Abstract
Background The distal radius fracture (DRF) is the most common fracture among adults. In recent years, there has been a shift toward volar locking plates in the treatment of DRFs, and this shift has taken place with a low degree of evidence.
Question/purposes Can combined volar T-plating and dorsal pi-plating of AO type C fractures yield a good functional and radiographic outcome 1 year postoperatively?
Patients and Methods In a retrospective cohort study, we evaluated 102 consecutive patients operated with combined dorsal and volar plating, of whom 80 completed the 1-year follow-up. The DRFs were operated between 2012 and 2013. All cases were AO type C2 and C3 fractures. The primary outcome was functional scoring including radiographic examination. Secondary outcome measures included range of motion, visual analog scale (VAS) pain scores, and hand grip strength.
Results The median Batra radiographic score was 84.5. Wrist extension was 74% of the uninjured side, flexion was 70%, pronation was 94%, and supination was 90%. The Patient-Rated Wrist Evaluation score was 21 points, and the Disabilities of the Arm, Shoulder, and Hand score was 19.4 points. VAS pain scores were 0 at rest and 3 during activity. Hand grip strength was 80% of the uninjured side. Radiographic outcome did not correspond to a patient-reported outcome. Hardware removal was performed in 15/80 cases.
Conclusions We conclude that a good outcome can be expected after combined dorsal and volar plating of DRFs. Radiographic outcome is not necessarily associated with functional outcome 1 year postoperatively. The rate of hardware removal was acceptable.
Level of Evidence III
Keywords: distal radius, fracture, plating
The distal radius fracture (DRF) is the most common fracture among adults, constituting 18% of all fractures in an orthopaedic trauma unit. 1 The annual incidence in Sweden is 26 per 10,000 inhabitants. 2 Nondisplaced and displaced but reducible fractures are usually treated nonoperatively. 3 Displaced fractures that cannot be reduced are often considered for operative treatment. 4 In recent years, there has been a trend toward more surgery in the treatment of DRFs. 5 Previously common interventions such as pinning, nonlocking plates, and external fixation have gradually been replaced by volar locking plates. 6 This shift has largely taken place with a low degree of evidence. 7 In recent years, some studies have indicated that volar locking plates have a better patient-reported outcome and better range of motion (ROM) compared with older techniques. 8 9 10 Biomechanical data have stressed the importance of correcting the dorsal angulation of the distal radius to less than 10 degrees of the dorsal tilt to prevent distal radioulnar joint(DRUJ) instability. 11 Others have found that restoring ulnar variance and volar tilt are the most important radiographic parameters to be restored to achieve a good functional result. 12 Anatomical reduction of intra-articular fractures has been assumed to reduce the incidence of posttraumatic arthritis. 13 The dorsal pi-plate is a modern low-profile plate designed to manage complex intra-articular fractures. Good results have been reported for combined volar and dorsal plate fixation of complex DRFs. 14 15 Some concern has been raised regarding extensor tendon problems with the pi-plate, whereas other authors have not found this to be a problem. 16 17
The purpose of this study was to assess the outcome after combined volar and dorsal pi-plating of complex intra-articular DRFs in a consecutive series of 102 patients with 1-year follow-up, all operated at a Swedish tertiary referral center. The questions to be answered specifically were if the technique with double plating can yield a satisfactory clinical and radiographic outcome and if the radiographic outcome corresponds with the clinical outcome. The study is a retrospective study with prospectively collected data.
Materials and Methods
The study was approved by the Regional Ethical Committee. All patients who underwent surgery for DRFs at the Department of Hand Surgery, Örebro University Hospital, between July 1, 2012, and June 30, 2013, were identified. Inclusion criteria for the study included AO (Arbeitsgemeinschaft für Osteosynthesefragen) type C fractures that were treated with a combined volar T-plate and a dorsal pi-plate (DePuy Synthes, Westchester, PA). 18 Exclusion criteria included dementia, mental illness, alcohol/substance abuse, metabolic bone disease, and difficulty to understand Swedish. A total number of 143 DRFs were treated at our institution during the timeframe for the study. Of these 143 cases, 102 cases met the inclusion criteria for the study. All operations were performed by fellowship-trained orthopaedic hand surgeons.
