Abstract
Maintenance of mammalian core body temperature within a narrow range is a fundamental homeostatic process to optimize cellular and tissue function, and to improve survival in adverse thermal environments. Body temperature is maintained during a broad range of environmental and physiological challenges by central nervous system circuits that process thermal afferent inputs from the skin and the body core to control the activity of thermoeffectors. These include thermoregulatory behaviors, cutaneous vasomotion (vasoconstriction and, in humans, active vasodilation), thermogenesis (shivering and brown adipose tissue), evaporative heat loss (salivary spreading in rodents, and human sweating). This review provides an overview of the central nervous system circuits for thermoregulatory reflex regulation of thermoeffectors.
Keywords: thermoregulation, brown adipose tissue, shivering, cutaneous vasomotion, sweating, saliva secretion
Introduction.
Homeostatic control of body temperature is critical to the survival of mammals. Body temperature in mammals is generally maintained within a narrow range by the activation of multiple thermoeffector responses which are primarily under the control of central nervous system circuits. Important thermoeffector systems have evolved to maintain tissue temperatures at an appropriately elevated level to optimize enzymatic reactions and cellular function, while preventing dangerous elevations in body temperature that might compromise cellular function due to protein denaturation. Thermoregulatory behaviors, driven by cutaneous thermal receptors and motivated by thermal comfort, often comprise a first line of defense in maintaining body temperature in non-normothermic environments. The primary thermoeffector tissues include cutaneous blood vessels whose level of constriction determines whether the heat energy in warm blood will be radiated from the body to the environment or conserved in the body core. Salivary (in rodents) and sweat (in humans) glands provide fluid that dissipates body surface heat to the environment during evaporation. Thermogenesis due to skeletal muscle shivering and to the uncoupling of metabolic energy from ATP production in mitochondria, particularly prominent in brown adipose tissue, is the primary physiological heat source for cold defense. This review will provide an overview of the central neural circuits, from thermal afferents to thermoeffector tissues, that comprise the core neural pathways for the thermoregulatory responses.
Thermal afferent pathways
Primary somatosensory neurons
Classic neurophysiological experiments have characterized two general classes of innocuous thermal afferent fibers, those activated by cooling and those activated by warming. The cold activated fibers are rapidly adapting A-delta fibers in humans and primates [19, 43] and mostly c-fibers in other mammals such as, cats and rats [52]; these fibers respond with a dynamic activation during cooling and a sustained but diminished activation during stable cool thermal conditions. The warm activated fibers are largely c-fibers that are activated by innocuous warm temperatures [30, 52]. Thermal TRP channels likely play a role in detecting innocuous temperatures. For example, TRPM8 agonists applied to the skin evoke responses that mimic cold exposure [131]. In addition, TRPM8-deficient mice have a deficit in their ability to detect cold [9, 24, 29] and have mildly impaired cold tolerance [130]. Furthermore, TRPM8 antagonists attenuate cold defense responses [3]. Diphtheria toxin-induced ablation of TRPM8-containing neurons decreases behavioral responses to cold even more than TRPM8 deficiency [108].
The TRPV1 channel is a primary candidate for the detection of warm temperature. TRPV1 is necessary for innocuous warmth sensitivity in trigeminal ganglion cells [145], however TRPV1 deficient mice have relatively normal thermosensitivity [63, 108, 116]. TRPV1 antagonists produce hyperthermia, but this effect occurs independently of body and skin temperatures [127] suggesting that non-thermal activation of the TRPV1 channel contributes significantly to this response. Nonetheless diphtheria toxin-induced ablation of TRPV1-containing neurons decreases behavioral responses to heat (35–50 °C) [108]. These data suggest that the TRPV1-containing neurons play an important role in sensing warm temperatures but that the TRPV1 channel itself may be dispensable for this detection and furthermore that the TRPV1 channel also contributes significantly to other non-thermal processes. These TRP-containing primary somatosensory neurons have cell bodies located in the dorsal root ganglia and provide input to the superficial lamina (primarily lamina I) of the spinal dorsal horn [132, 140].
Spinal and trigeminal dorsal horn (DH)
Separate groups of secondary somatosensory neurons in the dorsal horn are activated by innocuous cooling or warming of the skin [5, 23, 28, 109]. The responses of DH neurons to skin cooling is primarily mediated by glutamatergic input from TRPM8-containing primary somatosensory neurons as evidenced by the observations that activation of cooling responsive DH neuron is blocked by either ablation of TRPM8 neurons or glutamate receptor blockade in the DH [109]. The effect of glutamate receptor blockade on skin warming-induced activation of DH neurons has not been tested, but TRPV1-containing neurons contribute to the warming activation of DH neurons [109] Nonetheless, warming-induced activation of DH neurons is likely to be more complex than a simple activation of these cells by a glutamatergic input from warm-activated (presumably TRPV1-containing) primary somatosensory neurons since ablation of TRPM8-containing (cold-activated) neurons increases the DH neural responses to warming [109].
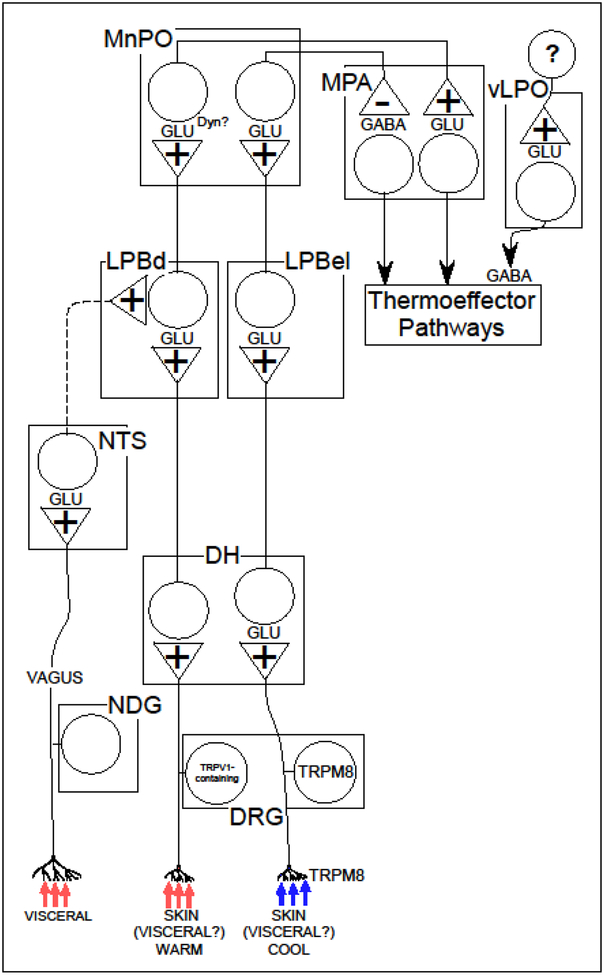
The DH contains neurons that project to the lateral parabrachial nucleus (LPB) [21, 95] and to the thalamus [49, 65]. The spinothalamic pathway relays thermal afferent input to the cortex for perception [26] but is not necessary for autonomic and behavioral responses to changes in skin temperature [94, 95, 144]. Temperature-responsive neurons in the DH send projections to the LPB [66] and the terminals of many DH neurons are in close apposition to LPB neurons that project to the POA [95]. Neurons in the LPB are necessary for thermoregulatory responses to cutaneous thermal input [60, 94, 95]. The LPB contains neurons that are activated by either warming or cooling of the skin [17, 94, 95]. The neurons that are activated by cold exposure are found predominantly in the external lateral subdivision of the LPB (LPBel), receive projections from the DH, and provide input to the median preoptic area (MnPO) [95]. Glutamatergic activation of neurons in the LPBel is necessary for cold defense responses such as shivering and BAT thermogenesis [95]. LPB neurons that are activated by heat exposure are located in the dorsal subdivision of the LPB (LPBd), provide input to the preoptic area, predominantly to the MnPO, and glutamatergic activation of the neurons in the LPBd is necessary for heat defense responses such as decreases in cutaneous vasoconstriction and inhibition of BAT thermogenesis [94]. In addition, in mice, the majority (83%) of the POA projecting neurons that are activated by heat exposure express preprodynorphin [38]. Furthermore, dynorphin microdialysis in the POA causes hypothermia [143]. The role of dynorphin in the POA during heat exposure remains unknown. Figure 1 illustrates the thermal afferent pathways.
Figure 1.
