Abstract
Pertussis remains a public health concern in most countries. This cross-sectional study aims to investigate the distribution of pertussis toxin antibodies (anti-PT IgG) in Tunisian children and adolescents aged 3–18 years, to define optimal age for booster vaccination. Anti-PT IgG concentrations of enrolled participants were measured using commercial enzyme-linked immunosorbent assay. Concentrations were classified as: indicative of current/recent infection if ⩾100 IU/ml, indicative of recent exposure to Bordetella pertussis within the last year if 40–100 IU/ml and less likely revealing a recent exposure to B. pertussis if <40 IU/ml. Between March and June 2018, a total of 304 participants (mean age: 9.3 years) were included in this study. Overall, 12.8% (95% confidence interval (CI) 9.1%–16.6%) were seropositive (IgG levels ⩾40 IU/ml). Among them, 14.7% (95% CI 2.3%–23.3%) had levels indicative of a current/recent infection. The multivariate Poisson regression analysis suggested associations between female gender, as well as age group 13–18 years and 3–5 years and higher anti-PT IgG concentrations. Our results are consistent with the notion that vaccine-induced immunity decline, as well as circulation of pertussis among school children and adolescents enables them to be reservoirs of infection and disease transmission to vulnerable infants. Booster dose of acellular pertussis vaccine for school entrants is therefore recommended.
Key words: Adolescents, children, pertussis, seroprevalence, Tunisia
Introduction
Pertussis, mainly caused by the bacterium Bordetella pertussis, is a highly contagious infectious disease [1]. Despite high-vaccination rates, pertussis remains a public health concern in several countries. New-borns and infants, not or partially vaccinated, are mostly affected [2]. They have the highest risk of eventual malignant pertussis manifested by severe complications including seizures, pneumonia, encephalopathy and a marked leucocytosis [3, 4].
An increase in pertussis incidence among old children and adolescents in some countries has been well-described [5]. In fact, these age categories, especially family members, seem to be a potential source of pertussis transmission to young infants [2, 6]. Contributing factors of this increase could be waning of vaccine-induced immunity, pathogen adaptation and changes in disease susceptibility [5, 7].
In Tunisia, infants are immunised with whole cell pertussis (wP) as a pentavalent combined vaccine (DTwP-HepB-Hib, Pentavac®, Serum Institute of India) at the age of 2, 3 and 6 months according to the National Immunization Program (NIP). A booster dose including diphtheria, tetanus and wP (DTwP) is administered at the age of 18 months [8]. Despite high-national vaccination coverage (98%), circulation of B. pertussis in Tunisian infants has been reported [9, 10] and three epidemics have been observed respectively in 2009, 2014 [10] and 2018 (unpublished observations). Moreover, circulation of pertussis among healthcare workers has been recently reported in a seroepidemiological study [11]. However, little is known about pertussis seroprevalence among children and adolescents, who are a potential reservoir of the disease.
Pertussis immunity, whether induced by vaccination or natural infection, is not lifelong [7]. Therefore, seroepidemiology is a powerful tool used to monitor effectiveness of vaccination programmes and identify age groups contributing to disease transmission [12]. In fact, determination of pertussis seroprevalence in a given population helps assess the immunity level and identify the target population for booster vaccination to reduce individual morbidity [12]. Moreover, small serosurveys in blood donors is a simple method for estimating a recent exposure to B. pertussis [13]. Unlike Tunisia, various countries have introduced booster doses of acellular pertussis vaccine (aP) for older children, adolescents and/or adults [14, 15].
This study aims to determine prevalence of immunoglobulin G (IgG) antibodies to pertussis toxin (PT) amongst a cohort of pre-school, school children and adolescents to evaluate the distribution of anti-PT IgG in different age groups and to assess age of decrease of vaccine-acquired immunity.
Materials and methods
Study design
This cross-sectional study was carried out from March 2018 to June 2018. Individuals aged 3–18 years, not having current respiratory infection and visiting the Children's Hospital of Tunis for check-up, were enrolled. All participants had received whole-cell pertussis primo-vaccination according to NIP. Information about age, DTwP booster vaccine history, sibling and history of long-lasting cough was obtained using a questionnaire.
