Abstract
Aim
To evaluate early results of management of radial neck fractures with Métaizeau technique in the paediatric age group and to elaborate on a surgical tip to improve stability of the fixation.
Method
A retrospective analysis of 21 patients, with fracture radial neck, who underwent closed reduction and internal fixation with elastic intramedullary nailing (Métaizeau technique), was performed. Mean age at injury was eight years, and the average follow-up was 4.5 months (range: 3–6 months). Follow up Clinical and radiological evaluation was performed at first and sixth postoperative weeks. At six weeks following removal of the nail, a clinical assessment was conducted to record the outcomes, and any later follow-up was arranged based on pain and range of motion.
Results
We recorded five excellent, eight good, one fair, results for type 3 fractures. For type 4 fractures, we had one excellent, five good and one fair, results. Altogether, we recorded 20 (90.5%) excellent or good results, and 2 (9.5%) fair results. Complications noted were superficial skin infection at the entry site in one patient that required a course of oral antibiotics. Prominent metal work was noticed in 14 cases, which didn't need any further intervention as it did not cause any functional discomfort.
Conclusion
With Metaizeau technique, there were reported poor results of about 10% in literature. In our study, with the modification of the shape of the nail tip, we have managed to achieve stable fixation of the reduction without any loss of position and consequently, better outcomes.
Keywords: Radial neck fractures, Paediatric, Metaizeau technique, Open reduction
Poor outcomes with the Metaizea technique were mostly attributed to the severity of the initial injury itself. In a small percentage of patients, the poor outcome was secondary to loss of fracture reduction which, in our opinion, could be addressed by improvising on the shape of the nail tip for better fixation.
1. Introduction
Radial neck fractures account for about 1% of all paediatric fractures,1 and they represent almost 5–10% of all elbow injuries.2 They typically affect children between 4 and 14 years of age with a peak of incidence ranging between 8 and ten years of age.1,3, 4, 5, 6, 7
The fracture Classification system used in our study (Table 1):
Table 1.
Judet classification of radial neck fractures.
| Type I | Nondisplaced |
| Type II | <30-degree angulation |
| Type III | 30-60-degree angulation |
| Type IV | 60-80-degree angulation |
| Type IVb | >80-degree angulation |
In recent years, the functional outcomes of radial neck fractures in children are discussed as a consequence of treatment methods. Non-operative option with cast immobilisation was suggested for minimally displaced or non-displaced fractures.8, 9, 10 The acceptable angulation for nonsurgical treatment was based on the age of the patient and ranging within 30–60°degrees5 in most of the discussions. However, there is a general covenant that displaced (Judet type-III and type-IV fractures) fractures (Table 1) may need reduction and stabilisation.3 In displaced radial neck fractures, several options were described, including Manipulation under anaesthesia, percutaneous K-wire leverage (PKWL), Metaizeau technique and open reduction with or without internal fixation.11 Open reduction was discouraged mainly due to its associated complications, such as premature epiphyseal closure, disruption of epiphyseal blood supply and ectopic calcification. Intramedullary nailing with correct technique combines the advantage of closed reduction and stable internal fixation. The purpose of this study was to review the early outcomes of the management of radial neck fractures in paediatric age group using Métaizeau technique. Also, we are describing a surgical technique which facilitated easy passage through fracture site and stable purchase to the radial head.
2. Method
A retrospective analysis was performed on 21 patients who underwent closed reduction and internal fixation with elastic intramedullary nailing (Métaizeau technique) for fracture neck of the radius in our paediatric orthopaedic tertiary referral centre. Mean age at injury was eight years, and the average follow-up was 4.5 months (range: 3–6 months). Follow up Clinical and radiological evaluation was performed at first and sixth postoperative weeks. The nail was removed after a mean 3 (2.5–4) months following insertion. At six weeks following removal of the nail, a clinical assessment was conducted to record the outcomes, and any later follow-up was arranged based on pain and range of motion.
