Abstract
Background
In most developed countries there is an increasing ageing population living in the community with long-term conditions and sensory impairment (sight; hearing; dual impairment). Community pharmacy personnel are key providers of pharmaceutical care to this patient population.
Objective
This study explored community pharmacy personnel's experiences with providing pharmaceutical care for older people with sensory impairment.
Methods
Semi-structured telephone interviews were conducted with community pharmacy personnel across Scotland between 2015 and 2016.
Results
Thirty interviews were completed with community pharmacists (n = 17) and other pharmacy personnel (n = 13). Two overarching themes emerged: safety and communication. Interviewees reported patients' reluctance to disclose their impairment “patients are very good at hiding it” and had considerable safety concerns “it's a fear that they're going to take too much … accidentally taking the same medicine twice”. Difficulties in communication were cited “no matter what you do or how you label things, leaflets and telling people, things can go wrong”. Additionally, interviewees identified training needs to increase their disability awareness and to identify strategies to provide safe and reliable pharmaceutical care to this vulnerable group “We don't specifically have anything in place to deal with anyone with impairments of that kind”.
Conclusions
This is the first in-depth exploration of providing pharmaceutical care to older people with sensory impairment from the perspective of community pharmacy personnel. Strategies are needed to encourage older people to disclose their sensory impairment. Education and training are also needed to optimise the provision of pharmaceutical care to this vulnerable population.
Keywords: Pharmaceutical services, Visual impairment, Hearing impairment, Community pharmacies, Health services for the aged
Sight and hearing impairment (hereafter referred to as sensory impairment) are significant global health concerns and are the most common conditions associated with ageing. Sight loss and age-related eye conditions are a major cause of disability worldwide.1 Age-related hearing loss affects approximately one third of people aged ≥65 years.2 Sight or hearing impairment is associated with higher mortality and mortality is higher with dual compared with single impairment i.e. visual and hearing impairments.3
The number of long-term conditions increases with age and this is also reflected in an increased number of medicines taken, known as polypharmacy if four medicines or more are used.4 The Health Survey for England (2013)5 reported that more than half of those aged ≥65 years were using at least three medicines, and more than a third of those aged ≥75 years were taking at least six medicines, thus increasing the risk of adverse effects and drug interactions.
Demographic and functional characteristics e.g. male gender, cognitive or sensory impairment, are associated with greater medicine management needs and challenges among the older population.6, 7, 8, 9, 10, 11, 12 Community dwelling older adults are at higher risk of adverse drug reactions (ADRs) and hospital admission.13 Theses risks are exacerbated by inappropriate prescribing and monitoring of medications and polypharmacy.14,15
Older people with sensory impairment have reduced ability to manage medications and to achieve medication adherence compared with older people without sensory impairment,16,17 While there is a growing body of literature that focuses on medicine management of older people, most of this work has focused on nursing home residents.18, 19, 20 A recent scoping review revealed a paucity of research in this area.21
Pharmacists are increasingly involved in medication review to improve the pharmacotherapy of older patients.22, 23, 24, 25 The Sensory impairment and Pharmaceutical Care study26 was a research programme which explored the pharmaceutical care needs of older people with sensory impairment and the study presented here explored the perspectives of community pharmacy personnel regarding the provision of pharmaceutical care to this patient population.
Methods
For this element of the study, semi-structured, telephone interviews were undertaken with community pharmacy personnel between 2015 and 2016. The interviews aimed to explore community pharmacy personnel’ experiences with pharmaceutical care provision to older people with sensory impairments.
Interviewees, sampling and recruitment
Community pharmacy personnel (pharmacists and pharmacy support staff) were recruited across Scotland. Individuals who were members of the community pharmacy team and working in a community pharmacy in Scotland were eligible to participate. Community Pharmacy Scotland (CPS),27 the Scottish national contractor organization, supported recruitment on behalf of the project team. Recruitment of pharmacy personnel was guided by theoretical sampling28 following interviews with older people with sensory impairments that identified pharmaceutical care needs being partly dependent on the size and location of pharmacies. Pharmacies were then purposively recruited through Community Pharmacy Scotland, stratified by geographical variation (urban and rural) and pharmacy organisational type (independent, small chain, large multiple). The purpose of this was to achieve a maximum variation sample. Interviewees were contacted by email or telephone. Pharmacist respondents who expressed an interest in participating in the study were also requested to nominate another non-pharmacist member of their pharmacy team to participate. Interviews were conducted until data saturation was deemed to have been reached i.e. no new information relating to the topics of interest were obtained. Preliminary data analysis confirmed this to be the case.29,30
Procedure for data collection
All interviewees received a study information pack and a summary of the interview topic guide prior to the interview date. Interviewees were required to complete and return their written consent form prior to the interview. The semi-structured topic guide (Appendix A) was developed by the research team in consultation with the Project Advisory Group. The topics explored included: the participant's role in the pharmaceutical care for older people with sensory impairments; barriers and facilitators to providing pharmaceutical care; perceived risks to patients; and, participants' perceptions of relevant training. Pilot interviews were conducted and since no changes were suggested, pilot data were included in the final analysis. Interviews were conducted by (KK), a post-doctoral female health psychologist researcher, PhD.
