Abstract
Nonalcoholic Fatty Liver Disease (NAFLD) represents the leading cause of liver disease in developed countries but its diffusion is currently also emerging in Asian countries, in South America and in other developing countries. It is progressively becoming one of the main diseases responsible for hepatic insufficiency, hepatocarcinoma and the need for orthotopic liver transplantation. NAFLD is linked with metabolic syndrome in a close and bidirectional relationship. To date, NAFLD is a diagnosis of exclusion, and liver biopsy is the gold standard for diagnosis. NAFLD pathogenesis is complex and multifactorial, mainly involving genetic, metabolic and environmental factors. New concepts are constantly arising in the literature promising new diagnostic and therapeutic tools. One of the challenges will be to better characterize not only NAFLD development but overall NAFLD progression, in order to better identify NAFLD patients at higher risk of metabolic, cardiovascular and neoplastic complications. This review analyses NAFLD epidemiology and the different prevalence of the disease in distinct groups, particularly according to sex, age, body mass index, type 2 diabetes and dyslipidemia. Furthermore, the work expands on the pathophysiology of NAFLD, examining multiple-hit pathogenesis and the role of different factors in hepatic steatosis development and progression: genetics, metabolic factors and insulin resistance, diet, adipose tissue, gut microbiota, iron deposits, bile acids and circadian clock. In conclusion, the current available therapies for NAFLD will be discussed.
Keywords: nonalcoholic fatty liver disease, insulin resistance, metabolic syndrome, steatosis, molecular mechanisms, pathogenesis, therapy
1. Nonalcoholic Fatty Liver Disease: Definition and Diagnosis
Nonalcoholic Fatty Liver Disease (NAFLD) describes liver steatosis in the absence of secondary causes of hepatic fat accumulation such as alcohol abuse, defined as a daily alcohol consumption >20 g/day for women or >30 g/day for men [1]. Alcoholic liver disease and NAFLD are histologically similar and not discernible by mere biopsy. In everyday practice, the two conditions may often coexist; these cases warrant clinical judgement. In fact, we still do not have reliable markers to recognize the percentage of damage due to metabolic factors and due to other toxins (e.g., ethanol). In addition, in NAFLD, alcohol consumption may act as a cofactor for cirrhosis development [2].
NAFLD is a diagnosis of exclusion, and conventionally there are two possible approaches to the diagnosis: invasive and non-invasive assessment. This is worthy of interest because according to the methodology used, there is great variability in the prevalence rates reported in various studies. Liver biopsy represents the gold standard for the diagnosis, requiring the presence of steatosis affecting >5% of hepatocytes. Also, non-invasive techniques can effectively quantify the composition of fat in liver tissue. For example, sonography is an easily available tool, it is cheap, and it effectively recognizes steatosis if fatty infiltration is >10% [3]. Moreover, ultrasound-based elastography, which includes transient elastography (TE), acoustic radiation force imaging (ARFI) and shear-wave elastography, shows an accuracy of approximately 90% in detecting advanced fibrosis and cirrhosis [4]. Unenhanced Computed Tomography (CT) provides high performance in diagnosing steatosis only if fatty infiltration is >30%, mainly evaluating the attenuation value of the liver, possibly compared to the spleen; moreover, CT is a more expensive method and it carries risks related to radiation exposure [5,6,7]. Magnetic resonance spectroscopy (MRS) and quantitative fat/water selective magnetic resonance imaging (MRI) are accepted methods to identify NAFLD [1,8]. MRI and MRS have higher sensitivity and specificity than ultrasonography; however, they are more expensive and not routinely available in clinical settings [9,10]. Other studies used blood tests, for example, elevated liver enzymes (e.g., Glutamic Pyruvic Transaminase GPT) as a marker of liver steatosis, but aminotransferase levels may be normal in up to 78% of patients with NAFLD [5,6,11]. Moreover, as demonstrated in the Dionysos nutrition and liver study, NAFLD shows a similar prevalence in people with and without suspected liver disease, which means that the use of markers such as GPT for a suspected fatty liver should be discouraged because of the intrinsic risk of disease underestimation [12]. Several scores, combining different serum biomarkers and metabolic parameters, have been proposed to estimate the probability of diagnosing liver steatosis [4]. This is very useful especially in population studies, where carrying out a liver sonography for mass screening is impractical, to say the least. Among the most accepted scores there are the fatty liver index (FLI) [13], the NAFLD liver fat score [14] and the SteatoTest [15]. While the last is a commercial kit, the FLI and the NAFLD liver fat score are based on serum triglycerides (TG), gamma-glutamyl transferase, insulin, aminotransferases, waist circumference, BMI and presence of metabolic syndrome or type 2 diabetes [16]. Other scores estimate the probability of having NASH or advanced fibrosis, which is very interesting since these scores allow the physician to bypass an invasive liver biopsy. Among them, the most validated scores are the NAFLD fibrosis score [17] and the FIB-4 [18], which are based on platelet count, aminotransferases and albumin. However, it seems that the best diagnostic performance to detect advanced fibrosis is obtained combining both imaging (e.g., magnetic resonance or transient elastography) and serum biomarkers [4,19,20]. Finally, an extremely interesting new area of research is the use of blood circulating RNA sequences, especially miRNA, for the diagnosis and staging of NAFLD (“liquid biopsy”) [21]; however, a full explanation of these techniques is beyond the scope of this review.
Differential Diagnosis
As mentioned above, NAFLD is a diagnosis of exclusion. It is mandatory to exclude excessive alcohol consumption and other causes of liver steatosis such as hepatitis C virus (HCV), which nowadays is drastically diminishing thanks to novel effective direct acting agents, autoimmune hepatitis, coeliac disease, Wilson’s disease, hemocromatosis, a/hypo-betalipoproteinemia, and other rare causes of liver steatosis (Table 1).
Table 1.
Differential diagnosis of NAFLD. Several conditions associated with liver steatosis are shown in this table, with possible pathogenetic mechanisms and associated references.
| Conditions Associated with Liver Steatosis | Mechanism of Action | References |
|---|---|---|
| Alcohol (>20 g/day (women) or >30 g/day (men)) | Redox state shift: fatty acid oxidation inhibition, induction of lipogenesis Altered VLDL secretion in the liver |
[22] |
| HCV | Altered VLDL secretion in the liver Insulin resistance Mitochondrial dysfunction and oxidative stress |
[23] |
| Medications (e.g., methotrexate, corticosteroids, valproate) | Fatty acid oxidation inhibition, induction of lipogenesis Mitochondrial dysfunction Impaired hepatic lipid secretion Insulin resistance |
[24] |
| Lipid metabolism disorders: a/hypo-betalipoproteinaemia, Wolman’s disease | Impaired hepatic lipid secretion Impaired hydrolysis of cholesteryl esters and triglycerides |
[25,26] |
| Metal storage disorders: Wilson’s disease | Copper-induced mitochondrial dysfunction | [27] |
| Autoimmune hepatitis | Drug-mediated effects | [28] |
| Coeliac disease | Weight gain on gluten-free diet Impaired hepatic lipid mobilization Intestinal malabsorption |
[29] |
| Endocrine disorders: hypothyroidism, hypopituitarism, polycystic ovary syndrome | Reduced hepatic lipid utilization Insulin resistance Impaired insulin secretion |
[30,31,32,33] |
| Starvation, parenteral nutrition | Impaired hepatic lipid secretion Reduced mitochondrial beta-oxidation |
[34] |
| Lipodystrophy | Insulin resistance and ectopic fat accumulation | [35] |
2. Epidemiologic Features and Relevance of NAFLD
NAFLD represents the leading cause of liver disease in Western countries; however, its diffusion is currently emerging also in developing countries [1,36,37]. According to a recent meta-analysis conducted by Younossi et al., the global prevalence of NAFLD in the adult population is 25% [37]. The most affected regions worldwide are South America (31%) and the Middle East (32%); also, some Asian countries show elevated prevalence rates, particularly in Japan where the prevalence exceeds 50%, it is almost 50% in Korea, followed by Singapore, India and China [38]. The United States and Europe show similar data (24%), with a reported prevalence rate in Italy of 20–25% [12,16]. As demonstrated by the Dionysos Study, fatty liver was present at sonography in 70% of a population from Northern Italy with elevated alanine transaminase levels [39,40]. On the other hand, Africa presents the lowest prevalence (14%). It is interesting to note that the incidence of NAFLD is constantly increasing, paralleling the epidemy of obesity and diabetes, though it is not clear if fatty liver is the cause or the consequence of an impaired metabolic status [41,42]. Data from National Health and Nutrition Examination Surveys report that NAFLD was responsible for chronic liver disease in 46.8% of cases between 1988 and 1994, while from 1994 to 2004, it accounted for 75.1% of cases [36]. A mathematical model has recently been used to forecast how the NAFLD disease burden will change from 2016 to 2030 in eight countries representing approximately 25% of the total global population [42]. According to this study, the NAFLD prevalence in Italy will evolve from 25.4 to 29.5%, which is the highest prevalence in the analyzed countries, with higher rates of NASH (6.3% in 2030 versus 4.4% in 2016). The increasing prevalence is observed in all the countries taken into account. The highest prevalence growth will be observed in China, as a consequence of urbanization. Finally, liver-related mortality will accordingly increase, with 10490 expected deaths for liver disease in Italy in 2030 instead of the 4870 deaths observed in 2016. This is probably the result of both population aging and “diabesity” epidemics.
NAFLD is also progressively becoming one of the main diseases responsible for hepatic insufficiency, HCC and the need for orthotopic liver transplantation (OLT) [43]. According to the American Association for the Study of Liver Disease (AASLD), Nonalcoholic Steatohepatitis (NASH) represents the second cause after HCV of HCC-related OLT [44]. Even though less data are available regarding NAFLD as a cause of liver transplantation in Europe, it is clear that NASH is emerging as the real cause of many OLTs carried out for “cryptogenic cirrhosis”, estimated to be responsible of 4% of European liver transplantation [45,46,47]. According to the 2018 Annual Report of the European Liver Transplant Registry (ELTR), NASH accounts for 1% of the OLTs carried out in Europe between 1988 and 2016, and almost all cases of OLTs for NASH have been reported in the last 15 years [48]. According to the authors of the report, NASH is going to become the leading cause of OLT within the next 10 years. Notably, coexisting metabolic risk factors in these patients considerably increase the periprocedural and postprocedural risks of surgical procedures [49], so that many patients may be excluded from the transplant waiting list because of severe comorbidities and likely poor outcome [49]. NAFLD recurrence and de novo NAFLD after OLT represent a novel challenge for hepatologists and transplant surgeons [50]. In fact, patients undergoing OLT often develop metabolic complications such as arterial hypertension, diabetes and dyslipidemia, probably also because of adverse effects of immunosuppressive drugs [51].
The prevalence of NAFLD increases with age [37], and older people seem to have a higher NASH prevalence rate and higher degree of fibrosis, evaluated by TE [52], and liver biopsy [53]. This could be explained by a lower metalloproteinases activity and consequently reduced collagenolysis [54]. Moreover, the hepatic volume appears to be reduced in the elderly, probably as a result of decreased hepatic blood flow [55]; this finding could influence the results of TE. Generally, older age is associated with increased susceptibility to oxidative stress and oxidative damage, albeit contrasting data are reported in the literature [55]. An interesting study by Collins et al. connected the enhanced fibrogenesis of the aged liver with changes in the immune system and particularly in macrophage response [56].
Children are not spared from liver steatosis. Pediatric NAFLD is a well-recognized entity that is increasingly raising concerns in the endocrine and pediatric community [57]. It has been demonstrated that, although the pathological factors are similar to the adults, patients with pediatric NAFLD exhibit some histological differences that probably warrant a different histological score [58]. Even in early onset, NAFLD seems to increase the risk of hepatic insufficiency and leads to greater mortality compared to the general population of the same age and sex [59]. As shown in a recent Swedish cohort study, an elevated body mass index (BMI) in young adults is significantly associated with an increased risk of developing severe liver disease later in life [60]. Notably, puberty is associated with insulin resistance; the reason for this phenomenon is not entirely defined, but a possible role may be played by sexual hormones. Since insulin resistance favors NAFLD development, puberty may increase the risk of fatty liver and may exacerbate NASH; however, literature data are discordant on this specific issue [57,61,62].
NAFLD is strongly associated with metabolic comorbidities such as obesity (51%), type 2 diabetes (22.5%), dyslipidemia (69%), and hypertension (39.3%) [37]. These prevalence rates increase considering patients with NASH (Table 2). On the other hand, according to a project carried out by the Italian Arteriosclerosis Society, the prevalence of ultrasound-diagnosed NAFLD in a nondiabetic population with metabolic syndrome was 78.8% [63].
Table 2.
Prevalence of metabolic comorbidities in patients with NAFLD and NASH—Data by Younossi [37].
| NAFLD | NASH | |
|---|---|---|
| Obesity | 51% | 82% |
| Diabetes mellitus | 23% | 47% |
| Metabolic syndrome | 41% | 71% |
| Hyperlipidemia/dyslipidemia | 69% | 72% |
| Hypertension | 39.34% | 67.97% |
As shown by Lomis et al., NAFLD prevalence increases linearly with BMI, reaching an up to 14-fold higher risk at BMIs of 37.5–40 Kg/m2, compared to the normal weight population [64]. As expected, the absolute risk was higher in diabetic patients, for any given BMI. Particularly, concerning NAFLD risk, the presence of diabetes in a normal weight population was equivalent to a 5–10 Kg/m2 increase in BMI. In fact, up to 70% of patients with diabetes mellitus show fatty liver disease [65,66] and patients with NAFLD and diabetes exhibit a more severe grade of inflammation at liver biopsies and a more rapid evolution toward HCC. Koehler et al., examining the data from the Rotterdam Study, demonstrated that the coexistence of NAFLD and diabetes was associated with a higher risk of developing liver fibrosis [37,52], and the elevated values of stiffness in these patients were not influenced by age. Moreover, not only a personal history of diabetes, but also familiarity for hyperglycemia has been associated with an increased risk of developing NASH in NAFLD patients [67]. Finally, the presence of diabetes increases mortality in NAFLD patients [68]. On the other hand, it is important to mention that the presence of NAFLD increases the risk of hyperglycemia and, in already diabetic patients, intensifies the risk of metabolic decompensation [41]. Thus, the relationship between NAFLD and insulin resistance is mutual.
Although the incidence of NAFLD directly correlates with BMI [64], it should be kept in mind that also the lean population can be affected with a reported prevalence of non-obese fatty liver disease ranging from 10 to 30% [69]. BMI and waist circumference are not perfectly reliable predictors of visceral adiposity, which is the main adipose form responsible for insulin resistance and NAFLD. In fact, it is believed that insulin resistance still plays a role in these metabolically obese but normal weight (MONW) patients [70,71,72]. Several studies have demonstrated an association between lean NAFLD and metabolic risk factors such as dyslipidemia, hyperglycemia and visceral adiposity [73,74]. Moreover, fructose consumption and a cholesterol-rich diet have been linked to non-obese NAFLD development [75,76,77]. Finally, genetic and epigenetic factors probably play a fundamental role [73,78]. Interestingly, the histologic features of non-obese NAFLD are equivalent to the obese form, and mortality is similarly increased in both groups when compared to the general population [69].
Similar to metabolic syndrome, lipid status in NAFLD includes elevated TG and low density lipoprotein cholesterol (LDL), and particularly increased small dense LDL (sdLDL), with low high-density lipoprotein cholesterol (HDL)-cholesterol [79,80,81]. This atherogenic dyslipidemia may, in part, justify the elevated cardiovascular risk of these patients. In addition, postprandial lipemia, defined as a rise in TG lipoproteins after the consumption of a meal, has been demonstrated to be higher in NAFLD patients compared to controls, with an emerging role in oxidative stress and cardiovascular disease [82,83,84]. Moreover, lipoprotein(a) increases with NAFLD severity [85]. Finally, as described below, several mutations of genes involved in lipidic metabolism have been associated with NAFLD development and severity [86,87].
It is widely accepted that NAFLD is more common in men than in women [88]. This is probably due to a protective role of estrogens in premenopausal women. It has been demonstrated, indeed, that these hormones have anti-inflammatory, antioxidant, antiapoptotic and probably antifibrotic effects, and thus hepatoprotective action [89,90,91]. In addition, estrogens favor subcutaneous fat accumulation rather than ectopic visceral fat, weakening the atherogenic effects typical of the distribution of the latter [92,93]. Remarkably, visceral adipose tissue deposits release free fatty acids directly in the portal venous flow, thus directly reaching the liver [94]. After menopause, ovarian senescence dramatically increases NAFLD risk, thus the idea of “sexual dimorphism” of NAFLD is arising to describe the increased incidence of the disease in men and postmenopausal women [91,95]. This concept is partly due to metabolic differences, in terms of insulin sensitivity, reduced lipogenesis and central-type body fat distribution [93,96,97]. Moreover, it seems that the duration of estrogen deficiency correlates with fibrosis risk in NAFLD [98].
3. NAFLD Natural History
NAFLD includes a wide spectrum of liver damage, extending from benign hepatic fat deposition in the absence of inflammation to liver fibrosis and hepatocarcinoma (HCC). Generally, two pathologically distinct conditions are identified: nonalcoholic fatty liver (NAFL) and NASH. While NAFL is characterized by simple liver steatosis, NASH is defined by the presence of steatosis and lobular inflammation with hepatocyte ballooning degeneration, with or without any fibrosis [8,16]. Therefore, biopsy is mandatory to distinguish the two entities [99,100]. Previous studies stated that up to one third of patients with NAFLD have the more severe form of the disease [16,101,102]. It has been shown that in almost 50% of NAFLD-related HCC, patients do not have a frank cirrhosis, even though they probably have NASH instead of mere NAFL [103]. Especially in the presence of metabolic syndrome, HCC may develop in the absence of significant liver fibrosis [104]. This problem is clinically relevant: indeed, a recent study showed that NAFLD is currently the most common cause of HCC among Medicare patients [105]; furthermore, the presence of liver fibrosis at biopsy has been shown to be the best predictor of liver-related events and mortality in NAFLD [106]. On the other hand, recent data emerging from a cross-sectional liver biopsy cohort showed that one third of patients with advanced fibrosis have no NASH; in these individuals, the severity of steatosis and genetics play a major role in determining fibrosis [107]. Moreover, it is still not clear whether NASH stems from NAFL or whether it represents a distinct entity characterized by a different prognosis. A recent retrospective study conducted by McPherson et al. demonstrates that 44% of patients with NAFL can progress to NASH during a median follow-up period of 8 years and consecutively 37% of these subjects show fibrosis progression [108].
People affected by NAFLD have an increased mortality compared to the general population, mainly due to cardiovascular deaths [8,109]. Furthermore, NASH patients exhibit greater liver-related mortality due to cirrhosis complications and HCC. Particularly, the evidence of any degree of fibrosis at liver biopsy leads to decreased survival time and greater need for liver transplantation [68].
4. Pathophysiological Features
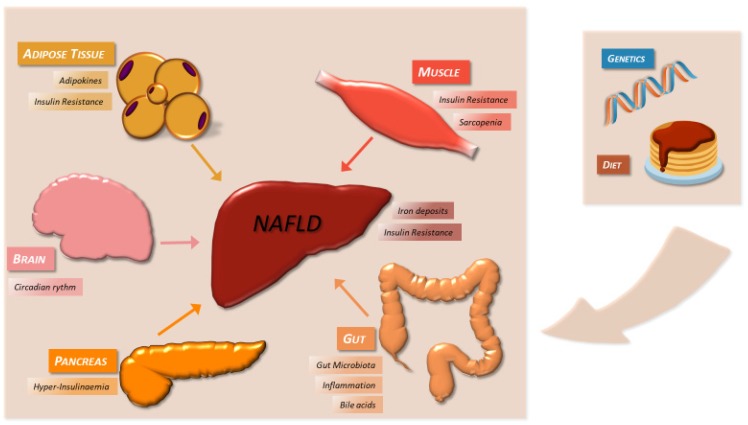
The pathogenesis of NAFLD is multifactorial. Genetic factors cooperate with metabolic and environmental factors to promote the accumulation of fat in hepatocytes. In the last decade of the 20th century, the most corroborated theory was the “two hit pathogenesis”. It stated that insulin resistance leads to TG deposition in the liver, thus steatosis, rendering it more susceptible to the action of second hits, such as oxidative stress, ATP depletion and endotoxins, finally leading to inflammation, fibrosis and cancer. Nowadays, this theory has been replaced by the “multiple hit pathogenesis”. This states that multiple etiopathogenic factors act in a parallel or sequential and somehow synergic way on a genetically predisposed subject, to cause NAFLD and thus defining the spectrum of the disease phenotype (Figure 1) [110]. Particularly, some patients will develop NAFL and consequently NASH, but others will directly present inflammation and fibrosis, probably because of the influence of genetic and epigenetic factors.
