Abstract
Objectives
To investigate the impact of provider payment reforms and associated care delivery models on cost and quality in cancer care.
Methods
Data sources/study setting: Review of English-language literature published in PubMed, Embase and Cochrane library (2007–2019).
Study design: We performed a systematic literature review (SLR) to identify the impact of cancer care reforms. Primary endpoints were resource use, cost, quality of care, and clinical outcomes.
Data collection/extraction methods: For each study, we extracted and categorized comparative data on the impact of policy reforms. Given the heterogeneity in patients, interventions and outcome measures, we did a qualitative synthesis rather than a meta-analysis.
Results
Of the 26 included studies, seven evaluations were in fact qualified as quasi experimental designs in retrospect. Alternative payment models were significantly associated with reduction in resource use and cost in cancer care. Across the seventeen studies reporting data on the implicit payment reforms through care coordination, the adoption of clinical pathways was found effective in reduction of unnecessary use of low value services and associated costs. The estimates of all measures in ACO models varied considerably across participating providers, and our review found a rather mixed impact on cancer care outcomes.
Conclusion
The findings suggest promising improvement in resource utilization and cost control after transition to prospective payment models, but, further primary research is needed to apply robust measures of performance and quality to better ensure that providers are delivering high-value care to their patients, while reducing the cost of care.
Introduction
Cancer care is moving toward more advanced, targeted treatments that have the potential to improve health outcomes. Despite the substantial progress in economic evaluations of medical interventions, policy makers are increasingly challenged to control rapidly rising healthcare costs. Available projections for cancer care cost in the United Kingdom, the United States (US), and Australia suggest a dramatic increase from 42% to 66% above their current levels by 2025 [1], [2],[3]. During the past five years, 68 high-cost, novel therapies were launched globally for the treatment of cancer [4], so now the challenge is developing more compelling evidence on whether this expensive paradigm shift leads to better outcomes. Additional increases in cancer treatment costs are associated with the availability of these high-cost novel agents, as well as use of combination therapies and multiple lines of treatment [4]. As treatment options increase, further efforts are required to ensure that providers apply efficient resource-utilization strategies without adversely affecting the quality of care.
Multiple policy reforms have been launched in cancer care, but provider payment models remain an area of contention among policy makers. Shifting the orientation of the provider reimbursement system from services to outcomes requires the identification and reward of high-quality, patient-centered care [5–9]. This transition is tied to care coordination and service delivery models to establish the components of a value-based system. Therefore, a wholesale change in practice is expected to take place while adapting performance metrics, operation systems, and legislative structures to provide value to patients [6, 9–11].
Although the interaction between payers and providers suggests a move from a volume-based to value-based model in oncology practice, there is still limited evidence on successful payment reforms. We conducted a systematic literature review (SLR) to identify and summarize existing evidence on the impact of provider payment reforms and care delivery models on cost and quality measures in cancer care. Previously published literature reviews on this topic were conducted on the basis of existing narrative reviews, expert opinions, and evaluation research studies [12–14]. However, this is the first SLR that focuses on methodological studies reporting comparative data on cost, quality, and clinical outcomes to first describe the landscape of policy reforms targeting inefficiency of care, and second to fill the existing knowledge gap on the effectiveness of such experiments in providing value to patients diagnosed with cancer.
Materials and method
Data sources and searches
The SLR was conducted in accordance with the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) guidelines to identify English-language articles published between January 1, 2007, and January 15, 2019, reporting the impact of provider payment reforms and care delivery models in cancer care. Searches were conducted in PubMed, Embase, and the Cochrane Library; S1, S2 and S3 Tables present the search algorithms for each database. This search was supplemented by manual bibliography searches of the identified studies and authors.
Study selection and data extraction
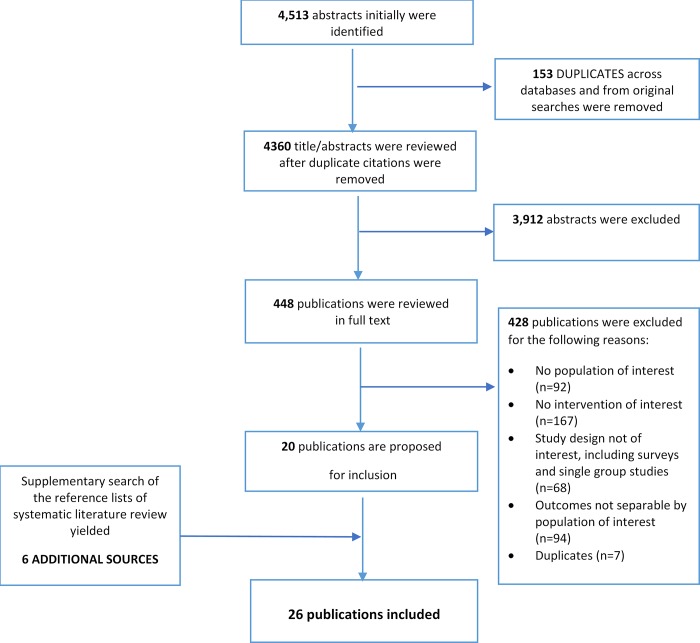
As show in the Patients, Interventions, Comparators, Outcomes, Time and Study design (PICOT) selection criteria table (Table 1). primary endpoints were healthcare resource use, quality, cost, and clinical outcomes. Eligible studies were required to report the impact of policy reforms comparatively in any cancer care setting. The impact was defined as consequences of identified interventions on any of these outcome measures. Interventions related to care delivery models were eligible if they were linked to the provider payments either directly or implicitly. Case reports of policy reforms were eligible if research methodology was clarified and met the inclusion criteria. Commentaries, editorials, narrative reviews, and genetic studies, as well as those with no separable outcomes for cancer care were excluded. Two rounds of screening took place to identify the relevant literature. In the first round, each title/abstract was reviewed by one reviewer for inclusion using the PICOT criteria. A 10% random sample of the articles rejected during this phase were validated by a second reviewer. In the second round of screening, the full texts of the articles identified during the first pass were reviewed and validated (see the flow of literature presented in the PRISMA diagram in Fig 1).
Table 1. PICOT inclusion and exclusion criteria for study selection in the SLR.
| Criteria | Inclusion criteria | Exclusion Criteria |
|---|---|---|
| Population | • Patients diagnosed with cancer • Physicians providing cancer care either in the outpatient or inpatient setting • Payers involved in cancer care reimbursement |
Publications that do not evaluate cancer care. |
| Intervention Comparator |
Explicit payment reforms directly involving financial incentives: Value-based payment, bundled payments, shared savings programs, partial or full capitation, fee-for-service (FFS), global budget, pay-for-performance (P4P), Medicare Modernization Act, other oncology-specific reimbursement models Implicit payment reforms through care coordination: Accountable care organizations (ACOs), oncology care model (OCM), patient-centred oncology medical home (PCMH), oncology pathways, Other cancer care delivery models under the umbrella of payment reforms |
Studies that do not report the interventions of interest in cancer care Local or small-size initiatives associated to the care delivery reforms including hiring patient navigators or implementing triage phone policies |
| Outcomes | • Utilization / healthcare resource use: hospitalization, physician visits, outpatient visits, ICU admissions, Emergency department visits, Specialist visits, length of stay, chemotherapy medication use, time on treatment • Direct and indirect costs of care: hospital costs, total costs, medication costs • Quality of care, adherence to standard of care • Clinical outcomes: survival rate, response to treatment and cancer related mortality |
Studies that do not report outcomes of interest for the study population or outcomes not reported separately for cancer care. |
| Study design | Economic analyses, all epidemiological and observational study designs including but not limited to prospective or retrospective cohort studies, cost-of-illness studies, Database/claims data analyses, case reports on policy reforms | Animal, in vitro, or genetic studies, comments/commentary, news, editorials, or narrative reviews |
| Other limits | limited to articles with an abstract published in English since January 1, 2007 to Jan 15, 2019 | Studies published prior to 2007 or after the final search date in 2019, or not published in English |
Fig 1. Overview of the systematic literature search: PRISMA flow chart.
