Abstract
Background
The purpose of low‐vision rehabilitation is to allow people to resume or to continue to perform daily living tasks, with reading being one of the most important. This is achieved by providing appropriate optical devices and special training in the use of residual‐vision and low‐vision aids, which range from simple optical magnifiers to high‐magnification video magnifiers.
Objectives
To assess the effects of different visual reading aids for adults with low vision.
Search methods
We searched the Cochrane Central Register of Controlled Trials (CENTRAL) (which contains the Cochrane Eyes and Vision Trials Register) (2017, Issue 12); MEDLINE Ovid; Embase Ovid; BIREME LILACS, OpenGrey, the ISRCTN registry; ClinicalTrials.gov and the World Health Organization (WHO) International Clinical Trials Registry Platform (ICTRP). The date of the search was 17 January 2018.
Selection criteria
This review includes randomised and quasi‐randomised trials that compared any device or aid used for reading to another device or aid in people aged 16 or over with low vision as defined by the study investigators. We did not compare low‐vision aids with no low‐vision aid since it is obviously not possible to measure reading speed, our primary outcome, in people that cannot read ordinary print. We considered reading aids that maximise the person's visual reading capacity, for example by increasing image magnification (optical and electronic magnifiers), augmenting text contrast (coloured filters) or trying to optimise the viewing angle or gaze position (such as prisms). We have not included studies investigating reading aids that allow reading through hearing, such as talking books or screen readers, or through touch, such as Braille‐based devices and we did not consider rehabilitation strategies or complex low‐vision interventions.
Data collection and analysis
We used standard methods expected by Cochrane. At least two authors independently assessed trial quality and extracted data. The primary outcome of the review was reading speed in words per minute. Secondary outcomes included reading duration and acuity, ease and frequency of use, quality of life and adverse outcomes. We graded the certainty of the evidence using GRADE.
Main results
We included 11 small studies with a cross‐over design (435 people overall), one study with two parallel arms (37 participants) and one study with three parallel arms (243 participants). These studies took place in the USA (7 studies), the UK (5 studies) and Canada (1 study). Age‐related macular degeneration (AMD) was the most frequent cause of low vision, with 10 studies reporting 50% or more participants with the condition. Participants were aged 9 to 97 years in these studies, but most were older (the median average age across studies was 71 years). None of the studies were masked; otherwise we largely judged the studies to be at low risk of bias. All studies reported the primary outcome: results for reading speed. None of the studies measured or reported adverse outcomes.
Reading speed may be higher with stand‐mounted closed circuit television (CCTV) than with optical devices (stand or hand magnifiers) (low‐certainty evidence, 2 studies, 92 participants). There was moderate‐certainty evidence that reading duration was longer with the electronic devices and that they were easier to use. Similar results were seen for electronic devices with the camera mounted in a 'mouse'. Mixed results were seen for head‐mounted devices with one study of 70 participants finding a mouse‐based head‐mounted device to be better than an optical device and another study of 20 participants finding optical devices better (low‐certainty evidence). Low‐certainty evidence from three studies (93 participants) suggested no important differences in reading speed, acuity or ease of use between stand‐mounted and head‐mounted electronic devices. Similarly, low‐certainty evidence from one study of 100 participants suggested no important differences between a 9.7'' tablet computer and stand‐mounted CCTV in reading speed, with imprecise estimates (other outcomes not reported).
Low‐certainty evidence showed little difference in reading speed in one study with 100 participants that added electronic portable devices to preferred optical devices. One parallel‐arm study in 37 participants found low‐certainty evidence of higher reading speed at one month if participants received a CCTV at the initial rehabilitation consultation instead of a standard low‐vision aids prescription alone.
A parallel‐arm study including 243 participants with AMD found no important differences in reading speed, reading acuity and quality of life between prism spectacles and conventional spectacles. One study in 10 people with AMD found that reading speed with several overlay coloured filters was no better and possibly worse than with a clear filter (low‐certainty evidence, other outcomes not reported).
Authors' conclusions
There is insufficient evidence supporting the use of a specific type of electronic or optical device for the most common profiles of low‐vision aid users. However, there is some evidence that stand‐mounted electronic devices may improve reading speeds compared with optical devices. There is less evidence to support the use of head‐mounted or portable electronic devices; however, the technology of electronic devices may have improved since the studies included in this review took place, and modern portable electronic devices have desirable properties such as flexible use of magnification. There is no good evidence to support the use of filters or prism spectacles. Future research should focus on assessing sustained long‐term use of each device and the effect of different training programmes on its use, combined with investigation of which patient characteristics predict performance with different devices, including some of the more costly electronic devices.
Plain language summary
Reading aids for adults with low vision
What is the aim of this review? The aim of this Cochrane Review was to compare different reading aids for people with low vision. Cochrane Review authors collected and analysed all relevant studies to answer this question and found 13 studies.
Key messages There is insufficient evidence supporting the use of a specific type of electronic or optical reading aid. The review suggests that reading speeds improve with the use of stand‐mounted electronic devices. There is little evidence for a difference between head‐mounted or portable electronic devices versus optical or other electronic devices, although technology may have improved since these studies took place. There is no evidence to support the use of filters or prism spectacles.
What was studied in the review? The number of people with low vision is increasing with the ageing population. Magnifying optical and electronic aids are commonly prescribed to help people maintain the ability to read when their vision starts to fade. Cochrane authors reviewed the evidence for the effect of reading aids on reading ability in people with low vision to find out whether there are differences in reading performance using conventional optical devices, such as hand‐held or stand‐based microscopic magnifiers, as compared to electronic devices such as stand‐based, closed circuit television and hand‐held electronic magnifiers.
Cochrane Review authors assessed how certain the evidence was for each review finding. They looked for factors that can make the evidence less certain, such as problems with the way the studies were done, very small studies, and inconsistent findings across studies. They also looked for factors that can make the evidence more certain, including very large effects. They graded each finding as being of very low, low, moderate or high certainty.
What are the main results of the review? Cochrane Review authors found 13 relevant studies. Seven were from the USA, five from the UK and one from Canada. These studies compared the effect of different reading aids on reading performance, mainly reading speed. The participants were adults attending low vision services. Most of the people were affected by macular degeneration, which causes of loss of central vision and is often age‐related. Because most of the studies were small, the results were often imprecise, and it is difficult to know whether they apply to everyone with low vision.
The results were as follows.
• Reading speed may be faster with electronic devices than with optical magnifiers (moderate‐ and low‐certainty evidence). • Provision of a closed circuit television (CCTV) at an initial rehabilitation consultation may increase reading speeds compared with standard low‐vision aids prescription alone (low‐certainty evidence). • Reading speed with head‐mounted electronic devices showed inconsistent differences compared to optical devices (moderate or low‐certainty evidence). • Reading speeds with a tablet computer compared with stand‐mounted CCTV were similar (low‐certainty evidence). • Addition of an electronic portable device to a preferred optical device did not appear to increase reading speed (low‐certainty evidence). • Coloured filters were no better and possibly worse than a clear filter for reading speed (low‐certainty evidence). • Custom or standard prism spectacles did not appear to convey additional benefit compared with conventional reading spectacles for people with age‐related macular degeneration (low‐certainty evidence).
How up‐to‐date is this review? Cochrane Review authors searched for studies that had been published up to 17 January 2018.
Summary of findings
Background
Description of the condition
There is no single, globally accepted definition of low vision (also known as partial sight, visual impairment and subnormal vision). However, there is general consensus that low vision is an uncorrectable loss of vision that interferes with daily activities. Definitions normally incorporate an estimate of visual loss in terms of impairment (e.g. measuring visual acuity or visual fields), or in terms of disability (measuring the ability to perform a certain task). One such definition states that low vision is the inability to read a newspaper at a normal reading distance (40 cm) with best refractive correction (Legge 1991).
The World Health Organization (WHO) has established criteria for low vision that are used in the International Classification of Diseases (WHO 2010). Low vision is defined as a best‐corrected visual acuity worse than 0.5 logMAR (Snellen 6/18 or 20/60) but equal to or better than 1.3 logMAR (3/60 or 20/400) in the better eye, or visual field loss corresponding to less than 20° in the better eye with best possible correction. Blindness is defined as a best‐corrected visual acuity worse than 1.3 logMAR or a visual field no greater than 10° around central fixation in the better eye with best possible correction. Visual impairment includes low vision as well as blindness. In the USA, legal blindness is defined as a visual acuity of 1.0 logMAR (6/60 or 20/200) or worse in the better eye.
Blindness is one of the most common disabilities (Congdon 2003): an estimated 39 million people were blind a decade ago, i.e. at the time of the last accurate assessment (Pascolini 2011). Among people older than 40 years in the USA, 937,000 were blind in 2002. Prevalence of blindness in the developing world (where 90% of total world blindness exists) and for the developed world is expected to increase significantly during the next decades as the world's population ages.
Causes of blindness are associated with race and ethnicity in the USA (Congdon 2004): age‐related macular degeneration (AMD) is the most common cause in white people, whereas cataract, glaucoma and diabetic retinopathy are the leading causes in Latinos and African Americans. Different treatable or preventable conditions are the most frequent causes of blindness in developing countries: infectious disease, nutritional causes, and especially cataract and refractive error (Congdon 2003; Pascolini 2011).
In industrialised countries, low vision is found principally in people aged 75 years or older (Margrain 1999; Tielsch 1990), and it has been ranked third (behind arthritis and heart disease) among conditions that cause people older than 70 years to need assistance in activities of daily living (Scott 1999). The ageing population, combined with the dramatic increase in visual impairment in the older age groups, explains the significant increase seen in the demand for low‐vision services.
Description of the intervention
The purpose of low‐vision rehabilitation is to allow the person to resume or to continue to perform daily living tasks. This is achieved by providing appropriate optical devices, environmental modifications and special training in the use of residual‐vision and low‐vision aids (Massof 1998). Without rehabilitation, people with decreased visual acuity often abandon reading and other tasks requiring detailed vision. For individuals with extensive loss of their visual field, orientation and mobility can become difficult.
For a person with low vision, reading is considered one of the most important tasks or goals to achieve (Leat 1994; Shuttleworth 1995). People using low‐vision aids have reported improvements in reading a specific letter size both during distance and near work, and they have found optical aids useful to perform tasks (Humphry 1986; Nilsson 1990; Virtanen 1991). A low‐vision aid (LVA) is any device that enables a person with low vision to improve visual performance.
Common optical LVAs include:
magnifiers – these sometimes have their own illumination and are either battery‐powered or rechargeable from mains electricity. They may be hand‐held or mounted on a stand or on spectacles;
telescopes – for work where the reading matter is distant, a telescope can be mounted on a spectacle frame. This gives a longer working distance, although less can be seen at one time because the field is necessarily restricted. Telescopes may also be hand‐held.
Electronic aids include primarily closed circuit television and other readers incorporating a monitor or a liquid‐crystal display (LCD) screen, which provide improved contrast and magnification.
How the intervention might work
Like many types of rehabilitation, low‐vision rehabilitation includes heterogeneous interventions, which may have several components. Moreover, people who are prescribed a low‐vision device usually receive training to use it. Several training techniques are employed, often using both office‐ and home‐based exercises with the device for a few hours in different sessions. Overall, multidisciplinary services tend to provide modern rehabilitation services (Langelaan 2007). Besides prescription of LVAs and training on their use, especially focused on reading tasks, services can provide psychological support, home environmental assessment, and – for people of working age – social worker support. Moreover, several types of professionals provide different types of follow‐up either in low‐vision clinics or at home.
As was intended, this review concentrates on reading aids that magnify text, sometimes also improving its contrast.
Why it is important to do this review
The most suitable device depends on the person's needs and the visual functioning they have. Rehabilitation should be tailored to correspond to the type of visual loss and may also be modified by the individual's choice or expectations or by more general cultural demands (Dickinson 1998; Margrain 1999). Besides the level of magnification, there are other factors that are important when choosing an optical device, such as ease of use and cosmetic appearance. Devices may be rejected if they have an unusual cosmetic appearance that calls attention to the person's disability.
Reading is an extremely complex visual task, which involves the integration of visual, cognitive and motor processes. In everyday reading, it is important for people to achieve their optimal reading rate (usually measured in words per minute), and, for people with low vision, a speed that is sufficient to complete the task within an acceptable amount of time. The effect of slow reading on comprehension is variable, as Dickinson 1998 found that low reading speed decreases comprehension but Legge 1989 did not.
Given the availability of a wide range of aids from simple magnifiers to high‐power video magnifiers, all of which have advantages and disadvantages, an assessment of their effects on reading would be very useful.
Objectives
To assess the effects of different visual reading aids for adults with low vision.
Methods
Criteria for considering studies for this review
Types of studies
We included randomised and quasi‐randomised trials.
Types of participants
We included trials in participants aged 16 or over with low vision as defined by the study investigators. Where possible we grouped participants according to the type or cause of visual impairment. We included studies that enrolled people aged younger than 16 provided most participants were over that age.
Types of interventions
We included trials comparing any device or aid used for reading visually versus another device or aid. We considered reading aids that maximise the person's visual reading capacity, including non‐electronic aids, that is, optical devices such as magnifiers and telescopes, and electronic aids, such as several types of closed circuit television (CCTV). These devices are rated in terms of the equivalent power measured in dioptres, which allows comparison of devices to each other (Sloan 1971). We also considered consumer electronics such as smartphones and tablets.
We also considered other LVAs such as coloured filters and optical prisms, which are commonly prescribed in low‐vision rehabilitation as they are supposed to improve reading in some people.
We excluded trials in which the intervention is a device to read though hearing, such as screen readers or talking books, or through touch, such as Braille‐based devices and haptic devices. Finally, we did not consider rehabilitation strategies or complex low‐vision interventions.
Types of outcome measures
Using World Health Organization (WHO) language on functioning, disability and health (WHO 2002), maximum reading speed and reading acuity is the person's capacity under ideal conditions of text magnification and contrast, such as when using the Minnesota Low‐Vision Reading test (MNREAD). Capacity may be partly an individual trait (slow or fast reader) and can be limited by several visually and non‐visually impairing diseases. Vision‐based reading aids aim at maximising the person's performance by compensating their diminished visual function, especially by magnification. The choice of outcome measures in this review is driven by its emphasis on the vision‐related component of performance.
Research on psychophysics of reading has shown that reading speed is typically stable across a range of print sizes (maximum reading speed) that are larger than a certain threshold (critical print size), whereas at smaller print sizes, below the critical print size, the reading speed slows, and the reading acuity limit is reached (Ahn 1995a; Ahn 1995b; Legge 1985a; Legge 2007). Font size at critical print size is usually two or three times larger than reading acuity. A similar pattern is also present in most people with low vision (Legge 1985b; Legge 2007). A plot of reading speed against font size (adjusted by reading distance and expressed in logMAR) can be obtained using reading charts such as the MNREAD charts (Legge 2007). The updated version of this review adopts the following definitions developed by the authors of the MNREAD charts (Ahn 1995a).
Reading acuity: the smallest print that the person can read without making significant errors.
Critical print size: the smallest print that the person can read with maximum speed.
Maximum reading speed: the person's reading speed when reading is not limited by print size, i.e. for print size larger than the critical print size.
Rubin 2013 reviewed the issue of measuring reading performance in LVA research, finding that the methods for assessing reading performance and the algorithms for scoring reading tests need to be optimised to improve the reliability and responsiveness of reading tests. A systematic review on effectiveness of low vision service provision also affords a broader perspective on outcome measures, including quality of life measures (Binns 2012).
Primary outcomes
Reading speed in words per minute, recorded using typical font size (i.e. approximately 10 to 14 points), in books or newspapers.
We also accepted maximum reading speed recorded across a range of point sizes, using MNREAD or Bailey‐Lovie charts. However, it may be unclear, unless specified, whether maximum reading speed is achieved for common book text size with each reading aid. Thus, we rated studies reporting only maximum reading speed as providing indirect evidence regarding the primary outcome of this review.
Secondary outcomes
Reading duration in minutes, defined as the time the person could read without visual discomfort causing the need to take a pause.
Reading acuity in logMAR. Because this is mostly a function of magnification, we analyse this outcome only if devices are matched by magnification (e.g. a difference between unmatched electronic and optical aids needs no demonstration).
Ease and frequency of use as reported by the participants.
Quality of life as measured by any validated scale that aims to measure the impact of visual function loss on quality of life.
Reported adverse outcomes.
Search methods for identification of studies
Electronic searches
The Cochrane Eyes and Vision Information Specialist conducted systematic searches in the following databases for randomised controlled trials and controlled clinical trials. There were no language or publication year restrictions. The date of the search was 17 January 2018.
Cochrane Central Register of Controlled Trials (CENTRAL; 2017, Issue 12) (which contains the Cochrane Eyes and Vision Trials Register) in the Cochrane Library (searched 17 January 2018) (Appendix 1).
MEDLINE Ovid (1946 to 17 January 2018) (Appendix 2).
Embase Ovid (1980 to 17 January 2018) (Appendix 3).
LILACS (1982 to 17 January 2018) (Appendix 4).
OpenGrey (System for Information on Grey Literature in Europe) (www.opengrey.eu; searched 17 January 2018) (Appendix 5).
ISRCTN registry (www.isrctn.com/editAdvancedSearch; searched 17 January 2018) (Appendix 6).
US National Institutes of Health Ongoing Trials Register ClinicalTrials.gov (www.clinicaltrials.gov; searched 17 January 2018) (Appendix 7).
World Health Organization (WHO) International Clinical Trials Registry Platform (ICTRP) (www.who.int/ictrp; searched 17 January 2018) (Appendix 8).
Searching other resources
We handsearched the British Journal of Visual Impairment from 1983 to 1999 and the Journal of Visual Impairment and Blindness from 1976 to 1991 for relevant trials. We searched the reference lists of relevant articles to find additional trials. We used the Science Citation Index to find articles that cited relevant articles. We contacted investigators and manufacturers of low‐vision aids to identify other published and unpublished reports.
Data collection and analysis
Selection of studies
Two authors working independently assessed the titles and abstracts resulting from the electronic searches. We obtained the full copy of all relevant or potentially relevant trials and assessed these according to the 'Criteria for considering studies for this review'. We assessed only trials meeting these criteria for methodological quality. The authors were not masked to any trial details when making their assessments. We resolved disagreements about whether a trial should be included by discussion and consensus. We attempted to obtain additional information where necessary.
Data extraction and management
Two authors working independently extracted data using Covidence, resolving any discrepancies by discussion. We contacted investigators to obtain missing data where necessary.
For three studies, individual data were reported in tables of the publication. We used these for further analyses.
Assessment of risk of bias in included studies
Two authors working independently assessed risk of bias according to the methods set out in Chapters 8 and 10 of the Cochrane Handbook for Systematic Reviews of Interventions (Higgins 2011a; Sterne 2011). We considered the following parameters: method of allocation to treatment; allocation concealment (selection bias); documentation of exclusions and completeness of follow‐up (attrition bias); selective outcome reporting (reporting bias). We did not consider masking of participants, study personnel (performance bias) and outcome assessors (detection bias) since it is not possible with most LVAs. Moreover, masking is meaningless for some outcomes, such as participant's preference for each device. We graded each parameter of trial quality as being at low, high or unclear risk of bias. We contacted study authors for clarification on any item graded as unclear. Authors were not masked to any trial details during the assessment.
Evaluation of cross‐over‐like studies was an issue in this review. Assessing the performance of the same participant who tries different LVAs is a common study design used by researchers into low vision, which is also known as a 'within‐person' design. This is an efficient design since we do not need to allow for all variations that occur between arms of parallel‐group studies. In practice this means that, for the same number of participants, a cross‐over design is likely to be more powerful. However, cross‐over trials are not always appropriate. The most important consideration is whether the participants start the second period in a similar state as how they started the first period. If the characteristics of the participant have changed in some way by the time the second period starts, then the comparison of treatments is not fair, and there will be within‐participant variation. Based on the Cochrane Collaboration's Open Learning Additional Module 2, (Alderson 2002) and on Chapter 16 of the Cochrane Handbook for Systematic Reviews of Interventions (Higgins 2011b), we addressed the following questions for cross‐over studies.
Is the condition of the participants chronic and stable?
Does the intervention provide temporary relief, and not permanent change?
Can the outcome be repeated in the second period if it occurs in the first?
Might the effect of the first intervention last into the second treatment period?
Does the trial go on long enough for the LVA to be properly used?
Assessment of randomisation procedures requires consideration of two components: sequence generation and allocation concealment. A discussion among the authors led to grading both components in cross‐over‐like studies included in this review as being at low risk of bias. In fact, in low‐vision studies adopting a cross‐over‐like design in this review, all participants used all devices and the order of presentation was randomised. We judged it necessary to address two questions when rating the quality of randomisation and allocation in this type of study.
Does knowledge of the first LVA selected affect recruitment into the trial?
Does the order in which the LVAs are used affect the results?
Regarding question 1, the answer should be no, since knowing the order of LVA presentation in the study should not affect recruitment into studies testing all devices in the same session. As to question 2, we considered two additional items: first, period effect (whether the condition can change during subsequent phases of testing of each device), and second, carry‐over effect or period‐by‐treatment interaction (whether the effect on performance of using a specific device affects the performance of the following device).
Measures of treatment effect
We obtained the mean difference (MD) and its standard error (SE), referred to as 'SE(MD)', when continuous data were available. We then used the generic inverse variance method when dealing with cross‐over studies (Higgins 2011b); see also Appendix 9 for details and additional methods used.
Unit of analysis issues
Participants, rather than eyes, are the unit of analysis in this review. We encountered specific unit of analysis issues in studies comparing several devices on the same participant, which we dealt with as described in other sections of this review and as shown in Appendix 9. We included studies measuring outcomes in the better eye but excluded studies adopting eyes rather than individuals as the unit of analysis.
Dealing with missing data
There were only two parallel‐arm trials in this review. We enumerate missing data for each treatment arm in these studies in the Characteristics of included studies table. The concept of missing data is more complex when several devices are tested on the same participant, since the participant may be able to read with some devices but not with others. These issues are related to study inclusion criteria and are discussed in the Results and Discussion sections.
Assessment of heterogeneity
We assessed heterogeneity considering the study characteristics (including type of intervention and participants). We inspected the forest plot to see the range of effects. We also considered the Chi² test for heterogeneity and the I² statistic (which gives an estimate of the extent to which the observed variation can be attributed to true variation rather than random error); these statistics may have low power with few studies (Deeks 2011b).
Assessment of reporting biases
We considered reporting biases only for reading speed as the primary outcome, since we found it difficult to consider other outcomes not reported in the absence of standard measurements tools, relative to the specific aim of this review.
Data synthesis
We conducted data analysis following guidance from Chapter 8 of the Cochrane Handbook for Systematic Reviews of Interventions (Deeks 2011b). We pooled data using a fixed‐effect model, as the number of studies contributing data to each analysis was three or fewer. Since a cross‐over design was common in research on the effectiveness of LVAs, we included these studies in the review provided that the order of presentation of the devices was randomised or quasi‐randomised and specific methods were used to deal with them. A number of minor statistical and data extraction issues arose from the inclusion of these cross‐over studies, e.g. methods to handle within‐person correlation and multiplicity of testing. Other items were small sample size issues, data skewness, and the availability of individual patient data in small studies. We dealt with these issues using methods suggested in Elbourne 2002 and in Chapter 16 of the Cochrane Handbook for Systematic Reviews of Interventions (Higgins 2011b), as summarised in Appendix 9.
Subgroup and sensitivity analyses
We did not do any subgroup or sensitivity analyses, as the number of studies was low for any analysis.
Summary of findings tables
We summarised the results in 'Summary of findings' tables as recommended in Chapter 11 of the Cochrane Handbook for Systematic Reviews of Interventions (Schünemann 2011). We graded the certainty of the evidence by consensus using the GRADE approach, which considers five parameters: imprecision, risk of bias, inconsistency, indirectness and publication bias (GRADEpro 2014).
Results
Description of studies
Results of the search
The electronic searches run in July 2006 yielded 488 reports. We screened the titles and abstracts and identified 20 studies that appeared relevant. We obtained full‐text copies of these reports and after further assessment, we included nine studies and excluded the remaining 11 studies.
An update search run in January 2013 yielded 528 references. The Trials Search Co‐ordinator removed 150 duplicates, scanned 378 references and removed 64 records that were not relevant to the scope of the review. We screened 314 references and obtained full‐text reports of eight studies, which we excluded after assessment. While this review was being updated, we retrieved studies in low‐vision research reported as conference abstracts. Currently we are unable to identify six full‐text reports of studies or make contact with the trialists. Relevant sections from the conference abstracts are shown in the Characteristics of studies awaiting classification. If we are able to collect sufficient data we will assess these studies for potential inclusion in further updates. In addition, handsearching references of other reports used for this review yielded two studies published in 2005, of which Watson 2005 is now included and Kaida 2005 is awaiting classification.
Updated searches conducted in January 2018 identified 1349 new records (Figure 1). After removing 345 duplicates, the Cochrane Information Specialist (CIS) screened the remaining 1004 records and removed 388 references that were not relevant to the scope of the review. We screened the remaining 616 records and obtained six full‐text reports and one conference abstract for further assessment. We excluded two studies (Alabdulkader 2012; Bailie 2013), and we identified five reports of three new studies (Jackson 2017; Morrice 2017; Taylor 2017); see Characteristics of included studies for details. We did not identify any ongoing studies from our searches of the clinical trials' registries.
1.

