Abstract
This study examined the effects of instrument-assisted soft tissue mobilization (IASTM) on ankle range of motion in college athletes. Twenty-five Division II college athletes (18–24 yrs) were randomly selected into two groups: experimental group (n = 11) and control group (n = 14). Baseline measurements for both groups included an initial squat assessment, which measured ankle dorsiflexion during the movement, followed by IASTM with ankle rehabilitation exercises, and a secondary squat assessment. During the following week, the experimental group participated in an additional IASTM with rehabilitation session and squat test, while the control group performed a squat test with no treatment. Finally, both groups performed a final squat assessment during the third week after no IASTM treatment. Angle of the ankle during the deepest part of the squat was measured for all four testing sessions for both groups. On average, the ankle angle significantly decreased from the third session to maintenance session. However, post-hoc analyses revealed that a significant decrease in ankle angle was measured from the third session to the maintenance session in the experimental group only. The decrease in ankle angle in the experimental group shows that IASTM increased range of motion by allowing more dorsiflexion during the deepest part of the squat with greatest gains in range of motion found over time during the maintenance period. Thus, IASTM may be used as a performance enhancing tool that has the potential to temporarily increase range of motion and flexibility in college athletes.
Keywords: Fascia, tissue extensibility, tissue tension, facial adhesion
INTRODUCTION
It is common knowledge that adequate range of motion within joints is a requirement to produce functional movements in activities of daily living. In athletes, optimal range of motion is necessary after any injury because it allows for correct biomechanical movement patterns. To achieve full weight bearing range of motion, the connective tissues that surround the joint must have the appropriate amount of flexibility. There are different factors that affect flexibility such as age, fatigue, fitness and the influence of prior warm-up (18). Flexibility training is considered an integral portion of any athletes’ training program, which will allow for reliable movement patterns during activity and can be used in injury prevention programs (1).
Injuries to the lower extremity are common occurrences in sports with ankle sprains among the top injuries reported from 2005–2014 in high school sports (17). According to Roos and colleagues, approximately 70% of all overuse injuries reported to the National Collegiate Athletic Association’s Injury Surveillance System (NCAA ISS) occur in the lower extremity for collegiate athletes (20). The knee and lower leg injuries are among the highest distribution of injured sites. A systematic review evaluating the prediction of ankle sprains suggested that individuals with inflexible ankles were almost five times more at risk to sprain their ankle than those individuals with average flexibility as defined by range of motion measurements taken in weight bearing (6). Because lower extremity injuries and ankle sprains are among the top injuries reported for athletes in both high school and collegiate athletes, it is important for clinicians to identify techniques and interventions that may help to prevent these types of injuries.
Injured musculature or ligaments naturally undergo tissue healing after an injury, but the healed tissue may develop fascia adhesions potentially altering the amount of flexibility of the muscle. Any change of flexibility within a muscle may also affect the corresponding joint. This could create range of motion (ROM) restrictions as a result of the healing process (11). One method clinicians may use to augment the healing process is known as instrument assisted soft-tissue mobilization (IASTM). IASTM purports to increase myofascial mobility and to decrease adhesions that can be formed between the fascial layers and the surrounding connective tissue (4). Clinicians can use this as a technique after an injury has occurred as part of a normal course of a therapeutic rehabilitation plan (22). IASTM may be used for various overuse type injuries including myofascial pain and restrictions, decreased ROM, acute and chronic sprains or strains and plantar fasciitis (4,22). Various literature articles also suggest that IASTM is a treatment method that may improve range of motion, flexibility and tissue extensibility as a way to prevent injury (2,22).