Surgical Technique
All fractures in this study were managed with combined volar and dorsal plate fixation. To optimally visualize the volar ulnar part of the distal radius, a central incision including a carpal tunnel release was used. The fracture was visualized in the interval between the finger flexors and the median nerve. The pronator quadratus was divided. The fracture was reduced, and a volar T-plate was applied to the volar surface of the distal radius. After volar reduction and application of the T-plate, a dorsal exposure through a longitudinal incision was centered over Lister's tubercle. The fourth extensor compartment was opened in a Z -shaped manner, and the fracture was exposed with a careful subperiosteal dissection. The radial extensors were retracted radially, and the brachioradialis insertion was released. Impacted articular fragments were reduced using the pi-plate as a reduction tool. The application of screws in a proximal-to-distal order and the shape of the pi-plate gathered the separate fracture fragments to a single unit and pushed them in position with the volar T-plate as a fulcrum. The fragments were then fixed with locking pegs ( Fig. 1 2 3 ). In cases with a concomitant ulnar styloid fracture and DRUJ instability (assessed intraoperatively after placement of the volar and dorsal plates), the ulnar styloid was fixated using either a 3-mm cannulated compression screw with a washer (DePuy Synthes), a 2-mm locking distal ulna plate (DePuy Synthes), or 1.2-mm Kirschner (K) wires. In case of a concomitant scapholunate dissociation, the ligament was sutured with 2.0 Ethibond (Ethicon, Somerville, NJ) osteosutures and the scapholunate articulation pinned using 1.2-mm K-wires. A splint was used for the first 2 weeks postoperatively, and thereafter gentle mobilization of the wrist with a removable splint was started under the guidance of a physiotherapist. In case of an ulnar styloid fracture that was fixated operatively, an above-the-elbow cast was used for 4 weeks, and in case of a scapholunate ligament suture, an above-the-elbow cast was used for 6 weeks. All patients were seen by an experienced hand therapist and given instructions on exercises to reduce edema before being discharged from the hospital. The patients were allowed to use the wrist without a splint, with the exception of lifting heavy objects, which was discouraged for the first 3 months postoperatively for patients with isolated DRFs.
Fig. 1.

( A , B ) Preoperative radiographs of a 39-year-old female with an intra-articular distal radius fracture after falling onto an outstretched hand. Note complex metaphyseal and articular comminution with substantial displacement.
Fig. 2.

( A , B ) Intraoperative radiographs after open reduction and combined plating of the distal radius fracture and fixation of the ulnar styloid using a 2-mm locking distal ulna plate. In our experience, the volar fragments are realigned and stabilized using the volar T-plate through a central incision to restore the length of the radius. The realignment is continued from the dorsal side using the Pi-plate as a reduction tool and the volar plate as a fulcrum.
Fig. 3.
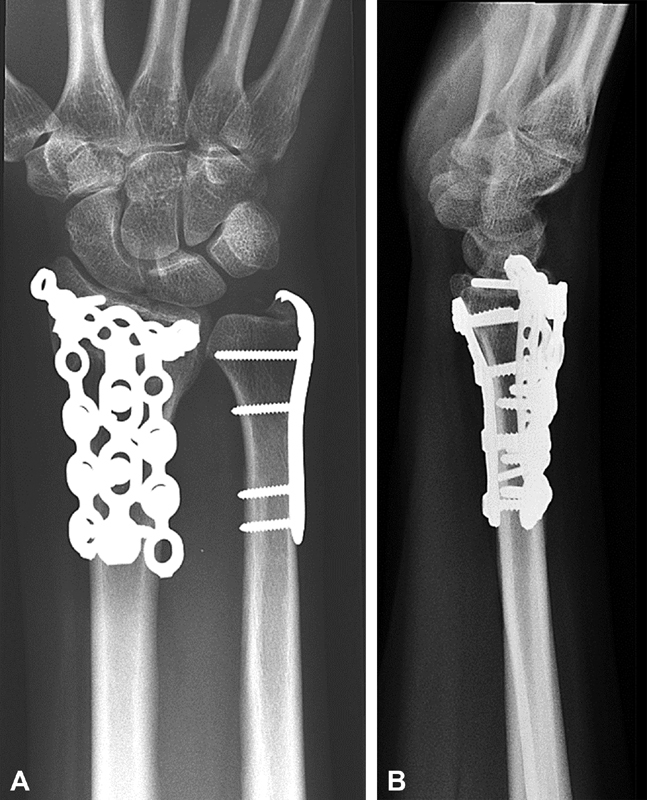
( A , B ) Radiographs 1 year postoperatively demonstrating restoration of length and alignment of the radius.
