Abstract
In the present study, LC-HRESIMS-assisted dereplication along with bioactivity-guided isolation led to targeting two brominated oxindole alkaloids (compounds 1 and 2) which probably play a key role in the previously reported antibacterial, antibiofilm, and cytotoxicity of Callyspongia siphonella crude extracts. Both metabolites showed potent antibacterial activity against Gram-positive bacteria, Staphylococcus aureus (minimum inhibitory concentration (MIC) = 8 and 4 µg/mL) and Bacillus subtilis (MIC = 16 and 4 µg/mL), respectively. Furthermore, they displayed moderate biofilm inhibitory activity in Pseudomonas aeruginosa (49.32% and 41.76% inhibition, respectively), and moderate in vitro antitrypanosomal activity (13.47 and 10.27 µM, respectively). In addition, they revealed a strong cytotoxic effect toward different human cancer cell lines, supposedly through induction of necrosis. This study sheds light on the possible role of these metabolites (compounds 1 and 2) in keeping fouling organisms away from the sponge outer surface, and the possible applications of these defensive molecules in the development of new anti-infective agents.
Keywords: Callyspongia siphonella, LC-HRESIMS, metabolomic profiling, oxindole alkaloids, tisindoline, antibacterial, antibiofilm, antitrypanosomal, anticancer
1. Introduction
Marine sponges are prolific producers of diverse bioactive secondary metabolites that were reported over the years [1,2]. These sessile marine animals developed a defensive chemical arsenal to keep small animals and plants (fouling organisms) away from settling on their outer surfaces [3]. Furthermore, these metabolites may also be used to regulate symbiotic bacterial populations known to associate with sponges [4]. The genus Callyspongia belongs to the order Haplosclerida, family Callyspongiidae. Callyspongia siphonella (Levi, 1965) is widely distributed throughout the Gulfs of Aqaba and Suez from shallow water, but mostly deeper than 5 m [5]. Several bioactive secondary metabolites including sipholane triterpenes [6], polyacetylenic alcohols [7], and amides [8] were isolated from different members of this genus. In addition to these anticancer metabolites, a number of steroidal anti-inflammatory compounds were also reported from this genus [9]. Pseudomonas aeruginosa biofilms can cause serious infections especially for the elderly and immunocompromised patients. Unfortunately, such infections often cannot be treated efficiently with common antibiotics [10,11]. A number of Callyspongia crude extracts showed potent antibacterial and antibiofilm activities toward several pathogenic bacterial strains, particularly Pseudomonas aeruginosa PA01 [12]. In the present study, bioactivity-guided fractionation together with LC-HRESIMS-assisted chemical investigation of the Red Sea sponge C. siphonella led to the isolation of two antibacterial brominated oxindole alkaloids (1,2) from a natural source for the first time along with several known metabolites. Compounds 1 and 2 showed considerable anti-biofilm activity in P. aeruginosa and moderate in vitro antitrypanosomal activity. Moreover, they induced strong cell death in HT29, OVCAR-3, and MM.1S cancer cell lines after 24-h stimulation.
2. Results and Discussion
2.1. Metabolomic Profiling
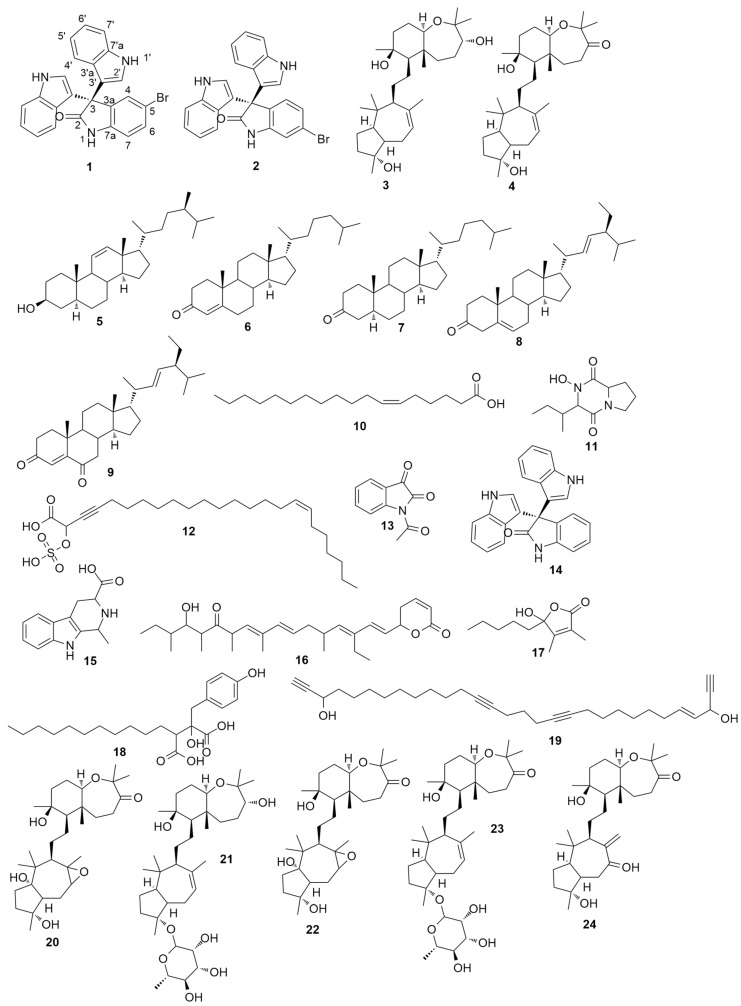
To date, a growing number of secondary metabolites were identified from Callyspongia siphonella with diverse pharmacological effects [13]. Sipholane triterpenoids are considered the main characteristic metabolites of this sponge. This class of metabolites was found to show a potent reversal of multidrug resistance in tumor cells that overexpressed P-glycoprotein (P-gp) [14]. In addition, there are many polyactylenes, polyketides, and alkaloids that were also reported from C. siphonella. In view of that, metabolomic profiling of the marine sponge C. siphonella using LC-HRESIMS for dereplication purpose resulted in the characterization of a variety of metabolites (Figure 1 and Figure S1) of which sipholane triterpenes were found to be prevalent (Table 1). From the AntiMarine and Dictionary of Natural Products (DNP) databases, a total of 24 compounds were tentatively identified. Seven compounds out of these were members of the P-glycoprotein inhibitors, sipholane triterpenoids (3,4,20–24). Additionally, the antiproliferative metabolites, callystatin A (16), hydroxydihydrobovolide (17), callyspongidic acid (18), and callyspongendiol (19), were also dereplicated in the n-hexane fraction [15]. All sipholane triterpenes are presumably derived from the cyclization of triepoxysqualenes. Detection of several mass ion peaks proposed to be the biosynthetic intermediates of sipholane triterpenes supported the previously suggested biosynthetic pathway (Scheme S1) [6]. Similarly, compounds 11, 12, 13, 14, and 15 were detected in the ethyl acetate fraction. Moreover, intermediate compounds suggesting that they were involved in the biosynthesis of trisindoline (14) and its brominated derivatives (compounds 1 and 2) from tryptophan [16,17] were also found (Scheme S2). Tisindoline (14) is an antibiotic indole trimer previously isolated from marine Vibrio and Shewanella species [18,19]. In addition to the identified hits (Figure 1), other unidentified molecular formulae were detected, particularly in the ethyl acetate fraction, suggesting the presence of further unknown metabolites. These findings, together with the primary antibacterial screening, prioritized the ethyl acetate fraction for a further chemical investigation to isolate the active metabolites.
