Abstract
Objective
To evaluate the frequency and morphometry of the Wrisberg's ligament and its relationships with the posterior cruciate ligament's femoral insertion.
Study design
Controlled laboratory study.
Methods
24 unpaired knee pieces, 12 right and 12 left were submitted to a deep dissection of the Wrisberg and posterior cruciate ligaments. The pieces were photographed with a digital camera and ruler; the Image J software was used to measure the ligaments’ insertion areas, in square millimeters.
Results
The Wrisberg ligament was present in 91.6% of the studied pieces. In those its shape was elliptical in 12 pieces (54.54%). In 68% of the knees, the WL insertion was proximal to the medial intercondilar ridge, close to the PCL posteromedial bundle. The average area for the WL was 20.46 ± 6.12 mm2. This number corresponded to 23.3% of the PCL's average area.
Conclusions
WL ligament is a common structure in knees. There is a wide variation of its insertion area. Proportionally to the PCL's insertion area the WL ones suggests that it may contribute to the posterior stability of the knee joint.
Keywords: Femur, Posterior cruciante ligament, Tibial menisci
Resumo
Objetivo
Avaliar a frequência e a morfometria do ligamento meniscofemoral de Wrisberg e a relação de suas inserções femorais com aquelas do ligamento cruzado posterior (LCP).
Desenho do estudo
Estudo laboratorial controlado.
Métodos
Foram feitas dissecções minuciosas das inserções femorais dos ligamentos de Wrisberg (LW) e do LCP em 24 peças anatômicas de joelhos. As peças foram fotografadas com uma câmera digital e marcador milimetrado; o programa Image J foi usado para medir a área das inserções ligamentares, em milímetros quadrados.
Resultados
O LW esteve presente em 91.6% das peças estudadas. Nessas, seu formato foi elíptico em 12 peças (54.54%). Em 68% dos joelhos a inserção do LW esteve proximal à crista intercondilar medial, próximo à banda posteromedial do LCP. A área média da inserção femoral do LW foi de 2046 ± 6.12 mm2, o que correspondeu a 23.3% da área de inserção do LCP.
Conclusões
O LW é estrutura frequente nos joelhos, com grande variabilidade de sua área média. Proporcionalmente ao LCP, sua área média sugere que esse ligamento pode contribuir para a estabilidade posterior do joelho.
Palavras-chave: Fêmur, Ligamento cruzado posterior, Meniscos tibiais
Introduction
The posterior meniscofemoral ligament, or Wrisberg ligament, goes from the lateral aspect of the medial femoral condyle to the posterior cornu of the lateral meniscus. It has a posterior location that is very close to the posterior cruciate ligament (PCL), with a slightly more oblique direction (Fig. 1). Its frequency of occurrence in humans ranges from 90% to 93%.1, 2, 3
Fig. 1.

Deep dissection showing the posterior cruciate ligament (PCL), Humphrey meniscofemoral ligament (H), Wrisberg ligament (W) and lateral meniscus (LM).
The first description of the meniscofemoral ligament in the medical literature was made by Humphrey in 1858. In 1899, Poirier and Charpy reported two distinct structures that started from the posterior cornu of the lateral meniscus and involved the PCL (apud Gupte et al.4).
Studies conducted more recently have also shown the Wrisberg ligament forms part of a complex together with the PCL and remains tense during knee extension. It contributes toward posterior stability and toward harmonious movement of the lateral meniscus during flexion and extension of the knee.5, 6
Together with the anterior meniscofemoral ligament, it acts as a secondary limiter of posterior translation of the tibia, and it accounts for 35–45% of this action with the knee flexed at 90°.6, 7
The objective of our study was to evaluate the frequency of occurrence of the Wrisberg ligament in the specimens analyzed, the shape and area of its femoral insertion and its relationship with the PCL. In this manner, we hoped to be able to contribute toward expanding the anatomical knowledge of the posterior stabilizing complex of the knee.
Methods
Twenty-four unpaired anatomical specimens of adult knees from cadavers were studied (12 right knees and 12 left knees). All of the specimens presented intact cruciate ligaments and joint cartilage. None of the knees presented any signs of arthrosis. The specimens used had been fixed in 10% formol and were conserved in a mixture of 2.5% phenol, 2.5% formol and 1% sodium chloride.
