Abstract
Background
Real-world data on non-vitamin K oral anticoagulants (NOACs) are essential in determining whether evidence from randomised controlled clinical trials translate into meaningful clinical benefits for patients in everyday practice. RIVER (RIVaroxaban Evaluation in Real life setting) is an ongoing international, prospective registry of patients with newly diagnosed non-valvular atrial fibrillation (NVAF) and at least one investigator-determined risk factor for stroke who received rivaroxaban as an initial treatment for the prevention of thromboembolic stroke. The aim of this paper is to describe the design of the RIVER registry and baseline characteristics of patients with newly diagnosed NVAF who received rivaroxaban as an initial treatment.
Methods and results
Between January 2014 and June 2017, RIVER investigators recruited 5072 patients at 309 centres in 17 countries. The aim was to enroll consecutive patients at sites where rivaroxaban was already routinely prescribed for stroke prevention. Each patient is being followed up prospectively for a minimum of 2-years. The registry will capture data on the rate and nature of all thromboembolic events (stroke / systemic embolism), bleeding complications, all-cause mortality and other major cardiovascular events as they occur. Data quality is assured through a combination of remote electronic monitoring and onsite monitoring (including source data verification in 10% of cases). Patients were mostly enrolled by cardiologists (n = 3776, 74.6%), by internal medicine specialists 14.2% (n = 718) and by primary care/general practice physicians 8.2% (n = 417). The mean (SD) age of the population was 69.5 (11.0) years, 44.3% were women. Mean (SD) CHADS2 score was 1.9 (1.2) and CHA2DS2-VASc scores was 3.2 (1.6). Almost all patients (98.5%) were prescribed with once daily dose of rivaroxaban, most commonly 20 mg (76.5%) and 15 mg (20.0%) as their initial treatment; 17.9% of patients received concomitant antiplatelet therapy. Most patients enrolled in RIVER met the recommended threshold for AC therapy (86.6% for 2012 ESC Guidelines, and 79.8% of patients according to 2016 ESC Guidelines).
Conclusions
The RIVER prospective registry will expand our knowledge of how rivaroxaban is prescribed in everyday practice and whether evidence from clinical trials can be translated to the broader cross-section of patients in the real world.
Trial registration
Unique identifier: NCT02444221. Registerd 14 May 2015; Retrospectively Registered.
Electronic supplementary material
The online version of this article (10.1186/s12959-019-0195-7) contains supplementary material, which is available to authorized users.
Keywords: Anticoagulant, Antithrombotic, Atrial fibrillation, Outcomes, Registry, Rivaroxaban
Introduction
Atrial fibrillation (AF) is the most common sustained arrhythmia reported in adult patients [1] and is associated with an at least a five-fold increase in the risk of stroke [2]. Vitamin K antagonists (VKAs) formed the cornerstone of thromboembolic prophylaxis in patients with AF for many years. The introduction of non-vitamin K anticoagulants (NOACs), dabigatran, rivaroxaban, apixaban and edoxaban, provided physicians with agents with comparative efficacy and reduced potential for bleeding compared with vitamin K antagonists, while removing the need for dose titration, periodic laboratory testing and dietary restrictions that are necessary with VKAs [3–5]. Evidence from phase III studies showed that rivaroxaban, one of several oral direct Factor Xa inhibitors, is noninferior to warfarin for the reduction of stroke or systemic embolism in patients with AF [6] and significantly reduces rates of intracranial and fatal haemorrhages, but not rates of bleeding overall. Based on these results, rivaroxaban is now licensed in more than 130 countries worldwide for stroke prevention in patients with AF.
Real-world studies (such as Global Anticoagulant Registry in the FIELD-AF [GARFIELD-AF] [7], ORBIT-AF I & II) [8] and GLORIA-AF [9, 10] have demonstrated that NOAC use is increasing while post-marketing surveillance (such as Xarelto® for Prevention of Stroke in Patients with Atrial Fibrillation [XANTUS]) [11] and national studies (such as the EXPAND) [12, 13] have provided data on the safety and efficacy of rivaroxaban. However, most of these registries are disease-specific and evaluate treatment patterns and outcomes across different treatments. Therefore, additional drug-specific observational studies are needed to assess the clinical and health economic risk-benefits of specific NOACs and in particular, the factors that could potentially influence outcomes (e.g. compliance with prescribing guidelines, persistence and comorbidities) for each treatment alternative separately. This paper describes the design of the RIVaroxaban Evaluation in Real life setting (RIVER) registry and baseline characteristics of patients who received rivaroxaban as part of routine care. This paper also includes an initial analysis of the doses of rivaroxaban used in everyday practice as well as a description of the use of rivaroxaban in combination with antiplatelets in different clinical scenarios, such as patients with renal impairment.
Methods
Registry design
RIVER (NCT02444221) is an ongoing international, multicentre, prospective registry of patients with newly diagnosed non-valvular AF and at least one investigator-determined risk factor for stroke. All patients in this study are initiated on an anticoagulant treatment with rivaroxaban at the start of the study, as part of routine care, for the prevention of thromboembolic stroke.
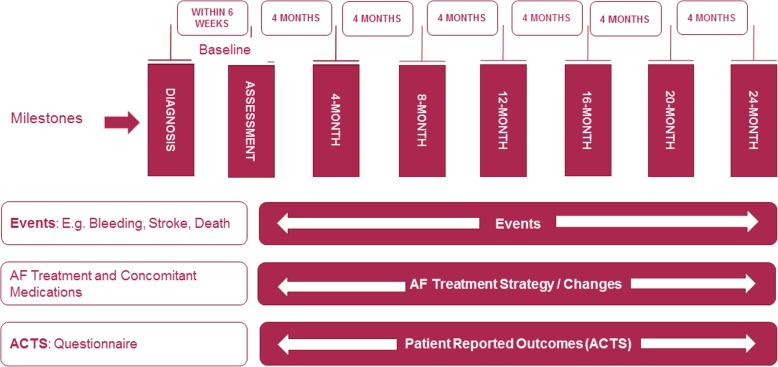
The goal of the RIVER registry is to provide insights into the clinical management and related outcomes of rivaroxaban-treated AF patients across a number of regions and across the spectrum of healthcare systems, in routine clinical management. Follow-up will be for a minimum of 2 years (and up to 3.5 years) after enrolment (Fig. 1). By capturing data from unselected patients treated in everyday practice, the registry has the potential to identify best practices as well as deficiencies in the use of rivaroxaban as an initial treatment for the prevention of thromboembolic events in patients with newly diagnosed AF. The decision to initiate treatment with rivaroxaban was based on clinicians’ judgement. The study was designed such that the collection of data would not interfere with the clinical management of patients or with the prescribing behaviours of attending physicians. No specific treatments, tests, or procedures were mandated or withheld from patients, and patients were free to withdraw from the registry at any time. The registry will not only assess the rates of clinical outcomes such as stroke and systemic embolization (SE), all-cause mortality, other major cardiovascular events (Table 1) and bleeding complications, but will also evaluate therapy persistence (including discontinuation, interruption and changes to the treatment regimen). Patients’ experiences using antithrombotic treatment will also be evaluated by the Anti-Clot Treatment Scale (ACTS) questionnaire.
Fig. 1.
Cohort design and data collection
Table 1.
