Abstract
Background. Because failed trial of labor after cesarean (TOLAC) is associated with greater morbidity than planned cesarean, it is important to distinguish women with a high likelihood of successful vaginal birth after cesarean (VBAC) from those likely to fail. The VBAC Calculator may help make this distinction but little is known about how often providers use it; nor whether use improves risk estimation and/or influences TOLAC counseling. Methods. In a cross-sectional survey, a convenience sample of obstetrical providers reported their likelihood (4-point Likert-type scale) to “Recommend,”“Offer,” or “Agree to” TOLAC for patients presented first through five clinical vignettes; then, in different order, by corresponding VBAC calculator estimates. Results. Of the 85 (of 101, 84% response rate) participants, 88% routinely performed TOLAC, but only 21% used the Calculator. The majority (67.1% to 89.3%) overestimated the likelihood of success for all but one vignette (which had the highest estimate of success). Most providers (42% to 89%) recommended TOLAC for all five vignettes. Given calculated estimates, the majority of providers (67% to 95%) recommended TOLAC for success estimates exceeding 40%. For estimates between 20% and 40%, most providers offered (58%) or agreed (68%) to TOLAC; and even below 20%, over half still agreed to TOLAC. The vignette with the lowest estimate of success (18.7%) had the weakest intraprovider agreement (kappa = 0.116; confidence interval [CI] = 0.045–0.187), whereas the strongest agreement was found in the two vignettes with highest success estimates: 77.9% (kappa = 0.549; CI = 0.382–0.716) and 96.6% (kappa = 0.527; CI = 0.284–0.770). Limitations. Survey responses may not reflect actual practice patterns. Conclusion. Providers are overly optimistic in their clinical estimation of VBAC success. Wider use of decision support could aid in risk stratification and TOLAC counseling to reduce patient morbidity.
Keywords: TOLAC, VBAC, risk estimation, obstetrics
Introduction
There has been a marked increase in the overall cesarean delivery rate in the United States, which rose from 22.7% in 1990 to 32.7% in 2013.1 This rise correlates to an increased number of patients eligible for a trial of labor after cesarean (TOLAC) and the potential for a successful vaginal birth after cesarean (VBAC).2 In ongoing efforts to reduce the rise of cesarean delivery and minimize complications related to repeated cesarean delivery, the American College of Obstetricians and Gynecologists (ACOG) recommends that “most women with one previous cesarean delivery with a low transverse incision are candidates for and should be counseled about VBAC and offered TOLAC.”3 However, it does not provide a guideline to adequately convey risks and benefits of TOLAC versus ERCD (elective repeat cesarean delivery); nor to adequately assess risk factors when counseling patients on the safest mode of delivery.
In an effort to improve counseling and clinical decision making, the VBAC Risk Calculator was developed based on a population of women who received care from hospitals within the Maternal-Fetal Medicine Units Network.4 The online tool can help providers predict the likelihood of a successful VBAC based on the presence or absence of clinical characteristics associated with increased risk of failed TOLAC, including advancing maternal age, high pre-pregnancy body mass index, non-white race, no history of prior vaginal delivery or VBAC, and history of arrest disorder.5,6 The calculator offers providers an objective estimate of a patient’s chance of having a successful vaginal delivery based on these clinical characteristics. Identifying patients likely to succeed in their trial of labor can help providers appropriately counsel patients after cesarean delivery. In particular, the calculator can potentially be used to minimize morbidity associated with TOLAC, because a failed trial of labor that results in an unplanned cesarean delivery is even more morbid than a planned cesarean.3
Unfortunately, little is known about whether and how physicians use the VBAC calculator and the extent to which they incorporate its calculated predictions into their clinical decision making and counseling.7 Additionally, it remains unclear if a provider’s recommendation for TOLAC is influenced by the calculated estimate of success versus their perceived chance of success based on clinical characteristics alone. As an initial step toward filling the gaps in our knowledge about the calculator’s effects on provider decision making, we conducted a study to explore 1) how prevalent knowledge and use of the VBAC calculator are among providers; 2) how closely providers’ estimates of VBAC success based on clinical characteristics (vignettes) align with estimates calculated by the VBAC calculator; and 3) whether provider’s recommendations for TOLAC differ when providers make recommendations based on clinical characteristics versus calculated estimates for VBAC success.
