Abstract
The aim of this study was to conduct a systematic mapping review of the literature that explored associations of pregnancy intentions with health-related lifestyle behaviours and psychological wellbeing before and during pregnancy. Six databases were searched (May 2017) for papers relating to pregnancy intentions, health-related lifestyle behaviours, and psychological wellbeing. The literature was mapped according to the preconception or pregnancy period; prospective or retrospective variable assessment; and reported lifestyle behaviours and psychological wellbeing outcomes. Of 19,430 retrieved records, 303 studies were eligible. Pregnancy intentions were considered during the preconception period in 103 studies (only 23 assessed prospectively), and during the pregnancy period in 208 studies (141 prospectively). Associations between pregnancy intention and preconception behaviours/psychological wellbeing were primarily reported for supplement use (n = 58) and were lacking for diet/exercise, and psychological factors. For behaviours/psychological wellbeing during pregnancy, associations with pregnancy intention were focused on prenatal care (n = 79), depression (n = 61), and smoking (n = 56) and were lacking for diet/exercise. Only 7 studies assessed pregnancy intentions with a validated tool. Despite a large body of literature, there were several methodological limitations identified, namely assessment of pregnancy intentions with non-validated measures and the reliance on retrospective assessment. Future primary studies are needed to fill gaps in our understanding regarding energy-balance-related behaviours. Future studies (including reviews/meta-analyses) should take care to address the noted limitations to provide a comprehensive and accurate understanding of the relationships between pregnancy intentions and health-related lifestyle behaviours and psychological wellbeing before and during pregnancy.
Keywords: Pregnancy intention, Pregnancy planning, Preconception, Pregnancy, Lifestyle, Behaviour, Psychological wellbeing
Highlights
-
•
Reliance on the assessment of pregnancy intentions with non-validated measures
-
•
Reliance on retrospective assessment
-
•
Studies on preconception pregnancy intentions and diet/exercise lacking
1. Introduction
Suboptimal lifestyle behaviours before and during pregnancy are associated with adverse maternal and infant outcomes. The maternal intrauterine environment is susceptible to epigenetic modifications as a result of poor maternal lifestyle periconceptionally, which are proposed to be implicated in adverse fetal and infant outcomes (Barua and Junaid, 2015; Lane et al., 2014). For example, low intake of folic acid periconception is associated with increased prevalence of neural tube defects in babies (Wolff et al., 2009). Before and during pregnancy, smoking and excessive alcohol consumption are linked with poor fetal and infant health (Flak et al., 2014; Patra et al., 2011; Pineles et al., 2014; U.S. Department of Health and Human Services, 2014). Poor lifestyle behaviours during this life phase also contribute to maternal overweight and obesity, which is linked to adverse maternal and offspring outcomes (Callaway et al., 2006; Pantasri and Norman, 2014). Poor psychological wellbeing can impact women's abilities to engage in positive health behaviours (Baskin et al., 2015; Hill et al., 2016; Teychenne and York, 2013). At times of increased risk of distress before and during pregnancy, this impact may be heightened. Facilitating positive behaviour change both before and during pregnancy is therefore essential for realising favourable maternal and infant outcomes (Gardner et al., 2011; Hill et al., 2013; Pearce et al., 2013; The International Weight Management in Pregnancy (i-WIP) Collaborative Group, 2017).
Pregnancy planning and intentions are important considerations in understanding motivations for behaviour change before and during pregnancy. Firstly, there is an association between unintended or unwanted pregnancies and adverse neonatal outcomes such as preterm birth and low birthweight (Hall et al., 2017; Shah et al., 2011). Secondly, up to approximately 50% of pregnancies are unplanned, albeit this varies geographically and by socioeconomic position and can be challenging to measure (Bearak et al., 2018; Finer and Zolna, 2016). Hence, understanding the modifiable determinants of health in women with and without pregnancy intentions presents a valuable opportunity for intervention, tailored to the needs of women, that may lead to more positive outcomes for mothers and babies. Indeed, Gipson et al. (2008) posit that a relationship between pregnancy intention and birth outcomes may be mediated by antenatal maternal behaviours. Women who are intending to get pregnant and therefore identify as “preconception” are a specific target population for healthy lifestyle (Lewis et al., 2013). Women who are not intending to become pregnant may still be a “preconception population” if they are of reproductive age and sexually active, but may need a different approach to motivate them to engage in or maintain healthy lifestyle behaviours. Women who are already pregnant and indicate that their pregnancy was unintended may have different ideas about their health needs than women with planned pregnancies. A recent Lancet series on preconception took the perspective of a life-course approach – public health approaches are needed for all women of reproductive age, but women planning pregnancy require specific, targeted health promotion (Stephenson et al., 2018). Given the potential for adverse health impacts of unintended pregnancies on mothers and babies, understanding the wellbeing and behaviours of women with unintended pregnancies is as important, if not more so, than women with intended pregnancies who are potentially primed for behaviour change and motivated to be healthy for the sake of their baby.
It is well established that psychological health (including mental health, happiness and quality of life) and lifestyle are intertwined (Bize et al., 2007; Rubin et al., 2014; Taylor et al., 2014). This is also true of the perinatal period (Hill et al., 2016). Given the importance of lifestyle behaviours and psychological wellbeing as key constructs of interest during preconception and pregnancy (Hall et al., 2017; Stephenson et al., 2018; Delissaint and McKyer, 2011), exploring these associations and identifying gaps in the literature is crucial for future research and/or for informing the development of interventions designed to optimise behaviours and health outcomes for mothers and their babies. A paucity of systematic reviews have been conducted with the key aim of exploring the association between pregnancy intentions and various lifestyle behaviours or psychological wellbeing factors (Abajobir et al., 2016; Dibaba et al., 2013). To our knowledge, only two reviews with a focus on pregnancy intentions were identified – exploring depression (Abajobir et al., 2016) and antenatal care (Dibaba et al., 2013). We could not locate any systematic reviews or meta-analyses that specifically synthesised the evidence of the relationship between pregnancy intentions and preconception folic acid intake, smoking behaviour or alcohol intake preconception or during pregnancy, albeit one study incorporated these relationships (smoking and alcohol) into a larger research question (Edelman et al., 2015). Furthermore, existing reviews do not account for several limitations within the literature such as variations in measurement of pregnancy intentions (e.g., categorisation of intendedness or timing of assessment). Furthermore, while a recent scoping review identified a range of important preconception health behaviours, only four of the included studies reported on assocations with pregnancy intentions (Toivonen et al., 2017). It is therefore apparent that, despite the importance of targeting the preconception and pregnancy periods as vital health risk prevention and promotion opportunities (e.g., as identified by the World Health Organization, 2016, World Health Organization, 2013, the UK National Institute for Health and Care Excellence (2010) and the US Institute of Medicine (2009)), work is needed to synthesise this body of literature. In particular, our understanding of the associations between lifestyle behaviours or psychological wellbeing and pregnancy intentions is lacking comprehensive and systematic evaluation, which is needed to inform future studies that can lead to effective interventions and move towards implementation, translation, and policy development.