Main Outcome Measures in the RIVER Registry
| Outcome | Category |
|---|---|
| Clinical events | Stroke (ischaemic and haemorrhagic) |
| Transient ischaemic attack | |
| Peripheral/non-central nervous system embolism | |
| Pulmonary embolism | |
| Heart failure | |
| Myocardial infarction | |
| Hospitalization | |
| Sudden cardiac death | |
| Non-cardiovascular death | |
| Bleeding events | |
| Severity | Major |
| Non-major clinically relevant | |
| Minor | |
| Location | Intracranial |
| Ears, nose, throat | |
| Gastrointestinal | |
| Genitourinary | |
| Vascular access site | |
| Outcome | Recovered |
| Permanently disabled | |
| Fatal | |
| Healthcare utilization used for bleeding event | Hospitalization |
| Emergency room visit | |
| Surgery for bleeding | |
| Transfusion | |
| Physician consultation | |
| Therapy persistence | Rate of discontinuation |
| Duration of time on therapy | |
| Reasons for discontinuation | |
| Hospitalization for any event | |
| Any other hospital visits | Inpatient, outpatient, and emergency room |
| Patients treated with vitamin K antagonists | Frequency and timing of monitoring |
| INR recordings in relation to therapeutic range | |
| Location of testing (self-monitoring, general practitioner clinic, anticoagulant clinic, etc.) | |
| Dose adjustments | |
| Use of bridging anticoagulation necessitated by interruption of vitamin-K antagonist | |
| Outcomes in relation to INR fluctuation | |
| Patients treated with additional antithrombotic therapy | Therapy changes (discontinuation, temporary interruptions and use of bridging therapy) |
| Reasons of therapy changes (if applicable) | |
| Patient treatment satisfaction using the Anti-Clot Treatment Scale (ACTS), depending on the cohort and country (at 4, 12, 24 months) | |
INR International normalise ratio
Independent ethics committee and hospital-based institutional review board approvals were obtained, as necessary, for the registry protocol. The registry is being conducted in accordance with the Declaration of Helsinki, local regulatory requirements, and the International Conference on Harmonisation–Good Pharmacoepidemiological and Clinical Practice guidelines.
RIVER is an independent academic research initiative, sponsored by the Thrombosis Research Institute, London, UK and funded by an unrestricted research grant from Bayer AG, Berlin, Germany. The authors are responsible for the design and conduct of this study, data analyses and the final content of this paper.
Registry population and site selection
The study population consists of consecutive patients enrolled prospectively at sites where rivaroxaban was already routinely prescribed for stroke prevention before the start of the study. Patients, receiving rivaroxaban as part of usual care, were eligible for enrolment in RIVER if they were 18 years of age or older, had a new diagnosis of non-valvular AF within the past 6 weeks and at least one additional risk factor for stroke as identified by the investigator. These risk factors were identified by clinicians and were not restricted to those in stroke prevention guidelines. Patients with a transient reversible cause of AF, those for whom follow-up is not foreseen or possible and all patients participating in interventional studies were excluded. All patients provided written informed consent to participate. Sites were chosen to be representative of AF care settings and included patients from multiple settings: office-based specialists, hospital departments (neurology, cardiology, geriatrics, internal medicine, and emergency room), anticoagulant clinics and general or family practice settings.
Data capture
Patient visits are not mandated, but data collection using the electronic case report form (eCRF) occurs at 4-monthly intervals and captures all relevant data from the patients’ medical notes (Fig. 1).
A summary of the evaluations performed at baseline and at follow-up visits are outlined in Additional file 1: Table S1. At entry into the study, data are collected on the care setting, patients’ demographics, vital signs, medical history, the nature of AF (paroxysmal versus persistent versus permanent), symptoms of AF, relevant medications, including antiplatelet and other concomitant therapy and investigator-identified risk factors for stroke. The results from investigations at diagnosis (including ECG morphology, left ventricular ejection fraction [LVEF] measurement, full blood count, haemoglobin, platelet count and creatinine) are recorded as well as the treatment strategy for AF (rate or rhythm control) and the date and outcome following cardioversion. Information is collected on initial rivaroxaban dosing regimen, start and stop dates, changes in therapy, compliance concerns and the reason for suspending or terminating therapy sooner than intended (such as bleeding, patient decision, and/or physician decision). Patients’ experiences using antithrombotic treatment are recorded on the Anti-Clot Treatment Scale (ACTS) questionnaire at 4, 12 and 24 months.
At 4-monthly intervals, all routinely performed tests (including INR, haemoglobin, platelet count and creatinine), vital signs as well as all major events (stroke/transient ischaemic attack [TIA], bleeding / site of bleeding, death, myocardial infarction [MI], acute coronary syndrome [ACS], peripheral embolism) and hospitalizations/medical consultations are documented. For patients who switch to VKAs, data are also collected on INR, INR frequency and outcome related to INR fluctuation.
Based on the data collected from the eCRF, healthcare resource consumption will be captured so that the economic burden of AF can be computed both overall and per patient per year from the perspective of the payer, e.g. national health service, public/private/statutory insurance etc.
Data management
Data are captured using an electronic case report form (eCRF) designed by eClinicalHealth Services, Stirling, UK and submitted electronically via a secure website to the registry-coordinating centre at the Thrombosis Research Institute who were responsible for checking the completeness and accuracy of data collected from medical records. All patients are assigned a unique identifier and personal identifiable data will be removed at the hospital source, ensuring anonymity and protecting confidentiality.
Data quality is assured through a combination of remote electronic monitoring and more conventional onsite monitoring (including source data verification in 10% of all cases), based on the validated quality assurance programmes developed in GARFIELD-AF [14]. The milestones for study eCRFs will be examined by the registry-coordinating centre at TRI, to ascertain completeness, accuracy and data queries sent to participating sites.
Statistical analysis
Continuous variables are expressed as mean ± standard deviation (SD). Categorical variables are expressed as frequencies and percentages. Statistical analysis was performed using SAS software version 9.4 (SAS Institute Inc., Cary, NC, USA).
Results
Baseline characteristics
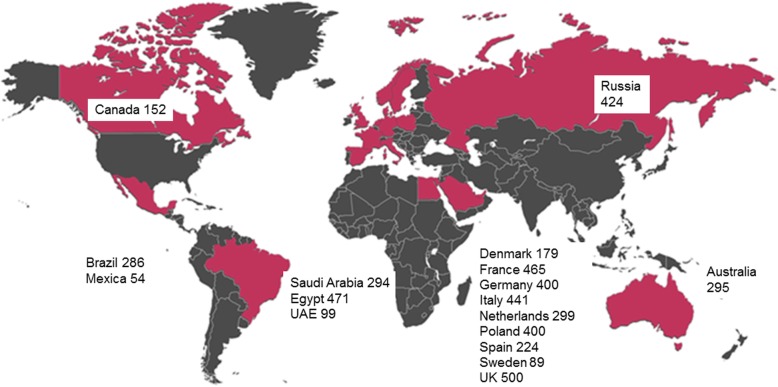
A total of 5282 patients were screened for inclusion into RIVER between January 2014 and June 2017 and 5072 eligible patients were included in the analysis of baseline characteristics. Reasons for the exclusion of 210 patients after screening were: age ≤ 18 years (n = 4), alternative AC treatment before rivaroxaban after AF diagnosis (n = 68), no risk factor for stroke (n = 22), patients having transient AF secondary to a reversible cause (n = 10), difficulty in long-term follow-up (n = 24), patients participating in other interventional studies (n = 9) and, finally, patients whose enrolment was not confirmed due to either patient’ decision (n = 27), death before consent (n = 1) or other reason (n = 77). Patients were recruited from 309 centres in 17 countries, including patients from Europe (67.5%) (Denmark, France, Germany, Italy, Netherlands, Poland, Russia, Spain, Sweden and UK), the Middle East (17.0%) (Egypt, Saudi Arabia and UAE), Australia (5.8%), Canada (3.0%), Brazil (5.6%) and Mexico (1.1%) (Fig. 2). Overall, 74.6% (n = 3779) of patients were enrolled by cardiologists, 14.2% (n = 718) by internal medicine specialists and 8.2% (n = 417) by primary care/general practice physicians.
Fig. 2.
Location of enrolling centres of the RIVER Registry. Australia, Brazil, Canada, Denmark, Egypt, France, Germany, Italy, Mexico, Netherlands, Poland, Russia, Saudi Arabia, Spain, Sweden, UAE, UK
Approximately one-third of patients (36.3%) in RIVER had asymptomatic AF. Among patients with symptomatic AF, the most common symptoms identified were: palpitations (38.4%), shortness of breath (31.8%) and tiredness (14.8%). At the time of enrolment, 34.2% of patients had new or unclassified AF, 34.2% paroxysmal AF, 15.9% persistent AF and 15.7% permanent AF.