Methods
Study Population
With approval from the Indiana University Institutional Review Board, we conducted a cross-sectional survey of providers attending the Indiana ACOG Section Meeting. For the purpose of this survey, we defined the term “provider” as any individual that counsels patients regarding VBAC, including certified nurse midwives, nurse practitioners, medical residents, and staff physicians. The study population was recruited as a cross-sectional, convenience sample. We distributed a paper-based survey to physicians and midlevel providers attending a state medical society (IN Section Meeting). Surveys were placed in the registration packet/program for all eligible attendees and returned to the research team at the registration table on completion. The survey was conducted anonymously. Participation was voluntary. No financial remuneration was provided.
Survey Development
After review of the literature, a four-page VBAC Counseling Survey was developed that included five clinical case vignettes, items soliciting provider’s opinions and preferences regarding TOLAC counseling, and a demographic questionnaire (see Online Appendix). Each vignette described a pregnant patient presenting for VBAC consultation with a history that included varying potential risk factors known to influence VBAC success rates and TOLAC counseling, specifically maternal age, pre-pregnancy body mass index, race, history of prior vaginal delivery or VBAC, or arrest of dilation. Each of the five vignettes was designed to correspond to an escalating chance of VBAC success based on the calculators’ estimation. The demographic questionnaire queried providers’ practice characteristics (practice setting, practice model, institutional TOLAC policy, [sub]specialty, and resident supervision) and personal characteristics (age, gender, race/ethnicity, and number of years out of training).
Study Measures
The survey was divided into series 1 and 2, and each provider completed both series. In series 1, providers were asked to read five clinical vignettes and then rate their likelihood to 1) offer TOLAC, 2) recommend TOLAC, and 3) agree to TOLAC (if requested by the patient) using a 4-point Likert-type scale ranging from 1 to 4, with 1 corresponding to “Definitely Would Not” and 4 corresponding to “Definitely Would.” Providers were then presented with an ordinal option set and asked to predict the patient’s likelihood of successful VBAC using the following percent ranges: 0% to 20%, 20% to 40%, 40% to 60%, 60% to 80%, and 80% to 100%. Additionally, providers were asked what, if any, additional information they would have liked to inform their management plan. Finally, providers were asked to report their current knowledge and use of the VBAC calculator in their clinical practice.
In series 2, providers were given the five different calculated estimates of VBAC success for each of the five vignettes, but without the clinical vignettes. Again, they were asked to rate their probability to offer, recommend, and agree to TOLAC using the same Likert-type scale for a patient with each calculated estimate of success. Providers were unaware that each calculated estimate generated by the VBAC calculator tool corresponded to one of the five previous clinical vignettes that they reviewed in series 1. Additionally, the calculated estimates were provided in a different order than their corresponding clinical vignettes.
Statistical Methods
Sociodemographic characteristics from the provider survey, providers knowledge and use of the VBAC calculator, and the providers’ perceived likelihood of success for each vignette (which was obtained as a categorical outcome: 0% to 20%, 20% to 40%, 40% to 60%, 60% to 80%, and 80% to 100%) are summarized with frequency and percent. The providers’ perceived likelihood of success for all five clinical vignettes in series 1 were categorized as either “overestimated, correct, or underestimated” based on the corresponding estimate computed by the VBAC calculator and descriptive statistics of frequency and percent are provided.