Model for the neuroanatomical pathways and neurotransmitters conveying thermal afferent input from the periphery to the preoptic area. Dashed projections indicate pathways that have not been conclusively demonstrated to function as suggested or that may involve indirect multisynaptic connections. DH, dorsal horn; DRG, dorsal root ganglia; Dyn, dynorphin; GLU, glutamate; LPBd, dorsal lateral parabrachial nucleus; LPBel, external lateral lateral parabrachial nucleus; MnPO, median preoptic nucleus; MPA, medial preoptic area; TRPM8, transient receptor potential subfamily M member 8; TRPV1, transient receptor potential vanilloid 1; NTS, nucleus tractus solitarius; vLPO, ventral portion of the lateral preoptic area.
In addition to the activation of DH neurons by thermally-activated cutaneous somatosensory input, thermoeffector activation can be elicited by directly changing the temperature of the spinal cord [139]. The mechanism of thermosensitivity of the spinal cord is unknown, but the TRP-mediated thermosensitivity of the central terminals of the cutaneous thermal afferents within the dorsal horn and the axons of thermal afferent nerve fibers [138], is a potential explanation [18, 86].
Abdominal thermal afferents
Abdominal thermosensitive afferents contribute to thermoregulation. For example, abdominal temperature influences the activity of sympathetic cutaneous vasoconstrictor fibers in the rat tail [122]. Furthermore, splanchnic nerve fibers from the abdominal wall are thermosensitive [114, 115], and contribute to thermoregulatory function in the ewe [113]. Similarly, in humans changes in abdominal temperature elicited by ingestion or gastric delivery of cold water can decrease sweat production during heat stress [81]. Conversely, ingestion of warm water can decrease shivering during cold exposure without affecting rectal, aural or skin temperatures [82]. In addition, there are thermosensitive vagal afferent neurons in the nodose ganglia [33], and the solitary tract-evoked responses of second order, vagal sensory neurons in the NTS are sensitive to local temperature [45, 124]. The degree to which thermally-sensitive vagal afferents contribute to thermoregulation is unknown. However, activation of vagal afferents [73] and activation of TRPV1 channels in the NTS, putatively on the central terminals of vagal afferent fibers, inhibits BAT thermogenesis [79], suggesting a potential role of thermally-responsive vagal afferents in thermoregulation. The details of the neural circuit by which these vagal afferents affect thermoregulation is unknown but given the robust inputs from the NTS to the LPB [44, 98] could involve inputs from neurons in the NTS to the thermal afferent neurons in the LPB (Figure 1). Additionally, these and other vagal afferent fibers could contribute to the regulation of metabolism and body temperature in response to non-thermal stimuli such as signals related to gastrointestinal stimuli for energy homeostasis (e.g. – GLP-1 [62], and lipids [13]).
Preoptic area (POA) neurons integrate thermal sensory information to control thermoeffector output.
Since the discovery of the anterior hypothalamus/POA as a site at which thermoregulatory response could be elicited by local temperature changes [74] and the subsequent demonstration of directly thermosensitive neurons in this region [96], the POA has received significant attention as a major locus in thermoregulation. Changes in POA temperature can elicit a broad array of thermoregulatory responses including both heat defense responses such as sweating, saliva secretion, panting, and cutaneous vasodilation, and cold defense responses such as shivering, BAT thermogenesis, and hormonal as well as behavioral responses [6–8, 10, 20, 40, 41, 50, 51, 55, 56, 76, 80, 106, 118, 125, 134].
The majority of temperature sensitive neurons in the anterior hypothalamus and POA are warm sensitive neurons (WSN, i.e.- neurons that increase their firing rate in response to increases in local temperature). WSN comprise ~30% of the neurons recorded in the POA compared to cold responsive neurons which make up <10% of the neurons recorded in this region, the remaining 60–70% of neurons are temperature insensitive [42, 46, 59]. In addition, WSNs have intrinsic thermosensitivity in the absence of synaptic input [58], whereas cold responsive neurons may require synaptic input for thermal sensitivity [32, 58], although it has also been reported that some neurons retain cold sensitivity during ionic conditions that would block synaptic inputs [47]. The mechanism(s) for the intrinsic thermosensitivity in WSNs is debated and may include depolarizing pacemaker potentials possibly mediated via decreases in outward potassium currents [14], and/or heat induced membrane depolarization [61]. TRPM2 channels may also contribute to the heat sensitivity of a subset of WSNs with a high threshold temperature for activation but are unlikely to mediate the majority of normal physiological responses since these channels only become activated at local temperatures above 42oC [126]. WSNs also integrate information about local temperature with cutaneous and spinal thermal afferent input [16, 39].
This integration of cutaneous thermal afferent input with intrinsic brain temperature has served to place these neurons in the role of a critical node for thermoregulation and it has become the convention that the POA contains the transition from the thermoafferent to the thermoeffector efferent pathways. Most WSNs are GABAergic [31, 67] and WSNs have been postulated to be output neurons of the POA for thermoregulation [15]. Consistent with this model, the predominant output of the POA is inhibitory to heat conserving (cutaneous vasoconstrictor) and thermogenic responses. For example, transections of the neuraxis caudal to the POA increase cutaneous sympathetic nerve activity (SNA) [111] and similarly, injections of the inhibitory neurotransmitter, GABA into several regions of the POA, including the median preoptic area (MnPO) or an area spanning the border between the medial and lateral preoptic areas increases cutaneous SNA to the rat tail [136]. In a parallel manner, transections of the neuraxis caudal to the POA increase BAT SNA and BAT thermogenesis [22, 141], and nanoinjections of the GABAA receptor agonist, muscimol into the ventral portion of the lateral preoptic area (vLPO) increase BAT SNA, BAT thermogenesis, and shivering [25]. The activity of neurons in the POA has also been implicated in driving heat defense responses such as sweating and saliva secretion. Functional MRI studies in humans have shown sweating-related activity in the POA [34]. Furthermore, lesions of the anterior hypothalamus/POA eliminate heat-induced salivation in the rat [128].
Connections between subregions of the POA have been suggested to play a role in thermoregulatory function. The preponderance of evidence suggests that MnPO neurons that receive thermal input from the cold-activated LPBel neurons inhibit the GABAergic output neurons of the POA, which are located in the medial preoptic area (MPA) [84, 88]. Conversely, the MnPO neurons receiving the warm afferent input from the LPBd have been suggested to activate the GABAergic MPA neurons [94, 133]. More detailed studies into the interactions of the neurocircuitry within the preoptic area are warranted especially given the recent appreciation of the complexity of the neural circuits within POA, including the roles in thermoregulation of additional recently recognized subregions (e.g.- the vLPO [25, 149]), recently described functional inputs to the POA [107], and the potential for divergent roles of heterogeneous cell populations within all regions of the POA.
Efferent pathways controlling thermoeffectors
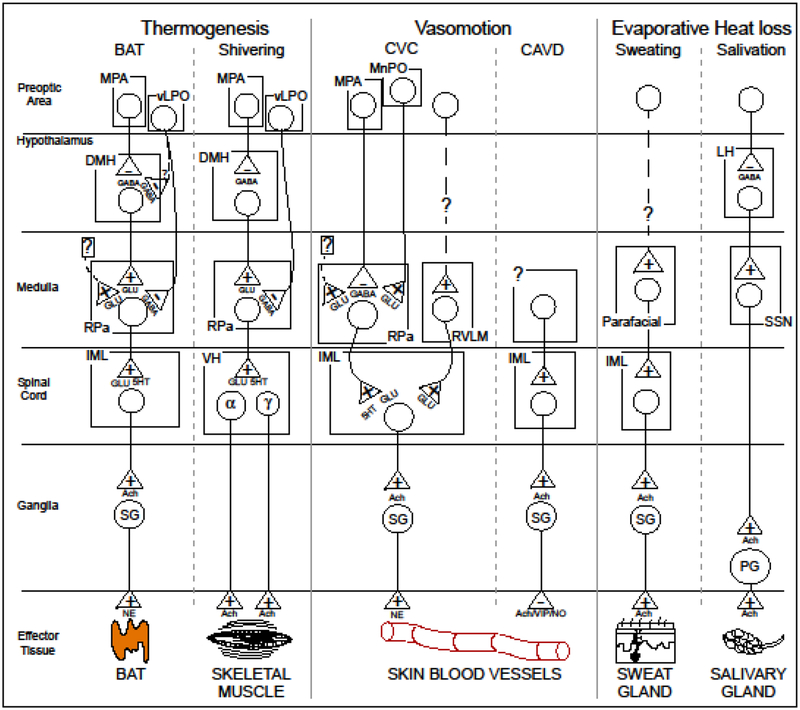
The efferent pathways controlling thermoeffectors can be defined into three general categories: thermogenic (BAT and shivering), vasomotor (cutaneous vasoconstrictor and cutaneous active vasodilator), and evaporative heat loss (sweating and saliva secretion) (Figure 2). The thermogenic efferent pathways are largely overlapping and involve an inhibitory output from the POA that impinges on hypothalamic neurons in the dorsomedial hypothalamus. The thermogenesis-promoting neurons of the DMH activate premotor neurons in the RPa which in turn send descending excitatory drive to spinal neurons (sympathetic preganglionic neurons for BAT and motor neurons for shivering). A similar pathway mediates cutaneous vasoconstriction with the exception that a relay in the DMH is not required, instead the inhibitory output from the POA impinges directly onto the cutaneous vasoconstrictor sympathetic premotor neurons in the raphe. In contrast, for sweating the pathway involves an excitation of neurons in the parafacial area which send descending excitatory drive to spinal sudomotor sympathetic preganglionic neurons. The efferent pathway for salivation has key features paralleling the other efferent pathways, the POA provides an inhibitory output to a hypothalamic relay neuron likely in the lateral hypothalamus. These LH neurons activate neurons in the superior salivatory nucleus (SSN). These SSN neurons are parasympathetic preganglionic neurons that drive the ganglion cells for salivation.