Baseline patient characteristics are described in Table 2. Caucasian patients represented the largest proportion of patients in RIVER (80.3%), followed by Asians (5.6%) and hispanic/latino (3.7%). Beyond the factors defined by CHA2DS2-VASc, physicians also considered the following as risk factors for stroke: smoking (12.8%), obesity (19.5%), renal impairment (5.9%), proteinuria (1.9%), enlarged left atrium (16.4%), thyroid disease (5.9%), thrombus in atrium (0.4%) and Chagas disease (0.3%) amongst others (5.3%).
Table 2.
Patient baseline characteristics
| Variable | All patients (N = 5072) |
|---|---|
| Agea, mean ± SD, years | 69.5 ± 11.0 |
| Age groupa, n (%) | |
| < 65 | 1444 (28.5) |
| 65–74 | 1861 (36.8) |
| ≥ 75 | 1758 (34.7) |
| Women, n (%) | 2248 (44.3) |
| Body mass indexb, mean ± SD, kg/m2 | 29.2 ± 5.7 |
| Smoking status (current/previous)c, n (%) | 1599 (35.3) |
| Pulsed, mean ± SD, bpm | 85.1 ± 23.8 |
| Medical history, n (%) | |
| Hypertensione | 3899 (77.0) |
| Hypercholesterolemiaf | 2208 (43.9) |
| Diabetes mellitusg | 1227 (24.3) |
| Congestive heart failureh | 1086 (21.5) |
| Family history of cardiac diseasei | 618 (19.5) |
| Coronary artery diseasej | 967 (19.2) |
| Current/History of myocardial infarction or unstable anginak | 718 (14.2) |
| Chronic renal diseasel | |
| Mild renal dysfunction (stage: I, II) | 629 (13.5) |
| Moderate renal dysfunction (stage: III) | 186 (4.0) |
| Severe renal dysfunction (stage: IV, V) | 26 (0.6) |
| Left ventricular ejection fraction < 40%m | 305 (9.5) |
| Stroken | 365 (7.2) |
| Transient ischaemic attacko | 331 (6.5) |
| Aortic or peripheral artery diseasep | 252 (5.0) |
| Carotid diseaseq | 212 (4.2) |
| History of bleedingr | 118 (2.3) |
| Heavy alcohol consumptions | 83 (2.1) |
| Venous thromboembolismt | 103 (2.0) |
| Systemic embolizationu | 56 (1.1) |
| Cirrhosisv | 20 (0.4) |
aData not available for 9 patients
bData not available for 586 patients
cData not available for 541 patients
dData not available for 236 patients
eData not available for 9 patients
fData not available for 44 patients
gData not available for 12 patients
hData not available for 10 patients
iData not available for 1906 patients
jData not available for 28 patients
kData not available for 21 patients
lData not available for 395 patients
mData not available for 1870 patients
nData not available for 11 patients
oData not available for 15 patients
pData not available for 29 patients
qData not available for 53 patients
rData not available for 12 patients
sData not available for 1087 patients
tData not available for 15 patients
uData not available for 17 patients
vData not available for 24 patients
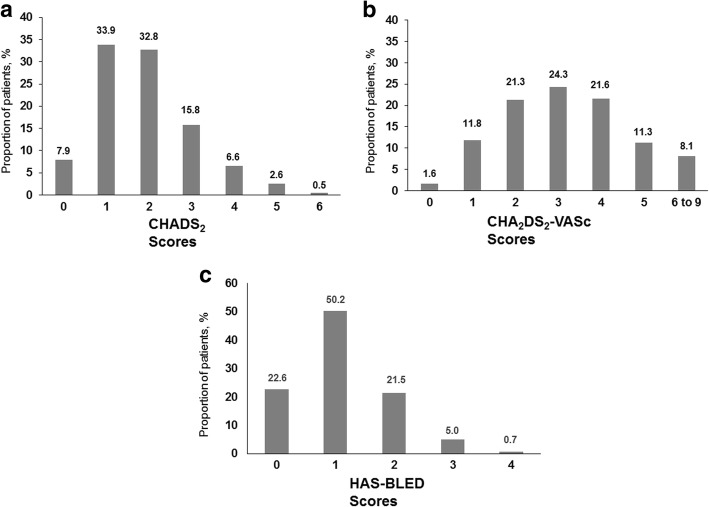
Figure 3 describes the prescribing of rivaroxaban according to the post-hoc calculation of CHADS2 and CHA2DS2-VASc risk scores. The mean (SD) CHADS2 score for patients in the RIVER was 1.9 (1.2) and 58.2% of patients had a score of ≥2. Mean (SD) CHA2DS2-VASc score was 3.2 (1.6). Most patients met the recommended threshold for AC therapy (86.6% for 2012 ESC Guidelines, and 79.8% of patients according to 2016 ESC Guidelines). The mean (SD) HAS-BLED score was 1.1 (0.8) and the most commonly observed bleeding risk factors were: hypertension (77.0%), stroke (7.2%) and moderate-to-severe chronic renal disease (4.6%).
Fig. 3.
a Distribution of CHADS2 b CHA2DS2-VASc and c HAS-BLED scores in RIVER registry
Rivaroxaban dosing
Almost all patients (98.5%) were prescribed a single daily dose of rivaroxaban, most commonly 20 mg (76.5%) and 15 mg (20.0%), while10 mg dose was prescribed in only 2.1% of patients. Creatinine clearance (CrCl) information at enrolment, estimated using the Cockcroft-Gault equation, was available for 3135 of 5072 (61.8%) patients. The mean (SD) CrCl was 83.7 (35.6) mL/min and 86.1% patients had CrCl ≥50 mL/min. Among patients with normal or mild renal function (CrCl ≥50 mL/min), 2246 (83.2%) were prescribed the recommended rivaroxaban dose of 20 mg once daily at baseline. Of patients with moderate or severe renal impairment (CrCl 15–49 mL/min), 246 (56.6%) patients received rivaroxaban 15 mg once daily, 173 (39.8%) 20 mg once daily and 16 (3.7%) 10 mg once daily as their initial treatment.
Concomitant antiplatelet therapy
Just under one in five (17.9%, n = 904) patients who were initiated on rivaroxaban at the time of diagnosis of AF also received concomitant antiplatelet therapy. Use of antiplatelets was higher in patients with a CHA2DS2-VASc score of 2–9 (19.4%) than in those with a score of 0 or 1 (9.2%) (Table 3); 229 (25.3%) had a coronary artery disease (CAD), peripheral artery disease (PAD) or carotid disease. The most frequently used antiplatelet was aspirin in 55.4% (501 of 904) of cases. Overall, 76 (1.5%) patients received dual AP therapy (ADP receptor/P2Y12 and aspirin).
Table 3.
Use of antithrombotic drugs at diagnosis, overall and according to CHA2DS2-VASc scores of 0 or 1 and 2–9
| Antiplatelet druga | All patients (N = 5072) | Patients with CHA2DS2-VASc score of 0 or 1 (N = 665) | Patients with CHA2DS2-VASc score 2–9 (N = 4289) |
|---|---|---|---|
| Acetylsalicylic acid (Aspirin/ASA) | 501 (9.9) | 28 (4.2) | 465 (10.8) |
| ADP receptor/P2Y12 inhibitor | 248 (4.9) | 13 (2.0) | 231 (5.4) |
| Glycoprotein IIb/IIIa inhibitor | 9 (0.2) | 2 (0.3) | 6 (0.1) |
| Prostaglandin analogue | 71 (1.4) | 5 (0.8) | 66 (1.5) |
| Other antiplatelet | 8 (0.2) | 2 (0.3) | 6 (0.1) |
aCategories are not mutually exclusive
Discussion
Observational or non-interventional studies play an important role in understanding and confirming the clinical effectiveness of interventions across the spectrum patients treated in routine practice.
RIVER is an independent treatment registry of patients from multiple care settings and patients were recruited from 17 countries. The RIVER registry provides an opportunity to examine the impact of different recruitment methodologies on the characteristics and treatment between the registries. RIVER will document the regional heterogeneity in the clinical presentation and assess the rate of stroke and systemic embolism and other outcomes with specific reference to the incidences of bleeding and therapy persistence. In addition to reporting on pre-specified clinical and economic outcomes, analyses from RIVER will be hypothesis generating, allowing the exploration of some aspects of the real world situation of AF treated with rivaroxaban and outcomes.
