Abstract
Background
Aneurysmal subarachnoid hemorrhage (SAH) is an acute cerebrovascular disease associated with high mortality and long-term functional impairment among survivors. Systemic inflammatory responses after acute injury and nosocomial infections are frequent complications, making the management of these patients challenging. Here, we hypothesized that sepsis might be associated with early and long-term mortality and functional outcomes. Our objective was to define the incidence of sepsis, diagnosed prospectively with the Sepsis-3 criteria, and to determine its impact on mortality and functional outcomes of patients with SAH.
Methods
We prospectively included all adult patients with aneurysmal SAH admitted to the intensive care unit (ICU) of a reference center between April 2016 and May 2018. Daily clinical and laboratory follow-up data were analyzed during the first 14 days, with data collected on sepsis according to the Sepsis-3 criteria. The main outcome was the functional outcome using the Modified Rankin Scale (mRS), which was assessed at hospital discharge and 3, 6 and 12 months post-discharge.
Results
In total, 149 patients were enrolled. The incidence of sepsis was 28%. Multivariable logistic regression analysis revealed that death or functional dependence (defined as an mRS score of 4 to 6) at hospital discharge was independently associated with sepsis (OR 3.4, 95% CI 1.16–9.96, p = 0.026) even after controlling for World Federation of Neurological Surgeons (WFNS) Scale (OR 4.66, 95% CI 1.69–12.88, p = 0.003), hydrocephalus (OR 4.55, 95% CI 1.61–12.85, p = 0.004) and DCI (OR 3.86, 95% CI 1.39–10.74, p = 0.01). Long-term follow-up mortality rates were significantly different in the septic and nonseptic groups (log-rank test p < 0.0001). The mortality rate of septic patients was 52.5%, and that of nonseptic patients was 16%.
Conclusion
Sepsis plays a significant role in the outcomes of patients with SAH, affecting both mortality and long-term functional outcomes. Combining high-level neurocritical care management of neurological complications and the optimal diagnosis and management of sepsis may effectively reduce secondary brain injury and improve patients’ outcomes after SAH.
Keywords: Subarachnoid hemorrhage, Sepsis, Infection, Critical care outcomes
Background
Aneurysmal subarachnoid hemorrhage (SAH) is an acute cerebrovascular disease with devastating consequences, including high mortality and long-term functional impairment among survivors [1]. Several brain-specific mechanisms of injuries secondary to SAH have been associated with worse functional outcomes, including early injuries, vasospasms and delayed cerebral ischemia (DCI), neuroinflammation or impaired cerebral autoregulation [2–6]. However, there are few options for treating or preventing such complications of SAH. On the other hand, systemic (and potentially preventable) complications such as nosocomial infections, sepsis and organ dysfunction may also alter the course of the disease and worsen survival as well as functional capacity [7]. The incidence of systemic inflammatory response syndrome (SIRS) after SAH may be up to 83% of patients, and the incidence of sepsis varies between 10 and 20%, with a strong association with poor outcomes [8, 9].
Approximately 30% of patients with SAH will develop nosocomial infection during the course of hospitalization [10]. However, most of the available data are derived from retrospective studies or cohort studies with imprecise definitions of infections or sepsis. The diagnosis of sepsis is challenging in patients with SAH due to the high incidence of early SIRS and the lack of reliable biomarkers that can be used to differentiate SIRS and sepsis [8, 9]. Therefore, there is a risk of sepsis misdiagnosis, which can potentially lead to the under- or overtreatment of SAH patients. Considering the previously exposed, the objective of this investigation was to define the incidence of sepsis, diagnosed prospectively with the Sepsis-3 criteria, and its impact on mortality and functional outcomes of patients with SAH.
Methods
Design and setting
We prospectively included all adult patients (≥ 18 years) admitted to the neurological intensive care unit (ICU) of the Paulo Niemeyer State Brain Institute (Rio de Janeiro, Brazil) with aneurysmal SAH between April 2016 and May 2018. The Institute is a reference center for neurovascular diseases and receives approximately 70–100 SAH patients per year from a statewide public healthcare network in Brazil.
The present study was approved by the Ethics Review Board of the Evandro Chagas National Institute of Infectious Diseases—Oswaldo Cruz Foundation (Rio de Janeiro). The data were deidentified by assigning each patient a unique identification number. SAH was diagnosed by findings from the initial computed tomography (CT) scan or by xanthochromia in the cerebrospinal fluid if the findings from the CT scan were normal. Patients who were admitted 30 days or more after a hemorrhagic ictus were excluded. We also excluded patients who were pregnant or had a life expectancy of less than 48 h after admission to the ICU.
