Abstract
Background
A dose-sparing inactivated polio vaccine (IPV-Al), obtained by adsorption of inactivated virus to an aluminium hydroxide adjuvant, can help mitigate global supply and the cost constraints of IPV. The objective of this trial was to demonstrate the non-inferiority of IPV-Al to standard IPV.
Methods
This phase 3, observer-blinded, randomised, controlled trial was conducted at 5 investigational sites in the Philippines. Infants not previously vaccinated with any polio vaccines were randomised to receive three IPV-Al (n = 502) or IPV vaccinations (n = 500) at 6, 10 and 14 weeks of age plus a booster vaccination at 9 months. The primary endpoint was type-specific seroconversion, defined as an antibody titre ≥4-fold higher than the estimated maternal antibody titre and a titre ≥8, one month after the primary vaccination series.
Results
Seroconversion rates following primary vaccination with IPV-Al (483 infants in the per-protocol analysis set) or IPV (478 infants) were: polio type 1, 97.1% versus 99.0%; type 2, 94.2% versus 99.0%; and type 3, 98.3% versus 99.6%. IPV-Al was non-inferior to IPV, as the lower 95% confidence limits of the treatment differences were above the predefined −10%-point limit: type 1, −1.85% (−3.85; −0.05); type 2, −4.75% (−7.28; −2.52); type 3, −1.24 (−2.84; 0.13). The booster effect (geometric mean titre (GMT) post-booster / GMT pre-booster) was: type 1, 63 versus 43; type 2, 54 versus 47; type 3, 112 versus 80. IPV-Al was well tolerated with a safety profile comparable to that of IPV. Serious adverse events were recorded for 29 infants (5.8%, 37 events) in the IPV-Al group compared to 28 (5.6%, 48 events) in the IPV group.
Conclusion
Non-inferiority of IPV-Al to IPV with respect to seroconversion was confirmed and a robust booster response was demonstrated. Both vaccines had a similar safety profile.
ClinicalTrials.gov identifier: NCT03032419.
Keywords: Affordable IPV, Aluminium hydroxide adjuvant, Booster vaccination, Immunogenicity, Polio, Primary vaccination
1. Introduction
The world is closer than ever to achieving the aim of polio eradication with more than 99.9% reduction in cases since the time The World Health Assembly launched the Global Polio Eradication Initiative (GPEI) in 1988 [1]. According to the Polio Eradication & Endgame Strategic Plan [2], withdrawal of the oral polio vaccine (OPV), as its use carries a small risk of vaccine-associated paralytic poliomyelitis (VAPP) and circulating vaccine-derived poliovirus (cVDPV) [3], and introduction of inactivated polio vaccine (IPV) are key strategic steps to complete and sustain eradication. The transition to IPV leads to increasing demand for IPV and requires that the constraints in terms of cost and supply availability of IPV are overcome [4]. AJ Vaccines has developed a dose sparing IPV, obtained by adsorption of the inactivated virus to an aluminium hydroxide (Al(OH)3) adjuvant, which has enabled the reduction of the amount of antigen by up to ten times compared to the currently used IPV. Promising results of nonclinical studies [5] and clinical trials [6], [7] have demonstrated that reduced-dose vaccines are safe, and their immunogenicity is retained. In a phase 2 observer-blinded, randomised, controlled trial, the immunogenicity and safety of three vaccines with doses of 1/3, 1/5 or 1/10 of the IPV dose were investigated in infants [7]. All three vaccines were non-inferior to IPV with respect to seroconversion rates, with absolute differences in percentage seroconversion for each poliovirus type being greater than the −10% non-inferiority margin. The phase 3 trials were conducted with the adjuvanted IPV with ten-times reduced antigen content (IPV-Al). Advantages of a reduction in antigen content are two-fold: increased availability of IPV and reduced cost, both of major importance for the global eradication programme.
In the present trial, healthy infants from the Philippines received 3 vaccinations of either IPV-Al or standard IPV at 6, 10 and 14 weeks of age, according to the World Health Organization (WHO) expanded programme of immunisation (EPI) schedule [2], plus a booster dose at 9 months. The primary objective was to demonstrate non-inferiority of seroconversion for poliovirus types 1, 2 and 3 for IPV-Al compared to IPV in infants one month after the primary vaccination series. The primary endpoint, type-specific seroconversion, was defined to include infants with both a titre ≥4 times higher than the estimated remaining maternal antibody at 18 weeks and a titre ≥8 at 18 weeks (seroprotection). The endpoint combined measures of the infant’s response to the vaccination (as titres were required to be ≥4 times higher than the estimated levels of maternal antibody) and seroprotection (the established correlate of protection for polio) [8], [9], [10]. Secondary immunogenicity objectives included evaluations of antibody titres one month after the primary vaccination series and the immunogenic responses to the two vaccines following the 9-month booster vaccination. An evaluation of the safety profile of each vaccine was also a secondary objective.