Figure 1.
Multiple-hit pathogenesis of NAFLD [86,110,111]. Genetic factors cooperate with metabolic and environmental factors to promote the accumulation of fat in hepatocytes and successively cause inflammation, cellular death and fibrosis. Anatomically, besides the liver, the main factors are insulin sensitive organs such as adipose tissue and muscle, which respectively produce adipokines and myokines, and also promote inflammation and oxidative stress in the liver. The gut microbiota releasing PAMPs, the bile acid system and the presence of iron deposits contribute to liver damage. Finally, all these mechanisms are modulated by the brain, particularly by circadian rhythm.
The hallmark feature determining NAFLD is TG accumulation in the liver, as a result of an imbalance between fatty acid (FA) influx and FA efflux [16]. An interesting study using stable isotope labelling techniques demonstrates that 74% of hepatic TG in NAFLD derives from exogenous sources, particularly from serum non-esterified fatty acids (NEFA) and from diet, while only 26% comes from hepatic de novo lipogenesis (DNL) [112]. DNL seems to be increased up to threefold in NAFLD patients compared to controls [111] and, curiously, it fails to increase postprandially, since its activity is already elevated in the fasting state. Regarding TG balance in the liver, an impaired hepatic beta-oxidation of FA contributes to NAFLD. One of the main contributors to impaired FA utilization is malonil-CoA generated during DNL. It is indeed a steric inhibitor of mithocondrial carnitine-O-palmitoyltransferase 1 (CPT1), which is the key rate-limiting enzyme for beta-oxidation [113]. TG excretion through very-low density lipoproteins (VLDL) seems to be increased in NAFLD but it is still not sufficient to compensate for the excessive inflow in the liver [111].
As mentioned above, up to one-third of NAFLD patients develop NASH, which increases the risk of fibrosis and cancer [16,101,102]. NASH develops when physiological adaptive mechanisms of the liver are overwhelmed by the excessive influx of TG, leading to lipotoxicity, inflammation, radical oxygen species (ROS) formation and hepatocellular dysfunction [16,111,114]. TG formation is a protective mechanism for the liver. However, when an excessive amount of FA reaches the hepatocyte, the mitochondria increase FA utilization through beta-oxidation and oxidative phosphorylation; furthermore, peroxisomes and endoplasmic reticulum (RE) also contribute to FA oxidation. The drawback of this process is ROS formation that, in excessive quantity, consumes the antioxidant mechanisms of the cell and leads to protein and lipid peroxidation, DNA damage and inflammation. Interestingly, mitochondrial function decreases in more advanced stages of NASH, generating a vicious cycle [115].
Concerning HCC, the pathogenesis of a cirrhotic liver has been widely described. Chronic injury with constant regeneration stimulus, oxidative stress and consequently DNA damage, act together to favor the development of liver cancer. In the presence of NASH, several other mechanisms contribute to carcinogenesis: hyperinsulinemia and anabolic stimulus [116], the lipogenic pathway with more available sources of energy [117], lipotoxicity through oxidative and probably direct pro-oncogenic effects [118,119], low-grade inflammation and visceral obesity with altered adipokine homeostasis [86,120].
4.1. Genetic Factors
Interethnic variations and familial aggregation, associated with the fact that NAFLD is not always sufficiently supported by the presence of environmental and metabolic factors, convinced the scientific community that genetic factors may play a key role in liver steatosis. Genome-wide association and gene expression profiling studies have associated several genes to the development and progression of NAFLD. These sequences play a central role in different pathways: lipogenesis, FA oxidation, lipoprotein transport, glucose homeostasis, detoxification and inflammation. Since the pathogenesis of NAFLD is multifactorial, the interaction with the environment is still crucial [118,121].
Palatin-like phospholipase domain containing 3 (PNPLA3) variant allele (rs738409). In 2008, Romeo et al. conducted the first genome-wide association study of nonsynonymous sequence variations in patients with NAFLD [122]. They found a strong association between fatty liver and the PNPLA3 variant rs738409 C>G p.I148M, which causes a loss of function that is statistically more prevalent in the Hispanic population, thus justifying the major incidence of NAFLD reported in this population. Interestingly, even though the I148M variant predisposes patients to liver steatosis, it seems to not influence insulin sensitivity. The presence of this variant also implies a major risk of progression of liver damage, independently from the presence of age, gender or other metabolic risk factors such as insulin sensitivity and BMI, not only in NAFLD but also in alcoholic and viral liver disease [107,123,124,125,126]. PNPLA3 is alternatively known as calcium-independent phospholipase A2 epsilon (iPLA2-ε) or adiponutrin and it is the member of a lipid metabolizing enzyme family. It owes its name to the strong analogy of sequence with patatin, a major protein of potato tubers with nonspecific lipid acyl hydrolase activity. PNPLA3 is involved in triglyceride hydrolysis in hepatocytes and it stimulates retinyl ester release from HSC. Its levels notably increase during the postprandial phase under stimulation of insulin through SREBP-1c and ChREBP [125]. This mechanism has been proposed to explain the association between liver steatosis and PNPLA3 variants: an interaction between different allele variants of PNPLA3 (E434K/434E/148I/148M) may determine liver damage, probably influencing TG release from lipid droplets [127]. Moreover, Bruschi et al. recently demonstrated that the PNPLA3 I148M variant modulates HSC activity, leading to a pro-inflammatory and pro-fibrogenetic phenotype [128]. On the other hand, the presence of the 453I variant of PNPLA3 was associated with a lower hepatic fat content. It seems reasonable that a loss of function of this gene causes a reduction in hepatic TG outflow, favoring hepatic steatosis.
Transmembrane 6 superfamily member 2 (TM6SF2) is involved in VLDL secretion [129], and a loss of function due to a single nucleotide polymorphism (rs58542926) has been linked to liver steatosis, inflammation and fibrosis [130,131,132]. It is noteworthy that this mutation seems to confer cardiovascular protection, questioning the relationship between NAFLD and cardiovascular disease. This is probably due not only to the reduction of circulating apolipoprotein B lipoproteins, but also to a complex anti-inflammatory effect [133,134].
Glucokinase regulator (GCKR) is a modulator of hepatic glucokinase, and the rs1260326-T variant leads to an uncontrolled glucose uptake by hepatocytes, with increased glycolysis, decreased beta-oxidation and hepatic lipid accumulation [135,136].
Cholesteryl ester transfer protein (CETP) is involved in reverse cholesterol transport, particularly in cholesterol esters and the TG exchange between HDL and ApoB-containing lipoproteins. It is primarily derived from Kupffer cells [137]. The variant rs1800777 of this gene has recently been associated with liver steatosis and lobular inflammation in patients with biopsy proven NAFLD [138].
Sterol regulatory element-binding protein 1c (SREBP-1c), as mentioned above, is the main inducer of hepatic DNL under insulin stimulation. Musso et al. demonstrated that a single nucleotide polymorphism of this gene (rs11868035 A/G) is associated with NAFLD development, along with insulin resistance and atherogenic dyslipidemia [139].
Membrane bound O-acyltransferase domain-containing 7 (MBOAT7) gene variant rs641738 C>T has been associated with liver steatosis development and severity, but not with insulin resistance [140]. A study conducted by Krawczyk et al., on the other hand, demonstrated an association between this variant and liver fibrosis but not with liver steatosis [141]. Finally, Umano et al. recently reported that the rs626283 variant may predispose obese Caucasian adolescents and children to NAFLD and insulin resistance [141]. MBOAT7 is a lysophosphatidylinositol acyltransferase involved in arachidonic acid metabolism [142].
Microsomal triglyceride transfer protein (MTTP) acts as a chaperon involved in apolipoprotein B (ApoB) lipoprotein assembly [143]. The 493 G/T polymorphism has been associated with NAFLD development and metabolic syndrome [144].
Besides the above-mentioned genes, many others have been studied, including Superoxide dismutase 2 (SOD2), Glutathione S-transferase (GST), TNF-α, Peroxisome proliferator-activated receptor α (PPARA), Apolipoprotein C-III (APOC3), and Interleukin-6 (IL6) [86].
4.2. Insulin Resistance and Metabolic Factors
Insulin resistance has traditionally been identified as the key pathophysiological factor in NAFLD [145]; thus, many authors consider NAFLD as the hepatic manifestation of metabolic syndrome. However, in recent years the causal role of insulin resistance in determining NAFLD has been questioned, since NAFLD often precedes and, to a larger extent, predicts the development of obesity, diabetes, dyslipidemia, arterial hypertension and cardiovascular disease [16,41,146,147,148]. In other words, NAFLD and metabolic syndrome are linked in a bidirectional way.
4.2.1. Does Insulin Resistance Cause NAFLD?
Insulin signaling stimulates glucose utilization and favors lipid accumulation by acting on insulin sensitive organs such as muscle, adipose tissue and liver. If insulin resistance develops, hormone-sensitive lipase is not suppressed and consequently the adipose tissue releases a great amount of NEFA into the bloodstream, leading to ectopic deposition of fat in organs such as the liver and pancreas. Several NEFA-specific transporters have been described, not only in hepatocytes, but generally in hepatic cells, including macrophages. These transporters, e.g., fatty acid transport protein (FATP5), could be a potential target of therapy aiming at reducing hepatic NEFA intake and consequently NAFLD [149].
Besides inhibiting lipolysis, insulin also stimulates hepatic DNL mainly through the sterol regulatory element binding protein 1c (SREBP1c) and the liver X receptor (LXR)—retinoid X receptor (RXR). Due to the lack of well-known reasons, this pathway seems to be spared from insulin resistance. This insulin signaling paradox, or so-called selective insulin resistance, explains the classic triad of type 2 diabetes, namely, hyperinsulinemia, hyperglycemia and hypertriglyceridemia [150]. Interestingly, it has been demonstrated that gluconeogenesis and DNL pathways diverge distally to the insulin receptor, since insulin receptor knockout (LIRKO) mice cut down not just the formation of glucose but also triglycerides [151]. An interesting point has been offered by Hijmans et al., who, embracing the concept of liver metabolic zonation, proposed a “model of zonation of insulin sensitivity along the portocentral axis” [152]. As a matter of fact, periportal hepatocytes seem to be the main factor responsible for gluconeogenesis and beta-oxidation, while pericentral cells are mainly involved in DNL and glycolisis. Characteristically, in NAFLD, steatosis is more abundant in the pericentral zone and is rare in the periportal zone [153]. Hijmans et al. propose that insulin resistance leads to increased lypolisis in adipose tissue and thus an increased amount of NEFA arriving at the liver, specifically to periportal hepatocytes due to a “first-pass” mechanism. These cells are consequently more prone to developing insulin resistance, and this explains the impaired inhibition of gluconeogenesis in an insulin resistant organism. Following this, the pancreas further increases the secretion of insulin, which through the portal flux reaches the liver. The pericentral cells, still susceptible to insulin signaling, respond by increasing DNL. Interestingly, pediatric NAFLD may characteristically involve periportal areas, presuming a different pathophysiological mechanism of formation [154]. In addition, insulin stimulates the formation of triglycerides by activating acetyl-CoA carboxylase. Therefore, in NAFLD, DNL is still aroused by insulin signaling and enhances liver fat deposits [155].
Even hyperglycemia activates DNL, but through a different pathway that involves the carbohydrate response element binding protein (ChREBP). This is activated by an intermediate of glycolysis such as glucose 6-phosphate or fructose-2,6-biphosphate. Moreover, it should be noticed that other conditions characterized by hyperglicemia do not necessarily result in steatosis. For example, type 1 diabetes leads to little accumulation of TG in the liver, maybe due to a compensation due to enhanced beta-oxidation [156].
4.2.2. Does NAFLD Cause Insulin Resistance?
The fatty acid deposits in the liver worsen hepatic insulin sensitivity, probably inducing the protein kinase C-ε (PKCε) to phosphorylate and inactivate the insulin receptor [157]. On the other hand, several studies demonstrate that metabolites such as ceramides may play a central role in mediating FA-induced insulin resistance, by acting at different levels of insulin signaling [158]. It is, however, important to recognize that even though PKCε and ceramides partly explain the bidirectional link between NAFLD and metabolic syndrome, others, such as the role of hepatokines, probably close the loop [41].
4.2.3. Other Metabolic Factors: The Role of Notch and The Skeletal Muscle
Notch signaling has been shown to influence virtually every metabolic organ, thus being involved in liver steatosis and fibrosis [159]. Notch signaling is an evolutionally highly conserved mechanism composed of ligands, receptors and intracellular proteins, regulated at different levels [160]. This pathway is a key mediator of cellular proliferation, differentiation and intercellular communication, especially during embryogenesis. During adulthood, it plays a role in organ regeneration and cancer [161,162]. Bi, in a recent review, analyzed the different influence of Notch signaling in metabolic organs: liver, adipose tissue, muscle, including central nervous system and the interaction with the immune system and angiogenesis [159]. Particularly, Notch signaling endorses gluconeogenesis and DNL, having a key role in hepatic insulin resistance. Notch signaling stimulates white adipose tissue differentiation, which is the main factor responsible for energy storage during hypercaloric diet. Moreover, it maintains cellular quiescence in the central nervous system and in the muscle, preserving stem cells but limiting tissue regeneration, and it favors the differentiation of an M1 macrophage phenotype, which is the main factor responsible for systemic inflammation, thus exacerbating peripheral insulin resistance. Finally, Notch signaling has been found to regulate angiogenesis, with a possible role in favoring atherosclerosis. All these mechanisms explain the concrete role of Notch signaling in NAFLD development, which is fundamentally mediated by the promotion of an insulin resistant phenotype. Confirming this concept, several animal studies show that Notch inhibition leads to an increased insulin sensitivity and novel drugs targeting Notch signaling are currently under evaluation with extremely promising results [163,164,165,166]. However, further studies are still needed to better understand Notch signaling and to definitely confirm the efficacy and safety of novel drugs targeting this pathway.
There is increasing interest in the role of sarcopenia in liver disease. The skeletal muscle plays a central role in insulin sensitivity, since it is one of the main factors responsible for insulin-induced glucose uptake [167]. Moreover, it sequesters NEFA from the blood and therefore blunts the burden of lipids reaching the liver. It seems therefore reasonable to hypothesize a role of muscle depletion in NAFLD development [168]. Accordingly, an association has recently been found between sarcopenia, steatosis and fibrosis in NAFLD [169]. In particular, recent reports are focusing on signaling molecules and hormones called ‘myokines’. They are molecules produced by the muscle, which is, indeed, not only a mere energy consumer, but is an active endocrine organ, capable of partly contrasting the inflammatory effect of adipokines [170]. Notably, this mechanism could partly explain the beneficial role of physical exercise on metabolic diseases [170]. The most studied myokine is irisin, which seems to stimulate brown adipose tissue differentiation and thermogenesis, with a protective function from metabolic syndrome, though clinical studies have shown contrasting data regarding its role in NAFLD patients [171].
4.3. Diet
As mentioned above, diet is responsible for 15% of liver TG in NAFLD [112]. The prevalence of NAFLD has increased remarkably worldwide with the spread of the diet of industrialized countries. Diet composition and energy intake seem to be related to NAFLD; however, more than fat consumption, it seems that carbohydrates are the main factors responsible for NAFLD [172,173]. They provide acetyl-CoA for DNL by entering the Krebs cycle, and they supply the glycerol skeleton for TG formation via triose-phosphate.
Even though glucose is the main precursor of acetyl-CoA used for DNL, fructose is an extremely lipogenic substrate [174]. It has a selective hepatic metabolism bypassing the checkpoint of phosphofructokinase-1 and supplying acetyl-Coa by entering in glycolysis through phosphorylation mediated by hepatic fructokinase. Moreover, it provides glycerol 3-phosphate for TG synthesis and seems to increase free ROS production through nonenzymatic fructosylation [172]. In contrast to glucose, fructose does not stimulate insulin secretion and chronic exposure facilitates insulin resistance [175,176]. Moreover, chronic intake of fructose has been demonstrated to alter the “microbiota fingerprint” and damage gut tight junctions; consequently, it increases bacterial translocation, favoring systemic inflammation and NASH [177,178]. Finally, fructose consumption seems to stimulate appetite by increasing the levels of ghrelin and by acting on the central nervous system, specifically on the endocannabinoid signaling pathway [178]. For all these reasons, European guidelines recommend against the consumption of fructose-containing beverages and foods [1].
4.4. Overweight and Obesity
As mentioned above, obesity is strictly related to NAFLD. Adipose tissue is a very active endocrine organ that produces hormones and cytokines known as adipokines or adipocytokines. It mediates endocrine, inflammatory and immune interactions, protecting or favoring insulin resistance and liver steatosis [179].
Adiponectin is the major adipose-specific adipokine and it has powerful anti-inflammatory and insulin sensitizer effects. Several studies demonstrated an inverse correlation between adiponectin levels and hepatic steatosis, TG and LDL levels [86,180,181,182]. Leptin has protective effects on the liver since it stimulates beta-oxidation and suppresses lipogenesis, besides favoring gluconeogenesis [183]. One of the most used models of NAFLD is the leptin-deficient ob/ob mouse, which is a model of hyperphagia and severe obesity with insulin resistance. Another widely studied adipokine is resistin, which is a hormone involved in glucose and lipidic homeostasis, contributing to the development of NAFLD, insulin resistance and inflammation [120,184,185]. Apart from adipokines, adipose tissue is also responsible for the production of pro-inflammatory cytokines such as tumor necrosis factor-alpha (TNF-α), which has been demonstrated to be elevated in NASH compared to simple steatosis, and IL-6, that may favor HCC development by inhibiting apoptosis and activating pro-oncogenic patterns [86,186]. Adiposity also enhances the effect of genetic variants and possibly triggers the development of NAFLD [121].
4.5. Gut Microbiota
In recent years, attention has been focused on the gut microbiota (GM). It seems that a leaky mucosal barrier, especially in the presence of bacterial overgrowth, allows bacterial translocation, implicating the presence in the blood of microbial products such as lipopolysaccharide (LPS). These substances, specifically pathogen-associated molecular patterns (PAMPs), interact with receptors lying not only on inflammatory cells but also on other cell types such as hepatic stellate cells (HSC) and endothelial cells [187,188]. The liver is one of the most exposed organs to bacterial translocation because it primarily receives blood from the portal vein. One of the most studied pathways is the one activated by the Toll-like receptor 4 (TLR4), which leads to NF-κB activation and release of pro-inflammatory cytokines such as IL-1β, TNF-α, IL-6, or type I interferon [189]. Moreover, TLR can also recognize damage-associated molecular patterns (DAMPs) released by damaged cells [190], and it seems to mediate FA-induced inflammation [191]. Therefore, bacterial translocation promotes the establishment of a pro-inflammatory milieu and thus, in the presence of NAFLD, promotes NASH.
4.6. Iron Deposits
Iron deposits seem to play a role in NAFLD progression towards inflammation and fibrosis, while their role in steatosis development is still debated. Indeed, the IIRON2 study has recently produced new evidence regarding the relationship between hepatic iron deposits and insulin sensitivity, demonstrating that higher iron concentrations are associated with higher serum adiponectin and superior insulin sensitivity [192]. On the other hand, based on the assumption that oxidative stress is one of the key physiopathological mechanisms underlying NASH, and that iron is a highly reactive element that in excessive quantities leads to ROS formation through the Fenton reaction, it is clear how iron deposits may favor hepatic lipid peroxidation and thus membrane and DNA damage with hepatic cell apoptosis and a direct cytotoxic effect [193,194,195]. Accordingly, Maliken et al. demonstrated that when iron deposits are present in liver biopsies of NAFLD patients, higher levels of oxidative stress can be observed [196]. The authors hypothesized that an excessive oxidative burden may induce apoptosis or necrosis in the hepatic cells of these patients. Moreover, iron accumulation in liver reticuloendothelial system cells has been shown to be associated with NAFLD advanced histological features such as fibrosis, portal inflammation, cellular ballooning and defined NASH [197]; these data have also been confirmed in animal models [198]. In addition, the role of iron overload in HCC development is currently under evaluation in NAFLD, apart from the well-established role in hemochromatosis patients [118]. Moreover, further studies are warranted to understand the real prognostic value of iron deposits at liver biopsy. Interestingly, hyperferritinemia, which probably identifies NAFLD patients with major hepatic iron deposition, has also been demonstrated to be an independent predictor, not only of liver steatosis, but also of fibrosis [199,200,201]. However, it should be mentioned that clinical trials examining the potential therapeutic role of phlebotomy in NAFLD have shown contrasting results regarding any benefits in terms of reduction of liver damage [202,203].