Figure 2.
Functional neuroanatomical model of the efferent thermoeffector pathways for thermogenesis, vasomotion, and evaporative heat loss. Dashed projections indicate pathways that are unknown and may involve multisynaptic connections. 5HT, 5-hydroxytryptamine (serotonin); α, alpha motor neuron; Ach, acetylcholine; BAT, brown adipose tissue; CAVD, cutaneous active vasodilation; CVC, cutaneous vasoconstriction; DMH, dorsomedial hypothalamus; γ, gamma motor neuron; GABA, gamma aminobutyric acid; GLU, glutamate; IML, intermediolateral cell column; LH, lateral hypothalamus; MnPO, median preoptic nucleus; MPA, medial preoptic area; NE, norepinephrine; NO, nitric oxide; PG, parasympathetic ganglion cell; RPa, raphe pallidus area; RVLM, rostral ventrolateral medulla; SG, sympathetic ganglion cell; SSN, superior salivatory nucleus; VH, ventral horn; VIP, vasoactive intestinal peptide; vLPO, ventral portion of the lateral preoptic area.
Sympathetic vasoconstriction reduces cutaneous blood flow
The amount of warm blood flow to the skin is a primary determinant of heat transfer to the environment. During cool ambient temperatures sympathetic nerve fibers innervating the cutaneous vasculature are activated to elicit cutaneous vasoconstriction, thereby decreasing heat transfer to the environment and conserving heat. Conversely during warm ambient conditions or when core body temperature is increased the cutaneous vasoconstrictor (CVC) sympathetic nerve fibers are inhibited thereby increasing blood flow to the skin and permitting heat transfer from the body to the environment. Neurons in the MnPO play a critical role in determining CVC SNA. In mice, activation of glutamatergic neurons in the MnPO increases tail vasodilation [1], presumably by decreasing CVC SNA. Conversely, inhibition of neurons in the MnPO causes vasoconstriction in the tail by increasing CVC SNA [136], suggesting that there is an output from the MnPO that is inhibitory to CVC SNA. The raphe pallidus area (RPa) contains sympathetic premotor neurons for cutaneous vasoconstriction [12]. The inhibitory output from the MnPO is likely to be an indirect input to the sympathetic CVC premotor neurons in the RPa and may involve activation of GABAergic neurons in the medial preoptic area (MPA) that have been suggested to directly inhibit the CVC premotor neurons in the RPa [91, 111]. Skin cooling also activates neurons in the POA that may directly excite RPa CVC premotor neurons via activation of glutamatergic receptors [135]. In turn, the RPa premotor neurons drive cutaneous vasoconstriction via excitatory glutamatergic and serotonergic projections to preganglionic neurons in the intermediolateral cell column of the spinal cord [11, 75, 101, 103]. In addition, some spinally-projecting RVLM neurons are inhibited by POA warming [78] and contribute to the CVC SNA [102, 104, 111], although the RVLM plays a minor role in CVC activity compared to sympathetic premotor neurons in the RPa [112]. The neural pathway conveying thermal information from the POA to the RVLM is not known.
Active cutaneous vasodilation
Humans, unlike rodents, have cutaneous sympathetic nerve fibers whose activation results in active cutaneous vasodilation (reviewed in [53]). The sympathetic fibers responsible for cutaneous active vasodilation are cholinergic, as opposed to the noradrenergic cutaneous vasoconstrictor fibers, and release acetylcholine as well as other co-transmitters including pituitary adenylate cyclase activating polypeptide and vasoactive intestinal peptide to elicit vasodilation. It is also likely that the peripheral production of nitric oxide mediates a component of active cutaneous vasodilation. The central pathways that drive cutaneous active vasodilation in human skin remain unknown
Evaporative heat loss is important for heat defense
Sweating
Sweating can be elicited by local heating of the POA [74], and humans show thermally-induced sweating-related activation in the POA [34]. In contrast to the RPa location of premotor neurons controlling CVC and thermogenic effectors the premotor neurons for cat paw sweating are located in the rostral ventromedial medulla (RVMM or parafacial area) [123]. A functional MRI study has demonstrated that a homologous parafacial region in humans shows activity during conditions that elicit sweating [35]. The descending pathway from the warm sensitive neurons in the POA to the sympathetic sudomotor neurons in the RVMM parafacial area has not been clearly defined. However, since WSNs are GABAergic and activation of neurons in the RVMM elicits sweating, the pathway from the WSNs to the RVMM sudomotor sympathoexcitatory neurons is unlikely to be direct. An area lateral to the periaqueductal gray (PAG) has been suggested as a potential synaptic relay for the sweating response [35].
Salivary secretion and saliva spreading behavior
Rodents do not sweat but instead use salivary secretion and grooming behavior to spread saliva over their cutaneous surface for evaporative heat loss. The submaxillary and sublingual glands are innervated by the chorda tympani and are responsible for thermally-induced largely parasympathetically –mediated saliva secretion [128]. The superior salivatory nucleus in the hindbrain contains the parasympathetic preganglionic neurons for salivation from the submaxillary and sublingual glands [48]. Salivation can be elicited by heating the anterior hypothalamus [54]. Details of the pathways from the anterior hypothalamus to the superior salivatory nucleus are still unclear. Thermal salivation was diminished by lesions in anterior hypothalamus [142], the lateral hypothalamus [128] and the ventromedial hypothalamus [36]. The lateral hypothalamus provides input to the superior salivary nucleus [117]. Therefore the most parsimonious pathway for thermal salivation would be that the POA activates lateral hypothalamic inputs to the SSN. Interestingly, grooming behavior can be elicited by heating the posterior but not anterior hypothalamus/POA, suggesting that at least some thermoregulatory behavioral responses can be elicited from areas other than the POA [134]. Evaporative cooling through panting is a warming-evoked response in some mammals. POA warming also elicits panting [74], however the efferent pathways from the POA to the respiratory generating networks in the medulla that elicit panting are unknown.
BAT thermogenesis and Shivering
Neural pathways regulating BAT have been comprehensively reviewed [84, 85]. We limit this review to the fundamental efferent neural circuit for thermal and febrile (see Febrile response section below) activations of BAT. During warm ambient conditions the warm-afferent input to the MnPO (see Thermal afferent pathways section above) increases the activity of a subset of MnPO neurons that in turn activate POA neurons that provide an inhibitory output to BAT thermogenesis-promoting neurons in the DMH and the RPa. This BAT sympathoinhibitory output from the POA likely arises from neurons in the MPA and the vLPO [25]. The warm-activated inhibitory output from the POA to neurons in the DMH and to sympathetic premotor neurons in the RPa suppresses the activation of the essential BAT thermogenesis-promoting neurons, thereby preventing BAT SNA and BAT thermogenesis during warm ambient conditions [25, 94]. Conversely, during cool ambient conditions the cool-afferent input to the MnPO (see Thermal afferent pathways section above) excites MnPO neurons that inhibit the activity of a population of inhibitory neurons in the MPA [93]. During cooling and fever, activation of BAT thermogenesis-promoting neurons in the DMH likely occurs due to removal of the active thermogenesis-suppressing output from MPA together with an activation of glutamatergic receptors on DMH neurons [71]. Subsequent activation of the BAT sympathetic premotor neurons in the RPa, likely via a glutamatergic input from the DMH to the RPa [57, 68] increases descending glutamatergic and serotonergic input to the spinal cord. Both glutamate [90] and serotonin [69, 70, 72] in the spinal cord contribute to BAT activation.
