Abstract
Background
Vazirani–Akinosi nerve block technique is an established and a reliable technique to achieve anaesthesia in mandible with high success rate and is useful in cases where Halstead’s technique fails to provide desired anaesthetic effect.
Materials and Methods
A total of 140 ASA-I or ASA-II patients, both genders, between 16 and 45 years who required extraction of mandibular tooth were divided into two groups. Group A received nerve block through Halstead technique, while Group B received nerve block through Vazirani–Akinosi technique with 2% lignocaine containing 1:200,000 adrenaline. We evaluated the subjective and objective onset of anaesthesia, outcome of the injection, outcome of the aspiration and patient satisfaction.
Results
In Group A, the altered sensation was experienced at 68.70 s, while in Group B it was 92.55 s and the difference was statistically highly significant (p < 0.001) between the two groups. The mean onset of anaesthesia (measured with Electric pulp tester) in Group A was 78.36 s, while for Group B it was 104.24 s and this difference was statistically highly significant (p < 0.001). Positive aspiration was seen in 11 (15.71%) patients in Group A and in 2 (2.86%) patients in Group B. The success rate for Group A was 81.42% and for Group B it was 97.14%.
Conclusion
Vazirani–Akinosi technique provides desirable surgical anaesthesia with relatively high success rate and lower incidence of positive aspiration and can be considered as a boon for oral and maxillofacial surgeons.
Keywords: Inferior alveolar nerve block, Vazirani–Akinosi technique, Closed mouth technique, Halstead technique
Introduction
Inferior alveolar nerve block (IANB) is the most frequently performed nerve block in dentistry for local anaesthesia (LA) in mandible. The different techniques to achieve IANB include “Halstead or Standard technique”, “Vazirani–Akinosi or Closed Mouth Technique” and “Gow-Gates or Open Mouth Technique” [1]. Dr. William Stewart Halstead on 6 December 1884 described a method for blocking the inferior alveolar nerve (IAN) using cocaine as the local anaesthetic; and since then, it has been the most frequently used method for blocking the IAN [2, 3]. The success rate of this technique, however, is considerably lower than those of most other nerve blocks [1]. Two important reasons causing failure of this technique are anatomical variation of mandibular foramen and accessory innervations. Accessory innervations to the pulps may arise from a distinct branch separating from inferior alveolar nerve in the pterygomandibular space, or supply from cervical accessory nerves; or in some situations, accessory nerves may accompany the mylohyoid nerve, as well as buccal, lingual or auriculotemporal nerves. In such situations, an alternative nerve block technique, that can help to overcome these reasons causing failure of Halstead technique, is highly indicated. Vazirani–Akinosi (VA) closed mouth technique is one such method that can provide successful anaesthesia in these circumstances [1, 4].
The aim of the present study was to evaluate the efficacy of VA nerve block technique in comparison with Halstead’s standard inferior alveolar nerve block (SIANB) technique.
Material and Method
The study was approved by the institutional ethical committee. A total of 140 ASA-I or ASA-II patients, of both genders, between 16 and 45 years of age group participated in the study. Only those patients who required extraction of mandibular posterior teeth, other than first molar, by conventional method were included. The patients excluded were pregnant and lactating females, medically compromised and mentally retarded patients, and those with acute dental infections. Before the start of the study, each subject was explained about the study design and a written informed consent was obtained from them before their enrolment. These 140 subjects were divided randomly into two groups of 70 each. Group A received local anaesthesia with 2% lignocaine containing 1:200,000 adrenaline as nerve block through Halstead technique. Group B received local anaesthesia with 2% lignocaine containing 1:200,000 adrenaline as nerve block through VA technique (Figs. 1, 2).
Fig. 1.