4.7. Bile Acids
There is also growing interest in bile acid (BA) metabolic effects, apart from the well-known digestive ones. In the last few decades, BA receptors such as farnesoid X receptor (FXR) and Takeda G-protein-coupled receptor 5 (TGR5) have been discovered [204]. As recently described in an interesting review by Arab et al. [205], these receptors seem to play important roles in glucose metabolism, by favoring insulin sensitivity, glycogen synthesis and repressing gluconeogenesis. They also play a role in lipid metabolism, by lowering LDL-cholesterol and TG levels, and mediate anti-inflammatory effects as well as acting on Kupffer cells [206]. Bile acids are physiologically metabolized by the GM in the distal small intestine and colon. Thus, there is an interesting interplay between them. On the other hand, BA can modulate GM by influencing the energy substrate and antimicrobial response [207,208]. For all these reasons, bile acid signaling may play a role in NAFLD development and progression. Novel drugs targeting BA receptors are currently under evaluation [209].
4.8. Circadian Clock
Many metabolic pathways typically exhibit a circadian rhythm, principally driven by sleeping/waking and fasting/feeding cycles. Bile acid synthesis is influenced by these mechanisms too, as are the immune system and inflammatory responses [210]. All these mechanisms underlie NAFLD; it is therefore legitimate to suppose a role of the circadian clock in this disease, with the central nervous system coordinating all of these factors [211,212]. Kettner et al. recently demonstrated in animal models that chronic jet lag is sufficient to induce liver steatosis and successively HCC, probably through neuroendocrine dysfunction and pro-inflammatory effects that ultimately lead to gene deregulation [213]. Moreover, other experimental models confirmed that gene mutations involved in the circadian clock system regulation predispose to NAFLD [213,214]. However, further studies are needed to better characterize the clinical and therapeutic implications of circadian rhythm regulation.
5. Therapy
Today, there is no licensed pharmacotherapy for NAFLD, so the treatment is fundamentally based on lifestyle intervention and every specific drug would be off label [1]. Numerous pharmacological strategies have been tested in clinical studies for NAFLD therapy and, in accordance with the above described NAFLD physiopathology, different classes of drugs can be identified: antidiabetic drugs, antioxidants, prebiotics, drugs acting on the bile acid system and lipid-lowering therapies. It should be kept in mind that, in order to prevent cardiovascular complications in these patients, it is mandatory to treat the associated cardiovascular risk factors such as dyslipidemia, arterial hypertension and diabetes [1,215].
5.1. Lifestyle Intervention
The cornerstone of NAFLD treatment is lifestyle intervention [16]. Physical activity should be implemented [216,217], aiming at a minimum of 150–200 min/week of moderate intensity aerobic physical activity; a dose-effect relationship has been demonstrated, pointing out that high intensity exercise should be preferred to moderate exercise whenever possible [1]. However, the most effective strategy to reduce liver fat is dietary restriction, thus the European guidelines recommend a 7–10% weight loss (“weight normative” approach) [1,218]. In fact, as demonstrated in a recent prospective real-world study, the degree of weight loss correlates with histological improvement of all NASH-related parameters, with moderate evidence if the weight loss reaches 5% and even greater results if it exceeds 10% (90% resolution of NASH in the latter case) [219]. Similar results have been shown in randomized prospective trials comparing hypocaloric diet plus vitamin E with or without orlistat; this trial showed that a greater weight loss was associated with an increased insulin sensitivity, higher adiponectin levels and reduced liver steatosis, inflammation and ballooning, independently from the adopted pharmacological intervention [220]. A hypocaloric (120–1600 Kcal/day) low-fat or low-carbohydrate diet should be encouraged [221]. In fact, it seems that as long as weight loss is achieved, the macronutrient composition of the diet is of little importance [221,222]. With this aim, bariatric surgery is giving promising results in patients with morbid obesity, leading to a reduction of biochemical markers of NAFLD and amelioration of steatosis, hepatocyte ballooning, lobular inflammation and fibrosis [223].
On the other hand, independent of weight loss, recent evidence has highlighted the importance of having a healthy diet (“weight inclusive” approach) [224,225]. In fact, Poperzi et al. demonstrated that the isocaloric Mediterranean diet reduces liver steatosis to the same extent as a low-fat diet, even though the first one is probably more effective on cardiometabolic risk factors [226]. Particularly, saturated fatty acids should be kept below the threshold of 10% of the total fat amount and replaced with polyunsaturated fatty acids [225,227,228]. Animal-derived proteins should be reduced and the consumption of olive oil, legumes, fruits, nuts, vegetables, grains and fish should be intensified. All these indications are fundamental also in accordance with the European Society of Cardiology for cardiovascular prevention, especially considering that NAFLD patients are considered at increased cardiovascular risk [225,227].
Expanding the issue of dietary considerations, it is mandatory to reduce fructose intake (e.g., soft drinks), while there are no liver-related limitations on coffee, which has been found to be beneficial for liver steatosis [1,229]. The effect of consuming alcoholic beverages is still debated, since recent evidence suggests that even a modest consumption may enhance liver damage [2,230,231].
5.2. Antidiabetic Drugs
Since NAFLD is often associated with insulin resistance, even though in a complex and bidirectional relationship, drugs increasing insulin sensitivity have been proposed to treat liver steatosis and prevent diabetes in these patients. Among them, the thiazolidinediones, acting on the nuclear transcription factor peroxisome proliferator-activated receptor gamma (PPAR)-γ and thus true insulin sensitizers drugs, have demonstrated the best efficacy, improving liver histology in NASH independently from the presence of diabetes [232,233]. For all these reasons, European guidelines recommend with a B2 GRADE the use of pioglitazone in diabetic and in non-diabetic (off-label) patients [1]. The drawbacks of thiazolidinediones are weight gain, bone fractures in women, bladder cancer and congestive heart failure [234].
While the cornerstone of antidiabetic therapy in type 2 diabetes is metformin, an AMP-activated protein kinase activator, its role in reducing steatosis and inflammation in NAFLD is still debated [1]. Bugianesi et al., in a Randomized Controlled Trial (RCT) with histological outcomes, demonstrated that compared to a dietary intervention or vitamin E, metformin significantly reduced aminotransferase levels and improved liver histology in nondiabetic NAFLD patients [235]. These findings were not confirmed by subsequent RCTs [236,237]. On the other hand, metformin appears to reduce HCC risk in a dose-response pattern [41,238], probably influencing the LKB1/AMPK/mTOR axis and reducing ROS formation by acting on the mitochondrial respiratory chain [239]. In conclusion, the evidence for metformin use in NAFLD patients is still inconsistent.
Glucagon-like peptide-1 (GLP1) receptor agonists are promising therapeutic agents in NAFLD. In fact, in the LEAN (Liraglutide efficacy and action in NASH) RCT phase 2 study in overweight NASH patients, liraglutide induced NASH resolution in 39% of individuals compared to 9% of the placebo group; moreover, it significantly halted fibrosis progression [240]. The adverse events were mainly diarrhea, constipation and loss of appetite. Interestingly, the authors hypothesized that the weight reduction and the better glycemic control of the liraglutide group could also reduce cardiovascular risk in overweight patients with NASH, as already demonstrated in diabetic patients at high cardiovascular risk [241]. However, it should be noted that the hepatoprotective effect of liraglutide is probably not entirely justified by an improvement of the metabolic phenotype, but it is also due to a direct hepatic effect [242]. Moreover, other GLP1 receptor agonists have been tested in clinical studies with promising results [243]. On the contrary, sitagliptin, an oral dipeptidyl peptidase-4 (DPP4) inhibitor, in a recent RCT did not significantly reduce liver steatosis in prediabetic or diabetic patients with NAFLD [244].
Finally, the sodium/glucose cotransporter 2 (SGLT2) inhibitors are raising growing interest for the treatment of NAFLD, also considering their known beneficial effect on cardiovascular prevention in people with diabetes [245]. In the E-LIFT (Effect of empagliflozin on liver fat in patients with type 2 diabetes and nonalcoholic fatty liver disease: A randomized controlled trial) Trial, empagliflozin reduced liver fat evaluated by MRI in diabetic NAFLD patients and reduced liver transaminase levels [246]. These findings did not seem to be related to a better glycemic control or a greater weight reduction in the treatment group. Similar results on liver steatosis were also reported by ipragliflozin and luseogliflozin [247,248]; dapagliflozin, in the EFFECT-II (Effects of Omega-3 Carboxylic Acids and Dapagliflozin on Liver Fat Content in Diabetic Patients) trial reduced hepatocyte injury biomarkers and liver fat content compared to placebo when used in association with omega 3 in diabetic NAFLD patients [249]. Several other studies examined the effects of SGLT2 inhibitors on NAFLD but, to the best of the authors’ knowledge, no histological data on the effect of gliflozin on NAFLD are available yet [250]. The negative energy balance derived from glucose urinary excretion and from the increased glucagon/insulin ratio that promotes substrate utilization shift from carbohydrates to lipids may explain the beneficial role of SGLT2 inhibitors in NAFLD [249,251]; the weight loss and the increased insulin sensitivity may contribute to the SGLT2 inhibitors effect though, as mentioned above, this is still unclear [248,250]. Finally, a direct anti-inflammatory effect of gliflozins has been proposed [252].
It should be mentioned that not all antidiabetic drugs are efficacious against liver steatosis [253]; for example, insulin and insulin secretagogues seem to exacerbate steatosis and increase the risk of HCC [41].
5.3. Antioxidants
Since oxidative stress represents one of the main etiopathogenic factors causing NASH, many antioxidant agents have been tested. Among them, vitamin E, in the PIVENS (Pioglitazone versus Vitamin E versus Placebo for the Treatment of Nondiabetic Patients with Nonalcoholic Steatohepatitis) trial, significantly reduced serum transaminases and improved steatosis, inflammation and ballooning in NAFLD compared to placebo [233,254]; these results were also confirmed by a recent meta-analysis on the effect of vitamin E [255]. Despite the concerns for long-term safety, because of the possible higher risk of mortality, hemorrhagic stroke and prostate cancer, the European guidelines recommend the use of vitamin E in NAFLD (B2, GRADE system) [1]. Notably, the dietary vitamin C intake inversely correlates with the incidence of NAFLD, suggesting that dietary supplementation may have a beneficial role [256]. Analogously, zinc and selenium supplementation ameliorated NAFLD histology in animal models [257].
Promising results have been given by omega 3 polyunsaturated fatty acids (PUFAs); they probably act on SREBP-1c, ChREBP and PPARs, reducing lipogenesis and increasing beta-oxidation [258,259]. Furthermore, omega 3 PUFAs exert anti-inflammatory effects through the interaction with active metabolites involved in inflammation such as TNF-alpha [260,261]; finally, they may increase insulin sensitivity [262]. Unfortunately, several differences in the design of the different studies makes it difficult to compare the PUFA efficacy on NAFLD treatment [259,260].
Pentoxifylline, a TNF-alpha inhibitor, has improved histology in NASH patients, independently from insulin sensitivity measures [263]. Although antioxidant and anti-inflammatory effects have been hypothesized, the real mechanisms underlying these effects remain unclear. The advantages of pentoxifylline are its affordability, its good tolerability and its long-term safety.
5.4. Drugs acting on The Gut Microbiota
As mentioned above, the gut microbiota, through bacterial translocations and PAMPs, nurtures inflammation. Prebiotics are nondigestible substances able to promote the growth of beneficial microorganisms in the gut, while probiotics are live microorganisms that, when administered in adequate amounts, confer a health benefit to the host [264]. A recent metanalysis demonstrated that prebiotics and probiotics reduce BMI and liver enzymes, also ameliorating the lipid profile but with no effect on inflammation [265]. A RCT recently proved that probiotics reduce liver fat content, serum aminotransferase levels, TNF-alpha and interleukin 6 levels [266]. A possible explanation of the beneficial effects of these therapies is the increased production of short-chain fatty acids, the delayed macronutrient absorption, the ameliorated barrier function, a modulation of the immune system and an effect on bile acid metabolism [265]. However, further studies are needed to better define the effects and the dosage needed for prebiotics and probiotics.
5.5. Drugs Acting on Bile Acids System
Obeticholic acid, a potent activator of the above-mentioned FXR already registered for the treatment of primary biliary cholangitis, has been tested for use in NASH patients in the FLINT (Farnesoid X Receptor Ligand Obeticholic Acid in NASH Treatment) trial. This study has been stopped for superiority, since the drug significantly improved necro-inflammation, reducing lipogenesis, increasing VLDL clearance but also through direct anti-inflammatory effects [267,268]. In a phase 2 RCT in NAFLD diabetic patients, obeticholic acid not only reduced markers of liver inflammation and fibrosis, but it also reduced insulin resistance [269]. Two phase 3 studies evaluating the role of obeticholic acid in non-cirrhotic NASH with liver fibrosis (REGENERATE ClinicalTrials.gov: NCT02548351) and in compensated cirrhosis due to NASH (REVERSE ClinicalTrials.gov: NCT03439254) are now ongoing. The adverse events of this drug are pruritus and increased LDL cholesterol. On the contrary, ursodeoxycholic acid (UDCA), a natural bile acid, did not prove to be superior to placebo in reducing steatosis, inflammation or fibrosis [270], even though it reduced serum transaminase levels and improved liver histology when used in combination with vitamin E [271].
5.6. Lipid-Lowering Therapies
As clearly demonstrated by the post-hoc analysis of the GREACE (GREek Atorvastatin and Coronary-heart-disease Evaluation) study [272] and the IDEAL (Incremental Decrease in Events through Aggressive Lipid Lowering) study [273], the use of statins is safe in patients with NAFLD and they also reduce the levels of serum transaminases. Moreover, statins ameliorate liver histology and, most importantly, reduce cardiovascular morbidity and mortality in NAFLD patients [272,273,274,275]. As demonstrated in a large cross-sectional cohort of patients with suspected NASH, statin use confers a dose-dependent protection towards all NAFLD spectrum, including steatosis, NASH and fibrosis [276]. The authors suppose an anti-inflammatory and possibly anti-fibrotic effect, besides the known inhibitory effect on lipid synthesis. Finally, a reduced risk of HCC has been demonstrated [277]. Despite all these beneficial effects, unfortunately, statins are still under-prescribed in NAFLD patients, principally because of an unjustified tendency to discourage their use in cases of elevated liver enzymes [278].
Another lipid-lowering agent is ezetimibe, a Niemann-Pick C1 like 1 (NPC1L1) protein inhibitor, which has been proposed to prevent and treat NAFLD [279]. The hypothesis is that a lower cholesterol inflow to the liver reduces inflammation, insulin resistance and apoptosis in hepatocytes [280]. However, according to a recent metanalysis, despite some studies showing a benefit for serum transaminase, liver steatosis and hepatocyte ballooning, the evidence for ezetimibe prescription in NAFLD is still scarce [280].
5.7. Novel Classes of Drugs
Novel classes of drugs are currently under clinical trials [281]. Selonsertib (GS-4997), a selective inhibitor of apoptosis signal-regulating kinase 1 (ASK1) with anti-inflammatory and anti-fibrotic properties, demonstrated a potential role in reducing fibrosis in NASH and stage 2–3 fibrosis [282]; it is now being tested in stage 3 fibrosis and compensated cirrhotic NASH patients (STELLAR3 study ClinicalTrials.gov: NCT03053050 and STELLAR4 study ClinicalTrials.gov: NCT03053063). Analogously, cenicriviroc, an antagonist of the C-C motif chemokine receptor 2/5 (CCR2 and CCR5) that plays a role in macrophage recruitment in the liver, has been tested in a randomized phase 2b study, showing anti-inflammatory and anti-fibrotic effects in NASH patients with fibrosis [283,284]; it is now being tested in a phase 3 clinical trial (AURORA study ClinicalTrials.gov: NCT03028740). Elafibranor is a dual agonist of PPARα/δ that, in a phase 2 RCT, resolved NASH and ameliorated steatosis, ballooning, lobular inflammation and fibrosis in patients with a NAFLD fibrosis score ≥ 4 [285]. Moreover, elafibranor improved serum liver enzymes, lipid profile, markers of inflammation and, in diabetic subjects, ameliorated insulin sensitivity, demonstrating a “broad spectrum activity” rather than a simple hepatic effect [286]. The exact mechanism of action of this drug is still unclear, but PPARα and PPARδ are transcription factors involved not only in glucose and fat metabolism, but also in immune response, inflammation, apoptosis and cell proliferation [286]. A multicenter phase 3 RCT study to evaluate the efficacy and safety of elafibranor in NASH without cirrhosis is ongoing (RESOLVE-IT ClinicalTrials.gov: NCT02704403). Aramchol is a fatty acid–bile acid conjugate that inhibits hepatic Stearoyl-CoA desaturase and, in a phase 2a study, reduced liver steatosis in a dose-dependent manner [287]. In the next phase 2b study, it significantly reduced liver fat, obtained NASH resolution without worsening of fibrosis, reduced serum transaminases and improved glycemic control compared to placebo in overweight or obese NASH patients with prediabetes or diabetes [288]. Emricasan, an oral pan-caspase inhibitor modulating apoptosis, in a recent RCT significantly decreased serum transaminases and caspase activity in patients with NAFLD and elevated serum aminotransferase [289]. It is noteworthy that an antifibrotic agent, Simtuzumab, which is an anti-lysyl oxidase-like monoclonal antibody, failed to reduce fibrosis in NASH patients with advanced fibrosis in a phase 2 RCT [290]. Finally, hepatokines are currently under evaluation as a potential target for NAFLD therapy and diabetes prevention [41,291].
6. Conclusions and Future Perspectives
NAFLD is a well-distinguished clinical entity affecting people worldwide. Its pathogenesis is complex and multifactorial, mainly involving genetic, environmental and metabolic factors. New concepts are constantly appearing in the literature, promising new diagnostic and therapeutic tools. Further studies are needed to better characterize not only NAFLD development but overall NAFLD progression, in order to better identify NAFLD patients at higher risk of metabolic, cardiovascular and neoplastic complications.
Acknowledgments
We wish to thank the Scientific Bureau of the University of Catania for language support.
Abbreviations
| NAFLD | Nonalcoholic Fatty Liver Disease |
| NASH | Nonalcoholic Steatohepatitis |
| CT | Computed Tomography |
| MRS | Magnetic Resonance Spectroscopy |
| MRI | Magnetic Resonance Imaging |
| GPT | Glutamic Pyruvic Transaminase |
| HCV | Hepatitis C Virus |
| OLT | Orthotopic Liver Transplantation |
| AASLD | American Association for the Study of Liver Disease |
| TE | Transient Elastography |
| BMI | Body Mass Index |
| MONW | Metabolically Obese but Normal Weight |
| TG | Triglycerides |
| LDL | Low Density Lipoprotein |
| sdLDL | Small dense Low Density Lipoprotein |
| HDL | High Density Lipoprotein |
| VLDL | Very Low Density Lipoprotein |
| HCC | Hepatocarcinoma |
| NAFL | Nonalcoholic Fatty Liver |
| FA | Fatty Acid |
| NEFA | Non-Esterified Fatty Acids |
| DNL | De Novo Lipogenesis |
| CPT1 | Carnitine-O-palmitoyltransferase 1 |
| ROS | Radical Oxygen Species |
| RE | Endoplasmic Reticulum |
| FATP5 | Fatty Acid Transport Protein |
| PKCε | Protein Kinase C-ε |
| SREBP1c | Sterol Regulatory Element Binding Protein 1c |
| LXR | Liver X Receptor |
| RXR | Retinoid X Receptor |
| LIRKO | Insulin Receptor Knockout |
| ChREBP | Carbohydrate Response Element Binding Protein |
| GM | Gut Microbiota |
| LPS | Lipopolysaccharide |
| PAMPs | Pathogen-Associated Molecular Patterns |
| HSC | Hepatic Stellate Cells |
| TLR4 | Toll-like Receptor 4 |
| DAMPs | Damage-Associated Molecular Patterns |
| PNPLA3 | Palatin-like Phospholipase Domain Containing 3 |
| iPLA2-ε | Calcium-Independent Phospholipase A2 Epsilon |
| TM6SF2 | Transmembrane 6 Superfamily Member 2 |
| GCKR | Glucokinase Regulator |
| CETP | Cholesteryl Ester Transfer Protein |
| SREBP-1c | Sterol Regulatory Element-Binding Protein 1c |
| MBOAT7 | Membrane Bound O-Acyltransferase Domain-Containing 7 |
| MTTP | Microsomal Triglyceride Transfer Protein |
| ApoB | Apolipoprotein B |
| SOD2 | Superoxide Dismutase 2 |
| GST | Glutathione S-Transferase |
| TNF-α | Tumor Necrosis Factor-alpha |
| PPARA | Peroxisome Proliferator-Activated Receptor α |
| APOC3 | APOLIPOPROTEIN C-III |
| IL6 | Interleukin-6 |
| BA | Bile acid |
| FXR | Farnesoid X Receptor |
| TGR5 | Takeda G-Protein-Coupled Receptor 5 |
| GLP1 | Glucagon-Like Peptide-1 |
| RCT | Randomized Controlled Trial |
Author Contributions
Conceptualization, S.M.; data curation, S.M.; writing—original draft preparation, S.M.; writing—review and editing, A.D.P., R.S., F.U., S.P., F.P.; supervision, A.M.R.
