Abstract
Objective:
Numerous researchers have suggested that certain coping styles (e.g., maladaptive cognitive coping strategies) interfere with recovery from traumatic experiences and contribute to the onset/maintenance of post-traumatic stress disorder (PTSD). Further, given that individuals with PTSD have a high rate of smoking (e.g., Mahaffey et al., 2016) and that maladaptive coping strategies in general are associated with lower smoking quit rates, it is possible that use of maladaptive cognitive coping strategies are particularly problematic for the recovery of smokers with PTSD. The present study examined whether specific cognitive coping strategies are associated with poorer outcome among smokers with PTSD following an integrated treatment for both disorders.
Method:
Patients with chronic PTSD and nicotine dependence (N = 142) received up to twelve sessions of smoking cessation counseling combined with varenicline (VARCC) or integrated prolonged exposure therapy and VARCC (PE+VARCC). We hypothesized that greater maladaptive, and lower adaptive, cognitive coping strategies at baseline would moderate degree of improvement in smoking and PTSD outcomes through to follow-up.
Results:
Multilevel modeling revealed that neither maladaptive or adaptive cognitive coping strategies moderated smoking abstinence outcomes over the course of the study (p-values ≥ .271). However, greater use of catastrophizing and lower use of positive reappraisal at baseline were associated with less improvement in the hyperarousal PTSD symptom cluster over the course of the study (p values ≤ .01).
Conclusions:
These findings suggest that maladaptive cognitive coping strategies are not necessarily a contraindication for overall outcomes in integrated PTSD and smoking treatment, although they may influence improvement in hyperarousal symptoms.
Keywords: cognitive coping, PTSD, smoking cessation, treatment outcome, moderators
Posttraumatic stress disorder (PTSD) is a debilitating disorder that develops in some individuals following exposure to traumatic events, with maladaptive coping strategies, being associated with PTSD symptoms (e.g., Ehring & Quack, 2010; Weiss, Tull, Anestis, & Gratz, 2013). Cognitive coping refers to mental strategies an individual uses to cope with having experienced a traumatic experience (Garnefski, Kraaij, & Spinhoven, 2001). In the case of PTSD specifically, a small but growing body of literature suggests that maladaptive ways of cognitively coping with a trauma (e.g., rumination, self-punishment) are associated with greater PTSD severity (e.g., Michael, Halligan, Clark, & Ehlers, 2007; Pietrzak, Harpaz-Rotem, & Southwick, 2011). Alternatively, greater use of adaptive cognitive coping strategies (such as cognitive reappraisal) has been shown to be associated with less severe PTSD symptoms in veterans (Boden, Bonn-Miller, Kashdan, Alvarez, & Gross, 2012). Another study examining cognitive coping strategies in a large sample of recently returning veterans with PTSD further found that greater baseline use of catastrophizing was significantly associated with greater symptoms on all the PTSD symptom clusters including intrusive thoughts, avoidance, negative alterations in cognitions/mood, and hyperarousal (Kaczkurkin et al., 2017).
However, all of these aforementioned studies examining the relationship between cognitive coping techniques and PTSD constructs have been cross-sectional in nature. Other studies examining a mix of cross-sectional and longitudinal data have found cognitive coping strategies to be associated with other variables of interest such as work potential following an accidental injury (Matthews, Harris, & Cumming, 2009), more chronic pain following physical injury (e.g., Carty, O’Donnell, Evans, Kazantzis, & Creamer, 2011), and greater incidence of PTSD following a terrorist attack (e.g., Jenness et al., 2016). To our knowledge, only one study has examined how the constructs of cognitive coping strategies and PTSD symptoms relate to each other within the context of a treatment-seeking sample of individuals with PTSD over the course of treatment (Wisco, Sloan, & Marx, 2013). This study was conducted in a sample of motor vehicular accident survivors and found no association between initial maladaptive cognitive coping strategies and changes in PTSD following written exposure-based treatment. Further, Wisco and colleagues (2013) also found that higher pre-treatment levels of positive reappraisal (an adaptive cognitive coping strategy) were actually associated with lower reductions in PTSD following treatment with written exposure therapy (WET), suggesting that the presence of more adaptive cognitive coping repertoires at the start of treatment do not necessarily translate into better PTSD treatment outcomes. This study used the Cognitive Emotion Regulation Questionnaire (CERQ; Garnefski et al., 2001), which specifically examines 9 different adaptive and maladaptive cognitive strategies employed by individuals who have experienced a traumatic event to better understand the cognitive coping techniques of trauma-exposed individuals, regardless of their behavioral coping approaches. Taken together, it appears that cognitive coping techniques seem to have an association with PTSD symptom severity and related secondary constructs, but it is unclear whether these cognitive coping repertoires are appreciably related to actual outcomes following a course of treatment for PTSD.
Even less is known about how maladaptive cognitive coping strategies are associated with nicotine dependence symptoms. There has been substantial investigation into the relationship between distress intolerance (which shares some overlap with cognitive coping) and smoking (e.g., Trujillo et al., 2017). However, literature specifically examining the construct of cognitive coping and its impact on smoking behaviors is lacking. This is an important consideration because notably, PTSD and nicotine dependence frequently co-occur, with rates of smoking in those with PTSD being disproportionately high compared to that of the general population (44.6% vs. 22.5%; Mahaffey et al., 2016). Further, compared to smokers without PTSD, smokers with PTSD smoke more heavily, demonstrate greater nicotine dependence (ND), and are less likely to quit successfully (Feldner, Babson, & Zvolensky, 2007; Lasser et al., 2000; Malte et al., 2015). Thus, this group carries a particularly high health burden, and warrants further examination into how cognitive coping strategies may interact with both smoking and PTSD symptoms.
