Overview
Introduction
Open treatment of extra-articular and intra-articular distal humeral fractures can be effectively accomplished through an extensor mechanism-on approach.
Step 1: Preoperative Planning
Assess all images for multiplane fracture lines involving the capitellum or trochlea.

Step 2: Operative Setup
Verify with fluoroscopy that the patient and arm positions allow for adequate imaging of the distal part of the humerus.
Step 3: Surgical Approach
Perform medial and lateral arthrotomies posterior to the collateral ligament complexes and excise the intra-articular fat pad and posterior aspect of the capsule.





Step 4: Fracture Reduction and Provisional Fixation
Reduce the distal humeral fragments anatomically under direct visualization posteriorly and indirectly with fluoroscopy using the intact sigmoid notch as a template for reduction.
Step 5: Definitive Fixation
Place multiple screws distally through the plates medially and laterally; each screw should be of maximal length and engage the opposite column.
Step 6: Wound Closure and Postoperative Management
Remove the dressing on postoperative day two and begin full active-assisted elbow range of motion and grip-strengthening therapy program.
Results
In our series of thirty-seven patients12, all fractures healed primarily with a median motion arc of 126° (range, 60° to 141°). The median triceps strength loss was 10% (range, 0% to 49%).
What to Watch For
Introduction
Open treatment of extra-articular and intra-articular distal humeral fractures can be effectively accomplished through an extensor mechanism-on approach.
The optimal approach for open reduction and internal fixation (ORIF) of distal humeral fractures that provides adequate visualization of the distal part of the humerus and articular surface but minimizes soft-tissue and extensor mechanism disruption is still a topic of controversy. Traditionally, these fractures have been managed operatively with various extensor-mechanism-disrupting approaches1-7, which are often associated with delayed union or nonunion of the olecranon, triceps muscle weakness, and osteotomy-related prominent implants8-10. We present a detailed description of the surgical technique and the experience of the two senior authors (M.A.M. and E.V.F.), who utilize the approach described by Schildhauer et al. in 20036.
The technique described here is an anconeus-muscle-preserving approach with bicolumnar visualization through medial and lateral windows that avoids disruption of the triceps muscle insertion or the olecranon. The intact sigmoid notch serves as a template for reduction. The distal part of the humerus is anatomically reduced with direct visualization posteriorly and indirect visualization with fluoroscopy. Provisional Kirschner-wire fixation is then converted to definitive parallel or orthogonal plate fixation.
The application of this approach to more simple fractures provides the surgeon with the experience needed to successfully reconstruct increasingly complex fracture patterns. The decision to apply the technique to more complex fracture types with substantial intra-articular comminution, such as AO type-C3 fractures, can be made on a case-by-case basis after careful review of imaging studies and consideration of the surgeon’s familiarity with the approach. Fracture patterns with complex articular comminution pose a substantial challenge to successful reconstruction and the ultimate patient outcome regardless of the surgical approach used. The approach described below can be easily converted to an olecranon osteotomy without additional soft-tissue injury if the reduction cannot be obtained or adequately assessed.
The six steps of the procedure include:
Step 1: Preoperative planning
Step 2: Operative setup
Step 3: Surgical approach
Step 4: Fracture reduction and provisional fixation
Step 5: Definitive fixation
Step 6: Wound closure and postoperative management
Step 1: Preoperative Planning
Assess all images for multiplane fracture lines involving the capitellum or trochlea.
Obtain preoperative anteroposterior, lateral, and oblique radiographs of the elbow.
In cases in which radiographs reveal comminution or more than a simple intra-articular fracture line, obtain computed tomography (CT) scans in the axial, coronal, and sagittal planes with or without three-dimensional reconstructions to better define fracture complexity and configuration (Figs. 1-A and 1-B).
Assess all images for multiplane fracture lines involving the capitellum or trochlea, as these lines can increase the complexity of the reconstruction of the articular surface in the setting of articular surface comminution.
Fig. 1-A.

CT three-dimensional reconstruction coronal view used to better define fracture complexity and configuration.
Fig. 1-B.
CT three-dimensional reconstruction lateral view used to better define fracture complexity and configuration.
Step 2: Operative Setup
Verify with fluoroscopy that the patient and arm positions allow for adequate imaging of the distal part of the humerus.