IASTM may also be utilized for non-pathological conditions, as it has been shown to affect flexibility and ROM in previous literature (2,23). It has been argued that using IASTM is an effective treatment for improving flexibility and ROM because of the ability to increase tissue temperature, decreased adhesions to the connective tissue and promoting collagen alignment (2,5,8). IASTM works on the fascial connective tissue within the body. This connective tissue contains “sheaths of primarily collagen that forms cavities and muscular septums that cover organs” (3). It is reasonable to conclude that even daily activities can create non-pathological adhesions or decreases in the lubrication between these types of connective tissue. Therefore, the purpose of this study was to examine if there was a change in ankle dorsiflexion in Division II athletes during a single squat after IASTM treatments. The researchers hypothesized that both groups would show an increase in ROM of the ankle joint initially after IASTM, but that the experimental group would maintain an increase in ankle ROM after IASTM treatment was terminated.
METHODS
Participants
The participants of this study consisted of 25 Division II student-athletes, aged 18–24 years. Both males and females participated. Specific positions of players in their respective sports were not identified, but activity level was self-reported as high due to the level of off-season workouts and in-season conditioning. According to the American College of Sports Medicine, the activity level of the student-athlete was described at a level 7, or an individual who is participating in vigorous exercise 3–5 times per week for 1–6 months (16). Participants were included in the study if they were able to perform a squat, had no injuries or surgeries to the lower extremity, and had NCAA Division II athlete status. Participation in this study was strictly voluntary, and participants could remove themselves from the study at any time. This study was approved by the Gannon University Institutional Review Board, and all participants signed a consent form prior to experimentation.
Initially, the study included 40 participants. Experimental mortality due to injury and loss of interest decreased the participation rate to 25 athletes for the duration of the study. A power analysis was performed, and it was determined that a sample size of 25 participants with >10 individuals per group would be sufficient to obtain statistical significance between groups with a power value of 0.80.
Protocol
Instrument Assisted Soft Tissue Mobilization (IASTM) is a widely used technique designed to manipulate the superficial and deep layers of the fascia. Técnica Gavilán (Tracy, CA) instruments were used for this study. These instruments are stainless steel; surgical grade IASTM tools (Figure 1). Each investigator was trained and certified in the use of Técnica Gavilán prior to experimentation and was certified to use the instruments for over a year.
Figure 1.

IASTM instrument tools.
During the initial assessment, participants were randomly selected into one of two groups: experimental (n = 11) or control (n = 14). Each participant was contacted by the researchers to schedule an appointment to perform an initial assessment. For the initial assessment protocol, participants were asked to warm up on a cycle ergometer for 10 minutes. Participants were asked to keep their rate of perceived exertion (RPE) at a 3 or 4 level throughout the warm-up. After the warm-up, shoes and socks were removed and participants were then asked to perform 2–3 practice squats in an open area.
For each squat measurement, markers were placed on the participant’s fibular head, lateral malleolus, and the base of the fifth metatarsal while patient is weight bearing. Participants were instructed to perform the squat to the deepest of their ability. The investigators also provided 1–2 demonstration squats before squat assessments to show the depth of squat needed for analysis. The investigators indicated to participants that an acceptable squat consisted of a bent knee with more than 90 degrees of flexion.
After the baseline squat, both groups received the IASTM intervention while performing 4-way plane ankle rehabilitation exercises for 20 repetitions in four directions: plantarflexion, dorsiflexion, inversion and eversion. Each participant used a yellow resistance band, which is 2.5 pounds of resistance while performing the rehabilitation exercises. The investigators then performed IASTM treatment on the lower leg, which included the triceps surae complex, anterior tibialis, posterior tibialis, and peroneal muscle grouping. The participants continued to receive IASTM treatment until he or she finished the range of motion exercises and before there were signs of skin irritation, such as, petechiae, or capillary bleeding. After the IASTM treatment, a second squat was then recorded again as part of a post-intervention assessment in both groups.
The control group consisted of participants who initially received IASTM during the baseline protocol. The initial IASTM treatment was performed on the control group in order to examine if an initial increase in ROM was observed for both groups. Participants then waited a week to return to the lab for a third squat assessment with no IASTM intervention during that period of time. Finally, the control group performed a fourth squat one week later, as part of the maintenance period. See also Figure 2 for an illustration of the Control Group protocol.
Figure 2.
Control group research protocol.
