Abstract
Ulnar neuropathy at the elbow is the second most common entrapment neuropathy of the upper extremity. Yet, there is a paucity of literature focusing on the imaging appearance following surgical decompression of the ulnar nerve at the elbow. Diagnostic imaging studies obtained after surgical decompression at The University of Michigan were reviewed and imaging findings were documented. We aim to describe the various techniques of ulnar nerve decompression and corresponding post-operative appearance on imaging. Potential complications following decompression will also be described with imaging and clinical correlation of recalcitrant ulnar neuropathy. It is important for the radiologist who performs MRI or ultrasound of the elbow to be aware of the various ulnar nerve decompression procedures. This knowledge will facilitate rapid and accurate diagnosis of normal and abnormal appearance of the ulnar nerve in this context.
Introduction:
Compression of the ulnar nerve at the elbow is the second most common type of entrapment neuropathy of the upper extremity with approximately 25 cases per 100,000 person-years.1,2 Ulnar neuropathy is accompanied by pain, paresthesia and muscle weakness with approximately half of all patients collecting disability prior to their diagnosis.1,2 Therefore, this entity has significant functional implications for the patient as well as economic implications for both patients and society. Surgical intervention for ulnar neuropathy is implemented when conservative treatment fails.3 In a retrospective study by Adkinson et al, it was found that 26,164 patients underwent surgery for ulnar nerve entrapment at the elbow between the years 2005 to 2012 in the state of Florida alone.2 While surgical intervention for this pathology is not uncommon, to our knowledge, little has been written on the imaging presentation following surgical decompression or transposition of the ulnar nerve.
In this pictorial review, we provide a brief background on ulnar nerve anatomy at the mid-arm to elbow followed by cases demonstrating various techniques of nerve decompression. Imaging findings in cases of recalcitrant ulnar neuropathy with surgical correlation are also presented.
Anatomy and background
Ulnar neuropathy at the elbow and arm can be caused by entrapment by adjacent structures or due to instability of the nerve.4 Entrapment can occur at multiple sites along the course of the ulnar nerve (Figure 1). The terminology relating to the different anatomic structures varies between studies and for purposes of this paper, we will describe the terminology and approach accepted at The University of Michigan. There are five common potential sites of ulnar nerve entrapment in the mid arm to distal elbow (Figure 1). The most proximal structure, the arcade of Struthers, is located approximately 8 cm proximal to the humeral epicondyle.5–7 There is doubt regarding the role this structure plays in primary entrapment of the ulnar nerve, however, the presence of such an arcade may be responsible for recurrence of ulnar neuropathy following anterior transposition.5–7
Figure 1.

Illustration depicts sites of ulnar nerve entrapment about the elbow.
Another potential site of entrapment is the intermuscular septum (IMS) (Figure 2). The IMS is a fibrous band that blends with the distal coracobrachialis tendon at the mid-humeral shaft, distal to the insertion of the teres major. It inserts on the medial epicondyle distally and remains an attachment site of the brachialis muscle anteriorly and medial head triceps brachii muscle posteriorly throughout its course. Cadaveric studies have depicted variant anatomical relationships between the IMS and ulnar nerve.5,8 The relevance of this structure in ulnar nerve entrapment is its role as a noncompliant structure against which the ulnar nerve can be compressed (e.g. by a hypertrophied triceps). The IMS may also be responsible for recurrence of ulnar neuropathy after anterior transposition in the elbow, as altering the nerve pathway can drape the nerve over the non-compliant intermuscular septum.9
Figure 2.

The intermuscular septum (arrows) separate the anterior (brachialis muscle) and posterior (triceps muscle) compartments of the arm with the ulnar nerve (*) coursing between the septum and medial head triceps muscle (T).
The post-condylar groove is an additional site of potential entrapment neuropathy (Figure 3). The ulnar nerve course through this osteofibrous tunnel is between the medial humeral epicondyle and the olecranon process. The floor and roof of this tunnel is formed by the posterior band of the ulnar collateral ligament and the fascia between the olecranon process of the ulna and the medial humeral epicondyle, accordingly.9
Figure 3.

Intraopearative photo demonstrate the post-condylar groove (elipse), an osteofiberous tunnel between the medial humeral epicondyle and olecranon process through which the ulnar nerve(*) courses. The structure tagged with the band is the MABC nerve. MABC, median antebrachial cutaneous.
The cubital tunnel is the fourth potential site of entrapment. This tunnel is located approximately 1 cm distal to the post-condylar groove and formed by the ulnar and humeral heads of the flexor carpi ulnaris (FCU) and superficial investing fascia (Figure 4). This fascia does not contact the ulnar nerve but needs to be incised in order to obtain access to the FCU heads (Figure 5). The ligament coursing deep to the FCU heads is called Osborne’s band/ligament (immediately superficial to the ulnar nerve) (Figure 5). At The University of Michigan, we identify Osborne’s ligament as a separate point of potential entrapment, proximal to the cubital tunnel proper.
Figure 4.

