Abstract
A 60-year-old man was diagnosed with psoriasis 4 years ago. Treatment with adalimumab (a monoclonal anti-TNF-α antibody) became ineffective 1 year ago, and proteinuria and urinary occult blood were detected. Treatment with topical medicine, ultraviolet therapy, and etretinate resulted in remission of psoriasis, and proteinuria and hematuria also improved. For maintenance of remission, treatment with secukinumab (a human anti-interleukin-17A monoclonal antibody) was initiated. After the induction phase, treatment was changed from once a week to once every 4 weeks. After 5 months, he developed nephritis with kidney dysfunction, hematuria, and severe proteinuria (14 g/g Cr) accompanied by pitting edema. After admission, treatment with secukinumab was continued. Kidney biopsy revealed IgA nephropathy with fibrocellular crescents, and immunofluorescence analysis did not detect galactose-deficient IgA1. With these findings, he was diagnosed as secondary IgA nephropathy associated with psoriasis. Tonsillectomy followed by steroid pulse therapy prevented proteinuria and kidney function. In this case, treatment of refractory psoriasis with secukinumab and tonsillectomy was effective, leading to remission of relapsing secondary IgA nephropathy. Therefore, secukinumab might play an immunological role in the treatment of nephropathy.
Keywords: IgA nephropathy, Psoriasis, Secukinumab, IL-17A, Biologics
Introduction
Psoriasis is an autoimmune-related disease that is characterized by chronic inflammation [1]. A common treatment for psoriasis is topical therapy, such as steroid ointment or systemic immunosuppressive drugs. Psoriasis is also known to be associated with kidney dysfunction. It is reported that defects in T cell function or increased immune complexes play a role [2], and the association between this activity and increased risk for kidney disease has also been reported [3]. Inflammatory diseases, such as psoriasis, are exacerbating factors of IgA nephropathy [4]. In recent years, biological drugs, such as adalimumab or secukinumab, have been reported to be effective for the treatment of resistant cases [5, 6]; however, the association between biologics treatment and the clinical course of nephritis has rarely been reported. Moreover, the underlying mechanisms of kidney injury in psoriasis remain unclear. Here, we describe the case with psoriasis who developed secondary IgA nephropathy during treatment with secukinumab and discuss some potential underlying relationships.
Case presentation
A 60-year-old man was diagnosed with psoriasis 4 years ago. Treatment was initiated with steroid ointment, but his psoriasis did not improve. His psoriasis area and severity index (PASI, range 0–72) score was 40. Treatment with adalimumab, a monoclonal anti-TNF-α antibody, was initiated, and psoriasis improved with treatment. The patient developed hypertension, and antihypertensive drugs including angiotensin II receptor blockers were started.
Although the psoriasis was well controlled for 3 years, it relapsed (month 0). The patient’s PASI score was 40 (Fig. 1). Symptoms of peripheral edema, fever, anorexia, and difficulty walking arose. The patient was hospitalized and diagnosed with secondary failure of adalimumab. He also developed nephritis with severe kidney dysfunction [estimated glomerular filtration rate (eGFR) 26 mL/min/1.73 m2], proteinuria, and hematuria. Adalimumab was discontinued, and treatment with a steroid ointment, ultraviolet therapy, etretinate, and systemic antibiotics was started. The psoriasis improved and the patient’s PASI score was 2.8 (Fig. 1). Treatment with secukinumab, a human monoclonal antibody for interleukin (IL)-17A, was introduced to maintain remission. As psoriasis improved, nephritis improved gradually, and remission was achieved in a few weeks (Fig. 2). The patient was in remission with treatment of secukinumab and was regularly followed up in our outpatient clinic. After the induction phase, treatment with an injection of secukinumab changed from once a week to once every 4 weeks.
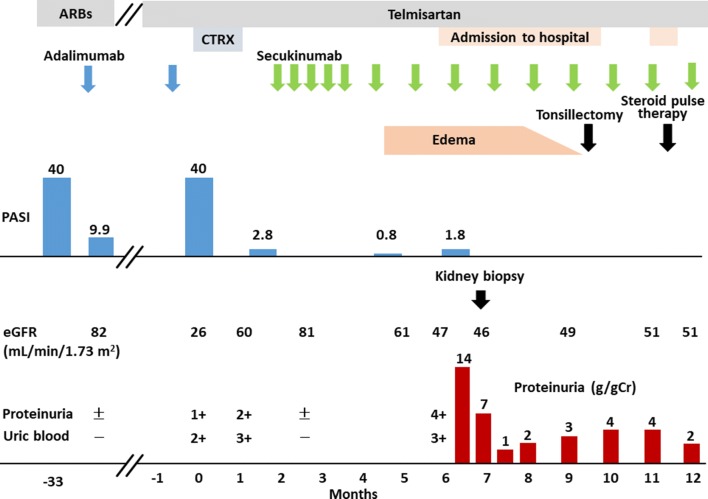
Fig. 1.