The overall aim of this study was, therefore, to conduct a systematic mapping review of the literature that explores associations of pregnancy intentions with health-related lifestyle behaviours and psychological wellbeing before and during pregnancy. Specifically, we sought to understand which behaviours and psychological wellbeing constructs have been investigated with regards to pregnancy intentions and explore methodological aspects pertaining to the assessment of variables in the studies. A mapping review enables identification of gaps in the evidence base, providing an overarching summary of the literature to guide the development of narrower research, policy or practice-relevant questions and inform priority areas for future reviews (Grant and Booth, 2009). Therefore, a mapping review may act as a precursor to one, or several, systematic reviews or meta-analyses. Given the relative lack of comprehensive systematic reviews exploring pregnancy intentions with lifestyle or psychological factors to date, this mapping review was required to help guide future reviews to focus on existing gaps in the literature and ensure future primary studies are aware of relevant methodological limitations that can be addressed.
2. Method
This review was prospectively registered on the International Prospective Register of Systematic Reviews (PROSPERO; CRD42016039485). Search and data extraction methods concord with the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) Statement (Moher et al., 2009).
2.1. Information sources and search strategy
The following databases were searched for all relevant papers relating to pregnancy intentions, health-related lifestyle behaviours, and psychological wellbeing: Medline Complete, PsycINFO, CINAHL Complete, Global Health, Embase, and INFORMIT: Health Subset. Search terms included (un)intended pregnancy, (un)planned pregnancy, (un)wanted pregnancy and derivatives; lifestyle behaviours including smoking, diet, physical activity/sedentary behaviour, weight management, alcohol intake, drug use, substance use, folic acid intake, medication adherence, prenatal or antenatal care, preconception care; behaviours relating to care in polycystic ovary syndrome, epilepsy, diabetes and thyroid disease; and terms pertaining to psychological wellbeing including depression, anxiety, stress, body image, wellbeing, quality of life, self-esteem, positive emotions, and mental health. Search concepts were combined as (1) pregnancy intentions AND health-related lifestyle behaviours, and (2) pregnancy intentions AND psychological wellbeing. The full search strategy for the Medline database is presented in Appendix Table 1. The search was conducted in May 2017. No date limits were applied. Reference lists of all included full texts were perused for additional eligible papers. Given the scope of this review and the large number of articles, study authors were not contacted for additional information.
2.2. Eligibility and exclusion criteria
Eligibility criteria were outlined using the PICO (participants, intervention/exposure, comparator, outcome) framework (see Appendix Table 2). Here, ‘outcome’ was indicated to be any health-related lifestyle behaviour or psychological wellbeing factor (whether or not it was treated as a dependent or independent variable in any given study). Studies exploring the association between pregnancy intention and health-related lifestyle behaviours and/or psychological wellbeing before (preconception) or during pregnancy were eligible for inclusion. Studies were limited to quantitative studies of any design (including cohort, case control and baseline data from intervention studies) published in English.
Studies relating to women seeking abortion, focused solely on contraception or relating only to the postpartum period that did not include an inter-partum perspective were excluded. Protocol papers, review articles, animal studies, unpublished/grey literature, and conference abstracts were also ineligible.
2.3. Study selection and screening
After removal of duplicates, titles and abstracts were screened by one of two authors (BH or SC) with discrepancies resolved by discussion. Inter-rater agreement on a subset of 10% of the total number of retrieved papers was conducted using Cohen's Kappa to establish reliability, (Kappa = 0.945; Cohen, 1960). Full text screening was conducted by one of four authors (BH, EJK, MD or SC); inter-rater agreement on a subset of 10% of the papers retained for full text screening was conducted using Fleiss' Kappa to establish reliability (Kappa = 0.744; Fleiss, 1971). Any discrepancies were resolved by discussion between two of the screening authors (BH and MD), with the opinion of a third author (EJK) requested if needed.
2.4. Data extraction and synthesis of results
Data were extracted in duplicate and then assessed by a third author (BH) to check for discrepancies. Any discrepancies were evaluated and resolved with direct reference to the paper. Data were entered into an online survey using Qualtrics software (Qualtrics, Provo, UT) and exported into Microsoft Excel (Version 16.2) before synthesis. Information were collected relating to the study author, year, country, and aims; participant characteristics (including population, sample size, setting, inclusion/exclusion criteria, age, and ethnicity); methods (study design, measures, analyses conducted); and main findings. As per the methods described by Grant and Booth (2009) risk of bias assessment was not conducted for the mapping review.
Findings were synthesised narratively across studies according to the following categories: whether the study related to the preconception or pregnancy period; timing of assessment of pregnancy intentions and/or lifestyle behaviours or psychological wellbeing; the lifestyle behaviours and psychological wellbeing outcomes represented in the literature; and whether the population related to developed or developing nations (classified according to the World Economic Situation and Prospects) (United Nations Department of Economic and Social Affairs, 2014).
3. Results
3.1. Study selection
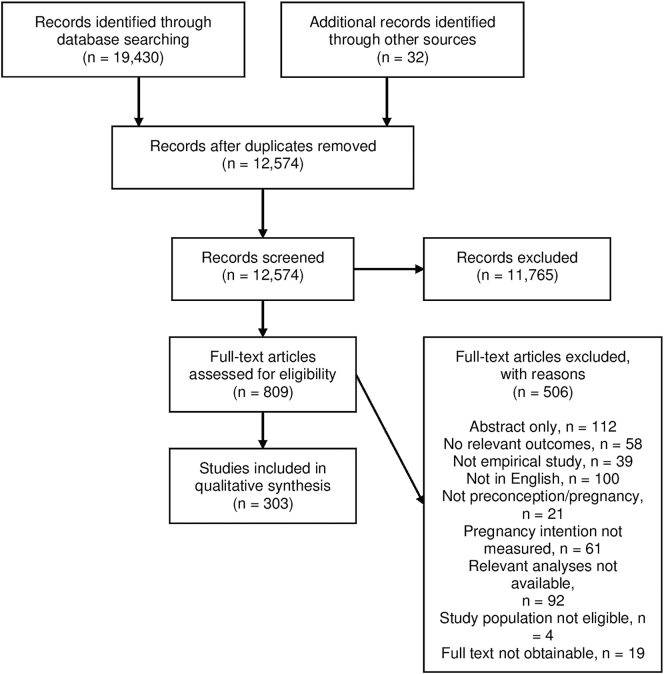
Fig. 1 presents the flow of studies in the review. The search retrieved 19,430 records for screening. After removal of duplicates, 12,574 titles and abstracts were screened, and 809 full-text articles assessed for eligibility. In total, 303 studies were eligible for inclusion and a full list of included studies is available in Appendix Table 3.
Fig. 1.
Flow of studies in the review.
3.2. Study characteristics
Details regarding study aims, participant characteristics, methods, and main findings are available in Appendix Table 4. In the 303 studies, 2,618,066 participants took part, with a minimum sample size of 50 (a UK-based study with women with diabetes) (Wills and Page, 2001) and maximum of 424,065 (a study of 30 sub-Saharan African nations) (Amo-Adjei and Anamaale Tuoyire, 2016). Two hundred and five studies were conducted in developed nations, 96 in developing nations, one study combined 32 low-income countries (Guliani et al., 2014), and in one study the country could not be identified (DeLuca and Lobel, 1995). Africa, Asia, Europe, Latin America and the Caribbean, North America and Oceania were all represented. One hundred and sixty-five studies were cross-sectional in design, 90 were cohort studies (e.g., Pregnancy Risk Assessment Monitoring System, Behavioral Risk Factor Surveillance System, National Survey of Family Growth), 27 were prospective observational studies, 15 were case-control studies, 3 were interventions, and there was 1 two-stage cluster sample design, 1 retrospective study, and 1 validation study.
