Abstract
Objective
To evaluate the role of locked compression plates (LCPs) in management of peri‐ and intra‐articular fractures around the knee.
Methods
Twenty distal femoral and 20 proximal tibial fractures were fixed with LCPs. The types of femoral fractures were A1 (four), A2 (three), A3 (two), C1 (one), C2 (seven) and C3 (three). The types of tibial fractures were A2 (one), A3 (two), B2 (two), C1 (four), C2 (five) and C3 (six). All patients were followed up for up to 18 months (mean, 12 months). Fourteen patients with distal femoral fractures and 19 with proximal tibial fractures underwent surgery using a minimally invasive percutaneous plate osteosynthesis (MIPPO) technique. The others were treated by open reduction. The average time of fixation was 8 days after injury (0–31 days). Knee Society scores were used for clinical and functional assessment.
Results
All fractures, except one of the distal femur and one of the proximal tibia, united. The mean union times for distal femoral and proximal tibial fractures were 15.2 and 14.9 weeks, respectively. One patient with a distal femoral fracture had implant failure. One patient was quadriplegic and did not recover the ability to walk. The average Knee Society scores of the remaining 18 patients were 82.66 (excellent) and 77.77 (functional score, good). There was one case of implant failure and one of screw breakage in distal femoral fractures. One case of nonunion occurred in a proximal tibial fracture.
Conclusion
Provided it is applied with proper understanding of biomechanics, LCP is one of the best available options for management of challenging peri‐ and intra‐articular fractures.
Keywords: Intra‐articular fracture, Knee, Locked compression plate, Proximal tibial fracture
Introduction
The ultimate goal of the orthopaedic trauma surgeon is to restore function and expedite recovery. For peri‐ and intra‐articular fractures around the knee, achievement of both of these goals remains challenging. These fractures require excellent articular reconstruction and early mobilization to prevent joint stiffness. Common problems with treatment of fractures around knee are articular malreduction, varus/valgus malalignment, infection, knee stiffness and nonunion. Intramedullary nailing of proximal tibial fractures is usually associated with malreduction of the proximal segment, most commonly flexion and valgus at the fracture site1, 2.
In management of distal femoral fractures, inherent disadvantages of fixed angle blade plates include poor fixation in osteoporotic bone and an inability to control coronal plane fractures. Interfragmentary screws used to secure comminuted fracture fragments may create obstacles for placement of fixed angle blade plates. In addition, insertion of the lag screw of sliding barrel plates requires removal of a large amount of bone from the femoral condyles.
Many biomechanical studies have demonstrated that intramedullary nailing and side plate constructs have similar axial strength3, 4. Intramedullary nailing may fail because of loss of distal fixation during axial loading, resulting in penetration of the nail into the knee joint3. Insufficient fracture reduction, a poor starting point, or eccentric reaming may lead to fracture malalignment. A notable disadvantage of retrograde intramedullary nailing is violation of the knee joint. Many recent studies have favored the use of locking plates over retrograde intramedullary nailing for distal femoral fractures. Careful insertion is required to protect the articular cartilage5. Association for Osteosynthesis/Association for the Study of Internal Fixation guidelines for conventional plating involve anatomical reduction and rigid fixation with inter‐fragmentary compression. Wide exposure of complex fractures to achieve anatomical fixation increases the chances of delayed union, nonunion and risk of infection.