Funding
This research received no external funding.
Conflicts of Interest
The authors declare no conflict of interest.
References
- 1.European Association for the Study of the Liver (EASL) European Association for the Study of Diabetes (EASD) European Association for the Study of Obesity (EASO) EASL–EASD–EASO Clinical Practice Guidelines for the management of non-alcoholic fatty liver disease. J. Hepatol. 2016;64:1388–1402. doi: 10.1016/j.jhep.2015.11.004. [DOI] [PubMed] [Google Scholar]
- 2.Chang Y., Cho Y.K., Kim Y., Sung E., Ahn J., Jung H.-S.S., Yun K.E., Shin H., Ryu S. Nonheavy Drinking and Worsening of Noninvasive Fibrosis Markers in Nonalcoholic Fatty Liver Disease: A Cohort Study. Hepatology. 2019;69:64–75. doi: 10.1002/hep.30170. [DOI] [PubMed] [Google Scholar]
- 3.Ballestri S., Nascimbeni F., Baldelli E., Marrazzo A., Romagnoli D., Targher G., Lonardo A. Ultrasonographic fatty liver indicator detects mild steatosis and correlates with metabolic/histological parameters in various liver diseases. Metabolism. 2017;72:57–65. doi: 10.1016/j.metabol.2017.04.003. [DOI] [PubMed] [Google Scholar]
- 4.Castera L., Friedrich-Rust M., Loomba R. Noninvasive Assessment of Liver Disease in Patients With Nonalcoholic Fatty Liver Disease. Gastroenterology. 2019;156:1264–1281.e4. doi: 10.1053/j.gastro.2018.12.036. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Torres D.M., Harrison S.A. Diagnosis and Therapy of Nonalcoholic Steatohepatitis. Gastroenterology. 2008;134:1682–1698. doi: 10.1053/j.gastro.2008.02.077. [DOI] [PubMed] [Google Scholar]
- 6.Obika M., Noguchi H. Diagnosis and evaluation of nonalcoholic fatty liver disease. Exp. Diabetes Res. 2012;2012:145754. doi: 10.1155/2012/145754. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Park S.H., Kim P.N., Kim K.W., Lee S.W., Yoon S.E., Park S.W., Ha H.K., Lee M.-G., Hwang S., Lee S.-G., et al. Macrovesicular Hepatic Steatosis in Living Liver Donors: Use of CT for Quantitative and Qualitative Assessment. Radiology. 2006;239:105–112. doi: 10.1148/radiol.2391050361. [DOI] [PubMed] [Google Scholar]
- 8.Charlton M., Sanyal A.J., Cusi K., Lavine J.E., Brunt E.M., Harrison S.A., Younossi Z., Rinella M., Chalasani N., Younossi Z., et al. The diagnosis and management of nonalcoholic fatty liver disease: Practice guidance from the American Association for the Study of Liver Diseases. Hepatology. 2017;67:328–357. doi: 10.1002/hep.29367. [DOI] [PubMed] [Google Scholar]
- 9.Reeder S.B., Cruite I., Hamilton G., Sirlin C.B. Quantitative assessment of liver fat with magnetic resonance imaging and spectroscopy. J. Magn. Reson. Imaging. 2011;34:4. doi: 10.1002/jmri.22775. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Idilman I.S., Keskin O., Celik A., Savas B., Halil Elhan A., Idilman R., Karcaaltincaba M. A comparison of liver fat content as determined by magnetic resonance imaging-proton density fat fraction and MRS versus liver histology in non-alcoholic fatty liver disease. Acta Radiol. 2016;57:271–278. doi: 10.1177/0284185115580488. [DOI] [PubMed] [Google Scholar]
- 11.Browning J.D., Szczepaniak L.S., Dobbins R., Nuremberg P., Horton J.D., Cohen J.C., Grundy S.M., Hobbs H.H. Prevalence of hepatic steatosis in an urban population in the United States: Impact of ethnicity. Hepatology. 2004;40:1387–1395. doi: 10.1002/hep.20466. [DOI] [PubMed] [Google Scholar]
- 12.Bedogni G., Miglioli L., Masutti F., Tiribelli C., Marchesini G., Bellentani S. Prevalence of and risk factors for nonalcoholic fatty liver disease: The Dionysos nutrition and liver study. Hepatology. 2005;42:44–52. doi: 10.1002/hep.20734. [DOI] [PubMed] [Google Scholar]
- 13.Bedogni G., Bellentani S., Miglioli L., Masutti F., Passalacqua M., Castiglione A., Tiribelli C. The Fatty Liver Index: A simple and accurate predictor of hepatic steatosis in the general population. BMC Gastroenterol. 2006;6:33. doi: 10.1186/1471-230X-6-33. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Kotronen A., Peltonen M., Hakkarainen A., Sevastianova K., Bergholm R., Johansson L.M., Lundbom N., Rissanen A., Ridderstråle M., Groop L., et al. Prediction of Non-Alcoholic Fatty Liver Disease and Liver Fat Using Metabolic and Genetic Factors. Gastroenterology. 2009;137:865–872. doi: 10.1053/j.gastro.2009.06.005. [DOI] [PubMed] [Google Scholar]
- 15.Poynard T., Lassailly G., Diaz E., Clement K., Caïazzo R., Tordjman J., Munteanu M., Perazzo H., Demol B., Callafe R., et al. Performance of Biomarkers FibroTest, ActiTest, SteatoTest, and NashTest in Patients with Severe Obesity: Meta Analysis of Individual Patient Data. PLoS ONE. 2012;7:e30325. doi: 10.1371/journal.pone.0030325. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Lonardo A., Nascimbeni F., Targher G., Bernardi M., Bonino F., Bugianesi E., Casini A., Gastaldelli A., Marchesini G., Marra F., et al. AISF position paper on nonalcoholic fatty liver disease (NAFLD): Updates and future directions. Dig. Liver Dis. 2017;49:471–483. doi: 10.1016/j.dld.2017.01.147. [DOI] [PubMed] [Google Scholar]
- 17.Angulo P., Hui J.M., Marchesini G., Bugianesi E., George J., Farrell G.C., Enders F., Saksena S., Burt A.D., Bida J.P., et al. The NAFLD fibrosis score: A noninvasive system that identifies liver fibrosis in patients with NAFLD. Hepatology. 2007;45:846–854. doi: 10.1002/hep.21496. [DOI] [PubMed] [Google Scholar]
- 18.Shah A.G., Lydecker A., Murray K., Tetri B.N., Contos M.J., Sanyal A.J., Nash Clinical Research Network Comparison of Noninvasive Markers of Fibrosis in Patients With Nonalcoholic Fatty Liver Disease. Clin. Gastroenterol. Hepatol. 2009;7:1104–1112. doi: 10.1016/j.cgh.2009.05.033. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Petta S., Vanni E., Bugianesi E., Di Marco V., Cammà C., Cabibi D., Mezzabotta L., Craxì A. The combination of liver stiffness measurement and NAFLD fibrosis score improves the noninvasive diagnostic accuracy for severe liver fibrosis in patients with nonalcoholic fatty liver disease. Liver Int. 2015;35:1566–1573. doi: 10.1111/liv.12584. [DOI] [PubMed] [Google Scholar]
- 20.Petta S., Wong V.W.-S., Cammà C., Hiriart J.-B., Wong G.L.-H., Vergniol J., Chan A.W.-H., Di Marco V., Merrouche W., Chan H.L.-Y., et al. Serial combination of non-invasive tools improves the diagnostic accuracy of severe liver fibrosis in patients with NAFLD. Aliment. Pharmacol. Ther. 2017;46:617–627. doi: 10.1111/apt.14219. [DOI] [PubMed] [Google Scholar]
- 21.Dongiovanni P., Meroni M., Longo M., Fargion S., Fracanzani A.L. miRNA Signature in NAFLD: A Turning Point for a Non-Invasive Diagnosis. Int. J. Mol. Sci. 2018;19:3966. doi: 10.3390/ijms19123966. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 22.Rasineni K., Casey C.A. Molecular mechanism of alcoholic fatty liver. Indian J. Pharmacol. 2012;44:299–303. doi: 10.4103/0253-7613.96297. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.Modaresi Esfeh J., Ansari-Gilani K. Steatosis and hepatitis C. Gastroenterol. Rep. 2016;4:24–29. doi: 10.1093/gastro/gov040. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.Amacher D., Chalasani N. Drug-Induced Hepatic Steatosis. Semin. Liver Dis. 2014;34:205–214. doi: 10.1055/s-0034-1375960. [DOI] [PubMed] [Google Scholar]
- 25.Whitfield A.J. Liver Dysfunction and Steatosis in Familial Hypobetalipoproteinemia. Clin. Chem. 2004;51:266–269. doi: 10.1373/clinchem.2004.037978. [DOI] [PubMed] [Google Scholar]
- 26.A-Kader H.H. Lysosomal acid lipase deficiency: A form of non-obese fatty liver disease (NOFLD) Expert Rev. Gastroenterol. Hepatol. 2017;11:911–924. doi: 10.1080/17474124.2017.1343144. [DOI] [PubMed] [Google Scholar]
- 27.Liggi M., Murgia D., Civolani A., Demelia E., Sorbello O., Demelia L. The relationship between copper and steatosis in Wilson’s disease. Clin. Res. Hepatol. Gastroenterol. 2013;37:36–40. doi: 10.1016/j.clinre.2012.03.038. [DOI] [PubMed] [Google Scholar]
- 28.Takahashi A., Arinaga-Hino T., Ohira H., Abe K., Torimura T., Zeniya M., Abe M., Yoshizawa K., Takaki A., Suzuki Y., et al. Non-alcoholic fatty liver disease in patients with autoimmune hepatitis. JGH Open. 2018;2:54–58. doi: 10.1002/jgh3.12046. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 29.Freeman H.J. Hepatic manifestations of celiac disease. Clin. Exp. Gastroenterol. 2010;3:33. doi: 10.2147/CEG.S7556. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 30.Marino L., Jornayvaz F.R. Endocrine causes of nonalcoholic fatty liver disease. World J. Gastroenterol. 2015;21:11053–11076. doi: 10.3748/wjg.v21.i39.11053. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 31.Ferrandino G., Kaspari R.R., Spadaro O., Reyna-Neyra A., Perry R.J., Cardone R., Kibbey R.G., Shulman G.I., Dixit V.D., Carrasco N. Pathogenesis of hypothyroidism-induced NAFLD is driven by intra- and extrahepatic mechanisms. Proc. Natl. Acad. Sci. 2017;114:E9172–E9180. doi: 10.1073/pnas.1707797114. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 32.Mantovani A., Nascimbeni F., Lonardo A., Zoppini G., Bonora E., Mantzoros C.S., Targher G. Association Between Primary Hypothyroidism and Nonalcoholic Fatty Liver Disease: A Systematic Review and Meta-Analysis. Thyroid. 2018;28:1270–1284. doi: 10.1089/thy.2018.0257. [DOI] [PubMed] [Google Scholar]
- 33.Petta S., Ciresi A., Bianco J., Geraci V., Boemi R., Galvano L., Magliozzo F., Merlino G., Craxì A., Giordano C. Insulin resistance and hyperandrogenism drive steatosis and fibrosis risk in young females with PCOS. PLoS ONE. 2017;12:e0186136. doi: 10.1371/journal.pone.0186136. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 34.Kneeman J.M., Misdraji J., Corey K.E. Secondary causes of nonalcoholic fatty liver disease. Therap. Adv. Gastroenterol. 2012;5:199–207. doi: 10.1177/1756283X11430859. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 35.Safar Zadeh E., Lungu A.O., Cochran E.K., Brown R.J., Ghany M.G., Heller T., Kleiner D.E., Gorden P. The liver diseases of lipodystrophy: The long-term effect of leptin treatment. J. Hepatol. 2013;59:131–137. doi: 10.1016/j.jhep.2013.02.007. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 36.Younossi Z.M., Stepanova M., Afendy M., Fang Y., Younossi Y., Mir H., Srishord M. Changes in the Prevalence of the Most Common Causes of Chronic Liver Diseases in the United States From 1988 to 2008. Clin. Gastroenterol. Hepatol. 2011;9:524–530. doi: 10.1016/j.cgh.2011.03.020. [DOI] [PubMed] [Google Scholar]
- 37.Younossi Z.M., Koenig A.B., Abdelatif D., Fazel Y., Henry L., Wymer M. Global epidemiology of nonalcoholic fatty liver disease—Meta-analytic assessment of prevalence, incidence, and outcomes. Hepatology. 2016;64:73–84. doi: 10.1002/hep.28431. [DOI] [PubMed] [Google Scholar]
- 38.Seto W.-K., Yuen M.-F. Nonalcoholic fatty liver disease in Asia: Emerging perspectives. J. Gastroenterol. 2017;52:164–174. doi: 10.1007/s00535-016-1264-3. [DOI] [PubMed] [Google Scholar]
- 39.Bellentani S., Tiribelli C., Saccoccio G., Sodde M., Fratti N., De Martin C., Cristianini G. Prevalence of chronic liver disease in the general population of northern Italy: The Dionysos Study. Hepatology. 1994;20:1442–1449. doi: 10.1002/hep.1840200611. [DOI] [PubMed] [Google Scholar]
- 40.Bedogni G., Bellentani S. Fatty liver: How frequent is it and why? Ann. Hepatol. 2004;3:63–65. [PubMed] [Google Scholar]
- 41.Lonardo A., Lugari S., Ballestri S., Nascimbeni F., Baldelli E., Maurantonio M. A round trip from nonalcoholic fatty liver disease to diabetes: Molecular targets to the rescue? Acta Diabetol. 2018:385–396. doi: 10.1007/s00592-018-1266-0. [DOI] [PubMed] [Google Scholar]
- 42.Estes C., Anstee Q.M., Arias-Loste M.T., Bantel H., Bellentani S., Caballeria J., Colombo M., Craxi A., Crespo J., Day C.P., et al. Modeling NAFLD disease burden in China, France, Germany, Italy, Japan, Spain, United Kingdom, and United States for the period 2016–2030. J. Hepatol. 2018;69:896–904. doi: 10.1016/j.jhep.2018.05.036. [DOI] [PubMed] [Google Scholar]
- 43.Charlton M.R., Burns J.M., Pedersen R.A., Watt K.D., Heimbach J.K., Dierkhising R.A. Frequency and Outcomes of Liver Transplantation for Nonalcoholic Steatohepatitis in the United States. Gastroenterology. 2011;141:1249–1253. doi: 10.1053/j.gastro.2011.06.061. [DOI] [PubMed] [Google Scholar]
- 44.Wong R.J., Cheung R., Ahmed A. Nonalcoholic steatohepatitis is the most rapidly growing indication for liver transplantation in patients with hepatocellular carcinoma in the U.S. Hepatology. 2014;59:2188–2195. doi: 10.1002/hep.26986. [DOI] [PubMed] [Google Scholar]
- 45.Adam R., Karam V., Delvart V., O’Grady J., Mirza D., Klempnauer J., Castaing D., Neuhaus P., Jamieson N., Salizzoni M., et al. Evolution of indications and results of liver transplantation in Europe. A report from the European Liver Transplant Registry (ELTR) J. Hepatol. 2012;57:675–688. doi: 10.1016/j.jhep.2012.04.015. [DOI] [PubMed] [Google Scholar]
- 46.Pais R., Barritt A.S., Calmus Y., Scatton O., Runge T., Lebray P., Poynard T., Ratziu V., Conti F., Conti F. NAFLD and liver transplantation: Current burden and expected challenges. J. Hepatol. 2016;65:1245–1257. doi: 10.1016/j.jhep.2016.07.033. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 47.Gitto S., Vukotic R., Vitale G., Pirillo M., Villa E., Andreone P. Non-alcoholic steatohepatitis and liver transplantation. Dig. Liver Dis. 2016;48:587–591. doi: 10.1016/j.dld.2016.02.014. [DOI] [PubMed] [Google Scholar]
- 48.Adam R., Karam V., Cailliez V., O Grady J.G., Mirza D., Cherqui D., Klempnauer J., Salizzoni M., Pratschke J., Jamieson N., et al. 2018 Annual Report of the European Liver Transplant Registry (ELTR)—50-year evolution of liver transplantation. Transpl. Int. 2018;31:1293–1317. doi: 10.1111/tri.13358. [DOI] [PubMed] [Google Scholar]
- 49.Dare A.J., Plank L.D., Phillips A.R.J., Gane E.J., Harrison B., Orr D., Jiang Y., Bartlett A.S.J.R. Additive effect of pretransplant obesity, diabetes, and cardiovascular risk factors on outcomes after liver transplantation. Liver Transplant. 2014;20:281–290. doi: 10.1002/lt.23818. [DOI] [PubMed] [Google Scholar]
- 50.Charlton M. Evolving aspects of liver transplantation for nonalcoholic steatohepatitis. Curr. Opin. Organ Transplant. 2013;18:251–258. doi: 10.1097/MOT.0b013e3283615d30. [DOI] [PubMed] [Google Scholar]
- 51.Zheng J., Wang W.L. Risk factors of metabolic syndrome after liver transplantation. Hepatobiliary Pancreat. Dis. Int. 2015;14:582–587. doi: 10.1016/S1499-3872(15)60037-6. [DOI] [PubMed] [Google Scholar]
- 52.Koehler E.M., Leebeek F.W.G., Stricker B.H., Schouten J.N.L., Janssen H.L.A., Hansen B.E., Darwish Murad S., Castera L., Taimr P., Plompen E.P.C., et al. Presence of diabetes mellitus and steatosis is associated with liver stiffness in a general population: The Rotterdam study. Hepatology. 2015;63:138–147. doi: 10.1002/hep.27981. [DOI] [PubMed] [Google Scholar]
- 53.Noureddin M., Yates K.P., Vaughn I.A., Neuschwander-Tetri B.A., Sanyal A.J., McCullough A., Merriman R., Hameed B., Doo E., Kleiner D.E., et al. Clinical and histological determinants of nonalcoholic steatohepatitis and advanced fibrosis in elderly patients. Hepatology. 2013;58:1644–1654. doi: 10.1002/hep.26465. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 54.Gagliano N., Arosio B., Grizzi F., Masson S., Tagliabue J., Dioguardi N., Vergani C., Annoni G. Reduced collagenolytic activity of matrix metalloproteinases and development of liver fibrosis in the aging rat. Mech. Ageing Dev. 2002;123:413–425. doi: 10.1016/S0047-6374(01)00398-0. [DOI] [PubMed] [Google Scholar]
- 55.Kim I.H., Kisseleva T., Brenner D.A. Aging and liver disease. Curr. Opin. Gastroenterol. 2015;31:184–191. doi: 10.1097/MOG.0000000000000176. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 56.Collins B.H., Holzknecht Z.E., Lynn K.A., Sempowski G.D., Smith C.C., Liu S., Parker W., Rockey D.C. Association of age-dependent liver injury and fibrosis with immune cell populations. Liver Int. 2013;33:1175–1186. doi: 10.1111/liv.12202. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 57.Mann J.P. Paediatric NAFLD: More than just small adults. Lancet Gastroenterol. Hepatol. 2018;3:222. doi: 10.1016/S2468-1253(18)30040-2. [DOI] [PubMed] [Google Scholar]
- 58.Yerian L., Lopez R., Alkhouri N., De Vito R., Nobili V., Feldstein A.E., Alisi A., Yerian L., Lopez R., Feldstein A.E., et al. Development and validation of a new histological score for pediatric non-alcoholic fatty liver disease. J. Hepatol. 2012;57:1312–1318. doi: 10.1016/j.jhep.2012.07.027. [DOI] [PubMed] [Google Scholar]
- 59.Feldstein A.E., Charatcharoenwitthaya P., Treeprasertsuk S., Benson J.T., Enders F.B., Angulo P. The natural history of non-alcoholic fatty liver disease in children: A follow-up study for up to 20 years. Gut. 2009;58:1538–1544. doi: 10.1136/gut.2008.171280. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 60.Hagström H., Stål P., Hultcrantz R., Hemmingsson T., Andreasson A., Hultcrantz R., Andreasson A., Stål P., Hagström H., Stål P., et al. Overweight in late adolescence predicts development of severe liver disease later in life: A 39years follow-up study. J. Hepatol. 2016;65:363–368. doi: 10.1016/j.jhep.2016.03.019. [DOI] [PubMed] [Google Scholar]
