Abstract
Many women living with HIV experience a range of physical, social, and psychological challenges linked to their HIV status. Psychosocial support interventions may help women cope with these challenges and may allow women to make better decisions around their sexual and reproductive health (SRH), yet no reviews have summarized the evidence for the impact of such interventions on well-being and SRH decision-making among women living with HIV. We systematically reviewed the evidence for non-specialist delivered psychosocial support interventions for women living with HIV, which are particularly relevant in low-resource settings. Outcomes of interest included mental, emotional, social well-being and/or quality of life, common mental health disorders, and SRH decision-making. Searching was conducted through four electronic databases and secondary reference screening. Systematic methods were used for screening and data abstraction. Nine articles met the inclusion criteria, showing positive or mixed results for well-being and depressive symptoms indicators. No studies reported on SRH decision-making outcomes. The available evidence suggests that psychosocial support interventions may improve self-esteem, coping and social support, and reduce depression, stress, and perceived stigma. However, evidence is mixed. Most studies placed greater emphasis on instrumental health outcomes to prevent HIV transmission than on the intrinsic well-being and SRH of women living with HIV. Many interventions included women living with HIV in their design and implementation. More research is required to understand the most effective interventions, and their effect on sexual and reproductive health and rights.
Keywords: HIV, psychosocial, women, review, systematic
Introduction
Living with HIV impacts physical, social and psychological aspects of a person’s health and life (Lingen-Stallard, Furber, & Lavender, 2016; WHO, 2016b). A higher proportion of people living with HIV experience depression and anxiety than the general population: some studies reported higher prevalence in females than males, and a negative impact of psychological distress on quality of life (Lowther et al., 2016; Niu, Luo, Liu, Silenzio, & Xiao, 2016; Vo et al., 2016). A large global survey led by, and for, women living with HIV on their sexual and reproductive health and rights found that 82% of women reported depressive symptoms and 78% reported experiencing rejection (Orza et al., 2015). These and other experiences, including social exclusion, stigma, insomnia, and rights violations, challenged their overall well-being, their sexual and reproductive health (SRH), and their ability to exercise their rights (Orza et al., 2015).
Psychosocial support addresses the ongoing psychological and social problems of people living with HIV, their partners, families and caregivers (WHO, 2016b). Despite high prevalence of psychosocial challenges among women living with HIV, identified associations between psychosocial concerns and SRH outcomes such as child-bearing and sexual desire (EngenderHealth, 2009; Malary, Khani, Pourasghar, Moosazadeh, & Hamzehgardeshi, 2015), and recommendations to include psychosocial support in HIV care (Paudel & Baral, 2015; WHO, 2016b), no reviews have investigated the impact of psychosocial support interventions on SRH health decision-making among women living with HIV. Existing reviews concerning psychosocial support have focused on: 1) clinical outcomes or care engagement outcomes (Bateganya, Amanyeiwe, Roxo, & Dong, 2015; Genberg et al., 2016), 2) specific intervention types including support groups (Bateganya et al., 2015; Mundell et al., 2011; Paudel & Baral, 2015), or 3) outcomes for mixed-gender groups (Crepaz et al., 2008; Scott-Sheldon, Kalichman, Carey, & Fielder, 2008b). More research has been recommended to understand psychosocial support interventions for people living with HIV, including gender considerations (Bateganya et al., 2015; Crepaz et al., 2008; Paudel & Baral, 2015). Many psychosocial support interventions can be delivered by non-specialist healthcare workers or lay providers (Kaaya et al., 2013; Mundell et al., 2011; Richter et al., 2014). This is particularly important in resource-limited settings (WHO, 2016b).
To inform the World Health Organization (WHO) Consolidated guideline on the sexual and reproductive health and rights of women living with HIV, we conducted a systematic literature review on psychosocial support for women living with HIV to identify effective forms of non-specialist psychosocial support for improving women’s intrinsic well-being and ability to make SRH decisions (for example, around contraceptive use, abortion, or prevention of sexually transmitted infections). We focused on intrinsic well-being – health outcomes that directly benefit the woman, herself – rather than secondary or instrumental outcomes that benefit others, such as onward HIV transmission to partners or children. Outcomes were guided by the holistic, interconnected priorities identified through a global survey on SRH priorities of women living with HIV (SalamanderTrust, 2014). We focused on health service providers without specialized training in mental health, as interventions with trained mental health practitioners providing formal mental health services are covered in other reviews and existing WHO guidelines (Genberg et al., 2016; Kennedy, Fonner, Armstrong, O’Reilly, & Sweat, 2015; Kennedy, Haberlen, Amin, Baggaley, & Narasimhan, 2015; Perazzo, Reyes, & Webel, 2016; WHO, 2013).
Methods
Inclusion criteria
Articles meeting the following criteria were included in the review:
Published in a peer-reviewed journal through the search date of February 25, 2016.
Measured one or more of the following primary or secondary outcomes: Primary: 1) Measures of mental/emotional/social well-being and/or quality of life (e.g. decision-making capacity, coping skills, stigma reduction). 2) Measures of common mental health disorders (e.g. depression, anxiety). Secondary: Decision-making around SRH services (e.g. contraception, abortion, cervical cancer screening, sexually transmitted infection services, etc.).
Controlled trials (randomized and non-randomized), comparing provision of psychosocial support by providers without specialized training in mental health to people who received alternative care or treatment. Providers could include a trained, certified health professional without specialized training in psychiatric or psychological care (e.g., doctor, nurse without specialized mental health training) or a lay provider with or without brief training in provision of psychosocial support services (WHO, 2012).
Presented data for women living with HIV who received the intervention, either because the study included only women living with HIV or because data were disaggregated by gender and HIV status.
Search Strategy, Screening, and Data Extraction and Analysis
We searched four electronic databases: PubMed, PsycINFO, CINAHL, and EMBASE. The following terms comprised the PubMed search, which was adapted for the other databases: (“HIV positive” [tiab] OR “living with HIV” [tiab] OR “HIV infected” [tiab]) AND (randomized controlled trial[pt] OR controlled clinical trial[pt] OR randomized[tiab] OR random*[tiab] OR clinical trials as topic[mesh:noexp] OR “non-randomized trial”[tiab]) AND (“psychosocial support” [tiab] OR “social support” [tiab] OR “support groups” [tiab] OR “counselling” [tiab] OR counseling [tiab]) AND (depression or stress OR coping OR cope OR self-esteem OR self-confidence OR wellness OR stigma OR “mental health” OR “well-being” OR “quality of life”). We also conducted secondary reference searching on nine systematic reviews identified in our search or known by the researchers to be related to the topic (Biswas, 2007; Carrico & Antoni, 2008; Feyissa, Lockwood, & Munn, 2015; Kennedy, Fonner, et al., 2015; Kennedy, Medley, Sweat, & O’Reilly, 2010; Mwai et al., 2013; Paudel & Baral, 2015; Scott-Sheldon, Kalichman, Carey, & Fielder, 2008a; Zajac et al., 2015).
