Abstract
Cancer is one of the leading causes of death worldwide, and conventional cancer therapies such as surgery, chemotherapy, and radiotherapy do not address the underlying molecular pathologies, leading to inadequate treatment and tumor recurrence. Angiogenic factors, such as EGF, PDGF, bFGF, TGF-β, TGF-α, VEGF, endoglin, and angiopoietins, play important roles in regulating tumor development and metastasis, and they serve as potential targets for developing cancer therapeutics. Nucleic acid-based therapeutic strategies have received significant attention in the last two decades, and antisense oligonucleotide-mediated intervention is a prominent therapeutic approach for targeted manipulation of gene expression. Clinical benefits of antisense oligonucleotides have been recognized by the U.S. Food and Drug Administration, with full or conditional approval of Vitravene, Kynamro, Exondys51, and Spinraza. Herein we review the scope of antisense oligonucleotides that target angiogenic factors toward tackling solid cancers.
Keywords: antisense oligonucleotides, nucleic acids, angiogenesis, antisense, modified oligonucleotides, cancer
Main Text
Antisense oligonucleotides (AOs) are a class of molecule that can specifically bind to RNA target molecules in order to manipulate gene expression.1, 2, 3, 4 Recent progress in AO-based therapeutics has attracted significant attention in drug development for different diseases.4, 5 To date, the U.S. Food and Drug Administration (FDA) has approved four antisense drugs: Vitravene for the treatment of cytomegalovirus (CMV) retinitis in immunocompromised patients,6 Kynamro for the treatment of homozygous familial hypercholesterolemia,7 Exondys51 for the treatment of Duchenne muscular dystrophy (DMD),8 and Spinraza for the treatment of spinal muscular atrophy (SMA).9, 10 These successful clinical translations demonstrate the scope of utilizing AOs as therapies for tackling various diseases through the induction of targeted degradation, exon skipping, or exon retention in the mature or pre-mRNA.
Angiogenesis is the physiological process of new blood vessel growth,11, 12, 13, 14 and the discovery of tumor angiogenesis nearly 50 years ago has opened up a new era in cancer drug development.15, 16, 17 Anti-angiogenesis has now become a discrete field of cancer research with over 35,000 published reports,18 and various strategies have been extensively studied in identifying potential angiogenic markers for therapeutic interventions.19, 20, 21, 22 Current cancer therapy involves a combination of different approaches, including surgery, chemotherapy, radiotherapy, immunotherapy, targeted therapy, and hormone therapy.23 In the last two decades, advances in antibody-based and small molecule treatment strategies have led to the translation and clinical use of various cancer drugs, including Avastin24, 25 (antibody targeting vascular endothelial growth factor [VEGF]-A) and Sunitinib26 (small molecule targeting VEGF receptor [VEGFR] and platelet-derived growth factor receptor [PDGFR]), which gained FDA approval in 2004 and 2006, respectively, for the treatment of several cancer types and age-related macular degeneration. However, these approaches are costly due to high required doses, and they commonly showed mild to serious toxic side effects in cancer patients.27, 28, 29
Unlike antibodies and small molecules, AO-based approaches target the cancer hallmark pathologies at the RNA level by sequence-specific binding of a synthetic AO to modulate the expression of pro-oncogenic genes.30, 31, 32 By specifically targeting an implicated causative gene, AO strategies provide explicit efficiency in modulating target gene expression and, thereby, limiting the required doses, which eventually reduce the side effects and cost of treatment. Angiogenic factors,33 such as epidermal growth factor (EGF),34, 35 PDGF,36, 37 basic fibroblastic growth factor (bFGF),38, 39 transforming growth factor (TGF)-β40, 41 and -α,42, 43 VEGFs (VEGF-A),44, 45 endoglin (ENG),46, 47 and angiopoietins (Ang1, 2, 3, and 4),48, 49 have been identified as potential targets for AO-mediated intervention. In this review, we focus on AOs targeting angiogenic factors as therapeutic molecules for treating cancers.
AOs: Therapeutic Benefits and Chemical Modifications
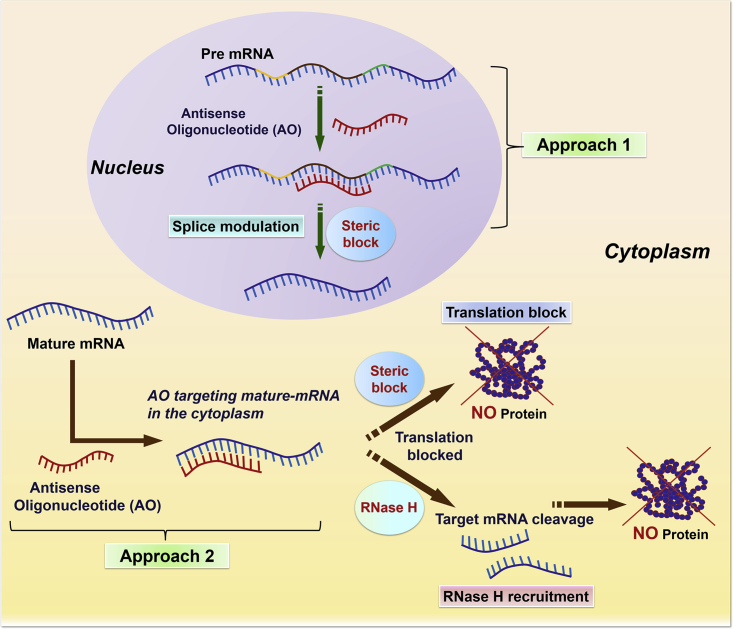
AOs are short synthetic single-stranded nucleic acid sequences that can anneal to cDNA or RNA targets following strict Watson and Crick base-pairing rules.1, 50 Typically, three different antisense mechanisms have been utilized therapeutically: (1) RNase-H-dependent target mRNA cleavage, (2) inhibition of translation by imposing steric block, and (3) modulation of RNA splicing to regulate gene expression (Figure 1).1
Figure 1.
Antisense Oligonucleotide Mechanisms to Alter Gene Expression
Different colors in pre-mRNA structure indicate introns and exons.
In the case of RNase-H-mediated cleavage, the AO binds to the complementary region in the target mature mRNA, forming a DNA or RNA hybrid, which then recruits the RNase-H enzyme that selectively cleaves the target mRNA sequence by hydrolyzing one of its inter-nucleotide phosphate linkages and ablates the target gene expression (Figure 1).50 In the steric block approach, AOs physically block the binding motifs of proteins of the cellular machinery such as the ribosome-binding site, 5′-cap site, or translation initiation site in the mature mRNA (Figure 1).51 Furthermore, the AO can be designed to target pre-mRNA and interfere with RNA-processing events, such as splicing or nuclear polyadenylation.52, 53, 54 The introduction of splice-switching AOs can therapeutically manipulate defective splicing by steric blocking of the splicing motifs, where the splicing factors bind to the pre-mRNA, and, thereby, alter subsequent processes, such as exon skipping, exon inclusion, and intron retention (Figure 1). Additionally, AOs can be targeted to other sites in the pre-mRNA, such as the polyadenylation signal sequence, cleavage or polyadenylation specificity factor (CPSF), or cleavage stimulation factor (CstF), to halt these processes for inducing mRNA degradation or translation arrest.53, 54
AO Limitations and Chemical Modifications
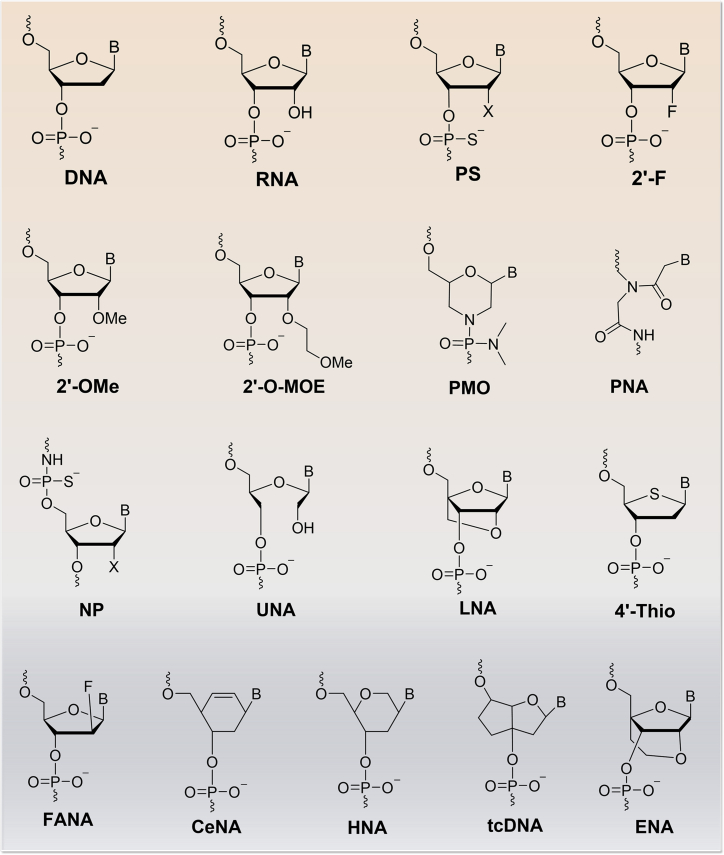
AOs composed of natural nucleotide monomers are not suitable for clinical applications. In fact, there are several factors that possibly influence the efficiency and biological potency of the AO, including stability against nucleases, specificity and binding affinity to the target, cellular uptake and tissue distribution, and toxicity. To overcome these limitations, chemically modified nucleic acid analogs are generally used.55, 56 Chemical modifications can be introduced into the inter-nucleotide linkage, sugar moiety, and/or nucleobase (Figure 2). In the case of inter-nucleotide linkage modification, the non-bridging oxygen atom of the phosphate backbone is replaced with sulfur (phosphorothioate [PS]) or other elements (as in phosphorodiamidate morpholino oligomer [PMO] and peptide nucleic acid), rendering stability against nuclease degradation (Figure 2). Likewise, the sugar moiety is modified to improve the AO-binding affinity and nuclease stability. Some of the prominent sugar-modified analogs are 2′-O-methyl (2′-OMe), 2′-O-methoxyethyl (2′-OMOE), 2′-fluoro RNA (2′-F), locked nucleic acid (LNA), unlocked nucleic acid (UNA), tricycloDNA (tcDNA), hexitol nucleic acid (HNA), and 2′-deoxy-2′-fluoro-βD-arabino nucleic acid (2′-FANA) (Figure 2). Chemically modified nucleobase analogs are not as commonly applied in constructing AOs compared to the sugar and inter-nucleotide linkage modifications. A comprehensive review of oligonucleotide chemical modifications can be found elsewhere.56
Figure 2.
Examples of Prominent Chemically Modified Nucleotides
AO Design Balance between Safety and Efficacy
Recent clinical translation of novel oligonucleotide therapeutic molecules demonstrates the importance of utilizing chemically modified monomers to improve the pharmacokinetics of AO-based drugs.10 However, to develop a successful nucleic acid-based molecule, the modified nucleotides need to be used in an appropriate way to meet the balance between efficacy and safety, which generally is considered to be a clinically relevant feature. One example to highlight the importance of this safety-efficacy balance is the approval of Exondys51 (Sarepta Therapeutics), a PMO drug, and the rejection of Drisapersen (BioMarin Pharmaceutical), a 2′-OMe AO on a PS backbone, by the FDA in 2016. While PMO chemistry has been shown to possess excellent safety data in DMD trials, life-threatening toxicity and poor efficacy were found with 2′-OMePS chemistry. It is worth mentioning that, due to the difference in synthesis approach, the cost to synthesize PMO is a lot higher than 2′-OMePS-based AOs, and, while 2′-OMePS AOs can be synthesized as gapmer or mixmer designs with other modified nucleotide monomers, this is impossible with PMOs. Therefore, AO design plays a pivotal role in the development of any successful nucleic acid-based therapeutics.
Chemically modified AOs can be generally designed as gapmer or mixmer constructs (Figure 3) for mRNA inhibition by RNase-H recruitment and steric blocking of translation or pre-mRNA splicing modulation by splice-switching. In the gapmer design, a central core of natural nucleotide monomers (including PS-linked DNA nucleotides) is flanked by short blocks of modified nucleotides on both the ends to enhance binding and RNase-H-mediated cleavage of the target mRNA. In the mixmer design, the modified nucleotides alternate with natural nucleotides throughout the AO. Mixmers are mainly used for imposing steric bulkiness on their target.
Figure 3.
Design of Gapmer and Mixmer AO Constructs
Green blocks: modified nucleotides; yellow blocks: normal nucleotides.
AO Delivery
Delivery is paramount for AOs to be effective in regulating gene expression.57 Different strategies have been proposed to improve AO delivery, including the use of cell-penetrating peptides, nanoparticles, or liposome complexes.58, 59 Another approach is to induce AO uptake through receptor-mediated endocytosis. This strategy involves conjugating an AO with antibodies or aptamers that readily target the surface receptors of targeted cells.60 In some cases, AOs can be introduced directly to the target tissues such as via intramuscular injection, intravitreal injection, or intranasal infusion. Pharmacokinetics, biodistribution, and cellular uptake of AOs have been comprehensively discussed in recent reviews.57, 61, 62, 63
AOs Targeting Angiogenic Factors
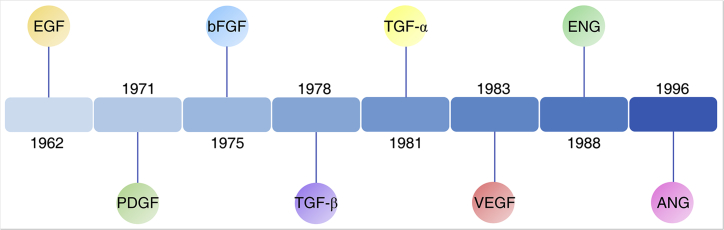
In this part, we mainly focus on AOs that target angiogenic factors as a therapeutic approach for cancer treatment, with a brief overview of each angiogenic factor, including its discovery, functions, and significance in cancer therapy. The angiogenic factors are discussed in a chronological order based on their discovery timeline (Figure 4).
Figure 4.