Study flow diagram.
Included studies
We included 13 studies in the review (see Characteristics of included studies). These studies took place in the USA (7 studies), UK (5 studies) and Canada (1 study). We provide summary descriptions for each, along with details of their 'Risk of bias' assessment, which is presented graphically in Figure 2. Interventions, outcome measures and their measurement tools were very variable and are summarised in Table 8.
2.

Risk of bias summary: review authors' judgements about each risk of bias item for each included study.
1. Interventions and outcomes in the included studies.
| Study | LVAs compared | RS measurement | Reading acuity | Reading duration | Subjective preference for specific devices | Quality of life | Other outcomes reported but not included in this review |
| Culham 2004 | 4 electronic head‐mounted versus participant's aids or spectacles | Small (N 5), typical medium (N1 0) and large (N 20) print size | Bailey‐Lovie charts | — | — | — | Reading accuracy, contrast sensitivity (Pelli Robson), daily living tasks: grocery identification (seconds), writing cheques (seconds) |
| Eperjesi 2004 | Coloured versus clear filter overlays | Rate of reading test (print size 4‐ to 18‐point) | Not available, but not relevant for filters which do not magnify text | — | — | — | — |
| Goodrich 2001 | Hand‐held CCTV, stand‐mounted CCTV versus prescribed optical aid | 1 M text (typical print size at 40 cm) | — | Cumulative time spent reading | Questions on subjective preference | — | Reading comprehension |
| Jackson 2017 | Standard visual rehabilitation, provision of a free CCTV | IReST | IReST | — | — | Rasch‐scaled IVI | — |
| Kleweno 2001 | Head‐mounted display versus standard CCTV | Next largest size close to near acuity (MNREAD electronic version) | MNREAD charts | — | Single question on preference in terms of brightness and clarity | — | Different contrast/colour condition for cathode ray tube or virtual retinal display |
| Morrice 2017 | CCTV, tablet | IReST | IReST | — | Frequency of device use on a 0‐4 scale. | — | — |
| Ortiz 1999 | Head‐mounted display (LVES) versus CCTV | News articles MNREAD |
MNREAD charts | — | — | — | Reading comprehension |
| Peterson 2003 | Head‐mounted display, hand‐held CCTV, standard CCTV versus the participant's optimum conventional optical magnifier | MNREAD reading speed across several print sizes available in figure | MNREAD‐like charts | — | Single question on subjective ease of use of each magnifier on a 5‐step scale | — | Ability to read specific print sizes (0.2‐1.0 logMAR); navigate a text, follow a route on a map, reading medicine bottle label |
| Spitzberg 1995 | Mirror, prism or zoom optical magnifiers versus conventional magnifier (same magnification) | 1M or 1.5M print (ordinary print size at 40 cm) | — | — | Preference for a specific device | — | Note: magnification was standardised at 3× for all devices |
| Smith 2005 | Custom or standard bilateral prism spectacles versus conventional spectacles | MNREAD reading speed "at the critical print size" | MNREAD charts | — | MLVQ measuring helpfulness and use | NEI‐VFQ 25, MLVAI | — |
| Stelmack 1991 | CCTV, illuminated stand magnifier, spectacles | Readers Digest (silent reading) | — | Reading time without visual discomfort | — | — | Reading comprehension |
| Taylor 2017 | Portable electronic devices, optical device in use | IReST, MNREAD | IReST, MNREAD | — | — | — | — |
| Watson 2005 | Hybrid‐diffractive spectacle magnifier compared with a refractive spectacle magnifier and an aplanatic spectacle magnifier (2 separate experiments) | MNREAD maximum RS with each reading aid; Pepper Visual skills for Reading Test | MNREAD charts | — | Self‐report of satisfaction with reading using a visual analogue scale | — | Reading accuracy, Morgan Low Vision reading Comprehension Assessment |
CCTV: closed circuit television;IReST: International Reading Speed Texts; IVI: Impact of Vision Impairment questionnaire NEI‐VFE: National Eye Institute Visual Functioning Questionnaire;MLVAI: Melbourne Low‐Vision ADL (Activities of Daily Living) Index; MLVQ: Manchester Low Vision Questionnaire; RS: reading speed.
Design
Eleven studies used a cross‐over design. This design is suitable for testing several aids in each participant during the same or in consecutive examination sessions. Studies using rotation of the order of presentation of devices could be considered quasi‐randomised (Goodrich 2001; Ortiz 1999; Spitzberg 1995), while randomisation methods were unclear in Watson 2005, and Morrice 2017 reported the adoption of a quasi‐randomised design. Nonetheless, they were scored as being at low risk of bias for reasons given in the Data collection and analysis section of this review. Jackson 2017 compared two parallel arms, and Smith 2005 used a three parallel‐arm randomised design.
Participants
All the participants recruited in the trials were from the low‐vision service where the trial was conducted. The number of participants randomised in the trials ranged from 10 to 243. Participants were aged 9 to 97 years in these studies, but most were elderly (median average age in the studies was 71 years). We accepted studies including children if most participants were adults. The percentage women (in studies that reported the gender of participants) ranged from 9% to 81% (median 59%).
Table A summarises the conditions causing visual loss in participants in these studies. AMD was the most frequent condition, with 10 studies reporting 50% or more participants with the condition.
Table A: Participants in included studies
| Study | Number of participants | Principal cause of low vision |
| Culham 2004 | 20 | AMD (n = 10), early onset macular disease (n = 10) |
| Eperjesi 2004 | 12 | AMD (n = 12) |
| Goodrich 2001 | 22 | AMD (n = 16), CRVO (n = 2), diabetic retinopathy (n = 2), macular hole (n = 1), cone dystrophy (1) |
| Jackson 2017 | 37 | AMD or juvenile onset macular degeneration (n = 27), optic nerve disease (n = 6), macular dystrophy or other maculopathy (n = 4) |
| Kleweno 2001 | 13 | Retinal (n = 7), optical (n = 3), amblyopic (n = 2), unknown (n = 1). No AMD cases |
| Morrice 2017 | 100 | AMD (n = 57), diabetic retinopathy (n = 6), glaucoma (n = 6), other (n = 25), unknown (n = 6) |
| Ortiz 1999 | 10 | Uveitis (n = 1), corneal opacity (n = 1), glaucoma (n = 1), optic neuritis (n = 1), macular degeneration (n = 2), other retinal diseases (n = 4) |
| Peterson 2003 | 70 | AMD (n = 40), vascular retinopathy (n = 11), diabetic retinopathy (n = 9), corneal condition (n = 6), glaucoma (n = 4) |
| Smith 2005 | 243 | AMD (n = 243) |
| Spitzberg 1995 | 39 | Not known |
| Stelmack 1991 | 37 | AMD or ocular histoplasmosis (n = 37) |
| Taylor 2017 | 82 | AMD (n = 47), Stargardt (n = 3), retinitis pigmentosa (n = 3) myopic degeneration (n = 5), glaucoma (n = 6), diabetic retinopathy (n = 2), nystagmus (n = 5), other (n = 11) |
| Watson 2005 | 30 | AMD or juvenile macular degeneration or diabetic retinopathy (number of participants unclear) |
AMD: age‐related macular degeneration.
Interventions
Included studies evaluated several types of reading aids.
-
Optical devices.
Stand magnifiers.
Hand magnifiers.
High‐powered spectacles (including prism or diffractive).
Filters.
-
Electronic devices.
Conventional, stand‐mounted electronic devices, often known as closed circuit television (CCTV).
Hand‐held or portable electronic device.
Head‐mounted.
Table B summarises the comparisons in each study. See also Table 8.
Table B: Interventions
| Study | Optical device(s) | Electronic device(s) | Comment |
| Culham 2004 | Participants's optical device | Head‐mounted; 4 types: Jordy, Flipperport, Maxport and NuVision | Maximum field of view (i.e. at minimum magnification) was 30° horizontal by 22.5° vertical for all the four electronic devices. There were differences in field of view with optical devices. |
| Eperjesi 2004 |
|
No electronic device | — |
| Goodrich 2001 | Participant's optical device |
|
— |
| Jackson 2017 | No optical device | Stand‐mounted CCTV (Clearview, Optelec) | Vision rehabilitation consultation (all participants) during which patients were educated about rehabilitation strategies, given information about remaining visual function, and shown a range of optical and electronic devices that they could purchase. |
| Kleweno 2001 | No optical device |
|
— |
| Morrice 2017 | No optical device |
|
— |
| 1999 | No optical device |
|
Unclear whether these were matched by field of view |
| Peterson 2003 | Participant's own optical magnifier |
|
Magnification and field‐of‐view matched. There were clear differences in field of view among these devices. |
| Smith 2005 |
|
No electronic device | Differences in field of view among these devices should be small. |
| Spitzberg 1995 |
|
No electronic device | 4 devices with the same nominal magnification (3×). There were clear differences in the field of view and working distance between each of these devices, with measurements given in the paper. |
| Stelmack 1991 |
|
Stand‐mounted CCTV (VTEK Voyager) | Although not specified, there were clear differences in the field of view and working distance between each of these devices. |
| Taylor 2017 | Participant's existing optical device | Hand‐held (not mouse‐based) electronic device (Optelec Compact+, Optelec Compact 4HD, Schweizer eMAG 43, Eschenbach Mobilux Digital) | Differences in field of view among these devices should be small. |
| Watson 2005 |
|
No electronic device | Differences in field of view among these devices should be small. |
CCTV: closed circuit television.
Training may affect performance and must be considered as part of the intervention. In Stelmack 1991, all participants developed eccentric viewing skills and received training in visual skills for reading with each device. Spitzberg 1995 also used a training period of up to 10 days. Ortiz 1999 did not train the participants, but all were proficient CCTV users. Goodrich 2001 administered one hour of training for five days with each device. Kleweno 2001 did not report training. Peterson 2003 wrote that although training with magnification aids improves reading speed and duration, there is no published information on an optimal training programme or evidence to suggest that the benefits of training are magnifier‐specific. They therefore tested participants after an explanation, a demonstration and a two‐minute active training period with each magnifying device. All but 24 of 70 participants were already optical device users. Eperjesi 2004 did not use training and stated that this did not affect the type of short reading test used. Culham 2004 provided basic training and loaned the devices to participants for use in their usual environments for one week. Smith 2005 delivered no training with prism or control spectacles, but participants were advised to gradually prolong their use of the test spectacles if they felt comfortable doing so and to give themselves time to adapt to the test spectacles, which could potentially replace their conventional spectacles. In Watson 2005 the research project began when the person was able to use a spectacle magnifier, maintain the correct focal distance and scan the print. Following initial consultation, Jackson 2017 offered occupational therapy evaluation to address training to use devices, evaluation of success with devices, and opportunities to modify tasks and strategies to improve visual performance. Morrice 2017 did not report training and tested both reading aids in the same session. Taylor 2017 trained participants in task‐based practice sessions with the clinician researcher at the start of each of the two‐month intervention periods.
Overall, the included studies were short‐term and not designed to investigate the effect of training on the reading performance with each device.
Outcome measures
Reading speed (primary outcome in this review)
All the trials reported reading speed in words per minute (Table 8).
Eleven studies recorded reading speed at a font size that was close to ordinary reading material, i.e. print size approximately 10 to 14 points (Culham 2004; Eperjesi 2004; Goodrich 2001; Ortiz 1999; Peterson 2003; Stelmack 1991Spitzberg 1995; Jackson 2017; ; Taylor 2017). The most recent studies used the International Reading Speed Texts (IReST). Ortiz 1999 also recorded MNREAD maximum reading speed. Peterson 2003 used MNREAD charts and provided reading speed (standard error) data across several point sizes in a figure. We obtained reading speed data regarding ordinary print size from the authors.
Kleweno 2001 used an electronic MNREAD version and reported speed at a text size near to the critical print size, which was highly variable between people. Smith 2005 only reported MNREAD maximum reading speed. Watson 2005 obtained MNREAD maximum reading speed and Pepper test reading rate.
Reading acuity
Seven studies measured reading acuity using Bailey‐Lovie, MNREAD, or other charts (Culham 2004; Kleweno 2001; Ortiz 1999; Peterson 2003; Smith 2005; Taylor 2017; Watson 2005). It is unclear whether or not reading acuity, measured and defined according to MNREAD‐like methods (Ahn 1995a; Ahn 1995b; Legge 1985a; Legge 2007), translates into the ability to read ordinary print size. This is largely related to the amount and range of magnification offered by each device compared to the person's needs and the type of reading task. Thus, the issue of whether or not to match by magnification arises, depending on the study question, which ultimately depends on the study objectives and main outcome measure. We extracted reading acuity data only if studies used MNREAD‐like methods (i.e. adjusting by distance or magnification) but accepted other definitions if devices were matched by magnification. In fact, reading acuity is nested within the ability to read with each device. This is relevant, since unmatched studies may record a large difference in the proportion of participants who are able to read with each device, thus leading to missing data with group imbalance, which can make it difficult to analyse and interpret reading acuity data. Paired studies could avoid this problem by restricting the analysis to participants who are able to read with all tested devices.
We extracted data for Kleweno 2001, Smith 2005 and Watson 2005. Watson 2005 provided the critical print size, which we used as a proxy for reading acuity because they are strictly related measures using the same scale, so differences between devices are expected to be similar.
In Culham 2004 it was unclear whether LVAs were matched by magnification, and the large differences found did not suggest so. Eperjesi 2004 compared filters, and we did not extract reading acuity data regarding these aids since they do not magnify text.
Quality of life
Smith 2005 also used quality of life questionnaires (National Eye Institute Visual Functioning Questionnaire, NEI‐VFQ), a performance assessment (Melbourne Low Vision Activities of Daily Living Index, MLVAI) and a questionnaire assessing participant experience with the spectacles. Jackson 2017 used the Impact of Vision Impairment (IVI) questionnaire and Rasch analysis to compute person measures. Taylor 2017 conducted a cost‐effectiveness analysis using different psychometric tools, and we extracted data for the NV‐VFQ‐15 questionnaire, which was developed with near vision items of the VFQ‐48 questionnaire, then we used it to compute perceived difficulty by means of Rasch analysis.
Reading duration
Goodrich 2001 and Stelmack 1991 measured reading duration, defined as the time the participant could read without visual discomfort, measured in minutes.
Preference for each device
Goodrich 2001,Kleweno 2001,Peterson 2003,Spitzberg 1995,Taylor 2017 and Watson 2005 recorded participants' preference for each device after their use. Due to the variability of methods, as well as the unclear quality of the instrument used for measurements, we summarise these data narratively in this review.
Outcomes not used in this review
Culham 2004, Goodrich 2001, Ortiz 1999, Stelmack 1991, Watson 2005 and Morrice 2017 measured reading comprehension and accuracy. However, the methods used were heterogeneous.
Peterson 2003 and Culham 2004 also used several tests chosen specifically to replicate daily living tasks, which this review did not use.
Excluded studies
We excluded 23 studies that we retrieved for full‐text review (see Characteristics of excluded studies). Some evaluated different settings of the same visual aid, such as Jacobs 1990, assessing whether the colour of the screen altered the performance of a CCTV. Goodrich 1977 and Goodrich 2004 did not report any information on the use of randomisation. We contacted the study authors, who informed us that they had not randomised presentation order. We excluded a large study, LOVIT 2008, since it assessed the effectiveness of a low‐vision rehabilitation programme using a visual function questionnaire and did not compare reading speed with different LVAs.
Through handsearching the references of included studies and other reviews, we found one small randomised study, Parodi 2004, plus one small quasi‐randomised study, Rosenberg 1989, which had assessed the effect of prismatic correction in low‐vision participants. We excluded both because they were designed to improve distance visual acuity rather than reading ability.
Risk of bias in included studies
We show the results of the 'Risk of bias' assessment in the Characteristics of included studies tables and summarise them in Figure 2. Overall, masking was impossible using LVAs in cross‐over studies, a feature that we expected and which led us to exclude masking as a methodological quality item in this review. Furthermore, it was difficult to assess other items specific to this design due to poor reporting.
Allocation
We considered the process of randomisation of presentation order of the devices and its concealment to be good for all cross‐over ('within‐person') studies, since the same individual used all devices and therefore selection bias was unlikely. We judged the two parallel‐arm trials as being at low risk of selection bias as well because a random allocation sequence was concealed from people enrolling participants (Jackson 2017; Smith 2005).
Goodrich 2001 and Spitzberg 1995 used rotation. All other studies described randomisation (Eperjesi 2004; Kleweno 2001; Peterson 2003; Culham 2004; Stelmack 1991), or they stated that they counterbalanced the order of presentation but did not describe the technique used (Morrice 2017; Ortiz 1999).
Blinding
We did not use masking as a marker of quality in this review but provide a brief description here. In cross‐over ('within‐person') studies, masking of participants and care providers was impossible because they identified the aid during use. We therefore considered all studies using conventional reading aids in this review to be at high risk of bias for this domain. Masking might have been possible for outcome assessors measuring reading speed if the participants' voices had been recorded. Eperjesi 2004 used a tape recorder to measure reading speed and could have masked examiners but did not report doing so. Smith 2005 did achieve masking, a parallel‐arm trial comparing prismatic and standard glasses.
Incomplete outcome data
There was no loss to follow‐up in these short‐term studies, some of which seemed to have been performed in a single testing session, with the exception of Jackson 2017, where 6 out of 36 participants were lost to follow‐up at one month.
Selective reporting
Few studies reported reading acuity or provided extractable data (Table 8). Only two studies measured reading duration, although all studies could have done so. Methods of measurement of subjective preferences for each device were too heterogeneous for us to draw any conclusions on selective reporting.
We conclude that the scoring of selective reporting bias for our secondary outcomes will only be feasible after the research community agrees on the tools for measuring these outcomes in broad consensus initiatives such as COMET or COSMIN,
Other potential sources of bias
The following is a description of methodological quality issues that are specific to studies adopting a 'within‐person' or cross‐over design.
Period effect: stability of disease during cross‐over phases
Because participation lasted a few weeks at most, we did not expect a 'period effect' (a particular type of selection bias due to the change of disease status during phases in cross‐over‐like studies) to be an issue when studies tested all aids in the same session or within a few days. As reported above, only Culham 2004 allowed a one‐week loan of each device before testing. Taylor 2017 compared two, two‐month periods but provided estimates that accounted for period and carry‐over effects. We therefore rated all studies as being at low risk of bias for this item.
Carry‐over effect and period‐by‐treatment interaction: the potential risk of learning effect or fatigue during repeated testing
Carry‐over effect may happen when the effect of the first intervention lasts into the following treatment period. In research on reading aids, testing can take place in a single session. Learning effect, or conversely fatigue due to prolonged testing, may be forms of this type of bias, although these biases will work in opposite directions. Randomisation is expected to balance these effects across LVAs used in the study, although it is possible the performance of some devices could be affected more than others when the participant becomes tired after repeated testing, which can be referred to as 'period‐by‐treatment interaction'. No studies provided details on the timing of testing sessions, particularly on time between longer reading duration tests. However, some provided details that were suggestive of little risk of carry‐over effect. Ortiz 1999 could not find a practice effect comparing the first and the last half of their tests, nor a decay in performance, but a quantitative assessment was not available. Two more studies reported short test duration, which most likely did not induce fatigue. Kleweno 2001 used a reading test based on the MNREAD. Nonetheless, one participant withdrew because of fatigue. Peterson 2003 used reading and real‐word tests of very short duration. Because it was difficult to evaluate the impact of these statements, we rated all studies as being at unclear risk of bias for this item, except for Taylor 2017, which accounted for period and carry‐over effects statistically.
Effects of interventions
See: Table 1; Table 2; Table 3; Table 4; Table 5; Table 6; Table 7
Summary of findings for the main comparison. Stand‐mounted closed circuit television (CCTV) versus optical device for adults with low vision.
| Stand‐mounted CCTV versus optical device for adults with low vision | |||||
| Patient or population: adults with low vision Settings: low vision services Intervention: stand mounted CCTV Comparison: optical device | |||||
| Outcomes | Illustrative comparative risks* (95% CI) | No of participants (studies) | Certainty of the evidence (GRADE) | Comments | |
| Assumed risk | Corresponding risk | ||||
| Optical device | Stand‐mounted CCTV | ||||
|
Reading speed (words per minute) Follow‐up: at time of assessment |
The mean reading speed using an optical device was 65.8 words per minute | The mean reading speed using a stand‐mounted CCTV was 45.5 words per minute more (26.0 fewer to 65.0 more) | 70 (1 study) | ⊕⊕⊝⊝ Lowa,b | Optical device was participant's own. In a different study of 22 participants the comparator was best prescribed optical device. The mean reading speed using a stand‐mounted CCTV was 12 words per minute more (2.5 fewer to 26.5 more) than with best prescribed optical device. |
|
Reading duration (minutes) Follow‐up: at time of assessment |
The mean reading duration using an optical device was 23 minutes | The mean reading duration using a stand‐mounted CCTV was was 13.7 minutes more (7.9 more to 19.5 more) | 22 (1 study) | ⊕⊕⊕⊝ Moderatec | In another study of 37 people people using a CCTV reported a longer duration (29 minutes) than with optical aids (13 minutes) but no analyses could be performed due to marked skewness problems. |
| Reading acuity | Not reported | ||||
|
Ease and frequency of use Task difficulty score (0 = very easy to use 5 = extremely difficult) Follow‐up: at time of assessment |
The mean task difficulty score with the optical device was 3.3 | The mean task difficulty score with the stand‐mounted CCTV was 2.0 lower (easier) (2.52 lower to 1.48 lower) | 70 (1 study) | ⊕⊕⊕⊝ Moderateb | — |
| Quality of life | Not reported | ||||
| Adverse outcomes | Not reported | ||||
| *The basis for the assumed risk (e.g. the median control group risk across studies) is provided in footnotes. The corresponding risk (and its 95% confidence interval) is based on the assumed risk in the comparison group and the relative effect of the intervention (and its 95% CI). CI: confidence interval. | |||||
| GRADE Working Group grades of evidence High‐certainty: we are very confident that the true effect lies close to that of the estimate of the effect. Moderate‐certainty: we are moderately confident in the effect estimate; the true effect is likely to be close to the estimate of effect, but there is a possibility that it is substantially different. Low‐certainty: we are moderately confident in the effect estimate; the true effect is likely to be close to the estimate of effect, but there is a possibility that it is substantially different. Very low‐certainty: we have very little confidence in the effect estimate; the true effect is likely to be substantially different from the estimate of effect. | |||||
aDowngraded for imprecision (−1): wide confidence intervals. bDowngraded for risk of bias (−1): not all participants in a paired study could read with both the electronic and the optical device. cDowngraded for indirectness (−1): small sample, unclear if widely applicable.
Summary of findings 2. Hand‐held mouse‐based electronic device versus optical device for adults with low vision.
| Hand‐held mouse‐based electronic device versus optical device for adults with low vision | |||||
| Patient or population: adults with low vision Settings: low vision services Intervention: hand‐held mouse‐based electronic device Comparison: optical device | |||||
| Outcomes | Illustrative comparative risks* (95% CI) | No of participants (studies) | Certainty of the evidence (GRADE) | Comments | |
| Assumed risk | Corresponding risk | ||||
| Optical device | Hand‐held mouse‐based electronic device | ||||
|
Reading speed (words per minute) Follow‐up: at time of assessment |
The mean reading speed using an optical device was 65.8 words per minute | The mean reading speed using a mouse‐based device (with 14'' monitor) was 40.5 words per minute more (23.7 more to 57.3 more) | 70 (1 study) | ⊕⊕⊕⊝ Moderatea | In a different study of 22 participants the mean reading speed using a mouse‐based device with a 27" monitor was 15.8 words per minute more (0.42 to 31.2 more) compared with best prescribed optical device (64 words per minute). |
|
Reading duration (minutes) Follow‐up: at time of assessment |
The mean reading duration using an optical device was 23 minutes | The mean reading duration with the mouse‐based electronic device was 12.8 minutes more (9.3 more to 16.3 more) | 22 (1 study) | ⊕⊕⊕⊝ Moderateb | — |
| Reading acuity | Not reported | ||||
|
Ease and frequency of use Task difficulty score (0=very easy to use 5=extremely difficult) Follow‐up: at time of assessment |
The mean task difficulty score with the optical device was 3.3 | The mean task difficulty score with the stand‐mounted CCTV was 1.3 lower (easier) (1.30 lower to 0.95 lower). | 70 (1 study) | ⊕⊕⊕⊝ Moderatea | — |
| Quality of life | Not reported | ||||
| Adverse outcomes | Not reported | ||||
| *The basis for the assumed risk (e.g. the median control group risk across studies) is provided in footnotes. The corresponding risk (and its 95% confidence interval) is based on the assumed risk in the comparison group and the relative effect of the intervention (and its 95% CI). CI: confidence interval. | |||||
| GRADE Working Group grades of evidence High‐certainty: we are very confident that the true effect lies close to that of the estimate of the effect. Moderate‐certainty: we are moderately confident in the effect estimate; the true effect is likely to be close to the estimate of effect, but there is a possibility that it is substantially different. Low‐certainty: we are moderately confident in the effect estimate; the true effect is likely to be close to the estimate of effect, but there is a possibility that it is substantially different. Very low‐certainty: we have very little confidence in the effect estimate; the true effect is likely to be substantially different from the estimate of effect. | |||||
aDowngraded for risk of bias (−1): not all participants in a paired study could read with both the electronic and the optical device. bDowngraded for indirectness (−1): small sample, unclear if widely applicable.