Citations identified through the search strategy underwent initial screening by one reviewer, based on title and abstract. Two reviewers then conducted second level screening of all potentially relevant citations, comprising those related to HIV and well-being, quality of life, mental health, or sexual or reproductive health decision-making, based on title, abstract, citation information, and descriptor terms, conferring as needed. One reviewer then screened potentially relevant full text articles for outcomes measured, study design, type of healthcare provider, and data exclusively disaggregated for women living with HIV to determine final study selection. We contacted, and received clarification from, two authors about articles for which we could not determine study eligibility based on published information. Queries about article eligibility were discussed among the research team and resolved through consensus. For the included studies, study identification, intervention descriptions, provider type, theoretical grounding, measurement approaches, study design, and outcomes were abstracted into standardized tables by the reviewer who conducted the full text screening. Quality assessment of included articles was conducted using an adapted version of the Evidence Project’s tool (Fonner, Armstrong, Kennedy, O’Reilly, & Sweat, 2014; Kennedy, Fonner, et al., 2015; Zajac et al., 2015).
Meta-analysis was not conducted due to the limited number of articles measuring the same outcomes using a consistent approach. We present a descriptive analysis of the study findings based on the data extracted. We conducted sub-group analyses of outcomes that were measured by three or more studies.
Results
Studies Identified
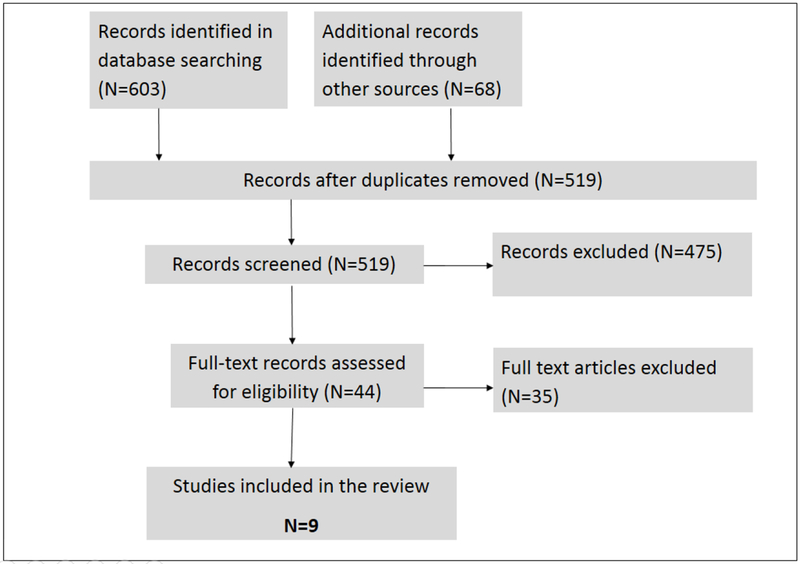
The search string identified 451 articles with duplicates removed (Figure 1). An additional 68 articles were identified through secondary reference searching. After initial abstract screening, 44 articles were pulled for full-text review. Nine studies met the inclusion criteria.
Figure 1.
PRISMA flow diagram of identified and included citations
Study Descriptions
A descriptive summary of included studies is presented in Table I.
Table I.
Summary of Included Study Interventions, Providers, Frameworks, and Outcomes
| Citation, Location, Design, Sample Size | Psychosocial Support Intervention Description | Intervention Provider | Theoretical Framework | Psychosocial Support Outcome Results, Follow-Up Time | |
|---|---|---|---|---|---|
|
Mundell et al., 2011 Location: Tshwane, South Africa Design: Non-randomized trial Sample Size: N=144, intervention N=217, control |
Serithi Project Modality: 10-session, weekly support group meetings Population: newly HIV-diagnosed pregnant women Topics covered: personal-level, HIV knowledge & emotional impact; relational-level, disclosure, coping with social relations, stress management and immune system; Stigma, human rights; Life planning, goal setting Control Group: standard antenatal care Primary Objective: Disclosure and well-being of women living with HIV |
Masters-level psychology students with women living with HIV | Hanson systems theory and experiential learning; Developed through action research with women living with HIV | Time: 2-month follow-up: Regression with Planned Contrast t, p-value •Active Coping:2.68, 0.01* •Avoidant coping: −2.02, 0.04* •Self-Esteem:1.92, 0.06 High Attendance Group Self-Esteem: 2.11, <0.05* •Depression:1.12, 0.27 •Positive social support:0.82, 0.41 Negative social support: 0.68, 0.47 |
Time: 8-month follow-up: Regression with Planned Contrast t, p-value •Active Coping:1.22, 0.22 •Avoidant coping: −0.35, 0.73 •Self-Esteem:1.27, 0.21 •Depression: −1.46, 0.15 •Positive social support:−0.42, 0.67 •Negative social support: −1.28, 0.20 High Attendance Group Negative social support: −2.41, <0.05* |
|
Kaaya et al., 2013 Location: Dar es Salaam, Tanzania Design: RCT, individual Sample Size: N=331, enrolled N=188, analyzed |
Structured, closed-group counselling intervention Modality: 6 weekly sessions Population: 6-8 women pregnant living with HIV Topics Covered: Session 1-Challenges of living with HIV, disclosure, MTCT, home and community support systems, future plans; Next 5 sessions-HIV transmission, safer sex, accessing healthcare, reduce MTCT, disclosure, risk & anxiety reduction; Skills training- relaxation breathing exercise, partner disclosure practice Control Group: standard antenatal care Primary Objective: Disclosure and reduced depression |
Nurse midwives | Problem-solving therapy approach, Developed based on field experience with support groups for women with high psychological distress and PMTCT concerns | Time: 8-10 weeks post intervention •Depression Relative Risk of Depression: Intervention: 60% Control: 73% RR: 0.82 (95%CI:0.67 – 1.01), p-value: 0.066 |
|
|
Eloff et al., 2014 Location: Tshwane, South Africa Design: RCT, mother-child pair Sample Size: N=390 |
Facilitated groups for mothers and children Modality: 24 weekly sessions, 75 minutes / session Population: 14 mother-child separated sessions for mothers living with HIV then 10 mother-child joint sessions Topics Covered: living positively, disclosure, healthy relationships, emotional experience of having HIV, coping, stress, problem solving, HIV stigma, human rights, HIV in the household, parenting skills, child development, life planning and goal setting, child-parent relationship, creating a legacy together, family celebration Control Group: provided information about local resources available for assistance related to young children living with their HIV positive mothers Primary Objective: Improved resilience of young children with HIV positive mothers |
Community care workers, trained & supervised by social worker | Developed with action research with women living with HIV; conceptual framework that maternal HIV psychological trauma affects mother, child, & their relationship | Time: 18-month follow up Intervention versus Control •Maternal depression: b= −1.07, p-value: 0.092 •Maternal self-coping: b= 0.05, p-value: 0.94 •Help from others: b=0.32, p-value:0.21 •Avoidant coping: b= −0.24, p-value:0.99 Increased attendance in the intervention was significantly associated with decreased maternal depression (b= −0.096, P=0.047) and an increase in the coping domain of seeking help from others (b=0.047, P=0.032) |
|
|
Futterman et al., 2010 Location: Peri-urban Cape Town, South Africa Design: Non-randomized trial Sample Size: N=71 |