Discovery Timeline of Angiogenic Factors
EGF and EGF Receptors
First isolated from the submaxillary gland of the mouse by Stanley Cohen in 1962, EGF was one of the first growth factors to be discovered.64 EGF plays a crucial role in regulating cell growth, differentiation, and proliferation through the interaction with tyrosine kinase receptor ErbB family. The ErbB family includes EGF receptor (EGFR) (ErbB1/HER1), ErbB2 (HER2/neu), ErbB3 (HER3), and ErbB4 (HER4), which create a complex network of signaling pathways.65, 66 Among those, EGFR can be activated by both homodimerization and heterodimerization (transactivation) of the HER family members. This elicits the downstream activation of the signaling peptides through the phosphotyrosin-binding SH2 domains, which are diligently involved in the functioning of various cellular pathways, such as c-Jun N-terminal kinase (JNK), protein kinase B (Akt/PKB), and mitogen-activated protein kinase (MAPK) pathways. These pathways are primarily involved in the DNA synthesis and cell proliferation. Thus, aberrant EGFR signaling is believed to be involved in the pathogenesis of many human diseases, including various types of cancers. This is pivotal in cancer development and progression, as EGFR-related tumors are associated with the poor prognoses and low survival rates of patients.67 Therefore, silencing the expression of EGFR could arrest the tumor development. In fact, EGF and EGFR have now emerged as potential targets for wound-healing and cancer therapy.65, 68 It is worth noting that EGFR is recognized as the primary receptor target for developing monoclonal antibody therapies in cancer.65
Protein localization studies performed on squamous cell carcinoma of the head and neck (SCCHN) suggested increased expression of EGFR and TGF-α in SCCHN cells.69 To determine the effect of EFGR inhibition on SCCHN cell growth, AOs were directed against the translation initiation site and at the first intron-exon splice junction. As a result, the cell growth was reduced by 80%, 6 days after combined treatment with both AOs, compared to untreated cells.69 Follow-up studies showed that a combination of docetaxel and an EGFR mRNA targeting PS AO via RNase-H recruitment synergistically inhibited SCCHN cell proliferation in vitro, and it also reduced tumor volume in a xenograft mice model.70 In another study, Low and colleagues71 reported the design of AOs (AEGFR2 and AEGFR2S) targeting positions 3,811–3,825 of the EGFR cDNA for downregulation of EGFR through an RNase-H mechanism. The AOs were then encapsulated in folate-polyethylene glycol (PEG)-liposomes for delivery into cultured KB cells.71 Remarkably, the AO complex effectively reduced KB cell proliferation by 90% after 48 hr of treatment, compared to untreated cells, 5-fold more effective than the AEGFR2 AO encapsulated in a non-targeted liposome.
EGF-related peptides, such as TGF-α, amphiregulin (AR), and CRIPTO-1, also proved to be attractive targets in experimental cancer treatments. De Luca et al.72, 73 suggested that combinations of AOs targeting different growth factors might be a relevant approach for treating human colon carcinomas. In their studies, 10 AOs were designed against TGF-α, CRIPTO-1, and AR, all of which were synthesized as either full DNA or as gapmers with 2′-OMe RNA on a PS backbone. Different AO cocktails were tested in a human colon cancer GEO cell line, and the most effective showed an approximately 50% reduction of AR, CRIPTO-1, and TGF-α protein expression when transfected at a 1-μM concentration for 48 hr, compared to the untreated cells. A dose of 10 mg/kg inhibited tumor growth by 60%–65% when injected into nude mice carrying GEO xenografts, compared to those treated with the scrambled sequence control. An additive growth-inhibitory effect was observed when the AOs were combined with conventional anti-tumor drugs, such as 5-fluorouracil, adriamycin, mitomycin C, and cis-platinum in GEO cells, increasing the efficacy to 70% reduction.72 Notably, these EGF-like growth factors were also found to be overexpressed in ovarian carcinoma cells. Casamassimi et al.74 reported a reduction in anchorage-dependent growth of NIH: OVCAR3 and OVCAR8 cells when treated with AOs directed against amphiregulin, CRIPTO-1, and TGF-α.
PDGF
PDGF was first characterized as an essential serum factor for 3T3 mouse fibroblast growth in 1971.75 Studies have shown that PDGF plays pivotal roles in cell growth stimulation, cell migration, and cell activation and is involved in blood vessel formation, especially angiogenesis by promoting the vascularity of the blood vessels and inducing the maturation of the vascular wall. PDGF has been found in both normal tissue and tumor, hence it is implicated in different diseases and conditions, including wound repair, atherosclerosis, and cancer.76, 77 The inhibition of PDGF would theoretically diminish tumor development, migration, and invasion.
Structurally, PDGF is a dimeric glycoprotein composed of two distinct but related chains, termed A and B.78 Sato et al.77 revealed that PDGF-BB is capable of enhancing in vitro capillary formation through direct action on myofibroblasts in an angiogenesis model using the rat microvascular fragments and myofibroblasts. This suggests that PDGF-BB plays a trivial paracrine role in the process of angiogenesis. Additionally, PDGF also acts as an autocrine stimulatory signal in regulating cell growth. Schlingensiepen and colleagues79 investigated the effect of PDGF-AA on HTZ-19 melanoma cell proliferation. AOs targeting PDGF-A mRNA for degradation reduced cell growth in vitro by 62% when applied at a 5-μM concentration for 48 hr. In another study, Yamamoto et al.80 reported that advanced glycation end-products (AGEs) can stimulate growth of MIA PaCa-2 pancreatic cells by upregulating PDGF-B mRNA levels through interaction with the cell surface receptor for AGE (RAGE). AOs targeting RAGE mRNA reversed this process. Vascular smooth muscle cell (VSMC) proliferation has been linked to diseases such as hypertensive vascular diseases, restenosis of coronary arteries after angioplasty, and atherosclerosis. Fukuda and colleagues81 explored the use of an antisense peptide nucleic acid (PNA) to study the effect of PDGF-A chain expression on VSMC growth. A 15-mer PNA oligomer was designed complementary to a region including the initiation codon of rat and human PDGF-A-chain mRNA. Not surprisingly, DNA synthesis in VSMCs was reduced by 6-fold when the AO was transfected at 0.5 μM, compared to the control PNA oligo, suggesting that PDGF-A chain expression might regulate VSMC proliferation and can serve as a potential therapeutic target for the abovementioned diseases.
bFGF
bFGF (also known as FGF-2 or FGF-β) belongs to the FGF family of proteins and encoded by the FGF2 gene.82 Gambarini and Armelin83 first identified bFGF as an active protein in mouse pituitary extracts that can promote mouse 3T3 cell growth. The growth factors are embedded in the basement membranes and the sub-endothelial extracellular matrices of blood vessels, and they function as signaling peptides, which are broadly involved in cell survival and mitogenic activities.84 By binding to its receptor, bFGF is reported to be directly involved in angiogenesis, thereby regulating subsequent processes such as wound healing, and it is also associated with tumor development. Overexpression of bFGF is implicated with poor cancer prognosis, and anti-bFGF administration has been shown to arrest the formation of tumor. Therefore, bFGF could be a desirable target for the treatment of cancer.85, 86
Inhibition of bFGF using AOs could decrease angiogenic activity in solid cancers. Ensoli and colleagues87 reported that PS-modified AOs targeting bFGF mRNA in cells from Kaposi sarcoma lesions efficiently reduced the cell growth and associated angiogenic activity. A similar result was observed in cells derived from nude mice inoculated with AIDS-Kaposi sarcoma cells. In another study, Murphy et al.88 demonstrated that AO treatment decreased the doubling time of the U87-MG glioblastoma cell line by 2-fold and reduced the cell number to 32%, and they showed that both 23- and 25-kDa isoforms of bFGF were reduced by 64% and 73.3%, respectively, in comparison to the untreated cells. Using short 15-mer AOs targeting bFGF mRNA, Bernardini et al.89 showed a significant decrease of up to 89% in the proliferation of V9/AP4 Chinese hamster fibroblasts at a 60-μM concentration, compared to the untreated cells, indicating an important role for bFGF in cell growth and survival. In a study by Becker et al.90, three 15-mer unmodified oligodeoxynucleotides targeting the bFGF mRNA translation initiation site in human vertical phase melanoma cells, derived from melanoma WM75, showed 50%–75% inhibition in cell growth. Expression of bFGF was significantly higher in the human glioma cell line, SNB-19, which may enable neoplastic progression of gliomas.91, 92 Morrison and colleagues93 showed that an AO targeting the first donor-acceptor splice sites of the bFGF mRNA effectively reduced SNB-19 cell growth by 68%, compared to the neutralizing bFGF antibody (48%) and an antagonist (inositol hexakisphosphate) (44%).
The translation initiation factor eIF4E has been linked with increased bFGF expression in breast cancer cells.94 AO targeting of eIF4E effectively reduced tumor vascularization and metastasis, coherently associated with the loss of bFGF.95 Similarly, another study has shown that AOs directed against TGF-β abrogated the anti-proliferative effects and inhibited the induction of p21/WAF1/CIP1 by bFGF in MCF-7 breast cancer cell lines.96 bFGF was also found to contribute to the development of non-small-cell lung cancer, and the downregulation of bFGF using AOs in combination with a monoclonal antibody showed a significant reduction in cell proliferation.97 Among the growth factors, bFGF plays a critical role in angiogenesis of renal cell carcinoma. Cenni et al.98, 99 has utilized a PS-modified AO targeting bFGF mRNA in the Caki-1 renal carcinoma cell line, and they showed a significant decrease in endothelial cell migration, but not cell proliferation.
TGF-β
TGF-β belongs to a class of TGF that comprises four different isoforms, TGF-β1–4, forming the TGF-β superfamily of cytokines.100 These multifunctional peptides are involved in various processes, including proliferation, differentiation, migration, cell survival, immunosurveillance, and angiogenesis.101 First termed as sarcoma growth factors (SGFs) by de Larco and Todaro in 1978,102 TGF-β is involved in many cellular processes, such as proliferation, differentiation, and apoptosis.40, 41 In addition, the growth factors also modulate extracellular processes, such as cell invasion, immune regulation, and microenvironment modification.103 During carcinogenesis, the role of TGF-β signaling as a tumor promoter or tumor suppressor is still under debate. Luwor et al.104 suggested that the growth-regulatory effects of TGF-β in tumor development are a two-stage process: TGF-β inhibited at early stages before switching to the TGF-β-promoted stage that triggers tumor growth and invasiveness. Others suggested that TGF-β1 has positive effects on T cell proliferation and cytokine production,100 whereas suppression of TGF-β2 in glioma models has been shown to prevent immunosuppression of lymphocytes in vitro.105 TGF-β was also reported to associate with a negative regulatory mechanism in arresting tumor formation through paracrine and autocrine pathways.106, 107 Hence, the inhibition of TGF-β could diminish tumor proliferation.
Several therapeutic approaches targeting the TGF-β pathway have been proposed, including the utilization of AOs against the TGF-β mRNA, antibodies, and small molecule inhibitors of TGF-β receptors.108, 109 Wright and colleagues110 described the design and synthesis of AOs targeting TGF-β1 mRNA, and they investigated the effects in H-ras-transformed fibrosarcoma cells. At a 1-μM concentration, all AOs were able to inhibit cell proliferation and induce morphological changes in a non-specific manner. However, the AO termed AS-5-OSO, containing a mixture of PS and phosphodiester linkages, caused a 50% reduction in cell growth, in comparison with the untreated cells. Additionally, this AO also markedly reduced the invasive and metastatic effects of the fibroscarcoma cells, highlighting the importance of AO design and chemistry, with mixed linkages conferring greater specificity and lower toxicity, compared to AOs composed of only PS linkage.110
Malignant mesothelioma (MM) is an aggressive tumor that is refractory to conventional cancer treatments, due to the acquired mechanisms that augment the ability of tumor cells to survive and proliferate. Marzo et al.105 assessed the hypothesis that TGF-β contributes directly or indirectly to MM growth and tumorigenesis, using DNA AOs targeting TGF-β1 and TGF- β2 mRNA in the AC29 murine MM cell line. Following transfection, the AOs induced 50% inhibition of AC29 cell proliferation over a 4-day period. To determine the effect of the AOs in vivo, tumor-bearing CBA/CAH (H-2k) mice were injected intra-tumorally with a TGF-β2 PS AO. There was a substantial reduction in TGF-β2 mRNA within mice after 5 days of treatment with the AO, but the reduction effect was halted after 9 days of treatment.
Bogdahn and coworkers111 employed 14-mer PS AOs targeting TGF-β1 and TGF-β2 mRNA in 12 patient-derived glioma cell lines (HTZ-10, -60, -340, -70, -243, -262, -85, -119, -121, -209, -326, and -341). Of the 12 cell lines tested, TGF-β1-targeting AOs were able to reduce cell growth in 6 cell lines (HTZ-10, -85, -209, -243, -262, and -326). The TGF-β2-targeting AOs showed an inhibitory effect in all 12 cell lines, and they also reduced the amount of secreted TGF-β1 and TGF-β2 proteins, suggesting that TGF-β2 plays a major role in regulating glioma cell proliferation. Evidence also shows that an increase in TGF-β2 secretion in glioma cells can lead to an immunosuppressed state that could be responsible for the failure of various immunotherapy strategies. Lillehei and colleagues112 showed the promise of an antisense approach to overcome tumor-induced immunosuppression and enhance tumor vaccine efficiency in high-grade gliomas. Tumor-bearing rats were treated with an AO specific for TGF-β2 mRNA in combination with systemic tumor vaccine, and the survival rate was monitored. The lifespan of the treated rats was significantly increased, with a mean survival time (MST) of 48.0 days compared to vaccine alone (29 days), AO alone (37.5 days), or PBS alone (31.5 days).
The potential of AO therapeutics was also evaluated in oral squamous cell carcinoma (OSCC). Kim and Song113 designed and assessed the efficacy of an 18-mer DNA AO targeting TGF-β1 in SCC-9 cells. AO-treated SCC-9 cells showed a significant decrease in TGF-β1 expression and cell growth, compared to the untreated cells. In addition, the AO treatment reduced the tumor size in vivo by approximately 50%, and it diminished the expression of a proliferating cell nuclear antigen (PCNA) and matrix metalloproteinase (MMP2), well-established indicators of cell proliferation. The AO AP12009 (Trabedersen), developed by Antisense Pharma, targets the TGF-β2 transcripts, and it has entered phase I/II clinical trials for the treatment of high-grade glioma, pancreatic cancer, and malignant melanoma.114
TGF-α
TGF-α, initially termed EGF-potentiated TGF in 1981,115 is encoded by the TGFA gene and belongs to the family of endothelial growth factors. Despite sharing the same prefix, TGF-α is neither structurally nor genetically related to TGF-β, instead associated with the EGF pathway and acting as a ligand for EGFR to promote angiogenesis.116, 117 By binding to EGFR and initiating events for cell proliferation, TGF-α is involved in wound healing and embryogenesis and indirectly involved in angiogenesis.118 Overexpression of TGF-α has been observed in a wide range of human tumors, such as gastric cancer, breast cancer, and liver cancer, demonstrating its role in tumor formation and development.119 TGF-α also facilitates the epithelial-to-mesenchymal transition process, which is crucial for metastasis and poor progonosis.120 These observations indicate that silencing the expression of TGF-α could be a potential therapeutic approach in cancer treatment.
