Abstract
Growth hormone (GH) is secreted by the anterior pituitary gland and regulates various metabolic processes throughout the body. GH and IGF-1 levels are markedly reduced in older humans, leading some to hypothesize GH supplementation could be a viable “anti-aging” therapy. However, there is still much debate over the benefits and risks of GH administration. While an early study of GH administration reported reduced adiposity and lipid levels and increased bone mineral density, subsequent studies failed to show significant benefits. Conversely, other studies found positive effects of GH deficiency including extended life span, improved cognitive function, resistance to diseases such as cancer and diabetes, and improved insulin sensitivity despite a higher fat percentage. Thus, the roles of GH in aging and cognition remain unclear, and there is currently not enough evidence to support use of GH as an anti-aging or cognitive impairment therapy. Additional robust and longer-duration studies of efficacy and safety of GH administration are needed to determine if modulating GH levels could be a successful strategy for treating aging and age-related diseases.
Keywords: Growth hormone, IGF-1, Aging, GH deficiency, Longevity, Cognition
Introduction
In 1921, Evans and Long reported that treating rats with bovine anterior pituitary extracts increased growth (Evans and Long 1922). The key factor in these extracts was later identified and named growth hormone (GH). Since 1981, genetic engineering and DNA recombinant technology has allowed production of unlimited amounts of GH for use in patients and research (Devesa et al. 2016a). GH is a 19- to 21-kDa cytokine secreted by the anterior pituitary gland that directly affects cellular proliferation and differentiation and is most often associated with tissue growth, particularly muscle and bone (Donahue et al. 2006). GH and its main anabolic mediator, insulin-like growth factor-1 (IGF-1), together with hypothalamic GH-releasing hormone (GHRH) make up the somatotropic axis, which is partially responsible for regulation of puberty and gonadal function, as well as structural and functional maintenance of tissues and growth (Bartke 2005). Many actions of GH, direct or mediated by IGF-1, promote anabolic processes including synthesis of DNA and RNA (Ramsey et al. 2004) and amino acid uptake and protein synthesis (Sonntag et al. 2005). While the liver is the main producer of IGF-1, accounting for ~ 70–90% of circulating levels, IGF-1 is produced in nearly all tissues and functions in an autocrine/paracrine fashion (Devesa et al. 2016a; List et al. 2014). IGF-1 is involved in a negative feedback loop regulating GH secretion via binding to IGF-1 receptors (IGF-1Rs) and insulin receptors (InsRs) in the hypothalamus and anterior pituitary. GH released from the anterior pituitary gland binds to its cognate receptors, which are ubiquitously expressed throughout the body. Activation of the pre-dimerized GH receptor (GHR) initiates signal transduction through the JAK-STAT pathway, leading to phosphorylation of various intermediate players and promotion of IGF-1 production.
GH and IGF-1 play key roles throughout lifespan and during aging. Soon after birth, pulsatile GH release occurs. In early infancy, rapid growth observed between 6 and 10 months of age is believed to depend on nutrients and the GH/IGF-1 axis. In fact, while growth in utero follows an exponential curve, growth in infancy follows a doubly exponential curve (Nielsen et al. 2015; Murray and Clayton 2000). GH and IGF-1 levels reach their peak as puberty approaches, supporting the idea that this axis plays a vital role in growth and control of normal growth velocity. After puberty, GH levels gradually decrease, and after the third decade of life, the decrease in GH is about 14% per decade (Devesa et al. 2016a). The decline in GH continues during aging, resulting in lower plasma GH levels in the elderly (Bartke 2008). Indeed, GH levels are substantially reduced in humans over the age of 50 to 60. This phenomenon, known as somatopause is well-documented, but a key question remains difficult to answer: How does GH deficiency (or treatment) affect aging, and specifically, the aging brain? The purpose of this review is to highlight recent reports pertinent to GH and aging, with special emphasis on the aging brain and cognitive function.
GH deficiency in humans
Systemic effects of GH deficiency
GH and IGF-1 levels dramatically increase during adolescence to promote growth, but it is less clear what GH’s role is later in life and how GH deficiency or age-related decline affects the body (Ashpole et al. 2015). In humans, GH deficiency (GHD) can occur in childhood or adulthood. GHD in childhood has been associated with growth and muscle impairments, while adult-onset GHD has been linked to poor metabolic function, increased adiposity, heart disease, and reduced quality of life (Hulthen et al. 2001; Cuneo et al. 1992; Gilchrist et al. 2002). As expected, GHD in adolescence results in reduced muscle mass and bone growth (Ashpole et al. 2015). In addition, genetic GHD is associated with visceral obesity and lipid metabolism disorders. In some of the examined cohorts, GHD also causes insulin resistance, and reduced vitality and energy levels. Some studies have also found evidence suggesting childhood-onset GHD is associated with diminished memory recognition and intelligence (van Dam et al. 2005).
Adult-onset GHD can be partial or complete, with complete GHD being better characterized in the research literature. Diagnosing GH deficiency in adults is challenging because of the lack of growth parameters to use as diagnostic markers. In addition, it is often hard to determine cause and effect because other conditions often co-present in affected individuals. For example, GHD in adults is correlated with central adiposity and abnormal body composition, decreased lean muscle mass and extracellular fluid volume, diminished muscle strength, decreased physical energy and stamina, depression, and impaired cognitive function in age-related diseases (Feldt-Rasmussen and Klose 2016; Janssen et al. 1999; Johannsson et al. 2002; Jorgensen et al. 1996; Merola et al. 1996; Moller et al. 1996; Littley et al. 1989; Modesto Mde et al. 2014; Simpson et al. 2001; Weaver et al. 1995; Widdowson and Gibney 2008). In contrast, growth alterations are key features of GHD in children. Effects of congenital isolated GHD were studied by Drs. M. Aguiar-Oliveira, R. Salvatori, and their colleagues, in a large cohort of individuals in northeastern Brazil who were homozygous for a mutation in the GH-releasing hormone receptor (Ghrhr) gene. These individuals are characterized by severe dwarfism, due to very low GH and IGF-1 levels, increased adiposity, reduced β-cell function, and increased insulin sensitivity (Salvatori et al. 2001). Lean body mass is reduced, but muscle function is adequate with increased muscle strength parameters (adjusted for body weight and composition), capacity for vigorous physical activity, and improved resistance to fatigue. Their longevity and quality of life are normal, and they are largely protected from cancer (except for the non-melanoma skin cancer) and less prone to atherosclerosis (Table 1) (Aguiar-Oliveira and Bartke 2019).
Table 1.
Major phenotypic characteristics of GH/IGF-1 signal suppression in human and most extensively studied mouse dwarfism
| Human | GHRH-R mutation | Dwarfism |
GH ↓ IGF-1 ↓ |
Adiposity ↑ Lean BM ↓ |
Insulin sensitivity ↑ | Cancer incidence ↓ | Longevity ??? |
| Human | Laron syndrome | Dwarfism |
GH ↑/resistance IGF-1 ↓ |
Adiposity ↑ Lean BM ↓ |
Insulin sensitivity ↑ | Cancer incidence ↓ | Longevity ??? |
| Mouse | Ames dwarf | Dwarfism |
GH ↓ IGF-1 ↓ |
Adiposity ↑ Lean BM ↓ |
Insulin sensitivity ↑ | Cancer incidence ↓ | Longevity ↑ |
| Mouse | Snell dwarf | Dwarfism |
GH ↓ IGF-1 ↓ |
Adiposity ↑ Lean BM ↓ |
Insulin sensitivity ↑ | Cancer incidence ↓ | Longevity ↑ |
| Mouse | GHRKO/Laron dwarf | Dwarfism |
GH ↑/resistance IGF-1 ↓ |
Adiposity ↑ Lean BM ↓ |
Insulin sensitivity ↑ | Cancer incidence ↓ | Longevity ↑ |
Studies of individuals with Laron syndrome (LS), a rare form of short stature caused by the body’s inability to utilize GH, also provide insight. Guevara-Aguirre (Guevara-Aguirre et al. 2011) reported on a large cohort of individuals with LS that had only one non-lethal malignancy and no cases of diabetes. This finding is significant because in relatives 20% of deaths were attributed to cancer and 5% to type 2 diabetes. Genetic analyses revealed significant differences in pathways involved in cell cycle regulation, gene expression, cell movement, and cell death. Apoptosis-regulating genes are found in the serum of patients with LS and Ras, PKA, and TOR/S6K, known central regulators of pro-aging and disease-promoting pathways, are downregulated. Mitochondrial superoxide dismutase mRNA levels (MnSOD/SOD2) are increased by 30%, suggesting increased protection against oxidative stress in LS (Guevara-Aguirre et al. 2011). Moreover, adults with LS have a higher percentage of body fat compared to controls, while contrary to expectations, patients with LS have improved glucose tolerance and lower fasting insulin and triglyceride levels. Importantly, the studies performed on LS individuals revealed that despite weighing only 65% of controls, LS adults had lower concentrations of glucose and one-third the insulin levels of controls after consumption of the same high-calorie meal. In sum, insulin sensitivity is greater in patients with LS than in healthy control individuals (Table 1) (Guevara-Aguirre et al. 2015).