The degree of the patient involvement in the generation of data is expected to provide unique insights into the patients-reported outcomes. Patients’ experiences using antithrombotic treatment are recorded on the Anti-Clot Treatment Scale (ACTS) questionnaire. It is important to recognise that registries differ in their design, recruitment strategies, care settings, geographical spread and duration of follow-up. Compared to other ongoing prospective registries, the RIVER registry has the potential to capture the medicosocial burden due to AF in large-scale populations by employing broad inclusion and exclusion criteria in widely representative populations of patients with AF who are treated with rivaroxaban, across a range of clinical settings and to capture long-term follow-up data. The value of RIVER registry is enhanced by a quality assurance programme and the supervision of an independent Audit Committee, which oversees site-dependent verification, remote site monitoring and electronic database monitoring to ensure data quality.
There are several phase IV studies (such as XANTUS [15], XAPASS [16], XASSURE (China; NCT02784717) and registries such as EXPAND [12]) are ongoing to investigate rivaroxaban in patients with NVAF in the real world clinical settings. The XANTUS program comprises three studies: the XANTUS (Europe, Israel plus enrollment in Canada; NCT01606995), XANTUS-EL (Eastern Europe, Eastern Mediterranean, Middle East, Latin America; NCT01800006) and XANAP (Asia-Pacific; NCT01750788) [15].
Other ongoing non-interventional registries also provide real-world data on the effectiveness and safety of rivaroxaban, including the Global Anticoagulant Registry in the FIELD (GARFIELD)-AF [17], Outcomes Registry for Better Informed Treatment of Atrial Fibrillation (ORBIT)-AF I and ORBIT-AF II [18–21], the Global Registry on Long-Term Oral Anthithrombotic Treatment in pateints with Atrial Fribrillation (GLORIA-AF) [22–26] and the Dresden NOAC Registry [4, 5, 27] (Additional file 1: Table S2).
In the presence of all these observational studies, it is important to highlight that there are a number of important differences in the design (Additional file 1: Table S2) and recruitment of patients (Table 4) in RIVER compared with these registries. RIVER is a drug-specific registry which allows studying of drug utilisation patterns including off-label use whereas other registries like GARFIELD-AF, ORBIT-AF I and II, GLORIA-AF and Dresden NOAC are disease-specific registries which allows studying of burden, management and adverse event profile for different treatments related to a specific disease. Patients in XANTUS study were enrolled from Europe, Israel and Canada whereas EXPAND and XAPASS are Japanese registries and ORBIT-AF registries are restricted to USA [19]. By contrast, RIVER has recruited patients more broadly from 17 countries (outside Asia) including Europe, the Middle East, Latin America, Canada and Australia. RIVER provides long-term follow-up data of 2 years where as XANTUS had 1-year follow-up data. RIVER is a more contemporary population in which physicians’ now have experience using the NOACs. It is a known phenomenon that, after approval of new treatments, physicians start to apply these first in well-defined, carefully selected populations and expand it to other populations only after a period of time, which is reflecting learning curves based on increased comfort levels, communication of real world evidence, newly reported and previously unknown side effects or changes in guideline recommendations [28–30] . As a consequence, treatment patterns and outcomes may shift over time, which is an additional justification for more contemporary registries in SPAF. All of these factors may have contributed to the observed differences in patients characteristics, compared to other observational studies. Patients in RIVER are younger (mean age: 69.5 years) than patients in EXPAND (72 yrs), XANTUS (71.5 yrs), and XAPASS (73.1 yrs). The mean BMI of patients in RIVER (29.2 ± 5.7) is higher than the Japanese cohort in XAPASS (23.7 ± 3.8) (Table 4). Patients studied in RIVER also had a lower risk of stroke, with a mean CHADS2 scores of 1.9 and 13.4% had a prior episode of stroke/TIA/SE when compared to XANTUS (2.0, 19%) and XAPASS (2.2; 23.7%) (Additional file 1: Table S3) and other NOAC trials, such as RE-LY (2.1; 20.0%) and ARISTOTLE (2.1; 19.4%) [31, 32]. Nevertheless, patients in RIVER had high rates of comorbid conditions, including hypertension, hypercholesterolemia, diabetes mellitus, heart failure and coronary artery disease. However, the proportion of patients (8.6%) with renal dysfunction (CrCl < 50 mL/min) in RIVER was similar to XANTUS (9.4%) and lower than Japanese cohorts in EXPAND (20.8%) and XAPASS (23.9%); although this observation may be due to the higher rates of missing CrCl measurements in both RIVER (38.0%) and XANTUS (34.4%). Patients in RIVER and XANTUS received higher doses of rivaroxaban (20 mg/day [76.5 and 78.7% patients, respectively], 15 mg/day [20.0 and 20.8% patients, respectively]) than those in EXPAND (15 mg/day [56.6% patients], 10 mg/day [43.4% patients]), suggesting differences in the guideline recommendations, which are based on patient characteristics and ethnicities. In Japan, the regular dosage of rivaroxaban is 15 mg od, which is lower than the global recommended dosage of 20 mg od [33].
Table 4.
Comparison of adjusted demographic and baseline clinical characteristics of patients from the international observational studies (RIVER and XANTUS), studies from Japan (EXPAND and XAPASS)
| RIVER | XANTUS | EXPAND | XAPASS | |
|---|---|---|---|---|
| Patients, n | 5072 | 6784 | 7141 | 11,308 |
| Patient characteristics | ||||
| Sex, male (%) | 55.7 | 59.2 | 67.7 | 61.9 |
| Age, mean (SD) | 69.5 (11.0) | 71.5 (10.0) | 71.6 (9.4) | 73.1 (9.9) |
| BMI (Kg/m2), mean (SD) | 29.2 (5.7) | 28.3 (5.0) | NA | 23.7 (3.8) |
| Creatinine clearance (mL/min), mean (SD) | 83.7 (35.6) | NA | 69.7 (26.2) | 67.7 (28.9) |
| < 15 mL/min (%) | 0.02 | 0.3 | NA | 0.03 |
| ≥ 15 to < 30 mL/min (%) | 0.7 | 1.1 | 1.9 | 2.8 |
| ≥ 30 to < 50 mL/min (%) | 7.9 | 8.0 | 18.9 | 21.1 |
| ≥ 50 mL/min (%) | 53.4 | 56.2 | 74.6 | 68.0 |
| Missing (%) | 38.0 | 34.4 | 4.7 | 8.2 |
| Rivaroxaban dose/dosing frequency | ||||
| 10 mg once daily | 105 (2.1) | NA | NA | NA |
| 15 mg once daily | 1008 (20.0) | 1410 (20.8) | NA | NA |
| 20 mg once daily | 3867 (76.5) | 5336 (78.7) | NA | NA |
| 10 mg twice daily | 10 (0.2) | NA | NA | NA |
| 15 mg twice daily | 29 (0.6) | NA | NA | NA |
| 20 mg twice daily | 22 (0.4) | NA | NA | NA |
| 10/15/20 mg other dosing Regimen | 12 (0.2) | 35 (0.5) | NA | NA |
| CHADS2 score, mean (SD) | 1.9 (1.2) | 2.0 (1.3) | 2.1 (1.3) | 2.2 (1.3) |
| CHA2DS2-VASc score, mean (SD) | 3.2 (1.6) | 3.4 (1.7) | 3.4 (1.7) | NA |
| Comorbidity/medical history | ||||
| Congestive heart failure (%) | 21.5 | 18.6 | 26.1 | 25.0 |
| Hypertension (%) | 77.0 | 74.7 | 70.9 | 74.3 |
| Diabetes mellitus (%) | 24.3 | 19.6 | 24.3 | 22.3 |
| History of stroke/systemic embolism/TIA (%) | 13.4 | 19.0 | 24.1 | 23.7 |
| Type of AF | ||||
| Paroxysmal (%) | 34.2 | 40.7 | 44.8 | NA |
| Non-paroxysmal (persistent/permanent) (%) | 31.6 | 40.8 | 55.2 | NA |
| First diagnosed (%) | 34.2 | 18.5 | NA | NA |
Limitations
Centres for recruitment of patients in RIVER are limited to the care settings where rivaroxaban is the standard of care and includes sites beyond those included in the clinical trials. Comparison of different treatments are not possible, as there is no comparator drug, while larger prospective disease registries such as GARFIELD-AF and drug registries such as GLORIA-AF and ORBIT-II have the potential to conduct comparative effectiveness studies between different treatment approaches in newly diagnosed patients with AF. Due to the observational design of the study, laboratory and other investigations could not mandated.