Results were considered as follows (10)
-
–
Excellent, if no limitation in the movement was noted,
-
–
Good, if the deficit in all ranges of motion was less than 20°,
-
–
Fair, if the restriction in mobility ranged between 20 and 40° and
-
–
Poor if the restriction of movement exceeded 40°
Radiographic investigations (10):
AP and lateral radiographs were obtained postoperatively to assess the residual angulation to categorise the outcomes as follows:
-
–
Excellent, if the reduction was anatomic,
-
–
Good, if a simple shift or inclination not exceeding 20° persisted,
-
–
Fair, if the tilt was between 20° and 40° and
-
–
Poor if it was beyond 40°.
No signs of Infection or neurologic (radial nerve injury) complications were noticed in our study. We did not come across with delayed or non-union and any signs of radio-ulnar synostosis at six weeks.
2.1. Surgical procedures
Standard operation table with radiolucent hand table was used, and the patient was positioned supine. Pillows as side support used to secure head and body. Tourniquet applied but not inflated, (in case if it needed open reduction).
2.2. Reduction method
Initially Closed reduction under general anaesthesia was attempted by applying traction to the extended elbow with the forearm in supination, followed by placing Varus stress to the elbow while applying direct pressure over the radial head (Patterson manoeuvre). In difficult reductions, the Israeli technique was used that is pronating and flexing the supinated and extended elbow while the thumb stabilises the proximal radial fragment with direct pressure. Two people applied traction. If manual reduction was successful, that is if < 30° of angulation and <30% of displacement was achieved, (or even if the radial neck-shaft angle was reduced to < 45°) then an elastic intramedullary nail (a diameter of 0.7 times of the narrowest width of radius) was used for fixation, especially in unstable fractures based on pre-op displacement (Fig. 1) and intra op stability on continuous screening of elbow, taking through the full range of movement under image intensifier. The nail tip was cut into a diamond/rhombus shape under sterile conditions for fixation of the nail at three points in the radial head; that is at the tip and on both sides of the flat proximal end of the nail in the proximal fragment (Fig. 16, Fig. 17, Fig. 18, Fig. 19, Fig. 20, Fig. 21). This reshaping helped in preventing the nail from slipping through the fracture site while passing the nail across the fracture as well as during the rotational manoeuvre of the nail to reduce the proximal fragment. The nail was inserted from proximal to the distal physis of radius and advanced through the fracture site into the radial head. The nail tip was positioned to the radial head, and the fracture ends were distracted before the nail was rotated up to 180° in combination with manual reduction, and following which, the elbow range of motion was assessed. In unsuccessful reduction, a 2-mm K-wire was percutaneously inserted from the side of displacement of radial neck into the proximal fragment, and the k wire was used as a joystick to reduce by leveraging. Radial neck fractures were reduced to <30° with a displacement of <30% but, in one patient 30-degree angulation was accepted before fixation. The injured arm was immobilised in the functional position using a plaster cast for two weeks. Early range of movement exercises was encouraged after removal of the plaster cast. Other used closed reduction techniques in our practice was Neher–Torch13 method; that is applying pressure over the radial head from the radial aspect while maintaining Varus stress on the extended elbow with the forearm in supination.
