Abstract
Introduction:
Outpatient procedures are an important component of primary care, yet few programs incorporate procedural training into their curriculum. We examined a 4-year procedural curriculum to improve understanding of ambulatory procedures and increase the number of procedures performed.
Methods:
A total of 56 resident and 8 faculty physicians participated in a procedural curriculum directed at joint injections (knee, shoulder, elbow, trochanteric bursa, carpal tunnel, wrist, and ankle), subdermal contraceptive insertion/removal, skin biopsies, and ultrasound use in primary care. We administered annual surveys and used generalized estimating equations to model changes.
Results:
Across the 4 years, there was an average 96% response rate. Mean comfort level with the indications for procedures increased for both resident (62.5 to 78.8; P < .0001) and faculty physicians (61.5 to 94.8; P < .0001). Similarly, mean comfort with performing procedures increased for both resident (32.1 to 62.3; P < .0001) and faculty physicians (42.2 to 85.4; P < .0001). Residents’ comfort level performing procedures increased for all individual procedures measured. The mean number of procedures performed per year increased for resident (1.9 to 8.2; P < .0001) and faculty physicians (14.7 to 25.2; P = .087).
Conclusions:
A longitudinal ambulatory-based procedural curriculum can increase resident and faculty physician understanding and comfort performing primary-care-based procedures. This, in turn, increased the total number of procedures performed.
Keywords: Education, primary care, procedures, ambulatory, joint injection, ultrasound
Introduction
Teaching procedural skills has been a long-standing challenge for many residency programs. The American Board of Internal Medicine (ABIM) requires all residents to demonstrate knowledge and understanding of a specific defined set of procedures1. However, residents and even many faculty feel inadequately trained to perform common office-based procedures.2-4 As a result, general internists are performing fewer ambulatory procedures.5 Improved training could reverse this trend, decrease the need for referrals, and minimize delays in treatment.
Overall, procedural training is taught largely by an apprenticeship model, despite the literature suggesting that this traditional “see one, do one, teach one” method is inadequate.6-8 The most robust literature on improving procedural training focuses on invasive inpatient procedures, which are generally not applicable to today’s office-based primary care physician.9-13 Meanwhile, residents are asked to master ambulatory procedural skills during chance patient encounters, brief workshops, or subspecialty electives outside of their required residency experience.14-22
Internal medicine residency programs’ approach to procedural training could be improved by including more evidence-based methods.23 For example, simulation-based training methods that incorporate deliberate and distributed practice are associated with enhanced performance and improved clinical outcomes.24
This article describes a longitudinal framework for ambulatory procedural training. We examined the influence of a 4-year procedural curriculum to (a) improve resident and faculty understanding of the indications for multiple ambulatory procedures, (b) increase comfort level for performing these procedures, and (c) increase the number of procedures performed. The longitudinal curriculum included didactic sessions, hands-on ultrasound training, simulated procedures with anatomic models, and repetition of important concepts. We hypothesized that this approach would lead to an increase in resident and faculty understanding of the indications for the procedures taught, comfort level performing these procedures, and the total number of ambulatory procedures performed.
Methods
Setting and description of intervention
The procedural curriculum was implemented in an academic freestanding outpatient primary care office that served as the primary training site for internal medicine and pediatric residents. The 4-year curriculum was aimed at improving the resident and attending comfort levels with performing common procedures in the primary care setting. The procedural curriculum included specific sessions directed at knee arthrocentesis, shoulder injections, subacromial injections, elbow injections, trochanteric bursa injections, carpal tunnel injections, wrist injections, ankle injections, skin biopsies, subdermal contraceptive insertion/removal (Nexplanon), and ultrasound use to identify pertinent anatomy and guide injections. Depending on the topic, the sessions were led by a faculty rheumatologist, emergency department physician, gynecologist, or internist. Each session lasted between 60 and 90 minutes and included didactic teaching followed by hands-on training. The didactic sessions included (a) indications for the procedure, (b) review of the relevant anatomy, (c) review of evidence-based benefits and risks of the procedure, (d) strategies to deal with procedural difficulties or complications, (e) aftercare and results of follow-up, and (f) tips from subspecialties regarding best practices. Hands-on training for joint injections was performed using procedural mannequins. Skin biopsies were taught with simulated skin. Primary-care-based ultrasound techniques were taught on volunteer subjects. Faculty and residents were exposed to the following sessions twice over the curriculum: knee injections, shoulder injections, elbow injections, trochanteric bursa injections, carpal tunnel injections, ultrasound use, and skin biopsy. Faculty received the same procedural training as residents. Incoming interns were trained on subdermal contraceptive insertion (Nexplanon) annually. In between formal sessions, residents received ongoing training and practice on mannequins with faculty support. Prior to performing procedures on patients, residents were required to have an understanding of the indications and techniques required for the procedure and to demonstrate proficiency on mannequins. These skills and proficiencies were confirmed by faculty and all procedures performed on patients were supervised by faculty.