Data management and analysis
All interviews were digitally recorded, transcribed verbatim and converted to anonymized word files. Transcripts were coded using NVivo (version 11) and analysed thematically.31,32 The process firstly used open coding which was followed by axial coding; categories and subcategories were identified and arranged conceptually in a hierarchy. Integrative memos were developed that linked the subcategories to each category to interpret the data.33 Two researchers (NA, AT) read all the interview transcripts and independently double-coded the first five to assess consistency of coding. Variations in coding were reviewed, discussed and agreed (NA, AT).34 The coding framework evolved inductively and iteratively from the data through this process. Detailed codes and theme descriptions were produced (NA, AT), and checked and finalised by NA, AT, MW, LM and AS (Appendix B). Due to the high levels of agreement achieved using this process, the remaining transcripts were coded by one researcher (NA). Illustrative quotes are presented with descriptors including anonymised health board (e.g. HB-A, HB-B) to protect the confidentiality of the interviewees (Health board is a term used in Scotland to describe a geographical area with relation to the delivery of health services in that area). Triangulation of these data is reported elsewhere using data from service user interviews and a national survey of community pharmacists.35
Formal ethical review approval was received from the University of Dundee Research Ethics Committee (January 2016: Ethics Review reference number 15187). NHS ethical approval was not required.
Results
The sample was diverse with respect to different types of pharmacy personnel. Thirty interviews were completed comprising pharmacists (n = 17), pre-registration pharmacists (n = 5), medicine counter assistants (n = 4), trainee pharmacy technicians (n = 2), dispensers (n = 1), and a pharmacy retail manager (n = 1). Just over half the interviewees (17) worked in independent, single outlet pharmacies (Table 1). Data saturation was achieved with no new themes emerging in the later interviews.29,30 The interviews lasted up to 27 min.
Table 1.
Demographic characteristics of Community pharmacy personnel interviewees.
| Role (total number interviewed) | Number of years in practice (mean ± SD) | Pharmacy ownership (number interviewed) | Health board (number of participants interviewed) |
|---|---|---|---|
| Pharmacist (17) | 21 ± 10.5 | Independent (11), Large multiple (3), Others (3) | Grampian (3), Tayside (5), Highlands & Islands (2), Edinburgh & Lothian (2), Others (5) |
| Pre-registration pharmacist (5) | <1 | Large multiple (5) | Edinburgh & Lothian (2), Others (5) |
| Other community pharmacy personnel: medicines counter assistant (4), trainee technician (2), dispenser (n = 1), pharmacy retail manager (n = 1) | 9 ± 8 | Independent (6), Small chain (2) | Grampian (3), Tayside (3), Others (2) |
Others: when the number is one, data were combined to avoid the risk of identification.
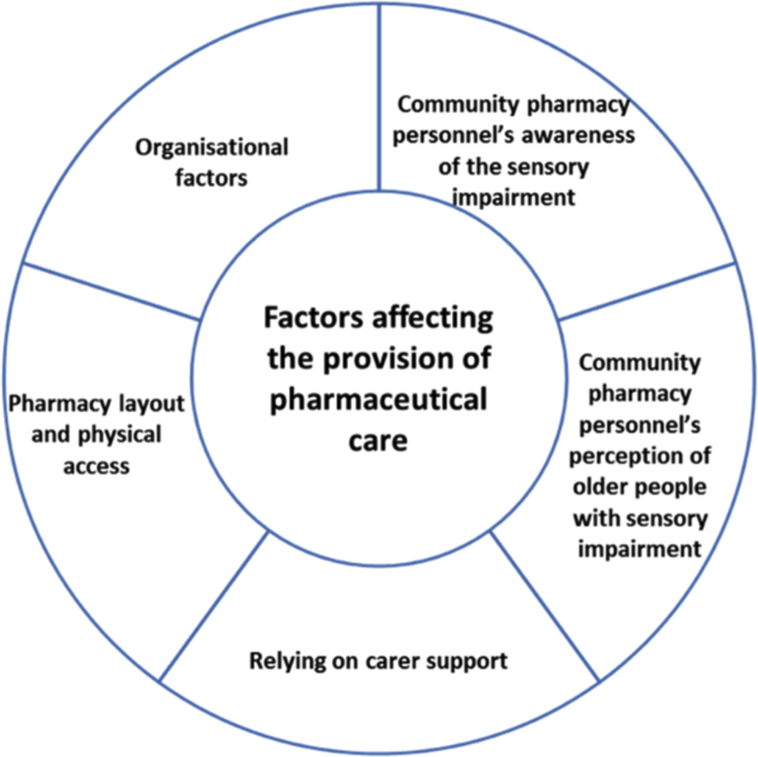
Four themes emerged from the analyses: two overarching inter-related themes, safety and communication; and two additional themes: factors affecting the provision of pharmaceutical care to this patient population (Fig. 1); and, solutions. Safety and communication concerns permeated all aspects of pharmaceutical care discussed.
Fig. 1.
Factors affecting the provision of pharmaceutical care to older people with sensory impairment from the perspective of Community pharmacy personnel.
Safety
Perceived failure to provide suitable pharmaceutical care caused community pharmacy personnel concerns about patient safety. Interviewees were concerned about patient safety at all stages of the pharmaceutical care journey i.e. from the ordering of medicines to their storage and administration.
