Abstract
The application of telehealth technology to conduct functional analysis (FA) and functional communication training (FCT) is emerging for children with developmental disabilities and behaviour support needs. The current study was designed to extend FA + FCT for self-injurious behaviour by using telehealth in home with parents as interventionists receiving real-time remote coaching. Two families with school-aged boys with developmental disabilities associated with intellectual disability participated, one with cerebral palsy and the other with autism spectrum disorder. Results indicated that parent-implemented FA + FCT via telehealth was effective for reducing self-injurious behaviour and increasing mands (communication requests) for both children. Both families successfully implemented the FA + FCT protocol with 95% overall fidelity via telehealth-supported coaching. Results are discussed in terms of their relationship to previous research, limitations and future directions.
Keywords: functional analysis, functional communication training, self-injurious behaviour, telehealth
Self-injurious behaviour (SIB) (e.g. hand to head hitting, eye poking and biting oneself) is aheterogenous behavioural disorder that can emerge early in life (e.g. Berkson, Tupa, & Sherman, 2001; Kurtz et al. 2003; Schroeder et al. 2014) and be highly persistent without effective treatment (Baghdadli et al. 2008; Chadwick et al. 2005; Emerson et al. 2001a; Murphy et al. 2005; Taylor, Oliver, & Murphy, 2011). Among individuals with intellectual and developmental disabilities (IDD), total population study SIB estimates range from approximately 4% (Cooper et al. 2009) to 30% (Emerson et al. 2001b). Children who engage in SIB tend to have poorer long-term outcomes in terms of adaptive behaviour (Chadwick et al. 2000), educational and community placements (more restrictive placements) (Emerson, 1990; Oliver et al. 1987; Rojahn et al. 2008) and overall quality of life (Symons et al. 1999). It is imperative that families and children have timely access to effective evidence-based interventions.
Behavioural assessment and treatment of self-injurious behaviour
Structured descriptive assessment (SDA) is a strategy wherein the common antecedents identified as functionally related to challenging behaviour are manipulated with the aim of providing greater depth to descriptive assessments (Anderson & Long, 2002). Functional analysis (FA) methodology (Iwata, Dorsey, Slifer, Bauman, & Richman, 1982/1994) is an experimental assessment approach designed to test social reinforcement contingencies maintaining SIB. Based on social reinforcers identified from an FA, a function-based intervention can be developed. Functional communication training (FCT; Carr & Durand, 1985) is a specific type of function-based intervention in which differential reinforcement is used to teach an appropriate communicative response (e.g. a mand) producing the same functional reinforcer as SIB (Carr & Durand, 1985).
Functional analysis + functional communication training procedures have a strong empirical basis (Iwata et al. 1994). Beavers and colleagues (2013) identified 435 studies using FA with over half of the studies specific to SIB. Similarly, FCT has been reliably shown to be an effective approach to reduce SIB (Greer et al. 2016; Kahng, Hendrickson, & Vu, 2000; Lalli, Casey, & Kates, 1995; Tiger, Hanley, & Bruzek, 2008). The efficacy of FA + FCT methodologies for treatment of SIB has been investigated and validated across various settings including inpatient (e.g. Hagopian et al. 1998) and outpatient clinics (e.g. Kurtz et al. 2003), schools (e.g. Carr & Durand, 1985) and homes (e.g. Harding, Wacker, Berg, Lee, & Dolezal, 2009; Lindgren et al. 2016; Wacker et al. 1998). There are several ‘barriers’ to timely and successful FA + FCT implementation, however, including cost. Lindgren et al. (2016) estimated the cost of in home delivered FA + FCT treatment was almost $6000 per child (USD), on average. Telehealth (i.e. internet-based videoconferencing) is an approach that could be both cost-effective as a service delivery mechanism and help to decrease some barriers to service access.
Telehealth increased access to expertise
In the emerging literature on telehealth and IDD, telehealth can be effective vehicle for delivering behavioural intervention to children with IDD and challenging behaviours in clinics (e.g. Wacker et al. 2013), schools [with preliminary evidence of a treatment demonstration, Barretto et al. (2006)] and homes (e.g. Suess et al. 2014). Wacker et al. (2013) demonstrated that trained behavioural experts could effectively coach parents via telehealth to deliver FA + FCT in satellite clinics and in home settings. Based on a post hoc aggregated analysis of the findings, Lindgren et al. (2016) estimated that in-clinic, inhome and telehealth models of delivering FA + FCT resulted in similar reductions in challenging behaviour for all participants, regardless of intervention delivery model.