Using a standardized data extraction form, the mean change and standard deviation of outcome measures within the intervention and comparator groups were extracted and validated accordingly for additional quality assurance. Studies published in multiple articles were extracted as one study. A risk-of-bias assessment for included publications was undertaken by independent reviewers using a checklist developed by the Cochrane Collaboration, the Risk of Bias in Non-Randomized Studies of Interventions (ROBINS-I) tool for non-interventional studies [15]. The seven domains used in the ROBINS-I tool determine the strength of evidence/risk of bias due to confounders, participant selection, classification of interventions, deviations from intended interventions, missing data, measurement of outcomes, and selection of the reported results. A three-point Likert scale was applied to score the bias from low to serious for each of the seven domains; this was later validated by a second reviewer.
Results
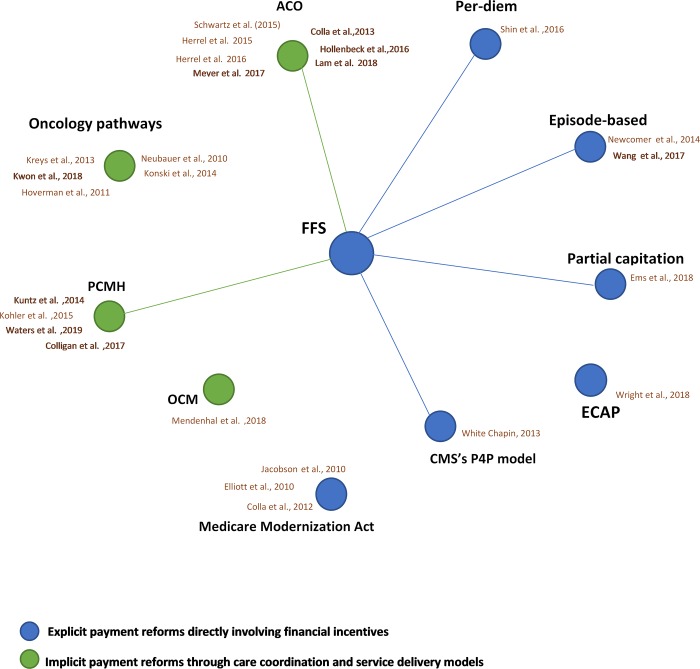
The database and hand-searches yielded 4,513 articles, 26 of which were included in the SLR. Fig 2 presents the network of evidence identified in the literature, providing a clear picture of the models that have been carried out in cancer care. Any studies that were conducted in non-cancer settings (n = 58) or reported no separable outcomes for cancer care (n = 13) were excluded from the SLR. Most of the studies were conducted in the US, except for two in South Korea and one in Taiwan.
Fig 2. Evidence network for the provider payment reforms in cancer care identified in the SLR.
Direct line indicates head-to-head comparison of the interventions as emerged from the data. ACO, accountable care organization; CMS, centers for Medicare and Medicaid services; ECAP, endometrial cancer alternative payment; FFS, fee-for-service; P4P, pay for performance; OCM, oncology care model; PCMH, patient centered medical home.
The included studies presented limited data on the definition of outcomes used, or similar outcomes were measured in different ways. Given the observed variation in study populations, interventions, and outcome measures, we found it inappropriate to perform a meta-analysis to estimate the effect size of each identified model. Taking statistical considerations into account, we used thematic analysis to generate descriptive and explanatory themes as they emerged from the data. Key themes were organized according to the type of reform. All reimbursement models directly involving financial incentives to providers were grouped as explicit payment models. Implicit payment reforms carried out following care-coordination programs, delivery models, or quality initiatives were categorized as implicit payment models.
Using the ROBINS-I tool, we found potential sources of bias in these studies. Of the seven domains scored, confounding and selection bias were found to be the main drivers of risk of bias, followed by outcome measurement and reporting the results. This is perhaps due to the nature of the included studies, with no to very limited control on confounders and outcome measurements. In total, findings indicated that the outcomes reported were moderately biased across the studies.
Explicit provider payment methods
The impact of financial incentives to cancer care providers was investigated in the context of the following models. The findings are summarized in Table 2.
Table 2. Summary of the studies reporting data on the impact of implicit payment reforms in oncology practice.
| Author, year | Geographic location | Payment Method; Intervention vs. comparator | Study design Data source | Cancer type Sample size | Outcomes measures | Findings |
|---|---|---|---|---|---|---|
| Newcomer et al. (2014) | US | Episode based payment vs. predicted costs in FFS setting | Retrospective cohort study using FFS-based registry data | Colon, lung and breast cancers Sample size.N = 810 | • Total treatment costs • Chemotherapy drug cost • Overall Survival |
Episode-based payment vs. FFS: • Actual treatment costs: -34% • Chemotherapy drug costs (CDC): +179% • No significant impact on patients’ survival and quality of care (subbgroup of lung cancer survivors) |
| White et al. (2015) | US | Care management and performance-based payment (P4P) vs. FFS | Simulation model developed by centers for Medicare and Medicaid services (CMS) using Medicare claims data from the chronic condition warehouse (CCW) | Eight cancer types.Sample size N = 330,647 episodes | Changes in total spending under three scenarios of behavioral responses to the P4P reform |
Total spending in P4P vs. FFS model: • Under the “no behavior” scenario: 4% increase • Under the “%5 reduction” scenario: 1% decrease • Scenario of “10% reduction”: 5% reduction |
| Shin et al. (2017) | South Korea | Per-diem Payment System (PDPS) vs. FFS | Quasi experimental model using claims data (Difference in difference method) | More than twelve cancer types.Sample size.N = 5464 | • Length of stays • Total medical costs • Treatment costs • Medications cost • Cost of laboratory and radiological tests |
PDPS vs. FFS-based hospitals: • Length of stays per episode: -2.56%, p = 0.0001 • Total medical costs: -2.46%, p = NR • Duration per episode: -2.5% (95% CI: -0.0324, -0.0194), p<0.0001 • Treatment costs per day: -4.4% (95% CI: -0.071, -0.018), p<0.0001 • Analgesic medications cost per day: -0.59% (95% CI: -0.007, -0.0047), p<0.0001 • Cost of lab tests: -6.62% (95% CI: -0.0688, -0.0683), p<0.0001 PDPS (Post-Implementation vs. baseline): • Total medical costs: -0.76%, p = NR |
| Elliott et al. (2010) | US | Physician reimbursement reform in the Medicare Modernization Act | Retrospective cohort study using surveillance, epidemiology, and end results database (SEER)and Medicare claims data | Prostate cancer.Sample size.N = 72,818 | Utilization of androgen suppression therapy (AST) at first year |
Post vs. pre-reform: • Non-indicated AST use in low risk patients: -39%, p<0.001 • No significant change in indicated AST among low risk patients • No significant change in AST use among metastatic patients |
| Ems et al. (2018) | US | Partial capitated-payment model (post-vs. pre) vs. FFS method | Quasi experimental model using data from a Medicare Advantage plan | Mix of cancer types (Not specified).Sample size.N = 713 | • Chemotherapy-related Complications • Ambulance transports |
Post- vs. pre-contract capitated: • Significant Increase in mean number of chemotherapy-related complications (p = 0.01) and ambulance transports (p<0.0001) Postcontract vs. Precontract FFS: • No difference in any outcome measure |
| Jacobson et al. (2010) | US | Physician reimbursement reform in the Medicare Modernization Act | Retrospective cohort study using data from SEER registry | Lung cancer.Sample size: not reported | • Chemotherapy use • Change in treatment choices |
Post vs. pre-reform: • Chemotherapy prescriptions within 1-month: +2.4%, p<0.001 • Increase in prescription rate of more expensive drugs (Docetaxel: 13%-20% increase) |
| Colla at al. (2012) | US | Physician reimbursement reform for end of life chemotherapy in the Medicare Modernization Act | Retrospective cohort study using Medicare claims data | Mix of cancer types (Not specified).Sample size: not reported | Chemotherapy use at the last 14 days, 3- month or 6-month of life |
