Abstract
The current study examined the association between perceived social support, depressive symptoms and alcohol use among people living with HIV (PLWH) 50 and older who identified as Black. Participants included 96 men and women ages 50 and older. Participants completed an interviewer-administered assessment examining mental and behavioral health functioning. Mediation analyses examined whether perceived support mediated the association between depressive symptoms and hazardous drinking. Depressive symptoms were significantly associated with hazardous drinking (B = .068, SE = .035, t = 1.92, p = 0.05) and negatively associated with having the desired amount of contact with a primary supporter (B = −.072, SE = .018, z = −3.96, p < 0.001). In addition, having the desired amount of contact with a confidant was negatively associated with hazardous drinking (B = −.543, SE = .208, t = −2.61, p 0 < .01). The effect of depressive symptoms on hazardous drinking when controlling for having adequate contact with a primary supporter was not significant (B = .033, SE = .04, t = .829, p = 0.41). Having a valued confidant mediated the association between depressive symptoms and hazardous drinking. Thus, social support interventions may be an effective method of reducing hazardous drinking among older PLWH.
Keywords: Perceived support, HIV, depressive symptoms & hazardous drinking
Introduction
Despite representing up to 12% of the US population, Black Americans account for 43% of all people living with HIV (CDC, 2018). Further, older adults account for approximately 17% of new HIV cases each year and those who identify as Black are disproportionately affected by the disease. Rates of HIV/AIDS among persons 50 and older were 12 times as high among blacks (51.7/100,000) than whites (CDC, 2018). The population of people living with HIV (PLWH) in the United States is aging, with 45% of the current population age 50 and older (CDC, 2017). In addition to new diagnoses, the prevalence of adults over 50 living with HIV is increasing greatly each year (High et al., 2012). Aging is a complex process physically, mentally, and socially, which takes place within social infrastructures such as the medical community, families, and intimate partnerships. This complexity increases when coping with a chronic illness such as HIV (Boeri et al., 2008; Briggs, Magnus, Lassiter, Patterson, & Smith, 2011; Grella & Lovinger, 2012; Hamilton & Grella, 2009). Both structural support which includes peer network size and frequency of contact, as well as functional support, which takes into account factors such as perceived quality and satisfaction with support aspects of social ties, are important factors to be addressed over the lifespan (Mavandadi, Zanjani, Ten Have, & Oslin, 2009).
The aging process is associated with increased social isolation and depressive symptoms (Arean et al., 2010; Chou, Mackenzie, Liang, & Sareen, 2011; Knowlton, Curry, Hua, & Wissow, 2009). Further, hazardous drinking is prevalent among older adults aging with HIV (High et al., 2012). However, perceived support has been identified as an important resource for PLWH but limited work has been done to understand the complex psychosocial factors affecting minorities aging with HIV (Whitehead, Hearn, & Burrell, 2014). Therefore, the current study sought to examine the extent to which perceived social support mediated the association between depressive symptoms and hazardous drinking among a sample of PLWH age 50 and older who identify as Black.
Methods
Participants and recruitment
Ninety-six PLWH 50 and older who self-identified as Black were recruited through the University of Florida Center for HIV/AIDS Research, Education and Service (UF CARES). UF CARES is a comprehensive HIV and AIDS medical treatment program; therefore all participants were engaged in care at the time of the survey. Data was collected using convenience sampling methods, a type of nonprobability sampling where members of the target population meeting inclusion criteria and willing to participate were included. Participants who met the eligibility criteria were approached by clinic staff, given a brief description of the study, and upon providing written informed consent, completed an interviewer-administered assessment examining mental and behavioral health functioning. This study was approved by the Institutional Review Board of the University of Florida. Eligible participants were HIV-positive, identified as Black/African American, and age 50 or older. Participants received a $25 gift card for completing the assessment.
Measures
Demographics
Sex, age, race, marital/partner status, number of children and other demographics were collected using a standard questionnaire.