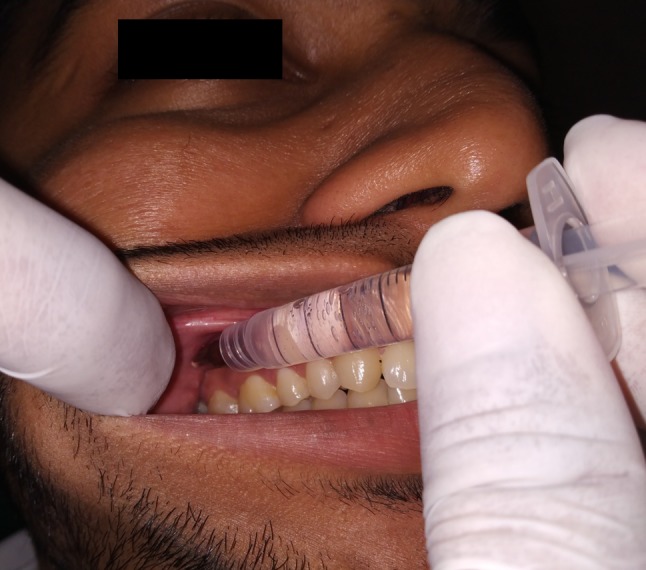
Clinical demonstration for performing the Vazirani–Akinosi closed mouth technique
Fig. 2.

Demonstration on the human dried skull for the area of insertion and needle position for Vazirani–Akinosi Technique
The injection was given under all aseptic precaution using 2-ml Luer-lock syringe with 27-gauge needle by the same investigator. After inserting the needle to the desired location, two planar aspirations were performed to verify whether the needle was in the blood vessel or not. If the aspiration was found negative (needle not in the blood vessel), then the injection was completed slowly at the rate of 1 ml/min to deposit a total of 2 ml of 2% lignocaine with 1:200,000 adrenaline. The patients were explained about the visual analogue scale (VAS) before the injection procedure that ranged from 0 to 10. The patients were asked to interpret the pain on injection as per the scores on VAS, and the same was recorded for each patient. After completion of injection, the time interval at which the patient experienced altered sensation on the lower lip was recorded using a stopwatch. The moment patient informed about tingling sensation, we checked the onset of anaesthesia by pricking the soft tissue in the region of the ipsilateral premolars with a dental probe. We performed Electric Pulp Testing over the first molar tooth on the ipsilateral side at two consecutive intervals which were 5 min apart. If the reading was 80/80 at both the times, then the block anaesthesia was considered as a success. We also recorded the patient’s feedback as poor, fair, good, very good and excellent.
Statistical Analysis
Descriptive statistics were expressed as mean ± standard deviation (SD) for each group. The two groups were compared for altered sensation and onset of anaesthesia by Independent ‘t’ test. The association among responses from patient (patient feedback), outcome of injection (success/failure) and aspiration (positive/negative) between the groups were analysed by Chi-square test. In the above tests, p value less than 0.05 (p < 0.05) was taken to be statistically significant. All analyses were performed using SPSS software version 17.
Result
A total of 140 patients divided into two groups of 70 each participated in this study. In Group A, there were 29 females and 41 males, while Group B had 26 females and 44 males. The mean age in Group A was 27.14 years, and in Group B it was 29.00 years. There was no significant difference for pain on injection between the two groups (p > 0.05). In Group A, the altered sensation was experienced at 68.70 s (1.145 min) with a SD of 20.59 s (0.343 min), while in Group B it was 92.55 s (1.542 min) with a SD of 21.07 s (0.351 min). The difference in onset of altered sensation was statistically highly significant (p < 0.001) between the two groups (Table 1). The highest onset of altered sensation was 125 s in Group A and 137 s in Group B, while lowest in Group A was 30 s and in Group B it was 60 s. The mean onset of anaesthesia (measured with Electric pulp tester) in Group A was 78.36 s (1.306 min) with a SD of 21.47 s (0.357 min), while for Group B it was 104.24 s (1.737 min) with a SD of 21.73 s (0.362 min). This difference was statistically highly significant (p < 0.001) (Table 2). The highest onset of anaesthesia in Group A was 2.25 min (135 s), and in Group B it was 2.45 min (147 s), while lowest in Group A was 45 s (0.75 min) and in Group B it was 70 s (1.166 min). Positive aspiration was seen in 11 (15.71%) patients in Group A and in 2 (2.86%) patients in Group B. This difference was statistically highly significant (p < 0.001) (Table 3). The success rate in Group A (for Halstead nerve block technique) was 81.42%, while in Group B (for Vazirani–Akinosi technique) it was 97.14%. The difference between the outcomes of injection between the two groups was highly significant (p < 0.001). Fourteen (20%) patients in Group A and five (7.1%) patients in Group B considered the injection procedure as fair, while 29 (41.4%) in Group A and 49 (70%) in Group B considered the procedure as good, while 14 (20%) in Group A and 16 (22.9%) in Group B considered the injection as very good. There was statistically significant difference in the patient satisfaction between the two groups (p < 0.05) (Table 4).