Surveys
We administered surveys every 6 to 12 months to assess resident and faculty comfort with the indications for procedure and comfort performing primary-care-based procedures. Comfort level for each procedure was assessed on a 0 to 10 scale, with 0 grounded as “Very Uncomfortable” and 10 as “Very Comfort-able.” The surveys also tracked the number of procedures performed. A copy of the survey is available in the Appendix.
Analyses
Our primary outcomes were resident and faculty physicians’ comfort with (a) indications for procedures, (b) performing procedures, and (c) number of procedures performed. We report mean comfort levels with all procedures combined and also report comfort levels with each individual procedure across the year in the procedural curriculum. The year can take a value from 1 to 4, depending on when the resident entered into the procedural curriculum. Given the longitudinal data and anticipation of correlated observations for residents and faculty during the observation period, we used a generalized estimating equation (GEE) approach, with the robust sandwich estimator to provide consistent estimates of the covariance matrix for parameter estimates. The GEE model provides a robust method to model the mean of the outcome without specifying a parametric distribution of the outcome. The slope represents the change in unit comfort level for each unit increase in year in the procedural curriculum. We present the associated lower and upper 95% confidence limits around the predicted value.
Ethical approval
This study was approved by the University of Rochester Research Subjects Review Board (RSRB).
Results
A total of 56 resident and 8 faculty physicians were included in the ambulatory procedural curriculum. A total of 50.0% of the respondents were 20 to 29 years old, 43.6% were 30 to 39 years old, 4.8% were 40 to 49 years old, and 1.6% were 50 years of age or more. Across the 4 years, there was an average 96% response rate on the surveys.
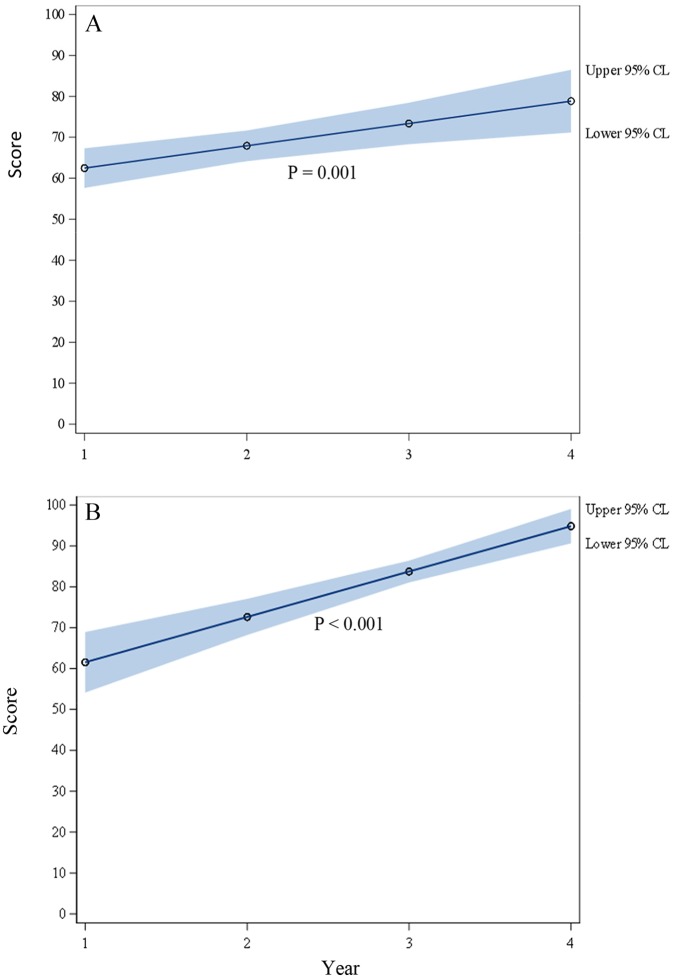
Figures 1 and 2 demonstrate the change in predicted mean comfort level for all procedures combined across the year in the procedural curriculum. Mean comfort level with the indications for procedures increased for both resident (62.5 to 78.8; P < .0001) and faculty physicians (61.5 to 94.8; P < .0001). Similarly, mean comfort with performing procedure increased for both resident (32.1 to 62.3; P < .0001) and faculty physicians (42.2 to 85.4; P < .0001).