Consequently, it is possible that patients with this particular comorbidity demonstrate different relationships between their ability to adaptively cope on a cognitive level and PTSD symptoms than patients with either disorder alone. For instance, relative to smokers without PTSD, smokers with PTSD report greater motivation to smoke as a means of reducing negative affect, as well as stronger cognitive beliefs that smoking is an effective method to regulate emotions (Calhoun, Levin, Dedert, Johnson, & Beckham, 2011; Mahaffey et al., 2016; Marshall et al., 2008). Further, it has been suggested that smokers with PTSD may lack more adaptive coping strategies overall, therefore utilize smoking to cope with high levels of distress (Calhoun et al., 2011). More specifically, a recent study concluded that the observed relationship between PTSD and heightened levels of nicotine dependence and problems experienced during quit attempts may, in part, be accounted for by the belief that smoking will reduce negative mood states and by the related desire among smokers with PTSD in particular to reduce negative affect (Mahaffey et al., 2016). This desire to reduce, rather than tolerate, negative affect may constitute a contraindication to confronting traumatic memories in the context of trauma-focused treatment for PTSD such as prolonged exposure (PE) therapy (Wolfsdorf & Zlotnick, 2001), especially among smokers with PTSD. Further, more frequent use of specific maladaptive cognitive coping skills (i.e., suppression) has been found to be associated with enhanced smoking urges (Szasz, Szentagotai, & Hofmann, 2012). Conversely, more frequent use of adaptive cognitive coping strategies (i.e., reappraisal) has been found to be associated with reduced cravings to smoke, fewer depressive symptoms, and greater positive mood (Wu et al., 2015; see also Fucito, Juliano, & Toll, 2010).
The aim of the current study was to investigate cognitive coping strategies in a sample of cigarette smokers with chronic PTSD undergoing PTSD and/or smoking cessation treatment. Given the general lack of research examining cognitive coping strategies in PTSD and smoking treatment outcomes, we tested two independent hypotheses. First, we hypothesized that concurrent PTSD/smoking cessation treatment would result in greater reductions in maladaptive cognitive coping strategies (rumination, catastrophizing, self-blame, and other-blame) and increases in adaptive cognitive coping strategies (acceptance, positive refocusing, refocusing on planning, positive reappraisal, and putting in perspective) than smoking cessation alone. Second, we hypothesized that more frequent use of maladaptive cognitive coping strategies (e.g., rumination, catastrophizing, self-blame, and other-blame) at baseline would result in poorer treatment outcomes in both smoking abstinence and PTSD symptoms. Finally, we predicted that more frequent use of adaptive cognitive coping strategies at baseline would result in better smoking abstinence and PTSD symptom outcomes.
Method
Participants
Participants included 142 male and female cigarette smokers with chronic PTSD who sought treatment at the Center for the Treatment and Study of Anxiety and the Philadelphia Veterans Affairs to improve their PTSD symptoms and to quit smoking. Baseline participant demographics are presented in Table 1 and information on types of trauma exposure in sample are in the Supplementary materials. There were no differences between treatment groups on demographic variables at baseline. Inclusion criteria were (1) smoking 10 or more cigarettes per day in the past year, (2) current PTSD diagnosis according to the Diagnostic and Statistical Manual of Mental Disorders (4th ed., text rev.; DSM-IV-TR; American Psychiatric Association, 2000), and (3) trauma-related symptoms deemed to be clinically significant, indicated by a score of at least 15 on the PTSD Symptom Severity Interview (PSSI-I; Foa, Riggs, Dancu, & Rothbaum, 1993), which corresponds to mild PTSD. Exclusion criteria included (1) history of drug or alcohol abuse or dependence in the prior 3 months, (2) unwillingness to stop marijuana use or to refrain from nicotine replacement therapy (e.g., the patch) over course of active treatment phase, (3) currently ongoing intimate partner violence, (4) suicidal ideation, (5) history of psychosis or bipolar disorder, (6) significant cardiovascular or hypertensive disease, and (7) pregnancy or nursing. For more details about participant enrollment, compliance to study procedures and training of evaluators on primary measures of interest, please refer to the main outcome study for this trial (Foa et al., 2017).
Table 1.
Sociodemographic characteristics of the participants
| Variable | VARCC+PE (n=72) |
VARCC (n=70) |
|---|---|---|
| Age in years, mean (SD) | 42.83 (9.70) | 42.59 (10.18) |
| Gender (%) | ||
| Male | 63.9 | 57.1 |
| Female | 36.1 | 42.9 |
| Ethnicity (%) | ||
| Not Hispanic | 95.8 | 87.1 |
| Hispanic | 4.2 | 10.0 |
| Missing | 0.0 | 2.9 |
| Race (%) | ||
| African American/Black | 77.8 | 70.0 |
| White | 20.8 | 24.3 |
| Asian | 0.0 | 0.0 |
| American Indian or Alaska Native | 1.4 | 2.8 |
| Missing | 0.0 | 2.9 |
| Education (%) | ||
| Grade school | 1.4 | 0.0 |
| Some high school | 15.3 | 10.0 |
| High school graduate or GED | 33.3 | 38.6 |
| Some college or technical school | 37.5 | 37.1 |
| College graduate or beyond | 12.5 | 11.4 |
| Missing | 0.0 | 2.9 |
Note. VARCC = Varenicline + smoking cessation counseling; PE = Prolonged Exposure.
Procedure
After providing written informed consent, participants completed an intake evaluation to determine eligibility. Eligible participants were randomized into either: (1) varenicline, smoking cessation counseling, and PE (VARCC+PE), or (2) varenicline and smoking cessation counseling only (VARCC). All participants then completed 12 weekly visits. At each visit, participants met with the study nurse to receive medication, and to monitor health status and medication compliance. Participants in the VARCC+PE group also received PE and smoking cessation counseling at each visit, both conducted by doctoral-level clinical psychologists. Participants in the VARCC group received only smoking cessation counseling at each visit. Assessments were conducted at baseline, post-treatment, and three months after treatment completion by doctoral-level independent evaluators who were blind to treatment assignment. Participants also completed self-report measures at these assessment points. All study procedures were approved by the institutional review board at University of Pennsylvania. For further details about the study, please refer to the main outcome study for this trial (Foa et al., 2017).