Once the patient is under general anesthesia and a Foley catheter has been placed under sterile conditions, roll the patient into the lateral decubitus position supported with a beanbag and with the operative arm up.
Place an axillary roll just distal to the axilla and pad the dependent leg to protect the peroneal nerve, ankle, and osseous prominences.
Flex the uninvolved shoulder 90°, externally rotate it 90°, pad it appropriately, and secure it to a standard arm-board.
Allow the operative arm to rest over a well-padded support, allowing at least 90° of elbow flexion (Fig. 2).
Roll the patient’s torso slightly forward to improve clearance of the elbow from the edge of the operating table.
Verify with fluoroscopy that patient and arm positions allow for adequate imaging of the distal part of the humerus (Figs. 3-A and 3-B).
Place a non-sterile U-drape around the upper arm as far proximally as possible.
After standard preparation and draping of the operative arm, a sterile tourniquet may or may not be utilized depending on the fracture configuration and humeral length; the tourniquet should be placed as far proximally as possible.
Administer preoperative antibiotics prior to tourniquet inflation and incision.
Fig. 2.
The operative arm over a well-padded support.
Fig. 3-A.
Anteroposterior c-arm image used to verify that the patient and arm positions allow for adequate imaging of the distal part of the humerus.
Fig. 3-B.
Lateral c-arm image used to verify that the patient and arm positions allow for adequate imaging of the distal part of the humerus.
Step 3: Surgical Approach
Perform medial and lateral arthrotomies posterior to the collateral ligament complexes and excise the intra-articular fat pad and posterior aspect of the capsule.
Longitudinally incise the skin slightly lateral to the midline posteriorly (Figs. 4-A and 4-B), extending 3 to 4 cm distal to the olecranon tip, and elevate full-thickness fasciocutaneous flaps medially and laterally (Fig. 4-C).
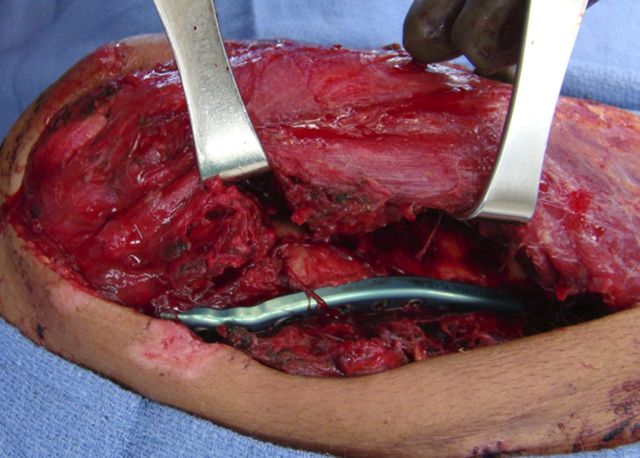
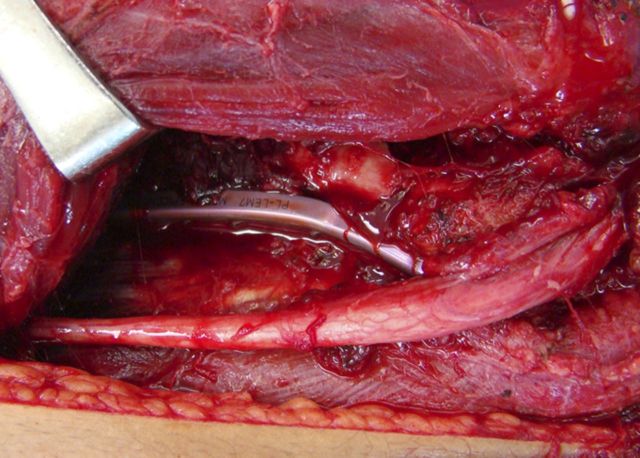
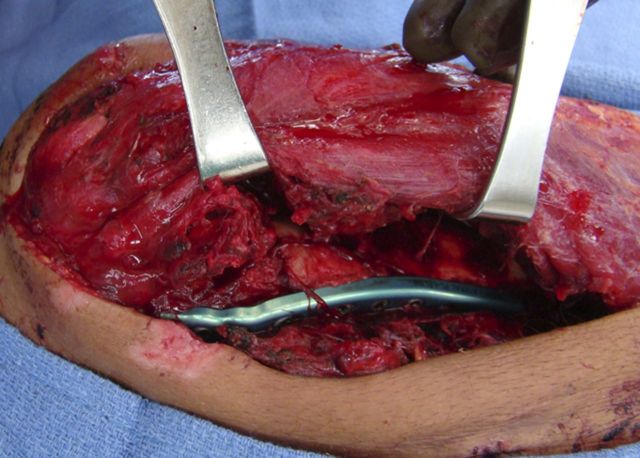
Medially, identify the ulnar nerve along the intermuscular septum and dissect along its course proximally to the arcade of Struthers and distally to the first motor branch in the flexor carpi ulnaris muscle belly (Figs. 5-A and 5-B).