Figure 1.
Identified compounds by dereplication with LC-HRESIMS.
Table 1.
Dereplication of the metabolites previously identified from Callyspongia siphonella.
| NP | Compound | RT (min) | [M + H]+ | Calculated Mass | Chemical Formula |
|---|---|---|---|---|---|
| 1 | Compound 1 a | 3.21 | 442.0552 | 442.0555 | C24H17N3OBr |
| 2 | Compound 2 a | 3.32 | 442.552 | 442.0555 | C24H17N3OBr |
| 3 | Sipholenol A c | 5.96 | 477.3941 | 477.3944 | C30H53O4 |
| 4 | Sipholenone A c | 6.41 | 475.3785 | 475.3787 | C30H51O4 |
| 5 | Callysterol c | 7.12 | 401.381 | 401.3783 | C28H49O |
| 6 | Cholestenone b | 7.38 | 385.3472 | 385.347 | C27H45O |
| 7 | 5α-cholestanone b | 7.41 | 387.3625 | 387.3627 | C27H47O |
| 8 | Stigmasterone b | 7.49 | 411.3634 | 411.3637 | C29H47O |
| 9 | stigmasta-4,22-dien-3,6-dione b | 6.95 | 425.345 | 425.342 | C29H45O2 |
| 10 | Petroselenic acid b | 8.91 | 283.2634 | 283.2637 | C18H35O2 |
| 11 | Callyspongidipeptide A | 2.26 | 227.139 | 227.1396 | C11H19N2O3 |
| 12 | Callysponginol sulfate A | 2.6 | 459.2783 | 459.278 | C24H43O6S |
| 13 | N-acetyl isatin b | 2.7 | 190.0501 | 190.0504 | C10H8NO3 |
| 14 | Trisindoline b | 2.86 | 364.1456 | 364.145 | C24H18N3O |
| 15 | 1,2,3,4-tetrahydro-1- methyl-β-carboline-3-carboxylic acid | 2.99 | 231.1133 | 231.1134 | C13H15N2O2 |
| 16 | Callystatin A | 3.83 | 457.3325 | 457.3318 | C29H45O4 |
| 17 | Hydroxydihydrobovolide | 3.88 | 199.1339 | 199.1334 | C11H19O3 |
| 18 | Callyspongidic acid | 3.95 | 395.2429 | 395.2434 | C22H35O6 |
| 19 | Callyspongendiol | 4.51 | 437.3413 | 437.3420 | C30H45O2 |
| 20 | 15,16-epoxy-22-hydroxysipholen-one A | 5.18 | 507.3676 | 507.3686 | C30H51O6 |
| 21 | Sipholenoside B | 5.34 | 623.452 | 623.4523 | C36H63O8 |
| 22 | Sipholenol G | 5.39 | 493.3889 | 493.3893 | C30H53O5 |
| 23 | Sipholenoside A | 5.63 | 621.4368 | 621.4366 | C36H61O8 |
| 24 | Sipholenone C | 6.26 | 489.3562 | 489.3580 | C30H49O5 |
a Isolated in the present study as a new natural product. b Isolated in the present study for the first time from C. siphonella. c Previously reported from C. siphonella and confirmed by isolation.
2.2. Structure Characterization of the Isolated Compounds
The ethanolic extract of C. siphonella was partitioned with different organic solvents with increasing polarity. The n-hexane and ethyl acetate fractions displayed weak to moderate antibacterial activities. Further bioactivity-guided fractionation of the ethyl acetate fraction, which showed several new hits upon LC-HRESIMS dereplication, led to the isolation of compounds 1 and 2.
Compound 1 was isolated as buff powder; the molecular formula C24H16ON3Br was suggested on the basis of a positive HRESIMS ion at m/z 442.0554 [M + H]+, indicating 18 degrees of unsaturation. 1H-NMR spectral data of 1 (Table 2) in deuterated dimethyl sulfoxide (DMSO-d6) suggested the presence of two exchangeable protons (δH 10.77, 11.03) due to NH. In addition, the splitting pattern of resonances at δH 6.97 (H-7), 7.42 (H-6), and 7.30 (H-4), together with the 1H–1H COSY correlation between (H-6) and (H-7), suggested the presence of a 1,3,4-trisubstituted benzene ring. The DEPTQ spectrum (Table 2) displayed 16 signals, with 15 sp2 aromatic carbons including eight CH groups and seven quaternary carbons, and one sp3 aliphatic quaternary carbon (C-3). The spectra also revealed an aminocarbonyl at δC178.9 (C-2). The assignment of protonated carbons was achieved by the 1H–13C HSQC data. The key HMBC correlations (Figure 2) from H-4 (δH 7.30, s, 1H) to C-3 (δC 53.2), and from the exchangeable proton H-1(δH 10.77) to the carbonyl carbons C-2 (δC 178.9) and C-3a (δC 137.44) together with the previous reported data [18], suggested the presence of a brominated indolin-2-one skeleton at C-5 (δC 114). The presence of two identical indole moieties linked to brominated oxindole moity at C-3 (δC 53.2) was figured out from the 1H-NMR spectral data (Table 2) and the 1H–13C HMBC correlations (Figure 2). According to these data, HRESIMS analysis, and previously published data [20], compound 1 was identified as 5-bromo trisindoline.
Table 2.