Clinical Evaluation
The following outcome measures were registered 1 year postoperatively as part of the departments clinical routine by the department's hand therapists in both the operated and uninjured wrist: pain (visual analog scale [VAS] at rest, VAS during activity), hand grip strength (kg), pinch grip strength (kg), key pinch grip strength (kg), ROM (flexion, extension, radial deviation, ulnar deviation, pronation, supination), Patient-Rated Wrist Evaluation (PRWE) score, and the Disabilities of the Arm, Shoulder, and Hand (DASH) score.
The patients rated wrist pain according to the VAS (0 = no pain; 10 = worst imaginable pain), both at rest and during activity. Hand grip strength measurements were performed by a physiotherapist with more than 5 years of clinical experience using a hydraulic hand dynamometer (North Coast Medical Inc., Morgan Hill, CA). For key pinch grip strength and pinch grip strength measurements, a pinch gauge was used (North Coast Medical Inc.). ROM for wrist flexion, extension, radial deviation, ulnar deviation, pronation, and supination was registered by a physiotherapist using a goniometer. Patients completed the Swedish validated translations of the questionnaires PRWE and DASH. 19 20 The PRWE is a validated wrist questionnaire designed to measure wrist pain and disabilities in daily living. Consisting of a 15-item questionnaire, it rates pain and disability equally in functional activities. A score of 100 is calculated, where 0 represents no pain or disability. The DASH is a region-specific outcome instrument that measures disabilities and symptoms in the upper extremity. The DASH score has a 30-item disability scale regarding the patient's health during the preceding week. A score is calculated from 0 to 100, where 100 represents the severest disability. Causes for secondary surgery were noted at regular follow-up visits and analyzed.
Radiographic Assessment
Radiographic examination of the wrist was performed preoperatively, immediately postoperatively, and 1 year postoperatively. Anteroposterior and lateral views were taken. Assessment of DRFs according to the AO classification was performed by the operating surgeon using preoperative radiographs and intraoperative findings. 18 Radiographic findings 1 year postoperatively were assessed according to the Batra anatomical scoring system. 21 The Batra anatomical score includes assessment of the radial angle, radial length, volar tilt, incongruency, and the radioulnar joint. A summarized score assessing the skeletal anatomy is calculated, where the maximum result is 100. The Batra anatomical score is divided into four groups: excellent (100–90), good (89–80), fair (79–70), and poor (<70). Assessment of the Batra score was performed by a consultant hand surgeon at our institution.
Statistics
Data are presented as median and interquartile range due to a nonnormal distribution. The normal distribution was assessed using the Shapiro–Wilk test (data not shown). The Wilcoxon rank sum test was used to assess the outcome between the injured and uninjured side. To assess differences between the four groups of radiographic Batra score regarding PRWE score, DASH score, VAS pain score in activity and summarized wrist flexion/extension, the Kruskal–Wallis test with Bonferroni-corrected posthoc tests were used. The Mann–Whitney U test was used to assess the differences between AO type C2 and C3 fractures regarding PRWE score, DASH score, VAS score in activity, and summarized wrist flexion/extension. A corrected p < 0.05 was considered to be statistically significant.