Sizeland and Burgess121 reported that a 23-mer DNA AO targeting the translation start site of TGF-α inhibited DNA synthesis (measured via 3H-thymidine uptake) in LIM 1215 colon cancer cells by 97% when applied at a 50-μM concentration, and it completely suppressed cell proliferation 5 days after transfection at 10 μM. Another study conducted by Grandis et al.122 showed that TGF-α also contributed to an autocrine-signaling pathway in head and neck cancer. To examine the effect of TGF-α downregulation on cell proliferation, the authors transfected SCCHN cells with a 19-mer PS DNA AO targeting TGF-α mRNA. At a 12.5-μM concentration, the AO showed higher efficacy, with 76% inhibition of SCCHN cell growth and 93% downregulation of TGF-α protein, 6 days after transfection.122 Normal mucosal epithelial cell proliferation was not affected by the AO treatment that induced an 83% reduction in TGF-α protein, suggesting an autocrine function for TGF-α in regulating malignant tumor growth.
Studies led by Rubenstein and colleagues123, 124 reported AO targeting of TGF-α in human-derived prostate tumor cells. Two gapmer AOs containing 3′ PS linkages at each end were directed against the translation initiation sites of the TGF-α and EGFR transcripts in PC-3 prostate cancer cells. The AOs showed significant inhibition of PC-3 cell growth in vitro, and they were effective in inducing hemorrhagic necrosis in PC-3 tumors in vivo in athymic nude mice. To enhance the efficacy of the AOs, Rubenstein et al.125 continued their work by designing bispecific AOs recognizing the binding sites of TGF-α and EGFR mRNA and EGFR and Bcl-2 mRNA, and they tested in both MCF-7 breast cancer cells and PC-3 prostate cancer cells. Notably, MCF-7 cells were more responsive to monospecific AOs, whereas the bispecific AOs performed better in PC-3 cells, in line with previous observations by the authors. Combination therapy involving rapamycin or paclitaxel and mono- or bispecific AOs showed improved efficacy.125
VEGF
First described in 1983 as a mitogenic soluble factor responsible for new capillary formation,126 VEGF or vascular permeability factor (VPF) has now been identified as an important signaling protein in vasculogenesis and angiogenesis. When a cell is in an oxygen-deficient state, VEGF production is stimulated through the activation of the hypoxia pathway, leading to the interaction of VEGF proteins and tyrosine kinase receptor VEGFRs available on the cell surface, inducing them to dimerize, and subsequently triggering the tyrosine kinase pathway that results in angiogenesis.127 Overexpression of VEGF is highly associated with tumor formation, as it promotes the growth of a blood vessel network surrounding the tumor.45, 128 Previous studies have observed increased VEGF circulation in different human cancers, including breast, liver, colorectal, brain, ovarian, and non-small-cell lung cancer.129 This indicates that increased vascularization induced by VEGF plays an important role in cancer pathology through tumor formation, progression, and metastasis. It is worth noting that the splicing of VEGF pre-mRNA generates several VEGF isoforms and the predominant ones are VEGF-165, VEGF-121, and VEGF-189, which are overexpressed in a wide range of cancer cell types.130 Various anti-VEGF inhibitors have been generated to target these isoforms and utilized as first- or second-line therapy in standard cancer treatment. Thus, VEGF could be a potential target toward tackling cancer.131
Gill and coworkers132 demonstrated the use of AOs to inhibit VEGF mRNA in KS. Six different cell lines, including AIDS-KS, human umbilical vein endothelial cells (HUVECs), human aortic smooth muscle (AoSM), Hut-78, 23-1 (a B lymphoma cell line), and T1 (a fibroblast cell line), were cultured and seeded into 24-well plates. The cells were then treated with five 21-mer DNA AOs containing PS linkages designed to target the human VEGF-coding region at concentrations ranging from 1 to 10 μM. The results showed that two AOs (AS-1 and AS-3) showed significant inhibition of KS cell growth in a dose-dependent manner, ranging from 53% (1 μM) to 81% (10 μM), compared to untreated cells. In contrast, the inhibitory effect was minimal for HUVEC (17%) and AoSM (26%) cells at 10 μM. The efficacy of the AOs was also confirmed with a reduction of VEGF protein by 80% in KS cells treated with AS-3 at 5 μM. To further examine AO efficacy, nude mice inoculated with KSY1 cells were injected daily with AS-1, AS-3, or a scrambled AO at 25 μg/g body weight for 5 days. After 14 days, tumors within mice treated with AS-1 and AS-3 showed 85% and 88% reductions in size, respectively, when compared with untreated mice.
Ciardiello et al.133 later explored the combination effect of AS-3 and an anti-EGFR monoclonal antibody (mAb) C225 in human GEO colon cancer cells. The group synthesized AS-3 with a PS backbone, and they treated the cells with mAb alone, AS-3 alone, or mAb and AS-3 in combination. In line with the previous report, AS-3 reduced 85% of VEGF protein expression at a 5-μM concentration. The outcome of in vivo experiments in immunodeficient mice (AS-3, 10 mg/kg/dose; and mAb C225, 0.5 mg/dose) demonstrated the synergistic effect of AS-3 and the mAb. Analysis of the tumors after 21 and 28 days of combination therapy showed 95% and 98% of VEGF protein inhibition, compared to 90% and 92% when treated with AS-3 alone and 75% and 70% when treated with mAb alone. Interestingly, 50% of the mice under combination treatment survived after 13 weeks, whereas all other groups died within 8 weeks of treatment.
Renal cell carcinoma (RCC) is a highly vascularized tumor that accounts for almost 2% of all adult malignancies.134 VEGF overexpression has been observed in Caki-1, an RCC cell line.135 Shi and Siemann136 reported the design of a 20-mer DNA AO on a PS backbone (V515) complementary to the 5′ UTR region of VEGF mRNA. Cationic liposome (prepared by mixing 1,2-dioleoyloxy-3- (trimethylammonium) propane [DOTAP] with a helper lipid 1,2-dioleoyl-3-sn-phosphatidylethanolamine [DOPE]) was used as a transfection agent to deliver V515 into Caki-1 cells. After 24 hr of treatment, VEGF levels were reduced in a dose-dependent manner, ranging from 35% to 85% at the 0.5- and 2-μM concentrations, respectively. Importantly, VEGF inhibition also affected endothelial cell growth and migration. Co-culturing of treated Caki-1 cells with either mouse heart endothelial (MHE) cells or human microvascular endothelial cell from the lung (HMVEC-L) indicated a significant decrease in both MHE (43%) and HMVEC-L (67%) cell proliferation and migration. In vivo injection with two doses of V515 (5 mg/kg) in Caki-1 xenograft-bearing mice triggered a 5.5-day delay in tumor growth, while two doses of 10 mg/kg resulted in an 8-day delay.
Exploring indirect targets toward VEGF inhibition has also offered attractive therapeutic avenues. One alternative approach is to target tyrosine kinase receptors (kinase insert domain receptor [KDR]/Flk-1 and Flt-1) to block the interaction between VEGF and its receptors. Shimada and coworkers137 studied the effect of AO on peritoneal dissemination and angiogenesis in human gastric cancer (HGC). After 5 days of AO incubation with the cells, including HUVEC, PC-3, and NUGC-4, the growth rate of all cell lines except NUGC-4 decreased to 43.6% (HUVEC) and 49.1% (PC-3), compared to untreated cells. NUGC-4 cells were not affected by the AO treatment. Notably, KDR/Flk-1 protein expression in PC-3-treated cells was reduced to 42%. Subsequently, NUGC-4 cells were transduced with GFP and implanted into BALB/c nu/nu male mice. Anti-VEGF AO was then injected intraperitonially for 8 days at 200 μg/mouse/day. After 14 days of treatment, 80% of the tumor nodules in treated mice could not be visualized by fluorescence microscopy. Tumor angiogenesis was significantly inhibited (95% compared to the untreated group), and mice showed increased tumor apoptosis (50%). Förster et al.138 also assessed the efficiency of AO targeting VEGF in MCF-7 breast cancer and EJ28 bladder cancer cell lines. The authors designed 25 AOs (20-mer) against VEGF and transfected these compounds into MCF-7 and EJ28 cell lines. Following transfection, ELISA analysis revealed 83.5% and 48.9% inhibition of VEGF protein expression in EJ28 and MCF-7 cells, respectively, with the most effective AO (VEGF723) at a 1-μM concentration. Further examination showed up to 79% inhibition of EJ28 cell proliferation was achieved with AO VEGF723 after 20 hr of treatment.
Hörmann and colleagues139 observed a significant induction of VEGF secretion from SCCHN UMSCC22b cells (approximately 3.5- and 2.75-fold above normal) upon treatment with chemotherapeutic agents, such as carboplatin (doses at 90 μg/mL) and cisplatin (2.5 μg/mL), in treated cells relative to sham control cells. The authors then designed a 21-mer PS DNA AO complementary to the translation start site of human VEGF gene, and they evaluated the AO efficacy in UMSCC22b cells treated with chemotherapeutic agents. After 48 hr of AO treatment, the VEGF level was significantly reduced by up to 4-fold compared to controls.
Treatment of unresectable hepatocellular carcinoma (HCC) is challenging, and transcatheter arterial embolization (TAE) is the accepted treatment strategy. However, the tumor cannot be treated completely, and the 3-year survival rate of patients’ stumbles at 14%–35%. There are reports on increased VEGF production in both HCC cells and non-carcinoma liver cells prior to TAE. Wu et al.140 transfected a 22-mer PS DNA AO targeting the linkage area of exons 2 and 3 of VEGF mRNA into Walker-256 carcinosarcoma cells at different concentrations (0.25, 0.5, 1.0, and 2.0 μM). At the 48-hr time point, secreted VEGF levels were found to have been decreased in a dose-dependent manner, ranging from 7% at 0.25 μM to 28% at 2.0 μM, compared to controls. For analyzing the efficacy in vivo, rats were implanted with Walker-256 cells and then treated with 0.2 mL Lipiodol (LP), LP + AO, or normal saline. Magnetic resonance (MR) scans of the LP and LP + AO groups showed a substantial reduction in growth rate in comparison to the control group.
VEGF also plays an important role in the development and metastasis of pancreatic cancer. Based on earlier reports, Hotz et al.141 transfected their AS-3 AO142 sequence, complementary to VEGF cDNA base +261–+281, into AsPC-1 and HPAF-2 pancreatic cancer cells at a concentration of 5 μM, and they examined the results 36 hr later. Western blot analysis showed a remarkable reduction in VEGF protein expression in both cell lines. Later, nude mice injected with either AsPC-1 or HPAF-2 cells were treated with AS-3 at 10 mg/kg/day intraperitoneally for 14 weeks. An 80% reduction in tumor volume was observed in HPAF-2-innoculated mice, but not in the other group. Also, metastasis ability significantly dropped in both groups, and microvessel density was recorded at a reduction by at least 50% in both groups.
To investigate the feasibility of VEGF-targeting antisense therapy in acute myeloid leukemia (AML), Ding et al.143 transfected HL-60 cells with 0.3 μM VEGF AO. A reduction in cell growth of nearly 50% was observed, in addition to enhanced chemo-sensitivity of the cells to arsenic trioxide (ATO), a traditional component of Chinese medicine.143 The synergistic effect of AO and ATO further proved its efficacy to inhibit VEGF protein production by 50% in treated cells.
ENG
ENG is a homodimeric hypoxia-inducible transmembrane glycoprotein. Initially recognized as an antigen produced against the human pre-B leukemic cell line in 1988, the peptide was named 44G4 because of its reaction with monoclonal antibody 44G4.144 Recent advances have gained more insights into its role as a membrane co-receptor for TGF-β in the endothelial cell-signaling pathway.145 Hence, ENG is closely involved in angiogenesis, and it may play an important role in tumor growth proliferation and metastasis.146 High levels of ENG are also expressed in continuously proliferating endothelial cells, such as endothelial cells involved in tissue injury and inflamed tissues, making ENG a logical target for cancer treatment.46 Different approaches targeting ENG have been proposed as therapeutic cancer treatments.
In normal placenta development, trophoblast growth and invasion are essential, and the TGF-β-signaling pathway has been identified as one of the main drivers for this process. ENG is expressed at high levels throughout pregnancy and binds to TGF-β1 and -β3 isoforms. Caniggia et al.147 used a 16-mer PS DNA AO targeting the translation initiation codon of human ENG mRNA, and they demonstrated that the AO, after transfection at 5–10 μM, promoted the outgrowth and invasiveness of extravillous trophoblasts (EVTs) in a human trophoblast villous explant culture, presumably due to ENG and TGF-β inhibition. Kumar and coworkers145 treated HUVECs with a 16-mer PS DNA AO to explore the effect of ENG on endothelial cell behavior. The results indicated that ENG protein levels were inhibited by 62% at a 0.25-μM concentration after 72 hr. Further analysis revealed that the AO-treated cells were more sensitive to TGF-β1, which reduced the growth and migration rate significantly by 38%, compared to the untreated cells. ENG was also implicated to be involved in hypoxia-initiated angiogenesis. Li et al.148 assessed the effect of a 16-mer PS DNA AO on ENG expression in human dermal microvascular endothelial cells (HDMECs). After 48 hr in normoxia, the transfected cells were exposed to a hypoxic condition for 24 hr. A significant increase (86.3%) in ENG protein levels was observed in untreated cells, but the AO-treated cells possessed a suppressed ENG protein level (55%–60%). Additionally, treated cells showed a significant increase in cell apoptosis (62%) compared to untreated cells (48.5%).