When these limitations of conventional plating became obvious in the late 1980s, efforts were made to develop plating systems and surgical techniques that preserved more of the biological factors contributing to bone healing. In high‐energy complex tibial plateau and distal femoral fractures, the soft tissue envelope is already damaged and conventional plating after excessive dissection further damages the already compromised blood supply to bone. This explains why conventional treatment of these fractures has been associated with a high rate of wound complications and deep sepsis6. Efforts to preserve structures around the fracture led to development of minimally invasive percutaneous plate osteosynthesis (MIPPO). Development of a precontoured locked internal fixator has made it possible to use the MIPPO technique in an effective and simple, but technically skilled, way. The locked plate system converts shear forces into compressive forces at the screw bone interface. By a variety of mechanisms, the screws in a locked plating system are designed to lock into the plate, eliminating screw toggle and creating a fixed‐angle, single‐beam construct. In a single beam construct there is no motion between the components of the beam, namely, the plate, screw and bone. Biomechanically, this makes fixation with locked compression plates (LCPs) stronger than with load‐sharing constructs, where motion occurs between the individual components of the beam construct. The purpose of this article is to present clinical and functional results of LCP of peri‐ and intra‐articular fractures around the knee.
Materials and Methods
This was a prospective study of patients presenting to our outpatient and emergency department from August 2010 to July 2012with peri‐ and intra‐articular fractures around the knee. In all, 38 patients with 40 fractures were enrolled and followed up for 23 months. Twenty patients had proximal tibial fractures and 20 distal femoral fractures. Three patients had both proximal tibial and distal femoral fractures; however, only two of them were included in both groups because one patient with both fractures refused proximal tibial plating. Cancellous screws were used to fix a minimally displaced proximal tibial fracture in this patient. The types of femoral fractures were A1 (four), A2 (three), A3 (two), C1 (one), C2 (seven) and C3 (three). The types of tibial fractures were A2 (one), A3 (two), B2 (two), C1 (four), C2 (five) and C3 (six). All fractures were treated by LCP. The MIPPO technique was used in 95% of proximal tibial fractures (19 cases) and 70% of distal femoral fractures (14 cases). Five to 10 hole femoral plates and 4 to 13 hole tibial plates were used. The mean screw density of locked plates in femoral fractures was 0.51 and in tibial fractures 0.53. Mean plate to fracture length ratio in femoral fractures was 3 and in tibial fractures 2.8. Healing was defined as callus bridging of one cortex visible on both anteroposterior and lateral X‐ray films together with full painless weight bearing or full painless weight bearing without visible callus formation. Periarticular fractures were defined according to the criteria of Muller7.
American Food and Drug Administration panel definitions of nonunion and delayed union were used. Healing within the first 6 months was defined as normal, 6–9 months as delayed and more than 9 months as nonunion. For distal femoral fractures, acceptable alignment was defined as varus malalignment <5° and valgus malalignment <10°8. For proximal tibial fractures, malalignment was defined as angulation >5° in either coronal or sagittal plane9, 10, 11, 12. The mode of injury was road traffic accidents in 75% of distal femoral fractures and 65% of proximal tibial fractures. Falls from heights were responsible for 25% of distal femoral fractures and 15% of proximal tibial fractures. Other mechanisms, including direct blows and assaults caused 20% of proximal tibial fractures.
The average time of fixation was 8 days after injury (0–31 days). Surgery was performed on 17 fractures (42.5%) on the day of injury. No temporary fixations in the form of external fixator were performed. All open fractures were treated by initial irrigation, surgical wound debridement and definitive fixation with locked plates. One patient with a compound proximal tibial fracture required a rotational flap to close the wound. Each patient received 1 g of ceftriaxone i.v. 30 min before surgery. Postoperatively, i.v. ceftriaxone and amikacin were used in all patients. Two patients whose proximal tibial fractures (AO 41 C3) were comminuted more medially underwent fixation with medial proximal tibial locked plates via a posteromedial approach. A minimally invasive anterolateral approach was used in all but one of the remaining proximal tibial fractures. A minimally invasive lateral approach was used for 70% of distal femoral fractures. The remaining distal femoral fractures were fixed by open reduction and internal fixation with LCPs. Active range of motion exercises were started on the day after surgery. All patients were followed up 2, 6 and 12 weeks after surgery. A standard regimen for weight bearing was followed by all patients, weight bearing starting 12–14 weeks postoperatively. Because secondary healing occurs after LCP, callus was not visible by this time in many patients. Many patients in whom callus was not visible were fully weight bearing without pain by the 12th–14th weeks (Fig. 1). Full weight bearing was delayed in patients in whom neither callus was visible nor weight bearing painless. Postoperatively, alignment was assessed by direct goniometric examination of X‐ray films. Knee Society scores were used for clinical and functional assessment.