Intraopearative photo demonstates the broad based fascia (arrowheads) superficial to the flexor carpi ulnaris elevated by instrument. Ulnar nerve (*).
Figure 5.

Intraopeartive photo demonstrates an intact osborne's ligament (arrow) following the incision of the superficial fascia and between the two heads of the flexor carpi ulnaris. Ulnar nerve (*) and MABC (tagged, arrowhead).
Surgical management
Various techniques of ulnar nerve decompression are performed in the setting of failed conservative management: in situ decompression, medial epicondylectomy, and anterior transposition with submuscular, intramuscular, and subcutaneous routes. It should be noted that there remains a lack of consensus on which type of decompression technique is the best. Recent prospective randomized trials have failed to show any difference between simple (e.g. in situ) decompression, submuscular, or subcutaneous transposition.1 Submuscular anterior nerve transposition, however, is widely used in revision surgery with superior results.9 The medial antebrachial nerve is a cutaneous nerve that originates from the medial cord of the brachial plexus and innervates the skin of the anteromedial arm distally (Figure 3).10 Regardless of surgical method, care must be taken to identify this nerve to limit post-operative morbidity.
Case 1: In situ release/decompression
A minimalist but effective approach, simple decompression (in situ release) refers to decompression of the ulnar nerve by transection of the compressive structures including the intermuscular septum, Struther’s arcade (when present), the soft tissues overlying the post-condylar groove, Osborne’s ligament, and opening of the cubital tunnel (Figures 6–8).1 An accessory anconeus epitrochlearis muscle, if present, is resected. This method is typically viewed as the treatment of choice for primary cubital tunnel syndrome and theoretically carries less risk of damage to the associated nerve branches and perineural vasculature.
Figure 6.

In situdecompression. Insert shows transection of the superficial investing fascia and osborne's ligament, releasing the deeper ulnar nerve (yellow). Release from the more proximal sites of compression is also noted.
Figure 7.
Ulnar nerve discompression at the postcondylar groove. (a) Short axis ultrasound depicts a gap (arrows) between the superficial fascia stumps (*) extending between the humeral epicondyle (H) and the olecranon process following simple decompression of the ulnar nerve (u). Axial T2 weighted images following fat saturation depicts (b) An intact fascia (arrows) superficial to a thickened ulnar nerve (U) and (c) increased T2 signal (arrowheads) involving the medial aspect of the fascia (arrows) following decompression. [Olecranon process (O)].
Figure 8.
(a) Short axis ultrasound depicts a hypoechoic cleft (*) involving the superficial fascia and deep osborne's ligment between the FCU muscles following decompression. Ulnar nerve (U). (b) Axial T1 weighted image depicts the more distal division (double arrow) between the FCU (arrows). Ulnar nerve (arrowhead).FCU, flexor carpi ulnaris.
Medial epicondylectomy
No evidence exists to support medial epicondylectomy as a primary surgical technique for the treatment of ulnar nerve entrapment. Medial epicondylectomy may be performed in combination with a decompression in cases with severe bony deformity at the elbow.3
Case 2: Anterior subcutaneous transposition
Anterior subcutaneous transposition for ulnar nerve decompression was first described in 1898.11 This technique is employed to stabilize the nerve in patients with ulnar nerve instability with subluxation/dislocation over the medial humeral epicondyle. Some authors prefer this method of decompression in patients undergoing ulnar collateral ligament reconstruction with concomitant symptoms of ulnar neuropathy.12 The surgical technique comprises a simple decompression followed by anterior transposition of the nerve lateral to the medial epicondyle into a subcutaneous fatty sling (Figures 9–10). Particular attention should be given to transection of Osborne’s ligament and the intermuscular septum so as not to cause new points of entrapment/ kinking at these sites.
Figure 9.