Ang Family
The Ang family consists of Ang1, Ang2, Ang3, and Ang4, and they were all discovered as VEGF-related factors.149, 150, 151 Apart from Ang3, an ortholog in mouse, the other three Ang proteins are expressed in humans and play complex roles in angiogenesis and vascular remodeling, due to their interactions with each other and the endothelium-specific tyrosine kinase receptor Tie-2.152 Ang and VEGF function closely complementing each other in the formation of blood vessels. Ang1 takes part in stabilizing the blood vessels and Ang2 functions in vascular remodeling.153 Previous reports have shown an increase in Ang activity in different tumors, which makes Ang an important target in cancer treatment (L.R. Huang et al., 2016, Mol. Cancer Res., abstract).142
To investigate the effect of Ang on endothelial cell survival, Li and colleagues154 constructed a 25-mer PS DNA AO targeting bovine Tie-2 mRNA, and they transfected this compound into cultured adult bovine aortic endothelial (ABAE) cells. At a concentration of 150 nM, the AO induced 90% cell death compared to the untreated cells. Further evaluation showed a 6-fold increase in cell apoptosis induced by AO treatment relative to control cells. Boulton and coworkers155 explored the function of the Ang-signaling system in diabetic retinopathy using the same AO reported earlier by Li et al.154 The Tie-2 AO was transfected into bovine retinal pericytes at 6 μM to evaluate its effect on cell survival and proliferation. Tie-2 inhibition reduced Ang1 expression and significantly decreased pericyte migration. These findings clearly indicated that targeted regulation of Ang isoforms could be a feasible approach in diabetic retinopathy treatment.
Clinical Trials
Additional clinical trials employing antisense and other therapeutic strategies targeting angiogenic markers, including approved drugs, are detailed in Table 1.
Table 1.
Approved Drugs and Clinical Trials Targeting Angiogenesis Factors in Cancers
| Number | Drug/Trade Name | Molecular Target | Development Stage | Drug Type | Target Tumor | Reference |
|---|---|---|---|---|---|---|
| Approved Drugs | ||||||
| 1 | aflibercept/Zaltrap | VEGF-A/B, PGF | approved drug | fusion antibody | metastatic colorectal cancer | 156 |
| 2 | apatinib/Rivoceranib | VEGFR-2 | approved drug | small molecule | late-stage gastric carcinoma | 157 |
| 3 | axitinib/Inlyta | VEGFR1, 2, 3; c-KIT; PDGFR | approved drug | small molecule | renal cell carcinoma | 158 |
| 4 | bevacizumab/Avastin | VEGF-A | approved drug | monoclonal antibody | lung cancers, renal cancers, ovarian cancers, glioblastoma multiforme | 25 |
| 5 | cabozantinib/Cabometyx | VEGFR, c-MET | approved drug | small molecule | medullary thyroid cancer, advanced renal cell carcinoma | 159 |
| 6 | cetuximab/Erbitux | EGFR | approved drug | monoclonal antibody | metastatic colorectal cancer, metastatic non-small-cell lung cancer, head and neck cancers | 160, 161 |
| 7 | erlotinib/Tarceva | EGFR | approved drug | small molecule | advanced or metastatic non-small-cell lung cancer; advanced, unresectable, or metastatic pancreatic cancer | 162, 163 |
| 8 | gefitinib/Iressa | EGFR | approved drug | small molecule | non-small-cell lung cancer | 164 |
| 9 | icotinib/Conmana | EGFR | approved drug | small molecule | non-small-cell lung cancer | 165 |
| 10 | lapatinib/Tykerb | EGFR | approved drug | small molecule | advanced or metastatic breast cancer | 166 |
| 11 | lenvatinib/Lenvima | VEGFR 1, 2, 3 | approved drug | small molecule | differentiated thyroid cancer, advanced renal cell carcinoma | 167 |
| 12 | nintedanib/Vargatef, Ofev | VEGFR, FGFR, PDGFR | approved drug | small molecule | non-small-cell lung cancer | 168 |
| 13 | osimertinib/ Tagrisso | EGFR | approved drug | small molecule | specific non-small-cell lung cancer (T790M mutation) | 169 |
| 14 | panitumumab/Vectibix | EGFR | approved drug | monoclonal antibody | colorectal cancer | 170 |
| 15 | pazopanib/Votrient | VEGFR, PDGFR, FGFR, c-KIT | approved drug | small molecule | renal cell carcinoma, soft tissue sarcoma | 171 |
| 16 | pertuzumab/Perjeta | EGFR, HER2 | approved drug | monoclonal antibody | HER2-positive metastatic breast cancer | 172 |
| 17 | ramucirumab/Cyramza | VEGFR2 | approved drug | monoclonal antibody | advanced gastric cancer, metastatic non-small-cell lung carcinoma | 173 |
| 18 | regorafenib/Stivarga | VEGFR2, TIE-2 | approved drug | small molecule | metastatic colorectal cancer, advanced gastrointestinal stromal tumors | 174 |
| 19 | sorafenib/Nexavar | VEGFR, PDGFR, Raf family kinases | approved drug | small molecule | advanced renal cell carcinoma, advanced primary liver cancer, advanced thyroid carcinoma | 175 |
| 20 | sunitinib/Sutent | VEGFR/PDGFR | approved drug | small molecule | renal cell carcinoma, progressive neuroendocrine cancerous tumors | 26 |
| 21 | temsirolimus (CCI-779) | mTOR | approved drug | small molecule | renal cell carcinoma | 176 |
| 22 | tivozanib/Fotivda | VEGFR 1, 2, 3 | approved drug | small molecule | renal cell carcinoma | 177 |
| 23 | trastuzumab/Herceptin | EGFR (HER2) | approved drug | monoclonal antibody | breast cancer | 178 |
| 24 | vandetanib/Caprelsa | VEGFR, EGFR, RET-tyrosine kinase | approved drug | small molecule | medullary thyroid cancer | 179 |
| Investigational Drugs | ||||||
| 25 | ALN-VSP02 | VEGF, KSP | investigational drug (phase I trial) | siRNA | liver cancer, liver metastases | 180, 181 |
| 26 | AP-12009 (trabedersen) | TGF-β2 | terminated (phase I/II trial) | antisense oligonucleotide | recurrent high-grade glioma, advanced pancreatic carcinoma, metastatic melanoma | 180, 181, 182 |
| 27 | AZD4547 | FGFR | investigational drug (phase II trial) | small molecule | non-small-cell lung cancer | 183, 184 |
| 28 | BB-401 | EGFR | investigational drug (phase II trial) | antisense oligonucleotide | recurrent or metastatic SCCHN | 185, 186 |
| 29 | brivanib alaninate | VEGFR, FGFR | investigational drug (phase III trial) | small molecule | hepatocellular carcinoma | 187 |
| 30 | cediranib/Recentin | VEGFR | investigational drug (phase III trial) | small molecule | advanced solid cancer, ovarian cancer | 188 |
| 31 | dovitinib | VEGFR, FGFR, PDGFR | investigational drug (phase II trial) | small molecule | gastrointestinal stromal tumor | 189 |
| 32 | fresolimumab | TGF-β1, 2, 3 | investigational drug (phase I trial) | monoclonal antibody | malignant melanoma and renal cancer | 190 |
| 33 | hVEGF26-104/RFASE | VEGF | investigational drug (phase I trial) | combined vaccine | solid tumors | M.Q. Wentink et al., 2015, Cancer Res., abstract, 191 |
| 34 | lucitanib | VEGFR 1, 2, 3; FGFR 1 and 2; PDGFR α and β | investigational drug (phase II trial) | small molecule | advanced solid cancer, metastatic breast cancer | 192, 193 |
| 35 | PF-03446962 | TGF-β receptor ALK-1 | investigational drug (phase II trial) | monoclonal antibody | malignant pleural mesothelioma | 194 |
| 36 | PTC299 | VEGF | investigational drug (phase I trial) | small molecule | metastatic breast cancer | 195 |
| 37 | rindopepimut | EGFR | investigational drug (phase III trial) | small molecule | glioblastoma | 196 |
| 38 | sevacizumab | VEGFA | investigational drug (phase Ib trial) | monoclonal antibody | colorectal cancer | 197 |
| 39 | Sym004 | EGFR | investigational drug (phase II trial) | monoclonal antibody mixture | metastatic colorectal cancer | 198 |
| 40 | TRC105 | endoglin | investigational drug (phase III trial) | monoclonal antibody + Pazopanib | advanced angiosarcoma | 199 |
| 41 | vactosertib | TGF-β receptor ALK4/ALK5 | investigational drug (phase I trial) | small molecule | multiple myeloma | B.G. Kim et al., 2017, Cancer Res., abstract |
| 42 | vatalanib | VEGFR, PDGFR, c-KIT | investigational drug (phase II trial) | small molecule | metastatic pancreatic cancer, malignant mesothelioma | 200, 201 |
| 43 | VEGF-AS/Veglin | VEGF | terminated (phase I trial) | antisense oligonucleotide | Kaposi sarcoma, mesothelioma, renal cancer | 182 |
Drugs are presented in an alphabetical order.
Conclusions
Current cancer treatment approaches using antibodies or small molecules pose several issues, such as severe toxic side effects, high dosage requirements, lack of tissue specificity, and inability to regulate pathogenic gene expression. In comparison, AOs may offer a better approach to specifically target the underlying genetic cause of the disease at the RNA level to regulate the expression of key proteins implicated in cancer pathologies, by selectively cleaving or imposing steric bulkiness to the causative gene transcripts. FDA approvals of four AO drugs, Vitravene (for cytomegalovirus retinitis), Kynamro (for familial hypercholesterolemia), Exondys51 (for DMD), and Spinraza (for spinal muscular atrophy), demonstrate the potential of the AO-based therapeutic approach. However, it should be noted that, so far, no drugs were approved for cancer treatments, although several AO drug candidates have entered different stages of clinical trials. In addition to the significant potential, AOs have unraveled some of their limitations along their developmental path. Poor cellular uptake and rapid renal clearance from the circulation are the major hurdles of AOs, which often result in frequent high dosing for achieving therapeutic efficacy. This could potentially lead to safety issues, including off-target effects, nephrotoxicity and hepatotoxicity, and thrombocytopenia. However, recent developments in the oligonucleotide backbone chemistries and new delivery platform technologies have allowed greater tissue penetration and internalization of AOs that result in significant improved intracellular targeting with less frequent dosing, all of which collectively contribute to diminish the AO toxicity.
Discovery of various angiogenic markers and their vital roles in cancer initiation, development, migration, and metastasis has opened up new horizons in cancer research with novel approaches for developing cancer therapeutics. Several angiogenic factors have served as potential targets for cancer treatment, given the number of antibodies and small molecules targeting these factors that have been approved for clinical use (Table 1). Targeting angiogenic markers using AO-based approaches may certainly be a potential approach for cancer treatment. In addition, AOs targeting potential angiogenic factors in combination with currently approved small molecule cancer drugs could be an effective way to maximize the efficacy of cancer therapy.
Author Contributions
B.T.L., P.R., T.R.K., and R.N.V. co-wrote the manuscript. R.N.V. conceived the idea. S.D.W. and S.F. provided suggestions, and all authors proofread and corrected the manuscript.
Conflicts of Interest
S.D.W. and S.F. are consultants to Sarepta Therapeutics. B.T.L., P.R., T.R.K., and R.N.V. declare no conflicts of interest.
Acknowledgments
R.N.V. greatly acknowledges financial support from the Department of Health (Merit Award), the Western Australian Government; the McCusker Charitable Foundation; and the Perron Institute for Neurological and Translational Science. B.T.L. thanks the Murdoch International Postgraduate Scholarship scheme of Murdoch University.