Summary of findings 3. Hand‐held (not mouse‐based) electronic device plus optical device versus optical device for adult with low vision.
| Hand‐held (not mouse‐based) electronic device in addition to optical device versus optical device | |||||
| Patient or population: adults with low vision Settings: low vision services Intervention: hand‐held electronic device in addition to optical device Comparison: optical device | |||||
| Outcomes | Illustrative comparative risks* (95% CI) | No of participants (studies) | Certainty of the evidence (GRADE) | Comments | |
| Assumed risk | Corresponding risk | ||||
| Optical device | Hand‐held electronic device in addition to optical device | ||||
|
Reading speed (words per minute) using the IReST test Follow‐up: two months |
The mean reading speed using optical device in the control groups ranged from 37 to 57 words per minutes | The mean reading speed with a hand‐held electronic device was 1.7 words per minute fewer (7.2 fewer to 3.8 more) | 100 participants (1 study) |
⊕⊕⊕⊝ Moderatea | — |
| Reading duration | Not reported | ||||
| Reading acuity | Not reported | ||||
|
Ease and frequency of use Frequency of use (0 = never to 4 = several times a day) Follow‐up: 2 months |
The mean frequency of use of the optical device was about 3.4 | The mean frequency of use of a hand‐held electronic device was −0.9 worse (−1.3 worse to −0.6 worse) | 100 participants (1 study) |
⊕⊕⊝⊝ Lowa,b | — |
|
Quality of life estimating perceived difficulty using the NV‐VFQ‐15 questionnaire Follow‐up: 2 months |
The mean perceived difficulty ranged in the control group was about 2 (SD: 1.3) | The mean perceived difficulty in the intervention groups was 0.57 less difficult (0.33 less to 0.81 less) | 100 participants (1 study) |
⊕⊕⊕⊝ Moderatea | NV‐VFQ‐15 questionnaire developed with near vision items of the VFQ‐48 questionnaire (Rasch analysis) |
| Adverse outcomes | Not reported | ||||
| *The basis for the assumed risk (e.g. the median control group risk across studies) is provided in footnotes. The corresponding risk (and its 95% confidence interval) is based on the assumed risk in the comparison group and the relative effect of the intervention (and its 95% CI). CI: confidence interval; IReST: International Reading Speed Texts; NV‐VFQ: Near Vision Visual Function Questionnaire. | |||||
| GRADE Working Group grades of evidence High‐certainty: we are very confident that the true effect lies close to that of the estimate of the effect. Moderate‐certainty: we are moderately confident in the effect estimate; the true effect is likely to be close to the estimate of effect, but there is a possibility that it is substantially different. Low‐certainty: we are moderately confident in the effect estimate; the true effect is likely to be close to the estimate of effect, but there is a possibility that it is substantially different. Very low‐certainty: we have very little confidence in the effect estimate; the true effect is likely to be substantially different from the estimate of effect. | |||||
aDowngraded for imprecision (−1): wide confidence intervals. bDowngraded for risk of bias (−1): skewed outcome measure.
Summary of findings 4. Stand‐mounted closed circuit television (CCTV) plus visual rehabilitation versus visual rehabilitation alone.
| Stand‐mounted CCTV with visual rehabilitation vs visual rehabilitation alone | ||||
| Patient or population: adults with low vision Settings: low vision services Intervention: stand‐mounted CCTV after visual rehabilitation consultation Comparison: visual rehabilitation consultation | ||||
| Outcomes | Illustrative comparative risks* (95% CI) | No of participants (studies) | Certainty of the evidence (GRADE) | |
| Assumed risk | Corresponding risk | |||
| visual rehabilitation only | stand‐mounted CCTV with visual rehabilitation | |||
|
Reading speed (maximum reading speed words per minute) Follow‐up: 1 month after visual rehabilitation consultation |
The mean reading speed with visual rehabilitation only was 34 words per minute | The mean reading speed in the intervention groups was 33.7 words per minute more (4.3 more to 63.1 more) | 31 (1 study) |
⊕⊕⊝⊝ Lowa,b |
| Reading duration | Not reported | |||
| Reading acuity | Not reported | |||
| Ease and frequency of use | Not reported | |||
|
Quality of life Follow‐up: 1 month after visual rehabilitation consultation |
The authors provided additional analysis results which showed no statistically significant difference between the 2 groups for the Rasch‐scaled person‐measures for any domain (emotional, mobility, reading); however, an overall quality of life measure could not be extracted for use in this review. | 31 (1 study) |
⊕⊕⊝⊝ Lowa,b | |
| Adverse outcomes | Not reported | |||
| *The basis for the assumed risk (e.g. the median control group risk across studies) is provided in footnotes. The corresponding risk (and its 95% confidence interval) is based on the assumed risk in the comparison group and the relative effect of the intervention (and its 95% CI). CCTV: closed circuit television; CI: confidence interval. | ||||
| GRADE Working Group grades of evidence High‐certainty: we are very confident that the true effect lies close to that of the estimate of the effect. Moderate‐certainty: we are moderately confident in the effect estimate; the true effect is likely to be close to the estimate of effect, but there is a possibility that it is substantially different. Low‐certainty: we are moderately confident in the effect estimate; the true effect is likely to be close to the estimate of effect, but there is a possibility that it is substantially different. Very low‐certainty: we have very little confidence in the effect estimate; the true effect is likely to be substantially different from the estimate of effect. | ||||
aDowngraded for imprecision (−1): wide confidence intervals. bDowngraded for indirectness (−1): small sample, unclear if widely applicable.
Summary of findings 5. Stand‐mounted closed circuit television (CCTV) versus head‐mounted electronic device (HMD) for adults with low vision.
| Stand‐mounted closed circuit television (CCTV) versus head‐mounted electronic device (HMD) for adults with low vision | |||||
| Patient or population: adults with low vision Settings: low vision services Intervention: stand‐mounted CCTV Comparison: HMD | |||||
| Outcomes | Illustrative comparative risks* (95% CI) | No of participants (studies) | Certainty of the evidence (GRADE) | Comments | |
| Assumed risk | Corresponding risk | ||||
| HMD | Stand‐mounted CCTV | ||||
|
Reading speed (words per minute)
MNREAD Charts Follow‐up: at time of assessment |
The mean reading speed using HMD was 66 words per minute | The mean reading speed using stand‐mounted CCTV 3.1 words per minute more (3.5 fewer to 9.7 more) | 93 (3 studies) | ⊕⊕⊝⊝ Lowa,b | — |
| Reading duration | Not reported | ||||
|
Reading acuity (logMAR)
MNREAD charts. Higher score is worse acuity. Follow‐up: at time of assessment |
The mean reading acuity with HMD was 0.92 logMAR | The mean reading acuity with stand‐mounted CCTV was 0.05 logMAR higher (i.e. same) (0.06 lower to 0.15 higher) | 13 (1 study) | ⊕⊝⊝⊝ Lowa,c | — |
|
Ease and frequency of use Task difficulty score (0 = very easy to use 5 = extremely difficult) Follow‐up: at time of assessment |
The mean task difficulty score with the optical device was 3.3 | The mean task difficulty score with the stand‐mounted CCTV was 0 lower (same difficulty) (0.37 lower to 0.37 higher) | 70 (1 study) |
⊕⊕⊝⊝ Lowa,b | One study with 13 participants collected data on perceived brightness and clarity of images. 10/13 people found the head‐mounted device to be brighter and 9/13 felt the head‐mounted device was clearer compared with the CCTV. |
| Quality of life | Not reported | ||||
| Adverse outcomes | Not reported | ||||
| *The basis for the assumed risk (e.g. the median control group risk across studies) is provided in footnotes. The corresponding risk (and its 95% confidence interval) is based on the assumed risk in the comparison group and the relative effect of the intervention (and its 95% CI). CCTV: closed circuit television; CI: confidence interval; HMD: head‐mounted device. | |||||
| GRADE Working Group grades of evidence High‐certainty: we are very confident that the true effect lies close to that of the estimate of the effect. Moderate‐certainty: we are moderately confident in the effect estimate; the true effect is likely to be close to the estimate of effect, but there is a possibility that it is substantially different. Low‐certainty: we are moderately confident in the effect estimate; the true effect is likely to be close to the estimate of effect, but there is a possibility that it is substantially different. Very low‐certainty: we have very little confidence in the effect estimate; the true effect is likely to be substantially different from the estimate of effect. | |||||
a Downgraded for imprecision (−1): wide confidence intervals. b Downgraded for risk of bias (−1): not all participants in the studies could read with both electronic devices. c Downgraded for indirectness (−1) and imprecision (−1): small sample, unclear if widely applicable
Summary of findings 6. Stand‐mounted closed circuit television (CCTV) versus hand‐held mouse‐based electronic device (HHD) for adults with low vision.
| Stand‐mounted closed circuit television (CCTV) versus hand‐held, mouse‐based electronic device (HHD) for adults with low vision | ||||
| Patient or population: adults with low vision Settings: low vision services Intervention: stand‐mounted CCTV Comparison: hand‐held, mouse‐based electronic device (HHD) | ||||
| Outcomes | Illustrative comparative risks* (95% CI) | No of participants (studies) | Certainty of the evidence (GRADE) | |
| Assumed risk | Corresponding risk | |||
| HHD | Stand‐mounted CCTV | |||
|
Reading speed (maximum reading speed words per minute)
MNREAD charts Follow‐up: at time of assessment |
The mean maximum reading speed (words per minute) in the control groups was 64 words per minute | The mean maximum reading speed (words per minute) with a stand‐mounted CCTV was 9.5 words per minute more (−0.3 fewer to 19.4 words per minute more) | 92 (2 studies) | ⊕⊕⊝⊝ Lowa,b |
|
Reading duration (minutes)
MNREAD charts Follow‐up: at time of assessment |
The mean reading duration (minutes) in the control groups was 35.3 minutes | The mean reading duration (minutes) with CCTV was 0.9 minutes more (4.4 fewer to 6.2 more) | 22 (1 study) | ⊕⊕⊝⊝ Lowa,c |
| Reading acuity | Not reported | |||
| Ease and frequency of use | Not reported | |||
| Quality of life | Not reported | |||
| Adverse outcomes | Not reported | |||
| *The basis for the assumed risk (e.g. the median control group risk across studies) is provided in footnotes. The corresponding risk (and its 95% confidence interval) is based on the assumed risk in the comparison group and the relative effect of the intervention (and its 95% CI). CCTV: closed circuit television; CI: confidence interval; HHD: hand‐held device. | ||||
| GRADE Working Group grades of evidence High‐certainty: we are very confident that the true effect lies close to that of the estimate of the effect. Moderate‐certainty: we are moderately confident in the effect estimate; the true effect is likely to be close to the estimate of effect, but there is a possibility that it is substantially different. Low‐certainty: we are moderately confident in the effect estimate; the true effect is likely to be close to the estimate of effect, but there is a possibility that it is substantially different. Very low‐certainty: we have very little confidence in the effect estimate; the true effect is likely to be substantially different from the estimate of effect. | ||||
aDowngraded for imprecision (−1): wide confidence intervals. bDowngraded for risk of bias (−1): not all participants in the largest study could read with both the electronic and the optical device. cDowngraded for indirectness (−1): small sample, unclear if widely applicable.
Summary of findings 7. Prism spectacles versus conventional spectacles for adults with low vision.
| Prism spectacles versus conventional spectacles for adults with low vision | |||||
| Patient or population: adults with low vision (people with AMD) Settings: low vision services Intervention: prism spectacles Comparison: conventional spectacles | |||||
| Outcomes | Illustrative comparative risks* (95% CI) | No of participants (studies) | Certainty of the evidence (GRADE) | Comments | |
| Assumed risk | Corresponding risk | ||||
| Conventional spectacles | Custom prism spectacles | ||||
|
Reading speed (words per minute) Follow‐up: 3 months |
The mean reading speed using conventional spectacles was 67 words per minute | The mean reading speed using custom prism spectacles was 6 fewer words per minute (25.4 fewer to 13.4 more) | 150 (1 study) | ⊕⊕⊝⊝ Lowa | In the same study, the mean reading speed using standard prism spectacles was 7 fewer words per minute (25.9 fewer to 11.9 more) compared with conventional spectacles |
| Reading duration | Not reported | ||||
|
Reading acuity in logMAR Follow‐up: 3 months |
The mean reading acuity using conventional spectacles was 1.50 logMAR | The mean reading acuity using custom prism spectacles was 0.07 logMAR higher (0.05 lower to 0.19 higher) | 150 (1 study) | ⊕⊕⊝⊝ Lowa | In the same study, the mean reading acuity using standard prism spectacles was 0.06 logMAR higher (0.06 lower to 0.18 higher) compared with conventional spectacles |
| Ease and frequency of use | Not reported | ||||
|
Quality of life (NEI‐VFQ score) Scale from: 0‐100. Higher scores are better Follow‐up: 3 months |
The mean quality of life score using conventional spectacles was 53 | The mean quality of life score using custom prism spectacles was 0 higher (same) (5.62 lower to 5.62 higher) | 153 (1 study) | ⊕⊕⊕⊝ Moderateb | In the same study, the mean quality of life score using standard prism spectacles was 1 higher (4.75 lower to 6.75 higher) compared with conventional spectacles. |
| Adverse outcomes | Not reported | ||||
| The basis for the assumed risk (e.g. the median control group risk across studies) is provided in footnotes. The corresponding risk (and its 95% confidence interval) is based on the assumed risk in the comparison group and the relative effect of the intervention (and its 95% CI). CI: confidence interval; NEI‐VFQ: National Eye Institute Visual Functioning Questionnaire. | |||||
| GRADE Working Group grades of evidence High‐certainty: we are very confident that the true effect lies close to that of the estimate of the effect. Moderate‐certainty: we are moderately confident in the effect estimate; the true effect is likely to be close to the estimate of effect, but there is a possibility that it is substantially different. Low‐certainty: we are moderately confident in the effect estimate; the true effect is likely to be close to the estimate of effect, but there is a possibility that it is substantially different. Very low‐certainty: we have very little confidence in the effect estimate; the true effect is likely to be substantially different from the estimate of effect. | |||||
aDowngraded for imprecision (−2): very wide confidence intervals. bDowngraded for imprecision (−1): wide confidence intervals.
1 Electronic versus optical devices
Four studies compared electronic devices with optical devices, mainly stand or hand magnifiers (Culham 2004; Goodrich 2001; Peterson 2003; Stelmack 1991). We could extract data from three studies (Culham 2004; Goodrich 2001; Peterson 2003), but not for Stelmack 1991 because of marked data skewness (see Appendix 9). Peterson 2003 presented data as reading time for various print sizes, and we obtained reading speed data from the authors at a visual angle equivalent to 0.5 logMAR, about 12 points at 40 cm. One further study compared a combination of the participant's existing optical aid plus a hand‐held device known as a portable electronic vision enhancement system (p‐EVES) versus optical aids alone (Taylor 2017). Another study evaluated the addition of a stand‐based CCTV to visual rehabilitation (Jackson 2017).
1.1 Stand‐mounted CCTV versus optical device
Table 1 compares stand‐mounted CCTV with optical devices. Figure 3 presents results for the primary outcome (reading speed).
3.

Forest plot of comparison: 1 Electronic device (various types of CCTV) versus optical device, outcome: 1.1 Reading speed (words per minute).
Reading speed (primary outcome)
In one study in 70 participants, people using an optical device read on average 65.8 words per minute (wpm). People using a stand‐mounted CCTV on average read 40.5 more wpm (95% confidence interval (CI) 26.0 to 65.0) (Peterson 2003). The optical device used was the participant's own. At a visual angle of print of 0.5 logMAR, about 55% of participants were able to read using an optical device compared with 82% of participants using a stand CCTV. The comparison was therefore based on a subset of participants and nested in the ability to read. Although this could be due to the larger field of view with an electronic device, it may be that the participant's optical device was not best prescribed (i.e. clinically evaluated and recommended as appropriate treatment) or matched by magnification with the electronic devices. Specifically, the authors reported that people used their own magnifier but also, in a following sentence, the optimum optical magnifier (also see Characteristics of included studies).
In a different study in 22 participants, the comparator was best prescribed optical device. The mean reading speed using a stand‐mounted CCTV was 12 wpm more (95% CI −2.5 to 26.5) than with the best prescribed optical device (Goodrich 2001).
The authors of the study for which data were not extracted, Stelmack 1991, stated that stand‐mounted or hand‐held electronic devices (mean speed 59 wpm, standard deviation 37 wpm) were better than optical devices (stand magnifiers mean 32 wpm, standard deviation 30 wpm; spectacle lenses mean 47 wpm, standard deviation 52 wpm).
We judged this to be low‐certainty evidence downgrading for imprecision and risk of bias.
Reading duration
In Goodrich 2001 the mean reading duration was about 36 minutes with the stand‐mounted CCTV compared with 23 minutes using an optical device i.e. the mean reading duration was 13.7 minutes more (95% CI 7.9 to 19.5). No data could be extracted from Stelmack 1991, who reported a longer duration with a CCTV (29 minutes) than with optical aids (13 minutes) and spectacles (11 minutes). We were unable to perform analyses due to marked skewness problems.
Reading acuity
Not reported
Ease and frequency of use
In Peterson 2003 participants found the stand‐mounted CCTV easier to use, as assessed using a Likert scale (0 = very easy to use; 5 = extremely difficult). People using the stand‐mounted CCTV found the device easier to use (mean score 1.3 points, SD 0.5) compared with using an optical device (mean score 3.3 points, SD 0.8) (mean difference (MD) −2 points, 95% CI −2.52 to −1.48).
Quality of life
Not reported.
Adverse outcomes
Not reported.
1.2 Hand‐held mouse‐based electronic device versus optical device
Table 2 compares hand‐held mouse‐based electronic device versus optical device. Results for the primary outcome (reading speed) are presented in Figure 3.
Reading speed (primary outcome)
In one study in 70 participants, mean reading speed using an optical device was 65.8 wpm. The mean reading speed using a mouse‐based device (14" monitor) was 111 wpm (MD 40.5 wpm, 95% CI 23.7 to 57.3) (Peterson 2003). At a visual angle of print of 0.5 logMAR, about 55% of participants were able to read using an optical device compared with 78% of participants using the mouse‐based device. We judged this to be moderate‐certainty evidence, downgrading one level for risk of bias as not all participants in this paired study could read with both the electronic and the optical device. In Goodrich 2001, a hand‐held mouse‐based electronic device with 27" monitor (mean reading speed 76 wpm) was superior to the participant's stand magnifier (n = 19) or microscopic spectacles (n = 3) (mean reading speed 64 wpm) (MD 15.8 wpm, 95% CI 0.42 to 31.2).
Reading duration
In one study in 22 participants, the mean reading duration using an optical device was 23 minutes. The mean reading duration with the mouse‐based electronic device was 12.8 minutes more (95% CI 9.3 to 16.3) (Goodrich 2001).
Reading acuity
Not reported.
Ease and frequency of use
In Peterson 2003 participants found the mouse‐based electronic device easier to use than the optical device. Task difficulty was assessed using a Likert scale (0 = very easy to use; 5 = extremely difficult). People using the mouse‐based electronic device found the device easier to use (mean score 2, SD 0.7) compared with using an optical device (mean score 3.3, SD 0.8) (MD −1.3, 95% CI −1.3 to −0.95). We judged this to be moderate‐certainty evidence, downgrading one level for risk of bias as not all participants in this paired study could read with both the electronic and the optical device.
Quality of life
Not reported.
Adverse effects
Not reported.
1.3 Head‐mounted CCTV versus optical device
Reading speed (primary outcome)
Peterson 2003 found that a mouse‐based head‐mounted device (HMD) (mean reading speed 85 wpm) was better than the participant's optimum optical device (mean reading speed 66 wpm). In one study of 22 people, Culham 2004 found that stand or hand optical devices (mean reading speed 95 wpm) were better than four types of head‐mounted electronic devices (mean reading speed from 55 wpm to 70 wpm), including one with a stand‐mounted camera (Figure 3 and Table C). The authors reported that one week of home practice improved reading, but it did not alter the pattern of the results. It was unclear whether optical devices were matched by magnification with electronic devices, and at least in some participants this was the optical device previously used by each participant. We judged this to be low‐certainty evidence, downgrading one level for indirectness as the sample size was small and it was unclear if these results are widely applicable, and one level for inconsistency as there were different results between the two studies.
Table C, comparison 1.3: Reading speed with head‐mounted CCTV (Culham 2004)
| Head‐mounted CCTV |
Mean difference in reading speed (words per minute) compared with reading speed of 95 words per minute using optical device (95% CI) |
| Flipperport (table stand camera) | −24.6 (−40.88 to −8.32) |
| Jordy | −33.7 (−50.34 to −17.06) |
| Maxport | −29.4 (−45.74 to −13.06) |
| NuVision | −40 (−56 to −23.3) |
Reading duration
Not reported.
Reading acuity
Not reported.
Ease and frequency of use
Peterson 2003 obtained patients' perceived ease of use (using task difficulty score from 0 to 5). People found the mouse‐based CCTV with HMD viewing as difficult to use as the optical magnifier.
Quality of life
Not reported.
Adverse outcomes
Not reported.
1.4 Hand‐held (not mouse‐based) electronic devices in addition to optical device versus optical devices
Taylor 2017 (100 participants) investigated the addition of portable electronic devices to optical devices. The study had a cross‐over design with two, two‐month periods in each study arm. The certainty of this evidence was moderate for the primary outcome, and low or moderate for the other outcomes, for reasons presented in the Table 3.
Reading speed (primary outcome)
We found little difference regarding reading speed (IReST test) adding portable electronic devices to optical devices (MD −1.7 wpm, 95% CI: −7.2 to 3.8, Analysis 2.1). This figure did not change using MNREAD charts, although this measure showed a higher reading speed.
2.1. Analysis.
Comparison 2 Hand‐held (not mouse‐based) electronic devices plus optical devices versus optical devices alone, Outcome 1 Reading speed (words per minute).
Reading duration
Not reported.
Reading acuity
Not reported.
Ease and frequency of use
Investigators assessed ease and frequency of use by means of the Manchester Low Vision Questionnaire (MLVQ), graded from 0 to 4. Participants used portable electronic devices less frequently than optical devices (MD −0.93, 95% CI −1.28 to −0.58; Analysis 2.2).
2.2. Analysis.
Comparison 2 Hand‐held (not mouse‐based) electronic devices plus optical devices versus optical devices alone, Outcome 2 Frequency of use (0‐4 scale).
Taylor 2017 assessed the use of portable electronic devices for a number of tasks, such as checking the telephone directory or writing. Despite the fact that preferences for each LVA varied for specific tasks, the authors reported that there were no significant differences in time taken, or graded accuracy of performance, on any task when comparing interventions A and B in the period using portable electronic devices plus optical aids versus optical aids only.
Quality of life
Taylor 2017 also conducted a cost‐effectiveness analysis using different psychometric tools. We extracted data for the NV‐VFQ‐15 questionnaire, which was developed with near vision items of the VFQ‐48 questionnaire then used to compute perceived difficulty by means of Rasch analysis. Participants reported decreased difficulty in the period using portable electronic devices plus optical aids versus optical aids alone (MD 0.57, 95% CI 0.33 to 0.81; Analysis 2.3). Since the sample standard deviation was 1.3 this value equals an effect size of 0.44, which is a small or moderate effect.
2.3. Analysis.
Comparison 2 Hand‐held (not mouse‐based) electronic devices plus optical devices versus optical devices alone, Outcome 3 Quality of life.
The cost‐effectiveness analysis in Taylor 2017 suggested that portable electronic devices are potentially cost‐effective means of improving 'near vision' visual function. However, using preference‐based utility and capability measures, including EQ‐5D‐5L, portable electronic devices "could not be proven to be a cost‐effective approach to improving health status or well‐being, therefore indicating that improvement to 'near vision' visual function does not drastically affect overall health status, or that standard measures of health and well‐being are not sufficiently sensitive to measure change in this population". We did not extract these data since we had not planned to analyse cost‐effectiveness.
Adverse outcomes
Not reported.
1.5 Provision of a stand‐based CCTV with visual rehabilitation versus visual rehabilitation only
Jackson 2017 (37 participants) investigated the effect of the immediate provision of a video magnifier (stand‐based CCTV) after an initial consultation for visual rehabilitation as compared to a visual rehabilitation consultation alone, in which optical devices were prescribed. Outcomes were measured after one month and prior to initiating occupational therapy. The certainty of this evidence was low for reasons presented in the Table 4.
Reading speed (primary outcome)
Sixteen participants who were provided a CCTV had a better reading speed (IReST test) than 15 participants who had only received a visual rehabilitation consultation (MD 33.7 wpm, 95% CI 4.3 to 63.1; Analysis 3.1).
3.1. Analysis.
Comparison 3 Stand‐based CCTV plus visual rehabilitation versus visual rehabilitation alone, Outcome 1 Maximum reading speed (words per minute).
Reading duration
Not reported.
Reading acuity
Not reported.
Ease and frequency of use
Not reported.
Quality of life
In Jackson 2017 patient‐reported outcomes (IVI score) were not available for the randomised groups but only for the whole sample. The authors provided additional analysis results that showed no statistically significant difference between the two groups for the Rasch‐scaled person‐measures for any domain (emotional, mobility, reading); however, we were unable to extract an overall quality of life measure for use in this review. Other outcomes, not used in this review, were the Activity Inventory and the Depression, Anxiety and Stress Scale.