Figure 1.
Comfort level with indications for procedures for (A) residents and (B) faculty. CL indicates confidence limit.
Figure 2.
Comfort level with performing procedures for (A) residents and (B) faculty. CL indicates confidence limit.
Table 1 presents the slopes for the changes in comfort levels with indications for individual procedures across the year in program. Residents’ mean comfort level with the indications for the procedure increased for shoulder injections, elbow injections, trochanteric bursa injections, carpal tunnel injections, and using primary-care-based ultrasound. Faculty physician mean comfort level increased for Nexplanon insertion/removal, elbow injections, ankle injections, skin biopsy, and using primary-care-based ultrasound.
Table 1.
Comfort level with indications for individual procedures.
| Resident |
Faculty |
|||||||
|---|---|---|---|---|---|---|---|---|
| Slope | 95% confidence interval | P-value | Slope | 95% confidence interval | P-value | |||
| Nexplanon insertion/removal | 0.44 | 0.01 | 0.87 | 0.042 | 1.89 | 0.64 | 3.15 | 0.003 |
| Knee arthrocentesis | 0.47 | 0.09 | 0.84 | 0.015 | 0.34 | −0.31 | 0.99 | 0.307 |
| Shoulder injections | 0.59 | 0.19 | 0.99 | 0.004 | 0.36 | −0.30 | 1.03 | 0.284 |
| Subacromial injections | 0.52 | 0.07 | 0.96 | 0.023 | 0.28 | −0.05 | 0.61 | 0.095 |
| Elbow injections | 0.44 | 0.03 | 0.85 | 0.035 | 0.72 | 0.20 | 1.23 | .006 |
| Trochanteric bursa injections | 0.77 | 0.42 | 1.13 | <0.0001 | 0.16 | −0.10 | 0.41 | 0.217 |
| Carpal tunnel injections/wrist injections | 0.58 | 0.23 | 0.93 | 0.001 | 0.77 | −0.22 | 1.77 | 0.129 |
| Ankle injections | 0.38 | −0.02 | 0.77 | 0.066 | 1.37 | 0.21 | 2.54 | 0.021 |
| Skin biopsy | 0.20 | −0.21 | 0.62 | 0.331 | 2.14 | 1.42 | 2.87 | <0.0001 |
| Using ultrasound | 0.69 | 0.32 | 1.07 | <0.001 | 2.31 | 1.82 | 2.80 | <0.0001 |
Table 2 presents the slopes for the changes in comfort levels with performing different procedures across the year in procedural training program. Residents’ mean comfort level with performing procedures increased for all individual procedures.
Table 2.
Comfort level with performing individual procedures.
| Resident |
Faculty |
|||||||
|---|---|---|---|---|---|---|---|---|
| Slope | 95% confidence interval | P-value | Slope | 95% confidence interval | P-value | |||
| Nexplanon insertion/removal | 2.05 | 1.57 | 2.53 | <0.0001 | 2.87 | 2.32 | 3.42 | <0.0001 |
| Knee arthrocentesis | 0.94 | 0.57 | 1.30 | <0.0001 | 0.73 | 0.15 | 1.30 | 0.013 |
| Shoulder injections | 0.90 | 0.50 | 1.29 | <0.0001 | 0.85 | 0.06 | 1.65 | 0.036 |
| Subacromial injections | 0.91 | 0.51 | 1.30 | <0.0001 | 0.39 | −0.15 | 0.93 | 0.153 |
| Elbow injections | 0.62 | 0.29 | 0.96 | <0.001 | 0.84 | −0.14 | 1.82 | 0.092 |
| Trochanteric bursa injections | 1.16 | 0.80 | 1.51 | <0.0001 | 0.31 | −0.01 | 0.64 | 0.057 |
| Carpal tunnel injections/wrist injections | 1.0 | 0.62 | 1.38 | <0.0001 | 1.56 | 0.50 | 2.61 | 0.004 |
| Ankle injections | 0.49 | 0.14 | 0.84 | 0.006 | 1.36 | 0.59 | 2.13 | 0.001 |
| Skin biopsy | 0.66 | 0.22 | 1.10 | 0.004 | 2.28 | 1.79 | 2.78 | <0.0001 |
| Using ultrasound | 0.97 | 0.58 | 1.37 | <0.0001 | 2.88 | 2.48 | 3.27 | <0.0001 |
Figure 3 depicts the predicted mean number of procedures performed per year over the year in the project. The mean number of procedures performed increased for both resident (1.9 to 8.2; P < .0001) and faculty physicians (14.7 to 25.2; P < .087) in the primary care setting.