References
- 1.Dias N., Stein C.A. Antisense oligonucleotides: basic concepts and mechanisms. Mol. Cancer Ther. 2002;1:347–355. [PubMed] [Google Scholar]
- 2.Agrawal S., Iyer R.P. Perspectives in antisense therapeutics. Pharmacol. Ther. 1997;76:151–160. doi: 10.1016/s0163-7258(97)00108-3. [DOI] [PubMed] [Google Scholar]
- 3.Sharma H.W., Narayanan R. The therapeutic potential of antisense oligonucleotides. BioEssays. 1995;17:1055–1063. doi: 10.1002/bies.950171210. [DOI] [PubMed] [Google Scholar]
- 4.Lundin K.E., Gissberg O., Smith C.I.E. Oligonucleotide Therapies: The Past and the Present. Hum. Gene Ther. 2015;26:475–485. doi: 10.1089/hum.2015.070. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.McClorey G., Wood M.J. An overview of the clinical application of antisense oligonucleotides for RNA-targeting therapies. Curr. Opin. Pharmacol. 2015;24:52–58. doi: 10.1016/j.coph.2015.07.005. [DOI] [PubMed] [Google Scholar]
- 6.Roehr B. Fomivirsen approved for CMV retinitis. J. Int. Assoc. Physicians AIDS Care. 1998;4:14–16. [PubMed] [Google Scholar]
- 7.Wong E., Goldberg T. Mipomersen (kynamro): a novel antisense oligonucleotide inhibitor for the management of homozygous familial hypercholesterolemia. P&T. 2014;39:119–122. [PMC free article] [PubMed] [Google Scholar]
- 8.Syed Y.Y. Eteplirsen: First Global Approval. Drugs. 2016;76:1699–1704. doi: 10.1007/s40265-016-0657-1. [DOI] [PubMed] [Google Scholar]
- 9.Corey D.R. Nusinersen, an antisense oligonucleotide drug for spinal muscular atrophy. Nat. Neurosci. 2017;20:497–499. doi: 10.1038/nn.4508. [DOI] [PubMed] [Google Scholar]
- 10.Stein C.A., Castanotto D. FDA-Approved Oligonucleotide Therapies in 2017. Mol. Ther. 2017;25:1069–1075. doi: 10.1016/j.ymthe.2017.03.023. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Kontos C.D., Annex B.H. Angiogenesis. Curr. Atheroscler. Rep. 1999;1:165–171. doi: 10.1007/s11883-999-0013-y. [DOI] [PubMed] [Google Scholar]
- 12.Tonini T., Rossi F., Claudio P.P. Molecular basis of angiogenesis and cancer. Oncogene. 2003;22:6549–6556. doi: 10.1038/sj.onc.1206816. [DOI] [PubMed] [Google Scholar]
- 13.Otrock Z.K., Mahfouz R.A.R., Makarem J.A., Shamseddine A.I. Understanding the biology of angiogenesis: review of the most important molecular mechanisms. Blood Cells Mol. Dis. 2007;39:212–220. doi: 10.1016/j.bcmd.2007.04.001. [DOI] [PubMed] [Google Scholar]
- 14.Potente M., Gerhardt H., Carmeliet P. Basic and therapeutic aspects of angiogenesis. Cell. 2011;146:873–887. doi: 10.1016/j.cell.2011.08.039. [DOI] [PubMed] [Google Scholar]
- 15.Greenblatt M., Shubi P. Tumor angiogenesis: transfilter diffusion studies in the hamster by the transparent chamber technique. J. Natl. Cancer Inst. 1968;41:111–124. [PubMed] [Google Scholar]
- 16.Folkman J. Tumor angiogenesis: therapeutic implications. N. Engl. J. Med. 1971;285:1182–1186. doi: 10.1056/NEJM197111182852108. [DOI] [PubMed] [Google Scholar]
- 17.Folkman J., Merler E., Abernathy C., Williams G. Isolation of a tumor factor responsible for angiogenesis. J. Exp. Med. 1971;133:275–288. doi: 10.1084/jem.133.2.275. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Cao Y., Langer R. A review of Judah Folkman’s remarkable achievements in biomedicine. Proc. Natl. Acad. Sci. USA. 2008;105:13203–13205. doi: 10.1073/pnas.0806582105. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Vasudev N.S., Reynolds A.R. Anti-angiogenic therapy for cancer: current progress, unresolved questions and future directions. Angiogenesis. 2014;17:471–494. doi: 10.1007/s10456-014-9420-y. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.Rajabi M., Mousa S.A. The Role of Angiogenesis in Cancer Treatment. Biomedicines. 2017;5:34. doi: 10.3390/biomedicines5020034. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.Viallard C., Larrivée B. Tumor angiogenesis and vascular normalization: alternative therapeutic targets. Angiogenesis. 2017;20:409–426. doi: 10.1007/s10456-017-9562-9. [DOI] [PubMed] [Google Scholar]
- 22.Cristofaro B., Emanueli C. Possible novel targets for therapeutic angiogenesis. Curr. Opin. Pharmacol. 2009;9:102–108. doi: 10.1016/j.coph.2008.11.006. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.Tannock I.F. Conventional cancer therapy: promise broken or promise delayed? Lancet. 1998;351(Suppl 2):SII9–SII16. doi: 10.1016/s0140-6736(98)90327-0. [DOI] [PubMed] [Google Scholar]
- 24.Ferrara N., Hillan K.J., Gerber H.-P., Novotny W. Discovery and development of bevacizumab, an anti-VEGF antibody for treating cancer. Nat. Rev. Drug Discov. 2004;3:391–400. doi: 10.1038/nrd1381. [DOI] [PubMed] [Google Scholar]
- 25.Keating G.M. Bevacizumab: a review of its use in advanced cancer. Drugs. 2014;74:1891–1925. doi: 10.1007/s40265-014-0302-9. [DOI] [PubMed] [Google Scholar]
- 26.Imbulgoda A., Heng D.Y., Kollmannsberger C. Sunitinib in the treatment of advanced solid tumors. Recent Results Cancer Res. 2014;201:165–184. doi: 10.1007/978-3-642-54490-3_9. [DOI] [PubMed] [Google Scholar]
- 27.Neal J.W., Sledge G.W. Decade in review-targeted therapy: successes, toxicities and challenges in solid tumours. Nat. Rev. Clin. Oncol. 2014;11:627–628. doi: 10.1038/nrclinonc.2014.171. [DOI] [PubMed] [Google Scholar]
- 28.Nicodemus C.F. Antibody-based immunotherapy of solid cancers: progress and possibilities. Immunotherapy. 2015;7:923–939. doi: 10.2217/imt.15.57. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 29.Hoelder S., Clarke P.A., Workman P. Discovery of small molecule cancer drugs: successes, challenges and opportunities. Mol. Oncol. 2012;6:155–176. doi: 10.1016/j.molonc.2012.02.004. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 30.Dean N.M., Bennett C.F. Antisense oligonucleotide-based therapeutics for cancer. Oncogene. 2003;22:9087–9096. doi: 10.1038/sj.onc.1207231. [DOI] [PubMed] [Google Scholar]
- 31.Wan J., Bauman J.A., Graziewicz M.A., Sazani P., Kole R. Oligonucleotide therapeutics in cancer. Cancer Treat. Res. 2013;158:213–233. doi: 10.1007/978-3-642-31659-3_9. [DOI] [PubMed] [Google Scholar]
- 32.Castanotto D., Stein C.A. Antisense oligonucleotides in cancer. Curr. Opin. Oncol. 2014;26:584–589. doi: 10.1097/CCO.0000000000000127. [DOI] [PubMed] [Google Scholar]
- 33.Ribatti D., Vacca A., Presta M. The discovery of angiogenic factors: a historical review. Gen. Pharmacol. 2000;35:227–231. doi: 10.1016/s0306-3623(01)00112-4. [DOI] [PubMed] [Google Scholar]
- 34.Modjtahedi H., Dean C. The receptor for EGF and its ligands - expression, prognostic value and target for therapy in cancer (review) Int. J. Oncol. 1994;4:277–296. doi: 10.3892/ijo.4.2.277. [DOI] [PubMed] [Google Scholar]
- 35.Zeng F., Harris R.C. Epidermal growth factor, from gene organization to bedside. Semin. Cell Dev. Biol. 2014;28:2–11. doi: 10.1016/j.semcdb.2014.01.011. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 36.Papadopoulos N., Lennartsson J. The PDGF/PDGFR pathway as a drug target. Mol. Aspects Med. 2018;62:75–88. doi: 10.1016/j.mam.2017.11.007. [DOI] [PubMed] [Google Scholar]
- 37.Kazlauskas A. PDGFs and their receptors. Gene. 2017;614:1–7. doi: 10.1016/j.gene.2017.03.003. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 38.Korc M., Friesel R.E. The role of fibroblast growth factors in tumor growth. Curr. Cancer Drug Targets. 2009;9:639–651. doi: 10.2174/156800909789057006. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 39.Klagsbrun M. The fibroblast growth factor family: structural and biological properties. Prog. Growth Factor Res. 1989;1:207–235. doi: 10.1016/0955-2235(89)90012-4. [DOI] [PubMed] [Google Scholar]
- 40.Colak S., Ten Dijke P. Targeting TGF-β Signaling in Cancer. Trends Cancer. 2017;3:56–71. doi: 10.1016/j.trecan.2016.11.008. [DOI] [PubMed] [Google Scholar]
- 41.Syed V. TGF-β Signaling in Cancer. J. Cell. Biochem. 2016;117:1279–1287. doi: 10.1002/jcb.25496. [DOI] [PubMed] [Google Scholar]
- 42.Dublin E.A., Barnes D.M., Wang D.Y., King R.J., Levison D.A. TGF alpha and TGF beta expression in mammary carcinoma. J. Pathol. 1993;170:15–22. doi: 10.1002/path.1711700104. [DOI] [PubMed] [Google Scholar]
- 43.Salomon D.S., Kim N., Saeki T., Ciardiello F. Transforming growth factor-alpha: an oncodevelopmental growth factor. Cancer Cells. 1990;2:389–397. [PubMed] [Google Scholar]
- 44.Carmeliet P., Collen D. Molecular basis of angiogenesis. Role of VEGF and VE-cadherin. Ann. N Y Acad. Sci. 2000;902:249–262, discussion 262–264. doi: 10.1111/j.1749-6632.2000.tb06320.x. [DOI] [PubMed] [Google Scholar]
- 45.Matsumoto K., Ema M. Roles of VEGF-A signalling in development, regeneration, and tumours. J. Biochem. 2014;156:1–10. doi: 10.1093/jb/mvu031. [DOI] [PubMed] [Google Scholar]
- 46.Nassiri F., Cusimano M.D., Scheithauer B.W., Rotondo F., Fazio A., Yousef G.M., Syro L.V., Kovacs K., Lloyd R.V. Endoglin (CD105): a review of its role in angiogenesis and tumor diagnosis, progression and therapy. Anticancer Res. 2011;31:2283–2290. [PubMed] [Google Scholar]
- 47.Rosen L.S., Gordon M.S., Robert F., Matei D.E. Endoglin for targeted cancer treatment. Curr. Oncol. Rep. 2014;16:365. doi: 10.1007/s11912-013-0365-x. [DOI] [PubMed] [Google Scholar]
- 48.Saharinen P., Eklund L., Pulkki K., Bono P., Alitalo K. VEGF and angiopoietin signaling in tumor angiogenesis and metastasis. Trends Mol. Med. 2011;17:347–362. doi: 10.1016/j.molmed.2011.01.015. [DOI] [PubMed] [Google Scholar]
- 49.Fagiani E., Christofori G. Angiopoietins in angiogenesis. Cancer Lett. 2013;328:18–26. doi: 10.1016/j.canlet.2012.08.018. [DOI] [PubMed] [Google Scholar]
- 50.Chan J.H., Lim S., Wong W.S. Antisense oligonucleotides: from design to therapeutic application. Clin. Exp. Pharmacol. Physiol. 2006;33:533–540. doi: 10.1111/j.1440-1681.2006.04403.x. [DOI] [PubMed] [Google Scholar]
- 51.Kole R., Krainer A.R., Altman S. RNA therapeutics: beyond RNA interference and antisense oligonucleotides. Nat. Rev. Drug Discov. 2012;11:125–140. doi: 10.1038/nrd3625. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 52.Lee Y., Rio D.C. Mechanisms and Regulation of Alternative Pre-mRNA Splicing. Annu. Rev. Biochem. 2015;84:291–323. doi: 10.1146/annurev-biochem-060614-034316. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 53.Du L., Gatti R.A. Progress toward therapy with antisense-mediated splicing modulation. Curr. Opin. Mol. Ther. 2009;11:116–123. [PMC free article] [PubMed] [Google Scholar]
- 54.Arechavala-Gomeza V., Khoo B., Aartsma-Rus A. Splicing modulation therapy in the treatment of genetic diseases. Appl. Clin. Genet. 2014;7:245–252. doi: 10.2147/TACG.S71506. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 55.Kurreck J. Antisense technologies. Improvement through novel chemical modifications. Eur. J. Biochem. 2003;270:1628–1644. doi: 10.1046/j.1432-1033.2003.03555.x. [DOI] [PubMed] [Google Scholar]
- 56.Wan W.B., Seth P.P. The Medicinal Chemistry of Therapeutic Oligonucleotides. J. Med. Chem. 2016;59:9645–9667. doi: 10.1021/acs.jmedchem.6b00551. [DOI] [PubMed] [Google Scholar]
- 57.Godfrey C., Desviat L.R., Smedsrød B., Piétri-Rouxel F., Denti M.A., Disterer P., Lorain S., Nogales-Gadea G., Sardone V., Anwar R. Delivery is key: lessons learnt from developing splice-switching antisense therapies. EMBO Mol. Med. 2017;9:545–557. doi: 10.15252/emmm.201607199. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 58.Juliano R.L. The delivery of therapeutic oligonucleotides. Nucleic Acids Res. 2016;44:6518–6548. doi: 10.1093/nar/gkw236. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 59.Boisguérin P., Deshayes S., Gait M.J., O’Donovan L., Godfrey C., Betts C.A., Wood M.J., Lebleu B. Delivery of therapeutic oligonucleotides with cell penetrating peptides. Adv. Drug Deliv. Rev. 2015;87:52–67. doi: 10.1016/j.addr.2015.02.008. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 60.Ulbrich K., Hekmatara T., Herbert E., Kreuter J. Transferrin- and transferrin-receptor-antibody-modified nanoparticles enable drug delivery across the blood-brain barrier (BBB) Eur. J. Pharm. Biopharm. 2009;71:251–256. doi: 10.1016/j.ejpb.2008.08.021. [DOI] [PubMed] [Google Scholar]
- 61.Kaczmarek J.C., Kowalski P.S., Anderson D.G. Advances in the delivery of RNA therapeutics: from concept to clinical reality. Genome Med. 2017;9:60. doi: 10.1186/s13073-017-0450-0. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 62.Draghici B., Ilies M.A. Synthetic nucleic acid delivery systems: present and perspectives. J. Med. Chem. 2015;58:4091–4130. doi: 10.1021/jm500330k. [DOI] [PubMed] [Google Scholar]
- 63.Jiang L., Vader P., Schiffelers R.M. Extracellular vesicles for nucleic acid delivery: progress and prospects for safe RNA-based gene therapy. Gene Ther. 2017;24:157–166. doi: 10.1038/gt.2017.8. [DOI] [PubMed] [Google Scholar]