Mamekhaya, based on Mothers2Mothers (M2M) Modality: 8 small group sessions Population: pregnant women living with HIV Topics Covered: Healthy Living- staying in care, dealing with symptoms, HIV, ARVs, family planning, condoms; Feeling Happy & Strong- disclosure, stigma, support, hope, negative emotions, domestic violence, substance abuse; Partnering & Preventing Transmission: infant feeding, partner testing, safer sex; Parenting: feeding, immunizations, infant testing, custody, attachment; in all sessions: music, meditation, active learning Control Group: standard PMTCT care from medical staff Primary Objective: PMTCT and maternal well-being |
M2M mentor mothers (women living with HIV) trained in cognitive behavioral interventions | Cognitive behavioral interventions, empowerment and support model | Time: Follow-up 6 months post-delivery Effect of Intervention Estimate from Regression-b, SE, p-value-significant •HIV discomfort: −0.50, 0.52 •Social support availability: 9.32, 3.53, <0.05* •Social support satisfaction: −0.62, 0.6 •Depression: −4.43, 1.62, <0.01* •Positive coping: 2.50, 1.38 |
|
|
Richter et al., 2014 Location: KwaZulu-Natal, South Africa Design: RCT, facility Sample Size: N=1,200 |
Adapted from Mothers2Mothers (M2M) Modality: 8 individual mentor sessions: 4 antenatal, 4 postnatal Population: pregnant women living with HIV Topics covered: destigmatizing HIV, PMTCT tasks, exclusive feeding, abstaining from traditional medicines, healthy daily routines, obtaining a child grant, maintaining strong social network, couples’ HIV testing, disclosure, condom use Control Group: national PMTCT program - dual therapy for PMTCT, referral for ARV if CD4 count <200 or WHO Stage 4 illness, single feeding method recommended; tins of powdered milk distributed throughout the study Primary Objective: Maternal and infant well-being |
Peer mentors | Empowerment and support model | Time: 1.5-months post-birth •Depression* Proportion without depression, GHQ<7: Intervention: 357 (94.7%) Control: 409 (87.8%) OR: 2.55 (95%CI: 1.37, 4.76) 1-sided p-value: 0.002 |
|
|
Wingood, et al., 2004 Location: Georgia & Alabama, USA Design: RCT, individual Sample Size: N=366 |
WiLLOW: ‘Women involved in life learning from other women’ Modality: 4, 4-hour interactive group sessions implemented over consecutive weeks with 8-10 group participants Population: Women living with HIV Topics Covered: Gender pride; supportive social network use and maintenance; HIV transmission risk behaviors, communication and safe sex negotiation, condom use, managing abusive relationships Control Group: 4, 4-hour interactive group sessions administered over consecutive weeks; topics covered: medication adherence, nutrition, and provider interaction skills Primary Objective: Reduction in unprotected vaginal sex |
Trained female health educator, co-facilitated by HIV-positive female peer educator | Social cognitive theory; Theory of gender power; designed with women living with HIV | Time: 12-month follow up •Number of social network ties* % relative change comparing intervention to control: 12.0 (95%CI: 0.5, 23.4), p-value: 0.02; Adjusted mean difference, 95%CI: 1.6 (0.4, 3.2) Unreported significant positive impact on self-esteem and coping according to Klein et al., 2013 |
|
|
Klein et al., 2013 Location: southern USA Design: RCT, individual Sample Size: N=175 |
Multimedia WiLLOW Modality: 2, 1-hour interactive computer session separated into 2-8 minute activity modules Population: African American women living with HIV Topics covered: pride, values, goals, using social support, stress management, risk reduction, condom management, building healthy relationships, HIV re-infection, STIs, partner communication, disclosure, condom self-efficacy, computer use instructions Control Group: reviewed HIV education brochures for people living with HIV Primary Objective: Increase in protective sexual behaviors and psychosocial mediators associated with HIV risk reduction |
Interactive computer modules | Social cognitive theory; Theory of gender power, built from each session of WiLLOW program | Time: 3-month follow-up •Stress* % relative change (95%CI): −12.08 (−3.76, −13.72) No significant differences in (no effect estimates given): •Coping •Self Esteem •Social support |
|
| Echenique et al., 2012 Location: Miami, FL USA Design: RCT, individual Sample Size: N=109 |
ROADMAP Modality: 4 weekly psycho-educational group sessions, 2-hours each Population: Sexually active, women living with HIV 45 years or older Topics covered: HIV, harm reduction, effects of HIV on sexual behaviors, assertive communication with partners, condom negotiation, de-escalating negative partner reactions, review of lessons learned, self-reward for maintaining safer behavior Control Group: usual care from primary care clinic serving people living with HIV and educational brochure on sexual risk reduction Primary Objective: Reduce high risk sexual behavior |
Peer educators | not specified | Time: 6-month follow-up •HIV stigma (perceived)* Mean stigma score baseline, endline; p-value Intervention group: 104.6, 96.5; 0.05 Control group: 100.7, 97.1; 0.38 |
|
|
Miles et al., 2003 Location: southeastern USA Design: RCT, individual Sample Size: N=106 |
Self-Care Symptom Management Intervention for Mothers Modality: 6 home visits Population: Mothers living with HIV Topics covered: HIV knowledge, self-care strategies, general health promotion, health problems, early care-seeking, HIV treatments and clinical trials, preventing and managing respiratory & gastrointestinal infections, gynecologic health, mental health, prevention-nutrition, rest, exercise Control Group: Usual care at clinics offering HIV services Primary Objective: Emotional distress reduction and increased perception of health |
Registered nurses, 2 African American, 1 White | Maternal HIV Self-Care Symptom Management Framework, African American culture | Time: 1-month follow-up GLM effect, p-value •Depression: −2.23, 034 •HIV stigma: −0.19, 0.09 •HIV worry: −0.01, 0.96 •Mood: no mood measures were significantly different |
Time: 6-month follow-up GLM effect, p-value •Depression: 2.31, 0.36 •HIV stigma (perceived): −0.25, 0.03* •HIV worry: −0.11, 0.65 •Mood: no mood measures were significantly different |
indicates significant difference between intervention and comparison groups
Settings
Included studies were conducted in three countries: South Africa (Eloff et al., 2014; Futterman et al., 2010; Mundell et al., 2011; Richter et al., 2014), Tanzania (Kaaya et al., 2013), and the southern United States (US) (Echenique et al., 2013; Klein, Lomonaco, Pavlescak, & Card, 2013; Miles et al., 2003; Wingood, DiClemente, Mikhail, Lang, McCree, Davies, Hardin, Hook 3rd, et al., 2004). All nine studies recruited participants from health facilities, care agencies, or health departments.