The efferent neural circuit regulating shivering closely parallels that for BAT. The shivering circuit involves the activation of essential thermogenesis-promoting neurons in both the DMH and the RPa [92]. During warm ambient conditions the POA provides inhibitory output for shivering [148], likely via inhibition of neurons in the DMH. This inhibitory input to the DMH may originate from the MPA and/or the vLPO [25]. Parallel to the pathway for BAT, cooling has been proposed to activate shivering-promoting neurons in the DMH by removing the tonically-active, inhibitory input from the POA [92], although whether removal of inhibitory inputs to the DMH evokes shivering remains to be determined. The shivering-promoting neurons in the DMH in turn activate somatic muscle premotor neurons for shivering in the RPa. In contrast to the neural circuit for the sympathetic control of BAT where RPa neurons activate sympathetic preganglionic neurons in the IML, descending input from the RPa for shivering activates alpha and gamma [137] motor neurons in the ventral horn of the spinal cord. Activation of the gamma motor neurons may contribute to the increase in muscle tone preceding overt shivering and to the threshold and intensity of shivering [120, 121]. Although direct descending projections from RPa neurons to the ventral horn somatomotor neurons have been demonstrated [2, 147], the precise pathways and neurochemical mechanism(s) by which the alpha and gamma motor neurons are activated during shivering remain to be defined.
Thermoregulatory behaviors
Behavior is an efficient and effective means of thermoregulation. Behavioral thermoregulation encompasses a broad range of activities including both preemptive and reactive responses. These behaviors include wearing clothing appropriate for predicted environmental conditions (such as putting on a jacket prior to going outside in the winter) and adjusting the thermostat in a room that is uncomfortably warm or cool. Another important behavioral response is the thermogenic contribution of increases in somatic motor activity [87, 105, 149]. Little is known about the central neural circuits involved in behavioral thermoregulation. Thermoregulatory behaviors are not affected by lesions of the thalamus even though these lesions eliminate cortical responses to thermal input [95, 144]. This observation is unexpected since the thalamocortical pathway is important for the perception of thermal input [26, 27] and our perceptions are so tightly linked to our behavior that we are apt to attribute the later to the former. These data serve to highlight the fact that thermal perception may not, at least in some circumstances, be the primary causal drive for thermoregulatory behaviors. Some thermoregulatory behaviors are unaffected by lesions of POA [4]. This observation is surprising given that direct changes in POA temperature or activation of neurons in this region can elicit thermoregulatory behaviors [6, 20, 118, 133, 146, 149]. Interestingly, lesions of the LPB impair some forms of behavioral thermoregulation [144]. Perhaps there are redundant pathways for behavioral thermoregulation involving both the thalamocortical pathway and the POA, such that removal of the LPB removes critical input to both of these pathways and is thereby capable of impairing behavioral thermoregulation.
Febrile response
Prostaglandin E2 (PGE2) produced by endothelial cells in the POA in response to pyrogens (such as lipopolysaccharide, a component of the outer membrane of gram-negative bacteria) acts on EP3 receptors in the POA to elicit febrile responses [64, 119]. Within the POA, EP3 receptors are located on neurons in the MPA and MnPO [89]. Some data have suggested that it is EP3 receptor activation in the MnPO that is necessary for febrile responses [64, 136]. Alternatively, putative warm-sensitive neurons in the MPA may be inhibited by PGE2 to elicit fever [83]. Consistent with this hypothesis, EP3 receptor activation couples to Gi proteins to decrease cAMP [97] and WSN activity is decreased by prostaglandin [110]. Nonetheless, several observations suggest that the prostaglandin evoked febrile response may be more complex than a simple model where EP3 receptor activation inhibits WSNs. For example, EP3 receptors can also couple to stimulatory GTP-binding proteins [97] and cold responsive neurons in the POA are activated by PGE2 [37, 77], suggesting the possibility that PGE2 may not only remove warm-defense inhibitory outputs from the POA but may also activate excitatory cold-defense outputs from the POA. In addition, EP3 receptor activation converts temperature-insensitive neurons into temperature-responsive neurons [129], although this mechanism has yet to be demonstrated in vivo. Although the EP3 receptor is required for fever [64], other prostaglandin receptors contribute to febrile responses. EP1 receptors are located in the POA [100], and EP1 receptor-deficient mice have an impaired fever response [99]. More studies are necessary to clarify the roles of specific neuronal populations and receptors within the POA that contribute to febrile responses.
Summary
The fundamental neural circuitry for body temperature homeostasis includes thermal afferent input impinging upon key neurons in the POA that integrate thermal input arriving via the spinal parabrachial-preoptic area afferent pathway (Figure 1) with local POA temperature to elicit thermoeffector outputs. These thermoeffector outputs include unique neural pathways regulating BAT thermogenesis, shivering, CVC, evaporative heat loss via sweating (and saliva spreading in rodents), as well as behavioral responses (Figure 2). Great progress over the last several decades has been made in defining these neural pathways. Future work aimed at further defining these pathways and adding newly discovered ancillary neural inputs to this fundamental neural circuitry will provide important information with implications for thermoregulation and metabolism.
Acknowledgments
Support of the authors’ research that contributed to this review came from National Institutes of Health grants R01NS40987 (S.F.M.), R01DK57838 (S.F.M.), and R01DK112198 (C.J.M.).
Footnotes
Publisher's Disclaimer: This is a PDF file of an unedited manuscript that has been accepted for publication. As a service to our customers we are providing this early version of the manuscript. The manuscript will undergo copyediting, typesetting, and review of the resulting proof before it is published in its final citable form. Please note that during the production process errors may be discovered which could affect the content, and all legal disclaimers that apply to the journal pertain.
References
- [1].Abbott SB, Machado NL, Geerling JC, Saper CB, Reciprocal Control of Drinking Behavior by Median Preoptic Neurons in Mice, The Journal of neuroscience : the official journal of the Society for Neuroscience 36 (2016) 8228–8237. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [2].Allen GV, Cechetto DF, Serotoninergic and nonserotoninergic neurons in the medullary raphe system have axon collateral projections to autonomic and somatic cell groups in the medulla and spinal cord, The Journal of comparative neurology 350 (1994) 357–366. [DOI] [PubMed] [Google Scholar]
- [3].Almeida MC, Hew-Butler T, Soriano RN, Rao S, Wang W, Wang J, Tamayo N, Oliveira DL, Nucci TB, Aryal P, Garami A, Bautista D, Gavva NR, Romanovsky AA, Pharmacological blockade of the cold receptor TRPM8 attenuates autonomic and behavioral cold defenses and decreases deep body temperature, The Journal of neuroscience : the official journal of the Society for Neuroscience 32 (2012) 2086–2099. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [4].Almeida MC, Steiner AA, Branco LG, Romanovsky AA, Neural substrate of cold-seeking behavior in endotoxin shock, PloS one 1 (2006) e1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [5].Andrew D, Craig AD, Spinothalamic lamina I neurones selectively responsive to cutaneous warming in cats, The Journal of physiology 537 (2001) 489–495. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [6].Baldwin BA, Ingram DL, Effect of heating & cooling the hypothalamus on behavioral thermoregulation in the pig, The Journal of physiology 191 (1967) 375–392. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [7].Banet M, Hensel H, Nonshivering thermogenesis induced by repetitive cooling of spinal cord in the rat, The American journal of physiology 230 (1976) 720–723. [DOI] [PubMed] [Google Scholar]