1H- (400 MHz) and 13C-NMR (100 MHz) for compounds 1 and 2 in DMSO-d6.
| Compound 1 | Compound 2 | |||
|---|---|---|---|---|
| Position | δH, mult. (J in Hz) | δC, Type | δH, mult. (J in Hz) | δC, Type |
| 1-NH | 10.77 (br s, 1H) | - | 10.75, (br s, 1H) | - |
| 2 | - | 178.9, C | - | 179, C |
| 3 | - | 53.2, C | - | 52.7, C |
| 3a | - | 137.4, C | - | 134.3, C |
| 4 | 7.30, (s, 1H) | 127.8, CH | 7.16, (d, 8Hz, 1H) | 127.1, CH |
| 5 | - | 114, C | 7.12, (dd, 2Hz, 8Hz, 1H) | 124.6, CH |
| 6 | 7.42, (d, 8Hz, 1H) | 131.2, CH | - | 120.7, C |
| 7 | 6.97, (d, 8Hz, 1H) | 112.2, CH | 7.14, (s, 1H) | 112.8, CH |
| 7a | - | 141.1, C | - | 143.5, C |
| 1-NH’, 1-NH’’ | 11.03 (br s, 2H) | - | 11.0, (br s, 1H) | - |
| 2′, 2′’ | 6.89, (s, 2H) | 124.9, CH | 6.85, (d, 2.5Hz, 2H) | 124.8, CH |
| 3′, 3′’ | - | 113.6, C | - | 114.0, C |
| 3′a, 3′’a | - | 126, C | - | 126, C |
| 4′, 4′’ | 7.22, (d, 8Hz, 2H) | 121, CH | 7.2, (d, 8Hz, 2H) | 121, CH |
| 5′, 5′’ | 6.83, (t, 8Hz, 2H) | 119, CH | 6.81, (t, 8Hz, 2H) | 118.8, CH |
| 6′, 6′’ | 7.04, (t, 8Hz, 2H) | 121.5, CH | 7.03, (t, 8Hz, 2H) | 121.5, CH |
| 7′, 7′’ | 7.39, (d, 8Hz, 2H) | 112.2, CH | 7.35, (d, 8Hz, 2H) | 112.1, CH |
| 7′a, 7′’a | - | 137.4, C | - | 137.4, C |
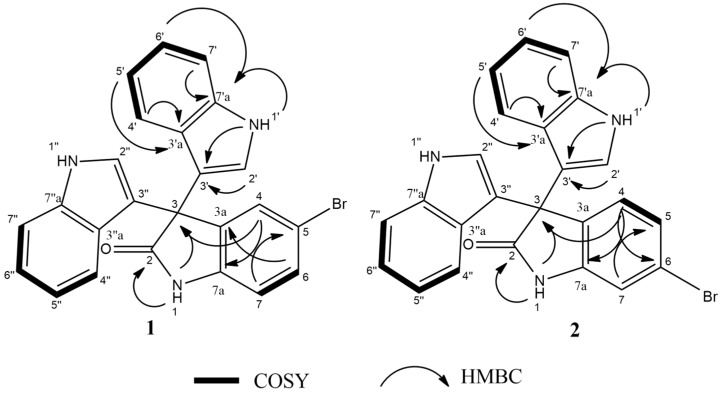
Figure 2.
1H–1H COSY and key HMBC correlations of compounds 1,2.
Compound 2 was isolated as a white amorphous powder. The molecular formula C24H16ON3Br was suggested on the basis of the positive HRESIMS ion at m/z 442.0554 [M + H]+, indicating 18 degrees of unsaturation. HRESIMS and 1H and 13C-NMR spectra of 2 (Table 2) were almost identical to that of compound 1. In addition, the similar two-dimensional (2D)-NMR correlations indicate that compounds 1 and 2 are positional isomers, where the bromine is attached to C-6 instead of C-5. This different attachment was confirmed from the 1H–13C HMBC correlation between H-4 (δH 7.16, d, 8Hz, 1H) and C-2 (δC 179); hence, compound 2 was identified as 6-bromo trisindoline.
Both 5-bromotrisindoline (1) and 6-bromotrisindoline (2) are brominated indole trimers, previously reported as synthetic intermediates [20,21] and isolated herein for the first time from a natural source. Their parent non-halogenated trisindoline (14) was previously isolated from a marine bacterium and exhibited significant antibacterial activity [18]. Only 5-bromotrisindoline (1) was reported as an α-glycosidase enzyme inhibitor [20]. 1H-NMR and 13C-NMR assignments of 5-bromotrisindoline (1) and 6-bromotrisindoline (2) are reported here for the first time based on extensive HSQC, COSY, and HMBC analysis (Figures S3–S21, Supplementary Materials).
Further known metabolites, sipholenol A (3) and sipholenone A (4) [22], along with five steroidal compounds, callysterol (5) [9], cholestenone (6), 5α-cholestanone (7) [23], stigmasterone (8) [24], and stigmasta-4,22-dien-3,6-dione (9) [25], and one major fatty acid, petroselenic acid (10) [26,27], were also isolated from the n-hexane fraction of C. siphonella (Figure 1). All isolated known metabolites were identified based on their accurate mass analyses and comparison of their NMR spectroscopic data with those reported in the literature (Figures S22–S47, Supplementary Materials). The triterpenes sipholenol A (3) and sipholenone A (4) are major metabolites in C. siphonella. Sipholenol A (3) was previously reported as a potent P-glycoprotein inhibitor in multidrug-resistant cancer cells [14]. Callysterol (5) is a characteristic sterol in C. siphonella which exhibited in vitro anti-inflammatory activity [9]. The steroidal compounds (6–9), along with the fatty acid petroselenic acid (10), were isolated here from C. siphonella for the first time.
2.3. Antibacterial Activity
For primary antibacterial screening, the crude ethanolic extracts, all fractions, and the isolated compounds were evaluated against Staphylococcus aureus (ATCC 25923), Bacillus subtilis (ATCC 5230), Escherichia coli (ATCC 25922), and Pseudomonas aeruginosa (ATCC 9027). The antibacterial activity was recorded as an inhibition zone diameter and measured as “mm” (Table 3). Ampicillin and gentamicin were used as a positive control. The ethyl acetate fraction showed the highest inhibition against Staphylococcus aureus (6.6 mm), Bacillus subtilis (5.4 mm), and Escherichia coli (1.5 mm), while the n-hexane fraction exhibited mild antibacterial activity with inhibition zones ranging from 1 to 2 mm. These findings are in great accordance with the previously reported antibacterial activity of C. siphonella extracts [28]. Compounds 1 and 2 derived from the ethyl acetate fraction displayed potent antibacterial activity against Gram-positive bacteria S. aureus and B. subtilis with inhibition zones of 17.5 mm and 18 mm, and 15 mm and 16.4 mm, respectively (Table 4). With respect to Gram-negative bacteria E. coli and P. aeruginosa, 1 and 2 showed weak antibacterial activity with inhibition zones of 0.5 mm and 1.3 mm, and 0.2 mm and 1.1 mm, respectively. The other isolated compounds (3–10) did not exhibit any inhibition against the tested bacterial strains. The minimum inhibitory concentration (MIC) values of 1 and 2 that showed antibiotic activity in disc diffusion tests were determined (Table 5). It was observed that the MIC value of 2 against S. aureus (16 µg/mL) was higher than that of 1 (8 µg/mL). However, both compounds exhibited potent inhibitory effect toward B. subtilis with an MIC value of 4 µg/mL. In a previous study [18], their parent compound, trisindoline (14), showed antibacterial activity against both Gram-positive and Gram-negative bacterial strains; hence, incorporation of a bromine atom into the oxindole moiety of trisindoline (14) reduces the antibacterial spectrum of these molecules. From the previous observations, we can conclude that the bromotrisindolines (1,2) may be the main metabolites responsible for the antibacterial activity of C. siphonella extract against Gram-positive bacteria.