Table 1.
Comparison between two groups for altered sensation (in seconds) by Independent ‘t’ test
| Group | Mean altered sensation (in seconds) | Standard deviation | t value | df | p value |
|---|---|---|---|---|---|
| − 6.410 | 125 | < 0.001* | |||
| Group A | 68.7018 | 20.59557 | |||
| Group B | 92.5571 | 21.07106 |
*p value < 0.05 is statistically significant; < 0.001 is highly significant
Table 2.
Comparison between two groups for onset of action (in seconds) by Independent ‘t’ test
| Group | Mean onset of action (in seconds) | Standard deviation | t value | df | p value |
|---|---|---|---|---|---|
| − 6.707 | 125 | < 0.001* | |||
| Group A | 78.3684 | 21.47892 | |||
| Group B | 104.2429 | 21.73852 |
*p value < 0.05 is statistically significant; < 0.001 is highly significant
Table 3.
Comparison between two groups for aspiration outcome by Chi-square test
| Group | Positive aspiration (no. of patients) | Negative aspiration (no. of patients) | df | p value |
|---|---|---|---|---|
| 2 | < 0.001* | |||
| Group A | 11 (15.7%) | 46 (65.7%) | ||
| Group B | 1 (1.43%) | 67 (95.71%) |
*p value < 0.05 is statistically significant; < 0.001 is highly significant
Table 4.
Comparison between two groups for satisfaction scores by Chi-square test
| Group | Bad | Fair | Good | Very good | df | p value |
|---|---|---|---|---|---|---|
| 4 | <0.001* | |||||
| Group A | 0 (0%) | 14 (20%) | 29 (41.4%) | 14 (20%) | ||
| Group B | 0 (0%) | 5 (7.1%) | 49 (70%) | 16 (22.9%) |
*p value < 0.05 is statistically significant; < 0.001 is highly significant
Discussion
One of the most important aspects of the practice of dentistry is the control or elimination of pain. The most frequently used injection technique in dentistry is supraperiosteal infiltration [1]. The success of this technique, however, is directly proportional to the diffusion of the anaesthetic solution through the periosteum and bone to come into contact with the nerves or nerve endings. Since maxilla is a porous bone, this technique has a high success rate when used for maxillary teeth anaesthesia. However, in mandible because of dense cortical bone this technique does not provide the desired anaesthetic effect except for the mandibular incisor region [5]. The inferior alveolar (dental) nerve, which is the major branch of the principal nerve supplying the mandible, supplies the pulps of the mandibular teeth in the form of inferior dental plexus. Therefore, blocking this nerve becomes an integral part of pain control for dental procedures in the mandible under local anaesthesia [1, 5].
The SIANB pioneered by Halstead is the most common technique used to obtain IAN anaesthesia [1, 2]. Peterson called this block as the mandibular foramen block [6]. However, a substantial failure rate for this method has been reported that ranges between 15% and 20%. Such failures may not be overcome even with a second attempt. The technique can fail even in the experienced hands due to anatomical variations such as variability in the location of the mandibular foramen on the medial aspect of the ramus or bifid IANs and bifid mandibular canals. It is evident that in a patient with limited mouth opening, performing an SIANB is intractable [1, 2, 5]. The various reasons for failure of Halstead technique are summarized in Table 5.