Figure 1.
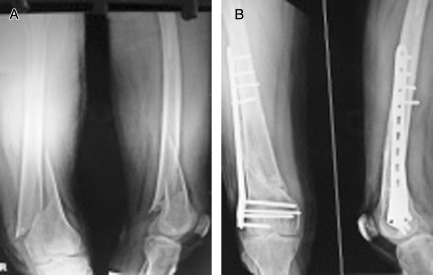
(A) AO type 33 A1 fracture and (B) union at 12 weeks. Note the scarcity of callus.
Results
Union Time
One patient with a proximal tibial fracture had no evidence of union 6 months after surgery. This patient underwent re‐operation with cancellous bone grafting and the fracture united in the next 14 weeks. The average union time of the remaining patients with proximal tibial fractures was 14.9 weeks, most fractures uniting between 13 and 16 weeks. One patient developed a deep infection and required serial debridement; union occurred in 24 weeks.
The average union time for distal femoral fractures was 15.2 weeks, most fractures uniting between 13 and 16 weeks. One patient developed a deep infection and healed in 24 weeks. Another patient in whom fracture healing took 24 weeks was quadriplegic. One patient presented with implant failure 7 weeks postoperatively. Union time was longer for compound fractures (18.6 weeks for distal femoral fractures as compared with an average of 15.2 weeks for all distal femoral fractures, 19.2 weeks for proximal tibial fractures as compared with an average of 14.9 weeks for all proximal tibial fractures). One important finding was that callus was visible at the onset of full painless weight bearing in only 56% of patients.
Functional Evaluation
Three patients who had both distal femoral and proximal tibial fractures were included in both groups. Three patients with proximal tibial fractures had extension lags of 10°–20°. The average range of motion of the knee joint in proximal tibial fractures was 109.5°. Two patients with distal femoral fractures developed extension lag of 20°. One quadriplegic patient with a distal femoral fracture developed a flexion contracture of 90°. A part one Knee Society score only was calculated for this patient. The average range of motion of the knee joint in distal femoral fractures was 95.83°.
The average Knee Society scores for proximal tibial fractures were 89.7 (excellent) and 88.75 (functional score, excellent). One patient with a distal femoral fracture had implant failure. One patient was quadriplegic and did not recover the ability to walk. The average Knee Society scores of the remaining 18 patients were 82.66 (excellent) and 77.77 (functional score, good).
Malalignment
Clinically significant coronal plane malreduction (10° varus) was observed in the immediate postoperative X‐ray films of one patient with a distal femoral fracture. However, revision surgery was not performed because the patient accepted this. Significant articular malreduction (>2 mm step‐off) was not seen in any case.
Complications
Superficial infection occurred in two patients with proximal tibial fractures. Of these patients also had hardware irritation. In one patient with a distal femoral and one with a proximal tibial fracture deep infection occurred. There was one case of implant failure and one of screw breakage in distal femoral fractures. One case of nonunion occurred in a proximal tibial fracture. No instances of loss of reduction or nerve injury were observed. Eighty percent of fractures healed without any complications. One patient with a proximal tibial fracture who went on to nonunion required cancellous bone grafting and ultimately healed in 38 weeks (14 weeks after grafting).
Minimally Invasive Percutaneous Plate Osteosynthesis Versus Open Reduction
Only 30% of distal femoral and 5% of proximal tibial fractures were treated by open reduction. Union time was more for fractures treated by open reduction than for those treated by the MIPPO technique (18.33 weeks for distal femoral fractures as compared with an average of 15.2 weeks). Both cases of deep infection occurred in compound fractures treated by open reduction. The only case of malreduction of a distal femur fracture had been treated by the MIPPO technique.