Populations
Four of the five studies in Africa included only pregnant women (Futterman et al., 2010; Kaaya et al., 2013; Mundell et al., 2011; Richter et al., 2014), with two specifically studying women with recent HIV diagnosis (Mundell et al., 2011; Richter et al., 2014). Participant mean age was 26-27 years; the youngest specified age was 16 years (Futterman et al., 2010). The remaining African study included women with mean age 33 years who had children aged 6-10 years (Eloff et al., 2014). Many women in these studies had low income. Three of the four US-based studies included only, or majority, African American women (Klein et al., 2013; Miles et al., 2003; Wingood, DiClemente, Mikhail, Lang, McCree, Davies, Hardin, Hook, et al., 2004). One of those included only mothers (Miles et al., 2003). Mean age in these studies ranged from 35-40 years. Most women had low or very low income. The remaining US-based study focused on older women (over age 45) including a mix of Hispanic, White, and Black women (Echenique et al., 2013). No literature included data specific to women living with HIV from key populations, such as women who inject drugs, are in prison, transgender, lesbian or bisexual, adolescents, or sex workers (WHO, 2016a).
Study designs, Quality, Interventions, and Outcomes
Study designs included six individually-randomized controlled trials (RCT) (Echenique et al., 2013; Eloff et al., 2014; Kaaya et al., 2013; Klein et al., 2013; Miles et al., 2003; Wingood, DiClemente, Mikhail, Lang, McCree, Davies, Hardin, Hook, et al., 2004), one facility-randomized controlled trial (Richter et al., 2014) and two non-randomized trial designs (Futterman et al., 2010; Mundell et al., 2011). Total sample size per study ranged from 71-1,200 participants. Follow-up time extended from eight weeks to eighteen months. Length of follow-up time was not consistently associated with improved outcomes. Study quality varied. Most studies were relatively methodologically rigorous, with randomization to study arms; however, not all were comparable between arms on baseline sociodemographic characteristics and outcome measures (see Table II).
Table II.
Study Rigor Assessment
| Study | Random assignment (group or individual) to the intervention | Comparison groups equivalent at baseline on socio-demographics | Comparison groups equivalent at baseline on outcome measures | Time period and follow-up rate |
|---|---|---|---|---|
| Mundell et al., 2011 | No | No | No: Depression higher in intervention group | 2 months & 8 months 69% comparison; 90% intervention |
| Kaaya et al., 2013 | Yes | Yes | Yes | 8-10 weeks 84.3% standard of care; 81.5% intervention |
| Eloff et al., 2014 | Yes | No | Yes | 18 months 88% standard of care; 81% intervention; 72% completed all 3 interviews |
| Futterman et al., 2010 | No | No | No: Depression higher in intervention group | 6 months 40% control; 48% intervention |
| Richter et al., 2014 | Yes | Yes | Yes | 1.5 months 71% standard of care; 69% intervention |
| Wingood, et al., 2004 | Yes | No | Yes | 12 months 90.3% comparison; 85.2% intervention |
| Klein et al., 2013 | Yes | Yes | No: Having someone to confide in about HIV lower in intervention groupa | 3 months 98.9% control; 93.1% intervention |
| Echenique et al., 2012 | Yes | Yes | Not reportedt | 6 months 41% control; 32.5% intervention |
| Miles et al., 2003 | Yes | No | Not reported | 1 month & 6 months 1 month: 74.0% control; 62.7% intervention 6 months: 58.0% control; 50.8% intervention |
Also not equivalent on other outcome measures not of direct interest to this review;
Equivalent on other outcome measure not of direct interest to this review
Psychosocial support interventions encompassed a range of intervention modalities and intended outcomes. Eight of the nine studies used an explicit theoretical framework that guided the intervention design and implementation (Eloff et al., 2014; Futterman et al., 2010; Kaaya et al., 2013; Klein et al., 2013; Miles et al., 2003; Mundell et al., 2011; Richter et al., 2014; Wingood, DiClemente, Mikhail, Lang, McCree, Davies, Hardin, Hook, et al., 2004). Four studies worked with women living with HIV to design and/or refine the intervention (Eloff et al., 2014; Kaaya et al., 2013; Mundell et al., 2011; Wingood, DiClemente, Mikhail, Lang, McCree, Davies, Hardin, Hook, et al., 2004).
The most common mode of intervention delivery was a support group or facilitated group (Echenique et al., 2013; Eloff et al., 2014; Futterman et al., 2010; Kaaya et al., 2013; Mundell et al., 2011; Wingood, DiClemente, Mikhail, Lang, McCree, Davies, Hardin, Hook, et al., 2004). Two studies used an individual mentorship approach (Miles et al., 2003; Richter et al., 2014), and one used interactive computer modules (Klein et al., 2013). Interventions were delivered in sessions, ranging from 2 – 24 exposures. Intervention providers included nurses, midwives, masters-level psychology students, community health workers and peer educators. Five studies utilized interventions delivered or co-delivered by women living openly with HIV (Echenique et al., 2013; Futterman et al., 2010; Mundell et al., 2011; Richter et al., 2014; Wingood, DiClemente, Mikhail, Lang, McCree, Davies, Hardin, Hook, et al., 2004). The women’s well-being was the primary objective in two studies (Miles et al., 2003; Richter et al., 2014). The other studies’ primary aims were risk reduction, disclosure or child health. The included studies used different metrics to measure a range of psychosocial support outcomes (Table III). None of the included studies measured our secondary outcome of interest, SRH decision-making.
Table III.