Clinical assessment
Demographic data, social and medical history, and clinical features at onset were obtained shortly after admission. Neurological status was assessed with the Glasgow Coma Scale (GCS) [11] and the World Federation of Neurological Surgeons (WFNS) Scale [12]. Systemic disease severity was assessed with the Acute Physiology and Chronic Health Evaluation II (APACHE II) score [13]. Admission and follow-up computed tomography (CT) scans during hospitalization were evaluated by using the modified Fisher scale [14] and for the presence of global cerebral edema and infarction. Daily clinical and laboratory follow-ups were analyzed during the first 14 days of hospitalization or up to the ICU discharge. Data were collected daily during the hospital stay by two investigators (TS and MP), using an electronic case report form (through Research Electronic Data Capture—REDCap). For all patients, the following daily evaluations were also performed: the presence of SIRS and the presence of sepsis or septic shock (according to the Sepsis-3 criteria) [7]; organ dysfunction using the sequential organ failure assessment (SOFA) [15]; and the presence of infection according to clinical and the Centers for Disease Control and Prevention (CDC) criteria. The clinical variables and the diagnosis of infection and sepsis were validated both by the research study team (BG, RT, PK and CR) and through adjudication by an independent infectious disease specialist.
Outcome assessment
The main outcome was the functional outcome, using the Modified Rankin Scale (mRS) score [16]. Scores were prospectively assessed at hospital discharge and 3, 6 and 12 months post-discharge. Long-term outcomes (at 3, 6 and 12 months) were assessed via a telephone interview with the validated mRS score [17]. The interviews were conducted three times during the course of the study; thus, patients included in the final months of the study only had the 3- or 6-month follow-up. Any patient without data available after hospital discharge was considered lost to follow-up. Functional outcome was dichotomized to a poor outcome (defined as mRS 4 to 6) and a good outcome (mRS 0 to 3). Hospital complications after SAH were diagnosed by the clinical team and adjudicated by the research study team (BG, RT, PK and CR) on a weekly basis. DCI was defined as an otherwise unexplained clinical deterioration (such as a new focal deficit, decrease in the level of consciousness or both) or a new infarct shown on the CT scan that was not visible in the admission or the immediate postoperative CT scan, or both, after the exclusion of other potential causes of clinical deterioration. Postoperative deterioration due to operative complications was defined as any neurological worsening or a new infarct within 48 h after the aneurysm repair procedure. Other complications, such as hydrocephalus (defined in this study as the need for cerebrospinal fluid drainage by external ventricular drain or lumbar puncture for that end), rebleeding (defined as a new brain hemorrhage on CT and not related to a surgical procedure), vasospasm (defined as arterial narrowing on cerebral angiogram or mean velocity higher than 120 cm/s and Lindegaard index higher than 3 on transcranial Doppler) and seizures, were also recorded. Aneurysm rebleeding was defined as an acute neurological deterioration with a new hemorrhage apparent on the CT scan.
Statistical analysis
Data are presented as means (standard deviations) or medians (interquartile ranges) for continuous variables and as absolute numbers and percentages for categorical variables. Univariate associations were tested by using the Chi-square or Fisher’s exact test for categorical variables, the two-tailed t test for normally distributed continuous variables and the Mann–Whitney U test for nonnormally distributed continuous variables. Logistic regression was used to test the association between sepsis and mortality and functional outcome using known predictors of poor outcome as covariates. An initial Multivariable analysis was performed to determine the relationship between premorbid demographic, admission clinical and radiographic variables, as well as complications and surgical treatment offered, with functional outcome at hospital discharge. We initially considered for the multivariable model variables associated with poor outcome with a p value lower than 0.1 in univariate analysis. Adjusted odds ratios for specific hospital complications, including sepsis, were calculated by sequentially adding each of these factors to the baseline model to evaluate their unique contribution. A Hosmer–Lemeshow test was used to test the goodness of fit of each model. The final model included age, sex and variables that remained significantly associated with the outcome variable. Potential multicollinearity between the parameters of the final regression model was assessed by calculating tolerance and variance inflation factor coefficients. A Kaplan–Meier survival curve was derived from the log-rank test for the septic and nonseptic groups. The significance was set to 0.05 for all analyses. All analyses were performed with commercially available statistical software (SPSS version 19.0; SPSS Inc., now part of IBM Corporation, Armonk, NY, USA).
Results
Baseline characteristics
In total, 149 patients were enrolled in the study. There were no patients admitted to the ICU who met the exclusion criteria during the period of the study. Age ranged from 22 to 79 years (median 55 years), and most patients were female (109–73%). The demographic and baseline characteristics of all patients are detailed in Table 1. In-hospital mortality was 17% (25 patients), and 69 patients (46%) had poor outcomes at hospital discharge (mRS of 4–6).
Table 1.