GH/IGF-1 deficiency and the nervous system
While the role of GH in tissues such as liver, bone, and skeletal muscle has been extensively investigated, the role of GH in the central nervous system (CNS) has been less thoroughly studied. GHRs are widely expressed in the CNS, suggesting GH/IGF-1 signaling pathway plays important roles in regulation of brain tissue and function (Ashpole et al. 2015). GH receptors have been found in the hippocampus, putamen, and thalamus and studies have identified positive and negative effects of GH in the CNS and peripheral nervous system (PNS). GH and IGF-1 axis, as well as IGF-2, are responsible for early brain development, maturation, and function, yet the role these growth factors play in maintaining cognitive health during aging is still somewhat controversial.
Patients with GHD can exhibit microcephaly and patients with autosomal recessive growth hormone deficiencies exhibit mild to severe cognitive impairments (Walenkamp et al. 2005; Netchine et al. 2009). It has been hypothesized that GH and IGF-1 might contribute to brain repair after injury because GHRs are expressed in regions of the brain in which neurogenesis occurs during embryonic development. Because of the location of GHRs in the brain, GH may play a role in learning, memory, cognition, and emotion (Ashpole et al. 2015). A study by Donahue et al. found GH may also modulate the stress response after exposure to acute stressful experiences. Stress-exposed rats exhibited altered levels of hippocampal GH and IGF-1 (Donahue et al. 2006). In agreement with these observations, some GHD adults experience impaired psychological well-being, emotions, memory, mood, and cognition (Brod et al. 2014).
In neuropsychological assessments, adults with GHD exhibit poor performance scores in tests related to verbal memory and planning of behavior and attention. Furthermore, magnetic resonance spectroscopy (MRS) studies have found increased choline in GHD patients, indicative of increased synthesis or breakdown of the neuronal membrane, and reduced N-acetylaspartate (NAA) and NAA/choline ratios compared to healthy controls. In a study of 11 childhood-onset GHD adults, subjects also exhibited reduced NAA/choline ratios and evidence of impaired memory and attention, which was attributed to reduced neuronal integrity (van Dam et al. 2005).
Several mechanisms have been proposed to explain the effects of GH on the brain. One hypothesis suggests GH might work by enhancing excitatory synaptic transmission through GH receptors. In addition, it is believed that GH affects neurotransmitters differently in several brain regions. According to Nyberg (2000), GH could act in at least three different ways in the brain (Nyberg 2000). First, GH might provoke release of secondary mediators from tissues, such as IGF-1, and these secondary mediators cross the blood brain barrier (BBB) to affect the CNS. Second, GH might be enzymatically degraded to bioactive fragments, which might then work on peptidergic receptors in the CNS. Finally, GH might enter the brain and directly influence areas responsive to GH. This final possibility is supported by the fact that GH has been detected in the CSF of animals and GH therapy in adult patients increases GH levels in CSF (Nyberg 2000). In addition, Pan et al. confirmed in rats and mice that GH can cross the BBB despite the absence of a specific transport system. They detected significant uptake of GH into the brain with no difference between species (Pan et al. 2005).
Importantly, somatotropic signaling and age-related changes in circulating levels of GH and IGF-1 have been related to aging of the central nervous system. Studies in rats provided early evidence that age-related decline in the function of GHRH-secreting neurons is a key reason why circulating levels of GH are progressively reduced during aging (Sonntag et al. 1981; Sonntag et al. 1980). The associated reduction of circulating IGF-1 levels emerged as a likely explanation for age-related decline in cognitive functions because IGF-1 has well-documented neurostimulatory and neuroprotective effects. Regulated by GH, the IGF-1 is also well known to be critical for neuronal structure and function, and models of IGF-1 deficiency demonstrate important hippocampal deficits, as evidenced by reduced structural complexity, excitability, learning, and memory. On the other hand, IGF-1 promotes neuronal cell survival and repair, neurogenesis, synaptogenesis, cerebrovascular integrity (Ashpole et al. 2015; Logan et al. 2018; Sonntag et al. 2013; Labandeira-Garcia et al. 2017), and autophagic function in cortical neurons (Renna et al. 2013), all of which could favorably impact possible underlying contributors to age-related cognitive decline, as well as neurological disease. It has to be recognized that age-dependent IGF-1 decline or IGF-1 deficiency may also impact aging through modulation of autonomic nervous system (Balasubramanian et al. 2019). Interestingly, low IGF-1 levels have been associated with subsequent risk for vascular dementias (Quinlan et al. 2017), while IGF-1 deficiency in young animals has been shown to impair cerebrovascular function and exacerbate hypertension-induced cerebrovascular microhemorrhages (Sonntag et al. 2013; Tarantini et al. 2017; Toth et al. 2015). In a recent study in mice, deletion of IGF-1 receptors selectively in the astrocytes was shown to impair working memory and induce various functional deficits in cultured astrocytes (Logan et al. 2018).
Several studies have shown that IGF-1 replacement to old animals reverses many age-related deficits including sensorimotor function and depressive-like behavior (Ramsey et al. 2004; Lichtenwalner et al. 2001; Sonntag et al. 2000; Markowska et al. 1998). More recently, intranasal delivery of IGF-1, which is a translatable strategy to target IGF-1 centrally, to 24 months old male mice for just 1 month was sufficient to improve learning, memory, and reverse depressive-like behavior while boosting neurogenesis and GluA2 content (Farias Quipildor et al. 2019). Therefore, these data collectively suggest that centrally acting IGF-1 may be a beneficial factor for the aging brain.
Consequently, it was unexpected that mice with genetic GH deficiency or GH resistance were reported to maintain cognitive function during aging and when examined at the age of approximately 2 years had better memory than their normal (wild-type siblings) (Kinney et al. 2001a; Kinney et al. 2001b). Importantly, human subjects with hereditary GH resistance (Laron syndrome) also show improved rather than impaired memory (Nashiro et al. 2017). The most likely explanation why suppression of GH signaling does not lead to deficits in brain development and function was provided by the demonstration that hippocampal IGF-1 expression is not reduced in GH-deficient mice (Sun et al. 2005a). Importantly, previous studies in the laboratory of A. Efstratiadis provided evidence that in contrast to hepatic IGF-1 expression, IGF-1 expression in the brain is not GH-dependent (Lupu et al. 2001).
GH deficiency in rodents
Systemic effects of GH deficiency
Similarly to humans, GHD mice exhibit different phenotypes than age- and sex-matched controls. GHD, hypopituitary, and GH-resistant adult mice are significantly smaller because of decreased postnatal growth rate (Berryman et al. 2004; Masternak et al. 2004; Berryman et al. 2010; Dominici et al. 2002; Bonkowski et al. 2009). For example, body weight of Snell and Ames dwarf mice is less than half of their normal siblings. Like GHD in humans, these mutant mice have increased adiposity, but remain metabolically healthy, exhibiting enhanced insulin sensitivity (Masternak and Bartke 2012) and partial resistance to cancer (Ikeno et al. 2003; Podlutsky et al. 2017). Ames dwarf mice, which carry a homozygous loss-of-function mutation at the Prop-1 locus, are deficient in GH, thyroid-stimulating hormone (TSH), and prolactin-producing cells in the adenohypophysis. Despite their smaller body size and unique phenotype, these mice have a significantly increased lifespan and maintain physiological and cognitive function at youthful levels longer than controls (Ikeno et al. 2003; Bartke et al. 2001). Snell mice, which have a Pit-1 transcription factor defect, are GH, prolactin, and thyroid hormone (TH) deficient and, like Ames dwarf mice, have greatly extended longevity (Laron 2005). GHR knockout (GHRKO) mice, a mammalian model for human LS, share physical and biochemical characteristics with LS patients. Specifically, both lack GHR, experience severe postnatal growth failure, and have depressed IGF-1 and elevated GH levels. The degree of growth retardation in mice is similar to the human syndrome (Zhou et al. 1997). GHRKO mice also exhibit altered sexual maturation and fecundity, which are delayed and reduced, respectively (Table 1) (Bartke 2008).
GH and IGF-1 effects on metabolism
Circulating insulin-like growth factor (IGF-1) is derived primarily from the liver and mediates growth-promoting actions of GH. However, actions of GH on other processes are complex and involve a combination of direct effects as well as effects of circulating or locally produced IGF-1. Actions of the somatotropic axis on the adipose tissue, body composition, and metabolism involve intricate interaction of the effects of GH and IGF-1 which may be overlapping, different, or even opposite. For example, GH is lipolytic while IGF1 promotes fat deposition by its insulin-like actions. In addition to affecting adiposity via its lipolytic action, GH influences distribution of adipose tissue among different depots. These actions are exemplified by striking increase of adiposity in GH-resistant GHRKO mice (particularly males) with preferential accumulation of white adipose tissue (WAT) in the subcutaneous depot with less pronounced and genetic background-dependent accumulation of WAT in the intra-abdominal (visceral) depots (Berryman et al. 2004, 2010; Masternak et al. 2012; Menon et al. 2014). Importantly, GH influences not only the amount and distribution of WAT but also its function including increased secretion of pro-inflammatory cytokines and reduced secretion of adiponectin (Berryman et al. 2004; Masternak et al. 2012). Moreover, GH influences the amount and the activity of brown adipose tissue (BAT) (Darcy and Bartke 2017; Darcy et al. 2016). Surprisingly, despite increased accumulation of adipose tissue in either Ames dwarf or GHRKO mice, these long-living animals maintain high insulin sensitivity (Masternak et al. 2012; Menon et al. 2014; Berryman and List 2017). The studies with surgical visceral fat removal indicated that removing visceral WAT improves insulin sensitivity and glucose tolerance in normal animals only, while the same surgical procedure had negative effects on insulin sensitivity and glucose clearance in metabolically healthy GHRKO or Ames dwarf animals (Masternak et al. 2012; Menon et al. 2014). Yet another study showed that transplanting intra-abdominal WAT from GHRKO mice into visceral cavity of normal littermates caused improvements of glucose tolerance and enhanced tissue specific insulin sensitivity in transplant recipient animals (Bennis et al. 2017). These important findings indicated that GH deficiency or resistance promotes increased adiposity; however, the suppression of GH signaling in fat tissue enhances insulin sensitivity and improves metabolic function of intra-abdominal fat in these long-living animals (Bennis et al. 2017).