We performed detailed dissection of the posterior aspect of the knee using a scalpel with a No. 11 blade. We isolated the Wrisberg ligament, the menisci and the PCL, and we also identified the anterolateral and posteromedial bands of the PCL.
After isolating the Wrisberg ligament and the bands of the PCL, we divided the distal femur along the sagittal plane, so as to have better viewing of the structures, and we delimited their areas of insertion.
We used a millimeter ruler placed as the same level as the insertions and we photographed the specimens using a Canon EOS Rebel T1i digital camera (Fig. 2). Since the insertions of the Wrisberg ligament and the PCL bands are not located exactly in the same plane, the images were produced as perpendicularly as possible to the anatomical structures, according to the region to be studied.
Fig. 2.
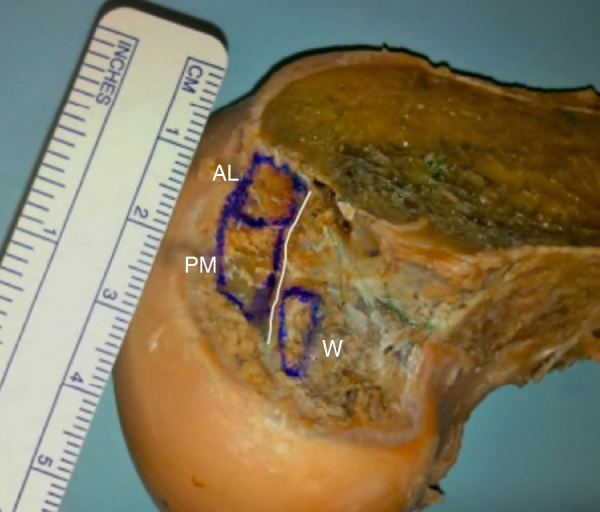
Lateral view of the medial femoral condyle showing the medial intercondylar ridge, the femoral insertions of the Wrisberg ligament (W) and the anterolateral (AL) and posteromedial (PM) bands of the PCL.
The Image J software was used to calculate the measurements of interest, in millimeters or in square millimeters.
Results
The Wrisberg ligament was identified in 22 of the 24 specimens analyzed (91.6%). In these, its shape was elliptical in 12 specimens (54.54%).
Its mean area of insertion was 20.26 ± 6.12 mm2 and the mean area of insertion of the PCL was 87.80 ± 28.21 mm2. The mean areas of insertion of the anterolateral and posteromedial bands were, respectively, 47.13 ± 19.14 and 40.67 ± 16.19 mm2.
In 68% of the knees, the insertion of the Wrisberg ligament was proximal to the medial intercondylar ridge. In most of the specimens (90.9%), the Wrisberg ligament was closer to the posteromedial band than to the anterolateral band (mean distances between the insertion centers of 9.15 mm and 14.18 mm, respectively), although in two specimens the situation was the inverse, probably because of an anatomical variation in the layout of the PCL bands that predisposed toward this situation (Fig. 3).
Fig. 3.

Lateral view of the medial femoral condyle showing the center of the femoral insertion of the Wrisberg ligament (W) and the anterolateral (AL) and posteromedial (PM) bands of the PCL.
The mean distances from the center of the area of insertion of the Wrisberg ligament to the posterior and distal joint cartilage of the medial femoral condyle were 7.05 mm and 10.16 mm, respectively. Table 1 shows the means found in our study.
Table 1.
Quantitative measurements on the femoral insertions of the Wrisberg ligament and their relationship with the posterior cruciate ligament.
