Abstract
Background
Though primary malignant tumours of the heart are rare, secondary metastatic affection of the heart is quite common. Common presentations include pericardial effusion, obstruction of inflow and outflow tracts and arrhythmias, most notably tachyarrhythmias, and very rarely complete heart blocks (CHBs).
Case summary
A 28-year-old man suffering from carcinoma of the tongue underwent a surgery in the form of radical hemimandibulectomy. He presented with recurrent syncope and CHB with broad complex escape rhythm. After performing echocardiography, he was found to have malignant infiltration of the interventricular septum. This was confirmed by performing cardiac positron emission tomography (PET). It was decided that a permanent pacemaker would then be implanted. Post-implantation of permanent pacemaker patient succumbed to massive haemoptysis after 5 days.
Discussion
Although CHBs are rare in malignancy and careful assessment of ECGs especially looking for first degree heart blocks which may progress to CHB later on is prudent. One must rule out hypercalcaemia as it is a reversible cause of CHB. Careful echocardiogram can show hyper enhancement on interventricular septum and presence of pericardial effusion. Further imaging like cardiac magnetic resonance imaging or cardiac PET is confirmatory.
Keywords: Malignancy, Metastasis, Complete heart block, Interventricular septum, Case report
Learning points
Patients with malignancy (especially disseminated ones) can present with rhythm disturbances.
Although tachycardia is much more common, rarely there can be complete heart blocks can be present.
Simple investigations like repeated ECGs and a careful echocardiogram is enough to suspect. Further confirmation can be done by cardiac magnetic resonance imaging and cardiac positron emission tomography.
Introduction
In recent years many papers have described the affection of the heart by malignancy. It is well known that secondary tumours involve the heart far more frequently than primary tumours. However, the exact rates of incidence are lacking due to fragmentary data. Clinically metastatic tumours most often affect the pericardium and cause pericardial effusion rather than direct infiltration of the myocardium. Common malignancies that result in metastasis to the heart include melanoma and primary mediastinal malignancies.1 They can present with inflow and outflow tract obstructive lesions and arrhythmias.2 It is rare for such malignancies to present with complete heart block (CHB).3 We describe such a case that presented to our hospital.
Timeline
| Time | Events |
|---|---|
| 11 September 2017 | Patient diagnosed with malignancy |
| 15 September 2017 | Hemimandibulectomy done |
| 17 September 2017 | Post-operative local radiotherapy |
| 21 December 2017 11:00 AM | Patient presents to Emergency Room with repeated syncope |
| 21 December 2017 11:45 AM | Temporary pacing done |
| 22 December 2017 12:00 PM | Permanent pacemaker implanted |
| 26 December 2017 2:00 PM | Patient succumbed to massive haemoptysis |
Case presentation
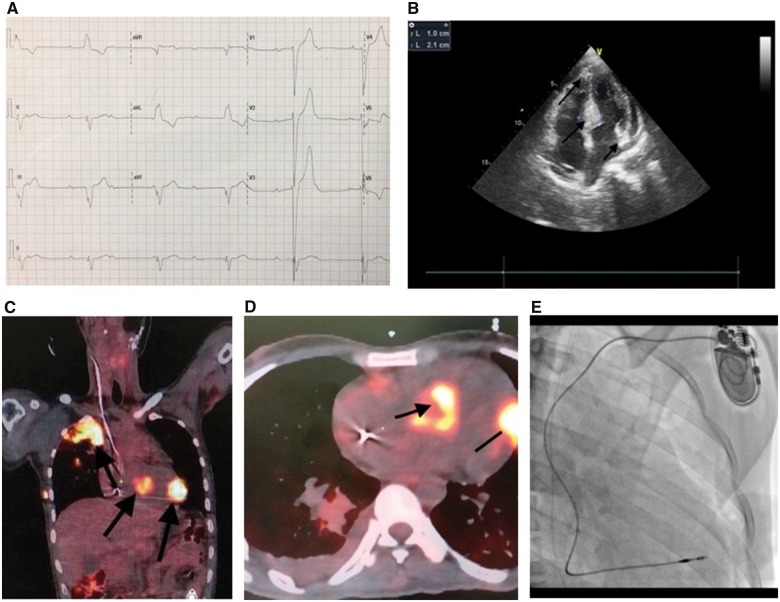
We report a 28-year-old man who was suffering from carcinoma of tongue and underwent hemimandibulectomy and post-operative radiotherapy. A histological diagnosis of squamous cell carcinoma was made. Three months later, he presented with multiple episodes of syncope to the emergency department. ECG showed CHB and a broad complex escape with left bundle branch block morphology (Figure 1A). These episodes were sudden in onset with no preceding symptoms. On physical examination, the patient had bradycardia with a regular heart rate of 32/min and normal blood pressure. On auscultation the chest was clear and there were no murmurs heard. Routine blood investigations were normal with normal serum creatinine 1.1 mg/dL (0.6–1.4 mg/dL) and normal serum sodium and potassium of 4.1 meq/dL (3.5–5.5 meq/dL). Echocardiography was performed which showed normal left ventricular ejection fraction and no valvular abnormalities. However, there were hyperechoic areas and hypertrophy of interventricular septum and the posterolateral wall of left ventricle as well (Figure 1B). The patient was paced using a temporary pacemaker as the patient was symptomatic with multiple episodes of syncope and had CHB on ECG with escape rate of 32 on ECG. The chest X-ray showed a large solitary nodule in the right upper zone. A positron emission tomography (PET) scan was performed and was suggestive of multiple metastasis in the interventricular septum, the right atrium, and the LV wall along with a large pulmonary metastasis (Figure 1C and D). The patient also developed paraneoplastic syndrome in the form of hypercalcaemia with serum calcium of 14 mg/dL (normal range: 8.5–10.2 mg/dL) which resolved on administering fluids and zoledronic acid intravenously. However, the CHB persisted despite normal calcium levels, so a decision to implant a permanent pacemaker was taken. The patient was then taken up for permanent pacemaker implantation and an active fixation lead was positioned into the low septal position in order to avoid metastatic site on the mid septal region. An active fixation lead was chosen as it is the institutional protocol to use active fixation lead (Figure 1E). A sensed R wave of 7 mV was achieved with a pacing threshold of 0.6 mV indicating a good position. Post-procedural ECG showed a ventricular paced rhythm. On the fifth day post-pacemaker implantation, the patient had massive haemoptysis. Crystalloids, and blood were transfused, but the patient succumbed before he could be taken up for bronchial artery embolization.