Figure 3.
Number of procedures performed by (A) residents and (B) faculty. CL indicates confidence limit.
Discussion
Training resident physicians in outpatient procedures is an important component of primary care education, yet few programs purposefully implement organized ambulatory procedural training into their outpatient curriculum. This study demonstrated that a longitudinal educational intervention that included anatomic models, ultrasound, and deliberate and reinforced practice increased both resident and faculty physician understanding of the indications for a broad range of ambulatory procedures as well as their comfort performing these procedures. This was, in turn, associated with an increase in the number of procedures performed within the clinical practice.
This educational intervention was unique in its comprehensive approach that (a) included training in a broad range of ambulatory procedures, (b) was based in an outpatient primary care setting, (c) was longitudinal with built-in repetition across 4 years allowing for distributed practice, (d) integrated both anatomic models and ultrasound into the intervention, and (e) targeted both attending and resident physicians to support sustainability. Prior studies have shown that educational interventions can increase both confidence and performance of invasive procedures.10-13 Most of these interventions, however, are more narrowly focused on either of one-time educational sessions, inpatient procedures, or subspecialty training.14-26 We found that our integrated, longitudinal approach incorporating ultrasound and multiple teaching modalities improved comfort performing procedures and increased the total number of procedures performed by residents.
Longitudinal training that includes repetition and the opportunity to revisit each procedure through distributed practice has been shown to improve acquisition and retention of procedural expertise.27 The opportunity to revisit each procedure at least once after a period of time provides a “booster dose” of training that results in better and more prolonged retention of knowledge and skill.27 Our intervention included this repetition and distributed practice and resulted in both an increased comfort level performing procedures and an increased number of procedures performed. Our longitudinal curriculum also incorporated a broad range of ambulatory primary-care-based procedures. The breadth of procedures taught further reinforced the acquisition of key primary-care-based procedural skills.
In addition to a broad range of procedures, our curriculum incorporated both anatomic models and the use of ultrasound. The use of ultrasound has been shown to enhance the teaching of anatomy and improve the accuracy of joint injections when compared with surface-landmark-guided procedures.28-31 Although ultrasound has been used extensively in the inpatient setting,9 the use of ultrasound for training residents in ambulatory procedures in a primary care has not been specifically studied. The use of ultrasound in primary care offers many advantages to help learners better visualize the real-time and dynamic details of the relevant anatomy. Furthermore, the use of ultrasound may strengthen and add enthusiasm to the overall educational experience.
Our intervention had the added advantage of being embedded in an existing resident-teacher relationship in a residency continuity clinic. We simultaneously included primary care faculty and residents into the intervention to support sustainability through a “teach the teachers” approach.8 By including both resident and faculty members in the same teaching activity, it reduces the psychological size difference perceived by the residents between themselves and the faculty members.32 In addition, by training the faculty in these procedures, it has the potential to lead to a more sustained increase in procedures in the primary care office over time.
Expanding primary-care-office-based procedures has several implications and offers multiple potential benefits to patients, providers, and the health care system. Patients benefit by having the procedure performed by their primary physician, at a familiar location, and with minimum delay, often during the same visit at which the procedure is deemed necessary. This facilitates the treatments for patients and may limit the need for external referrals. Providing ambulatory procedures within primary care offices thus offers the potential to limit dispersions and fragmentation of care and may in turn increase subspecialists’ availability.
This study examined a longitudinal procedural intervention in primary care, but has several limitations. First, our study involved a single residency program, which may impair the generalizability of the findings. Second, the ultrasound and anatomic models may not be available at all programs. Third, although both an increase in confidence and numbers of procedures performed were seen over the 4 years of the intervention, we do not have data on residents’ procedural performance post residency graduation. Last, although residents were required to demonstrate an understanding of the indications and techniques required for the procedure and to demonstrate proficiency on mannequins, the study was not set up to measure procedural technical performance on patients, clinical outcomes, or patient satisfaction. Future studies may expand on this initiative by collecting further implementation and patient-level data.
