Short abstract
Objective
To evaluate dentist-related factors associated with the use of vital pulp therapy (VPT) for the treatment of pulp exposures in permanent teeth.
Methods
This survey-based study sent an online questionnaire to collect data on the demographics of the respondents, the use of VPT and the choice of materials for VPT, to all members of the Society of Endodontology of Guangdong, China.
Results
A total 183 of 380 members responded (48.2%). The majority (89.6%; 164 of 183) had performed direct pulp capping (DPC) while 55.2% (101 of 183) had performed partial pulpotomy (PP) at least once. The most-cited reason for not performing VPT was unfamiliarity with the technique. Mineral trioxide aggregate was the most commonly used material for both DPC (67.1%; 110 of 164) and PP (73.3%; 74 of 101). Endodontists, compared with general practitioners, preferred to perform DPC and chose calcium silicate materials (CSMs) for VPT (odds ratios 5.81 and 8.07, respectively). DPC and CSMs for VPT were also favoured more by respondents who had practised for > 5 years. Senior respondents were more likely to use PP.
Conclusions
Speciality, years of practise and age of dentists influenced the decision making and the choice of materials for VPT. Continuing education is essential to promote the clinical use of VPT.
Keywords: Calcium silicate materials, dentist-related factors, direct pulp capping, partial pulpotomy, survey
Introduction
With the improved understanding of pulp biology, vital pulp therapy (VPT) is considered a viable alternative to root canal treatment (RCT) for permanent teeth,1 since preserving pulp vitality, even with inflamed pulp, is more attainable than previously thought.2,3 With strict case selection and a proper treatment protocol, VPT could serve as a viable treatment for the management of permanent teeth with inflamed pulp.4,5
Direct pulp capping (DPC) and partial pulpotomy (PP) are two VPT procedures, wherein a material is applied on the exposed pulp.6 Both procedures demonstrate favourable outcomes in vital permanent teeth with pulpitis or even apical periodontitis.7–10 High success rates above 91% were reported for VPT techniques, including indirect pulp capping, DPC, miniature pulpotomy and full pulpotomy using calcium-enriched mixture cement in mature permanent molars.10 However, for permanent teeth with carious pulp exposures, success rates for DPC are inconsistent, while that of partial or full pulpotomy is higher for 3 years or longer.4 Partial or full pulpotomy has been recommended for teeth with clinical signs and symptoms indicating irreversible pulpitis, in which the irreversibly inflamed portion of the coronal pulp could be removed.11 There is no consensus with regard to the depth of intervention while performing VPT, and the field lacks enough randomized controlled clinical trials to draw clinical conclusions.
The capping material of choice is an important factor affecting the prognosis of VPT.12 More recently, calcium silicate materials (CSMs) have been increasingly acknowledged as pulp capping materials, and their functional effects are mainly compared with calcium hydroxide (CH).13–15 A meta-analysis showed that mineral trioxide aggregate (MTA) achieved a higher success rate in VPT than CH, due to its better chemical and physical properties, antibacterial activity, biocompatibility and sealing properties.16–19 Currently, a new range of CSMs, such as Biodentine™ (Septodont, Saint-Maur-des- Fossés, France) and iRoot® BP Plus/BioAggregate® (Innovative BioCeramix, Burnaby, BC, Canada), are available; with manufacturers claiming that these materials have similar advantages to MTA but without its disadvantages.14,15 Despite the benefits of CSMs for VPT, they may not yet be widely adopted in clinical practice, as many dentists may still be unaware of their clinical performance and the doctrinal change towards VPT.20,21
Considering the developments in pulp-capping materials and notable advances of VPT techniques in clinical practice, information on the factors that influence the use of VPT is limited. The aim of this study was to survey the use of VPT (DPC or PP) in permanent teeth by dentists in Guangdong Province, a heavily populated and well-developed province in the southern part of China. All members of the Guangdong Society of Endodontology, including endodontists and general practitioners with qualified training in endodontics, were invited to participate in this survey. The purpose of the study was: (i) to investigate the frequency of the use of VPT in permanent teeth and current application of CSMs in VPT; and (ii) to explore the dentist-related factors associated with the adoption of VPT and the use of CSMs for VPT, which could assist tailoring implementation intervention in clinical education.22
Materials and methods
Study design
This clinical survey invited all dentists who had registered successfully as members of the Guangdong Society of Endodontology before December 2017 to participate in this survey. The questionnaire was presented online (www.sojump.com) and sent to all the members via an email or WeChat, a web-based multimedia messaging application, by the Department of Operative Dentistry and Endodontics, Guanghua School of Stomatology, Hospital of Stomatology, Sun Yat-sen University, Guangzhou, Guangdong Province, China. This survey commenced on 12 December 2017. A reminder was sent 3 weeks after the launch. After a total of 9 weeks, the survey was closed. This clinical survey was approved by the Ethics Review Committee, Guanghua School of Stomatology, Sun Yat-Sen University (no. ERC-[2017]-06). All responses from the participants were analysed anonymously so informed consent was not required.