Laboratory methods
Blood samples were collected via venepuncture and transported immediately to the Laboratory of Microbiology at the Children's Hospital of Tunis. After centrifugation, sera were extracted and stored at −20 °C until analysis. Measurement of anti-PT IgG concentrations was performed by using a commercial enzyme-linked immunosorbent assay (ELISA) kit (Euroimmun, Lübeck, Germany) according to the manufacturer's protocol. Concentrations were reported in International Units/ml (IU/ml). Results were interpreted following the manufacturer's instructions and as previously described [16]. Anti-PT IgG levels ⩾100 IU/ml were indicative of recent or active B. pertussis infection if the participant did not receive pertussis booster vaccine within the last 12 months. Concentrations between 40 and 100 IU/ml were considered to indicate a recent contact with B. pertussis within the last year, while anti-PT IgG levels <40 IU/ml were less likely revealing a recent exposure to B. pertussis. In fact, the cut-offs used were intended for diagnostic purposes, and levels below 40 IU/ml didn't mean seronegativity in an epidemiological sense, however they made a recent exposure to B. pertussis less likely.
Statistical analysis
Data were analysed using SPSS Software version 25 (SPSS Inc., Chicago, USA), with P < 0.05 considered to be significant. Subjects were stratified into three groups according to their ages. Values below the level of detection (5 IU/ml) were given a value of 2.5 IU/ml, whereas concentrations above the upper limit (200 IU/ml) were given a value of 175 IU/ml. Association of IgG anti-PT levels with gender, DTwP booster history, sibling, history of long-lasting cough and age groups was determined using the Pearson's chi-squared test (χ2). We used logistic as well as Poisson regression analysis to determine whether there are risk factors for children and adolescents that are associated with an increased chance on acquiring pertussis infection. Variables were expressed as odds ratios (OR) with their 95% confidence interval (CI).
Results
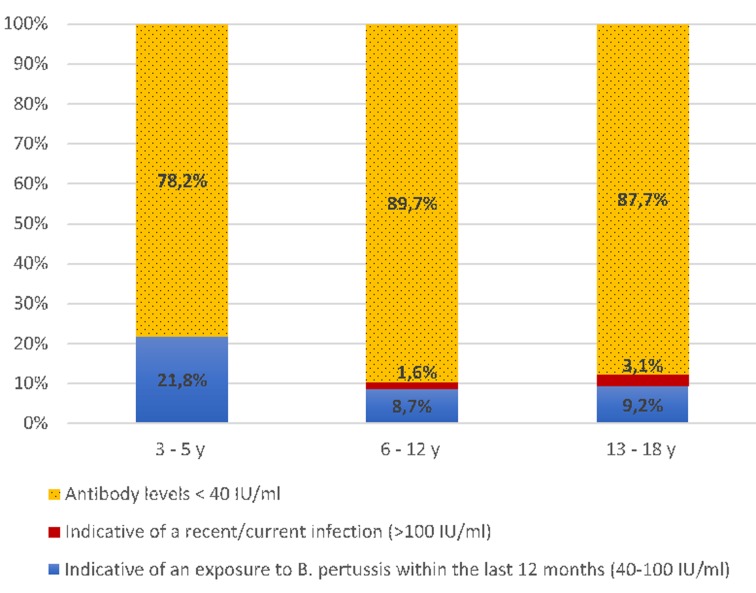
A total of 304 participants aged 3–18 years were enrolled in the current study. Mean age was 9.3 years and 51.3% were female. Population was divided into three age groups: pre-school children: 3–5 years (n = 55), school children: 6–12 years (n = 184) and high-school children: 13–18 years (n = 65). Distribution of ELISA results according to age categories is shown in Figure 1.
Fig. 1.
Frequency of anti-PT IgG levels in different age groups.
Overall, 39 (12.8%; 95% CI 9.1%–16.6%) subjects had antibody concentrations of ⩾40 IU/ml. Among them, 34 (11.2%) had ELISA results indicative of an infection/vaccination within the last 12 months, whereas five (1.6%) had ELISA results compatible with a recent or current infection (⩾100 IU/ml). Distribution of serology results according to age categories was not statistically significant (P > 0.05).
Using univariate and multivariate logistic regression analysis (Table 1), no significant association has been observed between seropositivity and demographic factors including gender, age category, sibling under 5 years and history of long-lasting cough (P > 0.05).
Table 1.