| Column 1 |
Column 2 |
Column 3 |
Column 5 |
Column 6 |
Column 7 |
Column 8 |
Column 9 |
Column 10 |
Column 11 |
Column 12 |
Column 13 |
|---|---|---|---|---|---|---|---|---|---|---|---|
| Area (cm2) | Greatest diameter (mm) | Distance to PM band (mm) | Distance to AL band (mm) | Distance to PCL center (mm) | Distance to posterior cart. (mm) | Distance to distal cart. (mm) | W/PM ratio (% area) | W/AL ratio (% area) | W/PCL ratio (% area) | ||
| 2 | D | 21.50 | 5.20 | 9.33 | 14.60 | 13.16 | 4.48 | 9.00 | 39.95 | 28.75 | 16.72 |
| 3 | E | 17.93 | 5.86 | 9.40 | 14.98 | 10.86 | 5.23 | 11.64 | 22.43 | 47.17 | 15.20 |
| 4 | E | 24.38 | 7.21 | 7.23 | 11.48 | 9.23 | 9.09 | 10.40 | 91.35 | 85.21 | 44.09 |
| 5 | E | 22.13 | 7.55 | 5.91 | 10.21 | 8.66 | 8.72 | 13.84 | 55.39 | 46.14 | 25.17 |
| 6 | E | 19.60 | 5.93 | 9.46 | 14.53 | 11.88 | 5.74 | 12.70 | 56.55 | 51.93 | 27.07 |
| 7 | D | 16.15 | 4.75 | 7.41 | 13.87 | 10.34 | 4.97 | 4.75 | 55.54 | 54.76 | 27.57 |
| 8 | D | 22.24 | 5.26 | 7.52 | 14.77 | 11.89 | 7.27 | 8.20 | 77.22 | 47.30 | 29.33 |
| 9 | E | 24.07 | 5.02 | 11.82 | 18.63 | 14.62 | 6.72 | 13.28 | 41.50 | 26.74 | 16.26 |
| 10 | D | 21.16 | 6.44 | 7.94 | 11.89 | 9.74 | 7.30 | 7.91 | 60.32 | 51.67 | 27.83 |
| 11 | D | 37.89 | 8.31 | 12.26 | 17.88 | 15.32 | 7.19 | 13.28 | 73.34 | 60.25 | 33.08 |
| 12 | D | 15.84 | 4.57 | 6.86 | 11.10 | 8.75 | 6.79 | 7.50 | 67.35 | 62.91 | 32.53 |
| 13 | D | 18.47 | 5.85 | 9.94 | 12.15 | 10.57 | 6.47 | 7.09 | 44.68 | 37.31 | 20.33 |
| 14 | D | 25.98 | 7.53 | 9.56 | 16.87 | 13.73 | 5.19 | 11.63 | 75.15 | 36.19 | 24.43 |
| 15 | E | 26.37 | 6.29 | 11.80 | 18.49 | 14.47 | 4.10 | 13.75 | 68.91 | 63.01 | 32.91 |
| 17 | E | 12.44 | 4.96 | 6.77 | 12.44 | 10.14 | 7.94 | 10.42 | 38.67 | 28.96 | 16.56 |
| 18 | E | 29.27 | 8.87 | 9.51 | 16.35 | 13.28 | 11.58 | 12.16 | 51.14 | 77.62 | 30.83 |
| 19 | E | 14.93 | 4.80 | 12.10 | 12.23 | 11.78 | 6.99 | 11.18 | 70.89 | 34.67 | 23.28 |
| 20 | E | 13.90 | 4.60 | 12.74 | 19.81 | 16.48 | 5.50 | 12.11 | 23.97 | 28.96 | 13.11 |
| 21 | D | 18.02 | 4.83 | 11.47 | 10.21 | 9.64 | 11.29 | 12.06 | 64.36 | 43.95 | 26.12 |
| 22 | D | 21.58 | 9.40 | 7.52 | 13.89 | 10.70 | 5.95 | 3.50 | 86.32 | 89.92 | 44.04 |
| 23 | E | 13.37 | 4.67 | 8.02 | 15.19 | 11.60 | 7.46 | 8.52 | 38.20 | 44.57 | 20.57 |
| 24 | E | 12.91 | 3.90 | 6.67 | 10.95 | 8.71 | 9.12 | 8.61 | 19.86 | 19.27 | 9.78 |
| Mean | 20.46 | 5.99 | 9.15 | 14.18 | 11.64 | 7.05 | 10.16 | 55.59 | 48.51 | 25.31 | |
| SD | 6.12 | 1.53 | 20.22 | 18.93 | 9.03 |
Discussion
The number of studies relating to the PCL has increased substantially in the medical literature. The structures of the posterior complex, such as the Wrisberg ligament, may equally gain in importance within reconstructive surgical procedures.