Questionnaire
The questionnaire was adopted with modification from a previously published questionnaire, after obtaining permission from the authors.23 An expert panel consisting of seven endodontists was invited to evaluate the questionnaire in the target language.24 After the expert panel reached an agreement on the equivalence in the concept and content of the questionnaire, it was back-translated by a bilingual dentist and compared with the original version to ensure that the fidelity of the original text was maintained.
Eighteen items were recorded, including respondents’ demographics (age, education level, years of practise, current work setting and specialty) and current status of their use of VPT. The following aspects of VPT use were investigated (Table 1), including the frequency of the use of VPT, the choice of materials for VPT, the period of use of CSMs in VPT, the reasons for not applying VPT or not using CSMs in the VPT procedure, and ways to learn VPT and CSMs. Prior to the formal survey, a pilot study was performed among 18 postgraduate students in Guanghua School of Stomatology, Sun Yat-Sen University to test suitability. After evaluating the responses, the questionnaire was considered appropriate and used as the final version in this survey.
Table 1.
Questions in relation to the use of vital pulp therapy (VPT) that were included in a questionnaire used to investigate the frequency of the use of VPT in permanent teeth and the current application of calcium silicate materials in VPT by dentists in Guangdong Province, China.
| 1 – Frequency of the use of direct pulp capping/ partial pulpotomy |
| (1). Have you ever practised direct pulp capping in permanent teeth in your daily routine? |
| (2). Have you ever practised partial pulpotomy in permanent teeth in your daily routine? |
| (3). If you have not used vital pulp therapy in permanent teeth, what are the reasons? |
| (4). How many cases of direct pulp capping have you performed per month in 2017? |
| (5). How many cases of partial pulpotomy have you performed per month in 2017? |
| 2 – The material of choice applied to the exposed pulp tissue |
| (1). Which materials have you used for direct pulp capping? |
| (2). Which materials have you used for partial pulpotomy? |
| 3 – Duration of use of calcium silicate materials for vital pulp therapy |
| (1). Have you ever used calcium silicate materials for vital pulp therapy? |
| (2). For how many years have you been using calcium silicate materials for direct pulp capping? |
| (3). For how many years have you been using calcium silicate materials for partial pulpotomy? |
| (4). If you have not used calcium silicate materials for vital pulp therapy, what are the reasons? |
| 4 – Ways to learn vital pulp therapy and calcium silicate materials |
| (1). How did you learn about vital pulp therapy? |
| (2). In your opinion, are continuing education courses useful to popularize the use of calcium silicate materials for vital pulp therapy? |
Statistical analyses
All statistical analyses were performed using PASW Statistics for Windows, Version 18.0 (SPSS Inc., Chicago, IL, USA). Data on the demographic profile of respondents, frequency of the use of VPT and application of CSMs in VPT were analysed using descriptive statistics. χ2-test was used to assess respondent characteristics (age, education level, years of practise, work setting and specialty) in relation to the adoption of VPT and use of CSMs for VPT. Multivariate binary logistic regression analysis was performed to identify independent dentist-related factors associated with the adoption of VPT and the use of CSMs for VPT, with variables being entered stepwise and then removed if P > 0.1. A P-value < 0.05 was considered statistically significant.
Results
A total of 183 registered members of Guangdong Society of Endodontology completed the questionnaire, representing a response rate of 48.2% (183 of 380 members). Guangdong Society of Endodontology, affiliated to the Guangdong Stomatological Association, is a society of endodontists and general practitioners with qualified training in endodontics. Table 2 summarizes the respondents’ demographic characteristics. Almost half of the respondents (86 of 183 respondents; 47.0%) had qualified and worked for over 10 years. A total of 123 of 183 respondents (67.2%) practised as endodontists while others were general practitioners. Endodontists were dentists who had postgraduate training (specialty training, master’s degree or above in endodontics) after obtaining a bachelor’s degree, exclusively performing endodontics. General practitioners were those who qualified on the endodontic course and had received clinical training as visiting dentists. They incorporated endodontic treatment in their daily clinical work.
Table 2.
Demographic characteristics of dentists (n = 183) who completed the questionnaire on their use of vital pulp therapy (VPT) in permanent teeth and their current application of calcium silicate materials in VPT.