Conclusions
Implementation of a longitudinal procedure training curriculum in the ambulatory setting that involves repetition, distributed practice, ultrasound, and anatomic models can improve physician understanding about the indications for procedures, enhance confidence in performing these procedures, and increase the total number of procedures performed. Expanding procedural training, in turn, offers the potential to strengthen the overall residency training experience, expand access to patients for necessary office-based procedures, and reduce fragmentation of care.
Appendix
Ambulatory Care Training Program: Procedural Curriculum
Name:________________________________
1. Please indicate your level of training:
| □ | Resident PGY-1 |
| □ | Resident PGY-2 |
| □ | Resident PGY-3 |
| □ | Resident PGY-4 |
| □ | Faculty |
2. Gender:
| □ | Male |
| □ | Female |
3. Age:
| □ | 20–29 |
| □ | 30–39 |
| □ | 40–49 |
| □ | 50–59 |
| □ | 60–69 |
4. Please indicate your comfort level with the indications for the following procedures:
| Procedure | Very Uncomfortable | Very Comfortable | ||||||||
|---|---|---|---|---|---|---|---|---|---|---|
| 1 | 2 | 3 | 4 | 5 | 6 | 7 | 8 | 9 | 10 | |
| Nexplanon Insertion/Removal | □ | □ | □ | □ | □ | □ | □ | □ | □ | □ |
| Knee Arthrocentesis | □ | □ | □ | □ | □ | □ | □ | □ | □ | □ |
| Shoulder Injections | □ | □ | □ | □ | □ | □ | □ | □ | □ | □ |
| Subacromial Injections | □ | □ | □ | □ | □ | □ | □ | □ | □ | □ |
| Elbow Injections | □ | □ | □ | □ | □ | □ | □ | □ | □ | □ |
| Trochanteric Bursa Injections | □ | □ | □ | □ | □ | □ | □ | □ | □ | □ |
| Carpal Tunnel Injections / Wrist Injections | □ | □ | □ | □ | □ | □ | □ | □ | □ | □ |
| Ankle Injections | □ | □ | □ | □ | □ | □ | □ | □ | □ | □ |
| Skin Biopsy | □ | □ | □ | □ | □ | □ | □ | □ | □ | □ |
| Using Ultrasound to guide injections | □ | □ | □ | □ | □ | □ | □ | □ | □ | □ |
5. Please indicate your comfort level with performing the following procedures:
| Procedure | Very Uncomfortable | Very Comfortable | ||||||||
|---|---|---|---|---|---|---|---|---|---|---|
| 1 | 2 | 3 | 4 | 5 | 6 | 7 | 8 | 9 | 10 | |
| Nexplanon Insertion/Removal | □ | □ | □ | □ | □ | □ | □ | □ | □ | □ |
| Knee Arthrocentesis | □ | □ | □ | □ | □ | □ | □ | □ | □ | □ |
| Shoulder Injections | □ | □ | □ | □ | □ | □ | □ | □ | □ | □ |
| Subacromial Injections | □ | □ | □ | □ | □ | □ | □ | □ | □ | □ |
| Elbow Injections | □ | □ | □ | □ | □ | □ | □ | □ | □ | □ |
| Trochanteric Bursa Injections | □ | □ | □ | □ | □ | □ | □ | □ | □ | □ |
| Carpal Tunnel Injections / Wrist Injections | □ | □ | □ | □ | □ | □ | □ | □ | □ | □ |
| Ankle Injections | □ | □ | □ | □ | □ | □ | □ | □ | □ | □ |
| Skin Biopsy | □ | □ | □ | □ | □ | □ | □ | □ | □ | □ |
| Using Ultrasound to guide injections | □ | □ | □ | □ | □ | □ | □ | □ | □ | □ |
6. Please indicate the number of the following procedure you have performed within the past 12 months:
| Procedure | 0 | 1 | 2 | 3 | 4 | 5 | 6 | 7 | 8 | 9 | 10+ |
|---|---|---|---|---|---|---|---|---|---|---|---|
| Nexplanon Insertion/Removal | □ | □ | □ | □ | □ | □ | □ | □ | □ | □ | □ |
| Knee Arthrocentesis | □ | □ | □ | □ | □ | □ | □ | □ | □ | □ | □ |
| Shoulder Injections | □ | □ | □ | □ | □ | □ | □ | □ | □ | □ | □ |
| Subacromial Injections | □ | □ | □ | □ | □ | □ | □ | □ | □ | □ | □ |
| Elbow Injections | □ | □ | □ | □ | □ | □ | □ | □ | □ | □ | □ |
| Trochanteric Bursa Injections | □ | □ | □ | □ | □ | □ | □ | □ | □ | □ | □ |
| Carpal Tunnel Injections / Wrist Injections | □ | □ | □ | □ | □ | □ | □ | □ | □ | □ | □ |
| Ankle Injections | □ | □ | □ | □ | □ | □ | □ | □ | □ | □ | □ |
| Skin Biopsy | □ | □ | □ | □ | □ | □ | □ | □ | □ | □ | □ |
| Using Ultrasound to guide injections | □ | □ | □ | □ | □ | □ | □ | □ | □ | □ | □ |
Footnotes
Funding:The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This project was supported by a grant from the Doctors across New York Ambulatory Care Training Program.