Patient demographics and baseline characteristics
| N = 149 | N (%) |
|---|---|
| Median age (range) | 55 (22–79) |
| Female | 109 (73%) |
| Arterial hypertension | 100 (67%) |
| Smoking | 44 (30%) |
| Alcoholism | 20 (13%) |
| Diabetes mellitus | 12 (8%) |
| WFNS grade (I–V) | |
| I | 63 (42%) |
| II | 32 (21%) |
| III | 7 (5%) |
| IV | 29 (19%) |
| V | 18 (12%) |
| Modified Fisher (0–4) | |
| 0 | 6 (4%) |
| 1 | 14 (9%) |
| 2 | 16 (11%) |
| 3 | 65 (44%) |
| 4 | 48 (32%) |
| Mechanical ventilation | 50 (34%) |
| SIRS | 122 (82%) |
| Sepsis | 41 (28%) |
| Hydrocephalus | 45 (30%) |
| Rebleeding | 9 (6%) |
| Vasospasm | 55 (37%) |
| Postoperative neurological deterioration | 47 (32%) |
| DCI | 47 (32%) |
| Hospital mortality | 25 (17%) |
| Poor outcome at discharge (Modified Rankin 4–6) | 69 (46%) |
Incidence of sepsis and SIRS
Fifty-six patients (38%) developed 60 infectious events (four patients had two distinct episodes of infection). The events were classified as follows: fourteen episodes of ventilator-associated pneumonias (VAP), thirteen nosocomial pneumonias, eleven tracheobronchitis, nine meningitis/ventriculitis, six urinary tract infections, two bloodstream infections, one infected pressure ulcer, one dental abscess and three indeterminate infections. Out of all episodes of infection, 27 (45%) were classified as pneumonias. The incidence of sepsis was 28% (41/149 patients), and among those, 18 patients developed septic shock (12% of all patients, 44% of the septic patients). Among septic patients, the initial infection was VAP in nine patients, nosocomial pneumonia in nine, tracheobronchitis in eight, meningitis/ventriculitis in three, urinary tract infections in six, bloodstream infections in two, infected pressure ulcer in one and infections of indeterminate origin in three patients. SIRS was present in 122 patients (82%). The median time between admission and the diagnosis of sepsis was 3 days (interval of 1–14 days). The characteristics of each group, septic and nonseptic, are detailed in Table 2.
Table 2.
Baseline characteristics of septic and nonseptic groups (N/percentage or range/mean)
| Septic | Nonseptic | p value | |
|---|---|---|---|
| N = 41 | N = 108 | ||
| Age | 23–77 (54) | 22–79 (52) | 0.4 |
| Female gender | 27 (66%) | 82 (76%) | 0.22 |
| Arterial hypertension | 34 (83%) | 66 (61%) | 0.01 |
| Diabetes mellitus | 5 (12%) | 7 (6%) | 0.31 |
| Alcoholism | 7 (17%) | 13 (12%) | 0.42 |
| Smoking | 12 (29%) | 32 (29%) | 1 |
| APACHE II | 5–36 (16.22) | 2–31 (10.81) | < 0.00001 |
| Cardiovascular SOFA at admission | 0–4 (0.9) | 0–4 (0.26) | 0.0005 |
| GCS at admission | 3–15 (9.51) | 3–15 (13.44) | < 0.00001 |
| WFNS 4–5 | 25 (61%) | 22 (20%) | < 0.0001 |
| Modified Fisher 3–4 | 34 (83%) | 79 (73%) | 0.28 |
| Mechanical ventilation | 31 (76%) | 19 (17%) | < 0.00001 |
| Hydrocephalus | 23 (56%) | 22 (20%) | < 0.0001 |
| Rebleeding | 1 (2%) | 8 (7%) | 0.45 |
| Endovascular treatment | 22 (54%) | 28 (26%) | 0.002 |
| Surgical treatment | 17 (41%) | 75 (69%) | 0.002 |
Outcomes at hospital discharge
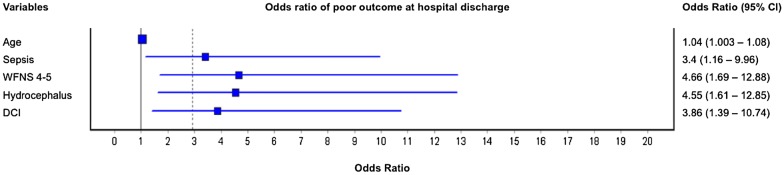
In the univariate analysis, age over 55 years (p = 0.049), sepsis (p < 0.0001), poor grade SAH (WFNS scale of 4–5) (p < 0.0001), modified Fisher scale of 3–4 (p = 0.01), hydrocephalus (p < 0.0001), vasospasm (p = 0.004), postoperative neurological deterioration (p = 0.027) and DCI (p < 0.0001) were associated with a poor outcome. Multivariable logistic regression analysis, with outcomes at hospital discharge, revealed that death or functional dependence (mRS of 4 to 6) at hospital discharge were independently associated with sepsis (OR 3.4, 95% CI 1.16–9.96, p = 0.026) even after controlling for WFNS (OR 4.66, 95% CI 1.69–12.88, p = 0.003), hydrocephalus (OR 4.55, 95% CI 1.61–12.85, p = 0.004) and DCI (OR 3.86, 95% CI 1.39–10.74, p = 0.01) (Table 3). SIRS, however, was not independently associated with a poor functional outcome. The data of the multivariable analysis are presented in Fig. 1.
Table 3.
