Abstract
Background
Acute coronary syndrome (ACS) is associated with emergency hospitalizations, and there are limited real-world data on clinical outcomes in post-ACS Asian patients. This article presents data on the Indian subgroup from the Long-term Follow-up of Antithrombotic Management Patterns in Acute Coronary Syndrome Patients in Asia (EPICOR-Asia) study.
Methods
EPICOR included patients with ACS [ST-segment elevation myocardial infarction (STEMI), non–ST-segment elevation myocardial infarction (NSTEMI), or unstable angina (UA)]. The study had two phases: acute phase and follow-up phase. The primary objective was to describe short- and long-term antithrombotic management patterns.
Results
EPICOR-India enrolled 2468 patients (STEMI-1482; NSTEMI-562; and UA-424). Cardiovascular risk factors were present in 1362 (55.2%) patients. Prehospital care was received by 879 (35.6%) patients, and the median time from the symptom onset to the first medical attention was 3 h (0.08, 100.33). The most common drug regimen prescribed during the acute phase was ≥2 antiplatelet agents + anticoagulants with no glycoprotein IIb/IIIa inhibitors and at discharge were aspirin + clopidogrel. About 78.8% of patients were discharged on dual antiplatelet therapy (DAPT) and 16%, on single antiplatelet therapy (SAPT). At 23 months after discharge, 55.6% were on DAPT, while 16.4% were on SAPT. Postdischarge outcomes at 2 years included death in 165 (6.7%) patients, composite events of death, myocardial infarction (MI), or ischemic stroke in 182 (7.4%) patients, and bleeding events in seven (0.3%) patients.
Conclusion
This study showed a gap between international recommendations and implementation for managing ACS in Indian patients. Most of the patients prefer to undergo invasive management instead of non-invasive therapy. At the end of the 2-year follow-up, more than half of the population was receiving DAPT, with most patients on receiving a combination of aspirin and clopidogrel. The mortality along with composite events of death, MI, or ischemic stroke was highest for patients with NSTEMI.
Keywords: EPICOR- India, ACS, Antithrombotic, DAPT, Myocardial infarction, STEMI, NSTEMI
1. Introduction
Cardiovascular diseases (CVDs) are rising in prevalence and are becoming responsible for increased mortality and morbidity. They are anticipated to become the leading cause of death around the world by 2020 and lead to more than 24 million fatalities by the year 2030.1 CVDs contribute to a total of 26% deaths in India, and the common risk factors contributing to CVDs are hypertension, diabetes, tobacco smoking, high cholesterol, dietary factors, obesity, and physical inactivity.2
Acute coronary syndrome (ACS) is characterized by acute myocardial ischemia events such as unstable angina (UA), non–ST-segment elevation myocardial infarction (NSTEMI), and STEMI. ACS treatments aim to reduce myocardial necrosis; prevent further major adverse cardiac events; and reduce the risk of complications viz. ventricular fibrillation, unstable tachycardia, and symptomatic bradycardias.3 The treatment protocol includes the use of oxygen therapy; antiplatelet therapy; anticoagulant therapy; and beta-blockers.4
Early initiation of treatment is highly recommended for patients with confirmed ACS.5 Most patients with ACS are recommended to continue their dual antiplatelet therapy (DAPT) for 12 months unless contraindicated. Use of DAPT beyond 12 months depends on the balance between ischemic and bleeding risk.6 The Clopidogrel for the Reduction of Events During Observation trial showed 27% risk reduction of death, stroke, and myocardial infarction (MI) in patients who had received DAPT for 1 year.7
The present study was a subgroup analysis of the EPICOR-Asia study which described the use of antithrombotic management patterns (AMPs) in a real-life setting and their relationship with the different invasive strategies. The aim of this study was to describe the short- and long-term AMPs in Indian patients hospitalized for an ACS who survived to discharge. The study evaluated the clinical outcomes, economic aspects, and association with quality of life (QoL) of these AMPs in a ‘real-life’ setting.
2. Materials and methods
The present study is a subgroup analysis of the EPICOR-Asia multinational, multicenter, observational, prospective, longitudinal, cohort study.8 This subgroup analysis was conducted in Indian patients in a real-life setting. The clinical trial registration number is NCT01361386.
A written informed consent was obtained from patients at the time of discharge from the hospital. The final protocol and patient informed consent form were reviewed and approved by the corresponding health authorities and ethics boards/institutional review board (IRB) for all the participating study sites.
2.1. Inclusion and exclusion criteria
Patients who were aged 18 years and older and diagnosed with STEMI, NSTEMI, or UA as per the prespecified criteria described elsewhere8 and hospitalized within 48 h of the symptom onset were included in the study.
Patients were excluded from the study if they had STEMI, NSTEMI, and UA, which was precipitated by or was a complication of surgery, trauma, or gastrointestinal bleeding or postpercutaneous coronary intervention (PCI) and had STEMI, NSTEMI, and UA during hospitalization for any other reason.