Psychosocial Support Outcome Measures in Included Studies
| Psychosocial Support Outcome Measured | Studies Utilizing Measure | Measurement Tool |
|---|---|---|
| Self-Esteem | Mundell et al., 2011; Klein et al., 2013 | Rosenberg Self-Esteem Scale 10-item likert; 10-item scale (unspecified) |
| Coping (Active, Positive, Self-Coping | Eloff et al., 2014; Futterman et al., 2010; Mundell et al., 2011; Klein et al., 2013 | Brief COPE (3 studies including active, self, positive), 18-item coping scale (unspecified) |
| Avoidant Coping | Mundell et al., 2011, Eloff et al., 2014 | Brief COPE (2 studies) |
| Coping: help from others | Eloff et al., 2014 | Brief COPE |
| Positive Social Support | Mundell et al., 2011; Klein et al., 2013 | Multidimensional Social Support Inventory, 23-question scale (unspecified) |
| Social Support Availability | Wingood, et al., 2004; Futterman et al., 2010 | Number of network ties; Medical Outcomes Study Social Support Survey |
| Social Support Satisfaction | Futterman et al., 2010 | Medical Outcomes Study Social Support Survey |
| Negative Social Support | Mundell et al., 2011 | Multidimensional Social Support Inventory |
| Depression | Eloff et al., 2014; Futterman et al., 2010; Miles et al., 2003; Mundell et al., 2011; Kaaya et al., 2013; Richter et al., 2014 | Center for Epidemiologic Studies Depression scale (CES-D) (4 studies); 15-item depression subscale of the Hopkins Symptom Checklist-25 (HSCL-25); General Health Questionnaire (GHQ) |
| HIV discomfort | Futterman et al., 2010 | Read scenarios, replied with discomfort level on Likert scale |
| HIV stigma (perceived) | Echenique et al., 2012; Miles et al., 2003 | HIV Stigma Scale; Demi HIV Stigma Scale |
| Mood | Miles et al., 2003 | Profile of Mood States |
| HIV worry | Miles et al., 2003 | HIV Worry Scale designed for study |
| Stress | Klein et al., 2013 | 14-item stress scale (unspecified) |
Study Results
Results for each outcome measured are presented in Table I.
Mental, Emotional, Social Well-Being and/or Quality of Life
Coping
Included studies measured three different types of coping: 1) active, positive self-coping (Eloff et al., 2014; Futterman et al., 2010; Klein et al., 2013; Mundell et al., 2011), 2) avoidant (Eloff et al., 2014; Mundell et al., 2011), and 3) coping: help from others (Eloff et al., 2014). Metrics included the brief COPE (Eloff et al., 2014; Futterman et al., 2010; Mundell et al., 2011) and an 18-item coping scale (Klein et al., 2013). Results were mixed. Only one study, using a non-randomized trial design, found significant improvements in active (t=2.68, p-value=0.01) and avoidant coping (t=−2.02, p-value=0.04) (Mundell et al., 2011); all other results were null. Active coping was the only coping outcome measured by three or more studies. There were no clear patterns in active coping outcomes based on types of interventions (group versus individual), target populations (pregnant women versus others), the amount or frequency of interactions (2 – 24 sessions), follow-up time (3 – 18 months), or primary intervention objective (well-being versus instrumental).
Social Support
Included studies measured four types of social support: positive support (Klein et al., 2013; Mundell et al., 2011), support availability (Futterman et al., 2010; Wingood, DiClemente, Mikhail, Lang, McCree, Davies, Hardin, Hook, et al., 2004), support satisfaction (Futterman et al., 2010), and negative support (Mundell et al., 2011). Metrics included the ‘multidimensional social support inventory’ for positive and negative support (Mundell et al., 2011), the ‘medical outcomes study social support survey’ for availability and satisfaction (Futterman et al., 2010), a 23-question scale for positive support (Klein et al., 2013), and the number of network ties for support availability (Wingood, DiClemente, Mikhail, Lang, McCree, Davies, Hardin, Hook, et al., 2004). No studies showed improvement in positive social support or social support satisfaction. However, both studies measuring social support availability, a facility-randomized controlled trial (regression-b=9.32, SE=3.53, p-value=<0.05) (Futterman et al., 2010) and an individually-randomized controlled trial (% relative change=12.0, 95% CI: 0.5, 23.4, p-value=0.02) (Wingood, DiClemente, Mikhail, Lang, McCree, Davies, Hardin, Hook, et al., 2004) saw significant improvements among intervention compared to control participants. The only study measuring negative social support, a non-randomized trial, saw a significant decline among a sub-analysis of participants with high attendance at 8 months of follow-up (t=−2.41, p-value=<0.05) (Mundell et al., 2011).
Self-Esteem
Self-esteem was measured by two studies with mixed results. One showed significant improvement in self-esteem among a sub-group of participants with high attendance at 2 months of follow-up using the Rosenberg Self-Esteem Scale (t=2.11, p-value= <0.05) (Mundell et al., 2011). Results from the second study, an RCT using an unspecified 10-item scale, were null (Klein et al., 2013).
Perceived HIV Stigma
Both studies that measured perceived HIV stigma, one using the HIV Stigma Scale (Echenique et al., 2013), and the other using the Demi HIV Stigma Scale (Miles et al., 2003), saw significant improvements using individual RCTs. The intervention group in the first study had a significant decline in mean stigma score (baseline=104.6, endline=96.5, p-value=0.05) (Echenique et al., 2013). The second study found a significant decrease in perceived stigma (glm effect=−0.25, p-value=0.03) (Miles et al., 2003).
Other Measures
The following outcomes were each measured by one study: HIV discomfort, using scenarios and discomfort levels on a Likert scale (Futterman et al., 2010); mood, using Profile of Mood States (Miles et al., 2003); HIV worry, using an HIV worry scale (Miles et al., 2003); and stress, using a 14-item stress scale (Klein et al., 2013). Findings were null for all outcomes other than stress, which declined significantly in the intervention group compared to the control group (% relative change= −12.08, 95% CI:−3.76, −13.72) (Klein et al., 2013).
Common Mental Health Disorders
Depressive Symptoms
Six of the nine studies measured depressive symptoms, with mixed results. Two studies, one facility RCT and one non-randomized, facility-based trial design, showed significant differences in depression: one measured odds of not having depressive symptoms (OR=2.55, 95%CI: 1.37, 4.76, p-value=0.002) (Richter et al., 2014), the other measured presence of depressive symptoms (Regression-b=−4.43, SE=1.62, p-value=<0.01) but had unequal prevalence of depressive symptoms between comparison groups at baseline (Futterman et al., 2010). All other study results for this outcome were null (Eloff et al., 2014; Kaaya et al., 2013; Miles et al., 2003; Mundell et al., 2011). Measurement tools included the CES-D (Eloff et al., 2014; Futterman et al., 2010; Miles et al., 2003; Mundell et al., 2011), the 15-item depression sub-scale of the Hopkins Symptom Checklist-25 (Kaaya et al., 2013), and the General Health Questionnaire (Richter et al., 2014). As with coping, there were no clear patterns in depressive symptom outcomes based on types of interventions (group versus individual), target populations (pregnant women versus others), amount or frequency of interactions (6-24 sessions), follow-up time (6 weeks-18 months), or the primary intervention objective (well-being versus instrumental).