- 64.Cohen S. Isolation of a mouse submaxillary gland protein accelerating incisor eruption and eyelid opening in the new-born animal. J. Biol. Chem. 1962;237:1555–1562. [PubMed] [Google Scholar]
- 65.Scaltriti M., Baselga J. The epidermal growth factor receptor pathway: a model for targeted therapy. Clin. Cancer Res. 2006;12:5268–5272. doi: 10.1158/1078-0432.CCR-05-1554. [DOI] [PubMed] [Google Scholar]
- 66.Normanno N., De Luca A., Bianco C., Strizzi L., Mancino M., Maiello M.R., Carotenuto A., De Feo G., Caponigro F., Salomon D.S. Epidermal growth factor receptor (EGFR) signaling in cancer. Gene. 2006;366:2–16. doi: 10.1016/j.gene.2005.10.018. [DOI] [PubMed] [Google Scholar]
- 67.Nicholson R.I., Gee J.M., Harper M.E. EGFR and cancer prognosis. Eur. J. Cancer. 2001;37(Suppl 4):S9–S15. doi: 10.1016/s0959-8049(01)00231-3. [DOI] [PubMed] [Google Scholar]
- 68.Mendelsohn J., Baselga J. Status of epidermal growth factor receptor antagonists in the biology and treatment of cancer. J. Clin. Oncol. 2003;21:2787–2799. doi: 10.1200/JCO.2003.01.504. [DOI] [PubMed] [Google Scholar]
- 69.Rubin Grandis J., Chakraborty A., Melhem M.F., Zeng Q., Tweardy D.J. Inhibition of epidermal growth factor receptor gene expression and function decreases proliferation of head and neck squamous carcinoma but not normal mucosal epithelial cells. Oncogene. 1997;15:409–416. doi: 10.1038/sj.onc.1201188. [DOI] [PubMed] [Google Scholar]
- 70.Niwa H., Wentzel A.L., Li M., Gooding W.E., Lui V.W., Grandis J.R. Antitumor effects of epidermal growth factor receptor antisense oligonucleotides in combination with docetaxel in squamous cell carcinoma of the head and neck. Clin. Cancer Res. 2003;9:5028–5035. [PubMed] [Google Scholar]
- 71.Wang S., Lee R.J., Cauchon G., Gorenstein D.G., Low P.S. Delivery of antisense oligodeoxyribonucleotides against the human epidermal growth factor receptor into cultured KB cells with liposomes conjugated to folate via polyethylene glycol. Proc. Natl. Acad. Sci. USA. 1995;92:3318–3322. doi: 10.1073/pnas.92.8.3318. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 72.De Luca A., Arra C., D’Antonio A., Casamassimi A., Losito S., Ferraro P., Ciardiello F., Salomon D.S., Normanno N. Simultaneous blockage of different EGF-like growth factors results in efficient growth inhibition of human colon carcinoma xenografts. Oncogene. 2000;19:5863–5871. doi: 10.1038/sj.onc.1203979. [DOI] [PubMed] [Google Scholar]
- 73.De Luca A., Selvam M.P., Sandomenico C., Pepe S., Bianco A.R., Ciardiello F., Salomon D.S., Normanno N. Anti-sense oligonucleotides directed against EGF-related growth factors enhance anti-proliferative effect of conventional anti-tumor drugs in human colon-cancer cells. Int. J. Cancer. 1997;73:277–282. doi: 10.1002/(sici)1097-0215(19971009)73:2<277::aid-ijc19>3.0.co;2-c. [DOI] [PubMed] [Google Scholar]
- 74.Casamassimi A., De Luca A., Agrawal S., Stromberg K., Salomon D.S., Normanno N. EGF-related antisense oligonucleotides inhibit the proliferation of human ovarian carcinoma cells. Ann. Oncol. 2000;11:319–325. doi: 10.1023/a:1008350811639. [DOI] [PubMed] [Google Scholar]
- 75.Paul D., Lipton A., Klinger I. Serum factor requirements of normal and simian virus 40-transformed 3T3 mouse fibroplasts. Proc. Natl. Acad. Sci. USA. 1971;68:645–652. doi: 10.1073/pnas.68.3.645. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 76.Raica M., Cimpean A.M. Platelet-Derived Growth Factor (PDGF)/PDGF Receptors (PDGFR) Axis as Target for Antitumor and Antiangiogenic Therapy. Pharmaceuticals (Basel) 2010;3:572–599. doi: 10.3390/ph3030572. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 77.Sato N., Beitz J.G., Kato J., Yamamoto M., Clark J.W., Calabresi P., Raymond A., Frackelton A.R., Jr. Platelet-derived growth factor indirectly stimulates angiogenesis in vitro. Am. J. Pathol. 1993;142:1119–1130. [PMC free article] [PubMed] [Google Scholar]
- 78.Ross R., Raines E.W., Bowen-Pope D.F. The biology of platelet-derived growth factor. Cell. 1986;46:155–169. doi: 10.1016/0092-8674(86)90733-6. [DOI] [PubMed] [Google Scholar]
- 79.Behl C., Bogdahn U., Winkler J., Apfel R., Brysch W., Schlingensiepen K.H. Autoinduction of platelet derived growth factor (PDGF) A-chain mRNA expression in a human malignant melanoma cell line and growth inhibitory effects of PDGF-A-chain mRNA-specific antisense molecules. Biochem. Biophys. Res. Commun. 1993;193:744–751. doi: 10.1006/bbrc.1993.1688. [DOI] [PubMed] [Google Scholar]
- 80.Yamamoto Y., Yamagishi S., Hsu C.C., Yamamoto H. Advanced glycation endproducts-receptor interactions stimulate the growth of human pancreatic cancer cells through the induction of platelet-derived growth factor-B. Biochem. Biophys. Res. Commun. 1996;222:700–705. doi: 10.1006/bbrc.1996.0807. [DOI] [PubMed] [Google Scholar]
- 81.Fukuda N., Furuya R., Kishioka H., Suzuki R., Matsuda H., Tahira Y., Takagi H., Ikeda Y., Saito S., Matsumoto K., Kanmatsuse K. Effects of antisense peptide nucleic acid to platelet-derived growth factor A-chain on growth of vascular smooth muscle cells. J. Cardiovasc. Pharmacol. 2003;42:224–231. doi: 10.1097/00005344-200308000-00011. [DOI] [PubMed] [Google Scholar]
- 82.Kim H.S. Assignment1 of the human basic fibroblast growth factor gene FGF2 to chromosome 4 band q26 by radiation hybrid mapping. Cytogenet. Cell Genet. 1998;83:73. doi: 10.1159/000015129. [DOI] [PubMed] [Google Scholar]
- 83.Gambarini A.G., Armelin H.A. Purification and partial characterization of an acidic fibroblast growth factor from bovine pituitary. J. Biol. Chem. 1982;257:9692–9697. [PubMed] [Google Scholar]
- 84.Montesano R., Vassalli J.D., Baird A., Guillemin R., Orci L. Basic fibroblast growth factor induces angiogenesis in vitro. Proc. Natl. Acad. Sci. USA. 1986;83:7297–7301. doi: 10.1073/pnas.83.19.7297. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 85.Nguyen M., Watanabe H., Budson A.E., Richie J.P., Hayes D.F., Folkman J. Elevated levels of an angiogenic peptide, basic fibroblast growth factor, in the urine of patients with a wide spectrum of cancers. J. Natl. Cancer Inst. 1994;86:356–361. doi: 10.1093/jnci/86.5.356. [DOI] [PubMed] [Google Scholar]
- 86.Hu M., Hu Y., He J., Li B. Prognostic Value of Basic Fibroblast Growth Factor (bFGF) in Lung Cancer: A Systematic Review with Meta-Analysis. PLoS ONE. 2016;11:e0147374. doi: 10.1371/journal.pone.0147374. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 87.Ensoli B., Markham P., Kao V., Barillari G., Fiorelli V., Gendelman R., Raffeld M., Zon G., Gallo R.C. Block of AIDS-Kaposi’s sarcoma (KS) cell growth, angiogenesis, and lesion formation in nude mice by antisense oligonucleotide targeting basic fibroblast growth factor. A novel strategy for the therapy of KS. J. Clin. Invest. 1994;94:1736–1746. doi: 10.1172/JCI117521. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 88.Murphy P.R., Sato Y., Knee R.S. Phosphorothioate antisense oligonucleotides against basic fibroblast growth factor inhibit anchorage-dependent and anchorage-independent growth of a malignant glioblastoma cell line. Mol. Endocrinol. 1992;6:877–884. doi: 10.1210/mend.6.6.1323055. [DOI] [PubMed] [Google Scholar]
- 89.Bernardini N., Giannessi F., Bianchi F., Dolfi A., Lupetti M., Citti L., Danesi R., Del Tacca M. Involvement of basic fibroblast growth factor in suramin-induced inhibition of V79/AP4 fibroblast cell proliferation. Br. J. Cancer. 1993;67:1209–1216. doi: 10.1038/bjc.1993.227. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 90.Becker D., Meier C.B., Herlyn M. Proliferation of human malignant melanomas is inhibited by antisense oligodeoxynucleotides targeted against basic fibroblast growth factor. EMBO J. 1989;8:3685–3691. doi: 10.1002/j.1460-2075.1989.tb08543.x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 91.Morrison R.S., Gross J.L., Herblin W.F., Reilly T.M., LaSala P.A., Alterman R.L., Moskal J.R., Kornblith P.L., Dexter D.L. Basic fibroblast growth factor-like activity and receptors are expressed in a human glioma cell line. Cancer Res. 1990;50:2524–2529. [PubMed] [Google Scholar]
- 92.Morrison R.S., Giordano S., Yamaguchi F., Hendrickson S., Berger M.S., Palczewski K. Basic fibroblast growth factor expression is required for clonogenic growth of human glioma cells. J. Neurosci. Res. 1993;34:502–509. doi: 10.1002/jnr.490340503. [DOI] [PubMed] [Google Scholar]
- 93.Morrison R., Sherman L., Ciment G. Antisense Oligodeoxynucleotides Suppress Basic Fibroblast Growth Factor Expression in Glioma Cell Lines and Primary Cultures of Neural Crest Cells. Neuroprotocols. 1993;2:51–58. [Google Scholar]
- 94.Kerekatte V., Smiley K., Hu B., Smith A., Gelder F., De Benedetti A. The proto-oncogene/translation factor eIF4E: a survey of its expression in breast carcinomas. Int. J. Cancer. 1995;64:27–31. doi: 10.1002/ijc.2910640107. [DOI] [PubMed] [Google Scholar]
- 95.Nathan C.O., Carter P., Liu L., Li B.D., Abreo F., Tudor A., Zimmer S.G., De Benedetti A. Elevated expression of eIF4E and FGF-2 isoforms during vascularization of breast carcinomas. Oncogene. 1997;15:1087–1094. doi: 10.1038/sj.onc.1201272. [DOI] [PubMed] [Google Scholar]
- 96.Fenig E., Kanfi Y., Wang Q., Beery E., Livnat T., Wasserman L., Lilling G., Yahalom J., Wieder R., Nordenberg J. Role of transforming growth factor beta in the growth inhibition of human breast cancer cells by basic fibroblast growth factor. Breast Cancer Res. Treat. 2001;70:27–37. doi: 10.1023/a:1012522321762. [DOI] [PubMed] [Google Scholar]
- 97.Kuhn H., Köpff C., Konrad J., Riedel A., Gessner C., Wirtz H. Influence of basic fibroblast growth factor on the proliferation of non-small cell lung cancer cell lines. Lung Cancer. 2004;44:167–174. doi: 10.1016/j.lungcan.2003.11.005. [DOI] [PubMed] [Google Scholar]
- 98.Cenni E., Perut F., Zuntini M., Granchi D., Amato I., Avnet S., Brandi M.L., Giunti A., Baldini N. Inhibition of angiogenic activity of renal carcinoma by an antisense oligonucleotide targeting fibroblast growth factor-2. Anticancer Res. 2005;25(2A):1109–1113. [PubMed] [Google Scholar]
- 99.Cenni E., Perut F., Granchi D., Avnet S., Amato I., Brandi M.L., Giunti A., Baldini N. Inhibition of angiogenesis via FGF-2 blockage in primitive and bone metastatic renal cell carcinoma. Anticancer Res. 2007;27(1A):315–319. [PubMed] [Google Scholar]
- 100.Li M.O., Flavell R.A. TGF-β: a master of all T cell trades. Cell. 2008;134:392–404. doi: 10.1016/j.cell.2008.07.025. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 101.Massagué J. TGFβ signalling in context. Nat. Rev. Mol. Cell Biol. 2012;13:616–630. doi: 10.1038/nrm3434. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 102.de Larco J.E., Todaro G.J. Growth factors from murine sarcoma virus-transformed cells. Proc. Natl. Acad. Sci. USA. 1978;75:4001–4005. doi: 10.1073/pnas.75.8.4001. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 103.Massagué J. TGFbeta in Cancer. Cell. 2008;134:215–230. doi: 10.1016/j.cell.2008.07.001. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 104.Luwor R.B., Kaye A.H., Zhu H.-J. Transforming growth factor-beta (TGF-beta) and brain tumours. J. Clin. Neurosci. 2008;15:845–855. doi: 10.1016/j.jocn.2008.01.003. [DOI] [PubMed] [Google Scholar]
- 105.Marzo A.L., Fitzpatrick D.R., Robinson B.W.S., Scott B. Antisense oligonucleotides specific for transforming growth factor β2 inhibit the growth of malignant mesothelioma both in vitro and in vivo. Cancer Res. 1997;57:3200–3207. [PubMed] [Google Scholar]
- 106.Elliott R.L., Blobe G.C. Role of transforming growth factor Beta in human cancer. J. Clin. Oncol. 2005;23:2078–2093. doi: 10.1200/JCO.2005.02.047. [DOI] [PubMed] [Google Scholar]
- 107.Pasche B. Role of transforming growth factor beta in cancer. J. Cell. Physiol. 2001;186:153–168. doi: 10.1002/1097-4652(200002)186:2<153::AID-JCP1016>3.0.CO;2-J. [DOI] [PubMed] [Google Scholar]
- 108.Otten J., Bokemeyer C., Fiedler W. Tgf-Beta superfamily receptors-targets for antiangiogenic therapy? J. Oncol. 2010;2010:317068. doi: 10.1155/2010/317068. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 109.Arteaga C.L. Inhibition of TGFbeta signaling in cancer therapy. Curr. Opin. Genet. Dev. 2006;16:30–37. doi: 10.1016/j.gde.2005.12.009. [DOI] [PubMed] [Google Scholar]
- 110.Spearman M., Taylor W.R., Greenberg A.H., Wright J.A. Antisense oligodeoxyribonucleotide inhibition of TGF-β 1 gene expression and alterations in the growth and malignant properties of mouse fibrosarcoma cells. Gene. 1994;149:25–29. doi: 10.1016/0378-1119(94)90408-1. [DOI] [PubMed] [Google Scholar]