To further describe how clinical decision making and counseling would be affected if providers used the VBAC calculated chance of success rather than their perceived likelihood of success, the 4-point Likert-type items were dichotomized into “Would” (Probably Would or Definitely Would) or “Would not” (Probably Would Not or Definitely Would Not) recommend, offer, or agree to a TOLAC, and the percentage of providers in each category were calculated for both the clinical vignette (series 1) and the corresponding calculated chance of success item (series 2).
To assess agreement between each provider’s response on how likely they would be to offer, recommend, or agree to TOLAC based on the clinical vignette and the providers’ response to the same question when only provided the estimate of success from the VBAC calculator, a weighted kappa and associated 95% confidence interval was estimated.8 The weighted kappa weights categories closer together as in more agreement than categories farther apart. The P-value reported corresponds to the hypothesis that the weighted kappa = 0. A weighted kappa of zero corresponds to no agreement beyond that expected by chance.
Results
One hundred and one provider surveys were distributed and 85 were completed (completion rate = 84%). Table 1 provides the sociodemographic and categorical breakdown of the providers surveyed. Of those surveyed, 62.7% practice general obstetrics and 39.5% have been out of training for less than 5 years. Despite 97.6% of providers reporting that TOLAC is permitted at their institution, only 88% routinely perform TOLAC in their practice. Thirty-four percent of providers were aware that the VBAC calculator exists, and 21% reported they had used it in their clinical practice.
Table 1.
Demographic Survey Data (N = 85)
| Characteristic | n (%) |
|---|---|
| Gender | |
| Female | 52 (65%) |
| Male | 28 (35%) |
| Years out of training | |
| <5 | 32 (39.5%) |
| 5–9 | 5 (6.2%) |
| 10–20 | 17 (21%) |
| >20 | 27 (33.3%) |
| Primary specialty | |
| General OB-GYN | 52 (62.7%) |
| MFM | 1 (1.2%) |
| Midwife | 3 (3.6%) |
| NP | 2 (2.4%) |
| OB resident | 21 (25.3%) |
| Other | 4 (4.8%) |
| Current practice | |
| Solo | 11 (17.5%) |
| Group | 32 (50.8%) |
| Multispecialty | 5 (7.9%) |
| University | 10 (15.9%) |
| Other | 5 (7.9%) |
| Location of practice | |
| Urban, inner city | 27 (33.8%) |
| Urban, non-inner city | 24 (30%) |
| Suburban | 22 (27.5%) |
| Rural, town of 50,000 or less | 6 (7.5%) |
| Other | 1 (1.3%) |
| Race/ethnicity | |
| White/Caucasian | 61 (71.7%) |
| Black/African American | 7 (8.2%) |
| Asian | 5 (5.9%) |
| American Indian/Alaskan Native | 1 (1.2%) |
| Biracial/Multiracial | 2 (2.4%) |
| Other | 3 (3.5%) |
| TOLAC permitted at institution? | |
| Yes | 82 (97.6%) |
| No | 2 (2.4%) |
| Provider offers TOLAC in practice | |
| Yes | 73 (88%) |
| No | 10 (12%) |
TOLAC, trial of labor after cesarean.
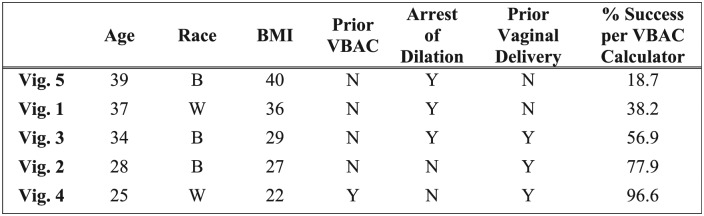
The pertinent clinical characteristics for each clinical vignette (Figure 1), which impact the likelihood of successful VBAC as determined by the VBAC calculator, is displayed in Table 2. Providers’ perceived likelihood of success was overly optimistic as providers overestimated the patient’s likelihood of successful VBAC for each clinical scenario except vignette 4, which had the highest likelihood of success, and therefore, could not be “overestimated” (Table 2). For this scenario 68.2% of providers answered correctly and 31.8% underestimated. For the other scenarios, the percent of providers who correctly estimated the likelihood of success ranged from 10.7% to 31.8%, increasing as the VBAC calculated likelihood of success increased, while the percent of providers who overestimated ranged from 67.1% to 89.3%.