Table 1 describes the timing of assessments for pregnancy intentions and the outcomes reported pertaining to health-related lifestyle behaviours and/or psychological wellbeing. The timing of assessment of pregnancy intention was ambiguous in many studies; in these instances, timing was assumed based on the information available (e.g., in pregnant women if the study asked only if the pregnancy was planned or unplanned, then it was assumed this pertained to the woman's current feelings). One hundred and three studies (33%) measured preconception pregnancy intentions; of these, 23 (7%) were prospectively measured during the preconception period, and the remaining 80 (26%) were focused on the preconception period retrospectively, with assessment during pregnancy or postpartum. Two hundred and eight (67%) studies assessed women's pregnancy intentions relating to when they were pregnant. Regarding timing of assessment of lifestyle and psychological variables, 109 (29%) studies measured these factors relating to preconception, with only 22 (6%) of these prospectively assessed before pregnancy, while 264 (71%) measured these outcomes as they related to the antenatal period (proportions add up to greater than 100% because variables could be measured in multiple ways in a study). Seven studies (Backhausen et al., 2014; Borges et al., 2016; Gariepy et al., 2017; Goossens et al., 2016; Lachance-Grzela and Bouchard, 2009; Rassi et al., 2013; Stephenson et al., 2014) assessed pregnancy intentions with the London Measure of Unplanned Pregnancy (LMUP) (Barrett et al., 2004) and the remaining studies used measures that have not been validated, with the exception of Backhausen et al. (2014) who used both the LMUP and the Swedish Pregnancy Planning Scale, a single item pregnancy planning scale that has been validated against the LMUP (Drevin et al., 2017).
Table 1.
Timing of assessments for pregnancy intentions and health-related lifestyle behaviours and/or psychological wellbeing factors.
| Timing of assessment | Example item and citation | Number of studies (n) |
|---|---|---|
| Pregnancy intentions | ||
| Measured preconception | Women were asked when they wanted to bear their next child, as soon as possible, within two years, after two years, or do not want more children (Barrick and Koenig, 2008). | 23 |
| Measured during pregnancy | Pregnant women were asked whether or not the pregnancy was wanted or planned (Alderliesten et al., 2007). | 141 |
| Assessed retrospectively during pregnancy about preconception | Pregnant women were asked: “Now think back to just before you became pregnant. Which of the following statements best describes how you felt at that time?” (1) I wanted to get pregnant; (2) I didn't want to get pregnant, but I didn't mind getting pregnant; (3) 1 didn't want to get pregnant when I did; (4) neither (Altfeld et al., 1997). | 28 |
| Assessed retrospectively during postpartum about preconception | Postpartum women were asked: “Thinking back to just before you got pregnant, how did you feel about becoming pregnant?” (1) I wanted to be pregnant sooner; (2) I wanted to be pregnant later; (3) I wanted to be pregnant then; (4) I didn't want to be pregnant then or at any time in the future; (5) I don't know; or, (6) I refuse to answer (Humbert et al., 2011). | 52 |
| Assessed retrospectively during postpartum about pregnancy | Postpartum women were asked whether or not their last pregnancy was planned (Mikhail, 2000). | 67 |
| Outcomes | ||
| Measured preconception | Preconception women were asked to report their exercise in the last week (Berenson et al., 2014). | 22 |
| Measured during pregnancy | Pregnant women completed the Center for Epidemiologic Studies – Depression Scale (Littleton, 2015). | 161 |
| Assessed retrospectively during pregnancy about preconception | Pregnant women were asked whether they had taken folic acid before their current pregnancy (McDonnell et al., 1999). | 37 |
| Assessed retrospectively during postpartum about preconception | Postpartum women were asked: “How many times did you drink 5 or more alcoholic drinks at 1 sitting in the preconception period? The preconception period was defined as “the 3 months before you got pregnant”” (Naimi et al., 2003). | 50 |
| Assessed retrospectively during postpartum about pregnancy | Postpartum women were asked about their smoking habits during their pregnancy (Paterson et al., 2003). | 104 |
3.3. Studies assessing the relationship between pregnancy intentions and health-related lifestyle behaviours or psychological wellbeing
3.3.1. Preconception lifestyle behaviours or psychological wellbeing
Although 109 studies reported measuring preconception health-related lifestyle behaviours or psychological wellbeing, only 102 of these reported an assessment of these variables in conjunction with pregnancy intention (this discrepancy arises due to some studies not reporting the analyses or where pregnancy but not preconception data were reported). Table 2 presents the frequency counts for preconception variables (studies can report more than one variable). Supplement use (including folic acid) was the most commonly reported behaviour (n = 58), followed by alcohol use (n = 36) and smoking (n = 32). Of note, preconception weight-related lifestyle behaviours such as exercise/physical activity and diet/nutrition were assessed in relation to pregnancy intention in only 13 studies. Few studies (n = 8) assessed psychological wellbeing in relation to pregnancy intention.
Table 2.
Number of studies reporting associations between pregnancy intentions and preconception lifestyle behaviour or psychological wellbeing.
| Preconception outcome | Number of studies (n) |
|---|---|
| Preconception care | 8 |
| Smoking | 32 |
| Alcohol intake/use | 36 |
| Substance use (other than tobacco or alcohol) | 6 |
| Exercise/physical activity | 7 |
| Diet and nutrition | 6 |
| Supplement use (including folic acid) | 58 |
| Medication adherence (other than supplement use) | 1 |
| Depression | 4 |
| Anxiety | 1 |
| Stress | 3 |
| Body image/body dissatisfaction | 0 |
| Quality of life | 0 |
| Psychiatric diagnosis | 0 |
| Othera | 9 |
“Other” included unhealthy weight loss behaviours; caffeine; blood glucose control/diabetes control; combined health actions/behaviours; self-efficacy; paracetamol use; and overall mental health symptoms.
3.3.2. Pregnancy lifestyle behaviours or psychological wellbeing
Although 265 studies reported measuring antenatal psychological wellbeing or health-related lifestyle behaviours, only 235 of these reported an assessment of these outcomes in conjunction with pregnancy intention (this discrepancy arises due to some studies not reporting the analyses or where preconception but not pregnancy data were reported). Table 3 presents the frequency counts for antenatal variables (studies can report more than one variable). The most commonly reported outcome was prenatal care (including timely initiation and adequacy of care; n = 79). Sixty-one studies explored the association between antenatal depression and pregnancy intention, while 56 studies investigated smoking and 43 reported on alcohol intake/use. Only two studies reported on the association between pregnancy intention and exercise/physical activity in pregnancy (Cheng et al., 2016; Rodriguez et al., 2000). Five studies evaluated the association between pregnancy intention and diet/nutrition, however only three of these studies included a measure of healthy eating or adequate nutrition (Arslan Ozkan and Mete, 2010; Leeper et al., 1992; Okesene-Gafa et al., 2016); the other two studies assessed only intake of specific fortified foods (Bower et al., 2005; Mallard and Houghton, 2014).
