Abstract
Background
This study aims to assess the association between body mass index (BMI) and health-related quality of life (HRQOL), and to further explore gender differences in BMI-HRQOL association among adults.
Methods
We used data from the fifth Health Service Survey of Shandong Province, which was part of China’s National Health Service Survey (NHSS), a total of 27,257 adults aged 18 and over were interviewed. The HRQOL was measured using the EuroQOL-5 Dimensions (EQ-5D) instrument. One-way ANOVA and Post hoc tests were used to compare EQ-5D utility values and visual analogue scale (VAS) scores between BMI categories. Tobit regression models were used to identify the association between BMI and HRQOL for male and female separately after controlling for influential confounders, and to assess gender differences on the relationship between BMI and HRQOL.
Results
The prevalence of underweight in men and women were 3.2 and 5.3%, respectively, while the prevalence of overweight/obesity in men and women were 35.7 and 34.6%, respectively. Men had higher EQ-5D utility values and VAS scores than women. The mean EQ-5D utility value and VAS score was highest in obese men and normal-weight women, respectively. After controlling potential confounders, being underweight was significantly and negatively associated with lower HRQOL among adults. The relationship between obesity and gender was that in women obesity was negatively and significantly associated with HRQOL, whereas in men this association was positive but not statistically significant. Results of gender by BMI interaction in regression model showed that this difference between men and women in this respect was significant.
Conclusions
The association between BMI and HRQOL differed by gender and the so-called “obesity-HRQOL paradox” phenomenon was verified in male adults. Gender difference should be considered when implementing targeted weight control programs and appropriate interventions to improve HRQOL.
Keywords: Body mass index, Health-related quality of life, Gender, Underweight, Obesity
Background
A recent pooled analysis of 1698 population-based study with 19.2 million participants from 200 countries estimated that global age-standardized mean body mass index (BMI) was in an increasing trend for both men and women from 1975 to 2014, which will become a serious public health concern if post-2000 trends continue [1]. Some previous research showed that high BMI (overweight or obese) was an important risk factor for a variety of chronic diseases [2–5], and that may result heavy health and economic burden, such as increased mortality and morbidity and higher annual medical care cost [6–9]. In China, the prevalence of high BMI (overweight and obesity) has been increasing and is fast approaching epidemic proportions [10]. The Report on Nutrition and Chronic Diseases of Chinese Residents (2015) revealed that the prevalence of overweight and obesity among adults aged 18 years were 30.1 and 11.9%, increased by 7.3 and 4.8 percentage compared with that in 2002 separately. Whether for young people or adults, the growth rate of high BMI in China was higher than that in the most developed countries [11]. Simultaneously, much lower BMI (underweight) remained prevalent and was also a serious problem in China [12]. There was evidence that much lower BMI (underweight) was associated with physical, functional, and psychological impairment and increased risk of chronic disease and mortality [13, 14]. Therefore, both much higher and lower BMI are likely to impair the overall health of population.
Health-related quality of life (HRQOL) has been recognized as a valid health indicator with the realization that biomedically oriented measures of a population’s well-being, such as mortality and morbidity rates, to provide a partial picture of public health needs and prevention outcomes [15, 16]. Some studies have examined the association between BMI and HRQOL in general population or specific population [17–19].
However, the impact of BMI on HRQOL may vary by gender. Some studies have showed that much higher or lower BMI was negatively associated with HRQOL in both men and women, including decreasing physical or emotional well-being or both [18, 19], while some study indicated that at higher BMI values, men reported higher HRQOL than women; at lower BMI values, HRQOL was lower in men than women [20], and another study reported that the association between obesity and lower HRQOL remained significant for women, but not for men [21]. In the current sociocultural context, people still value physical attractiveness and thinness, particularly in women, which may contribute in higher risk of experiencing low self-esteem, negative body image, and depression for women than men. By contrast, some people regard obesity a protective factor, especially for men or patients with chronic diseases. As a few studies have reported, high BMI (overweight or obesity) was associated with slightly better HRQOL as compared to those with normal weight [22–24]. Excess weight is paradoxically associated with a decreased risk of adverse outcomes, and the ‘obesity paradox’ has been proposed as a label for above unexpected results [25, 26]. Another study conducted by Yanbo Zhu [27] showed that those with the class I obese (25–29.9 kg/m2) had better HRQOL in both the physical and the mental domains than those with normal weight, especially in the mental well-being, which extended the “obesity paradox” to HRQOL outcomes. Therefore, there is no consistent recognition of the association between high or low BMI and HRQOL.
Most studies assessing the association between BMI and HRQOL among Chinese adults focused on obesity group or weight in age-specific groups [28–30], or did not further explore the gender difference explicitly for the above association [12]. A better understanding of the mechanisms will help in the design of more targeted and appropriate interventions. However, the differences on BMI- HRQOL association between men and women are still inconclusive, and no similar in-depth investigations were conducted among adults from Shandong Province, where the total population ranks second in China. To fill the gap literature, the aims of our study are 1) to evaluate the association between BMI and HRQOL among adults sampled from Shandong Province, China, and 2) to further explore gender differences on association between BMI category and HRQOL among adults.
Methods
Data and sample
We used data from the fifth Health Service Survey of Shandong Province, which was part of China’s National Health Service Survey (NHSS), conducted in 2013. The NHSS is a national survey commissioned by the Nation Health and Family Planning Commission of China every 5 years since 1993, which used multistage stratified cluster sampling to select 94 of 2,859 counties from China’s 31 provinces and municipalities. The Shandong’s NHSS in 2013 covered total 17 prefectures across the province, and 20 counties, 100 towns were randomly selected through a multistage stratified cluster sampling method. In the first stage, 20 counties were selected from total 137 counties as the primary sampling units (PSUs) throughout the province. In every PSU, 10 villages were selected as the secondary sampling units (SSUs). In the last stage, 60 households were randomly selected from every SSU. Finally, a total of 12,010 households, consisting of 33,070 individuals, were included in the sample. After verbal informed consent was obtained from interviewees, a face-to-face interview was conducted individually for all members in every selected household using a structured household questionnaire. The sample population was, therefore, an excellent source of health and sociodemographic variables within the population of Shandong.