Several interviewees raised concerns and safety issues about the use of multi-compartment compliance aids i.e. devices divided into compartments, each one denoting a single dosing occasion.36 These problems included: the small font size on the dosage form; the risk of overdose when switching to use these systems; dropping tablets due to packaging access problems; losing independence; and side effects due to a concurrent administration of several medicines (Table 2). One participant suggested doing home visits to provide explanation about the devices and follow-up visits to patients benefiting from delivery service or the multi-compartment compliance aids service.
“so if it's a new one [multi-compartment compliance aid] I would go out to the house and we explain it [how to use the multi-compartment compliance aids] to them [patients] first, and you know how to take their medicine, and how they get into the pack, and exactly what is going to happen” (ID8, Trainee Technician, Independent, HB-H)
Table 2.
Perceived risks related to multi-compartment compliance aids for older people with sensory impairment.
| Small Print | “so the [multi-compartment compliance aids] is Monday, Tuesday, Wednesday, Thursday, Friday, morning, lunchtime, teatime, bedtime, and this gentleman had taken morning, morning, morning, morning … but with a little bit of impaired sight he just kept going down the line” (ID12, pharmacist, independent, HB-H) |
| Danger of overdose when starting a multi-compartment compliance aids | “There is the other option of us putting them into the bubble packs [multi-compartment compliance aids] and you'll often find patients will start on the bubble pack [multi-compartment compliance aids] who weren't taking them properly before and we'd put them in the right times and they'd start taking them at the right times … and then they're overprescribed. They're hospitalized … It does expose a big problem in some cases” (ID17, pharmacist, small chain, HB-B) |
| Dropping medicine form the multi-compartment compliance aids | “For example, I remember an elderly lady who was in her 90s who had some form of visual impairment … She said yes, I pop them out and they fall on the floor I can't find them because I can't see. Even if I could see them I couldn't bend down to pick them up, I'm 94” (ID21, pharmacist, independent, HB-D) |
| Losing independence and confidence | “It can become quite messy. I just think it removes the independence and thinking behind the medicines and actually that is not necessarily the safest way to go” (ID22, pharmacist, independent, HB-F) |
| Side effects | “So, there's one medication has to be taken on its own and tends not to go in a tray, but the GP had insisted it went in the tray. She was having all sorts of gastro-intestinal problems” (ID12, pharmacist, independent, HB-H) |
| Can't distinguish between the tablets | “if you made it up with a patient pack, if for example a doctor stops then one of the medications, if they've not good sight, it's then that they've got problems over which tablet they actually take out” (ID25, pharmacist, independent, HB-C) |
| Pressure on the pharmacy | “We are a small pharmacy; we do about 4000 [prescription items] per month. But I have between 65 and 75 patients on trays at the moment” (ID14, pharmacist, independent, HB-F) |
Most interviewees acknowledged that patients with sight impairment rely on the texture, shape, size, and colour of the tablets and their boxes to identify medicines. Several interviewees reported using extra identification marks to help their patients, for example coloured stickers, rubber bands, different box sizes. Many interviewees also reported that pharmaceutical companies frequently change a medicine's brand image and this added to the complexities that these patients experience in managing their medicines.
“We have medications out there that one day it'll come in a box that size, and from another manufacturer it'll be in a box that size. They go from big, white round things, to little pink triangular shape things, and that's a problem” (ID12, Pharmacist, independent, HB-H).
Several adverse incidents were reported by the interviewees.
“I told him to take eight tablets, all at once, every day for five days. His carer was with him who also repeated it, then he went away home and had [took] it all at once and took them all … because all he heard was all at once” (ID24, Pharmacist, HB-I)
Other concerns included the risk of using narrow therapeutic index medicines, where there is only a small difference between the minimum effective concentrations and the minimum toxic concentrations in the blood, such as anticoagulants in this patient population.
“If they are on … an anticoagulant or something you would need to communicate with them what to look out for, extra bleeding and things like that; depends if they would understand that, depends if you get that across to them” (ID3, Pre-registration Pharmacist, Small chain, HB-A)
Communication
Ineffective communication between community pharmacy personnel and older patients with sensory impairment was reported to influence the quality of the pharmaceutical care journey. For example, some patients with hearing impairment were perceived to nod and indicate that they heard the pharmacist while actually having heard only part of the instructions. Additional concerns regarding hearing impairment included: provision of information to patients; inability to test the understanding of patients; not understanding the patient's needs; not using hearing loops; and difficulties with telephone communication.
“you do get halfway through a consultation and you realise that someone's … smiling and not saying anything …” (ID30, pre-registration pharmacist, multiple chain)
Some interviewees reported speaking louder and gesturing with people with hearing impairment. Others reported writing instructions, giving reading material or lip reading. Sign language was used when a member of staff had this expertise. Some interviewees reported using images and videos from the internet, text messages, and emails as communication aids. However, several interviewees noted that not all patients use sign language and written information might be complex for deaf people.