Table 3.
Number of studies reporting associations between pregnancy intentions and pregnancy lifestyle behaviour or psychological wellbeing.
| Pregnancy outcome | Number of studies (n) |
|---|---|
| Antenatal (prenatal) care | 79 |
| Smoking | 56 |
| Alcohol intake/use | 43 |
| Substance use (other than tobacco or alcohol) | 13 |
| Exercise/physical activity | 2 |
| Diet and nutrition | 5 |
| Supplement use (including folic acid) | 29 |
| Medication adherence (other than supplement use) | 2 |
| Depression | 61 |
| Anxiety | 15 |
| Stress | 10 |
| Body image/body dissatisfaction | 0 |
| Quality of life | 3 |
| Psychiatric diagnosis | 7 |
| Othera | 19 |
“Other” included mood; caffeine; diabetes/blood sugar control; general mental health/affective disorder; wellbeing/happiness; medication use (not adherence); overall health behaviours; paracetamol use; dental care; overall healthy lifestyle; self-esteem.
4. Conclusions
The aim of this study was to conduct a systematic search and create a map of the literature that reported on associations of pregnancy intentions with health-related lifestyle behaviours and psychological wellbeing before and during pregnancy. Here, we advance the literature beyond previous narrow and more limited reviews and identify areas requiring additional investigation. While a large number of identified studies (n = 303) measured pregnancy intentions and a range of psychological and lifestyle variables, there was a focus on a small subset of behaviours, primarly preconception folic acid intake, initation of antenatal care, smoking and alcohol use. This is consistent with a recent scoping review of preconception health behaviours (Toivonen et al., 2017).
Our search revealed a limited number of studies reporting obesity-related behaviours such as physical activity/sedentary behaviour and diet/nutrition. Given that both unintended pregnancy and obesity are associated with adverse obstetric and fetal outcomes (Hall et al., 2017; Shah et al., 2011; Catalano and Shankar, 2017), exploring the relationship between these factors is an essential step to: (1) understanding the relationships between individual determinants of health and, (2) beginning to unpack the pathways by which pregnancy intentions and lifestyle behaviours impact on health outcomes. This is particularly important for the preconception period, which is a relatively new area of research in terms of weight management across the reproductive life phase, and where women can potentially be targeted via their pregnancy intention status to improve their diet and physical activity behaviours (Stephenson et al., 2018; Lan et al., 2017).
Psychological factors were also rarely assessed in the literature in relation to preconception pregnancy intentions. In contrast, both depression and anxiety were evaluated frequently in pregnancy; these relationships have been assessed in several reviews as a primary or secondary research question (Abajobir et al., 2016; Biaggi et al., 2016; Fisher et al., 2012; Lancaster et al., 2010). The number of studies included in these reviews ranged from three to 22, much lower than the current study where 61 studies reporting on depression and 15 for anxiety were identified. Depression and anxiety history are commonly cited as risk factors for the development of antenatal and postnatal depression (Biaggi et al., 2016; Silverman et al., 2017). Hence, furthering our understanding of the association between psychological factors and pregnancy intentions preconceptually may shed additional light on potential opportunties for screening and/or intervention to prevent mental health issues and their impact on mothers and their infants. It is clear that additional preconception primary studies and comprehensive meta-analyses for pregnancy are needed in this research space.
The timing of assessment of pregnancy intentions varied considerably across studies. The majority of preconception pregnancy intentions were evaluated during pregnancy, while only 7% of studies measured pregnancy intentions during the preconception period. This lack of prospective evaluation of pregnancy intentions introduces a potential source of bias. Pregnancy intention is not static and retrospective assessment of pregnancy intention results in pregnancies that were prospectively classified as unwanted to be re-classified as wanted or mistimed (i.e., wanted but not at this time), perhaps because mothers are reluctant to describe an existing child as unwanted (Koenig et al., 2006). Indeed, women appear able to clearly distinguish between their thoughts on events before pregnancy and amend, in light of new experiences, their thoughts on events after conception (Barrett et al., 2004). This potential inaccuracy in pregnancy intention assessment makes it difficult to draw conclusions about the relationship between intentions and lifestyle behaviours or psychological wellbeing as pregnancy intentions may change over time. Only one existing review has tried to account for this issue, conducting sub-group analysis by study design (cross-sectional vs. longitudinal), but did not specifically investigate retrospective versus prospective assessment of pregnancy intentions (Delissaint and McKyer, 2011). Future research should consider classifying studies according to retrospective/prospective assessment of pregnancy intention and/or conducting sub-group analyses based on mode of intention assessment. As such, where behavioural and psychological measures have not been assessed extensively in relation to pregnancy intention, additional primary studies are needed to build the evidence base, particularly for prospective evaluation of pregnancy intention.
An additional issue with the asessment of pregnancy intentions was that intentions were often assessed by a single item question (e.g., “was your pregnancy intended?”) and at times the measure was not even provided (i.e., pregnancy intention was reported in the results as yes/no with no mention of how it was assessed in the method). Furthermore, pregnancy intentions were evaluated in a multitude of ways including unintended, intended, mistimed, unplanned, planned, unwanted, wanted, reactions to pregnancy (e.g., happy), or contraceptive use (or lack of). Some studies also combined unintended and mistimed pregnancies together (e.g., Adams et al., 1993; Ali, 2016), while others combined intended and mistimed together (e.g., Blake et al., 2007). Only seven of the 303 studies used a validated scale to assess pregnancy planning (albeit to our knowledge, neither the LMUP nor Swedish Pregnancy Planning Scare are validated for preconception) (Barrett et al., 2004; Drevin et al., 2017). Hence, the range of measures used does not necessarily tap into the same aspects of pregnancy intentions and are a potential source of heterogeneity among the literature. Of two reviews that specifically evaluated the relationship between pregnancy intention and antenatal care or depression, only the study by Abajobir et al. (2016) conducted a sub-group analysis by measurement type (unwanted and mistimed). Furthermore, many of these measures do not encompass the complexity of pregnancy intendedness, which may incorporate cognitive, affective, cultural and contextual dimensions (Tsui et al., 2010). The variation in the assessment and reporting of pregnancy intentions may be evident across the literature because the current review utilised broad inclusion criteria whereby all studies exploring the association between pregnancy intention and health-related lifestyle behaviours and/or psychological wellbeing preconception or during pregnancy were eligible. This means that studies were included in this review where the relationship between variables of interest was reported but were not necessarily the primary aim or outcome of the study. This strategy was selected to gain a comprehensive perspective of the state of the literature. It has also resulted in a greater number of studies identified than have been included in the two existing systematic reviews of pregnancy intentions (i.e., depression and antenatal care use) and which may provide opportunities for further insight into how depression and antenatal care use are associated with pregnancy intention. Finally, with pregnancy intentions being such an important part of our efforts to strategically target and tailor behaviour change interventions for preconception women, reliable and valid evaluation of pregnancy intentions (e.g., using the LMUP) is essential.