Decompress the ulnar nerve in situ and allow it to rest in this position at the time of closure, or transpose it to an anterior subcutaneous position if implant proximity will cause postoperative irritation. If the nerve is transposed, eliminate any potential nerve constrictors such as the medial intermuscular septum.
Elevate the medial and lateral borders of the triceps muscle from their respective intermuscular septae.
Laterally, continue the distal dissection anterior to the anconeus muscle, allowing it to be elevated along with the triceps muscle and preserving its neurovascular supply (Figs. 5-C and 5-D).
Use areas where the triceps muscle has been buttonholed by the fracture to facilitate reduction and ultimately repair these with a figure-of-eight absorbable suture. A longitudinal split in the triceps tendon overlying the olecranon fossa may also be utilized for the same purpose.
Free the triceps muscle from the posterior aspect of the humerus in an extraperiosteal fashion and connect the medial and lateral windows with blunt dissection.
Perform medial and lateral elbow arthrotomies posterior to the collateral ligament complexes and excise the intra-articular fat pad and posterior aspect of the capsule. This will allow visualization of roughly 60% of the overall articular cartilage surface of the distal part of the humerus (Figs. 5-D and 6-B).
You can release the posterior band of the ulnar collateral ligament medially to allow better trochlea visualization without compromising elbow stability.
Fig. 4-A.

Photograph showing the dorsal longitudinal incision line.
Fig. 4-B.
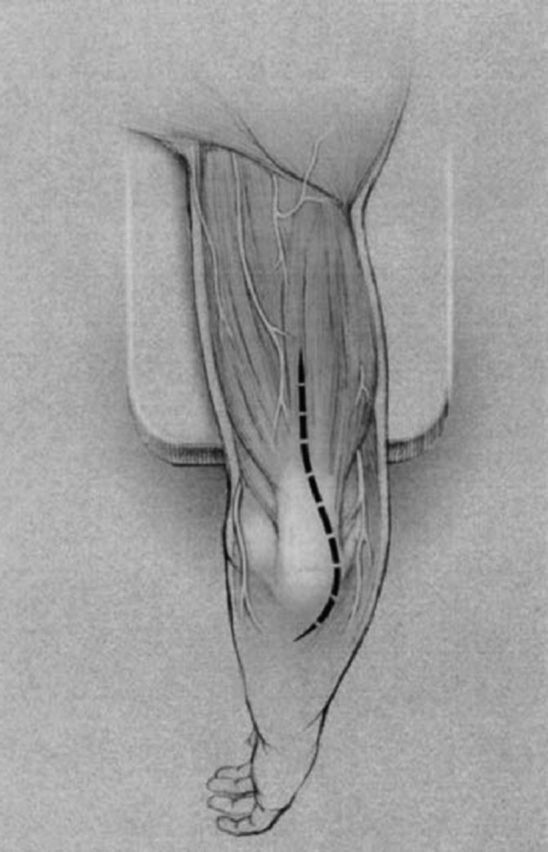
Illustration of the dorsal incision. (Reproduced, with permission, from: Schildhauer TA, Nork SE, Mills WJ, Henley MB. Extensor mechanism-sparing paratricipital posterior approach to the distal humerus. J Orthop Trauma. 2003 May;17[5]:374-8.)
Fig. 4-C.

Full-thickness medial and lateral fasciocutaneous flaps.
Fig. 5-A.

Photograph of the medial exposure identifying and protecting the ulnar nerve.
Fig. 5-B.

