Abstract
Objective:
To evaluate the factors affecting the length of hospital stay (LOS) after percutaneous transhepatic biliary drainage (PTBD).
Methods:
A retrospective review of all patients who had undergone PTBD with or without stenting at a UK specialist centre between 2005 and 2016 was conducted.
Results:
692 patients underwent 1976 procedures over 731 clinical episodes for which, the median age was 65 (range 18–100) years, and the median Charlson Index was 3. PTBD was performed for malignant (n = 563) and benign strictures (n = 60), stones (n = 62), and bile leaks (n = 46). The median LOS was 13 (range 0–157) days, and the median interprocedure duration was 9 (range 0–304) days. The median number of procedures per patient was 2 and the median number of days required to complete a set of procedures for a patient (TBID) ranged from 0 to 557 days, with a median of 16 (interquartile range: 8–32) days. Patients with biliary leak had the highest LOS. Biliary stents were mostly placed at the second stage at a median of 6 (range 0–120) days from the first procedure day. Placement of a biliary stent in the first stage of the procedure was associated with shorter LOS (p < 0.001).
Conclusions:
Biliary stenting at index procedure reduces LOS, although it is not always technically possible. Patients with bile leak managed with PTBD have longer LOS.
Advances in knowledge:
This study provides data which can help in appropriate consenting, better planning, and efficient resource utilization for patients undergoing PTBD.
Introduction
Percutaneous transhepatic biliary drainage and stenting (PTBD) is performed to manage patients with biliary obstruction or leak either as definitive treatment or as a prelude to definitive surgery. In such patients, PTBD is usually performed when endoscopic retrograde cholangiopancreatography1,2 has failed or is not suitable, such as for a proximal (hilar or above) obstruction or when previous gastrointestinal surgery precludes endoscopic access.3 PTBD is usually performed in a stepwise fashion including placement of an external biliary drain, followed by a stent, and finally a check cholangiogram to confirm adequate drainage. In some clinical scenarios such as a suspected palliative malignant biliary obstruction, a temporary plastic stent may be placed in the first instance, which upon histological confirmation and absence of resection options, is exchanged for a permanent metallic stent. In certain instances, the patient is discharged in between each individual procedure. However, if the patient is kept in the hospital during all these procedures because of any reason then it can lead to an extended length of hospital stay (LOS) and substantial economic costs. Accordingly, the LOS for patients undergoing PTBD is higher compared to endoscopic drainage.4
Information about LOS can be very useful for both clinicians and managers for efficient resource utilization. The average LOS for a patient undergoing PTBD varies between 8 and 17 days (Table 1).5–7,10,11 There may be significant differences in patients’ LOS determined by their pathology. A complication of PTBD or logistical delays between each procedure can prolong LOS. The British Society of Interventional Radiology registry pooled data from 44 centres in the UK to evaluate 844 patients who underwent PTBD.9 The study reported average time to stent placement as 14 (range 1–379) days, but there was no evaluation of overall LOS. The US national inpatient database showed a LOS of 10 days (6) but there was no assessment of factors affecting LOS.
Table 1.
Length of stay after biliary intervention
| No. | Study | Year | Number of patients | Time for conversion to stent | Length of stay |
| 1. | Lammer5 | 1996 | 110 | NA | 8 days |
| 2. | Inal6 | 2002 | 126 | 5 days | 12 days |
| 3. | Indar7 | 2003 | 89 | 14 days | 16 days |
| 4. | Robson8 | 2010 | 109 | 33 days | NA |
| 5. | Uberoi9 | 2012 | 833 | 14 days | NA |
| 6. | Teixeira10 | 2013 | 71 | NA | 16.6 days |
| 7. | Inamdar11 | 2016 | 1690 | NA | 10.4 days |
NA, data not available.
There are no data on interprocedure duration (IPD), total biliary intervention duration (TBID) and factors affecting LOS after PTBD. Identification of these factors can help in predicting patients who may have an extended LOS, and patients who can be safely discharged in between their procedure. It can also help in better communication with the patient.
The aim of this study was to evaluate the LOS, IPD, TBID, and factors affecting the LOS after PTBD from a single high-volume UK centre.