Study variables and association with functional outcome (at discharge)
| Unfavorable outcome | Favorable outcome | Univariate analysis | Multivariable analysis | ||
|---|---|---|---|---|---|
| (Modified Rankin 4–6) N = 69 | (Modified Rankin 0–3) N = 80 | p value | OR (95% CI) | p value | |
| Age | 57 (45.5–62) | 52 (44–58) | 0.049 | 1.04 (1.003–1.08) | 0.033 |
| Female gender | 51 (73.9%) | 58 (72.5%) | 0.846 | ||
| Infection | 42 (60.9%) | 14 (17.5%) | < 0.0001 | ||
| Pneumoniaa | 23 (33.3%) | 4 (5%) | < 0.0001 | ||
| SIRS | 65 (94.2%) | 57 (71.2%) | 0.0006 | ||
| Sepsis | 34 (49.3%) | 7 (8.8%) | < 0.0001 | 3.4 (1.16–9.96) | 0.026 |
| WFNS 4–5 | 38 (55.1%) | 9 (11.3%) | < 0.0001 | 4.66 (1.69–12.88) | 0.003 |
| Modified Fisher 3–4 | 59 (85.5%) | 54 (67.5%) | 0.01 | ||
| Hydrocephalus | 36 (52.2%) | 9 (11.3%) | < 0.0001 | 4.55 (1.61–12.85) | 0.004 |
| Rebleeding | 4 (5.8%) | 5 (6.3%) | 1 | ||
| Vasospasm | 34 (49.3%) | 21 (26.3%) | 0.004 | ||
| Post-op deterioration | 28 (40.6%) | 19 (23.8%) | 0.027 | ||
| DCI | 38 (55.1%) | 9 (11.3%) | < 0.0001 | 3.86 (1.39–10.74) | 0.01 |
aBoth ventilator-associated pneumonia and nosocomial pneumonia
Fig. 1.
Risk factors for poor outcome at discharge—multivariate analysis
Long-term outcomes
Follow-up data were acquired for 136 patients (13 patients were lost to follow-up—9%, 12 of those patients were in the nonseptic group). Data were available for 95 patients at 12 months (70%), 28 patients at 6 months (20.5%) and 13 patients at 3 months (9.5%). The long-term mortality rate (using the last follow-up available for each patient until 12 months) was 26% (36 out of 136 patients), and the poor outcome rate was 33% (46 out of 136 patients).
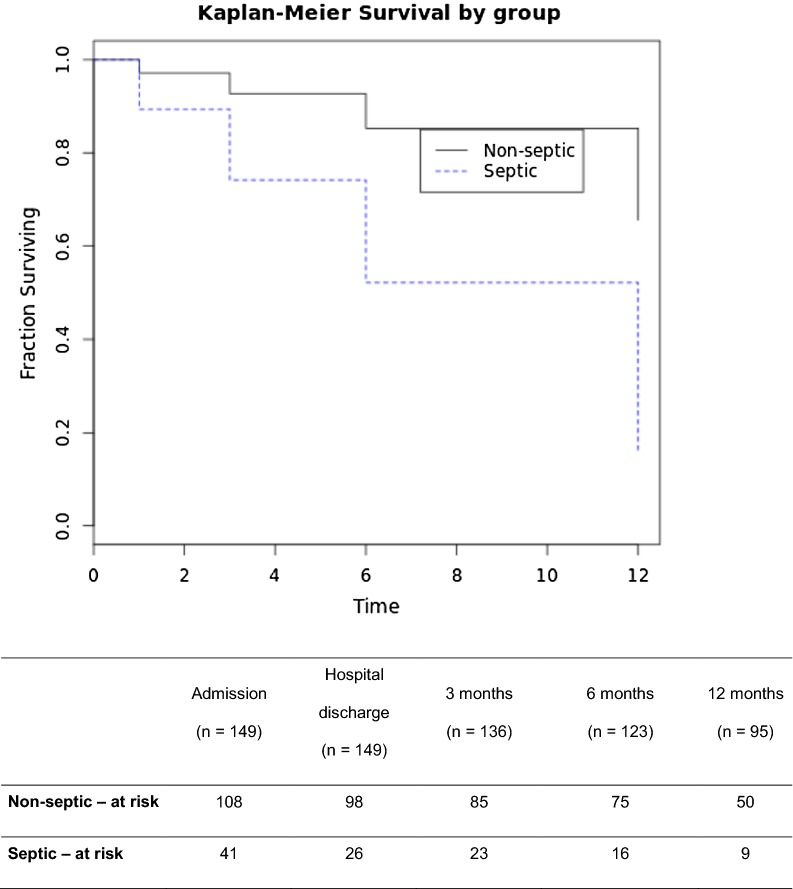
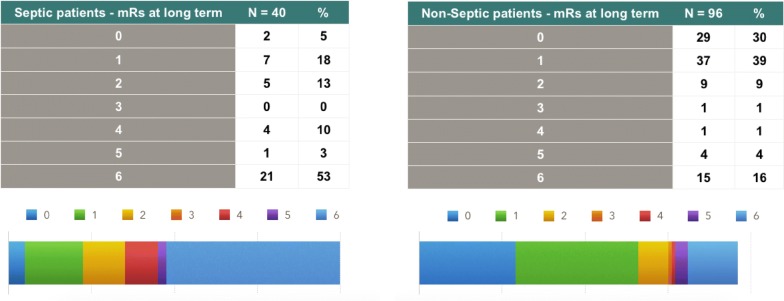
Mortality rates and functional outcomes for the long-term follow-up were significantly different in the septic and nonseptic groups, with higher rates in septic patients (log-rank test p < 0.0001). The long-term mortality rate of septic patients was 52.5% (21 out of 40 patients), and that of nonseptic patients was 16% (15 out of 96). Long-term poor outcome rates were 66% (26 out of 40) for the septic group and 21% (20 out of 96) for nonseptic patients. The Kaplan–Meier survival curve is depicted in Fig. 2, and Fig. 3 shows the long-term outcomes, divided by the mRS, in both the septic and nonseptic groups.