Families of children with autism, in particular, have reported a multitude of barriers to accessing treatment including long provider waitlists, shortages of providers and living in rural areas (Dingfelder & Mandell, 2011; Kazdin, 2008; Ludlow, Conner, & Schechter, 2005; McLeskey, Tyler, & Flippin, 2004; Sperry et al. 1999; Symon, 2005; Thomas et al. 2007). Similar barriers may affect families of children who engage in SIB leaving them without access to behavioural expertise. Of primary concern is that limited access to services or a delay to services may worsen challenging behaviour (Oliver et al. 2012; Rogers & Wallace 2011). Telehealth is a service delivery mechanism with the potential to connect children with needed behavioural expertise, regardless of geographic distances.
In summary, a telehealth model of delivering FA + FCT based approaches to intervention may result in increased intervention access with reduced costs (Lindgren et al. 2016). To move telehealth-supported FA + FCT interventions into evidence-based practice, replications and studies demonstrating for whom and under what conditions this approach to intervention delivery is effective are needed. The available evidence on the use of tele-supported FA + FCT explicitly targeting families with children with SIB is extremely limited. Given the severity of outcomes associated with SIB (e.g. Chadwick et al. 2000), further investigation of telehealth for parent-implemented interventions aimed at SIB reduction with the potential to expand intervention access is warranted. The specific purpose of the current study was to extend the application of tele-supported live home-based parent coaching FA + FCT to explicitly assess and intervene for SIB with two school-aged children with developmental disabilities in their homes.
Method
Participants and setting
Following Institutional Review Board approval from the University of Minnesota and informed parental consent, the first author recruited two elementary-aged boys from regional medical and behavioural service providers. Both boys lived at home with their parent(s). Both boys were recruited because of behavioural problems specific to SIB.
Connor was an 8-year-old Caucasian male, who was diagnosed with cerebral palsy and limited ambulation. Connor’s spoken language was limited to an approximation of ‘I want’, no other spoken language was reported or observed. Connor received special education services at his elementary school. He wore a protective helmet and arm limiting devices due to the severity of his SIB at times. Parents also reported previous medical interventions for the treatment of tissue damage (cauliflower ear) resulting from Connor’s SIB. Connor’s FA began in-home but due to distance and scheduling, assessment sessions transitioned to telehealth to allow for more frequent visits. All telehealth procedures were conducted in the living room of Connor’s home.
Nick was a 5-year-old Caucasian male who had been identified as having autism spectrum disorder. Nick had no spoken language and received applied behavior analysis services in his home 35–40 h per week as well as occupational and physical therapies. As per maternal report, the services were not directly addressing Nick’s SIB. All sessions with Nick were conducted via telehealth in the family’s home in a living room.
Materials
Functional analysis materials for each participant consisted of toys and food found within each participant’s home. During FCT, Connor used a 5- inch diameter BIGmack® switch on which was recorded his mother saying, ‘Come here, please’. Nick used a 3 inch by 3 inch picture card displaying a symbol of a person signing ‘More’.
A functional analysis interview (O’Neill et al. 1997) was used to lead a conversation with the participant’s mother by asking a variety of questions surrounding the participant’s SIB (e.g. events that occur directly before and after the SIB).
Tele behaviour lab-videoconferencing equipment and coaches
All procedures were conducted in the participating families’ homes by the participant’s parent(s). Coaches delivered remote instruction and support for conducting FA + FCT sessions from the designated tele behaviour lab at the University of Minnesota. Coaches located at the lab site conducted videoconferencing using a Dell™ Desktop computer, an external Logitech camera, a broadband internet connection and Hangouts™ communications platform. Video was collected using Debut video capture software on the host computer and were stored on a secure server at the University of Minnesota tele behaviour lab. Each family used their own iPad or tablet with an internal camera to transmit audio and video. All direct parent-coaching was delivered by the first author, a graduate student in Educational Psychology at the University of Minnesota, who had 3 years of experience implementing FA + FCT procedures in homes with parents.
Target behaviour and data collection
Child behaviour
Connor’s SIB was in the form of head hitting and defined as any strike to his head with any body part or object. Nick’s SIB was defined as face slapping, specifically, any strike to his face with an open palm or any hit of the head to the floor. For Connor, mands were defined as any press of the BIGmack® switch with either hand that produces the voice output or the first press of the BIGmack® switch during reversal sessions where successive presses that were separated by 3 s. For Nick, mands were defined as any touch to the picture card or handing the picture card to his parent. For both participants, the coach and parents collaborated to create criteria for terminating an experimental session (available upon request) in the event that SIB was too severe. No sessions were terminated due to severity of SIB.
Parent behaviour
Parent behaviour was measured during SDA (for Nick) and FA + FCT (for both participants). Task analyses (breaking a task down into smaller component sequential steps) were created for each participant’s FA and FCT conditions (available upon request). Each individual step of the task analysis was considered an opportunity for the parent to respond correctly or incorrectly to the procedure. The steps of the task analysis could be repeated throughout each session. A response was scored correct if the parent implemented the step as described in the task analysis, both independent implementation and coached steps were scored as correct. An incorrect response was scored if the parent implemented the step incorrectly by omitting part of the step, adding a component to the step or conducted a step out of order. If there were multiple opportunities to perform a response, it was marked as correct or incorrect at each new opportunity.