Table 3.
Inhibition zone diameter (mm) of the ethanol extract and fractions of C. siphonella on different bacterial strains (mean ± standard error (SE).
| Tested Extract | Staphylococcus aureus | Bacillus subtilis | Escherichia coli | Pseudomonas aeruginosa |
|---|---|---|---|---|
| EtOH Ext | 1.1 ± 0.5 | 1.2 ± 0.2 | - | - |
| Hex | 2.3 ± 0.9 | 1.1 ± 0.4 | - | 1 ± 0.4 |
| EtOAc | 6.6 ± 0.2 | 5.4 ± 0.3 | 1.5 ± 0.7 | - |
| ButOH | - | 0.5 ± 0.2 | - | - |
| Ampicillin | 13.7 ± 0.9 | 12.3 ± 1.2 | 3.9 ± 0.9 | 3.6 ± 0.3 |
| Gentamicin | 9.8± 1.2 | 10.1 ± 1.1 | 15.5 ± 0.1 | 14.8 ± 1.3 |
Ampicillin, gentamicin, extracts, and fractions (20 µg/mL DMSO). EtOH, ethanol extract; Hex, n-hexane fraction; EtOAc, ethyl acetate fraction; ButOH, n-butanol fraction. (-) indicates no growth inhibition found.
Table 4.
Inhibition zone diameter (mm) of 1 and 2 on different bacterial strains (mean ± SE).
| Tested compound | S. aureus | B. subtilis | E. coli | P. aeruginosa |
|---|---|---|---|---|
| 1 | 17.5 ± 0.8 | 18 ± 0.1 | 0.5 ± 0.1 | 1.3 ± 0.3 |
| 2 | 15 ± 1.1 | 16.4 ± 0.9 | 0.2 ± 0.2 | 1.1 ± 0.7 |
| Amikacin | 23.5 ± 0.8 | 20.2 ± 0.6 | 15.4 ± 0.4 | 16.3 ± 0.9 |
Table 5.
Minimal inhibitory concentration (MIC) (µg/mL) values of 1 and 2.
| Fungal metabolite | S. aureus | B. subtilis | E. coli | P. aeruginosa |
|---|---|---|---|---|
| 1 | 8 | 4 | >256 | 256 |
| 2 | 16 | 4 | >256 | 256 |
| Ampicillin | 2 | 2 | 4 | 8 |
| Gentamicin | 16 | 8 | 0.5 | 1 |
2.4. Antibiofilm Activity
As demonstrated from the antibacterial screening, metabolites 1 and 2 did not exhibit any inhibition against the Gram-negative bacteria, P. aeruginosa PAO1. However, compounds that have no direct growth inhibitory effect on the pathogenic organisms still have the potential to act as biofilm formation inhibitors. As outlined in a recent review [29], many categories of natural products, including marine invertebrate-derived metabolites can stop the formation of biofilms and, thus, comprise candidates for adjuvant therapy as boosters of the common antibiotics. Therefore, all isolated compounds were tested against P. aeruginosa to determine if they could inhibit biofilm formation. Compound 1 reduced biofilm formation slightly more (49.32% inhibition) than 2 (41.76%) at concentrations of 128 µg/mL (0.5 MIC) (Table 6). The remaining compounds were inactive at tested concentrations. To the best of our knowledge, none of the derivatives of trisindoline antibiotic are so far associated with inhibition of biofilm formation in human pathogens. Therefore, further mechanistic studies on these compounds are needed.
Table 6.
Antibiofilm activity of 1 and 2 in Pseudomonas aeruginosa PA01.
| Isolated compound | % Inhibition |
|---|---|
| 1 | 49.32 ± 1.18 |
| 2 | 41.76 ± 1.33 |
| Azithromycin | 52.62 ±1.23 |
Each compound was tested at concentration of 128 µg/mL (0.5 MIC). Azithromycin was tested at a concentration of 16 µg/mL (0.5 MIC).
2.5. Antitrypanosomal Activity
African trypanosomiasis, which is also known as sleeping sickness, is a fatal and neglected disease caused by Trypanosoma brucei, affecting mostly the poor people living in tropical and subtropical zones [30]. The increasing resistance to the current medications necessitated the development of novel alternatives to fight this disease. Natural products will continue to play a vital role in the search for new antitrypanosomal drugs. All isolated compounds were tested against the sleeping sickness parasite, T. brucei. Both metabolites 1 and 2 demonstrated moderate antitrypanosomal activity after 48 and 72 h with half maximal inhibitory concentration (IC50) values of 15.36 (48 h) and 13.47 (72 h), and 12.35 (48 h), and 10.27 (72 h) µM, respectively. However, the other isolated compounds were found inactive against T. brucei.
2.6. Cytotoxic Activity
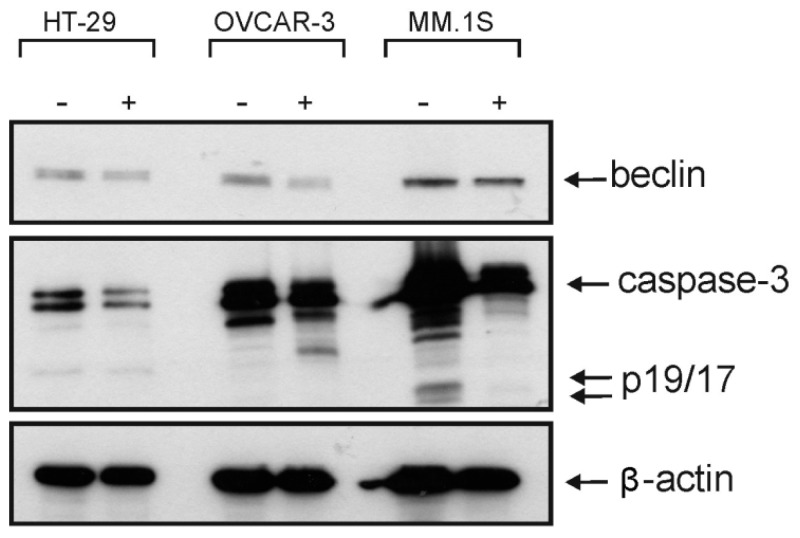
Crystal violet and 3-(4,5-dimethylthiazol-2-yl)-2,5-diphenyltetrazolium bromide (MTT) assays were used to assess the cytotoxicity of all isolated metabolites against three different cancer cell lines over a concentration range of 0.01–50 µM. Both 1 and 2 revealed significant cytotoxic effects (Table 7) against all cell lines under investigation (human colon cancer cell line: HT-29, human ovarian cancer cell line: OVCAR-3, and multiple myeloma cell line: MM.1S). Furthermore, the microscopic pictures showed clear changes in cell morphology after overnight treatment with 1 (Figure 3 and Figure 4). However, the Western blotting analysis showed only a decrease in the level of procaspase-3 but unfortunately, we neither detected any split caspase-3 products, the key protein of apoptosis, nor changes in the level of beclin protein, one of the master proteins of autophagy (Figure 5). Moreover, 1 was not able to induce the upregulation of proinflammatory cytokines such as interleukin-8 (IL8) in MM.1S and HT-29 (Figure S2, Supplementary Materials). Our previous results and many previous publications showed that the programmed cell death is usually accompanied by the induction of proinflammatory signals such as IL8 [31,32]. This confirms the Western blotting results that compound 1 kills the cancer cells by non-programmed cell necrosis but not by programmed cell death mechanisms such as necroptosis, apoptosis, or autophagy.