Fig. 2.
Kaplan–Meier survival curves of septic × nonseptic patients with SAH. Log-rank test p < 0.0001. Time to death or last follow-up in months
Fig. 3.
Long-term outcomes on septic and nonseptic patients (poor outcome—mRS 4 to 6 p < 0.0001)
Discussion
In this study, we present the results of a prospective cohort study of SAH patients with functional outcomes (measured by the mRS score) and mortality collected during a maximum of 12 months of follow-up. We prospectively investigated the incidence of sepsis during the first 14 days of the hospital stay, with an incidence of 28%. Sepsis was independently associated with a threefold increase in poor functional outcomes and long-term (using the last data point for each patient) mortality (52.5% for septic patients and 16% for nonseptic patients—log-rank test p < 0.0001).
Aneurysmal SAH is a severe cerebrovascular event that may lead to lifelong disabilities. Mortality can be as high as 15% prior to hospital admission and may reach 40 to 45% in the 30 days after the bleed [3, 18]. After the initial ictus, a number of complications leading to secondary brain injury can further impact outcomes. Sepsis, a complex syndrome where a dysregulated inflammatory response to an infection leads to organ dysfunction, is one of these complications [7].
Regardless of adjustment, in the multivariable analysis, for known neurological factors that affect outcomes (poor grade, hydrocephalus and DCI), sepsis was still independently associated with an unfavorable outcome in our cohort. Some of these neurological factors, such as poor clinical presentation, depend on the initial brain injury—such as a loss of consciousness, seizures and the bleed volume [14]. Others, such as DCI, remain poorly understood and have limited therapeutic options. Sepsis, on the other hand, may be prevented through measures that effectively reduce nosocomial infections. Moreover, accurate and early diagnosis of sepsis combined with an aggressive treatment for organ dysfunction may potentially improve outcomes for SAH patients [3, 19].
Although some studies have shown an association between sepsis and unfavorable outcomes after SAH [20–23], none used the current definition of sepsis (Sepsis-3.0). The previous definitions, which included the SIRS criteria, were less specific and did not clearly discriminate sepsis from a systemic inflammatory response due to noninfectious causes, such as an SAH. Two retrospective studies [24, 25] found associations between the SIRS burden and worse outcomes in SAH, with SIRS incidence ranging from 69 to 85%. Although present in 82% of our patients, SIRS was not associated with a poor outcome after adjusting for confounders. SIRS could be related to the severity of SAH presentation. Sepsis, on the other hand, could play a role in brain dysfunction developed after SAH, working as a second attack on a vulnerable brain. This phenomenon has been shown in other populations where sepsis leads to brain dysfunction, cognitive impairment, muscular loss and exacerbated end-organ dysfunction [19, 26].
The incidence of sepsis is higher than previously reported [8, 9]. The incidence of infection was also higher than previous reports (38%), with 45% of those infections presenting as pneumonia. This study is the first large cohort study of SAH patients with a sepsis diagnosis from low- and middle-income countries, which may explain the differences from the current literature, which mostly comprises European and North American data. Recently, a multicenter study from Brazil [27] has evaluated the national prevalence of sepsis on a single day and reported an incidence of 16.7% and a prevalence of 25% (meaning 30% of patients were septic on the day of the study). The in-hospital mortality rate was 56%. In contrast, the PRISM meta-analysis [28], which reported data from the USA, the UK and Australasia, showed a sepsis-related mortality rate of 25%. Again, data on sepsis, with the use of new criteria, is scarce in low- and middle-income countries and almost nonexistent in the neurocritical population, which may limit such comparisons.