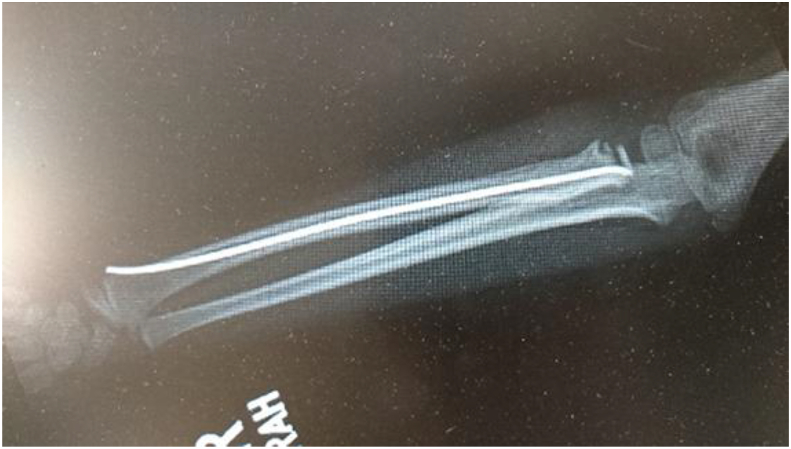
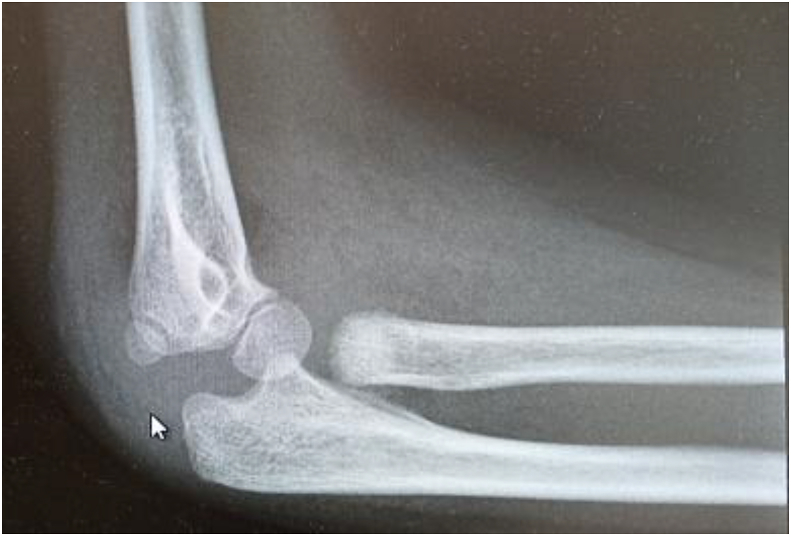
Fig. 1.
Pre-op AP and Lateral views of elbow depicting displaced and angulated radial neck fracture.
Fig. 16.
Manual reshaping of the tip of a Nail into a rhombus/diamond shape using a pliers (for illustration purpose only; normally done intraoperatively under sterile conditions with gloves on).
Fig. 17.
Cutting a piece of a nail from the inside of the curve of a nail tip using a pliers.
Fig. 18.

Tip of the nail in a Rhombus shape, without changing the proximal curve of the nail.
Fig. 19.

Side on view of the tip of the nail.
Fig. 20.

Face on view of the cut tip of the nail.
Fig. 21.

Schematic diagram of the tip of nail on frontal profile.
3. Results
Fourteen patients had Judet type 3 fractures, six patients had Judet type 4a, and one presented with type 4b fracture (Fig. 2, Fig. 3, Fig. 4, Fig. 5, Fig. 6, Fig. 7, Fig. 8, Fig. 9, Fig. 10, Fig. 11, Fig. 12, Fig. 13, Fig. 14). Average follow-up of these patients was 4.5 months (range: 3–6 months). Based on the clinical evaluation criteria mentioned above, we recorded five excellent, eight good, one fair results for type 3 fractures at the final follow up. For type 4 fractures, we had one excellent, five good and one fair, results. One patient with type 4b fracture had a combined restriction of about 35 to 40-degrees in flexion, extension, supination and pronation of the forearm in the affected extremity. One patient, in type 3 fractures, had 20- degree limitation of extension with full forearm pronation and supination. At final follow-up, there were 19 (90.5%) excellent or good results, and 2 (9.5%) fair results. Complications noted were superficial skin infection at the entry site in one patient which was treated with a course of oral antibiotics. Prominent metal work was noticed in 14 cases which didn't cause any functional discomfort, and it did not require any further medical intervention, hence, considered as a minor complication. In a 13 yr old boy who appeared to have more age physiologically, had the tip of the nail left outside the skin deliberately for removal under Entonox sedation in the clinic at two months follow up. It did not compromise the good outcome, and it can be considered as an option to avoid second general anaesthesia in suitable patients. In a six-year-old with complete displacement, 30° of angulation was accepted before stabilising with our modified elastic nail method with no subsequent displacement on follow up assessment, and the patient went on achieving an excellent result at the time of discharge after five months. Neurovascular deficit or deep infection was not reported in our patients. No change in reduction was observed radiologically in all 7 type 4 fractures and 14 type 3 Fractures before fracture union and subsequent removal of the nail. We have not noticed any penetration of the nail into the joint with this technique in our study.