Table 7.
Cytotoxic effects of 1 and 2 expressed by half maximal inhibitory concentration (IC50) values.
| Compounds | IC50 (µM) a | ||
|---|---|---|---|
| HT-29 | OVCAR-3 | MM. 1S | |
| 1 | 8 ± 0.8 | 7 ± 0.3 | 9 ± 0.7 |
| 2 | 12.5 ± 0.3 | 9 ± 0.6 | 11 ± 0.9 |
a Values are means of three independent experiments. human colon cancer cell line: HT-29; human ovarian cancer cell line: OVCAR-3; multiple myeloma cell line: MM.1S.
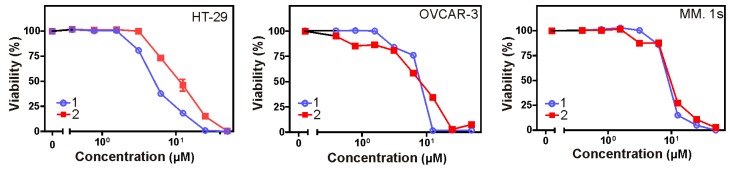
Figure 3.
Cytotoxic effects of compounds 1 and 2 on human colon cancer (HT-29), human ovarian cancer (OVACR-3), and multiple myeloma (MM.1s) cell lines. The cells were stimulated overnight with increasing concentrations of compounds 1 and 2. on the next day, cellular viability was determined by crystal violet staining for HT-29 and OVACR-3, and 3-(4,5-dimethylthiazol-2-yl)-2,5-diphenyltetrazolium bromide (MTT) assay for MM.1s.
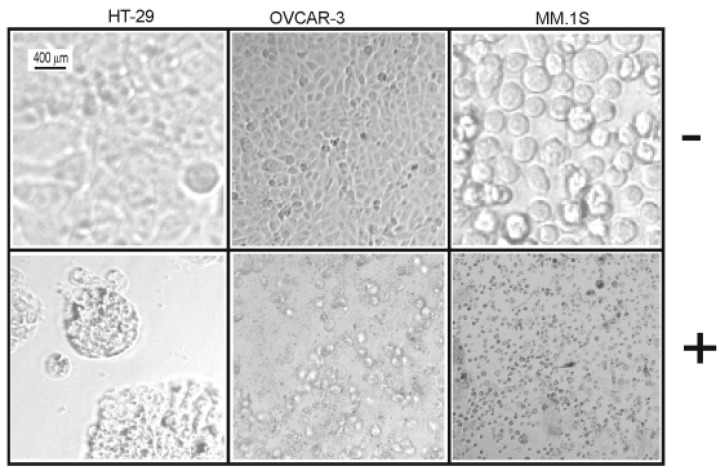
Figure 4.
Morphological changes of HT-29, OVCAR-3, and MM.1S cells incubated overnight with compound (1) (20 µM) in comparison to untreated cells using an EVOS FL digital microscope.
Figure 5.
Western blotting analysis of 1 against beclin and caspase 3, the key proteins of autophagy and apoptosis, respectively.
3. Material and Methods
3.1. Extraction and Fractionation
The marine sponge C. siphonella (2 kg) was collected in November 2015 from Hurghada along the Red Sea Coast (27°15048” north (N), 33°4903” east (E)) at depth of 7 m. A voucher sample (NIOF204/2015) was reserved at the Invertebrates Department, National Institute of Oceanography and Fisheries, Red Sea Branch, Hurghada, Egypt. Subsequently, sponge material was cut into small pieces, and then subjected to ultrasonic-assisted extraction with ethanol (3 × 500 mL). The resulted liquid extract was concentrated using a rotary evaporator (IKA®, Staufen, Germany). The obtained concentrated extract was suspended in distilled water and fractionated with n-hexane (4 × 200 mL), ethyl acetate (3 × 200 mL), and n-butanol (3 × 200 mL). All fractions were separately concentrated under reduced pressure and screened for their antibacterial activities.
3.2. Metabolomics Analysis
Metabolomic profiling was performed on the crude extract of C. siphonella on an Acquity Ultra Performance Liquid Chromatography system coupled to a Synapt G2 HDMS quadrupole time-of-flight hybrid mass spectrometer (Waters, Milford, CT, USA). Chromatographic separation was carried out on a BEH C18 column (2.1 × 100 mm, 1.7 μm particle size; Waters, Milford, CT, USA) with a guard column (2.1 × 5 mm, 1.7 μm particle size) and a linear binary solvent gradient of 0–100% eluent B over 6 min at a flow rate of 0.3 mL∙min−1, using 0.1% formic acid in water (v/v) as solvent A and acetonitrile as solvent B. The injection volume was 2 μL and the column temperature was 40 °C. Ms converter software was used in order to convert the raw data into divided positive and negative ionization files. Obtained files were then subjected to the data mining software MZmine 2.10 (Okinawa Institute of Science and Technology Graduate University, Japan) for deconvolution, peak picking, alignment, deisotoping, and formula prediction. The databases used for the identification of compounds were: MarinLit: http://pubs.rsc.org/marinlit/, and Dictionary of Natural Products (DNP) 2018: http://dnp.chemnetbase.com/faces/chemical/ChemicalSearch.xhtml.
3.3. Assessment of Antibacterial Activity
The tested microorganisms used in this study included Gram-positive (Staphylococcus aureus, ATCC 25923 and Bacillus subtilis ATCC 5230) and Gram-negative (Escherichia coli ATCC 25922 and Pseudomonas aeruginosa ATCC 9027) pathogenic bacteria. An agar well diffusion assay was used to investigate the antibacterial activity of all sponge extracts and fractions [33]. Minimal inhibitory concentrations (MIC) were determined by the broth dilution method for isolated compounds according to Clinical and Laboratory Standards Institute (CLSI) protocol [34].