| Characteristic |
Study cohortn = 183 |
|
|---|---|---|
| n | % | |
| Age, years | ||
| ≤30 | 43 | 23.5% |
| 31–40 | 88 | 48.1% |
| 41–50 | 32 | 17.5% |
| >50 | 20 | 10.9% |
| Education level* | ||
| Vocational diploma | 12 | 6.6% |
| Bachelor’s degree | 37 | 20.2% |
| Master’s degree | 64 | 35.0% |
| Doctorate degree | 70 | 38.3% |
| Work setting | ||
| Private clinics | 20 | 10.9% |
| Public hospital | 52 | 28.4% |
| University affiliated hospitals | 111 | 60.7% |
| Years of practise | ||
| <5 | 45 | 24.6% |
| 5–10 | 52 | 28.4% |
| 11–20 | 52 | 28.4% |
| >20 | 34 | 18.6% |
| Specialty | ||
| General practitioner | 60 | 32.8% |
| Endodontist | 123 | 67.2% |
*The levels of education are based on the Chinese medical education system. Vocational diploma, 3 years of study in the junior dental school after high school can lead to a vocational diploma in dentistry. The holder of a vocational diploma becomes an assistant dentist after passing the National Medical Licensing Examination (NMLE). Then they can practise under the supervision of a licensed dentist. With a minimum of 2 years of supervised practise, they can obtain a dental license after passing the NMLE. Bachelor’s degree, 5 years of undergraduate study in the dental school after high school can lead to a bachelor’s degree. Master’s degree/doctorate degree, 3–6 years of postgraduate study in the dental school can lead to a master’s/doctorate degree.
A total of 165 of 183 respondents (90.2%) had ever used VPT as a procedure in the remit of their service. Among the respondents, 89.6% (n = 164) had used DPC, while 55.2% (n = 101) had used PP. Figure 1 shows the distribution of monthly performance of DPC and PP in 2017, indicating that VPT (DPC or PP) was performed infrequently. Eighty-two of 164 respondents (50.0%) performed DPC at least once a month, whereas 31 of 101 respondents (30.7%) performed PP at least once a month (Figure 1). The two most common reasons selected by the 18 respondents who had never used VPT were ‘unfamiliarity with VPT’ (61.1%; n = 11) and ‘uncertain outcome’ (55.6%; n = 10). In addition, ‘difficulty in operation’ (38.9%; n = 7), ‘time’ (11.1%; n = 2) and ‘cost’ (5.6%; n = 1) were also cited as barriers to the use of VPT.
Figure 1.
Monthly cases of direct pulp capping (n = 164) (a) and partial pulpotomy (n = 101) (b) performed in 2017 among respondents (n = 183) who completed the questionnaire on their use of vital pulp therapy (VPT) in permanent teeth and their current application of calcium silicate materials in VPT. The colour version of this figure is available at: http://imr.sagepub.com.
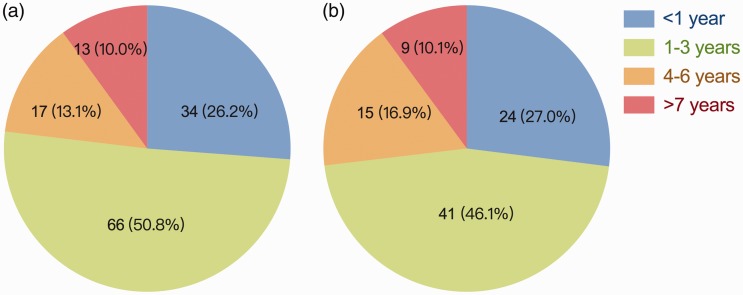
Mineral trioxide aggregate was the most commonly selected material for DPC (67.1%; 110 of 164 respondents) and PP (73.3%; 74 of 101 respondents), followed by other CSMs (Figure 2). Overall, 79.4% of respondents who had ever used VPT (131 of 165 respondents) practised VPT using CSMs as a capping material on pulp exposures. Approximately half of the respondents had used CSMs for VPT for 1–3 years (50.8%, 66 of 130 for DPC; 46.1%, 41 of 89 for PP) (Figure 3). Only 13 of 130 respondents (10.0%) and nine of 89 respondents (10.1%) had utilized CSMs for DPC and PP for at least 7 years, respectively. A total of 34 of 165 respondents had never applied CSMs to VPT: of these, 70.6% (n = 24) of them cited ‘cost’ as the major barrier to the use of CSMs in VPT, while 58.8% (n = 20) selected ‘lack of training’ as the barrier to use.
Figure 2.
Choices of capping materials among respondents who had ever performed direct pulp capping (DPC; n = 164) or partial pulpotomy (PP; n = 101). Respondents could choose more than one material that had been used as capping materials. The colour version of this figure is available at: http://imr.sagepub.com.
Figure 3.
Duration of use of calcium silicate materials for direct pulp capping (a; n = 130) and partial pulpotomy (b; n = 98) among respondents who completed the questionnaire on their use of vital pulp therapy (VPT) in permanent teeth and their current application of calcium silicate materials in VPT. The colour version of this figure is available at: http://imr.sagepub.com.
The χ2-test revealed a significant association between all five dentist-related factors and the uptake of DPC (P < 0.05) (Table 3). The impacts of ‘age’ and ‘years of practise’ on the use of PP were significant (P < 0.05). Three characteristics, including ‘education level’, ‘work setting’ and ‘specialty’ had significant effects on the use of CSMs for VPT (P < 0.05). Compared with other age groups, the respondents in the age group of 41–50 years had the largest proportion using DPC (100.0%; 32 of 32), PP (78.1%; 25 of 32) and CSMs for VPT (87.5%; 28 of 32). CSMs were the materials of choice for 90.6% (106 of 117) of endodontists and 52.1% (25 of 48) of general practitioners. Logistic regression analysis showed that endodontists were more likely to perform DPC and to use CSMs for VPT than general practitioners (odds ratios 5.81 and 8.07, respectively, P < 0.05) (Table 4). Respondents with more work experience tended to perform DPC and use CSMs for VPT more often than those having less than 5 years of practise (P < 0.05). Older respondents were more likely to perform PP, up to 50 years of age (P < 0.05).