Treatments
Varenicline.
Varenicline (Chantix) is an FDA-approved medication that can be used to help people to successfully quit smoking. All participants received medication throughout the 12 weekly visits.
Smoking Cessation Counseling.
Smoking cessation counseling followed the medical management model used in Project COMBINE (Anton et al., 2006). Main components included motivational interviewing, monitoring progress, providing encouragement, reinforcing abstinence, and problem solving, and was administered to all participants at each of the 12 weekly visits for 20–30 minutes.
Integrated Prolonged Exposure (PE) with Smoking Cessation Counseling.
Participants in the VARCC+PE group received an integrated protocol which consisted of 20–30 minutes of smoking cessation counseling (identical to the VARCC only group), followed by 90 minutes of PE (Foa, Hembree, & Rothbaum, 2007) at each visit. The two main components of PE are: (1) imaginal exposure, which consists of revisiting and recounting aloud the most upsetting traumatic memory, followed by processing the revisiting experience with the therapist, and (2) gradual in vivo exposures to objectively safe but avoided trauma reminders. Treatment was delivered for a total of 12 weekly 110–120 minute long sessions. For further details on all treatments, please refer to the main outcome study for this trial (Foa et al., 2017).
Measures
Cognitive Emotion Regulation Questionnaire (CERQ; Garnefski, et al., 2001).
The CERQ is a 36-item self-report measure designed to assess the cognitive strategies that are used to cope after experiencing a negative life event. It consists of nine conceptually distinct scales, each comprised of four items, including: 1) Self-blame (e.g., “I think that basically the cause must lie within myself”), 2) Acceptance (e.g., “I think that I have to accept that this has happened”), 3) Rumination (e.g., “I dwell upon the feelings the situation has evoked in me”), 4) Positive Refocusing (e.g., “I think of something nice instead of what has happened”), 5) Refocus on Planning (e.g., “I think about how I can best cope with the situation”), 6) Positive Reappraisal (e.g., “I think I can learn something from the situation”), 7) Putting into Perspective (e.g., “I think that it all could have been much worse”), 8) Catastrophizing (e.g., “I continually think how horrible the situation has been”), and 9) Other-blame (e.g., “I feel that others are responsible for what has happened”). Each item is rated on a 5-point Likert scale from 1, “(almost) never,” to 5, “(almost) always.” In the current sample, each CERQ subscale individually demonstrated good to very good internal consistency across timepoints (Cronbach’s α = .75-.83).
PTSD Symptom Scale, Interview Version (PSS-I; Foa et al., 1993).
The PSS-I is a 17-item clinical interview that assesses DSM-IV PTSD symptoms occurring in the prior two weeks on a frequency/severity scale. The first five items assess the re-experiencing symptom cluster (e.g., “Have you had recurrent or intrusive distressing thoughts or recollections about the trauma?”). The next seven items assess the avoidance and numbing symptom cluster (e.g., “Have you persistently been making efforts to avoid activities, situations, or places that remind you of the trauma?” and “Do you feel less able to have positive feelings?”). And the last five items assess the increased arousal symptom cluster (e.g. “Are you overly alert since the trauma?”). Total scores range from 0 to 51, with higher scores demonstrating more severe PTSD symptoms. The PSS-I has been shown to have excellent internal consistency (Cronbach’s α = .90) and very good one-month test-retest reliability (r = .80). In the current study, the PSS-I demonstrated good to excellent internal consistency (Cronbach’s α = .66-.93) across assessments.
Smoking Abstinence.
The Timeline Follow Back Interview (TLFB) was used in conjunction with measured serum cotinine and exhaled carbon monoxide to assess smoking status. The TLFB utilizes a calendar method to assess when and how many cigarettes each participant smoked over the past 30 days. A dichotomous smoking outcome was calculated using the seven-day point prevalence abstinence (PPA), which was defined as self-reported abstinence for the seven days on the TLFB, in addition to threshold levels of the serum cotinine (<15 ng/ml) and carbon monoxide (<10 ppm).
Data Analysis
Multilevel modeling was used to test the hypotheses of this study. All variables were collected at three time points (pre-treatment, post-treatment, and 3-months follow-up). Data analyses were conducted using the IBM SPSS Statistics program (version 24) with the procedures outlined in Heck, Thomas, and Tabata (2014; 2012). Measures of interest included PPA, PTSD symptoms, and the CERQ subscales. Because PPA was binary, we used a generalized linear mixed model (GLMM) analysis with a logistic link function. PTSD symptoms and the CERQ subscales were analyzed with a general linear mixed model. PTSD outcomes included the three clusters of re-experiencing, avoidance/numbing, and arousal as measured by the PSS-I. Each CERQ subscale (Self-blame, Acceptance, Rumination, Positive Refocusing, Refocus on Planning, Positive Reappraisal, Putting into Perspective, Catastrophizing, and Other-blame) was individually tested for change over the course of treatment and as a moderator of PTSD or smoking outcomes. No item-level data was missing in the sample. In this study, 18 patients dropped out of treatment and 17 were lost to follow-up. As multilevel modeling is robust to missing data due to dropouts, all analyses were intent-to-treat and included both completers and dropouts. Prior to analyzing our hypotheses, model fitting was conducted as described in detail in the supplementary materials.
First, we examined the correlations between the CERQ subscales and the PTSD symptom clusters at baseline. We then examined change in the CERQ subscales over the course of treatment. We next used GLMM with a logistic link function to examine whether baseline levels of each CERQ subscale moderated change over time in PPA. We used linear mixed models to test whether the baseline CERQ subscales moderated change in each of the three PSS-I clusters of re-experiencing, avoidance/numbing, and arousal. Finally, we tested whether any of the moderating effects differed by treatment group (VARCC+PE vs. VARCC).