Strengths
RIVER is an independent academic research initiative. This prospective registry was designed with a novel approach to outcomes research, including the following features: sites representation of national AF care settings, randomised site selection, unselected eligible patients enrolled consecutively with a follow-up period of minimum 2 years and extensive monitoring and audit including source data verification of 10% of all eCRFs. Like other prospective registries, such as GARFIELD-AF [34], RIVER aims to overcome the inherent bias of retrospective cohort studies from national registries and claims databases [35–39].
Conclusion
The RIVER prospective registry will expand our knowledge of how rivaroxaban is prescribed in everyday practice and whether evidence from clinical trials can be translated to the broader cross-section of patients treated in the real world.
Additional file
Table S1. Evaluations performed at Baseline and at Follow-Up Visits. Table S2. Study design of ongoing real-world studies of rivaroxaban. Table S3. Comparison of distribution of baseline CHADS2, CHA2DS2-VASc or HAS-BLED scores of patients from observational RIVER, XANTUS, EXPAND and XAPASS studies. (DOC 155 kb)
Acknowledgments
We thank the physicians, nurses, and patients involved in the RIVER Registry. SAS programming support was provided by Madhusudana Rao (Thrombosis Research Institute, London, UK). Editorial support was provided by Surekha Damineni (Thrombosis Research Institute, London, UK).
RIVER Registry Investigators
Global Steering Committee
Ajay K. Kakkar (UK) (Chair), A. John Camm (UK), Jean-Yves Le Heuzey (France), Keith A.A. Fox (UK), Jan Beyer-Westendorf (Germany), Sylvia Haas (Germany), Alexander G.G. Turpie (Canada).
Publications Committee
A. John Camm (UK) (Chair), Ajay K. Kakkar (UK), Karen S. Pieper (USA), Gloria Kayani (UK).
Audit Committee
Keith A.A. Fox (UK), Bernard J. Gersh (USA).
RIVER Principal Investigators
Europe
Denmark: P. Hildebrandt, H. Dominguez, W. Comuth, L. Frost, D.S. Moller, H. Christensen, L.M. Bruun.
France: A. Milhem, J. Gauthier, C. Mielot, S. Chanseaume, S. Chopra, A. Amlaiky, O. Tricot, V. Sierra, A. Dompnier, N. Zannad, A. Pinzani, A. Quatre, J. Mansourati, L. Fauchier, N. Badenco, E. Gandjbakhch, K.F. Chachoua, V. Malquarti, F. Pierron, F. Sacher, J. Taieb, J.M. Davy, E. Marijon, N. Lellouche, A. Leenhardt, A. Salem, I. Lesto, J.J. Muller, R. Garcia, J.P. Neau, J.B. Berneau.
Germany: N. Schön, D. Gulba, K.F. Appel, J. Merke, J. Dshabrailov, C. Bauknecht, O. Scheuermann, T. Schröder, W. Jung, A. Kopf, J. Brachmann, M. Leschke, J. Taggeselle, M. Seige, T. Läßig, S. Appel, M. Schmiedl, K. Müller, G.U. Heinz, C. Axthelm, K. Eberhard, B. Hügl, T. Schwarz, U. Sechtem.
Italy: A. Falanga, V. Rubino, L. Calo, W. Ageno, F. Massari, D. Imberti, L. Di Gennaro, F. Gaita, A. Margonato, G. Cannava, F. Capasso, I. Diemberger, F. Pelliccia, A. Cafolla, S. Bardari, L. Mattei, L. Ruocco, G. Boriani, D. Poli, S. Testa, C. Indolfi, R. Quintavalla, L. Mos.
Netherlands: G. Ladyjanskaia, I. Aksoy, M. Van De Wetering, L. Theunissen, F. Den Hartog, R. Nijmeijer, R. Van De Wal, S. Reinders, M. Patterson, E.D. Melker, R. Troquay.
Poland: J. Korecki, A. Szyszka, F. Diks, J. Sumis, J. Cygler, B. Miklaszewicz, E. Litwiejko-Pietrynczak, P. Napora, G. Drelich, T. Kawka-Urbanek, J.K. Wranicz, M. Mierzejewski, A. Drzewiecka, D. Wronska, I. Fares, J. Baska, K. Stania, W. Krzyzanowski, P. Miekus, M. Tyminski.
Russia: D. Dronov, S. Zenin, E. Isaeva, A. Lopukhov, V. Yakusevich, D. Kuznetsov, T. Kameneva, E. Pokushalov, V. Karetnikova, I. Dik, I. Karpushina, D. Nikolin, A. Doletsky, A. Ardashev, A. Timofeeva, O. Miller, N. Lyamina, Y. Shubik, S. Boldueva.
Spain: J.L. Blanco Coronado, C. Gonzalez Juanatey, E. Otero, D. Alonso, J. Torres Llergo, J. Gonzalez Lama, J.A.V. De Prada Tiffe, F.J. Garcia Seara, J.J. Gomez Doblas, J.A. Riancho, J.L. Clua-Espuny, J. Motero, V.I. Arrarte, D. Martin Raymondi, G. Isasti Aizpurua, F. Marin, J.A. Nieto, J. Fernandez Portales, P. Alvarez Garcia.
Sweden: I. Torstensson, B. Cederin, T. Kalm, U. Rosenqvist, J. Thulin, A. Hajimirsadeghi, M. Crisby.
UK: A. Manoj, A. Bakhai, A. Mistri, M. Krishnan, S. Kumar, S. Kirubakaran, H. Thomas, J. Camm, F. Ahmed, A.M. Ross, K. Barry, R. Stockwell, A. Broadley, M. Mamun, K. Chatterjee, J. Cooke, J. McCready, D. Dutta, K. John, P. Pandya, R. Howlett, P.Vinson, Lim, P. Foley, D. Bruce, A. Dixit, D. Broughton, J. Taylor, R. Schilling.
Middle East
Egypt: K. Leon, K. Saeed, S. Shaheen, M. Tawfik, A. Mortadda, M. Seleem, M.S.I Aly, G. Kazamel, M. Elbadry, S. Kamal, M. Hassan, M. Mostafa, M.E.S. Medhat, Ekhlas, R. Ghaleb, M.O. Taha, I. Daoud, H. Al Din, A.M. Imam, M.A. El Hameed, Helmy.
Saudi Arabia: M. Al-Murayeh, N. Akhtar, B.M. Matto, M.A. Ghani, O.A. Amoudi, M.M. Morsy, A.A.F Bashir, Y. M. Al Hossni, B. Al Ghamdi, Zia-ul-Sabah, S. Mir, D. Dardir, A. Masswary, A.R. Al Shehri, A. Masswary, J. Iqbal, M.A.J. Almansori.
UAE: C.G Venkitachalam, J. Kurian, J. Rao, A. Aisheh, A.A. Albawab, B. Subbaraman, A. Amanat, K.J. Esfehani, R. Lochan, A. Bin Brek, B. Mittal, Y. Ghazi, M. Krishna, S.B. Tabatabaei, P.S. Thoppil, S. Nasim, S. El Khider Nour.
Latin America
Brazil: P. Barros, A.P. Almeida, M. Andrade, B. Garbelini Jr., T.L. Silvestrini, Á.R. Alves Junior, C.E.B. de Lima, A. Kormann, G.G. de Lima, C. Halperin, D. Salvadori Junior, A.F. Freitas Jr., J.R. Gemelli, C.E. Ornelas, J.M.M. Dantas, J.L. Aziz, L.M. Backes, W.S. Barroso, M.S. Paiva, J. A. de Figueiredo Neto, F.R. dos Santos, J.A. de Lima Neto, R. Bergo, P.R. Salvador Junior.
Mexico: A.G. López, J.C.P Alva, M.A.A. Gamba, F.G. Padilla-Padilla, A.E.B. Ruiz.