- [8].Banet M, Hensel H, Liebermann H, The central control of shivering and non-shivering thermogenesis in the rat, The Journal of physiology 283 (1978) 569–584. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [9].Bautista DM, Siemens J, Glazer JM, Tsuruda PR, Basbaum AI, Stucky CL, Jordt SE, Julius D, The menthol receptor TRPM8 is the principal detector of environmental cold, Nature 448 (2007) 204–208. [DOI] [PubMed] [Google Scholar]
- [10].Beaton LE, Mckinley WA, Berry CM, Ranson SW, Localization of cerebral center activating heat-loss mechanisms in monkeys, Journal of neurophysiology (1941) 478–485. [Google Scholar]
- [11].Blessing WW, Seaman B, 5-hydroxytryptamine(2A) receptors regulate sympathetic nerves constricting the cutaneous vascular bed in rabbits and rats, Neuroscience 117 (2003) 939–948. [DOI] [PubMed] [Google Scholar]
- [12].Blessing WW, Yu YH, Nalivaiko E, Raphe pallidus and parapyramidal neurons regulate ear pinna vascular conductance in the rabbit, Neuroscience letters 270 (1999) 33–36. [DOI] [PubMed] [Google Scholar]
- [13].Blouet C, Schwartz GJ, Duodenal lipid sensing activates vagal afferents to regulate non-shivering brown fat thermogenesis in rats, PloS one 7 (2012) e51898. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [14].Boulant JA, Counterpoint: Heat-induced membrane depolarization of hypothalamic neurons: an unlikely mechanism of central thermosensitivity, American journal of physiology. Regulatory, integrative and comparative physiology 290 (2006) R1481–1484; [DOI] [PubMed] [Google Scholar]
- [15].Boulant JA, Neuronal basis of Hammel’s model for set-point thermoregulation, J Appl Physiol (1985) 100 (2006) 1347–1354. [DOI] [PubMed] [Google Scholar]
- [16].Boulant JA, Hardy JD, The effect of spinal and skin temperatures on the firing rate and thermosensitivity of preoptic neurones, The Journal of physiology 240 (1974) 639–660. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [17].Bratincsak A, Palkovits M, Activation of brain areas in rat following warm and cold ambient exposure, Neuroscience 127 (2004) 385–397. [DOI] [PubMed] [Google Scholar]
- [18].Brock JA, McAllen RM, Spinal cord thermosensitivity: An afferent phenomenon?, Temperature (Austin) 3 (2016) 232–239. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [19].Campero M, Baumann TK, Bostock H, Ochoa JL, Human cutaneous C fibres activated by cooling, heating and menthol, The Journal of physiology 587 (2009) 5633–5652. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [20].Carlisle HJ, Laudenslager ML, Observations on the thermoregulatory effects of preoptic warming in rats, Physiology & behavior 23 (1979) 723–732. [DOI] [PubMed] [Google Scholar]
- [21].Cechetto DF, Standaert DG, Saper CB, Spinal and trigeminal dorsal horn projections to the parabrachial nucleus in the rat, The Journal of comparative neurology 240 (1985) 153–160. [DOI] [PubMed] [Google Scholar]
- [22].Chen XM, Hosono T, Yoda T, Fukuda Y, Kanosue K, Efferent projection from the preoptic area for the control of non-shivering thermogenesis in rats, The Journal of physiology 512 (Pt 3) (1998) 883–892. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [23].Christensen BN, Perl ER, Spinal neurons specifically excited by noxious or thermal stimuli: marginal zone of the dorsal horn, Journal of neurophysiology 33 (1970) 293–307. [DOI] [PubMed] [Google Scholar]
- [24].Colburn RW, Lubin ML, Stone DJ Jr., Wang Y, Lawrence D, D’Andrea MR, Brandt MR, Liu Y, Flores CM, Qin N, Attenuated cold sensitivity in TRPM8 null mice, Neuron 54 (2007) 379–386. [DOI] [PubMed] [Google Scholar]
- [25].Conceicao EP, Madden CJ, Morrison SF, Neurons in the rat ventral lateral preoptic area are essential for the warm-evoked inhibition of brown adipose tissue and shivering thermogenesis, Acta Physiologica in press (2018). [DOI] [PMC free article] [PubMed] [Google Scholar]
- [26].Craig AD, How do you feel? Interoception: the sense of the physiological condition of the body, Nature reviews. Neuroscience 3 (2002) 655–666. [DOI] [PubMed] [Google Scholar]
- [27].Craig AD, Bushnell MC, Zhang ET, Blomqvist A, A thalamic nucleus specific for pain and temperature sensation, Nature 372 (1994) 770–773. [DOI] [PubMed] [Google Scholar]
- [28].Craig AD, Krout K, Andrew D, Quantitative response characteristics of thermoreceptive and nociceptive lamina I spinothalamic neurons in the cat, Journal of neurophysiology 86 (2001) 1459–1480. [DOI] [PubMed] [Google Scholar]
- [29].Dhaka A, Murray AN, Mathur J, Earley TJ, Petrus MJ, Patapoutian A, TRPM8 is required for cold sensation in mice, Neuron 54 (2007) 371–378. [DOI] [PubMed] [Google Scholar]
- [30].Duclaux R, Kenshalo DR Sr., Response characteristics of cutaneous warm receptors in the monkey, Journal of neurophysiology 43 (1980) 1–15. [DOI] [PubMed] [Google Scholar]
- [31].Eberwine J, Bartfai T, Single cell transcriptomics of hypothalamic warm sensitive neurons that control core body temperature and fever response Signaling asymmetry and an extension of chemical neuroanatomy, Pharmacology & therapeutics 129 (2011) 241–259. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [32].Eisenman JS, Jackson DC, Thermal response patterns of septal and preoptic neurons in cats, Experimental neurology 19 (1967) 33–45. [DOI] [PubMed] [Google Scholar]
- [33].el Ouazzani T, Thermoreceptors in the digestive tract and their role, Journal of the Autonomic Nervous System 10 (1984) 246–254. [Google Scholar]
- [34].Farrell MJ, Trevaks D, McAllen RM, Preoptic activation and connectivity during thermal sweating in humans, Temperature (Austin) 1 (2014) 135–141. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [35].Farrell MJ, Trevaks D, Taylor NA, McAllen RM, Brain stem representation of thermal and psychogenic sweating in humans, American journal of physiology. Regulatory, integrative and comparative physiology 304 (2013) R810–817. [DOI] [PubMed] [Google Scholar]
- [36].Flynn FW, Evey LA, Mitchell JC, Heat-induced saliva secretion and thermoregulation in female rats with ventromedial hypothalamic lesions, Physiology & behavior 26 (1981) 779–782. [DOI] [PubMed] [Google Scholar]
- [37].Ford DM, A selective action of prostaglandin E1 on hypothalamic neurones in the cat which respond to brain cooling, J. Physiol. (Lond.) 242 (1975) 142–143P. [PubMed] [Google Scholar]
- [38].Geerling JC, Kim M, Mahoney CE, Abbott SB, Agostinelli LJ, Garfield AS, Krashes MJ, Lowell BB, Scammell TE, Genetic identity of thermosensory relay neurons in the lateral parabrachial nucleus, American journal of physiology. Regulatory, integrative and comparative physiology 310 (2016) R41–54. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [39].Guieu JD, Hardy JD, Effects of heating and cooling of the spinal cord on preoptic unit activity, Journal of applied physiology 29 (1970) 675–683. [DOI] [PubMed] [Google Scholar]
- [40].Hammel HT, Hardy JD, Fusco MM, Thermoregulatory responses to hypothalamic cooling in unanesthetized dogs, The American journal of physiology 198 (1960) 481–486. [DOI] [PubMed] [Google Scholar]
- [41].Hayward JN, Baker MA, Diuretic and thermoregulatory responses to preoptic cooling in the monkey, The American journal of physiology 214 (1968) 843–850. [DOI] [PubMed] [Google Scholar]
- [42].Hellon RF, Thermal stimulation of hypothalamic neurones in unanaesthetized rabbits, The Journal of physiology 193 (1967) 381–395. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [43].Hensel H, Iggo A, Analysis of cutaneous warm and cold fibres in primates, Pflugers Archiv : European journal of physiology 329 (1971) 1–8. [DOI] [PubMed] [Google Scholar]
- [44].Herbert H, Moga MM, Saper CB, Connections of the parabrachial nucleus with the nucleus of the solitary tract and the medullary reticular formation in the rat, The Journal of comparative neurology 293 (1990) 540–580. [DOI] [PubMed] [Google Scholar]
- [45].Hofmann ME, Andresen MC, Vanilloids selectively sensitize thermal glutamate release from TRPV1 expressing solitary tract afferents, Neuropharmacology 101 (2016) 401–411. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [46].Hori T, Nakashima T, Hori N, Kiyohara T, Thermo-sensitive neurons in hypothalamic tissue slices in vitro, Brain research 186 (1980) 203–207. [DOI] [PubMed] [Google Scholar]
- [47].Hori T, Nakashima T, Kiyohara T, Shibata M, Hori N, Effect of calcium removal on thermosensitivity of preoptic neurons in hypothalamic slices, Neuroscience letters 20 (1980) 171–175. [DOI] [PubMed] [Google Scholar]