Discussion
Many advantages of LCPs are well established. They cause less compression of periosteal blood supply and promote healing. Their advantages in osteoporotic fractures13 and their sub‐muscular minimally invasive insertion make them a viable option for periarticular fractures. Precontouring of these plates according to condyle design enhances the surgeon's ability to insert the plate in a submuscular manner for minimally invasive application14.
In this prospective study of locked plate fixation, all surgeries were performed by experienced surgeons with years of experience of management of orthopaedic trauma at a tertiary level referral center. Various techniques for treatment of peri and intra‐articular fractures around the knee have been described. The goal of this series was to evaluate the role of locked plates. Limitations of this study were the short follow up (maximum 23 months) and small cohort (n = 40). However, because our main concern was to evaluate the union rate and complications, these limitations do not invalidate our results. Contrary to other similar recent studies, we included both distal femoral and proximal tibial fractures in our series for many reasons, including the many similar anatomical features of these fractures (broadened condyles and tapering shaft, which make use of prebent anatomical plates feasible), similar mechanisms of injuries (valgus or varus forces with axial loading as in dashboard and bumper strike injuries) and their frequent association with each other.
Most published studies of LCPs do not include both distal femoral and proximal tibial fractures. We therefore compared our results with those of other studies of locked plates (mainly less invasive stabilization system [LISS]) for either proximal tibial or distal femoral fractures. The average age of all cases of distal femoral fractures was 37.05 years and of proximal tibial fractures 35.05 years. Thus, these fractures are more common in middle age, as was true in our study: most patients were between 31 and 40 years of age. This may be partly due to the fact that in India more than 65% of people are <35 years old.
There were 15 men (75%) and 5 women (25%) with distal femoral fractures and 16 men (80%) and 4 women (20%) with proximal tibial fractures, showing a preponderance of men. In other studies of distal femoral fractures, Baumgaertel and Gotzen reported a male preponderance15, whereas a female preponderance was reported by Ostrum and Geel16, Schütz et al.17 and Kregor et al.18 In other studies of proximal tibial fractures, Cole et al. reported a male preponderance 19, whereas more patients were female in Boldin et al.'s study20. In our study, the male preponderance was attributable to the fact that mainly males are involved in road traffic accidents (RTA), which were the commonest mode of injury (75% of distal femoral fractures, 65% cases of proximal tibial fractures). RTA was also the commonest mechanism of injury in other studies of proximal tibial fractures by Cole et al.19 and Boldin et al.20 Markmiller et al., in their study of distal femoral fractures, reported high energy trauma, including RTAs, as the commonest mode of injury21.
Ipsilateral lower limb traumas (either proximal tibial or distal femoral fractures) were the most commonly associated injuries in our series. We found a right sided preponderance of distal femoral fractures and a left sided preponderance of proximal tibial fractures. Eleven distal femoral fractures (55%) and 15 proximal tibial fractures (75%) were AO type C (intra articular). Markmiller et al., in their study of distal femoral fractures, reported 46% type C fractures21. Most of the studies on fixation of proximal tibial fractures (Schütz et al.8, Cole et al.19, Stannard et al.10 and Ricci et al.11) also reported that intra‐articular type C fractures outnumbered extra‐articular fractures.
The average time for union of distal femoral fractures was 15.2 weeks, most fractures uniting between 13 and 16 weeks. The average healing time in other studies also ranges between 14 and 18 weeks. The average union time for proximal tibial fractures was 14.9 weeks, most fractures uniting between 13 and 16 weeks. The average union time in other proximal tibial studies is between 11 and 15 weeks, which compares well with this study (14.9, 12–38 weeks).