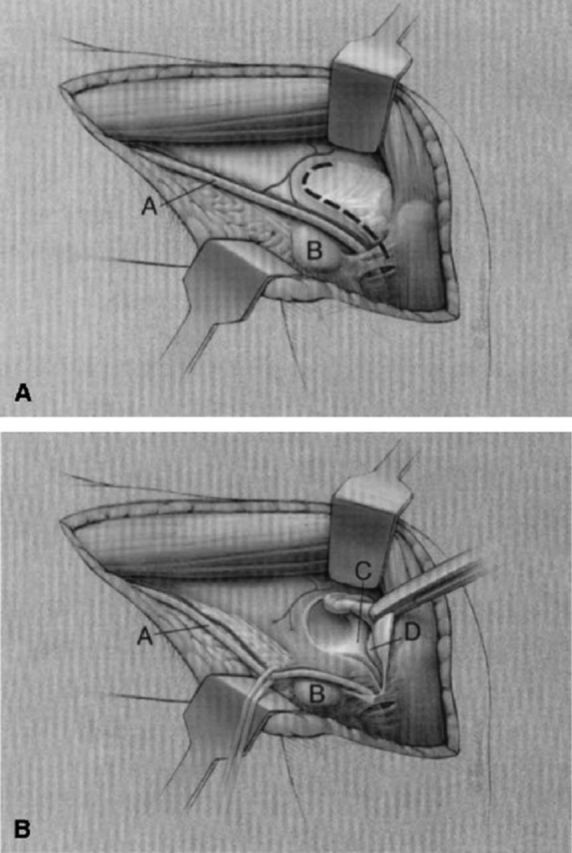
Illustration of the medial exposure. A = ulnar nerve, B = medial epicondyle, C = trochlea, D = olecranon tip, and dotted line = arthrotomy. (Reproduced, with permission, from: Schildhauer TA, Nork SE, Mills WJ, Henley MB. Extensor mechanism-sparing paratricipital posterior approach to the distal humerus. J Orthop Trauma. 2003 May;17[5]:374-8.)
Fig. 5-C.

Illustration of the lateral exposure. A = radial nerve, B = lateral epicondyle, C = reflected anconeus muscle and capsule, D = trochlea, and E = olecranon tip. (Reproduced, with permission, from: Schildhauer TA, Nork SE, Mills WJ, Henley MB. Extensor mechanism-sparing paratricipital posterior approach to the distal humerus. J Orthop Trauma. 2003 May;17[5]:374-8.)
Fig. 5-D.
Lateral distal humeral fracture.
Fig. 6-B.
Placement of a sponge to allow ulnohumeral joint distraction and visualization.
Step 4: Fracture Reduction and Provisional Fixation
Reduce the distal humeral fragments anatomically under direct visualization posteriorly and indirectly with fluoroscopy using the intact sigmoid notch as a template for reduction.
Reduce the distal humeral fragments anatomically under direct visualization posteriorly and indirectly with fluoroscopy using the intact sigmoid notch as a template for reduction (Fig. 6-A).
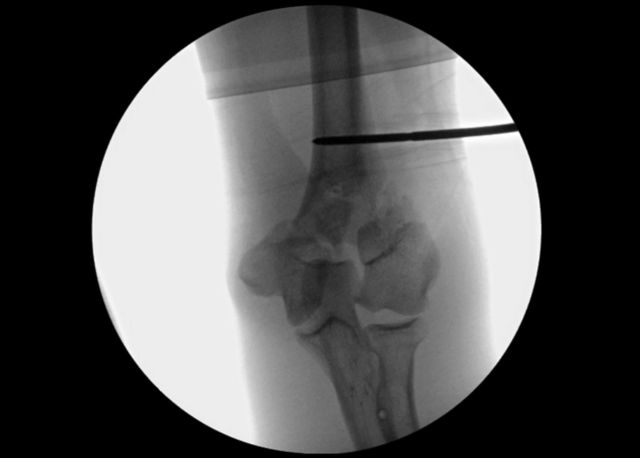
A sponge or 0.25-in (6.35-mm) Penrose drain can be placed into the ulnohumeral joint to allow distraction of the joint by pulling distally on the olecranon via the sigmoid notch to aid in visualization and facilitate the reduction through ligamentotaxis (Fig. 6-B). Extreme flexion can also be helpful to further visualize the posterior aspect of the distal part of the humerus.