Results
Relevant information from the main outcome of this trial
Overall, main outcomes of this trial identified VARCC+PE as enhancing smoking cessation compared to VARCC only for participants with moderate or severe PTSD symptom severity, but not for participants with low baseline PTSD severity. Additionally, participants who received PE demonstrated significantly greater reductions in PTSD and depression symptoms compared to those who did not receive PE (Foa et al., 2017).
Association between CERQ subscales and PTSD outcomes
We first examined the correlations between the CERQ subscales and the PTSD symptom clusters at baseline (see Supplementary Table 1). PSS-I re-experiencing symptoms were associated with greater Self-blame, Rumination, and Other-blame (p-values ≤ .045). Avoidance symptoms as measured by the PSS-I were associated with less Refocus on Planning and Positive Reappraisal, and greater Catastrophizing (p-values ≤ .024). PSS-I hyperarousal symptoms were not significantly associated with any of the CERQ subscales (p-values ≥ .063).
Change in CERQ subscales with treatment
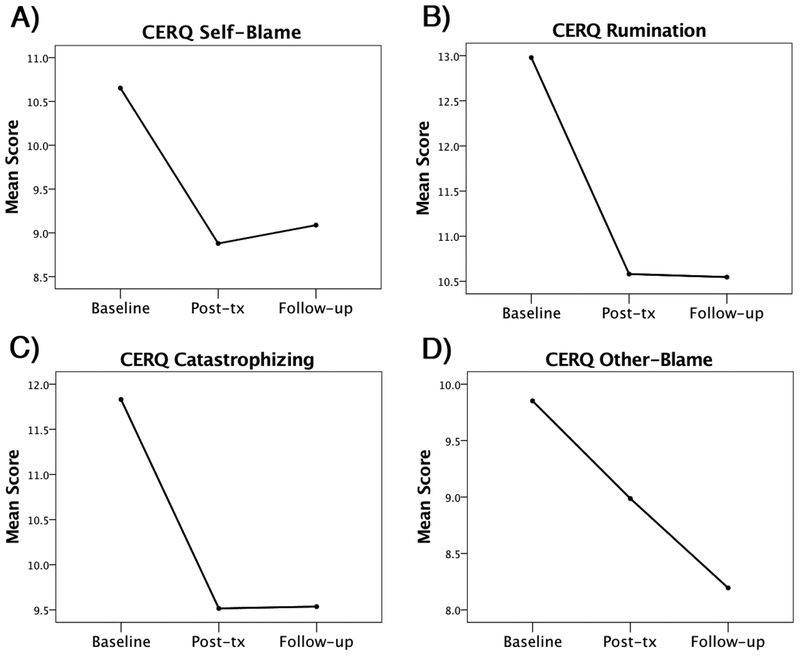
We next examined change in the CERQ subscales over the course of treatment. Self-blame decreased significantly from baseline to post-treatment (B = −2.49, SE = .57, t(135.60) = −4.37, p < .001), and remained fairly stable at follow-up (Figure 1a). Likewise, Rumination (B = −4.26, SE = .56, t(334.64) = −7.68, p < .001; Figure 1b) and Catastrophizing (B = −3.62, SE = .56, t(132.89) = −6.47, p < .001; Figure 1c) both decreased significantly, which was maintained at follow-up. Other-blame significantly decreased in a much more linear fashion from baseline through follow-up (B = −.85, SE = .19, t(153.66) = −4.42, p < .001; Figure 1d). No significant change over time was found for any of the positive coping strategies, specifically, Acceptance, Positive Refocusing, Refocus on Planning, Positive Reappraisal, or Putting into Perspective (p-values ≥ .143). Change in scores over time did not differ between the treatment groups for any of the CERQ subscales (p-values ≥ .264). See Supplementary Table 2 for means and standard deviations by group for all measures at the three timepoints.
Figure 1.
Reduction in CERQ subscales over the course of treatment. CERQ Self-blame (1a), Rumination (1b), and Catastrophizing (1c) significantly decreased from baseline to post-treatment, which remained stable at follow-up. CERQ Other-blame (1d) significantly decreased in linear fashion from baseline through follow-up. CERQ = Cognitive Emotion Regulation Questionnaire; tx = treatment.
CERQ subscales as moderators of smoking abstinence
We were also interested in whether baseline CERQ scores affected treatment outcomes. To test this, we examined the baseline CERQ subscales as moderators of change in smoking abstinence outcomes over time. Smoking abstinence increased significantly from baseline to post-treatment for all participants (B = 4.03, SE = .38, t(387) = 10.71, p < .001). However, the CERQ subscales did not significantly moderate smoking outcomes (p-values ≥ .271). In addition, the three-way interactions (time x CERQ subscale x treatment group) were not significant (p-values ≥ .05), indicating that the results did not differ based on treatment condition.
CERQ subscales as moderators of change in PTSD symptoms
We then tested whether baseline CERQ subscale scores moderated the reduction in the PSS-I clusters of re-experiencing, avoidance/numbing, and hyperarousal over time. PSS-I symptoms decreased significantly from baseline to post-treatment for all participants, including total (B = −21.65, SE = 1.41, t(127.31) = −15.32, p < .001), re-experiencing (B = −6.44, SE = .49, t(133.66) = −13.24, p < .001), avoidance/numbing (B = −8.49, SE = .69, t(128.76) = −12.39, p < .001), and hyperarousal scores (B = −7.26, SE = .53, t(129.11) = −13.58, p < .001).