Anterior subcutaneous ulnar nerve transposition. In subcutaneous transposition, the ulnar nerve is secured in a sling fashioned with the subcutaneous fat (insert).
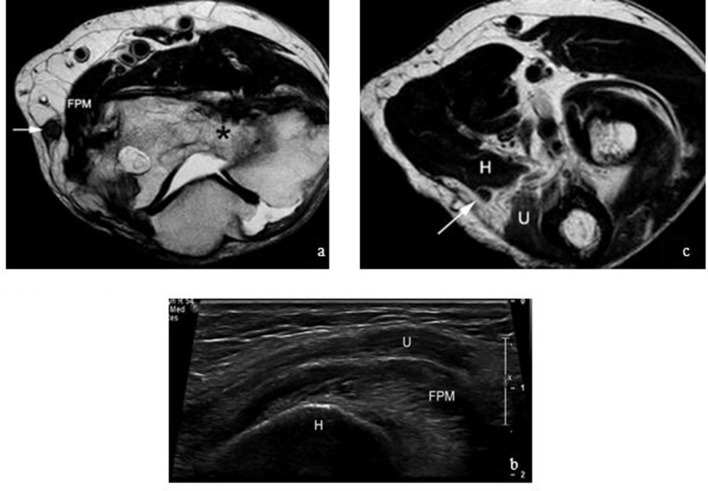
Figure 10.
Axial T2 weighted images (a) and long axis ultrasound (b) depict the course of the ulnar nerve (arrow, a; U, b) superficial to the flexor pronator muscle mass (FPM) . (c) more distally, the nerve (arrow) courses between the ulnar (U) and humeral (H) heads of the flexor carpi ulnaris muscles. (Post-traumatic deformity of the humerus -*, a). .
Case 3: Anterior submuscular transposition
Submuscular transposition of the ulnar nerve was developed to address some of the risks of subcutaneous transposition, notably post-traumatic ulnar neuritis from the superficial location of the nerve.11 Submuscular transposition is believed by many to be the treatment of choice with redo ulnar nerve decompressions and in the setting of extensive neurodesis from scar tissue with superior results over other techniques.9 In cases with inadequate subcutaneous fat, submuscular transposition may be preferred over subcutaneous transposition. The surgical technique comprises simple decompression followed by placement of the nerve under the pronator teres via a Z-plasty (Figures 11–12). Similar to the subcutaneous transposition, particular attention should be given to transection of Osborne’s ligament and the intermuscular septum.
Figure 11.

Anterior submuscular transposition. The ulnar nerve is positioned deep to a lengthened pronator teres muscle via a z-plasty (insert).
Figure 12.
(a) Axial T2 weighted image with fat saturation and (b). Long axis ultrasound image depict an anterier submuscular transposition with the ulnar nerve (arrow) deep to the FPM mass. Humerus (H). FPM, flexor pronator muscle.
Intramuscular transposition
Intramuscular transposition has been described in a few case reports but is not within the standards of care in the current literature.9
Endoscopic ulnar nerve decompression
Endoscopic ulnar nerve decompression has been practiced with positive results.12 The benefits include a smaller incision and less soft tissue dissection which causes less vascular insult to the nerve and results in faster recovery for the patient.13
Recalcitrant ulnar neuropathy
Failure to recognize dynamic ulnar nerve instability—idiopathic or induced after in situ nerve decompression—represents the most frequent procedural cause of unsuccessful surgery. This results in continuous snapping of the nerve over the epicondyle, causing friction of the nerve and kinking. Recurrent or persistent symptoms can also be attributed to: incomplete decompression, perineural fibrosis which creates new sites of nerve entrapment, and elbow stiffening in the flexed position.
Case 4: Focal kinking/angulation
Abrupt focal changes in the ulnar nerve caliber/morphology is suggestive of focal entrapment (Figure 13). Focal kinking/angulation or localized thickening in the area of the IMS and Osborne’s ligament are suggestive of incomplete dissection of these structures.
Figure 13.

Entrapment following anterior submuscluar transposition. Saggital T2 weighted images following fat saturation depict increased signal within the ulnar nerve and focal kinking/angulation of the ulnar nerve (arrows) due to inadequate release of osborne's ligament.
Case 5: Abnormal position
Dynamic evaluation of the ulnar nerve on ultrasound may identify ulnar nerve instability; not identified in the initial surgery or secondary to suboptimal anchoring of the ulnar nerve in the subcutaneous flap during anterior subcutaneous transposition (Figure 14). Instability and subluxation of the nerve following decompression should be addressed, typically with subcutaneous transposition.12
Figure 14.