Methods and materials
This study was conducted in accordance with STROBE guidelines.12 A retrospective review of all patients who had undergone PTBD with or without biliary stenting at a large UK tertiary hepatobiliary centre between January 2005 and December 2016 was performed. Cases were identified using a prospectively maintained surgical database and cross-verified with data from the picture archiving and communication system. A separate clinical episode was documented if a patient had more than six procedures or the procedure was carried out for a different pathology from the original one. The cut-off for “six procedures” as a separate clinical episode was decided after conducting an initial audit of 200 patients. Most patients (99.7%) had their primary problem managed within six procedures.
Variables and definitions
Patients were stratified according to their comorbidities as per the Charlson comorbidity index, a well-studied determinant of outcomes.13 Reintervention was defined as an unplanned intervention to remedy a complication (e.g. blockage, or migration of drain or stent) from a previous procedure, which may be in the same admission or different admission within 6 months. “Stage of stent placement” was defined by the first procedure where a stent was placed.
The initial (pre-procedure) bilirubin was recorded just before the PTBD. The final (post-procedure) bilirubin level was recorded as the lowest level reached within 3 months of the procedure. The daily diminution of bilirubin was calculated by subtracting the minimum value within 30 days of PTBD from the maximum value just before PTBD and dividing the result by the number of days.
The total LOS was defined as the total number of days a patient stayed in the hospital to undergo the whole set of biliary procedures. LOS was stratified into LOS 1–6 depending upon the number of biliary procedures, and if the patient was discharged in between each procedure. TBID was defined as the total number of days between the first procedure and discharge after the final procedure. TBID was stated as TBID 1–6 depending upon the number of procedures performed. IPD was defined as the time in days between each subsequent biliary procedure. IPD was classified as IPD 1–5. Figure 1 represents a schema for two patients who underwent three biliary procedures. Patient 1 was discharged in between three procedures, whereas Patient 2 was not discharged in between three procedures. LOS, TBID and IPD was calculated accordingly.
Figure 1. .
Schematic representation of LOS, TBID and IPD. Comparison of two patients who have undergone three biliary procedure. IPD, inter procedure duration; LOS, length of hospital stay; TBID, total biliary intervention duration.
Follow-up data were censored at December 2017 allowing time for quality checks.
Data quality and approval
All radiological images were reviewed by an interventional radiologist and a hepatopancreatobiliary surgeon. If there was any doubt, then the images were cross-checked with another senior radiologist. All data were cross-checked by three different authors and finally audited again by the primary author to maintain reliability and consistency. The study was approved by the Barts Health NHS Trust clinical effectiveness unit (clinical audit no: 7740).
Statistical analysis
All analyses were performed using SPSS 23.0 (SPSS Inc., Chicago, IL). Categorical variables were analysed using the χ2 test and the Fisher exact test. Mann–Whitney U test or Kruskal–Wallis test was performed for non-parametric data. All significant variables used in the univariable analysis were used in performing a multivariable analysis. Multivariable analysis of a continuous outcome variable (LOS) was performed by a multiple linear regression model. p-value less than 0.05 was considered significant.
Results
Demographics and diagnosis
A total of 1976 procedures in 692 patients over 731 clinical episodes (361 male, 370 female) were performed over the period (Figure 2a). The median age was 65 (range 18–100) years (average age of 64 ± 15 years) and the median Charlson index was 3. Reasons for performing PTBD included strictures (n = 623, 85%), stones (n = 62, 9%), and leaks (n = 46, 6%) in 731 clinical episodes. Some patients from the pre-procedure malignant group were confirmed to have a benign aetiology upon final histological diagnosis (Figure 2b).
Figure 2. .
Percutaneous biliary data capture. (a) 692 patients who underwent percutaneous biliary intervention between January 2005 December 2016. (b) Categaration of diagnosis into malignant, benign, post-opearative and biliary stone.