Figure 1.
Vignette clinical characteristics.
Each vignette included varying risk factors that could potentially influence the patient’s VBAC success and were arranged to correspond to an escalating chance of success based on the calculators’ estimation.
Table 2.
Provider Predictionsa
| Vignette | VBAC Calculator Estimate of Success (%) | Provider’s Perceived Likelihood of Success | N (%) | Overestimated (%) | Correct (%) | Underestimated (%) |
|---|---|---|---|---|---|---|
| 5 | 18.7 | 0-20% | 9 (10.7) | 89.3 | 10.7 | 0 |
| 21-40% | 29 (34.5) | |||||
| 41-60% | 28 (33.3) | |||||
| 61-80% | 15 (17.9) | |||||
| 81-100% | 3 (3.6) | |||||
| ** | ||||||
| 1 | 38.2 | 0-20% | 5 (6.0) | 67.9 | 26.2 | 6.0 |
| 21-40% | 22 (26.2) | |||||
| 41-60% | 31 (36.9) | |||||
| 61-80% | 24 (28.6) | |||||
| 81-100% | 2 (2.4) | |||||
| ** | ||||||
| 3 | 56.9 | 0-20% | 0 | 67.5 | 28.9 | 3.6 |
| 21-40% | 3 (3.6) | |||||
| 41-60% | 24 (28.9) | |||||
| 61-80% | 40 (48.2) | |||||
| 81-100% | 16 (19.3) | |||||
| *** | ||||||
| 2 | 77.9 | 0-20% | 0 | 67.1 | 31.8 | 1.2 |
| 21-40% | 0 | |||||
| 41-60% | 1 (1.2) | |||||
| 61-80% | 27 (31.8) | |||||
| 81-100% | 57 (67.0) | |||||
| * | ||||||
| 4 | 96.6 | 0-20% | 0 | 0 | 68.2 | 31.8 |
| 21-40% | 0 | |||||
| 41-60% | 4 (4.7) | |||||
| 61-80% | 23 (27.1) | |||||
| 81-100% | 58 (68.2) | |||||
| * |
Percentages were calculated based on the number of item respondents rather than the total N of 85.
Number of missing respondents = 0.
Number of missing respondents = 1.
Number of missing respondents = 2.
Based on the percentage of providers who would recommend, offer, or agree to TOLAC for both the clinical vignette (series 1) and the calculated chance of success item (series 2) (see Table 3), the willingness of providers to recommend, offer, and agree to a TOLAC tended to increase as the calculator prediction values increased. Based on clinical characteristics alone, recommendations for TOLAC were high for all scenarios, ranging from 42% to 89%. Indeed, for all vignettes except the vignette corresponding to the very lowest likelihood of success (18.7%), the majority of providers were willing to recommend, offer, or agree to a TOLAC. Given calculated likelihoods of success, the majority, though unwilling to recommend TOLAC for the estimates of less than 40% success, were still willing to offer and agree to TOLAC. There was, however, a significant discrepancy between provider responses in series 1 and series 2 when the VBAC calculator estimate fell below 40%. In fact, 41.7% of providers were willing to recommend a TOLAC in clinical vignette 5 based on clinical characteristics alone; however, when providers were given only the corresponding VBAC calculator estimate (18.7% success) in series 2, only 3.61% of providers were willing to recommend a TOLAC. Notably, even with less than 20% chance of success, most providers (53%) would agree to TOLAC though most would not recommend or offer it.
Table 3.