Following the initial assessment, participants were asked to return within a week for 3 separate IASTM treatments, with 24 hours of rest between each treatment. IASTM was also combined with ankle ROM exercises using the yellow Thera-band. After the first week’s session, the experimental group was recorded performing a third squat assessment (session 3). At this time, the experimental group received a total of four IASTM treatments. After the third session of squat assessment, the experimental group did not receive IASTM treatments the following week. A fourth squat assessment was performed during this maintenance period after no treatment (Figure 3).
Figure 3.
Experimental Group Research Protocol.
For data analysis, the videos of the squats were imported into the Dartfish 7 Pro Suite software (Fribourg, Switzerland), where the three markers were used (fibular head, lateral malleolus, and the base of the fifth metatarsal) to create an angle at the ankle joint. The ankle angle was then digitized at the deepest portion of the squat movement, and this value was recorded. For our study, we defined a decrease in the ankle angle as an increased dorsiflexion ROM. This method of measuring the ankle angle as a measure of dorsiflexion in weight bearing has been used in previous research as a valid method of data collection (19). Although this is an uncommon method of measuring ROM, the researchers believed that this would accurately show angles on the Dartfish video analyzer.
Statistical Analysis
For the statistical analysis, squat assessment sessions were defined as Session 1 (baseline measurement pre-IASTM during the initial assessment period), Session 2 (post-IASTM during the initial assessment period), Session 3 (after 1 additional week with treatment or no treatment, for the experimental and control groups, respectively), and Session 4 (maintenance session after an additional week, no treatment for both groups). For each Session, the angle of the ankle was measured during the end of the squat movement. Three total ankle angle measurements were collected per session per individual, and the average value was used for the statistical analysis. A 4 (Session) x 2 (Group) mixed-design analysis of variance (ANOVA) was performed to determine statistical differences between conditions for the measurement of the ankle angle. Session (1, 2, 3, and 4) was used as the within-subjects factor, while Group (Experimental versus Control) was used as the between-subjects factor. Statistical significance for this test was set at α = 0.05. Post-hoc analyses using a Bonferroni correction were used to determine significance between variables for any significant interactions (Session x Group) found. All statistical tests were performed using IBM SPSS Statistics 23 software.
RESULTS
A significant main effect of Session was found for changes in ankle angle, F(3, 69) = 5.08, p < 0.05, η2 = 0.181. Pairwise comparisons revealed a significant 5% decrease in the magnitude of the angle from Session 3 to Session 4 (p < 0.05), indicating greater dorsiflexion of the ankle during the squat movement during the maintenance period (Figure 4). There was no significant main effect of Group for ankle angle.
Figure 4.
Main effect of Session for ankle angle. * indicates p < 0.05.
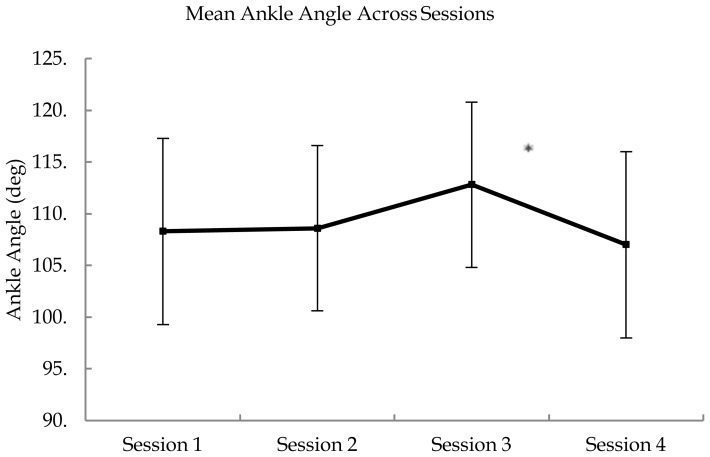
A significant Session x Group interaction was also found for ankle angle (increased dorsiflexion), F(3, 69) = 3.61, p < 0.05, η2 = 0.136 (Figure 5). Post-hoc analysis revealed a significant decrease in angle at the ankle (indicating increased dorsiflexion) between Sessions 3 and 4, which occurred for the experimental group only (p < 0.05). In addition, there was a significant difference in mean ankle angle between groups for Session 4 (p < 0.05). For this condition, the angle was significantly smaller for the experimental group compared to the control group, which indicates a deeper squat was performed and an increased amount of dorsiflexion.