Post vs. pre-reform: • The last 14 days of life (visited in physician offices) = -20% (95% CI: -4.2 to -1.0, P = 0.002) • The last 14 days of life (hospital outpatients): no changes (95% CI: -2.4 to 4.4; P = 0.541). • last 3 and 6 months of life (any practice setting): Significant reduction in number of treatments per patient p<0.001. |
| Wang et al. (2017) | Taiwan | Episode-based (bundled-payment) vs. FFS | Retrospective cohort study with a matched control group using national registry and claims data | Breast cancer.Sample size.N = 17,940 | • Adherence • 5-year event-free survival rate • 5-year medical payments |
Bundled payment vs. FFS: • Greater adherence to quality indicators (p<0.001) • Greater 5-year event-free survival (p<0.01) • Stable 5-year medical payments in bundled payment model vs. 20% increase in FFS arrangement |
| Wright et al. (2018) | US | Endometrial cancer (EC) alternative payment (ECAP) model | A decision model used data from MarketScan and Medicare | Endometrial cancer (EC).Sample size.N = 29,558 | Potential cost savings through lower case reimbursement |
In the optimized care model: Reduction in average case reimbursement in both public (-2.9%) and commercial payers (-5.9%) |
■ Per-diem vs. FFS
A single study examined the transition from fee-for-service (FFS) reimbursement to a per-diem payment system (PDPS). This study involved patients from seven hospitals in a PDPS program with FFS-based centers [16]. Compared to the controls in the FFS setting, per-diem reimbursement significantly reduced length of hospital stays (p = 0.0001) and total medical costs for PDPS participants. Besides a 2.5% decrease in duration of care (p<0.0001), costs associated with lab tests, cancer treatment, and analgesic medications dropped by 6.62%, 4.4%, and 0.59%, respectively (p<0.0001). The average reduction in length of hospital stays was 3.19 days post implementation of the per-diem model [16].
■ Episode-based payment vs. FFS
The impact of episode-based reimbursement in cancer care was investigated in two studies, conducted in Taiwan [17] and the US [18], where significant improvements in the five-year cost and quality outcomes were reported compared to the regular FFS payment. A large cohort of Tai patients with stage 0-III breast cancer (n = 17940) in the bundled-payment program were matched with controls in an FFS setting; the results indicated significantly better adherence to quality indicators (p<0.001) and an improved five-year survival rate (p<0.01) within the bundled-payment system. Although the cumulative medical payments for the FFS group increased by 20%, the five-year medical payments of the bundled-payment group remained stable[17]. Similarly, in the US-based healthcare system, direct costs of cancer care in an episode-based program dropped by 34% compared to the predicted costs in a large FFS-based registry, resulting in a net savings of $33,361,272 [18]. However, drug costs increased by 179%, with a net rise of $13,459,913 due to the change in chemotherapy prescriptions. A subset analysis of 50 medical groups with at least 70 participants per episode demonstrated the same cost impacts as the base-case analysis. When using data from another subgroup of lung cancer survivors, no significant difference was found in patients’ survival between the two payment groups.
■ Pay-for-Performance (P4P) vs. FFS
A simulation model investigated the impact of a performance-based payment on specialty oncology services compared to FFS spending [19]. Using historical episodes from Medicare claims for FFS beneficiaries, the Centers for Medicare and Medicaid (CMS) established a model for prevalent cancers (n = 330,647 oncology episodes). Assuming a target spending for chemotherapy episodes, an extra performance-based compensation per episode was paid to physicians in addition to the standard FFS-based payment in practices with episode costs falling below the target. Changes in the quantity and intensity of services in response to the P4P reform were measured under one of three scenarios: “no change”, “5% reduction” and “10% reduction” from the initial FFS spending. The study found a range of -5% to +4% change in total spending under the “10% reduction” and “no behavior” scenarios, respectively, indicating a substantial drop in total costs after implementing the P4P model [19].
■ Capitated-payment model vs. FFS
We identified a single study reporting the impact of an oncology group’s transition from FFS arrangement to a partial-capitated model [20]. A six-month follow-up of Medical Advantage enrollees from a single health plan in the US indicated that there were no significant differences in all-cause hospitalizations between the two payment cohorts. Although the mean number of chemotherapy-related complications and ambulance transports were greater post-transition, the subset analysis indicated that the post-capitated group was sicker than the pre-capitated cohort (according to the Deyo-Charlson Comorbidity Index (CCI) and the Rx-Risk scores).
■ Other explicit payment reforms
Three studies reported the impact of provider payment reform implemented as part of the Medicare Modernization Act, and determined it was effective in switching treatment patterns and chemotherapy use [21–23]. According to the findings, regardless of the practice setting, dropping reimbursement rates significantly reduced chemotherapy prescriptions per patient at three and six last months of life for patients diagnosed with a variety of cancer types (p<0.001)[21]. Similarly, a major reduction (64%) in reimbursement for androgen suppression therapy (AST) in prostate cancer (n = 72,818) significantly reduced the odds of receiving non-indicated AST (given without other therapies such as radical prostatectomy or radiation) in low-risk patients (p<0.001) [22]. In contrast, in a cohort of lung cancer patients, outpatient chemotherapy prescriptions significantly increased, with the pattern of switching to high-margin drugs because of the reduction in reimbursement rates. A 2.4% increase was observed in chemotherapy use less than one month after reducing payment rates for lung cancer services (p<0.001)[23].In one study, the endometrial cancer alternative payment (ECAP) model, a value-based healthcare reform initiated based on the Physician Payment Reform Taskforce (PPRTF) in the Society of Gynecologic Oncology (SGO), was investigated for sources of potential cost savings while promoting quality of care[24]. An optimized care model was created using claims data from MarketScan and Medicare databases. The model focused on the rate of minimally invasive surgery, length of stays, and emergency department (ED) visits/readmissions to compare mean reimbursement per episode of surgical care among low-risk, early-stage EC patients (n = 29,935). Outcomes were stratified by three surgical approaches, from 30 days preoperatively to 60 days postoperatively. The model derived a cost savings of $903 per patient (2.9% of baseline) in MarketScan, and $1243 (5.9% of baseline) in Medicare, as reflected in the proposed value-based reimbursement strategy.
Implicit payment reforms targeting delivery of care
Eleven studies in the review reported data on care delivery reforms, including adoption of clinical pathways and participation in patient-centered medical home (PCMH), accountable care organization (ACO), or oncology care model (OCM) programs. The findings are synthesized and summarized by type of reform within the following sub-sections and Table 3.