- 61.Kelsey M.M., Zeitler P.S. Insulin Resistance of Puberty. Curr. Diab. Rep. 2016;16:64. doi: 10.1007/s11892-016-0751-5. [DOI] [PubMed] [Google Scholar]
- 62.Temple J.L., Cordero P., Li J., Nguyen V., Oben J.A. A Guide to Non-Alcoholic Fatty Liver Disease in Childhood and Adolescence. Int. J. Mol. Sci. 2016;17:947. doi: 10.3390/ijms17060947. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 63.Soresi M., Noto D., Cefalù A.B., Martini S., Vigna G.B., Fonda M., Manzato E., Cattin L., Fellin R., Averna M.R., et al. Nonalcoholic fatty liver and metabolic syndrome in Italy: Results from a multicentric study of the Italian Arteriosclerosis society. Acta Diabetol. 2013;50:241–249. doi: 10.1007/s00592-012-0406-1. [DOI] [PubMed] [Google Scholar]
- 64.Katrina Loomis A., Kabadi S., Preiss D., Hyde C., Bonato V., Louis M.S., Desai J., Gill J.M.R., Welsh P., Waterworth D., et al. Body mass index and risk of nonalcoholic fatty liver disease: Two electronic health record prospective studies. J. Clin. Endocrinol. Metab. 2016;101:945–952. doi: 10.1210/jc.2015-3444. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 65.Tilg H., Moschen A.R., Roden M. NAFLD and diabetes mellitus. Nat. Rev. Gastroenterol. Hepatol. 2017;14:32–42. doi: 10.1038/nrgastro.2016.147. [DOI] [PubMed] [Google Scholar]
- 66.Calanna S., Scicali R., Di Pino A., Knop F.K., Piro S., Rabuazzo A.M., Purrello F. Lipid and liver abnormalities in haemoglobin A1c-defined prediabetes and type 2 diabetes. Nutr. Metab. Cardiovasc. Dis. 2014;24:670–676. doi: 10.1016/j.numecd.2014.01.013. [DOI] [PubMed] [Google Scholar]
- 67.Loomba R., Abraham M., Unalp A., Wilson L., Lavine J., Doo E., Bass N.M., Nonalcoholic Steatohepatitis Clinical Research Network Association between diabetes, family history of diabetes, and risk of nonalcoholic steatohepatitis and fibrosis. Hepatology. 2012;56:943–951. doi: 10.1002/hep.25772. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 68.Angulo P., Kleiner D.E., Dam-Larsen S., Adams L.A., Bjornsson E.S., Charatcharoenwitthaya P., Mills P.R., Keach J.C., Lafferty H.D., Stahler A., et al. Liver Fibrosis, but No Other Histologic Features, Is Associated With Long-term Outcomes of Patients With Nonalcoholic Fatty Liver Disease. Gastroenterology. 2015;149:389–397.e10. doi: 10.1053/j.gastro.2015.04.043. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 69.Kim D., Kim W.R. Nonobese Fatty Liver Disease. Clin. Gastroenterol. Hepatol. 2017;15:474–485. doi: 10.1016/j.cgh.2016.08.028. [DOI] [PubMed] [Google Scholar]
- 70.Ruderman N., Chisholm D., Pi-Sunyer X., Schneider S. The metabolically obese, normal-weight individual revisited. Diabetes. 1998;47:699–713. doi: 10.2337/diabetes.47.5.699. [DOI] [PubMed] [Google Scholar]
- 71.Sinn D.H., Gwak G.-Y., Park H.N., Kim J.E., Min Y.W., Kim K.M., Kim Y.J., Choi M.S., Lee J.H., Koh K.C., et al. Ultrasonographically Detected Non-Alcoholic Fatty Liver Disease Is an Independent Predictor for Identifying Patients With Insulin Resistance in Non-Obese, Non-Diabetic Middle-Aged Asian Adults. Am. J. Gastroenterol. 2012;107:561–567. doi: 10.1038/ajg.2011.400. [DOI] [PubMed] [Google Scholar]
- 72.Calanna S., Piro S., Di Pino A., Maria Zagami R., Urbano F., Purrello F., Maria Rabuazzo A. Beta and alpha cell function in metabolically healthy but obese subjects: Relationship with entero-insular axis. Obesity. 2013;21:320–325. doi: 10.1002/oby.20017. [DOI] [PubMed] [Google Scholar]
- 73.Kumar R., Mohan S. Non-alcoholic Fatty Liver Disease in Lean Subjects: Characteristics and Implications. J. Clin. Transl. Hepatol. 2017;5:216–223. doi: 10.14218/JCTH.2016.00068. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 74.Wei J.L., Leung J.C.-F., Loong T.C.-W., Wong G.L.-H., Yeung D.K.-W., Chan R.S.-M., Chan H.L.-Y., Chim A.M.-L., Woo J., Chu W.C.-W., et al. Prevalence and Severity of Nonalcoholic Fatty Liver Disease in Non-Obese Patients: A Population Study Using Proton-Magnetic Resonance Spectroscopy. Am. J. Gastroenterol. 2015;110:1306–1314. doi: 10.1038/ajg.2015.235. [DOI] [PubMed] [Google Scholar]
- 75.Enjoji M., Yasutake K., Kohjima M., Nakamuta M. Nutrition and Nonalcoholic Fatty Liver Disease: The Significance of Cholesterol. Int. J. Hepatol. 2012;2012:1–6. doi: 10.1155/2012/925807. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 76.Musso G., Gambino R., De Michieli F., Cassader M., Rizzetto M., Durazzo M., Fagà E., Silli B., Pagano G. Dietary habits and their relations to insulin resistance and postprandial lipemia in nonalcoholic steatohepatitis. Hepatology. 2003;37:909–916. doi: 10.1053/jhep.2003.50132. [DOI] [PubMed] [Google Scholar]
- 77.Assy N., Nasser G., Kamayse I., Nseir W., Beniashvili Z., Djibre A., Grosovski M. Soft drink consumption linked with fatty liver in the absence of traditional risk factors. Can. J. Gastroenterol. 2008;22:811–816. doi: 10.1155/2008/810961. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 78.Fracanzani A.L., Petta S., Lombardi R., Pisano G., Russello M., Consonni D., Di Marco V., Cammà C., Mensi L., Dongiovanni P., et al. Liver and Cardiovascular Damage in Patients With Lean Nonalcoholic Fatty Liver Disease, and Association With Visceral Obesity. Clin. Gastroenterol. Hepatol. 2017;15:1604–1611.e1. doi: 10.1016/j.cgh.2017.04.045. [DOI] [PubMed] [Google Scholar]
- 79.Zhang Q.-Q., Lu L.-G. Nonalcoholic Fatty Liver Disease: Dyslipidemia, Risk for Cardiovascular Complications, and Treatment Strategy. J. Clin. Transl. Hepatol. 2015;3:78–84. doi: 10.14218/JCTH.2014.00037. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 80.Kikkawa K., Nakajima K., Shimomura Y., Tokita Y., Machida T., Sumino H., Murakami M. Small dense LDL cholesterol measured by homogeneous assay in Japanese healthy controls, metabolic syndrome and diabetes patients with or without a fatty liver. Clin. Chim. Acta. 2015;438:70–79. doi: 10.1016/j.cca.2014.07.017. [DOI] [PubMed] [Google Scholar]
- 81.Imajo K., Hyogo H., Yoneda M., Honda Y., Kessoku T., Tomeno W., Ogawa Y., Taguri M., Mawatari H., Nozaki Y., et al. LDL-Migration Index (LDL-MI), an Indicator of Small Dense Low-Density Lipoprotein (sdLDL), Is Higher in Non-Alcoholic Steatohepatitis than in Non-Alcoholic Fatty Liver: A Multicenter Cross-Sectional Study. PLoS ONE. 2014;9:e115403. doi: 10.1371/journal.pone.0115403. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 82.Dias C.B., Moughan P.J., Wood L.G., Singh H., Garg M.L. Postprandial lipemia: Factoring in lipemic response for ranking foods for their healthiness. Lipids Health Dis. 2017;16:178. doi: 10.1186/s12944-017-0568-5. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 83.Musso G., Gambino R., Durazzo M., Biroli G., Carello M., Fagà E., Pacini G., De Michieli F., Rabbione L., Premoli A., et al. Adipokines in NASH: Postprandial lipid metabolism as a link between adiponectin and liver disease. Hepatology. 2005;42:1175–1183. doi: 10.1002/hep.20896. [DOI] [PubMed] [Google Scholar]
- 84.Katsiki N., Mikhailidis D.P., Mantzoros C.S. Non-alcoholic fatty liver disease and dyslipidemia: An update. Metabolism. 2016;65:1109–1123. doi: 10.1016/j.metabol.2016.05.003. [DOI] [PubMed] [Google Scholar]
- 85.Nam J.S., Jo S., Kang S., Ahn C.W., Kim K.R., Park J.S. Association between lipoprotein(a) and nonalcoholic fatty liver disease among Korean adults. Clin. Chim. Acta. 2016;461:14–18. doi: 10.1016/j.cca.2016.07.003. [DOI] [PubMed] [Google Scholar]
- 86.Naik A., Košir R., Rozman D. Genomic aspects of NAFLD pathogenesis. Genomics. 2013;102:84–95. doi: 10.1016/j.ygeno.2013.03.007. [DOI] [PubMed] [Google Scholar]
- 87.Eslam M., Valenti L., Romeo S. Genetics and epigenetics of NAFLD and NASH: Clinical impact. J. Hepatol. 2018;68:268–279. doi: 10.1016/j.jhep.2017.09.003. [DOI] [PubMed] [Google Scholar]
- 88.Lonardo A., Bellentani S., Argo C.K., Ballestri S., Byrne C.D., Caldwell S.H., Cortez-Pinto H., Grieco A., Machado M.V., Miele L., et al. Epidemiological modifiers of non-alcoholic fatty liver disease: Focus on high-risk groups. Dig. Liver Dis. 2015;47:997–1006. doi: 10.1016/j.dld.2015.08.004. [DOI] [PubMed] [Google Scholar]
- 89.Lu G., Shimizu I., Cui X., Itonaga M., Tamaki K., Fukuno H., Inoue H., Honda H., Ito S. Antioxidant and antiapoptotic activities of idoxifene and estradiol in hepatic fibrosis in rats. Life Sci. 2004;74:897–907. doi: 10.1016/j.lfs.2003.08.004. [DOI] [PubMed] [Google Scholar]
- 90.Yasuda M., Shimizu I., Shiba M., Ito S. Suppressive effects of estradiol on dimethylnitrosamine-induced fibrosis of the liver in rats. Hepatology. 1999;29:719–727. doi: 10.1002/hep.510290307. [DOI] [PubMed] [Google Scholar]
- 91.Ballestri S., Nascimbeni F., Baldelli E., Marrazzo A., Romagnoli D., Lonardo A. NAFLD as a Sexual Dimorphic Disease: Role of Gender and Reproductive Status in the Development and Progression of Nonalcoholic Fatty Liver Disease and Inherent Cardiovascular Risk. Adv. Ther. 2017;34:1291–1326. doi: 10.1007/s12325-017-0556-1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 92.Després J.-P. Body Fat Distribution and Risk of Cardiovascular Disease. Circulation. 2012;126:1301–1313. doi: 10.1161/CIRCULATIONAHA.111.067264. [DOI] [PubMed] [Google Scholar]
- 93.Varlamov O., Bethea C.L., Roberts C.T. Sex-Specific Differences in Lipid and Glucose Metabolism. Front. Endocrinol. (Lausanne) 2015;5:241. doi: 10.3389/fendo.2014.00241. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 94.Nielsen S., Guo Z., Johnson C.M., Hensrud D.D., Jensen M.D. Splanchnic lipolysis in human obesity. J. Clin. Investig. 2004;113:1582–1588. doi: 10.1172/JCI21047. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 95.Turola E., Petta S., Vanni E., Milosa F., Valenti L., Critelli R., Miele L., Maccio L., Calvaruso V., Fracanzani A.L., et al. Ovarian senescence increases liver fibrosis in humans and zebrafish with steatosis. Dis. Model. Mech. 2015;8:1037–1046. doi: 10.1242/dmm.019950. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 96.Lonardo A., Trande P. Are there any sex differences in fatty liver? A study of glucose metabolism and body fat distribution. J. Gastroenterol. Hepatol. 2000;15:775–782. doi: 10.1046/j.1440-1746.2000.02226.x. [DOI] [PubMed] [Google Scholar]
- 97.Lundholm L., Zang H., Hirschberg A.L., Gustafsson J.-Å., Arner P., Dahlman-Wright K. Key lipogenic gene expression can be decreased by estrogen in human adipose tissue. Fertil. Steril. 2008;90:44–48. doi: 10.1016/j.fertnstert.2007.06.011. [DOI] [PubMed] [Google Scholar]
- 98.Klair J.S., Yang J.D., Abdelmalek M.F., Guy C.D., Gill R.M., Yates K., Unalp-Arida A., Lavine J.E., Clark J.M., Diehl A.M., et al. A longer duration of estrogen deficiency increases fibrosis risk among postmenopausal women with nonalcoholic fatty liver disease. Hepatology. 2016;64:85–91. doi: 10.1002/hep.28514. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 99.Kleiner D.E., Brunt E.M., Van Natta M., Behling C., Contos M.J., Cummings O.W., Ferrell L.D., Liu Y.-C., Torbenson M.S., Unalp-Arida A., et al. Design and validation of a histological scoring system for nonalcoholic fatty liver disease. Hepatology. 2005;41:1313–1321. doi: 10.1002/hep.20701. [DOI] [PubMed] [Google Scholar]
- 100.Brunt E.M., Kleiner D.E., Wilson L.A., Unalp A., Behling C.E., Lavine J.E., Neuschwander-Tetri B.A., NASH Clinical Research NetworkA list of members of the Nonalcoholic Steatohepatitis Clinical Research Network can be found in the Appendix Portal chronic inflammation in nonalcoholic fatty liver disease (NAFLD): A histologic marker of advanced NAFLD-Clinicopathologic correlations from the nonalcoholic steatohepatitis clinical research network. Hepatology. 2009;49:809–820. doi: 10.1002/hep.22724. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 101.Williams C.D., Stengel J., Asike M.I., Torres D.M., Shaw J., Contreras M., Landt C.L., Harrison S.A. Prevalence of Nonalcoholic Fatty Liver Disease and Nonalcoholic Steatohepatitis Among a Largely Middle-Aged Population Utilizing Ultrasound and Liver Biopsy: A Prospective Study. Gastroenterology. 2011;140:124–131. doi: 10.1053/j.gastro.2010.09.038. [DOI] [PubMed] [Google Scholar]
- 102.Farrell G.C., Larter C.Z. Nonalcoholic fatty liver disease: From steatosis to cirrhosis. Hepatology. 2006;43:99–112. doi: 10.1002/hep.20973. [DOI] [PubMed] [Google Scholar]
- 103.Piscaglia F., Svegliati-Baroni G., Barchetti A., Pecorelli A., Marinelli S., Tiribelli C., Bellentani S., HCC-NAFLD Italian Study Group. Tiribelli C., Svegliati-Baroni G., et al. Clinical patterns of hepatocellular carcinoma in nonalcoholic fatty liver disease: A multicenter prospective study. Hepatology. 2015;63:827–838. doi: 10.1002/hep.28368. [DOI] [PubMed] [Google Scholar]
- 104.Paradis V., Zalinski S., Chelbi E., Guedj N., Degos F., Vilgrain V., Bedossa P., Belghiti J. Hepatocellular carcinomas in patients with metabolic syndrome often develop without significant liver fibrosis: A pathological analysis. Hepatology. 2009;49:851–859. doi: 10.1002/hep.22734. [DOI] [PubMed] [Google Scholar]
- 105.Hester D., Golabi P., Paik J., Younossi I., Mishra A., Younossi Z.M. Among Medicare Patients With Hepatocellular Carcinoma, Non–alcoholic Fatty Liver Disease is the Most Common Etiology and Cause of Mortality. J. Clin. Gastroenterol. 2019 doi: 10.1097/MCG.0000000000001172. [DOI] [PubMed] [Google Scholar]
- 106.Hultcrantz R., Nasr P., Hagström H., Ekstedt M., Kechagias S., Stål P., Fredrikson M., Hagström H., Nasr P., Fredrikson M., et al. Fibrosis stage is the strongest predictor for disease-specific mortality in NAFLD after up to 33 years of follow-up. Hepatology. 2014;61:1547–1554. doi: 10.1002/hep.27368. [DOI] [PubMed] [Google Scholar]
- 107.Pelusi S., Cespiati A., Rametta R., Pennisi G., Mannisto V., Rosso C., Baselli G., Dongiovanni P., Fracanzani A.L., Badiali S., et al. Prevalence and Risk Factors of Significant Fibrosis in Patients With Nonalcoholic Fatty Liver Without Steatohepatitis. Clin. Gastroenterol. Hepatol. 2019 doi: 10.1016/j.cgh.2019.01.027. [DOI] [PubMed] [Google Scholar]
- 108.McPherson S., Hardy T., Henderson E., Burt A.D., Day C.P., Anstee Q.M. Evidence of NAFLD progression from steatosis to fibrosing-steatohepatitis using paired biopsies: Implications for prognosis and clinical management. J. Hepatol. 2015;62:1148–1155. doi: 10.1016/j.jhep.2014.11.034. [DOI] [PubMed] [Google Scholar]
- 109.Byrne C.D., Targher G. NAFLD: A multisystem disease. J. Hepatol. 2015;62:S47–S64. doi: 10.1016/j.jhep.2014.12.012. [DOI] [PubMed] [Google Scholar]
- 110.Lonardo A., Nascimbeni F., Maurantonio M., Marrazzo A., Rinaldi L., Adinolfi L.E. Nonalcoholic fatty liver disease: Evolving paradigms. World J. Gastroenterol. 2017;23:6571–6592. doi: 10.3748/wjg.v23.i36.6571. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 111.Arab J.P., Arrese M., Trauner M. Recent Insights into the Pathogenesis of Nonalcoholic Fatty Liver Disease. Annu. Rev. Pathol. Mech. Dis. 2018;13:321–350. doi: 10.1146/annurev-pathol-020117-043617. [DOI] [PubMed] [Google Scholar]
- 112.Donnelly K.L. Sources of fatty acids stored in liver and secreted via lipoporteins in patients with NAFLD. J. Clin. Investig. 2012;115:1343–1351. doi: 10.1172/JCI23621. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 113.McGarry J.D., Brown N.F. The mitochondrial carnitine palmitoyltransferase system. From concept to molecular analysis. Eur. J. Biochem. 1997;244:1–14. doi: 10.1111/j.1432-1033.1997.00001.x. [DOI] [PubMed] [Google Scholar]
- 114.Trauner M., Arrese M., Wagner M. Fatty liver and lipotoxicity. Biochim. Biophys. Acta-Mol. Cell Biol. Lipids. 2010;1801:299–310. doi: 10.1016/j.bbalip.2009.10.007. [DOI] [PubMed] [Google Scholar]
- 115.Koliaki C., Szendroedi J., Kaul K., Jelenik T., Nowotny P., Jankowiak F., Herder C., Carstensen M., Krausch M., Knoefel W.T., et al. Adaptation of Hepatic Mitochondrial Function in Humans with Non-Alcoholic Fatty Liver Is Lost in Steatohepatitis. Cell Metab. 2015;21:739–746. doi: 10.1016/j.cmet.2015.04.004. [DOI] [PubMed] [Google Scholar]
- 116.Gallagher E.J., LeRoith D. Minireview: IGF, Insulin, and Cancer. Endocrinology. 2011;152:2546–2551. doi: 10.1210/en.2011-0231. [DOI] [PubMed] [Google Scholar]
- 117.Yamashita T., Honda M., Takatori H., Nishino R., Minato H., Takamura H., Ohta T., Kaneko S. Activation of lipogenic pathway correlates with cell proliferation and poor prognosis in hepatocellular carcinoma. J. Hepatol. 2009;50:100–110. doi: 10.1016/j.jhep.2008.07.036. [DOI] [PubMed] [Google Scholar]
- 118.Dongiovanni P., Romeo S., Valenti L. Hepatocellular carcinoma in nonalcoholic fatty liver: Role of environmental and genetic factors. World J. Gastroenterol. 2014;20:12945–12955. doi: 10.3748/wjg.v20.i36.12945. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 119.Vinciguerra M., Carrozzino F., Peyrou M., Carlone S., Montesano R., Benelli R., Foti M. Unsaturated fatty acids promote hepatoma proliferation and progression through downregulation of the tumor suppressor PTEN. J. Hepatol. 2009;50:1132–1141. doi: 10.1016/j.jhep.2009.01.027. [DOI] [PubMed] [Google Scholar]