Data collection and coders
Videos from live telehealth sessions for all participants were recorded directly from the computer screen using Debut video capture software. Independent coders viewed recorded videos to measure SIB and mands for each participant using paper–pencil 10 s frequency within interval recording. Coders were graduate students in Educational Psychology; one student was trained to record SIB and mands, two other students were trained to independently code fidelity of parent implementation of the FCT protocol.
Experimental design
The SDA for Nick and FA for both participants was conducted within a multi-element design to identify possible functional patterns of SIB in relation to environmental events and context. Following the FA, an ABAB single-case experimental design was used to evaluate the effect of FCT.
Procedures
The primary coach conducted the functional analysis interview (O’Neill et al. 1997) with each participant’s mother. This information, as well as subsequent observations [approx. 3 h informal for Connor and structured for Nick (described below)], was used to develop the operational definitions of SIB and to select and design analogue analysis conditions.
Structured descriptive assessment
For Nick, SDA conditions were conducted to generate hypotheses regarding the conditions in which SIB occurred. The coach instructed Nick’s mom to engage in different activities such as instructing him to complete a task or restricting his access to a preferred tangible item. Further, the coach asked Nick’s mom to respond as she normally would if she was not being observed. Sessions were 3 to 5 min long and the data were used to determine the specifics of Nick’s analogue FA conditions.
Functional analysis
An experimental FA of SIB was conducted for each participant using conditions similar to those described in Iwata et al. (1982/1994), with the addition of a tangible condition. Each session was 5 min in length. Prior to each session, the coach described to the child’s mother the condition they were about to conduct, how to respond to target behaviours and what materials to have available for the session. The coach instructed the child’s mother to either ignore or block SIB while refraining from eye contact and verbal interactions. All sessions were 5 min long.
Free play
The free play condition was conducted as a control condition. The coach instructed the parent to engage the participant in preferred leisure activities, such as playing with preferred toys, to deliver non-contingent attention to the participant, and not to deliver any task demands.
Escape
The escape condition was designed to test SIB’s sensitivity to negative reinforcement in the form of escape from demands. The escape condition consisted of typically required but non-preferred tasks such as cleaning up toys or fine motor activity, as suggested by the parent. The coach instructed the parent to remove the task demand for 10–15 s contingent on each occurrence of SIB.
Attention
The attention condition was designed to test SIB’s sensitivity to positive reinforcement in the form of contingent parent attention. The coach instructed the parent to engage the participant in an independent activity. Next, the coach instructed the parent to divert their attention from the participant and to engage in a different activity, such as reading a magazine. The coach instructed the parent to provide attention for 10–20 s contingent on each occurrence of SIB.
Tangible
The tangible condition was designed to test SIB’s sensitivity to positive reinforcement in the form of contingent access to preferred tangible items (swing, ottoman, heater, music, toys, hat or towel). The coach instructed the parent to provide 10–15 s access to an item the parent reported as preferred by the child. Next, the coach instructed the parent to restrict access to the preferred item. The coach instructed the parent to provide 10–15 s access to the tangible item contingent on each occurrence of SIB.
Functional communication training
Functional communication training was evaluated using an ABAB design. During baseline conditions (A), the functional reinforcer was provided contingent on occurrences of SIB and was not delivered contingent on any other behaviour. During intervention conditions (B), each occurrence of the mand produced reinforcement and reinforcement was withheld contingent on SIB (i.e. SIB was on extinction).
Functional communication training-attention (Connor)
Each FCT session began with Connor’s mother providing 20–30 s of attention by singing songs or playing brief interactive games. After this short period of time, Connor’s mother withdrew her attention by pausing the interaction and moving to a position at least 3 feet away. Connor was then prompted from behind by a second person to request his mother’s attention by pressing the microswitch programmed with his mother’s voice to say, ‘Come here please’. Immediately after Connor activated the switch, his mother approached him and provided attention for 20–30 s. All SIB was ignored or blocked while refraining from talking or making eye contact by a second person. If Connor engaged in SIB while he was receiving reinforcement, his mother stepped away and attention was removed. During the second baseline condition, Connor’s mother began by providing attention for 20–30 s. She then withdrew by moving to a position at least 3 feet away. The switch was available but the power was turned off. Each occurrence of SIB was reinforced with contingent access to maternal attention for 20–30 s.