Table 3.
Associations of dentist-related factors with the management decisions made by dentists (n = 183) who completed the questionnaire on their use of vital pulp therapy (VPT) in permanent teeth and their current application of calcium silicate materials (CSMs) in VPT.
|
DPC, n = 183 |
PP, n = 183 |
CSMs used for VPT, n = 131 |
|||||||
|---|---|---|---|---|---|---|---|---|---|
| Characteristic | YESn = 164 | NOn = 19 | Statistical significancea | YESn = 101 | NOn = 72 | Statistical significancea | YESn = 131 | NOn = 34 | Statistical significancea |
| Age, years | P < 0.01 | P < 0.01 | NS | ||||||
| ≤30 | 32 (74.4) | 11 (25.6) | 9 (20.9) | 34 (79.1) | 22 (66.7) | 11 (33.3) | |||
| 31–40 | 83 (94.3) | 5 (5.7) | 52 (59.1) | 36 (40.9) | 67 (80.7) | 16 (19.3) | |||
| 41–50 | 32 (100.0) | 0 (0.0) | 25 (78.1) | 7 (21.9) | 28 (87.5) | 4 (12.5) | |||
| >50 | 17 (85.0) | 3 (15.0) | 15 (75.0) | 5 (25.0) | 14 (82.4) | 3 (17.6) | |||
| Education level | P < 0.01 | NS | P < 0.01 | ||||||
| Vocational diploma | 8 (66.7) | 4 (33.3) | 3 (25.0) | 9 (75.0) | 3 (37.5) | 5 (62.5) | |||
| Bachelor’s degree | 30 (81.1) | 7 (18.9) | 19 (51.4) | 18 (48.6) | 21 (70.0) | 9 (30.0) | |||
| Master’s degree | 59 (92.2) | 5 (7.8) | 40 (62.5) | 24 (37.5) | 51 (85.0) | 9 (15.0) | |||
| Doctorate degree | 67 (95.7) | 3 (4.3) | 39 (55.7) | 31 (44.3) | 56 (83.6) | 11 (16.4) | |||
| Work setting | P < 0.01 | NS | P < 0.01 | ||||||
| Private clinics | 14 (70.0) | 6 (30.0) | 7 (35.0) | 13 (65.0) | 8 (57.1) | 6 (42.9) | |||
| Public hospital | 47 (90.4) | 5 (9.6) | 33 (63.5) | 19 (36.5) | 29 (61.7) | 18 (38.3) | |||
| University affiliated hospitals | 103 (92.8) | 8 (7.2) | 61 (55.0) | 50 (45.0) | 94 (90.4) | 10 (9.6) | |||
| Years of practise | P < 0.01 | P < 0.01 | NS | ||||||
| <5 | 33 (73.3) | 12 (26.7) | 14 (31.1) | 31 (68.9) | 22 (64.7) | 12 (35.3) | |||
| 5–10 | 49 (94.2) | 3 (5.8) | 26 (50.0) | 26 (50.0) | 38 (77.6) | 11 (22.4) | |||
| 11–20 | 51 (98.1) | 1 (1.9) | 34 (65.4) | 18 (34.6) | 45 (88.2) | 6 (11.8) | |||
| >20 | 31 (91.2) | 3 (8.8) | 27 (79.4) | 7 (20.6) | 26 (83.9) | 5 (16.1) | |||
| Specialty | P < 0.01 | NS | P < 0.01 | ||||||
| General practitioner | 47 (78.3) | 13 (21.7) | 29 (48.3) | 31 (51.7) | 25 (52.1) | 23 (47.9) | |||
| Endodontist | 117 (95.1) | 6 (4.9) | 72 (58.5) | 51 (41.5) | 106 (90.6) | 11 (9.4) | |||
Data presented as n of respondents (%).
aχ2-test was used to assess respondent characteristics in relation to the adoption of VPT and use of CSMs for VPT; NS, no significant association (P ≥ 0.05).
DPC, direct pulp capping; PP, partial pulpotomy.
Table 4.