Procedure
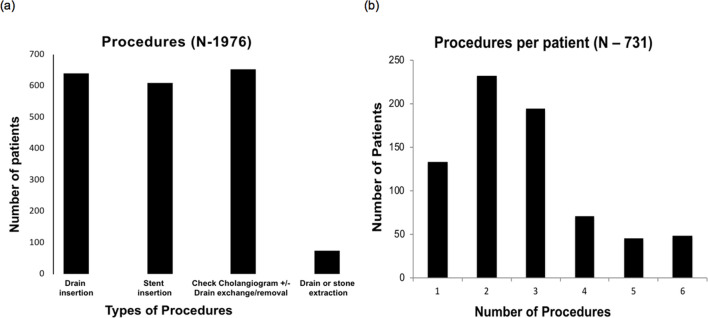
1976 procedures included 609 stent episodes (Figure 3a), with most patients undergoing 2–3 procedures (Figure 3b). Most stents were placed in the second stage of the procedure (Figure 4a, χ 2 = 532.345, df = 5, p < 0.001) at a median of 6 (range: 0–120) days from the first biliary procedure. Initial [167 µmol l–1 (range: 3–1021)] and final [32 µmol l–1 (range: 3–598)] bilirubin levels from 667 patients demonstrated a daily diminution of approximately 8 µmol l–1 day–1 (range: −24–301) (Figure 4b). Bilirubin went up after the procedure in a minor proportion of cases, which caused the negative value. Bilirubin level dropped post procedure in 81.5% of patients.
Figure 3. .
Percutneous biliary procedure. (a) Type of procedures: draininsertion. stent insertion: check cholangiogram ± drain exchange/removal; drain or stone extraction. (b) Procedure per patient.
Figure 4. .
Percetneous biliary intervention outcome. (a) Stent placement in diffrent stages (1–6). “stage of stent placement” was defined by the first procedure where a stent was placed. (b) Clinical outcome measured by initial, final and daily diminution of bilirubin in micromole/litre.
Length of hospital stay (LOS), total biliary intervention duration (TBID) & interprocedure duration (IPD)
LOS, TBID, and IPD are summarized in Figures 5–7 respectively. LOS, ranged from 0 to 157 days, with a median of 13 (interquartile range: 7–24) days. The median number of procedures per patient was 2 and the median number of days required to complete a set of procedures for a patient (TBID) ranged from 0 to 557 days, with a median of 16 (interquartile range: 8–32) days. Total IPD ranged from 0 to 304 days, with a median of 9 (interquartile range: 3–27) days. There was a progressive increase in LOS, IPD and TBID as the number of procedures required increased (Kruskal–Wallis test, p < 0.001).
Figure 5. .

LOS for patients undergoing percutaneous biliary interventions startified according to the number of biliary interventions. LOS, length of hospital stay.
Figure 6. .

TBID representing the total number of days between the first procedure and discharge after the final procedure. TBID, total biliary intervention duration.
Figure 7. .

IPD representing the time period between each procedure. IPD, interprocedure duration.
On univariable analysis, diagnosis (p < 0.001), biliary leak (p < 0.001), reintervention (p < 0.006), placement of stent in the first stage (p < 0.001), IPD (p < 0.001) and final bilirubin level (p = 0.02) were statistically significant in predicting LOS (Table 2). On multivariable analysis using multiple linear regression model, certain diagnoses (p = 0.05), placement of a stent after the first stage (i.e. after the first procedure) (p < 0.001), and long IPD (p < 0.001) were statistically significant in predicting prolonged LOS (Table 2). A break-up of IPD as per different diagnosis shows longest IPD for biliary leak, post-hepaticojejunostomy stricture, and post-cholecystectomy stricture (Table 3).
Table 2.
Univariable and multivariable analysis of factors affecting LOS
| Variable | Groupings (n) | LOS in days median | Univariable p-value | Multivariable p-value |
| Categorical variables | ||||
| Gender | Male (361) | 13 | 0.54 a | |
| Female (370) | 13 | |||
| Age | 20–29 (9) | 13 | 0.76 b | |
| 30–39 (41) | 12 | |||
| 40–49 (80) | 13 | |||
| 50–59 (123) | 13 | |||
| 60–69 (188) | 13 | |||
| 70–79 (202) | 14 | |||
| 80–89 (80) | 11 | |||
| 90–100 (8) | 15 | |||
| Charlson Index | 0 (135) | 14 | 0.32 b | |
| 1 (86) | 16 | |||
| 2 (111) | 14 | |||
| 3 (64) | 12 | |||
| 4 (34) | 14 | |||
| 5 (22) | 14 | |||
| 6 (97) | 19 | |||