Our study has limitations. First, our institution is a reference center, and the majority of patients are admitted 24 h after ictus. The delay in transfer may introduce selection bias, as patients with a very severe disease presentation, such as evidence of intracranial hypertension, may die before reaching our ICU. Also, that those patients who died early were excluded from our sample may be a reason for the overestimation in the incidence of sepsis in this cohort. Additionally, being a convenience sample, our cohort may be underpowered. Second, follow-up data were acquired for 136 patients (95 patients at 12 months, 28 patients at 6 months and 13 patients at 3 months), with 13 patients lost to follow-up. Third, sepsis diagnosis remains difficult in these patients, even with the new criteria. Confounders such as vasoactive drugs for induced hypertension, neurogenic pulmonary edema and stress-induced myocardial depression may simulate sepsis-induced organ dysfunction. In this population, it is even more difficult due to the neurological impairment due to the bleeding itself, which can elevate the SOFA score (specifically, the neurological SOFA) without sepsis, confounding the diagnosis. To avoid such bias, our sepsis diagnosis was validated by an external specialist (an infectious diseases’ specialist), and for the neurological SOFA, only the rise in the score was considered (not the baseline, if already altered) and when not due to SAH complications (such as DCI or hydrocephalus for instance). Finally, we do not have data on all of the patients’ brain images after discharge, so we cannot explore the hypothesis of sepsis worsening brain damage in more detail—however, this was already addressed by other authors [26] in previous studies.
Though the data indicate a relationship between sepsis and worse outcomes in this cohort, it is still scarce to define a cause–effect association with certainty, especially since the septic group was clearly more severe than the nonseptic group on presentation. However, the multivariate analysis still shows sepsis as an independent variable of worse outcomes. Thus, our study in fact serves to formulate and empower this hypothesis—further studies, with larger cohorts, should be analyzed in order to better clarify the matter.
That aside, a number of potential opportunities arise from a better understanding of the impact of sepsis in patients with SAH. Future studies should aim to develop novel and more accurate methods to improve sepsis diagnosis, such as early molecular detection of bacteria in the blood or monitoring of blood biomarkers (e.g., procalcitonin and C-reactive protein) [9, 10]. Additionally, strategies that aim to reduce early pneumonia, such as the preemptive administration of antibiotics in comatose patients, may potentially reduce the incidence of sepsis and benefit poor grade SAH patients [29].
Sepsis mortality has dropped in recent years in the general ICU population, mainly due to early recognition and effective treatment [30]. Our study shows an association between sepsis and outcomes in SAH; though it is underpowered to determine a cause–effect relationship, it still provides data to create this hypothesis. Based on our results, we believe that nosocomial infection prevention, improved diagnosis and optimal management of infection and sepsis in SAH patients may have a major impact on patients’ outcomes, especially in low- and middle-income countries.
Conclusion
Sepsis can play a significant role in the outcomes of patients with SAH, affecting both mortality and long-term functional outcomes. Combining high-level neurocritical care management of neurological complications and optimal diagnosis and management of sepsis may effectively reduce secondary brain injury and improve patients’ outcomes after SAH.
Acknowledgements
The authors would like to acknowledge Professors André Miguel Japiassú, Charles André and Rodrigo Amâncio for their significant contributions as advisors.
Abbreviations
- SAH
aneurysmal subarachnoid hemorrhage
- DCI
delayed cerebral ischemia
- SIRS
systemic inflammatory response syndrome
- ICU
intensive care unit
- CT
computed tomography
- GCS
Glasgow Coma Scale
- WFNS
World Federation of Neurological Surgeons Scale
- APACHE II
Acute Physiology and Chronic Health Evaluation II
- REDCap
Research Electronic Data Capture
- SOFA
sequential organ failure assessment
- CDC
Centers for Disease Control and Prevention
- mRS
Modified Rankin Scale
- VAP
ventilator-associated pneumonia
Authors’ contributions
MP and TS were responsible for the data collection. BG, PK, RT and CR were responsible for the validation of the data. BG, PK, FAB and CR were responsible for the statistical analysis and the data interpretation. All authors contributed to writing and editing the manuscript. All authors read and approved the final manuscript.
Funding
FAB is a scholar from the Conselho Nacional de Desenvolvimento Cientifico e Tecnológico (BP1C, CNPq) and the Fundação de Amparo à Pesquisa do Estado do Rio de Janeiro (CNE, FAPERJ). We thank the Programa Print-Capes for financial support.
Availability of data and materials
The datasets used and/or analyzed during the current study are available from the corresponding author upon reasonable request.
Ethics approval and consent to participate
The present study was approved by the Ethics Review Board of the Evandro Chagas National Institute of Infectious Diseases—Oswaldo Cruz Foundation (Rio de Janeiro)—Reference Number 52532815.4.0000.5262, and consent to participate was waived due to the observational nature of the study.
Consent for publication
Not applicable.
Competing interests
The authors declare that they have no competing interests.
Footnotes
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Contributor Information
Bruno Gonçalves, Email: brunogs@gmail.com.
Pedro Kurtz, Email: kurtzpedro@mac.com.
Ricardo Turon, Email: ricardoturon@uol.com.br.
Thayana Santos, Email: thayana.ns@gmail.com.
Marco Prazeres, Email: rialarj@gmail.com.