Figure 5.
Ankle angle across the four Sessions for each Group. * indicates p < 0.05
DISCUSSION
The purpose of the study was to determine if there was an observed change in ankle dorsiflexion in Division II college athletes while receiving IASTM. Further, it was hypothesized that both groups would show an increase in ROM of the ankle joint initially, but that the experimental group would maintain that increase in ankle ROM. The results showed there was a significant decrease in the ankle angle from Session 3 to Session 4, indicating an increase in total dorsiflexion ROM during the maintenance period. This effect was driven by the experimental group, who showed a significant decrease in ankle angle from Session 3 to Session 4. Thus, the use of the IASTM appeared to enable the athletes to perform a deeper squat due to greater available ROM at the talocrural joint, as evidenced by the decreasing ankle angle (increased ankle dorsiflexion) observed across the sessions. These findings also suggest that the use of IASTM was instrumental in improving the athlete’s ROM, particularly during the maintenance period.
The use of IASTM is proposed to release adhesions, promote scar tissue breakdown, improve collagen alignment, and increase ROM and flexibility (2, 4). Previous studies that utilized IASTM to increase ROM revealed a necessary warm-up period required to heat the tissues prior to use of the intervention (2, 4, 13, 15). The use of IASTM to improve joint ROM as a measure of flexibility has been described in the literature previously (2). According to Baker, their experimental group maintained a greater ROM after the IASTM was applied when compared with the control group, and therapeutic benefits were indicated (2). A main difference between both the current study and Baker and colleagues (2) is the use of passive motion and active/functional ROM. While Baker utilized the hip and goniometric measurements, investigators in this study used active ROM and functional weight bearing movements to record the change of ROM. Both studies showed that using IASTM increased ROM available around the joint and thereby increased extensibility of the tissues.
In this study, there were no changes between groups when considering increases in ROM within the first two trials; both groups showed increased ROM at the ankle, which was hypothesized. This is consistent with a systematic review performed on the efficacy of IASTM, which indicated that there were increases in ROM in the short-term but limited studies identifying long-term effects (24-hours) of utilizing IASTM for joint ROM (4).
The increase in ROM and soft tissue extensibility has been reported in the literature to occur not only in the lower extremity but also in the overhead throwing athletes, and in the lumbar spine region (2,4,9,10). In the cases of athletes, applying IASTM treatments for as little as one or two sessions increased ROM in hamstrings (12). IASTM has also been utilized to prevent the loss of ROM in the shoulder for collegiate softball and volleyball athletes (10).
An additional explanation regarding the increase in ROM may be related to the mechanical pressure that is inherently applied during the IASTM intervention. The results from this study indicated there was an increase in ROM in the ankle joint, which may be explained by the mechanical stress that is exerted on the fascia. This mechanical stress stimulates mechanoreceptors which alters input received by the central nervous system and then changes the tension in tissues (21). This alteration and tension change are based on theory that describes the improvement in the change in ROM; however scientific proof is still lacking in this area (21). The current study demonstrated that using IASTM may affect long term tissue extensibility and therefore maintain functional ROM over a longer period of time than if IASTM was not used on the musculature and joint area. The mechanical pressure exerted on the patient by the instrument works to realign the collagen fibers that have created the fascia adhesions (14).
IASTM is an increasingly popular clinical intervention for acute and overuse conditions (4). This study suggests that IASTM is able to increase ROM in the ankle for both the short term and over a period of time. As such, maintaining appropriate ROM in the ankle is imperative for appropriate biomechanical function. Clinicians should consider using IASTM as a tool to maintain appropriate functional ROM to possibly prevent injuries through maintaining tissue extensibility. IASTM may also be utilized as a rehabilitation tool to decrease fascial adhesions that result from the natural healing process after injury and to restore normal ROM. Chronic as well as acute injuries may be treated effectively as reported in other studies (2,7). As indicated by previous research, lower extremity injuries are common in collegiate athletes (20). Of these injuries, ankle sprains are one of the most common injuries within a 10-year span (17). Although the current study was found to be significant in the college-aged athlete, there is a possibility of IASTM working for other populations.