Association between demographic factors and seropositivity: univariate and multivariate analysis
| Variables | Univariate analysis | Multivariate analysis | ||||
|---|---|---|---|---|---|---|
| OR | 95% CI of OR | P value | OR | 95% CI of OR | P value | |
| Gender | ||||||
| Male | 1 | – | – | 1 | – | – |
| Female | 0.888 | 0.453–1.739 | 0.7282 | 0.876 | 0.439–1.750 | 0.7077 |
| Age category | ||||||
| 13–18 years | 1 | – | – | 1 | – | – |
| 3–5 years | 1.988 | 0.748–5.289 | 0.1685 | 2.314 | 0.828–6.467 | 0.1096 |
| 6–12 years | 0.820 | 0.341–1.977 | 0.6591 | 0.870 | 0.356–2.124 | 0.7593 |
| History of prolonged cough | 1.059 | 0.518–2.162 | 0.8753 | 0.975 | 0.465–2.043 | 0.9457 |
| Existence of sibling ⩽5 years | 0.794 | 0.348–1.814 | 0.5843 | 0.692 | 0.288–1.663 | 0.4101 |
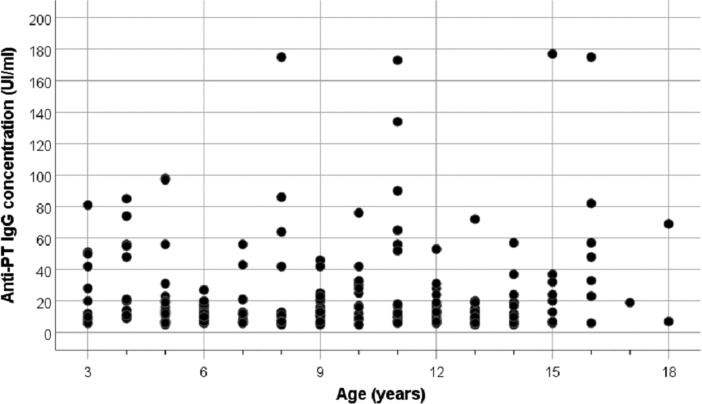
The highest IgG titres (⩾40 IU/ml) were detected among individuals aged 8–18 years (Fig. 2). Table 2 shows arithmetic and geometric mean anti-PT IgG titres in female, male and various age categories. No significant differences between groups were observed (P > 0.1). Overall, 107 (35.2%) cases were found to have undetectable anti-PT IgG antibodies (<5 IU/ml). The proportions were significantly highest in participants aged 7, 8 and 12 years (P = 0.001), confirming the hypothesis of rapid loss of immunity over time.
Fig. 2.
Distribution of anti-PT IgG levels according to age.
Table 2.
Arithmetic and geometric anti-PT IgG titre means according to gender and age groups
| Variable | Number | Arithmetic titres (IU/ml) | Geometric titres (IU/ml) | ||||
|---|---|---|---|---|---|---|---|
| Mean | Std | Median | Mean | Std | Median | ||
| Gender | |||||||
| Male | 148 | 18.1 | 27.9 | 9.0 | 9.0 | 3.3 | 8.2 |
| Female | 156 | 17.1 | 26.6 | 7.0 | 8.2 | 3.3 | 6.7 |
| P value | 0.75 | 0.54 | |||||
| Age groups | |||||||
| 3–5 years | 55 | 21.8 | 26.2 | 11.0 | 11.0 | 3.3 | 11.0 |
| 6–12 years | 184 | 15.4 | 24.9 | 7.0 | 7.4 | 3.0 | 6.7 |
| 13–18 years | 65 | 20.3 | 33.4 | 7.0 | 9.0 | 3.3 | 6.7 |
| P value | 0.21 | 0.15 | |||||
| Total | 304 | 17.6 | 27.2 | 8.0 | 8.2 | 3.3 | 8.2 |
Given the fact that a pertussis outbreak has started during the study period, we performed Poisson regression model to assess the impact in anti-PT IgG levels according to time, reflecting exposure to B. pertussis, to demographic factors (including age groups, gender, prolonged cough and sibling ⩽5 year) and to interaction time × age groups (Table 3). Our findings suggested that age groups 3–5 years, 13–18 years and female gender were significantly positively associated with increased anti-PT IgG levels. While the interaction delay×age group 13–18 years was negatively associated with anti-PT IgG levels.
Table 3.