Provider TOLAC Recommendations
| Vignette 5 | Question 12 | Vignette 1 | Question 11 | Vignette 3 | Question 10 | Vignette 2 | Question 9 | Vignette 4 | Question 8 | |
|---|---|---|---|---|---|---|---|---|---|---|
| VBAC calculator estimate | 18.7% | 38.2% | 56.9% | 77.9% | 96.6% | |||||
| Recommenda | 41.7 | 3.61 | 61.2 | 20.5 | 84.7 | 66.7 | 92.9 | 92.9 | 89.4 | 95.3 |
| Offera | 76.2 | 37.6 | 89.4 | 57.8 | 95.3 | 85.4 | 97.6 | 97.6 | 96.5 | 97.6 |
| Agreea | 84.7 | 53.6 | 94.0 | 67.5 | 96.5 | 91.1 | 96.4 | 97.6 | 95.2 | 97.6 |
TOLAC, trial of labor after cesarean.
Probably Would or Definitely Would.
Based on the weighted Kappa, across all vignettes, agreement between providers’ responses to whether they would recommend, offer, or agree to TOLAC based on clinical vignette and the corresponding response based on calculated likelihood of success was significantly better than chance (P < 0.05, Table 4). However, agreement ranged from poor to moderate with kappa coefficients ranging from 0.116 to 0.549. The weakest agreement was seen in provider willingness to recommend a TOLAC in the vignette with the lowest chance of success (18.7% success) with a kappa of 0.116 (confidence interval [CI] = 0.045-0.187). Whereas the strongest intraprovider agreement was demonstrated in provider willingness to recommend a TOLAC in vignettes 2 and 4 (corresponding to a likelihood of successful VBAC of 77.9% and 96.6%, respectively) with a kappa score of 0.549 (CI = 0.382-0.716) and 0.527 (CI = 0.284-0.770), respectively.
Table 4.
Agreement Between Provider Responses Based on Clinical Vignette and Calculated Chance of Success From VBAC Calculator (Weighted Kappa)
| Vignette | True Calculated Chance of Successa | In Counseling This Patient, How Likely Would You Be To: | Kappab | 95% CI | P Valuec |
|---|---|---|---|---|---|
| Offer TOLAC | 0.283 | [0.174, 0.391] | <0.0001 | ||
| 5 | 18.7% | Recommend TOLAC | 0.116 | [0.045, 0.187] | 0.001 |
| Agree to TOLAC | 0.288 | [0.163, 0.413] | <0.0001 | ||
| Offer TOLAC | 0.343 | [0.226, 0.461] | <0.0001 | ||
| 1 | 38.2% | Recommend TOLAC | 0.260 | [0.130, 0.389] | <0.0001 |
| Agree to TOLAC | 0.320 | [0.196, 0.444] | <0.0001 | ||
| Offer TOLAC | 0.429 | [0.276, 0.583] | <0.0001 | ||
| 3 | 56.9% | Recommend TOLAC | 0.343 | [0.197, 0.489] | <0.0001 |
| Agree to TOLAC | 0.371 | [0.201, 0.541] | <0.0001 | ||
| Offer TOLAC | 0.269 | [0.072, 0.466] | 0.0004 | ||
| 2 | 77.9% | Recommend TOLAC | 0.549 | [0.382, 0.716] | <0.0001 |
| Agree to TOLAC | 0.424 | [0.131, 0.718] | <0.0001 | ||
| Offer TOLAC | 0.425 | [0.112, 0.732] | <0.0001 | ||
| 96.6% | Recommend TOLAC | 0.527 | [0.284, 0.770] | <0.0001 | |
| Agree to TOLAC | 0.526 | [0.144, 0.908] | <0.0001 |
CI, confidence interval; TOLAC, trial of labor after cesarean; VBAC, vaginal birth after cesarean.
Obtained from VBAC calculator.
Interpretation of Kappa strength of agreement: 0.01 to 0.20 Poor; 0.21 to 0.40 Fair; 0.41 to 0.60 Moderate; 0.61 to 0.80 Substantial; 0.81 to 1.00 Almost perfect.
Test of H0: Weighted Kappa = 0.