2. Methods
2.1. Trial design and participants
This was a phase 3, non-inferiority, observer-blinded, randomised (1:1), controlled, multicentre clinical trial with two parallel groups of infants who received three IPV-Al (n = 502) or IPV vaccinations (n = 500) at 6, 10 and 14 weeks of age (primary series) plus a booster vaccination at 9 months of age (a total of 4 vaccinations). Blood samples were taken prior to the vaccination at 6 weeks and at 18 weeks (pre- and post-primary vaccination series) and prior to the vaccination at 9 months and at 10 months (pre- and post-booster vaccination).
The trial was conducted at five investigational sites in Manila or greater Manila, the Philippines. Trial participants were recruited by contacting parents during late pregnancy or when attending the maternity ward. The participants were healthy infants aged 6 weeks on the date of the first vaccination who had not previously been vaccinated with any polio vaccine. Parents/guardians of the infants were informed about the trial and signed consent allowing their child to be included and to receive the trial vaccine. They also granted access to the infant's trial-related medical records. Key exclusion criteria included known exposure to OPV or any wild or vaccine-derived poliovirus in the household within 3 months before inclusion, a low birth weight (<2.5 kg), known or suspected immunodeficiency or family history of congenital or hereditary immunodeficiency, severe uncontrolled chronic disease, and known or suspected allergy to the vaccine constituents.
The trial protocol was approved by the relevant ethics committees and competent authorities prior to trial commencement and the trial was conducted according to the principles of good clinical practice [11] and the Declaration of Helsinki [12]. The trial is registered with ClinicalTrials.gov (NCT03032419).
2.2. Trial vaccines
The investigational and comparator vaccines were both manufactured by Statens Serum Institut (now manufactured by AJ Vaccines) (Copenhagen S, Denmark)1 and contained inactivated poliovirus types 1 (Brunhilde), 2 (MEF-1) and 3 (Saukett). The comparator vaccine was a licenced non-adjuvanted standard IPV vaccine containing 40 D-antigen units (DU) of poliovirus type 1, 8 DU of type 2 and 32 DU of type 3, and appearing as a clear solution for injection. The investigational IPV-Al vaccine was also a trivalent IPV vaccine containing approximately one tenth of the amount of each antigen in the IPV vaccine, adjuvanted to aluminium hydroxide (0.5 mg aluminium), appearing as an opaque suspension for injection.
One vaccine dose of 0.5 mL IPV-Al or standard IPV was administered intramuscularly perpendicular to the skin in the anterolateral aspect of the thigh using a sterile disposable syringe fitted with a 23-gauge, 25 mm needle. In addition to the trial vaccinations, the infants received concomitant childhood vaccinations during the trial period. The trial vaccines were administered in the right thigh, whereas the other injectable childhood vaccines were administered in the left thigh.
2.3. Randomisation and blinding
A randomisation list was generated by an unblinded statistician using SAS software, version 9.4 (SAS Institute, Cary, NC, USA), who did not otherwise participate in the trial. The list was uploaded into the electronic case report form so that the site could automatically randomise the trial participants. Each randomised infant was given the lowest available subject number.
As the two vaccine formulations were visually distinguishable, the observer-blinded nature of the trial meant that only prespecified unblinded site staff and the trial monitor had access to the trial vaccines and dispensing logs during the trial. Only unblinded site personnel and parents were present during administration of the vaccines, and the investigators and other individuals associated with the trial remained blinded.
2.4. Immunogenicity endpoints
The primary endpoint was the proportion of infants with type-specific seroconversion one month after the primary vaccination series, defined as (1) a post-vaccination antibody titre ≥4-fold higher than the estimated maternal antibody titre, based on the pre-vaccination titre declining by a half-life of 28 days, and (2) a post-vaccination titre ≥8. The established correlate of protection against polio is a neutralising antibody titre of ≥8 for the poliovirus types 1, 2 and 3 [8], [9], [10].
The two components of the primary endpoint were also included separately as secondary endpoints. Thus, secondary immunogenicity-related endpoints included the proportion of infants with seroprotection (antibody titre ≥8) against poliovirus types 1, 2 and 3, respectively, one month after the primary vaccination series and before and one month after the booster vaccination at 9 months. Geometric mean titres (GMTs) and median antibody titres were also measured. The proportion of infants with post-vaccination titres ≥4-fold higher than the estimated maternal antibody titre was evaluated for both vaccines. The booster effects (GMT post-booster/GMT pre-booster = GMTR) were assessed, as well as the booster effect ratios (GMTR IPV-Al/GMTR IPV) from the 9 months (pre-booster) and 10 months (post-booster) antibody titre measurements for the three poliovirus types. Antibody persistence, measured as the decline in titres from one month after the primary vaccination series to the time of the booster vaccination, was compared between the two vaccines.