| 7 (56) | 10 | |||
| 8 (48) | 13.5 | |||
| 9 (38) | 14 | |||
| 10 (19) | 15 | |||
| 11 (15) | 11 | |||
| 12 (4) | 30 | |||
| 14 (2) | 13 | |||
| Reintervention | Yes (49) | 21 | 0.006 b | 0.79 d |
| No (682) | 13 | |||
| PTBD indications | Obstruction (623) | 13 | <0.001 b | 0.99 d |
| Leak (46) | 23.5 | |||
| Stones (62) | 11 | |||
| Diagnosis category | Malignant (501) | 13 | 0.42 b | |
| Benign (60) | 14 | |||
| Postoperative (108) | 11 | |||
| Common bile duct stone (62) | 14 | |||
| Stent | Stage 1 (179) | 7 | <0.001 b | 0.001 d |
| Stage 2 (235) | 14 | |||
| Stage 3 (80) | 19.5 | |||
| Stage 4 (23) | 32 | |||
| Stage 5 (10) | 32 | |||
| Diagnosis | Post-hepatectomy stricture (4) | 43.5 | <0.001 a | 0.05 d |
| Post-hepatectomy leak (7) | 41 | |||
| Post-hepaticojejunostomy leak (17) | 28 | |||
| Neuroendocrine tumour (6) | 25.5 | |||
| Lymphoma (6) | 25.5 | |||
| Post-cholecystectomy leak (21) | 17 | |||
| Cholangiocarcinoma (166) | 16.5 | |||
| Colorectal liver metastases (23) | 14 | |||
| Benign biliary stricture (60) | 14 | |||
| Pancreatic adenocarcinoma (163) | 11 | |||
| Common bile duct stones (62) | 11 | |||
| Ampullary cancer (13) | 11 | |||
| Post-hepaticojejunostomy stricture (40) | 10.5 | |||
| Metastatic tumour (72) | 10 | |||
| Hepatocellular cancer (5) | 10 | |||
| Post-cholecystectomy stricture (19) | 10 | |||
| Gallbladder cancer (29) | 8 | |||
| Duodenal cancer (18) | 4.5 | |||
| Continuous variables | ||||
| Initial bilirubin | 667 | 0.97 c | ||
| Final bilirubin | 667 | 0.02 c | 0.95 d | |
| IPD | 731 | <0.001 c | <0.001 d | |
IPD, Interprocedure duration; LOS, Length of Stay;PTBD, percutaneous transhepatic biliary drainage;
Values that met the defined p-value of significant p < 0.05 were bolded
Mann–Whitney U test
Kruskal–Wallis test
Linear regression
Multiple Linear regression model
Table 3.
IPD for various diagnosis
| Diagnosis | Median (Range) in days |
| Post hepatectomy leak (7) | 100 (11–304) |
| Post hepatectomy stricture (4) | 62.5 (37–189) |
| Post cholecystectomy leak (21) | 56 (0–169) |
| Post hepaticojejunostomy leak (17) | 50 (0–140) |
| Post hepaticojejunostomy stricture (40) | 39.5 (0–204) |
| Post cholecystectomy stricture (19) | 32 (0–203) |
| Cholangiocarcinoma (166) | 11.5 (0–192) |
| Benign biliary stricture (60) | 11.5 (0–196) |
| Colorectal liver metastases (23) | 10 (0–123) |
| Lymphoma (6) | 9.5 (0–42) |
| Pancreatic adenocarcinoma (163) | 7 (0–179) |
| Gallbladder cancer (29) | 7 (0–139) |
| Duodenal cancer (18) | 6.5 (0–125) |
| Hepatocellular cancer (5) | 6 (3–156) |
| Common bile duct stones (62) | 5 (0–156) |
| Ampullary cancer (13) | 5 (0–28) |
| Metastatic tumor (72) | 4 (0–115) |
| Neuroendocrine tumor (6) | 0.5 (0–5) |
| Total (731) | 9 (0–304) |
Discussion
We present the largest single-centre study, to our knowledge, to evaluate PTBD in a tertiary referral centre, focusing on factors affecting LOS. Recent literature examining LOS after PTBD4,7,8,10,11,14 is limited because of either a small sample size or has focused on a specific subpopulation (usually malignant group), with none evaluating factors determining prolonged LOS. Furthermore, our data on total duration to get completion (TBID) or intervals in between procedures (IPD) are the first ever report for PTBD, an important metric for clinicians and patients. LOS, TBID, and IPD in combination can be useful in better planning and hospital resource utilization. While LOS is important for a physician, TBID can be very useful information from patient’s perspective. IPD can be useful in identification of reasons for delay such as awaiting histology between each procedure or other logistical delays.