2.2. Study design and variables of analysis
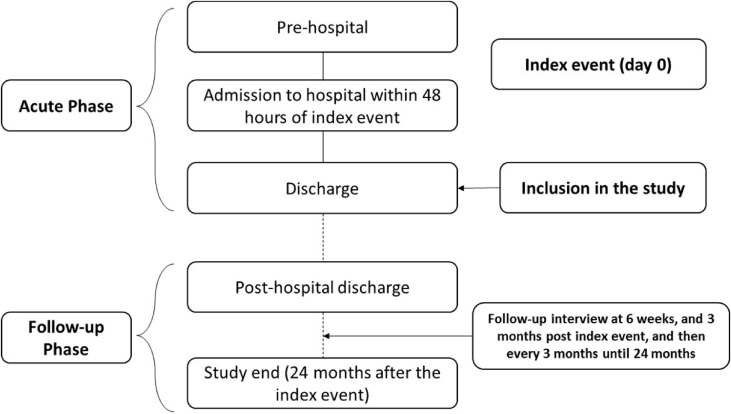
The study was split into two phases: acute phase which included prehospital and inhospital data collection and the follow-up phase which included collection of information for up to 2 years after discharge from the hospital (Fig. 1). All information was collected in an electronic case report form. During the follow-up phase, data collected included the following: occurrence of events (cardiac ischemic complications; recurrent ischemia; other cardiac complications including heart failure, cardiogenic shock, dyspnea, arrhythmias, atrial fibrillation, sustained ventricular tachycardia, high-degree atrioventricular (AV) block, and stroke; and other complications), treatment information (evaluation of AMPs), utilization of health-care resources [prehospital care such as electrocardiogram (ECG) and use of medications and inhospital medical management such as coronary/intensive care units and cath lab facilities], and EQ-5D QoL assessment.
Fig. 1.
Study design.
The primary variables included AMPs (inhospital and posthospital discharge). The secondary variables included identifying clinical outcomes such as death, ischemic events, bleeding events, composite of death, MI, and stroke.
2.3. Statistical analysis
A descriptive analysis approach was used. For continuous parameters, mean, standard deviation (SD), median, minimum, and maximum values were provided. For categorical parameters, the frequency and percentage of patients in each category were provided. Patient demographics, the baseline characteristics, inhospital outcomes, antithrombotic medication and other medication/therapies, EQ-5D, economic outcomes, and clinical outcomes were assessed in a descriptive manner. All calculations and summaries were produced using SAS®, version 8.2 or later (SAS 2009).
3. Results
3.1. Patient characteristics
A total of 2468 patients were included in the study, of which 1482 patients (60%) had STEMI; 562 patients (22.7%) had NSTEMI; and 424 patients (17.2%) had UA. The mean age of the patients was 57 years, and most of them were men (n = 2039; 82.6%). More than half of the patients had a previous history of CV risk factors (n = 1362, 55.2%). Previous CVD was observed in 14.3%. Overall, 215 patients (8.7%) were previously taking antiplatelet agents including aspirin (n = 186, 7.5%) and clopidogrel (n = 163, 6.6%). Only 11 patients (0.4%) were previously taking anticoagulants. Previous CV medications were taken by 434 (17.6%) patients. Detailed patient demographics and the baseline characteristics are presented in Table 1.
Table 1.
Patient demographics and characteristics.
| Demographics | STEMI (n = 1482) | NSTEMI (n = 562) | UA (n = 424) | Total (N = 2468) |
|---|---|---|---|---|
| Gender | ||||
| Male | 1259 (85.0%) | 450 (80.1%) | 330 (77.8%) | 2039 (82.6%) |
| Age in years; mean (SD) | 55.7 (11.20) | 59.0 (12.06) | 59.2 (10.48) | 57.0 (11.40) |
| Age group | ||||
| ≤55 yr | 751 (50.7%) | 229 (40.7%) | 154 (36.3%) | 1134 (45.9%) |
| ≥75 yr | 74 (5.0%) | 64 (11.4%) | 25 (5.9%) | 163 (6.6%) |
| BMI(Kg/m2); mean (SD) | 24.8 (3.42) | 25.0 (4.11) | 25.6 (4.36) | 25.0 (3.77) |
| Place of residence | ||||
| Rural | 810 (54.7%) | 244 (43.4%) | 193 (45.5%) | 1247 (50.5%) |
| Metropolitan | 672 (45.3%) | 318 (56.6%) | 231 (54.5%) | 1221 (49.5%) |
| Education level | ||||
| No formal education | 120 (8.1%) | 32 (5.7%) | 34 (8%) | 186 (7.5%) |
| Primary | 287 (19.4%) | 139 (24.7%) | 72 (17%) | 498 (20.2%) |
| Secondary | 368 (24.8%) | 108 (19.2%) | 109 (25.7%) | 585 (23.7%) |
| University | 394 (26.6%) | 205 (36.5%) | 120 (28.3%) | 719 (29.1%) |
| Previous CV risk factors | 759 (51.2%) | 352 (62.6%) | 251 (59.2%) | 1362 (55.2%) |
| Family history of CAD | 66 (4.5%) | 42 (7.5%) | 24 (5.7%) | 132 (5.3%) |
| Previous CVD | 161 (10.9%) | 90 (16%) | 102 (24.1%) | 353 (14.3%) |
| Hypertension | 564 (38.1%) | 284 (50.5%) | 201 (47.4%) | 1049 (42.5%) |
| Hypercholesterolemia | 84 (5.7%) | 31 (5.5%) | 21 (5%) | 136 (5.5%) |
| Type II diabetes mellitus | 383 (25.8%) | 202 (35.9%) | 125 (29.5%) | 710 (5.3%) |
| Current smoker | 333 (22.5%) | 142 (25.3%) | 45 (10.6%) | 520 (21.1%) |
STEMI, ST-segment elevation myocardial infarction; NSTEMI, non–ST-segment elevation myocardial infarction; UA, unstable angina; SD, standard deviation; BMI, body mass index; CVD, cardiovascular disease; CAD, coronary artery disease.