As compared with other studies, the infection rate was slightly higher for distal femoral fractures. Clinically significant malunion was seen in one case. This patient's fracture healed in 10° of varus. In this series two patients had implant failure, one of these returning 7 weeks postoperatively with plate breakage. This patient underwent revision surgery with interlocking nailing. In this patient, bridge plating had been done with adequate reduction and the length of plate was adequate (more than three times the length of comminution). Two screw holes had been left empty on either side of comminution. Four screws had been inserted in the shaft and five in the condylar area. The screw to hole ratio in the shaft was 0.4. This patient started early weight bearing in contravention of our standard postoperative protocol of delayed weight bearing; this probably explained the plate breakage. However, Haak et al., in their study of 32 patients with partial articular proximal tibial fractures fixed with locking plates, suggested that early weight bearing can be allowed22.
One patient, who was quadriplegic and completely unable to walk, presented at 24 weeks with all proximal screws broken: in this patient reduction, working length and screw density had also all been adequate. Although radiological union had occurred, all the proximal screws had broken. We were unable to identify a cause for this screw failure.
We saw no cases of nerve injury, implant failure or compartment syndrome, as reported by other studies. One case went on to nonunion. In this case reduction was not adequate and a fracture site gap was present in postoperative X‐ray films (Fig. 2). Because LCPs do not provide compression of the fracture fragments, locked screws should be tightened after adequate reduction or after lag screw to provide compression. This patient underwent reoperation with bone grafting and the fracture healed 14 weeks after the second surgery. In their experimental study, Dee M et al. raised a particular concern about popliteal artery injury in LCP23. We encountered no cases of popliteal artery injury. We achieved comparable results to other recent series on LCPs around knees24, 25, 26. Haidukewych et al., in their study of 54 patients with periarticular fractures around the knee (25 distal femoral and 31 proximal tibial fractures), reported a 94% union rate without any varus collapse or implant failure24.
Figure 2.
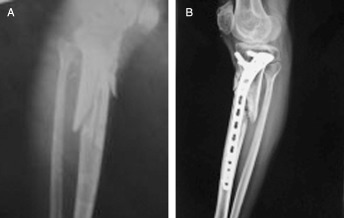
LCP without adequate reduction can lead to nonunion. (A) This AO 41A3 fracture was fixed with LCP with a gap between the fracture fragments (B). This fracture went on to nonunion and required reoperation and bone grafting.
We concluded from our study that LCPs may provide an improvement in the treatment of complex peri‐ & intra‐articular fractures. The decreased soft tissue dissection compared with traditional plating is an important advantage. LCPs are one of the best available options for management of comminuted metaphyseal fractures, in which bridge plating gives excellent results (Figs 3 and 4). They are very useful implants in difficult cases in which both distal femur and proximal tibia are severely comminuted. They give excellent clinical and functional results in management of peri‐ and intra‐articular fractures provided they are applied with proper understanding of biomechanics; however, their advantages appear to be offset by difficulties in fracture reduction and plate application. Working length and position of screws are the most crucial factors for preventing implant failure and nonunion27. An increase in working length increases inter fragmentary motion in comminuted fractures and also distributes stress over a large area. This promotes fracture healing with formation of callus and also reduces chances of implant breakage. The technology of the application of TCPs and understanding of the biomechanics involved is still evolving: in future we may implement this potentially helpful technology in a better way.
Figure 3.
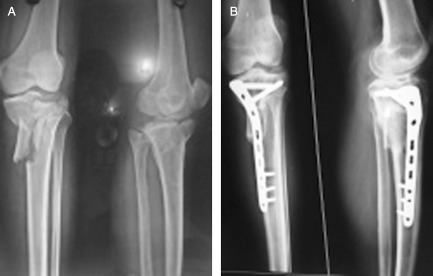
(A) AO type 41 C3 fracture. (B) This fracture was fixed with LCP and union was achieved by the 14th week.
Figure 4.