Adverse outcomes
Not reported
2 Comparison between electronic devices
Five studies compared different electronic devices (Goodrich 2001; Kleweno 2001; Morrice 2017; Ortiz 1999; Peterson 2003).
Additionally, Culham 2004 tested four types of electronic HMDs against an optical device. Comparing electronic devices of the same class was not the main objective of our study, but Figure 3 shows that the performance of these devices was similar.
2.1 Stand‐mounted CCTV versus electronic HMD
Table 5 compares stand‐mounted CCTV versus electronic HMD.
Reading speed (primary outcome)
Three studies showed no clinically meaningful differences between a stand‐mounted CCTV and an electronic HMD (Kleweno 2001; Ortiz 1999; Peterson 2003) as seen in Figure 4. The confidence interval around the pooled estimate was sufficiently narrow to suggest an equivalence of the two types of devices (Table 5). This is in contrast with indirect comparisons between electronic and optical devices: Peterson 2003 found that a stand‐based CCTV was better than optical devices, but Culham 2004 found that electronic HMDs were worse than optical devices. We judged this to be low‐certainty evidence after downgrading for imprecision and risk of bias.
4.

Forest plot of comparison: 2 Stand‐based closed‐circuit television (CCTV) versus head‐mounted electronic device (HMD), outcome: 2.1 Reading speed (words per minute).
Reading duration
Not reported.
Reading acuity
In Kleweno 2001, reading acuity was 1.5 logMAR both for the conventional CCTV and for an HMD, the Virtual Retinal Display. However, this estimate was imprecise and did not exlcude a clinically relevant difference (Analysis 4.2; Table 5), such as at least 0.1 logMAR which means being able to read a smaller MNREAD sentence by one step.
4.2. Analysis.
Comparison 4 Stand‐mounted CCTV versus head‐mounted electronic device, Outcome 2 Reading acuity (logMAR).
Ease and frequency of use
Peterson 2003 reported task difficulty score on a 0 to 5 scale. The mean task difficulty score with both the optical device and the stand‐mounted CCTV was 3.3 points (MD 0 points, 95% CI −0.37 to 0.37; low‐certainty evidence).
Kleweno 2001 collected data on participant's views on which was the better display for reading. Five of 13 preferred the head‐mounted device and 8/13 preferred the CCTV. However, more people felt the head‐mounted device was apparently clearer (9/13) and apparently brighter (10/13). We judged this to be low‐certainty evidence after downgrading for risk of bias and imprecision.
Quality of life
Not reported.
Adverse outcomes
Not reported.
2.2 Stand‐mounted CCTV versus hand‐held mouse‐based electronic device
Two studies (92 participants) compared a stand‐mounted CCTV versus a hand‐held mouse‐based CCTV plus optical magnifier, generally a stand magnifier, and less frequently a hand magnifier or microscopic lenses (Goodrich 2001; Peterson 2003).
Reading speed (primary outcome)
Goodrich 2001 could not find any differences, but Peterson 2003 found that reading using a stand‐mounted CCTV was faster (Analysis 5.1; Figure 5; Table 6). We pooled these effects since they were in the same direction and also considered that statistical heterogeneity can hardly be estimated with only two small trials in the analysis. Furthermore, we found no other sources of clinical and methodological heterogeneity. Although Goodrich 2001 included only 22 participants, it had a greater weight than Peterson 2003 (70 participants) in the meta‐analysis because there was less between‐person variability. This highlights the problem of generalisability of results of paired studies including few and highly selected homogeneous participants.
5.1. Analysis.
Comparison 5 Stand‐mounted CCTV versus hand‐held, mouse‐based electronic device, Outcome 1 Reading speed (words per minute).
5.

Forest plot of comparison: 3 Stand‐based closed‐circuit television (CCTV) versus hand‐held, mouse‐based electronic device (HHD), outcome: 3.1 Reading speed (words per minute).
Reading duration
In Goodrich 2001 the mean reading duration was about 36 minutes with both the stand‐mounted and the hand‐held CCTV (Analysis 5.2; Table 6).
5.2. Analysis.
Comparison 5 Stand‐mounted CCTV versus hand‐held, mouse‐based electronic device, Outcome 2 Reading duration in minutes.
Reading acuity
Not reported.
Ease and frequency of use
As an overall measure of preference, Goodrich 2001 reported that 73% of participants preferred the CCTV.
Peterson 2003 assessed participant‐reported ease of use, finding that the stand CCTV with monitor viewing was easier to use than the mouse‐based CCTV with monitor viewing.
Quality of life
Not reported.
Adverse outcomes
Not reported.
2.3 Tablet computer versus stand‐mounted CCTV
Morrice 2017 compared a CCTV (ClearView+model, Optelec, Longueuil, QC, Canada) versus a tablet computer (iPad Air; 9.7'' display, version 2013) in the same session in 100 participants.
Reading speed (primary outcome)
Reading speed was 76.7 wpm with the CCTV and comparable using the tablet, but estimates were very imprecise (MD 2.8 wpm, 95% CI −53.1 to 58.7). We judged this to be low‐certainty evidence after downgrading two levels for imprecision due to wide confidence intervals.
Morrice 2017 reported font size, finding this was smaller and less variable with the tablet compared to the CCTV, but we were not able to convert this data to logMAR reading acuity for use in our review. Other review outcomes as listed below were not reported.
Reading duration.
Reading acuity.
Ease and frequency of use.
Quality of life.
Adverse outcomes.
3 Comparison between optical devices
Four studies compared optical LVAs (Spitzberg 1995; Stelmack 1991, Smith 2005; Watson 2005). We could not extract data from Spitzberg 1995 and Stelmack 1991 because of data skewness, according to criteria described in the Data collection and analysis section. In Stelmack 1991, mean reading speed was 47 wpm for spectacle reading compared to 32 wpm for stand magnifiers. Spitzberg 1995 reported no improvement in reading speed with four new stand magnifiers versus a conventional one with the same power; the reading speed was about 80 wpm for all devices.
3.1 Comparison of different types of spectacle‐mounted magnifier
Reading speed (primary outcome)
Watson 2005 compared a new hybrid‐diffractive spectacle‐mounted magnifier to either a refractive aspheric (experiment 1) or an aplanatic spectacle‐mounted magnifier (experiment 2), with each comparison conducted on the same participant in two groups of 15 people. MNREAD maximum reading rate was about 100 wpm in both groups, with a 95% CI excluding a difference of more than 17 wpm (Analysis 6.1; Figure 6).
6.1. Analysis.
Comparison 6 Diffractive spectacle mounted magnifiers vs control, Outcome 1 MNREAD maximum reading speed (words per minute).
6.
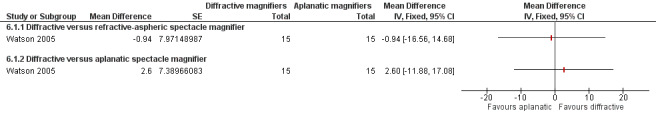
Forest plot of comparison: 6 Diffractive spectacle mounted magnifiers versus control, outcome: 6.1 MNREAD maximum reading speed (words/minute).
Reading duration
Not reported.
Reading acuity
Critical print size was approximately 1 M for all devices (Analysis 6.2).
6.2. Analysis.
Comparison 6 Diffractive spectacle mounted magnifiers vs control, Outcome 2 MNREAD critical print size (M print size).
Ease and frequency of use
Watson 2005 measured participant's preference using a 125 mm visual analogue scale to record satisfaction and comfort with reading and cosmesis; however, we decided not to use these data because we could not extract them in full.
As reported above, we could not extract reading speed data from Spitzberg 1995, who reported that 74% of 39 participants preferred the new device to their usual one.
Quality of life
Not reported.
Adverse outcomes
Not reported.
3.2 Prism spectacles versus conventional spectacles
We found one three‐arm randomised trial for this comparison (Smith 2005, 150 participants with AMD).
Using GRADE, the certainty of this evidence was always moderate or low for reasons given in Table 7, specifically because a single small study was available and estimates were imprecise.
Reading speed (primary outcome)
Smith 2005 found no significant difference between either custom (mean reading speed 73 wpm) or standard prism spectacles (74 wpm) versus conventional spectacles (67 wpm). The confidence intervals around these differences were wide, as seen in Analysis 7.1.
7.1. Analysis.
Comparison 7 Prism spectacles versus conventional spectacles, Outcome 1 Reading speed (words per minute).
Reading duration
Not reported.
Reading acuity
In Smith 2005 both custom (mean reading acuity 0.88 logMAR) and standard prism spectacles (0.89 logMAR) were not demonstrated to be different from conventional spectacles (0.95 logMAR). The confidence intervals around these differences excluded a difference of any more than 0.2 logMAR, as seen in Analysis 7.2.
7.2. Analysis.
Comparison 7 Prism spectacles versus conventional spectacles, Outcome 2 Critical print size in logMAR.
Ease and frequency of use
Not reported.
Quality of life
Smith 2005 found the total National Eye Institute Visual Functioning Questionnaire (NEI‐VFQ) score did not differ for custom or standard prism spectacles compared to conventional spectacles (Analysis 7.3; Table 7). This comparison was based on evidence of moderate quality.
7.3. Analysis.
Comparison 7 Prism spectacles versus conventional spectacles, Outcome 3 Quality of life (NEI‐VFQ score).
Adverse outcomes
Not reported.
4 Coloured light filter overlays versus clear filter
A single paired study was available for this comparison (Eperjesi 2004, 12 participants with AMD). The coloured light filter overlays used in this study (Intuitive Coloured Overlays1; IOO Marketing Ltd, London, UK) consisted of 10 A5‐sized, plastic sheets.
Reading speed (primary outcome)
Although the width of the confidence intervals could exclude a clinically significant benefit with any colour filter, Eperjesi 2004 reported that overlay colour filters tended to be less beneficial than a clear filter (reading speed 83.7 wpm) and found a statistically significant difference only for pink, aqua and purple filters (see Table D and Analysis 8.1). We judged this to be low‐certainty evidence after downgrading one level for imprecision and one level for indirectness as it was unclear if the small sample is widely applicable.
8.1. Analysis.
Comparison 8 Overlay coloured filters versus clear filter, Outcome 1 Reading speed (words per minute).
Table D, comparison 4: Reading speed with coloured light filter overlays (Eperjesi 2004)
|
Type of filter (% transmission) |
Mean difference in reading speed (words per minute) compared with reading speed of 84 words per minute in the control (clear overlay 100% transmission, reading speed 83.7 wpm) group (95% confidence interval) |
| Rose (78) | −9 (−24 to 6) |
| Pink (78) | −9 (−15 to −3) |
| Yellow (93) | −7 (−20 to 6) |
| Orange (83) | −13 (−29 to 2) |
| Mint‐green (85) | 8 (−17 to 2) |
| Lime‐green (86) | −6 (−24 to 6) |
| Grey (71) | −4 (−25 to 17) |
| Blue (74) | −12 (−24 to 1) |
| Aqua (81) | −9 (−15 to −3) |
| Purple (67) | −14 (−25 to −3) |
No studies reported the other review outcomes listed below.
Reading duration.
Reading acuity.
Ease and frequency of use.
Quality of life.
Adverse outcomes.
Outcomes extracted but not considered in this review
Watson 2005 provided usable data for comprehension (using the Morgan Low Vision Reading Comprehension test). Comprehension was better for the hybrid diffractive spectacle‐mounted magnifier versus the refractive aspheric magnifier, but there was no apparent difference between the aplanatic magnifier and the refractive aspheric magnifier (Analysis 6.3). Watson 2005 also measured reading accuracy using the Pepper test and found no significant differences, but we could not extract these data.
6.3. Analysis.
Comparison 6 Diffractive spectacle mounted magnifiers vs control, Outcome 3 Morgan Low Vision Reading Comprehension Assessment.
Factors influencing reading performance
Some studies described the effect of factors that might influence the performance with specific LVAs. We could not extract data for these outcomes.
Effect of training
Culham 2004 and Spitzberg 1995 reported that reading speed increased after five days of training or with prior CCTV use. Conversely, Peterson 2003 reported that having already used either electronic or optical aids was not associated with an increase in reading speed.
Print size
Peterson 2003 reported that CCTV superiority compared to optical devices tended to decrease as print size approached 1.0 logMAR acuity. This is probably due to the fact that the magnification provided by a CCTV is larger than that with optical devices, which may be critical for people with more severe visual loss to be able to read. We could not extract any data.
Younger age
Culham 2004 found younger age was a predictor of higher reading speed when using an HMD for medium and large print size (16 wpm per decade), but we could not extract any data.
Discussion
Summary of main results
A few small studies have compared reading speed with several LVAs that are commonly used in low‐vision rehabilitation. Using GRADE, the certainty of the evidence was consistently moderate or low due to several problems.
Eleven of the 13 studies used a cross‐over‐like design (referred to as a 'within‐person' design by most of the authors). Quality was difficult to evaluate because trialists reported relevant sources of design‐related bias insufficiently, which is a common finding in other systematic reviews that include cross‐over studies (Elbourne 2002).
Electronic versus optical devices
In two studies, electronic stand‐based (camera and monitor) CCTV and a hand‐held CCTV (14" monitor at 40 cm) allowed faster reading than optical devices. This difference was of borderline significance in one study using best‐prescribed optical device, and highly significant in another using the participant's optimal device.
In another study, participants performed significantly worse with four types of head‐mounted electronic devices than with an optical device.
Improvements in technology, especially for electronic devices, may have occurred since these trials were published.
More recently, one study provided insufficient evidence of the additional effect of portable electronic devices when they were added to the preferred optical devices, Another study found a benefit on reading speed at one month with the provision of a CCTV in addition to a standard consultation and aids prescription.
Comparisons between electronic devices
In five studies, various types of electronic devices tended to perform similarly. Overall, the performance of HMDs compared to conventional CCTVs is unclear, as is the potential effect of age and type or severity of disease on the performance with each device. Furthermore, technological advances may mean that these devices could be outdated. In view of this and the problematic quality assessment, the results of these studies are insufficient for drawing robust conclusions.
Comparisons between optical devices
There was insufficient evidence of a difference between a new diffractive spectacle‐mounted magnifier compared to a refractive and an aplanatic magnifier in one small study.
Comparison of overlay coloured filters versus clear filter
Several overlay coloured filters tended to reduce reading speed compared to a clear filter in one small study.
Prism spectacles versus conventional spectacles
One study found that prism spectacles are unlikely to be beneficial in people with age‐related macular degeneration (AMD), although the data did not allow the calculation of precise estimates of performance.
Overall completeness and applicability of evidence
Problems with outcome measures used in systematic reviews of low‐vision aids
Research on LVAs is typically based on multiple outcome measures in the attempt to capture the whole experience of people using them. Reading speed and reading acuity have been outcomes of interest in early LVA research focusing on the reading performance obtained with each device. No studies have used validated measurement methods to investigate important secondary outcomes such as subjective preference for each device or sustained use.
Low‐vision and reading rehabilitation is a complex intervention, and LVA users value aspects other than reading speed. A survey among consumers of an earlier version of this review highlighted a number of issues that are of interest to users of reading aids.
Portability, usability and cost of LVAs, especially electronic devices, which were also found to evolve very rapidly and have a shelf‐life as short as two years, according to consumer comments on this review. This type of information should be tailored according to intended use (e.g. "watching television, shopping, checking timetables, reading street names and bus numbers, and reading notices posted in clinics and elsewhere").
The effect of factors influencing the use of reading devices, such as training and environmental and lighting conditions.
Offering information on such issues probably goes beyond the scope of a Cochrane Review such as this one, which we planned several years ago as being restricted to assessing people's reading performance with each LVA.
Quality of life measures were available in only two included studies. We acknowledge that our review is a partial investigation of the needs of people with low vision, and that another Cochrane Review currently underway will include studies using multidisciplinary or monodisciplinary rehabilitation for adults with low vision, with quality of life as the primary outcome (Langelaan 2007).
Finally, we did not report on cost issues in this review, since these were not an outcome in the included studies. VA HTA 2003 observed that "sustained use of these devices in the subject's life setting, resources required in terms of costs and training associated with each alternative, and the link between device use and health related quality of life were unknown". This review also provided information on unit cost of devices in the Veteran Affairs reimbursement framework. Among excluded studies in this review, Rees 2006 compared the reading performance of low‐cost and gold‐standard magnifiers and found no difference between them. However, this study was available only as an abstract and there were insufficient data to include it.
Culham 2009 is an example of a well‐structured study investigating which performance aspects influence LVA user opinion, and may help us understand what users seek or reject in low‐vision devices. The study investigators considered participants' assessment of several features of LVAs both before and after their home loan, as well as participants' willingness to pay for each device. In this study, image quality and magnification facilities were the most important factors determining overall subjective rating of the devices. They concluded that there is much to learn from listening to patients. They also commented that impressions may change with familiarity and environment, and a single clinical assessment may not provide an accurate evaluation of how useful a device might become with time. We could not include this study because our review is restricted to reading speed as the primary outcome measure, but we found that the methodology and research scope in Culham 2009 are an important research field regarding LVAs.
Rubin 2013 provides an extensive technical discussion on the methods for assessing reading performance. A broader perspective on outcome measures, including quality of life measures, in low vision service research is also available by Binns 2012, who have conducted a systematic review on effectiveness of low vision service provision.
Problems with generalisability of results from systematic reviews of low‐vision aids
A further complication is that reading performance using electronic or optical devices might potentially be confounded by participant characteristics such as age, physical and mental health, and the type and severity of low vision. The type of task can also make a difference; tasks such as reading mail do not require long reading duration or a fast reading speed, while reading a magazine or a newspaper involves longer reading duration, and reading speed is more critical to complete the task. It is therefore important that authors of future studies provide details on these characteristics.
Another question is whether or not a participant's ability to use all of the LVAs under investigation should be an inclusion criterion for reading performance studies. In fact, reading speed as an outcome measure is nested in the ability to read. This methodological problem is similar to that of outcome‐based subgroup analysis in Hirji 2009. In studies testing several devices on the same participant, some may be able to read with one device but not with others if the devices do not provide the same magnification. As a result, a missing data problem with group imbalance may arise for reading acuity if many more participants are unable to read with a specific, usually low‐magnification, device. Whether to match for appropriate magnification depends on the research question, particularly whether people with low vision use devices with optimal magnification (i.e. enabling them to read standard print size), and surveys may be more appropriate than randomised controlled trials to investigate this question.
Other questions include whether or not devices are cost‐effective and effective in the long term.
Sample sizes were small, with 10 out of 13 studies involving fewer than 40 participants. No study reported sample size calculation. Nonetheless, cross‐over trials are more powerful than a two‐parallel‐arm study of equal sample size. The equivalent sample size can be obtained by multiplying sample size (N) by 1/(1‐R), where R is the correlation coefficient between repeated measures in the same participant. In the studies included in this review for which R could be computed, the efficiency ranged from 3 times (R = 0.66 in Kleweno 2001) to 12 times (R = 0.92 in Ortiz 1999) that of an equally sized two‐parallel‐arm trial. However, the gain in power is counterbalanced by a number of potential issues, including generalisability of the findings if conducted using a small sample of homogeneous participants.
Quality of the evidence
In the original version of this review, we judged that randomisation technique and allocation concealment were of good quality in only three studies. However, in the following updated version we decided that there is no risk of selection bias in studies testing several LVAs on the same participant in the same session, so we scored all studies as being at low risk of bias for this item. We maintained this decision in the current update.
We did not consider masking of participants, study personnel and outcome assessors, since this is not possible with most LVAs, and it may be meaningless for secondary outcomes such as preference‐based measures. Only one study evaluating prism spectacles declared masking participants, care providers or outcome assessors.
Quality issues specific to cross‐over‐like trials were unclear because of poor reporting. We suggest that the risk of bias is likely to be low or moderate in the included studies. Simultaneous testing of devices avoids the risk of a period effect or a change of disease status between cross‐over phases. The interventions should have limited carry‐over effect, but this was formally assessed in only one study. Repeated testing may have induced learning effect or fatigue. Most studies addressed the issue of training regarding learning effects and seemed to reproduce testing conditions similar to the current LVA rehabilitation practice. No firm conclusion is possible. Methodological studies have shown that insufficient reporting often makes quality assessment of cross‐over trials difficult (Elbourne 2002).
We were conscious that we could not assess inconsistency because only one or few studies were available for each comparison. However, we did not specifically downgrade the certainty of the evidence for this. In many cases, effect estimates were imprecise, and we downgraded for imprecision. We also considered that we could not be sure how much we could generalise from very small studies, and we downgraded for this as well.
Potential biases in the review process
Small studies are typical of low‐vision rehabilitation, and we cannot exclude the possibility that other small studies exist in the grey literature. Noticeably, two other reviews, described below, did not find any additional studies that met our inclusion criteria.
Agreements and disagreements with other studies or reviews
Although the purpose of this review was not to systematically search for other systematic reviews, we found two others on the use of low vision aids (Hooper 2008; VA HTA 2003), one review on the use of prisms (Markowitz 2013), and a broad purpose review on low vision service provision (Binns 2012).
VA HTA 2003 is a health technology assessment conducted by the US Veteran Affairs and available at www.va.gov/VATAP/docs/OpticalDevicesAdultsLowVision2003tm.pdf. The review included studies assessing the use of devices for reading and driving, and it included 11 studies. Regarding reading data, VA HTA 2003 included seven studies of which three were also in our review (Goodrich 2001; Spitzberg 1995; Stelmack 1991). Two studies included participants with hemianopia or stroke (Kuyk 1990; Rossi 1990, respectively). Lavinsky 2001 tried to enhance visual fields perception rather than reading performance, and Cheng 2001 compared different prisms. The authors concluded that the evidence for the use of LVAs is insufficient.
Hooper 2008 reviewed studies assessing any type of rehabilitation intervention in people with low vision, including rehabilitation programmes. They included five studies also used in our review (Culham 2004; Eperjesi 2004; Goodrich 2001; Smith 2005; Stelmack 1991), as well as a number of studies investigating rehabilitation programmes and other studies not included in our review because of study design. They concluded that "no single device emerges as the most effective device in people with AMD, because no device provides an identical level of functionality to another, nor do device users have precisely the same needs and expectations. Other differentiating factors include cost, ease of use, versatility, safety, universality, cosmetics, availability, serviceability, practicality, and adaptability". They also commented that "there appears to be no particular advantage in using one optical low‐vision aid over another and no apparent advantage in using electronic magnification systems over conventional optical devices".
We cannot formally compare the results of our review with the two mentioned above concerning quantitative findings, because there were differences in inclusion criteria, and their conclusions were broad, rather than focused on specific comparisons. Nonetheless, we largely agree with Hooper 2008 on the views quoted above, since we also found it hard to constrain the complexity of the use of each type of low‐vision aid, by participants with different needs and characteristics, to a single psychophysical measure of performance such as reading speed.
Markowitz 2013 conducted a systematic review to assess the effect of prisms for vision rehabilitation in people with macular function loss, including three randomised studies and six non‐randomised studies or case series (727 participants). The primary outcome was distance visual acuity, which improved by −0.158 logMAR (95% CI 0.014 to 0.302 logMAR) in people wearing a prismatic correction. These results are not comparable with ours since we assessed reading ability and not visual acuity, and their interpretation is also made difficult by the inclusion of non‐randomised studies and case series.
Binns 2012 has conducted a broad scope systematic review of effectiveness of low vision service provision. The results of this review are also difficult to compare with ours, since the presentation of quantitative results was not standard and review authors did not attempt any meta‐analysis. They found 58 studies that met their liberal inclusion criteria, only seven of which were randomised controlled trials. They concluded that "although the literature is sufficient to confirm that rehabilitation services result in improved clinical and functional ability outcomes, the effects on mood, vision‐related quality of life (QoL) and health‐related QoL are less clear". They also concluded that "the number of well‐designed and adequately reported studies is pitifully small; visual rehabilitation research needs higher quality research".
Smallfield 2013 conducted a systematic review of the available evidence regarding the effectiveness of occupational therapy interventions for improving the reading performance of older adults with low vision. The authors found 32 studies and concluded there was strong evidence supporting low vision programs that included occupational therapy and moderately strong evidence supporting the use of electronic magnification. However, Smallfield 2013 reported the results narratively and their results are difficult to compare with those of our review.
Authors' conclusions
Implications for practice.
While provision of low‐vision aids is useful for accessing smaller print sizes, there is insufficient evidence that a specific type of device allows faster reading speeds than other devices.
Two small studies found low‐certainty evidence that stand‐based CCTV and hand‐held CCTV allows faster reading of ordinary print size than optical devices. However, better reading speed should be matched with portability, ease of use and affordability. Furthermore, it is unclear how we can identify the people who benefit more with electronic devices, some of which are more costly than optical devices. The technology of electronic devices may have improved since these studies took place.
One study found that prism spectacles are unlikely to be beneficial for people with AMD, although the data did not allow calculation of precise estimates of performance.
Implications for research.
Low‐vision researchers who design studies comparing reading performance using different LVAs consider a cross‐over‐like design appropriate. The advantage of this design is its greater efficiency compared to parallel‐arms studies. However, poor reporting of cross‐over trials is a limitation for systematic reviews and meta‐analyses.
Moreover, we suggest that results from parallel‐group randomised controlled studies are easier to interpret than cross‐over‐like studies in people with low vision. The need for a larger sample size in parallel‐group studies makes them substantially more costly than cross‐over‐like studies. On the other hand, the inclusion of a large number of people may favour generalisability of the results.