“She has no hearing, she lip-reads and signs, and it wasn't until maybe five or ten minutes of trying to understand what was wrong with her, that I realised one of the girls who works in the shop actually does have sign language, and from that within a minute we were able to find out what was wrong” (ID11, Pharmacist, Independent, HB-H)
“Does Mr so and so read, does he write? If I wrote something down would that help? … So if he is a ‘signer’ [uses sign language] and has never learned the English language as such, then maybe I've been doing it wrong.” (ID17, Pharmacist, Small chain, HB-B)
For older patients with sight impairment, concerns were raised relating to their ability to read patient information sheets and labels. Using large print, Braille and giving verbal instructions were examples of information provision or communicating with people with varying degrees of sight impairment. Whilst large print was popular between the interviewees, several limitations were highlighted and included the extent to which it could actually help, and how much information could be printed in large font. Whilst the provision of verbal instructions was suggested as a solution to these difficulties, interviewees were concerned that patients who were receiving polypharmacy and/or with memory loss would be unable to retain all the relevant information. One interviewee suggested that speaking labels might help.
I would say none of my visual impaired people could read Braille because they're not blind and they haven't been blind since birth” (ID22, pharmacist, independent, HB-F)
“I think the sight loss is the most challenging because they can't read any labels and if someone tells you what to do by the time you get home you have forgotten, so I imagine if I had polypharmacy and it was all being done verbally it would be very, very confusing” (ID2, pharmacist, small multiple, HB-A)
Interviewees identified that patients with sight impairment often needed help in signing the prescription (a legal requirement in Scotland to prevent fraud) and those with hearing impairment may not hear their names called in the pharmacy when their prescription medicines were ready. Some respondents commented that home delivery schemes (delivering prescription medicines to the patient's address) meant that they had less direct, in-person contact with patients, and thus missed opportunities for involvement in their ongoing pharmaceutical care needs.
“These patients are now being cared for with delivery services and things. So it's more the delivery driver who sees them on a week to week and a month to month basis rather than the pharmacist, which is a bit of shame” (ID1, Pharmacist, Supermarket, HB-A)
Most responses from interviewees addressed either hearing or sight impairment; there was little mention of dual sensory impairment. Interviewees tended to be unsure how to communicate with patients with dual sensory impairment and when dual impairment was identified, there was strong reliance on the carer (if the patient had one).
“Usually the people like that [with dual impairment] would come in with a carer or usually next of kin or wife, husband, anything like that but I honestly don't know to be honest … Um-hum, which obviously isn't the best way; ideally we would be providing the information directly to him” (ID3, Pre-registration Pharmacist, Small chain, HB-A)
Factors affecting the provision of pharmaceutical care
Five factors were identified within this theme, which were perceived to influence the pharmaceutical care of older patients with sensory impairment: community pharmacy personnel's awareness of the sensory impairment; community pharmacy personnel's perception of older people with sensory impairment; relying on carer support; pharmacy layout and physical access and organisational factors (Fig. 1).
Interviewees were not always aware of a patient's sensory impairment. Where they were aware, the impairment was often inferred from the presence of visual cues such as sensory aids (e.g. hearing aids) or requests to speak up. Interviewees suggested that people with sensory impairment ‘hid’ their impairment, commenting that this was possibly as means of maintaining their independence or avoiding feelings of embarrassment.
“Sometimes people are very good at hiding their impairment … you do get halfway through a consultation and you realise that someone's just been “kind of smiling and not saying anything … there might be an element of embarrassment … to ask you to repeat things or when they need that little extra help” (ID30, pre-registration pharmacist, multiple chain, HB-E)
“Really good at hiding it and especially if it is really hectic. When they are coming into an environment that they are very familiar with they know how many steps to take forward to the counter and that the biro is on the left and they really can look like they are managing very well” (ID5, Pharmacist, Independent, HB-A)
The need/desire for independence was perceived by pharmacy personnel to be the main characteristic of this patient population. There was uncertainty about whether patients would accept additional assistance. Problems with medicines adherence were attributed to patients “being stubborn” and not accepting assistance offered. Other interviewees suggested that due to sensory impairment, patients were probably fearful of taking the wrong medicine at the wrong time, not understanding their medicines, fearing overdose and side effects alongside depression, loss of control and lack of confidence.
“She's so feisty and so independent, you know if you looked at her medical record, you'd think ‘how is she living?’ Independently, she's clearly found ways to deal with it and to be extremely independent, and we have a role to help keep her living as independently as she'd like to be” (ID15, pharmacist, independent, HB-G)
Some interviewees assumed that older people usually have carers helping them in their everyday activities, and that this included managing their medicines. Other interviewees discussed that when the carer was the spouse, they might also have sensory impairment or other conditions such as dementia, or may have died leaving the person with sensory impairment living alone. When formal carers were present, there were variations in services offered by different agencies.
“Most of these patients would have some support that would take on that role and we could do that via a third party. I can't think of any instance where we have an isolated patient that would have no help in that situation, so it hasn't proved to be a problem for us … I mean carers of some kind to help them with any medication, polypharmacy” (ID2, pharmacist, small multiple, HB-A)
Other factors included organisational and environmental (pharmacy layout) problems such as noise levels in the pharmacy which affects hearing, and problems with pharmacy lighting and signage, social stigma around hearing impairment, lack of access to patient records, time constraints – since this patient group needed more time to ensure good consultations, workload, insufficient staffing, role delegation in the pharmacy and compliance with regulations.