Metabolic actions of the somatotropic axis also include major impacts of both GH and IGF-1 on glucose homeostasis. Actions of these hormones on carbohydrate metabolism are, again, largely opposite. IGF-1 mimics and augments insulin actions acting via the same intracellular signaling pathway involving insulin receptor substrates and Akt leading to enhanced insulin sensitivity and reduced blood glucose levels. In contrast, GH actions are primarily anti-insulinemic leading to insulin resistance and hyperglycemia. Thus GH, along with glucagon, glucocorticoids, and catecholamines, plays a role of a “counter-regulatory” hormone in glucose homeostasis. Another level of complexity in the impact of the somatotropic axis on carbohydrate and lipid metabolism is related to stimulatory actions of both GH and IGF-1 on the development of pancreatic beta cells. These complex relationships are well illustrated by the demonstration that GH-resistant and GH-deficient mice are hypo-insulinemic, remarkably insulin sensitive and either euglycemic or mildly hypo-glycemic (Bartke 2017, 2019; Masternak et al. 2018). In addition to these actions, GH was also shown to affect mitochondrial substrate utilization and energy metabolism (Westbrook et al. 2009; Bartke and Westbrook 2012).
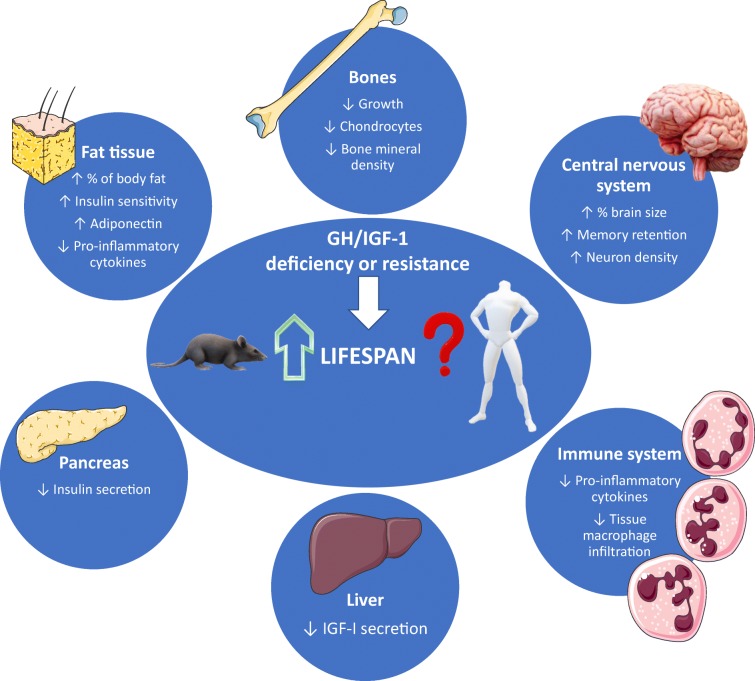
Overall, the studies of animals and humans with dwarfism showed several phenotypic and physiological similarities; however, while GH deficiency or resistance in different laboratory animal models showed significant lifespan extension, there is still lack of consensus in regard to potential impact of suppression of GH/IGF-1 on human longevity and process of aging (Fig. 1).
Fig. 1.
The effects of GH deficiency or resistance on aging
CNS function in long-lived dwarf mice with GH deficiency
Like in humans, circulating GH and IGF-1 levels decline with age in rodents. In addition, IGF-1 levels have been found to be decreased in the CNS of older rats (Sonntag et al. 2012). However, despite low overall GH/IGF-1 levels, old Ames dwarf mice have elevated levels of GH and IGF-1 in the hippocampus and similar concentrations of corresponding mRNAs to those observed in normal mice (Sun et al. 2005b). Sun et al. (2005a, b) found that Ames dwarf mice had an increased number of dividing cells in the subgranular zone (SGZ) of the dentate gyrus in the hippocampus. In addition to an increase in the number of dividing cells, dwarf animals also demonstrated an increased number of newly generated cells and newborn neurons (Sun et al. 2005b). Furthermore, a comparative analysis of CNS populations in GHRKO mice found, despite their reduced brain size, these animals had a higher ratio of neurons to glia than wild-type mice and did not differ significantly in neuron density (Ransome et al. 2004). Finally, Sanz et al. (2002) reported that Ames dwarf mice had lower levels of 8-oxodG, indicating reduced levels of mitochondrial DNA (mtDNA) damage in their brains. After comparing to sex-matched controls, 8-oxodG concentrations in the Ames dwarf mice were 36% lower in females and 32% lower in male dwarf animals (Sanz et al. 2002).
Collectively, such studies raise important questions: How can we reconcile the apparently conflicting roles of the GH/IGF-1 axis in CNS function? Are the beneficial and detrimental effects of GH and IGF-1 on the aging brain context dependent?
GH and cognition
As discussed above, human observational studies have suggested a beneficial relationship between GH and cognition. However, clinical administration of GH to counteract functional decline is not considered an appropriate intervention except in cases of GHD. GH therapy has undesirable side effects including arthralgias, edema, insulin resistance, carpal tunnel syndrome, and increased cancer risk (Bartke 2008). In addition, while some studies have found short-term GH therapy improves memory or cognition (Sonntag et al. 2000), the totality of the data does not clearly indicate that GH treatment is beneficial, and data from rodents actually suggests the opposite—GHD and GHRD mice, which have longer life expectancies than wild-type, also perform better on cognitive tasks (Masternak and Bartke 2012). Furthermore, three prominent models of GH signaling disruption—Snell dwarf, Ames dwarf, and GHRKO mice—all suggest reduced GH/IGF-1 is beneficial to the CNS. Furthermore, a preliminary report published by Shevah & Laron (2007) found that of 222 patients surveyed with congenital IGF-1 deficiencies (LS GH gene deletion, GH releasing hormone receptor defects, and IGF-1 resistance), had no cancer whereas 9-24% of their family members had a medical history of malignant tumors [82].
GH deficiency and the brain: evidence for a beneficial relationship
GH deficiency, aging, and cognition in rodents
A foundational study by Kinney et al. (2001a, b) found that Ames dwarf mice not only age at different rates than their normal siblings, but also perform better in learning and memory tasks. Older Ames dwarf mice exhibit higher levels of locomotor activity, as measured by the elevated plus maze and inhibitory avoidance test, compared to younger dwarf animals. In addition, old Ames dwarf mice performed the same as young, normal mice on the elevated plus maze (Kinney et al. 2001b). More recently, Basu et al. found a similar trend in GHR antagonist (GHA) transgenic mice, indicating benefits of a decrease in GH action are not exclusive to the Ames dwarf model (Basu et al. 2017). In this study, the GHA dwarf transgenic mouse strain was generated and tested alongside another mouse model, bovine GH transgenic (bGH) mice. bGH mice exhibit increased GH secretion due to expression of a bovine GH transgene, and they mimic human gigantism and many features of acromegaly, conditions of GH excess which result in reduced life expectancy. GHA mice had better cognitive performance than bGH mice, suggesting increased GH action negatively affects cognition. Specifically, in the Barnes maze and open field test, bGH mice exhibited significantly reduced exploration and retention times, while latency, path length, and number of errors were increased. On the other hand, GHA mice exhibited normal or better spatial learning and memory. GHA mice not only showed significantly shorter latency to reach the target, but also exhibited better learning capacity in making direct searches. Long-term retention of spatial memory was also significantly enhanced in GHA mice compared to wild-type. In summary, these data suggest reduced GH action is more beneficial to learning and memory then GH excess (Basu et al. 2017).
Kinney et al. also found benefits of reduced GH action in GHRKO mice. To measure cognitive aging in control and GHRKO mice, researchers employed the inhibitory avoidance task. Interestingly, old wild-type mice exhibited a decline in memory retention while old GHRKO mice showed no decline, leading the authors to conclude GH resistance works through an unknown mechanism to promote better long-term memory in these LS mice (Kinney et al. 2001a).
To elucidate possible physiological differences between GHRKO mice and controls, a more recent study examined differences in cognition and glutamatergic signaling (Hascup et al. 2017). Older female GHRKO mice and age-matched controls (20–24 months) underwent cognitive assessments, in vivo glutamatergic recordings, and histological analysis of brain tissue. Mice were subjected to the Morris Water Maze (MWM) test as part of their cognitive battery. Consistent with results from other studies in dwarf models, GHRKO mice demonstrated superior memory retention after a 48-h delay. Because the glutamatergic system is crucial to aging, age-related cognitive decline, and cognitive disorders, this study also examined basal glutamate levels and stimulus-evoked glutamate release and uptake in three different regions of the hippocampus. In the dentate gyrus (DG), basal glutamate was elevated in controls compared with GHRKO mice, and a negative correlation was found between basal glutamate levels in the CA3 region of the hippocampus and path efficiency while completing the MWM (Hascup et al. 2017). In addition, glial fibrillary acidic protein (GFAP) was used as an indicator of astrocytes, which are predominantly responsible for maintenance of glutamate in the CNS. Compared to littermate controls, GHRKO mice exhibited increased GFAP density in the DG, indicating these mice have more glia, and therefore, greater capacity to clear glutamate from the hippocampus. Furthermore, Vesicular Glutamate Transporter (VGLUT) 1, which is responsible for transport of glutamate in the excitatory terminals of the hippocampus, was lower in the DG of littermates. Taken together, these studies support the notion that a decrease in GH action is beneficial to maintaining CNS integrity and function during aging.