Depressive symptoms
The 21-item Beck Depression Inventory-II (BDI-II) assessed the severity of depressive symptoms by respondents selecting the statements that best reflects how they have felt in the past two weeks. Sum scores range from 0–68. Depressive symptoms was analyzed as a continuous variable for the purpose of this study.
Hazardous drinking
Self-reported drinks per week were dichotomized according to whether or not individuals met the National Institute on Alcohol and Alcoholism (NIAAA) criteria for hazardous drinking (greater than 7 drinks per week for women and greater than 14 drinks per week for men) (Reid, Fiellin, & O’connor, 1999).
Perceived social support
The ENRICHD Social Support Inventory (ESSI) assesses perceived social support with six Likert-type scale items and an additional item assessing the presence or absence of a spouse or partner (Mitchell et al., 2003).
Statistical analyses
Mediation analyses using the Preacher and Hayes method (2004) was used to examine whether the perceived social support of a confidant mediated the association between depressive symptoms and hazardous drinking, followed by bootstrapping with 5,000 samples, to test the strength of the indirect effect. The covariates sex, CD4 count, and annual income were added to the model in order to control for confounding variables that may influence the association between depressive symptoms and Hazardous drinking.
Results
The mean age of the sample was 55.77 years (SD = 5.27; range: 50–76 years), and 62.9% were female (see Table 1). The majority of the sample (82.05%) reported incomes of less than 20,000 dollars/year. The average number of years since HIV diagnosis was 14.80 years (SD = 10.61; range: 0–35 years). Participants reported an average number of 6.46 (SD = 2.85) medical comorbidities, and based on medical chart abstraction, 28.6% of the sample had a detectable viral load (greater than 50 copies of viral RNA) with an average CD4 cell count of 540.81 (SD = 277.83). Participants had an average score of 11.15(M) 8.69 (SD) on the BDI. Perceived support of a valued confidant was the only aspect of social support that was significantly correlated with both depressive symptoms (r = −.337, p = 0.001) and hazardous drinking (r = −.325, p = 0.001).
Table 1.
Participant demographics (N = 96).
| Sex % Female (N) | 63.16% (60) | Annual household income % (N) | |
|---|---|---|---|
| Age M(SD) | 55.78 (5.26) | < 10,000 | 49.47% (47) |
| Race % Black/African-Am (N) | 100% (96) | 10,000–14,999 | 23.16% (22) |
| Marital Status %(N) | 15,000–19,999 | 12.63% (12) | |
| Single, Never Married | 50.53% (48) | 20,000–24,999 | 2.11% (2) |
| Divorced | 25.26% (24) | > 25,000 | 3.16% (3) |
| Separated | 6.32% (6) | Declined | 9.47% (9) |
| Widowed | 7.37% (7) | HIV Related Variables M(SD) | |
| Married or Common Law | 10.53% (10) | Years since diagnosis | 14.83 (10.63) |
| Do you have children? | 75.79% (72) | CD4 Count | 533.15 (275.76) |
| Living with a Partner %(N) | 14.74% (14) | Detectable Viral Load | 28.6% |
| Number of Medical Comorbidities M(SD) | 6.37 (2.80) | Self-reported Non-adherence %(N) | 15.79% (15) |
Note. N may vary according to missing values.
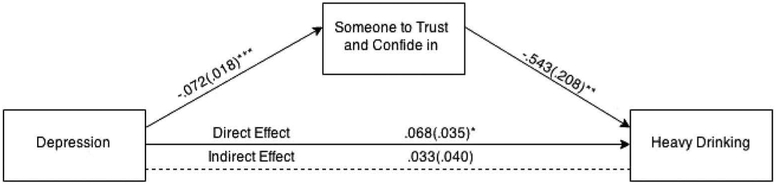
To test the hypothesis that sufficient contact with a primary supporter would mediate the association between depressive symptoms and hazardous drinking, a regression model using the Preacher and Hayes approach was run. Depressive symptoms was significantly associated with hazardous drinking (B = .068, SE = .035, t = 1.92, p = 0.05) and negatively associated with having the desired amount of contact with a primary supporter (B = −.072, SE = .018, z = −3.96, p < 0.001). In addition, having the desired amount of contact with a primary supporter was negatively associated with hazardous drinking (B = −.543, SE = .208, t = −2.61, p < 0.01). The effect of depressive symptoms on hazardous drinking when controlling for having adequate contact with a primary supporter was not significant (B = .033, SE = .04, t = .829, p = 0.41). (See Figure 1).