Fig. 2.
Post op AP with anatomical reduction and stable fixation with reshaped nail.
Fig. 3.
Post op Lateral view with reduced fracture and nail.
Fig. 4.

Pre-op AP with angulated and displaced fracture.
Fig. 5.
Pre-op Lateral view with angulated and displaced fracture.
Fig. 6.

Post op AP with nail tip in the subchondral bone facilitating anatomical reduction and stable fixation of the fracture.
Fig. 7.

Post op Lateral view with nail tip in the subchondral bone facilitating anatomical reduction and satisfactory alignment of the fracture.
Fig. 8.
Lateral view Pre-op X ray showing angulated and displaced fracture.
Fig. 9.

Pre-op AP X ray showing angulated and displaced fracture.
Fig. 10.

Pre-op AP X ray showing angulated and displaced fracture.
Fig. 11.

Post op AP with stable fixation.
Fig. 12.
Post op Lateral view showing the position of (modified) tip of the nail in the subchondral bone of radial head.
Fig. 13.
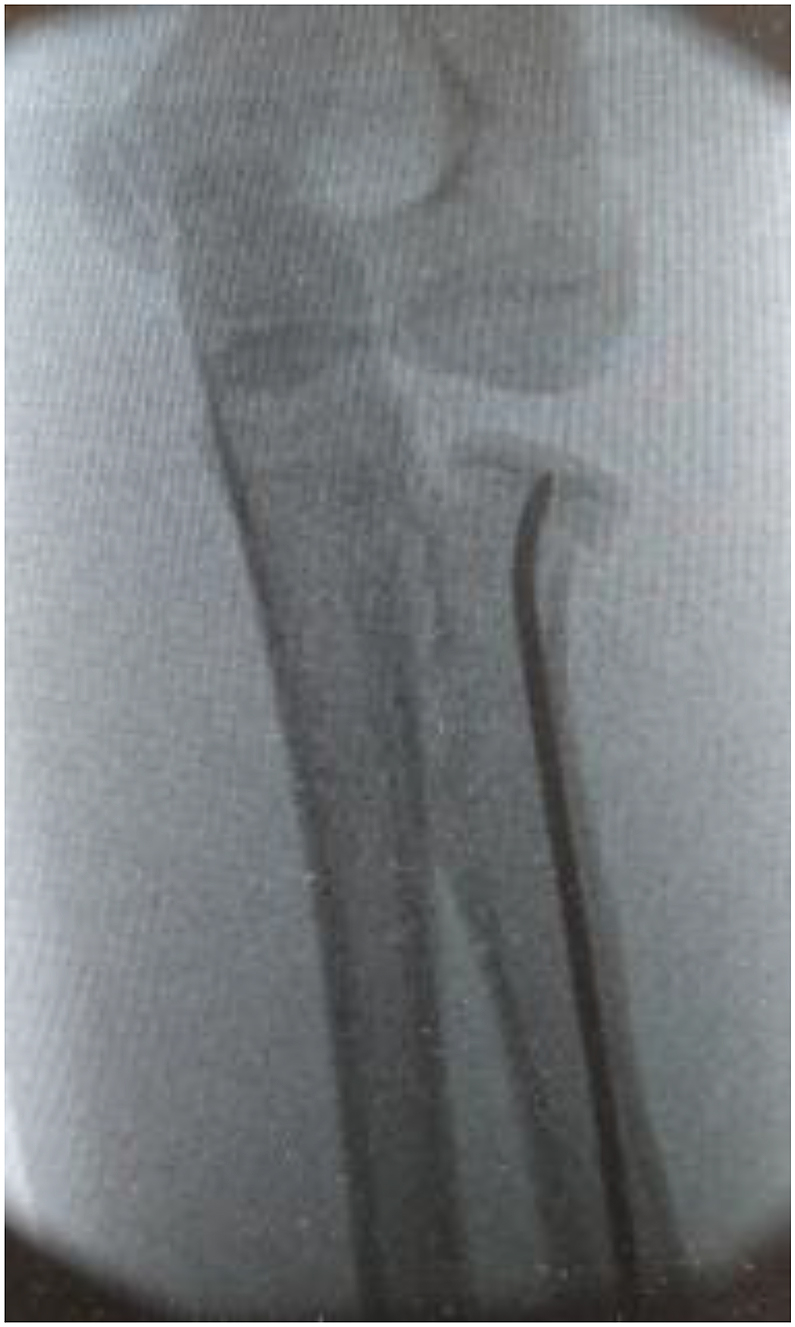
Post op AP with stable fixation of fracture with acceptable (<30 deg) residual angulation.
Fig. 14.
Lateral view depicting stable fixation of fracture.
4. Discussion
In general, the non-surgical option is suggested for children younger than five years of age, who present with full pronation and supination,12, 13, 14, 15, 16, 17, 18 and a radial neck-shaft angle of less than 50°-60°5,12,13 together with minimal displacement or translation (<2–3 mm).14 Satisfactory outcomes have been reported with conservative management in most series.5,8,17, 18, 19 The non-surgical option can also be considered in children up to 10 years of age with an angle of <30°. Fractures with angulation more than 30° and displacement of more than 50% (or >4 mm) should undergo an attempt of closed reduction.20,21 Authors differ widely about the acceptable angulation for good results, which ranges from 15 to 60° based on the age of the patients.8,9,22, 23, 24, 25, 26, 27, 28, 29, 30, 31, 32, 33, 34, 35
In a study20 the severity of initial fracture displacement and inadequate fixation technique contributed to radial neck non-union, and the authors suggested that treatment of the non-union should depend on patient's pain, deformity, and functional restriction.