GH deficiency, aging, and cognition in humans
Studies have correlated declining levels of GH during aging in humans with negative effects on brain function and cognition. For example, Aleman et al. (Aleman et al. 1999) reported an association between low levels of GH/IGF-1 and decreased perceptual motor performance and information processing speed in participants 65–76 years of age. In addition, high levels of IGF-1/IGF binding proteins were associated with better maintenance of cognition (Kalmijn et al. 2000), and a similar correlation was noted among centenarians (Paolisso et al. 1997). By contrast, a recent study in GHD subjects from Nashiro et al. compared brain structure, function, white matter integrity, hippocampal volume, cortical thickness, and surface area in select brain regions in the brain of 13 GHD individuals and 12 unaffected relatives. Using a pattern separation task, participants’ resting brain activity was also evaluated. Following whole brain analysis, researchers determined GHRD patients had greater activation in the bilateral superior frontal gyrus. In addition, those in the GHD group exhibited greater activation in the left superior lobe and left frontal pole. After responses to the pattern separation task were controlled for age, sex, and education, GHRD participants had greater separation bias scores than controls, a pattern of group difference that had previously been observed in younger adults. Furthermore, the GHRD group showed greater functional synchronicity of activity between regions of the brain, such as the precuneus and left and right hippocampi, indicating healthier brain function. Thus, GHRD participants have preserved brain structure and function similar to that seen in much younger adults (Nashiro et al. 2017).
Based on accumulating evidence that GH might play a crucial role in modulating aging, studies have begun to examine the GHR gene and its isoforms. A recent study analyzed the potential roles in human longevity of two isoforms of GHR (full length and a shorter form with a deletion in exon 3). Researchers genotyped the d3-GHR locus (participants with the deleted GHR isoform) in four human cohorts with long-lived participants (Longevity Genes Project, Old Order Amish, Cardiovascular Health Study, and French Long-lived study) and tested its association with longevity-related phenotypes and stature (Ben-Avraham et al. 2017). The Longevity Genes Project was made up of the Ashkenazi Jew (AJ) centenarian cohort. The AJ cohort consisted of three groups in this study: centenarians, their offspring, and controls. The other three cohorts in the study were used for validation. The percentage of d3-GHR homozygosity among male centenarians was significantly higher than controls. Results in the other three cohorts suggested a similar trend as homozygosity for d3-GHR increased with age among males in the Old Order Amish (OOA) cohort and French Long-lived cohort. Additionally, homozygosity increased in percentage with age in the Cardiovascular Health study, but this numerical difference was not significant (P = 0.14). Researchers then conducted a meta-analysis, which included males from all four cohorts, and found that d3-GHR homozygosity also showed a significant increase with age, suggesting sexual dimorphism for GH action in longevity. Multivariate regression analysis indicated the d3/d3 genotype was associated with ten additional lifespan years. It is also important to note, when compared to wild-type lymphocytes, the d3/d3-GHR-transformed lymphocytes demonstrated superior growth and extracellular signal-regulated kinase activity. Thus, researchers concluded the d3-GHR variant is a common polymorphism that modulates GH responsiveness throughout an individual’s lifespan and has positive effects on male longevity (Ben-Avraham et al. 2017). Such an observation is unique among dwarf models, which generally do not show a sex difference, and among IGF-1R haploinsufficient mice, humans with functional mutations in the IGF-1R, and nonagenarians with low IGF-1 levels, in which effects appear to be female specific (van Heemst et al. 2005; Ashpole et al. 2017).
GH replacement and aging: weighing the evidence
Age-related decline in the GH/IGF-1 axis, also known as somatopause, has inspired numerous studies aimed at investigating whether GH therapy can prevent or reverse aging. In an initial study by Rudman et al., male subjects (> 65 years old) with reduced IGF-1 levels received GH therapy and markers of aging were monitored. After 6 months of GH treatment, participants showed reduced adiposity, increased muscle mass, and increased bone density (Rudman et al. 1990). However, despite this initial promising result, several subsequent studies could not consistently replicate these outcomes. Further studies identified negative side effects of GH treatment including joint pain, edema, carpal tunnel syndrome, increased risk of metabolic syndrome, diabetes, and cancer (Blackman et al. 2002; Liu et al. 2007; Swerdlow et al. 2017; Boguszewski et al. 2016). However, a study by Ramsey et al. reported positive outcomes similar to the initial study and revealed GH could potentially alleviate age-related changes in metabolic characteristics, brain vascularity, and cognitive function in older rats (Ramsey et al. 2004).
Studies of patients with isolated GHD suggest GH is crucial for healthy aging and longevity. For example, a study compared outcomes of 11 GHD subjects from an isolated valley in Switzerland who had never been treated for their deficiency, their relatives, and 100 males and females from the normal population. Although cause of death did not vary among groups, the median lifespan of GHD subjects was significantly shorter than their siblings (Besson et al. 2003). Importantly, although not statistically significant in this study, differences were observed between GH-deficient males and females. GH-deficient males lived longer than GH-deficient females, while among relatives and the normal population, females lived longer than males (Besson et al. 2003).
While some studies have advocated for GH therapy, others have found GH replacement in mice can have undesirable effects on aging and longevity (Sun et al. 2017) (Vergara et al. 2004). For example, a study of Snell dwarf mice found GH treatment and thyroxine treatment restored fertility in male Snell mice and increased weight by 45% without affecting longevity or disease resistance (Vergara et al. 2004). By contrast, a study of Ames dwarf mice reported negative effects of early-life GH treatment (Sun et al. 2017). Ames dwarf and littermate controls were treated with GH from 1 to 7 weeks of age and left untreated for the remainder of their lifespan. Short-term exposure to GH reduced median lifespan in dwarf mice, compared to their untreated counterparts. However, this overall decrease in survival was specific to males, as no significant life-shortening effect was observed in females, suggesting sex dimorphism in the response to early postnatal GH (and IGF-1) exposure. Furthermore, phenotypic characteristics were found to be altered in mice treated with GH. Metabolic testing after treatment revealed that following early-life GH exposure, 18-month-old dwarf mice had completely lost the ability to increase O2 consumption. The respiratory exchange ratio, which is an indicator of fuel utilization, was increased in treated dwarf mice, indicating mice were less efficient at using fat as an energy substrate. Early-life GH treatment also led to increased insulin and glucose levels at older ages, while adiponectin levels, which are reflective of insulin sensitivity, were no longer upregulated in GH-treated mice. Finally, GH exposure had significant effects on hepatic stress response pathways and expression of inflammation genes and hypothalamic markers of inflammation such as Jun N-terminal kinase (JNK) and NF-kB. These results suggest developmental programming of aging by early-life exposure to growth signals contributes to developmental origins of adult disease (Sun et al. 2017).
Regarding GH and the brain, GH treatment has been shown to protect from age-related decline in the ratio of ionotropic glutamatergic NMDA receptor subunits (NR1 and NR2) in both young and old male rats. Furthermore, the observed GH-induced increase in hippocampal mRNA supported a previous study, which reported over-expression of the NR2 subunit enhanced cognition (Le Greves et al. 2002). Spatial memory tests are a commonly used tool in GH treatment studies aimed at studying the correlation between GH and attenuation of age-related deficits. Thornton et al. (2000) conducted a study using the MWM and place discrimination testing to assess spatial learning in 6-month-old and 28-month-old rats. Prior to testing, animals were injected with GHRH or saline. While no changes were noted in sensory motor performance, administration of GHRH improved MWM performance compared to controls. GHRH was also found to attenuate decline in concentrations of IGF-1 that are typically observed in elderly animals (Thornton et al. 2000). However, the results did not indicate improvements in learning in the animals, a contradiction that was not fully explained.
A study Baum et al. (1998) sought to evaluate effects on learning and cognition by administering GH to patients diagnosed with adult-onset GHD. For a period of 18 months, GH replacement therapy was provided, and effects of the treatment were assessed using cognitive testing. The investigators concluded there were no improvements in cognitive function following GH replacement (Baum et al. 1998). While previous studies had suggested GH replacement could improve quality of life in GHD patients, researchers in this study were unable to come to a similar conclusion.
Effects of GH on cognition have also been studied in populations of healthy, older adults (Vitiello et al. 2006). A group of 89 healthy patients were administered GHRH over a 6-month treatment period. Cognitive assessments included tests in which results are known to decline with advancing age: Weschler Adult Intelligence Scale (WAIS) performance, single-dual task, and verbal sets. Overall, results of the study were found to be independent of gender, estrogen status, or baseline cognitive capacity, and showed GHRH treatment significantly improved cognitive function in the healthy adults. Novel problem-solving tasks, cognitive speed, and working memory all showed significant improvements after GHRH treatment. However, out of the six cognitive tests used, three cognitive tasks (category fluency, verbal fluency, and WAIS-R vocabulary) showed no change with GHRH treatment. The authors proposed this could be due to a “ceiling effect” often observed in crystallized intelligence.