Reasearchers should consider that important determinants of reading performance with respect to the optical device are magnification, field of view, working distance, illumination and clarity of the optics, which all need to be taken into account when designing a study of the use of LVAs or devices. Moreover, reading performance with a device can be influenced by the duration and type of training received. We suggest that future studies consider training as a fundamental component of the study design and its reporting.
We recognise that achieving better reading speed is only one of the desirable properties of an LVA compared to another. Researchers should also assess ease of use, frequency of use, sustained use and satisfaction by means of validated tools. Other considerations that are important to patients are physical comfort, weight, cosmesis and cost. Success in using an LVA may also be dependent on a person's needs and the training received, as well as other components of a multidisciplinary low‐vision rehabilitation approach (Langelaan 2007). We refer to Binns 2012 and to Rubin 2013 for a broader discussion on outcome measures in low vision research.
The authors of this review believe that low‐vision research should take into account the complexity of visual rehabilitation, including the impact of low‐vision rehabilitation on an individual's daily functioning and quality of life. This would require a qualitative or mixed methods approach. A Cochrane Review focusing on vision or health‐related quality of life outcomes and grouping interventions into broad categories, ranging from psychological therapies to methods of enhancing vision will soon be published (Langelaan 2007). There is a need for reviews with such a broad scope; however, we also need primary research that recognises the complexity of low vision rehabilitation and measures long‐term, patient‐centred outcomes.
What's new
| Date | Event | Description |
|---|---|---|
| 12 January 2018 | New search has been performed | Electronic searches updated |
| 12 January 2018 | New citation required but conclusions have not changed | This update includes three new studies (Jackson 2017; Morrice 2017; Taylor 2017). |
History
Protocol first published: Issue 4, 2001 Review first published: Issue 4, 2006
| Date | Event | Description |
|---|---|---|
| 9 October 2013 | New search has been performed | 2013, Issue 10: Searches updated: one additional trial (Watson 2005) has been included in the review; risk of bias tables have been completed for all trials and the text of the review has been updated. |
| 3 October 2013 | New citation required but conclusions have not changed | 2013, Issue 10: Two new authors, Lori Grover and Sharon Bentley, have joined the review team for this update. |
| 27 October 2008 | Amended | Converted to new review format. |
| 14 July 2006 | New citation required and conclusions have changed | Substantive amendment |
Acknowledgements
For the original version and the updates of this review we thank the following study authors for providing additional data on their studies: Stelmack 2005 (pers comm); Culham 2005 (pers comm); Goodrich 2007 (pers comm); Wolffsohn 2003 who provided data on Peterson 2003; Jackson 2017 (pers comm); Dickinson C 2017 (pers comm) who provided data on Taylor 2017. Johnson 2017 who provided data on Morrice 2017.
For the 2013 update (Virgili 2013), we thank Lori Grover for co‐authoring and Harold Burton, a low‐vision aid user for commenting on the plain language summary, abstract and conclusions.
We are grateful to Louise Culham, Gary Rubin, Roberta Scherer, Alicja Rudnicka and Catey Bunce for peer review comments on earlier versions of this review. We thank Michael Crossland, Keziah Latham, Ersilia Lucenteforte and Andrew Miller for their comments on the 2018 update.
We thank Cochrane Eyes and Vision (CEV) editorial staff, Anupa Shah and Iris Gordon, for their assistance with the search strategies and general support throughout the review process. Elizabeth Hawes contributed to the original idea and early work on the protocol for this review.
Appendices
Appendix 1. CENTRAL search strategy
#1 MeSH descriptor: [Vision, Low] explode all trees #2 low near/2 vision* #3 MeSH descriptor: [Visually Impaired Persons] explode all trees #4 MeSH descriptor: [Blindness] explode all trees #5 MeSH descriptor: [Hemianopsia] explode all trees #6 hemianop* or quadrantanop* or amauros* #7 (handicap* or disabil* or disabl* or impair* or partial*) near/3 vision* #8 (handicap* or disabil* or disabl* or impair* or partial*) near/3 visual* #9 (handicap* or disabil* or disabl* or impair* or partial*) near/3 sight* #10 #1 or #2 or #3 or #4 or #5 or #6 or #7 or #8 or #9 #11 MeSH descriptor: [Lenses] this term only #12 MeSH descriptor: [Optics and Photonics] this term only #13 MeSH descriptor: [Optical Devices] this term only #14 "low vision aid" #15 MeSH descriptor: [Reading] explode all trees #16 (aid* or device* or instrument* or equipment or apparatus) near/3 read* #17 (aid* or device* or instrument* or equipment or apparatus) near/3 optic* #18 telescop* or magnifi* or binocular* #19 MeSH descriptor: [User‐Computer Interface] this term only #20 MeSH descriptor: [Computer Graphics] explode all trees #21 MeSH descriptor: [Image Enhancement] explode all trees #22 MeSH descriptor: [Programming Languages] this term only #23 MeSH descriptor: [Software] this term only #24 MeSH descriptor: [Software Design] this term only #25 MeSH descriptor: [Semantics] this term only #26 MeSH descriptor: [Data Display] this term only #27 MeSH descriptor: [Hypermedia] this term only #28 MeSH descriptor: [Image Processing, Computer‐Assisted] this term only #29 MeSH descriptor: [Signal Processing, Computer‐Assisted] this term only #30 MeSH descriptor: [Microcomputers] this term only #31 MeSH descriptor: [Computer Terminals] this term only #32 MeSH descriptor: [Sensory Aids] this term only #33 MeSH descriptor: [Communication Aids for Disabled] this term only #34 MeSH descriptor: [Audiovisual Aids] this term only #35 MeSH descriptor: [Self‐Help Devices] this term only #36 MeSH descriptor: [Equipment Design] this term only #37 assistive near/2 (technolog* or product*) #38 electronic vision enhancement #39 EVES #40 screen near/2 (reader* or magnif*) #41 software near/2 (reader* or magnif*) #42 image near/2 (enhance* or camera* or monitor*) #43 view* near/2 (enhance* or camera* or monitor*) #44 optical character recognition #45 haptic icon* #46 closed‐circuit television or CCTV or video or scanner #47 MeSH descriptor: [Cell Phones] this term only #48 MeSH descriptor: [Mobile Applications] this term only #49 phone* next (smart or cell) #50 smartphone* or cellphone* #51 hand next held next device* #52 ipad or tablet #53 #19 or #20 or #21 or #22 or #23 or #24 or #25 or #26 or #27 or #28 or #29 or #30 or #31 or #32 or #33 or #34 or #35 or #36 or #37 or #38 or #39 or #40 or #41 or #42 or #43 or #44 or #45 or #46 or #47 or #48 or #49 or #50 or #51 or #52
Appendix 2. MEDLINE Ovid search strategy
1. randomized controlled trial.pt. 2. (randomized or randomised).ab,ti. 3. placebo.ab,ti. 4. dt.fs. 5. randomly.ab,ti. 6. trial.ab,ti. 7. groups.ab,ti. 8. or/1‐7 9. exp animals/ 10. exp humans/ 11. 9 not (9 and 10) 12. 8 not 11 13. exp vision low/ 14. (low adj2 vision$).tw. 15. exp visually impaired persons/ 16. exp blindness/ 17. exp hemianopsia/ 18. hemianop$.tw. 19. exp quadrantanopsia/ 20. quadrantanop$.tw. 21. amauros$.tw. 22. ((handicap$ or disabil$ or disabl$ or impair$ or partial$) adj3 vision$).tw. 23. ((handicap$ or disabil$ or disabl$ or impair$ or partial$) adj3 visual$).tw. 24. ((handicap$ or disabil$ or disabl$ or impair$ or partial$) adj3 sight$).tw. 25. or/13‐24 26. Lenses/ 27. "Optics and Photonics"/ 28. Optical Devices/ 29. "low vision aid$".tw. 30. exp reading/ 31. ((aid$ or device$ or instrument$ or equipment or apparatus) adj3 read$).tw. 32. ((aid$ or device$ or instrument$ or equipment or apparatus) adj3 optic$).tw. 33. (telescop$ or magnifi$ or binocular$).tw. 34. user‐computer interface/ 35. exp Computer Graphics/ 36. Image Enhancement/ 37. Programming Languages/ 38. Software/ 39. Software Design/ 40. Semantics/ 41. Data Display/ 42. Hypermedia/ 43. Image Processing, Computer‐Assisted/ 44. Signal Processing, Computer‐Assisted/ 45. Microcomputers/ 46. Computer Terminals/ 47. Sensory Aids/ 48. Communication Aids for Disabled/ 49. Audiovisual Aids/ 50. Self‐Help Devices/ 51. Equipment Design/ 52. (assistive adj2 (technolog$ or product$)).tw. 53. electronic vision enhancement.tw. 54. EVES.tw. 55. (screen adj2 (reader$ or magnif$)).tw. 56. (software adj2 (reader$ or magnif$)).tw. 57. (image adj2 (enhance$ or camera$ or monitor$)).tw. 58. (view$ adj2 (enhance$ or camera$ or monitor$)).tw. 59. optical character recognition.tw. 60. haptic icon$.tw. 61. (closed‐circuit television or CCTV or video or scanner).tw. 62. Cell Phones/ 63. Mobile Applications/ 64. (phone$ adj1 (smart or cell)).tw. 65. (smartphone$ or cellphone$).tw. 66. (hand adj1 held device$).tw. 67. (ipad or tablet).tw. 68. or/26‐67 69. 25 and 68
The search filter for trials at the beginning of the MEDLINE strategy is from the published paper by Glanville 2006.
Appendix 3. Embase Ovid search strategy
1. exp randomized controlled trial/ 2. exp randomization/ 3. exp double blind procedure/ 4. exp single blind procedure/ 5. random$.tw. 6. or/1‐5 7. (animal or animal experiment).sh. 8. human.sh. 9. 7 and 8 10. 7 not 9 11. 6 not 10 12. exp clinical trial/ 13. (clin$ adj3 trial$).tw. 14. ((singl$ or doubl$ or trebl$ or tripl$) adj3 (blind$ or mask$)).tw. 15. exp placebo/ 16. placebo$.tw. 17. random$.tw. 18. exp experimental design/ 19. exp crossover procedure/ 20. exp control group/ 21. exp latin square design/ 22. or/12‐21 23. 22 not 10 24. 23 not 11 25. exp comparative study/ 26. exp evaluation/ 27. exp prospective study/ 28. (control$ or prospectiv$ or volunteer$).tw. 29. or/25‐28 30. 29 not 10 31. 30 not (11 or 23) 32. 11 or 24 or 31 33. low vision/ 34. visual impairment/ 35. blindness/ 36. (low adj2 vision$).tw. 37. hemianopia/ 38. hemianop$.tw. 39. quadrantanop$.tw. 40. amauros$.tw. 41. ((handicap$ or disabil$ or disabl$ or impair$ or partial$) adj3 vision$).tw. 42. ((handicap$ or disabil$ or disabl$ or impair$ or partial$) adj3 visual$).tw. 43. ((handicap$ or disabil$ or disabl$ or impair$ or partial$) adj3 sight$).tw. 44. or/33‐43 45. exp visual aid/ 46. general medical device/ 47. optics/ 48. optical instrumentation/ 49. "low vision aid$".tw. 50. exp reading/ 51. ((aid$ or device$ or instrument$ or equipment or apparatus) adj3 read$).tw. 52. ((aid$ or device$ or instrument$ or equipment or apparatus) adj3 optic$).tw. 53. (telescop$ or magnifi$ or binocular$).tw. 54. computer interface/ 55. computer graphics/ 56. image enhancement/ 57. computer language/ 58. semantics/ 59. information processing/ 60. hypermedia/ 61. image processing/ 62. signal processing/ 63. microcomputer/ 64. computer terminal/ 65. sensory aid/ 66. communication aid/ 67. audiovisual aid/ 68. self help/ 69. equipment design/ 70. (assistive adj2 (technolog$ or product$)).tw. 71. electronic vision enhancement.tw. 72. EVES.tw. 73. (screen adj2 (reader$ or magnif$)).tw. 74. (software adj2 (reader$ or magnif$)).tw. 75. (image adj2 (enhance$ or camera$ or monitor$)).tw. 76. (view$ adj2 (enhance$ or camera$ or monitor$)).tw. 77. optical character recognition.tw. 78. haptic icon$.tw. 79. (closed‐circuit television or CCTV or video or scanner).tw. 80. mobile phone/ 81. smartphone/ 82. mobile application/ 83. (phone$ adj1 (smart or cell)).tw. 84. (smartphone$ or cellphone$).tw. 85. (hand adj1 held device$).tw. 86. (ipad or tablet).tw. 87. or/45‐86 88. 44 and 87
Appendix 4. LILACS search strategy
visual impairment OR low vision and reading OR aid$ OR technology OR computer OR tablet OR software OR electronic OR device OR phone OR smartphone OR cellphone OR camera OR monitor OR Telescope OR Magnifier OR CCTV OR closed circuit OR closed‐circuit OR cctv$ OR video$ OR computer$ OR scanner$
Appendix 5. OpenGrey search strategy
("Visual Impairment" OR "Low Vision") AND (Reading OR Aid OR Technology OR Computer OR Tablet OR Software OR Electronic OR Device OR Phone OR Camera OR Monitor OR Telescope OR Magnifier OR CCTV)
Appendix 6. ISRCTN search strategy
"Visual Impairment" OR "Low Vision" within Interventions: Reading OR Aid OR Technology OR Computer OR Tablet OR Software OR Electronic OR Device OR Phone OR Camera OR Monitor OR Telescope OR Magnifier OR CCTV)
Appendix 7. ClinicalTrials.gov search strategy
visual impairment OR low vision = Condition or disease
reading OR aid OR technology OR computer OR tablet OR software OR electronic OR device OR phone OR smartphone OR cellphone OR camera OR monitor OR Telescope OR Magnifier OR CCTV OR closed circuit OR video OR computer OR scanner = other term
Appendix 8. WHO ICTRP search strategy
low vision AND Reading OR low vision AND Aid OR low vision AND Technology OR low vision AND Computer OR low vision AND Tablet OR low vision AND Software OR low vision AND Electronic OR low vision AND Device OR low vision AND Phone OR low vision AND Camera OR low vision AND Monitor OR low vision AND Telescope OR low vision AND Magnifier OR low vision AND CCTV OR low vision AND closed circuit OR low vision AND closed‐circuit OR low vision AND video OR low vision AND scanner
visual impairment AND Reading OR visual impairment AND Aid OR visual impairment AND Technology OR visual impairment AND Computer OR visual impairment AND Tablet OR visual impairment AND Software OR visual impairment AND Electronic OR visual impairment AND Device OR visual impairment AND Phone OR visual impairment AND Camera OR visual impairment AND Monitor OR visual impairment AND Telescope OR visual impairment AND Magnifier OR visual impairment AND CCTV OR visual impairment AND closed circuit OR visual impairment AND closed‐circuit OR visual impairment AND video OR visual impairment AND scanner
Appendix 9. Additional data extraction and statistical issues
Sample size and multiplicity issues
If more than two LVAs were simultaneously compared in a publication (Culham 2004; Eperjesi 2004; Goodrich 2001; Smith 2005), 95% confidence intervals (CI) of the estimates of effectiveness were adjusted using a conservative Bonferroni approach. As an example, performing three pairwise comparisons among three LVAs, such as in Goodrich 2001, requires that 95% CIs are calculated dividing the conventional probability of type I error of 0.05 by 3. The adjusted probability is therefore 0.0167. Furthermore, sample size was small in most studies, suggesting the use of a t‐distribution to compute confidence intervals. To exploit the intuitive graphical presentation allowed by Review Manager 5 (RevMan), which uses the Gaussian distribution and therefore large sample statistics (> 30 people) while maintaining their correct coverage, we inflated the SE(MD) by an appropriate factor. Using Goodrich 2001 as an example, this factor was estimated as follows.
The t‐value with the appropriate degrees of freedom (22 participants, df = 21) corresponding to a two‐tailed probability of 0.0167 is 2.60.
The SE(MD) is obtained from the paper.
Since the z‐value of 1.96 is used as a multiplier of the SE(MD) in RevMan to obtain the 95% CI, the factor used to inflate the SE(MD) is computed from the ratio 2.60/1.96 = 1.33.
Finally, the inflated SE is introduced in the 'Comparisons and data' RevMan tool in order to present forest plots that accommodate both the multiple comparisons (if any) and the small‐sample statistical issues.
Correlation in cross‐over studies
In Culham 2004 the mean and the standard deviation (SD) for each of the four head‐mounted electronic devices compared to the participant's optical device were available. The SE(MD), which is necessary to extract data from cross‐over studies, were not presented. According to Higgins 2011b the SE(MD) can still be estimated provided that the correlation coefficient among measurements is known from similar studies. The correlation coefficient for reading speed between the stand‐mounted CCTV and the electronic head‐mounted device (HMD) was 0.92 in Ortiz 1999, while it was 0.66 in Kleweno 2001, who used the Virtual Retinal Display as an HMD, as derived from published individual data. We used an intermediate value of 0.82 as an estimate of the correlation coefficient in Culham 2004, Goodrich 2001 and Peterson 2003. This is a conservative assumption since the type of HMD in Culham 2004 is more similar to Ortiz 1999 and considering that a lower correlation coefficient within participants leads to larger standard errors in cross‐over studies. This can be calculated from the formulas suggested by Deeks 2011, which we used to compute the SE(MD).
Problems with data skewness
As suggested by Deeks 2011, we chose not to extract data from Stelmack 1991 since there was evidence of marked skewness, with the standard deviations being larger than the mean in at least one group, and taking into consideration that reading speed cannot take negative values. Skewness was also suggested by the asymmetry of the mean within the reported range of values.
In the first version of this review, individual reading speed data from Eperjesi 2004 were log‐transformed to approach normality before undertaking calculations. In the 2011 update, we decided to use raw data (words per minute) since skewness was mild and results are more interpretable on this scale.
Analyses of individual data
In three publications (Eperjesi 2004; Kleweno 2001; Ortiz 1999), individual data were available in tables in the published reports. They were processed with repeated‐measures techniques to obtain MD and SE(MD) using the Stata 9.2 software (StataCorp, College Station, Texas, USA). A paired t‐test was used when two LVAs were compared, and generalised estimating equations were used when more than two groups were compared. These techniques allowed estimates of SEs(MD) to be obtained that are adjusted for the correlation among measurements in the same participant. We used the Huber‐White variance estimator for this purpose.
Data and analyses
Comparison 1. Electronic device (various types of CCTV) versus optical device.
| Outcome or subgroup title | No. of studies | No. of participants | Statistical method | Effect size |
|---|---|---|---|---|
| 1 Reading speed (words per minute) | 3 | Mean difference (Fixed, 95% CI) | Totals not selected | |
| 1.1 Stand‐mounted CCTV versus participant's optical device | 1 | Mean difference (Fixed, 95% CI) | 0.0 [0.0, 0.0] | |
| 1.2 Stand‐mounted CCTV versus best prescribed optical device | 1 | Mean difference (Fixed, 95% CI) | 0.0 [0.0, 0.0] | |
| 1.3 Mouse‐based device (27'' TV monitor) versus best prescribed optical device | 1 | Mean difference (Fixed, 95% CI) | 0.0 [0.0, 0.0] | |
| 1.4 Mouse‐based device (14'' monitor) versus participant's optical device | 1 | Mean difference (Fixed, 95% CI) | 0.0 [0.0, 0.0] | |
| 1.5 Mouse‐based head‐mounted device versus participant's optical device | 1 | Mean difference (Fixed, 95% CI) | 0.0 [0.0, 0.0] | |
| 1.6 Flipperport head‐mounted CCTV (table stand camera) versus optical device | 1 | Mean difference (Fixed, 95% CI) | 0.0 [0.0, 0.0] | |
| 1.7 Jordy head‐mounted CCTV versus optical device | 1 | Mean difference (Fixed, 95% CI) | 0.0 [0.0, 0.0] | |
| 1.8 Maxport head‐mounted CCTV versus optical device | 1 | Mean difference (Fixed, 95% CI) | 0.0 [0.0, 0.0] | |
| 1.9 NuVision head‐mounted CCTV versus optical device | 1 | Mean difference (Fixed, 95% CI) | 0.0 [0.0, 0.0] | |
| 2 Reading duration in minutes | 1 | Mean difference (Fixed, 95% CI) | Totals not selected | |
| 2.1 Stand CCTV versus optical device | 1 | Mean difference (Fixed, 95% CI) | 0.0 [0.0, 0.0] | |
| 2.2 Hand‐held CCTV versus optical device | 1 | Mean difference (Fixed, 95% CI) | 0.0 [0.0, 0.0] |
1.1. Analysis.
Comparison 1 Electronic device (various types of CCTV) versus optical device, Outcome 1 Reading speed (words per minute).
1.2. Analysis.
Comparison 1 Electronic device (various types of CCTV) versus optical device, Outcome 2 Reading duration in minutes.
Comparison 2. Hand‐held (not mouse‐based) electronic devices plus optical devices versus optical devices alone.
| Outcome or subgroup title | No. of studies | No. of participants | Statistical method | Effect size |
|---|---|---|---|---|
| 1 Reading speed (words per minute) | 1 | Mean Difference (Fixed, 95% CI) | Totals not selected | |
| 2 Frequency of use (0‐4 scale) | 1 | Mean Difference (Fixed, 95% CI) | Totals not selected | |
| 3 Quality of life | 1 | Mean Difference (Fixed, 95% CI) | Totals not selected |
Comparison 3. Stand‐based CCTV plus visual rehabilitation versus visual rehabilitation alone.
| Outcome or subgroup title | No. of studies | No. of participants | Statistical method | Effect size |
|---|---|---|---|---|
| 1 Maximum reading speed (words per minute) | 1 | Mean Difference (IV, Fixed, 95% CI) | Totals not selected |
Comparison 4. Stand‐mounted CCTV versus head‐mounted electronic device.
| Outcome or subgroup title | No. of studies | No. of participants | Statistical method | Effect size |
|---|---|---|---|---|
| 1 Reading speed (words per minute) | 3 | Mean difference (Fixed, 95% CI) | 3.13 [‐3.47, 9.73] | |
| 2 Reading acuity (logMAR) | 1 | Mean difference (Fixed, 95% CI) | Totals not selected |
4.1. Analysis.
Comparison 4 Stand‐mounted CCTV versus head‐mounted electronic device, Outcome 1 Reading speed (words per minute).
