially toxic materials in order to prevent some cancers.
SURVIVAL NOW AND IN THE FUTURE
Table 1 shows the changes in relative cancer survival rates related to events in science, and Figures 1 and 2 show changes in cancer incidence and mortality, with notations in the charts when the rates of death from a specific cancer began to fall. Soon after the development of successful treatments in the 1970s, disease-specific death rates began to fall dramatically for childhood leukemia and Hodgkin’s disease. The incidence of these diseases was too low to affect overall rates of death from cancer. Overall rates began to decline soon after the introduction of better early diagnosis and preventive measures and effective adjuvant treatment of common cancers, such as cancer of the breast and colon. The 5-year relative survival rate for all cancers, which was 38% in the late 1960s, just before the passage of the National Cancer Act, is now 68%. Straight-line projections indicate that the survival rate will rise to 80% by 2015.53,54 Overall rates of death from cancer, which began to decline in 1990 in the United States, have decreased by 24% overall since then.53,54 Straight-line projections to the year 2015 indicate that the overall absolute reduction in cancer mortality will be about 38 percentage points.
However, these projections are almost certainly underestimates, since they are based on the assumption that there will be little change in the management of cancer between now and 2015. Most of the current declines are the result of the widespread implementation of old technology for diagnosis, prevention, and treatment, stimulated by funds provided by the war on cancer. However, the biggest payoff from that investment — the clinical application of the fruits of the extraordinary molecular revolution initiated by the National Cancer Act — is yet to come and cannot be measured with the use of current statistics.
THE FUTURE
The sequencing of the human genome in 2000 has had a profound effect on all of medicine. The cost of sequencing is reminiscent of Moore’s law, with the cost halving every 2 years. It is not difficult to foresee a time when a person’s individual genome can be sequenced for as little as $100, putting genetic studies in the realm of a routine laboratory test. Starter companies with this aim already exist.
Second- and third-generation deep sequencing is revealing the complexity of the cancer blueprint and no doubt will reveal networks not yet imagined. Nonetheless, we are clearly facing a future in which patients with cancer or those at increased risk will have their genome sequenced as a matter of routine, with comparisons between the premalignant tissue and the malignant tissue. Detected abnormalities will become targets of relatively simple drug therapies, and if the effects mirror what we have seen in recent years with targeted therapy, the ability to prevent or treat cancers in the future will be impressive. The economic and social consequences of converting cancer into a curable or chronic disease will be both gratifying and daunting. This overview of 200 years of the cancer field provides support for the principle of the value of patience and investment in research.
Footnotes
Disclosure forms provided by the authors are available with the full text of this article at NEJM.org.
References
- 1.Virchow R Cellular pathology as based upon physiological and pathological histology. Philadelphia: J.B. Lippincott, 1863. [DOI] [PubMed] [Google Scholar]
- 2.Paget S The distribution of secondary growths in cancer of the breast. Lancet 1889;1:571–3. [PubMed] [Google Scholar]
- 3.Rous P A transmissible avian neoplasm (sarcoma of the common fowl). J Exp Med 1910;12:696–705. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Boveri T Zur Frage der Entwicklung maligner Tumoren. Jena, Germany: Gustav Fischer-Verlag, 1914. [Google Scholar]
- 5.Avery OT, Macleod CM, McCarty M. Studies of the chemical nature of the substance inducing transformation of pneumococcal types: induction of transformation by a desoxyribonucleic acid fraction isolated from pneumococcus type III. J Exp Med 1944;79:137–58. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Watson JD, Crick FHC. Molecular structure of nucleic acids: structure for deoxyribose nucleic acid. Nature 1953; 171:737–8. [DOI] [PubMed] [Google Scholar]
- 7.Nirenberg MW, Matthaei JH. The dependence of cell-free protein synthesis in E. coli upon naturally occurring or synthetic polyribonucleotides. Proc Natl Acad Sci U S A 1961;47:1588–602. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Temin HM, Mizutani S. RNA-dependent DNA polymerase in virions of rous sarcoma virus. Nature 1970;226:1211–3. [Erratum, Nature 1970;227:102.] [DOI] [PubMed] [Google Scholar]