- [48].Hubschle T, Mathai ML, McKinley MJ, Oldfield BJ, Multisynaptic neuronal pathways from the submandibular and sublingual glands to the lamina terminalis in the rat: a model for the role of the lamina terminalis in the control of osmo- and thermoregulatory behavior, Clinical and experimental pharmacology & physiology 28 (2001) 558–569. [DOI] [PubMed] [Google Scholar]
- [49].Hylden JL, Hayashi H, Dubner R, Bennett GJ, Physiology and morphology of the lamina I spinomesencephalic projection, The Journal of comparative neurology 247 (1986) 505–515. [DOI] [PubMed] [Google Scholar]
- [50].Imai-Matsumura K, Nakayama T, The central efferent mechanism of brown adipose tissue thermogenesis induced by preoptic cooling, Canadian journal of physiology and pharmacology 65 (1987) 1299–1303. [DOI] [PubMed] [Google Scholar]
- [51].Iriki M, Riedel W, Simon E, Regional differentiation of sympathetic activity during hypothalamic heating and cooling in anesthetized rabbits, Pflugers Archiv : European journal of physiology 328 (1971) 320–331. [DOI] [PubMed] [Google Scholar]
- [52].Iriuchijima J, Zotterman Y, The specificity of afferent cutaneous C fibres in mammals, Acta physiologica Scandinavica 49 (1960) 267–278. [DOI] [PubMed] [Google Scholar]
- [53].Johnson JM, Minson CT, Kellogg DL Jr., Cutaneous vasodilator and vasoconstrictor mechanisms in temperature regulation, Comprehensive Physiology 4 (2014) 33–89. [DOI] [PubMed] [Google Scholar]
- [54].Kanosue K, Nakayama T, Tanaka H, Yanase M, Yasuda H, Modes of action of local hypothalamic and skin thermal stimulation on salivary secretion in rats, The Journal of physiology 424 (1990) 459–471. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [55].Kanosue K, Yanase-Fujiwara M, Hosono T, Hypothalamic network for thermoregulatory vasomotor control, The American journal of physiology 267 (1994) R283–288. [DOI] [PubMed] [Google Scholar]
- [56].Kanosue K, Zhang YH, Yanase-Fujiwara M, Hosono T, Hypothalamic network for thermoregulatory shivering, Am J Physiol 267 (1994) R275–282. [DOI] [PubMed] [Google Scholar]
- [57].Kataoka N, Hioki H, Kaneko T, Nakamura K, Psychological stress activates a dorsomedial hypothalamus-medullary raphe circuit driving brown adipose tissue thermogenesis and hyperthermia, Cell metabolism 20 (2014) 346–358. [DOI] [PubMed] [Google Scholar]
- [58].Kelso SR, Boulant JA, Effect of synaptic blockade on thermosensitive neurons in hypothalamic tissue slices, The American journal of physiology 243 (1982) R480–490. [DOI] [PubMed] [Google Scholar]
- [59].Kelso SR, Perlmutter MN, Boulant JA, Thermosensitive single-unit activity of in vitro hypothalamic slices, The American journal of physiology 242 (1982) R77–84. [DOI] [PubMed] [Google Scholar]
- [60].Kobayashi A, Osaka T, Involvement of the parabrachial nucleus in thermogenesis induced by environmental cooling in the rat, Pflugers Archiv : European journal of physiology 446 (2003) 760–765. [DOI] [PubMed] [Google Scholar]
- [61].Kobayashi S, Hori A, Matsumura K, Hosokawa H, Point: Heat-induced membrane depolarization of hypothalamic neurons: a putative mechanism of central thermosensitivity, American journal of physiology. Regulatory, integrative and comparative physiology 290 (2006) R1479–1480; discussion R1484. [DOI] [PubMed] [Google Scholar]
- [62].Krieger JP, Santos da Conceicao EP, Sanchez-Watts G, Arnold M, Pettersen KG, Mohammed M, Modica S, Lossel P, Morrison SF, Madden CJ, Watts AG, Langhans W, Lee SJ, Glucagon-like peptide-1 regulates brown adipose tissue thermogenesis via the gut-brain axis in rats, American journal of physiology. Regulatory, integrative and comparative physiology (2018). [DOI] [PMC free article] [PubMed] [Google Scholar]
- [63].Kwan KY, Allchorne AJ, Vollrath MA, Christensen AP, Zhang DS, Woolf CJ, Corey DP, TRPA1 contributes to cold, mechanical, and chemical nociception but is not essential for hair-cell transduction, Neuron 50 (2006) 277–289. [DOI] [PubMed] [Google Scholar]
- [64].Lazarus M, Yoshida K, Coppari R, Bass CE, Mochizuki T, Lowell BB, Saper CB, EP3 prostaglandin receptors in the median preoptic nucleus are critical for fever responses, Nature neuroscience 10 (2007) 1131–1133. [DOI] [PubMed] [Google Scholar]
- [65].Li J, Xiong K, Pang Y, Dong Y, Kaneko T, Mizuno N, Medullary dorsal horn neurons providing axons to both the parabrachial nucleus and thalamus, The Journal of comparative neurology 498 (2006) 539–551. [DOI] [PubMed] [Google Scholar]
- [66].Light AR, Sedivec MJ, Casale EJ, Jones SL, Physiological and morphological characteristics of spinal neurons projecting to the parabrachial region of the cat, Somatosensory & motor research 10 (1993) 309–325. [DOI] [PubMed] [Google Scholar]
- [67].Lundius EG, Sanchez-Alavez M, Ghochani Y, Klaus J, Tabarean IV, Histamine influences body temperature by acting at H1 and H3 receptors on distinct populations of preoptic neurons, The Journal of neuroscience : the official journal of the Society for Neuroscience 30 (2010) 4369–4381. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [68].Machado NLS, Abbott SBG, Resch JM, Zhu L, Arrigoni E, Lowell BB, Fuller PM, Fontes MAP, Saper CB, A Glutamatergic Hypothalamomedullary Circuit Mediates Thermogenesis, but Not Heat Conservation, during Stress-Induced Hyperthermia, Current biology : CB 28 (2018) 2291–2301 e2295. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [69].Madden CJ, Morrison SF, Brown adipose tissue sympathetic nerve activity is potentiated by activation of 5-hydroxytryptamine (5-HT)1A/5-HT7 receptors in the rat spinal cord, Neuropharmacology 54 (2008) 487–496. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [70].Madden CJ, Morrison SF, Endogenous activation of spinal 5-hydroxytryptamine (5-HT) receptors contributes to the thermoregulatory activation of brown adipose tissue, American journal of physiology. Regulatory, integrative and comparative physiology 298 (2010) R776–783. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [71].Madden CJ, Morrison SF, Excitatory amino acid receptors in the dorsomedial hypothalamus mediate prostaglandin-evoked thermogenesis in brown adipose tissue, American journal of physiology. Regulatory, integrative and comparative physiology 286 (2004) R320–325. [DOI] [PubMed] [Google Scholar]
- [72].Madden CJ, Morrison SF, Serotonin potentiates sympathetic responses evoked by spinal NMDA, The Journal of physiology 577 (2006) 525–537. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [73].Madden CJ, Santos da Conceicao EP, Morrison SF, Vagal afferent activation decreases brown adipose tissue (BAT) sympathetic nerve activity and BAT thermogenesis, Temperature (Austin) 4 (2017) 89–96. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [74].Magoun HW, Harrison F, Brobeck JR, Ranson SW, Activation of heat loss mechanisms by local heating of the brain, Journal of neurophysiology 1 (1938) 101–114. [Google Scholar]
- [75].Marina N, Taheri M, Gilbey MP, Generation of a physiological sympathetic motor rhythm in the rat following spinal application of 5-HT, The Journal of physiology 571 (2006) 441–450. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [76].Martelli D, Luppi M, Cerri M, Tupone D, Mastrotto M, Perez E, Zamboni G, Amici R, The direct cooling of the preoptic-hypothalamic area elicits the release of thyroid stimulating hormone during wakefulness but not during REM sleep, PloS one 9 (2014) e87793. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [77].Matsuda T, Hori T, Nakashima T, Thermal and PGE2 sensitivity of the organum vasculosum lamina terminalis region and preoptic area in rat brain slices, The Journal of physiology 454 (1992) 197–212. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [78].McAllen RM, May CN, Effects of preoptic warming on subretrofacial and cutaneous vasoconstrictor neurons in anaesthetized cats, The Journal of physiology 481 (Pt 3) (1994) 719–730. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [79].Mohammed M, Madden CJ, Andresen MC, Morrison SF, Activation of TRPV1 in nucleus tractus solitarius reduces brown adipose tissue thermogenesis, arterial pressure, and heart rate, Am J Physiol Regul Integr Comp Physiol 315 (2018) R134–R143. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [80].Mohammed M, Madden CJ, Burchiel KJ, Morrison SF, Preoptic area cooling increases the sympathetic outflow to brown adipose tissue (BAT) and BAT thermogenesis, American journal of physiology. Regulatory, integrative and comparative physiology (2018). [DOI] [PMC free article] [PubMed] [Google Scholar]