The detailed specific function of the Wrisberg ligament is still not fully understood. Anatomical studies have suggested that it is important in relation to the harmony of normal mobility of the lateral meniscus and lateral femoral condyle.8, 9, 10, 11 Thus, it would also contribute indirectly toward the health of the lateral compartment of the knee joint.12
In our study, the Wrisberg ligament was found in 91.6% of the knees evaluated. In anatomical studies in the literature, its incidence may range from 35% to 76%.9, 13, 14, 15, 16 It is possible that we found the Wrisberg ligament in a greater percentage of specimens than was seen in other studies because our dissection was done in a very detailed manner, using a scalpel with a No. 11 blade, with isolation of the structures always starting from the posterior cornu of the lateral meniscus.
Cho et al.3 and Watanabe et al.17 identified the Wrisberg ligament in 66% and 93% of the magnetic resonance images evaluated, respectively. These percentages would probably have been even higher if equipment of greater resolution had been used.
In 68% of the knees of our sample, the insertion of the Wrisberg ligament was proximal to the medial intercondylar ridge. However, according to Gupte et al.,4 and also Yamamoto and Hirohata,13 the Wrisberg ligament was always in a proximal location in relation to the medial intercondylar ridge.
In our evaluation, the mean area of insertion of the Wrisberg ligament was 20.46 ± 6.12 mm2 and the mean area of insertion of the PCL was 87.80 ± 28.21 mm2. The mean areas of insertion of the anterolateral and posteromedial bands were, respectively, 47.13 ± 19.14 and 40.67 ± 16.19 mm2. Thus, the mean area of the Wrisberg ligament corresponded to 23.3% of the area of the PCL, 43.41% of the area of the anterolateral band and 50.3% of the area of the posteromedial band.
According to Takahashi et al.,16 the mean area of insertion of the Wrisberg (W) ligament was 39.4 ± 13.7 mm2 and of the PCL, 122.6 ± 50.1 mm2. The mean area of insertion of the anterolateral (AL) band was 58.0 ± 25.4 mm2 and of the posteromedial (PM) band, 64.6 ± 24.7 mm2. According to these authors, the W/PCL, W/AL and W/PM area ratios were, respectively, 32.13%, 67.93% and 60.99%.
The areas obtained in our study were smaller possibly because in addition to the likely sex and ethnicity-related variations among the samples studied, we exclusively delimited the bone sites for femoral insertion of the ligaments, with careful dissection, without including the fibrous expansions that are inserted on the periphery of the bone sites for the insertions.
In our study, like in the study by Takahashi et al.,16 we found a high standard deviation for the mean area of insertion of the Wrisberg ligament in the femur (29.91% and 34.77% of the total area, respectively). This probably demonstrates that there were considerable differences between the individual measurements within the sample.
Our study has some limitations: the number of knees studied might be considered small, given the great anatomical variation encountered and also the impossibility of achieving three-dimensional viewing of the insertion of the Wrisberg ligament by means of a digital camera.
Conclusion
In conclusion, our findings suggest that the Wrisberg ligament is a frequently occurring structure in knees and that, because it represents an average of 23.3% of the area of insertion of the PCL, it ought to contribute toward the posterior stability of the knee.
Future studies on selective ligament sectioning and biomechanical tests may be able to determine what the specific role of this ligament is, in relation to posterior stabilization of the joint. Meanwhile, every effort should be made toward preserving the Wrisberg ligament in reconstructions of the PCL.
Conflicts of interest
The authors declare no conflicts of interest.
Footnotes
Please cite this article as: Oliveira HCdS, Gali JC, Caetano EB. Relações anatômicas entre as inserções femorais dos ligamentos meniscofemoral de Wrisberg e cruzado posterior. Rev Bras Ortop. 2013;48;412–416.
Study conducted at the Sorocaba School of Medical Sciences and Healthcare, Pontifícia Universidade Católica de São Paulo, Sorocaba, SP, Brazil.