- 120.Marra F., Bertolani C. Adipokines in liver diseases. Hepatology. 2009;50:957–969. doi: 10.1002/hep.23046. [DOI] [PubMed] [Google Scholar]
- 121.Stender S., Kozlitina J., Nordestgaard B.G., Tybjærg-Hansen A., Hobbs H.H., Cohen J.C. Adiposity amplifies the genetic risk of fatty liver disease conferred by multiple loci. Nat. Genet. 2017;49:842–847. doi: 10.1038/ng.3855. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 122.Romeo S., Kozlitina J., Xing C., Pertsemlidis A., Cox D., Pennacchio L.A., Boerwinkle E., Cohen J.C., Hobbs H.H. Genetic variation in PNPLA3 confers susceptibility to nonalcoholic fatty liver disease. Nat. Genet. 2008;40:1461–1465. doi: 10.1038/ng.257. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 123.Sookoian S., Pirola C.J. Meta-analysis of the influence of I148M variant of patatin-like phospholipase domain containing 3 gene (PNPLA3) on the susceptibility and histological severity of nonalcoholic fatty liver disease. Hepatology. 2011;53:1883–1894. doi: 10.1002/hep.24283. [DOI] [PubMed] [Google Scholar]
- 124.Sookoian S., Castaño G.O., Burgueño A.L., Gianotti T.F., Rosselli M.S., Pirola C.J. A nonsynonymous gene variant in the adiponutrin gene is associated with nonalcoholic fatty liver disease severity. J. Lipid Res. 2009;50:2111–2116. doi: 10.1194/jlr.P900013-JLR200. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 125.Trépo E., Romeo S., Zucman-Rossi J., Nahon P. PNPLA3 gene in liver diseases. J. Hepatol. 2016;65:399–412. doi: 10.1016/j.jhep.2016.03.011. [DOI] [PubMed] [Google Scholar]
- 126.Salameh H., Raff E., Erwin A., Seth D., Nischalke H.D., Falleti E., Burza M.A., Leathert J., Romeo S., Molinaro A., et al. PNPLA3 Gene Polymorphism Is Associated With Predisposition to and Severity of Alcoholic Liver Disease. Am. J. Gastroenterol. 2015;110:846–856. doi: 10.1038/ajg.2015.137. [DOI] [PubMed] [Google Scholar]
- 127.Alisi A., Mancina R.M., Xing C., Petta S., Rametta R., Nobili V., del Menico B., Valenti L., Craxì A., Fracanzani A.L., et al. The rs2294918 E434K variant modulates patatin-like phospholipase domain-containing 3 expression and liver damage. Hepatology. 2015;63:787–798. doi: 10.1002/hep.28370. [DOI] [PubMed] [Google Scholar]
- 128.Bruschi F.V., Claudel T., Tardelli M., Caligiuri A., Stulnig T.M., Marra F., Trauner M. The PNPLA3 I148M variant modulates the fibrogenic phenotype of human hepatic stellate cells. Hepatology. 2017;65:1875–1890. doi: 10.1002/hep.29041. [DOI] [PubMed] [Google Scholar]
- 129.Mahdessian H., Taxiarchis A., Popov S., Silveira A., Franco-Cereceda A., Hamsten A., Eriksson P., van’t Hooft F. TM6SF2 is a regulator of liver fat metabolism influencing triglyceride secretion and hepatic lipid droplet content. Proc. Natl. Acad. Sci. 2014;111:8913–8918. doi: 10.1073/pnas.1323785111. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 130.Kozlitina J., Smagris E., Stender S., Nordestgaard B.G., Zhou H.H., Tybjærg-Hansen A., Vogt T.F., Hobbs H.H., Cohen J.C. Exome-wide association study identifies a TM6SF2 variant that confers susceptibility to nonalcoholic fatty liver disease. Nat. Genet. 2014;46:352–356. doi: 10.1038/ng.2901. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 131.Liu Y.-L., Reeves H.L., Burt A.D., Tiniakos D., McPherson S., Leathart J.B.S., Allison M.E.D., Alexander G.J., Piguet A.-C., Anty R., et al. TM6SF2 rs58542926 influences hepatic fibrosis progression in patients with non-alcoholic fatty liver disease. Nat. Commun. 2014;5:4309. doi: 10.1038/ncomms5309. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 132.Goffredo M., Caprio S., Feldstein A.E., D’Adamo E., Shaw M.M., Pierpont B., Savoye M., Zhao H., Bale A.E., Santoro N. Role of TM6SF2 rs58542926 in the pathogenesis of nonalcoholic pediatric fatty liver disease: A multiethnic study. Hepatology. 2016;63:117–125. doi: 10.1002/hep.28283. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 133.Pirola C.J., Sookoian S. The dual and opposite role of the TM6SF2 -rs58542926 variant in protecting against cardiovascular disease and conferring risk for nonalcoholic fatty liver: A meta-analysis. Hepatology. 2015;62:1742–1756. doi: 10.1002/hep.28142. [DOI] [PubMed] [Google Scholar]
- 134.Sliz E., Sebert S., Würtz P., Kangas A.J., Soininen P., Lehtimäki T., Kähönen M., Viikari J., Männikkö M., Ala-Korpela M., et al. NAFLD risk alleles in PNPLA3, TM6SF2, GCKR and LYPLAL1 show divergent metabolic effects. Hum. Mol. Genet. 2018;27:2214–2223. doi: 10.1093/hmg/ddy124. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 135.Santoro N., Zhang C.K., Zhao H., Pakstis A.J., Kim G., Kursawe R., Dykas D.J., Bale A.E., Giannini C., Pierpont B., et al. Variant in the glucokinase regulatory protein (GCKR) gene is associated with fatty liver in obese children and adolescents. Hepatology. 2012;55:781–789. doi: 10.1002/hep.24806. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 136.Beer N.L., Tribble N.D., McCulloch L.J., Roos C., Johnson P.R.V., Orho-Melander M., Gloyn A.L. The P446L variant in GCKR associated with fasting plasma glucose and triglyceride levels exerts its effect through increased glucokinase activity in liver. Hum. Mol. Genet. 2009;18:4081–4088. doi: 10.1093/hmg/ddp357. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 137.Wang Y., van der Tuin S., Tjeerdema N., van Dam A.D., Rensen S.S., Hendrikx T., Berbée J.F.P., Atanasovska B., Fu J., Hoekstra M., et al. Plasma cholesteryl ester transfer protein is predominantly derived from Kupffer cells. Hepatology. 2015;62:1710–1722. doi: 10.1002/hep.27985. [DOI] [PubMed] [Google Scholar]
- 138.Aller R., Izaola O., Primo D., de Luis D., De Luis D. Cholesteryl ester transfer protein variant (RS1800777) with liver histology in non-alcoholic fatty liver disease patients. Ann. Nutr. Metab. 2018;73:265–270. doi: 10.1159/000493552. [DOI] [PubMed] [Google Scholar]
- 139.Musso G., Bo S., Cassader M., De Michieli F., Gambino R. Impact of sterol regulatory element-binding factor-1c polymorphism on incidence of nonalcoholic fatty liver disease and on the severity of liver disease and of glucose and lipid dysmetabolism. Am. J. Clin. Nutr. 2013;98:895–906. doi: 10.3945/ajcn.113.063792. [DOI] [PubMed] [Google Scholar]
- 140.Mancina R.M., Dongiovanni P., Petta S., Pingitore P., Meroni M., Rametta R., Borén J., Montalcini T., Pujia A., Wiklund O., et al. The MBOAT7-TMC4 Variant rs641738 Increases Risk of Nonalcoholic Fatty Liver Disease in Individuals of European Descent. Gastroenterology. 2016;150:1219–1230.e6. doi: 10.1053/j.gastro.2016.01.032. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 141.Krawczyk M., Rau M., Schattenberg J.M., Bantel H., Pathil A., Demir M., Kluwe J., Boettler T., Lammert F., Geier A., et al. Combined effects of the PNPLA3 rs738409, TM6SF2 rs58542926, and MBOAT7 rs641738 variants on NAFLD severity: A multicenter biopsy-based study. J. Lipid Res. 2017;58:247–255. doi: 10.1194/jlr.P067454. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 142.Umano G.R., Caprio S., Di Sessa A., Chalasani N., Dykas D.J., Pierpont B., Bale A.E., Santoro N. The rs626283 variant in the MBOAT7 gene is associated with insulin resistance and fatty liver in Caucasian obese youth. Am. J. Gastroenterol. 2018;113:376–383. doi: 10.1038/ajg.2018.1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 143.Hussain M.M., Rava P., Walsh M., Rana M., Iqbal J. Multiple functions of microsomal triglyceride transfer protein. Nutr. Metab. (Lond.) 2012;9:14. doi: 10.1186/1743-7075-9-14. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 144.Gouda W., Ashour E., Shaker Y., Ezzat W. MTP genetic variants associated with non-alcoholic fatty liver in metabolic syndrome patients. Genes Dis. 2017;4:222–228. doi: 10.1016/j.gendis.2017.09.002. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 145.Marchesini G., Brizi M., Morselli-Labate A.M., Bianchi G., Bugianesi E., McCullough A.J., Forlani G., Melchionda N. Association of nonalcoholic fatty liver disease with insulin resistance. Am. J. Med. 1999;107:450–455. doi: 10.1016/S0002-9343(99)00271-5. [DOI] [PubMed] [Google Scholar]
- 146.Lonardo A., Nascimbeni F., Mantovani A., Targher G. Hypertension, diabetes, atherosclerosis and NASH: Cause or consequence? J. Hepatol. 2018;68:335–352. doi: 10.1016/j.jhep.2017.09.021. [DOI] [PubMed] [Google Scholar]
- 147.Ballestri S., Zona S., Targher G., Romagnoli D., Baldelli E., Nascimbeni F., Roverato A., Guaraldi G., Lonardo A. Nonalcoholic fatty liver disease is associated with an almost twofold increased risk of incident type 2 diabetes and metabolic syndrome. Evidence from a systematic review and meta-analysis. J. Gastroenterol. Hepatol. 2016;31:936–944. doi: 10.1111/jgh.13264. [DOI] [PubMed] [Google Scholar]
- 148.Mantovani A., Byrne C.D., Bonora E., Targher G. Nonalcoholic Fatty Liver Disease and Risk of Incident Type 2 Diabetes: A Meta-analysis. Diabetes Care. 2018;41:372–382. doi: 10.2337/dc17-1902. [DOI] [PubMed] [Google Scholar]
- 149.Grimm D., Falcon A., Storm T.A., Kazantzis M., Kay M.A., Doege H., Stahl A., Tsang B., Xu H., Ortegon A.M. Silencing of Hepatic Fatty Acid Transporter Protein 5 in Vivo Reverses Diet-induced Non-alcoholic Fatty Liver Disease and Improves Hyperglycemia. J. Biol. Chem. 2008;283:22186–22192. doi: 10.1074/jbc.M803510200. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 150.Brown M.S., Goldstein J.L. Selective versus Total Insulin Resistance: A Pathogenic Paradox. Cell Metab. 2008;7:95–96. doi: 10.1016/j.cmet.2007.12.009. [DOI] [PubMed] [Google Scholar]
- 151.Biddinger S.B., Hernandez-Ono A., Rask-Madsen C., Haas J.T., Alemán J.O., Suzuki R., Scapa E.F., Agarwal C., Carey M.C., Stephanopoulos G., et al. Hepatic insulin resistance is sufficient to produce dyslipidemia and susceptibility to atherosclerosis. Cell Metab. 2015;27:320–331. doi: 10.1016/j.cmet.2007.11.013. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 152.Hijmans B.S., Grefhorst A., Oosterveer M.H., Groen A.K. Zonation of glucose and fatty acid metabolism in the liver: Mechanism and metabolic consequences. Biochimie. 2014;96:121–129. doi: 10.1016/j.biochi.2013.06.007. [DOI] [PubMed] [Google Scholar]
- 153.Chalasani N., Wilson L., Kleiner D.E., Cummings O.W., Brunt E.M., Ünalp A., NASH Clinical Research Network Relationship of steatosis grade and zonal location to histological features of steatohepatitis in adult patients with non-alcoholic fatty liver disease. J. Hepatol. 2008;48:829–834. doi: 10.1016/j.jhep.2008.01.016. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 154.Kleiner D.E., Makhlouf H.R. Histology of Nonalcoholic Fatty Liver Disease and Nonalcoholic Steatohepatitis in Adults and Children. Clin. Liver Dis. 2016;20:293–312. doi: 10.1016/j.cld.2015.10.011. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 155.Sanders F.W.B., Griffin J.L. De novo lipogenesis in the liver in health and disease: More than just a shunting yard for glucose. Biol. Rev. 2016;91:452–468. doi: 10.1111/brv.12178. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 156.Perseghin G., Lattuada G., De Cobelli F., Esposito A., Costantino F., Canu T., Scifo P., De Taddeo F., Maffi P., Secchi A., et al. Reduced intrahepatic fat content is associated with increased whole-body lipid oxidation in patients with type 1 diabetes. Diabetologia. 2005;48:2615–2621. doi: 10.1007/s00125-005-0014-5. [DOI] [PubMed] [Google Scholar]
- 157.Petersen M.C., Rinehart J., Shulman G.I., Petersen M.C., Madiraju A.K., Gassaway B.M., Marcel M., Nasiri A.R., Butrico G., Marcucci M.J., et al. Insulin receptor Thr 1160 phosphorylation mediates lipid-induced hepatic insulin resistance Find the latest version: Insulin receptor Thr 1160 phosphorylation mediates lipid-induced hepatic insulin resistance. J. Clin. Investig. 2016;126:4361–4371. doi: 10.1172/JCI86013. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 158.Galadari S., Rahman A., Pallichankandy S., Galadari A., Thayyullathil F. Role of ceramide in diabetes mellitus: Evidence and mechanisms: MedSök Region Skåne. Lipids Health Dis. 2013;12:98. doi: 10.1186/1476-511X-12-98. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 159.Bi P., Kuang S. Notch signaling as a novel regulator of metabolism. Trends Endocrinol. Metab. 2015;26:248–255. doi: 10.1016/j.tem.2015.02.006. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 160.Kopan R., Ilagan M.X.G. The Canonical Notch Signaling Pathway: Unfolding the Activation Mechanism. Cell. 2009;137:216–233. doi: 10.1016/j.cell.2009.03.045. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 161.Guruharsha K.G., Kankel M.W., Artavanis-Tsakonas S. The Notch signalling system: Recent insights into the complexity of a conserved pathway. Nat. Rev. Genet. 2012;13:654–666. doi: 10.1038/nrg3272. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 162.Geisler F., Strazzabosco M. Emerging roles of Notch signaling in liver disease. Hepatology. 2015;61:382–392. doi: 10.1002/hep.27268. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 163.Zhu C., Kim K., Wang X., Bartolome A., Salomao M., Dongiovanni P., Meroni M., Graham M.J., Yates K.P., Diehl A.M., et al. Hepatocyte Notch activation induces liver fibrosis in nonalcoholic steatohepatitis. Sci. Transl. Med. 2018;10:eaat0344. doi: 10.1126/scitranslmed.aat0344. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 164.Romeo S. Notch and Nonalcoholic Fatty Liver and Fibrosis. N. Engl. J. Med. 2019;380:681–683. doi: 10.1056/NEJMcibr1815636. [DOI] [PubMed] [Google Scholar]
- 165.Bi P., Shan T., Liu W., Yue F., Yang X., Liang X.-R., Wang J., Li J., Carlesso N., Liu X., et al. Inhibition of Notch signaling promotes browning of white adipose tissue and ameliorates obesity. Nat. Med. 2014;20:911–918. doi: 10.1038/nm.3615. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 166.Pajvani U.B., Shawber C.J., Samuel V.T., Birkenfeld A.L., Shulman G.I., Kitajewski J., Accili D. Inhibition of Notch signaling ameliorates insulin resistance in a FoxO1-dependent manner. Nat. Med. 2011;17:961–967. doi: 10.1038/nm.2378. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 167.DeFronzo R.A., Jacot E., Jequier E., Maeder E., Wahren J., Felber J.P. The effect of insulin on the disposal of intravenous glucose. Results from indirect calorimetry and hepatic and femoral venous catheterization. Diabetes. 1981;30:1000–1007. doi: 10.2337/diab.30.12.1000. [DOI] [PubMed] [Google Scholar]
- 168.Yu R., Shi Q., Liu L., Chen L. Relationship of sarcopenia with steatohepatitis and advanced liver fibrosis in non-alcoholic fatty liver disease: A meta-analysis. BMC Gastroenterol. 2018;18:51. doi: 10.1186/s12876-018-0776-0. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 169.Petta S., Ciminnisi S., Di Marco V., Cabibi D., Cammà C., Licata A., Marchesini G., Craxì A. Sarcopenia is associated with severe liver fibrosis in patients with non-alcoholic fatty liver disease. Aliment. Pharmacol. Ther. 2017;45:510–518. doi: 10.1111/apt.13889. [DOI] [PubMed] [Google Scholar]
- 170.Pedersen B.K., Febbraio M.A. Muscles, exercise and obesity: Skeletal muscle as a secretory organ. Nat. Rev. Endocrinol. 2012;8:457–465. doi: 10.1038/nrendo.2012.49. [DOI] [PubMed] [Google Scholar]
- 171.Pappachan J.M., Babu S., Krishnan B., Ravindran N.C. Non-alcoholic Fatty Liver Disease: A Clinical Update. J. Clin. Transl. Hepatol. 2017;5:384–393. doi: 10.14218/JCTH.2017.00013. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 172.Lim J.S., Mietus-Snyder M., Valente A., Schwarz J.M., Lustig R.H. The role of fructose in the pathogenesis of NAFLD and the metabolic syndrome. Nat. Rev. Gastroenterol. Hepatol. 2010;7:251–264. doi: 10.1038/nrgastro.2010.41. [DOI] [PubMed] [Google Scholar]
- 173.Basarnoglu M., Basarnoglu G., Bugianesi E. Carbohydrate intake and nonalcoholic fatty liver disease: Fructose as a weapon of mass destruction. HepatoBiliary Surg Nutr. 2015;4:109–116. doi: 10.3978/j.issn.2304-3881.2014.11.05. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 174.Adeli K., Su Q., Rutledge A.C., Dekker M.J., Baker C. Fructose: A highly lipogenic nutrient implicated in insulin resistance, hepatic steatosis, and the metabolic syndrome. Am. J. Physiol. Metab. 2010;299:E685–E694. doi: 10.1152/ajpendo.00283.2010. [DOI] [PubMed] [Google Scholar]
- 175.Basaranoglu M., Basaranoglu G., Sabuncu T., Sentürk H. Fructose as a key player in the development of fatty liver disease. World J. Gastroenterol. 2013;19:1166–1172. doi: 10.3748/wjg.v19.i8.1166. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 176.Vos M.B., Lavine J.E. Dietary fructose in nonalcoholic fatty liver disease. Hepatology. 2013;57:2525–2531. doi: 10.1002/hep.26299. [DOI] [PubMed] [Google Scholar]
- 177.Barrera F., George J. The role of diet and nutritional intervention for the management of patients with NAFLD. Clin. Liver Dis. 2014;18:91–112. doi: 10.1016/j.cld.2013.09.009. [DOI] [PubMed] [Google Scholar]