Comparison 5. Stand‐mounted CCTV versus hand‐held, mouse‐based electronic device.
| Outcome or subgroup title | No. of studies | No. of participants | Statistical method | Effect size |
|---|---|---|---|---|
| 1 Reading speed (words per minute) | 2 | Mean difference (Fixed, 95% CI) | 9.54 [‐0.27, 19.36] | |
| 2 Reading duration in minutes | 1 | Mean difference (Fixed, 95% CI) | Totals not selected |
Comparison 6. Diffractive spectacle mounted magnifiers vs control.
| Outcome or subgroup title | No. of studies | No. of participants | Statistical method | Effect size |
|---|---|---|---|---|
| 1 MNREAD maximum reading speed (words per minute) | 1 | Mean Difference (Fixed, 95% CI) | Totals not selected | |
| 1.1 Diffractive versus refractive‐aspheric spectacle magnifier | 1 | Mean Difference (Fixed, 95% CI) | 0.0 [0.0, 0.0] | |
| 1.2 Diffractive versus aplanatic spectacle magnifier | 1 | Mean Difference (Fixed, 95% CI) | 0.0 [0.0, 0.0] | |
| 2 MNREAD critical print size (M print size) | 1 | Mean Difference (Fixed, 95% CI) | Totals not selected | |
| 2.1 Diffractive versus refractive‐aspheric spectacle magnifier | 1 | Mean Difference (Fixed, 95% CI) | 0.0 [0.0, 0.0] | |
| 2.2 Diffractive versus aplanatic spectacle magnifier | 1 | Mean Difference (Fixed, 95% CI) | 0.0 [0.0, 0.0] | |
| 3 Morgan Low Vision Reading Comprehension Assessment | 1 | Mean Difference (Fixed, 95% CI) | Totals not selected | |
| 3.1 Diffractive versus refractive‐aspheric spectacle magnifier | 1 | Mean Difference (Fixed, 95% CI) | 0.0 [0.0, 0.0] | |
| 3.2 Diffractive versus aplanatic spectacle magnifier | 1 | Mean Difference (Fixed, 95% CI) | 0.0 [0.0, 0.0] |
Comparison 7. Prism spectacles versus conventional spectacles.
| Outcome or subgroup title | No. of studies | No. of participants | Statistical method | Effect size |
|---|---|---|---|---|
| 1 Reading speed (words per minute) | 1 | Mean difference (Fixed, 95% CI) | Totals not selected | |
| 1.1 Custom prism spectacles versus conventional spectacles | 1 | Mean difference (Fixed, 95% CI) | 0.0 [0.0, 0.0] | |
| 1.2 Standard prism spectacles versus conventional spectacles | 1 | Mean difference (Fixed, 95% CI) | 0.0 [0.0, 0.0] | |
| 2 Critical print size in logMAR | 1 | Mean difference (Fixed, 95% CI) | Totals not selected | |
| 2.1 Custom prism spectacles versus conventional spectacles | 1 | Mean difference (Fixed, 95% CI) | 0.0 [0.0, 0.0] | |
| 2.2 Standard prism spectacles versus conventional spectacles | 1 | Mean difference (Fixed, 95% CI) | 0.0 [0.0, 0.0] | |
| 3 Quality of life (NEI‐VFQ score) | 1 | Mean difference (Fixed, 95% CI) | Totals not selected | |
| 3.1 Custom prism spectacles versus conventional spectacles | 1 | Mean difference (Fixed, 95% CI) | 0.0 [0.0, 0.0] | |
| 3.2 Standard prism spectacles versus conventional spectacles | 1 | Mean difference (Fixed, 95% CI) | 0.0 [0.0, 0.0] |
Comparison 8. Overlay coloured filters versus clear filter.
| Outcome or subgroup title | No. of studies | No. of participants | Statistical method | Effect size |
|---|---|---|---|---|
| 1 Reading speed (words per minute) | 1 | Mean difference (Fixed, 95% CI) | Totals not selected | |
| 1.1 Rose filter | 1 | Mean difference (Fixed, 95% CI) | 0.0 [0.0, 0.0] | |
| 1.2 Pink filter | 1 | Mean difference (Fixed, 95% CI) | 0.0 [0.0, 0.0] | |
| 1.3 Yellow filter | 1 | Mean difference (Fixed, 95% CI) | 0.0 [0.0, 0.0] | |
| 1.4 Orange filter | 1 | Mean difference (Fixed, 95% CI) | 0.0 [0.0, 0.0] | |
| 1.5 Mint filter | 1 | Mean difference (Fixed, 95% CI) | 0.0 [0.0, 0.0] | |
| 1.6 Lime filter | 1 | Mean difference (Fixed, 95% CI) | 0.0 [0.0, 0.0] | |
| 1.7 Grey filter | 1 | Mean difference (Fixed, 95% CI) | 0.0 [0.0, 0.0] | |
| 1.8 Blue filter | 1 | Mean difference (Fixed, 95% CI) | 0.0 [0.0, 0.0] | |
| 1.9 Aqua filter | 1 | Mean difference (Fixed, 95% CI) | 0.0 [0.0, 0.0] | |
| 1.10 Purple filter | 1 | Mean difference (Fixed, 95% CI) | 0.0 [0.0, 0.0] |
Characteristics of studies
Characteristics of included studies [ordered by study ID]
Culham 2004.
| Methods | Study design: cross‐over randomised controlled trial Randomised presentation of devices. First, the clinician determined as many unique combinations of the order of showing each device and listed them. Second, an independent non‐clinician was then asked to randomly rearrange the order of the possible combinations on the list. On completion of the clinical evaluation, participants were loaned 2 of the electronic devices, each for a period of 1 week, for use at home. Masking: participant ‐ masking issues are not described but the study participants, providers and outcome assessors were likely to be unmasked given the use of recognisable devices Exclusions after randomisation: none reported Losses to follow‐up: none reported Unusual study design: within‐person design, i.e. a cross‐over study in which all participants try all 4 devices. After training the use is restricted to 2 devices per participant | |
| Participants | Country: UK Number randomised: 20 people recruited from the low‐vision clinic and specialist medical clinics at Moorfields Eye Hospital Cause of low vision: AMD (n = 10), early onset macular disease (n = 10) Age: estimated average age 58 years, range 21 to 82 Sex: 9 men, 11 women, 55% women Inclusion criteria: English‐speaking and prepared to attend 5 appointments; visual acuity between 6/18 and 1/60 in the better eye and stable vision for at least 3 months; to be experienced in the use of optical LVAs (i.e. for 1 year or more); prior to recruitment all participants had to have received standard hospital care and any medical intervention required had been completed. Exclusion criteria: any co‐existing conditions which may have affected the handling of devices or performance with them | |
| Interventions |
Intervention:
Comparator:
Duration: 1 week |
|
| Outcomes | Use of the devices for a range of clinical and practical visual tasks. Assessment was based on clinical and practical visual tasks measured in the laboratory. On completion of the clinical evaluation, devices were also loaned to participants for use in their habitual environments for a period of 1 week, on a random basis.
|
|
| Notes | Date study conducted: not reported Funding: supported by the Macular Disease Society Declaration of interest: the authors had no financial interest in any device used in the study. Trial registration number: not reported | |
| Risk of bias | ||
| Bias | Authors' judgement | Support for judgement |
| Random sequence generation (selection bias) | Low risk | Randomised presentation of devices; although no further detail was given on how randomisation sequence was generated, selection bias should be avoided since all participants used all devices (cross‐over study design) |
| Allocation concealment (selection bias) | Low risk | Randomised presentation of devices; although no further detail was given on how randomisation sequence was concealed, selection bias should be avoided since all participants used all devices (cross‐over study design) |
| Incomplete outcome data (attrition bias) All outcomes | Low risk | No loss to follow‐up reported |
| Selective reporting (reporting bias) | Low risk | No protocol available, but primary outcome reported |
| Period effect | Low risk | Stable vision required during the last 3 months to include participants |
| Carry‐over effect and period‐by‐treatment interaction | Unclear risk | No details reported |
Eperjesi 2004.
| Methods | Study design: cross‐over randomised controlled trial Masking: masking issues are not described, but study participants, providers and outcome assessors were likely to be unmasked given the use of recognisable coloured filters Exclusions after randomisation: none reported Losses to follow‐up: none reported Unusual study design: within‐person design, i.e. a cross‐over study in which all participants try all 10 coloured overlay filters and the control clear one | |
| Participants | Country: UK Number randomised: 12 consecutive participants were recruited over a 3‐month period from the Focus on Blindness Low Vision Centre in Birmingham, a charitable voluntary organisation Cause of low vision: non‐exudative AMD Age: mean age 81 years, range 70 to 87 years Sex: 3 men, 9 women, 75% women Inclusion criteria: non‐exudative AMD resulting in a relative scotoma with central fixation Exclusion criteria: near working reading acuity poorer than logMAR 1.00 (approximately equivalent to large print); crystalline opacities greater than grade 1 on the Lens Opacity Classification System; participants undergoing ophthalmological treatment | |
| Interventions |
Intervention:
Comparator:
Duration: single test session |
|
| Outcomes | Reading rate calculated as the number of correct words per minute measured with the Rate of Reading Test (printed, nonsense, lower case sans serif, stationary text) To measure reading rate, tape recordings were replayed after each testing session and each participant scored by measuring the total time taken to read each block of test print and noting the errors on a score sheet. |
|
| Notes | Date study conducted: not reported Funding: not reported Declaration of interest: the authors have no financial interest in any device or reading test used in the study. Trial registration number: not reported | |
| Risk of bias | ||
| Bias | Authors' judgement | Support for judgement |
| Random sequence generation (selection bias) | Low risk | Randomised presentation of devices; although no further detail was given on how randomisation sequence was generated, selection bias should be avoided since all participants used all devices (cross‐over study design) |
| Allocation concealment (selection bias) | Low risk | Randomised presentation of devices; although no further detail was given on how randomisation sequence was concealed, selection bias should be avoided since all participants used all devices (cross‐over study design) |
| Incomplete outcome data (attrition bias) All outcomes | Low risk | No loss to follow‐up or exclusion after randomisation reported |
| Selective reporting (reporting bias) | Low risk | No protocol available, but primary outcome reported |
| Period effect | Low risk | Participants with non‐exudative AMD were included who are expected to have stable vision in the study period |
| Carry‐over effect and period‐by‐treatment interaction | Unclear risk | No details reported |
Goodrich 2001.
| Methods | Study design: quasi‐randomised cross‐over trial Masking: masking issues are not described, but study participants, providers and outcome assessors were likely to be unmasked given the use of recognisable devices Exclusions after randomisation: none reported Losses to follow‐up: none reported Unusual study design: within‐person design, i.e. a cross‐over study in which all participants try the devices consecutively | |
| Participants | Country: USA Number randomised: 22 veterans enrolled in the residential rehabilitation programme of the Western Blind Rehabilitation Center (none with previous reading training) Cause of low vision: AMD (n = 16), CRVO (n = 2), diabetic retinopathy (n = 2), macular hole (n = 1), cone dystrophy (n = 1) Age: mean age 73 years, range 53 to 87 years Sex: 20 men, 2 women, 9% women Inclusion criteria: legal blindness; central scotoma with a intact peripheral field; stated desire for reading rehabilitation Exclusion criteria: cognitive deficits or current use of medication that would impair reading ability; illiteracy | |
| Interventions |
Intervention:
Comparator:
5 days "hands‐on" training with each of the 3 types of devices (the prescribed optical device considered as control). Eccentric viewing training preceded reading training. Duration: 15 training sessions plus sessions needed for evaluation |
|
| Outcomes | Reading speed using paragraphs of 250 words in Times New Roman (1 M font) with 5th‐grade difficulty reading comprehension assessed with 5 question for each paragraph; Reading duration during each training session; Participants' preferences for a specific device with forced and open‐ended questions | |
| Notes | Date study conducted: not reported Funding: supported by a grant from Innovations Inc and the Veteran Afffairs Palo Alto HEalth Care System Declaration of interest: not reported Trial registration number: not reported | |
| Risk of bias | ||
| Bias | Authors' judgement | Support for judgement |
| Random sequence generation (selection bias) | Low risk | Quasi‐randomised study: the order of presentation of the devices was rotated for consecutive participants; despite this, selection bias should be avoided since all participants used all devices (cross‐over nature of the study design) |
| Allocation concealment (selection bias) | Low risk | Order of randomisation can be foreseen because rotation was used; despite this, selection bias should be avoided since all participants used all devices (cross‐over nature of the study design) |
| Incomplete outcome data (attrition bias) All outcomes | Low risk | No loss to follow‐up or exclusion after randomisation reported |
| Selective reporting (reporting bias) | Low risk | No protocol available, but primary outcome reported |
| Period effect | Low risk | No details reported, but same‐session, short duration testing made this type of bias unlikely |
| Carry‐over effect and period‐by‐treatment interaction | Unclear risk | No details reported |
Jackson 2017.
| Methods | Study design: parallel group randomised controlled trial Masking: not reported, but not possible for these interventions Losses to follow‐up: 7 withdrawals, 2 in intervention group and 5 in comparator (4 in comparator group at 1 month) Unusual study design: no | |
| Participants | Country: USA Number randomised: 37 people with central field loss recruited at the multidisciplinary outpatient vision rehabilitation clinic at the Massachusetts Eye and Ear Hospital Cause of low vision: AMD or juvenile onset macular degeneration (n = 27), optic nerve disease (n = 6), macular dystrophy or other maculopathy (n = 4) Age: mean age 73 years, range 40 to 91 years Sex: 19 men, 18 women, 49% women Inclusion criteria: age ≥ 40 years, central visual field loss, visual acuity worse than 20/40 in each eye and better than 20/400 in the better seeing eye, cumulative score of > 20 (of 30) on the 6‐question modified Mini Mental State Examination (MMSE) questionnaire for visually impaired, sufficient hearing to participate in interviews, and no previous experience with vision rehabilitation or video camera magnifiers. Exclusion criteria: none | |
| Interventions |
Intervention:
Comparator:
All participants underwent an initial vision rehabilitation consultation, during which patients were educated about rehabilitation strategies, given information about remaining visual function, and shown a range of optical and electronic devices, which they could purchase. Patients in the video magnifier group received a free desk video magnifier when they presented for initial consultation. Patients in the visual rehabilitation group were free to purchase devices at any time, and they were advised that they would also receive a free video magnifier after the completion of rehabilitation training with an occupational therapist. Everyone returned after 1 month to begin an occupational therapy evaluation and subsequent training. Duration: 1 month |
|
| Outcomes | Reading speed assessed in words per minute (wpm) using the International Reading Speed Texts (IReST); quality of life and self‐perceived visual functioning using the Impact of Vision Impairment questionnaire (IVI) and 10 reading questions from the Activity Inventor. Results were evaluated at enrolment, when all participants used pre‐rehabilitation devices, and at 1 month after enrolment, when participants who had had access to a video magnifier completed reading assessment using the video magnifier. Planned 1 year follow‐up not reported. |
|
| Notes | Date study conducted: February 2010 to May 2011 Funding: devices provided by Optelec USA Declaration of interest: not reported Trial registration number: NCT01670643 | |
| Risk of bias | ||
| Bias | Authors' judgement | Support for judgement |
| Random sequence generation (selection bias) | Low risk | Computer‐generated numerical series |
| Allocation concealment (selection bias) | Low risk | Randomisation "was assigned at the initial consultation when the subject signed consent" (author's information) |
| Incomplete outcome data (attrition bias) All outcomes | Unclear risk | 6 out of 36 participants were lost to follow‐up at one month due to withdrawals, of which 2 in the intervention group and 4 in the comparator group, with causes of withdrawal not reported |
| Selective reporting (reporting bias) | Low risk | Pre‐specified outcomes on Clinical Trials registry entry include objective and subjective reading tests and standard international tool was used (IReST) |
Kleweno 2001.
| Methods | Study design: cross‐over randomised controlled trial Masking: masking issues are not described, but study participants, providers and outcome assessors were likely to be unmasked given the use of recognisable devices Exclusions after randomisation: 2 participants removed from the study (1 requested to be withdrawn from the testing because of fatigue, 1 was unable to locate the VRD exit pupil and maintain a stable image on the small functional portions of peripheral retina) Losses to follow‐up: none reported Unusual study design: within‐person design, i.e. a cross‐over study in which all participants try the 2 devices consecutively | |
| Participants | Country: USA Number randomised: 13 low‐vision volunteers selected to represent the broad range of partially sighted individuals actively involved in the work force Cause of low vision: retinal (n = 7), optical (n = 3), amblyopic (n = 2) or unknown (n = 1) conditions. There were no AMD cases. Age: mean age 41 years, range 28 to 59 years Sex: not reported Inclusion criteria: either actively employed or in graduate school Exclusion criteria: none | |
| Interventions |
Intervention:
Comparator:
Duration: single test session |
|
| Outcomes | Reading speed, measured with a unique reading speed test based on the Minnesota Low‐Vision Reading test (MNREAD). 3 words at a time were presented to the participant in an unrelated manner. Subjective preference for 1 of the devices: at the conclusion of the reading tests, participants were asked to rate the VRD as "better, the same, or worse than the CRT'' in terms of perceived brightness and perceived clarity | |
| Notes | Date study conducted: not reported Funding: supported by the National Science Foundation (award #9801294) and Howard Hughes Medical Institute Declaration of interest: not reported Trial registration number: not reported | |
| Risk of bias | ||
| Bias | Authors' judgement | Support for judgement |
| Random sequence generation (selection bias) | Low risk | Randomised presentation of devices; although no further detail was given on how randomisation sequence was generated, selection bias was likely to be avoided since all participants used all devices (cross‐over nature of the study design) |
| Allocation concealment (selection bias) | Low risk | Randomised presentation of devices; although no further detail was given on how randomisation sequence was concealed, selection bias should be avoided since all participants used all devices (cross‐over study design) |
| Incomplete outcome data (attrition bias) All outcomes | Low risk | No loss to follow‐up or exclusion after randomisation reported |
| Selective reporting (reporting bias) | Low risk | No protocol available, but primary outcome reported |
| Period effect | Low risk | No details reported, but same‐session, short duration testing made this type of bias unlikely. |
| Carry‐over effect and period‐by‐treatment interaction | Unclear risk | No details provided. They used a reading test based on the MNREAD, which has short duration. Nonetheless, 1 participant withdrew because of fatigue |
Morrice 2017.
| Methods | Study design: quasi randomised cross‐over trial Masking: masking issues are not described, but study participants, providers and outcome assessors were likely to be unmasked given the use of recognisable devices Exclusions after randomisation: none reported Losses to follow‐up: none reported Unusual study design: within‐person design, i.e. a cross‐over study in which all participants try the devices consecutively | |
| Participants | Country: Canada Number randomised: 100 participants from low‐vision services who were literate and cognitively capable Cause of low vision: AMD (n = 57), diabetic retinopathy (n = 6), glaucoma (n = 6), other (n = 25), unknown (n = 6) Age: estimated mean age 75 years, range 24 to 97 years Sex: 39 men, 161 women, 81% women Inclusion criteria: visual acuity better than 6/90, but worse than 6/24 in the better eye with best standard correction, as measured by the ETDRS chart, or qualify for low‐vision rehabilitation in the province of Quebec Exclusion criteria: mild cognitive impairment | |
| Interventions |
Intervention:
Comparator:
Home magnification not considered since not optimised Duration: single test session |
|
| Outcomes | Reading speed, measured with the International Reading Speed Texts (IReST) Quality of life: visual function index (VF‐14) | |
| Notes | Date study conducted: not reported Funding:Quote "This work was supported in part by the Vision Research Network, the Fonds de recherche du Québéc ‐ Santé (#28881, #30620, and #32643), the Antoine Turmel Foundation and the MAB‐Mackay Foundation." Declaration of interest: reported no conflict of interest Trial registration number: not reported | |
| Risk of bias | ||
| Bias | Authors' judgement | Support for judgement |
| Random sequence generation (selection bias) | Low risk | Order of presentation of the devices was reported to be pseudo‐randomised to reduce practice or fatigue effects (quasi‐random assignment). Although no further detail was given on how randomisation sequence was generated, selection bias should be avoided since all participants used all devices (cross‐over study design) |
| Allocation concealment (selection bias) | Low risk | Randomised presentation of devices; although no further detail was given on how randomisation sequence was concealed, selection bias should be avoided since all participants used all devices (cross‐over study design) |
| Incomplete outcome data (attrition bias) All outcomes | Low risk | No loss to follow‐up or exclusion reported |
| Selective reporting (reporting bias) | Low risk | No protocol available, but primary outcome reported |
| Period effect | Low risk | No details reported, but same‐session, short duration testing made this type of bias unlikely |
| Carry‐over effect and period‐by‐treatment interaction | Unclear risk | No details provided |
Ortiz 1999.
| Methods | Study design: quasi‐randomised cross‐over trial Masking: masking issues are not described, but study participants, providers and outcome assessors were likely to be unmasked given the use of recognisable devices Exclusions after randomisation: none reported Losses to follow‐up: none reported Unusual study design: within‐person design, i.e. a cross‐over study in which all participants try the devices consecutively | |
| Participants | Country: USA Number randomised: 10 Cause of low vision: not known Age: mean age 47 years, range 24 to 79 years Sex: not reported Inclusion criteria: proficient CCTV users Exclusion criteria: none reported | |
| Interventions |
Intervention:
Comparator:
Duration: not reported |
|
| Outcomes | Reading performance measured with an MNREAD Chart: reading speed; critical print size; reading acuity News article reading: 7 articles for each device randomly chosen form a pool of 45 Reading comprehension as measured with multiple choice questions about the article's content. | |
| Notes | Date study conducted: not reported Funding: grant from McKnight Foundation and NIH grant EY02934 and HD‐07151 Declaration of interest: not reported Trial registration number: not reported | |
| Risk of bias | ||
| Bias | Authors' judgement | Support for judgement |
| Random sequence generation (selection bias) | Low risk | Quasi‐randomised study: the order of presentation of the devices was rotated (counterbalanced) for consecutive participants; even so, selection bias should be avoided since all participants used all devices (cross‐over study design) |
| Allocation concealment (selection bias) | Low risk | Order of randomisation can be foreseen because rotation was used; despite this, selection bias was likely to be avoided since all participants used all devices (cross‐over study design) |
| Incomplete outcome data (attrition bias) All outcomes | Low risk | No loss to follow‐up or exclusion after randomisation reported |
| Selective reporting (reporting bias) | Low risk | No protocol available, but primary outcome reported |
| Period effect | Low risk | No details reported, but same‐session, short duration testing made this type of bias unlikely |
| Carry‐over effect and period‐by‐treatment interaction | Unclear risk | Authors reported they could not find a practice effect comparing the first and the last half of their tests, nor a decay of performance, but a quantitative assessment was not available |
Peterson 2003.
| Methods | Study design: cross‐over randomised controlled trial Masking: masking issues are not described, but study participants, providers and outcome assessors were likely to be unmasked given the use of recognisable devices Exclusions after randomisation: none reported Losses to follow‐up: none reported Unusual study design: within‐person design, i.e. a cross‐over study in which all participants try the devices consecutively | |
| Participants | Country: UK Number randomised: 70 people with low vision Cause of low vision: AMD (n = 40), vascular retinopathy (n = 11), diabetic retinopathy (n = 9), corneal condition (n = 6), glaucoma (n = 4) Age: mean average age 70 years, range not reported Sex: 35 men, 35 women, 50% women Inclusion criteria: consecutive visually impaired participants. Each had previously undergone ophthalmologic care and a full low‐vision examination including optimisation of their refraction and their optical magnifier. Minimum magnification for comfortable reading of the participants' chosen print size was prescribed. Exclusion criteria: none | |
| Interventions |
Intervention:
Comparator:
Duration: single test session |
|
| Outcomes | After an explanation, demonstration and a 2‐minute active training period with each magnifying device the participants were asked to randomly complete a series of 4 tests chosen to replicate daily living tasks.
4 versions of each task, equal in difficulty (in terms of number, length, and difficulty of words and page distance), were constructed and used in a randomised order to control fatigue effects. |
|
| Notes | Date study conducted: not reported Funding: partly funded by a College of Optometrists summer studentship grant Declaration of interest: the authors declared no financial interest in any of the devices evaluated Trial registration number: not reported | |
| Risk of bias | ||
| Bias | Authors' judgement | Support for judgement |
| Random sequence generation (selection bias) | Low risk | Randomised presentation of devices; although no further detail was given on how the randomisation sequence was generated, selection bias should be avoided since all participants used all devices (cross‐over study design) |
| Allocation concealment (selection bias) | Low risk | Randomised presentation of devices; although no further detail was given on how randomisation sequence was concealed, selection bias was likely to be avoided since all participants used all devices (cross‐over study design) |
| Incomplete outcome data (attrition bias) All outcomes | High risk | Not all participants could read using all devices; thus, the analysis is not intention‐to‐treat |
| Selective reporting (reporting bias) | Low risk | No protocol available, but primary outcome reported |
| Period effect | Low risk | No details reported, but same‐session, short duration testing made this type of bias unlikely |
| Carry‐over effect and period‐by‐treatment interaction | Unclear risk | Authors reported they used reading and real‐word tests of very short duration, but no quantitative details are available |
Smith 2005.
| Methods | Study design: parallel group randomised controlled trial Masking: participant: yes; provider: no; outcome: yes Exclusions after randomisation: none reported Losses to follow‐up: 10 in the custom prism group, 6 in the standard prism group, and 2 in the placebo group. | |
| Participants | Country: UK Number randomised: 243 people recruited from Manchester Royal Eye Hospital, England Cause of low vision: AMD Age: median age 81 years, interquartile range 76 to 86 Sex: 86 men, 157 women, 65% women Inclusion criteria: English‐speaking Exclusion criteria: illiterate, resident in a hospital or a nursing home | |
| Interventions |
Intervention: 2 types of test spectacles.