- [81].Morris NB, Bain AR, Cramer MN, Jay O, Evidence that transient changes in sudomotor output with cold and warm fluid ingestion are independently modulated by abdominal, but not oral thermoreceptors, J Appl Physiol (1985) 116 (2014) 1088–1095. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [82].Morris NB, Filingeri D, Halaki M, Jay O, Evidence of viscerally-mediated cold-defence thermoeffector responses in man, The Journal of physiology 595 (2017) 1201–1212. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [83].Morrison SF, Central neural control of thermoregulation and brown adipose tissue, Autonomic neuroscience : basic & clinical 196 (2016) 14–24. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [84].Morrison SF, Madden CJ, Central nervous system regulation of brown adipose tissue, Comprehensive Physiology 4 (2014) 1677–1713. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [85].Morrison SF, Nakamura K, Central Mechanisms for Thermoregulation, Ann. Rev. Physiol. in press (2018). [DOI] [PubMed] [Google Scholar]
- [86].Morrison SF, Nakamura K, Central neural pathways for thermoregulation, Front Biosci (Landmark Ed) 16 (2011) 74–104. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [87].Mount LE, Willmott JV, The relation between spontaneous activity, metabolic rate and the 24 hour cycle in mice at different environmental temperatures, The Journal of physiology 190 (1967) 371–380. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [88].Nakamura K, Central circuitries for body temperature regulation and fever, American journal of physiology. Regulatory, integrative and comparative physiology 301 (2011) R1207–1228. [DOI] [PubMed] [Google Scholar]
- [89].Nakamura K, Kaneko T, Yamashita Y, Hasegawa H, Katoh H, Ichikawa A, Negishi M, Immunocytochemical localization of prostaglandin EP3 receptor in the rat hypothalamus, Neuroscience letters 260 (1999) 117–120. [DOI] [PubMed] [Google Scholar]
- [90].Nakamura K, Matsumura K, Hubschle T, Nakamura Y, Hioki H, Fujiyama F, Boldogkoi Z, Konig M, Thiel HJ, Gerstberger R, Kobayashi S, Kaneko T, Identification of sympathetic premotor neurons in medullary raphe regions mediating fever and other thermoregulatory functions, The Journal of neuroscience : the official journal of the Society for Neuroscience 24 (2004) 5370–5380. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [91].Nakamura K, Matsumura K, Kaneko T, Kobayashi S, Katoh H, Negishi M, The rostral raphe pallidus nucleus mediates pyrogenic transmission from the preoptic area, The Journal of neuroscience : the official journal of the Society for Neuroscience 22 (2002) 4600–4610. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [92].Nakamura K, Morrison SF, Central efferent pathways for cold-defensive and febrile shivering, The Journal of physiology 589 (2011) 3641–3658. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [93].Nakamura K, Morrison SF, Preoptic mechanism for cold-defensive responses to skin cooling, The Journal of physiology 586 (2008) 2611–2620. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [94].Nakamura K, Morrison SF, A thermosensory pathway mediating heat-defense responses, Proceedings of the National Academy of Sciences of the United States of America 107 (2010) 8848–8853. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [95].Nakamura K, Morrison SF, A thermosensory pathway that controls body temperature, Nature neuroscience 11 (2008) 62–71. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [96].Nakayama T, Eisenman JS, Hardy JD, Single unit activity of anterior hypothalamus during local heating, Science 134 (1961) 560–561. [DOI] [PubMed] [Google Scholar]
- [97].Negishi M, Irie A, Sugimoto Y, Namba T, Ichikawa A, Selective coupling of prostaglandin E receptor EP3D to Gi and Gs through interaction of alpha-carboxylic acid of agonist and arginine residue of seventh transmembrane domain, The Journal of biological chemistry 270 (1995) 16122–16127. [DOI] [PubMed] [Google Scholar]
- [98].Norgren R, Projections from the nucleus of the solitary tract in the rat, Neuroscience 3 (1978) 207–218. [DOI] [PubMed] [Google Scholar]
- [99].Oka T, Oka K, Kobayashi T, Sugimoto Y, Ichikawa A, Ushikubi F, Narumiya S, Saper CB, Characteristics of thermoregulatory and febrile responses in mice deficient in prostaglandin EP1 and EP3 receptors, The Journal of physiology 551 (2003) 945–954. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [100].Oka T, Oka K, Scammell TE, Lee C, Kelly JF, Nantel F, Elmquist JK, Saper CB, Relationship of EP(1–4) prostaglandin receptors with rat hypothalamic cell groups involved in lipopolysaccharide fever responses, The Journal of comparative neurology 428 (2000) 20–32. [DOI] [PubMed] [Google Scholar]
- [101].Ootsuka Y, Blessing WW, Activation of slowly conducting medullary raphe-spinal neurons, including serotonergic neurons, increases cutaneous sympathetic vasomotor discharge in rabbit, American journal of physiology. Regulatory, integrative and comparative physiology 288 (2005) R909–918. [DOI] [PubMed] [Google Scholar]
- [102].Ootsuka Y, McAllen RM, Interactive drives from two brain stem premotor nuclei are essential to support rat tail sympathetic activity, American journal of physiology. Regulatory, integrative and comparative physiology 289 (2005) R1107–1115. [DOI] [PubMed] [Google Scholar]
- [103].Ootsuka Y, Nalivaiko E, Blessing WW, Spinal 5-HT2A receptors regulate cutaneous sympathetic vasomotor outflow in rabbits and rats; relevance for cutaneous vasoconstriction elicited by MDMA (3,4-methylenedioxymethamphetamine, “Ecstasy”) and its reversal by clozapine, Brain Res 1014 (2004) 34–44. [DOI] [PubMed] [Google Scholar]
- [104].Ootsuka Y, Terui N, Functionally different neurons are organized topographically in the rostral ventrolateral medulla of rabbits, J Auton Nerv Syst 67 (1997) 67–78. [DOI] [PubMed] [Google Scholar]
- [105].Overton JM, Phenotyping small animals as models for the human metabolic syndrome: thermoneutrality matters, Int J Obes (Lond) 34 Suppl 2 (2010) S53–58. [DOI] [PubMed] [Google Scholar]
- [106].Owens NC, Ootsuka Y, Kanosue K, McAllen RM, Thermoregulatory control of sympathetic fibres supplying the rat’s tail, The Journal of physiology 543 (2002) 849–858. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [107].Padilla SL, Johnson CW, Barker FD, Patterson MA, Palmiter RD, A Neural Circuit Underlying the Generation of Hot Flushes, Cell reports 24 (2018) 271–277. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [108].Pogorzala LA, Mishra SK, Hoon MA, The cellular code for mammalian thermosensation, The Journal of neuroscience : the official journal of the Society for Neuroscience 33 (2013) 5533–5541. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [109].Ran C, Hoon MA, Chen X, The coding of cutaneous temperature in the spinal cord, Nature neuroscience 19 (2016) 1201–1209. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [110].Ranels HJ, Griffin JD, The effects of prostaglandin E2 on the firing rate activity of thermosensitive and temperature insensitive neurons in the ventromedial preoptic area of the rat hypothalamus, Brain research 964 (2003) 42–50. [DOI] [PubMed] [Google Scholar]
- [111].Rathner JA, Madden CJ, Morrison SF, Central pathway for spontaneous and prostaglandin E2-evoked cutaneous vasoconstriction, American journal of physiology. Regulatory, integrative and comparative physiology 295 (2008) R343–354. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [112].Rathner JA, McAllen RM, Differential control of sympathetic drive to the rat tail artery and kidney by medullary premotor cell groups, Brain research 834 (1999) 196–199. [DOI] [PubMed] [Google Scholar]
- [113].Rawson RO, Quick KP, Localization of intra-abdominal thermoreceptors in the ewe, The Journal of physiology 222 (1972) 665–667. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [114].Riedel W, Warm receptors in the dorsal abdominal wall of the rabbit, Pflugers Archiv : European journal of physiology 361 (1976) 205–206. [DOI] [PubMed] [Google Scholar]
- [115].Riedel W, Siaplauras G, Simon E, Intra-abdominal thermosensitivity in the rabbit as compared with spinal thermosensitivity, Pflugers Archiv : European journal of physiology 340 (1973) 59–70. [DOI] [PubMed] [Google Scholar]
- [116].Romanovsky AA, Almeida MC, Garami A, Steiner AA, Norman MH, Morrison SF, Nakamura K, Burmeister JJ, Nucci TB, The transient receptor potential vanilloid-1 channel in thermoregulation: a thermosensor it is not, Pharmacological reviews 61 (2009) 228–261. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [117].Saper CB, Loewy AD, Efferent connections of the parabrachial nucleus in the rat, Brain research 197 (1980) 291–317. [DOI] [PubMed] [Google Scholar]