Fractures with large angles and displacement may need percutaneous K-wire leverage.9,15 These fractures need proper fixation as removal of K-wire immediately may cause loss of reduction,34 and in these cases, closed intramedullary pinning (CIMP) as proposed by Métaizeau et al.,22 is an appropriate non-invasive closed reduction method.22 In a retrospective analysis22 of 151 children, two (10.5%) of nineteen fractures treated with intramedullary nailing lost reduction and required additional intervention; Several other studies quoted similar results with metazieau technique. Moreover, the worse outcome has been reported for Judet-IV fractures than for Judet-III fractures.12
Compared to the failure rates quoted in the literature with this technique, which was almost more than 10% and related to the failure of fixation needing a second surgery; our results are encouraging in achieving stable fixation to avoid further surgery due to loss of reduction. In our study, we found no poor results secondary to loss of reduction. Initially, we had experienced the blunt tip of the nail slipping out through the fracture site when passing through the fracture and had a similar experience when rotating the nail to reduce the proximal fragment [Fig. 15]. By cutting the tip of the nail into a rhombus or diamond shape, the passage of the nail through the fracture site was smooth, and the nail tip remained in the proximal fragment as it caught the fragment at three points. We didn't come across with the slippage of the nail through the fracture site while inserting it into the proximal fragment. Epiphyseal plate damage during reduction using CIMP is a possibility, especially in impacted fractures. Due to its facility to achieve stable fixation to the proximal fragment, the distraction of the fragments and reduction of the proximal fragment with the rotation of the nail was poised without scuffling the growth plate. Due to assurance in fixation, it was more comfortable to initiate an early range of movement, which avoid any formation of tissue adhesions and consequent stiffness of the joint in these patients.