In a placebo-controlled 12-month study conducted in older patients with adult-onset GHD, positive results were not as evident (Sathiavageeswaran et al. 2007). To assess cognitive function in elderly GH therapy naïve patients, researchers administered either GH therapy or placebo in a double-blind study. After 24 weeks, results showed GH had discrete benefits on cognition in older GHD adults. Among the battery or cognitive assays performed, differences in performance between the GH group and placebo group were only significant for serial digit learning error. Thus, researchers were unable to determine definitively whether GH therapy in these subjects was entirely beneficial. However, they concluded GH therapy replacement may be accompanied by improvement in certain measures of cognitive function (Sathiavageeswaran et al. 2007).
In another case report of GH administration, it was found that GH treatment might help counteract cognitive deficits during neurorehabilitation in children with brain damage suffered during delivery (Devesa et al. 2016b). GH was administered to a non-GHD 10-year-old patient at doses of 0.5 mg for 3 months, 0.9 mg every 2 weeks for 3 months, 1.2 mg 3 days a week, and 0.3 mg 2 days a week. The patient was provided neurorehabilitation therapy for 9 months in the form of neurostimulation, speech therapy, occupational therapy, and auditory stimulation. At discharge, the patient had increased cognitive abilities, memory and language competency, intelligence quotient, and index of functional independence. While the overall conclusion of the study suggested neurorehabilitation due to GH therapy, the researchers were unable to define what percentages of the positive effects observed were due to GH, neurorehabilitation, or both. Because there was only one patient and no controls, a controlled trial would be necessary to establish a stronger correlation between GH and neurorehabilitation (Devesa et al. 2016b).
The proposed action of GH treatment on aging, particularly the aging brain, has raised questions about its potential role in treating adults with mild cognitive impairment (MCI) or Alzheimer’s disease. To test the effects of GHRH on cognitive function in older adults and adults with MCI, a randomized, double-blind, placebo-controlled trial was conducted. In this trial, participants self-administered subcutaneous injections of a stabilized analogue of GHRH. After 20 weeks of treatment, cognitive results were assessed using scores from executive function, verbal memory, and visual memory tests. GHRH treatment was found to have positive metabolic and cognitive effects. Specifically, GHRH increased IGF-1 levels by 117%, reduced body fat percentage by 7.4%, and increased fasting insulin levels within the normal range by 35% in adults with MCI. Similarly, GHRH treatment had a positive effect on executive function and could possibly have a similar effect on verbal memory. In addition, significant and favorable effects of treatment were observed in healthy adults and adults with MCI. Although side effects were mild, the GHRH-treated adults reported 68% of these effects. Researchers concluded that, based on the favorable effects observed on cognition in both groups, longer-duration study trials were needed to examine the therapeutic potential of GHRH (Baker et al. 2012).
To follow-up on findings and examine neurochemical effects of GHRH, the same researchers conducted another randomized, double-blind, placebo-controlled sub-study with a similar design (Friedman et al. 2013). Participants in this study underwent brain MRI, cognitive testing, glucose tolerance tests, and provided fasting blood samples before and after treatment. Consistent with the results from the parent study, GHRH treatment had a significant positive effect on cognition. In addition, inhibitory transmitter (GABA and NAAG) levels were increased in all tested brain regions of the dorsolateral frontal cortex in older adults with normal cognitive function and in adults with MCI. In summary, these confirmatory findings suggest GHRH could have a role in alleviating age-related declines in brain and synaptic function (Friedman et al. 2013). However, in a study of AD patients receiving GH secretagogues, there was no evidence of slowed progression of AD-like symptoms at follow-up (Sevigny et al. 2008).
Neurochemical effects of GH on cognitive dysfunction have also been studied in a controlled cortical impact (CCI) rat model of traumatic brain injury (Zhang et al. 2014). Three-month-old rats were tested for synaptophysin (SYN), a protein involved in vesicle import, transit, and neurotransmitter release, and Brain Derived Neurotrophic Factor (BDNF) and TrkB, which are associated with neuronal survival and synaptic function, respectively. Recombinant human GH (rhGH) was delivered to CCI rats 8 weeks post-injury for a period of 2 weeks. Researchers reported that rhGH treatment resulted in improved cognitive function in CCI rats. In addition, they observed a positive correlation between BDNF and SYN expression after therapy and water maze test scores. Finally, rhGH treatment had a positive effect on cognitive function as evidenced by increased expression of hippocampal and prefrontal BDNF and TrkB mRNA after treatment (Zhang et al. 2014). Interpretation of the available data is complicated by the possibility that GHRH may affect some of the examined response parameters by mechanisms not mediated by increased GH secretion and by the well-documented ability of human GH to signal through both GH receptors and prolactin receptors in rodents (Bartke and Kopchick 2015).
Despite the fact that GH has not been approved for anti-aging therapy by FDA, its use for this indication is widespread and increasing. Until future clinical research in this area is conducted, in particular carefully designed, long-term studies, the Growth Hormone Research Society cannot recommend normal, older adults use GH or GH secretagogues (GHS), alone or in combination with testosterone (Thorner 2009).
Conclusions
The debate over GH therapy in the elderly, which began in 1990 with the seminal work by Rudman et al., remains unsettled. As discussed in this review, research and clinical studies of GH therapy have produced ambiguous and often contradictory data. Positive results of GH therapy trials have led to GH gaining traction in some circles as an “anti-aging” therapy. In fact, a systematic review found use of GH as an anti-aging therapy was one of the most popular health-related internet searches (Liu et al. 2007). In addition, an estimated 20,000 to 30,000 people used GH as an anti-aging therapy in 2004 and annual sales of GH worldwide exceed $1.5 billion (Perls et al. 2005).
Proponents of GH therapy argue that because GH promotes health and vitality in younger individuals, and its levels decline with age, replenishing levels of GH can not only mitigate aging, but reverse negative effects of age-related processes and diseases. However, the body of scientific evidence suggests constitutive GHD is more beneficial for overall health and longevity than excess GH. Furthermore, well-established side effects of GH have discouraged the use of GH as an anti-aging treatment. Clearly, more information is needed to make definitive conclusions about the effect of GH on the aging body and to establish whether older adults or adults with cognitive impairment should undergo GH treatments.
GH administration studies often find patients have improved body composition, lipid levels, adiposity, and bone mineral density. However, many of these studies have been small-sample, short-duration studies with no placebo controls and results have not always been reliable or significant. In fact, successful GH administration studies have been, on average, no longer than 6 months with the exception of a one-person case study that lasted 9 months and claimed positive results but admitted direct causality was difficult to establish. Of the studies analyzed in this review, longer-duration GH therapy studies have been unable to find robust evidence supporting efficacy of GH administration (Baum et al. 1998; Sathiavageeswaran et al. 2007), which calls into question claims that GH therapy is beneficial in humans, except for patients with established GHD.
A review by Liu et al. (2007), which set out to evaluate the safety and efficacy of GH therapy in the healthy elderly, analyzed 31 articles for significant effects of GH administration. After review of these articles, which described 18 unique studies and included 220 participants, researchers concluded GH therapy could not be recommended as an anti-aging therapy based on the fact that risks of treatment seemed to outweigh benefits (Liu et al. 2007).
It is important to note that sex differences are a vital aspect of this axis that should always be considered, while onset of deficiency seems to be another important consideration. Furthermore, many GH transgenic and replacement models result in excess GH, that is not pulsatile in nature and that use of supraphysiological doses of GH, which also needs to be considered. Additional studies will be needed to evaluate risks and benefits of treatment with novel long-acting GH preparations in elderly humans without established GHD. Potential anti-aging benefits of treatment with analogs or mimetics of ghrelin, which produce a more physiological profile of circulating GH than can be achieved with once-daily rhGH injections (Nass et al. 2008), also remain to be evaluated. Finally, there could be a “time window” in development where GH would be more effective or less harmful.
Clearly, the role of GH deficiency or excess in aging, and in what context(s) it should be treated or modulated, is highly complex and will require additional studies that account for many variables including sex, dose, timing, tissue specificity, and duration of treatment as modifiers of the response. Adding to the complexity, additional therapeutic options are now available (e.g., GH short versus long acting, GHRH, and GH antagonist), which could allow subtler and more sustained modulation of GH action than has been previously tested. Collectively, these studies are needed to clarify whether modulation of GH action can be successfully harnessed to improve quality of life, combat disease, improve brain function, and increase life expectancy in humans.
Funding information
This work was supported by NIH grants AG059190 (M. M. M.), AG059846 (M. M. M.), AG13925 (J.L.K.), AG041122 (J.L.K.), AG31736 (Project 4: J.L.K.), and AG044396 (J.L.K.), Robert and Arlene Kogod, the Connor Group (J.L.K.), Robert J. and Theresa W. Ryan (J.L.K.), and the Ted Nash Long Life (J.L.K.) and Noaber Foundations (J.L.K.). N.M. is supported by a grants from the American Diabetes Association (7-13-GSK-01), the National Institutes of Health (AG030979, DK80157, DK089229, and DK080157), the San Antonio Nathan Shock Center (AG013319), and the San Antonio Claude D. Pepper Older Americans Independence Center (AG044271). Pathology Core in the San Antonio Nathan Shock Center: P30-AG013319 (Y. I.) also supported this work. D.M.H. is supported by AG037574, AG055026, AG057429; the American Federation for Aging Research (AFAR); and the Einstein Nathan Shock Center (P30 AG038072).