“the background noise can be a problem in the pharmacy. I find it difficult to hear sometimes,” (ID12, pharmacist, independent, HB-H)
“So we've tried to make the environment great for, or better, because community pharmacies are traditionally pretty poor in terms of lighting and signage and things. And that involves getting the person through the door. So I think if somebody comes through the door, then we have lots of tools available” (ID15, pharmacist, independent, HB-G)
“[Pharmacy] companies are taking away staff or not replacing staff when they leave. So therefore, everyone becomes more stretched and everyone has to do more with that same amount of time. Therefore, you don't have the same amount of time to spend with customers or your patients” (ID1, pharmacist, supermarket, HB-A)
Solutions
Participants in the study suggested generic and focussed solutions for improving pharmaceutical care that included raising awareness of the difficulties faced by patients with sensory impairment as a result of communications and environmental barriers and good examples of practice where the pharmaceutical care needs of this patient population had been met. Most interviewees discussed training needs in relation to providing appropriate pharmaceutical care for this patient population. A range of training needs was identified for pharmacists as well as other pharmacy personnel - counter assistants, technicians and drivers – and included: skills in identifying people with sensory impairment; enhanced communication techniques, for example, interpersonal skills on how to approach someone with a sensory impairment without patronising them; training in sign language; and use of sensory aids such as hearing loops.
“It [training course] opened my eyes to some things. I just assumed, I think like a lot of people, that deaf people are just able to read. I was really shocked that a lot of them can't. The other thing is that BSL [British Sign Language] is completely different. I just thought it'd be our spoken language translated visually but the fact is that it’s a completely different language really. I thought as well hearing aids and the implant … I thought that just fixed your hearing” (ID19, Trainee Technician, Small chain, HB-I)
Some interviewees described specific approaches to help with providing pharmaceutical care for older people with sensory impairment, including: simplifying complex dosing schemes; counselling at home; notes on sensory needs in patient files; medicines administration records chart; consulting the patient about what could help them and providing hearing tests in the pharmacy. One participant also suggested having a referral system to specialist pharmacists trained to communicate with people with hearing or sight impairment.
“We have one patient with sight loss who can't see at all so what we actually do for that patient is we have an arrangement with her that she gets tablets she takes in the morning and tablets she takes at night. We deliver to this patient because she finds it difficult to get [here] because she can't see and she lives in the countryside” (ID20, pharmacist, independent, HB-H)
“I went out and did a house visit to an elderly gentleman who is struggling with his medicine. He was fairly, in fact almost completely deaf … and was being aided by his carer, but the carer was concerned when she wasn't there because he was an elderly gentleman living by himself. He was taking extra tablets and things like that. So we decided to do a full review and the upshot of it was he ended up getting a [multi-compartment compliance aid] but we had to ascertain what he had taken, what time suited him and things like that” (ID21, pharmacist, independent, HB-D)
Discussion
This study has highlighted the experiences and perspectives of community pharmacy personnel in relation to providing pharmaceutical care for older people with sensory impairment and polypharmacy. Of importance (and concern) is that interviewees reported that these patients do not tend to disclose their sensory impairment to community pharmacy personnel and the latter seldom have systems for identifying people with these types of impairment. The results indicate a need to train pharmacy personnel to: recognise sensory impairments; understand disability etiquette and communication skills in interacting with older people with sensory impairments; raise awareness of the challenges encountered by this patient population; use sign language and/or sensory aids such as hearing loops and other innovative technologies; and, how to best manage medication for older people with sensory impairment.
Previous studies report that patients with hearing impairment do not report medication side effects to their pharmacists37 and that individuals with sight impairment do not tell their healthcare professionals about their difficulties with their medicines.38 Non-disclosure, or failure to identify the sensory impairment, means that the pharmaceutical care provided is unlikely to reflect individual patient's needs in addition to increasing risk with medication safety. This problem is further compounded by the lack of direct contact with community pharmacy personnel on pharmacy premises due to the increasing use of delivery services.
Some problems identified are common across people with sensory impairment irrespective of age. Others, however, are unique to older individuals who are more likely to receive polypharmacy (the focus of this study), such as: the use of multi-compartment compliance aids and delivery services; dropping tablets on the floor due to packaging problems and motor disorders; inability to retain information due to memory loss; pharmacy personnel's perception of older people as stubborn; and the inability of older people to use sign language or Braille. There is also a concern that older people with sensory impairment are more likely to develop Alzheimer's disease or dementia, compared with those unaffected by these conditions.39 This adds to the problem of managing medicines in this patient population.
To tackle these challenges, Health and Social Services and older people with sensory impairment could be consulted to develop strategies to develop approaches for supportive disclosure of patients' sensory impairment to health care professionals in general, including community pharmacy personnel. For example ‘SEE HEAR’, a strategic framework for meeting the needs of people with a sensory impairment in Scotland,40 recommends: “the introduction of basic sensory checks for people of a certain age, and at agreed times in their care pathway”; the provision of training programs for frontline staff to increase their awareness of sensory impairments; and sharing information between agencies in relation to people who have received a diagnosis of a sensory impairment at any time from birth onwards.