Given our focus on adult sample, we restricted our analysis to respondents aged 18 years or older, and 27,257 adult respondents were included in this study after excluding respondents whose BMI or HRQOL data were missing.
Variables
Body mass index
Body mass index (BMI) was collected by physical measurement and was calculated as weight (kg) divided by the square of height (m2). BMI was classified based on WHO guidelines as follows: underweight was a BMI<18.50; normal weight was 18.5 ≤ BMI<25.0; overweight was 25.0 ≤ BMI<30.0; obese was BMI ≥ 30.0 [31]. Category “very obese” was combined into “obese” since only 105/27,257 (0.39%) population with BMI ≥ 35.0 kg/m2 in our study. Although BMI itself has been questioned as the optimal measurement to use for assessing obesity, other measures such as waist circumference, waist: hip ratio, and waist: height ratio, may be better. However, BMI remains the most commonly used, widely accepted, and practical measure of obesity in both children and adults, particularly for surveillance [32].
Heath-related quality of life
The Chinese version EQ-5D-3 L, was preselected as a measure in Shandong’s NHSS 2013. The EQ-5D-3 L was a generic, preference-based instrument comprising a health classification system with five dimensions (mobility, self-care, usual activities, pain/discomfort and anxiety/depression), each dimension with three response levels (no problem, some problems, extreme problems) and a visual analogue scale (VAS), which recorded the respondent’s perception of overall health status on a scale from 0 (indicating the worst imaginable health) to 100 (indicating the best imaginable health). The health classification system described a total of 243 health states, each of which was assigned a utility weight, range − 0.149 to 1, using a utility scoring function derived from Chinese general population using the time trade-off method [33]. Higher utility values represent higher HRQOL.
Other variables
Data on demographic characteristics, health behaviors and self-reported diseases/conditions were included in this study as follows: gender (Male, Female), age (continuous), area (Urban, Rural), education attainment (Primary school or below: illiteracy or primary school, Junior school, Senior school or above: senior school or technical school or secondary school or associate’ degree or bachelor’s degree and above), smoking status (Yes: daily smoker or casual smoker, No: nonsmoker) and drinking status (Have you had any alcohol in the past 12 months? Response: Yes/No), exercise times weekly (< 1: never or less than once, 1–5: 1–2 times or 3–5 times, > 6: 6 times and above), health examination (Have you had a physical examination in the past 12 months that does not include a medical examination? Response: Yes/No), number of chronic diseases (Have you been diagnosed with hypertension/diabetes/chronic obstructive pulmonary disease/cancer/periodontitis/other chronic diseases? Response for each item: Yes/No; The total number of answers to “yes” was divided into four categories: 0, 1, 2, > 3), family members with cancers (Are there cancer patients in your family? Response: Yes/No).
Statistical analysis
Data were described using either means (standard deviations) or numbers (proportion), where appropriate. Gender differences in sociodemographic characteristics were analyzed using a t-test (for continuous variables) or Chi-square test (for categorical variables) as appropriate. One-way ANOVA and Post hoc tests were used to compare EQ-5D utility values and VAS scores between BMI category. Our dependent variable (EQ-5D utility value) was censored (− 0.149, 1) and our data were skewed, and many respondents were at the upper limit. Tobit regression model was employed in our study based on the above reasons, which was appropriate to evaluate factors related to HRQOL measured by the EQ-5D utility value as discussed in many studies [34–36]. Thus, Tobit regression models were undertaken for men and women separately to assess the association between BMI category and HRQOL after controlling for influential sociodemographic and health-related factors, with EQ-5D utility values as the dependent variable. Then, gender differences on the association between BMI category and HRQOL were examined by adding the gender by BMI interaction term into the regression model. All data were analyzed using SPSS 24.0 and STATA 14.0. P-values<0.05 were considered to be statistically significant.
Results
Respondents’ characteristics
Descriptive statistics for the sample are shown in Table 1. In a total of 27,257 adults, men and women accounted for 47.8 and 52.2% separately. Men had a slightly lower mean age and significantly higher mean BMI (P<0.001) and comprised a higher proportion of the population who were highly educated (P<0.001), smoker (P<0.001), drinker (P<0.001) than women. The proportion of men with one or more chronic diseases was 30.9%, slightly lower than that of women (P<0.01). The mean (SD) BMI of respondents were 24.02 ± 3.40 and 23.68 ± 3.51 for men and women, respectively. The prevalence of underweight in men and women were 3.2 and 5.3%, respectively, while the prevalence of overweight/obesity in men and women were 35.7 and 34.6%, respectively. The mean (SD) EQ-5D utility values and VAS scores in men were 0.95 ± 0.14 and 83.24 ± 15.03 respectively, both of which were higher than that in women (P<0.001).
Table 1.