Factors associated with changes in anti-PT IgG titres during the outbreak – Poisson regression modela
| Factors | Coefficient (95% CI) | P value |
|---|---|---|
| Female | 0.0893 (0.0424–0.0063) | <0.0001 |
| Age category 3–5 yearsb | 0.3859 (0.2807–0.4912) | <0.0001 |
| Age category 13–18 years | 0.2092 (0.1084–0.3099) | <0.0001 |
| Delayc | 0.0027 (−0.0006 to 0.0061) | 0.1088 |
| Prolonged cough | 0.0718 (−0.0155 to 0.1591) | 0.1069 |
| Sibling ⩽5 years | 0.0203 (−0.0731 to 0.1137) | 0.6703 |
Patients investigated before the starting of outbreak were excluded.
Age group 6–12 years and masculine gender have been considered as reference categories for comparison.
Time between patients' investigation and outbreak starting.
Discussion
As in other countries, possible explanations of pertussis cases increase in Tunisia include: improved diagnosis testing, better awareness of medical community, increased reporting of pertussis cases and waning of vaccine-induced immunity [7, 9, 17]. In fact, immunity induced by pertussis infection or vaccination is not lifelong [7]. In our study, we focused on the assessment of anti-PT IgG levels, specific marker of B. pertussis infection/vaccination with no reported cross-reactivity [16], in participants aged 3–18 years. To our knowledge, the current study is the first to provide information about seroprevalence of pertussis among Tunisian children and adolescents.
Among the study population, 87.2% (95% CI 83.4%–90.9%) had anti-PT concentrations <40 IU/ml. The highest rate (89.7%; 95% CI 85.3%–94.1%) was observed among school children aged 6–12 years. This suggests rapid decrease of vaccine-acquired immunity after the last DTwP booster dose received at 18 months. This is consistent with the study of Schwartz et al., who reported that pertussis vaccine effectiveness declines after 4 years and there is little to no protection beyond 7 years from last vaccination [18].
Demographic characteristics including age, gender, sibling under 5 years and history of long-lasting cough were not significantly associated with serology rates (P > 0.05). Varied results have been described elsewhere [13, 19, 20].
Our findings revealed that 12.8% (95% CI 9.1%–16.6%) of study population were seropositive (IgG levels ⩾40 IU/ml). The most increased seropositivity rate (21.8%; 95% CI 10.9%–32.7%) was observed among children aged 3–5 years. This is likely due to the persisting vaccine-acquired immunity, that still be observed within 3 years from the last vaccination dose [18, 21]. Increased anti-PT IgG levels have been observed in countries using the acellular vaccine, including the Netherlands [22] and Germany [13]. Moreover, it has been reported that DTwP primed-children are better protected against pertussis than DTaP primed adolescents [23].
Our results confirmed an overall significant increase in titres according to female and age categories 3–5 years and 13–18 years. However, associations of following variables: delay, sibling ⩽5 years and prolonged cough were not significant. In fact, data from seroprevalence studies suggest that re-exposure to B. pertussis can boost antibody titres, without developing clinical symptoms or causing a transmissible infection. Therefore, prolonged cough was not a significantly associate variable [24].
Besides, the results of age stratified Poisson regression analysis revealed that the coefficient for delay × age group 3–5 years is positive, suggesting an increase in titres as time progressed (Table 4). However, the coefficient for delay × age group 13–18 years was negative meaning a temporal decline in titres for participants aged 13–18 years, suggesting that those adolescents played a disproportionate role in propagating the epidemic. The latter would be consistent with previous studies [25, 26]. Besides, various models studying the immune response to B. pertussis infection provided evidence that secondary exposure is less likely to boost immunity than primary exposure, given equal levels of contact with B. pertussis. Moreover, immunity to pertussis wanes before re-exposure occurs, because of low pathogen circulation [24] (Table 4).
Table 4.
Stratified analysis of changes in anti-PT IgG titres during the outbreak and time between patients' investigation and outbreak starting – Poisson regression model
| Factors | Coefficient (95% CI) | p value | |
|---|---|---|---|
| Delay | Age group 3–5 years | 0.0168 (0.0108–0.0227) | <0.0001 |
| Age group 6–12 years | 0.0026 (−0.0024 to 0.0076) | 0.3149 | |
| Age group 13–18 years | −0.0143 (−0.0218 to −0.0069) | 0.0002 |
Delay = time between patients' investigation and outbreak starting.
Children and adolescents represent a potential source of infection of infants and toddlers around them. Given the fact that Tunisia is a high vaccine coverage country [27], pertussis occurrence among this age category is likely due to waning immunity after both vaccination and infection [12]. Therefore, increased awareness of medical community is required to involve the differential diagnosis of chronic cough caused by pertussis disease and treat it with macrolides. Besides, introducing a booster dose for Tunisian school children would be efficient to strengthen their immunity and protect new-borns and infants too young to be fully vaccinated.