4.1. Strengths and limitations
This study employed a comprehensive search strategy, a dual reviewer screening process with reliability checks, and double data extraction with arbitrator checking. While risk of bias assessment was not undertaken due to the volume of included studies and is not necessary for a mapping review (Grant and Booth, 2009), future reviews synthesising this body of literature should formally evaluate the quality of included literature. Combining terms such as pregnancy intentions and planning, as was done here, may have masked some nuances of the impact pregnancy intention or planning status may have on behavioural or psychological variables; this can be evaluated in future reviews that extend the work done here. Additionally, this review explored only whether relationships between variables were reported; synthesis of the direction or strength of the relationship, the type of analyses that were conducted and whether studies accounted for relevant covariates is beyond the scope of this mapping review, albeit these are essential factors in future reviews with more specific research questions. We considered providing a summary of the overall findings for each lifestyle behaviour or psychological wellbeing variable, however, given the limitations revealed in the literature (i.e., reliance on retrospective assessment and non-validated measurement of pregnancy intentions), such a summary would not be able to account for these limitations and may provide a skewed view of the findings. Finally, it is important to note that this review focused on literature evaluating women's pregnancy intentions only and excluded studies with men. However, the influence of men's family intentions and their lifestyle factors before conception on the health of their offspring are important and must continue to be explored in future studies (Lindberg and Kost, 2014; Fleming et al., 2018).
4.2. Recommendations
This mapping review identified 303 studies that explored the relationshp between pregnancy intentions and a range of lifestyle behaviour and psychological variables. Meta-analyses are needed to comprehensively synthesise the large amount of data available into useful and relevant findings and several specific opportunities for future research have been revealed. These include:
-
(1)
Additional primary studies that explore and report on the relationship between pregnancy intentions and preconception variables including preconception care, substance use (not including alcohol and tobacco), and psychological factors.
-
(2)
Additional primary studies that explore and report on the relationship between pregnancy intentions (assessed prospectively where practicable) and lifestyle behaviours and psychological factors during pregnancy, including medication adherence, body image and quality of life.
-
(3)
A focus on obesity-related lifestyle behaviours such as diet and physical activity and how they are associated with pregnancy intentions.
-
(4)
Systematic reviews and meta-analyses synthesising the literature on prospectively assessed preconception pregnancy intentions and folic acid; and the relationship of pregnancy intentions both preconception and during pregnancy with smoking/alcohol intake.
-
(5)
Consideration of factors such as the prospective, comprehensive and uniform assessment of pregnancy intentions, including the use of validated measures, in future primary and review studies. Meta-analyses should consider sub-group and/or sensitivity analyses to explore any effects of different measurement tools and categorisations of pregnancy intentions.
4.3. Conclusions
Addressing the gaps in the pregnancy intentions literature will contribute significantly to our understanding of when and how to intervene appropriately prior to and during pregnancy to promote maternal wellbeing, complementing broader life-course approaches and may identify additional opportunities to prevent unplanned pregnancies and promote pregnancy planning. By meaningfully synthesising the existing literature we can gain a comprehensive and accurate understanding of the interaction between pregnancy intentions preconceptually and during pregnancy with relevant behavioural and psychological factors; we can minimise duplication of effort; and we can generate high-quality evidence to offer insights that will drive the development of policy and practice-based guidelines, rather than relying on assumptions made from the inadequate current syntheses of the literature. This course of study is important to improving women's lifestyle behaviours, psychological wellbeing, and, in turn, maternal and infant outcomes.
Conflict of interest and funding
Dr. Briony Hill is supported by a National Health and Medical Research Council (NHMRC) Early Career Fellowship (GNT1120477). Adina Y. Lang is supported by an NHMRC Postgraduate Research Scholarship (GNT1114924). Associate Professor Lisa Moran is supported by a National Heart Foundation of Australia Future Leader Fellowship (101169). Professor Helena Teede is supported by a Medical Research Future Fund NHMRC Practitioner fellowship (MRF1139455). The authors declare no conflict of interest. The grant organisations had no involvement or decision in any aspect of the study.
Acknowledgements
The authors would like to thank Nicola Ivory and Dr. Mathew Ling for their contribution to various aspects of data acquisition for this article. The authors would also like to thank Tze Lin Chai for her assistance with preparation of supplementary material.
Footnotes
Supplementary data to this article can be found online at https://doi.org/10.1016/j.pmedr.2019.100869.
Contributor Information
Briony Hill, Email: briony.hill@monash.edu.
Emily J. Kothe, Email: emily.kothe@deakin.edu.au.
Sinéad Currie, Email: sinead.currie@stir.ac.uk.
Meaghan Danby, Email: meaghan.danby@deakin.edu.au.
Adina Y. Lang, Email: adina.lang@monash.edu.
Cate Bailey, Email: cate.bailey@monash.edu.
Lisa J. Moran, Email: lisa.moran@monash.edu.
Helena Teede, Email: helena.teede@monash.edu.
Madelon North, Email: maddie.north@deakin.edu.au.
Lauren J. Bruce, Email: lauren.bruce@monash.edu.
Helen Skouteris, Email: helen.skouteris@monash.edu.