Functional communication training-tangible (Nick)
Each baseline session began with 20–30 s of Nick’s mother providing access to a preferred tangible item. Next, restricted access to the preferred item was implemented by saying, ‘Mom’s turn’ and restricting his access to the item. The picture card was available during this time but use of the picture card was not reinforced with access to the tangible item. Only engagement in SIB was reinforced with contingent access to the tangible item. Each FCT session began with Nick’s mother providing 20–30 s of a preferred tangible item. Next, Nick’s mother restricted access to the tangible item while saying, ‘Mom’s turn’. Nick was prompted to use the picture card with Nick’s mother using a most-to-least prompting hierarchy. During FCT sessions, only engagement in the mand resulted in contingent access to the preferred tangible item. SIB was ignored/blocked with no eye contact or verbal interactions.
Inter-observer agreement
A second observer independently observed 33% of Nick’s SDA sessions. Inter-observer agreement (IOA) was calculated as (agreements /(agreements + disagreements) × 100) and averaged 99% (range = 94–100%). Thirty per cent of Connor’s FA sessions were independently coded by a second observer. Overall IOA averaged 96% (range = 87– 100%). Thirty per cent of Nick’s FA sessions were independently coded by a second observer. Overall, IOA averaged 97% (range = 87–100%). A second observer independently observed 31% of the FCT sessions for Connor and IOA averaged 93% (range = 87–100%). Thirty-eight per cent of Nick’s FCT sessions were coded by a second observer and IOA averaged 97% (range 93–100%). Parent behaviour in the form of implementation fidelity was assessed by two independent coders. Both coders independently observed 32% of SDA sessions for Nick. Fidelity IOA averaged 98% (range = 87.5– 100%). Both coders scored 58% of the FA sessions for Connor. Fidelity IOA averaged 95% (range = 75– 100%). Both coders scored 26% of Nick’s FA sessions. Fidelity IOA averaged 97% (range 80– 100%). Thirty-four per cent and twenty-five per cent of FCT sessions were coded for Connor and Nick, respectively. Fidelity IOA averaged 94% (range = 88–100%) for Connor and 93% (range = 85.5–100%) for Nick.
Results
Connor’s FA (Fig. 1a) showed that the highest rates of SIB occurred during the attention condition, and the lowest rates of SIB occurred during the free play and tangible conditions. The FA results suggested that adult attention functioned as a reinforcer for Connor’s SIB. Based on the results of the FA, FCT was implemented to teach Connor to request adult attention by pressing a microswitch.
Figure 1.
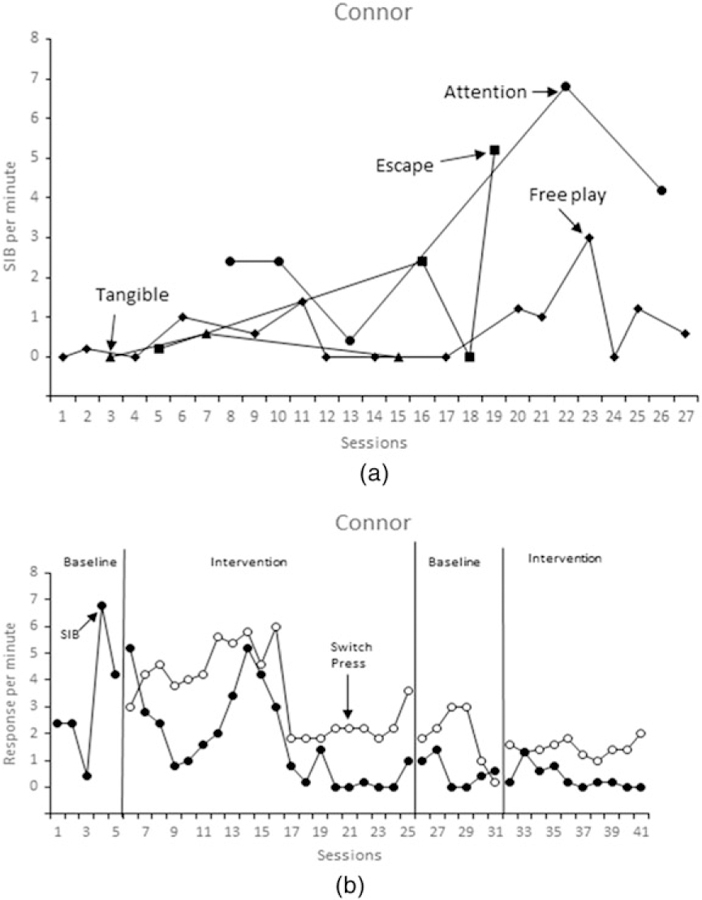
(a) Results of Connor’s functional analysis. Closed circles denote attention conditions, closed triangles denote tangible conditions, closed squares denote escape conditions and closed diamonds denote free play conditions. (b) Results of Connor’s functional communication training. Open circles denote mands, closed circles denote SIB. SIB, self-injurious behaviour.