Axial T2 weighted image with fat saturation depicts an inadequately positioned ulnar nerve following anterior subcutaneous transposition with the ulnar nerve in a posterier location (arrows) abutting the medial humeral epicondyle (*). FPM, Flexor pronator muscle mass.
Case 6: Scarring
The anterior soft tissue around the transposed nerve and epitrochlear region are known to be the most common sites for postoperative fibrosis (Figure 15).9 Early patient mobilization has been attributed to lower rates of perineural fibrosis and greater range of motion. On ultrasound, echogenic soft tissue change encompassing the nerve are suggestive of nerve entrapment by scar tissue. The goal in revision surgery is to free the nerve from the surrounding fibrosis and extend the ulnar nerve release.
Figure 15.
(a) Long axis ultrasound depicts a surgically coinfirmed “belt like” scarring (arrow) with focal narrowing of an ulnar nerve (U) at the level of the medial humeral epicondyle. Humerus (H). (b) short axis ultrasound image depicts a thick irregular IMS (arrows) correlating with surgically confirmed scarring with subluxation of the ulnar nerve (arrowheads) over the IMS. (Brachilias muscle, B; medial head triceps, T; humerus, H). IMS,intermuscular septum.
Summary
It is important for the radiologist who performs MRI or ultrasound of the elbow to be aware of the various points of ulnar nerve entrapment and the various types of transposition/decompression procedures that are performed. This will facilitate accurate and efficient diagnosis of abnormal and normal appearance of the ulnar nerve following ulnar nerve decompression or transposition.
Contributor Information
Nicholson Chadwick, Email: nicholson.s.chadwick@gmail.com.
Yoav Morag, Email: yoavm@med.umich.edu.
Brandon W Smith, Email: smithbw@med.umich.edu.
Corrie Yablon, Email: cyablon@med.umich.edu.
Sung Moon Kim, Email: sungmoon@med.umich.edu.
Lynda JS Yang, Email: ljsyang@med.umich.edu.
REFERENCES
- 1.Assmus H, Antoniadis G, Bischoff C, Hoffmann R, Martini AK, Preissler P, et al. Cubital tunnel syndrome - a review and management guidelines. Cent Eur Neurosurg 2011; 72: 90–8. doi: 10.1055/s-0031-1271800 [DOI] [PubMed] [Google Scholar]
- 2.Adkinson JM, Zhong L, Aliu O, Chung KC. Surgical treatment of cubital tunnel syndrome: trends and the influence ofpatient and surgeon characteristics. J Hand Surg Am 2015; 40: 1824–31. doi: 10.1016/j.jhsa.2015.05.009 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Bartels RH, Menovsky T, Van Overbeeke JJ, Verhagen WI. Surgical management of ulnar nerve compression at the elbow: an analysis of the literature. J Neurosurg 1998; 89: 722–7. doi: 10.3171/jns.1998.89.5.0722 [DOI] [PubMed] [Google Scholar]
- 4.Tagliafico AS, Bignotti B, Martinoli C. Elbow US: anatomy, variants, and scanning technique. Radiology 2015; 275: 636–50. doi: 10.1148/radiol.2015141950 [DOI] [PubMed] [Google Scholar]
- 5.Won HS, Han SH, Oh CS, Chung IH, Kim SM, Lim SY. Topographic relationship between the medial intermuscular septum and the ulnar nerve in the upper arm. J Neurosurg 2011; 114: 1534–7. doi: 10.3171/2011.1.JNS10210 [DOI] [PubMed] [Google Scholar]
- 6.Zhong S, Zhong Z, Yu Y, Yang L, Gao Y, Song J, et al. Ultrasonic observation and clinical application of arcade of struthers in the Mid-Arm. World Neurosurg 2016; 91: 560–6. doi: 10.1016/j.wneu.2016.03.061 [DOI] [PubMed] [Google Scholar]
- 7.Caetano EB, Sabongi Neto JJ, Vieira LA, Caetano MF. The arcade of struthers: an anatomical study and clinical implications. Rev Bras Ortop 2017; 52: 331–6. doi: 10.1016/j.rboe.2016.07.006 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Spinner M, Kaplan EB. The relationship of the ulnar nerve to the medial intermuscular septum in the arm and its clinical significance. Hand 1976; 8: 239–42. doi: 10.1016/0072-968X(76)90008-5 [DOI] [PubMed] [Google Scholar]
- 9.Vigasio A, Marcoccio I, Morandini E. Recalcitrant cubital tunnel syndrome. Plast Aesthet Res 2015; 2: 176–82. [Google Scholar]
- 10.Benedikt S, Parvizi D, Feigl G, Koch H. Anatomy of the medial antebrachial cutaneous nerve and its significance in ulnar nerve surgery: An anatomical study. J Plast Reconstr Aesthet Surg 2017; 70: 1582–8. doi: 10.1016/j.bjps.2017.06.025 [DOI] [PubMed] [Google Scholar]
- 11.Eberlin KR, Marjoua Y, Jupiter JB. Compressive neuropathy of the ulnar nerve: a perspective on history andcurrent controversies. J Hand Surg Am 2017; 42: 464–9. doi: 10.1016/j.jhsa.2017.03.027 [DOI] [PubMed] [Google Scholar]
- 12.Conti MS, Camp CL, Elattrache NS, Altchek DW, Dines JS. Treatment of the ulnar nerve for overhead throwing athletes undergoing ulnar collateral ligament reconstruction. World J Orthop 2016; 7: 650–6. doi: 10.5312/wjo.v7.i10.650 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Lui TH. Endoscopically assisted anterior subcutaneous transposition of ulnar nerve. Arthrosc Tech 2016; 5: e643–e647. doi: 10.1016/j.eats.2016.02.010 [DOI] [PMC free article] [PubMed] [Google Scholar]