3.2. Prehospital care
Prehospital care (defined as ECG and/or medications) was received by 879 patients (35.6%). Of the patients who had received prehospital care (879, 35.6%), a total of 97 (11%) patients contributed to the calculation of the median time from the symptom onset to the first medical attention for the event. The other patients who received prehospital care and did not report the exact time of the symptom onset were excluded from the calculation of median time from the symptom onset to the first medical attention for the event. The median time from the symptom onset to receiving the first medical attention for the event was 3 h (0.08, 100.33) [STEMI: 3.625 h (0.08, 100.33); UA: 1.750 h (0.08, 35.0); and NSTEMI: 1.625 h (0.08, 23.50)]. The data for the proportion of patients receiving their first medical attention at different facilities were available for 200 (22.7%) patients. Of these, majority of the patients received first medical attention for the event at physician's office (135, 67.5%).
Prehospital medications were received by 4.1% patients. Thrombolytic agents (1.2%); antiplatelet agents (3.6%); and anticoagulants (1%) were the drugs received by the patients. Prehospital ECG was performed in 846 patients (34.3%). The total median length of hospital stay in all patients was 5.0 days (1.0, 97.0).
3.3. Inhospital stage: medical management and inhospital outcomes
Coronary/intensive care units and cath lab facilities were available in all the 47 hospitals. Facility for 24/7 primary PCI was available for 2419 patients (98%). Cardiac surgery on site could be performed in 2431 patients (98.5%). On admission, fewer patients received thrombolysis (19.4%) compared with cardiac catheterization (74%). PCI was received by 49.1% patients. Overall, the management patterns for patients with STEMI revealed that 798 patients (53.8%) received reperfusion. Of which, 431 patients (29.1%) received thrombolysis therapy, and 367 patients (24.8%) underwent primary PCI. The remaining 684 patients (46.2%) did not receive reperfusion. The management patterns for patients with NSTEMI and UA revealed that most of the patients underwent invasive procedures (NSTEMI: 394, 70.1% and UA: 301, 71%) and fewer patients underwent non-invasive procedures (NSTEMI: 160, 28.5% and UA: 61, 14.4%). The median time from the symptom onset to primary PCI was 20.9 h (0.0, 768.0). While patients with NSTEMI underwent PCI at a median time of 38 h (0.0, 208.4), patients with STEMI underwent PCI at a median time of 14.7 h (0.0, 768.0). Patients with UA underwent PCI at a median time of 24 h (0.0, 384.0) after the onset of symptoms.
A total of 366 patients (14.8%) received at least one type of thrombolytic agent for treatment. Of the different thrombolytic agents, 242 patients received streptokinase (9.8%); 12 patients received t-PA and TNK-t-PA each (0.5%); 2 patients received r-PA (0.1%); and 98 received other thrombolytics (4%). In 2445 patients, antiplatelet agents were prescribed majorly (99.1%), which included aspirin (n = 2109, 85.5%), clopidogrel (n = 2012, 81.5%), prasugrel (n = 389, 15.8%), cilostazol (n = 53, 2.1%), and ticlopidine (n = 3, 0.1%). Any glycoprotein (GP) IIb/IIIa inhibitors were received by 11.8% patients and included tirofiban (n = 227, 9.2%), eptifibatide (n = 60, 2.4%), and abciximab (n = 3, 0.1%). Anticoagulant agents were received by 54.5% patients and included low molecular weight (LMW) heparin (n = 848, 34.4%); unfractioned heparin (n = 560, 22.7%); bivalirudin (n = 101, 4.1%); fondaparinux (n = 21, 0.9%); and warfarin/acenocoumarol (n = 9, 0.4%).
Cardiac ischemic complications experienced by the patients included MI in 293 patients (11.9%) and recurrent ischemia in 70 patients (2.8%). Other cardiac complications experienced by the patients included heart failure in 38 patients (1.5%), cardiogenic shock in 24 patients (1%), dyspnea in 80 patients (3.2%), cardiac arrest in eight patients (0.3%), atrial fibrillation in seven patients (0.3%), sustained ventricular tachycardia in 10 patients (0.4%), high-degree AV block in 18 patients (0.7%), stroke in two patients (0.1%), and other complications (n = 55, 2.2%) were majorly observed among patients. Hemorrhagic complications were observed in 18 (0.7%) patients during hospital stay. Of the 18 hemorrhagic complications, seven (38.9%) were related to the medical procedure and 13 (72.2%) were of minimal clinical significance, while 12 (66.6%) showed minimal hemodynamic compromise. The most common sites of hemorrhagic complications were gastrointestinal (5, 27.8%); vascular access (3, 16.7%); genitourinary (2, 11.1%); and other sites (6, 33.3%).
3.4. At discharge: AMPs
At the time of discharge, most patients were prescribed DAPT (1960, 79.4%) or were taking one antiplatelet agent (395, 16%). The antiplatelet agents at the time of discharge included aspirin only (138, 5.6%); clopidogrel only (240, 9.7%); and combination of aspirin and clopidogrel (1578, 63.9%). Discharge AMPs included two antiplatelet agents and no anticoagulants (78.8%) or one antiplatelet agent and no anticoagulant (14.5%). Warfarin was the most prescribed anticoagulant agent to patients (53, 2.1%) at the time of discharge. Three antiplatelet agents were received by only 2.4% of subjects. The detailed discharge AMPs are presented in Table 2.
Table 2.