The median LOS in our study (13 days) is within the range of other published studies.6,7,10,11 As expected, increased IPD will lead to increased LOS and TBID. Placement of a stent at index procedure, where feasible, reduces the number of procedures and reduces the IPD leading to shorter total LOS and TBID. In a study evaluating benign biliary strictures, patients underwent a mean of 4.3 tube changes during their upsizing treatment, and the mean duration of stent treatment at the maximal tube size was 118 days (median, 103 d; range, 0–336 d) 15 (15). However, unlike our study, this study only evaluated 53 patients with benign strictures who completed the study protocol.
Waiting for the determination of the MDT meeting to guide initial and subsequent interventions, availability of time in the intervention radiology department and waiting for histology are possible reasons for increased IPD. In our institution (The Royal London Hospital), the absence of onsite rapid histological assessment results in delay in obtaining histological diagnosis, a factor which may not affect other institutions. However, histology may be essential in some cases as there may be discrepancy between the radiological diagnosis and post-biopsy diagnosis as demonstrated in our study (2% of the patients under the malignant category shifted to the benign category on final diagnosis). This IPD may be shortened if frozen section is available.
PTBD done for certain diagnosis such as post-hepatectomy leak or post-cholecystectomy leak had a much higher LOS compared to other diagnoses. Since increased IPD was demonstrated to be an important cause for prolonged LOS in biliary leak cases; these patients should be targeted for discharge in between the procedures if their clinical condition improves. The LOS for post-hepatectomy stricture was very high but there were only four patients in that group.
Whilst a single-centre retrospective dataset has its limitations, we have the advantage of reduced cross-centre problems of data harmonization in multi-institutional studies. In addition, the high volume in our centre, and the outcomes being within the acceptable range makes the findings of this study applicable to other high-volume centres. Bilirubin level was not available for every clinical episode because of missing data. Notwithstanding these minor shortcomings, our detailed data set forms a benchmark for future studies aimed at improving resource utilisation.
Conclusions
This data set gives us a broad perspective on the timeline for any patient undergoing PTBD regardless of their diagnosis. Combined information from LOS, TBID, and IPD can help radiologists, surgeons, and hospital managers in planning hospital admission and better resource utilization. Future studies can investigate the time delay between the day an interventional procedure was requested and when it was performed, and the factors predicting safe discharge of patients in between procedures.
Contributor Information
Mayank Roy, Email: mayankroy@hotmail.com.
Jimmy Kyaw Tun, Email: jimmy.kyawtun2@bartshealth.nhs.uk.
Abhirup Banerjee, Email: a.banerjee@qmul.ac.uk.
Shailesh Mohandas, Email: shailesh.mohandas@bartshealth.nhs.uk.
Ajit T Abraham, Email: ajit.abraham@bartshealth.nhs.uk.
Robert R Hutchins, Email: Robert.Hutchins@bartshealth.nhs.uk.
Satyajit Bhattacharya, Email: Satya.bhattacharya@bartshealth.nhs.uk.
Ian Renfrew, Email: ian.renfrew@bartshealth.nhs.uk.
Deborah Low, Email: deborah.low@bartshealth.nhs.uk.
Tim Fotheringham, Email: tim.fotheringham@bartshealth.nhs.uk.
Hemant M Kocher, Email: h.kocher@qmul.ac.uk.