Table 3. Summary of the studies reporting data on implicit payment reforms through care coordination in oncology practice.
| Author, year | Country | Cancer care delivery models;.Intervention vs. comparator | Study design.Data source | Cancer type.Setting.Sample size | Outcomes measures | Findings |
|---|---|---|---|---|---|---|
| Hoverman et al. (2011) | US | Adopting level-I colon cancer pathways vs. off pathway treatments | Retrospective cohort study using data form US Oncology Network and MedStat databases | Colon cancer.Sample size.N = 1130 patients | • Total costs per case • Total costs per patient per month • Chemotherapy cost • Chemotherapy duration • Chemotherapy related admissions • Overall survival (OS) • Disease-free Survival (DFS) |
On vs. off pathway treatment in adjuvant group • Total costs per case: -35%, p<0.001 • Treatment costs per patient: -35%, p≤0.01 • Chemotherapy costs: -63%, p<0.001 • Chemotherapy period: -34%, p<0.001 • Chemotherapy admissions: -23%, p = 0.236 • DFS: HR = 4.98 (95% CI, 2.11 to 11.74), P<0 .05 In metastatic patients only OS was significantly longer: 26.9 vs. 20.1 months,P = 0.03 |
| Konski et al. (2014) | US | Pathway-based vs. off-pathway hypofractionation | Simulation Model using a sample hospital-based data from a radiationoncology practice | Breast, prostate and lung cancers.Sample size.N = 221 | • Per-patient revenue • Changes in technical workflow • Professional relative value unit per case (RVU) |
On vs. off-pathway treatment: • Annual reduction in global revenue: $540,661 • Workflow reduction: five patients or 1 to 1.5 operating hours per day RVU reduction: -2,121 |
| Kreys et al. (2013) | US | Before vs. after adopting clinical pathways | Retrospective cohort study using claims data from CareFirst BlueCross BlueShield of Maryland | Breast, colorectal, lung.Sample size.N = 4,713 (across 46 cancer centers) | • Hospitalization costs • Drug costs • Hospitalization days • Number of hospitalizations • Total cost savings |
Two-year after vs. 1-year before adoption: • hospitalization costs per patient: -75%, p = 0 .004 • Number of hospitalizations per patient (30 days post-chemotherapy): -8.7%, p = 0.255 • Hospitalization days per patient: -32.8%, p = 0.057 • Total drug costs per patient: +2.5%, p = 0.587 • Total cost savings compared to the projected costs: $10.3 million |
| Kwon et al. (2018) | South Korea | Pathway-based vs. off-pathway treatment of thyroid cancer | Retrospective cohort study | Thyroid cancer.Sample size.N = 361 | • Length of hospital stays • Total costs per patient |
On vs. off-pathway treatment: Length of hospital stays: -0.8 days (p = 0.02) Cost per patient: -14.8% (p<0.001) |
| Neubauer et al. (2010) | US | Before vs. after adopting level I clinical pathways for the treatment of lung cancer | Retrospective cohort study using data form US Oncology Network | Non-small cell lung cancer.Sample size.N = 1,409 patients across eight cancer centers | 12-month costs • Outpatient costs • Cost of medications • OS |
On vs. off-pathway treatment: • Outpatient costs: -35% • Cost of chemotherapy: -37% • Non-chemotherapy medications: -39% • 12-month OS: +2.2%, p = 0.867 |
| Kohler et al. (2015) | US | PCMH vs. non-PCMH arrangement | Retrospective cohort study using North Carolina Medicaid claims | Breast cancer Sample size N = 758 (9407 person-month observations) |
• Outpatient visits • Inpatient hospitalizations • Emergency Department (ED) visits • Medicaid expenditures |
PCMH vs. non-PCMH enrollees: • Monthly Medicaid expenditures within the first 15-month from diagnosis: -22.9%, p<0.001 • Outpatient visits: -22.2%, p<0.001 • Inpatient hospitalizations: no differences, p = NR • ED visits: no differences, p = NR |
| Kuntz et al. (2014) | US | Michigan Oncology Medical Home Demonstration Project at first year vs. 3-year data from a historical control group | Retrospective cohort study using historical data | Mix of cancer types (Not specified).Sample size.N = 519 | • ED visits • Inpatient admissions |
After vs. before implementing the model: • ED visits per patient: -47% Inpatient admissions per patient: -68.2% • Cost savings per patient: $550 |
| Waters et al. (2019) | US | Community Oncology Medical Home program (COME HOME) vs. FFS | Quasi experimental model using claims data (Difference in difference method) | Seven cancer types.Sample size.N = not reported (across seven cancer centers) | • Medical spending • ED visits • Ambulatory care • Hospitalizations • Readmission rate • Length of stay |
Medical home vs. FFS: • Change in 6-month medical spending post implementation: -$2,657, p = 0.008 • ED visits per 1,000 patients: -10.2%, p = 0.024 • No significant change was observed in other outcome measures |
| Colligan at al. (2017) | US | Community Oncology Medical Home program (COME HOME) vs. FFS | Retrospective study using matched control group from Medicare claims | Seven cancer types.Sample size.N = not reported (across seven cancer centers) | Average costs over the last 30, 90 and 180 days of life | Medical home vs. FFS • Last 30-day costs: -$959 (-6%) • Last 90-day costs: -$3,346 • Last 180-day costs: -$5,790 |
| Colla et al. (2013) | US | The Physician Group Practice Demonstration project for ACO participants vs. non-ACO | Quasi experimental model using Medicare claims (Difference in difference method) | Mix of cancer types (Not specified).Sample size.N = 988,781 person-years | Annual per-beneficiary change in payments |
ACO vs. non-ACO enrollees post-reform: Annual per-beneficiary change in payments: -3.9% |
| Herrel et al. (2015) | US | ACO participating hospitals vs. non-ACO hospitals | Retrospective cohort study using national inpatient sample | Patients with urologic cancer who underwent elective major surgery Sample size: • Non-ACO hospitals: n = 352 • ACO hospitals: n = 176 |
• In-hospital mortality Prolonged length of stay (LOS, >90th percentile) • Total hospital costs |
ACO vs. non-ACO hospitals: • Mortality rate: no significant difference, p = NR • Length of stay: no significant difference, p = NR • Total inpatient costs: no significant impact on prostatectomy (p = 0.07), nephrectomy (p = 0.07) and cystectomy (p = 0.25) services |
| Herrel et al. (2016) | US | ACO vs. non-ACO practices | Quasi experimental model using Medicare claims (Difference in difference method) | Nine cancer types Sample size: 384,519 patients across: • ACO hospitals: 106 • Non-ACO hospitals: 2,561 |
• 30-day mortality rate • Complication rate • Readmission rate • Length of stay |
ACO vs. non-ACO hospitals: • 30-day mortality rate: 3.3% vs. 3.4%, p = 0.54 • 30-day readmission rate:12.5% vs. 12.4%, p = 0.69 • Complications rate: 43.6% vs. 43.4%, p = 0.65 Length of stays: 10.1% vs. 10.2%, p = 0.56 |
| Hollenbeck et al. (2017) | US | ACO vs. non-ACO practices | Retrospective cohort study using Medicare claims | Prostate cancer.Sample size.N = 15,640 | • Use of curative treatment • Total spending |
ACO vs. non-ACO enrollees • Use of curative treatment: no significant change, p = 0.33 Spending one-year after diagnosis: +5.8%, p = 0.03 |
| Lam et al. (2018) | US | ACO vs. non-ACO practices | Quasi experimental model using Medicare claims (Difference in difference method) | Eleven cancer types.Sample size.N = 622,080 | • Total spending • Inpatient spending • Outpatient spending • Physician services • Chemotheray spending |
ACO vs. non-ACO enrollees post-reform: • Total spending: no significant change, p = 0.94 • No significant change in inpatient (p = 0.31), outpatient (p = 0.32), physician services (p = 0.81), and chemotherapy spending (p = 0.81) |
| Meyer et al. (2017) | US | ACO vs. non-ACO practices | Retrospective cohort study with a matched control group using Medicare claims | Breast and prostate cancers.Sample size.N = 1,480,414 | The prevalence of breast and prostate cancer screening |
ACO vs. non-ACO enrollees • The prevalence of breast cancer screening: +40%, p<0.001 • The prevalence of prostate cancer screening: +31.7%, p<0.001 |