Antithrombotic management patterns in patients during the prehospital, inhospital, and at discharge stages.
| Description | STEMI (N = 1482) | NSTEMI (N = 562) | UA (N = 424) | Total (N = 2468) |
|---|---|---|---|---|
| Prehospital and inhospital AMP | ||||
| ≥2AP+heparin/AC, no GPI | 505 (34.1%) | 215 (38.3%) | 121 (28.5%) | 841 (34.1%) |
| ≥2AP+GPI+heparin/AC | 178 (12.0%) | 22 (3.9%) | 70 (16.5%) | 270 (10.9%) |
| ≥2AP only | 370 (25.0%) | 164 (29.2%) | 115 (27.1%) | 649 (26.3%) |
| Underuse of antithrombotic therapy | 416 (28.1%) | 159 (28.3%) | 113 (26.7%) | 688 (27.9%) |
| 2AP+GPI | 9 (0.6%) | 1 (0.2%) | 5 (1.2%) | 15 (0.6%) |
| Unassigned | 4 (0.3%) | 1 (0.2%) | 0 | 5 (0.2%) |
| Discharge AMP | ||||
| 0 AP/0 AC | 28 (1.9%) | 12 (2.1%) | 14 (3.3%) | 54 (2.2%) |
| 1 AP/0 AC | 185 (12.5%) | 119 (21.2%) | 55 (13.0%) | 359 (14.5%) |
| 2 AP/0 AC | 1177 (79.4%) | 418 (74.4%) | 349 (82.3%) | 1944 (78.8%) |
| 3 AP/0 AC | 49 (3.3%) | 6 (1.1%) | 3 (0.7%) | 58 (2.4%) |
| Any AC | 43 (2.9%) | 7 (1.2%) | 3 (0.7%) | 53 (2.1%) |
| Discharge any anticoagulant | ||||
| 0 AP/any AC | 0 | 0 | 0 | 0 |
| 1 AP/any AC | 31 (2.1%) | 3 (0.5%) | 2 (0.5%) | 36 (1.5%) |
| 2 AP/any AC | 11 (0.7%) | 4 (0.7%) | 1 (0.2%) | 16 (0.6%) |
| Other | 1 (0.1%) | 0 | 0 | 1 (0%) |
AMP, antithrombotic management pattern; AP, antiplatelet; GPI, glycoprotein IIb/IIIa inhibitor; AC, anticoagulant; STEMI, ST-segment elevation myocardial infarction; NSTEMI, non–ST-segment elevation myocardial infarction; UA, unstable angina.
Underuse of antithrombotic therapy: 0–1 AP, No GPI, 0 or 1 of heparin or anticoagulants.
3.5. Postdischarge follow-up
The 2-year follow-up data were available for almost all the patients (2467, 99.9%) after discharge from the hospital. The patients were evaluated for improvement in QoL parameters using the EQ-5D questionnaire at different time points during the follow-up period. At the time of discharge from index hospitalization, 1715 patients (69.9%) reported no problems in mobility, 1721 (70.1%) could take care of themselves, 1610 patients (65.8%) performed their usual activities without hassle, 1711 patients (69.6%) did not have anxiety/depression, and 1453 patients (59.1%) had no pain or discomfort (Table 3). The overall mean EQ-5D index score at discharge was 0.802 ± 0.1789 (mean ± SD). Over the period of 2 years after discharge, 1549 patients (90.0%) still did not experience any problems in walking around, 1645 patients (95.4%) had no problems with self-care, 1591 patients (92.3%) could perform their usual activities without hassle, 1460 patients (84.9%) had no pain/discomfort, and 1544 patients (89.8%) did not have anxiety/depression. The overall EQ-5D index score at 2 years after discharge was 0.917 ± 0.0992, and the change in EQ-5D index score from discharge was 0.102 ± 0.1887.
Table 3.
Quality of life (EQ-5D) at discharge and during follow-up.
| Time period | Study groups | EQ-5D dimensions |
|||||
|---|---|---|---|---|---|---|---|
| Mobility | Self-care | Performing usual activities | Pain/discomfort | Anxiety/depression | EQ-5D index | ||
| At discharge | STEMI (1482) | 1033 (70.0%) | 1043 (70.8%) | 997 (67.9%) | 879 (59.5%) | 1070 (72.4%) | 0.808 (0.1790) |
| NSTEMI (562) | 357 (64.0%) | 385 (68.9%) | 358 (64.4%) | 312 (55.7%) | 360 (64.4%) | 0.786 (0.1878) | |
| UA (424) | 325 (77.0%) | 293 (69.4%) | 255 (60.6%) | 262 (62.2%) | 281 (66.7%) | 0.804 (0.1648) | |
| Total (2468) | 1715 (69.9%) | 1721 (70.1%) | 1610 (65.8%) | 1453 (59.1%) | 1711 (69.6%) | 0.802 (0.1789) | |
| 6 months after discharge | STEMI (1482) | 1148 (91.3%) | 1167 (92.9%) | 1114 (88.7%) | 996 (79.2%) | 1047 (83.3%) | 0.902 (0.1024) |
| NSTEMI (562) | 429 (90.9%) | 424 (89.8%) | 406 (86.2%) | 362 (76.7%) | 389 (82.6%) | 0.893 (0.1177) | |
| UA (424) | 298 (90.0%) | 303 (91.5%) | 291 (87.9%) | 265 (80.1%) | 279 (84.3%) | 0.900 (0.0987) | |
| Total (2468) | 1875 (91.0%) | 1894 (92.0%) | 1811 (88.0%) | 1623 (78.8%) | 1715 (83.3%) | 0.900 (0.1055) | |
| 1 year after discharge | STEMI (1482) | 995 (90.6%) | 1027 (93.6%) | 986 (89.6%) | 878 (80.0%) | 911 (83.0%) | 0.904 (0.0983) |
| NSTEMI (562) | 374 (89.0%) | 387 (92.1%) | 370 (88.3%) | 336 (80.2%) | 355 (84.7%) | 0.902 (0.1106) | |
| UA (424) | 256 (89.8%) | 260 (91.2%) | 244 (85.6%) | 213 (74.7%) | 234 (82.4%) | 0.891 (0.1199) | |
| Total (2468) | 1625 (90.1%) | 1674 (92.9%) | 1600 (88.7%) | 1427 (79.2%) | 1500 (83.3%) | 0.901 (0.1050) | |
| 2 years after discharge | STEMI (1482) | 941 (88.7%) | 1017 (95.8%) | 993 (93.5%) | 896 (84.5%) | 957 (90.3%) | 0.917 (0.0940) |
| NSTEMI (562) | 336 (90.8%) | 350 (94.6%) | 338 (91.4%) | 323 (87.3%) | 325 (88.3%) | 0.916 (0.1077)) | |
| UA (424) | 272 (93.5%) | 278 (95.2%) | 260 (89.0%) | 241 (83.1%) | 262 (89.7%) | 0.915 (0.1066) | |
| Total (2468) | 1549 (90.0%) | 1645 (95.4%) | 1591 (92.3%) | 1460 (84.9%) | 1544 (89.8%) | 0.917 (0.0992) | |
STEMI, ST-segment elevation myocardial infarction; NSTEMI, non–ST-segment elevation myocardial infarction; UA, unstable angina.