Results
Of the 102 cases, one bilateral case was excluded, one patient underwent arthrodesis (radio-lunate), and one died of unrelated causes. Eighty patients completed the 1-year follow-up examination. The ulnar styloid was fractured in 25 of the 102 cases. in 12 of these 25 cases, it was fixated operatively: with an ulnar hook plate in 9 cases, with a cannulated screw in 2 cases, and with a 1.2-mm K-wire in one case. Four scapholunate ligament injuries were sutured. Demographic characteristics regarding age, sex, dominant side injury, and AO fracture type are found in Table 1 . Mean dorsal extension was 74% of the uninjured side, and flexion was 70% of the uninjured side. Grip strength was 80% of the uninjured side. The VAS pain score at rest was 0, and VAS pain score during activity was 3. The median PRWE score was 21, and the median DASH score was 19.4 ( Table 2 ). Hardware removal was performed during the first year postoperatively in 15/80 patients; the reason for hardware removal was dorsal wrist pain/extensor tenosynovitis. Three cases had a postoperative infection, which healed with antibiotics treatment. Two of the three infected cases were open fractures. There were no cases of tendon rupture or complex regional pain syndrome. Radiographic evaluation 1 year postoperatively was available for 75/80 cases. The median Batra-score was 84.5, the radial angle was 12 degrees, and the volar tilt was 5.5 degrees ( Table 3 ). Of the 80 cases, 50 had a good-to-excellent Batra score ( Table 4 ).
Table 1. Demographic data.
| Male/female | Median age (range) | Hand dominance right/left | Dominant extremity fractured: right/left | AO type C2/C3 |
|---|---|---|---|---|
| 26/54 | 55 (18–75) | 74/6 | 43/37 | 11/69 |
Table 2. Wrist function 1 year postoperatively.
| Outcome measure | Injured side | Mean percentage of uninjured side | Uninjured side | p -Value |
|---|---|---|---|---|
| Pronation (degrees) | 75 (70, 80) | 94 | 80 (75, 85) | <0.001 |
| Supination (degrees) | 75 (65, 85) | 90 | 80 (76, 90) | <0.001 |
| Volar flexion (degrees) | 55 (45, 64) | 70 | 75 (70, 80) | <0.001 |
| Dorsal extension (degrees) | 50 (40, 60) | 74 | 70 (60, 75) | <0.001 |
| Radial deviation (degrees) | 20 (15, 24) | 79 | 25 (20, 30) | <0.001 |
| Ulnar deviation (degrees) | 25 (20, 30) | 75 | 35 (30, 40) | <0.001 |
| Grip strength (kg) | 27 (20, 36.8) | 80 | 34 (29, 47.5) | <0.001 |
| Pinch grip (kg) | 4.5 (3.5, 6.0) | 90 | 5 (4.0, 6.5) | <0.001 |
| Key pinch grip (kg) | 7.5 (6, 9.5) | 89 | 8 (7, 11) | <0.001 |
| VAS at rest (mm) | 0 (0–0) | |||
| VAS during activity (mm) | 3 (1–5) | |||
| PRWE score (points) | 21 (5.6, 39.4) | |||
| DASH score (points) | 19.4 (4.5, 36,4) |
Abbreviations: DASH, Disabilities of the Arm, Shoulder and Hand; PRWE, Patient-Rated Wrist Evaluation; VAS, visual analog scale.
Note: the values are given as the median and interquartile range. P -values were assessed using Wilcoxon's rank sum test.
Table 3. X-ray findings 1 year postoperatively.
| Batra score (points) | Radial angle (degrees) | Radial length (mm) | Volar tilt (degrees) | Incongruency (mm) | Radioulnar joint (subluxation/dislocation) (mm) |
|---|---|---|---|---|---|
| 84.5 (70, 94) | 23.3 (19, 25) | 12 (10, 14) | 6 (0, 12) | 0.0 (0, 0) | 0 (0, 0) |
Note: the values are presented as median and interquartile range.