Intervention Characteristics
All studies that included a woman living with HIV as at least one of the intervention providers showed significant results (Echenique et al., 2013; Futterman et al., 2010; Mundell et al., 2011; Richter et al., 2014; Wingood, DiClemente, Mikhail, Lang, McCree, Davies, Hardin, Hook 3rd, et al., 2004). Five of the six studies that showed significant results where people, not a computer, delivered the intervention had women living with HIV as providers (Echenique et al., 2013; Futterman et al., 2010; Mundell et al., 2011; Richter et al., 2014; Wingood, DiClemente, Mikhail, Lang, McCree, Davies, Hardin, Hook 3rd, et al., 2004). All but one of the studies that showed significant results reported extensive grounding in theory and formative work to tailor the intervention to the target population (Futterman et al., 2010; Klein et al., 2013; Miles et al., 2003; Mundell et al., 2011; Richter et al., 2014; Wingood, DiClemente, Mikhail, Lang, McCree, Davies, Hardin, Hook 3rd, et al., 2004). All but four of the studies (Eloff et al., 2014; Kaaya et al., 2013; Klein et al., 2013; Wingood, DiClemente, Mikhail, Lang, McCree, Davies, Hardin, Hook, et al., 2004) experienced poor participant retention of less than 80% retained, with three studies experiencing retention of 51% or lower (Echenique et al., 2013; Futterman et al., 2010; Miles et al., 2003).
Discussion
Our systematic review identified 9 articles measuring the impact of psychosocial support interventions delivered by non-specialist providers to women living with HIV. Study designs were of variable quality and generally showed mixed or positive results for well-being and depressive symptoms indicators. In the literature, psychosocial support interventions were primarily designed and evaluated with regard to instrumental outcomes, such as care engagement (Wanyenze et al., 2011), medication adherence (Cook, Carrington, Schmiege, Starr, & Reeder, 2015; van Loggerenberg et al., 2015), sexual risk reduction (Echenique et al., 2013; Klein et al., 2013; Morin et al., 2007; Wingood, DiClemente, Mikhail, Lang, McCree, Davies, Hardin, Hook, et al., 2004), and disclosure (Mundell et al., 2011). No studies measured SRH decision-making. Women are more often supported in their role as expecting mothers or mothers (Eloff et al., 2014; Futterman et al., 2010; Richter et al., 2014), and less frequently supported as individuals with multiple, interactive identities and priorities. These gaps reflect several priority issues raised in the global survey of women living with HIV, including the desire for affordable, accessible, continuous, holistic, and integrated psychological support in HIV and SRH care from well-trained, compassionate providers covering topics including self-confidence, self-stigma, anxiety, isolation, acceptance and positive body image, and knowing and believing in rights (SalamanderTrust, 2014). To improve well-being, SRH, and uphold women’s rights, both physical and psychological health must be prioritized. Priorities and SRH preferences of women living with HIV as individuals should remain at the center of healthcare provision, and consequently focus solely on reducing HIV transmission. More research is needed on the role of psychosocial support in SRH and rights.
Most articles included in this review reported the meaningful involvement of women living with HIV in the design and delivery of interventions. Meaningful inclusion of women living with HIV was noted as a critical element of HIV interventions in the global survey (SalamanderTrust, 2014). This, and formative research conducted with women living with HIV, will help to ensure that interventions are contextually appropriate (Kako, Wendorf, Stevens, Ngui, & Otto-Salaj, 2016) and uphold the rights of women living with HIV (Orza et al., 2015). Theoretically-grounded research helps identify anticipated mechanisms and pathways of change, which is particularly important given the multi-faceted nature of psychosocial support (Glanz, Rimer, & Viswanath, 2008). Understanding the explicit theoretical grounding guiding behavior change interventions may help to support replication. However, further research is needed. Until more studies using similar outcome metrics are available, it is difficult to evaluate the effect of theoretical grounding on outcomes for women living with HIV.
Women living with HIV from key populations may have multiple additional identities which can render them even more socially disadvantaged (Orza et al., 2015). This disadvantage is associated with an increased experience of mental health issues, and these women are thereby more vulnerable to human rights violations and intersectional violence (Orza et al., 2015; WHO, 2016a). It is critical that future studies actively include them and conduct analyses to understand sub-group intervention effectiveness.
Implementation of psychosocial support interventions should work to increase participation retention, which may be related to study follow-up procedures, intervention timing (evening or weekend v. weekday), participant engagement with the subject matter and delivery, or other factors. The instrumental versus intrinsic focus of the intervention may also play a role. Also, research on psychosocial support interventions should also consider long-term follow-up post-intervention to determine the length of intervention effect, its perceived relevance to the women concerned, and possible follow-on support required.
Evidence Base and Study Limitations
The narrow population and geographical scope of the existing evidence base may limit the generalizability of the results. Four of the nine studies included only pregnant women with two more focused on mothers or primary caregivers. Only three countries were represented. The included studies all recruited women from healthcare organizations, so women living with HIV not currently engaged in formal care were not included.
Seventeen articles, including two from China and several with alternative delivery modalities (e.g. telephone), were not included because they did not disaggregate results by gender. While the intervention modalities included in this review, support groups and individual mentorship, reflect common intervention approaches, several approaches hypothesized to improve psychosocial wellbeing, such as physical exercise, were not used in any of the nine included articles.
This systematic review was limited to peer-reviewed articles. This helps ensure the inclusion of high quality research, but may miss potentially valuable, unpublished interventions, which may be more likely to be voluntary, locally-appropriate or sustainable without external support. Also, a single reviewer screened articles and conducted data abstraction, though a second coauthor did review coding results.
Conclusions
While outcomes were mixed, the available evidence suggests that support group and individual mentorship psychosocial support interventions may improve coping, self-esteem, and social support, and reduce depression, stress, and perceived stigma among women living with HIV. Interventions are optimally delivered by women living openly with HIV or by them together with others. Interventions should be relevant, acceptable and tailored to the health of women living with HIV. This may be best facilitated through theoretically-grounded interventions designed using formative research. Future studies using consistent outcome metrics are needed to understand the most effective intervention types and delivery mechanisms, as well as the relationship between psychosocial support and sexual and reproductive health and rights.
Acknowledgments
We wish to acknowledge the contributions of Dr. Sabina Haberlen.
Funding
This work was supported by the World Health Organization, Department of Reproductive Health and Research.