- [118].Satinoff E, Behavioral Thermoregulation in Response to Local Cooling of the Rat Brain, Am J Physiol 206 (1964) 1389–1394. [DOI] [PubMed] [Google Scholar]
- [119].Scammell TE, Griffin JD, Elmquist JK, Saper CB, Microinjection of a cyclooxygenase inhibitor into the anteroventral preoptic region attenuates LPS fever, The American journal of physiology 274 (1998) R783–789. [DOI] [PubMed] [Google Scholar]
- [120].Schafer SS, Schafer S, The behavior of the proprioceptors of the muscle and the innervation of the fusimotor system during cold shivering, Experimental brain research 17 (1973) 364–380. [DOI] [PubMed] [Google Scholar]
- [121].Schafer SS, Schafer S, The role of the primary afference in the generation of a cold shivering tremor, Experimental brain research 17 (1973) 381–393. [DOI] [PubMed] [Google Scholar]
- [122].Shafton AD, Kitchener P, McKinley MJ, McAllen RM, Reflex control of rat tail sympathetic nerve activity by abdominal temperature, Temperature (Austin) 1 (2014) 37–41. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [123].Shafton AD, McAllen RM, Location of cat brain stem neurons that drive sweating, American journal of physiology. Regulatory, integrative and comparative physiology 304 (2013) R804–809. [DOI] [PubMed] [Google Scholar]
- [124].Shoudai K, Peters JH, McDougall SJ, Fawley JA, Andresen MC, Thermally active TRPV1 tonically drives central spontaneous glutamate release, The Journal of neuroscience : the official journal of the Society for Neuroscience 30 (2010) 14470–14475. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [125].Smiles KA, Elizondo RS, Barney CC, Sweating responses during changes of hypothalamic temperature in the rhesus monkey, Journal of applied physiology 40 (1976) 653–657. [DOI] [PubMed] [Google Scholar]
- [126].Song K, Wang H, Kamm GB, Pohle J, Reis FC, Heppenstall P, Wende H, Siemens J, The TRPM2 channel is a hypothalamic heat sensor that limits fever and can drive hypothermia, Science 353 (2016) 1393–1398. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [127].Steiner AA, Turek VF, Almeida MC, Burmeister JJ, Oliveira DL, Roberts JL, Bannon AW, Norman MH, Louis JC, Treanor JJ, Gavva NR, Romanovsky AA, Nonthermal activation of transient receptor potential vanilloid-1 channels in abdominal viscera tonically inhibits autonomic cold-defense effectors, The Journal of neuroscience : the official journal of the Society for Neuroscience 27 (2007) 7459–7468. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [128].Stricker EM, Hainsworth FR, Evaporative cooling in the rat: Effects of hypthalamic lesions and chorda tympani damage, Canadian journal of physiology and pharmacology 48 (1970) 11–17. [DOI] [PubMed] [Google Scholar]
- [129].Tabarean IV, Behrens MM, Bartfai T, Korn H, Prostaglandin E2-increased thermosensitivity of anterior hypothalamic neurons is associated with depressed inhibition, Proceedings of the National Academy of Sciences of the United States of America 101 (2004) 2590–2595. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [130].Tajino K, Hosokawa H, Maegawa S, Matsumura K, Dhaka A, Kobayashi S, Cooling-sensitive TRPM8 is thermostat of skin temperature against cooling, PloS one 6 (2011) e17504. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [131].Tajino K, Matsumura K, Kosada K, Shibakusa T, Inoue K, Fushiki T, Hosokawa H, Kobayashi S, Application of menthol to the skin of whole trunk in mice induces autonomic and behavioral heat- gain responses, American journal of physiology. Regulatory, integrative and comparative physiology 293 (2007) R2128–2135. [DOI] [PubMed] [Google Scholar]
- [132].Takashima Y, Daniels RL, Knowlton W, Teng J, Liman ER, McKemy DD, Diversity in the neural circuitry of cold sensing revealed by genetic axonal labeling of transient receptor potential melastatin 8 neurons, The Journal of neuroscience : the official journal of the Society for Neuroscience 27 (2007) 14147–14157. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [133].Tan CL, Cooke EK, Leib DE, Lin YC, Daly GE, Zimmerman CA, Knight ZA, Warm-Sensitive Neurons that Control Body Temperature, Cell 167 (2016) 47–59 e15. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [134].Tanaka H, Kanosue K, Nakayama T, Shen Z, Grooming, body extension, and vasomotor responses induced by hypothalamic warming at different ambient temperatures in rats, Physiology & behavior 38 (1986) 145–151. [DOI] [PubMed] [Google Scholar]
- [135].Tanaka M, McKinley MJ, McAllen RM, Preoptic-raphe connections for thermoregulatory vasomotor control, The Journal of neuroscience : the official journal of the Society for Neuroscience 31 (2011) 5078–5088. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [136].Tanaka M, McKinley MJ, McAllen RM, Roles of two preoptic cell groups in tonic and febrile control of rat tail sympathetic fibers, American journal of physiology. Regulatory, integrative and comparative physiology 296 (2009) R1248–1257. [DOI] [PubMed] [Google Scholar]
- [137].Tanaka M, Owens NC, Nagashima K, Kanosue K, McAllen RM, Reflex activation of rat fusimotor neurons by body surface cooling, and its dependence on the medullary raphe, The Journal of physiology 572 (2006) 569–583. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [138].Teliban A, Bartsch F, Struck M, Baron R, Janig W, Axonal thermosensitivity and mechanosensitivity of cutaneous afferent neurons, The European journal of neuroscience 33 (2011) 110–118. [DOI] [PubMed] [Google Scholar]
- [139].Thauer R, Thermosensitivity of the Spinal Cord In: Hardy JD, Gagge AP, Stolwijk JAJ (Eds.), Physiological and Behavioral Temperature Regulation, Charles C Thomas, Springfield, Illinois, USA, 1968, pp. 472–492. [Google Scholar]
- [140].Tominaga M, Caterina MJ, Malmberg AB, Rosen TA, Gilbert H, Skinner K, Raumann BE, Basbaum AI, Julius D, The cloned capsaicin receptor integrates multiple pain-producing stimuli, Neuron 21 (1998) 531–543. [DOI] [PubMed] [Google Scholar]
- [141].Tupone D, Cano G, Morrison SF, Thermoregulatory inversion: a novel thermoregulatory paradigm, American journal of physiology. Regulatory, integrative and comparative physiology 312 (2017) R779–R786. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [142].Whyte DG, Johnson AK, Thermoregulatory role of periventricular tissue surrounding the anteroventral third ventricle (AV3V) during acute heat stress in the rat, Clinical and experimental pharmacology & physiology 32 (2005) 457–461. [DOI] [PubMed] [Google Scholar]
- [143].Xin L, Geller EB, Adler MW, Body temperature and analgesic effects of selective mu and kappa opioid receptor agonists microdialyzed into rat brain, The Journal of pharmacology and experimental therapeutics 281 (1997) 499–507. [PubMed] [Google Scholar]
- [144].Yahiro T, Kataoka N, Nakamura Y, Nakamura K, The lateral parabrachial nucleus, but not the thalamus, mediates thermosensory pathways for behavioural thermoregulation, Sci Rep 7 (2017) 5031. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [145].Yarmolinsky DA, Peng Y, Pogorzala LA, Rutlin M, Hoon MA, Zuker CS, Coding and Plasticity in the Mammalian Thermosensory System, Neuron 92 (2016) 1079–1092. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [146].Yu S, Qualls-Creekmore E, Rezai-Zadeh K, Jiang Y, Berthoud HR, Morrison CD, Derbenev AV, Zsombok A, Munzberg H, Glutamatergic Preoptic Area Neurons That Express Leptin Receptors Drive Temperature-Dependent Body Weight Homeostasis, The Journal of neuroscience : the official journal of the Society for Neuroscience 36 (2016) 5034–5046. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [147].Zagon A, Bacon SJ, Evidence of a Monosynaptic Pathway Between Cells of the Ventromedial Medulla and the Motoneuron Pool of the Thoracic Spinal Cord in Rat: Electron Microscopic Analysis of Synaptic Contacts, The European journal of neuroscience 3 (1991) 55–65. [DOI] [PubMed] [Google Scholar]
- [148].Zhang YH, Yanase-Fujiwara M, Hosono T, Kanosue K, Warm and cold signals from the preoptic area: which contribute more to the control of shivering in rats?, The Journal of physiology 485 (Pt 1) (1995) 195–202. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [149].Zhao ZD, Yang WZ, Gao C, Fu X, Zhang W, Zhou Q, Chen W, Ni X, Lin JK, Yang J, Xu XH, Shen WL, A hypothalamic circuit that controls body temperature, Proceedings of the National Academy of Sciences of the United States of America 114 (2017) 2042–2047. [DOI] [PMC free article] [PubMed] [Google Scholar]