Table 4. Radiographic outcome according to the Batra score.
| Groups | Anatomical score | No. of cases |
|---|---|---|
| Excellent | 100–90 | 28 |
| Good | 89–80 | 22 |
| Fair | 79–70 | 20 |
| Poor | <70 | 5 |
There was no statistically significant difference between the four groups of radiographic Batra score (excellent, good, fair, and poor) and the outcome regarding PRWE, DASH, summarized flexion/extension, and VAS in activity. In addition, there was no statistically significant difference between the AO type C2 and C3 fractures and the outcome regarding PRWE, DASH, summarized flexion/extension, and VAS in activity. The 20 patients who did not complete the 1-year follow-up were contacted by a hand surgeon at our institution. The charts were reviewed, and 14 of them were reexamined clinically and radiographically 5 years postoperatively. Hardware removal was performed in 12/20 patients, but besides that, no secondary procedures had been performed. The mean Batra score of the 14 reexamined cases was 81 and the mean DASH score was 23, and there were no tendon ruptures during the 5-year postoperative period for these 20 cases.
Discussion
Our study shows a functional clinical and radiographic outcome after the combined dorsal and volar fixation of complex fractures of the distal part of the radius. ROM was somewhat reduced compared with the uninjured side, but the results were similar to those reported in previous studies on combined dorsal and volar plating. 15 22 The optimal operative treatment of DRFs remains debated. Most recently, volar locking plates have assumed a dominant role in stabilizing DRFs. However, a register-based study involving 3,666 patients showed that the shift in surgical treatment had no influence on the subjective outcome for the cohort. 23 A recent randomized study comparing fragment-specific fixation with volar locking plates in the treatment of DRFs found that both methods achieved a good and similar patient-reported outcome. 24
The median DASH and PRWE scores in our study were similar to those reported by other authors: DASH score was 16 and PRWE score was 20 for volar locking plates. 25
This subjective outcome can be considered favorable since all cases in our study were complex, unstable intra-articular fractures. Adverse events after volar locking plates include tendon rupture and loss of reduction. 26 One study on volar locking plates, with a majority of female patients, reported postoperative fracture collapse and screw penetration of the radiocarpal joint in 11/40 patients. 27 This could indicate that a volar plate alone is not always sufficient to maintain skeletal anatomy despite using locking screws. This is in line with our clinical experience and could support the use of a dorsal pi-plate. The patients in our study had a median VAS pain score of 0 at rest and 3 during activity. Several studies have linked articular incongruity to the development of degenerative changes. 13 28 A study by Ng and McQueen assessing the radiological predictors of functional outcome following DRFs recommends articular reconstruction with less than 2-mm step-off, restoration of the radius to within 2 mm of its normal length, and restoration of carpal alignment. 29 Radial length has been proposed as the most important factor affecting functional outcome, and a study on patients with DRFs treated either with closed reduction and a splint or external fixation found that better radiological results were associated with a better DASH score. 21 30 Restoration of volar angulation deformities to less than 20 degrees is important to maintain the normal range of forearm rotation. 31 The importance of anatomical reduction of DRFs and the importance of the distal oblique bundle of the interosseous membrane as a DRUJ stabilizer have been discussed by Moritomo. 32 In our study, we found a median articular incongruity of 0 mm and a radial length of 12 mm. A majority of the cases had a good/excellent radiographic Batra score. We believe this to be a good result considering that all fractures in the study were complex intra-articular AO type C2 and C3 fractures. In addition, a majority of the cases were AO type C3. Interestingly, we found no correlation between neither the patients radiographic Batra score 1 year postoperatively nor the AO fracture type and the outcome regarding VAS pain score during activity, summarized flexion/extension, DASH score, and PRWE score. The cause for this may be that a 1-year follow-up is too short or that a larger number of patients are needed. It may also be that today's outcome instruments are too crude to detect a significant difference. 33 The overall good radiographic results in our study are reflected in a hand grip strength of 80% of the uninjured side. This is in line with the results of Ring et al, who found a grip strength of 78% of the contralateral, uninjured side in combined dorsal and volar plating of DRFs using the pi-plate. 15 A significant association has been shown between AO type C fracture and complications in DRFs treated with volar locking plates. 34 One of the patients in our study underwent arthrodesis within the first year postoperatively. We believe that this is acceptable given this study's case mix with only AO type C fractures. Hardware removal, extensor tendon synovitis, and extensor tendon rupture have been a concern in previous studies on combined dorsal and volar plating of DRFs with the pi-plate. A Swiss study found extensor tendon ruptures in 5 out of 389 patients treated with the pi-plate and concluded that ruptures may be attributable to suboptimal placement of the implant. 17 However, tendon ruptures are also seen after volar plating of DRFs. A recent study found 5 flexor and 12 extensor tendon ruptures in a series of 576 patients. 34 In our study, there were no tendon ruptures during the study period. In addition, there were no ruptures in the 20 cases that did not complete the 1-year follow-up. One explanation may be that combined dorsal and volar plating has a learning curve. All surgeons at our institution are accustomed to the technique using a central volar approach. This enables visualization of the ulnar corner of the radius and optimal placement of the volar plate. The frequency of hardware removal in our patients seems reasonable given the advantages of combined dorsal and volar plate fixation to maintain reduction and facilitate rehabilitation.