| Schwartz et al. (2015) | US | ACO vs. non-ACO practices | Quasi experimental model using claims data (Difference in difference method) using Medicare data | Mix of cancer types (Not specified).Sample size.N = 17516641 | Reduction in Low-value service use |
ACO vs. non-ACO hospitals: • Utilization of cancer screening/imaging services per 100 beneficiaries: -2.4% (95% CI: -4.1, -0.7). • Total spending on low-value services: -4.5% (p = 0.004). |
| Mendenhal et al. (2018) | US | Oncology Care Model (OCM) program | Retrospective cohort study using data from Chronic Condition Warehouse | Mix of cancer types (Not specified).Sample size.N = 1,600 | • Acute care admissions • Inpatient costs |
OCM vs. non-OCM participants: • Acute care admissions rate: -16%, p = 0.005 • Net savings in inpatient costs in the first year: $798,000 |
■ Adopting clinical pathways
The adoption of clinical pathways was consistently associated with reductions in resource use and costs for a variety of cancer types. Pathway-based treatment of patients with thyroid cancer (n = 361) was significantly effective in reducing length of hospital stays (p = 0.02) and cost per patient (p<0.001) compared to the controls with off-pathway treatment [25]. Likewise, adopting a clinical pathway program across 46 cancer settings (N = 4,713) was associated with a 75% reduction in hospitalization costs per patient over three years (p = 0 .004), as well as a 30% drop in cost of supportive care per patient (p<0.001). Chemotherapy drugs and hospitalization costs were found to be the main drivers of these trends, corresponding to 68% and 32% of the total savings, respectively [26]. The same impact was observed for the pathway-based treatment of colon cancer, with a substantial reduction in total adjuvant treatment costs for non-metastatic disease, and a longer survival time for metastatic patients, compared to the off-pathway group [27]. Significant reductions were also found in mean total costs per case (p<0.001), treatment costs per patient per month (p≤0.01), chemotherapy costs (p<0.001), and chemotherapy period (p<0.001) for on- versus off-pathway treatment [27]. A 35% reduction in outpatient costs was observed for patients with non-small-cell lung cancer (NSCLC); however, no significant difference was found in 12-month survival of such patients treated in the on-pathway versus off-pathway groups (p = 0.867)[28]. Regarding the impact on resource use and hospital-based billing, evidence-based hypofractionation was found to be effective in reducing five patients per day equivalent to one to 1.5 daily operating hours in a radiotherapy department [29].
■ PCMH vs. FFS
The impact of the Community Oncology Medical Home program on cancer care spending was compared with FFS Medicare beneficiaries diagnosed with various cancer types. After adjustment for clinical and sociodemographic differences, implementing PCMH model was found to be associated with significantly reduced (10.2%) ED visits per 1,000 patients (p = 0.024), resulting in 8.1% savings relative to average spending per beneficiary over six months [30]. A similar result was observed for Medicare expenditures in the last year of life for beneficiaries with cancer. The average end-of-life costs in the last 30, 90, and 180 days dropped for patients in a PCMH program compared to the FFS Medicare claims for similar outpatient oncology practices [31]. Michigan Oncology Medical Home was also effective in reducing the first-year costs through avoiding unnecessary ED visits and inpatient admissions across four cancer practices, with an average estimated cost savings of $550 per patient [32]. However, according to another study, the impact of PCMH enrollment was, in some measure, associated with increased resource use and cost. A significant increase in monthly Medicaid expenditures and the number of outpatient visits for PCMH enrollees was observed over the first 15 months from diagnosis compared to non-PCMH participants (p<0.001), with no significant impact on inpatient hospitalizations or ED visits [33].
■ ACO vs. non-ACO (FFS)
Compared to the non-ACO participants, Medicare beneficiaries with prostate cancer who were aligned with ACOs (n = 1,100) had similar rates of treatment (p = 0.33), but significantly increased spending in the year after diagnosis [34]. In another study on patients with urologic cancer who underwent elective major surgery, no significant differences were observed in total inpatient costs, length of hospital stays, and mortality rate among patients within 176 ACO hospitals compared to 352 non-ACO sites [35]. Similarly, the ACO model was found to have no significant association with post-surgery complication rate (p = 0.65), prolonged length of stays (p = 0.56), and readmission rate (p = 0.69) among patients undergoing major resection surgeries (n = 384,519) in ACO hospitals, compared to the non-ACO enrollees within 2,516 cancer centers [36]. In a larger scope, across 11 different cancer types from five-year national Medicare claims, having a cancer diagnosis in a Medicare ACO had no significant impact on healthcare spending and resource utilization [37]. However, in specific medical scenarios, the first year of the Medicare Pioneer ACO program was found to be effective in reducing the utilization of low-value services, defined as providing minimal or no average clinical benefit. Compared to the control group, a reduction of 0.8 services per 100 beneficiaries was observed in the ACO model with 693,218 person-years. This corresponds to a 4.5% drop in total spending on low-value services (p = 0.004). The greatest absolute reductions in service utilization post-ACO participation was observed in cancer screening and imaging tests, the most frequently delivered services [38].
Similarly, in a study by Colla et.al [39],the Physician Group Practice Demonstration ([PGPD] used as a proxy for ACO) was significantly associated with an annual reduction of 3.9% in payments per beneficiary. Major reductions in inpatient service use, hospital discharges, and intensive care unit (ICU) stays were identified, but no changes in cancer-specific procedures or chemotherapy were observed post-PGPD program. In cancer preventive care, ACO enrollment was also effective in increasing the utilization of preventive screening tests among patients with breast or prostate cancer. The prevalence of screening tests for both cancers was higher among ACO participants compared to non-ACO enrollees (p<0.001) [40]. Although the screening for prostate cancer was in the ACO model, it was not recommended by the US Preventive Services Task Force (USPSTF). Thus, delivering high-quality care in ACO models needs to be linked to the standard of care in order to control unnecessary use of low-value services.
■ OCM
The SLR identified a cancer care delivery reform, implemented as a five-year model by CMS to provide coordinated, high-quality care for oncology practices using alternative payment arrangements with CMS; this included financial and clinical performance accountability for episodes of care. Mendenhall et.al [41] used risk-adjusted national averages of all practices providing cancer care in the same patient risk quartile as the comparator cohort to evaluate the impact of a multifaceted care delivery approach targeting unnecessary ED and hospital admissions. The strategy included increased care coordination, adopting standardized pathways, urgent care tactics, and patient education. The findings indicated that there was a statistically significant reduction (16%) in hospital admissions (p = 0.005), resulting in a net saving of $798,000 in inpatient costs per quarter for 1,600 patients in the first year of the OCM program. Additionally, quarterly basis surveys demonstrated that OCM patient satisfaction scores improved over the course of year 1 in the program.