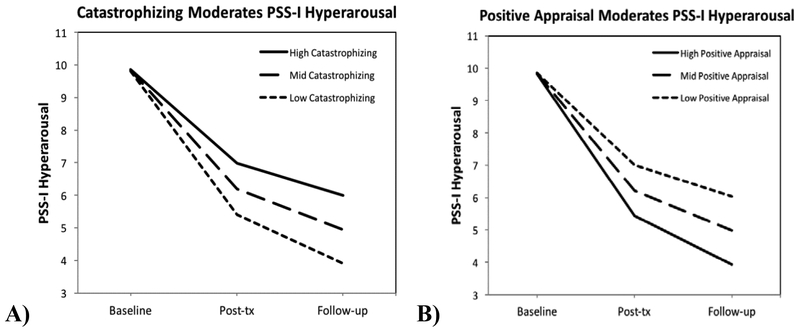
Of the CERQ subscales, the results showed that Catastrophizing at baseline significantly moderated the reduction in PSS-I hyperarousal scores (B = .37, SE = .13, t(128.88) = 2.95, p = .004). Plotting the results shows that those with higher scores on Catastrophizing showed less improvement by follow-up in PTSD hyperarousal symptoms than those with lower Catastrophizing scores (see Figure 2a). When time was centered at baseline, the relationship between Catastrophizing and PSS-I hyperarousal scores was not significant (p = .913); however, this relationship became significant by post-treatment (B = .19, SE = .07, t(135.38) = 2.72, p = .007) and remained significant at follow-up (B = .26, SE = .09, t(131.44) = 2.95, p = .004). The moderating effect of Catastrophizing did not depend on treatment condition as the three-way interaction between time, Catastrophizing, and treatment group was not significant (p = .741).
Figure 2.
Moderation of PSS-I hyperarousal symptoms. Catastrophizing (2a) moderates PSS-I hyperarousal symptoms, such that higher levels of CERQ Catastrophizing were associated with less improvement in PTSD hyperarousal symptoms, as measured by the PSS-I, compared to lower levels of Catastrophizing. Positive Reappraisal (2b) also moderates PSS-I hyperarousal symptoms, such that lower levels of CERQ Positive Reappraisal were associated with less improvement in PTSD hyperarousal symptoms, as measured by the PSS-I, compared to higher levels of Positive Reappraisal. PSS-I = PTSD Symptom Scale Interview; CERQ = Cognitive Emotion Regulation Questionnaire; tx = treatment.
Positive Reappraisal also significantly moderated the reduction in PSS-I hyperarousal scores (B = −.35, SE = .11, t(127.25) = −3.07, p = .003). Specifically, those with lower scores on Positive Reappraisal showed less improvement in PTSD hyperarousal symptoms (Figure 2b). At baseline, the relationship between Positive Reappraisal and PSS-I hyperarousal scores was not significant (p = .958), but this relationship was significant at post-treatment (B = −.18, SE = .06, t(131.90) = −2.80, p = .006) and follow-up (B = −.24, SE = .08, t(129.11) = −3.06, p = .003). The moderating effect of Positive Reappraisal did not differ based on treatment condition (p = .463). The other CERQ subscales showed no significant moderating effects (p-values ≥ .087).
Discussion
The current study aimed to elucidate the relationship between cognitive coping strategies and treatment outcomes in a sample of smokers with PTSD. First, we found that each of the maladaptive cognitive coping strategies on the CERQ declined over the course of treatment. However, contrary to our hypotheses, adaptive cognitive coping strategies did not significantly change over time. These findings are somewhat in line with previous findings showing that presence of more adaptive cognitive coping strategies at the start of treatment were unrelated to better PTSD treatment outcomes (Wisco et al., 2013), but it was surprising nonetheless that the use of these strategies after a course of successful treatment of smoking and PTSD did not increase. In terms of smoking outcomes, cognitive coping strategies at baseline did not seem to influence improvement in smoking abstinence, PTSD re-experiencing or PTSD avoidance/numbing symptoms over the course of treatment in our sample of smokers with PTSD, contrary to our expectations. However, study results indicated that individuals (regardless of condition) with greater use of catastrophizing strategies and less use of positive reappraisal strategies had worse trajectories of change in PTSD hyperarousal symptoms in particular.
To our knowledge, this study is the first to examine the impact of cognitive coping strategies on smoking and PTSD treatment outcomes in a sample of smokers with PTSD, who have been previously found to have elevated levels of PTSD and nicotine dependence due to maladaptive coping strategies and beliefs (e.g., Calhoun et al., 2011; Pietrzak et al., 2011). The findings are highly relevant from a clinical perspective, as they suggest that smokers with PTSD benefit from both exposure-based PTSD treatment with smoking cessation and smoking cessation only in terms of smoking outcomes, regardless of their cognitive coping repertoires.
Notably, there is scant previous examination of the influence of cognitive coping strategies on smoking outcomes, and the current study did not indicate a particular association with such cognitive processes and nicotine abstinence over the course of treatment. This lack of association may indicate that, similar to findings of other coping strategies (such as use of emotion regulation skills in smokers), that cognitive coping approaches (particularly maladaptive ones) do not have an amplifying effect on psychopathology, but rather may be considered one of many indicators of psychological health (Farris, Zvolensky, & Schmidt, 2016). This view may explain the discrepancy between the current findings and those from the smoking literature suggesting a strong link between maladaptive beliefs and smoking behavior (e.g., Szasz et al., 2012; Mahaffey et al., 2016; Marshall et al., 2008). In other words, once psychopathology (in this case, PTSD) is taken into consideration, maladaptive cognitive coping strategies may not confer any additional vulnerability to poor smoking outcomes.
Relatedly, the finding that cognitive coping strategy use did not impact re-experiencing or avoidance/numbing PTSD symptom outcomes is consistent with the only one previous study examining these cognitive approaches within the context of exposure therapy for PTSD (Wisco et al., 2013), which examined associations between cognitive coping strategies and overall PTSD severity, although not individual symptom clusters. That is, even though we found that greater use of catastrophizing and lower use of positive appraisal impeded improvement in hyperarousal symptoms of PTSD, there was no evidence to suggest that either of these strategies were associated with the frequency or intensity of memories related to traumas experienced by patients (i.e., re-experiencing symptoms), or more avoidance of trauma-related triggers or emotional and general emotional responsiveness in patients (i.e., avoidance/numbing symptoms), in either treatment group.