A limitation of our study is that the patients were not randomized; however, data were collected prospectively as part of our department's clinical routine. Additionally, the attrition rates were acceptable, and the majority of the patients who did not complete the 1-year follow-up were reexamined. Perhaps, a longer follow-up is necessary to demonstrate a correlation between the degree of anatomical restoration radiographically and the clinical outcome.
In this group of patients with complex intra-articular fractures, there is no acceptable alternative to surgical treatment. The optimal way to internally stabilize a complex intra-articular DRF remains debated. We believe that anatomical restoration is essential in managing complex, intra-articular DRFs and combined dorsal and volar fixation is our treatment of choice in these cases. The question of optimal fixation should be addressed with randomized studies; this could further refine indications and clarify the role of combined dorsal and volar plate fixation in modern hand surgery.
Acknowledgments
The authors wish to thank Dr. Dominik Grzegorek for assistance, Ole Brus, MSc, for statistical advice, and Dr. Anders Amilon for help with assessing X-rays.
Conflict of Interest None declared.
Ethical Review Committee Statement
The study was approved by the regional ethical committee reference number 2016/455.
Location
Örebro, Sweden.
References
- 1.Court-Brown C M, Caesar B. Epidemiology of adult fractures: a review. Injury. 2006;37(08):691–697. doi: 10.1016/j.injury.2006.04.130. [DOI] [PubMed] [Google Scholar]
- 2.Brogren E, Petranek M, Atroshi I. Incidence and characteristics of distal radius fractures in a southern Swedish region. BMC Musculoskelet Disord. 2007;8:48. doi: 10.1186/1471-2474-8-48. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Handoll H H, Madhok R.Conservative interventions for treating distal radial fractures in adults Cochrane Database Syst Rev 2003; (02CD000314. [DOI] [PubMed] [Google Scholar]
- 4.Handoll H H, Madhok R.Surgical interventions for treating distal radial fractures in adults Cochrane Database Syst Rev 2003; (03CD003209. [DOI] [PubMed] [Google Scholar]
- 5.Mattila V M, Huttunen T T, Sillanpää P, Niemi S, Pihlajamäki H, Kannus P.Significant change in the surgical treatment of distal radius fractures: a nationwide study between 1998 and 2008 in Finland J Trauma 20117104939–942., discussion 942–943 [DOI] [PubMed] [Google Scholar]
- 6.Mellstrand-Navarro C, Pettersson H J, Tornqvist H, Ponzer S. The operative treatment of fractures of the distal radius is increasing: results from a nationwide Swedish study. Bone Joint J. 2014;96-B(07):963–969. doi: 10.1302/0301-620X.96B7.33149. [DOI] [PubMed] [Google Scholar]
- 7.Koval K J, Harrast J J, Anglen J O, Weinstein J N. Fractures of the distal part of the radius. The evolution of practice over time. Where's the evidence? J Bone Joint Surg Am. 2008;90(09):1855–1861. doi: 10.2106/JBJS.G.01569. [DOI] [PubMed] [Google Scholar]