Other countries:
Canada: J. Berlingieri, A. Bakbak, M. Gupta, K. Saunders, A. Costa-Vitali, P.R. Beaudry, R. Bhargava, Y. Khaykin, J.S. Healey, E. Crystal, Nadeau, Dhillon.
Australia: Alistair Begg, C. Anderson, S. Baveja, D. Cross, A. Catanchin, D. Brieger, K.T. Lim, P. Davidson, R. Tan, R. Bhindi, J. Hickey, J. Layland, M. Bloch, C. Itty, B. Singh, P. Carroll, A. Lee, G. Starmer, R. Lehman.
Funding
This work is supported by an unrestricted research grant from Bayer AG (Berlin, Germany) to the Thrombosis Research Institute (London, UK), which sponsors the RIVER registry. The funding source had no involvement in the data collection, data analysis or data interpretation.
Availability of data and materials
No additional data is available.
Abbreviations
- AC
Anticoagulant
- ACTS
Anti-Clot Treatment Scale
- AF
Atrial fibrillation
- AP
Antiplatelet
- CAD
Coronary artery disease
- CHF
Congestive heart failure
- CrCl
Creatinine clearance
- LVEF
Left ventricular ejection fraction
- MI
Myocardial infarction
- NOACs
Non-vitamin K anticoagulants
- NVAF
Non-valvular atrial fibrillation
- PAD
Peripheral artery disease
- SE
Systemic embolism
- TIA
Transient ischaemic attack
- VKA
Vitamin K antagonist
Authors’ contributions
JBW, AJC, KAAF, JYLH, SH, AGGT and AKK contributed to the study design. SV analysed the data. All authors contributed to data interpretation. JBW and AJC drafted the report. All authors critically reviewed the report and approved the final manuscript.
Ethics approval and consent to participate
Independent ethics committee and hospital-based institutional review board approvals were obtained, as necessary, for the registry protocol.
Consent for publication
Not applicable.
Competing interests
JB-W has received grants and personal fees from Bayer, Daiichi, Janssen, Pfizer and Portola and has received grants from Boehringer. AJC has received personal fees from Bayer, Boehringer Ingelheim, Pfizer/BMS, Daiichi Sankyo, Portola and Verseon and has received grants from Bayer, Boehringer Ingelheim, Pfizer/BMS and Daiichi Sankyo. KAAF has received grants and personal fees from Bayer/Janssen and AstraZeneca and personal fees from Sanofi/Regeneron and Verseon outside the submitted work. JYLH has received personal fee from AstraZeneca, Bayer, Boehringer Ingelheim, BMS/Pfizer, Daiichi Sankyo, Meda, Sanofi, and Servier. SH has received personal fees from Aspen, Bayer Healthcare, BMS/Pfizer, Daiichi-Sankyo, Portola and Sanofi. AGGT has received personal fees from Bayer Healthcare, Janssen Pharmaceutical Research & Development LLC, Astellas, Portola, and Takeda.SV has no disclosures. AKK has received research support from Bayer AG; personal fees from Bayer AG, Boehringer-Ingelheim Pharma, Daiichi Sankyo Europe, Janssen Pharma, Sanofi SA and Verseon.
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Contributor Information
Jan Beyer-Westendorf, Phone: +49-351-4583659, Email: Jan.Beyer@uniklinikum-dresden.de.
A. John Camm, Email: jcamm@sgul.ac.uk.
Keith A. A. Fox, Email: k.a.a.fox@ed.ac.uk
Jean-Yves Le Heuzey, Email: jyleheu@gmail.com.
Sylvia Haas, Email: sylvia@sylviahaas.com.
Alexander G. G. Turpie, Email: turpiea@mcmaster.ca
Saverio Virdone, Email: SVirdone@tri-london.ac.uk.
Ajay K. Kakkar, Email: akkakkar@tri-london.ac.uk
for the RIVER Registry Investigators:
Ajay K. Kakkar, A. John Camm, Jean-Yves Le Heuzey, Keith A. A. Fox, Jan Beyer-Westendorf, Sylvia Haas, Alexander G. G. Turpie, Karen S. Pieper, Gloria Kayani, Bernard J. Gersh, P. Hildebrandt, H. Dominguez, W. Comuth, L. Frost, D. S. Moller, H. Christensen, L. M. Bruun, A. Milhem, J. Gauthier, C. Mielot, S. Chanseaume, S. Chopra, A. Amlaiky, O. Tricot, V. Sierra, A. Dompnier, N. Zannad, A. Pinzani, A. Quatre, J. Mansourati, L. Fauchier, N. Badenco, E. Gandjbakhch, K. F. Chachoua, V. Malquarti, F. Pierron, F. Sacher, J. Taieb, J. M. Davy, E. Marijon, N. Lellouche, A. Leenhardt, A. Salem, I. Lesto, J. J. Muller, R. Garcia, J. P. Neau, J. B. Berneau, N. Schön, D. Gulba, K. F. Appel, J. Merke, J. Dshabrailov, C. Bauknecht, O. Scheuermann, T. Schröder, W. Jung, A. Kopf, J. Brachmann, M. Leschke, J. Taggeselle, M. Seige, T. Läßig, S. Appel, M. Schmiedl, K. Müller, G. U. Heinz, C. Axthelm, K. Eberhard, B. Hügl, T. Schwarz, U. Sechtem, A. Falanga, V. Rubino, L. Calo, W. Ageno, F. Massari, D. Imberti, L. Di Gennaro, F. Gaita, A. Margonato, G. Cannava, F. Capasso, I. Diemberger, F. Pelliccia, A. Cafolla, S. Bardari, L. Mattei, L. Ruocco, G. Boriani, D. Poli, S. Testa, C. Indolfi, R. Quintavalla, L. Mos, G. Ladyjanskaia, I. Aksoy, M. Van De Wetering, L. Theunissen, F. Den Hartog, R. Nijmeijer, R. Van De Wal, S. Reinders, M. Patterson, E. D. Melker, R. Troquay, J. Korecki, A. Szyszka, F. Diks, J. Sumis, J. Cygler, B. Miklaszewicz, E. Litwiejko-Pietrynczak, P. Napora, G. Drelich, T. Kawka-Urbanek, J. K. Wranicz, M. Mierzejewski, A. Drzewiecka, D. Wronska, I. Fares, J. Baska, K. Stania, W. Krzyzanowski, P. Miekus, M. Tyminski, D. Dronov, S. Zenin, E. Isaeva, A. Lopukhov, V. Yakusevich, D. Kuznetsov, T. Kameneva, E. Pokushalov, V. Karetnikova, I. Dik, I. Karpushina, D. Nikolin, A. Doletsky, A. Ardashev, A. Timofeeva, O. Miller, N. Lyamina, Y. Shubik, S. Boldueva, J. L. Blanco Coronado, C. Gonzalez Juanatey, E. Otero, D. Alonso, J. Torres Llergo, J. Gonzalez Lama, J. A. V. De Prada Tiffe, F. J. Garcia Seara, J. J. Gomez Doblas, J. A. Riancho, J. L. Clua-Espuny, J. Motero, V. I. Arrarte, D. Martin Raymondi, G. Isasti Aizpurua, F. Marin, J. A. Nieto, J. Fernandez Portales, P. Alvarez Garcia, I. Torstensson, B. Cederin, T. Kalm, U. Rosenqvist, J. Thulin, A. Hajimirsadeghi, M. Crisby, A. Manoj, A. Bakhai, A. Mistri, M. Krishnan, S. Kumar, S. Kirubakaran, H. Thomas, J. Camm, F. Ahmed, A. M. Ross, K. Barry, R. Stockwell, A. Broadley, M. Mamun, K. Chatterjee, J. Cooke, J. McCready, D. Dutta, K. John, P. Pandya, R. Howlett, P. Vinson, Lim, P. Foley, D. Bruce, A. Dixit, D. Broughton, J. Taylor, R. Schilling, K. Leon, K. Saeed, S. Shaheen, M. Tawfik, A. Mortadda, M. Seleem, M. S. I. Aly, G. Kazamel, M. Elbadry, S. Kamal, M. Hassan, M. Mostafa, M. E. S. Medhat, Ekhlas, R. Ghaleb, M. O. Taha, I. Daoud, H. Al Din, A. M. Imam, M. A. El Hameed, Helmy, M. Al-Murayeh, N. Akhtar, B. M. Matto, M. A. Ghani, O. A. Amoudi, M. M. Morsy, A. A. F. Bashir, Y. M. Al Hossni, B. Al Ghamdi, Zia-ul-Sabah, S. Mir, D. Dardir, A. Masswary, A. R. Al Shehri, A. Masswary, J. Iqbal, M. A. J. Almansori, C. G. Venkitachalam, J. Kurian, J. Rao, A. Aisheh, A. A. Albawab, B. Subbaraman, A. Amanat, K. J. Esfehani, R. Lochan, A. Bin Brek, B. Mittal, Y. Ghazi, M. Krishna, S. B. Tabatabaei, P. S. Thoppil, S. Nasim, S. El Khider Nour, P. Barros, A. P. Almeida, M. Andrade, B. Garbelini, Jr, T. L. Silvestrini, Á. R. Alves Junior, C. E. B. de Lima, A. Kormann, G. G. de Lima, C. Halperin, D. Salvadori Junior, A. F. Freitas, Jr, J. R. Gemelli, C. E. Ornelas, J. M. M. Dantas, J. L. Aziz, L. M. Backes, W. S. Barroso, M. S. Paiva, J. A. de Figueiredo Neto, F. R. dos Santos, J. A. de Lima Neto, R. Bergo, P. R. Salvador Junior, A. G. López, J. C. P. Alva, M. A. A. Gamba, F. G. Padilla-Padilla, A. E. B. Ruiz, J. Berlingieri, A. Bakbak, M. Gupta, K. Saunders, A. Costa-Vitali, P. R. Beaudry, R. Bhargava, Y. Khaykin, J. S. Healey, E. Crystal, Nadeau, Dhillon, Alistair Begg, C. Anderson, S. Baveja, D. Cross, A. Catanchin, D. Brieger, K. T. Lim, P. Davidson, R. Tan, R. Bhindi, J. Hickey, J. Layland, M. Bloch, C. Itty, B. Singh, P. Carroll, A. Lee, G. Starmer, and R. Lehman