Logistic regression analysis of dentist-related factors associated with the management decisions made by dentists (n = 183) who completed the questionnaire on their use of vital pulp therapy (VPT) in permanent teeth and their current application of calcium silicate materials (CSMs) in VPT.
| Characteristic | Odds ratio | 95% confidence interval | Statistical significance |
|---|---|---|---|
| Application of DPC (NO versus YES) | |||
| Years of practise | P = 0.004 | ||
| <5 (reference) | 1.00 | ||
| 5–10 | 6.18 | 1.53, 24.96 | P = 0.011 |
| 11–20 | 18.37 | 2.20, 153.49 | P = 0.007 |
| >20 | 5.33 | 1.27, 22.48 | P = 0.023 |
| Specialty | P = 0.002 | ||
| General practitioner (reference) | 1.00 | ||
| Endodontist | 5.81 | 1.92, 17.58 | P = 0.002 |
| Application of PP (NO versus YES) | |||
| Age, years | P < 0.001 | ||
| ≤30 (reference) | 1.00 | ||
| 31–40 | 5.46 | 2.34, 12.75 | P < 0.001 |
| 41–50 | 13.49 | 4.43, 41.13 | P < 0.001 |
| >50 | 11.33 | 3.25, 39.58 | P < 0.001 |
| Application of CSMs used for VPT (NO versus YES) | |||
| Work setting | P = 0.048 | ||
| Private clinics (reference) | 1.00 | ||
| Public hospital | 0.41 | 0.09, 1.86 | NS |
| University affiliated hospitals | 1.49 | 0.31, 7.03 | NS |
| Years of practise | P = 0.035 | ||
| <5 (reference) | 1.00 | ||
| 5–10 | 2.64 | 0.79, 8.84 | NS |
| 11–20 | 6.59 | 1.70, 25.57 | P = 0.006 |
| >20 | 5.96 | 1.26, 28.10 | P = 0.024 |
| Specialty | P < 0.001 | ||
| General practitioner (reference) | 1.00 | ||
| Endodontist | 8.07 | 2.81, 23.17 | P < 0.001 |
DPC, direct pulp capping; PP, partial pulpotomy; NS, no significant association (P ≥ 0.05).
Ways to learn VPT were investigated among respondents who performed VPT (n = 165). According to this current survey, the most popular way to learn about VPT was published literature/books (85.5%; n = 141), followed by lectures (66.7%; n = 110), continuing education courses (65.5%; n = 108) and colleague recommendation (54.5%; n = 90). The internet (27.3%; n = 45) appeared to be a novel approach to learn about VPT. When investigating dentists’ attitudes to continuing education courses, a total of 154 of 165 respondents (93.3%) agreed that continuing education courses were useful to popularize the use of CSMs for VPT.
Discussion
In light of the favourable outcomes following the use of VPT for exposed pulps,6,14 surveys on the management of pulp exposure with VPT among dental practitioners have been done in other countries and regions with the response rates ranging from 25% to 68%.23,25,26 Although an optimal response rate of 70–80% is preferred to minimize the risk of bias,27 a response rate as low as 43% could be considered the least nonresponse bias.28,29 The response rate of 48.2% in this current study is therefore considered acceptable to control the risk of bias. However, incentive strategies such as personalized mailing and prompts and follow-up contacts, are highly recommended to improve the response rate in further survey research involving dental practitioners.30 Data from 123 endodontists and 60 general practitioners presented the current management of pulp exposures with VPT among members of Guangdong Society of Endodontology, which helped provide preliminary insights into the current situation in Southern China.
Responses from this current survey showed that although most respondents had attempted VPT, DPC was performed infrequently and PP was rarely performed on a monthly basis in 2017. This was similar to another survey mainly among general practitioners in Wales, UK, which showed that a low frequency of VPT was undertaken on a monthly basis, although most of the respondents had considered VPT in the remit of their services.23 These current results indicated that VPT techniques are not currently adopted as a routine treatment modality by dentists in Guangdong Province. In the present survey, ‘unfamiliarity with VPT’ was the most frequently cited barrier to the use of VPT by those respondents that had not used VPT. It appears that the lack of specific training among respondents might hinder the spread of VPT use in Southern China. Since endodontic therapy has been shown to be a predictable treatment of choice for cases with inflamed pulps,31 standardized RCT procedures have been incorporated into undergraduate programmes and continuing education courses in China during the past 30 years. Most premier, city dwelling Chinese dentists who are well trained may prefer to choose RCT for teeth with potential pulp infection when the pulp is exposed. ‘Uncertain outcome’ was the second most frequently cited reason preventing respondents from using VPT. The present study revealed that more than half of respondents who had never used VPT doubted the effectiveness of VPT when treating pulp exposures in permanent teeth. This finding may be attributed to the fact that VPT using CH produces variable results,32 which makes practitioners prudent with VPT. Furthermore, the currently available diagnostic tools fail to provide dentists with directions as to what is saveable pulp, or a pulp that should be removed and replaced by a root filling.33,34 When the pulp is exposed, practitioners may prefer to adopt other treatment modalities with more predictability. A series of clinical studies have shown that the advent of CSMs extends the clinical indications for VPT and makes the outcomes more predictable.3,12,14 However, respondents in this current survey might not realize the improved clinical outcomes of VPT accompanied with the development of new materials for exposed pulps, which may hamper the application of VPT. In this current study, it is interesting to find that PP is less widely used than DPC, which is in line with other surveys.23,25,35 This finding might indicate that the majority of dentists are concerned about the operational difficulty of PP in permanent teeth.25
With regard to the selection of materials for VPT, ‘high cost’ and ‘lack of training’ heavily resulted in the avoidance of CSMs in VPT despite the favourable outcome of VPT with CSMs, which is similar to the outcomes of the survey in Wales, UK.23 When selecting an appropriate material, dentists may take into account the profitability, with there being such a high market price of CSMs, especially for those without funding support. However, from a patient’s perspective, a cost-effectiveness analysis based on the German healthcare system indicated that MTA was a more cost-effective material than CH for DPC despite higher initial treatment costs, since expensive retreatments were avoided.36 In spite of the potential financial dilemma for practitioners, CSMs should be the preferred materials of choice for VPT in order to take advantage of their better chemical and physical properties than CH.36 Further specific cost-effectiveness analyses based on disparate healthcare systems are required.