Discussion
We set out to determine if providers’ estimates of the likelihood of successful VBAC based on clinical characteristics was similar to estimates obtained from the VBAC calculator, and whether provider counseling practices would differ based on VBAC calculator predictions as compared to the providers’ perceived likelihood of success based on clinical characteristics. Overall, we found that providers were unable to accurately estimate a patient’s calculated likelihood of successful VBAC when provided the clinical characteristics. In fact, as compared to the calculator, the majority of providers grossly overestimated the likelihood of successful VBAC in each clinical vignette. When provided calculated estimates of success, as long as the calculated estimate was above 40%, the vast majority of providers would recommend, offer, and agree to TOLAC; at 40% most did not recommend, but would offer or agree to TOLAC; and at lower than 20%, most would not recommend or offer TOLAC, but more than half would still agree to a patient’s request. With the exception of the two clinical vignettes in which patients had over a 75% chance of successful VBAC, physician counseling practices varied significantly when based on clinical characteristics compared to calculated predictions of VBAC success.
While discussions surrounding the option of VBAC versus ERCD have improved,9 discussions surrounding the potential failure of a TOLAC may be lacking. Our findings support prior study findings that suggest that obstetrical providers are poor at gauging risk in TOLAC counseling. According to a report from ACOG fellows, only 61% are proficient in identifying which patients have a high likelihood of successful VBAC.9 This is a cause for concern if by overestimating the likelihood for a successful VBAC, we potentially place patients at an increased risk for morbidity. In particular, “Women with a failed trial of labor had an increased rate of chorioamnionitis, postpartum hemorrhage, blood transfusion, uterine rupture, and hysterectomy.”10 Additionally, after a failed trial of labor, neonates have a higher incidence of neonatal jaundice, sepsis, low Apgar scores, birth trauma, and neonatal intensive care admissions over 24 hours. Furthermore, though it is estimated that among the third of women who choose a TOLAC, two thirds will achieve a successful VBAC,11 given the growing obesity epidemic and aging maternity population, relying on this 2/3 success rate for “all comers” as a rule of thumb puts providers at risk of overestimating success for growing segments of the obstetrical population.11 Use of decision support tools could aid physicians in accurately identify individuals at higher risk of failed trial of labor to counsel them appropriately.
There have been a number of decision aids developed in recent years as the health care community attempts to improve shared clinical decision making in obstetrical care.12,13 Currently, the majority of decision aids are targeted toward women in order to help them clarify their values and make informed decisions. In fact, a recent study conducted in southwest England and Scotland reported that decisions aids helped women cope with the uncertainties of labor and delivery by increasing their knowledge without increasing their anxiety about the situation.11 However, patient decision aids do little to help providers determine whether a recommendation should be made for or against TOLAC. Development and dissemination of additional decision support targeting providers, such as the VBAC calculator, could have important clinical implications. Given the increased risk for the morbidity associated with a failed TOLAC,3 if the likelihood of TOLAC failure is high, it could be argued that the provider has an obligation to recommend against (or potentially “nudge” women away from) TOLAC, rather than approaching the decision as a “shared decision” for which there is “no right answer.” This does not eliminate patient preference and patient autonomy; nor does it mean that patients who value the experience of a TOLAC cannot still pursue it. It simply raises the question regarding the ethical and professional obligations of providers with regard to recommending and/or offering a potentially more morbid course of care.