Figure 1.
Mediation model of social support on depressive symptoms and hazardous drinking.
Note. Estimate of the indirect effect (B = .046); Bootstrapped confidence interval (95%) = [.0053 – .0998]. * p < .05, **p < .01, *** p < .001.
Discussion
Older adults living with HIV in the United States misuse alcohol at rates higher than the general population (Green et al., 2010; Moore et al., 2009). Further, PLWH 50 years and older are frailer than their chronological age indicates due to their disease status, making them more vulnerable to the consequences (i.e. greater intoxication with even lower levels of consumption) of substance misuse such as hazardous drinking (Dowling, Weiss, & Condon, 2008; Karpiak, Shippy, & Cantor, 2006; Vance, 2010). Our findings show that having enough contact with someone ‘you feel close to’ mediated the association between depressive symptoms and hazardous drinking. Hazardous drinking is associated with decreased medication adherence, decreased engagement in HIV care, greater medical comorbidities, and poorer quality of life (Eldred, 2007; Rothlind et al., 2005; Waldrop-Valverde et al., 2006; Weber et al., 2013). An important factor underscoring the significance of these findings is that depressive symptoms and substance use among older, chronically ill populations are associated with transition from informal community based care by family and friends to institutionalization (Chou et al., 2011; Kelly et al., 2012; Knowlton, 2003; Latkin, Forman, Knowlton, & Sherman, 2003). Therefore, addressing the relationship between depressive symptoms and hazardous drinking not only improves quality of life but may substantively reduce long-term healthcare costs.
Our work shows perceived social support can mitigate health risks such as substance misuse. This is critical because the burgeoning population of older adults with HIV face considerable psychosocial challenges with regard to social engagement, adequacy of informal social networks, and caregiving resources to meet their needs. Research has documented that those aging with HIV tend to have limited and/or inadequate social networks (Bohnert, Bradshaw, & Latkin, 2009; Shippy & Karpiak, 2005a, 2005b). This work provides evidence that social support interventions could address social network insufficiency among those aging with HIV and have a positive effect on reducing detrimental health behaviors such as hazardous drinking.
Strengths and limitations
While this study provides evidence for the importance of supportive relationships, there are limitations to be considered. First, the majority of the sample was women and research shows that women benefit most from social relationships mitigating negative mood states. Second, the cross-sectional design inhibits the ability to find causal relationships between constructs in this study. Although the self-report of having ‘enough contact with someone you feel close to’ mediated the association between depressive symptoms and hazardous drinking, we are unable to determine the temporality of these constructs. Third, convenience sampling methods were used to collect the data and may not be representative of PLWH 50 and older. Moreover, because the study’s population included only older PLWH who identify as black, generalizing the findings to other populations is difficult. However, despite the limitations, the results presented have direct implications for addressing hazardous drinking among PLWH 50 and older. Specifically, perceived support may serve as an important intervention point through peer support interventions to address hazardous drinking in this population. Though literature has shown that social support can have a positive impact on psychological health in PLWH, this study identifies the particular importance of having sufficient contact with a perceived confidant for older HIV-positive minority adults.
Acknowledgments
Funding
This work was supported by the National Institute of Mental Health (NIH) under grant number R25MH080665 and the National Institute on Drug Abuse under grant number K23039769-01
Footnotes
Disclosure statement
No potential conflict of interest was reported by the authors.