The effects of FCT on SIB and mands for adult attention are depicted in Fig. 1b. The first baseline condition was based on data from the FA sessions in which the switch was not present and rates of SIB were elevated but variable across sessions. During FCT (intervention) when mands produced adult attention and attention was withheld contingent on SIB, Connor engaged in variable rates of SIB until eventually decreasing to near-zero rates in the last five sessions of the condition. Connor began using the microswitch to request attention and after the second session of FCT, mands consistently occurred at higher rates than SIB. When the baseline condition was reinstated, mands continued to occur at a higher rate than SIB, but SIB occurred more often than during the last five sessions of the preceding FCT condition. However, only in the final data point of the second baseline phase did the mands decrease to a level below SIB. Connor’s mother expressed having a difficult time ignoring mands during the second baseline phase, and therefore, the phase was terminated as soon as the data paths overlapped in session 31. When FCT (intervention) was reintroduced, mands continued to occur at a higher rate than SIB and the rate of SIB decreased across sessions and was at or near zero in the final four sessions of the condition.
The results of the Nick’s SDA are depicted in Fig. 2a. During the SDA, no SIB occurred during the diverted attention or free play conditions. Relatively high rates of SIB occurred during both the demand and restricted tangible conditions. During the FA, Nick’s SIB was variable and occurred in at least one session of all conditions except attention. Nick engaged in the highest rates of SIB during the tangible condition (Fig. 2b). After the first three escape sessions, SIB did not recur during the escape condition. However, SIB occurred intermittently during the tangible condition. Therefore, based on the SDA and FA data, FCT was used to teach Nick to use a picture card to request a tangible item.
Figure 2.
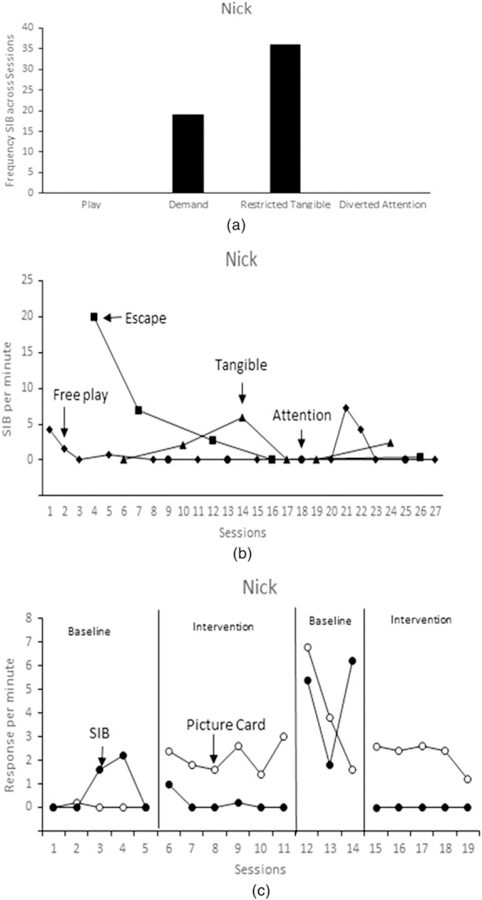
(a) Results of Nick’s structured descriptive assessment. Bar graphs report frequency of SIB. (b) Results of Nick’s functional analysis. Closed circles denote attention conditions, closed triangles denote tangible conditions, closed squares denote escape conditions and closed diamonds denote free play conditions. (c) Results of Nick’s functional communication training. Open circles denote mands, close circles denote SIB. SIB, self-injurious behaviour.
The effects of FCT on SIB and mands for tangible items for Nick are depicted in Fig. 2c. During the first baseline condition, reinforcement contingent on SIB but not use of the picture card resulted in virtually no picture card use and high but variable rates of SIB. Next, during FCT (intervention), when picture card use produced access to tangible items and tangible items were withheld for SIB, there was an immediate increase in the rate of picture card use and a decrease in SIB to near-zero levels. When the baseline condition was reinstated and SIB produced access to tangible items, there was an immediate increase in rate of SIB and a decreasing trend was observed for the use of the picture card. Finally, when FCT was reintroduced and SIB did not produce tangible items but use of the picture card did, there was an immediate decrease in SIB back to zero for all five sessions and picture card use returned to stable elevated levels.
Parent fidelity of implementation
Fidelity of implementation was examined across all phases of assessment and intervention for both participants. Parent fidelity was examined across the FA and FCT conditions for Connor. Average percent correct implementation of the FA procedures in the attention condition was 99% (range = 96–100%; 27/28–45/45 steps). Similarly, fidelity of escape procedures averaged 98% (range = 88–100%; 14/16– 30/30). Average per cent correct implementation of the tangible condition procedures was 100% (5/5 steps). The free play condition had the lowest fidelity of implementation averaging 83% (range = 50–100%; 1/2–3/3 steps). The most common error during free play was the delivery of task demands. Implementation across FCT conditions averaged 99% correct (range = 98–100%; 97/99–100/100 steps).