Generally, practitioners with a longer clinical experience showed a stronger inclination to use DPC and CSMs for VPT in this study, indicating that experienced dentists might have a better understanding of pulp biology and better access to newly marketed materials. It has been reported in several surveys that ‘years of experience’ is an important dentist-related factor regarding clinical diagnosis, material selection and treatment strategy.37–39 On the other hand, this current study showed that endodontists have a higher chance of using DPC and CSMs for VPT than general practitioners. Endodontists are more likely to be updated with the current literature, thus being well-informed about the potentially better outcome presented for VPT using CSMs.26 Previous studies also found that differences in specialty backgrounds might affect endodontic diagnosis and treatment decisions, and endodontists showed the most consistent agreement for treatment decision than other groups (including general practitioners, undergraduate students and postgraduate students).40,41 Currently, it seems necessary to develop a VPT training strategy to promote this clinical practice among general practitioners in Southern China. Continuing education courses, by which 65.5% of respondents learned new approaches to VPT in this current study, have been reported to be beneficial for general practitioners to adopt new technologies when performing endodontic treatment.42 Hence, specific continuing education courses might be one of the primary ways to update the knowledge on VPT and to incorporate VPT with CSMs for dentists, especially for general practitioners.
In this current study, ‘age’ was the factor associated with the application of PP. Dentists over 30 years old were more likely to perform PP treatment in potentially infected pulp in permanent teeth than dentists ≤30 years old. In consideration of the possibility of bacterial invasion beneath the exposure site, older practitioners might implement PP more easily by removing part of the pulp before capping the medication than younger practitioners, while younger dentists ≤30 years might prefer other treatment modalities. It is notable that the factor ‘age’ partly reflected the respondents’ working experience, which is somewhat similar to factor ‘years of practise’. The associations of these two factors with VPT reflect the differences in the therapeutic ideas and treatment options between beginners and veterans when managing pulp exposures. Beginners might tend to follow established treatment procedures, while experienced practitioners might try to improve themselves with advanced knowledge and techniques.
Although this study showed that dentist-related factors (speciality, years of practise and age of dentists) were associated with the use of VPT, the interpretation of survey data must consider the risk of participation bias, since the survey was carried out in members of Guangdong Society of Endodontology. It is noteworthy that the general practitioners who registered as members of Guangdong Society of Endodontology are those having a special interest in endodontics; thus the general practitioners in this survey may not be representative of general practitioners who were not members of the Society of Endodontology.43 The clinical details related to VPT, such as the management of deep caries and diagnostic criteria of pulp status, will be investigated in future studies. In addition, investigations on tooth-related factors and patient-related factors with the use of VPT are also needed to be able to develop guidelines. Evidence of the impact of factors, such as the types of VPT used and clinical symptoms correlated with the histological state of the inflamed pulp, on treatment prognosis is needed.
In conclusion, speciality, years of practise and age of dentists influenced the decision-making process and the choice of materials for VPT. Continuing education to train practising dentists is essential to promote the clinical use of VPT.
Acknowledgement
The authors thank Dr Prasanna Neelakantan (Department of Endodontology, Faculty of Dentistry, The University of Hong Kong, Hong Kong) for carefully proofreading this manuscript.
Declaration of conflicting interest
The authors declare that there are no conflicts of interest.
Funding
This work was supported by grants from the National Natural Science Foundation of China (no. 81670983, no.11772361) and the Natural Science Foundation of Guangdong Province (no. 2017A030308011).