- 178.Lambertz J., Weiskirchen S., Landert S., Weiskirchen R. Fructose: A dietary sugar in crosstalk with microbiota contributing to the development and progression of non-alcoholic liver disease. Front. Immunol. 2017;8 doi: 10.3389/fimmu.2017.01159. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 179.Tarantino G., Savastano S., Colao A. Hepatic steatosis, low-grade chronic inflammation and hormone/growth factor/adipokine imbalance. World J. Gastroenterol. 2010;16:4773–4783. doi: 10.3748/wjg.v16.i38.4773. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 180.Finelli C., Tarantino G. What is the role of adiponectin in obesity related non-alcoholic fatty liver disease? World J. Gastroenterol. 2013;19:802–812. doi: 10.3748/wjg.v19.i6.802. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 181.Musso G., Gambino R., Biroli G., Carello M., Faga E., Pacini G., De Michieli F., Cassader M., Durazzo M., Rizzetto M., et al. Hypoadiponectinemia Predicts the Severity of Hepatic Fibrosis and Pancreatic Beta-Cell Dysfunction in Nondiabetic Nonobese Patients with Nonalcoholic Steatohepatitis. Am. J. Gastroenterol. 2005;100:2438–2446. doi: 10.1111/j.1572-0241.2005.00297.x. [DOI] [PubMed] [Google Scholar]
- 182.Polyzos S.A., Toulis K.A., Goulis D.G., Zavos C., Kountouras J. Serum total adiponectin in nonalcoholic fatty liver disease: A systematic review and meta-analysis. Metabolism. 2011;60:313–326. doi: 10.1016/j.metabol.2010.09.003. [DOI] [PubMed] [Google Scholar]
- 183.Minokoshi Y., Kim Y.-B., Peroni O.D., Fryer L.G.D., Müller C., Carling D., Kahn B.B. Leptin stimulates fatty-acid oxidation by activating AMP-activated protein kinase. Nature. 2002;415:339–343. doi: 10.1038/415339a. [DOI] [PubMed] [Google Scholar]
- 184.Abenavoli L., Peta V. Role of adipokines and cytokines in non-alcoholic fatty liver disease. Rev. Recent Clin. Trials. 2014;9:134–140. doi: 10.2174/1574887109666141216102458. [DOI] [PubMed] [Google Scholar]
- 185.Adolph T.E., Grander C., Grabherr F., Tilg H. Adipokines and Non-Alcoholic Fatty Liver Disease: Multiple Interactions. Int. J. Mol. Sci. 2017;18:1649. doi: 10.3390/ijms18081649. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 186.Crespo J., Cayón A., Fernández-Gil P., Hernández-Guerra M., Mayorga M., Domínguez-Díez A., Fernández-Escalante J.C., Pons-Romero F. Gene expression of tumor necrosis factor [alpha ] and TNF-receptors, p55 and p75, in nonalcoholic steatohepatitis patients. Hepatology. 2001;34:1158–1163. doi: 10.1053/jhep.2001.29628. [DOI] [PubMed] [Google Scholar]
- 187.Kumar H., Kawai T., Akira S. Pathogen Recognition by the Innate Immune System. Int. Rev. Immunol. 2011;30:16–34. doi: 10.3109/08830185.2010.529976. [DOI] [PubMed] [Google Scholar]
- 188.Seki E., Brenner D.A. Toll-like receptors and adaptor molecules in liver disease: Update. Hepatology. 2008;48:322–335. doi: 10.1002/hep.22306. [DOI] [PubMed] [Google Scholar]
- 189.Lawrence T. The Nuclear Factor NF- B Pathway in Inflammation. Cold Spring Harb. Perspect. Biol. 2009;1:a001651. doi: 10.1101/cshperspect.a001651. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 190.Arrese M., Cabrera D., Kalergis A.M., Feldstein A.E. Innate Immunity and Inflammation in NAFLD/NASH. Dig. Dis. Sci. 2016;61:1294–1303. doi: 10.1007/s10620-016-4049-x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 191.Lancaster G.I., Langley K.G., Berglund N.A., Kammoun H.L., Reibe S., Estevez E., Weir J., Mellett N.A., Pernes G., Conway J.R.W., et al. Evidence that TLR4 Is Not a Receptor for Saturated Fatty Acids but Mediates Lipid-Induced Inflammation by Reprogramming Macrophage Metabolism. Cell Metab. 2018;27:1096–1110.e5. doi: 10.1016/j.cmet.2018.03.014. [DOI] [PubMed] [Google Scholar]
- 192.Britton L., Bridle K., Reiling J., Santrampurwala N., Wockner L., Ching H., Stuart K., Subramaniam V.N., Jeffrey G., St. Pierre T., et al. Hepatic iron concentration correlates with insulin sensitivity in nonalcoholic fatty liver disease. Hepatol. Commun. 2018;2:644–653. doi: 10.1002/hep4.1190. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 193.Eaton J.W., Qian M. Molecular bases of cellular iron toxicity. Free Radic. Biol. Med. 2002;32:833–840. doi: 10.1016/S0891-5849(02)00772-4. [DOI] [PubMed] [Google Scholar]
- 194.Puntarulo S. Iron, oxidative stress and human health. Mol. Aspects Med. 2005;26:299–312. doi: 10.1016/j.mam.2005.07.001. [DOI] [PubMed] [Google Scholar]
- 195.MacDonald G.A., Bridle K.R., Ward P.J., Walker N.I., Houglum K., George D.K., Smith J.L., Powell L.W., Crawford D.H., Ramm G.A. Lipid peroxidation in hepatic steatosis in humans is associated with hepatic fibrosis and occurs predominately in acinar zone 3. J. Gastroenterol. Hepatol. 2001;16:599–606. doi: 10.1046/j.1440-1746.2001.02445.x. [DOI] [PubMed] [Google Scholar]
- 196.Maliken B.D., Nelson J.E., Klintworth H.M., Beauchamp M., Yeh M.M., Kowdley K.V. Hepatic reticuloendothelial system cell iron deposition is associated with increased apoptosis in nonalcoholic fatty liver disease. Hepatology. 2013;57:1806–1813. doi: 10.1002/hep.26238. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 197.Nelson J.E., Wilson L., Brunt E.M., Yeh M.M., Kleiner D.E., Unalp-Arida A., Kowdley K.V., Nonalcoholic Steatohepatitis Clinical Research Network Relationship between the pattern of hepatic iron deposition and histological severity in nonalcoholic fatty liver disease. Hepatology. 2011;53:448–457. doi: 10.1002/hep.24038. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 198.Handa P., Morgan-Stevenson V., Maliken B.D., Nelson J.E., Washington S., Westerman M., Yeh M.M., Kowdley K.V. Iron overload results in hepatic oxidative stress, immune cell activation, and hepatocellular ballooning injury, leading to nonalcoholic steatohepatitis in genetically obese mice. Am. J. Physiol. Liver Physiol. 2016;310:G117–G127. doi: 10.1152/ajpgi.00246.2015. [DOI] [PubMed] [Google Scholar]
- 199.Kowdley K.V., Belt P., Wilson L.A., Yeh M.M., Neuschwander-Tetri B.A., Chalasani N., Sanyal A.J., Nelson J.E., NASH Clinical Research Network Serum ferritin is an independent predictor of histologic severity and advanced fibrosis in patients with nonalcoholic fatty liver disease. Hepatology. 2012;55:77–85. doi: 10.1002/hep.24706. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 200.Licata A., Nebbia M.E., Cabibbo G., Iacono G.L., Barbaria F., Brucato V., Alessi N., Porrovecchio S., Di Marco V., Craxì A., et al. Hyperferritinemia is a risk factor for steatosis in chronic liver disease. World J. Gastroenterol. 2009;15:2132–2138. doi: 10.3748/wjg.15.2132. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 201.Buzzetti E., Petta S., Manuguerra R., Luong T.V., Cabibi D., Corradini E., Craxì A., Pinzani M., Tsochatzis E., Pietrangelo A. Evaluating the association of serum ferritin and hepatic iron with disease severity in non-alcoholic fatty liver disease. Liver Int. 2019 doi: 10.1111/liv.14096. [DOI] [PubMed] [Google Scholar]
- 202.Adams L.A., Crawford D.H., Stuart K., House M.J., St. Pierre T.G., Webb M., Ching H.L.I., Kava J., Bynevelt M., MacQuillan G.C., et al. The impact of phlebotomy in nonalcoholic fatty liver disease: A prospective, randomized, controlled trial. Hepatology. 2015;61:1555–1564. doi: 10.1002/hep.27662. [DOI] [PubMed] [Google Scholar]
- 203.Valenti L., Fracanzani A.L., Dongiovanni P., Rovida S., Rametta R., Fatta E., Pulixi E.A., Maggioni M., Fargion S. A randomized trial of iron depletion in patients with nonalcoholic fatty liver disease and hyperferritinemia. World J. Gastroenterol. 2014;20:3002. doi: 10.3748/wjg.v20.i11.3002. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 204.Schaap F.G., Trauner M., Jansen P.L.M. Bile acid receptors as targets for drug development. Nat. Rev. Gastroenterol. Hepatol. 2014;11:55–67. doi: 10.1038/nrgastro.2013.151. [DOI] [PubMed] [Google Scholar]
- 205.Arab J.P., Karpen S.J., Dawson P.A., Arrese M., Trauner M., Arab J.P., Dawson P.A., Arrese M. Bile acids and nonalcoholic fatty liver disease: Molecular insights and therapeutic perspectives. Hepatology. 2016;65:350–362. doi: 10.1002/hep.28709. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 206.Perino A., Schoonjans K. TGR5 and Immunometabolism: Insights from Physiology and Pharmacology. Trends Pharmacol. Sci. 2015;36:847–857. doi: 10.1016/j.tips.2015.08.002. [DOI] [PubMed] [Google Scholar]
- 207.Ridlon J.M., Kang D.J., Hylemon P.B., Bajaj J.S. Bile acids and the gut microbiome. Curr. Opin. Gastroenterol. 2014;30:332–338. doi: 10.1097/MOG.0000000000000057. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 208.Inagaki T., Moschetta A., Lee Y.-K., Peng L., Zhao G., Downes M., Yu R.T., Shelton J.M., Richardson J.A., Repa J.J., et al. Regulation of antibacterial defense in the small intestine by the nuclear bile acid receptor. Proc. Natl. Acad. Sci. USA. 2006;103:3920–3925. doi: 10.1073/pnas.0509592103. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 209.Lin C.-H., Kohli R. Bile acid metabolism and signaling: Potential therapeutic target for nonalcoholic fatty liver disease. Clin. Transl. Gastroenterol. 2018;9:1–3. doi: 10.1038/s41424-018-0034-3. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 210.Mazzoccoli G., De Cosmo S., Mazza T. The biological clock: A pivotal hub in non-alcoholic fatty liver disease pathogenesis. Front. Physiol. 2018;9:1–16. doi: 10.3389/fphys.2018.00193. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 211.Moore R.Y. The Suprachiasmatic Nucleus and the Circadian Timing System. Prog. Mol. Biol. Transl. Sci. 2013;119:1–28. doi: 10.1016/B978-0-12-396971-2.00001-4. [DOI] [PubMed] [Google Scholar]
- 212.Reinke H., Asher G. Circadian Clock Control of Liver Metabolic Functions. Gastroenterology. 2016;150:574–580. doi: 10.1053/j.gastro.2015.11.043. [DOI] [PubMed] [Google Scholar]
- 213.Kettner N.M., Voicu H., Finegold M.J., Coarfa C., Sreekumar A., Putluri N., Katchy C.A., Lee C., Moore D.D., Fu L. Circadian Homeostasis of Liver Metabolism Suppresses Hepatocarcinogenesis. Cancer Cell. 2016;30:909–924. doi: 10.1016/j.ccell.2016.10.007. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 214.Tahara Y., Shibata S. Circadian rhythms of liver physiology and disease: Experimental and clinical evidence. Nat. Rev. Gastroenterol. Hepatol. 2016;13:217–226. doi: 10.1038/nrgastro.2016.8. [DOI] [PubMed] [Google Scholar]
- 215.Zagami R.M., Di Pino A., Urbano F., Piro S., Purrello F., Rabuazzo A.M. Low circulating vitamin D levels are associated with increased arterial stiffness in prediabetic subjects identified according to HbA1c. Atherosclerosis. 2015;243:395–401. doi: 10.1016/j.atherosclerosis.2015.09.038. [DOI] [PubMed] [Google Scholar]
- 216.Sung K.-C., Ryu S., Lee J.-Y., Kim J.-Y., Wild S.H., Byrne C.D. Effect of exercise on the development of new fatty liver and the resolution of existing fatty liver. J. Hepatol. 2016;65:791–797. doi: 10.1016/j.jhep.2016.05.026. [DOI] [PubMed] [Google Scholar]
- 217.Prenner S., Rinella M.E. Moderate Exercise for Nonalcoholic Fatty Liver Disease. JAMA Intern. Med. 2016;176:1083. doi: 10.1001/jamainternmed.2016.3221. [DOI] [PubMed] [Google Scholar]
- 218.Marchesini G., Petta S., Dalle Grave R. Diet, weight loss, and liver health in nonalcoholic fatty liver disease: Pathophysiology, evidence, and practice. Hepatology. 2016;63:2032–2043. doi: 10.1002/hep.28392. [DOI] [PubMed] [Google Scholar]
- 219.Vilar-Gomez E., Martinez-Perez Y., Calzadilla-Bertot L., Torres-Gonzalez A., Gra-Oramas B., Gonzalez-Fabian L., Friedman S.L., Diago M., Romero-Gomez M. Weight Loss Through Lifestyle Modification Significantly Reduces Features of Nonalcoholic Steatohepatitis. Gastroenterology. 2015;149:367–378.e5. doi: 10.1053/j.gastro.2015.04.005. [DOI] [PubMed] [Google Scholar]
- 220.Harrison S.A., Fecht W., Brunt E.M., Neuschwander-Tetri B.A. Orlistat for overweight subjects with nonalcoholic steatohepatitis: A randomized, prospective trial. Hepatology. 2009;49:80–86. doi: 10.1002/hep.22575. [DOI] [PubMed] [Google Scholar]
- 221.Haufe S., Engeli S., Kast P., Böhnke J., Utz W., Haas V., Hermsdorf M., Mähler A., Wiesner S., Birkenfeld A.L., et al. Randomized comparison of reduced fat and reduced carbohydrate hypocaloric diets on intrahepatic fat in overweight and obese human subjects. Hepatology. 2011;53:1504–1514. doi: 10.1002/hep.24242. [DOI] [PubMed] [Google Scholar]
- 222.Boden G. High- or low-carbohydrate diets: Which is better for weight loss, insulin resistance, and fatty livers? Gastroenterology. 2009;136:1490–1492. doi: 10.1053/j.gastro.2009.03.019. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 223.Bower G., Toma T., Harling L., Jiao L.R., Efthimiou E., Darzi A., Athanasiou T., Ashrafian H. Bariatric Surgery and Non-Alcoholic Fatty Liver Disease: A Systematic Review of Liver Biochemistry and Histology. Obes. Surg. 2015;25:2280–2289. doi: 10.1007/s11695-015-1691-x. [DOI] [PubMed] [Google Scholar]
- 224.Zelber-Sagi S., Salomone F., Mlynarsky L. The Mediterranean dietary pattern as the diet of choice for non-alcoholic fatty liver disease: Evidence and plausible mechanisms. Liver Int. 2017;37:936–949. doi: 10.1111/liv.13435. [DOI] [PubMed] [Google Scholar]
- 225.Targher G., Byrne C.D. Ad Libitum Mediterranean or Low-Fat Diets as Treatments for Nonalcoholic Fatty Liver Disease? Hepatology. 2018;68:1668–1671. doi: 10.1002/hep.30142. [DOI] [PubMed] [Google Scholar]
- 226.Properzi C., O’Sullivan T.A., Sherriff J.L., Ching H.L., Jeffrey G.P., Buckley R.F., Tibballs J., MacQuillan G.C., Garas G., Adams L.A. Ad Libitum Mediterranean and Low-Fat Diets Both Significantly Reduce Hepatic Steatosis: A Randomized Controlled Trial. Hepatology. 2018;68:1741–1754. doi: 10.1002/hep.30076. [DOI] [PubMed] [Google Scholar]
- 227.Piepoli M.F., Hoes A.W., Agewall S., Albus C., Brotons C., Catapano A.L., Cooney M.-T., Corrà U., Cosyns B., Deaton C., et al. 2016 European Guidelines on cardiovascular disease prevention in clinical practice. Eur. Heart J. 2016;37:2315–2381. doi: 10.1093/eurheartj/ehw106. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 228.Perumpail B.J., Cholankeril R., Yoo E.R., Kim D., Ahmed A. An Overview of Dietary Interventions and Strategies to Optimize the Management of Non-Alcoholic Fatty Liver Disease. Diseases. 2017;5:23. doi: 10.3390/diseases5040023. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 229.Saab S., Mallam D., Cox G.A., Tong M.J. Impact of coffee on liver diseases: A systematic review. Liver Int. 2014;34:495–504. doi: 10.1111/liv.12304. [DOI] [PubMed] [Google Scholar]
- 230.Mantovani A. Time to revise the definition of NAFLD: A purist vision. Dig. Liver Dis. 2019;51:457–458. doi: 10.1016/j.dld.2018.12.018. [DOI] [PubMed] [Google Scholar]
- 231.Griswold M.G., Fullman N., Hawley C., Arian N., Zimsen S.R.M., Tymeson H.D., Venkateswaran V., Tapp A.D., Forouzanfar M.H., Salama J.S., et al. Alcohol use and burden for 195 countries and territories, 1990–2016: A systematic analysis for the Global Burden of Disease Study 2016. Lancet. 2018;392:1015–1035. doi: 10.1016/S0140-6736(18)31310-2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 232.Aithal G.P., Thomas J.A., Kaye P.V., Lawson A., Ryder S.D., Spendlove I., Austin A.S., Freeman J.G., Morgan L., Webber J. Randomized, Placebo-Controlled Trial of Pioglitazone in Nondiabetic Subjects With Nonalcoholic Steatohepatitis. Gastroenterology. 2008;135:1176–1184. doi: 10.1053/j.gastro.2008.06.047. [DOI] [PubMed] [Google Scholar]
- 233.Sanyal A.J., Chalasani N., Kowdley K.V., McCullough A., Diehl A.M., Bass N.M., Neuschwander-Tetri B.A., Lavine J.E., Tonascia J., Unalp A., et al. Pioglitazone, Vitamin E, or Placebo for Nonalcoholic Steatohepatitis. N. Engl. J. Med. 2010;362:1675–1685. doi: 10.1056/NEJMoa0907929. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 234.Shah P., Mudaliar S. Pioglitazone: Side effect and safety profile. Expert Opin. Drug Saf. 2010;9:347–354. doi: 10.1517/14740331003623218. [DOI] [PubMed] [Google Scholar]
- 235.Bugianesi E., Gentilcore E., Manini R., Natale S., Vanni E., Villanova N., David E., Rizzetto M., Marchesini G. A Randomized Controlled Trial of Metformin versus Vitamin E or Prescriptive Diet in Nonalcoholic Fatty Liver Disease. Am. J. Gastroenterol. 2005;100:1082–1090. doi: 10.1111/j.1572-0241.2005.41583.x. [DOI] [PubMed] [Google Scholar]
- 236.Haukeland J.W., Konopski Z., Eggesbø H.B., von Volkmann H.L., Raschpichler G., Bjøro K., Haaland T., Løberg E.M., Birkeland K. Metformin in patients with non-alcoholic fatty liver disease: A randomized, controlled trial. Scand. J. Gastroenterol. 2009;44:853–860. doi: 10.1080/00365520902845268. [DOI] [PubMed] [Google Scholar]