Appendix A. Appendix tables 1–4
Supplementary tables
References
- Abajobir A.A., Maravilla J.C., Alati R., Najman J.M. A systematic review and meta-analysis of the association between unintended pregnancy and perinatal depression. J. Affect. Disord. 2016;192:56–63. doi: 10.1016/j.jad.2015.12.008. [DOI] [PubMed] [Google Scholar]
- Adams M.M., Bruce F.C., Shulman H.B., Kendrick J.S., Brogan D.J. Pregnancy planning and pre-conception counseling. The PRAMS Working Group. Obstet. Gynecol. 1993;82(6):955–959. [PubMed] [Google Scholar]
- Alderliesten M.E., Vrijkotte T.G., van der Wal M.F., Bonsel G.J. Late start of antenatal care among ethnic minorities in a large cohort of pregnant women. BJOG. 2007;114(10):1232–1239. doi: 10.1111/j.1471-0528.2007.01438.x. [DOI] [PubMed] [Google Scholar]
- Ali A. Relationship between unwanted pregnancy and health-related quality of life in pregnant women. J. Coll. Physicians Surg. Pak..2016;26(6):507–12. ID:2352. [PubMed]
- Altfeld S., Handler A., Burton D., Berman L. Wantedness of pregnancy and prenatal health behaviors. Womens Health. 1997;26(4):29–43. doi: 10.1300/j013v26n04_03. [DOI] [PubMed] [Google Scholar]
- Amo-Adjei J., Anamaale Tuoyire D. Effects of planned, mistimed and unwanted pregnancies on the use of prenatal health services in sub-Saharan Africa: a multicountry analysis of Demographic and Health Survey data. Tropical Med. Int. Health. 2016;21(12):1552–1561. doi: 10.1111/tmi.12788. [DOI] [PubMed] [Google Scholar]
- Arslan Ozkan I., Mete S. Pregnancy planning and antenatal health behaviour: findings from one maternity unit in Turkey. Midwifery. 2010;26(3):338–347. doi: 10.1016/j.midw.2008.07.005. [DOI] [PubMed] [Google Scholar]
- Backhausen M.G., Ekstrand M., Tyden T., Magnussen B.K., Shawe J., Stern J., Hegaard H.K. Pregnancy planning and lifestyle prior to conception and during early pregnancy among Danish women. Eur J Contracept Reprod Health Care. 2014;19(1):57–65. doi: 10.3109/13625187.2013.851183. [DOI] [PubMed] [Google Scholar]
- Barrett G., Smith S.C., Wellings K. Conceptualisation, development, and evaluation of a measure of unplanned pregnancy. J. Epidemiol. Community Health. 2004;58(5):426–433. doi: 10.1136/jech.2003.014787. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Barrick L., Koenig M.A. Pregnancy intention and antenatal care use in two rural north Indian States. World Health Popul. 2008;10(4):21–37. [PMC free article] [PubMed] [Google Scholar]
- Barua S., Junaid M.A. Lifestyle, pregnancy and epigenetic effects. Epigenomics. 2015;7(1):85–102. doi: 10.2217/epi.14.71. [DOI] [PubMed] [Google Scholar]
- Baskin R., Hill B., Jacka F.N., O'Neil A., Skouteris H. The association between diet quality and mental health during the perinatal period. A systematic review. Appetite. 2015;91(41–7) doi: 10.1016/j.appet.2015.03.017. [DOI] [PubMed] [Google Scholar]
- Bearak J., Popinchalk A., Alkema L., Sedgh G. Global, regional, and subregional trends in unintended pregnancy and its outcomes from 1990 to 2014: estimates from a Bayesian hierarchical model. Lancet Glob. Health. 2018;6(4):e380–e389. doi: 10.1016/S2214-109X(18)30029-9. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Berenson A.B., Pohlmeier A.M., Laz T.H., Rahman M., McGrath C.J. Nutritional and weight management behaviors in low-income women trying to conceive. Obstet. Gynecol. 2014;124(3):579–584. doi: 10.1097/AOG.0000000000000416. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Biaggi A., Conroy S., Pawlby S., Pariante C.M. Identifying the women at risk of antenatal anxiety and depression: a systematic review. J. Affect. Disord. 2016;191:62–77. doi: 10.1016/j.jad.2015.11.014. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Bize, Johnson J.A., Plotnikoff R.C. Physical activity level and health-related quality of life in the general adult population: a systematic review. Prev. Med. 2007;45(6):401–415. doi: 10.1016/j.ypmed.2007.07.017. [DOI] [PubMed] [Google Scholar]
- Blake S.M., Kiely M., Gard C.C., El-Mohandes A.A., El-Khorazaty M.N. Pregnancy intentions and happiness among pregnant black women at high risk for adverse infant health outcomes. Perspect. Sex. Reprod. Health. 2007;39(4):194–205. doi: 10.1363/3919407. [DOI] [PubMed] [Google Scholar]
- Borges A.L.V., Santos OAd, Nascimento NdC, Chofakian N., Gomes-Sponholz F.A. Preconception health behaviors associated with pregnancy planning status among Brazilian women. Revista da Escola de Enfermagem da USP. 2016;50:208–216. doi: 10.1590/S0080-623420160000200005. [DOI] [PubMed] [Google Scholar]
- Bower C., Miller M., Payne J., Serna P. Promotion of folate for the prevention of neural tube defects: who benefits? Paediatr. Perinat. Epidemiol. 2005;19(6):435–444. doi: 10.1111/j.1365-3016.2005.00675.x. [DOI] [PubMed] [Google Scholar]
- Callaway L.K., Prins J.B., Chang A.M., McIntyre H.D. The prevalence and impact of overweight and obesity in an Australian obstetric population. Med. J. Aust. 2006;184(2):56–59. doi: 10.5694/j.1326-5377.2006.tb00115.x. [DOI] [PubMed] [Google Scholar]
- Catalano P.M., Shankar K. Obesity and pregnancy: mechanisms of short term and long term adverse consequences for mother and child. BMJ. 2017;356:j1. doi: 10.1136/bmj.j1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Cheng T.S., Loy S.L., Cheung T.B., Godfrey K.M., Gluckman P.D., Kwek K., Saw S.M., Chong Y.S., Lee Y.S., Yap F., Yen Chan J.K., Lek N. Demographic characteristics, health behaviors before and during pregnancy, and pregnancy and birth outcomes in mothers with different pregnancy planning status. Prev. Sci. 2016;17(8):960–969. doi: 10.1007/s11121-016-0694-8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Cohen J. A coefficient of agreement for nominal scales. Educ. Psychol. Meas. 1960;20(1):37–46. [Google Scholar]
- Delissaint D., McKyer E.L. A systematic review of factors utilized in preconception health behavior research. Health Educ. Behav. 2011;38(6):603–616. doi: 10.1177/1090198110389709. [DOI] [PubMed] [Google Scholar]
- DeLuca R.S., Lobel M. Conception, commitment, and health behavior practices in medically high-risk pregnant women. Womens Health. 1995;1(3):257–271. [PubMed] [Google Scholar]
- Dibaba Y., Fantahun M., Hindin M.J. The effects of pregnancy intention on the use of antenatal care services: systematic review and meta-analysis. Reprod. Health. 2013;10(50) doi: 10.1186/1742-4755-10-50. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Drevin J., Kristiansson P., Stern J., Rosenblad A. Measuring pregnancy planning: a psychometric evaluation and comparison of two scales. J. Adv. Nurs. 2017;73(11):2765–2775. doi: 10.1111/jan.13364. [DOI] [PubMed] [Google Scholar]
- Edelman N.L., de Visser R.O., Mercer C.H., McCabe L., Cassell J.A. Targeting sexual health services in primary care: a systematic review of the psychosocial correlates of adverse sexual health outcomes reported in probability surveys of women of reproductive age. Prev. Med. 2015;81(345–56) doi: 10.1016/j.ypmed.2015.09.019. [DOI] [PubMed] [Google Scholar]