Sociodemographic and health-related conditions by gender
| Variable | Total | Men | Women | P-value |
|---|---|---|---|---|
| 27257 | 13032 (47.8) | 14225 (52.2) | ||
| Age, mean ± SD | 50.03 ± 16.04 | 49.83 ± 15.85 | 50.21 ± 16.2 | 0.036a |
| Area [n (%)] | <0.001b | |||
| Urban | 18371 (67.4) | 8646 (66.3) | 9725 (68.4) | |
| Rural | 8886 (32.6) | 4386 (33.7) | 4500 (31.6) | |
| Education attainment [n (%)] | <0.001b | |||
| Primary school or below | 9740 (35.7) | 3404 (26.1) | 6336 (44.5) | |
| Junior school | 9906 (36.3) | 5357 (41.1) | 4549 (32.0) | |
| Senior school or above | 7611 (27.9) | 4271 (32.8) | 3340 (23.5) | |
| Smoking status [n (%)] | <0.001b | |||
| Yes | 6216 (22.8) | 5976 (45.9) | 240 (1.7) | |
| No | 21041 (77.2) | 7056 (54.1) | 13985 (98.3) | |
| Drinking status [n (%)] | <0.001b | |||
| Yes | 7623 (28.0) | 7136 (54.8) | 487 (3.4) | |
| No | 19634 (72.0) | 5896 (45.2) | 13738 (96.6) | |
| Exercise times weekly [n (%)] | 0.227b | |||
| ≥6 | 3501 (12.8) | 1722 (13.2) | 1779 (12.5) | |
| 1–5 | 4050 (14.9) | 1919 (14.7) | 2131 (15.0) | |
| <1 | 19706 (72.3) | 9391 (72.1) | 10315 (72.5) | |
| Health examination [n (%)] | <0.001b | |||
| Yes | 12581 (46.2) | 5727 (43.9) | 6854 (48.2) | |
| No | 14676 (53.8) | 7305 (56.1) | 7371 (51.8) | |
| Number of chronic diseases [n (%)] | 0.001b | |||
| 0 | 18546 (68.0) | 9005 (69.1) | 9541 (67.1) | |
| 1 | 5838 (21.4) | 2739 (21.0) | 3099 (21.8) | |
| 2 | 2214 (8.1) | 988 (7.6) | 1226 (8.6) | |
| ≥3 | 659 (2.4) | 300 (2.3) | 359 (2.5) | |
| Family members with cancers | 0.640b | |||
| Yes | 243 (0.9) | 123 (0.9) | 120 (0.8) | |
| No | 27014 (99.1) | 12859 (98.7) | 14054 (98.8) | |
| BMI categories [n (%)] | <0.001b | |||
| Underweight | 1173 (4.3) | 417 (3.2) | 756 (5.3) | |
| Normal weight | 16516 (60.6) | 7960 (61.1) | 8556 (60.1) | |
| Overweight | 8376 (30.7) | 4068 (31.2) | 4308 (30.3) | |
| Obese | 1192 (4.4) | 587 (4.5) | 605 (4.3) | |
| BMI, mean ± SD | 23.84 ± 3.46 | 24.01 ± 3.40 | 23.68 ± 3.51 | <0.001a |
| EQ-5D, mean ± SD | 0.95 ± 0.14 | 0.95 ± 0.14 | 0.94 ± 0.14 | <0.001a |
| VAS, mean ± SD | 82.56 ± 15.29 | 83.24 ± 15.03 | 81.94 ± 15.50 | <0.001a |
SD standard deviation, BMI body mass index, EQ-5D EuroQOL-5 Dimensions, VAS visual analogue scale, a t-test, b Chi-square test
Comparison of HRQOL between BMI category
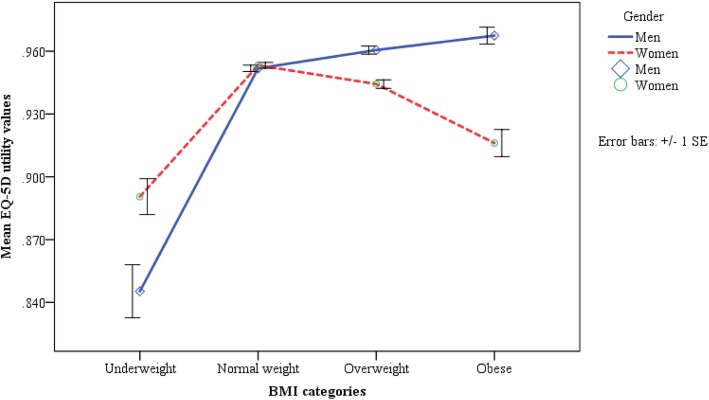
Table 2 shows the results of comparing EQ-5D utility values and VAS scores between BMI category in men and women separately. There were gender differences in both mean EQ-5D utility values and VAS scores between four BMI categories. For men, post hoc test results showed that underweight group had lower HRQOL (P<0.001), while overweight (P<0.01) and obese groups (P<0.001) had significant higher HRQOL, compared with the normal weight group. For women, however, some different pattern was revealed. Women with both underweight (P<0.001) and overweight (P<0.01) or obesity (P<0.01) were likely to report lower HRQOL than those with normal weight. The mean EQ-5D utility value was highest in obese men and normal-weight women (See also in Fig. 1). Similar results were also found for men and women regarding VAS scores.
Table 2.
Comparisons of EQ-5D utility values and VAS scores between BMI category
| Underweight | Normal weight | Overweight | Obese | P-value a | |
|---|---|---|---|---|---|
| Men | |||||
| EQ-5D utility values, mean ± SD | 0.85 ± 0.26 | 0.95 ± 0.14 | 0.96 ± 0.12 | 0.97 ± 0.10 | <0.001 |
| VAS scores, mean ± SD | 73.85 ± 21.06 | 83.33 ± 14.92 | 83.94 ± 14.22 | 84.06 ± 14.21 | <0.001 |
| Women | |||||
| EQ-5D utility values, mean ± SD | 0.89 ± 0.24 | 0.95 ± 0.13 | 0.94 ± 0.13 | 0.92 ± 0.16 | <0.001 |
| VAS scores, mean ± SD | 78.35 ± 19.41 | 83.01 ± 15.12 | 80.85 ± 15.20 | 79.29 ± 15.44 | <0.001 |
SD standard deviation, a One-way ANOVA test for differences of BMI category
Fig. 1.