Reduce and provisionally fix the fracture fragments with large clamps and smooth Kirschner wires strategically to achieve the desired stable provisional fixation and not interfere with initial plate and screw placement (Fig. 6-C). Small fracture fragments may require definitive fixation by threaded wires, absorbable pins, or small screws.
Bring the c-arm parallel to the bed from either the “foot” or the “head” of the bed, and verify reduction in orthogonal and oblique planes to assess for articular surface step-off. Obtain lateral images of the elbow by swinging the c-arm through its arc so that it is not necessary to internally or externally rotate the shoulder and place the fracture reduction at risk.
Approximate the reconstructed distal articular block to the humeral diaphysis.
In some fracture patterns, it can be helpful to reduce the column with the simplest fracture pattern first to its respective diaphyseal component (e.g., restoring the medial column) and then reduce the remaining condyle to the previously reduced column.
Kirschner wires placed as joysticks in each condyle can be particularly helpful in derotating a condylar segment that is rotated by its collateral ligament.
Fig. 6-A.
Provisional fracture reduction and fixation.
Fig. 6-C.
Anteroposterior c-arm image verifying provisional reduction.
Step 5: Definitive Fixation
Place multiple screws distally through the plates medially and laterally; each screw should be of maximal length and engage the opposite column.
Apply distal humeral plates and provisionally secure them with Kirschner wires in either parallel or orthogonal orientation depending on your preference, your philosophy regarding distal humeral fracture fixation, and the fracture pattern.
Proximally, secure each plate to bone with a screw through a slotted hole.
Place multiple screws distally through the plates medially and laterally. Each screw should be of maximal length and engage the opposite column11.
Often, one long “spool” screw can be placed through or outside of the plate to increase stability. Ultimately, there will be some interdigitation of screws in the “spool.”
Loosen one of the previously placed slotted screws a few turns, and apply a large bone clamp distally on the same side as the screw and proximally on the contralateral side to achieve compression in the supracondylar area.
Apply a proximal screw in compression mode and place and tighten the remainder of the diaphyseal screws (Figs. 7-A and 7-B). Compression should be avoided in cases of substantial comminution.
Apply the same technique to the contralateral plate.
Remove provisional Kirschner wires, identify any intra-articular implants, and assess fixation stability and smooth motion arcs prior to closure (Figs. 8-A and 8-B).
Fig. 7-A.
Anteroposterior c-arm image of definitive fixation.
Fig. 7-B.
Lateral c-arm image of definitive fixation.
Fig. 8-A.
Medial definitive fixation.
Fig. 8-B.
Lateral definitive fixation.
Step 6: Wound Closure and Postoperative Management
Remove the dressing on postoperative day two and begin full active-assisted elbow range of motion and grip-strengthening therapy program.
Repair the triceps fascia laterally with an absorbable suture followed by skin closure.
You can leave the medial side as is to allow the nerve to “find” its position.
If an ulnar nerve transposition is performed, placement of the nerve depends on surgeon preference.
A suction drain is not typically required.
Place the elbow in a bulky dressing with the elbow in full extension.
Remove the dressing on postoperative day two and begin full active-assisted elbow range of motion and grip-strengthening therapy program.
Obtain routine postoperative radiographs at regular intervals to assess for fracture union.
Results
In our series of thirty-seven patients12, all fractures healed primarily with a median motion arc of 126° (range, 60° to 141°). The median triceps strength loss was 10% (range, 0% to 49%).
What to Watch For
Indications
Extra-articular and intra-articular distal humeral fractures
AO type-C1 and C2 intra-articular distal humeral fractures
Select type-C3 intra-articular distal humeral fractures
Contraindications
Elbow osteoarthritis with severe comminution of the articular surface
Severely comminuted type-C3 intra-articular distal humeral fractures, particularly those with multiplane patterns
Coronal shear fracture patterns
Pitfalls & Challenges
The decision to apply the technique to more complex type-C3 fractures should be made on a case-by-case basis after careful review of imaging studies and consideration of the surgeon’s familiarity with this approach.
Ulnar or radial nerve neuropathy. Take care to identify, carefully dissect, and protect the ulnar and radial nerves throughout the procedure. Higher fracture patterns, particularly in smaller female patients, may require formal radial nerve exploration in addition to ulnar nerve exploration.