Declaration of conflicting interests:The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Author Contributions: RJF made substantial contributions to the conception, design and analysis; educational content; analysis and interpretation of data; and writing the manuscript. BM, GW, SS, EC, KN, TB, and BWR made substantial contributions to the conception and design of the work/analysis; educational content; acquisition and interpretation of data; and writing the manuscript. SM made contributions to the analysis and interpretation of data; and writing the manuscript. TLP made contributions to the educational content and acquisition of surveys.
References
- 1. American Board of Internal Medicine (ABIM). Policies and procedures for certification. https://www.abim.org/~/media/ABIM%20Public/Files/pdf/publications/certification-guides/policies-and-procedures.pdf.Up-dated2019.
- 2. Hicks CM, Gonzalez R, Morton MT, Gibbons RV, Wigton RS, Anderson RJ. Procedural experience and comfort level in internal medicine trainees. J Gen Intern Med. 2000;15:716–722. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3. Wickstrom GC, Kolar MM, Keyserling TC, et al. Confidence of graduating internal medicine residents to perform ambulatory procedures. J Gen Intern Med. 2000;15:361–365. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4. Schnobrich DJ, Gladding S, Olson AP, Duran-Nelson A. Point-of-care ultrasound in internal medicine: a national survey of educational leadership. J Grad Med Educ. 2013;5:498–502. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5. Wigton RS, Alguire P. The declining number and variety of procedures done by general internists: a resurvey of members of the American College of Physicians. Ann Intern Med. 2007;146:355–360. [DOI] [PubMed] [Google Scholar]
- 6. Lenchus JD. End of the “see one, do one, teach one” era: the next generation of invasive bedside procedural instruction. J Am Osteopath Assoc. 2010;110:340–346. [PubMed] [Google Scholar]
- 7. Boots RJ, Egerton W, McKeering H, Winter H. They just don’t get enough! Variable intern experience in bedside procedural skills. Intern Med J. 2009;39:222–227. [DOI] [PubMed] [Google Scholar]
- 8. Mourad M, Kohlwes J, Maselli J, Auerbach AD. Supervising the supervisors—procedural training and supervision in internal medicine residency. J Gen Intern Med. 2010;25:351–356. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9. Tukey MH, Wiener RS. The impact of a medical procedure service on patient safety, procedure quality and resident training opportunities. J Gen Intern Med. 2014;29:485–490. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10. Habeeb K, Axelband J. Incoming medical resident perception of competency and knowledge base of basic medical procedure enhanced by procedural workshop and educational material. Intens Care Med 2014;40:S160. [Google Scholar]
- 11. Lenchus J, Issenberg SB, Murphy D, et al. A blended approach to invasive bedside procedural instruction. Med Teach. 2011;33:116–123. [DOI] [PubMed] [Google Scholar]
- 12. Brydges R, Stroud L, Wong BM, Holmboe ES, Imrie K, Hatala R. Core competencies or a competent core? A scoping review and realist synthesis of invasive bedside procedural skills training in internal medicine. Acad Med. 2017;92:1632–1643. [DOI] [PubMed] [Google Scholar]
- 13. Huang GC, McSparron JI, Balk EM, et al. Procedural instruction in invasive bedside procedures: a systematic review and meta-analysis of effective teaching approaches. BMJ Qual Saf. 2016;25:281–294. [DOI] [PubMed] [Google Scholar]
- 14. Barilla-Labarca ML, Tsang JC, Goldsmith M, Furie R. Design, implementation, and outcome of a hands-on arthrocentesis workshop J Clin Rheumatol. 2009;15:275–279. [DOI] [PubMed] [Google Scholar]