Fig. 15.

AP view demonstrating escape of blunt nail tip through the fracture site and loss of reduction (nail with non-modified tip).
Our retrospective study is not free of any flaws, especially considering the small number of patients and lack of biomechanical analysis of the postulated extractability achieved from reshaping the nail tip. Further prospective randomised studies with a large number of patients, biomechanical assessment, and robust statistical analysis with extended periods of follow-up may help in establishing the significance of this method.
5. Conclusion
Increased fracture severity and open reduction were associated with poor results, though the presence of associated injuries was not in most of the series. There is >10% risk of poor results with closed reduction and internal fixation even with Métaizeau technique due to loss of reduction.30, 31, 32, 33, 34, 35, 36, 37, 38 Our results support the Métaizeau technique and postulate that the usage of a nail with reshaped tip may help in avoiding revision surgery by minimising the loss of reduction. In our series, though, not big enough to substantially conclude and extrapolate the effectiveness of this technique, we have not noticed any poor outcomes due to loss of reduction. Our results are within the acceptable range of satisfactory outcomes, if not more towards the better end of the outcomes quoted in literature.
Patient declaration statement
“The authors certify that they have obtained all appropriate patient consent forms. In the form, the patient(s) has/have given his/her/their consent for his/her/their images and other clinical information to be reported in the journal. The patients understand that their names and initials will not be published and due efforts will be made to conceal their identity, but anonymity cannot be guaranteed.”
Conflicts of interest
The authors declare that they have no conflict of interest.
Funding
There is no funding source.
Ethical approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Footnotes
Supplementary data to this article can be found online at https://doi.org/10.1016/j.jor.2019.06.001.
Appendix A. Supplementary data
The following is the Supplementary data to this article:
References
- 1.Fuentes-Salguero L., Downey-Carmona F.J., Tatay-Diaz A. [Radial head and neck fractures in children] Rev Española Cirugía Ortopédica Traumatol. 2012;56(4):300–305. doi: 10.1016/j.recot.2012.01.002. [DOI] [PubMed] [Google Scholar]
- 2.Novoth B. Closed reduction and intramedullary pinning of radial neck fractures in children. Orthop Trauma. 2002:313–322. [Google Scholar]
- 3.Eberl R., Singer G., Fruhmann J., Saxena A., Hoellwarth M.E. Intramedullary nailing for the treatment of dislocated pediatric radial neck fractures. Eur J Pediatr Surg. 2010;20(4):250–252. doi: 10.1055/s-0030-1249104. [DOI] [PubMed] [Google Scholar]
- 4.Okcu G., Aktuglu K. Surgical treatment of displaced radial neck fractures in children with Metaizeau technique. Ulus Travma Acil Cerrahi Derg. 2007;13(2):122–127. [PubMed] [Google Scholar]
- 5.Zhang F.-Y., Wang X.-D., Zhen Y.-F., Guo Z.-X., Dai J., Zhu L.-Q. Treatment of severely displaced radial neck fractures in children with percutaneous K-wire leverage and closed intramedullary pinning. Mayr J., editor. Medicine. 2016;95(1):e2346. doi: 10.1097/MD.0000000000002346. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Falciglia F., Giordano M., Aulisa A.G., Di Lazzaro A., Guzzanti V. Radial neck fractures in children: results when open reduction is indicated. J Pediatr Orthop. 2014;34(8):756–762. doi: 10.1097/BPO.0000000000000299. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Fowles J.V., Kassab M.T. Observations concerning radial neck fractures in children. J Pediatr Orthop. 1986;6:51–57. [PubMed] [Google Scholar]