3.5.1. Events and deaths at 2-year follow-up
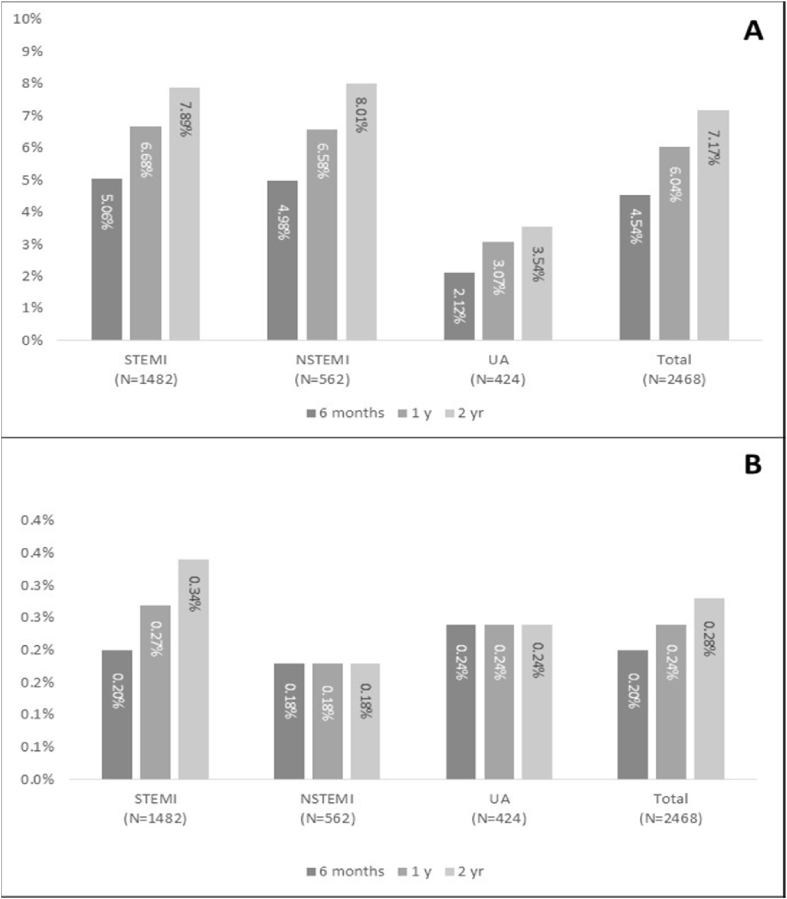
The incidence of composite events of death, MI, or ischemic stroke was observed in 182 patients (7.4%). Overall, 165 deaths (6.7%) were reported during the 2-year follow-up period (Fig. 2). At the end of the 2-year follow-up, MI was reported in 17 (0.7%) patients and ischemic stroke, in seven (0.3%) patients. Bleeding events were observed in only seven (0.3%) patients, of which none were fatal bleeding events. It is important to mention that the EPICOR-Asia study reported 675 (5.2%) deaths, composite events of death, nonfatal MI, or nonfatal ischemic stroke in 1088 (8.4%), and bleeding events in 744 (5.8%) patients (data not published).
Fig. 2.
Incidence of cardiovascular events (A) and bleeding events (B) in patients with STEMI, NSTEMI, and UA over the 2-year follow-up period. STEMI, ST-segment elevation myocardial infarction; NSTEMI, non–ST-segment elevation myocardial infarction; UA, unstable angina.
3.5.2. Change in postdischarge AMPs
At 23-month follow-up period, more than half of the patients (1342, 55.6%) were on either DAPT. Of the different DAPTs, aspirin and clopidogrel were being taken by the highest proportion patients (n = 1336, 55.3%). The single antiplatelet therapy (SAPT) was being taken by 395 patients (16.4%) at the 2-year follow-up period. Among the different SAPTs, clopidogrel was the taken among highest proportion of patients (NSTEMI: 53, 9.6%; STEMI: 121, 8.3%; and UA: 21, 5.1%; total: 195, 8.1%) followed by aspirin, which was taken by 194 (8.0%) patients (NSTEMI: 36, 6.5%; STEMI: 98, 6.7%; and UA: 60, 14.6%, Table 4).
Table 4.