Mean EQ-5D utility values between BMI category by gender
Association between BMI and HRQOL and its gender differences
Table 3 summarizes Tobit regression models of HRQOL measured by EQ-5D. First, we presented separate regression models for both men and women (Table 3, Model I and Model II). Compared with the normal weight group, the underweight group reported significantly lower HRQOL in both men (β = − 0.148, P<0.001) and women (β = − 0.099, P<0.001). However, for overweight and obese group, a slightly different pattern was shown between men and women. Obesity had a significant negative effect on HRQOL in women (β = − 0.068, P<0.01, Model II), but not in men (Model I). More importantly, the difference between men and women in this respect was significant (β = 0.103, P<0.01, Model III).
Table 3.
Tobit regression models for association between BMI category and HRQOL and its gender difference
| Variable | Model I Men | Model II Women | Model III Interaction: Gender × BMI |
|||
|---|---|---|---|---|---|---|
| Coefficient | 95%CI | Coefficient | 95%CI | Coefficient | 95%CI | |
| Age | −.011*** | (−.012, −.010) | −.012*** | (−.013, −.011) | −.011*** | (−.012, −.011) |
| Urban (vs rural) | .055*** | (.026, .083) | .045*** | (.023, .071) | .048*** | (.030, .066) |
| Education attainment (vs Primary school or below) | ||||||
| Junior school | .102*** | (.074, .130) | .055*** | (.031, .079) | .077*** | (.059, .095) |
| Senior school or above | .115*** | (.081, .150) | .071*** | (.039, .104) | .091*** | (.068, .114) |
| Smokers | .026* | (.002, .049) | .014 | (−.044, .073) | .025* | (.004, .045) |
| Drinkers | .096*** | (.072, .119) | −.026 | (−.072, .020) | .072*** | (.052, .092) |
| Exercise times weekly (vs ≥ 6) | ||||||
| 1–5 | −.092*** | (−.136, −.048) | −.098*** | (−.133, −.062) | −.095*** | (−.123, −.068) |
| <1 | −.140*** | (−.177, −.103) | −.147*** | (−.177, −.117) | −.143*** | (−.166, −.120) |
| Health examination | −.063*** | (−.087, −.039) | −.064*** | (−.082, −.046) | −.064*** | (−.079, −.049) |
| Number of chronic diseases (vs 0) | ||||||
| 1 | −.186*** | (−.213, −.159) | −.177*** | (−.199, −.156) | −.181*** | (−.198, −.164) |
| 2 | −.299*** | (−.336, −.262) | −.271*** | (−.299, −.243) | −.283*** | (−.306, −.261) |
| ≥ 3 | −.385*** | (−.442, −.327) | −.347*** | (−.392, −.303) | −.365*** | (−.400, −.329) |
| Family members with cancers | −.175*** | (−.261, −.089) | −.208*** | (−.283, −.132) | −.193*** | (−.249, −.136) |
| BMI categories (vs Normal weight) | ||||||
| Underweight | −.148*** | (−.200, −.095) | −.099*** | (−.137, −.061) | −.106*** | (−.147, −.066) |
| Overweight | .023 | (−.002, .049) | −.002 | (−.021, .018) | −.004 | (−.024, .017) |
| Obese | .032 | (−.026, .090) | −.068** | (−.107, −.028) | −.074** | (−.116, −.032) |
| Men (vs Women) | −.047*** | (−.069, −.025) | ||||
| Gender × BMI | ||||||
| Men × underweight | −.034 | (−.097, .028) | ||||
| Men × overweight | .026 | (−.006, .057) | ||||
| Men × obese | .103** | (.035, .171) | ||||
| Constant | 2.083*** | (1.998, 2.168) | 2.163*** | (2.097, 2.229) | 2.156*** | (2.103, 2.208) |
| Respondents | 13032 | 14225 | 27257 | |||
| R 2 | .237 | .285 | .262 | |||
CI confidence interval,* P<0.05, **P<0.01, ***P<0.001, Gender×BMI = interaction effect between gender and BMI category
Discussion
Gender differences on association between BMI and HRQOL was investigated explicitly in our study. Overall, overweight and obese adults accounted for 30.7 and 4.4%, respectively, and there was a higher proportion of overweight/obese men than women. The highest mean EQ-5D utility value and VAS score was achieved by men of obese group and by women of normal weight group, respectively. After controlling potential confounders, gender had a significant effect in the association between BMI categories and HRQOL, especially for obese group.
A lot of attention was paid to dealing with obesity-HRQOL, and the relationship between underweight and HRQOL was likely to be ignored. Nevertheless, an obvious fact in our study was that being underweight was associated with the worst HRQOL and our findings were broadly consistent with those reported in many studies [12, 17, 23, 27, 37]. Previous studies have reported that underweight was associated with increased risk of excess mortality [38], poor cognition [39, 40], and poor self-rated health [41]. A previous study based on population in five cities of China also showed that there was more percentage of underweight persons (8.64%) than obesity (3.27%) in China [29]. In view of this, the neglected underweight problems need as much attention as obesity.