- 8.Cui Z, Pan J, Yu B, Zhang K, Xiong X. Internal versus external fixation for unstable distal radius fractures: an up-to-date meta-analysis. Int Orthop. 2011;35(09):1333–1341. doi: 10.1007/s00264-011-1300-0. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Xie X, Xie X, Qin H, Shen L, Zhang C. Comparison of internal and external fixation of distal radius fractures. Acta Orthop. 2013;84(03):286–291. doi: 10.3109/17453674.2013.792029. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Li-hai Z, Ya-nan W, Zhi M et al. Volar locking plate versus external fixation for the treatment of unstable distal radial fractures: a meta-analysis of randomized controlled trials. J Surg Res. 2015;193(01):324–333. doi: 10.1016/j.jss.2014.06.018. [DOI] [PubMed] [Google Scholar]
- 11.Saito T, Nakamura T, Nagura T, Nishiwaki M, Sato K, Toyama Y. The effects of dorsally angulated distal radius fractures on distal radioulnar joint stability: a biomechanical study. J Hand Surg Eur Vol. 2013;38(07):739–745. doi: 10.1177/1753193412473036. [DOI] [PubMed] [Google Scholar]
- 12.Dario P, Matteo G, Carolina C et al. Is it really necessary to restore radial anatomic parameters after distal radius fractures? Injury. 2014;45 06:S21–S26. doi: 10.1016/j.injury.2014.10.018. [DOI] [PubMed] [Google Scholar]
- 13.Knirk J L, Jupiter J B. Intra-articular fractures of the distal end of the radius in young adults. J Bone Joint Surg Am. 1986;68(05):647–659. [PubMed] [Google Scholar]
- 14.Ring D, Jupiter J B. Operative fixation of fractures of the distal radius using the pi plate. Tech Hand Up Extrem Surg. 1997;1(02):125–130. doi: 10.1097/00130911-199706000-00009. [DOI] [PubMed] [Google Scholar]
- 15.Ring D, Prommersberger K, Jupiter J B. Combined dorsal and volar plate fixation of complex fractures of the distal part of the radius. J Bone Joint Surg Am. 2004;86-A(08):1646–1652. doi: 10.2106/00004623-200408000-00007. [DOI] [PubMed] [Google Scholar]
- 16.Grewal R, Perey B, Wilmink M, Stothers K. A randomized prospective study on the treatment of intra-articular distal radius fractures: open reduction and internal fixation with dorsal plating versus mini open reduction, percutaneous fixation, and external fixation. J Hand Surg Am. 2005;30(04):764–772. doi: 10.1016/j.jhsa.2005.04.019. [DOI] [PubMed] [Google Scholar]
- 17.Sánchez T, Jakubietz M, Jakubietz R, Mayer J, Beutel F K, Grünert J. Complications after Pi Plate osteosynthesis. Plast Reconstr Surg. 2005;116(01):153–158. doi: 10.1097/01.prs.0000169713.49004.7b. [DOI] [PubMed] [Google Scholar]
- 18.Muller M, Nazarian S, Koch P, Schatzker J. Berlin: Springer-Verlag; 1990. The comprehensive classification of fractures of long bones. [Google Scholar]
- 19.Mellstrand Navarro C, Ponzer S, Törnkvist H, Ahrengart L, Bergström G. Measuring outcome after wrist injury: translation and validation of the Swedish version of the patient-rated wrist evaluation (PRWE-Swe) BMC Musculoskelet Disord. 2011;12:171. doi: 10.1186/1471-2474-12-171. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.Atroshi I, Gummesson C, Andersson B, Dahlgren E, Johansson A. The disabilities of the arm, shoulder and hand (DASH) outcome questionnaire: reliability and validity of the Swedish version evaluated in 176 patients. Acta Orthop Scand. 2000;71(06):613–618. doi: 10.1080/000164700317362262. [DOI] [PubMed] [Google Scholar]
- 21.Batra S, Gupta A. The effect of fracture-related factors on the functional outcome at 1 year in distal radius fractures. Injury. 2002;33(06):499–502. doi: 10.1016/s0020-1383(01)00174-7. [DOI] [PubMed] [Google Scholar]