Discussion
Payment reform requires more compelling evidence to ensure providers are delivering high-value, quality care to their patients, while reducing the cost of such care. An SLR such as this can help stakeholders and payers understand the successes and failures of the reforms. Our review found that alternative payment models demonstrated promising outcomes in reducing healthcare resource use and costs, although they are still lacking robust measures of performance and quality. Of the interventions involving reimbursement reforms either directly or implicitly through care coordination models, most improved resource utilization and/or cost of care. Consistent with the previously published literature [42–45], adopting oncology pathways significantly reduced chemotherapy duration, hospitalizations, length of stays, and associated costs by avoiding unnecessary use of low-value services. The common method used to determine the effectiveness of pathways was evaluating whether their use resulted in cost savings relative to off-pathway treatments across all studies. However, this savings could not be linked to the cost drivers, which vary across cancer types and mainly depend on patient characteristics, disease stage, goals of therapy, available treatment options, and patient preferences. Although standardization of care appeared to be an effective strategy in targeting expensive chemotherapy treatments, little information was available regarding the impact of adherence to guidelines on clinical outcomes, treatment complications, and patient’s quality of life and satisfaction. It is unlikely to find a randomized trial with off-pathway versus pathway-based treatment arms; therefore, the strength of retrospective evaluation is in the ability to examine comprehensive electronic health records and claims data. The impact of adherence to standards can be more definitively measured as pathways are further adopted and implemented in cancer care, allowing for assessments of different modalities in a variety of settings in the short versus long term.
This review also identified notable findings regarding other implicit payment models that involve care coordination across providers. With the PCMH model, most studies reported potential savings in costs of care derived from significant drops in ED visits and inpatient admissions; in contrast, longer follow-up of patients until 15 months post-diagnosis indicated significant increase in outpatient service use and average expenditures per month. The increase in outpatient services for breast cancer is likely due to the greater access to care through PCMH that can result in addressing unmet needs of patients. However, a lack of evidence on time-varying characteristics and risk profiles of patients across PCMH models requires further research to extend the evaluation time span beyond the initial months post-diagnosis with more intensive treatment per cancer type.
The estimates of all measures in ACO models varied considerably across participating providers, and our review found a rather mixed impact on cancer care outcomes. It appears that improvements in some of the key cancer care domains, including screening, surveillance, and end-of-life care are more responsive to the ACO model than surgical outcomes in certain settings. Improvement in specialized outcome measures in cancer care may be more difficult to achieve through the ACO model, as most of the ACO quality metrics are not specifically focused on the complex care coordination in oncology practice. Additionally, the effects derived from ACO policies may become stronger over time as organizational changes take place, and the culture of coordination takes shape. As more data become available, covering the existing gap in time trends and lack of value-based metrics will be important to better evaluate the impact of the ACO model in cancer care.
The findings of this study also suggest promising cost savings from transition to prospective reimbursement models, in which financial risks and accountability are redistributed towards providers in cancer care; these results are consistent with such findings in non-cancer settings [6, 9–11]. Although there is lack of evidence on whether quality of care was compromised in alternative payment models, resource use improvements were somewhat evident in per-diem payment, pay for performance, episode-based reimbursement, and Medicare Modernization Act reforms. Despite this, the effect size of the cost savings seemed to fall short in bending the cost curve, due to the absence of more aggressive payment reforms in cancer practice. Understanding the multiple factors influencing the impact of value-based purchasing models is crucial to evaluating these types of reform that are tailored to the specific setting and target population. At a higher level, general healthcare policies and regulations as well as other quality improvement initiatives are important to the success of alternative payment models. However, the structure of the healthcare systems, provider characteristics, patient population and preferences, and their risk profiles are the key components in designing, implementing, and evaluating payment reforms, for which there was no evidence available according to our findings. In addition, the complexity of quality metrics is important to consider in evaluating the appropriateness and effectiveness of financial incentives, as providers need to understand the metrics and link them to the incentives.
Our study should be interpreted in the context of several important limitations. First, there is possibility of publication bias, as is part of the challenges associated with conducting SLRs. However, additional resources were identified through hand-searching the reference list of publications. Second, the possibility of selection bias in patients and policy interventions is inherent to the design of the included studies. Our careful attention to the quality of the evaluation research from which we captured data allowed for transparency and a full understanding of the strength of evidence using the ROBINS-I risk-assessment tool. According to our findings provided in Table 4, nearly half of the studies were subject to confounding bias, which highlights the difficulty of evaluating health policy reforms using observational data. Failure to evaluate potential confounders across the included studies may have biased our results towards erroneous conclusions on the impact of payment reforms. This observation warrants future studies that are at the very least quasi experimental designs with either interrupted time series or pre-post difference in differences construct. Furthermore, the use of manual or propensity score matching is essential to mitigate the imbalances due to selection bias.
Table 4. Risk of bias assessment using ROBINS-I tool for non-interventional studies.
| Study (Author, year) |
Risk of confounding bias | Risk of selection bias | Risk of bias in classification of interventions | Risk of bias to deviations from intended interventions | Risk of bias due to missing data | Risk of bias in measurement of outcomes |
Risk of bias in reporting the results |
Overall risk of bias |
|---|---|---|---|---|---|---|---|---|
| Colla, 2012 | Serious | Moderate | Moderate | Low | Low | Moderate | Low | Moderate |
| Colla, 2013 | Low | Low | Moderate | Low | Low | Moderate | Low | Low |
| Colligan, 2017 | Low | Low | Moderate | Low | Low | Moderate | Low | Low |
| Elliott, 2010 | Low | Low | Moderate | Low | Low | Moderate | Low | Low |
| Ems, 2018 | Low | Low | Moderate | Low | Low | Moderate | Low | Low |
| Herrel, 2015 | Serious | Moderate | Moderate | Low | Low | Moderate | Low | Moderate |
| Herrel, 2016 | Low | Low | Moderate | Low | Low | Moderate | Low | Low |
| Hollenbeck, 2017 | Serious | Moderate | Moderate | Low | Low | Moderate | Low | Moderate |
| Hoverman,2011 | Serious | Moderate | Moderate | Low | Low | Moderate | Low | Moderate |
| Jacobson, 2010 | Serious | Moderate | Moderate | Low | Low | Moderate | Low | Moderate |
| Kohler,2015 | Serious | Low | Moderate | Low | Low | Moderate | Low | Low |
| Konski,2014 | Moderate | Moderate | Moderate | Low | Low | Moderate | Low | Moderate |
| Kreys, 2013 | Serious | Moderate | Moderate | Low | Low | Moderate | Low | Moderate |
| Kuntz, 2014 | Moderate | Moderate | Low | Low | Low | Moderate | Low | Moderate |
| Kwon, 2018 | Serious | Moderate | Moderate | Low | Low | Moderate | Low | Moderate |
| Lam, 2018 | Low | Low | Moderate | Low | Low | Moderate | Low | Low |
| Mendenhal, 2018 | Moderate | Moderate | Moderate | Low | Low | Moderate | Low | Moderate |
| Meyer, 2017 | Low | Low | Moderate | Low | Low | Moderate | Low | Low |
| Neubauer, 2010 | Serious | Moderate | Moderate | Low | Low | Moderate | Low | Moderate |
| Newcomer, 2014 | Serious | Moderate | Moderate | Low | Low | Moderate | Low | Moderate |
| Schwartz, 2015 | Low | Low | Moderate | Low | Low | Moderate | Low | Low |
| Shin, 2017 | Serious | Moderate | Moderate | Low | Low | Moderate | Low | Moderate |
| Wang, 2017 | Low | Low | Moderate | Low | Low | Moderate | Low | Low |
| Waters, 2019 | Low | Low | Moderate | Low | Low | Moderate | Low | Low |
| White, 2015 | Moderate | Moderate | Moderate | Low | Low | Low | Low | Low |
| Wright, 2018 | Low | Low | Moderate | Low | Low | Moderate | Low | Low |
The nature of variability across the studies, together with clinical, methodological, and statistical sources of heterogeneity were other barriers to evaluating the impact of reforms. There was no group of studies sufficiently homogeneous in terms of patients, interventions, or outcome measures to pool data or perform a meta-analysis to estimate the overall impact of each model. This likely reflects the developing nature of the policy reforms in the fast-evolving field of cancer. From a practical point of view, this study provides a tabular summary of all studies related to each key piece of information identified as important for resource use and quality improvement in cancer care. The findings from this evidence review should be useful to policymakers, providers, and payers since it covers an important aspect of cancer care reform.