- 8.Métaizeau J.P., Lascombes P., Lemelle J.L., Finlayson D., Prevot J. Reduction and fixation of displaced radial neck fractures by closed intramedullary pinning. J Pediatr Orthop. 1993;13:355–360. doi: 10.1097/01241398-199305000-00015. [DOI] [PubMed] [Google Scholar]
- 9.Stiefel D., Meuli M., Altermatt S. Fractures of the neck of the radius in children. Early experience with intramedullary pinning. J Bone Joint Surg Br. 2001;83(4):536–541. doi: 10.1302/0301-620x.83b4.11060. [DOI] [PubMed] [Google Scholar]
- 10.Ursei M, Sales de Gauzy J, Knorr J, Abid A, Darodes P, Cahuzac J P. Surgical Treatment of Radial Neck Fractures in Children by Intramedullary Pinning. [PubMed]
- 11.Kang S.1, Park S.S. Predisposing effect of elbow alignment on the elbow fracture type in children. J Orthop Trauma. 2015 Aug;29(8):e253–e258. doi: 10.1097/BOT.0000000000000322. [DOI] [PubMed] [Google Scholar]
- 12.Pring M.E. Pediatric radial neck fractures: when and how to fix. J Pediatr Orthop. 2012;32(Suppl 1):S14–S21. doi: 10.1097/BPO.0b013e31824b251d. [DOI] [PubMed] [Google Scholar]
- 13.Tan B.H., Mahadev A. Radial neck fractures in children. J Orthop Surg (Hong Kong) 2011;19:209–212. doi: 10.1177/230949901101900216. [PubMed] [DOI] [PubMed] [Google Scholar]
- 14.Ligier J.N., Metaizeau J.P., Prévot J. Closed flexible medullary nailing in pediatric traumatology. Chir Pediatr. 1983;24:383–385. [PubMed] [Google Scholar]
- 15.Klitscher D., Richter S., Bodenschatz K. Evaluation of severely displaced radial neck fractures in children treated with elastic stable intramedullary nailing. J Pediatr Orthop. 2009;29:698–703. doi: 10.1097/BPO.0b013e3181b76895. [PubMed] [DOI] [PubMed] [Google Scholar]
- 16.D'souza S., Vaishya Raju, Klenerman L. Management of radial neck fractures in children: a retrospective analysis of one hundred patients. J Pediatr Orthop. 1993;13:232–238. [PubMed] [Google Scholar]
- 17.van Vugt A.B. Surgical treatment of fractures of the proximal end of the radius in childhood. Arch Orthop Trauma Surg. 1985;104:37. doi: 10.1007/BF00449955. [DOI] [PubMed] [Google Scholar]
- 18.Jones E.R.L., Esah M. Displaced fractures of the neck of the radius in children. J Bone Jt. Surg. 1971;53B:423439. [PubMed] [Google Scholar]
- 19.Sharrard W.J.W. Blackwell; Oxford: 1971. Paediatric Orthopaedics and Fractures; pp. 972–975. [Google Scholar]
- 20.Waters P.M., Stewart S.L. Radial neck fracture nonunion in children. J Pediatr Orthop. 2001;21:570–576. [PubMed] [PubMed] [Google Scholar]
- 21.Schmittenbecher P.P., Haevernick B., Herold A. Treatment decision, method of osteosynthesis, and outcome in radial neck fractures in children: a multicenter study. J Pediatr Orthop. 2005;25:45–50. doi: 10.1097/00004694-200501000-00011. [PubMed] [DOI] [PubMed] [Google Scholar]
- 22.Zimmerman R.M. Surgical management of pediatric radial neck fractures. J Bone Joint Surg Am. 2013;95:1825–1832. doi: 10.2106/JBJS.L.01130. [DOI] [PubMed] [Google Scholar]
- 23.De Mattos C.B., Ramski D.E., Kushare I.V. Radial neck fractures in children and adolescents: an examination of operative and nonoperative treatment and outcomes. J Pediatr Orthop. 2015;36:6–12. doi: 10.1097/BPO.0000000000000387. [DOI] [PubMed] [Google Scholar]