3.4. Bioactivity-Guided Isolation of the Major Metabolites
After a preliminary assessment of all prepared fractions and extracts for antibacterial activities, the ethyl acetate fraction (2 g) was the most active against Gram-positive bacteria. Further fractionation on silica gel column (60–120 mesh, Fluka®) using n-hexane/ethyl acetate in a gradient elution, resulted in three sub-fractions (codes F1–F3). Afterward, the active sub-fraction F3 (400 mg) was chromatographed on Agilent® 1260 Infinity preparative HPLC using acetonitrile in water (70–100%) for 20 min followed by 100% acetonitrile for the next 10 min at a 20 mL/min flow rate to afford 1 (21 mg) and 2 (25 mg). Similarly, the less active n-hexane fraction was fractionated on a silica gel column using n-hexane/ethyl acetate in a gradient elution to give six sub-fractions (codes F1–F6). Subfraction F1 (600 mg) was chromatographed on a silica gel column using n-hexane/ethyl acetate in a gradient elution to afford 10 (40 mg) and 7 (15 mg). In the same manner, subfraction F2 (350 mg) was chromatographed on silica gel column using n-hexane/ethyl acetate in a gradient elution to afford 6 (15 mg) and 8 (20 mg). Furthermore, subfractions F3–F5 (250 mg) were combined and chromatographed on a silica gel column using dichloromethane/methanol in a gradient elution to afford 9 (15 mg), 5 (30 mg), 4 (50 mg), and 3 (100 mg). The structure of the isolated compounds was elucidated by comparison of their spectral data (MS and NMR) with those reported in the literature. MS and NMR spectra were recorded on Agilent series 1100 SL (Agilent CO, Santa Clara, CA, USA) and Bruker Avance III 400 MHz (Bruker AG, Switzerland), respectively.
3.5. Screening of Antibiofilm Activity
The assay was performed as previously described by Drenkard and Ausubel (2002) [35] with minor modifications. Briefly, PseudomonasaeruginosaPAO1 was cultured in lysogeny broth (LB) medium (Himedia®, Mumbai, India). After incubation, cultures were vortexed, diluted 1:100 in fresh LB medium for biofilm formation, and cultured with or without the tested natural products and azithromycin (AZM) (Sigma Aldrich®, Munich, Germany) for 24 h at 37 °C. Then, the non-adherent cells were washed with phosphate-buffered saline (PBS), while adherent ones were subjected to 1% crystal violet staining for 15 min. The wells were washed again with water to get rid of excess stain. After the wells dried, the crystal violet obligated to the biofilm was extracted with 95% ethanol. The crystal violet solution absorbance (in optical density units, OD) was measured at 570 nm. AZM was reported as a biofilm inhibitor at the sub-inhibitory concentration [36]; thus, it was used as a positive control in the bioassay. Percentage inhibition was calculated according to the following rule:
3.6. Antitrypanosomal Activity Testing
The antitrypanosomal activity was tested against Trypanosoma brucei strain TC221 according to the Huber and Koella protocol [37]. The growth inhibitory activity was measured using an MR 700 microplate reader at wavelengths of 550 and 650 nm. IC50 values were calculated by linear interpolation of three independent measurements. Samples were considered active when their IC50 values were less than 20 μM.
3.7. Cytotoxic Activity Assessment
Cell lines were maintained in earth RPMI 1640 medium (HT-29 and MM.1S cells) or in DMEM medium (OVCAR-3 cells) containing 10% heat-inactivated fetal bovine serum (FBS), and were grown at 37 °C and 5% CO2. Anti-caspase-3 (#9662) and anti-beclin (#3495S) were purchased from Cell Signaling (Beverly, MA, USA), and anti-β-actin (monoclonal AC015) from Sigma (Louis, Mo 363103 USA). Cell lines were counted and seeded on 96-well cell culture plates (2 × 104 cells/well in the case of HT-29 and OVCAR-3 and 6 × 104 cells/well in the case of MM.1S cells). Cells were stimulated either in the next day in the case of HT-29 and OVCAR-3 or on the same day in the case of MM.1S cells with the indicated concentrations of each compound overnight in triplicates. Cell viability was assessed either by crystal violet staining in the case of HT-29 and OVCAR-3 or by 3-(4,5-dimethylthiazol-2-yl)-2,5-diphenyltetrazolium bromide (MTT) assay in the case of MM.1S cells [38]. To normalize cell viability values, each plate included a triplicate of untreated cells considered as 100% viability, and a triplicate of cells treated with a cytotoxic mixture (200 ng/mL TNF, 200 ng/mL CD95L, 200 ng/mL TRAIL, 5 μg/mL CHX, 1% (w/v) sodium azide 20%) considered as 0% viability. All other viability values were normalized according to the averages of these triplicates and analyzed by the Graph Pad Prism 5 software (La Jolla, CA, USA).
3.8. Western Blotting
Cells were seeded in six-well plates (1 × 106/well) and stimulated with 40 µM of compound 4. In the next day, cells were harvested in ice-cold PBS and washed by centrifuging cells twice in PBS and centrifuged for 4 min at 1200 rpm (4°C). Then, total cell lysates were prepared as described before in our previous work [32]. The membranes were incubated overnight with primary antibodies and antigen-antibody reactions were performed in the next day using the corresponding secondary antibodies (anti-mouse-HRP, Dako-Cytomation, Hamburg, Germany; anti-rabbit-HRP, Cell Signaling Technology). The specific bands were visualized using ECL detection reagents for Western blotting (Amersham Biosciences, Germany).
3.9. IL8 ELISA
Firstly, 2 × 104 of MM.1S and HT-29 cells per well were seeded in 96-well plates. On the next day, the medium was changed to reduce the background of constitutive IL8 production, and cells were incubated with the indicated reagent(s) for 16 h. The supernatants were collected and analyzed for production of IL8 using the human IL8 ELISA (enzyme-linked immunosorbent assay) kit BD Biosciences (Heidelberg, Germany) according to the instructions of the supplier.
4. Conclusion
The present study clearly highlighted the efficacy of LC–MS profiling when coupled to bio-guided drug discovery from marine invertebrates to speed up the traditionally long processes of identifying an active metabolite by consecutive isolation from crude extracts. Dereplication studies based on the chemotaxonomic sorting helped in the identification of putative active metabolites, whereas structural assignment of the isolated compounds, employing both HR-MS and NMR, confirmed the identified hits. Thus, bio-guided isolation coupled to LC–MS metabolomic profiling of the Red Sea sponge C. siphonella led to the characterization of two brominated indole alkaloids (1,2), which were not isolated from natural sources before. Moreover, metabolomics analysis gave insight into the metabolic pathways required for the biosynthesis of compounds 1 and 2 from tryptophan, together with the characteristic sipholane triterpenoids from squalene. Compounds 1 and 2 showed excellent in vitro antibacterial activity against the tested Gram-positive strains and displayed significant anti-biofilm activity in P. aeruginosa. Moreover, they exhibited considerable in vitro antitrypanosomal activity, and were able to trigger potent cell death in a few tumor cell lines. Western blotting together with IL8 assay results suggested that compounds 1 and 2 could mediate their cytotoxicity via necrosis induction. The present investigation sheds the light on how C. siphonella can defend itself chemically within its hostile marine environment and the possible utilization of its defensive metabolites in the future development of new anti-infective agents. Further in vivo biological evaluation of these interesting bis-indoles will be of value for future drug development.