References
- 1.Franken RA, Rosa RF, Santos SC. Atrial fibrillation in the elderly. J Geriatr Cardiol. 2012;9(2):91–100. doi: 10.3724/SP.J.1263.2011.12293. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Ezekowitz MD. Atrial fibrillation: the epidemic of the new millennium. Ann Intern Med. 1999;131(7):537–538. doi: 10.7326/0003-4819-131-7-199910050-00011. [DOI] [PubMed] [Google Scholar]
- 3.Ruff CT, Giugliano RP, Braunwald E, Hoffman EB, Deenadayalu N, Ezekowitz MD, et al. Comparison of the efficacy and safety of new oral anticoagulants with warfarin in patients with atrial fibrillation: a meta-analysis of randomised trials. Lancet. 2014;383(9921):955–962. doi: 10.1016/S0140-6736(13)62343-0. [DOI] [PubMed] [Google Scholar]
- 4.Beyer-Westendorf J, Ebertz F, Forster K, Gelbricht V, Michalski F, Kohler C, et al. Effectiveness and safety of dabigatran therapy in daily-care patients with atrial fibrillation. Results from the Dresden NOAC registry. Thromb Haemost. 2015;113(6):1247–1257. doi: 10.1160/TH14-11-0954. [DOI] [PubMed] [Google Scholar]
- 5.Helmert S, Marten S, Mizera H, Reitter A, Sahin K, Tittl L, et al. Effectiveness and safety of apixaban therapy in daily-care patients with atrial fibrillation: results from the Dresden NOAC registry. J Thromb Thrombolysis. 2017;44(2):169–178. doi: 10.1007/s11239-017-1519-8. [DOI] [PubMed] [Google Scholar]
- 6.Patel P, Pandya J, Goldberg M. NOACs vs. Warfarin for stroke prevention in nonvalvular atrial fibrillation. Cureus. 2017;9(6):e1395. doi: 10.7759/cureus.1395. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Camm AJ, Accetta G, Ambrosio G, Atar D, Bassand JP, Berge E, et al. Evolving antithrombotic treatment patterns for patients with newly diagnosed atrial fibrillation. Heart. 2017;103(4):307–314. doi: 10.1136/heartjnl-2016-309832. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Steinberg BA, Gao H, Shrader P, Pieper K, Thomas L, Camm AJ, et al. International trends in clinical characteristics and oral anticoagulation treatment for patients with atrial fibrillation: results from the GARFIELD-AF, ORBIT-AF I, and ORBIT-AF II registries. Am Heart J. 2017;194:132–140. doi: 10.1016/j.ahj.2017.08.011. [DOI] [PubMed] [Google Scholar]
- 9.Huisman MV, Rothman KJ, Paquette M, Teutsch C, Diener HC, Dubner SJ, et al. The changing landscape for stroke prevention in AF: findings from the GLORIA-AF registry phase 2. J Am Coll Cardiol. 2017;69(7):777–785. doi: 10.1016/j.jacc.2016.11.061. [DOI] [PubMed] [Google Scholar]
- 10.Huisman MV, Lip GY, Diener HC, Dubner SJ, Halperin JL, Ma CS, et al. Design and rationale of global registry on long-term Oral antithrombotic treatment in patients with atrial fibrillation: a global registry program on long-term oral antithrombotic treatment in patients with atrial fibrillation. Am Heart J. 2014;167(3):329–334. doi: 10.1016/j.ahj.2013.12.006. [DOI] [PubMed] [Google Scholar]
- 11.Camm AJ, Amarenco P, Haas S, Hess S, Kirchhof P, Kuhls S, et al. XANTUS: a real-world, prospective, observational study of patients treated with rivaroxaban for stroke prevention in atrial fibrillation. Eur Heart J. 2016;37(14):1145–1153. doi: 10.1093/eurheartj/ehv466. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Shimokawa H, Yamashita T, Uchiyama S, Kitazono T, Shimizu W, Ikeda T, et al. The EXPAND study: efficacy and safety of rivaroxaban in Japanese patients with non-valvular atrial fibrillation. Int J Cardiol. 2018;258:126–132. doi: 10.1016/j.ijcard.2018.01.141. [DOI] [PubMed] [Google Scholar]
- 13.Ikeda T, Atarashi H, Inoue H, Uchiyama S, Kitazono T, Yamashita T, et al. Study design and baseline characteristics of the EXPAND study: evaluation of effectiveness and safety of Xa inhibitor, rivaroxaban for the prevention of stroke and systemic embolism in a Nationwide cohort of Japanese patients diagnosed as non-Valvular atrial fibrillation. Tohoku J Exp Med. 2016;240(4):259–268. doi: 10.1620/tjem.240.259. [DOI] [PubMed] [Google Scholar]
- 14.Fox KAA, Gersh BJ, Traore S, Camm AJ, Kayani G, Krogh A, et al. Evolving quality standards for large-scale registries: the GARFIELD-AF experience. Eur Heart J Qual Care Clin Outcomes. 2017;3:114–122. doi: 10.1093/ehjqcco/qcx024. [DOI] [PubMed] [Google Scholar]
- 15.Camm AJ, Amarenco P, Haas S, Hess S, Kirchhof P, van Eickels M, et al. XANTUS: rationale and design of a noninterventional study of rivaroxaban for the prevention of stroke in patients with atrial fibrillation. Vasc Health Risk Manag. 2014;10:425–434. doi: 10.2147/VHRM.S63298. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Ogawa S, Minematsu K, Ikeda T, Kitazono T, Nakagawara J, Miyamoto S, et al. Design and baseline characteristics of the xarelto post-authorization safety & effectiveness study in Japanese patients with atrial fibrillation (XAPASS). J Arrhythm. 2018;34(2):167–175. [DOI] [PMC free article] [PubMed]
- 17.Kakkar AK, Mueller I, Bassand JP, Fitzmaurice DA, Goldhaber SZ, Goto S, et al. International longitudinal registry of patients with atrial fibrillation at risk of stroke: global anticoagulant registry in the FIELD (GARFIELD) Am Heart J. 2012;163(1):13–9.e1. doi: 10.1016/j.ahj.2011.09.011. [DOI] [PubMed] [Google Scholar]
- 18.Piccini JP, Fraulo ES, Ansell JE, Fonarow GC, Gersh BJ, Go AS, et al. Outcomes registry for better informed treatment of atrial fibrillation: rationale and design of ORBIT-AF. Am Heart J. 2011;162(4):606–12.e1. doi: 10.1016/j.ahj.2011.07.001. [DOI] [PubMed] [Google Scholar]