Antithrombotic medications at 23 months after discharge in patients discharged on drug by STEMI/NSTEMI/UA.
| Patient status | STEMI (N = 1454) | NSTEMI (N = 550) | UA (N = 410) | Total (N = 2414) |
|---|---|---|---|---|
| On DAPT | 796 (54.7%) | 319 (58.0%) | 227 (55.4%) | 1342 (55.6%) |
| On ASA + clopidogrel | 790 (54.3%) | 319 (58.0%) | 227 (55.4%) | 1336 (55.3%) |
| On ASA + prasugrel | 33 (2.3%) | 3 (0.5%) | 0 (0.0%) | 36 (1.5%) |
| On ASA + cilostazol | 0 (0.0%) | 0 (0.0%) | 0 (0.0%) | 0 (0.0%) |
| On SAPT | 225 (15.5%) | 89 (16.2%) | 81 (19.8%) | 395 (16.4%) |
| On ASA only | 98 (6.7%) | 36 (6.5%) | 60 (14.6%) | 194 (8.0%) |
| On clopidogrel only | 121 (8.3%) | 53 (9.6%) | 21 (5.1%) | 195 (8.1%) |
| On prasugrel only | 6 (0.4%) | 0 (0.0%) | 0 (0.0%) | 6 (0.2%) |
| On cilostazol only | 0 (0.0%) | 0 (0.0%) | 0 (0.0%) | 0 (0.0%) |
STEMI, ST-segment elevation myocardial infarction; NSTEMI, non–ST-segment elevation myocardial infarction; UA, unstable angina; DAPT, dual antiplatelet therapy; SAPT, single antiplatelet therapy; ASP, Aspirin.
4. Discussion
Receiving medical attention after symptom onset is a critical step which may contribute to the outcomes of the patients at high risk of ACS. Although all the hospitals which enrolled patients in the present study had adequate facilities for appropriate management, only 97 (11%) patients contributed to the evaluation of the median time between the symptom onset and the first medical attention. Several reasons may contribute to delayed medical attention, including the lack of ambulatory services or inadequate medical facilities.
Previous CVD is one of the most prevailing risk factors, which results in ACS. The results of the present study showed that most of the patients had CV risk factors, hypertension, hypercholesterolemia, diabetes mellitus (predominately type II), and coronary artery disease. Bacci et al.9 reported that patients with ACS had comorbid conditions such as hypertension, heart failure, and high cholesterol in addition to being diabetic. The study showed that patients with UA (85.2%) were more likely to have hypertension compared with patients with STEMI (72%) and NSTEMI (79.3%).
Evaluation of AMPs at different stages showed a change at every stage. According to a study conducted by Umbrasiene et al, continuing the same treatment for a longer period of time can significantly improve CV mortality rates.10 Although initial therapy stabilizes the patient's condition, relieves ischemic pain, and reduces the risk of myocardial damage to prevent further ischemia,11 studies recommending the use of specific therapeutic agents are scarce. While in hospital, most patients received anti-thrombotic agents (streptokinase, t-PA, r-PA, and TNK-t-PA), antiplatelet agents (aspirin, clopidogrel, prasugrel, cilostazol, and ticlopidine), GP IIb/IIIa inhibitors (tirofiban, eptifibatide, and abciximab), or anticoagulant agents (LMW heparin, unfractionated heparin, bivalirudin, and fondaparinux). Evidence for the use of other therapeutic agents, viz. beta-blockers, angiotensin-converting enzyme inhibitors (ACEi), and statins in patients with NSTEMI during hospitalization, is available.12
The European society of cardiology (ESC) guidelines recommend a specific protocol for the management of patients with ACS. The guidelines recommend initiation of therapy with aspirin along with loading doses of either clopidogrel or ticagrelor. The anticoagulation therapies recommended included fondaparinux, enoxaparin, unfractionated heparin, and bivalirudin (in patients planned to receive invasive therapies). The use of beta-blockers is recommended in patients with tachycardia or hypertension without any signs of heart failure.11 The National Health Service in the UK recommends the use of aspirin, clopidogrel, bisoprolol, fondaparinux, GTN, atorvastatin, or ramipril for the treatment of patients with high risk and intermediate risk of ACS.13
Most of the patients in the study received antiplatelet agents including aspirin, clopidogrel, prasugrel, cilostazol, and ticlopidine through all stages including prehospital, inhospital, and postdischarge stages. However, the pattern of AMPs changed over a period of time. Most of the patients were receiving more than two antiplatelet agents with heparin and GP IIb/IIIa inhibitor (34.1%) in the prehospital stage, and at the time of discharge, majority of the patients were prescribed two antiplatelet agents and no anticoagulant (78.8%). A review conducted by Bhatt et al.14 reported that the use of aspirin and clopidogrel is most abundant compared with other antiplatelet and anticoagulant therapies available. The antiplatelet agents reduce the risk of MI and stroke by blocking the synthesis of TXa2, which is a powerful platelet activator, and also inhibiting P2Y12 receptor.15 GP IIb/IIIa inhibitors such as tirofiban; eptifibatide; and abciximab were received by a considerably smaller proportion of patients. Fewer patients received GP IIb/IIIa inhibitors in the present study compared with other agents. The use of GP IIb/IIIa inhibitors is associated with improved outcomes in patients with ACS. According to the American Heart Association, early initiation of GP IIb/IIIa inhibitors is associated with improved adherence, resulting in improved outcomes.16 A little more than half of the patients received anticoagulant agents, viz. LMW heparin; unfractioned heparin; bivalirudin; fondaparinux; and warfarin/acenocoumarol. Although the use of anticoagulants such as unfractionated heparin is well established in patients with ACS, it may be associated with unpredictable anticoagulant response secondary to its neutralization by protein binding and activating platelets.17
At the time of discharge from the hospital, most patients were taking DAPT (78.8%), with aspirin and clopidogrel being the most common combination. Warfarin was prescribed in 2.1% of patients at discharge. The use of DAPTs is associated with a lower incidence of major CV events and bleeding complications compared with the use of SAPT.18 A review reported that use of DAPT with clopidogrel and aspirin reduced the risk of CV death, MI, or stroke to a significant extent (p = 0.031).19 The study reported that the use of clopidogrel reduced CV mortality to a statistically significant (p = 0.004) extent. The study further added that the use of evidence-based treatment algorithm is effective for the management of CV complications in patients with ACS to a significant extent (p < 0.001).10 Ruff et al further elaborated that the time duration for which anticoagulant therapy is continued is extremely important and must be decided on careful assessment because of increased risk of bleeding events on long-term use.20 In addition, bleeding events observed in the Indian subset of patients were considerably lower compared with the entire population included in the EPICOR-Asia study. These differences in the incidence of bleeding events in Indian and the entire Asian population may be attributed to differences in the availability of ambulatory care in different regions of Asia, heterogeneity in the way NSTE-ACS patients are managed in different regions included in the study, and country-specific reasons including cost of treatment and the distance of the hospital from where the patient is situated.