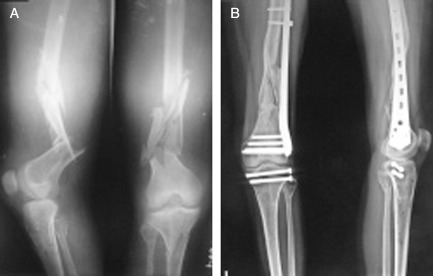
(A) AO 33A3 fracture and (B) union at the 20th week. Bridge plating with LCP is an excellent option for comminuted metaphyseal fractures around the knee. Cancellous screws were used for proximal tibial fracture as patient was not ready for proximal tibial plating.
Disclosure: The authors declare that they have received no financial support for this study. They have no conflicts of interest.
References
- 1. Freedman EL, Johnson EE. Radiographic analysis of tibial fracture malalignment following intramedullary nailing. Clin Orthop Relat Res, 1995, 315: 25–33. [PubMed] [Google Scholar]
- 2. Lang GJ, Cohen BE, Bosse MJ, Kellam JF. Proximal third tibial shaft fractures. Should they be nailed? Clin Orthop Relat Res, 1995, 315: 64–74. [PubMed] [Google Scholar]
- 3. Zlowodzki M, Williamson S, Cole PA, Zardiackas LD, Kregor PJ. Biomechanical evaluation of the less invasive stabilization system, angled blade plate, and retrograde intramedullary nail for the internal fixation of distal femur fractures. J Orthop Trauma, 2004, 18: 494–502. [DOI] [PubMed] [Google Scholar]
- 4. Ito K, Grass R, Zwipp H. Internal fixation of supracondylar femoral fractures: comparative biomechanical performance of the 95‐degree blade plate and two retrograde nails. J Orthop Trauma, 1998, 12: 259 – 266. [DOI] [PubMed] [Google Scholar]
- 5. Mukherjee P, Bovell C, Davis J. Less invasive stabilising system plate versus retrograde intramedullary nail for osteoporotic distal femoral fracture. Eur J Orthop Surg Traumatol, 2010, 20: 281–284. [Google Scholar]
- 6. Lachiewicz PF, Funcik T. Factors influencing the results of open reduction and internal fixation of tibial plateau fractures. Clin Orthop Relat Res, 1990, 259: 210–215. [PubMed] [Google Scholar]
- 7. Muller ME, Nazarian S, Koch P, Schatzker J. The Comprehensive Classification of Fractures of Long Bones. Berlin: Springer‐Verlag, 1990. [Google Scholar]
- 8. Schütz M, Kääb MJ, Haas N. Stabilization of proximal tibial fractures with the LIS‐system: early clinical experience in Berlin. Injury, 2003, 34 (Suppl 1): A30–A35. [DOI] [PubMed] [Google Scholar]
- 9. Cole PA, Zlowodzki M, Kregor PJ. Less Invasive Stabilization System (LISS) for fractures of the proximal tibia: indications, surgical technique and preliminary results of the UMC Clinical Trial. Injury, 2003, 34 (Suppl 1): A16–A29. [DOI] [PubMed] [Google Scholar]
- 10. Stannard JP, Wilson TC, Volgas DA, Alonso JE. Fracture stabilization of proximal tibial fractures with the proximal tibial LISS: early experience in Birmingham, Alabama (USA). Injury, 2003, 34 (Suppl 1): A36–A42. [DOI] [PubMed] [Google Scholar]
- 11. Ricci WM, Rudzki JR, Borrelli J Jr. Treatment of complex proximal tibia fractures with the less invasive skeletal stabilization system. J Orthop Trauma, 2004, 18: 521–527. [DOI] [PubMed] [Google Scholar]
- 12. Schandelmaier P, Partenheimer A, Koenemann B, Grün OA, Krettek C. Distal femoral fractures and LISS stabilization. Injury, 2001, 32 (Suppl 3): SC55–SC63. [DOI] [PubMed] [Google Scholar]
- 13. Fulkerson E, Egol KA, Kubiak EN, Liporace F, Kummer FJ, Koval KJ. Fixation of diaphyseal fractures with a segmental defect: a biomechanical comparison of locked and conventional plating techniques. J Trauma, 2006, 60: 830–835. [DOI] [PubMed] [Google Scholar]