Generally, overweight and obesity were negatively associated with HRQOL, a surprising but interesting finding in our study was that obesity had a negative impact on women’ HRQOL after adjusting for other influential factors including chronic diseases, but not for men. A possible explanation about gender differences in obesity was that women might be more susceptible to distress to body weight or body image than men [42, 43]. Excessive dieting may result in lower HRQOL among obese women. It could also be explained by cultural perceptions about personal body weight and more discrimination against women with excess body weight in their work-related life and social roles [44]. Considering this, we performed another Tobit regression analysis to estimate the effects of the interactions of gender by BMI on HRQOL. As the results showed, women suffered from the negative effects of obesity on HRQOL even after adjusting for demographic, life style and chronic condition variables. All of those imply that we need to pay more attention on the overweight and obese females when improving HRQOL. Awareness to challenges facing those women can help health care providers work more effectively with them to develop different plans for losing weight, adopting healthier lifestyles.
The relationship between BMI and HRQOL in our study varied by gender, especially for population with obesity. Many studies have shown that the “obesity paradox”, a “paradoxical” decrease in morbidity and mortality with increasing BMI, existed in elderly or patients with chronic conditions [24, 45–47]. Recent studies extended the “obesity paradox” to HRQOL outcomes, suggesting that overweight and obesity may paradoxically correlate with higher HRQOL, called “obesity-HRQOL paradox” [22, 27, 48]. There has been some emerging evidence that the association between obesity and HRQOL may be stronger in women than men [29, 49, 50]. According to the available data, our finding is first to verify that this “obesity-HRQOL paradox” phenomenon appeared in Chinese male adults. Cultural and social atmosphere could well explain why obese men was positively associated with HRQOL. In Chinese traditional culture, being fat was not a symbol of unhealthiness because only the wealthier people can afford eating more and can put on more weight. A more recent Chinese saying described becoming fat during middle age as acquiring a good fortune [51]. Also, it may be a matter of special concept in China that some people regarded fat as “robust”, “affluent” state, especially for men [52]. Our results were also consistent with the results reported by Audureau et al. [53] that the significant “obesity-HRQOL paradox” were found in men for mentally oriented HRQOL domains. The increased amounts of nonfat and muscle mass, which are important contributors to fitness or overall health, might be another important concept in understanding this obesity paradox [54]. However, there is wide agreement that BMI is seriously flawed because it is unable to distinguish between lean body mass and fat mass, and BMI may underestimate the number of people for whom fatness impacts health [55]. Therefore, further studies based on other measures should be carried out to was needed to explain the phenomenon, but in this study, we confirmed that gender as a moderator had a significant effect on the relationship between BMI on HRQOL among adults. Accordingly, more targeted and appropriate interventions should be conducted, especially in women, to decrease the detrimental obesity effects associated with HRQOL. Furthermore, given that HRQOL was used as input for cost-effectiveness analyses, findings from our study are important for identifying population subgroups in which weight management programs are potentially most cost-effective.
The limitations of this study should be acknowledged. Firstly, this was a cross-sectional study which may result that the causality between BMI and HRQOL cannot be inferred despite the clear association. Secondly, our analyses were not weighted by the appropriate sampling weights. However, a series of quality and consistency tests including Myer’s Index (Myer’s index =2.99), Test of Goodness for Fit(χ2 = 12.59, P>0.05), DELTA No-similarity Coefficient (Δ = 0.0915) and GINI Concentration Ratio (GINI = 0.1079) showed that our survey data had high quality and the sample had a strong population representativeness of Shandong Province. Thirdly, we did not conduct more different subgroup analyses in this study, and will have a more explicit analysis in the follow-up study. In addition, the NHSS only collected the BMI data as a measure of obesity, we could not compare BMI with other measures, such as waist-to-hip ratio and visceral measurement, to explore more accurately and comprehensively gender difference in the association. However, there are also several strengths in this study. Firstly, the data we used were sampled from the general population of the Shandong’ NHSS 2013, which gave this analysis excellent power. More importantly, we confirmed that the gender differences on relationship of BMI and HRQOL by adding the interaction term of gender by BMI into regression model. Finally, our present study verified the “obesity paradox” to HRQOL outcomes in the male adults.
Conclusion
In this population-based study, we found that the underweight group had the lowest HRQOL, which deserved more attention. The effect of obesity on HRQOL in adults differed by gender, and it is critical to develop effective gender-specific weight control programs. The counter-intuitive “obesity- HRQOL” phenomenon was verified in male adults. Further research based on other measures are needed to investigate the mechanisms that underpin the gendered nature of obesity prevalence.
Acknowledgements
We would like to thank the officials of local health agencies and all participants and staff at the study sites for their cooperate. We also thank the support of Shandong University Center for Health Economics Experiment and Public Policy Research.
Abbreviations
- BMI
Body Mass Index
- CI
Confidence Interval.
- EQ-5D
EuroQOL-5 Dimensions
- HRQOL
Health-related Quality of Life;
- NHSS
National Health Service Survey
- PSU
Primary Sampling Unit
- SD
Standard Deviation
- SSU
Secondary Sampling Unit
- VAS
Visual Analogue Scale
- WHO
World Health Organization
Authors’ contributions
ZhaJ designed the study, performed the analysis, interpreted the data, drafted the initial manuscript, reviewed and revised the manuscript; LZ contributed to the study design, analyzed the data and approved the final manuscript as submitted; JJ, LS and CC supervised the data analysis and interpretation, critically reviewed and revised the manuscript for important intellectual content; WZ, DG and WQ interpreted the results, reviewed and revised the manuscript for important intellectual content. ZhuJ, ZH and XS revised the grammar and language. All authors read and approved the final manuscript.
Funding
This study was funded by two grants of National Natural Science Foundation of China (grant numbers: 71673169 and 71673170). The funding body had no role in design of study, data collection and analysis, interpretation of data or writing of manuscript.
Availability of data and materials
The datasets used in the current study are not publicly available due to the confidential policy but are available from the corresponding author on reasonable request.