However, this study also showed that smokers with PTSD who have high levels of catastrophizing about their previous traumatic experience (e.g., “I keep thinking about how terrible it is what I have experienced” and “I often think about what I have experienced is the worst that can happen to a person”) tend to experience less reductions in their hyperarousal symptoms. Our previous work with the CERQ in an active military sample of non-smokers with PTSD found catastrophizing to be related to all of the DSM-5 PTSD symptom clusters including intrusive thoughts, avoidance, negative alterations in cognitions/mood, and hyperarousal; however, this study did not examine the moderating effect of cognitive coping strategies on treatment outcomes (Kaczkurkin, et al., 2017). Other studies have extensively and consistently found evidence for an association with CERQ Catastrophizing immediately following a physical injury and higher PTSD symptoms 3 months post-injury (e.g., Carty et al., 2011), but the association of catastrophizing with specific clusters of PTSD was not examined in these PTSD, pain and CERQ studies. Similarly, lower levels of an adaptive cognitive coping strategy, positive reappraisal (e.g., “I think the situation also has its positive sides” and “I think I can learn something from the situation”), were associated with less reductions in hyperarousal symptoms over the course of treatment. This particular finding is in contrast to the Wisco et al., (2013) study which actually found that higher positive reappraisal was associated with poorer PTSD outcome. Importantly, this previous study was conducted in a considerably smaller sample (n = 40) of individuals with a homogenous index trauma (motor vehicular accident). The current study employed a considerably larger, more diverse comorbid PTSD/smoking sample.
Rather, the two findings regarding catastrophizing and positive reappraisal in this sample make intuitive sense given that positive reappraisal is conceptually the inverse of catastrophizing; cognitive approaches to PTSD treatment are well-supported and often focus on reframing one’s catastrophic beliefs about a trauma to more adaptive interpretations, using techniques such as positive reappraisal (Ehlers & Clark, 2008). Further, given the significant literature implicating negative cognitive beliefs/interpretations in the maintenance of both smoking (e.g., Mahaffey et al., 2016) and PTSD (e.g., Brown, Belli, Asnaani, & Foa, in press), it is possible that specific cognitive coping strategies are more influential in specific symptoms of PTSD in individuals who smoke (as examined here), rather than in non-smokers with PTSD. The reasons for these findings thus warrant further exploration and replication in other studies using samples with this combined comorbidity.
The current study offers several distinct strengths over previous examinations of cognitive coping strategies and its impact on PTSD. First, this is one of very few studies to examine strength of associations between use of cognitive coping strategies and treatment outcomes over the course of evidence-based treatment for PTSD and smoking. Second, this study examined the unique and important population of smokers with PTSD, who present with particular disability due to this comorbidity, and elucidated how cognitive coping impacts both PTSD and smoking outcomes in this population. Third, this study used robust, objective measures of the constructs of interest for smoking (biologically confirmed PPA) and PTSD (clinician interviews for severity of PTSD), rather than relying only on self-report. Fourth, the study design also allowed us to examine relationships among constructs of interest not only during the course of acute treatment, but also at 3-month follow-up as well, to better understand the longitudinal nature of these relationships.
One drawback of the current study is the use of a self-report measure for cognitive coping strategies; future studies should also consider incorporating objective measures of cognitive coping approaches to better assess how patients’ abilities improve in this domain and how these changes are related to PTSD. In addition, there were limited time-points for assessment in the current study for the CERQ; future studies would benefit from more frequent assessments of the constructs of interest in order to better understand the trajectories of change for individuals with varying levels of maladaptive and adaptive cognitive coping ability. Future work would also benefit from examining whether cognitive coping approaches mediate treatment outcome, which would also be facilitated by more frequent measurement of the constructs of interest. Further, we were not able to examine whether the association between cognitive coping and PTSD reduction was different between smokers and non-smokers. Indeed, while a handful of previous studies have examined the relationship between cognitive coping strategies and PTSD in general (e.g., Kaczkurkin et al., 2017; Boden et al., 2012), these previous studies did not examine subgroups of participants based on smoking status and our study only included smokers. Therefore, future studies might benefit from examining cognitive coping strategies in smokers versus non-smokers with PTSD over the course of treatment. Finally, additional investigation into the current relationships among these constructs using DSM-5 PTSD symptom clusters would be helpful.
These limitations notwithstanding, the present findings can help inform clinicians in their work with smokers who have PTSD. First, the study suggests that treatment with either varenicline and PE or smoking cessation counseling is robust, with smoking outcomes being largely unaffected by use of either maladaptive or adaptive cognitive coping strategies. Second, the findings highlight the utility of assessing PTSD symptom clusters separately when monitoring patients’ progress over the course of treatment, especially among smokers with PTSD. Indeed, a lack of movement in any one symptom cluster may prompt clinicians to examine how treatment is being implemented in order to ensure that patients are approaching situations in a manner that will maximize opportunities for corrective learning. For instance, clinicians may want to assess for the types of beliefs patients may be holding on to, such as beliefs around catastrophic outcomes stemming from their experience of trauma or an inability to positively reappraise what they have experienced, and how these may be maintaining symptoms of hyperarousal such as hypervigilance or sleep disturbances.
Importantly, however, none of these suggestions involve appreciable modifications to existing treatments. Instead, the current findings lend further support to the recommendation that “traditional” PTSD treatment can continue to be routinely offered, even in the context of maladaptive cognitive coping strategies and other complex presentations (De Jongh et al., 2016). In addition, given that the relationships observed among cognitive coping repertoires, smoking and PTSD were similar regardless of whether individuals were receiving just smoking cessation or a combined smoking cessation and trauma-focused treatment, these findings provide support for the ongoing use of the most effective treatment options (such as smoking cessation and PE) for the high number of smokers with comorbid PTSD, and support the continued dissemination of such evidence-based treatments for this population. However, the current findings also suggest that in smokers with PTSD utilizing specific maladaptive or adaptive cognitive coping strategies, particular attention should be paid to hyperarousal symptoms to ensure that these symptoms are adequately targeted over the course of such evidence-based psychosocial treatments, in order to yield the most desirable outcomes for these patients.