Table 5.
Causes for SIANB failure
| Reasons for failure of standard IANB (Halstead technique) | |
|---|---|
|
1. Technical error 2. Infected tissues at the injection site 3. Patient Apprehension 4. Anatomical variation 5. Accessory innervations |
The closed mouth technique for achieving anaesthesia in mandible was first described by Vazirani in 1960 and was brought to the attention of educators by Akinosi in 1977, and hence the name Vazirani–Akinosi became popular to address this method [5]. Akinosi called this technique as “the tuberosity approach to the mandibular nerve”. The success of this technique can be attributed to the anatomy of the upper part of the pterygomandibular space where the trunk of three nerves, namely IAN, lingual and buccal, come to lie in close proximity suitable for simultaneous injection (Fig. 3) [7]. This technique is having many advantages over the one described by Halstead (Table 6). For performing SIANB, the mouth opening should be wide so as to visualize and palpate the landmarks for successful completion of the injection [1]. However, apprehensive patients sometimes may not co-operate to open their mouth wide, thus making the injection difficult to be perform. In the SIANB, the needle is inserted near the throat; thus, patient may become more apprehensive. Because in VA method the mouth is kept closed and the injection is performed adjacent to the cheek region, the patient co-operates better. Also, in SIANB the fingers of the operator and the syringe lie between the patient’s teeth, so there exists a fear that the patient may bite on either of the two. In VA technique, this fear is eliminated since neither the syringe nor the operator’s finger is between the occlusion and it has a relatively less danger for the needle fracture. Often, the SIANB becomes unsuitable for achieving anaesthesia in the lower third molar area due to acute alveolar abscess or pericoronitis because the inflammation may spread over the area of injection and the presence of trismus that limits the desired mouth opening. In such clinical situations, VA method can prove to be a better alternative [7]. We have been using VA technique since more than 6 years in our practice, and we did not find any complications so far, whereas, not often, but in SIANB, trismus and haematoma have been witnessed post-injection.
Fig. 3.

A schematic diagram showing the relationship of the main branches of the mandibular nerve and the relationship of the needle during injection
Table 6.
Various advantages of closed mouth method
| Advantages of Vazirani–Akinosi closed mouth technique | |
|---|---|
|
1. Relatively less patient apprehension 2. Relatively painless 3. Single injection blocks buccal & lingual nerves as well 4. Easy to perform 5. Complications are less likely 6. Very useful in trismus condition |
According to the findings of Akinosi, the LA effect initiated at about 40 s after injection and surgical anaesthesia was obtained in about 90 s with closed mouth technique [7]. Fanyuan Yu in a meta-analysis reported that VA technique has a more rapid onset time than SIANB technique [8]. In a recent study by Sarat et al. [9], it was reported that the difference in mean time of onset between VA and SIANB techniques was 15 s that was statistically not significant and the mean value for VA technique was 192.86 ± 61.20 s, while for SIANB technique it was 177.43 ± 59.94 s. In the present study, although the difference in onset of anaesthetic effect was 25.86 s, it was found to be statistically significant. That VA technique has a relatively delayed onset is an intriguing portray in this comparative study and is in accordance with the study reported by Donkor et al. [10]. This is contrary to the antecedent findings reported in the literature that VA technique has a rapid onset of action compared to SIANB [7, 11]. The difference in onset of two techniques in this study can be explained by the fact that the onset of anaesthesia for a nerve block is influenced by the proximity at which the LA solution is deposited. In other words, the more closer the solution deposited to the nerve, the more faster is the onset of anaesthesia [12]. VA technique is a “blind” method for blocking the inferior alveolar nerve due to non-existence of bony endpoints, and the solution is deposited into the soft tissues medial to the ramus [13]; while the exact point of deposition is hard to find, hence at times LA solution may get deposited at a distance more away from the nerve. The depth of penetration in VA technique is about half the width of the ramus that is approximately 25 mm in adults; however, a variation to the anatomy of ramus may exist among different individuals [1, 13, 14]. In Halstead technique due to the utilization of the bony landmark as a reference, it is workable to deliver the LA agent in close proximity to the IAN, and hence, it has a more rapid onset of anaesthesia when compared to VA technique.