- Finer L.B., Zolna M.R. Declines in unintended pregnancy in the United States, 2008–2011. New Engl. J. Med. 2016;374(9):843–852. doi: 10.1056/NEJMsa1506575. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Fisher J., Cabral de Mello M., Patel V., Rahman A., Tran T., Holton S., Holmes W. Prevalence and determinants of common perinatal mental disorders in women in low- and lower-middle-income countries: a systematic review. Bull. World Health Organ. 2012;90(2):139G–149G. doi: 10.2471/BLT.11.091850. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Flak A.L., Su S., Bertrand J., Denny C.H., Kesmodel U.S., Cogswell M.E. The association of mild, moderate, and binge prenatal alcohol exposure and child neuropsychological outcomes: a meta-analysis. Alcohol. Clin. Exp. Res. 2014;38(1):214–226. doi: 10.1111/acer.12214. [DOI] [PubMed] [Google Scholar]
- Fleiss J.L. Measuring nominal scale agreement among many raters. Psychol. Bull. 1971;76(5):378–382. [Google Scholar]
- Fleming T.P., Watkins A.J., Velazquez M.A., Mathers J.C., Prentice A.M., Stephenson J., Barker M., Saffery R., Yajnik C.S., Eckert J.J., Hanson M.A., Forrester T., Gluckman P.D., Godfrey K.M. Origins of lifetime health around the time of conception: causes and consequences. Lancet. 2018;391(10132):1842–1852. doi: 10.1016/S0140-6736(18)30312-X. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Gardner B., Wardle J., Poston L., Croker H. Changing diet and physical activity to reduce gestational weight gain: a meta-analysis. Obes. Rev. 2011;12(7):e602–e620. doi: 10.1111/j.1467-789X.2011.00884.x. [DOI] [PubMed] [Google Scholar]
- Gariepy A., Lundsberg L.S., Vilardo N., Stanwood N., Yonkers K., Schwarz E.B. Pregnancy context and women's health-related quality of life. Contraception. 2017;95(5):491–499. doi: 10.1016/j.contraception.2017.02.001. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Gipson J.D., Koenig M.A., Hindin M.J. The effects of unintended pregnancy on infant, child, and parental health: a review of the literature. Stud. Fam. Plan. 2008;39(1):18–38. doi: 10.1111/j.1728-4465.2008.00148.x. [DOI] [PubMed] [Google Scholar]
- Goossens J., Van Den Branden Y., Van der Sluys L., Delbaere I., Van Hecke A., Verhaeghe S., Beeckman D. The prevalence of unplanned pregnancy ending in birth, associated factors, and health outcomes. Hum. Reprod. 2016;31(12):2821–2833. doi: 10.1093/humrep/dew266. [DOI] [PubMed] [Google Scholar]
- Grant M.J., Booth A. A typology of reviews: an analysis of 14 review types and associated methodologies. Health Inf. Libr. J. 2009;26(2):91–108. doi: 10.1111/j.1471-1842.2009.00848.x. [DOI] [PubMed] [Google Scholar]
- Guliani H., Sepehri A., Serieux J. Determinants of prenatal care use: evidence from 32 low-income countries across Asia, sub-Saharan Africa and Latin America. Health Policy Plan. 2014;29(5):589–602. doi: 10.1093/heapol/czt045. [DOI] [PubMed] [Google Scholar]
- Hall J.A., Benton L., Copas A., Stephenson J. Pregnancy intention and pregnancy outcome: systematic review and meta-analysis. Matern. Child Health J. 2017;21(3):670–704. doi: 10.1007/s10995-016-2237-0. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Hill B., Skouteris H., Fuller-Tyszkiewicz M. Interventions designed to limit gestational weight gain: a systematic review of theory and meta-analysis of intervention components. Obes. Rev. 2013;14(6):435–450. doi: 10.1111/obr.12022. [DOI] [PubMed] [Google Scholar]
- Hill B., McPhie S., Fuller-Tyszkiewicz M., Gillman M.W., Skouteris H. Psychological health and lifestyle management preconception and in pregnancy. Semin. Reprod. Med. 2016;34(2):121–128. doi: 10.1055/s-0036-1571352. [DOI] [PubMed] [Google Scholar]
- Humbert L., Saywell R.M., Jr., Zollinger T.W., Priest C.F., Reger M.K., Kochhar K. The effect of pregnancy intention on important maternal behaviors and satisfaction with care in a socially and economically at-risk population. Matern. Child Health J. 2011;15(7):1055–1066. doi: 10.1007/s10995-010-0646-z. [DOI] [PubMed] [Google Scholar]
- IOM (Institite of Medicine), NRC (National Research Council) The National Acadamies Press; Washington, DC: 2009. Weight Gain during Pregnancy: Reexamining the Guidelines. [PubMed] [Google Scholar]
- Koenig M.A., Acharya R., Singh S., Roy T.K. Do current measurement approaches underestimate levels of unwanted childbearing? Evidence from rural India. Popul. Stud. (Camb.) 2006;60(3):243–256. doi: 10.1080/00324720600895819. [DOI] [PubMed] [Google Scholar]
- Lachance-Grzela M., Bouchard G. The well-being of cohabiting and married couples during pregnancy: does pregnancy planning matter? J. Soc. Pers. Relat. 2009;26:141–159. [Google Scholar]
- Lan L., Harrison C.L., Misso M., Hill B., Teede H.J., Mol B.W., Moran L.J. Systematic review and meta-analysis of the impact of preconception lifestyle interventions on fertility, obstetric, fetal, anthropometric and metabolic outcomes in men and women. Hum. Reprod. 2017;32(9):1925–1940. doi: 10.1093/humrep/dex241. [DOI] [PubMed] [Google Scholar]
- Lancaster C.A., Gold K.J., Flynn H.A., Yoo H., Marcus S.M., Davis M.M. Risk factors for depressive symptoms during pregnancy: a systematic review. Am. J. Obstet. Gynecol. 2010;202(1):5–14. doi: 10.1016/j.ajog.2009.09.007. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Lane M., Robker R.L., Robertson S.A. Parenting from before conception. Science. 2014;345(6198):756–760. doi: 10.1126/science.1254400. [DOI] [PubMed] [Google Scholar]
- Leeper J.D., Nagy C., Hullett-Robertson S. Prenatal diet adequacy among rural Alabama blacks. J. Rural. Health. 1992;8(2):134–138. [Google Scholar]
- Lewis M.A., Mitchell E.W., Levis D.M., Isenberg K., Kish-Doto J. Couples' notions about preconception health: implications for framing social marketing plans. Am. J. Health Promot. 2013;27(3 Suppl):S20–S27. doi: 10.4278/ajhp.120127-QUAL-65. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Lindberg L.D., Kost K. Exploring U.S. men's birth intentions. Matern. Child Health J. 2014;18(3):625–633. doi: 10.1007/s10995-013-1286-x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Littleton H. Sexual victimization and somatic complaints in pregnancy: examination of depression as a mediator. Womens Health Issues. 2015;25(6):696–702. doi: 10.1016/j.whi.2015.06.013. [DOI] [PubMed] [Google Scholar]
- Mallard S.R., Houghton L.A. Public health policy to redress iodine insufficiency in pregnant women may widen sociodemographic disparities. Public Health Nutr. 2014;17(6):1421–1429. doi: 10.1017/S1368980013001626. [DOI] [PMC free article] [PubMed] [Google Scholar]
- McDonnell R., Johnson Z., Doyle A., Sayers G. Determinants of folic acid knowledge and use among antenatal women. J. Public Health Med. 1999;21(2):145–149. doi: 10.1093/pubmed/21.2.145. [DOI] [PubMed] [Google Scholar]
- Mikhail B. Prenatal care utilization among low-income African American women. J. Community Health Nurs. 2000;17(4):235–246. doi: 10.1207/S15327655JCHN1704_5. [DOI] [PubMed] [Google Scholar]