Clinical course of the patient. ARBs, Angiotensin II Receptor Blockers; CTRX, ceftriaxone; PASI, Psoriasis Area and Severity Index; eGFR, estimated glomerular filtration rate
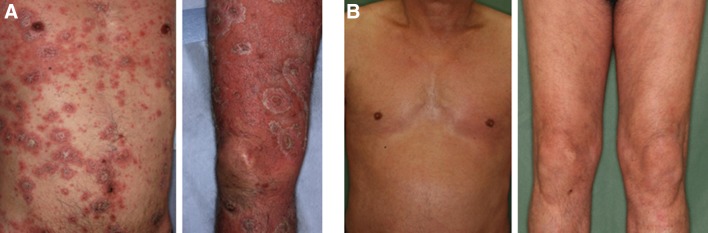
Fig. 2.
Photographs of the skin lesion. Upon recurrence of psoriasis (month 0), the PASI score was 40 (a). After 3 months of treatment with secukinumab (month 5), the PASI score was 0.8 (b)
Five months later (month 6), pitting edema in the lower legs appeared and worsened. The patient was diagnosed with nephrotic syndrome and admitted to our hospital for further investigation. On admission, his height was 164.8 cm and weight was 74.9 kg, which increased by 13 kg within 5 months. A CT scan demonstrated an increased visceral fat. His waist circumference was 92 cm. The patient had hypertension and dyslipidemia and he met the diagnostic criteria for metabolic syndrome.
The patient’s blood pressure, heart rate, and body temperature were 134/76 mmHg, 75 bpm, and 36.4 °C, respectively. A mild psoriasis lesion was observed in the extensor surfaces of extremities. Laboratory data were as follows: proteinuria, 7.2 g/g Cr; hematuria, 3+; red blood cell casts, 1+; hemoglobin level, 14.8 g/dL; BUN, 18 mg/dL; serum Cr level, 1.15 mg/dL; eGFR, 49.8 mL/min/1.73 m2; total protein level, 5.9 g/dL; serum albumin level, 3.2 g/dL; IgG level, 777 mg/dL; IgA level, 844 mg/dL; IgM level, 43 mg/dL; C3, 98 mg/dL; C4, 17 mg/dL; CH50, 55 U/mL; ASO, < 70 IU/mL; ASK, 40 times; and C-reactive protein level, 0.2 mg/dL. We could not detect antinuclear antibodies, anti-double stranded DNA antibodies, proteinase-3 antineutrophil cytoplasmic antibodies (PR3-ANCA), myeloperoxidase-ANCA (MPO-ANCA), anti-glomerular basement membrane (GBM) antibodies, or cryoglobulin. An immunofixation electrophoresis test showed the presence of IgG kappa monoclonal protein. No evidence of amyloidosis or bone marrow disease was found after examination of the serum-free light-chain ratio and bone marrow examination.
Treatment continued with secukinumab and telmisartan, an angiotensin II receptor blocker. After 1 week on a sodium-restricted diet with bed rest, his blood pressure was under control, and proteinuria decreased gradually. Psoriasis also showed improvement. Hematuria and red blood cell casts persisted, even after the improvement of nephrotic syndrome. Kidney dysfunction with eGFR < 50 mL/min/1.73 m2 remained. To identify the cause of nephritis, kidney biopsy was performed on the 14th day after admission.
Light microscopy showed 14 glomeruli: two showed global sclerosis, four showed fibrocellular crescents, and two showed cellular crescents (Fig. 3). GBM thickening was not obvious. Diffuse mesangial hypercellularity and focal Bowman’s capsule adhesion were observed. Focal infiltration of lymphocytes was observed in the interstitial tissue, which accompanied mild fibrosis and tubular atrophy. Neutrophils and eosinophils were not found. No hyaline changes or fibrinoid necrosis was observed in arterioles. Immunofluorescence studies showed mesangial deposition of IgA, IgM, and β1c. Immunofluorescence analysis with KM55 monoclonal antibody [7] did not detect galactose-deficient IgA1 (Gd-IgA1) (Fig. 4). Electron microscopy showed electron dense deposits in the mesangial lesion. Based on these findings and the clinical course, we diagnosed the patient with secondary IgA nephropathy associated with psoriasis. Tonsillectomy followed by steroid pulse therapy was performed for the treatment of IgA nephropathy as well as psoriasis.