VA technique has a lower incidence of positive aspiration (< 10%) when compared to the SIANB which is about 10–15%. SIANB is considered to be having the highest rate of positive aspiration when compared with other intraoral nerve blocks [1, 5]. The incidence of positive aspiration with VA has been reported to be 1.43% by Sarat et al. [9]. We found positive aspiration to be 1.43% which is similar to the finding of Sarat et al. According to the meta-analysis by Yu et al., there is no statistical difference in success rate between VA and SIANB techniques; however, Sarat et al. reported the success rate to be more for VA technique (95.71%) than SIANB technique (92.86%) [8, 9]. Aggrawal et al. [15] reported no statistical significant difference in success rate between SIANB (36%) and VA (41%) techniques. Akinosi reported success rate for closed mouth technique to be 86% with single injection and 96% when a second injection was repeated. The success rate reported by Sarat et al. [9] is 95.71% with single injection. In our study, we achieved a success rate of 97.14% with VA technique, while for Halstead technique it was 81.42% with single injection and the difference was highly significant. Goldberg et al. [16] reported the success rate of 13–50% and comparatively late onset for VA technique in vital, asymptomatic teeth and found no significant difference in success rate between VA and SIANB methods. Aggrawal et al. [15] reported a success rate of 41% for VA method and 36% for SIANB in patients with irreversible pulpitis with no statistically significant difference. Yu et al. [8] in a meta-analysis found that VA method has a faster onset of action than SIANB with significantly lower incidence of positive aspiration, and there was no significant difference in success rate between these two techniques.
The limitations of VA technique cannot be overlooked. When the maxillary tuberosity is deformed or any tumour exists in the area of insertion of needle, it is inconvenient to perform VA method. If the teeth in the maxillary arch are missing, particularly the posterior teeth, then this method becomes difficult to perform. However, this can be managed by utilizing the alveolar ridge as a reference instead of gingival margin. This method is not reliable in paediatric patients [1, 5, 7].
The facts unique to the present study are summarized as follows:
There is no difference in pain on injection between VA and SIANB methods. Both the techniques are well tolerated by the patients.
This study reveals that the time of onset of anaesthesia with VA method is longer than SIANB, whereas most of the other studies in literature reported VA method to have a faster onset comparatively.
The success rate achieved in this study was 97.14% with single injection for VA with highly significant difference when compared to the success rate of SIANB (81.42%).
The incidence of positive aspiration in VA technique (1.43%) is incredibly low when compared to that of SIANB (15.71%).
Conclusion
VA technique provides desirable surgical anaesthesia with relatively high success rate and lower incidence of positive aspiration and can be considered as a boon for oral and maxillofacial surgeons. The technique is much easier to learn as well as to implement in routine practice and should be adopted by all dental practitioners to successfully provide profound anaesthesia in patients where even repeated injections of standard IANB are unsuccessful such as in the case of anatomic variation. The authors strongly recommend teaching the dental students Vazirani–Akinosi technique, so that they get acquainted with and utilize this method in their future practice.
Acknowledgement
I am thankful to Dr. Sneha Jadhav, Dr. Alfiya Halde and Dr. Sanika Kadam for their assistance in photography and sketching the schematic diagram. I would also like to acknowledge my teachers Dr Syed Ahmed, Dr Sheeraz Badal and Dr Amol Doiphode who have influenced and made me to stand where I am today.