Acknowledgments
We would also like to thank Mostafa Nasr Taha, Microbiology Department, Nahda University for helping us in the anti-biofilm activity evaluation.
Supplementary Materials
The following are available online at https://www.mdpi.com/1660-3397/17/8/465/s1: Schemes S1 and S2: Proposed metabolic pathways for sipholane triterpenoids and alkaloids in Callyspongia siphonilla; Figures S1–S47: One-dimensional and two-dimensional (1D and 2D) NMR spectra of isolated compounds.
Author Contributions
Conceptualization, S.S.E.-H., A.M.S., R.M. and H.M.H.; T.A.M. collected and identified the marine sponge; methodology and compounds isolation, A.M.S.; formal analysis, A.M.S. and M.E.R.; biological assays, M.A.A.; funding acquisition, E.A., M.E.-M., A.B.M., A.A., H.W., U.R.A.; writing—review and editing, All authors.
Funding
This publication was funded by the German Research Foundation (DFG) and the University of Wuerzburg in the funding program Open Access Publishing.
Conflicts of Interest
The authors declare no conflict of interest.
References
- 1.Hertiani T., Edrada-Ebel R., Ortlepp S., van Soes R.W., de Voogd N.J., Wray V., Hentschel U., Kozytska S., Müller W.E., Proksch P. From anti-fouling to biofilm inhibition: New cytotoxic secondary metabolites from two Indonesian Agelas sponges. Bioorg. Med. Chem. 2010;18:1297–1311. doi: 10.1016/j.bmc.2009.12.028. [DOI] [PubMed] [Google Scholar]
- 2.Faulkner D.J. Marine natural products. Nat. Prod. Rep. 2001;19:1–48. doi: 10.1039/b006897g. [DOI] [PubMed] [Google Scholar]
- 3.Hentschel U., Usher K.M., Taylor M.W. Marine sponges as microbial fermenters. FEMS Microbiol. Ecol. 2006;55:167–177. doi: 10.1111/j.1574-6941.2005.00046.x. [DOI] [PubMed] [Google Scholar]
- 4.Bergquist P.R. Sponges. University of California Press; Berkeley, CA, USA: 1978. [Google Scholar]
- 5.Ilan M., Gugel J., Van Soest R. Taxonomy, reproduction and ecology of new and known Res Sea Sponges North Atlantic. Mar. Sci. 2004;89:388–410. [Google Scholar]
- 6.Kashman Y., Yosief T., Carmeli S. New Triterpenoids from the Red Sea sponge Siphonochalina siphonella. J. Nat. Prod. 2001;64:175–180. doi: 10.1021/np0003950. [DOI] [PubMed] [Google Scholar]
- 7.Tsukamoto S., Kato H., Hirota H., Fusetani N. Seven new polyacetylene derivatives, showing both potent metamorphosis-inducing activity in ascidian larvae and antifouling activity against barnacle larvae, from the marine sponge Callyspongia truncate. J. Nat. Prod. 1997;60:126–130. doi: 10.1021/np9606097. [DOI] [Google Scholar]
- 8.Sera Y., Adachi K., Shizuri Y. A new epidioxy sterol as an antifouling substance from a Palauan marine sponge, Lendenfeldia chondrodes. J. Nat. Prod. 1999;62:152–154. doi: 10.1021/np980263v. [DOI] [PubMed] [Google Scholar]
- 9.Youssef D.T., Ibrahim A.K., Khalifa S.I., Mesbah M.K., Mayer A.M., van Soest R.W. New anti-inflammatory sterols from the two Red Sea sponges Scalarispongia aqabaensis and Callyspongia siphonella. Nat. Prod. Commun. 2010;5:27–31. [PubMed] [Google Scholar]
- 10.Bjarnshoit T., Jensen P.Q., Jakobsen T.H., Phipps R., Nielsen A.K., Rybtke M.T., Tolker-Nielsen T., Givskov M., Haiby N., Ciofu O. Quorum sensing and virulence of Pseudomonas aeruginosa during lung infection of cystic fibrosis patients. PLoS ONE. 2010;5:e10115. doi: 10.1371/journal.pone.0010115. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Li Y.H., Tian X. Quorum sensing and bacterial social interactions in biofilms. Sensors. 2012;12:2519–2538. doi: 10.3390/s120302519. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Pejin B., Talevska A., Ciric A., Glamoclija J., Nikolic M., Talevski T., Sokovic M. Anti-quorum sensing activity of selected sponge extracts: A case study of Pseudomonas aeruginosa. Nat. Prod. Res. 2014;28:2330–2333. doi: 10.1080/14786419.2014.934239. [DOI] [PubMed] [Google Scholar]
- 13.Azcuna M., Tun J.O., Yap H.T., Concepcion G.P. Callyspongia samarensis (Porifera) extracts exhibit anticancer activity and induce bleaching in Porites cylindrica (Scleractinia) Chem. Ecol. 2018;34:397–411. doi: 10.1080/02757540.2018.1437148. [DOI] [Google Scholar]
- 14.Shi Z., Jain S., Kim I.W., Peng X.X., Abraham I., Youssef D.T.A., Fu L.W., El-Sayed K., Ambudkar S.V., Chen Z.S. Sipholenol A, a marine-derived sipholane triterpene, potently reverses P-glycoprotein (ABCB1)-mediated multidrug resistance in cancer cells. Cancer Sci. 2007;98:1373–1380. doi: 10.1111/j.1349-7006.2007.00554.x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Yang B., Hu J., Lei H., Chen X.Q., Zhou X.F., Liu Y.H. Chemical constituents of marine sponge Callyspongia sp. from the South China Sea. Chem. Nat. Compd. 2012;48:350–351. doi: 10.1007/s10600-012-0248-7. [DOI] [Google Scholar]
- 16.Johansen S.S., Licht D., Arvin E., Mosbæk H., Hansen A.B. Metabolic pathways of quinoline, indole and their methylated analogs by Desulfobacterium indolicum (DSM 3383) Appl. Microbiol. Biotechnol. 1997;47:292–300. doi: 10.1007/s002530050929. [DOI] [Google Scholar]
- 17.Mujahid M., Sasikala C., Ramana C.V. Production of indole-3-acetic acid and related indole derivatives from L-tryptophan by Rubrivivax benzoatilyticus JA2. Appl. Microbiol. Biotechnol. 2011;89:1001–1008. doi: 10.1007/s00253-010-2951-2. [DOI] [PubMed] [Google Scholar]