- 111.Jachimczak P., Hessdörfer B., Fabel-Schulte K., Wismeth C., Brysch W., Schlingensiepen K.H., Bauer A., Blesch A., Bogdahn U. Transforming growth factor-beta-mediated autocrine growth regulation of gliomas as detected with phosphorothioate antisense oligonucleotides. Int. J. Cancer. 1996;65:332–337. doi: 10.1002/(SICI)1097-0215(19960126)65:3<332::AID-IJC10>3.0.CO;2-C. [DOI] [PubMed] [Google Scholar]
- 112.Liu Y., Wang Q., Kleinschmidt-DeMasters B.K., Franzusoff A., Ng K.Y., Lillehei K.O. TGF-β2 inhibition augments the effect of tumor vaccine and improves the survival of animals with pre-established brain tumors. J. Neurooncol. 2007;81:149–162. doi: 10.1007/s11060-006-9222-1. [DOI] [PubMed] [Google Scholar]
- 113.Kim S.G., Song J.Y. Therapeutic targeting of oncogenic transforming growth factor-β1 signaling by antisense oligonucleotides in oral squamous cell carcinoma. Oncol. Rep. 2012;28:539–544. doi: 10.3892/or.2012.1811. [DOI] [PubMed] [Google Scholar]
- 114.Schlingensiepen K.H., Fischer-Blass B., Schmaus S., Ludwig S. Antisense therapeutics for tumor treatment: the TGF-beta2 inhibitor AP 12009 in clinical development against malignant tumors. Recent Results Cancer Res. 2008;177:137–150. doi: 10.1007/978-3-540-71279-4_16. [DOI] [PubMed] [Google Scholar]
- 115.Roberts A.B., Anzano M.A., Lamb L.C., Smith J.M., Sporn M.B. New class of transforming growth factors potentiated by epidermal growth factor: isolation from non-neoplastic tissues. Proc. Natl. Acad. Sci. USA. 1981;78:5339–5343. doi: 10.1073/pnas.78.9.5339. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 116.Massagué J. Epidermal growth factor-like transforming growth factor. I. Isolation, chemical characterization, and potentiation by other transforming factors from feline sarcoma virus-transformed rat cells. J. Biol. Chem. 1983;258:13606–13613. [PubMed] [Google Scholar]
- 117.Massagué J. Epidermal growth factor-like transforming growth factor. II. Interaction with epidermal growth factor receptors in human placenta membranes and A431 cells. J. Biol. Chem. 1983;258:13614–13620. [PubMed] [Google Scholar]
- 118.McInnes C., Wang J., Al Moustafa A.E., Yansouni C., O’Connor-McCourt M., Sykes B.D. Structure-based minimization of transforming growth factor-alpha (TGF-alpha) through NMR analysis of the receptor-bound ligand. Design, solution structure, and activity of TGF-alpha 8-50. J. Biol. Chem. 1998;273:27357–27363. doi: 10.1074/jbc.273.42.27357. [DOI] [PubMed] [Google Scholar]
- 119.Yeh J., Yeh Y.C. Transforming growth factor-alpha and human cancer. Biomed. Pharmacother. 1989;43:651–659. doi: 10.1016/0753-3322(89)90083-8. [DOI] [PubMed] [Google Scholar]
- 120.Fanelli M.F., Chinen L.T., Begnami M.D., Costa W.L., Jr., Fregnami J.H., Soares F.A., Montagnini A.L. The influence of transforming growth factor-α, cyclooxygenase-2, matrix metalloproteinase (MMP)-7, MMP-9 and CXCR4 proteins involved in epithelial-mesenchymal transition on overall survival of patients with gastric cancer. Histopathology. 2012;61:153–161. doi: 10.1111/j.1365-2559.2011.04139.x. [DOI] [PubMed] [Google Scholar]
- 121.Sizeland A.M., Burgess A.W. Anti-sense transforming growth factor alpha oligonucleotides inhibit autocrine stimulated proliferation of a colon carcinoma cell line. Mol. Biol. Cell. 1992;3:1235–1243. doi: 10.1091/mbc.3.11.1235. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 122.Grandis J.R., Chakraborty A., Zeng Q., Melhem M.F., Tweardy D.J. Downmodulation of TGF-α protein expression with antisense oligonucleotides inhibits proliferation of head and neck squamous carcinoma but not normal mucosal epithelial cells. J. Cell. Biochem. 1998;69:55–62. [PubMed] [Google Scholar]
- 123.Rubenstein M., Mirochnik Y., Chou P., Guinan P. Antisense oligonucleotide intralesional therapy for human PC-3 prostate tumors carried in athymic nude mice. J. Surg. Oncol. 1996;62:194–200. doi: 10.1002/(SICI)1096-9098(199607)62:3<194::AID-JSO9>3.0.CO;2-2. [DOI] [PubMed] [Google Scholar]
- 124.Rubenstein M., Mirochnik Y., Chou P., Guinan P. Growth factor deprivation therapy of hormone insensitive prostate and breast cancers utilizing antisense oligonucleotides. Methods Find. Exp. Clin. Pharmacol. 1998;20:825–831. doi: 10.1358/mf.1998.20.10.487534. [DOI] [PubMed] [Google Scholar]
- 125.Rubenstein M., Tsui P., Guinan P. Multigene targeting of signal transduction pathways for the treatment of breast and prostate tumors: comparison between combination therapies employing bispecific oligonucleotides with either Rapamycin or Paclitaxel. Med. Oncol. 2009;26:124–130. doi: 10.1007/s12032-008-9088-5. [DOI] [PubMed] [Google Scholar]
- 126.Senger D.R., Galli S.J., Dvorak A.M., Perruzzi C.A., Harvey V.S., Dvorak H.F. Tumor cells secrete a vascular permeability factor that promotes accumulation of ascites fluid. Science. 1983;219:983–985. doi: 10.1126/science.6823562. [DOI] [PubMed] [Google Scholar]
- 127.Ramakrishnan S., Anand V., Roy S. Vascular endothelial growth factor signaling in hypoxia and inflammation. J. Neuroimmune Pharmacol. 2014;9:142–160. doi: 10.1007/s11481-014-9531-7. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 128.Carmeliet P. VEGF as a key mediator of angiogenesis in cancer. Oncology. 2005;69(Suppl 3):4–10. doi: 10.1159/000088478. [DOI] [PubMed] [Google Scholar]
- 129.Goel H.L., Mercurio A.M. VEGF targets the tumour cell. Nat. Rev. Cancer. 2013;13:871–882. doi: 10.1038/nrc3627. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 130.Harper S.J., Bates D.O. VEGF-A splicing: the key to anti-angiogenic therapeutics? Nat. Rev. Cancer. 2008;8:880–887. doi: 10.1038/nrc2505. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 131.Niu G., Chen X. Vascular endothelial growth factor as an anti-angiogenic target for cancer therapy. Curr. Drug Targets. 2010;11:1000–1017. doi: 10.2174/138945010791591395. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 132.Masood R., Cai J., Zheng T., Smith D.L., Naidu Y., Gill P.S. Vascular endothelial growth factor/vascular permeability factor is an autocrine growth factor for AIDS-Kaposi sarcoma. Proc. Natl. Acad. Sci. USA. 1997;94:979–984. doi: 10.1073/pnas.94.3.979. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 133.Ciardiello F., Bianco R., Damiano V., Fontanini G., Caputo R., Pomatico G., De Placido S., Bianco A.R., Mendelsohn J., Tortora G. Antiangiogenic and antitumor activity of anti-epidermal growth factor receptor C225 monoclonal antibody in combination with vascular endothelial growth factor antisense oligonucleotide in human GEO colon cancer cells. Clin. Cancer Res. 2000;6:3739–3747. [PubMed] [Google Scholar]
- 134.McLaughlin J.K., Lipworth L., Tarone R.E. Epidemiologic aspects of renal cell carcinoma. Semin. Oncol. 2006;33:527–533. doi: 10.1053/j.seminoncol.2006.06.010. [DOI] [PubMed] [Google Scholar]
- 135.Paradis V., Lagha N.B., Zeimoura L., Blanchet P., Eschwege P., Ba N., Benoît G., Jardin A., Bedossa P. Expression of vascular endothelial growth factor in renal cell carcinomas. Virchows Arch. 2000;436:351–356. doi: 10.1007/s004280050458. [DOI] [PubMed] [Google Scholar]
- 136.Shi W., Siemann D.W. Inhibition of renal cell carcinoma angiogenesis and growth by antisense oligonucleotides targeting vascular endothelial growth factor. Br. J. Cancer. 2002;87:119–126. doi: 10.1038/sj.bjc.6600416. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 137.Kamiyama M., Ichikawa Y., Ishikawa T., Chishima T., Hasegawa S., Hamaguchi Y., Nagashima Y., Miyagi Y., Mitsuhashi M., Hyndman D. VEGF receptor antisense therapy inhibits angiogenesis and peritoneal dissemination of human gastric cancer in nude mice. Cancer Gene Ther. 2002;9:197–201. doi: 10.1038/sj.cgt.7700428. [DOI] [PubMed] [Google Scholar]
- 138.Förster Y., Meye A., Krause S., Schwenzer B. Antisense-mediated VEGF suppression in bladder and breast cancer cells. Cancer Lett. 2004;212:95–103. doi: 10.1016/j.canlet.2004.02.020. [DOI] [PubMed] [Google Scholar]
- 139.Riedel F., Götte K., Goessler U., Sadick H., Hörmann K. Targeting chemotherapy-induced VEGF up-regulation by VEGF antisense oligonucleotides in HNSCC cell lines. Anticancer Res. 2004;24:2179–2183. [PubMed] [Google Scholar]
- 140.Wu H.-P., Feng G.-S., Liang H.-M., Zheng C.-S., Li X. Vascular endothelial growth factor antisense oligodeoxynucleotides with lipiodol in arterial embolization of liver cancer in rats. World J. Gastroenterol. 2004;10:813–818. doi: 10.3748/wjg.v10.i6.813. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 141.Hotz H.G., Hines O.J., Masood R., Hotz B., Foitzik T., Buhr H.J., Gill P.S., Reber H.A. VEGF antisense therapy inhibits tumor growth and improves survival in experimental pancreatic cancer. Surgery. 2005;137:192–199. doi: 10.1016/j.surg.2004.07.015. [DOI] [PubMed] [Google Scholar]
- 142.Etoh T., Inoue H., Tanaka S., Barnard G.F., Kitano S., Mori M. Angiopoietin-2 is related to tumor angiogenesis in gastric carcinoma: possible in vivo regulation via induction of proteases. Cancer Res. 2001;61:2145–2153. [PubMed] [Google Scholar]
- 143.Ding Y., Zhu X., Li Y., Fei J., Zhang Y. Targeted inhibition of VEGF-modulated survival and arsenic sensitivity in acute myeloid leukemia (AML) Hematology. 2012;17:157–162. doi: 10.1179/102453312X13376952196458. [DOI] [PubMed] [Google Scholar]
- 144.Gougos A., Letarte M. Identification of a human endothelial cell antigen with monoclonal antibody 44G4 produced against a pre-B leukemic cell line. J. Immunol. 1988;141:1925–1933. [PubMed] [Google Scholar]
- 145.Warrington K., Hillarby M.C., Li C., Letarte M., Kumar S. Functional role of CD105 in TGF-beta1 signalling in murine and human endothelial cells. Anticancer Res. 2005;25(3B):1851–1864. [PubMed] [Google Scholar]
- 146.Seon B.K., Haba A., Matsuno F., Takahashi N., Tsujie M., She X., Harada N., Uneda S., Tsujie T., Toi H. Endoglin-targeted cancer therapy. Curr. Drug Deliv. 2011;8:135–143. doi: 10.2174/156720111793663570. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 147.Caniggia I., Taylor C.V., Ritchie J.W., Lye S.J., Letarte M. Endoglin regulates trophoblast differentiation along the invasive pathway in human placental villous explants. Endocrinology. 1997;138:4977–4988. doi: 10.1210/endo.138.11.5475. [DOI] [PubMed] [Google Scholar]
- 148.Li C., Hampson I.N., Hampson L., Kumar P., Bernabeu C., Kumar S. CD105 antagonizes the inhibitory signaling of transforming growth factor beta1 on human vascular endothelial cells. FASEB J. 2000;14:55–64. doi: 10.1096/fasebj.14.1.55. [DOI] [PubMed] [Google Scholar]
- 149.Davis S., Aldrich T.H., Jones P.F., Acheson A., Compton D.L., Jain V., Ryan T.E., Bruno J., Radziejewski C., Maisonpierre P.C., Yancopoulos G.D. Isolation of angiopoietin-1, a ligand for the TIE2 receptor, by secretion-trap expression cloning. Cell. 1996;87:1161–1169. doi: 10.1016/s0092-8674(00)81812-7. [DOI] [PubMed] [Google Scholar]
- 150.Maisonpierre P.C., Suri C., Jones P.F., Bartunkova S., Wiegand S.J., Radziejewski C., Compton D., McClain J., Aldrich T.H., Papadopoulos N. Angiopoietin-2, a natural antagonist for Tie2 that disrupts in vivo angiogenesis. Science. 1997;277:55–60. doi: 10.1126/science.277.5322.55. [DOI] [PubMed] [Google Scholar]
- 151.Valenzuela D.M., Griffiths J.A., Rojas J., Aldrich T.H., Jones P.F., Zhou H., McClain J., Copeland N.G., Gilbert D.J., Jenkins N.A. Angiopoietins 3 and 4: diverging gene counterparts in mice and humans. Proc. Natl. Acad. Sci. USA. 1999;96:1904–1909. doi: 10.1073/pnas.96.5.1904. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 152.Peters K.G. Vascular endothelial growth factor and the angiopoietins: working together to build a better blood vessel. Circ. Res. 1998;83:342–343. doi: 10.1161/01.res.83.3.342. [DOI] [PubMed] [Google Scholar]
- 153.Conway E.M., Collen D., Carmeliet P. Molecular mechanisms of blood vessel growth. Cardiovasc. Res. 2001;49:507–521. doi: 10.1016/s0008-6363(00)00281-9. [DOI] [PubMed] [Google Scholar]
- 154.Hayes A.J., Huang W.Q., Mallah J., Yang D., Lippman M.E., Li L.Y. Angiopoietin-1 and its receptor Tie-2 participate in the regulation of capillary-like tubule formation and survival of endothelial cells. Microvasc. Res. 1999;58:224–237. doi: 10.1006/mvre.1999.2179. [DOI] [PubMed] [Google Scholar]
- 155.Cai J., Kehoe O., Smith G.M., Hykin P., Boulton M.E. The angiopoietin/Tie-2 system regulates pericyte survival and recruitment in diabetic retinopathy. Invest. Ophthalmol. Vis. Sci. 2008;49:2163–2171. doi: 10.1167/iovs.07-1206. [DOI] [PubMed] [Google Scholar]