Conclusion
Of the implicit payment models driving quality improvements in cancer care, provider’s adherence to oncology pathways was significantly effective in resource use improvement. Despite this, it was difficult to get a clear picture of the effect that participating in PCMHs has on cancer care outcomes in the long term due to an insufficient number of evaluations. Much anticipated, but overdue, is the impact of ACO models with ambitions to capitalize on the cost savings of better care coordination in management of chronic diseases. However, the evaluations of ACOs in cancer care found mixed results, with Medicare Pioneer ACO demonstrating some reduction in utilization of certain low-value services in the first year. The findings also suggest promising improvement in resource utilization and cost control after transition to prospective payment models, but, further primary research is needed to apply robust measures of performance and quality to better ensure that providers are delivering high-value, quality care to their patients, while reducing the cost of care.
Supporting information
(DOCX)
(DOCX)
(DOCX)
(DOCX)
(DOCX)
Data Availability
All relevant data are within the manuscript and its Supporting Information files.
Funding Statement
The author(s) received no specific funding for this work.
References
- 1.Mariotto AB, Robin Yabroff K, Shao Y, Feuer EJ, Brown ML. Projections of the Cost of Cancer Care in the United States: 2010–2020. JNCI Journal of the National Cancer Institute. 2011;103(2):117–28. 10.1093/jnci/djq495 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Bupa. Cancer diagnosis and treatment: A 2021 projection. London: Bupa; 2011. [Google Scholar]
- 3.AIHW. Projection of Australian health care expenditure by disease, 2003 to 2033. Canberra:: Australian Institute of Health and welfare; 2008, Cat. no. HWE 43. [Google Scholar]
- 4.QuintilesIMS. Global oncology trends. NJ, USA: QuintilesIMS Institute; 2017. [Google Scholar]
- 5.Gal RA, Volkert P, Malik I, Schmidt DH, Kubota J, Sarnoski J. Fee-for-service versus capitation-based reimbursement: how the payment method affects utilization of echocardiographic services by referring physicians. Echocardiography (Mount Kisco, NY). 1995;12(2):207–11. [DOI] [PubMed] [Google Scholar]
- 6.Ransom SB, McNeeley SG, Kruger ML, Doot G, Cotton DB. The effect of capitated and fee-for-service remuneration on physician decision making in gynecology. Obstetrics and gynecology. 1996;87(5 Pt 1):707–10. [DOI] [PubMed] [Google Scholar]
- 7.Erus B, Hatipoglu O. Physician payment schemes and physician productivity: Analysis of Turkish healthcare reforms. Health policy (Amsterdam, Netherlands). 2017;121(5):553–7. [DOI] [PubMed] [Google Scholar]
- 8.Pawaskar M, Burch S, Seiber E, Nahata M, Iaconi A, Balkrishnan R. Medicaid payment mechanisms: impact on medication adherence and health care service utilization in type 2 diabetes enrollees. Population health management. 2010;13(4):209–18. 10.1089/pop.2009.0046 [DOI] [PubMed] [Google Scholar]
- 9.Gosden T, Forland F, Kristiansen IS, Sutton M, Leese B, Giuffrida A, et al. Capitation, salary, fee-for-service and mixed systems of payment: effects on the behaviour of primary care physicians. The Cochrane database of systematic reviews. 2000(3):Cd002215 10.1002/14651858.CD002215 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Abduljawad A, Al-Assaf AF. Incentives for Better Performance in Health Care. Sultan Qaboos University Medical Journal. 2011;11(2):201–6. [PMC free article] [PubMed] [Google Scholar]
- 11.Tan SY, Melendez-Torres GJ. Do prospective payment systems (PPSs) lead to desirable providers' incentives and patients' outcomes? A systematic review of evidence from developing countries. Health policy and planning. 2017. [DOI] [PubMed] [Google Scholar]
- 12.McPherson E, Hedden L, Regier DA. Impact of oncologist payment method on health care outcomes, costs, quality: a rapid review. Syst Rev. 2016;5(1):160 10.1186/s13643-016-0341-2 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Aviki EM, Schleicher SM, Mullangi S, Matsoukas K, Korenstein D. Alternative payment and care-delivery models in oncology: A systematic review. Cancer. 2018;124(16):3293–306. 10.1002/cncr.31367 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Wen L, Divers C, Lingohr-Smith M, Lin J, Ramsey S. Improving quality of care in oncology through healthcare payment reform. Am J Manag Care. 2018;24(3):e93–e8. [PubMed] [Google Scholar]
- 15.Sterne JA, Hernán MA, Reeves BC, Savović J, Berkman ND, Viswanathan M, et al. ROBINS-I: a tool for assessing risk of bias in non-randomised studies of interventions. BMJ. 2016;355. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Shin JY, Yoon SJ, Ahn HS, Yun YH. Effects of Per-diem payment on the duration of hospitalization and medical expenses according to the palliative care demonstration project in Korea. Int J Health Plann Manage. 2017;32(2):e206–e17. 10.1002/hpm.2366 [DOI] [PubMed] [Google Scholar]
- 17.Wang CJ, Cheng SH, Wu JY, Lin YP, Kao WH, Lin CL, et al. Association of a Bundled-Payment Program With Cost and Outcomes in Full-Cycle Breast Cancer Care. JAMA Oncol. 2017;3(3):327–34. 10.1001/jamaoncol.2016.4549 [DOI] [PubMed] [Google Scholar]
- 18.Newcomer LN, Gould B, Page RD, Donelan SA, Perkins M. Changing physician incentives for affordable, quality cancer care: results of an episode payment model. J Oncol Pract. 2014;10(5):322–6. 10.1200/JOP.2014.001488 [DOI] [PubMed] [Google Scholar]
- 19.White Chapin CC, Huckfeldt Peter J., Kofner Aaron, Mulcahy Andrew W., Pollak Julia, Popescu Ioana, Justin W. Speciality payment model opprtunities and assessment: Oncology simulation report. Santa Monica: RAND Corporation; 2015. [PMC free article] [PubMed] [Google Scholar]
- 20.Ems D, Murty S, Loy B, Gallagher J, Happe LE, Rogstad TL, et al. Alternative Payment Models in Medical Oncology: Assessing Quality-of-Care Outcomes Under Partial Capitation. American health & drug benefits. 2018;11(7):371–8. [PMC free article] [PubMed] [Google Scholar]
- 21.Colla CH, Morden NE, Skinner JS, Hoverman JR, Meara E. Impact of payment reform on chemotherapy at the end of life. J Oncol Pract. 2012;8(3 Suppl):e6s–e13s. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 22.Elliott SP, Jarosek SL, Wilt TJ, Virnig BA. Reduction in physician reimbursement and use of hormone therapy in prostate cancer. J Natl Cancer Inst. 2010;102(24):1826–34. 10.1093/jnci/djq417 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.Jacobson M, Earle CC, Price M, Newhouse JP. How Medicare's payment cuts for cancer chemotherapy drugs changed patterns of treatment. Health affairs (Project Hope). 2010;29(7):1391–9. [DOI] [PubMed] [Google Scholar]