Ethics approval and consent to participate
The survey was approved and organized by Health Commission of Shandong Province. This study was reviewed and approved by the Institutional Review Board (Academic Research Ethics Committee) of Shandong University School of Public Health. All procedures were in accordance with the ethical standards of the Helsinki Declaration. Participants provided informed consent prior to data collection.
Consent for publication
Not applicable.
Competing interests
The authors declare that they have no competing interests.
Footnotes
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Contributor Information
Jiao Zhang, Email: 1874658919@qq.com.
Lingzhong Xu, Phone: +86-0531-88382648, Email: lzxu@sdu.edu.cn.
Jiajia Li, Email: lijiajia@sdu.edu.cn.
Long Sun, Email: sunlong@sdu.edu.cn.
Wenzhe Qin, Email: qinwenzhe09@163.com.
Gan Ding, Email: dinggan90@163.com.
Qian Wang, Email: 1835372504@qq.com.
Jing Zhu, Email: 1176559133@qq.com.
Zihang Yu, Email: yuzihang2010gd@163.com.
Su Xie, Email: xs340823@163.com.
Chengchao Zhou, Email: zhouchengchao@sdu.edu.cn.
References
- 1.Di CM, Bentham J, Stevens GA, Zhou B, Danaei G, Lu Y, Bixby H, Cowan MJ, Riley LM, Hajifathalian K. Trends in adult body-mass index in 200 countries from 1975 to 2014: a pooled analysis of 1698 population-based measurement studies with 19·2 million participants. Lancet. 2016;387(10026):1377. doi: 10.1016/S0140-6736(16)30054-X. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Zhou B, Wu Y, Yang J, Li Y, Zhang H, Zhao L. Overweight is an independent risk factor for cardiovascular disease in Chinese populations. Obes Rev. 2002;3(3):147. doi: 10.1046/j.1467-789x.2002.00068.x. [DOI] [PubMed] [Google Scholar]
- 3.Parr CL, Batty GD, Lam TH, Barzi F, Fang X, Ho SC, Jee SH, Ansary-Moghaddam A, Jamrozik K, Ueshima H. Body-mass index and cancer mortality in the Asia-Pacific cohort studies collaboration: pooled analyses of 424,519 participants. Lancet Oncol. 2010;11(8):741. doi: 10.1016/S1470-2045(10)70141-8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Cai L, He J, Song Y, Zhao K, Cui W. Association of obesity with socio-economic factors and obesity-related chronic diseases in rural Southwest China. Public Health. 2013;127(3):247. doi: 10.1016/j.puhe.2012.12.027. [DOI] [PubMed] [Google Scholar]
- 5.Cao X, Zhou J, Yuan H, Wu L, Chen Z. Chronic kidney disease among overweight and obesity with and without metabolic syndrome in an urban Chinese cohort. BMC Nephrol. 2015;16(1):1–9. doi: 10.1186/s12882-015-0083-8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Cawley J, Meyerhoefer C. The medical care costs of obesity: an instrumental variables approach. J Health Econ. 2012;31(1):219–230. doi: 10.1016/j.jhealeco.2011.10.003. [DOI] [PubMed] [Google Scholar]
- 7.Odlaug BL, Lust K, Wimmelmann CL, Chamberlain SR, Mortensen EL, Derbyshire K, Christenson G, Grant JE. Prevalence and correlates of being overweight or obese in college. Psychiatry Res. 2015;227(1):58. doi: 10.1016/j.psychres.2015.01.029. [DOI] [PubMed] [Google Scholar]
- 8.Flegal KM, Panagiotou OA, Graubard BI. Estimating population attributable fractions to quantify the health burden of obesity. Ann Epidemiol. 2015;25(3):201. doi: 10.1016/j.annepidem.2014.11.010. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Kang H, Shim J, Lee H, Park B, Linton JA, Lee Y. Trends in prevalence of overweight and obesity in Korean adults, 1998-2009: the Korean National Health and nutrition examination survey. J Epidemiol. 2014;24(2):109–116. doi: 10.2188/jea.JE20130017. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Ma GS, Li YP, Wu YF, Zhai FY, Cui ZH, Hu XQ, Luan DC, Hu YH, Yang XG. The prevalence of body overweight and obesity and its changes among Chinese people during 1992 to 2002. Zhonghua Yu Fang Yi Xue Za Zhi. 2005;39(5):311–315. [PubMed] [Google Scholar]
- 11.NHFPC . The Report on Nutrition and Chronic Diseases of Chinese Residents.|.*2018*2018. 2015. [Google Scholar]
- 12.Xu Y, Zhou Z, Li Y, Yang J, Guo X, Gao J, Yan J, Chen G. Exploring the nonlinear relationship between body mass index and health-related quality of life among adults: a cross-sectional study in Shaanxi Province, China. Health Qual Life Outcomes. 2015;13(1):1–9. doi: 10.1186/s12955-015-0347-9. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Sergi G, Perissinotto E, Pisent C, Buja A, Maggi S, Coin A, Grigoletto F, Enzi G. An adequate threshold for body mass index to detect underweight condition in elderly persons: the Italian longitudinal study on aging (ILSA) J Gerontol. 2005;60(7):866. doi: 10.1093/gerona/60.7.866. [DOI] [PubMed] [Google Scholar]
- 14.Katzmarzyk PT, Craig CL, Bouchard C. Original article underweight, overweight and obesity : relationships with mortality in the 13-year follow-up of the Canada fitness survey. J Clin Epidemiol. 2001;54(9):916–920. doi: 10.1016/s0895-4356(01)00356-0. [DOI] [PubMed] [Google Scholar]