Cassia Righy, Email: cassiarighy@gmail.com.
Fernando Augusto Bozza, Email: bozza.fernando@gmail.com.
References
- 1.Okazaki T, Kuroda Y. Aneurysmal subarachnoid hemorrhage: intensive care for improving neurological outcome. J Intensive Care. 2018;6:28. doi: 10.1186/s40560-018-0297-5. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Nieuwkamp DJ, Setz LE, Algra A, Linn FHH, de Rooij NK, Rinkel GJE. Changes in case fatality of aneurysmal subarachnoid haemorrhage over time, according to age, sex, and region: a meta-analysis. Lancet Neurol. 2009;8(7):635–642. doi: 10.1016/S1474-4422(09)70126-7. [DOI] [PubMed] [Google Scholar]
- 3.Flynn L, Andrews P. Advances in the understanding of delayed cerebral ischaemia after aneurysmal subarachnoid haemorrhage. F1000Res. 2015;4:1000. doi: 10.12688/f1000research.6635.1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Francoeur CL, Mayer SA. Management of delayed cerebral ischemia after subarachnoid hemorrhage. Crit Care Lond Engl. 2016;20(1):277. doi: 10.1186/s13054-016-1447-6. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Macdonald RL, Pluta RM, Zhang JH. Cerebral vasospasm after subarachnoid hemorrhage: the emerging revolution. Nat Clin Pract Neurol. 2007;3(5):256–263. doi: 10.1038/ncpneuro0490. [DOI] [PubMed] [Google Scholar]
- 6.Gonçalves B, Turon R, Mendes A, Melo N, Lacerda P, Brasil P, et al. Effect of early brain infarction after subarachnoid hemorrhage: a systematic review and meta-analysis. World Neurosurg. 2018;115:e292–e298. doi: 10.1016/j.wneu.2018.04.037. [DOI] [PubMed] [Google Scholar]
- 7.Singer M, Deutschman CS, Seymour CW, Shankar-Hari M, Annane D, Bauer M, et al. The third international consensus definitions for sepsis and septic shock (Sepsis-3) JAMA. 2016;315(8):801–810. doi: 10.1001/jama.2016.0287. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Festic E, Siegel J, Stritt M, Freeman WD. The utility of serum procalcitonin in distinguishing systemic inflammatory response syndrome from infection after aneurysmal subarachnoid hemorrhage. Neurocrit Care. 2014;20(3):375–381. doi: 10.1007/s12028-014-9960-4. [DOI] [PubMed] [Google Scholar]
- 9.Oconnor E, Venkatesh B, Mashongonyika C, Lipman J, Hall J, Thomas P. Serum procalcitonin and C-reactive protein as markers of sepsis and outcome in patients with neurotrauma and subarachnoid haemorrhage. Anaesth Intensive Care. 2004;32(4):465–470. doi: 10.1177/0310057X0403200402. [DOI] [PubMed] [Google Scholar]
- 10.Connolly ES, Rabinstein AA, Carhuapoma JR, Derdeyn CP, Dion J, Higashida RT, et al. Guidelines for the management of aneurysmal subarachnoid hemorrhage: a guideline for healthcare professionals from the American Heart Association/American Stroke Association. Stroke. 2012;43(6):1711–1737. doi: 10.1161/STR.0b013e3182587839. [DOI] [PubMed] [Google Scholar]
- 11.Teasdale G, Jennett B. Assessment and prognosis of coma after head injury. Acta Neurochir (Wien). 1976;34(1–4):45–55. doi: 10.1007/BF01405862. [DOI] [PubMed] [Google Scholar]
- 12.Report of World Federation Of Neurological Surgeons committee on a universal subarachnoid hemorrhage grading scale. J Neurosurg. 1988;68(6):985–6. [DOI] [PubMed]
- 13.Knaus WA, Draper EA, Wagner DP, Zimmerman JE. APACHE II: a severity of disease classification system. Crit Care Med. 1985;13(10):818–829. doi: 10.1097/00003246-198510000-00009. [DOI] [PubMed] [Google Scholar]
- 14.Claassen J, Bernardini GL, Kreiter K, Bates J, Du YE, Copeland D, et al. Effect of cisternal and ventricular blood on risk of delayed cerebral ischemia after subarachnoid hemorrhage: the Fisher scale revisited. Stroke. 2001;32(9):2012–2020. doi: 10.1161/hs0901.095677. [DOI] [PubMed] [Google Scholar]
- 15.Vincent JL, Moreno R, Takala J, Willatts S, De Mendonça A, Bruining H, et al. The SOFA (Sepsis-related Organ Failure Assessment) score to describe organ dysfunction/failure On behalf of the Working Group on Sepsis-Related Problems of the European Society of Intensive Care Medicine. Intensive Care Med. 1996;22(7):707–710. doi: 10.1007/BF01709751. [DOI] [PubMed] [Google Scholar]