- 14. Smith WR, Ziran BH, Anglen JO, Stahel PF. Locking plates: tips and tricks. J Bone Joint Surg Am, 2007, 89: 2298–2307. [DOI] [PubMed] [Google Scholar]
- 15. Baumgaertel F, Gotzen L. The “biological” plate osteosynthesis in multi‐fragment fractures of the para‐articular femur. A prospective study. Unfallchirurg, 1994, 97: 78–84. [PubMed] [Google Scholar]
- 16. Ostrum RF, Geel C. Indirect reduction and internal fixation of supracondylar femur fractures without bone graft. J Orthop Trauma, 1995, 9: 278–284. [DOI] [PubMed] [Google Scholar]
- 17. Schütz M, Müller M, Krettek C, et al Minimally invasive fracture stabilization of distal femoral fractures with the LISS: a prospective multicenter study. Results of a clinical study with special emphasis on difficult cases. Injury, 2001, 32 (Suppl 3): SC48–SC54. [DOI] [PubMed] [Google Scholar]
- 18. Kregor PJ, Stannard J, Zlowodzki M, Cole PA, Alonso J. Distal femoral fracture fixation utilizing the Less Invasive Stabilization System (L.I.S.S.): the technique and early results. Injury, 2001, 32 (Suppl 3): SC32–SC47. [DOI] [PubMed] [Google Scholar]
- 19. Cole PA, Zlowodzki M, Kregor PJ. Treatment of proximal tibia fractures using the less invasive stabilization system: surgical experience and early clinical results in 77 fractures. J Orthop Trauma, 2004, 18: 528–535. [DOI] [PubMed] [Google Scholar]
- 20. Boldin C, Fankhauser F, Hofer HP, Szyszkowitz R. Three‐year results of proximal tibia fractures treated with the LISS. Clin Orthop Relat Res, 2006, 445: 222–229. [DOI] [PubMed] [Google Scholar]
- 21. Markmiller M, Konrad G, Femur SN. LISS and distal femoral nail for fixation of distal femoral fractures: are there differences in outcome and complications. Clin Orthop Relat Res, 2004, 426: 252–257. [DOI] [PubMed] [Google Scholar]
- 22. Haak KT, Palm H, Holck K, Krasheninnikoff M, Gebuhr P, Troelsen A. Immediate weight‐bearing after osteosynthesis of proximal tibial fractures may be allowed. Dan Med J, 2012, 59: A4515. [PubMed] [Google Scholar]
- 23. Dee M, Sojka JM, Daccarett MS, Mormino MA. Evaluation of popliteal artery injury risk with locked lateral plating of the tibial plateau. J Orthop Trauma, 2011, 25: 603–607. [DOI] [PubMed] [Google Scholar]
- 24. Haidukewych G, Sems SA, Huebner D, Horwitz D, Levy B. Results of polyaxial locked‐plate fixation of periarticular fractures of the knee. J Bone Joint Surg Am, 2007, 89: 614–620. [DOI] [PubMed] [Google Scholar]
- 25. Ehlinger M, Rahme M, Moor BK, et al Reliability of locked plating in tibial plateau fractures with a medial component. Orthop Traumatol Surg Res, 2012, 98: 173–179. [DOI] [PubMed] [Google Scholar]
- 26. Nayak RM, Koichade MR, Umre AN, Ingle MV. Minimally invasive plate osteosynthesis using a locking compression plate for distal femoral fractures. J Orthop Surg (Hong Kong), 2011, 19: 185–190. [DOI] [PubMed] [Google Scholar]
- 27. Nassiri M, MacDonald B, O'Byrne JM. Locking compression plate breakage and fracture non‐union: a finite element study of three patient‐specific cases. Eur J Orthop Surg Traumatol, 2012, 22: 275–281. [Google Scholar]