- 9.Baltimore D RNA-dependent DNA polymerase in virions of RNA tumour viruses. Nature 1970;226:1209–11. [DOI] [PubMed] [Google Scholar]
- 10.Smith HO, Wilcox KW. A restriction enzyme from Hemophilus influenzae. I. Purification and general properties. J Mol Biol 1970;51:379–91. [DOI] [PubMed] [Google Scholar]
- 11.Warren JC. Inhalation of ethereal vapor for the prevention of pain in surgical operations. Boston Med Surg J 1846;35: 375–9. [Google Scholar]
- 12.Lister J On the antiseptic principle in the practice of surgery. Br Med J 1867;2: 246–8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Whipple AO, Parsons WB, Mullins CR. Treatment of carcinoma of the ampulla of Vater. Ann Surg 1935;102:763–79. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Halsted WS. The results of operations for the cure of cancer of the breast performed at the Johns Hopkins Hospital from June, 1889, to January, 1894. Ann Surg 1894;20:497–555. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Fisher B, Carbone P, Economou SG, et al. L-phenylalanine mustard (L-PAM) in the management of primary breast cancer. N Engl J Med 1975;292:110–22. [DOI] [PubMed] [Google Scholar]
- 16.Fisher B, Redmund C, Brown A. Treatment of primary breast cancer with chemotherapy and tamoxifen. N Engl J Med 1981;305:1–6. [DOI] [PubMed] [Google Scholar]
- 17.Fisher B, Bauer M, Margolese R. Five-year results of a randomized clinical trial comparing total mastectomy and segmental mastectomy with or without radiation in the treatment of breast cancer. N Engl J Med 1985;312:665–73. [DOI] [PubMed] [Google Scholar]
- 18.Fisher B, Redmond C, Fisher ER. Ten-year results of a randomized clinical trial comparing radical mastectomy and total mastectomy with or without radiation. N Engl J Med 1985;312:674–81. [DOI] [PubMed] [Google Scholar]
- 19.Fisher B, Redmond C, Dimitrov NV, et al. A randomized clinical trial evaluating sequential methotrexate and fluorouracil in the treatment of patients with node-negative breast cancer who have estrogen-receptor-negative tumors. N Engl J Med 1989;320:473–8. [DOI] [PubMed] [Google Scholar]
- 20.Fisher B, Costantino J, Redmond C, et al. A randomized clinical trial evaluating tamoxifen in the treatment of patients with node-negative breast cancer who have estrogen-receptor–positive tumors. N Engl J Med 1989;320:479–84. [DOI] [PubMed] [Google Scholar]
- 21.Fisher B, Redmond C, Poisson R, et al. Eight-year results of a randomized clinical trial comparing total mastectomy and lumpectomy with or without irradiation in the treatment of breast cancer. N Engl J Med 1989;320:822–8. [Erratum, N Engl J Med 1994;330:1467.] [DOI] [PubMed] [Google Scholar]
- 22.Fisher B, Costantino J, Redmond C, et al. Lumpectomy compared with lumpectomy and radiation therapy for the treatment of intraductal breast cancer. N Engl J Med 1993;328:1581–6. [DOI] [PubMed] [Google Scholar]
- 23.Fisher B, Anderson S, Redmond CK, Wolmark N, Wickerham L, Cronin WM. Reanalysis and results after 12 years of follow-up in a randomized clinical trial comparing total mastectomy with lumpectomy with or without irradiation in the treatment of breast cancer. N Engl J Med 1995;333:1456–61. [DOI] [PubMed] [Google Scholar]
- 24.Fisher B, Anderson S, Bryant J, et al. Twenty-year follow-up of a randomized trial comparing total mastectomy, lumpectomy, and lumpectomy plus irradiation for the treatment of invasive breast cancer. N Engl J Med 2002;347:1233–41. [DOI] [PubMed] [Google Scholar]
- 25.Fisher B, Anderson SJ. Local therapy and survival in breast cancer. N Engl J Med 2007;357:1051–2. [DOI] [PubMed] [Google Scholar]
- 26.Roentgen K On a new kind of rays. Stanton A, trans. Nature 1896;53:274. [Google Scholar]
- 27.Curie P, Curie M, Bémont G. On a new, strongly radioactive substance contained in pitchblende. CR (East Lansing, Mich) 1898;127:1215–7. [Google Scholar]
- 28.Coutard H Roentgen therapy of epitheliomas of the tonsillar region, hypopharynx, and larynx from 1920 to 1926. AJR Am J Roentgenol 1932;28:313–31. [Google Scholar]
- 29.Clowes GHA, Baeslack FW. Further evidence of immunity against cancer in mice after spontaneous recovery: sixth annual report. Albany: New York State Cancer Laboratory, 1904–5. [Google Scholar]
- 30.Goodman LS, Wintrobe MM, Dameshek W, et al. Nitrogen mustard therapy: use of methyl-bis(beta-chloroethyl) amine hydrochloride and tris (beta-chloroethyl) amine hydrochloride for Hodgkin’s disease, lymphosarcoma, leukemia, and certain allied and miscellaneous disorders. JAMA 1946;105:475–6. [DOI] [PubMed] [Google Scholar]
- 31.Farber S, Diamond LK, Mercer RD, Sylvester RF Jr, Wolff JA. Temporary remissions in acute leukemia in children produced by folic acid antagonist, 4-amino-pteroyl-glutamic acid (aminopterin). N Engl J Med 1948;238:787–93. [DOI] [PubMed] [Google Scholar]