References
- Arean PA, Raue P, Mackin RS, Kanellopoulos D, McCulloch C, & Alexopoulos GS (2010). Problem-solving therapy and supportive therapy in older adults with major depression and executive dysfunction. American Journal of Psychiatry, 167(11), 1391–1398. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Boeri MW, Sterk CE, & Elifson KW (2008). Reconceptualizing early and late onset: A life course analysis of older heroin users. The Gerontologist, 48(5), 637–645. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Bohnert ASB, Bradshaw CP, & Latkin CA (2009). A social network perspective on heroin and cocaine use among adults: Evidence of bidirectional influences. Addiction, 104(7), 1210–1218. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Briggs WP, Magnus VA, Lassiter P, Patterson A, & Smith L (2011). Substance use, misuse, and abuse among older adults: Implications for mental health counselors. Journal of Mental Health Counseling, 33(2), 112–127. [Google Scholar]
- Chou KL, Mackenzie CS, Liang K, & Sareen J (2011). Three-year incidence and predictors of first-onset of DSM-IV mood, anxiety, and substance use disorders in older adults: results from wave 2 of the national epidemiologic survey on alcohol and related conditions. Journal of Clinical Psychiatry, 72(2), 144–155. [DOI] [PubMed] [Google Scholar]
- Division of HIV/AIDS Prevention, National Center for HIV/AIDS, Viral Hepatitis, STD, and TB Prevention, Centers for Disease Control and Prevention (2017). Retrieved from https://www.cdc.gov/hiv/group/age/olderamericans/index.html
- Dowling GJ, Weiss SRB, & Condon TP (2008). Drugs of abuse and the aging brain. Neuropsychopharmacology, 33(2), 209–218. [DOI] [PubMed] [Google Scholar]
- Eldred SL (2007). HIV and the older adult: Challenges in prevention and treatment. Geriatrics and Aging, 10, 393–396. [Google Scholar]
- Green TC, Bryant K, Fiellin DA, Justice AC, Kershaw T, Lin H, … Day NL (2010). Patterns of drug use and abuse among aging adults with and without HIV: A latent class analysis of a US Veteran cohort. Drug and Alcohol Dependence, 110(3), 208–220. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Grella CE, & Lovinger K (2012). Gender differences in physical and mental health outcomes among an aging cohort of individuals with a history of heroin dependence. Addictive Behaviors, 37(3), 306–312. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Hamilton AB, & Grella CE (2009). Gender differences among older heroin users. Journal of Women & Aging, 21(2), 111–124. [DOI] [PMC free article] [PubMed] [Google Scholar]
- High KP, Brennan-Ing M, Clifford DB, Cohen MH, Currier J, Deeks SG, … Volberding P (2012). HIV and aging: state of knowledge and areas of critical need for research. A report to the NIH office of AIDS research by the HIV and aging working group. Jaids-Journal of Acquired Immune Deficiency Syndromes, 60, S1–S18. [DOI] [PMC free article] [PubMed] [Google Scholar]
- HIV and African Americans. (2018). CDC. Retrieved April 22, 2018 from https://urldefense.proofpoint.com/v2/url?u=https-3A__www.cdc.gov_hiv_pdf_group_racialethnic_africanamericans_cdc-2Dhiv-2Dafricanamericans.pdf&d=DwIFaQ&c=pZJPUDQ3SB9JplYbifm4nt2lEVG5pWx2KikqINpWlZM&r=ANIAzolJq6dbkNoBGuB8U3mOAHsNXYTOWSy3bUNN8a0&m=jOVzxyJ61lFxyzwxv8jyFFqtgIghYdgCDMj12pBmx2U&s=5aNwjCxBCtH5aWKJL7XZVPytlwMgczUPZLPXxrO0wmI&e=
- Karpiak SE, Shippy RA, & Cantor MH (2006). ROAH: Research on older adults with HIV. New York: AIDS Community. [Google Scholar]