- Moher D., Liberati A., Tetzlaff J., Altman G.D. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. Ann. Intern. Med. 2009;151(4):264–269. doi: 10.7326/0003-4819-151-4-20090810-00135. w64. [DOI] [PubMed] [Google Scholar]
- Naimi T.S., Lipscomb L.E., Brewer R.D., Gilbert B.C. Binge drinking in the preconception period and the risk of unintended pregnancy: implications for women and their children. Pediatrics. 2003;111(5 Pt 2):1136–1141. [PubMed] [Google Scholar]
- National Institute for Health and Care Excellence . National Institute for Health and Care Excellence. 2010. Weight Management Before, During, and After Pregnancy (PH27) [Google Scholar]
- Okesene-Gafa K., Chelimo C., Chua S., Henning M., McCowan L. Knowledge and beliefs about nutrition and physical activity during pregnancy in women from South Auckland region, New Zealand. Aust. N. Z. J. Obstet. Gynaecol. 2016;56(5):471–483. doi: 10.1111/ajo.12456. [DOI] [PubMed] [Google Scholar]
- Pantasri T., Norman R.J. The effects of being overweight and obese on female reproduction: a review. Gynecol. Endocrinol. 2014;30(2):90–94. doi: 10.3109/09513590.2013.850660. [DOI] [PubMed] [Google Scholar]
- Paterson J.M., Neimanis I.M., Bain E. Stopping smoking during pregnancy: are we on the right track? Can. J. Public Health. 2003;94(4):297–299. doi: 10.1007/BF03403609. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Patra J., Bakker R., Irving H., Jaddoe V.W., Malini S., Rehm J. Dose-response relationship between alcohol consumption before and during pregnancy and the risks of low birthweight, preterm birth and small for gestational age (SGA) - a systematic review and meta-analyses. BJOG. 2011;118(12):1411–1421. doi: 10.1111/j.1471-0528.2011.03050.x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Pearce E.E., Evenson K.R., Downs D.S., Steckler A. Strategies to promote physical activity during pregnancy: a systematic review of intervention evidence. Am. J. Lifestyle Med. 2013;7(1) doi: 10.1177/1559827612446416. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Pineles B.L., Park E., Samet J.M. Systematic review and meta-analysis of miscarriage and maternal exposure to tobacco smoke during pregnancy. Am. J. Epidemiol. 2014;179(7):807–823. doi: 10.1093/aje/kwt334. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Rassi A., Wattimena J., Black K. Pregnancy intention in an urban Australian antenatal population. Aust. NZ J. Public Health. 2013;37(6):568–573. doi: 10.1111/1753-6405.12098. [DOI] [PubMed] [Google Scholar]
- Rodriguez A., Bohlin G., Lindmark G. Psychosocial predictors of smoking and exercise during pregnancy. J. Reprod. Infant Psychol. 2000;18(3):203–223. [Google Scholar]
- Rubin R.R., Wadden T.A., Bahnson J.L., Blackburn G.L., Brancati F.L., Bray G.A., Coday M., Crow S.J., Curtis J.M., Dutton G., Egan C., Evans M., Ewing L., Faulconbridge L., Foreyt J., Gaussoin S.A., Gregg E.W., Hazuda H.P., Hill J.O., Horton E.S., Hubbard V.S., Jakicic J.M., Jeffery R.W., Johnson K.C., Kahn S.E., Knowler W.C., Lang W., Lewis C.E., Montez M.G., Murillo A., Nathan D.M., Patricio J., Peters A., Pi-Sunyer X., Pownall H., Rejeski W.J., Rosenthal R.H., Ruelas V., Toledo K., Van Dorsten B., Vitolins M., Williamson D., Wing R.R., Yanovski S.Z., Zhang P. Impact of intensive lifestyle intervention on depression and health-related quality of life in type 2 diabetes: the Look AHEAD Trial. Diabetes Care. 2014;37(6):1544–1553. doi: 10.2337/dc13-1928. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Shah P.S., Balkhair T., Ohlsson A., Beyene J., Scott F., Frick C. Intention to become pregnant and low birth weight and preterm birth: a systematic review. Matern. Child Health J. 2011;15(2):205–216. doi: 10.1007/s10995-009-0546-2. [DOI] [PubMed] [Google Scholar]
- Silverman M.E., Reichenberg A., Savitz D.A., Cnattingius S., Lichtenstein P., Hultman C.M., Larsson H., Sandin S. The risk factors for postpartum depression: a population-based study. Depress. Anxiety. 2017;34(2):178–187. doi: 10.1002/da.22597. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Stephenson J., Patel D., Barrett G., Howden B., Copas A., Ojukwu O., Pandya P., Shawe J. How do women prepare for pregnancy? Preconception experiences of women attending antenatal services and views of health professionals. PLoS One. 2014;9(7) doi: 10.1371/journal.pone.0103085. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Stephenson J., Heslehurst N., Hall J., Schoenaker D., Hutchinson J., Cade J.E., Poston L., Barrett G., Crozier S.R., Barker M., Kumaran K., Yajnik C.S., Baird J., Mishra G.D. Before the beginning: nutrition and lifestyle in the preconception period and its importance for future health. Lancet. 2018;391(10132):1830–1841. doi: 10.1016/S0140-6736(18)30311-8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Taylor G., McNeill A., Girling A., Farley A., Lindson-Hawley N., Aveyard P. Change in mental health after smoking cessation: systematic review and meta-analysis. BMJ. 2014;348:g1151. doi: 10.1136/bmj.g1151. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Teychenne M., York R. Physical activity, sedentary behavior, and postnatal depressive symptoms: a review. Am. J. Prev. Med. 2013;45(2):217–227. doi: 10.1016/j.amepre.2013.04.004. [DOI] [PubMed] [Google Scholar]
- The International Weight Management in Pregnancy (i-WIP) Collaborative Group Effect of diet and physical activity based interventions in pregnancy on gestational weight gain and pregnancy outcomes: meta-analysis of individual participant data from randomised trials. BMJ. 2017;358 doi: 10.1136/bmj.j3119. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Toivonen K.I., Oinonen K.A., Duchene K.M. Preconception health behaviours: a scoping review. Prev. Med. 2017;96:1–15. doi: 10.1016/j.ypmed.2016.11.022. [DOI] [PubMed] [Google Scholar]
- Tsui A.O., McDonald-Mosley R., Burke A.E. Family planning and the burden of unintended pregnancies. Epidemiol. Rev. 2010;32(152–74) doi: 10.1093/epirev/mxq012. [DOI] [PMC free article] [PubMed] [Google Scholar]
- U.S. Department of Health and Human Services . 2014. The Health Consequences of Smoking: 50 Years of Progress. A Report of the Surgeon General. [Google Scholar]
- United Nations Department of Economic and Social Affairs . 2014. World Economic Situation and Prospects. [Google Scholar]
- Wills C.J., Page S.R. Peri-conceptual folic acid supplementation in type 1 diabetes. Practical Diabetes. 2001;vol. 18:123–125. [Google Scholar]
- Wolff T., Witkop C.T., Miller T., Syed S.B. Folic acid supplementation for the prevention of neural tube defects: an update of the evidence for the U.S. Preventive Services Task Force. Ann. Intern. Med. 2009;150(9):632–639. doi: 10.7326/0003-4819-150-9-200905050-00010. [DOI] [PubMed] [Google Scholar]
- World Health Organization . 2013. Meeting to Develop a Global Consensus on Preconception Care to Reduce Maternal and Childhood Mortality and Morbidity. [Google Scholar]
- World Health Organization . 2016. WHO Recommendations on Antenatal Care for a Positive Pregnancy Experience. [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Supplementary Materials
Supplementary tables