- 18.Kobayashi M., Aoki S., Gato K., Matsunami K., Kurosu M., Kitagawa I. Marine natural products. XXXIV. Trisindoline, a new antibiotic indole trimer, produced by a bacterium of Vibrio sp. separated from the marine sponge Hyrtios altum. Chem. Pharm. Bull. 1994;42:2449–2451. doi: 10.1248/cpb.42.2449. [DOI] [PubMed] [Google Scholar]
- 19.Wang Y., Tang X., Shao Z., Ren J., Liu D., Proksch P., Lin W. Indole-based alkaloids from deep-sea bacterium Shewanella piezotolerans with antitumor activities. J. Antibiot. 2014;67:395. doi: 10.1038/ja.2014.3. [DOI] [PubMed] [Google Scholar]
- 20.Wang G., Wang J., Xie Z., Chen M., Li L., Peng Y., Chen S., Li W., Deng B. Discovery of 3,3-di(indolyl)indolin-2-one as a novel scaffold for α-glucosidase inhibitors: In silico studies and SAR predictions. Bioorg. Chem. 2017;72:228–233. doi: 10.1016/j.bioorg.2017.05.006. [DOI] [PubMed] [Google Scholar]
- 21.Wang S.Y., Ji S.J. Facile synthesis of 3,3-di(heteroaryl)indolin-2-one derivatives catalyzed by ceric ammonium nitrate (CAN) under ultrasound irradiation. Tetrahedron. 2006;62:1527–1535. doi: 10.1016/j.tet.2005.11.011. [DOI] [Google Scholar]
- 22.Carmely S., Kashman Y. The Sipholanes: A novel group of triterpenes from the marine sponge Siphonochalina siphonella. J. Org. Chem. 1983;48:3517–3525. doi: 10.1021/jo00168a029. [DOI] [Google Scholar]
- 23.Wishart D.S., Tzur D., Knox C., Eisner R., Guo A.C., Young N., Cheng D., Jewell K., Arndt D., Sawhney S., et al. HMDB: The Human Metabolome Database. Nucleic Acids Res. 2007;35(Suppl. 1):D521–D526. doi: 10.1093/nar/gkl923. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.Chang H.S., Lee S.J., Yang C.W., Chen I.S. Cytotoxic sesquiterpenes from Magnolia kachirachirai. Chem. Biodivers. 2010;7:2737–2747. doi: 10.1002/cbdv.200900418. [DOI] [PubMed] [Google Scholar]
- 25.Fernandez M., Pedro J.R.I., Seoane E. Constituents of a hexane extract of Phoenix dactylifera. Phytochemistry. 1983;22:2087–2088. [Google Scholar]
- 26.Delbeke E.I.P., Everaert J., Uitterhaegen E., Verweire S., Verlee A., Talou T., Soetaert W., Van Bogaert I.N.A., Stevens C.V. Petroselinic acid purifcation and its use for the fermentation of new sophorolipids. AMB Express. 2016;6:28. doi: 10.1186/s13568-016-0199-7. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 27.Knothe G., Steidley K.R. Composition of Some Apiaceae Seed Oils Includes Phytochemicals, and Mass Spectrometry of Fatty Acid 2-Methoxyethyl Esters. Eur. J. Lipid. Sci. Tech. 2019;121:1800386. doi: 10.1002/ejlt.201800386. [DOI] [Google Scholar]
- 28.Afifi R., Khabour O.F. Antibacterial activity of the Saudi Red Sea sponges against Gram-positive pathogens. J. King Saud Univ. Sci. 2017 doi: 10.1016/j.jksus.2017.08.009. [DOI] [Google Scholar]
- 29.Buommino E., Scognamiglio M., Donnarumma G., Fiorentino A., D0Abrosca B. Recent advances in natural product-based anti-biofilm approaches to control infections. Mini Rev. Med. Chem. 2014;14:1169–1182. doi: 10.2174/1389557515666150101095853. [DOI] [PubMed] [Google Scholar]
- 30.Brun R., Blum J., Chappuis F., Burri C. Human african trypanosomiasis. Lancet. 2010;375:148–159. doi: 10.1016/S0140-6736(09)60829-1. [DOI] [PubMed] [Google Scholar]
- 31.Thirumangalakudi L., Yin L., Rao H.V., Grammas P. IL-8 induces expression of matrix metalloproteinases, cell cycle and pro-apoptotic proteins, and cell death in cultured neurons. J. Alzheimers Dis. 2007;11:305–311. doi: 10.3233/JAD-2007-11307. [DOI] [PubMed] [Google Scholar]
- 32.Anany M.A., Kreckel J., Füllsack S., Rosenthal A., Otto C., Siegmund D., Wajant H. Soluble TNF-like weak inducer of apoptosis (TWEAK) enhances poly (I: C)-induced RIPK1-mediated necroptosis. Cell Death Dis. 2018;9:1084. doi: 10.1038/s41419-018-1137-1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 33.Valgas C., Souza S.M.D., Smânia E.F., Smânia J.A. Screening methods to determine antibacterial activity of natural products. Braz. J. Microbiol. 2007;38:369–380. doi: 10.1590/S1517-83822007000200034. [DOI] [Google Scholar]
- 34.Clinical and Laboratory Standards Institute (CLSI) Performance Standards for Antimicrobial Susceptibility Testing. CLSI; Wayne, PA, USA: 2006. Sixteenth Informational Supplement; CLSI Document M100-S16CLSI. [Google Scholar]
- 35.Drenkard E., Ausubel F.M. Pseudomonas biofilm formation and antibiotic resistance are linked to phenotypic variation. Nature. 2002;416:740–743. doi: 10.1038/416740a. [DOI] [PubMed] [Google Scholar]
- 36.Morita Y., Tomida J., Kawamura Y. Responses of Pseudomonas aeruginosa to antimicrobials. Front. Microbiol. 2014;4:422. doi: 10.3389/fmicb.2013.00422. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 37.Huber W., Koella J.C. A comparison of three methods of estimating EC50 in studies of drug resistance of malaria parasites. Acta Trop. 1993;55:257–261. doi: 10.1016/0001-706X(93)90083-N. [DOI] [PubMed] [Google Scholar]
- 38.Cheng C., Othman E.M., Stopper H., Edrada-Ebel R., Hentschel U., Abdelmohsen U.R. Isolation of Petrocidin A, a New Cytotoxic Cyclic Dipeptide from the Marine Sponge-Derived Bacterium Streptomyces sp. SBT348. Mar. Drugs. 2017;15:383. doi: 10.3390/md15120383. [DOI] [PMC free article] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.