REFERENCES
- 1. Lai EC , Mok FP , Tan ES , Lo CM , Fan ST , You KT , et al. . Endoscopic biliary drainage for severe acute cholangitis . N Engl J Med 1992. ; 326 : 1582 – 6 . doi: 10.1056/NEJM199206113262401 [DOI] [PubMed] [Google Scholar]
- 2. Zhao XQ , Dong JH , Jiang K , Huang XQ , Zhang WZ . Comparison of percutaneous transhepatic biliary drainage and endoscopic biliary drainage in the management of malignant biliary tract obstruction: a meta-analysis . Dig Endosc 2015. ; 27 : 137 – 45 . doi: 10.1111/den.12320 [DOI] [PubMed] [Google Scholar]
- 3. Covey AM , Brown KT . Palliative percutaneous drainage in malignant biliary obstruction. Part 2: Mechanisms and postprocedure management . J Support Oncol 2006. ; 4 : 329 – 35 . [PubMed] [Google Scholar]
- 4. McNabb-Baltar J , Trinh QD , Barkun AN . Biliary drainage method and temporal trends in patients admitted with cholangitis: a national audit . Can J Gastroenterol 2013. ; 27 : 513 – 8 . doi: 10.1155/2013/175143 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5. Lammer J , Hausegger KA , Flückiger F , Winkelbauer FW , Wildling R , Klein GE , et al. . Common bile duct obstruction due to malignancy: treatment with plastic versus metal stents . Radiology 1996. ; 201 : 167 – 72 . doi: 10.1148/radiology.201.1.8816539 [DOI] [PubMed] [Google Scholar]
- 6. Inal M , Akgül E , Aksungur E , Demiryürek H , Yağmur O . Percutaneous self-expandable uncovered metallic stents in malignant biliary obstruction. Complications, follow-up and reintervention in 154 patients . Acta Radiol 2003. ; 44 : 139 – 46 . doi: 10.1034/j.1600-0455.2003.00049.x [DOI] [PubMed] [Google Scholar]
- 7. Indar AA , Lobo DN , Gilliam AD , Gregson R , Davidson I , Whittaker S , et al. . Percutaneous biliary metal wall stenting in malignant obstructive jaundice . Eur J Gastroenterol Hepatol 2003. ; 15 : 915 – 9 . doi: 10.1097/00042737-200308000-00013 [DOI] [PubMed] [Google Scholar]
- 8. Robson PC , Heffernan N , Gonen M , Thornton R , Brody LA , Holmes R , et al. . Prospective study of outcomes after percutaneous biliary drainage for malignant biliary obstruction . Ann Surg Oncol 2010. ; 17 : 2303 – 11 . doi: 10.1245/s10434-010-1045-9 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9. Uberoi R , Das N , Moss J , Robertson I . British Society of Interventional Radiology: Biliary Drainage and Stenting Registry (BDSR . Cardiovasc Intervent Radiol 2012. ; 35 : 127 – 38 . doi: 10.1007/s00270-011-0103-4 [DOI] [PubMed] [Google Scholar]
- 10. Crosara Teixeira M , Mak MP , Marques DF , Capareli F , Carnevale FC , Moreira AM , et al. . Percutaneous transhepatic biliary drainage in patients with advanced solid malignancies: prognostic factors and clinical outcomes . J Gastrointest Cancer 2013. ; 44 : 398 – 403 . doi: 10.1007/s12029-013-9509-3 [DOI] [PubMed] [Google Scholar]
- 11. Inamdar S , Slattery E , Bhalla R , Sejpal DV , Trindade AJ . Comparison of Adverse Events for Endoscopic vs Percutaneous Biliary Drainage in the Treatment of Malignant Biliary Tract Obstruction in an Inpatient National Cohort . JAMA Oncol 2016. ; 2 : 112 – 7 . doi: 10.1001/jamaoncol.2015.3670 [DOI] [PubMed] [Google Scholar]
- 12. von Elm E , Altman DG , Egger M , Pocock SJ , Gøtzsche PC , Vandenbroucke JP , et al. . The Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) statement: guidelines for reporting observational studies . Lancet 2007. ; 370 : 1453 – 7 . doi: 10.1016/S0140-6736(07)61602-X [DOI] [PubMed] [Google Scholar]
- 13. Charlson ME , Pompei P , Ales KL , MacKenzie CR . A new method of classifying prognostic comorbidity in longitudinal studies: development and validation . J Chronic Dis 1987. ; 40 : 373 – 83 . doi: 10.1016/0021-9681(87)90171-8 [DOI] [PubMed] [Google Scholar]
- 14. Paik WH , Park YS , Hwang JH , Lee SH , Yoon CJ , Kang SG , et al. . Palliative treatment with self-expandable metallic stents in patients with advanced type III or IV hilar cholangiocarcinoma: a percutaneous versus endoscopic approach . Gastrointest Endosc 2009. ; 69 : 55 – 62 . doi: 10.1016/j.gie.2008.04.005 [DOI] [PubMed] [Google Scholar]
- 15. DePietro DM , Shlansky-Goldberg RD , Soulen MC , Stavropoulos SW , Mondschein JI , Dagli MS , et al. . Long-term outcomes of a benign biliary stricture protocol . J Vasc Interv Radiol 2015. ; 26 : 1032 – 9 . doi: 10.1016/j.jvir.2015.03.002 [DOI] [PubMed] [Google Scholar]