Waning of vaccine-acquired immunity could be rectifiable by booster vaccination with less reactogenic aP-containing vaccines [28]. The Global Pertussis Initiative recommends booster vaccination of persons at risk, including school entrants and adolescents based on available logistics, resources and access to aP vaccines [29]. In Tunisia, booster vaccination is not logistically feasible in the absence of TdaP (tetanus-diphtheriae-acellular pertussis) vaccine. Therefore, it would be suitable to consider introducing it in our country, where pertussis is occurring in infants and children in epidemiologic waves [10].
Our study presents preliminary results about pertussis seroprevalence in a cohort of Tunisian children and adolescents during the second quarter of 2018. Nevertheless, it has some limitations. Sampling was based on population attending a university paediatric hospital. Therefore, the results may not represent the whole population. However, they are consistent with seroepidemiological studies performed elsewhere. Moreover, enrolled participants were asymptomatic and had no current respiratory infectious disease to avoid bias. Another limitation was the small study population. Therefore, further serosurveys with larger populations are required to better estimate the optimal age for booster vaccination and adapt the national vaccination schedule.
Conclusions
The evidence of pertussis infection in Tunisian school children and adolescents confirms the rapid decline of wP vaccine-acquired immunity and highlights the importance of increased awareness among medical community about this disease. Given the fact that high-school children aged 13–18 years had a higher attack rate during the pertussis epidemic, a TdaP booster dose would be suitable to reinforce their immunity and protect young infants, for whom pertussis could be deadly.
Acknowledgements
The authors would like to thank Dr Nicole Guiso for her valuable comments. We also thank all participants for their contribution in this study.
Conflict of interest
None.
Author ORCIDs
I. Ben Fraj, 0000-0001-7837-7391; H. Smaoui, 0000-0002-4026-0259.
Author contributions
IBF, AK and HS contributed to the study design. MZ collected specimens and performed experiments. IBF analysed generated data and wrote the manuscript. HS gave critical comments on the manuscript. All authors read and approved the final manuscript.
Financial support
This research received no specific grant from any funding agency, commercial or not-for-profit sectors.
Ethical standards
The authors assert that all procedures contributing to this work comply with the ethical standards of the Helsinki Declaration of 1975, as revised in 2008. The study was approved by the Ethics Committee of the Children's Hospital of Tunis (Reference no. 05/2018) and written informed consent was obtained from each participant or tutor.
References
- 1.Guiso N (2015) Chapter 85 – Bordetella pertussis In Tang Y-W et al. (eds), Molecular Medical Microbiology, 2nd Edn. Boston: Academic Press, pp. 1507–1527. [Google Scholar]
- 2.Bisgard KM et al. (2004) Infant pertussis: who was the source? The Pediatric Infectious Disease Journal 23, 985–989. [DOI] [PubMed] [Google Scholar]
- 3.Tozzi AE et al. (2005) Diagnosis and management of pertussis. CMAJ: Canadian Medical Association Journal 172, 509–515. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Bouziri A et al. (2010) Malignant pertussis: an underdiagnosed illness. Medecine Tropicale: Revue Du Corps De Sante Colonial 70, 245–248. [PubMed] [Google Scholar]
- 5.Zepp F et al. (2011) Rationale for pertussis booster vaccination throughout life in Europe. The Lancet. Infectious Diseases 11, 557–570. [DOI] [PubMed] [Google Scholar]
- 6.Zouari A et al. (2011) The new health legacy: when pertussis becomes a heritage transmitted from mothers to infants. Journal of Medical Microbiology 60, 1546–1549. [DOI] [PubMed] [Google Scholar]
- 7.Cherry JD (2013) Pertussis: challenges today and for the future. PLoS Pathogens 9, e1003418. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Ministry of Health (2014) National Immunization Program, Tunisia. Available at http://www.santetunisie.rns.tn/images/articles/calend-vaccination2014.pdf (Accessed 17 March 2018).