References
- 1.Poyton A.R., Javadpour S.M., Finegan P.J., O’Brien M. The meniscofemoral ligaments of the knee. J Bone Surg Br. 1997;79:327–330. doi: 10.1302/0301-620x.79b2.6893. [DOI] [PubMed] [Google Scholar]
- 2.Wan A.C.T., Felle P. The menisco-femoral ligaments. Clin Anat. 1995;8:323–326. doi: 10.1002/ca.980080503. [DOI] [PubMed] [Google Scholar]
- 3.Cho J.M., Suh J.S., Na J.B., Cho J.H., Kim Y., Yoo W.K. Variations in meniscofemoral ligaments at anatomical stydy and MR imaging. Skeletal Radiol. 1999;28:189–195. doi: 10.1007/s002560050499. [DOI] [PubMed] [Google Scholar]
- 4.Gupte C.M., Bull A.M., Thomas R.D., Amis A.A. A review of the function and biomechanics of the meniscofemoral ligaments. Arthroscopy. 2003;19:161–171. doi: 10.1053/jars.2003.50011. [DOI] [PubMed] [Google Scholar]
- 5.Matava M.J., Ellis E., Gruber B. Surgical treatment of posterior cruciate ligament tears: an evolving eechnique. J Am Acad Orthop Surg. 2009;17:435–446. doi: 10.5435/00124635-200907000-00004. [DOI] [PubMed] [Google Scholar]
- 6.Gupte C.M., Smith A., McDermott I.D., Bull A.M., Thomas R.D., Amis A.A. Meniscofemoral ligaments revisited. Anatomical study, age correlation, and clinical implications. J Bone Joint Surg Br. 2002;84:846–851. doi: 10.1302/0301-620x.84b6.13110. [DOI] [PubMed] [Google Scholar]
- 7.Cho S., Ko S., Woo J.K. Meniscus-stabilizing function of the meniscofemoral ligament: experimental study of pig knee joints. Arthroscopy. 2006;22:872–877. doi: 10.1016/j.arthro.2006.04.081. [DOI] [PubMed] [Google Scholar]
- 8.Moran C.J., Poynton A.R., Moran R., O’Brien M. Analysis of meniscofemoral ligament tension during knee motion. Arthroscopy. 2006;22:362–366. doi: 10.1016/j.arthro.2005.09.023. [DOI] [PubMed] [Google Scholar]
- 9.Heller L., Langman J. The menisco-femoral ligaments of the human knee. J Bone Joint Surg Br. 1964;46:307–313. [PubMed] [Google Scholar]
- 10.Last R.J. Some anatomical details of the knee joint. J Bone Joint Surg Br. 1948;30:683–688. [PubMed] [Google Scholar]
- 11.Candiollo L., Gautero G. Morphologie et fonction des ligaments ménisco-femoraux de l’articulation de genou chez l’homme. Acta Anat. 1959;38:304–323. [PubMed] [Google Scholar]
- 12.Poynton A., Moran C.J., Moran R., O’Brien M. The meniscofemoral ligaments influence lateral meniscal motion at the human knee joint. Arthroscopy. 2011;27:365–371. doi: 10.1016/j.arthro.2010.07.025. [DOI] [PubMed] [Google Scholar]
- 13.Yamamoto M., Hirohata K. Anatomical study on the meniscofemoral ligaments of the knee. Kobe J Med Sci. 1991;37:209–226. [PubMed] [Google Scholar]
- 14.Kohn D., Moreno B. Meniscus insertion anatomy as a basis for meniscus replacement: a morphological cadaveric study. Arthroscopy. 1995;11:96–103. doi: 10.1016/0749-8063(95)90095-0. [DOI] [PubMed] [Google Scholar]
- 15.Ramos L.A., de Carvalho R.T., Cohen M., Abdalla R.J. Anatomic relation between the posterior cruciate ligament and the joint capsule. Arthroscopy. 2008;24:1367–1372. doi: 10.1016/j.arthro.2008.07.011. [DOI] [PubMed] [Google Scholar]
- 16.Takahashi M., Matsubara T., Doi M., Suzuki D., Nagano A. Anatomical study of the femoral and tibial insertions of the anterolateral and posteromedial bundles of human posterior cruciate ligament. Knee Surg Sports Traumatol Arthrosc. 2006;14:1055–1059. doi: 10.1007/s00167-006-0192-9. [DOI] [PubMed] [Google Scholar]
- 17.Watanabe A.T., Carter B.C., Teitelbaum G.P., Bradley W.G., Jr. Common pitfalls in magnetic resonance imaging of the knee. J Bone Joint Surg Am. 1989;71:857–862. [PubMed] [Google Scholar]