This study is not without limitations. While the numbers of athletes tested were sufficient enough for statistical power, the 37% mortality rate raised concern. The loss of participants was attributed to injuries acquired and loss of interest. In addition, scheduling conflicts and missed appointment times made data collection challenging. Ideally, more participants tested would also be more representative of the athletic population when interpreting the results. Another challenge included not having direct control over the depth of the squat when performing the squat assessments. Although a proper squat was demonstrated to each participant prior to data collection, the researchers did not provide corrective feedback nor terminated the trial if the squat was performed incorrectly. This may have contributed to the overall variability in performance that was apparent in Figures 4 and 5. It is possible that there was variability within IASTM application due to the fact that there were three trained individuals utilizing the instruments; however, interrater variability was reduced by incorporating a strict IASTM protocol that each investigator adhered to. Additionally, the researchers had no control of the activities that the athletes participated in outside of data collection. This includes additional workouts, massage, hydration, or other factors that may have influenced ROM. Finally, this study lasted for a total of 3 weeks, with IASTM given to the experimental group for four sessions. It is unclear whether additional treatments given for an extended duration would have even greater ROM benefits than what was originally observed. Future studies are geared toward examining tissue extensibility in athletes for a longer treatment intervention and a longer maintenance period.
In summary, this study not only demonstrated the increase in ankle ROM after an IASTM intervention in college athletes, but over a maintained period of time if applied properly. A significant reduction in overall ankle angle was observed in the experimental group but not the control group, which was observed for the maintenance period when IASTM treatments were terminated. This data suggests that IASTM is an intervention that would have to be applied for multiple sessions and not a single treatment. Consideration of the use of IASTM as a rehabilitation tool to restore ROM in addition to treatment in acute and overuse injuries is warranted.
REFERENCES
- 1.Armiger P. Preventing musculotendinous injuries: a focus on flexibility. Athl Ther Today. 2000;5(4):20–25. [Google Scholar]
- 2.Baker R, Nasypany A, Seegmiller J, Baker J. Instrument-assisted soft tissue mobilization in treatment for tissue extensibility dysfunction. J Athl Train. 2013;18(5):16–21. [Google Scholar]
- 3.Barnes MF. The basic science of myofascial release: morphologic change in connective tissue. J Bodyw Mov Ther. 1997;1(4):231–238. [Google Scholar]
- 4.Cheatham SW, Lee M, Cain M, Baker R. The efficacy of instrument assisted soft tissue mobilization: A systematic review. J Can Chiropr Assoc. 2016;60(3):200–211. [PMC free article] [PubMed] [Google Scholar]
- 5.Davidson CJ, Ganion LR, Gehlsen GM, Verhoestra B, Roepke JE, Sevier TL. Rat tendon morphologic and functional changes resulting from soft tissue mobilization. Med Sci Sports Exerc. 1997;29(3):313–319. doi: 10.1097/00005768-199703000-00005. [DOI] [PubMed] [Google Scholar]