Figure 1.
(A) An ECG showing complete heart block and broad complex escape. (B) Four-chamber two-dimensional echocardiography showing infiltration in the interventricular septum and left ventricle (black arrows). (C and D) Secondaries in the positron emission tomography–computed tomographic images in coronal planes and transverse planes are shown. (E) Post-PPI image.
Discussion
Common malignancies known to metastasize to the heart are malignant melanomas and primary thoracic malignancies.1 Ours is the first case report published literature, in which metastatic spread of squamous cell carcinomas involving the tongue spread so extensively to the heart to cause a CHB. Initially when the patient was diagnosed with CHB and was found to have hypercalcaemia, it was thought that the CHB might be reversible on resolution of hypercalcaemia.5 However, when it did not resolve and hyper-echoic masses were seen of echocardiography, direct infiltration of interventricular septum was suspected. A cardiac PET was done to confirm infiltration. A permanent pacemaker was implanted. It is not yet known whether such metastatic malignant infiltrations respond to chemotherapy. More importantly it is also unknown whether the CHB would be reversible or not after treatment.6
Conclusions
The take-home message from this case report is that, in patients with history of malignancy or those who are suffering from malignancy, clinicians should be alert to the possibility of cardiac metastasis and hypercalcaemia-related rhythm disturbances even without clinical symptoms.2 Regular echocardiograms to look for effusion, hyperechoic masses on the interventricular septum on echocardiography should be looked for. Small prolongations in PR interval on routine ECGs during follow-up visits may be due to involvement of the conduction system, which may later lead to complete AV block, as in our case. Serum calcium levels should be done and if hypercalcaemia is found it must be corrected.5 However, even after resolution of hypercalcaemia if the CHB does not resolve then direct infiltration of septum by malignant cells should be suspected. Cardiac magnetic resonance imaging (MRI) and cardiac PET are useful investigations to look for direct infiltration of septum by malignant cells. We could not perform cardiac MRI as the patient was on a temporary pacemaker.2 Keen vigilance to rule out direct or indirect causes in patients with proven or suspected malignancies will help in planning management of such cases.
Supplementary Material
Acknowledgements
The authors thank Charan Lanjewar, DM Cardiology (Associate Professor and Head of Unit), Hetan C. Shah, DNB Cardiology (Associate Professor), and Prafulla G. Kerkar DM, DNB (Professor and Head) from the Department of Cardiology, Seth GS Medical College, KEM Hospital.
Slide sets: A fully edited slide set detailing this case and suitable for local presentation is available online as Supplementary data.
Consent: The author/s confirm that written consent for submission and publication of this case report including image(s) and associated text has been obtained from the patient in line with COPE guidance.
Conflict of interest: none declared.
References
- 1. Bussani R, De-Giorgio F, Abbate A, Silvestri F.. Cardiac metastases: a review. J Clin Pathol 2007;60:27–34. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2. Ozyuncu N, Sahin M, Altin T, Karaoguz R, Guldal M, Akyurek O.. Cardiac metastasis of malignant melanoma: a rare cause of complete atrioventricular block. Europace 2006;8:545–548. [DOI] [PubMed] [Google Scholar]
- 3. Vaduganathan M, Patel NK, Lubitz SA, Neilan TG, Dudzinski DM.. A “Malignant” arrhythmia: cardiac metastasis and ventricular tachycardia. Tex Heart Inst J 2016;43:559–560. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4. Buckberg GD, Noble O.. Fowler complete atrioventricular block due to cardiac metastasis of bronchogenic carcinoma. Circulation 1961;24:657–661. [Google Scholar]
- 5. Sudhir T, Joey S, Brian B.. Complete atrioventricular nodal block due to malignancy related hypercalcemia. Fed Pract 2016;33:23–25. [PMC free article] [PubMed] [Google Scholar]
- 6. Fotouhi Ghiam A, Dawson LA, Abuzeid W, Rauth S, Jang RW, Horlick E, Bezjak A.. Role of palliative radiotherapy in the management of mural cardiac metastases: who, when and how to treat? A case series of 10 patients. Cancer Med 2016;5:989–996. [DOI] [PMC free article] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.