- 15.Wright SP, Doughty RN. Measuring health-related quality of life. J Am Acad Dermatol. 1999;38(3):64–68. [Google Scholar]
- 16.Guyatt GH, Feeny DH, Patrick DL. Measuring health-related quality of life. J Am Acad Dermatol. 1993;38(5):64–68. [Google Scholar]
- 17.Wee HL, Cheung YB, Loke WC, Tan CB, Chow MH, Li SC, Fong KY, Feeny D, Machin D, Luo N. The Association of Body Mass Index with health-related quality of life: An exploratory study in a multiethnic Asian population. Value Health. 2008;11(s1):S105–S114. doi: 10.1111/j.1524-4733.2008.00374.x. [DOI] [PubMed] [Google Scholar]
- 18.Renzaho A, Wooden M, Houng B. Associations between body mass index and health-related quality of life among Australian adults. Qual Life Res. 2010;19(4):515–520. doi: 10.1007/s11136-010-9610-z. [DOI] [PubMed] [Google Scholar]
- 19.Korhonen PE, Kautiainen H. Body mass index and health-related quality of life in apparently healthy individuals. Qual Life Res. 2014;23(1):67–74. doi: 10.1007/s11136-013-0433-6. [DOI] [PubMed] [Google Scholar]
- 20.Søltoft F, Hammer M, Kragh N. The association of body mass index and health-related quality of life in the general population: data from the 2003 health survey of England. Qual Life Res. 2009;18(10):1293–1299. doi: 10.1007/s11136-009-9541-8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.Jina C, Seonhui J, Juneyoung L. Gender differences in health-related quality of life associated with abdominal obesity in a Korean population. BMJ Open. 2014;4(1):e3954. doi: 10.1136/bmjopen-2013-003954. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 22.Lópezgarcía E, Banegas JRB, Gutiérrezfisac JL, Pérezregadera AG, Gañán LD, Rodríguezartalejo F. Relation between body weight and health-related quality of life among the elderly in Spain. Int J Obes Relat Metab Disord. 2003;27(6):701. doi: 10.1038/sj.ijo.0802275. [DOI] [PubMed] [Google Scholar]
- 23.Hopman WM, Berger C, Joseph L, Barr SI, Gao Y, Prior JC, Poliquin S, Towheed T, Anastassiades T. The association between body mass index and health-related quality of life: data from CaMos, a stratified population study. Qual Life Res. 2007;16(10):1595–1603. doi: 10.1007/s11136-007-9273-6. [DOI] [PubMed] [Google Scholar]
- 24.Curtis JP, Selter JG, Wang Y, Rathore SS, Jovin IS, Jadbabaie F, Kosiborod M, Portnay EL, Sokol SI, Bader F. The obesity paradox: body mass index and outcomes in patients with heart failure. Arch Intern Med. 2005;165(1):55–61. doi: 10.1001/archinte.165.1.55. [DOI] [PubMed] [Google Scholar]
- 25.Uretsky S, Messerli FH, Bangalore S, Champion A, Cooper-DeHoff RM, Zhou Q, Pepine CJ. Obesity paradox in patients with hypertension and coronary artery disease. Am J Med. 2007;120(10):863–870. doi: 10.1016/j.amjmed.2007.05.011. [DOI] [PubMed] [Google Scholar]
- 26.Doehner W, Clark A, Anker SD. The obesity paradox: weighing the benefit. Eur Heart J. 2010;31(2):146–148. doi: 10.1093/eurheartj/ehp339. [DOI] [PubMed] [Google Scholar]
- 27.Zhu Y, Wang Q, Pang G, Lin L, Origasa H, Wang Y, Di J, Shi M, Fan C, Shi H. Association between body mass index and health-related quality of life: the "obesity paradox" in 21,218 adults of the Chinese general population. PLoS One. 2015;10(6):e130613. doi: 10.1371/journal.pone.0130613. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 28.Zhu YB, Luo XX, Wang Q. Study on the relationship between body mass index and health-related quality of life in middle-aged or older Chinese adults. Zhonghua Liu Xing Bing Xue Za Zhi. 2009;30(7):687. [PubMed] [Google Scholar]
- 29.Wang R, Wu MJ, Ma XQ, Zhao YF, Yan XY, Gao QB, He J. Body mass index and health-related quality of life in adults: a population based study in five cities of China. Eur J Pub Health. 2012;22(4):497. doi: 10.1093/eurpub/ckr080. [DOI] [PubMed] [Google Scholar]
- 30.Lu J, Zhu Y, Feng S, Shi H. Logistic regression analysis of the relationship between abdominal obesity and health-related quality of life in adults. Chin J Behav Med Brain Sci. 2016;25(5):446–451. [Google Scholar]
- 31.WHO . BMI classification. 2015. [Google Scholar]
- 32.Adab P, Pallan M, Whincup PH. Is BMI the best measure of obesity? BMJ. 2018;360:k1274. 10.1136/bmj.k1274. [DOI] [PubMed]
- 33.Liu GG, Wu H, Li M, Gao C, Luo N. Chinese time trade-off values for EQ-5D health states. Value Health. 2014;17(5):597. doi: 10.1016/j.jval.2014.05.007. [DOI] [PubMed] [Google Scholar]
- 34.Sullivan PW, Ghushchyan V. Mapping the EQ-5D index from the SF-12: US general population preferences in a nationally representative sample. Med Decis Mak. 2016;26(4):401–409. doi: 10.1177/0272989X06290496. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 35.Sullivan PW, Ghushchyan V. Preference-based EQ-5D index scores for chronic conditions in the United States. Med Decis Mak. 2016;26(4):410–420. doi: 10.1177/0272989X06290495. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 36.Hong JY, Kim SY, Chung KS, Kim EY, Jung JY, Park MS, Kang YA, Kim SK, Chang J, Kim YS. Factors associated with the quality of life of Korean COPD patients as measured by the EQ-5D. Qual Life Res. 2015;24(10):2549–2558. doi: 10.1007/s11136-015-0979-6. [DOI] [PubMed] [Google Scholar]