Coronal shear fractures involving the trochlea and capitellum often require separate fixation with headless screws or threaded wires. These fractures can be very challenging to address with this surgical technique, and we do not recommend its use for this fracture pattern.
Reduction cannot be obtained or adequately assessed. An advantage of this approach is the ease of converting to an olecranon osteotomy without additional soft-tissue trauma.
Utilization of a longitudinal split in the triceps tendon overlying the olecranon fossa can be helpful for provisional and definitive reductions.
Clinical Comments
What type-C3 fractures patterns are amenable to this approach versus those that exceed its limitations?
Should the ulnar nerve be transposed?
Based on an original article: J Bone Joint Surg Am. 2012 Mar 21;94(6):548-53.
Disclosure: None of the authors received payments or services, either directly or indirectly (i.e., via his or her institution), from a third party in support of any aspect of this work. One or more of the authors, or his or her institution, has had a financial relationship, in the thirty-six months prior to submission of this work, with an entity in the biomedical arena that could be perceived to influence or have the potential to influence what is written in this work. No author has had any other relationships, or has engaged in any other activities, that could be perceived to influence or have the potential to influence what is written in this work. The complete Disclosures of Potential Conflicts of Interest submitted by authors are always provided with the online version of the article.
References
- 1. Anglen J. Distal humerus fractures. J Am Acad Orthop Surg. 2005 Sep;13(5):291-7. [DOI] [PubMed] [Google Scholar]
- 2. Bryan RS Morrey BF. Extensive posterior exposure of the elbow. A triceps-sparing approach. Clin Orthop Relat Res. 1982 Jun;166:188-92. [PubMed] [Google Scholar]
- 3. Canale ST Beaty JH, Campbell’s operative orthopaedics. 11th ed. Philadelphia: Mosby; 2008. [Google Scholar]
- 4. Cassebaum WH. Operative treatment of T and Y fractures of the lower end of the humerus. Am J Surg. 1952 Mar;83(3):265-70. [DOI] [PubMed] [Google Scholar]
- 5. Mühldorfer-Fodor M Bekler H Wolfe VM McKean J Rosenwasser MP. Paratricipital-triceps splitting “two-window” approach for distal humerus fractures. Tech Hand Up Extrem Surg. 2011 Sep;15(3):156-61. [DOI] [PubMed] [Google Scholar]
- 6. Schildhauer TA Nork SE Mills WJ Henley MB. Extensor mechanism-sparing paratricipital posterior approach to the distal humerus. J Orthop Trauma. 2003 May;17(5):374-8. [DOI] [PubMed] [Google Scholar]
- 7. Zlotolow DA Catalano LW 3rd Barron OA Glickel SZ. Surgical exposures of the humerus. J Am Acad Orthop Surg. 2006 Dec;14(13):754-65. [DOI] [PubMed] [Google Scholar]
- 8. Coles CP Barei DP Nork SE Taitsman LA Hanel DP Bradford Henley M. The olecranon osteotomy: a six-year experience in the treatment of intraarticular fractures of the distal humerus. J Orthop Trauma. 2006 Mar;20(3):164-71. [DOI] [PubMed] [Google Scholar]
- 9. McKee MD Wilson TL Winston L Schemitsch EH Richards RR. Functional outcome following surgical treatment of intra-articular distal humeral fractures through a posterior approach. J Bone Joint Surg Am. 2000 Dec;82-A(12):1701-7. [DOI] [PubMed] [Google Scholar]
- 10. Ring D Gulotta L Chin K Jupiter JB. Olecranon osteotomy for exposure of fractures and nonunions of the distal humerus. J Orthop Trauma. 2004 Aug;18(7):446-9. [DOI] [PubMed] [Google Scholar]
- 11. Sanchez-Sotelo J Torchia ME O’Driscoll SW. Complex distal humerus fractures: internal fixation with a principle-based parallel-plate technique. J Bone Joint Surg Am. 2007 May;89(5):961-9. [DOI] [PubMed] [Google Scholar]
- 12. Erpelding JM Mailander A High R Mormino MA Fehringer EV. Outcomes following distal humeral fracture fixation with an extensor mechanism-on approach. J Bone Joint Surg Am. 2012 Mar 21;94(6):548-53. [DOI] [PubMed] [Google Scholar]