Comparator:
The spectacles prescribed to each group included the optimal refractive correction for distance and near vision. Duration: 3 months follow‐up during the period |
|
| Outcomes |
|
|
| Notes | Date study conducted: July 2001 to March 2003 Funding: supported by the Health Foundation; London, England Declaration of interest: the authors declare no financial disclosure Trial registration number: ISRCTN00821605 | |
| Risk of bias | ||
| Bias | Authors' judgement | Support for judgement |
| Random sequence generation (selection bias) | Low risk | Participants were allocated to a group using computer‐generated randomisation codes prepared in advance |
| Allocation concealment (selection bias) | Low risk | Randomisation and the ordering of spectacles were performed by a principal investigator who had no contact with participants during the study |
| Incomplete outcome data (attrition bias) All outcomes | Low risk | Low number of losses to follow‐up: 10 in the custom prism group, 6 in the standard prism group, and 2 in the placebo group |
| Selective reporting (reporting bias) | Low risk | No protocol available, but primary outcome reported |
Spitzberg 1995.
| Methods | Study design: quasi‐randomised cross‐over trial Masking: masking issues are not described, but study participants, providers and outcome assessors were likely to be unmasked given the use of recognisable devices Exclusions after randomisation: none reported Losses to follow‐up: none reported Unusual study design: within‐person design, i.e. a cross‐over study in which all participants try the devices consecutively | |
| Participants | Country: USA Number randomised: 39 people from 5 low‐vision clinics Cause of low vision: not known Age: mean age not reported, range 9 to 77 years. Sex: not reported Inclusion criteria: all participants were selected based on a need to use 3× magnification to read 1.0 M or 1. 5 M print Exclusion criteria: none reported | |
| Interventions |
Intervention: 3 new stand magnifiers with equivalent power
Comparator:
Each participant trained daily with 4 low‐vision aids including at least 2 prototype devices for a minimum of 5 days. All participants practiced reading for 1 hour each day using materials developed for the study. Duration: 10 days |
|
| Outcomes | Reading speed; Preference for each device including reporting detailed information on their looks, clarity, portability, comfort, ease of use, field and glare | |
| Notes | Date study conducted: not reported Funding: NIH SBIR grant #2R44EY0S156 Ergonomic Magnifiers for Improved REading and Writing, given to Optical Designs, Inc. Declaration of interest: Dr Larry Spitzberg has a financial interest in these products. Trial registration number: not reported | |
| Risk of bias | ||
| Bias | Authors' judgement | Support for judgement |
| Random sequence generation (selection bias) | Low risk | Quasi‐randomised study: the order of presentation of the devices was rotated (counterbalanced) for consecutive participants; even so, selection bias should be low since all participants used all devices (cross‐over study design) |
| Allocation concealment (selection bias) | Low risk | Order of randomisation can be foreseen because rotation was used; despite this, selection bias should be low since all participants used all devices (cross‐over study design) |
| Incomplete outcome data (attrition bias) All outcomes | Low risk | No loss to follow‐up or exclusion after randomisation reported |
| Selective reporting (reporting bias) | Low risk | No protocol available, but primary outcome reported |
| Period effect | Low risk | No details reported, but same‐session, short duration testing made this type of bias unlikely |
| Carry‐over effect and period‐by‐treatment interaction | Unclear risk | No details reported |
Stelmack 1991.
| Methods | Study design: quasi‐randomised cross‐over study Masking: masking issues are not described, but study participants, providers and outcome assessors were likely to be unmasked given the use of recognisable devices Exclusions after randomisation: none reported Losses to follow‐up: none reported Unusual study design: within‐person design, i.e. a cross‐over study in which all participants try the devices consecutively | |
| Participants | Country: USA Number randomised: 37 participants admitted to the Central Blind Rehabilitation Center Cause of low vision: AMD or ocular histoplasmosis Age: mean and range not reported, participants were aged 50 years or older Sex: not reported Inclusion criteria: 50 or older, diagnosis of postdisciform stage AMD or ocular histoplasmosis Exclusion criteria: eye pathologies which would affect study results by compromising visual function | |
| Interventions |
Intervention:
Comparator:
Before allocation all participants were trained by a visual skills instructor to use his or her best retinal viewing area. Modifications of standard techniques were used, including stand with the bar, the clock method of distance training, the fixation and reading techniques. Participant progress in eccentric viewing training was monitored with the Pepper Visual Skills for Reading Test. The magnification used for each device was the lowest that enabled the participant to consistently read excerpts from the Readers Digest using the preferred level of illumination and a reading stand. Prior to testing each participant had a 1‐hour training/practice session under the supervision of a visual skills instructor from the Central Blind Rehabilitation Center teaching staff Duration: single test session |
|
| Outcomes | Silent reading speed recorded in words per minute; reading comprehension tested at the end of the article using 5 general questions graded from 0‐5. Testing was considered invalid if the score was less than 4; reading duration measured in minutes and defined as the time the participant could read without visual discomfort | |
| Notes | Date study conducted: not reported Funding: supported by Medical Research Service, Department of Veterans Affairs Declaration of interest: not reported Trial registration number: not reported | |
| Risk of bias | ||
| Bias | Authors' judgement | Support for judgement |
| Random sequence generation (selection bias) | Low risk | Quasi‐randomised study: the VA Cooperative Studies Center generated the randomisation sequence and the code envelopes for randomising the order of device presentation. The set of envelopes was handed to the investigators at the beginning of the study. The research assistant opened an envelope at the time needed to assign the treatment order. Methods for the randomisation sequence: the 6 different possible orders of presentation of the devices were numbered in advance. A list of random numbers was computer‐generated. The 7, 8, 9 and 0 were deleted and the remaining numbers used to identify the group (information provided by investigators). |
| Allocation concealment (selection bias) | Low risk | Order of randomisation can be foreseen because rotation was used; despite this, selection bias should be low since all participants used all devices (cross‐over study design) |
| Incomplete outcome data (attrition bias) All outcomes | Low risk | No loss to follow‐up or exclusion after randomisation reported |
| Selective reporting (reporting bias) | Low risk | No protocol available, but primary outcome reported |
| Period effect | Low risk | Participants with disciform neovascular maculopathy were included who are expected to have stable vision during the study period |
| Carry‐over effect and period‐by‐treatment interaction | Unclear risk | No details reported |
Taylor 2017.
| Methods | Study design: cross‐over randomised controlled trial Masking: participant ‐ no, investigator ‐ quote "The study researcher was masked to the group allocation of the participant when the baseline assessment was carried out, but not at any subsequent study visits." Exclusions after randomisation: 6 participants due to reported reasons, balanced between groups Losses to follow‐up: 15 participants due to reported reasons, balanced between groups Unusual study design: within‐person design, i.e. a cross‐over study in which all participants try the devices in two subsequent 2‐month periods | |
| Participants | Country: UK Number randomised: 100 (82 completed study), mostly affected by AMD, recruited from low vision clinics at Manchester Royal Eye Hospital, Manchester, UK Cause of low vision: AMD (n = 47), Stargardt (n = 3), retinitis pigmentosa (n = 3), myopic degeneration (n = 5), glaucoma (n = 6), diabetic retinopathy (n = 2), nystagmus (n = 5), other (n = 11) Age: mean age 71 years, range 20 to 93 years Sex: 38 men, 62 women, 62% women Inclusion criteria: criteria for the study were adults (over 18 years), currently using optical LVAs only (not used p‐EVES before), stable VI, and visual acuity (VA) of 0.7 logMAR (6/30) or worse and/or log contrast sensitivity (CS) of 1.20 or worse (in the better eye) Exclusion criteria: physical disability that prevented the participant operating the p‐EVES device, or a score of < 19 on the Mini‐Mental State Examination. | |
| Interventions |
Intervention:
Comparator:
Portable optical devices were: Optelec Compact+ (n.4), Optelec Compact 4HD, (n.28), Schweizer eMAG 43 (n. 46), Eschenbach Mobilux Digital (n.4) Duration: 4 months (each participants had 2 months for intervention, 2 months for comparator) |
|
| Outcomes |
|
|
| Notes | Date study conducted: May 2013 to October 2014 Funding: quote: "This publication presents independent research funded by the National Institute of Health Research (NIHR) under its Research for Patient Benefit (RfPB) Programme (Grant Reference Number PB‐PG‐0211‐24105)." Declaration of interest: reported no conflict of interest. Quote: "We thank Associated Optical, Bierley, Humanware, Optima Low Vision and Optelec for supplying electronic magnifiers to be used in the study" Trial registration number: NCT01701700 | |
| Risk of bias | ||
| Bias | Authors' judgement | Support for judgement |
| Random sequence generation (selection bias) | Low risk | Computer‐generated random sequence, delivered with secure password‐protected web‐based randomisation procedure only after each patient's inclusion was confirmed. Within each study arm, age (< 60, ≥ 60 years) and visual acuity (VA; < 1.3 logMAR (6/120), ≥ 1.3 logMAR (6/120)), were binary stratification variables. Selection bias should be avoided since all participants used all devices (cross‐over study design). |
| Allocation concealment (selection bias) | Low risk | Allocation was delivered with secure password‐protected web‐based randomisation procedure only after each patient's inclusion was confirmed |
| Incomplete outcome data (attrition bias) All outcomes | Low risk | Causes of loss to follow‐up adequately reported and balanced across cross‐over phases |
| Selective reporting (reporting bias) | Low risk | Study protocol available and outcomes are consistent |
| Period effect | Low risk | The main analysis used methods accounting for treatment, period and carry‐over effects |
| Carry‐over effect and period‐by‐treatment interaction | Low risk | The main analysis used methods accounting for treatment, period and carry‐over effects |
Watson 2005.
| Methods | Study design: cross‐over randomised controlled trial Method of allocation: random Masking: not reported Exclusions after randomisation: none reported Losses to follow‐up: none reported Unnusual study design: within‐person study with random assignment of the first device used | |
| Participants | Country: USA Number randomised: 30 veteran participants Cause of low vision: AMD or juvenile macular degeneration or diabetic retinopathy (number of participants unclear Age: mean age 71 years, range 45 to 90 years Sex: not reported Inclusion criteria: AMD, juvenile macular degeneration or diabetic retinopathy, 20/50 or less in the better‐seeing eye, bilateral central scotoma or metamorphopsia, goal for rehabilitation to read newspapers, magazines etc. Exclusion criteria: scoring less than 26 on the Folstein Mini‐mental Health Examination, having more than 10 sick days in bed in the last 6 months, illness that would affect stamina for reading e.g. congestive hear failure, chromic obstructive pulmonary disorder, etc. | |
| Interventions |
Intervention:
Comparator:
Two separate cross‐over experiments: 15 participants used refractive‐aspheric and hybrid‐diffractive and 15 participants used aplanatic and hybrid‐diffractive lenses Duration: single test session |
|
| Outcomes |
|
|
| Notes | Date study conducted: not reported Funding: quote "This material is the result of work supported with resources and the use of facilities at the Kansas City VA Medical Center and the Atlanta VA Rehabilitation Research and Development Center on Aging Veterans with Vision Loss". Declaration of interest: the authors declare no financial interest in the products evaluated Trial registration number: not reported | |
| Risk of bias | ||
| Bias | Authors' judgement | Support for judgement |
| Random sequence generation (selection bias) | Low risk | Random presentation of first device, but sequence generation method not described; even so, selection bias should be low since all participants used all devices (cross‐over study design) |
| Allocation concealment (selection bias) | Low risk | Unclear if order of randomisation could be foreseen since no detail given; despite this, selection bias should be low since all participants used all devices (cross‐over study design) |
| Incomplete outcome data (attrition bias) All outcomes | Low risk | No loss to follow‐up or exclusion after randomisation reported |
| Selective reporting (reporting bias) | Low risk | No protocol available, but primary outcome reported |
| Period effect | Low risk | No details reported, but same‐session, short duration testing made this type of bias unlikely |
| Carry‐over effect and period‐by‐treatment interaction | Unclear risk | No details reported |
AMD: age‐related macular degeneration; CCTV: closed circuit television; CRT: cathode ray tube; EOMD: early onset macular disease; ETDRS: Early Treatment of Diabetic Retinopathy Study; HMD: head‐mounted device; IReST: International Reading Speed Texts; LVA: low‐vision aid; LVES: Low Vision Enhancement System; MNREAD: Minnesota Low‐Vision Reading test; SD: standard deviation; SLO: scanning laser ophthalmoscope; VA: visual acuity; VFQ: Visual Functioning Questionnaire; VRD: virtual retinal display.
Characteristics of excluded studies [ordered by study ID]
| Study | Reason for exclusion |
|---|---|
| Alabdulkader 2012 | Only one device type was adopted |
| Bailie 2013 | Not a randomised or quasi‐randomised controlled trial |
| Blaskey 1990 | Assessment of Irlen filters in people with reading difficulty not due to low vision |
| Bonatti 2008 | Stand magnifier compared to hand magnifier regarding subjective preference, but reading speed or reading acuity data not assessed |
| Cheong 2005 | Large‐print reading training effect and not LVA effect studied |
| Cheong 2009 | Reading performance of 29 participants with AMD assessed using their habitual stand magnifier with and without a temporary line guide attached; no comparison of different LVAs |
| Cohen 1991 | LVAs compared in normal observers |
| Culham 2009 | The study aims to elicit the users' responses to 4 electronic HMDs and to correlate users' opinion with performance, but reading speed or acuity data for each device were not assessed |
| Goodrich 1977 | Participants assigned to 2 groups but no randomisation used (information obtained by the first author) |
| Goodrich 2004 | Within‐person or cross‐over study but all participants underwent training and testing with the 3 devices in the same order |
| Jacobs 1990 | Evaluated whether the colour of the screen altered performance of CCTV |
| Kuyk 1990 | Comparison of motorised and manual focus Keplerian telescopes, but target spotting and not reading performance assessed |
| Lawton 1989 | Before‐and‐after study on compensation filters boosting the amplitudes of the intermediate spatial frequencies more than the amplitude of the lower spatial frequencies. No control group |
| LOVIT 2008 | Multicentre randomised study comparing the effectiveness of a low‐vision rehabilitation programme with control (waiting list); outcome measure was change in participants' visual reading ability estimated from participant responses to the Veterans Affairs Low‐Vision Visual Functioning Questionnaire (LV VFQ–48) reading items completed at baseline compared with 4 months after enrolment for the treatment and control groups. No comparison of different reading aids |
| Margrain 2000 | No comparisons between LVAs |
| Parodi 2004 | RCT including 28 participants comparing the effect of prisms (5 to 7 prismatic dioptres) in the better eye versus control. Excluded because the aim was to improve visual acuity |
| Rees 2006 | Comparison of low‐cost and high‐cost hand‐held magnifiers, but no comparison of different LVAs |
| Reeves 2004 | The effectiveness of 3 models of low‐vision rehabilitation for people with AMD compared rather than the efficacy of specific types of LVAs |
| Rohrschneider 1998 | Assessed reading speed in CCTV with different image refresh rates (50 Hz, 60 Hz and 70 Hz of frequency) |
| Rosenberg 1989 | Quasi‐randomised study comparing prismatic correction in 19 participants versus 11 controls. Excluded because the aim of the study was to improve visual acuity not reading acuity |
| Rossi 1990 | Effect on walking and transfer assessed in stroke patients with hemianopsia or visual neglect using Fresnel prisms vs control. No reading speed data |
| Scott 2002 | Evaluation of performance in icon identification tasks while the screen features of the graphical user interface were varied |
| Wolffshon 2002 | Coloured lenses compared with no filter in 10 AMD people and 5 healthy controls, but reading speed not assessed |
AMD: age‐related macular degeneration; CCTV: closed circuit television; HMD: head‐mounted device; LVA: low‐vision aid;RCT: randomised controlled trial.
Characteristics of studies awaiting assessment [ordered by study ID]
Demers‐Turco 2001.
| Methods | Quote: "Twenty‐nine adults (distance visual acuity 20/80‐20/320) from the Vision Rehabilitation Center read short paragraphs (41‐44 words) using three 10× devices (a portable electronic magnification system (EMS), a hand held magnifier (MAG) and table top CCTV). Subjects read three font sizes (18, 12, and 8 pt, san serif) with each device. We defined a weighted words per minute reading rate from the time taken to read and approximate number of words read from each paragraph. We also recorded age (19‐91), diagnosis (41% ARMD) and previous use of each device. " |
| Participants | 29 adults |
| Interventions | A portable electronic magnification system (EMS), a hand held magnifier (MAG) and table top CCTV |
| Outcomes | Quote: "The group as a whole read faster with the CCTV, then magnifier, then portable EMS (P<0.0001). To our surprise, with each device, reading was slowest with 18 pt and fastest with 8 pt. There was no effect of familiarity with device. For subjects with ARMD, again, reading was fastest with CCTV but there was no difference between MAG and EMS. Unlike the group as a whole, reading rate was the same for all font sizes except with CCTV, where reading was fastest with 8 pt type. Conclusions: the portable EMS provides no benefit for low vision patients. The increase in reading performance with decreasing font size may be due to increased field of view. Further research is required. " |
| Notes | ARVO abstract only |
Goodrich 1998.
| Methods | Quote: "In this study we explored the effect reading training and device type (optical aid closed circuit television (CCTV)) on reading performance of individuals with central field loss. While a central field loss reduces reading performance, rehabilitation can restore function, but the question of how much rehabilitative training is necessary to optimize reading has not been addressed. Reading performance with low vision aids has similarly been shown to be effective, but the value of optics aids versus CCTV has not been extensively explored. METHOD: 50 subjects with central field loss who participated in the rehabilitation program of the Western Blind Rehabilitation Center volunteered to participate in the study; which used a randomised, counter‐balances design. All subjects received comprehensive optometric examinations, were prescribed an optimum near vision optical aid and CCTV. The training group received ten days of instructor training with their optical aid and fifteen days of instructor training with their CCTV. The other group received five days of instructor training with the optical aid followed by five days of independent practice and seven days of training with the CCTV and eight days of independent practice. The variables of acuity, contrast sensitivity, reading speed and reading duration were measured." |
| Participants | 50 people with central loss |
| Interventions | Optimum near vision optical aid and CCTV |
| Outcomes | Quote: "Short term instructor training combined with independent practice was as effective in optimizing reading speed and duration as was the longer term instructor training. CCTVs provided greater reading speed and duration than did optical aids. Reading performance with an optical aid was only moderately correlated with reading performance with a CCTV. CONCLUSION. Instructor training combined with independent practice is an effective method of rehabilitating reading skills. CCTVs offer advantages in terms of reading speed and duration. Reading training is a variable which, if taken into account, can improve both low vision clinical practice and research" |
| Notes | American Academy of Optometry abstract only |
Goodrich 2000a.
| Methods | Quote: "Reading aids are arguably the most frequently prescribed low vision device, yet there is little comparative information on the performance to be expected for different low vision devices prescribed for patients having different characteristics. PURPOSE. This study sought to provide comparative information for clinicians to assist in prescribing low vision reading devices, and for patients in selecting which device will best meet their needs in relation to its cost. METHOD. Subjects were 133 patients (mean age = 68.5 yrs) of the Western Blind Rehabilitation Center. Subjects were assigned to one of three groups based upon field loss: central (N = 90); peripheral (N = 28); or mixed central and peripheral field loss (N = 15). The study used a within‐person, counterbalanced design with all subjects trained in reading with an optical aid (primarily stand magnifiers or microscopic lenses) and CCTV. Reading speeds and durations were recorded." |
| Participants | 132 low‐vision participants |
| Interventions | Optical aid (primarily stand magnifiers or microscopic lenses) and CCTV |
| Outcomes | Quote: "Central loss subjects read 20% faster and 34% longer with the CCTV than their best optical aid. Peripheral loss subjects read only 12% faster and 23% longer with CCTV than their best optical aid, and mixed loss subjects read only 9% faster and 34% longer. CONCLUSIONS. CCTVs, as a low vision reading device, provided all subjects in this study with an average of 23% to 34% longer reading durations. Reading speeds averaged between 9% and 20% greater. Central loss subjects appear to gain the greatest benefit from CCTV, while mixed and peripheral loss subjects gain a greater reading duration with the CCTV. The relative benefits of devices for each patient group will be discussed in the context of information that may assist the clinician in prescribing low vision reading devices. Prescribing information should encompass the patient's reading needs and the cost of the devices, as well as, information about the performance patient's can expect from the device." |
| Notes | American Academy of Optometry abstract only |
Goodrich 2001a.
| Methods | Quote: "Low power lasers have been used for purposes ranging from scanning laser ophthalmoscopes to heads‐up displays for aircraft pilots. In this study we have begun a formal examination of one possible application as a reading display for low vision patients. The prototype device, called Nomad, is a monocular, head‐mounted display that uses a red laser to display text onto the retina. A CCTV camera and XY table provided input. METHODS: 20 subjects read with the prescribed optical device, CCTV, and Nomad. Data was collected on subject visual acuity, pathology, contrast sensitivity, duration of visual disability, and reading speed and reading duration with each device. In addition subjective impressions of the Nomad were gathered using both forced choice and open‐ended questions." |
| Participants | 20 low vision participants |
| Interventions | Prescribed optical device, CCTV, and Nomad |
| Outcomes | "Subject reading speeds with the Nomad were faster than optical devices, but slower than CCTV. Reading durations with the Nomad were similar to that with CCTV; both of which were about 3X longer than optical devices. Subjective data indicated that subjects would prefer another color, or full‐color laser for the Nomad and would like a more comfortable head‐mount. Most subjects preferred the brightness and sharpness of the Nomad display to the displays of the optical devices and CCTVs. The brightness and high contrast may allow patients with extremely low vision to maintain, the ability to read visually even when conventional devices are no longer effective. CONCLUSIONS: the Nomad is a prototype display with potential as both a distance and near vision aid. At present it is a useful research tool to begin examining the potential benefits of new visual display technology. We will discuss our findings in relation to this potential." |
| Notes | American Academy of Optometry abstract only |
Kaida 2005.
| Methods | Within‐person study (2 low‐vision aids tested on the same participant); order of presentation randomised (coin toss, as notified by the authors) |
| Participants | 13 low‐vision persons participated in the study. Their ages ranged from 57‐82 years, average 70 years. Their best corrected visual acuity ranged from 0.01‐0.30, average 0.04. They were asked to read characters with these 2 devices for 20 seconds text of decreasing print size |
| Interventions | A hand‐held retinal projection system was compared with a face‐mounted video display using a CCTV system |
| Outcomes | Reading speed, critical print size |
| Notes | Article in Japanese; authors have been contacted to collect data and there was no answer |
Sonsino 2000.
| Methods | Quote: "Portability and ease of text and spot reading is a challenge for low vision patients needing high levels of magnification. 'Powervision,' a new, head‐mounted electronic magnification system, offers portable high magnification for reading. This pilot study compared the speed and accuracy of text and spot reading by low vision patients using 'Powervision' (P), traditional CCTV (C) and a comparable hand held magnifier (H). METHODS. Twenty patients from the Vision Rehabilitation Center of the Mass. Eye and Ear Infirmary best corrected to < or = 20/80, could read English, and consented to participate were included. Patients were scored on time and accuracy of reading three short paragraphs of text (8, 12, 18 pt print) and spot reading of a hospital bill. Patients reported ease of reading with each of the three devices. " |
| Participants | 20 low‐vision participants |
| Interventions | Powervision, traditional CCTV and a comparable hand held magnifier |
| Outcomes | Quote: "Ages ranged 22‐92 (mean 58.3), with acuities of 20/80‐20/800 (mean 20/267), and primary diagnoses of ARMD (23%) and other etiologies of visual loss. Text reading mean scores (360s maximum) were P: 313s, C: 180s, H: 248s, and accuracy (12.0=whole paragraph correct, 0=could not read) was P: 8.4, C: 11.3, H: 8.9. Spot reading mean times were P: 95s, C: 60s, H: 83s and accuracy (4.0= all correct, 8.0= all incorrect) measured P: 5.4, C: 4.2, H: 5.1. Mean patient reports of ease of use (1=Very Easy, 5=Very Difficult) were P: 3.5, C: 1.9, H: 3.1 for text reading and P: 3.6, C: 1.7, H: 2.8 for spot reading. DISCUSSION. In this pilot population, despite its portability, Powervision scored less well on speed and accuracy of spot and test reading and for patient report of ease of use. Planned redesign and training in use may improve patient performance." |
| Notes | ARVO abstract only |
ARMD: age‐related macular degeneration; ARVO: Association for Research in Vision and Ophthalmology; CCTV: closed circuit television.
Differences between protocol and review
Modifications to the protocol
Types of outcome measures: we changed our primary outcome, as defined in the original protocol (reading speed), by including print size in its definition in order to make it more similar to real‐world tasks. We also specified that reading speed had to be measured at ordinary print size because this is the outcome most relevant to patients in terms of performance using a specific low‐vision aid. We also specified that MNREAD definitions of maximum reading speed and reading acuity were adopted in our review, and we discuss the consequences of this choice in the update. We used raw reading acuity (words per minute) rather than its log transformation as done in the original version using individual values, because results are more interpretable on this scale, despite mild skewness.
Types of intervention: we updated the inclusion criteria to include consumer electronics such as smart phones and tablets. We also specified the inclusion of coloured filters and prisms and clarified the exclusion of studies in which the intervention is a device to read though hearing, such as screen readers or talking books, or through touch, such as Braille‐based devices and haptic devices.
Risk of bias assessment: we adapted the 'Risk of bias' assessment following new guidance. We reconsidered the scoring of 'within‐person' or cross‐over‐like studies, leading to adapted criteria to score the quality of randomisation and allocation concealment.
Search strategy: we removed the RCT filter from the electronic searches in order to identify as many potentially relevant studies as possible.
Methods not implemented
We did not implement the following planned methods because the relevant data were not available or not enough studies contributed data to any one analysis. We will implement these in future updates of this review as needed.
Measures of treatment effect: for dichotomous data, we will express results as a risk ratio with 95% confidence interval. We will also calculate the risk difference or the number needed to treat for an additional beneficial outcome.
Subgroup analyses: we will assess the effect of low‐vision severity (e.g. proportion of participants below 20/100 in the better eye), matching of LVAs by magnification versus no matching, participant age (e.g. proportion of people aged 55 years or more), study design (parallel‐arm versus 'within‐person').
Sensitivity analyses: we will conduct sensitivity analyses with the following adjustments: excluding studies of lower methodological quality (scoring high risk of bias on any parameter of quality); excluding unpublished studies.
The search strategies were updated for the 2018 version of this review to reflect new technologies and devices being developed.
Contributions of authors
Designing the review: RA, GV Co‐ordinating the review: GV, RA, JE Undertaking manual searches: GV, RA Screening search results: GV, RA, SB, LG, JE Organising retrieval of papers: GV, GG, RA, Cochrane Eyes and Vision Group Screening retrieved papers against inclusion criteria: GV, RA, SB, LG, JE Appraising quality of papers: GV, GG, RA, JE Extracting data from papers: GV, RA, JE Writing to authors of papers for additional information: GV, RA Providing additional data about papers: GV, RA Obtaining and screening data on unpublished studies: GV, GG, RA Data management for the review: GV, GG, RA Entering data into Review Manager 5: GV, RA Analysis of data: GV, RA Interpretation of data: GV, RA, SB, LG, GG, JE Writing the review: GV, RA, SB, LG, GG, CA
Sources of support
Internal sources
No sources of support supplied
External sources
-
The College of Optometrists, UK.
The College provided funding to Cochrane Eyes and Vision to update this review (2018).
-
National Institute for Health Research (NIHR), UK.
- Richard Wormald, Co‐ordinating Editor for Cochrane Eyes and Vision (CEV) acknowledges financial support for his CEV research sessions from the Department of Health through the award made by the NIHR to Moorfields Eye Hospital NHS Foundation Trust and UCL Institute of Ophthalmology for a Specialist Biomedical Research Centre for Ophthalmology.
- This review update was supported by the NIHR, via Cochrane Infrastructure funding to the CEV UK editorial base.