Footnotes
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
References
- Aguiar-Oliveira MH, Bartke A. Growth hormone deficiency: health and longevity. Endocr Rev. 2019;40(2):575–601. doi: 10.1210/er.2018-00216. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Aleman A, et al. Insulin-like growth factor-I and cognitive function in healthy older men. J Clin Endocrinol Metab. 1999;84(2):471–475. doi: 10.1210/jcem.84.2.5455. [DOI] [PubMed] [Google Scholar]
- Ashpole NM, et al. Growth hormone, insulin-like growth factor-1 and the aging brain. Exp Gerontol. 2015;68:76–81. doi: 10.1016/j.exger.2014.10.002. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Ashpole NM, et al. IGF-1 has sexually dimorphic, pleiotropic, and time-dependent effects on healthspan, pathology, and lifespan. Geroscience. 2017;39(2):129–145. doi: 10.1007/s11357-017-9971-0. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Baker LD, et al. Effects of growth hormone-releasing hormone on cognitive function in adults with mild cognitive impairment and healthy older adults: results of a controlled trial. Arch Neurol. 2012;69(11):1420–1429. doi: 10.1001/archneurol.2012.1970. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Balasubramanian P, Hall D, Subramanian M. Sympathetic nervous system as a target for aging and obesity-related cardiovascular diseases. Geroscience. 2019;41(1):13–24. doi: 10.1007/s11357-018-0048-5. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Bartke A. Minireview: role of the growth hormone/insulin-like growth factor system in mammalian aging. Endocrinology. 2005;146(9):3718–3723. doi: 10.1210/en.2005-0411. [DOI] [PubMed] [Google Scholar]
- Bartke A. Growth hormone and aging: a challenging controversy. Clin Interv Aging. 2008;3(4):659–665. doi: 10.2147/cia.s3697. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Bartke A. Somatic growth, aging, and longevity. NPJ Aging Mech Dis. 2017;3:14. doi: 10.1038/s41514-017-0014-y. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Bartke A. Growth hormone and aging: updated review. World J Mens Health. 2019;37(1):19–30. doi: 10.5534/wjmh.180018. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Bartke A, Kopchick JJ. The forgotten lactogenic activity of growth hormone: important implications for rodent studies. Endocrinology. 2015;156(5):1620–1622. doi: 10.1210/en.2015-1097. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Bartke A, Westbrook R. Metabolic characteristics of long-lived mice. Front Genet. 2012;3:288. doi: 10.3389/fgene.2012.00288. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Bartke A, et al. Extending the lifespan of long-lived mice. Nature. 2001;414(6862):412. doi: 10.1038/35106646. [DOI] [PubMed] [Google Scholar]
- Basu A, McFarlane HG, Kopchick JJ. Spatial learning and memory in male mice with altered growth hormone action. Horm Behav. 2017;93:18–30. doi: 10.1016/j.yhbeh.2017.04.001. [DOI] [PubMed] [Google Scholar]
- Baum HB, et al. Effects of physiological growth hormone (GH) therapy on cognition and quality of life in patients with adult-onset GH deficiency. J Clin Endocrinol Metab. 1998;83(9):3184–3189. doi: 10.1210/jcem.83.9.5112. [DOI] [PubMed] [Google Scholar]
- Ben-Avraham D, et al. The GH receptor exon 3 deletion is a marker of male-specific exceptional longevity associated with increased GH sensitivity and taller stature. Sci Adv. 2017;3(6):e1602025. doi: 10.1126/sciadv.1602025. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Bennis MT, et al. The role of transplanted visceral fat from the long-lived growth hormone receptor knockout mice on insulin signaling. Geroscience. 2017;39(1):51–59. doi: 10.1007/s11357-017-9957-y. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Berryman Darlene, List Edward. Growth Hormone’s Effect on Adipose Tissue: Quality versus Quantity. International Journal of Molecular Sciences. 2017;18(8):1621. doi: 10.3390/ijms18081621. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Berryman DE, et al. Comparing adiposity profiles in three mouse models with altered GH signaling. Growth Hormon IGF Res. 2004;14(4):309–318. doi: 10.1016/j.ghir.2004.02.005. [DOI] [PubMed] [Google Scholar]
- Berryman DE, et al. Two-year body composition analyses of long-lived GHR null mice. J Gerontol A Biol Sci Med Sci. 2010;65(1):31–40. doi: 10.1093/gerona/glp175. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Besson A, et al. Reduced longevity in untreated patients with isolated growth hormone deficiency. J Clin Endocrinol Metab. 2003;88(8):3664–3667. doi: 10.1210/jc.2002-021938. [DOI] [PubMed] [Google Scholar]
- Blackman MR, et al. Growth hormone and sex steroid administration in healthy aged women and men: a randomized controlled trial. JAMA. 2002;288(18):2282–2292. doi: 10.1001/jama.288.18.2282. [DOI] [PubMed] [Google Scholar]
- Boguszewski CL, Boguszewski MC, Kopchick JJ. Growth hormone, insulin-like growth factor system and carcinogenesis. Endokrynol Pol. 2016;67(4):414–426. doi: 10.5603/EP.a2016.0053. [DOI] [PubMed] [Google Scholar]
- Bonkowski MS, et al. Disruption of growth hormone receptor prevents calorie restriction from improving insulin action and longevity. PLoS One. 2009;4(2):e4567. doi: 10.1371/journal.pone.0004567. [DOI] [PMC free article] [PubMed] [Google Scholar] [Retracted]
- Brod M, et al. Impact of adult growth hormone deficiency on daily functioning and well-being. BMC Res Notes. 2014;7:813. doi: 10.1186/1756-0500-7-813. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Cuneo RC, et al. The growth hormone deficiency syndrome in adults. Clin Endocrinol. 1992;37(5):387–397. doi: 10.1111/j.1365-2265.1992.tb02347.x. [DOI] [PubMed] [Google Scholar]
- Darcy J, Bartke A. Functionally enhanced brown adipose tissue in Ames dwarf mice. Adipocyte. 2017;6(1):62–67. doi: 10.1080/21623945.2016.1274470. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Darcy J, et al. Brown adipose tissue function is enhanced in long-lived, male Ames dwarf mice. Endocrinology. 2016;157(12):4744–4753. doi: 10.1210/en.2016-1593. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Devesa J, Almenglo C, Devesa P. Multiple effects of growth hormone in the body: is it really the hormone for growth? Clin Med Insights Endocrinol Diabetes. 2016;9:47–71. doi: 10.4137/CMED.S38201. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Devesa Jesús, Lema Hortensia, Zas Eva, Munín Borja, Taboada Pilar, Devesa Pablo. Learning and Memory Recoveries in a Young Girl Treated with Growth Hormone and Neurorehabilitation. Journal of Clinical Medicine. 2016;5(2):14. doi: 10.3390/jcm5020014. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Dominici FP, et al. Increased insulin sensitivity and upregulation of insulin receptor, insulin receptor substrate (IRS)-1 and IRS-2 in liver of Ames dwarf mice. J Endocrinol. 2002;173(1):81–94. doi: 10.1677/joe.0.1730081. [DOI] [PubMed] [Google Scholar]
- Donahue CP, Kosik KS, Shors TJ. Growth hormone is produced within the hippocampus where it responds to age, sex, and stress. Proc Natl Acad Sci U S A. 2006;103(15):6031–6036. doi: 10.1073/pnas.0507776103. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Evans HM, Long JA. Characteristic effects upon growth, oestrus and ovulation induced by the intraperitoneal administration of fresh anterior hypophyseal substance. Proc Natl Acad Sci U S A. 1922;8(3):38–39. doi: 10.1073/pnas.8.3.38. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Farias Quipildor GE, et al. Central IGF-1 protects against features of cognitive and sensorimotor decline with aging in male mice. Geroscience. 2019;41(2):185–208. doi: 10.1007/s11357-019-00065-3. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Feldt-Rasmussen U, Klose M. Central hypothyroidism and its role for cardiovascular risk factors in hypopituitary patients. Endocrine. 2016;54(1):15–23. doi: 10.1007/s12020-016-1047-x. [DOI] [PubMed] [Google Scholar]
- Friedman SD, et al. Growth hormone-releasing hormone effects on brain gamma-aminobutyric acid levels in mild cognitive impairment and healthy aging. JAMA Neurol. 2013;70(7):883–890. doi: 10.1001/jamaneurol.2013.1425. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Gilchrist FJ, Murray RD, Shalet SM. The effect of long-term untreated growth hormone deficiency (GHD) and 9 years of GH replacement on the quality of life (QoL) of GH-deficient adults. Clin Endocrinol. 2002;57(3):363–370. doi: 10.1046/j.1365-2265.2002.01608.x. [DOI] [PubMed] [Google Scholar]