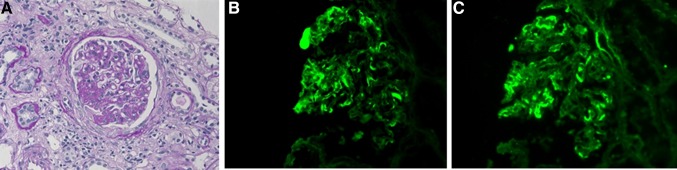
Fig. 3.
Photographs of light microscopy and immunofluorescence studies. Light microscopy of the kidney biopsy shows mild proliferation of mesangial cells and fibrocellular crescent (a; PAS staining × 400). Immunofluorescence studies showed mesangial deposition of IgA (b; × 400) and β1c (c; × 400)
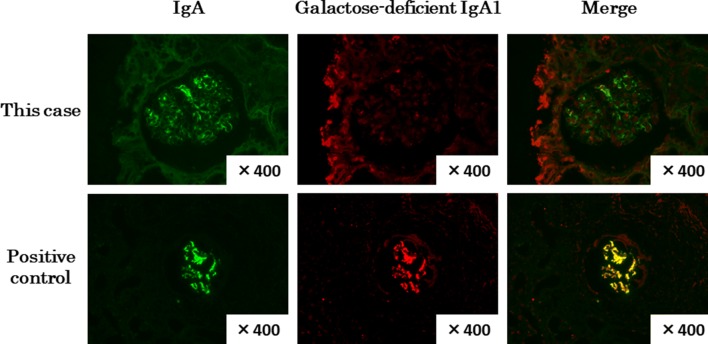
Fig. 4.
Photographs of immunofluorescence studies for the detection of galactose-deficient IgA1. In this case, galactose-deficient IgA1 in the mesangial lesion was not detected. The positive control was a case with 30-year-old man with primary IgA nephropathy. The primary antibody was an anti-human Gd-IgA1(KM-55) rat IgG MoAb (IBL, Gunma, Japan)
Proteinuria and edema improved after bed rest with continuation of treatment with secukinumab and telmisartan. After treatment, proteinuria, kidney function, and hematuria all improved, and remission of psoriasis was maintained.
Discussion
We describe the case of a 60-year-old man with remission of secondary IgA nephropathy during the course of psoriasis treatment with secukinumab, a human monoclonal anti-IL-17A antibody, as well as tonsillectomy followed by steroid pulse therapy. IgA nephropathy is a common comorbidity of psoriasis [2] and it usually correlates with the disease activity of psoriasis [8, 9]. Because Gd-IgA1 was not detected, this case was supposed to be a secondary IgA nephropathy [7]. Our patient’s case followed a typical course, starting with secondary failure of adalimumab. Psoriasis and secondary IgA nephropathy worsened by changing the dosing interval of secukinumab. We suggest that secukinumab plays an important role in secondary IgA nephropathy accompanied by psoriasis.
The patient was treated with secukinumab, an IL-17A-specific monoclonal antibody, for psoriasis. IL-17A is a key mediator of inflammation in psoriasis and IgA nephropathy. In animal models of crescentic glomerulonephritis, IL-17A-producing γδ T-cells play an important role in inflammatory response in the kidney [10]. γδ T-cells are major producers of IL-17 in inflammatory diseases [11], including psoriasis [12], and are associated with progressive IgA nephropathy [13]. We did not confirm infiltration of γδ T-cells or γδ T-cell-produced IL-17A in the biopsy specimen, but secukinumab might play a beneficial effect in the remission of proteinuria.
The patient’s nephropathy was more aggravated than his psoriasis. One possible cause was a rapid, worsening weight increase in the last 4 months of his treatment coupled with existing hypertension, which could have exaggerated his kidney disease. The weight gained mainly because he changed his job to a commercial driver with a nighttime shift and the irregular lifestyle might be the cause of metabolic syndrome. He was not treated with oral steroids and did not show the clinical symptoms of endocrine diseases including Cushing’s syndrome. It is known that excessive body weight is a risk factor for IgA nephropathy [14]. Therefore, we speculate that obesity has some additional effect on the development of proteinuria during treatment of nephropathy. The other possible cause was secukinumab. However, his nephropathy was improved under the treatment with secukinumab. Thus, we considered that secukinumab had little harmful effect on his nephropathy.
In summary, we present the case of a patient with psoriasis and remission of secondary IgA nephropathy undergoing treatment with secukinumab. Considering the patient’s clinical course, it seems plausible that IL-17 modulates the progression of secondary IgA nephropathy. Further clinical and basic research is required for establishing causal relationships between psoriasis and kidney lesions during treatment with biologics.
Compliance with ethical standards
Conflict of interest
All the authors have declared no conflict of interest.