As a survey-based study, several limitations should be considered when interpreting our findings. For instance, due to the small sample size the generalizability of this study may be limited. Additionally, the surveys were collected as a convenience sample of providers attending an ACOG district meeting and may not be representative of obstetrical providers nationally. This study was regionally limited and practice patterns may differ substantially depending on the availability of in-house anesthesia and hospital policy. We recognize that attendees of a professional meeting, by virtue of their involvement in their professional organization, may be more knowledgeable about current clinical guidelines, evidence-based practices, and available resources. Additionally, we acknowledge that the survey did not evaluate actual provider practice patterns, and their responses regarding potential behavior in vignette-based cases may not reflect their response in actual clinical scenarios. There is an artificial distinction created by asking providers to make a clinical judgment based solely on a number. In actual practice, the number provided by the calculator would always be used or viewed in concert with the rest of the clinical picture. However, due to a concern for a participant fatigue, the survey did not include a “series 3” that presented providers with both the clinical characteristics and likelihood of success for comparison. Additionally, our Likert-type scale response set failed to include an “I don’t know” option, which may have contributed to potential participant nonresponse if they were unsure. Last, we compare provider estimates with calculated estimates of success, not actual VBAC outcomes. Larger questions regarding the predictive power and accuracy of the VBAC calculator compared to provider’s clinical gestalt were beyond the scope of this project. That said, the tool has been previously studied and validated.14,15 Despite these limitations, this study provides important insight into current provider practice patterns surrounding a patient’s decision to undergo TOLAC and reveals the need for more individualized counseling practices. As we continue to strive to lower cesarean delivery rates, increasing TOLAC will be an important part of the strategy; however, this study helps highlight the need for extra vigilance in distinguishing women with a high likelihood of successful VBAC from those likely to fail their trial of labor.
Future research is needed to further explore physician decision making and counseling when identifying optimal candidates for TOLAC. Because this is a small study of hypothetical patients, future studies of actual VBAC calculator usage and clinical decision making among a larger, more representative population, are needed to understand more about obstetricians’ clinical judgment and practices on a larger scale. Such studies may reveal additional barriers that limit providers’ abilities to successfully incorporate the VBAC calculator into their practice or to recommend and perform TOLAC with eligible patients, and thus, create new educational opportunities to improve their confidence, counseling, and decision making.
Tools such as the VBAC calculator have the potential to play an important role in helping providers risk stratify patients to guide their counseling and recommendations for care. In doing so, providers could have more individualized and tailored discussion of risks and benefits. Of course, while the VBAC calculator can facilitate risk assessment, it is intended to augment, not replace, a provider’s clinical judgement. Likewise, use of a calculator does not negate the importance of taking into account the patient’s values and preferences, specific family dynamics and other medical conditions unique to each encounter. When used appropriately, decision support tools targeting providers may serve an important role in promoting risk reduction and informed decision making.
Supplemental Material
Supplemental material, Impact_of_the_VBAC_Calculator_survey_Appendix_3.22.18.rjf_online_supp for Examining the Impact of the Vaginal Birth After Cesarean Risk Calculator Estimation on Trial of Labor After Cesarean Counseling by Erin Jeffries, Amy Falcone-Wharton, Joanne Daggy and Brownsyne Tucker Edmonds in MDM Policy & Practice
Footnotes
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Authors’ Note: This study was presented at the 2015 American College of Obstetricians and Gynecologists Annual Meeting in San Francisco, California (Abstract #324).
Supplemental Material: Supplementary material for this article is available on the Medical Decision Making Policy & Practice website at https://journals.sagepub.com/home/mpp.
ORCID iD: Brownsyne Tucker Edmonds  https://orcid.org/0000-0003-0023-4440
https://orcid.org/0000-0003-0023-4440
Contributor Information
Erin Jeffries, Department of OB/GYN, Indiana University School of Medicine, Indianapolis, Indiana.
Amy Falcone-Wharton, Department of OB/GYN, Indiana University School of Medicine, Indianapolis, Indiana.
Joanne Daggy, Department of Biostatistics, Indiana University School of Medicine, Indianapolis, Indiana.
Brownsyne Tucker Edmonds, Department of OB/GYN, Indiana University School of Medicine, Indianapolis, Indiana.