Compliance with Ethical Standards
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in this study (involving human participants) were in accordance with the ethical standards of the institutional research committee and with the 1964 Declaration of Helsinki and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Footnotes
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
References
- 1.Malamed SF. Handbook of local anesthesia. 6. St. Louis: Mosby; 2013. [Google Scholar]
- 2.Calatayud J, Gonzalez A. History of the development and evolution of local anesthesia since the coca leaf. Anesthesiology. 2003;98(6):1503–1508. doi: 10.1097/00000542-200306000-00031. [DOI] [PubMed] [Google Scholar]
- 3.McLure HA, Rubin AP. Review of local anaesthetic agents. Min Anestesiol. 2005;71(3):59–74. [PubMed] [Google Scholar]
- 4.Haas DA. Alternative mandibular nerve block techniques. A review of the Gow-Gates and Akinosi–Vazirani closed-mouth mandibular nerve block techniques. J Am Dent Assoc. 2011;142(9 suppl):8S–12S. doi: 10.14219/jada.archive.2011.0341. [DOI] [PubMed] [Google Scholar]
- 5.Bennett CR. Monheim’s local anesthesia and pain control in dental practice. 7. Hamilton: B.C. Decker; 1990. [Google Scholar]
- 6.Peterson JK. The mandibular foramen block. A radiographic study of the spread of local analgesic solution. Br J Oral Surg. 1971;9(21):126–138. doi: 10.1016/S0007-117X(71)80060-4. [DOI] [PubMed] [Google Scholar]
- 7.Akinosi JO. A new approach to the mandibular nerve block. Br J Oral Surg. 1977;15(1):83–87. doi: 10.1016/0007-117X(77)90011-7. [DOI] [PubMed] [Google Scholar]
- 8.Yu F, Xiao Y, Liu H, Wu F, Lou F, Chen D, Bai M, Huang D, Wang C, Ye L. Evaluation of three block anesthesia methods for pain management during mandibular third molar extraction: a meta-analysis. Sci Rep. 2017;20(7):40987. doi: 10.1038/srep40987. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Sarat RK, Kashyap VM, Uppada UK, Tiwari P, Mishra A, Sachdeva A. Comparison of efficacy of Halstead, Vazirani Akinosi and Gow Gates techniques for mandibular anesthesia. J Maxillofac Oral Surg. 2018;17(4):570–575. doi: 10.1007/s12663-018-1092-5. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Donkor P, Wong J, Punnia-Moorthy A. An evaluation of the closed mouth mandibular block technique. Int J Oral Maxillofac Surg. 1990;19(4):216–219. doi: 10.1016/S0901-5027(05)80395-9. [DOI] [PubMed] [Google Scholar]
- 11.Mishra S, Tripathy R, Sabhlok S, Panda PK, Patnaik S. Comparative analysis between direct Conventional Mandibular nerve block and Vazirani–Akinosi closed mouth Mandibular nerve block technique. Int J Adv Res Technol. 2012;1(6):112–117. [Google Scholar]
- 12.Haas DA. An update on local anesthetics in dentistry. J Can Dent Assoc. 2002;68(9):546–551. [PubMed] [Google Scholar]
- 13.Reed KL, Malamed SF, Fonner AM. Local anesthesia part 2: technical considerations. Anesth Prog. 2012;59(3):127–137. doi: 10.2344/0003-3006-59.3.127. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Khoury J, Townsend G. Neural blockade anaesthesia of the mandibular nerve and its terminal branches: rationale for different anaesthetic techniques including their advantages and disadvantages. Anesthesiol Res Pract. 2011;2011:307423. doi: 10.1155/2011/307423. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Aggarwal V, Singla M, Kabi D. Comparative evaluation of anesthetic efficacy of Gow-Gates mandibular conduction anesthesia, Vazirani–Akinosi technique, buccal-plus- lingual infiltrations, and conventional inferior alveolar nerve anesthesia in patients with irreversible pulpitis. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2010;109(2):303–308. doi: 10.1016/j.tripleo.2009.09.016. [DOI] [PubMed] [Google Scholar]
- 16.Goldberg S, Reader A, Drum M, Nusstein J, Beck M. Comparison of the anesthetic efficacy of the conventional inferior alveolar, Gow-Gates, and Vazirani–Akinosi techniques. J Endod. 2008;34(11):1306–1311. doi: 10.1016/j.joen.2008.07.025. [DOI] [PubMed] [Google Scholar]