Ethical approval
This article does not contain any studies with human participants performed by any of the authors.
Informed consent
Informed consent was obtained from the participant included in this article.
Footnotes
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
References
- 1.Nestle FO, Kaplan DH, Barker J. Psoriasis. N Engl J Med. 2009;361(5):496–509. doi: 10.1056/NEJMra0804595. [DOI] [PubMed] [Google Scholar]
- 2.Wan J, Wang S, Haynes K, Denburg MR, Shin DB, Gelfand JM. Risk of moderate to advanced kidney disease in patients with psoriasis: population based cohort study. BMJ. 2013;347:f5961. doi: 10.1136/bmj.f5961. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Chiu HY, Huang HL, Li CH, Yin YJ, Chen HA, Hsu ST, et al. Increased risk of glomerulonephritis and chronic kidney disease in relation to the severity of psoriasis, concomitant medication, and comorbidity: a nationwide population-based cohort study. Br J Dermatol. 2015;173(1):146–154. doi: 10.1111/bjd.13599. [DOI] [PubMed] [Google Scholar]
- 4.Pouria S, Barratt J. Secondary IgA nephropathy. Semin Nephrol. 2008;28(1):27–37. doi: 10.1016/j.semnephrol.2007.10.004. [DOI] [PubMed] [Google Scholar]
- 5.Bagel J, Duffin KC, Moore A, Ferris LK, Siu K, Steadman J, et al. The effect of secukinumab on moderate-to-severe scalp psoriasis: results of a 24-week, randomized, double-blind, placebo-controlled phase 3b study. J Am Acad Dermatol. 2017;77:667–674. doi: 10.1016/j.jaad.2017.05.033. [DOI] [PubMed] [Google Scholar]
- 6.Armstrong AW, Villanueva Quintero DG, Echeverria CM, Gu Y, Karunaratne M, Reyes Servin O. Body region involvement and quality of life in psoriasis: analysis of a randomized controlled trial of adalimumab. Am J Clin Dermatol. 2016;17(6):691–699. doi: 10.1007/s40257-016-0229-x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Suzuki H, Yasutake J, Makita Y, Tanbo Y, Yamasaki K, Sofue T, et al. IgA nephropathy and IgA vasculitis with nephritis have a shared feature involving galactose-deficient IgA1-oriented pathogenesis. Kidney Int. 2018;93(3):700–705. doi: 10.1016/j.kint.2017.10.019. [DOI] [PubMed] [Google Scholar]
- 8.Ahuja TS, Funtanilla M, de Groot JJ, Velasco A, Badalamenti J, Wilson S. IgA nephropathy in psoriasis. Am J Nephrol. 1998;18(5):425–429. doi: 10.1159/000013388. [DOI] [PubMed] [Google Scholar]
- 9.Zadrazil J, Tichý T, Horák P, Nikorjaková I, Zíma P, Krejcí K, et al. IgA nephropathy associated with psoriasis vulgaris: a contribution to the entity of’psoriatic nephropathy’. J Nephrol. 2006;19(3):382–386. [PubMed] [Google Scholar]
- 10.Turner JE, Krebs C, Tittel AP, Paust HJ, Meyer-Schwesinger C, Bennstein SB, et al. IL-17A production by renal gammadelta T cells promotes kidney injury in crescentic GN. J Am Soc Nephrol JASN. 2012;23(9):1486–1495. doi: 10.1681/ASN.2012010040. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Papotto PH, Ribot JC, Silva-Santos B. IL-17 + gammadelta T cells as kick-starters of inflammation. Nat Immunol. 2017;18(6):604–611. doi: 10.1038/ni.3726. [DOI] [PubMed] [Google Scholar]
- 12.Cai Y, Shen X, Ding C, Qi C, Li K, Li X, et al. Pivotal role of dermal IL-17-producing gammadelta T cells in skin inflammation. Immunity. 2011;35(4):596–610. doi: 10.1016/j.immuni.2011.08.001. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Falk MC, Ng G, Zhang GY, Fanning GC, Roy LP, Bannister KM, et al. Infiltration of the kidney by alpha beta and gamma delta T cells: effect on progression in IgA nephropathy. Kidney Int. 1995;47(1):177–185. doi: 10.1038/ki.1995.21. [DOI] [PubMed] [Google Scholar]
- 14.Bonnet F, Deprele C, Sassolas A, Moulin P, Berthezène F, Berthoux F. Excessive body weight as a new independent risk factor for clinical and pathological progression in primary IgA nephritis. Am J Kidney Dis. 2001;37(4):720–727. doi: 10.1016/S0272-6386(01)80120-7. [DOI] [PubMed] [Google Scholar]