- 24.Basmajian H.G., Choi P.D., Huh K. Radial neck fractures in children: experience from two level-1 trauma centres. J Pediatr Orthop B. 2014;23:369–374. doi: 10.1097/BPB.0000000000000057. [DOI] [PubMed] [Google Scholar]
- 25.Tarallo L., Mugnai R., Fiacchi F. Management of displaced radial neck fractures in children: percutaneous pinning vs. elastic stable intramedullary nailing. J Orthop Traumatol. 2013;14:291–297. doi: 10.1007/s10195-013-0252-0. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26.Evans M.C., Graham H.K. Radial neck fractures in children: a management algorithm. J Pediatr Orthop B. 1999;8:93–99. [PubMed] [Google Scholar]
- 27.Cha S.M., Shin H.D., Kim K.C. Percutaneous reduction and leverage fixation using K-wires in paediatric angulated radial neck fractures. Int Orthop. 2012;36:803–809. doi: 10.1007/s00264-011-1387-3. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 28.Eberl R., Singer G., Fruhmann J. Intramedullary nailing for the treatment of dislocated pediatric radial neck fractures. Eur J Pediatr Surg. 2010;20:250–252. doi: 10.1055/s-0030-1249104. [DOI] [PubMed] [Google Scholar]
- 29.Brandao G.F., Soares C.B., Teixeira L.E. Displaced radial neck fractures in children: association of the Metaizeau and Bohler surgical techniques. J Pediatr Orthop. 2010;30:110–114. doi: 10.1097/BPO.0b013e3181cf118a. [DOI] [PubMed] [Google Scholar]
- 30.Bernstein S.M., Mckeever P., Bernstein L. Percutaneous reduction of displaced radial neck fracture in children. J Pediatr Orthop. 1993;13:85–88. doi: 10.1097/01241398-199301000-00017. [DOI] [PubMed] [Google Scholar]
- 31.Ugutmen E., Ozkan K., Ozkan F.U. Reduction and fixation of radius neck fractures in children with intramedullary pin. J Pediatr Orthop B. 2010;19:289–293. doi: 10.1097/bpb.0b013e32833918a0. [DOI] [PubMed] [Google Scholar]
- 32.Leung A.G., Peterson H.A. Fractures of the proximal radial head and neck in children with emphasis on those that involve the articular cartilage. J Pediatr Orthop. 2000;20:7–14. [PubMed] [Google Scholar]
- 33.Waters P.M., Stewart S.L. Radial neck fracture nonunion in children. J Pediatr Orthop. 2001;21:570–576. [PubMed] [Google Scholar]
- 34.Tiefel D., Meuli M., Altermatt S. Fractures of the neck of the radius in children, early experience with intramedullary pinning. J Bone Jt Surg. 2001;83-B:536–541. doi: 10.1302/0301-620x.83b4.11060. [DOI] [PubMed] [Google Scholar]
- 35.Radomisli T.E., Rosen A.L. Controversies regarding radial neck fractures in children. Clin Orthop Relat Res. 1998;353:30–39. doi: 10.1097/00003086-199808000-00005. [DOI] [PubMed] [Google Scholar]
- 36.Endele S.M., Wirth T., Eberhardt O. The treatment of radial neck fractures in children according to Metaizeau. J Pediatr Orthop B. 2010;19:246–255. doi: 10.1097/bpb.0b013e32833918c0. [DOI] [PubMed] [Google Scholar]
- 37.Kaiser Margarita, Eberl Robert, Castellani Christoph, Kraus Tanja. Judet type-IV radial neck fractures in children: comparison of the outcome of fractures with and without bony contact. Acta Orthop. 2016;87(5):529–532. doi: 10.1080/17453674.2016.1203700. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 38.Monson R., Black B., Reed M. A new closed reduction technique for the treatment of radial neck fractures in children. J Pediatr Orthop. 2009;29:243–247. doi: 10.1097/BPO.0b013e3181990745. [DOI] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.