References
- 1. Coleman VH, Erickson K, Schulkin J, Zinberg S, Sachs BP. Vaginal birth after cesarean delivery: practice patterns of obstetrician-gynecologists. J Reprod Med. 2005;50(4):261–6. [PubMed] [Google Scholar]
- 2. Armstrong C. ACOG updates recommendations on vaginal birth after previous cesarean delivery. Am Fam Phys. 2011;83(2):215–7. [Google Scholar]
- 3. National Institutes of Health. National Institutes of Health Consensus Development Conference Statement vaginal birth after cesarean: new insights March 8–10, 2010. Semin Perinatol. 2010;34(5):351–65. [DOI] [PubMed] [Google Scholar]
- 4. Grobman WA, Lai Y, Landon MB, et al. National Institute of Child Health and Human Development (NICHD); Maternal-Fetal Medicine Units Network (MFMU). Development of a nomogram for prediction of vaginal birth after cesarean delivery. Obstet Gynecol. 2007;109(4):806–12. [DOI] [PubMed] [Google Scholar]
- 5. Cheng YW, Eden KB, Marshall N, Pereira L, Caughey AB, Guise JM. Delivery after prior cesarean: maternal morbidity and mortality. Clin Perinatol. 2011;38:297–309. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6. Metz TD, Allshouse AA, Faucett AM, Grobman WA. Validation of vaginal birth after cesarean delivery prediction model in women with two prior cesareans. Obstet Gynecol. 2015;125(4):948–52. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7. Rezai S, Labine M, Gottimukkala S, et al. Trial of Labor after Cesarean (TOLAC) for Vaginal Birth after Previous Cesarean Section (VBAC) versus repeat cesarean section: a review. Obstet Gynecol Int J. 2016;4(6):00135. [Google Scholar]
- 8. Landis JR, Koch GG. The measurement of observer agreement for categorical data. Biometrics. 1977;33(1):159–74. [PubMed] [Google Scholar]
- 9. Little MO, Lyerly AD, Mitchell LM, et al. Mode of delivery: toward responsible inclusion of patient preferences. Obstet Gynecol. 2008;112:913–8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10. El-Sayed YY, Watkins MM, Fix M, Druzin ML, Pullen KM, Caughey AB. Perinatal outcomes after successful and failed trials of labor after cesarean delivery. Am J Obstet Gynecol. 2007;196(6):583.e1–e5. [DOI] [PubMed] [Google Scholar]
- 11. Frost J, Shaw A, Montgomery A, Murphy DJ. Women’s views on the use of decision aids for decision making about the method of delivery following a previous caesarean section: qualitative interview study. BJOG. 2009;116(7):896–905. [DOI] [PubMed] [Google Scholar]
- 12. Dugas M, Shorten A, Dubé E, Wassef M, Bujold E, Chaillet N. Decision aid tools to support women’s decision making in pregnancy and birth: a systematic review and meta-analysis. Soc Sci Med. 2012;74(12):1968–78. [DOI] [PubMed] [Google Scholar]
- 13. Vlemmix F, Warendorf J, Rosman A, et al. Decision aids to improve informed decision-making in pregnancy care: a systematic review. BJOG. 2013;120:257–66. [DOI] [PubMed] [Google Scholar]
- 14. Maykin MM, Mularz AJ, Lee LK, Valderramos SG. Validation of a prediction model for vaginal birth after cesarean delivery reveals unexpected success in a diverse American population. AJP Rep. 2017;7(1):e31–e38. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15. Grobman WA, Lai Y, Landon MB, et al. Does information available at admission for delivery improve prediction of vaginal birth after cesarean? Am J Perinatol. 2009;26(10):693–701. [DOI] [PMC free article] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Supplementary Materials
Supplemental material, Impact_of_the_VBAC_Calculator_survey_Appendix_3.22.18.rjf_online_supp for Examining the Impact of the Vaginal Birth After Cesarean Risk Calculator Estimation on Trial of Labor After Cesarean Counseling by Erin Jeffries, Amy Falcone-Wharton, Joanne Daggy and Brownsyne Tucker Edmonds in MDM Policy & Practice