Fidelity of implementation for the SDA conditions with Nick were variable, with the lowest percent correct implementation of 50% of steps (range = 2/4– 4/4) occurring during the free play condition. The most common step performed incorrectly was placing demands on Nick during the free play condition. In contrast, fidelity of implementation was highest in the demand session, with 100% of steps (4/4) implemented correctly. Fidelity was also relatively high in both the diverted attention (80%; 4/5 steps), and restricted tangible sessions (range = 87.5–100%; M= 94%; 7/8–8/8 steps).
Overall fidelity of implementation was high across all conditions during the FA for Nick. Average per cent correct implementation of the FA procedures was highest in the free play (100%; 2/2 steps) and tangible (100%; 8/8–18/18 steps) conditions with slightly lower fidelity in the escape (75%; 12/16 steps). Per cent correct implementation was lowest in the attention condition (33%; 1/3 steps). Fidelity may have been lower during the attention condition as the participant would often attempt to remove his diaper during recorded sessions. Nick’s mother was coached to respond by not speaking to him and redirecting to appropriate attire as quickly as possible. Per cent correct implementation across FCT conditions averaged 88% (range = 84–92%; 42/50–48/52 steps).
Discussion
The current study aimed to extend the application of telehealth delivered FA + FCT to untreated self-injury. The results provide additional evidence that parents can implement FA + FCT procedures for their child with SIB when supported by live coaching via telehealth. These results are consistent with previous findings (Barretto et al. 2006; Suess et al. 2014; Wacker et al. 2013). Suess et al. (2014) documented implementation fidelity evidence for three families conducting home-based FA + FCT during coached and uncoached FCT sessions. Their results provided initial evidence that parents can implement FCT sessions with fidelity. This study supports and extends results providing evidence that parents can not only implement FCT sessions with fidelity but can also be coached to implement SDA and FA sessions with fidelity.
The preliminary results are promising with respect to extending the use of home-based parent coaching to conduct FA + FCT with families with children with SIB via telehealth. In two prior telehealth-based studies of destructive behaviour (Suess et al. 2014; Wacker et al. 2013), the samples were preschool children with ‘destructive behaviour’ that included SIB for some cases. In those studies, the severity of the topographies were not clear (i.e. ‘throwing self to the floor’) and all children were preschool aged. In our study, untreated SIB from two older children was the primary referral reason with SIB severe enough to warrant protective devices in one instance (Connor).
For both participants, based on visual inspection, SIB appeared to be reduced and functionally equivalent behaviour increased. Our approach included termination criteria based on SIB severity and parental concerns, but no sessions terminated early. Overall, in both cases, parents reported being supportive of implementing FA + FCT procedures in the absence of therapists in home.
There have been some demonstrations to date providing evidence that telehealth-supported coaching is feasible in multiple settings including clinics (Wacker et al. 2013) and homes (Suess et al. 2014). There are fewer direct assessments of fidelity of implementation. Suess et al. (2014) investigated parent fidelity and child outcomes in a retrospective assessment from FA + FCT delivered by parents with coaching via telehealth for three children (diagnosed with autism spectrum disorder, all under the age of seven). All parents implemented the interventions with acceptable levels of fidelity that improved over time for two parents and remained high throughout phases for one parent. The parents delivering intervention in our study also demonstrated very good fidelity. We think the fidelity results of this investigation provide further preliminary evidence that parents can be coached live in their homes to implement FA + FCT.
Limitations & future directions
Although this study shows that telehealth may be a useful tool for coaching parents to assess and intervene with their child’s SIB, there were several limitations to note. There were only two subjects included which limits the generalizability of the findings. No baseline sessions with the microswitch present were conducted for Connor, and in his second baseline condition, the data were more variable which limits inferences about the effect of FCT on his SIB. Parent implementation fidelity was evaluated post hoc therefore no conclusions about the effect of fidelity on SIB can be made. Finally, we did not systematically collect social validity data and future research should use measures to document the degree of satisfaction with outcomes. As the evidence base for tele-supported FA + FCT applications continues to grow, studies should also be simultaneously designed to improve our understanding of the conditions under which tele-supported approaches can be successfully implemented by parents and other providers.
Acknowledgements
The study was supported, in part, by Eunice Kennedy Shriver NICHD (grant no. 44763). We thank the families for their patience and support. We also thank Chris Lindgren for his help coding data.