References
- Bateganya MH, Amanyeiwe U, Roxo U, & Dong M (2015). Impact of support groups for people living with HIV on clinical outcomes: a systematic review of the literature. J Acquir Immune Defic Syndr, 68 Suppl 3, S368–374. doi: 10.1097/qai.0000000000000519 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Biswas UN (2007). Promoting health and well-being in lives of people living with HIV and AIDS. Psychology and Developing Societies, 19(2), 215–247. doi: 10.1177/097133360701900205 [DOI] [Google Scholar]
- Carrico AW, & Antoni MH (2008). Effects of psychological interventions on neuroendocrine hormone regulation and immune status in HIV-positive persons: a review of randomized controlled trials. Psychosom Med, 70(5), 575–584. doi: 10.1097/PSY.0b013e31817a5d30 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Cook PF, Carrington JM, Schmiege SJ, Starr W, & Reeder B (2015). A counselor in your pocket: Feasibility of mobile health tailored messages to support HIV medication adherence. [No - instrumental outcome, adherence]. Patient Preference and Adherence, 9, 1353–1366. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Crepaz N, Passin WF, Herbst JH, Rama SM, Malow RM, Purcell DW, & Wolitski RJ (2008). Meta-analysis of cognitive-behavioral interventions on HIV-positive persons’ mental health and immune functioning. Health Psychol, 27(1), 4–14. doi: 10.1037/0278-6133.27.1.4 [DOI] [PubMed] [Google Scholar]
- Echenique M, Illa L, Saint-Jean G, Avellaneda VB, Sanchez-Martinez M, & Eisdorfer C (2013). Impact of a secondary prevention intervention among HIV-positive older women. AIDS Care, 25(4), 443–446. doi: 10.1080/09540121.2012.712666 [DOI] [PubMed] [Google Scholar]
- Eloff I, Finestone M, Makin JD, Boeving-Allen A, Visser M, Ebersohn L, … Forsyth BW (2014). A randomized clinical trial of an intervention to promote resilience in young children of HIV-positive mothers in South Africa. Aids, 28 Suppl 3, S347–357. doi: 10.1097/qad.0000000000000335 [DOI] [PMC free article] [PubMed] [Google Scholar]
- EngenderHealth, G., ICW, IPPF, UNAIDS, Young Positives. . (2009). Advancing the Sexual and Reproductive Health and Human Rights of People Living With HIV: A Guidance Package. Retrieved from Amsterdam: [Google Scholar]
- Feyissa GT, Lockwood C, & Munn Z (2015). The effectiveness of home-based HIV counseling and testing on reducing stigma and risky sexual behavior among adults and adolescents: A systematic review and meta-analyses. JBI Database System Rev Implement Rep, 13(6), 318–372. doi: 10.11124/jbisrir-2015-2235 [DOI] [PubMed] [Google Scholar]
- Fonner VA, Armstrong KS, Kennedy CE, O’Reilly KR, & Sweat MD (2014). School based sex education and HIV prevention in low- and middle-income countries: a systematic review and meta-analysis. PLoS ONE, 9(3), e89692. doi: 10.1371/journal.pone.0089692 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Futterman D, Shea J, Besser M, Stafford S, Desmond K, Comulada WS, & Greco E (2010). Mamekhaya: a pilot study combining a cognitive-behavioral intervention and mentor mothers with PMTCT services in South Africa. AIDS Care, 22(9), 1093–1100. doi: 10.1080/09540121003600352 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Genberg BL, Shangani S, Sabatino K, Rachlis B, Wachira J, Braitstein P, & Operario D (2016). Improving Engagement in the HIV Care Cascade: A Systematic Review of Interventions Involving People Living with HIV/AIDS as Peers. AIDS Behav. doi: 10.1007/s10461-016-1307-z [DOI] [PMC free article] [PubMed] [Google Scholar]
- Glanz KR, Rimer BK, & Viswanath K (Eds.). (2008). Health Behavior and Health Education: Theory, Research, and Practice (4th ed.). San Francisco: Jossey-Bass. [Google Scholar]
- Kaaya SF, Blander J, Antelman G, Cyprian F, Emmons KM, Matsumoto K, … Fawzi MCS. (2013). Randomized controlled trial evaluating the effect of an interactive group counseling intervention for HIV-positive women on prenatal depression and disclosure of HIV status. [Yes]. AIDS Care, 25(7), 854–862. doi: 10.1080/09540121.2013.763891 [DOI] [PubMed] [Google Scholar]
- Kako PM, Wendorf AR, Stevens PE, Ngui E, & Otto-Salaj LL (2016). Contending with Psychological Distress in Contexts with Limited Mental Health Resources: HIV-Positive Kenyan Women’s Experiences. Issues Ment Health Nurs, 37(1), 2–9. doi: 10.3109/01612840.2015.1058446 [DOI] [PubMed] [Google Scholar]
- Kennedy CE, Fonner VA, Armstrong KA, O’Reilly KR, & Sweat MD (2015). Increasing HIV serostatus disclosure in low and middle-income countries: a systematic review of intervention evaluations. AIDS, 29 Suppl 1, S7–s23. doi: 10.1097/qad.0000000000000671 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Kennedy CE, Haberlen S, Amin A, Baggaley R, & Narasimhan M (2015). Safer disclosure of HIV serostatus for women living with HIV who experience or fear violence: a systematic review. J Int AIDS Soc, 18(6 Suppl 5), 20292. doi: 10.7448/ias.18.6.20292 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Kennedy CE, Medley AM, Sweat MD, & O’Reilly KR (2010). Behavioural interventions for HIV positive prevention in developing countries: a systematic review and meta-analysis. [No]. Bull World Health Organ, 88(8), 615–623. doi: 10.2471/blt.09.068213 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Klein CH, Lomonaco CG, Pavlescak R, & Card JJ (2013). WiLLOW: reaching HIV-positive African-American women through a computer-delivered intervention. AIDS Behav, 17(9), 3013–3023. doi: 10.1007/s10461-013-0479-z [DOI] [PMC free article] [PubMed] [Google Scholar]
- Lingen-Stallard A, Furber C, & Lavender T (2016). Testing HIV positive in pregnancy: A phenomenological study of womens experiences. Midwifery, 35, 31–38. doi: 10.1016/j.midw.2016.02.008 [DOI] [PubMed] [Google Scholar]
- Lowther K, Harding R, Ahmed A, Gikaara N, Ali Z, Kariuki H, … Selman L (2016). Conducting experimental research in marginalised populations: clinical and methodological implications from a mixed-methods randomised controlled trial in Kenya. AIDS Care, 1–4. doi: 10.1080/09540121.2016.1146214 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Malary M, Khani S, Pourasghar M, Moosazadeh M, & Hamzehgardeshi Z (2015). BIOPSYCHOSOCIAL DETERMINANTS OF HYPOACTIVE SEXUAL DESIRE IN WOMEN: A NARRATIVE REVIEW. Mater Sociomed, 27(6), 383–389. doi: 10.5455/msm.2015.27.383-389 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Miles MS, Holditch-Davis D, Eron J, Black BP, Pedersen C, & Harris DA (2003). An HIV self-care symptom management intervention for African American mothers. Nurs Res, 52(6), 350–360. [DOI] [PubMed] [Google Scholar]