- 6.de Noronha M, Refshauge KM, Herbert RD, Kilbreath SL. Do voluntary strength, proprioception, range of motion, or postural sway predict occurrence of lateral ankle sprain? Br J Sports Med. 2009;40:824–828. doi: 10.1136/bjsm.2006.029645. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.de Vries JS, Krips R, Sierevelt IN, Blankevoort L, van Dijk CN. Interventions for treating chronic ankle instability. Cochrane Database Syst Rev. 2011;8 doi: 10.1002/14651858.CD004124.pub3. [DOI] [PubMed] [Google Scholar]
- 8.Gehlsen GM, Ganion LR, Helfst RH. Fibroblast responses to variation in soft tissue mobilization pressure. Med Sci Sports Exerc. 1999;31(4):531–535. doi: 10.1097/00005768-199904000-00006. [DOI] [PubMed] [Google Scholar]
- 9.Hammer WI, Pfefer MT. Treatment of a case of subacute lumbar compartment syndrome using the Graston technique. J Manipulative Physiol Ther. 2005;28:199–204. doi: 10.1016/j.jmpt.2005.02.010. [DOI] [PubMed] [Google Scholar]
- 10.Heinecke ML, Thuesen ST, Stow RC. Graston technique on shoulder motion in overhead athletes. J Undergrad Kinesiol Res. 2014;10:27–39. [Google Scholar]
- 11.Houglum PA. Therapeutic exercise for musculoskeletal injuries. Champaign, IL: Human Kinetics; 2016. [Google Scholar]
- 12.Kim DH, Kim TH, Jung DY, Weon JH. Effects of the Graston technique and self-myofascial release on the range of motion of a knee join. J Korean Soc Phys Med. 2014;9:455–565. [Google Scholar]
- 13.Kim J, Sung DJ, Lee J. Therapeutic effectiveness of instrument-assisted soft tissue mobilization for soft tissue injury: Mechanisms and practical application. J Exerc Rehabil. 2017;12(1):12–11. doi: 10.12965/jer.1732824.412. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Loghmani MT, Whitted M. Soft tissue manipuation: a power form of mechanotherapy. Physiother Rehabil. 2016;1(4):1–6. [Google Scholar]
- 15.Markovic G. Acute effects of instrument assisted soft tissue mobilization vs. foam rolling on knee and hip range of motion in soccer players. J Bodyw Mov Ther. 2015;19(4):690–696. doi: 10.1016/j.jbmt.2015.04.010. [DOI] [PubMed] [Google Scholar]
- 16.Martin SB, Morrow JR, Jr, Jackson AW, Dunn AL. Variables related to meeting the CDC/ACSM physical activity guidelines. Med Sci Sports Exerc. 2000;32(12):2087–2092. doi: 10.1097/00005768-200012000-00019. [DOI] [PubMed] [Google Scholar]
- 17.Nagle K, Johnson B, Brou L, Landman T, Sochanska A, Comstock RD. Timing of lower extremity injuries in competition and practice in high school sports. Sports Health. 2017;9(3):238–246. doi: 10.1177/1941738116685704. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Obradovic J, Vukadinovic M, Pantovic M, Dimitric G. Acute effects of different warm-up program on flexibility performance. PESH. 2014;3(2):29–33. [Google Scholar]
- 19.Pope R, Herbert R, Kirwan J. Effects of ankle dorsiflexion range and pre-exercise calf muscle stretching on injury risk in Army recruits. Aust J Physiother. 1998;44(3):165–172. doi: 10.1016/s0004-9514(14)60376-7. [DOI] [PubMed] [Google Scholar]
- 20.Roos KG, Marshall SW, Kerr ZY, Golightly YM, Kucera KL, Myers JB, Rosamond WD, Comstock RD. Epidemiology of overuse injuries in collegiate and high school athletics in the United States. J Sports Med. 2015;43(7):1790–1797. doi: 10.1177/0363546515580790. [DOI] [PubMed] [Google Scholar]
- 21.Schleip R. Fascial mechanoreceptors and their potential role in deep tissue manipulation. J Bodyw Mov Ther. 2003;7:104–116. [Google Scholar]
- 22.Stow R. Instrument-assisted soft tissue mobilization. Int J Athl Ther Train. 2011;16(3):5–8. [Google Scholar]
- 23.Vardiman JP, Siedlik J, Herda T, Hawkins W, Cooper M, Graham ZA, Deckert J, Gallagher P. Instrumentassisted soft tissue mobilization: Effects on the properties of human plantar flexors. Int J Sports Med. 2015;36(3):197–203. doi: 10.1055/s-0034-1384543. [DOI] [PubMed] [Google Scholar]