The views and opinions expressed therein are those of the authors and do not necessarily reflect those of the Systematic Reviews Programme, NIHR, NHS or the Department of Health.
Declarations of interest
Gianni Virgili shares the patent on the MNREAD Italian charts with the University of Minnesota, Minneapolis, USA.
New search for studies and content updated (no change to conclusions)
References
References to studies included in this review
Culham 2004 {published and unpublished data}
- Culham LE, Chabra A, Rubin GS. Clinical performance of electronic, head‐mounted, low‐vision devices. Ophthalmic and Physiological Optics 2004;24(4):281‐90. [DOI] [PubMed] [Google Scholar]
Eperjesi 2004 {published data only}
- Eperjesi F, Fowler CW, Evans BJ. The effects of coloured light filter overlays on reading rates in age‐related macular degeneration. Acta Ophthalmologica Scandinavica 2004;82(6):695‐700. [DOI] [PubMed] [Google Scholar]
Goodrich 2001 {published and unpublished data}
- Goodrich GL, Kirby J. A comparison of low vision reading performance with hand‐held and stand‐mounted CCTV. Optometry and Vision Science 2000;77(12):125. [Google Scholar]
- Goodrich GL, Kirby J. A comparison of patient reading performance and preference: optical devices, handheld CCTV (Innoventions Magni‐Cam), or stand‐mounted CCTV (Optelec Clearview or TSI Genie). Optometry 2001;72(8):519‐28. [PubMed] [Google Scholar]
Jackson 2017 {published data only}
- Jackson ML, Schoessow KA, Selivanova A, Wallis J. Adding access to a video magnifier to standard vision rehabilitation: initial results on reading performance and well‐being from a prospective, randomized study. Digital Journal of Ophthalmology 2017;23(1):1‐10. [DOI] [PMC free article] [PubMed] [Google Scholar]
Kleweno 2001 {published data only}
- Kleweno CP, Seibel EJ, Viirre ES, Kelly JP, Furness TA 3rd. The virtual retinal display as a low‐vision computer interface: A pilot study. Journal of Rehabilitation Research and Development 2001;38(4):431‐42. [PubMed] [Google Scholar]
Morrice 2017 {published data only}
- Morrice E, Johnson AP, Marinier JA, Wittich W. Assessment of the Apple iPad as a low‐vision reading aid. Eye 2017;31(6):865‐71. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Riley AK, Johnson AP. Apple iPad and CCTV reading performance comparison in persons with low vision. Investigative Ophthalmology and Visual Science 2016;57(12):5169. [Google Scholar]
Ortiz 1999 {published data only}
- Ortiz A, Chung ST, Legge GE, Jobling JT. Reading with a head‐mounted video magnifier. Optometry and Vision Science 1999;76(11):755‐63. [DOI] [PubMed] [Google Scholar]
Peterson 2003 {published data only}
- Peterson RC, Wolffsohn JS, Rubinstein M, Lowe J. Benefits of electronic vision enhancement systems (EVES) for the visually impaired. American Journal of Ophthalmology 2003;136(6):1129‐35. [DOI] [PubMed] [Google Scholar]
Smith 2005 {published data only}
- Smith HJ, Dickinson CM, Cacho I, Reeves BC, Harper RA. A randomized controlled trial to determine the effectiveness of prism spectacles for patients with age‐related macular degeneration. Archives of Ophthalmology 2005;123(8):1042‐50. [DOI] [PubMed] [Google Scholar]
Spitzberg 1995 {published and unpublished data}
- Spitzberg LA, Goodrich GL. New ergonomic stand magnifiers. Journal of the American Optometric Association 1995;66(1):25‐30. [PubMed] [Google Scholar]
Stelmack 1991 {published and unpublished data}
- Stelmack J, Reda D, Ahlers S, Bainbridge L, McCray J. Reading performance of geriatric patients post exudative maculopathy. Journal of the American Optometric Association 1991;62(1):53‐7. [PubMed] [Google Scholar]
Taylor 2017 {published data only}
- Bray N, Brand A, Taylor J, Hoare Z, Dickinson C, Edwards RT. Portable electronic vision enhancement systems in comparison with optical magnifiers for near vision activities: an economic evaluation alongside a randomized crossover trial. Acta Ophthalmologica 2017;95(5):415‐23. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Taylor JJ, Bambrick R, Brand A, Bray N, Dutton M, Harper RA, et al. Effectiveness of portable electronic and optical magnifiers for near vision activities in low vision: a randomised crossover trial. Ophthalmic and Physiological Optics 2017;37(4):370‐84. [DOI] [PubMed] [Google Scholar]
Watson 2005 {published data only}
- Watson GR, Maino JM, l'Aune W. Comparison of low‐vision reading with spectacle mounted magnifiers. Journal of Rehabilitation Research and Development 2005;42(4):459‐70. [DOI] [PubMed] [Google Scholar]
References to studies excluded from this review
Alabdulkader 2012 {published data only}
- Alabdulkader B, Leat S. Do reading additions improve reading in pre‐presbyopes with low vision?. Optometry and Vision Science 2012;89(9):1327‐35. [DOI] [PubMed] [Google Scholar]
Bailie 2013 {published data only}
- Bailie M, Wolffsohn JS, Stevenson M, Jackson AJ. Functional and perceived benefits of wearing coloured filters by patients with age‐related macular degeneration. Clinical and Experimental Optometry 2013;96(5):450‐4. [DOI] [PubMed] [Google Scholar]
Blaskey 1990 {published data only}
- Blaskey P, Scheiman M, Parisi M, Ciner EB, Gallaway M, Selznick R. The effectiveness of Irlen filters for improving reading performance: a pilot study. Journal of Learning Disability 1990;23(10):604‐12. [DOI] [PubMed] [Google Scholar]
Bonatti 2008 {published data only}
- Bonatti FA, Bonatti JA, Sampaio MW, Haddad MA, Souza PR, José NK. Evaluation of patients using an innovative low‐vision aid [Avaliacao de pacientes utilizando equipamento inovador de auxilio a visao subnormal]. Arquivos Brasileiros de Oftalmologia 2008;71(3):385‐8. [DOI] [PubMed] [Google Scholar]
Cheong 2005 {published data only}
- Cheong AM, Lovie‐Kitchin JE, Bowers AR, Brown B. Short‐term in‐office practice improves reading performance with stand magnifiers for people with AMD. Optometry and Vision Science 2005;82(2):114‐27. [DOI] [PubMed] [Google Scholar]
Cheong 2009 {published data only}
- Cheong AM, Bowers AR, Lovie‐Kitchin J. Does a line guide improve reading performance with stand magnifiers?. Optometry and Vision Science 2009;86(9):1078‐85. [DOI] [PubMed] [Google Scholar]
Cohen 1991 {published data only}
- Cohen JM, Waiss B. Reading speed through different equivalent power low vision devices with identical field of view. Optometry and Vision Science 1991;68(10):795‐7. [DOI] [PubMed] [Google Scholar]
Culham 2009 {published data only}
- Culham LE, Chabra A, Rubin GS. Users' subjective evaluation of electronic vision enhancement systems. Ophthalmic and Physiological Optics 2009;29(2):138‐49. [DOI] [PubMed] [Google Scholar]
Goodrich 1977 {published and unpublished data}
- Goodrich GL, Mehr EB, Quillman RD, Shaw HK, Wiley JK. Training and practice effects in performance with low‐vision aids: a preliminary study. American Journal of Optometry and Physiological Optics 1977;54(5):312‐8. [DOI] [PubMed] [Google Scholar]
Goodrich 2004 {published and unpublished data}
- Goodrich GL, Kirby J, Wagstaff P, Oros T, McDevitt B. A comparative study of reading performance with a head‐mounted laser display and conventional low vision devices. Journal of Visual Impairment and Blindness 2004;98(3):148‐59. [Google Scholar]
Jacobs 1990 {published data only}
- Jacobs RJ. Screen color and reading performance on closed‐circuit television. Journal of Visual Impairment and Blindness 1990;84(10):569‐72. [Google Scholar]
Kuyk 1990 {published data only}
- Kuyk T, James J. A pilot study of a telescopic low vision aid with a motorized focus. Journal of Vision Rehabilitation 1990;4:21‐9. [Google Scholar]
Lawton 1989 {published data only}
- Lawton TB. Improved reading performance using individualized compensation filters for observers with losses in central vision. Ophthalmology 1989;96(1):115‐26. [DOI] [PubMed] [Google Scholar]
LOVIT 2008 {published data only}
- Stelmack JA, Tang XC, Reda DJ, Rinne S, Mancil RM, Massof RW, et al. Outcomes of the Veterans Affairs Low Vision Intervention Trial (LOVIT). Archives of Ophthalmology 2008;126(5):608‐17. [DOI] [PubMed] [Google Scholar]
Margrain 2000 {published data only}
- Margrain TH. Helping blind and partially sighted people to read: the effectiveness of low vision aids. British Journal of Ophthalmology 2000;84(8):919‐21. [DOI] [PMC free article] [PubMed] [Google Scholar]
Parodi 2004 {published data only}
- Parodi MB, Toto L, Mastropasqua L, Depollo M, Ravalico G. Prismatic correction in patients affected by age‐related macular degeneration. Clinical Rehabilitation 2004;18:828‐32. [DOI] [PubMed] [Google Scholar]
Rees 2006 {published data only}
- Rees G, Ferraro JG, Lamoureux E, Keeffe JE. Evaluation of low cost low vision devices. Investigative Ophthalmology and Visual Science 2006; Vol. 47:ARVO Abstract 4403.
Reeves 2004 {published data only}
- Reeves BC, Harper RA, Russell WB. Enhanced low vision rehabilitation for people with age related macular degeneration: a randomised controlled trial. British Journal of Ophthalmology 2004;88(11):1443‐9. [DOI] [PMC free article] [PubMed] [Google Scholar]
Rohrschneider 1998 {published data only}
- Rohrschneider K, Riede B, Blankenagel A. Image flicker frequency of television reading aids. Effect on reading comfort for visually handicapped patients [Bildwiederholfrequenz von Bildschirmlesegeraten. Einfluss auf die Lesefahigkeit von Sehbehinderten]. Ophthalmologe 1998;95(2):110‐3. [DOI] [PubMed] [Google Scholar]
Rosenberg 1989 {published data only}
- Rosenberg R, Faye E, Fischer M, Budick D. Role of prism relocation in improving visual performance of patients with macular dysfunction. Optometry and Vision Science 1989;66:747‐50. [DOI] [PubMed] [Google Scholar]
Rossi 1990 {published data only}
- Rossi PW, Kheyfets EJ, Reding MJ. Fresnel prisms improve visual perception in stroke patients with homonymous hemianopia or unilateral visual neglect. Neurology 1990;40(10):1597‐9. [DOI] [PubMed] [Google Scholar]
Scott 2002 {published data only}
- Scott IU, Feuer WJ, Jacko JA. Impact of graphical user interface screen features on computer task accuracy and speed in a cohort of patients with age‐related macular degeneration. American Journal of Ophthalmology 2002;134(6):857‐62. [DOI] [PubMed] [Google Scholar]
Wolffshon 2002 {published data only}
- Wolffsohn JS, Dinardo C, Vingrys AJ. Benefit of coloured lenses for age‐related macular degeneration. Ophthalmic and Physiological Optics 2002;22(4):300‐11. [DOI] [PubMed] [Google Scholar]
References to studies awaiting assessment
Demers‐Turco 2001 {published data only}
- Demers‐Turco P, Sonsino J, Arai M, Hirose T. Comparison of three low vision reading devices. Investigative Ophthalmology and Visual Science 2001;42:ARVO Abstract 4598. [Google Scholar]
Goodrich 1998 {published data only}
- Goodrich GL, Kirby J, Keswick C, Donald B, Oros T, Wagstaff P, et al. Low vision reading: effect of field loss, training and device. American Academy of Optometry 1998:25.
Goodrich 2000a {published data only}
- Goodrich GL, Kirby J. A comparison of low vision reading performance by type of reading aid and patient field characteristic. Optometry and Vision Science 2000;77(12):126. [Google Scholar]
Goodrich 2001a {published data only}
- Goodrich G. Nomad: a preliminary study of possible rehabilitation applications. Optometry and Vision Science 2001;78(12):291. [Google Scholar]
Kaida 2005 {published and unpublished data}
- Kaida M, Maeda J, Inoue K, Murasawa M, Yamaguchi M, Nakamura H, et al. A hand‐held retinal projection system as a low‐vision aid. Japanese Journal of Clinical Ophthalmology 2005;59(4):437‐40. [Google Scholar]
Sonsino 2000 {published data only}
- Sonsino J, Demers‐Turco P, Arai M, Fujita K, McCabe P, Hirose T. Reading performance of a new portable head‐mounted closed circuit television for low vision patients: Powervision. Optometry and Vision Science 2000;77(12):239. [Google Scholar]
Additional references
Ahn 1995a
- Ahn JS, Legge GE, Luebker A. Printed cards for measuring low‐vision reading speed. Vision Research 1995;35(13):1939‐44. [DOI] [PubMed] [Google Scholar]
Ahn 1995b
- Ahn SJ, Legge GE. Psychophysics of reading. XIII. Clinical predictors of magnifier‐aided reading speed in low vision. Vision Research 1995;35(13):1931‐8. [DOI] [PubMed] [Google Scholar]
Alderson 2002
- Alderson P, Green S. Additional Module 2 In: The Cochrane Collaboration open learning material for reviewers. 2002. www.cochrane‐net.org/openlearning/PDF/Openlearning‐full.pdf (accessed 15 June 2006).
Binns 2012
- Binns AM, Bunce C, Dickinson C, Harper R, Tudor‐Edwards R, Woodhouse M, et al. How effective is low vision service provision? A systematic review. Survey of Ophthalmology 2012;57(1):34‐65. [DOI] [PubMed] [Google Scholar]
Cheng 2001
- Cheng D, Woo GC. The effect of conventional CR39 and Fresnel prisms on high and low contrast acuity. Ophthalmic and Physiological Optics 2001;21(4):312‐6. [DOI] [PubMed] [Google Scholar]
Congdon 2003
- Congdon NG, Friedman DS, Lietman T. Important causes of visual impairment in the world today. JAMA 2003;290(15):2057‐60. [DOI] [PubMed] [Google Scholar]
Congdon 2004
- Congdon N, O'Colmain B, Klaver CC, Klein R, Muñoz B, Friedman DS, et al. Causes and prevalence of visual impairment among adults in the United States. Archives of Ophthalmology 2004;122(4):477‐85. [DOI] [PubMed] [Google Scholar]
Covidence [Computer program]
- Veritas Health Innovation. Covidence. Version accessed 19 January 2018. Melbourne, Australia: Veritas Health Innovation, 2015.
Culham 2005 (pers comm)
- Culham 2005. Randomisation used in the trial. Email to: L Culham 20 Aug 2005.
Deeks 2011
- Deeks JJ, Higgins JPT, Altman DG, editors. Analysing data and undertaking meta‐analyses. Higgins JPT, Green S (editors). Cochrane Handbook for Systematic Reviews of Interventions Version 5.1.0 (updated March 2011). The Cochrane Collaboration, 2011. Available from www.cochrane‐handbook.org. March 2011.
Deeks 2011b
- Deeks JJ, Higgins JP, Altman DG, editor(s). Chapter 9: Analysing data and undertaking meta‐analyses. In: Higgins JPT, Green S (editors). Cochrane Handbook for Systematic Reviews of Interventions Version 5.1.0 (updated March 2011). The Cochrane Collaboration, 2011. Available from www.handbook.cochrane.org.
Dickinson 1998
- Dickinson C. Low Vision: Principles and Practice. 4th Edition. Oxford: Butterworth‐Heinemann, 1998. [Google Scholar]
Dickinson C 2017 (pers comm)
- Dickinson C. information on randomisation sequence generation on the trial Taylor 2017. Email to: C dickinson 9 DEC 2017.
Elbourne 2002
- Elbourne DR, Altman DG, Higgins JPT, Curtin F, Worthington HV, Veil A. Meta‐analyses involving cross‐over trials: methodological issues. Journal of Clinical Epidemiology 2002;31(1):140‐9. [DOI] [PubMed] [Google Scholar]
Glanville 2006
- Glanville JM, Lefebvre C, Miles JN, Camosso‐Stefinovic J. How to identify randomized controlled trials in MEDLINE: ten years on. Journal of the Medical Library Association 2006;94(2):130‐6. [PMC free article] [PubMed] [Google Scholar]
Goodrich 2007 (pers comm)
- Goodrich 2007. Randomisation sequence generation in the trial. Email to: G Goodrich 21 JAN 2007.
GRADEpro 2014 [Computer program]
- McMaster University (developed by Evidence Prime). GRADEpro GDT. Version accessed 4 December 2017. Hamilton (ON): McMaster University (developed by Evidence Prime), 2014.
Higgins 2011a
- Higgins JP, Altman DG, Sterne JAC, editor(s). Chapter 8: Assessing risk of bias in included studies. In: Higgins JP, Green S, editor(s). Cochrane Handbook for Systematic Reviews of Interventions Version 5.1.0 (updated March 2011). The Cochrane Collaboration, 2011. Available from handbook.cochrane.org.
Higgins 2011b
- Higgins JP, Deeks JJ, Altman DG, editor(s). Chapter 16: Special topics in statistics. In: Higgins JPT, Green S (editors). Cochrane Handbook for Systematic Reviews of Interventions Version 5.1.0 (updated March 2011). The Cochrane Collaboration, 2011. Available from www.handbook.cochrane.org.
Hirji 2009
- Hirji KF, Fagerland MW. Outcome based subgroup analysis: a neglected concern. Trials 2009;10:33. [DOI] [PMC free article] [PubMed] [Google Scholar]
Hooper 2008
- Hooper P, Jutai JW, Strong G, Russel‐Minda E. Age‐related macular degeneration and low‐vision rehabilitation: a systematic review. Canadian Journal of Ophthalmology 2008;43(2):180‐7. [DOI] [PubMed] [Google Scholar]
Humphry 1986
- Humphry RC, Thompson GM. Low vision aids ‐ evaluation in a general eye department. Transactions of the Ophthalmological Societies of the United Kingdom 1986;105(Pt 3):296‐303. [PubMed] [Google Scholar]
Jackson 2017 (pers comm)
- Jackson ML. Additional data on trial results. Email to: ML Jackson 14 DEC 2017.
Johnson 2017
- Johnson A (pers comm). Additional data and the identification of an earlier duplicate publication of Morrice 2017 as an ARVO abstract. Email to: A Johnson 9 DEC 2017.
Langelaan 2007
- Langelaan M, Nispen RMA. Multidisciplinary rehabilitation and monodisciplinary rehabilitation for visually impaired adults. Cochrane Database of Systematic Reviews 2007, Issue 2. [DOI: 10.1002/14651858.CD006543] [DOI] [Google Scholar]
Lavinsky 2001
- Lavinsky J, Tomasetto G, Soares E. Use of a contact lens telescopic system in low vision patients. International Journal of Rehabilitation Research 2001;24(4):337‐40. [DOI] [PubMed] [Google Scholar]
Leat 1994
- Leat SJ, Fryer A, Rumney NJ. Outcome of low vision aid provision: the effectiveness of a low vision clinic. Optometry and Visual Science 1994;71(3):199‐206. [DOI] [PubMed] [Google Scholar]
Legge 1985a
- Legge GE, Pelli DG, Rubin GS, Schleske MM. Psychophysics of reading. I. Normal vision. Vision Research 1985;25(2):239‐52. [DOI] [PubMed] [Google Scholar]
Legge 1985b
- Legge GE, Rubin GS, Pelli DG, Schleske MM. Psychophysics of reading. II. Low vision. Vision Research 1985;25(2):253‐65. [DOI] [PubMed] [Google Scholar]
Legge 1989
- Legge GE, Ross JA, Maxwell KT, Luebker A. Psychophysics of reading. VII. Comprehension in normal and low vision. Clinical Vision Sciences 1989;4:51‐60. [Google Scholar]
Legge 1991
- Legge G, Glenn A. Fry Award Lecture 1990: three perspectives on low vision reading. Optometry and Vision Science 1991;68(10):763‐9. [DOI] [PubMed] [Google Scholar]
Legge 2007
- Legge GE. Psychophysics of Reading in Normal and Low Vision. Mahwah, NJ & London: Lawrence Erlbaum Associates, 2007. [Google Scholar]
Margrain 1999
- Margrain TH. Minimising the impact of visual impairment. Low vision aids are a simple way of alleviating impairment. BMJ 1999;318(7197):1504. [DOI] [PMC free article] [PubMed] [Google Scholar]
Markowitz 2013
- Markowitz SN, Reyes SV, Sheng L. The use of prisms for vision rehabilitation after macular function loss: an evidence‐based review. Acta Ophthalmologica 2013;91:207‐11. [DOI] [PubMed] [Google Scholar]
Massof 1998
- Massof RW. A systems model for low vision rehabilitation. II. Measurement of vision disabilities. Optometry and Visual Science 1998;75(5):349‐73. [DOI] [PubMed] [Google Scholar]
Nilsson 1990
- Nilsson UL. Visual rehabilitation with and without educational training in the use of optical aids and residual vision. A prospective study of patients with advanced age‐related macular degeneration. Clinical Vision Sciences 1990;6(1):3‐10. [Google Scholar]
Pascolini 2011
- Pascolini D, Mariotti SP. Global estimates of visual impairment: 2010. British Journal of Ophthalmology 2012;96(5):614‐8. [DOI] [PubMed] [Google Scholar]
Rubin 2013
- Rubin GS. Measuring reading performance. Vision Research 2013;90:43‐51. [DOI] [PubMed] [Google Scholar]
Schünemann 2011
- Schünemann HJ, Oxman AD, Higgins JPT, Vist GE, Glasziou P, Guyatt GH. Chapter 11: Presenting results and 'Summary of findings' tables. In: Higgins JPT, Green S (editors), Cochrane Handbook for Systematic Reviews of Interventions. Version 5.1.0 (updated March 2011). The Cochrane Collaboration, 2011. Available from handbook.cochrane.org.
Scott 1999
- Scott I, Smiddy W, Schiffman J, Feuer W, Pappas C. Quality of life of low vision patients and the impact of low vision services. American Journal of Ophthalmology 1999;128(1):54‐61. [DOI] [PubMed] [Google Scholar]
Shuttleworth 1995
- Shuttleworth GN, Dunlop A, Collins JK, James CR. How effective is an integrated approach to low vision rehabilitation? Two year follow up results from south Devon. British Journal of Ophthalmology 1995;79(8):719‐23. [DOI] [PMC free article] [PubMed] [Google Scholar]
Sloan 1971
- Sloan LL, Ryan SJ Jr. Reading aids for the partially sighted. A nontechnical explanation of basic optical principles. International Ophthalmology Clinics 1971;11(1):19‐55. [PubMed] [Google Scholar]
Smallfield 2013
- Smallfield S, Clem K, Myers A. Occupational therapy interventions to improve the reading ability of older adults with low vision: a systematic review. American Journal of Occupational Therapy 2013;67(3):288‐95. [DOI] [PubMed] [Google Scholar]
Stelmack 2005 (pers comm)
- Stelmack J. Randomisation generation and allocation concealment used in trial. Email to: J Stelmack 10 Aug 2005.
Sterne 2011
- Sterne JAC, Egger M, Moher D editor(s). Chapter 10: Addressing reporting biases. In: Higgins JPT, Green S (editors). Cochrane Handbook for Systematic Reviews of Interventions Version 5.1.0 (updated March 2011). The Cochrane Collaboration, 2011. Available from www.handbook.cochrane.org.
Tielsch 1990
- Tielsch JM, Sommer A, Witt K, Katz J, Royall RM. Blindness and visual impairment in an American urban population. The Baltimore Eye Survey. Archives of Ophthalmology 1990;108(2):286‐90. [DOI] [PubMed] [Google Scholar]
VA HTA 2003
- Veteran Affairs Technology Assessment Program. Optical devices for adults with low vision. A systematic review of published studies of effectiveness. www.va.gov/VATAP/docs/OpticalDevicesAdultsLowVision2003tm.pdf 2003.
Virtanen 1991
- Virtanen P, Laatikainen L. Primary success with low vision aids in age‐related macular degeneration. Acta Ophthalmologica Copenhagen 1991;69(4):484‐90. [DOI] [PubMed] [Google Scholar]
WHO 2002
- World Health Organization. Towards a common language for functioning, disability and health. www.who.int/classifications/icf/training/icfbeginnersguide.pdf (accessed 17 July 2011).
WHO 2010
- World Health Organization. International Classification of Diseases (ICD). www.who.int/classifications/icd/en/index.html (accessed 15 Jan 2012).
Wolffsohn 2003
- Wolffsohn 2003 (pers comm). Additional data on Peterson 2003. Email to: JSW Wolffsohn 31 JAN 2007.
References to other published versions of this review
Virgili 2006
- Virgili G, Acosta R. Reading aids for adults with low vision. Cochrane Database of Systematic Reviews 2006, Issue 4. [DOI: 10.1002/14651858.CD003303.pub2] [DOI] [PubMed] [Google Scholar]
Virgili 2013
- Virgili G, Acosta R, Grover LL, Bentley SA, Giacomelli G. Reading aids for adults with low vision. Cochrane Database of Systematic Reviews 2013, Issue 10. [DOI: 10.1002/14651858.CD003303.pub3] [DOI] [PMC free article] [PubMed] [Google Scholar]