- 16.van Swieten JC, Koudstaal PJ, Visser MC, Schouten HJ, van Gijn J. Interobserver agreement for the assessment of handicap in stroke patients. Stroke. 1988;19(5):604–607. doi: 10.1161/01.STR.19.5.604. [DOI] [PubMed] [Google Scholar]
- 17.Baggio JAO, Santos-Pontelli TEG, Cougo-Pinto PT, Camilo M, Silva NF, Antunes P, et al. Validation of a structured interview for telephone assessment of the modified Rankin Scale in Brazilian stroke patients. Cerebrovasc Dis Basel Switz. 2014;38(4):297–301. doi: 10.1159/000367646. [DOI] [PubMed] [Google Scholar]
- 18.van Gijn J, Kerr RS, Rinkel GJE. Subarachnoid haemorrhage. Lancet Lond Engl. 2007;369(9558):306–318. doi: 10.1016/S0140-6736(07)60153-6. [DOI] [PubMed] [Google Scholar]
- 19.Cecconi M, Evans L, Levy M, Rhodes A. Sepsis and septic shock. Lancet Lond Engl. 2018;392:75–87. doi: 10.1016/S0140-6736(18)30696-2. [DOI] [PubMed] [Google Scholar]
- 20.Abulhasan YB, Alabdulraheem N, Schiller I, Rachel SP, Dendukuri N, Angle MR, et al. Health care-associated infections after subarachnoid hemorrhage. World Neurosurg. 2018;115:e393–e403. doi: 10.1016/j.wneu.2018.04.061. [DOI] [PubMed] [Google Scholar]
- 21.Frontera JA, Fernandez A, Schmidt JM, Claassen J, Wartenberg KE, Badjatia N, et al. Impact of nosocomial infectious complications after subarachnoid hemorrhage. Neurosurgery. 2008;62(1):80–87. doi: 10.1227/01.NEU.0000311064.18368.EA. [DOI] [PubMed] [Google Scholar]
- 22.Taufique Z, May T, Meyers E, Falo C, Mayer SA, Agarwal S, et al. Predictors of poor quality of life 1 year after subarachnoid hemorrhage. Neurosurgery. 2016;78(2):256–264. doi: 10.1227/NEU.0000000000001042. [DOI] [PubMed] [Google Scholar]
- 23.Tseng M-Y, Hutchinson PJ, Kirkpatrick PJ. Interaction of neurovascular protection of erythropoietin with age, sepsis, and statin therapy following aneurysmal subarachnoid hemorrhage. J Neurosurg. 2010;112(6):1235–1239. doi: 10.3171/2009.10.JNS09954. [DOI] [PubMed] [Google Scholar]
- 24.Dhar R, Diringer MN. The burden of the systemic inflammatory response predicts vasospasm and outcome after subarachnoid hemorrhage. Neurocrit Care. 2008;8(3):404–412. doi: 10.1007/s12028-008-9054-2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25.Rass V, Gaasch M, Kofler M, Schiefecker AJ, Ianosi B-A, Rhomberg P, et al. Systemic inflammatory response syndrome as predictor of poor outcome in nontraumatic subarachnoid hemorrhage patients. Crit Care Med. 2018;46(12):e1152–e1159. doi: 10.1097/CCM.0000000000003429. [DOI] [PubMed] [Google Scholar]
- 26.Annane D, Sharshar T. Cognitive decline after sepsis. Lancet Respir Med. 2015;3(1):61–69. doi: 10.1016/S2213-2600(14)70246-2. [DOI] [PubMed] [Google Scholar]
- 27.Machado FR, Cavalcanti AB, Bozza FA, Ferreira EM, Angotti Carrara FS, Sousa JL, et al. The epidemiology of sepsis in Brazilian intensive care units (the Sepsis PREvalence Assessment Database, SPREAD): an observational study. Lancet Infect Dis. 2017;17(11):1180–1189. doi: 10.1016/S1473-3099(17)30322-5. [DOI] [PubMed] [Google Scholar]
- 28.PRISM Investigators. Rowan KM, Angus DC, Bailey M, Barnato AE, Bellomo R, et al. Early, goal-directed therapy for septic shock—a patient-level meta-analysis. N Engl J Med. 2017;376(23):2223–2234. doi: 10.1056/NEJMoa1701380. [DOI] [PubMed] [Google Scholar]
- 29.Righy C, do Brasil PEA, Vallés J, Bozza FA, Martin-Loeches I. Systemic antibiotics for preventing ventilator-associated pneumonia in comatose patients: a systematic review and meta-analysis. Ann Intensive Care. 2017;7(1):67. doi: 10.1186/s13613-017-0291-4. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 30.Kaukonen K-M, Bailey M, Suzuki S, Pilcher D, Bellomo R. Mortality related to severe sepsis and septic shock among critically ill patients in Australia and New Zealand, 2000–2012. JAMA. 2014;311(13):1308–1316. doi: 10.1001/jama.2014.2637. [DOI] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Data Availability Statement
The datasets used and/or analyzed during the current study are available from the corresponding author upon reasonable request.