References
- Anderson C & Long E (2002) Use of a structured descriptive assessment methodology to identify variables affecting problem behavior. Journal of Applied Behavior Analysis 35, 137–54. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Baghdadli A, Picot MC, Pry R, Michelon C, Burzstejn C, Lazartigues A et al. (2008) What factors are related to a negative outcome of self-injurious behavior during childhood in pervasive developmental disorders? Journal of Applied Research in Intellectual Disabilities 21, 142–9. [Google Scholar]
- Barretto A, Wacker DP, Harding J, Lee J & Berg WK (2006) Using telemedicine to conduct behavioral assessments. Journal of Applied Behavior Analysis 39, 333–40. 10.1901/jaba.2006.173-04. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Beavers GA, Iwata BA & Lerman DC (2013) Thirty years of research on the functional analysis of problem behavior. Journal of Applied Behavior Analysis 46, 1–21. [DOI] [PubMed] [Google Scholar]
- Berkson G, Tupa M & Sherman L (2001) Early development of stereotyped and self injurious behaviors: I. incidence. American Journal on Mental Retardation 106, 539–47. [DOI] [PubMed] [Google Scholar]
- Carr EG & Durand M (1985) Reducing behavior problems through functional communication training. Journal of Applied Behavior Analysis 2, 111–26. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Chadwick O, Kusel Y, Cuddy M & Taylor E (2005) Psychiatric diagnoses and behaviour problems from childhood to early adolescence in young people with severe intellectual disabilities. Psychological Medicine 35, 751–60. [DOI] [PubMed] [Google Scholar]
- Chadwick O, Piroth N, Walker J, Bernard S & Taylor E (2000) Factors affecting the risk of behaviour problems in children with severe intellectual disability. Journal of Intellectual Disability Research 44, 108–23. [DOI] [PubMed] [Google Scholar]
- Cooper SA, Smiley E, Allan LM, Jackson A, Finlayson J, Mantry D et al. (2009) Adults with intellectual disabilities: Prevalence, incidence and remission of self-injurious behaviour, and related factors. Journal of Intellectual Disability Research 53, 200–16. [DOI] [PubMed] [Google Scholar]
- Dingfelder HE & Mandell DS (2011) Bridging the research to practice gap in autism intervention: An application of diffusion of innovation theory. Journal of Autism and Developmental Disorders 41, 597–609. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Emerson E (1990) Self-injurious behaviour: some of the challenges it presents. Mental Handicap 18, 92–8. [Google Scholar]
- Emerson E, Kiernan C, Alborz A, Reeves D, Mason H, Swarbrick R et al. (2001a) Predicting the persistence of severe self-injurious behavior. Research in Developmental Disabilities 22, 67–75. [DOI] [PubMed] [Google Scholar]
- Emerson E, Kiernan C, Alborz A, Reeves D, Mason H, Swarbrick R et al. (2001b) The prevalence of challenging behaviors: A total population study. Research in Developmental Disabilities 22, 77–93. [DOI] [PubMed] [Google Scholar]
- Greer BD, Fisher WW, Saini V, Owen TM & Jones JK (2016) Functional communication training during reinforcement schedule thinning: An analysis of 25 applications. Journal of Applied Behavior Analysis 49, 105–21. 10.1002/jaba.265. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Hagopian LP, Fisher WW, Sullivan MT, Acquisto J & LeBlanc LA (1998) Effectiveness of functional communication training with and without extinction and punishment: A summary of 21 inpatient cases. Journal of Applied Behavior Analysis 31, 211–35. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Harding JW, Wacker DP, Berg WK, Lee JF & Dolezal D (2009) Conducting functional communication training in home settings: A case study and recommendations for practitioners. Behavior Analysis in Practice 2, 21–33. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Iwata BA, Dorsey MF, Slifer KJ, Bauman KE & Richman GS (1982/1994) Toward a Functional Analysis of Self-Injury. Analysis and Intervention In Developmental Disablities 2, 3–20. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Iwata BA, Pace GM, Dorsey MF, Zarcone JR, Vollmer TR et al. (1994) The functions of self-injurious behavior: An experimental-epidemiological analysis. Journal of Applied Behavior Analysis 27, 215–40. 10.1901/jaba.1994.27-215. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Kahng S, Hendrickson DJ & Vu CP (2000) Comparison of single and multiple functional communication training responses for the treatment of problem behavior. Journal of Applied Behavior Analysis 33, 321–4. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Kazdin AE (2008) Evidence-based treatments and delivery of psychological services: Shifting our emphases to increase impact. Psychological Services 5, 201–15. 10.1037/a0012573. [DOI] [Google Scholar]