- 237.Shields W.W., Thompson K.E., Grice G.A., Harrison S.A., Coyle W.J. The Effect of Metformin and Standard Therapy versus Standard Therapy alone in Nondiabetic Patients with Insulin Resistance and Nonalcoholic Steatohepatitis (NASH): A Pilot Trial. Therap. Adv. Gastroenterol. 2009;2:157–163. doi: 10.1177/1756283X09105462. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 238.Tseng C.-H. Metformin and Risk of Hepatocellular Carcinoma in Taiwanese Patients with Type 2 Diabetes. Diabetes. 2018;38:2018–2027. doi: 10.2337/db18-1622-P. [DOI] [PubMed] [Google Scholar]
- 239.Fujita K., Iwama H., Miyoshi H., Tani J., Oura K., Tadokoro T., Sakamoto T., Nomura T., Morishita A., Yoneyama H., et al. Diabetes mellitus and metformin in hepatocellular carcinoma. World J. Gastroenterol. 2016;22:6100–6113. doi: 10.3748/wjg.v22.i27.6100. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 240.Armstrong M.J., Gaunt P., Aithal G.P., Barton D., Hull D., Parker R., Hazlehurst J.M., Guo K., Abouda G., Aldersley M.A., et al. Liraglutide safety and efficacy in patients with non-alcoholic steatohepatitis (LEAN): A multicentre, double-blind, randomised, placebo-controlled phase 2 study. Lancet. 2016;387:679–690. doi: 10.1016/S0140-6736(15)00803-X. [DOI] [PubMed] [Google Scholar]
- 241.Marso S.P., Daniels G.H., Brown-Frandsen K., Kristensen P., Mann J.F.E., Nauck M.A., Nissen S.E., Pocock S., Poulter N.R., Ravn L.S., et al. Liraglutide and Cardiovascular Outcomes in Type 2 Diabetes. N. Engl. J. Med. 2016;375:311–322. doi: 10.1056/NEJMoa1603827. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 242.Gastaldelli A., Marchesini G. Time for Glucagon like peptide-1 receptor agonists treatment for patients with NAFLD? J. Hepatol. 2016;64:262–264. doi: 10.1016/j.jhep.2015.11.031. [DOI] [PubMed] [Google Scholar]
- 243.Seghieri M., Christensen A.S., Andersen A., Solini A., Knop F.K., Vilsbøll T. Future Perspectives on GLP-1 Receptor Agonists and GLP-1/glucagon Receptor Co-agonists in the Treatment of NAFLD. Front. Endocrinol. (Lausanne) 2018;9 doi: 10.3389/fendo.2018.00649. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 244.Cui J., Philo L., Nguyen P., Hofflich H., Hernandez C., Bettencourt R., Richards L., Salotti J., Bhatt A., Hooker J., et al. Sitagliptin vs. placebo for non-alcoholic fatty liver disease: A randomized controlled trial. J. Hepatol. 2016;65:369–376. doi: 10.1016/j.jhep.2016.04.021. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 245.Scheen A.J. Cardiovascular Effects of New Oral Glucose-Lowering Agents. Circ. Res. 2018;122:1439–1459. doi: 10.1161/CIRCRESAHA.117.311588. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 246.Kuchay M.S., Krishan S., Mishra S.K., Farooqui K.J., Singh M.K., Wasir J.S., Bansal B., Kaur P., Jevalikar G., Gill H.K., et al. Effect of Empagliflozin on Liver Fat in Patients With Type 2 Diabetes and Nonalcoholic Fatty Liver Disease: A Randomized Controlled Trial (E-LIFT Trial) Diabetes Care. 2018;41:dc180165. doi: 10.2337/dc18-0165. [DOI] [PubMed] [Google Scholar]
- 247.Takase T., Nakamura A., Miyoshi H., Yamamoto C., Atsumi T. Amelioration of fatty liver index in patients with type 2 diabetes on ipragliflozin: An association with glucose-lowering effects. Endocr. J. 2017;64:363–367. doi: 10.1507/endocrj.EJ16-0295. [DOI] [PubMed] [Google Scholar]
- 248.Shibuya T., Fushimi N., Kawai M., Yoshida Y., Hachiya H., Ito S., Kawai H., Ohashi N., Mori A. Luseogliflozin improves liver fat deposition compared to metformin in type 2 diabetes patients with non-alcoholic fatty liver disease: A prospective randomized controlled pilot study. Diabetes, Obes. Metab. 2018;20:438–442. doi: 10.1111/dom.13061. [DOI] [PubMed] [Google Scholar]
- 249.Eriksson J.W., Lundkvist P., Jansson P.-A., Johansson L., Kvarnström M., Moris L., Miliotis T., Forsberg G.-B., Risérus U., Lind L., et al. Effects of dapagliflozin and n-3 carboxylic acids on non-alcoholic fatty liver disease in people with type 2 diabetes: A double-blind randomised placebo-controlled study. Diabetologia. 2018;61:1923–1934. doi: 10.1007/s00125-018-4675-2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 250.Scheen A.J. Effect of sodium-glucose cotransporter type 2 inhibitors on liver fat in patients with type 2 diabetes: Hepatic beyond cardiovascular and renal protection? Ann. Transl. Med. 2018;6:S68. doi: 10.21037/atm.2018.10.39. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 251.Ferrannini E., Muscelli E., Frascerra S., Baldi S., Mari A., Heise T., Broedl U.C., Woerle H.-J. Metabolic response to sodium-glucose cotransporter 2 inhibition in type 2 diabetic patients. J. Clin. Investig. 2014;124:499–508. doi: 10.1172/JCI72227. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 252.Bonnet F., Scheen A.J. Effects of SGLT2 inhibitors on systemic and tissue low-grade inflammation: The potential contribution to diabetes complications and cardiovascular disease. Diabetes Metab. 2018;44:457–464. doi: 10.1016/j.diabet.2018.09.005. [DOI] [PubMed] [Google Scholar]
- 253.Lonardo A., Bellentani S., Ratziu V., Loria P. Insulin resistance in nonalcoholic steatohepatitis: Necessary but not sufficient – death of a dogma from analysis of therapeutic studies? Expert Rev. Gastroenterol. Hepatol. 2011;5:279–289. doi: 10.1586/egh.11.19. [DOI] [PubMed] [Google Scholar]
- 254.Perumpail B., Li A., John N., Sallam S., Shah N., Kwong W., Cholankeril G., Kim D., Ahmed A. The Role of Vitamin E in the Treatment of NAFLD. Diseases. 2018;6:86. doi: 10.3390/diseases6040086. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 255.Sato K., Gosho M., Yamamoto T., Kobayashi Y., Ishii N., Ohashi T., Nakade Y., Ito K., Fukuzawa Y., Yoneda M. Vitamin E has a beneficial effect on nonalcoholic fatty liver disease: A meta-analysis of randomized controlled trials. Nutrition. 2015;31:923–930. doi: 10.1016/j.nut.2014.11.018. [DOI] [PubMed] [Google Scholar]
- 256.Wei J., Lei G.-H., Fu L., Zeng C., Yang T., Peng S.-F. Association between Dietary Vitamin C Intake and Non-Alcoholic Fatty Liver Disease: A Cross-Sectional Study among Middle-Aged and Older Adults. PLoS ONE. 2016;11:e0147985. doi: 10.1371/journal.pone.0147985. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 257.Shidfar F., Faghihi A., Amiri H.L., Mousavi S.N. Regression of Nonalcoholic Fatty Liver Disease with Zinc and Selenium Co-supplementation after Disease Progression in Rats. Iran. J. Med. Sci. 2018;43:26–31. [PMC free article] [PubMed] [Google Scholar]
- 258.Couet C., Delarue J., Ritz P., Antoine J.M., Lamisse F. Effect of dietary fish oil on body fat mass and basal fat oxidation in healthy adults. Int. J. Obes. Relat. Metab. Disord. 1997;21:637–643. doi: 10.1038/sj.ijo.0800451. [DOI] [PubMed] [Google Scholar]
- 259.de Castro G.S., Calder P.C. Non-alcoholic fatty liver disease and its treatment with n-3 polyunsaturated fatty acids. Clin. Nutr. 2018;37:37–55. doi: 10.1016/j.clnu.2017.01.006. [DOI] [PubMed] [Google Scholar]
- 260.Scorletti E., Byrne C.D. Omega-3 fatty acids and non-alcoholic fatty liver disease: Evidence of efficacy and mechanism of action. Mol. Aspects Med. 2018;64:135–146. doi: 10.1016/j.mam.2018.03.001. [DOI] [PubMed] [Google Scholar]
- 261.Spadaro L., Magliocco O., Spampinato D., Piro S., Oliveri C., Alagona C., Papa G., Rabuazzo A.M., Purrello F. Effects of n-3 polyunsaturated fatty acids in subjects with nonalcoholic fatty liver disease. Dig. Liver Dis. 2008;40:194–199. doi: 10.1016/j.dld.2007.10.003. [DOI] [PubMed] [Google Scholar]
- 262.Hodson L., Bhatia L., Scorletti E., Smith D.E., Jackson N.C., Shojaee-Moradie F., Umpleby M., Calder P.C., Byrne C.D. Docosahexaenoic acid enrichment in NAFLD is associated with improvements in hepatic metabolism and hepatic insulin sensitivity: A pilot study. Eur. J. Clin. Nutr. 2017;71:973–979. doi: 10.1038/ejcn.2017.9. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 263.Zein C.O., Yerian L.M., Gogate P., Lopez R., Kirwan J.P., Feldstein A.E., McCullough A.J. Pentoxifylline improves nonalcoholic steatohepatitis: A randomized placebo-controlled trial. Hepatology. 2011;54:1610–1619. doi: 10.1002/hep.24544. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 264.Floch M.H. Probiotics and Prebiotics. Gastroenterol. Hepatol. (N. Y.) 2014;10:680–681. [PMC free article] [PubMed] [Google Scholar]
- 265.Loman B.R., Hernández-Saavedra D., An R., Rector R.S. Prebiotic and probiotic treatment of nonalcoholic fatty liver disease: A systematic review and meta-analysis. Nutr. Rev. 2018;76:822–839. doi: 10.1093/nutrit/nuy031. [DOI] [PubMed] [Google Scholar]
- 266.Kobyliak N., Abenavoli L., Mykhalchyshyn G., Kononenko L., Boccuto L., Kyriienko D., Dynnyk O. A Multi-strain Probiotic Reduces the Fatty Liver Index, Cytokines and Aminotransferase levels in NAFLD Patients: Evidence from a Randomized Clinical Trial. J. Gastrointestin. Liver Dis. 2018;27:41–49. doi: 10.15403/jgld.2014.1121.271.kby. [DOI] [PubMed] [Google Scholar]
- 267.Neuschwander-Tetri B.A., Loomba R., Sanyal A.J., Lavine J.E., Van Natta M.L., Abdelmalek M.F., Chalasani N., Dasarathy S., Diehl A.M., Hameed B., et al. Farnesoid X nuclear receptor ligand obeticholic acid for non-cirrhotic, non-alcoholic steatohepatitis (FLINT): A multicentre, randomised, placebo-controlled trial. Lancet. 2015;385:956–965. doi: 10.1016/S0140-6736(14)61933-4. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 268.Abenavoli L., Falalyeyeva T., Boccuto L., Tsyryuk O., Kobyliak N. Obeticholic Acid: A New Era in the Treatment of Nonalcoholic Fatty Liver Disease. Pharmaceuticals. 2018;11:104. doi: 10.3390/ph11040104. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 269.Mudaliar S., Henry R.R., Sanyal A.J., Morrow L., Marschall H., Kipnes M., Adorini L., Sciacca C.I., Clopton P., Castelloe E., et al. Efficacy and Safety of the Farnesoid X Receptor Agonist Obeticholic Acid in Patients With Type 2 Diabetes and Nonalcoholic Fatty Liver Disease. Gastroenterology. 2013;145:574–582.e1. doi: 10.1053/j.gastro.2013.05.042. [DOI] [PubMed] [Google Scholar]
- 270.Lindor K.D., Kowdley K.V., Heathcote E.J., Harrison M.E., Jorgensen R., Angulo P., Lymp J.F., Burgart L., Colin P. Ursodeoxycholic acid for treatment of nonalcoholic steatohepatitis: Results of a randomized trial. Hepatology. 2004;39:770–778. doi: 10.1002/hep.20092. [DOI] [PubMed] [Google Scholar]
- 271.Dufour J., Oneta C.M., Gonvers J., Bihl F., Cerny A., Cereda J., Zala J., Helbling B., Steuerwald M., Zimmermann A. Randomized Placebo-Controlled Trial of Ursodeoxycholic Acid With Vitamin E in Nonalcoholic Steatohepatitis. Clin. Gastroenterol. Hepatol. 2006;4:1537–1543. doi: 10.1016/j.cgh.2006.09.025. [DOI] [PubMed] [Google Scholar]
- 272.Athyros V.G., Tziomalos K., Gossios T.D., Griva T., Anagnostis P., Kargiotis K., Pagourelias E.D., Theocharidou E., Karagiannis A., Mikhailidis D.P., et al. Safety and efficacy of long-term statin treatment for cardiovascular events in patients with coronary heart disease and abnormal liver tests in the Greek Atorvastatin and Coronary Heart Disease Evaluation (GREACE) Study: A post-hoc analysis. Lancet. 2010;376:1916–1922. doi: 10.1016/S0140-6736(10)61272-X. [DOI] [PubMed] [Google Scholar]
- 273.Tikkanen M.J., Fayyad R., Faergeman O., Olsson A.G., Wun C.-C., Laskey R., Kastelein J.J., Holme I., Pedersen T.R., IDEAL Investigators IDEAL Investigators Effect of intensive lipid lowering with atorvastatin on cardiovascular outcomes in coronary heart disease patients with mild-to-moderate baseline elevations in alanine aminotransferase levels. Int. J. Cardiol. 2013;168:3846–3852. doi: 10.1016/j.ijcard.2013.06.024. [DOI] [PubMed] [Google Scholar]
- 274.Athyros V.G., Boutari C., Stavropoulos K., Anagnostis P., Imprialos K.P., Doumas M., Karagiannis A. Statins: An Under-Appreciated Asset for the Prevention and the Treatment of NAFLD or NASH and the Related Cardiovascular Risk. Curr. Vasc. Pharmacol. 2018;16:246–253. doi: 10.2174/1570161115666170621082910. [DOI] [PubMed] [Google Scholar]
- 275.Scicali R., Di Pino A., Ferrara V., Urbano F., Piro S., Rabuazzo A.M., Purrello F. New treatment options for lipid-lowering therapy in subjects with type 2 diabetes. Acta Diabetol. 2018;55:209–218. doi: 10.1007/s00592-017-1089-4. [DOI] [PubMed] [Google Scholar]
- 276.Dongiovanni P., Petta S., Mannisto V., Mancina R.M., Pipitone R., Karja V., Maggioni M., Kakela P., Wiklund O., Mozzi E., et al. Statin use and non-alcoholic steatohepatitis in at risk individuals. J. Hepatol. 2015;63:705–712. doi: 10.1016/j.jhep.2015.05.006. [DOI] [PubMed] [Google Scholar]
- 277.McGlynn K.A., Divine G.W., Sahasrabuddhe V.V., Engel L.S., VanSlooten A., Wells K., Yood M.U., Alford S.H. Statin use and risk of hepatocellular carcinoma in a U.S. population. Cancer Epidemiol. 2014;38:523–527. doi: 10.1016/j.canep.2014.06.009. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 278.Del Ben M., Baratta F., Polimeni L., Pastori D., Loffredo L., Averna M., Violi F., Angelico F. Under-prescription of statins in patients with non-alcoholic fatty liver disease. Nutr. Metab. Cardiovasc. Dis. 2017;27:161–167. doi: 10.1016/j.numecd.2016.09.011. [DOI] [PubMed] [Google Scholar]
- 279.Averna M. The effect of ezetimibe on NAFLD. Atheroscler. Suppl. 2015;17:27–34. doi: 10.1016/S1567-5688(15)50007-X. [DOI] [PubMed] [Google Scholar]
- 280.Nakade Y., Murotani K., Inoue T., Kobayashi Y., Yamamoto T., Ishii N., Ohashi T., Ito K., Fukuzawa Y., Yoneda M. Ezetimibe for the treatment of non-alcoholic fatty liver disease: A meta-analysis. Hepatol. Res. 2017;47:1417–1428. doi: 10.1111/hepr.12887. [DOI] [PubMed] [Google Scholar]
- 281.Tanaka N., Kimura T., Fujimori N., Nagaya T., Komatsu M., Tanaka E. Current status, problems, and perspectives of non-alcoholic fatty liver disease research. World J. Gastroenterol. 2019;25:163–177. doi: 10.3748/wjg.v25.i2.163. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 282.Loomba R., Lawitz E., Mantry P.S., Jayakumar S., Caldwell S.H., Arnold H., Diehl A.M., Djedjos C.S., Han L., Myers R.P., et al. The ASK1 inhibitor selonsertib in patients with nonalcoholic steatohepatitis: A randomized, phase 2 trial. Hepatology. 2017;67:549. doi: 10.1002/hep.29514. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 283.Friedman S.L., Ratziu V., Harrison S.A., Abdelmalek M.F., Aithal G.P., Caballeria J., Francque S., Farrell G., Kowdley K.V., Craxi A., et al. A randomized, placebo-controlled trial of cenicriviroc for treatment of nonalcoholic steatohepatitis with fibrosis. Hepatology. 2018;67:1754–1767. doi: 10.1002/hep.29477. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 284.Gawrieh S., Chalasani N. Emerging Treatments for Nonalcoholic Fatty Liver Disease and Nonalcoholic Steatohepatitis. Clin. Liver Dis. 2018;22:189–199. doi: 10.1016/j.cld.2017.08.013. [DOI] [PubMed] [Google Scholar]
- 285.Ratziu V., Harrison S.A., Francque S., Bedossa P., Lehert P., Serfaty L., Romero-Gomez M., Boursier J., Abdelmalek M., Caldwell S., et al. Elafibranor, an Agonist of the Peroxisome Proliferator-Activated Receptor-α and -δ, Induces Resolution of Nonalcoholic Steatohepatitis Without Fibrosis Worsening. Gastroenterology. 2016;150:1147–1159.e5. doi: 10.1053/j.gastro.2016.01.038. [DOI] [PubMed] [Google Scholar]
- 286.Sookoian S., Pirola C.J. Elafibranor for the treatment of NAFLD: One pill, two molecular targets and multiple effects in a complex phenotype. Ann. Hepatol. 2016;15:604–609. [PubMed] [Google Scholar]
- 287.Safadi R., Konikoff F.M., Mahamid M., Zelber-Sagi S., Halpern M., Gilat T., Oren R., Group F. The Fatty Acid-Bile Acid Conjugate Aramchol Reduces Liver Fat Content in Patients With Nonalcoholic Fatty Liver Disease. Clin. Gastroenterol. Hepatol. 2014 doi: 10.1016/j.cgh.2014.04.038. [DOI] [PubMed] [Google Scholar]
- 288.Ratziu V., Ladron-De-Guevara L., Safadi R., Poordad F., Fuster F., Flores-Figueroa J., Harrison S.A., Arrese M., Fargion S., Ben-Bashat D., et al. One-year results of the global phase 2b randomized placebo-controlled arrest trial of aramchol, a stearoyl CoA desaturase inhibitor, in patients with NASH; Proceedings of the AASLD Liver Meeting; San Francisco, CA, USA. 9–13 November 2018. [Google Scholar]
- 289.Shiffman M., Freilich B., Vuppalanchi R., Watt K., Chan J.L., Spada A., Hagerty D.T., Schiff E. Randomised clinical trial: Emricasan versus placebo significantly decreases ALT and caspase 3/7 activation in subjects with non-alcoholic fatty liver disease. Aliment. Pharmacol. Ther. 2019;49:64–73. doi: 10.1111/apt.15030. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 290.Sanyal A., Abdelmalek M.F., Diehl A.M., Caldwell S., Shiffman M.L., Ghalib R., Lawitz E., Rockey D.C., Schall R.A., Jia C., et al. Efficacy and safety of simtuzumab for the treatment of nonalcoholic steatohepatitis with bridging fibrosis or cirrhosis: Results of two phase 2b, dose-ranging, randomized, placebo-controlled trials. J. Hepatol. 2017;66:S54. doi: 10.1016/S0168-8278(17)30370-7. [DOI] [Google Scholar]
- 291.Meex R.C., Hoy A.J., Morris A., Brown R.D., Lo J.C.Y., Burke M., Goode R.J.A., Kingwell B.A., Kraakman M.J., Febbraio M.A., et al. Fetuin B Is a Secreted Hepatocyte Factor Linking Steatosis to Impaired Glucose Metabolism. Cell Metab. 2015;22:1078–1089. doi: 10.1016/j.cmet.2015.09.023. [DOI] [PubMed] [Google Scholar]