- 19.Steinberg BA, Blanco RG, Ollis D, Kim S, Holmes DN, Kowey PR, et al. Outcomes registry for better informed treatment of atrial fibrillation II: rationale and design of the ORBIT-AF II registry. Am Heart J. 2014;168(2):160–167. doi: 10.1016/j.ahj.2014.04.005. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.Steinberg BA, Shrader P, Thomas L, Ansell J, Fonarow GC, Gersh BJ, et al. Off-label dosing of non-vitamin K antagonist Oral anticoagulants and adverse outcomes: the ORBIT-AF II registry. J Am Coll Cardiol. 2016;68(24):2597–2604. doi: 10.1016/j.jacc.2016.09.966. [DOI] [PubMed] [Google Scholar]
- 21.Kaufman BG, Kim S, Pieper K, Allen LA, Gersh BJ, Naccarelli GV, et al. Disease understanding in patients newly diagnosed with atrial fibrillation. Heart. 2018;104(6):494–501. doi: 10.1136/heartjnl-2017-311800. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 22.Mazurek M, Huisman MV, Rothman KJ, Paquette M, Teutsch C, Diener HC, et al. Gender differences in antithrombotic treatment for newly diagnosed atrial fibrillation: the GLORIA-AF registry program. Am J Med. 2018;131(8):945–55.e3. doi: 10.1016/j.amjmed.2018.03.024. [DOI] [PubMed] [Google Scholar]
- 23.Huisman MV, Rothman KJ, Paquette M, Teutsch C, Diener HC, Dubner SJ, et al. Two-year follow-up of patients treated with dabigatran for stroke prevention in atrial fibrillation: global registry on long-term antithrombotic treatment in patients with atrial fibrillation (GLORIA-AF) registry. Am Heart J. 2018;198:55–63. doi: 10.1016/j.ahj.2017.08.018. [DOI] [PubMed] [Google Scholar]
- 24.McIntyre WF, Conen D, Olshansky B, Halperin JL, Hayek E, Huisman MV, et al. Stroke-prevention strategies in north American patients with atrial fibrillation: the GLORIA-AF registry program. Clin Cardiol. 2018;41(6):744–751. doi: 10.1002/clc.22936. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25.Huisman MV, Ma CS, Diener HC, Dubner SJ, Halperin JL, Rothman KJ, et al. Antithrombotic therapy use in patients with atrial fibrillation before the era of non-vitamin K antagonist Oral anticoagulants: the global registry on long-term oral antithrombotic treatment in patients with atrial fibrillation (GLORIA-AF) phase I cohort. Europace. 2016;18(9):1308–1318. doi: 10.1093/europace/euw073. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26.Mazurek M, Huisman MV, Rothman KJ, Paquette M, Teutsch C, Diener HC, et al. Regional differences in antithrombotic treatment for atrial fibrillation: insights from the GLORIA-AF phase II registry. Thromb Haemost. 2017;117(12):2376–2388. doi: 10.1160/TH17-08-0555. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 27.Hecker J, Marten S, Keller L, Helmert S, Michalski F, Werth S, et al. Effectiveness and safety of rivaroxaban therapy in daily-care patients with atrial fibrillation. Results from the Dresden NOAC registry. Thromb Haemost. 2016;115(5):939–949. doi: 10.1160/TH15-10-0840. [DOI] [PubMed] [Google Scholar]
- 28.Anderson TS, Lo-Ciganic WH, Gellad WF, Zhang R, Huskamp HA, Choudhry NK, et al. Patterns and predictors of physician adoption of new cardiovascular drugs. Healthc (Amst) 2018;6(1):33–40. doi: 10.1016/j.hjdsi.2017.09.004. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 29.Loo SY, Dell'Aniello S, Huiart L, Renoux C. Trends in the prescription of novel oral anticoagulants in UK primary care. Br J Clin Pharmacol. 2017;83(9):2096–2106. doi: 10.1111/bcp.13299. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 30.Lubloy A. Factors affecting the uptake of new medicines: a systematic literature review. BMC Health Serv Res. 2014;14:469. doi: 10.1186/1472-6963-14-469. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 31.Connolly SJ, Ezekowitz MD, Yusuf S, Eikelboom J, Oldgren J, Parekh A, et al. Dabigatran versus warfarin in patients with atrial fibrillation. N Engl J Med. 2009;361(12):1139–1151. doi: 10.1056/NEJMoa0905561. [DOI] [PubMed] [Google Scholar]
- 32.Granger CB, Alexander JH, McMurray JJ, Lopes RD, Hylek EM, Hanna M, et al. Apixaban versus warfarin in patients with atrial fibrillation. N Engl J Med. 2011;365(11):981–992. doi: 10.1056/NEJMoa1107039. [DOI] [PubMed] [Google Scholar]
- 33.JCS Joint Working Group Guidelines for pharmacotherapy of atrial fibrillation (JCS 2013) Circ J. 2014;78(8):1997–2021. doi: 10.1253/circj.CJ-66-0092. [DOI] [PubMed] [Google Scholar]
- 34.Fox KAA, Accetta G, Pieper KS, Bassand JP, Camm AJ, Fitzmaurice DA, et al. Why are outcomes different for registry patients enrolled prospectively and retrospectively? Insights from the global anticoagulant registry in the FIELD-atrial fibrillation (GARFIELD-AF) Eur Heart J Qual Care Clin Outcomes. 2018;4(1):27–35. doi: 10.1093/ehjqcco/qcx030. [DOI] [PubMed] [Google Scholar]
- 35.Chan YH, See LC, Tu HT, Yeh YH, Chang SH, Wu LS, et al. Efficacy and safety of apixaban, dabigatran, rivaroxaban, and warfarin in Asians with nonvalvular atrial fibrillation. J Am Heart Assoc. 2018;7(8). 10.1161/JAHA.117.008150. [DOI] [PMC free article] [PubMed]
- 36.Lip GYH, Pan X, Kamble S, Kawabata H, Mardekian J, Masseria C, et al. Discontinuation risk comparison among ‘real-world’ newly anticoagulated atrial fibrillation patients: Apixaban, warfarin, dabigatran, or rivaroxaban. PLoS One. 2018;13(4):e0195950. doi: 10.1371/journal.pone.0195950. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 37.Lip GY, Pan X, Kamble S, Kawabata H, Mardekian J, Masseria C, et al. Major bleeding risk among non-valvular atrial fibrillation patients initiated on apixaban, dabigatran, rivaroxaban or warfarin: a “real-world” observational study in the United States. Int J Clin Pract. 2016;70(9):752–763. doi: 10.1111/ijcp.12863. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 38.Nielsen PB, Skjoth F, Sogaard M, Kjaeldgaard JN, Lip GY, Larsen TB. Effectiveness and safety of reduced dose non-vitamin K antagonist oral anticoagulants and warfarin in patients with atrial fibrillation: propensity weighted nationwide cohort study. BMJ. 2017;356:j510. doi: 10.1136/bmj.j510. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 39.Beyer-Westendorf J, Gelbricht V, Forster K, Ebertz F, Kohler C, Werth S, et al. Peri-interventional management of novel oral anticoagulants in daily care: results from the prospective Dresden NOAC registry. Eur Heart J. 2014;35(28):1888–1896. doi: 10.1093/eurheartj/eht557. [DOI] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Supplementary Materials
Table S1. Evaluations performed at Baseline and at Follow-Up Visits. Table S2. Study design of ongoing real-world studies of rivaroxaban. Table S3. Comparison of distribution of baseline CHADS2, CHA2DS2-VASc or HAS-BLED scores of patients from observational RIVER, XANTUS, EXPAND and XAPASS studies. (DOC 155 kb)
Data Availability Statement
No additional data is available.