- Guevara-Aguirre J, et al. Growth hormone receptor deficiency is associated with a major reduction in pro-aging signaling, cancer, and diabetes in humans. Sci Transl Med. 2011;3(70):70ra13. doi: 10.1126/scitranslmed.3001845. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Guevara-Aguirre J, et al. GH receptor deficiency in Ecuadorian adults is associated with obesity and enhanced insulin sensitivity. J Clin Endocrinol Metab. 2015;100(7):2589–2596. doi: 10.1210/jc.2015-1678. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Hascup KN, et al. Enhanced cognition and hypoglutamatergic signaling in a growth hormone receptor knockout mouse model of successful aging. J Gerontol A Biol Sci Med Sci. 2017;72(3):329–337. doi: 10.1093/gerona/glw088. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Hulthen L, et al. GH is needed for the maturation of muscle mass and strength in adolescents. J Clin Endocrinol Metab. 2001;86(10):4765–4770. doi: 10.1210/jcem.86.10.7897. [DOI] [PubMed] [Google Scholar]
- Ikeno Y, et al. Delayed occurrence of fatal neoplastic diseases in Ames dwarf mice: correlation to extended longevity. J Gerontol A Biol Sci Med Sci. 2003;58(4):291–296. doi: 10.1093/gerona/58.4.b291. [DOI] [PubMed] [Google Scholar]
- Janssen YJ, Doornbos J, Roelfsema F. Changes in muscle volume, strength, and bioenergetics during recombinant human growth hormone (GH) therapy in adults with GH deficiency. J Clin Endocrinol Metab. 1999;84(1):279–284. doi: 10.1210/jcem.84.1.5411. [DOI] [PubMed] [Google Scholar]
- Johannsson G, et al. GH increases extracellular volume by stimulating sodium reabsorption in the distal nephron and preventing pressure natriuresis. J Clin Endocrinol Metab. 2002;87(4):1743–1749. doi: 10.1210/jcem.87.4.8394. [DOI] [PubMed] [Google Scholar]
- Jorgensen JO, et al. Growth hormone versus placebo treatment for one year in growth hormone deficient adults: increase in exercise capacity and normalization of body composition. Clin Endocrinol. 1996;45(6):681–688. doi: 10.1046/j.1365-2265.1996.8720883.x. [DOI] [PubMed] [Google Scholar]
- Kalmijn S, et al. A prospective study on circulating insulin-like growth factor I (IGF-I), IGF-binding proteins, and cognitive function in the elderly. J Clin Endocrinol Metab. 2000;85(12):4551–4555. doi: 10.1210/jcem.85.12.7033. [DOI] [PubMed] [Google Scholar]
- Kinney BA, et al. Evidence that age-induced decline in memory retention is delayed in growth hormone resistant GH-R-KO (Laron) mice. Physiol Behav. 2001;72(5):653–660. doi: 10.1016/s0031-9384(01)00423-1. [DOI] [PubMed] [Google Scholar]
- Kinney BA, et al. Evidence that Ames dwarf mice age differently from their normal siblings in behavioral and learning and memory parameters. Horm Behav. 2001;39(4):277–284. doi: 10.1006/hbeh.2001.1654. [DOI] [PubMed] [Google Scholar]
- Labandeira-Garcia JL, et al. Insulin-like growth factor-1 and neuroinflammation. Front Aging Neurosci. 2017;9:365. doi: 10.3389/fnagi.2017.00365. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Laron Z. Do deficiencies in growth hormone and insulin-like growth factor-1 (IGF-1) shorten or prolong longevity? Mech Ageing Dev. 2005;126(2):305–307. doi: 10.1016/j.mad.2004.08.022. [DOI] [PubMed] [Google Scholar]
- Le Greves M, et al. Growth hormone induces age-dependent alteration in the expression of hippocampal growth hormone receptor and N-methyl-D-aspartate receptor subunits gene transcripts in male rats. Proc Natl Acad Sci U S A. 2002;99(10):7119–7123. doi: 10.1073/pnas.092135399. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Lichtenwalner RJ, et al. Intracerebroventricular infusion of insulin-like growth factor-I ameliorates the age-related decline in hippocampal neurogenesis. Neuroscience. 2001;107(4):603–613. doi: 10.1016/s0306-4522(01)00378-5. [DOI] [PubMed] [Google Scholar]
- List EO, et al (2014) Liver-specific GH receptor gene disrupted (LiGHRKO) mice have decreased endocrine IGF-1, increased local IGF-1 as well as altered body size, body composition and adipokine profiles. Endocrinology en20132086 [DOI] [PMC free article] [PubMed]
- Littley MD, et al. Hypopituitarism following external radiotherapy for pituitary tumours in adults. Q J Med. 1989;70(262):145–160. [PubMed] [Google Scholar]
- Liu H, et al. Systematic review: the safety and efficacy of growth hormone in the healthy elderly. Ann Intern Med. 2007;146(2):104–115. doi: 10.7326/0003-4819-146-2-200701160-00005. [DOI] [PubMed] [Google Scholar]
- Logan S, et al. Insulin-like growth factor receptor signaling regulates working memory, mitochondrial metabolism, and amyloid-beta uptake in astrocytes. Mol Metab. 2018;9:141–155. doi: 10.1016/j.molmet.2018.01.013. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Lupu F, et al. Roles of growth hormone and insulin-like growth factor 1 in mouse postnatal growth. Dev Biol. 2001;229(1):141–162. doi: 10.1006/dbio.2000.9975. [DOI] [PubMed] [Google Scholar]
- Markowska AL, Mooney M, Sonntag WE. Insulin-like growth factor-1 ameliorates age-related behavioral deficits. Neuroscience. 1998;87(3):559–569. doi: 10.1016/s0306-4522(98)00143-2. [DOI] [PubMed] [Google Scholar]
- Masternak MM, Bartke A (2012) Growth hormone, inflammation and aging. Pathobiol Aging Age Relat Dis. 2 [DOI] [PMC free article] [PubMed]
- Masternak MM, et al. Divergent effects of caloric restriction on gene expression in normal and long-lived mice. J Gerontol A Biol Sci Med Sci. 2004;59(8):784–788. doi: 10.1093/gerona/59.8.b784. [DOI] [PubMed] [Google Scholar]
- Masternak MM, et al. Metabolic effects of intra-abdominal fat in GHRKO mice. Aging Cell. 2012;11(1):73–81. doi: 10.1111/j.1474-9726.2011.00763.x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Masternak MM, et al. Dwarf mice and aging. Prog Mol Biol Transl Sci. 2018;155:69–83. doi: 10.1016/bs.pmbts.2017.12.002. [DOI] [PubMed] [Google Scholar]
- Menon V, et al. The contribution of visceral fat to improved insulin signaling in Ames dwarf mice. Aging Cell. 2014;13:497–506. doi: 10.1111/acel.12201. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Merola B, et al. Lung volumes and respiratory muscle strength in adult patients with childhood- or adult-onset growth hormone deficiency: effect of 12 months’ growth hormone replacement therapy. Eur J Endocrinol. 1996;135(5):553–558. doi: 10.1530/eje.0.1350553. [DOI] [PubMed] [Google Scholar]
- Modesto Mde J, et al. Muscle strength and body composition during the transition phase in patients treated with recombinant GH to final height. J Pediatr Endocrinol Metab. 2014;27(9–10):813–820. doi: 10.1515/jpem-2013-0317. [DOI] [PubMed] [Google Scholar]
- Moller J, et al. Decreased plasma and extracellular volume in growth hormone deficient adults and the acute and prolonged effects of GH administration: a controlled experimental study. Clin Endocrinol. 1996;44(5):533–539. doi: 10.1046/j.1365-2265.1996.728550.x. [DOI] [PubMed] [Google Scholar]
- Murray PG, Clayton PE (2000) Disorders of growth hormone in childhood [PubMed]
- Nashiro K, et al. Brain structure and function associated with younger adults in growth hormone receptor-deficient humans. J Neurosci. 2017;37(7):1696–1707. doi: 10.1523/JNEUROSCI.1929-16.2016. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Nass R, et al. Effects of an oral ghrelin mimetic on body composition and clinical outcomes in healthy older adults: a randomized trial. Ann Intern Med. 2008;149(9):601–611. doi: 10.7326/0003-4819-149-9-200811040-00003. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Netchine I, et al. Partial primary deficiency of insulin-like growth factor (IGF)-I activity associated with IGF1 mutation demonstrates its critical role in growth and brain development. J Clin Endocrinol Metab. 2009;94(10):3913–3921. doi: 10.1210/jc.2009-0452. [DOI] [PubMed] [Google Scholar]
- Nielsen J, Jensen RB, Afdeling AJ. Growth hormone deficiency in children. Ugeskr Laeger. 2015;177(26):1260–1263. [PubMed] [Google Scholar]
- Nyberg F. Growth hormone in the brain: characteristics of specific brain targets for the hormone and their functional significance. Front Neuroendocrinol. 2000;21(4):330–348. doi: 10.1006/frne.2000.0200. [DOI] [PubMed] [Google Scholar]
- Pan W, et al. Permeation of growth hormone across the blood-brain barrier. Endocrinology. 2005;146(11):4898–4904. doi: 10.1210/en.2005-0587. [DOI] [PubMed] [Google Scholar]
- Paolisso G, et al. Serum levels of insulin-like growth factor-I (IGF-I) and IGF-binding protein-3 in healthy centenarians: relationship with plasma leptin and lipid concentrations, insulin action, and cognitive function. J Clin Endocrinol Metab. 1997;82(7):2204–2209. doi: 10.1210/jcem.82.7.4087. [DOI] [PubMed] [Google Scholar]