- Morin SF, Chesney MA, Ehrhardt AA, Kelly JA, Pequegnat W, Rotheram-Borus MJ, … Stover E (2007). Effects of a behavioral intervention to reduce risk of transmission among people living with HIV: The Healthy Living Project randomized controlled study. Journal of Acquired Immune Deficiency Syndromes, 44(2), 213–221. [DOI] [PubMed] [Google Scholar]
- Mundell JP, Visser MJ, Makin JD, Kershaw TS, Forsyth BWC, Jeffery B, & Sikkema KJ (2011). The impact of structured support groups for pregnant South African women recently diagnosed HIV positive. [Yes]. Women & Health, 51(6), 546–565. doi: 10.1080/03630242.2011.606356 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Mwai GW, Mburu G, Torpey K, Frost P, Ford N, & Seeley J (2013). Role and outcomes of community health workers in HIV care in sub-Saharan Africa: A systematic review. J Int AIDS Soc, 16. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Niu L, Luo D, Liu Y, Silenzio VM, & Xiao S (2016). The Mental Health of People Living with HIV in China, 1998-2014: A Systematic Review. PLoS ONE, 11(4), e0153489. doi: 10.1371/journal.pone.0153489 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Orza L, Bewley S, Logie CH, Crone ET, Moroz S, Strachan S, … Welbourn A (2015). How does living with HIV impact on women’s mental health? Voices from a global survey. J Int AIDS Soc, 18(Suppl 5), 20289. doi: 10.7448/ias.18.6.20289 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Paudel V, & Baral KP (2015). Women living with HIV/AIDS (WLHA), battling stigma, discrimination and denial and the role of support groups as a coping strategy: A review of literature. [No - review sources?***]. Reproductive Health, 12(1). [DOI] [PMC free article] [PubMed] [Google Scholar]
- Perazzo J, Reyes D, & Webel A (2016). A Systematic Review of Health Literacy Interventions for People Living with HIV. AIDS Behav. doi: 10.1007/s10461-016-1329-6 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Richter L, Rotheram-Borus MJ, Van Heerden A, Stein A, Tomlinson M, Harwood JM, … Tang Z (2014). Pregnant women living with HIV (WLH) supported at clinics by peer WLH: a cluster randomized controlled trial. AIDS Behav, 18(4), 706–715. doi: 10.1007/s10461-014-0694-2 [DOI] [PMC free article] [PubMed] [Google Scholar]
- SalamanderTrust. (2014). Building a safe house on firm ground: key findings from a global values and preferences survey regarding sexual and reproductive health and human rights of women living with HIV. Retrieved from Geneva: [Google Scholar]
- Scott-Sheldon LA, Kalichman SC, Carey MP, & Fielder RL (2008a). Stress management interventions for HIV+ adults: a meta-analysis of randomized controlled trials, 1989 to 2006. Health Psychology, 27(2), 129–139 111p. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Scott-Sheldon LA, Kalichman SC, Carey MP, & Fielder RL (2008b). Stress management interventions for HIV+ adults: a meta-analysis of randomized controlled trials, 1989 to 2006. Health Psychol, 27(2), 129–139. doi: 10.1037/0278-6133.27.2.129 [DOI] [PMC free article] [PubMed] [Google Scholar]
- van Loggerenberg F, Grant AD, Naidoo K, Murrman M, Gengiah S, Gengiah TN, … Abdool Karim SS (2015). Individualised motivational counselling to enhance adherence to antiretroviral therapy is not superior to didactic counselling in South African patients: findings of the CAPRISA 058 randomised controlled trial. AIDS Behav, 19(1), 145–156. doi: 10.1007/s10461-014-0763-6 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Vo QT, Hoffman S, Nash D, El-Sadr WM, Tymejczyk OA, Gadisa T, … Elul B (2016). Gender Differences and Psychosocial Factors Associated with Quality of Life Among ART Initiators in Oromia, Ethiopia. AIDS Behav. doi: 10.1007/s10461-016-1396-8 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Wanyenze RK, Hahn JA, Liechty CA, Ragland K, Ronald A, Mayanja-Kizza H, … Bangsberg DR (2011). Linkage to HIV care and survival following inpatient HIV counseling and testing. AIDS Behav, 15(4), 751–760. doi: 10.1007/s10461-010-9704-1 [DOI] [PMC free article] [PubMed] [Google Scholar]
- WHO. (2012). WHO recommendations: optimizing health worker roles to improve access to key maternal and newborn health interventions through task shifting. Retrieved from Geneva: [PubMed] [Google Scholar]
- WHO. (2013). Mental Health Action Plan 2013 - 2020. Retrieved from Switzerland: http://apps.who.int/iris/bitstream/10665/89966/1/9789241506021_eng.pdf?ua=1 [Google Scholar]
- WHO. (2016a). Consolidated Guidelines on HIV Prevention, Diagnosis, Treatment and Care for Key Populations. Retrieved from Geneva: http://www.who.int/hiv/pub/guidelines/keypopulations-2016/en/ [PubMed] [Google Scholar]
- WHO. (2016b). Psychosocial Support. Retrieved from http://www.who.int/hiv/topics/psychosocial/support/en/
- Wingood GM, DiClemente RJ, Mikhail I, Lang DL, McCree DH, Davies SL, … Saag M (2004). A randomized controlled trial to reduce HIV transmission risk behaviors and sexually transmitted diseases among women living with HIV: The WiLLOW Program. Journal of acquired immune deficiency syndromes (1999), 37 Suppl 2, S58–67. [DOI] [PubMed] [Google Scholar]
- Wingood GM, DiClemente RJ, Mikhail I, Lang DL, McCree DH, Davies SL, … Saag M (2004). A randomized controlled trial to reduce HIV transmission risk behaviors and sexually transmitted diseases among women living with HIV: The WiLLOW Program. J Acquir Immune Defic Syndr, 37 Suppl 2, S58–67. [DOI] [PubMed] [Google Scholar]
- Zajac K, Kennedy CE, Fonner VA, Armstrong KS, O’Reilly KR, & Sweat MD (2015). A Systematic Review of the Effects of Behavioral Counseling on Sexual Risk Behaviors and HIV/STI Prevalence in Low- and Middle-Income Countries. AIDS Behav, 19(7), 1178–1202. doi: 10.1007/s10461-014-0893-x [DOI] [PMC free article] [PubMed] [Google Scholar]