- 37.Avery AJ. The relationship between body mass index and health-related quality of life: comparing the EQ-5D, EuroQol VAS and SF-6D. Int J Obes (London) 2007;31(1):189–196. doi: 10.1038/sj.ijo.0803365. [DOI] [PubMed] [Google Scholar]
- 38.Hong S, Yi S, Sull JW, Hong J, Jee SH, Ohrr H. Body mass index and mortality among Korean elderly in rural communities: Kangwha cohort study. PLoS One. 2015;10(2):e117731. doi: 10.1371/journal.pone.0117731. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 39.Selvamani Y, Singh P. Socioeconomic patterns of underweight and its association with self-rated health, cognition and quality of life among older adults in India. PLoS One. 2018;13(3):e193979. doi: 10.1371/journal.pone.0193979. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 40.Xiang X, An R. Body weight status and onset of cognitive impairment among U.S. middle-aged and older adults. Arch Gerontol Geriatr. 2015;60(3):394–400. doi: 10.1016/j.archger.2015.02.008. [DOI] [PubMed] [Google Scholar]
- 41.Wu S, Wang R, Zhao Y, Ma X, Wu M, Yan X, He J. The relationship between self-rated health and objective health status: a population-based study. BMC Public Health. 2013;13(1):320. doi: 10.1186/1471-2458-13-320. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 42.Demarest J, Allen R. Body image: gender, ethnic, and age differences. J Soc Psychol. 2000;140(4):465. doi: 10.1080/00224540009600485. [DOI] [PubMed] [Google Scholar]
- 43.Joshi R, Herman CP, Polivy J. Self-enhancing effects of exposure to thin-body images. int J Eat Disord. 2004;35(3):333. doi: 10.1002/eat.10253. [DOI] [PubMed] [Google Scholar]
- 44.Paquette MC, Raine K. Sociocultural context of women's body image. Soc Sci Med. 2004;59(5):1047–1058. doi: 10.1016/j.socscimed.2003.12.016. [DOI] [PubMed] [Google Scholar]
- 45.Lavie CJ, Milani RV, Ventura HO, Romero-Corral A. Body composition and heart failure prevalence and prognosis: getting to the fat of the matter in the “obesity paradox”. Mayo Clin Proc. 2010;85(7):605–608. doi: 10.4065/mcp.2010.0333. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 46.Lavie CJ, De SA, Patel DA, Romerocorral A, Artham SM, Milani RV. Body composition and survival in stable coronary heart disease: impact of lean mass index and body fat in the "obesity paradox". J Am Coll Cardiol. 2012;60(15):1374–1380. doi: 10.1016/j.jacc.2012.05.037. [DOI] [PubMed] [Google Scholar]
- 47.Lavie CJ, Mcauley PA, Church TS, Milani RV, Blair SN. Obesity and cardiovascular diseases : implications regarding fitness, fatness, and severity in the obesity paradox. J Am Coll Cardiol. 2014;63(14):1345. doi: 10.1016/j.jacc.2014.01.022. [DOI] [PubMed] [Google Scholar]
- 48.Tsai WL, Yang CY, Lin SF, Fang FM. Impact of obesity on medical problems and quality of life in Taiwan. Am J Epidemiol. 2004;160(6):557. doi: 10.1093/aje/kwh251. [DOI] [PubMed] [Google Scholar]
- 49.Larsson U, Karlsson J, Sullivan M. Impact of overweight and obesity on health-related quality of life--a Swedish population study. Int J Obes Relat Metab Disord. 2002;26(3):417–424. doi: 10.1038/sj.ijo.0801919. [DOI] [PubMed] [Google Scholar]
- 50.Park S. Pathways linking obesity to health-related quality of life. Qual Life Res. 2017;26(8):2209–2218. doi: 10.1007/s11136-017-1565-x. [DOI] [PubMed] [Google Scholar]
- 51.Li ZB, Ho SY, Chan WM, Ho KS, Li MP, Leung GM, Lam TH. Obesity and depressive symptoms in Chinese elderly. Int J Geriatr Psychiatry. 2004;19(1):68. doi: 10.1002/gps.1040. [DOI] [PubMed] [Google Scholar]
- 52.French P, Crabbe M. Fat China: how expanding waistlines are changing a nation[M]. Anthem Press, 2010.
- 53.Audureau E, Pouchot J, Coste J. Gender-related differential effects of obesity on health-related quality of life via obesity-related comorbidities: a mediation analysis of a French Nationwide survey. Circ Cardiovasc Qual Outcomes. 2016;9(3):246–256. doi: 10.1161/CIRCOUTCOMES.115.002127. [DOI] [PubMed] [Google Scholar]
- 54.Lavie CJ, De Schutter A, Milani RV. Healthy obese versus unhealthy lean: the obesity paradox. Nat Rev Endocrinol. 2015;11(1):55–62. doi: 10.1038/nrendo.2014.165. [DOI] [PubMed] [Google Scholar]
- 55.Lin TY, Lim PS, Hung SC. Impact of misclassification of obesity by body mass index on mortality in patients with CKD. Kidney Int Rep. 2018;3(2):447–455. doi: 10.1016/j.ekir.2017.12.009. [DOI] [PMC free article] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Data Availability Statement
The datasets used in the current study are not publicly available due to the confidential policy but are available from the corresponding author on reasonable request.