Supplementary Material
Clinical Impact Statement.
Maladaptive cognitive coping strategies (e.g., catastrophizing) contribute to the maintenance of both posttraumatic stress disorder (PTSD) and smoking. In the current study, a combination of prolonged exposure (PE) and smoking cessation and smoking cessation alone led to significant reductions in maladaptive cognitive coping. However, participants with greater catastrophizing and less positive reappraisal at baseline showed significantly less improvement in PTSD hyperarousal symptoms across the sample. Thus, while PE and smoking cessation each generally target maladaptive coping strategies, clinicians should pay particular attention to the role of catastrophizing and positive reappraisal in order to bolster treatment outcomes in this comorbid population.
Acknowledgments
This manuscript is based on data previously reported in The Journal of Consulting and Clinical Psychology (doi: 10.1037/ccp0000213). Dr. Edna B. Foa developed Prolonged Exposure, a therapy used in this study. Drs. Asnaani, Kaczkurkin, Jerud and Ms. Fitzgerald report no competing interests. This work was funded by National Institute on Drug Abuse grant awarded to Dr. Edna B. Foa (R01-DA023507–01A1). Dr. Foa receives royalties from the sale of Reclaiming your Life from a Traumatic Experience Workbook and Prolonged Exposure Therapy for PTSD: Emotional Processing of Traumatic Experiences Therapist Guide by Oxford University Press. Dr. Foa also receives payment for training workshops she conducts on Prolonged Exposure therapy.
Dr. Kaczkurkin’s efforts on this manuscript were supported by a Research Supplement to Promote Diversity in Health-Related Research to Dr. Antonia N. Kaczkurkin (NIH grant number: R01MH107703), by a NARSAD Young Investigator Award (ANK), and by a Penn PROMOTES Research on Sex and Gender in Health grant (ANK) awarded through the Building Interdisciplinary Research Careers in Women’s Health (BIRCWH) grant (K12 HD085848) at the University of Pennsylvania.
References
- American Psychiatric Association. (2000). Diagnostic and statistical manual of mental disorders: DSM-IV-TR. Washington, DC: American Psychiatric Association. [Google Scholar]
- Anton RF, O’Malley SS, Ciraulo DA, Cisler RA, Couper D, Donovan DM, & … Zweben A (2006). Combined pharmacotherapies and behavioral interventions for alcohol dependence: The COMBINE study: A randomized controlled trial. Journal of The American Medical Association, 295(17), 2003–2017. doi: 10.1001/jama.295.17.2003 [DOI] [PubMed] [Google Scholar]
- Boden MT, Bonn-Miller MO, Kashdan TB, Alvarez J, & Gross JJ (2012). The interactive effects of emotional clarity and cognitive reappraisal in posttraumatic stress disorder. Journal of Anxiety Disorders, 26(1), 233–238. doi: 10.1016/j.janxdis.2011.11.007 [DOI] [PubMed] [Google Scholar]
- Brown LA, Belli GM, Asnaani A, & Foa EB (in press). A review of the role of negative cognitions about oneself, others, and the world in the treatment of PTSD. Cognitive Therapy and Research. doi: 10.1007/s10608-018-9938-1 [DOI] [Google Scholar]
- Calhoun PS, Levin HF, Dedert EA, Johnson Y, & Beckham JC (2011). The relationship between posttraumatic stress disorder and smoking outcome expectancies among U.S. military veterans who served since September 11, 2001. Journal of Traumatic Stress, 24(3), 303–308. doi: 10.1002/jts.20634 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Carty J, O’Donnell M, Evans L, Kazantzis N, & Creamer M (2011). Predicting posttraumatic stress disorder symptoms and pain intensity following severe injury: The role of catastrophizing. European Journal of Psychotraumatology, 2, 10. doi: 10.3402/ejpt.v2i0.5652 [DOI] [PMC free article] [PubMed] [Google Scholar]
- De Jongh A, Resick PA, Zoellner LA, van Minnen A, Lee CW, Monson CM, & … Bicanic IE (2016). Critical analysis of the current treatment guidelines for Complex PTSD in adults. Depression and Anxiety, 33(5), 359–369. doi: 10.1002/da.22469 [DOI] [PubMed] [Google Scholar]
- Ehlers A, & Clark DM (2008). Post-traumatic stress disorder: The development of effective psychological treatments. Nordic Journal of Psychiatry, 62, 11–18. doi: 10.1080/08039480802315608 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Ehring T, & Quack D (2010). Emotion regulation difficulties in trauma survivors: The role of trauma type and PTSD symptom severity. Behavior Therapy, 41(4), 587–598. doi: 10.1016/j.beth.2010.04.004 [DOI] [PubMed] [Google Scholar]
- Farris SG, Zvolensky MJ, & Schmidt NB (2016). Difficulties with emotion regulation and psychopathology interact to predict early smoking cessation lapse. Cognitive Therapy and Research, 40(3), 357–367. doi: 10.1007/s10608-015-9705-5 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Feldner MT, Babson KA, & Zvolensky MJ (2007). Smoking, traumatic event exposure, and post-traumatic stress: A critical review of the empirical literature. Clinical Psychology Review, 27(1), 14–45. doi: 10.1016/j.cpr.2006.08.004 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Foa EB, Asnaani A, Rosenfield D, Zandberg LJ, Gariti P, & Imms P (2017). Concurrent varenicline and prolonged exposure for patients with nicotine dependence and PTSD: A randomized controlled trial. Journal of Consulting and ClinicalPsychology, 85(9), 862–872. doi: 10.1037/ccp0000213 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Foa EB, Hembree EA, & Rothbaum BO (2007). Prolonged exposure therapy for PTSD: Emotional processing of traumatic experiences: Therapist guide. New York, NY, US: Oxford University Press. doi: 10.1093/med:psych/9780195308501.001.0001 [DOI] [Google Scholar]