In this study, methods that were used to support older people with sensory impairment in community pharmacy included writing instructions, sign language, Braille and large print. Although considered beneficial, these methods were of limited value for some individuals as demonstrated by the examples above. Similarly, in a study of the communication of patients with altered hearing ability, patients struggled with the complexity of written information given to them.37 This earlier study suggest that if written instructions are provided, the patient's reading ability should be accommodated and their comprehension of the information assessed, for example, by using Teach Back (when the health professional asks the patient to feedback what they understood from the information given to them).41
The European Commission issued general guidelines to improve the readability of medical product labelling.42 These recommendations include the use of Braille, font size: Sans serif typefaces, 16–20 point for text and/or in a format perceptible by hearing for the blind and partially sighted patients. The use of 22 point Arial significantly improved the comprehension and adherence of patients with visual acuity less than 6/18.43 However, most prescription directions are currently printed in font sizes two to three times smaller than this.43 In the UK, the Design for Patient Safety series44 considered “how better design can reduce risk, improve the working environment, and ensure better, patient-centred care”. Their guidelines included recommendations about packaging design, labelling, the design of the dispensing environment and the graphic design of medication packaging. Other guidelines have recently (after the interviews in this study were conducted) been produced in the UK for pharmacy staff regarding how to support patients with sight impairment in pharmacy.45 All the above recommendations and guidelines could be adopted by pharmaceutical companies and pharmacies to address the safety problems caused by current difficulties in communication with this patient group, in particular packaging and the dispensing environment.
This study revealed that most interviewees addressed either hearing or sight impairment; there was little mention of dual sensory impairment. This points to the need for improving guidelines and resources for community pharmacy personnel to help people with a dual sensory impairment. Most recently, a group of international experts identified eight future research priorities to optimise geriatric pharmacotherapy,46 which highlighted vulnerable patient groups, polypharmacy and person-centred practices.
There is a need for the development of evidence-based strategies to support older people with sensory impairment managing their medicines safely and effectively. Pharmacy curricula in undergraduate and post-graduate training programmes require review to ensure that the training needs identified in this study are addressed. Strategies to improve medication adherence of older people include the use of personal systems, regular medication review and community-driven support systems and medical advocates.47 It also follows that taking the aforementioned steps will also have positive impact on the pharmaceutical care the wider population living sensory impairment.
Study limitations and strengths
The study generated rich data and a range of perspectives by interviewing different members of the pharmacy team and not solely pharmacists. Whilst data collection was only conducted to Scotland, it is likely that the findings will be of relevance to community pharmacy personnel elsewhere, due to the nature of the topic under investigation. Due to time constraints arising mainly from an extended period of recruitment, the interviewees were not asked to review or comment on their transcripts or the findings.
Conclusion
Despite the growing prevalence of sensory impairment due to the ageing population, this is the first comprehensive exploration of community pharmacy personnel's perspectives and experiences of providing pharmaceutical care to older people with sensory impairment. It is also one of the first studies to consider intersectional challenges in the development of support guidelines that are not single condition-focused in the pharmaceutical management of older people. Whilst many challenges were identified, a number of potential solutions were also suggested. Strategies which encourage sensory impairment disclosure or identification need to be established. The unmet training and educational needs of community pharmacy personnel, as well as the need for technological innovations, warrant attention to optimise the provision of pharmaceutical care to this patient population.
Disclosures/conflict of interest
All authors confirm no conflict of interest.
Funding
We are grateful to the Chief Scientist Office, Scottish Government which funded this study (CZH/4/1113).
Acknowledgements
We thank all the community pharmacy personnel who participated in these interviews and Community Pharmacy Scotland for assisting with the dissemination of information as part of the recruitment process.
Footnotes
Supplementary data to this article can be found online at https://doi.org/10.1016/j.dhjo.2018.10.006.
Contributor Information
N. Alhusein, Email: N.alhusein@bath.ac.uk.
K. Killick, Email: k.killick@napier.ac.uk.
L. Macaden, Email: leah.macaden@uhi.ac.uk.
A. Smith, Email: annetta.smith@uhi.ac.uk.
K. Stoddart, Email: k.m.stoddart@stir.ac.uk.
A. Taylor, Email: A.D.J.Taylor@bath.ac.uk.
T. Kroll, Email: Thilo.kroll@ucd.ie.
M.C. Watson, Email: m.c.watson@bath.ac.uk.
Appendix A. Supplementary data
The following are the Supplementary data to this article:
References
- 1.Bourne R., Price H., Stevens G. Global burden of visual impairment and blindness. Arch Ophthalmol. 2012;130(5):645–647. doi: 10.1001/archophthalmol.2012.1032. [DOI] [PubMed] [Google Scholar]
- 2.World Health Organisation. http://www.who.int/en/news-room/fact-sheets/detail/deafness-and-hearing-loss (Access date 18/7/2018).