- Perls TT, Reisman NR, Olshansky SJ. Provision or distribution of growth hormone for “antiaging”: clinical and legal issues. JAMA. 2005;294(16):2086–2090. doi: 10.1001/jama.294.16.2086. [DOI] [PubMed] [Google Scholar]
- Podlutsky A, et al. The GH/IGF-1 axis in a critical period early in life determines cellular DNA repair capacity by altering transcriptional regulation of DNA repair-related genes: implications for the developmental origins of cancer. Geroscience. 2017;39(2):147–160. doi: 10.1007/s11357-017-9966-x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Quinlan P, et al. Low serum insulin-like growth factor-I (IGF-I) level is associated with increased risk of vascular dementia. Psychoneuroendocrinology. 2017;86:169–175. doi: 10.1016/j.psyneuen.2017.09.018. [DOI] [PubMed] [Google Scholar]
- Ramsey MM, et al. Growth hormone treatment attenuates age-related changes in hippocampal short-term plasticity and spatial learning. Neuroscience. 2004;129(1):119–127. doi: 10.1016/j.neuroscience.2004.08.001. [DOI] [PubMed] [Google Scholar]
- Ransome MI, et al. Comparative analysis of CNS populations in knockout mice with altered growth hormone responsiveness. Eur J Neurosci. 2004;19(8):2069–2079. doi: 10.1111/j.0953-816X.2004.03308.x. [DOI] [PubMed] [Google Scholar]
- Renna M, et al. IGF-1 receptor antagonism inhibits autophagy. Hum Mol Genet. 2013;22(22):4528–4544. doi: 10.1093/hmg/ddt300. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Rudman D, et al. Effects of human growth hormone in men over 60 years old. N Engl J Med. 1990;323(1):1–6. doi: 10.1056/NEJM199007053230101. [DOI] [PubMed] [Google Scholar]
- Salvatori R, et al. Three new mutations in the gene for the growth hormone (gh)-releasing hormone receptor in familial isolated gh deficiency type ib. J Clin Endocrinol Metab. 2001;86(1):273–279. doi: 10.1210/jcem.86.1.7156. [DOI] [PubMed] [Google Scholar]
- Sanz A, Bartke A, Barja G. Long-lived Ames dwarf mice: oxidative damage to mitochondrial DNA in heart and brain. J Am Aging Assoc. 2002;25(3):119–122. doi: 10.1007/s11357-002-0010-3. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Sathiavageeswaran M, et al. Effects of GH on cognitive function in elderly patients with adult-onset GH deficiency: a placebo-controlled 12-month study. Eur J Endocrinol. 2007;156(4):439–447. doi: 10.1530/eje.1.02346. [DOI] [PubMed] [Google Scholar]
- Sevigny JJ, et al. Growth hormone secretagogue MK-677: no clinical effect on AD progression in a randomized trial. Neurology. 2008;71(21):1702–1708. doi: 10.1212/01.wnl.0000335163.88054.e7. [DOI] [PubMed] [Google Scholar]
- Shevah O, Laron Z. Patients with congenital deficiency of IGF-I seem protected from the development of malignancies: a preliminary report. Growth Hormon IGF Res. 2007;17(1):54–57. doi: 10.1016/j.ghir.2006.10.007. [DOI] [PubMed] [Google Scholar]
- Simpson JA, et al. Body water compartment measurements: a comparison of bioelectrical impedance analysis with tritium and sodium bromide dilution techniques. Clin Nutr. 2001;20(4):339–343. doi: 10.1054/clnu.2001.0398. [DOI] [PubMed] [Google Scholar]
- Sonntag WE, et al. Decreased pulsatile release of growth hormone in old male rats. Endocrinology. 1980;107(6):1875–1879. doi: 10.1210/endo-107-6-1875. [DOI] [PubMed] [Google Scholar]
- Sonntag WE, et al. Effects of CNS active drugs and somatostatin antiserum on growth hormone release in young and old male rats. Neuroendocrinology. 1981;33(2):73–78. doi: 10.1159/000123205. [DOI] [PubMed] [Google Scholar]
- Sonntag WE, et al. The effects of growth hormone and IGF-1 deficiency on cerebrovascular and brain ageing. J Anat. 2000;197(Pt 4):575–585. doi: 10.1046/j.1469-7580.2000.19740575.x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Sonntag WE, Ramsey M, Carter CS. Growth hormone and insulin-like growth factor-1 (IGF-1) and their influence on cognitive aging. Ageing Res Rev. 2005;4(2):195–212. doi: 10.1016/j.arr.2005.02.001. [DOI] [PubMed] [Google Scholar]
- Sonntag WE, et al. Diverse roles of growth hormone and insulin-like growth factor-1 in mammalian aging: progress and controversies. J Gerontol A Biol Sci Med Sci. 2012;67(6):587–598. doi: 10.1093/gerona/gls115. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Sonntag WE, et al. Insulin-like growth factor-1 in CNS and cerebrovascular aging. Front Aging Neurosci. 2013;5:27. doi: 10.3389/fnagi.2013.00027. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Sun LY, et al. Local expression of GH and IGF-1 in the hippocampus of GH-deficient long-lived mice. Neurobiol Aging. 2005;26(6):929–937. doi: 10.1016/j.neurobiolaging.2004.07.010. [DOI] [PubMed] [Google Scholar]
- Sun LY, et al. Increased neurogenesis in dentate gyrus of long-lived Ames dwarf mice. Endocrinology. 2005;146(3):1138–1144. doi: 10.1210/en.2004-1115. [DOI] [PubMed] [Google Scholar]
- Sun LY et al (2017) Longevity is impacted by growth hormone action during early postnatal period. Elife 6 [DOI] [PMC free article] [PubMed]
- Swerdlow AJ, et al. Cancer risks in patients treated with growth hormone in childhood: the SAGhE European cohort study. J Clin Endocrinol Metab. 2017;102(5):1661–1672. doi: 10.1210/jc.2016-2046. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Tarantini S, et al. Insulin-like growth factor 1 deficiency exacerbates hypertension-induced cerebral microhemorrhages in mice, mimicking the aging phenotype. Aging Cell. 2017;16(3):469–479. doi: 10.1111/acel.12583. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Thorner MO. Statement by the growth hormone research society on the GH/IGF-I axis in extending health span. J Gerontol A Biol Sci Med Sci. 2009;64(10):1039–1044. doi: 10.1093/gerona/glp091. [DOI] [PubMed] [Google Scholar]
- Thornton PL, Ingram RL, Sonntag WE. Chronic [D-Ala2]-growth hormone-releasing hormone administration attenuates age-related deficits in spatial memory. J Gerontol A Biol Sci Med Sci. 2000;55(2):B106–B112. doi: 10.1093/gerona/55.2.b106. [DOI] [PubMed] [Google Scholar]
- Toth P, et al. IGF-1 deficiency impairs neurovascular coupling in mice: implications for cerebromicrovascular aging. Aging Cell. 2015;14(6):1034–1044. doi: 10.1111/acel.12372. [DOI] [PMC free article] [PubMed] [Google Scholar]
- van Dam PS, et al. Childhood-onset growth hormone deficiency, cognitive function and brain N-acetylaspartate. Psychoneuroendocrinology. 2005;30(4):357–363. doi: 10.1016/j.psyneuen.2004.10.002. [DOI] [PubMed] [Google Scholar]
- van Heemst D, et al. Reduced insulin/IGF-1 signalling and human longevity. Aging Cell. 2005;4(2):79–85. doi: 10.1111/j.1474-9728.2005.00148.x. [DOI] [PubMed] [Google Scholar]
- Vergara M, et al. Hormone-treated Snell dwarf mice regain fertility but remain long lived and disease resistant. J Gerontol A Biol Sci Med Sci. 2004;59(12):1244–1250. doi: 10.1093/gerona/59.12.1244. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Vitiello MV, et al. Growth hormone releasing hormone improves the cognition of healthy older adults. Neurobiol Aging. 2006;27(2):318–323. doi: 10.1016/j.neurobiolaging.2005.01.010. [DOI] [PubMed] [Google Scholar]
- Walenkamp MJ, et al. Homozygous and heterozygous expression of a novel insulin-like growth factor-I mutation. J Clin Endocrinol Metab. 2005;90(5):2855–2864. doi: 10.1210/jc.2004-1254. [DOI] [PubMed] [Google Scholar]
- Weaver JU, et al. The effect of low dose recombinant human growth hormone replacement on regional fat distribution, insulin sensitivity, and cardiovascular risk factors in hypopituitary adults. J Clin Endocrinol Metab. 1995;80(1):153–159. doi: 10.1210/jcem.80.1.7829604. [DOI] [PubMed] [Google Scholar]
- Westbrook R, et al. Alterations in oxygen consumption, respiratory quotient, and heat production in long-lived GHRKO and Ames dwarf mice, and short-lived bGH transgenic mice. J Gerontol A Biol Sci Med Sci. 2009;64(4):443–451. doi: 10.1093/gerona/gln075. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Widdowson WM, Gibney J. The effect of growth hormone replacement on exercise capacity in patients with GH deficiency: a metaanalysis. J Clin Endocrinol Metab. 2008;93(11):4413–4417. doi: 10.1210/jc.2008-1239. [DOI] [PubMed] [Google Scholar]
- Zhang H, et al. The effect and mechanism of growth hormone replacement on cognitive function in rats with traumatic brain injury. PLoS One. 2014;9(9):e108518. doi: 10.1371/journal.pone.0108518. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Zhou Y, et al. A mammalian model for Laron syndrome produced by targeted disruption of the mouse growth hormone receptor/binding protein gene (the Laron mouse) Proc Natl Acad Sci U S A. 1997;94(24):13215–13220. doi: 10.1073/pnas.94.24.13215. [DOI] [PMC free article] [PubMed] [Google Scholar]