- 22.Krukhaug Y, Hove L M. Experience with the AO Pi-plate for displaced intra-articular fractures of the distal radius. Scand J Plast Reconstr Surg Hand Surg. 2004;38(05):293–296. doi: 10.1080/02844310410029516. [DOI] [PubMed] [Google Scholar]
- 23.Landgren M, Abramo A, Geijer M, Kopylov P, Tägil M. Similar 1-year subjective outcome after a distal radius fracture during the 10-year-period 2003-2012. Acta Orthop. 2017;88(04):451–456. doi: 10.1080/17453674.2017.1303601. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.Landgren M, Abramo A, Geijer M, Kopylov P, Tägil M.Fragment-specific fixation versus volar locking plates in primarily nonreducible or secondarily redisplaced distal radius fractures: a randomized controlled study J Hand Surg Am 20174203156–165..e1 [DOI] [PubMed] [Google Scholar]
- 25.Wright T W, Horodyski M, Smith D W. Functional outcome of unstable distal radius fractures: ORIF with a volar fixed-angle tine plate versus external fixation. J Hand Surg Am. 2005;30(02):289–299. doi: 10.1016/j.jhsa.2004.11.014. [DOI] [PubMed] [Google Scholar]
- 26.Teunis T, Mulder F, Nota S P, Milne L W, Dyer G S, Ring D. No difference in adverse events between surgically treated reduced and unreduced distal radius fractures. J Orthop Trauma. 2015;29(11):521–525. doi: 10.1097/BOT.0000000000000379. [DOI] [PubMed] [Google Scholar]
- 27.Knight D, Hajducka C, Will E, McQueen M. Locked volar plating for unstable distal radial fractures: clinical and radiological outcomes. Injury. 2010;41(02):184–189. doi: 10.1016/j.injury.2009.08.024. [DOI] [PubMed] [Google Scholar]
- 28.Catalano L W, III, Cole R J, Gelberman R H, Evanoff B A, Gilula L A, Borrelli J., Jr Displaced intra-articular fractures of the distal aspect of the radius. Long-term results in young adults after open reduction and internal fixation. J Bone Joint Surg Am. 1997;79(09):1290–1302. doi: 10.2106/00004623-199709000-00003. [DOI] [PubMed] [Google Scholar]
- 29.Ng C Y, McQueen M M. What are the radiological predictors of functional outcome following fractures of the distal radius? J Bone Joint Surg Br. 2011;93(02):145–150. doi: 10.1302/0301-620X.93B2.25631. [DOI] [PubMed] [Google Scholar]
- 30.Wilcke M K, Abbaszadegan H, Adolphson P Y.Patient-perceived outcome after displaced distal radius fractures. A comparison between radiological parameters, objective physical variables, and the DASH score J Hand Ther 20072004290–298., quiz 299 [DOI] [PubMed] [Google Scholar]
- 31.Cardoso R, Szabo R M. Wrist anatomy and surgical approaches. Hand Clin. 2010;26(01):1–19. doi: 10.1016/j.hcl.2009.08.009. [DOI] [PubMed] [Google Scholar]
- 32.Moritomo H. The distal interosseous membrane: current concepts in wrist anatomy and biomechanics. J Hand Surg Am. 2012;37(07):1501–1507. doi: 10.1016/j.jhsa.2012.04.037. [DOI] [PubMed] [Google Scholar]
- 33.MacDermid J C, Donner A, Richards R S, Roth J H. Patient versus injury factors as predictors of pain and disability six months after a distal radius fracture. J Clin Epidemiol. 2002;55(09):849–854. doi: 10.1016/s0895-4356(02)00445-6. [DOI] [PubMed] [Google Scholar]
- 34.Thorninger R, Madsen M L, Wæver D, Borris L C, Rölfing J HD. Complications of volar locking plating of distal radius fractures in 576 patients with 3.2 years follow-up. Injury. 2017;48(06):1104–1109. doi: 10.1016/j.injury.2017.03.008. [DOI] [PubMed] [Google Scholar]