- 3.Lam B.L., Lee D.J., Gómez-Marín O., Zheng D.D., Caban A.J. Concurrent visual and hearing impairment and risk of mortality: the National Health Interview Survey. Arch Ophthalmol. 2006;124(1):95–101. doi: 10.1001/archopht.124.1.95. [DOI] [PubMed] [Google Scholar]
- 4.Hughes C.M., Cooper J.A., Ryan C. Going beyond the numbers - a call to redefine polypharmacy. Br J Clin Pharmacol. 2014;77(6):915–916. doi: 10.1111/bcp.12284. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Scholes S., Faulding S., Mindell J. Use of prescribed medicines. NHS health survey for England–2013. London. Health Soc Care Inform Centre. 2014;2 http://digital.nhs.uk/catalogue/PUB16076 [Google Scholar]
- 6.Jamerson B.D., Fillenbaum G.G., Sloane R., Morey M.C. A new method of identifying characteristics of needing help to take medications in an older representative community-dwelling population: the older adults medication assist scale. J Am Geriatr Soc. 2016;64(6):1195–1202. doi: 10.1111/jgs.14166. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Marcum Z.A., Duncan N.A., Makris U.E. Pharmacotherapies in geriatric chronic pain management. Clin Geriatr Med. 2016;32(4):705–724. doi: 10.1016/j.cger.2016.06.007. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Wood K., Gibson F., Radley A., Williams B. Pharmaceutical care of older people: what do older people want from community pharmacy? Int J Pharm Pract. 2015;23(2):121–130. doi: 10.1111/ijpp.12127. [DOI] [PubMed] [Google Scholar]
- 9.Stauffer Y., Spichiger E., Mischke C. Complex drug regimen in multimorbid elderly patients after hospital discharge - a qualitative study. Pflege. 2015;28(1):7–18. doi: 10.1024/1012-5302/a000400. [DOI] [PubMed] [Google Scholar]
- 10.Sinnige J., Braspenning J.C., Schellevis F.G. Inter-practice variation in polypharmacy prevalence amongst older patients in primary care. Pharmacoepidemiol Drug Saf. 2016;25(9):1033–1041. doi: 10.1002/pds.4016. [DOI] [PubMed] [Google Scholar]
- 11.Sinnige J., Korevaar J.C., van Lieshout J., Westert G.P., Schellevis F.G., Braspenning J.C. Medication management strategy for older people with polypharmacy in general practice: a qualitative study on prescribing behaviour in primary care. Br J Gen Pract. 2016;66(649):e540–e551. doi: 10.3399/bjgp16X685681. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Orlu-Gul M., Raimi-Abraham B., Jamieson E. Public engagement workshop: how to improve medicines for older people? Int J Pharm. 2014;459(1-2):65–69. doi: 10.1016/j.ijpharm.2013.11.024. [DOI] [PubMed] [Google Scholar]
- 13.Beijer H.J., de Blaey C.J. Hospitalisations caused by adverse drug reactions (ADR): a meta-analysis of observational studies. Pharm World Sci. 2002;24(2):46–54. doi: 10.1023/a:1015570104121. [DOI] [PubMed] [Google Scholar]
- 14.Spinewine A., Schmader K.E., Barber N. Appropriate prescribing in elderly people: how well can it be measured and optimised? Lancet. 2007;370(9582):173–184. doi: 10.1016/S0140-6736(07)61091-5. [DOI] [PubMed] [Google Scholar]
- 15.Maher R.L., Hanlon J., Hajjar E.R. Clinical consequences of polypharmacy in elderly. Expet Opin Drug Saf. 2014;13(1):57–65. doi: 10.1517/14740338.2013.827660. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Crews J.E., Campbell V.A. Vision impairment and hearing loss among community-dwelling older Americans: implications for health and functioning. Am J Public Health. 2004;94(5):823–829. doi: 10.2105/ajph.94.5.823. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.McCann R.M., Jackson A.J., Stevenson M., Dempster M., McElnay J.C., Cupples M.E. Help needed in medication self-management for people with visual impairment: case-control study. Br J Gen Pract. 2012;62(601):e530–e537. doi: 10.3399/bjgp12X653570. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Ahmad Nizaruddin M., Omar M.S., Mhd-Ali A., Makmor-Bakry M. A qualitative study exploring issues related to medication management in residential aged care facilities. Patient Prefer Adherence. 2017;11:1869–1877. doi: 10.2147/PPA.S144513. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Lerch M., Decker-Maruska M., Dettmar-Flügge A. The EAMA project “Hearing impairment in geriatrics”-a European multicenter survey. Eur Geriatr Med. 2010;1S:S90–S160. doi: 10.1016/j.eurger.2010.07.009. [DOI] [Google Scholar]
- 20.Saliba D., Solomon D., Rubenstein L. Quality indicators for the management of medical conditions in nursing home residents. J Am Med Dir Assoc. 2004;5:297–309. doi: 10.1097/01.JAM.0000136960.25327.61. [DOI] [PubMed] [Google Scholar]
- 21.Killick K., Macaden L., Smith A., Kroll T., Stoddart K., Watson M.C. A scoping review of the pharmaceutical care needs of people with sensory loss. Int J Pharm Pract. 2018;26:380–386. doi: 10.1111/ijpp.12456. [DOI] [PubMed] [Google Scholar]
- 22.Lee J.K., Alshehri S., Kutbi H.I., Martin J.R. Optimizing pharmacotherapy in elderly patients: the role of pharmacists. Integrated Pharm Res Pract. 2015;4:101–111. doi: 10.2147/IPRP.S70404. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.Spinewine A., Fialova D., Byrne S. The role of the pharmacist in optimizing pharmacotherapy in older people. Drugs Aging. 2012;29(6):495–510. doi: 10.2165/11631720-000000000-00000. [DOI] [PubMed] [Google Scholar]
- 24.Lee J.K., Alshehri S., Kutbi H.I., Martin J.R. Optimizing pharmacotherapy in elderly patients: the role of pharmacists. Integrated Pharm Res Pract. 2015;4:101–111. doi: 10.2147/IPRP.S70404. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25.Ellitt G.R., Brien J.A., Aslani P., Chen T.F. Quality patient care and pharmacists' role in its continuity--a systematic review. Ann Pharmacother. 2009;43(4):677–691. doi: 10.1345/aph.1L505. [DOI] [PubMed] [Google Scholar]
- 26.Sensory Impairment and Pharmaceutical Care, https://sipaproject.wordpress.com/. (Accessed 02 March 2018).