- 15. Sterrett AG, Bateman H, Guthrie J, et al. Virtual rheumatology: using simulators and a formal workshop to teach medical students, internal medicine residents, and rheumatology subspecialty residents arthrocentesis J Clin Rheumatol. 2011;17:121–123. [DOI] [PubMed] [Google Scholar]
- 16. Jolly M, Hill A, Mataria M, Agarwal S. Influence of an interactive joint model injection workshop on physicians’ musculoskeletal procedural skills J Rheumatol. 2007;34:1576–1579. [PubMed] [Google Scholar]
- 17. Wilcox T, Oyler J, Harada C, Utset T. Musculoskeletal exam and joint injection training for internal medicine residents. J Gen Intern Med. 2006;21:521–523. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18. Schumacher HR, Chen LX, Glick L. Evaluation of a knee and shoulder arthrocentesis training program for primary care providers. J Rheumatol. 2008;35:2083–2084. [PubMed] [Google Scholar]
- 19. Berman JR, Ben-Artzi A, Fisher MC, Bass AR, Pillinger MH. A comparison of arthrocentesis teaching tools: cadavers, synthetic joint models, and the relative utility of different educational modalities in improving trainees’ comfort with procedures. J Clin Rheumatol. 2012;18:175–179. [DOI] [PubMed] [Google Scholar]
- 20. Gormley GJ, Steele WK, Stevenson M, et al. A randomised study of two training programmes for general practitioners in the techniques of shoulder injection. Ann Rheum Dis. 2003;62:1006–1009. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21. Ojeda JC, Colbert JA, Lin X, et al. Pocket-sized ultrasound as an aid to physical diagnosis for internal medicine residents: a randomized trial. J Gen Intern Med. 2015;30:199–206. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 22. Town JA, Bergl PA, Narang A, McConville JF. Internal medicine residents’ retention of knowledge and skills in bedside ultrasound. J Grad Med Educ. 2016;8:553–557. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23. Ma IWY, Arishenkoff S, Wiseman J, et al. Internal medicine point-of-care ultrasound curriculum: consensus recommendations from the Canadian Internal Medicine Ultrasound (CIMUS) Group. J Gen Intern Med. 2017;32:1052–1057. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24. McGaghie WC, Issenberg SB, Barsuk JH, Wayne DB. A critical review of simulation-based mastery learning with translational outcomes. Med Educ. 2014;48:375–385. [DOI] [PubMed] [Google Scholar]
- 25. Oxentenko AS, Ebbert JO, Ward LE, Pankratz VS, Wood KE. A multidimensional workshop using human cadavers to teach bedside procedures Teach Learn Med. 2003;15:127–130. [DOI] [PubMed] [Google Scholar]
- 26. Vogelgesang SA, Karplus TM, Kreiter CD. An instructional program to facilitate teaching joint/soft-tissue injection and aspiration. J Gen Intern Med. 2002;17:441–445. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 27. Benjamin AS, Tullis J. What makes distributed practice effective? Cogn Psychol. 2010;61:228–247. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 28. Cunnington J, Marshall N, Hide G, et al. A randomized, double-blind, controlled study of ultrasound-guided corticosteroid injection into the joint of patients with inflammatory arthritis. Arthritis Rheum. 2010;62:1862–1869. [DOI] [PubMed] [Google Scholar]
- 29. Patel SG, Benninger B, Mirjalili SA. Integrating ultrasound into modern medical curricula. Clin Anat. 2017;30:452–460. [DOI] [PubMed] [Google Scholar]
- 30. So S, Patel RM, Orebaugh SL. Ultrasound imaging in medical student education: impact on learning anatomy and physical diagnosis. Anat Sci Educ. 2017;10:176–189. [DOI] [PubMed] [Google Scholar]
- 31. Keddis MT, Cullen MW, Reed DA, et al. Effectiveness of an ultrasound training module for internal medicine residents. BMC Med Educ. 2011;11:75. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 32. Vaughn LM, Baker RC. Psychological size and distance: emphasising the interpersonal relationship as a pathway to optimal teaching and learning conditions. Med Educ. 2004;38:1053–1060. [DOI] [PubMed] [Google Scholar]