On evaluating the complications reported by the patients during the inhospital stage and the postdischarge stages, CV complications were the most prevalent inhospital outcomes in the patients included in the study apart from the hemorrhagic complications. The prevention of atherothrombotic incidents following ischemic coronary attack registry reported major cardiac and cerebrovascular events in 6.4% patients and all-cause mortality in 6.3% patients. In addition, most patients underwent successful PCI in the study (93.9%).21 Another study was conducted to identify the clinical complications of ACS reported in hospital outcomes including the left ventricular failure (2.2%); mitral regurgitation (0.7%); and upper gastrointestinal bleeding (0.9%).22
The effect of antithrombotic therapy on the QoL of patients revealed a gradual improvement in all QoL parameters over a period of time after discharge from the hospital. On discharge from the hospital, most patients showed improved QoL with respect to mobility, self-care, performing usual activities, pain/discomfort, and anxiety/depression. A study evaluating the QoL of patients who were initiated on clopidogrel therapy for ACS demonstrated an improvement in QoL parameters with the increase in time into therapy.23 The antiplatelet treatment observational registry (APTOR II) study showed an improvement in QoL in patients treated with clopidogrel. A greater improvement was observed among the patients with STEMI.24 Although these studies demonstrated that the use of clopidogrel improved the QoL, these studies did not evaluate the deterioration in QoL after discharge/withdrawal of therapy.
Inclusion of only those patients who had survived ACS after being discharged from the hospital and exclusion of the patients who did not survive the index hospitalization may be considered as a limitation of the present study. In addition, exclusion of the patients who had been transferred to or discharged from a nonparticipating hospital may be considered as a limitation of the study. Although the type of drug being received by the patients was reported, specific combinations and doses were not evaluated. This resulted in insufficient insights with respect to treatment modalities and costs that were borne by the patients.
5. Conclusion
In conclusion, at the end of the 2-year follow-up period after discharge, the pattern of AMPs changed to a considerable extent. DAPT was prescribed in 78.8% of patients at discharge and 2.4% of patients receiving three antiplatelets; while 55.6% continued to be on DAPT, none of the patients were on triple antiplatelets at 23 months. Aspirin and clopidogrel combination was most commonly prescribed at discharge and at 23-month follow-up. This study has observed a gap between international recommendations and implementation for managing ACS in Indian patients. The mortality along with composite events of death, MI, or ischemic stroke was highest for patients with NSTEMI. The reported CV events were similar in STEMI and NSTEMI groups. Going forward, steps need to be taken to improve identification, diagnosis, and management of patients with ACS to improve patient outcomes.
Conflicts of interest
All authors have none to declare.
Acknowledgments
This study is funded by AstraZeneca Pharma India Ltd. The authors also acknowledge Turacoz Healthcare Solutions, Delhi, for their writing support.
References
- 1.Fuster V. Global burden of cardiovascular disease: time to implement feasible strategies and to monitor results. J Am Coll Cardiol. 2014 Aug 5;64(5):520–522. doi: 10.1016/j.jacc.2014.06.1151. [DOI] [PubMed] [Google Scholar]
- 2.Shokeen D., Aeri B.T. Risk factors associated with the increasing cardiovascular diseases prevalence in India: a review. J Nutr Food Sci. 2015;5:331. [Google Scholar]
- 3.O'Connor R.E., Brady W., Brooks S.C. Part 10: acute coronary syndromes: 2010 American heart association guidelines for cardiopulmonary resuscitation and emergency cardiovascular care. Circulation. 2010;122(suppl 3):S787–S817. doi: 10.1161/CIRCULATIONAHA.110.971028. [DOI] [PubMed] [Google Scholar]
- 4.Scottish Intercollegiate Guidelines Network (SIGN) SIGN; Edinburgh: 2013. Acute Coronary Syndromes.http://www.sign.ac.uk (SIGN publication no. 93). [February 2013]. Available from URL: [Google Scholar]
- 5.Kumar A., Cannon C.P. Acute coronary syndromes: diagnosis and management, Part I. Mayo Clin Proc. 2009;84(10):917–938. doi: 10.4065/84.10.917. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Cohen M., Iyer D. The “dual-pathway” strategy after acute coronary syndrome: rivaroxaban and antiplatelet agents in the ATLAS ACS 2-TIMI 51 trial. Cardiovasc Ther. 2014 Oct;32(5):224–232. doi: 10.1111/1755-5922.12083. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Steinhubl S.R., Berger P.B., Mann J.T., 3rd Early and sustained dual oral antiplatelet therapy following percutaneous coronary intervention: a randomized controlled trial. JAMA. 2002 Nov 20;288(19):2411–2420. doi: 10.1001/jama.288.19.2411. [DOI] [PubMed] [Google Scholar]