- 156.Ricci V., Ronzoni M., Fabozzi T. Aflibercept a new target therapy in cancer treatment: a review. Crit. Rev. Oncol. Hematol. 2015;96:569–576. doi: 10.1016/j.critrevonc.2015.07.001. [DOI] [PubMed] [Google Scholar]
- 157.Zhang H. Apatinib for molecular targeted therapy in tumor. Drug Des. Devel. Ther. 2015;9:6075–6081. doi: 10.2147/DDDT.S97235. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 158.Keating G.M. Axitinib: a review in advanced renal cell carcinoma. Drugs. 2015;75:1903–1913. doi: 10.1007/s40265-015-0483-x. [DOI] [PubMed] [Google Scholar]
- 159.Escudier B., Powles T., Motzer R.J., Olencki T., Arén Frontera O., Oudard S., Rolland F., Tomczak P., Castellano D., Appleman L.J. Cabozantinib, a New Standard of Care for Patients With Advanced Renal Cell Carcinoma and Bone Metastases? Subgroup Analysis of the METEOR Trial. J. Clin. Oncol. 2018;36:765–772. doi: 10.1200/JCO.2017.74.7352. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 160.Li X.X., Liang L., Huang L.Y., Cai S.J. Standard chemotherapy with cetuximab for treatment of colorectal cancer. World J. Gastroenterol. 2015;21:7022–7035. doi: 10.3748/wjg.v21.i22.7022. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 161.Kabolizadeh P., Kubicek G.J., Heron D.E., Ferris R.L., Gibson M.K. The role of cetuximab in the management of head and neck cancers. Expert Opin. Biol. Ther. 2012;12:517–528. doi: 10.1517/14712598.2012.667397. [DOI] [PubMed] [Google Scholar]
- 162.Landi L., Cappuzzo F. Experience with erlotinib in the treatment of non-small cell lung cancer. Ther. Adv. Respir. Dis. 2015;9:146–163. doi: 10.1177/1753465815588053. [DOI] [PubMed] [Google Scholar]
- 163.Wang J.P., Wu C.Y., Yeh Y.C., Shyr Y.M., Wu Y.Y., Kuo C.Y., Hung Y.P., Chen M.H., Lee W.P., Luo J.C. Erlotinib is effective in pancreatic cancer with epidermal growth factor receptor mutations: a randomized, open-label, prospective trial. Oncotarget. 2015;6:18162–18173. doi: 10.18632/oncotarget.4216. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 164.Dhillon S. Gefitinib: a review of its use in adults with advanced non-small cell lung cancer. Target. Oncol. 2015;10:153–170. doi: 10.1007/s11523-015-0358-9. [DOI] [PubMed] [Google Scholar]
- 165.Tan F., Shi Y., Wang Y., Ding L., Yuan X., Sun Y. Icotinib, a selective EGF receptor tyrosine kinase inhibitor, for the treatment of non-small-cell lung cancer. Future Oncol. 2015;11:385–397. doi: 10.2217/fon.14.249. [DOI] [PubMed] [Google Scholar]
- 166.Opdam F.L., Guchelaar H.J., Beijnen J.H., Schellens J.H.M. Lapatinib for advanced or metastatic breast cancer. Oncologist. 2012;17:536–542. doi: 10.1634/theoncologist.2011-0461. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 167.Cabanillas M.E., Habra M.A. Lenvatinib: Role in thyroid cancer and other solid tumors. Cancer Treat. Rev. 2016;42:47–55. doi: 10.1016/j.ctrv.2015.11.003. [DOI] [PubMed] [Google Scholar]
- 168.Roth G.J., Binder R., Colbatzky F., Dallinger C., Schlenker-Herceg R., Hilberg F., Wollin S.L., Kaiser R. Nintedanib: from discovery to the clinic. J. Med. Chem. 2015;58:1053–1063. doi: 10.1021/jm501562a. [DOI] [PubMed] [Google Scholar]
- 169.Soria J.C., Ohe Y., Vansteenkiste J., Reungwetwattana T., Chewaskulyong B., Lee K.H., Dechaphunkul A., Imamura F., Nogami N., Kurata T., FLAURA Investigators Osimertinib in Untreated EGFR-Mutated Advanced Non-Small-Cell Lung Cancer. N. Engl. J. Med. 2018;378:113–125. doi: 10.1056/NEJMoa1713137. [DOI] [PubMed] [Google Scholar]
- 170.Battaglin F., Dadduzio V., Bergamo F., Manai C., Schirripa M., Lonardi S., Zagonel V., Loupakis F. Anti-EGFR monoclonal antibody panitumumab for the treatment of patients with metastatic colorectal cancer: an overview of current practice and future perspectives. Expert Opin. Biol. Ther. 2017;17:1297–1308. doi: 10.1080/14712598.2017.1356815. [DOI] [PubMed] [Google Scholar]
- 171.van Geel R.M., Beijnen J.H., Schellens J.H. Concise drug review: pazopanib and axitinib. Oncologist. 2012;17:1081–1089. doi: 10.1634/theoncologist.2012-0055. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 172.Swain S.M., Baselga J., Kim S.B., Ro J., Semiglazov V., Campone M., Ciruelos E., Ferrero J.M., Schneeweiss A., Heeson S., CLEOPATRA Study Group Pertuzumab, trastuzumab, and docetaxel in HER2-positive metastatic breast cancer. N. Engl. J. Med. 2015;372:724–734. doi: 10.1056/NEJMoa1413513. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 173.Greig S.L., Keating G.M. Ramucirumab: A Review in Advanced Gastric Cancer. BioDrugs. 2015;29:341–351. doi: 10.1007/s40259-015-0138-1. [DOI] [PubMed] [Google Scholar]
- 174.Ettrich T.J., Seufferlein T. Regorafenib. Recent Results Cancer Res. 2014;201:185–196. doi: 10.1007/978-3-642-54490-3_10. [DOI] [PubMed] [Google Scholar]
- 175.Gadaleta-Caldarola G., Infusino S., Divella R., Ferraro E., Mazzocca A., De Rose F., Filippelli G., Abbate I., Brandi M. Sorafenib: 10 years after the first pivotal trial. Future Oncol. 2015;11:1863–1880. doi: 10.2217/fon.15.85. [DOI] [PubMed] [Google Scholar]
- 176.Schulze M., Stock C., Zaccagnini M., Teber D., Rassweiler J.J. Temsirolimus. Recent Results Cancer Res. 2014;201:393–403. doi: 10.1007/978-3-642-54490-3_24. [DOI] [PubMed] [Google Scholar]
- 177.Jamil M.O., Hathaway A., Mehta A. Tivozanib: status of development. Curr. Oncol. Rep. 2015;17:24. doi: 10.1007/s11912-015-0451-3. [DOI] [PubMed] [Google Scholar]
- 178.Maximiano S., Magalhães P., Guerreiro M.P., Morgado M. Trastuzumab in the Treatment of Breast Cancer. BioDrugs. 2016;30:75–86. doi: 10.1007/s40259-016-0162-9. [DOI] [PubMed] [Google Scholar]
- 179.Fallahi P., Di Bari F., Ferrari S.M., Spisni R., Materazzi G., Miccoli P., Benvenga S., Antonelli A. Selective use of vandetanib in the treatment of thyroid cancer. Drug Des. Devel. Ther. 2015;9:3459–3470. doi: 10.2147/DDDT.S72495. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 180.Chakraborty C., Sharma A.R., Sharma G., Doss C.G.P., Lee S.S. Therapeutic miRNA and siRNA: Moving from Bench to Clinic as Next Generation Medicine. Mol. Ther. Nucleic Acids. 2017;8:132–143. doi: 10.1016/j.omtn.2017.06.005. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 181.Ozcan G., Ozpolat B., Coleman R.L., Sood A.K., Lopez-Berestein G. Preclinical and clinical development of siRNA-based therapeutics. Adv. Drug Deliv. Rev. 2015;87:108–119. doi: 10.1016/j.addr.2015.01.007. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 182.Sharma V.K., Sharmab R.K., Singh S.K. Antisense oligonucleotides: modifications and clinical trials. MedChemComm. 2014;5:1454–1471. [Google Scholar]
- 183.Aggarwal C., Redman M.W., Lara P., Borghaei H., Hoffman P.C., Bradley J.D., Griffin K., Miao J., Mack P.C., Papadimitrakopoulou V. Phase II study of the FGFR inhibitor AZD4547 in previously treated patients with FGF pathway-activated stage IV squamous cell lung cancer (SqNSCLC): LUNG-MAP sub-study SWOG S1400D. J. Clin. Oncol. 2017;35:9055. [Google Scholar]
- 184.Katoh M. FGFR inhibitors: Effects on cancer cells, tumor microenvironment and whole-body homeostasis (Review) Int. J. Mol. Med. 2016;38:3–15. doi: 10.3892/ijmm.2016.2620. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 185.A study of BB-401 in recurrent or metastatic head and neck squamous cell carcinoma. https://clinicaltrials.gov/ct2/show/NCT03433027.
- 186.Benitec starts phase II trial of BB-401 for HNSCC. https://www.drugdevelopment-technology.com/news/benitec-starts-phase-ii-trial-bb-401-hnscc/.
- 187.Diaz-Padilla I., Siu L.L. Brivanib alaninate for cancer. Expert Opin. Investig. Drugs. 2011;20:577–586. doi: 10.1517/13543784.2011.565329. [DOI] [PubMed] [Google Scholar]
- 188.Ledermann J.A., Embleton A.C., Raja F., Perren T.J., Jayson G.C., Rustin G.J.S., Kaye S.B., Hirte H., Eisenhauer E., Vaughan M., ICON6 collaborators Cediranib in patients with relapsed platinum-sensitive ovarian cancer (ICON6): a randomised, double-blind, placebo-controlled phase 3 trial. Lancet. 2016;387:1066–1074. doi: 10.1016/S0140-6736(15)01167-8. [DOI] [PubMed] [Google Scholar]
- 189.Joensuu H., Blay J.Y., Comandone A., Martin-Broto J., Fumagalli E., Grignani G., Del Muro X.G., Adenis A., Valverde C., Pousa A.L. Dovitinib in patients with gastrointestinal stromal tumour refractory and/or intolerant to imatinib. Br. J. Cancer. 2017;117:1278–1285. doi: 10.1038/bjc.2017.290. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 190.Morris J.C., Tan A.R., Olencki T.E., Shapiro G.I., Dezube B.J., Reiss M., Hsu F.J., Berzofsky J.A., Lawrence D.P. Phase I study of GC1008 (fresolimumab): a human anti-transforming growth factor-beta (TGFβ) monoclonal antibody in patients with advanced malignant melanoma or renal cell carcinoma. PLoS ONE. 2014;9:e90353. doi: 10.1371/journal.pone.0090353. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 191.Wentink M.Q., Hackeng T.M., Tabruyn S.P., Puijk W.C., Schwamborn K., Altschuh D., Meloen R.H., Schuurman T., Griffioen A.W., Timmerman P. Targeted vaccination against the bevacizumab binding site on VEGF using 3D-structured peptides elicits efficient antitumor activity. Proc. Natl. Acad. Sci. USA. 2016;113:12532–12537. doi: 10.1073/pnas.1610258113. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 192.Soria J.C., DeBraud F., Bahleda R., Adamo B., Andre F., Dienstmann R., Delmonte A., Cereda R., Isaacson J., Litten J. Phase I/IIa study evaluating the safety, efficacy, pharmacokinetics, and pharmacodynamics of lucitanib in advanced solid tumors. Ann. Oncol. 2014;25:2244–2251. doi: 10.1093/annonc/mdu390. [DOI] [PubMed] [Google Scholar]
- 193.Guffanti F., Chilà R., Bello E., Zucchetti M., Zangarini M., Ceriani L., Ferrari M., Lupi M., Jacquet-Bescond A., Burbridge M.F. In Vitro and In Vivo Activity of Lucitanib in FGFR1/2 Amplified or Mutated Cancer Models. Neoplasia. 2017;19:35–42. doi: 10.1016/j.neo.2016.11.008. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 194.Wheatley-Price P., Chu Q., Bonomi M., Seely J., Gupta A., Goss G., Hilton J., Feld R., Lee C.W., Goffin J.R. A Phase II Study of PF-03446962 in Patients with Advanced Malignant Pleural Mesothelioma. CCTG Trial IND.207. J. Thorac. Oncol. 2016;11:2018–2021. doi: 10.1016/j.jtho.2016.06.024. [DOI] [PubMed] [Google Scholar]
- 195.Weetall M., Davis T., Elfring G., Northcutt V., Cao L., Moon Y.C., Riebling P., Dali M., Hirawat S., Babiak J. Phase 1 Study of Safety, Tolerability, and Pharmacokinetics of PTC299, an Inhibitor of Stress-Regulated Protein Translation. Clin. Pharmacol. Drug Dev. 2016;5:296–305. doi: 10.1002/cpdd.240. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 196.Weller M., Butowski N., Tran D.D., Recht L.D., Lim M., Hirte H., Ashby L., Mechtler L., Goldlust S.A., Iwamoto F., ACT IV trial investigators Rindopepimut with temozolomide for patients with newly diagnosed, EGFRvIII-expressing glioblastoma (ACT IV): a randomised, double-blind, international phase 3 trial. Lancet Oncol. 2017;18:1373–1385. doi: 10.1016/S1470-2045(17)30517-X. [DOI] [PubMed] [Google Scholar]
- 197.Tampellini M., Sonetto C., Scagliotti G.V. Novel anti-angiogenic therapeutic strategies in colorectal cancer. Expert Opin. Investig. Drugs. 2016;25:507–520. doi: 10.1517/13543784.2016.1161754. [DOI] [PubMed] [Google Scholar]
- 198.Montagut C., Argilés G., Ciardiello F., Poulsen T.T., Dienstmann R., Kragh M., Kopetz S., Lindsted T., Ding C., Vidal J. Efficacy of Sym004 in Patients With Metastatic Colorectal Cancer With Acquired Resistance to Anti-EGFR Therapy and Molecularly Selected by Circulating Tumor DNA Analyses: A Phase 2 Randomized Clinical Trial. JAMA Oncol. 2018;4:e175245. doi: 10.1001/jamaoncol.2017.5245. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 199.Jones R.L., Attia S., Mehta C.R., Liu L., Sankhala K.K., Robinson S.I., Ravi V., Penel N., Stacchiotti S., Tap W.D. Tappas: An adaptive enrichment phase 3 trial of TRC105 and pazopanib versus pazopanib alone in patients with advanced angiosarcoma (AAS) J. Clin. Oncol. 2017;35:TPS11081. [Google Scholar]
- 200.Jahan T., Gu L., Kratzke R., Dudek A., Otterson G.A., Wang X., Green M., Vokes E.E., Kindler H.L. Vatalanib in malignant mesothelioma: a phase II trial by the Cancer and Leukemia Group B (CALGB 30107) Lung Cancer. 2012;76:393–396. doi: 10.1016/j.lungcan.2011.11.014. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 201.Dragovich T., Laheru D., Dayyani F., Bolejack V., Smith L., Seng J., Burris H., Rosen P., Hidalgo M., Ritch P. Phase II trial of vatalanib in patients with advanced or metastatic pancreatic adenocarcinoma after first-line gemcitabine therapy (PCRT O4-001) Cancer Chemother. Pharmacol. 2014;74:379–387. doi: 10.1007/s00280-014-2499-4. [DOI] [PMC free article] [PubMed] [Google Scholar]