- 32.Frei E III, Karon M, Levin RH, et al. The effectiveness of combinations of anti-leukemic agents in inducing and maintaining remission in children with acute leukemia. Blood 1965;26:642–56. [PubMed] [Google Scholar]
- 33.DeVita VT, Moxley JH, Brace K, Frei E III. Intensive combination chemotherapy and X-irradiation in the treatment of Hodgkin’s disease. Proc Am Assoc Cancer Res 1965;6:15. [Google Scholar]
- 34.DeVita VT Jr, Serpick AA, Carbone PP. Combination chemotherapy in the treatment of advanced Hodgkin’s disease. Ann Intern Med 1970;73:881–95. [DOI] [PubMed] [Google Scholar]
- 35.Bonadonna G, Brusamolino E, Valagussa P, et al. Combination chemotherapy as an adjuvant treatment in operable breast cancer. N Engl J Med 1976;294:405–10. [DOI] [PubMed] [Google Scholar]
- 36.Brawley O A strategic approach to the control of cancer. National Press Foundation; (http://nationalpress.org/images/uploads/programs/10cancer_brawley.ppt). [Google Scholar]
- 37.Druker BJ, Guilhot F, O’Brien SG, et al. Five-year follow-up of patients receiving imatinib for chronic myeloid leukemia. N Engl J Med 2006;355:2408–17. [DOI] [PubMed] [Google Scholar]
- 38.Chapman PB, Hauschild A, Robert C, et al. Improved survival with vemurafenib in melanoma with BRAF V600E mutation. N Engl J Med 2011;364:2507–16. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 39.Kwak EL, Bang Y-J, Camidge DR, et al. Anaplastic lymphoma kinase inhibition in non–small-cell lung cancer. N Engl J Med 2010;363:1693–703. [Erratum, N Engl J Med 2011;364:588.] [DOI] [PMC free article] [PubMed] [Google Scholar]
- 40.Köhler G, Milstein C. Continuous cultures of fused cells secreting antibody of predefined specificity. Nature 1975;256: 495–7. [DOI] [PubMed] [Google Scholar]
- 41.Maloney DG, Grillo-López AJ, White CA, et al. IDEC-C2B8 (rituximab) anti-CD20 monoclonal antibody therapy in patients with relapsed low-grade non-Hodgkin’s lymphoma. Blood 1997;90:2188–95. [PubMed] [Google Scholar]
- 42.Morgan DA, Ruscetti FW, Gallo RG. Selective in vitro growth of T lymphocytes from normal bone marrows. Science 1976;193:1007–8. [DOI] [PubMed] [Google Scholar]
- 43.Rosenberg SA, Lotze MT, Muul LM, et al. Observations on the systemic administration of autologous lymphokine-activated killer cells and recombinant interleukin-2 to patients with metastatic cancer. N Engl J Med 1985;313:1485–92. [DOI] [PubMed] [Google Scholar]
- 44.Hodi FS, O’Day SJ, McDermott DF, et al. Improved survival with ipilimumab in patients with metastatic melanoma. N Engl J Med 2010;363:711–23. [Erratum, N Engl J Med 2010;363:1290.] [DOI] [PMC free article] [PubMed] [Google Scholar]
- 45.Rosenberg SA, Packard BS, Aebersold PM, et al. Use of tumor infiltrating lymphocytes and interleukin-2 in the immunotherapy of patients with metastatic melanoma: preliminary report. N Engl J Med 1988;319:1676–80. [DOI] [PubMed] [Google Scholar]
- 46.Dudley ME, Wunderlich JR, Robbins PF, et al. Cancer regression and autoimmunity in patients after clonal repopulation with antitumor lymphocytes. Science 2002;298:850–4. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 47.Morgan RA, Dudley ME, Wunderlich JR, et al. Cancer regression in patients after transfer of genetically engineered lymphocytes. Science 2006;314:126–9. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 48.Adler L Primary malignant growth of the lungs and bronchi. London: Longmans-Green, 1912. [Google Scholar]
- 49.Smoking and health: report of the Advisory Committee to the Surgeon General of the Public Health Service. Washington, DC: Department of Health, Education, and Welfare, Public Health Service, 1964. (Publication no. (PHS) 1103.) [Google Scholar]
- 50.zur Hausen H Condylomata acuminata and human genital cancer. Cancer Res 1976;36:794. [PubMed] [Google Scholar]
- 51.Wong VC, Ip HM, Reesink HW, et al. Prevention of the HBsAg carrier state in newborn infants of mothers who are chronic carriers of HBsAg and HBeAg by administration of hepatitis-B vaccine and hepatitis-B immunoglobulin: double-blind randomised placebo-controlled study. Lancet 1984;1:921–6. [DOI] [PubMed] [Google Scholar]
- 52.Hong WK, Lippman SM, Itri LM, Karp DD. Prevention of second primary tumors with isotretinoin in squamous-cell carcinoma of the head and neck. N Engl J Med 1990;323:795–801. [DOI] [PubMed] [Google Scholar]
- 53.Byers TE. Trends in cancer mortality In: DeVita VT Jr, Lawrence TS, Rosenberg SA, DePinho RA, Weinberg RA, eds. DeVita, Hellman, and Rosenberg’s cancer: principles & practices of oncology. 9th ed. Philadelphia: Wolters Kluwer Health/Lippincott Williams & Wilkins, 2011:261–8. [Google Scholar]
- 54.Byers T, Barrera E, Fontham ET, et al. A midpoint assessment of the American Cancer Society challenge goal to halve the U.S. cancer mortality rates between the years 1990 and 2015. Cancer 2006;107: 396–405. [DOI] [PubMed] [Google Scholar]