References
- 1.Simon S, Perard M, Zanini M, et al. Should pulp chamber pulpotomy be seen as a permanent treatment? Some preliminary thoughts. Int Endod J 2013; 46: 79–87. [DOI] [PubMed] [Google Scholar]
- 2.Schmalz G, Smith AJ. Pulp development, repair, and regeneration: challenges of the transition from traditional dentistry to biologically based therapies. J Endod 2014; 40: S2–S5. [DOI] [PubMed] [Google Scholar]
- 3.Taha NA, Khazali MA. Partial pulpotomy in mature permanent teeth with clinical signs indicative of irreversible pulpitis: a randomized clinical trial. J Endod 2017; 43: 1417–1421. [DOI] [PubMed] [Google Scholar]
- 4.Aguilar P, Linsuwanont P. Vital pulp therapy in vital permanent teeth with cariously exposed pulp: a systematic review. J Endod 2011; 37: 581–587. [DOI] [PubMed] [Google Scholar]
- 5.Morotomi T, Washio A, Kitamura C. Current and future options for dental pulp therapy. Jpn Dent Sci Rev 2019; 55: 5–11. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Fransson H, Wolf E, Petersson K. Formation of a hard tissue barrier after experimental pulp capping or partial pulpotomy in humans: an updated systematic review. Int Endod J 2016; 49: 533–542. [DOI] [PubMed] [Google Scholar]
- 7.Asgary S, Fazlyab M, Sabbagh S, et al. Outcomes of different vital pulp therapy techniques on symptomatic permanent teeth: a case series. Iran Endod J 2014; 9: 295–300. [PMC free article] [PubMed] [Google Scholar]
- 8.Caliskan MK, Guneri P. Prognostic factors in direct pulp capping with mineral trioxide aggregate or calcium hydroxide: 2- to 6-year follow-up. Clin Oral Investig 2017; 21: 357–367. [DOI] [PubMed] [Google Scholar]
- 9.Kundzina R, Stangvaltaite L, Eriksen HM, et al. Capping carious exposures in adults: a randomized controlled trial investigating mineral trioxide aggregate versus calcium hydroxide. Int Endod J 2017; 50: 924–932. [DOI] [PubMed] [Google Scholar]
- 10.Asgary S, Hassanizadeh R, Torabzadeh H, et al. Treatment outcomes of 4 vital pulp therapies in mature molars. J Endod 2018; 44: 529–535. [DOI] [PubMed] [Google Scholar]
- 11.Ricucci D, Loghin S, Siqueira JF., Jr. Correlation between clinical and histologic pulp diagnoses. J Endod 2014; 40: 1932–1939. [DOI] [PubMed] [Google Scholar]
- 12.Linu S, Lekshmi MS, Varunkumar VS, et al. Treatment outcome following direct pulp capping using bioceramic materials in mature permanent teeth with carious exposure: a pilot retrospective study. J Endod 2017; 43: 1635–1639. [DOI] [PubMed] [Google Scholar]
- 13.Brizuela C, Ormeno A, Cabrera C, et al. Direct pulp capping with calcium hydroxide, mineral trioxide aggregate, and biodentine in permanent young teeth with caries: a randomized clinical trial. J Endod 2017; 43: 1776–1780. [DOI] [PubMed] [Google Scholar]
- 14.Parirokh M, Torabinejad M, Dummer PMH. Mineral trioxide aggregate and other bioactive endodontic cements: an updated overview - part I: vital pulp therapy. Int Endod J 2018; 51: 177–205. [DOI] [PubMed] [Google Scholar]
- 15.Rajasekharan S, Martens LC, Cauwels RGEC, et al. Biodentine™ material characteristics and clinical applications: a 3 year literature review and update. Eur Arch Paediatr Dent 2018; 19: 1–22. [DOI] [PubMed] [Google Scholar]
- 16.Parirokh M, Torabinejad M. Mineral trioxide aggregate: a comprehensive literature review–Part I: chemical, physical, and antibacterial properties. J Endod 2010; 36: 16–27. [DOI] [PubMed] [Google Scholar]
- 17.Torabinejad M, Parirokh M. Mineral trioxide aggregate: a comprehensive literature review–part II: leakage and biocompatibility investigations. J Endod 2010; 36: 190–202. [DOI] [PubMed] [Google Scholar]
- 18.Mente J, Hufnagel S, Leo M, et al. Treatment outcome of mineral trioxide aggregate or calcium hydroxide direct pulp capping: long-term results. J Endod 2014; 40: 1746–1751. [DOI] [PubMed] [Google Scholar]
- 19.Li Z, Cao L, Fan M, et al. Direct pulp capping with calcium hydroxide or mineral trioxide aggregate: a meta-analysis. J Endod 2015; 41: 1412–1417. [DOI] [PubMed] [Google Scholar]
- 20.Wolters WJ, Duncan HF, Tomson PL, et al. Minimally invasive endodontics: a new diagnostic system for assessing pulpitis and subsequent treatment needs. Int Endod J 2017; 50: 825–829. [DOI] [PubMed] [Google Scholar]
- 21.Jitaru S, Hodisan I, Timis L, et al. The use of bioceramics in endodontics - literature review. Clujul Med 2016; 89: 470–473. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 22.Schwendicke F, Gostemeyer G. Understanding dentists' management of deep carious lesions in permanent teeth: a systematic review and meta-analysis. Implement Sci 2016; 11: 142. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.Chin JS, Thomas MB, Locke M, et al. A survey of dental practitioners in Wales to evaluate the management of deep carious lesions with vital pulp therapy in permanent teeth. Br Dent J 2016; 221: 331–338. [DOI] [PubMed] [Google Scholar]