- 24.Wright JD, Havrilesky LJ, Cohn DE, Huang Y, Rathbun J, Rice LW, et al. Estimating potential for savings for low risk endometrial cancer using the Endometrial Cancer Alternative Payment Model (ECAP): A companion paper to the Society of Gynecologic Oncology Report on the Endometrial Cancer Alternative Payment Model. Gynecol Oncol. 2018;149(2):241–7. 10.1016/j.ygyno.2018.02.011 [DOI] [PubMed] [Google Scholar]
- 25.Kwon H, Lee JH, Woo J, Lim W, Moon BI, Paik NS. Efficacy of a clinical pathway for patients with thyroid cancer. Head & neck. 2018;40(9):1909–16. [DOI] [PubMed] [Google Scholar]
- 26.Kreys ED, Koeller JM. Documenting the benefits and cost savings of a large multistate cancer pathway program from a payer's perspective. J Oncol Pract. 2013;9(5):e241–7. 10.1200/JOP.2012.000871 [DOI] [PubMed] [Google Scholar]
- 27.Hoverman JR, Cartwright TH, Patt DA, Espirito JL, Clayton MP, Garey JS, et al. Pathways, outcomes, and costs in colon cancer: retrospective evaluations in two distinct databases. Journal of oncology practice. 2011;7(3 Suppl):52s–9s. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 28.Neubauer MA, Hoverman JR, Kolodziej M, Reisman L, Gruschkus SK, Hoang S, et al. Cost effectiveness of evidence-based treatment guidelines for the treatment of non-small-cell lung cancer in the community setting. Journal of oncology practice. 2010;6(1):12–8. 10.1200/JOP.091058 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 29.Konski A, Yu JB, Freedman G, Harrison LB, Johnstone PA. Radiation Oncology Practice: Adjusting to a New Reimbursement Model. J Oncol Pract. 2016;12(5):e576–83. 10.1200/JOP.2015.007385 [DOI] [PubMed] [Google Scholar]
- 30.Waters TM, Kaplan CM, Graetz I, Price MM, Stevens LA, McAneny BL. Patient-Centered Medical Homes in Community Oncology Practices: Changes in Spending and Care Quality Associated With the COME HOME Experience. J Oncol Pract. 2019;15(1):e56–e64. 10.1200/JOP.18.00479 [DOI] [PubMed] [Google Scholar]
- 31.Colligan EM, Ewald E, Ruiz S, Spafford M, Cross-Barnet C, Parashuram S. Innovative Oncology Care Models Improve End-Of-Life Quality, Reduce Utilization And Spending. Health affairs (Project Hope). 2017;36(3):433–40. [DOI] [PubMed] [Google Scholar]
- 32.Kuntz G, Tozer JM, Snegosky J, Fox J, Neumann K. Michigan Oncology Medical Home Demonstration Project: first-year results. J Oncol Pract. 2014;10(5):294–7. 10.1200/JOP.2013.001365 [DOI] [PubMed] [Google Scholar]
- 33.Kohler RE, Goyal RK, Lich KH, Domino ME, Wheeler SB. Association between medical home enrollment and health care utilization and costs among breast cancer patients in a state Medicaid program. Cancer. 2015;121(22):3975–81. 10.1002/cncr.29596 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 34.Hollenbeck BK, Kaufman SR, Borza T, Yan P, Herrel LA, Miller DC, et al. Accountable care organizations and prostate cancer care. Urol Pract. 2017;4(6):454–61. 10.1016/j.urpr.2016.11.001 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 35.Herrel L, Hawken S, Ellimoottil C, Montgomery Z, Ye Z, Miller D. MP9-18 ANTICIPATING THE IMPACT OF ACCOUNTABLE CARE ORGANIZATIONS ON THE COST AND QUALITY OF UROLOGIC CANCER CARE. The Journal of urology.193(4):e108–e9. [Google Scholar]
- 36.Herrel LA, Norton EC, Hawken SR, Ye Z, Hollenbeck BK, Miller DC. Early impact of Medicare accountable care organizations on cancer surgery outcomes. Cancer. 2016;122(17):2739–46. 10.1002/cncr.30111 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 37.Lam MB, Figueroa JF, Zheng J, Orav EJ, Jha AK. Spending Among Patients With Cancer in the First 2 Years of Accountable Care Organization Participation. Journal of clinical oncology: official journal of the American Society of Clinical Oncology. 2018;36(29):2955–60. [DOI] [PubMed] [Google Scholar]
- 38.Schwartz AL, Chernew ME, Landon BE, McWilliams JM. Changes in Low-Value Services in Year 1 of the Medicare Pioneer Accountable Care Organization Program. JAMA internal medicine. 2015;175(11):1815–25. 10.1001/jamainternmed.2015.4525 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 39.Colla CH, Lewis VA, Gottlieb DJ, Fisher ES. Cancer spending and accountable care organizations: Evidence from the Physician Group Practice Demonstration. Healthcare (Amsterdam, Netherlands). 2013;1(3–4):100–7. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 40.Meyer CP, Krasnova A, Sammon JD, Lipsitz SR, Weissman JS, Sun M, et al. Accountable care organizations and the use of cancer screening. Prev Med. 2017;101:15–7. 10.1016/j.ypmed.2017.05.017 [DOI] [PubMed] [Google Scholar]
- 41.Mendenhall MA, Dyehouse K, Hayes J, Manzo J, Meyer-Smith T, Guinigundo A, et al. Practice Transformation: Early Impact of the Oncology Care Model on Hospital Admissions. J Oncol Pract. 2018:Jop1800409 10.1200/JOP.18.00409 [DOI] [PubMed] [Google Scholar]
- 42.Kopetz S, Chang GJ, Overman MJ, Eng C, Sargent DJ, Larson DW, et al. Improved survival in metastatic colorectal cancer is associated with adoption of hepatic resection and improved chemotherapy. Journal of clinical oncology: official journal of the American Society of Clinical Oncology. 2009;27(22):3677–83. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 43.Song XP, Tian JH, Cui Q, Zhang TT, Yang KH, Ding GW. Could clinical pathways improve the quality of care in patients with gastrointestinal cancer? A meta-analysis. Asian Pac J Cancer Prev. 2014;15(19):8361–6. [DOI] [PubMed] [Google Scholar]
- 44.Andre T, Boni C, Mounedji-Boudiaf L, Navarro M, Tabernero J, Hickish T, et al. Oxaliplatin, fluorouracil, and leucovorin as adjuvant treatment for colon cancer. The New England journal of medicine. 2004;350(23):2343–51. 10.1056/NEJMoa032709 [DOI] [PubMed] [Google Scholar]
- 45.Sargent DJ, Wieand HS, Haller DG, Gray R, Benedetti JK, Buyse M, et al. Disease-free survival versus overall survival as a primary end point for adjuvant colon cancer studies: individual patient data from 20,898 patients on 18 randomized trials. Journal of clinical oncology: official journal of the American Society of Clinical Oncology. 2005;23(34):8664–70. [DOI] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Supplementary Materials
(DOCX)
(DOCX)
(DOCX)
(DOCX)
(DOCX)
Data Availability Statement
All relevant data are within the manuscript and its Supporting Information files.