- Foa EB, Riggs DS, Dancu CV, & Rothbaum BO (1993). Reliability and validity of a brief instrument for assessing post-traumatic stress disorder. Journal of Traumatic Stress, 6(4), 459–473. doi: 10.1002/jts.2490060405 [DOI] [Google Scholar]
- Fucito LM, Juliano LM, & Toll BA (2010). Cognitive reappraisal and expressive suppression emotion regulation strategies in cigarette smokers. Nicotine & Tobacco Research, 12(11), 1156–1161. doi: 10.1093/ntr/ntq146 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Garnefski N, Kraaij V, & Spinhoven P (2001). Negative life events, cognitive emotion regulation and emotional problems. Personality and Individual Differences, 30(8), 1311–1327. doi: 10.1016/S0191-8869(00)00113-6 [DOI] [Google Scholar]
- Heck RH, Thomas SL, & Tabata LN (2014). Multilevel and longitudinal modeling with IBM SPSS, 2nd ed. New York, NY, US: Routledge/Taylor & Francis Group. [Google Scholar]
- Heck RH, Thomas SL, & Tabata LN (2012). Multilevel modeling of categorical outcomes using IBM SPSS. New York, NY, US: Routledge/Taylor & Francis Group. [Google Scholar]
- Jenness JL, Jager-Hyman S, Heleniak C, Beck AT, Sheridan MA, & McLaughlin KA (2016). Catastrophizing, rumination, and reappraisal prospectively predict adolescent PTSD symptom onset following a terrorist attack. Depression and Anxiety, 33, 1039–1047. doi: 10.1002/da.22548 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Kaczkurkin AN, Zang Y, Gay NG, Peterson AL, Yarvis JS, Borah EV, … Foa EB (2017). Cognitive emotion regulation strategies associated with the DSM-5 posttraumatic stress disorder criteria. Journal of Traumatic Stress, 30(4), 343–350. doi: 10.1002/jts.22202 [DOI] [PubMed] [Google Scholar]
- Lasser K, Boyd JW, Woolhandler S, Himmelstein DU, McCormick D, & Bor DH (2000). Smoking and mental illness: A population-based prevalence study. Journal Of The American Medical Association, 284(20), 2606–2610. doi: 10.1001/jama.284.20.2606 [DOI] [PubMed] [Google Scholar]
- Mahaffey BL, Gonzalez A, Farris SG, Zvolensky MJ, Bromet EJ, Luft BJ, & Kotov R (2016). Smoking to regulate negative affect: Disentangling the relationship between posttraumatic stress and emotional disorder symptoms, nicotine dependence, and cessation-related problems. Nicotine & Tobacco Research, 18(6), 1471–1478. doi: 10.1093/ntr/ntv175 [DOI] [PubMed] [Google Scholar]
- Marshall EC, Zvolensky MJ, Vujanovic AA, Gibson LE, Gregor K, & Bernstein A (2008). Evaluation of smoking characteristics among community-recruited daily smokers with and without posttraumatic stress disorder and panic psychopathology. Journal of Anxiety Disorders, 22(7), 1214–1226. doi: 10.1016/j.janxdis.2008.01.003 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Matthews LR, Harris LM, & Cumming S (2009). Trauma-related appraisals and coping styles of injured adults with and without symptoms of PTSD and their relationship to work potential. Disability and Rehabilitation, 31(19), 1577–1583. doi: 10.1080/09638280802639012 [DOI] [PubMed] [Google Scholar]
- Michael T, Halligan SL, Clark DM, & Ehlers A (2007). Rumination in posttraumatic stress disorder. Depression and Anxiety, 24(5), 307–317. doi: 10.1002/da.20228 [DOI] [PubMed] [Google Scholar]
- Pietrzak RH, Harpaz-Rotem I, & Southwick SM (2011). Cognitive-behavioral coping strategies associated with combat-related PTSD in treatment-seeking OEF-OIF veterans. Psychiatry Research, 189(2), 251–258. doi: 10.1016/j.psychres.2011.07.019 [DOI] [PubMed] [Google Scholar]
- Szasz PL, Szentagotai A, & Hofmann SG (2012). Effects of emotion regulation strategies on smoking craving, attentional bias, and task persistence. Behaviour Research and Therapy, 50(5), 333–340. doi: 10.1016/j.brat.2012.02.010 [DOI] [PubMed] [Google Scholar]
- Trujillo MA, Khoddam R, Greenberg JB, Dyal SR, Ameringer KJ, Zvolensky MJ, & Leventhal AM (2017). Distress tolerance as a correlate of tobacco dependence and motivation: Incremental relations over and above anxiety and depressive symptoms. Behavioral Medicine, 43(2), 120–128. doi: 10.1080/08964289.2015.1110559 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Weiss NH, Tull MT, Anestis MD, & Gratz KL (2013). The relative and unique contributions of emotion dysregulation and impulsivity to posttraumatic stress disorder among substance dependent inpatients. Drug And Alcohol Dependence, 128(1–2), 45–51. doi: 10.1016/j.drugalcdep.2012.07.017 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Wisco BE, Sloan DM, & Marx BP (2013). Cognitive emotion regulation and written exposure therapy for posttraumatic stress disorder. Clinical Psychological Science, 1(4), 435–442. doi: 10.1177/2167702613486630 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Wolfsdorf BA, & Zlotnick C (2001). Affect management in group therapy for women with posttraumatic stress disorder and histories of childhood sexual abuse. Journal of Clinical Psychology, 57(2), 169–181. doi: [DOI] [PubMed] [Google Scholar]
- Wu L, Winkler MH, Wieser MJ, Andreatta M, Li Y, & Pauli P (2015). Emotion regulation in heavy smokers: Experiential, expressive and physiological consequences of cognitive reappraisal. Frontiers in Psychology, 6, 1–11. doi: 10.3389/fpsyg.2015.01555 [DOI] [PMC free article] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.