- Kurtz PF, Chin MD, Huete JM, Tarbox RSF, O’Connor JT et al. (2003) Functional analysis and treatment of self-injurious behavior in young children: A summary of 30 cases. Journal of Applied Behavior Analysis 36, 205–19. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Lalli JS, Casey S & Kates K (1995) Reducing escape behavior and increasing task completion with functional communication training, extinction and response chaining. Journal of Applied Behavior Analysis 28, 261–8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Lindgren S, Wacker D, Suess A et al. (2016) Telehealth and autism: Treating challenging behavior at lower cost. Pediatrics 137, S167–S175. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Ludlow BL, Conner D & Schechter J (2005) Low incidence disabilities and personnel preparation for rural areas: Current status and future trends. Rural Special Education Quarterly 24, 15. [Google Scholar]
- McLeskey J, Tyler NC & Flippin SS (2004) The supply of and demand for special education teachers a review of research regarding the chronic shortage of special education teachers. The Journal of Special Education 38, 5–21. [Google Scholar]
- Murphy GH, Beadle-Brown J, Wing L, Gould J, Shah A & Holmes N (2005) Chronicity of challenging behaviours in people with severe intellectual disabilities and/or autism: A total population sample. Journal of Autism and Developmental Disorders 35, 405–18. [DOI] [PubMed] [Google Scholar]
- Oliver C, Murphy GH & Corbett JA (1987) Self-injurious behaviour in people with mental handicap: A total population study. Journal of Mental Deficiency Research 31, 147–62. [DOI] [PubMed] [Google Scholar]
- Oliver C, Petty J, Ruddick L & Bacarese-Hamilton M (2012) The association between repetitive, self-injurious and aggressive behavior in children with severe intellectual disability. Journal of Autism and Developmental Disorders 42, 910–9. [DOI] [PubMed] [Google Scholar]
- O’Neill RE, Horner RH, Albin RW, Storey K, Sprague JR, & Newton JS (1997) Functional assessment of problem behavior: A practical assessment guide Pacific Grove, CA: Brooks/Cole. [Google Scholar]
- Rogers S, & Wallace K (2011) Intervention for infants and toddlers with autism spectrum disorders. In: Autism spectrum disorders (eds. Amaral D, Dawson G, Geschwind D), pp. 1081–94. Oxford University Press, Oxford, UK. [Google Scholar]
- Rojahn J, Schroeder SR & Hoch TA (2008) Self-injurious Behavior in Intellectual Disabilities Elsevier, Oxford, UK. [Google Scholar]
- Schroeder SR, Marquis JG, Reese RM, Richman DM, Mayo-Ortega R et al. (2014) Risk factors for self-injury, aggression, and stereotyped behavior among young children at risk for intellectual and developmental disabilities. American Journal of Intellectual and Developmental Disabilities 119, 351–70. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Sperry LA, Whaley KT, Shaw E & Brame K (1999) Services for young children with autism spectrum disorder: Voices of parents and providers. Infants and Young Children 11, 17–33. [Google Scholar]
- Suess AN, Romani PW, Wacker DP, Dyson SM, Kuhle JL, Lee JF et al. (2014) Evaluating the treatment fidelity of parents who conduct in-home functional communication training with coaching via telehealth. Journal of Behavioral Education 23, 34–59. [Google Scholar]
- Symon J (2005) Expanding interventions for children with autism: Parents as trainers. Journal of Positive Behavior Interventions 7, 159–73. 10.1177/10983007050070030501. [DOI] [Google Scholar]
- Symons FJ, Koppekin A & Wehby JH (1999) Treatment of self-injurious behavior and quality of life for persons with mental retardation. Mental Retardation 37, 297–307. [DOI] [PubMed] [Google Scholar]
- Taylor L, Oliver C & Murphy G (2011) The chronicity of self-injurious behaviour: A long-term follow-up of a total population study. Journal of Applied Research in Intellectual Disabilities 24, 105–17. [Google Scholar]
- Tiger JH, Hanley GP & Bruzek J (2008) Functional communication training: A review and practical guide. Behavior Analysis in Practice 1, 16–23. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Thomas KC, Ellis AR, McLaurin C, Daniels J & Morrissey JP (2007) Access to care for autism related services. Journal of Autism and Developmental Disorders 37, 1902–12. 10.1007/s10803-006-0323-7. [DOI] [PubMed] [Google Scholar]
- Wacker DP, Berg WK, Harding JW, Derby MK, Asmus JM, & Healy A (1998) Evaluation and long-term treatment of aberrant behavior displayed by young children with disabilities. Journal of Developmental & Behavioral Pediatrics 19, 260–6. [DOI] [PubMed] [Google Scholar]
- Wacker DP, Lee JF, Dalmau YCP, Kopelman TG, Lindgren SD, Kuhle J et al. (2013) Conducting functional communication training via telehealth to reduce the problem behavior of young children with autism. Journal of Developmental and Physical Disabilities 25, 35–48. [DOI] [PMC free article] [PubMed] [Google Scholar]