- 24.Sousa VD, Rojjanasrirat W. Translation, adaptation and validation of instruments or scales for use in cross-cultural health care research: a clear and user-friendly guideline. J Eval Clin Pract 2011; 17: 268–274. [DOI] [PubMed] [Google Scholar]
- 25.Stangvaltaite L, Schwendicke F, Holmgren C, et al. Management of pulps exposed during carious tissue removal in adults: a multi-national questionnaire-based survey. Clin Oral Investig 2017; 21: 2303–2309. [DOI] [PubMed] [Google Scholar]
- 26.Chisini LA, Conde MC, Correa MB, et al. Vital pulp therapies in clinical practice: findings from a survey with dentist in Southern Brazil. Braz Dent J 2015; 26: 566–571. [DOI] [PubMed] [Google Scholar]
- 27.Parashos P, Morgan MV, Messer HH. Response rate and nonresponse bias in a questionnaire survey of dentists. Community Dent Oral Epidemiol 2005; 33: 9–16. [DOI] [PubMed] [Google Scholar]
- 28.Hovland EJ, Romberg E, Moreland EF. Nonresponse bias to mail survey questionnaires within a professional population. J Dent Educ 1980; 44: 270–274. [PubMed] [Google Scholar]
- 29.Madarati AA. Why dentists don't use rubber dam during endodontics and how to promote its usage? BMC Oral Health 2016; 16: 24. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 30.Cho YI, Johnson TP, Vangeest JB. Enhancing surveys of health care professionals: a meta-analysis of techniques to improve response. Eval Health Prof 2013; 36: 382–407. [DOI] [PubMed] [Google Scholar]
- 31.Ng YL, Mann V, Gulabivala K. Tooth survival following non-surgical root canal treatment: a systematic review of the literature. Int Endod J 2010; 43: 171–189. [DOI] [PubMed] [Google Scholar]
- 32.Akhlaghi N, Khademi A. Outcomes of vital pulp therapy in permanent teeth with different medicaments based on review of the literature. Dent Res J (Isfahan) 2015; 12: 406–417. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 33.Bergenholtz G, Axelsson S, Davidson T, et al. Treatment of pulps in teeth affected by deep caries - a systematic review of the literature. Singapore Dent J 2013; 34: 1–12. [DOI] [PubMed] [Google Scholar]
- 34.Zanini M, Meyer E, Simon S. Pulp inflammation diagnosis from clinical to inflammatory mediators: a systematic review. J Endod 2017; 43: 1033–1051. [DOI] [PubMed] [Google Scholar]
- 35.Croft K, Kervanto-Seppala S, Stangvaltaite L, et al. Management of deep carious lesions and pulps exposed during carious tissue removal in adults: a questionnaire study among dentists in Finland. Clin Oral Investig 2018. DOI: 10.1007/s00784-018-2556-1 [Epub ahead of print]. [DOI] [PubMed]
- 36.Schwendicke F, Brouwer F, Stolpe M. Calcium hydroxide versus mineral trioxide aggregate for direct pulp capping: a cost-effectiveness analysis. J Endod 2015; 41: 1969–1974. [DOI] [PubMed] [Google Scholar]
- 37.Demarco FF, Conde MC, Ely C, et al. Preferences on vital and nonvital tooth bleaching: a survey among dentists from a city of southern Brazil. Braz Dent J 2013; 24: 527–531. [DOI] [PubMed] [Google Scholar]
- 38.Nascimento GG, Correa MB, Opdam N, et al. Do clinical experience time and postgraduate training influence the choice of materials for posterior restorations? Results of a survey with Brazilian general dentists. Braz Dent J 2013; 24: 642–646. [DOI] [PubMed] [Google Scholar]
- 39.Geibel MA, Carstens S, Braisch U, et al. Radiographic diagnosis of proximal caries – influence of experience and gender of the dental staff. Clin Oral Investig 2017; 21: 2761–2770. [DOI] [PubMed] [Google Scholar]
- 40.Dechouniotis G, Petridis XM, Georgopoulou MK. Influence of specialty training and experience on endodontic decision making. J Endod 2010; 36: 1130–1134. [DOI] [PubMed] [Google Scholar]
- 41.McCaul LK, McHugh S, Saunders WP. The influence of specialty training and experience on decision making in endodontic diagnosis and treatment planning. Int Endod J 2001; 34: 594–606. [DOI] [PubMed] [Google Scholar]
- 42.Savani GM, Sabbah W, Sedgley CM, et al. Current trends in endodontic treatment by general dental practitioners: report of a United States national survey. J Endod 2014; 40: 618–624. [DOI] [PubMed] [Google Scholar]
- 43.Ha WN, Duckmanton P, Kahler B, et al. A survey of various endodontic procedures related to mineral trioxide aggregate usage by members of the Australian Society of Endodontology. Aust Endod J 2016; 42: 132–138. [DOI] [PubMed] [Google Scholar]