- 9.Zouari A et al. (2012) Prevalence of Bordetella pertussis and Bordetella parapertussis infections in Tunisian hospitalized infants: results of a 4-year prospective study. Diagnostic Microbiology and Infectious Disease 72, 303–317. [DOI] [PubMed] [Google Scholar]
- 10.Ben Fraj I et al. (2019) Pertussis epidemiology in Tunisian infants and children and characterization of Bordetella pertussis isolates: results of a 9-year surveillance study, 2007 to 2016. Journal of Medical Microbiology 68, 241–247. [DOI] [PubMed] [Google Scholar]
- 11.Ben Fraj I et al. (2019) Seroprevalence of pertussis among healthcare workers: a cross-sectional study from Tunisia. Vaccine 37, 109–112. [DOI] [PubMed] [Google Scholar]
- 12.Cutts FT and Hanson M (2016) Seroepidemiology: an underused tool for designing and monitoring vaccination programmes in low- and middle-income countries. Tropical Medicine & International Health 21, 1086–1098. [DOI] [PubMed] [Google Scholar]
- 13.Kennerknecht N et al. (2018) Pertussis surveillance by small serosurveys of blood donors. Epidemiology and Infection 146, 1807–1810. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.de Greeff SC et al. (2008) Impact of acellular pertussis preschool booster vaccination on disease burden of pertussis in The Netherlands. The Pediatric Infectious Disease Journal 27, 218. [DOI] [PubMed] [Google Scholar]
- 15.Barkoff A-M, Gröndahl-Yli-Hannuksela K and He Q (2015) Seroprevalence studies of pertussis: what have we learned from different immunized populations. Pathogens and Disease 73, ftv050. [DOI] [PubMed] [Google Scholar]
- 16.Guiso N et al. (2011) What to do and what not to do in serological diagnosis of pertussis: recommendations from EU reference laboratories. European Journal of Clinical Microbiology & Infectious Diseases 30, 307–312. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.Mattoo S and Cherry JD (2005) Molecular pathogenesis, epidemiology, and clinical manifestations of respiratory infections due to Bordetella pertussis and other Bordetella subspecies. Clinical Microbiology Reviews 18, 326–382. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Schwartz KL et al. (2016) Effectiveness of pertussis vaccination and duration of immunity. CMAJ: Canadian Medical Association Journal 188, E399–E406. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Cevik M et al. (2008) Seroprevalence of IgG antibodies against Bordetella pertussis in healthy individuals aged 4–24 years in Turkey. Clinical Microbiology and Infection 14, 388–390. [DOI] [PubMed] [Google Scholar]
- 20.Wang C-Q and Zhu Q-R (2011) Seroprevalence of Bordetella pertussis antibody in children and adolescents in China. The Pediatric Infectious Disease Journal 30, 593–596. [DOI] [PubMed] [Google Scholar]
- 21.Wendelboe AM et al. (2005) Duration of immunity against pertussis after natural infection or vaccination. The Pediatric Infectious Disease Journal 24, S58–S61. [DOI] [PubMed] [Google Scholar]
- 22.de Greeff SC et al. (2010) Seroprevalence of pertussis in the Netherlands: evidence for increased circulation of Bordetella pertussis. PLoS ONE 5, e14183. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.van der Lee S et al. (2018) Whole-cell or acellular pertussis primary immunizations in infancy determines adolescent cellular immune profiles. Frontiers in Immunology 9, 51. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.Lavine JS, King AA and Bjornstad ON (2011) Natural immune boosting in pertussis dynamics and the potential for long-term vaccine failure. Proceedings of the National Academy of Sciences 108, 7259–7264. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25.Mahmud A, Lipsitch M and Goldstein E (2018) On the role of different age groups during pertussis epidemics in California, 2010 and 2014. bioRxiv. Available at 10.1101/405076 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26.Goldstein E, Worby CJ and Lipsitch M (2018) On the role of different age groups and pertussis vaccines during the 2012 outbreak in Wisconsin. Open Forum Infectious Diseases 5, ofy082. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 27.World Health Organization (2016) WHO and UNICEF estimates of immunization coverage, Tunisia: 2016 revision. Available at https://data.unicef.org/wp-content/uploads/country_profiles/Tunisia/immunization_country_profiles/immunization_tun.pdf) (Accessed 28 April 2018).
- 28.World Health Organization (2016) Pertussis vaccines: WHO position paper, August 2015 – Recommendations. Vaccine 34, 1423–1425. [DOI] [PubMed] [Google Scholar]
- 29.Muloiwa R, et al. (2018) Pertussis in Africa: Findings and recommendations of the Global Pertussis Initiative (GPI). Vaccine 36, 2385–2393. [DOI] [PubMed] [Google Scholar]