- 27.Community Pharmacy Scotland. http://www.communitypharmacyscotland.org.uk/(Access date 2/3/2018).
- 28.Draucker C.B., Martsolf D.S., Ross R., Rusk T.B. Theoretical sampling and category development in grounded theory. Qual Health Res. 2007;17(8):1137–1148. doi: 10.1177/1049732307308450. [DOI] [PubMed] [Google Scholar]
- 29.Marshall M.N. Sampling for qualitative research. Fam Pract. 1996;13(6):522–525. doi: 10.1093/fampra/13.6.522. [DOI] [PubMed] [Google Scholar]
- 30.Fusch P., Ness L. Are we there yet? Data saturation in qualitative research. Qual Rep. 2015;20(9):1408–1416. [Google Scholar]
- 31.Braun V., Clarke V. Using thematic analysis in psychology. Qual Res Psychol. 2006;3(2):77–101. [Google Scholar]
- 32.Saldana J. third ed. ed. Sage; London, Thousand Oaks: 2015. The Coding Manual for Qualitative Researchers. [Google Scholar]
- 33.Sarker S., Lau F., Sahay S. Using an adapted grounded theory approach for inductive theory building about virtual team development. ACM SIGMIS - Data Base: Database Adv Inform Syst. 2001;32(1):38–56. doi: 10.1145/506740.506745. [DOI] [Google Scholar]
- 34.Campbell J.L., Quincy C., Osserman J., Pedersen O.K. Coding in-depth semi-structured interviews: problems of unitization and intercoder reliability and agreement. Socio Methods Res. 2013;42(3):294–320. http://psycnet.apa.org/doi/10.1177/0049124113500475 [Google Scholar]
- 35.Alhusein N., Macaden L., Smith A. “Has she seen me?”: a multiple methods study of the pharmaceutical care needs of older people with sensory impairment in Scotland. BMJ open. 2018;8 doi: 10.1136/bmjopen-2018-023198. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 36.National Institute for Health and Care Excellent Medicines Adherence: Medicines Problems Associated with Use of Multi-compartment Compliance Aids in a UK Community Setting. 2017. http://arms.evidence.nhs.uk/resources/hub/1059852/attachment
- 37.Ferguson M., Liu M. Communication needs of patients with altered hearing ability: informing pharmacists' patient care services through focus groups. J Am Pharmaceut Assoc. 2003;55(2):153–160. doi: 10.1331/JAPhA.2015.14147. 2015. [DOI] [PubMed] [Google Scholar]
- 38.Zhi-Han L., Hui-Yin Y., Makmor-Bakry M. Medication-handling challenges among visually impaired population. Arch Pharm Pract. 2017;8(1):8–17. [Google Scholar]
- 39.Davis A. Sensory impairment. Annual report of the Chief Medical Officer, Surveillance volume 2012: on the state of public's health. (Chapter 4), page 56-57. https://www.gov.uk/government/uploads/system/uploads/attachment_data/file/298297/cmo-report-2012.pdf (Access date 2/3/2018).
- 40.Scottish Government . 2014. See Hear.http://www.gov.scot/Publications/2014/04/7863/downloads [Google Scholar]
- 41.Scottish Health Council . 2014. Teach-back.http://www.scottishhealthcouncil.org/patient__public_participation/participation_toolkit/teach-back.aspx#.WplWBdOrTBI [Google Scholar]
- 42.European Commission Guidelines on the Readability of the Labelling and Package Leaflet of Medicinal Products for Human Use. 2009. https://ec.europa.eu/health/sites/health/files/files/eudralex/vol-2/c/2009_01_12_readability_guideline_final_en.pdf
- 43.Drummond S.R., Drummond R.S., Dutton G.N. Visual acuity and the ability of the visually impaired to read medication instructions. Br J Ophthalmol. 2004;88(12):1541–1542. doi: 10.1136/bjo.2003.029918. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 44.National Health Service . 2003. Design for Patient Safety; p. 2010.http://www.nrls.npsa.nhs.uk/resources/collections/design-for-patient-safety/ [Google Scholar]
- 45.Barnett N, El Bushra A, Huddy H, Majekodumni F, Thomas S, Chiu F. How to support patients with sight loss in pharmacy. Pharm J. http://www.pharmaceutical-journal.com/pharmacy-learning-centre/how-to-support-patients-with-sight-loss-in-pharmacy/20203346.article (access date: 2/3/2018).
- 46.Tan E.C.K., Sluggett J.K., Johnell K. Research priorities for optimizing geriatric pharmacotherapy: an international consensus. J Am Med Dir Assoc. 2018;19(3):193–199. doi: 10.1016/j.jamda.2017.12.002. [DOI] [PubMed] [Google Scholar]
- 47.O'Quin K.E., Semalulu T., Orom H. Elder and caregiver solutions to improve medication adherence. Health Educ Res. 2015;30(2):323–335. doi: 10.1093/her/cyv009. [DOI] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.