- 8.Huo Y., Lee S.W., Sawhney J.P. Rationale, Design, and baseline characteristics of the EPICOR Asia study (Long-tErmfollow-uP of antithrombotic management patterns in acute CORonary syndrome patients in Asia) Clin Cardiol. 2015 Sep;38(9):511–519. doi: 10.1002/clc.22431. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Bacci M.R., Fonseca F.L., Nogueira L.F. Predominance of STEMI and severity of coronary artery disease in a cohort of patients hospitalized with acute coronary syndrome: a report from ABC Medical School. Rev Assoc Med Bras. 2015 May-Jun;61(3):240–243. doi: 10.1590/1806-9282.61.03.24. [DOI] [PubMed] [Google Scholar]
- 10.Umbrasienė J., Vanagas G., Venclovienė J. Does treatment impact health outcomes for patients after acute coronary syndrome? Int J Environ Res Publ Health. 2015;12:6136–6147. doi: 10.3390/ijerph120606136. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Authors/Task Force Members, Roffi M., Patrono C. 2015 ESC guidelines for the management of acute coronary syndromes in patients presenting without persistent ST-segment elevation: task force for the management of acute coronary syndromes in patients presenting without persistent ST-segment elevation of the European Society of cardiology (ESC) Eur Heart J. 2016 Jan 14:267–315. doi: 10.1093/eurheartj/ehv320. [DOI] [PubMed] [Google Scholar]
- 12.Fox K.A.A., Goodman S.G., Anderson F.A. From guidelines to clinical practice: the impact of hospital and geographical characteristics on temporal trends in the management of acute coronary syndromes. The Global Registry of Acute Coronary Events (GRACE) Eur Heart J. 2003;24:1414–1424. doi: 10.1016/s0195-668x(03)00315-4. [DOI] [PubMed] [Google Scholar]
- 13.Trevelyan J. Acute Coronary Syndrome Guideline (Including management of ST elevation and non-ST elevation myocardial infarction). WAHT-CAR-043: Version 4.2; Available from: http://www.treatmentpathways.worcsacute.nhs.uk/EasysiteWeb/getresource.axd?AssetID=156027&servicetype=Attachment. Accessed 3 Feburary 2019.
- 14.Bhatt D.L., Hulot J.S., Moliterno D.J., Harrington R.A. Antiplatelet and anticoagulation therapy for acute coronary syndromes. Circ Res. 2014 Jun 6;114(12):1929–1943. doi: 10.1161/CIRCRESAHA.114.302737. [DOI] [PubMed] [Google Scholar]
- 15.Brizzio ME. Antiplatelet Therapy in Cardiovascular Disease – Past, Present and Future. Available from: http://cdn.intechopen.com/pdfs-wm/29319.pdf. Accessed 6 Feburary 2019.
- 16.Hoekstra J.W., Roe M.T., Peterson E.D. Early glycoprotein IIb/IIIa inhibitor use for non-ST-segment elevation acute coronary syndrome: patient selection and associated treatment patterns. Acad Emerg Med. 2005 May;12(5):431–438. doi: 10.1197/j.aem.2004.11.029. [DOI] [PubMed] [Google Scholar]
- 17.Fanari Z., Weiss S., Weintraub W.S. Cost effectiveness of antiplatelet and antithrombotic therapy in the setting of acute coronary syndrome: current perspective and literature review. Am J Cardiovasc Drugs. 2015 Dec 15:415–427. doi: 10.1007/s40256-015-0131-6. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Knight S., Klaskala W., Woller S.C. Antithrombotic therapy in patients with acute coronary syndrome in the intermountain heart collaborative study. Cardiol Res Pract. 2015;2015:270508. doi: 10.1155/2015/270508. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Montalescot G., Sabatine M.S. Oral dual antiplatelet therapy: what have we learnt from recent trials? Eur Heart J. 2015 Jan 21:344–352. doi: 10.1093/eurheartj/ehv377. [DOI] [PubMed] [Google Scholar]
- 20.Ruff C.T. The challenge of getting it just right: optimizing long-term antithrombotic therapy after acute coronary syndrome. J Am Coll Cardiol. 2015 Aug 18;66(7):788–790. doi: 10.1016/j.jacc.2015.06.1082. [DOI] [PubMed] [Google Scholar]
- 21.Daida H., Miyauchi K., Ogawa H. Management and two-year long-term clinical outcome of acute coronary syndrome in Japan: prevention of atherothrombotic incidents following ischemic coronary attack (PACIFIC) registry. Circ J. 2013;77(4):934–943. doi: 10.1253/circj.cj-13-0174. [DOI] [PubMed] [Google Scholar]
- 22.Misiriya K.J., Sudhayakumar N., Khadar S.A., George R., Jayaprakasht V.L., Pappachan J.M. The clinical spectrum of acute coronary syndromes: experience from a major center in Kerala. J Assoc Phys India. 2009 May;57:377–383. [PubMed] [Google Scholar]
- 23.Chudek J., Kowalczyk A., Kowalczyk A.K., Kwiatkowska J., Raczak G., Kozłowski D. Quality of life (QOL) evaluation after acute coronary syndrome with simultaneous clopidogrel treatment. Arch Med Sci. 2014 Feb 24;10(1):33–38. doi: 10.5114/aoms.2013.38708. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.Pavlides G., Drossinos V., Dafni C. Current management and quality of life of patients with acute coronary syndrome undergoing percutaneous coronary intervention in Greece: 12-Month results from antiplatelet therapy observational study II (APTOR II) Hellenic J Cardiol. 2013 Jul-Aug;54(4):255–263. [PubMed] [Google Scholar]