- Kelly PJ, Ramaswamy M, Li X, Litwin AH, Berg KM, & Arnsten JH (2012). Social networks of substance users with HIV infection: Application of the norbeck social support scale. Western Journal of Nursing Research, 34(5), 621–634. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Knowlton AR (2003). Informal HIV caregiving in a vulnerable population: Toward a network resource framework. Social Science & Medicine, 56(6), 1307–1320. [DOI] [PubMed] [Google Scholar]
- Knowlton AR, Curry A, Hua W, & Wissow L (2009). Depression and social context: Primary supporter association factors associated with depressive symptoms among a disadvantaged population with HIV/AIDS. Journal of Community Psychology, 37(4), 526–541. [Google Scholar]
- Latkin CA, Forman V, Knowlton A, & Sherman S (2003). Norms, social networks, and HIV-related risk behaviors among urban disadvantaged drug users. Social Science & Medicine, 56(3), 465–476. [DOI] [PubMed] [Google Scholar]
- Mavandadi S, Zanjani F, Ten Have TR, & Oslin DW (2009). Psychological wellbeing among individuals aging with HIV: The value of social relationships. Journal of Acquired Immune Deficiency Syndromes, 51(1), 91. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Mitchell PH, Powell L, Blumenthal J, Norten J, Ironson G, Pitula CR, … Berkman LF (2003). A short social support measure for patients recovering from myocardial infarction: The ENRICHD social support inventory. Journal of Cardiopulmonary Rehabilitation and Prevention, 23(6), 398–403. [DOI] [PubMed] [Google Scholar]
- Moore AA, Karno MP, Grella CE, Lin JC, Warda U, Liao DH, & Hu P (2009). Alcohol, tobacco, and nonmedical drug use in older U.S. adults: Data from the 2001/02 National epidemiologic survey of alcohol and related conditions. Journal of the American Geriatrics Society, 57(12), 2275–2281. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Preacher KJ, & Hayes AF (2004). SPSS and SAS procedures for estimating indirect effects in simple mediation models. Behavior Research Methods, Instruments, & Computers, 36(4), 717–731. [DOI] [PubMed] [Google Scholar]
- Reid MC, Fiellin DA, & O’connor PG (1999). Hazardous and harmful alcohol consumption in primary care. Archives of Internal Medicine, 159(15), 16. [DOI] [PubMed] [Google Scholar]
- Rothlind JC, Greenfield TM, Bruce AV, Meyerhoff DJ, Flenniken DL, Lindgren JA, & Weiner MW (2005). Heavy alcohol consumption in individuals with HIV infection: Effects on neuropsychological performance. Journal of the International Neuropsychological Society, 11(1), 70–83. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Shippy RA, & Karpiak SE (2005a). The aging HIV/AIDS population: Fragile social networks. Aging & Mental Health, 9(3), 246–254. [DOI] [PubMed] [Google Scholar]
- Shippy RA, & Karpiak SE (2005b). Perceptions of support among older adults with HIV. Research on Aging, 27(3), 290–306. [Google Scholar]
- Vance DE (2010). Aging with HIV: Clinical considerations for an emerging population. American Journal of Nursing, 110(3), 42–47. doi: 10.1097/01.Naj.0000368952.80634.42 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Waldrop-Valverde D, Ownby RL, Wilkie FL, Mack A, Kumar M, & Metsch L (2006). Neurocognitive aspects of medication adherence in HIV-positive injecting drug users. Aids and Behavior, 10(3), 287–297. [DOI] [PubMed] [Google Scholar]
- Weber E, Smith DM, Moore DJ, Woods SP, Morgan EE, Iudicello JE, & Grp T (2013). Substance use is a risk factor for neurocognitive deficits and neuropsychiatric distress in acute and early HIV infection. Journal of NeuroVirology, 19(1), 65–74. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Whitehead NE, Hearn LE, & Burrell L (2014). The association between depressive symptoms, anger, and perceived support resources among underserved older HIV positive Black/African American adults. AIDS Patient Care and STDs, 28(9), 507–512. [DOI] [PMC free article] [PubMed] [Google Scholar]