A subgroup analysis of the proportion of infants with seroconversion one month after the primary vaccination series, as defined by the primary endpoint, was performed in infants with seroprotection (titre ≥8) and without seroprotection (titre <8) at baseline (week 6). The proportion with seroprotection (titre ≥8) one month after the primary vaccination series as well as one month after the booster vaccination at 9 months was also analysed.
A validated Vero cell assay was used for the antibody titre determinations and has been described previously [6], [13].
2.5. Safety endpoints
The infants remained at the investigational site for 30 min after each vaccination under observation by the trial staff in case of adverse events (AEs). Thereafter, the parents/guardians were given a diary, ruler and thermometer and, on the vaccination day and subsequent 2 days, were to measure and report in the diary details of any injection site redness (erythema)/swelling (measured in mm) at the injection site of the study vaccines, axillary temperature, persistent crying, irritability, drowsiness, loss of appetite and vomiting (solicited AEs), as well as any other AEs. Information on any concomitant medication or other vaccines administered between the trial visits was also reported. During days 3–6 after each vaccination, the parents/guardians were to complete details in the diary only if they detected an AE, or if the infant received medication or other vaccines between the trial visits. The site investigator interviewed the parents/guardians at the subsequent trial visit, assessed all AEs according to their causality, intensity, outcome and seriousness, and transferred the information to the electronic case report form. Safety endpoints were solicited injection site events, solicited systemic AEs and all other AEs following the vaccinations.
2.6. Statistical analyses
Randomised controlled clinical vaccine trials tend to use a non-inferiority margin of either 5% or 10% [14]; the choice of margin is dependent on different factors. For the primary immunogenicity endpoint, a non-inferiority margin of 10% was applied. This margin was justified by the strict primary endpoint requiring both seroconversion (a post-vaccination titre ≥4-fold higher than the estimated maternal antibody titre) and seroprotection (a post-vaccination titre ≥8), which is stricter than seroprotection only, together with the fact that the risk of poliomyelitis infection has decreased significantly in recent years. For the secondary immunogenicity endpoint, seroprotection, a narrower non-inferiority margin of 5% was chosen.
The sample size calculation was based on seroconversion rates (ranging from 94.6% to 100%) demonstrated in the phase 2 dose-investigation clinical trial [7]. If the true seroconversion for IPV-Al was lower than for IPV, e.g. by 5 percentage points for all 3 poliovirus types, then 350 participants per treatment group was considered sufficient to achieve a power of >80%. Based on these considerations, a non-inferiority margin of 10% for the primary immunogenicity endpoint analysis, and allowing for possible exclusion of up to 15% of infants (due to withdrawals or major protocol deviations), as well as advice from the European Medicines Agency, a sample size of 500 infants per group was to be included.
The primary immunogenicity analyses were based on the per-protocol (PP) analysis set (defined as all participants in the full analysis set (FAS) who had no major protocol deviations). Sensitivity analyses of the primary endpoint were performed using the FAS (defined as all randomised and vaccinated infants with a valid primary endpoint for at least 1 poliovirus type). In order to qualify for the primary analysis, the availability of each of the components of the primary endpoint (a type-specific post-vaccination antibody titre ≥4-fold higher than the estimated maternal antibody titre as well as a type-specific post-vaccination titre ≥8) was required. For a given poliovirus type, if either baseline or post-vaccination titres were missing, the seroconversion result was assigned a missing value. The estimated maternal antibody titre was calculated as:
where t was the time in days since baseline and t½ was the expected half-life of maternal antibodies of 28 days [15].
Non-inferiority of IPV-Al to IPV was demonstrated only if non-inferiority of the seroconversion rates was achieved for each of the 3 poliovirus types 1, 2 and 3; hence, no multiplicity adjustment was needed. Each of the primary immunogenicity analyses was evaluated by calculating the rate difference (Pi, IPV-Al – Pi, IPV) with a two-sided 95% confidence interval (CI) based on observed cases, i.e. disregarding missing values. The 95% CI was calculated as an approximative Newcombe-Wilson interval [16], and non-inferiority could be claimed if the lower 95% confidence limit was greater than the −10% non-inferiority margin. This comparison corresponded to a one-sided test at a significance level of 2.5%.
The non-inferiority testing used for the primary endpoint in the PP analysis set was repeated for the seroprotection endpoint one month after the primary vaccination series, using a 5% margin. The rate differences and confidence limits for the secondary immunogenicity endpoints were derived in the same way as for the primary endpoint. Geometric mean and median titres for poliovirus types 1, 2 and 3 as well as safety endpoints were summarised using descriptive statistics. SAS software, version 9.4, was used for the analyses.
3. Results
3.1. Population characteristics
The trial was conducted between 6 February 2017 (the first trial visit) and 12 March 2018 (the last trial visit). In the trial, 1042 potential participants were screened and assessed for eligibility, of which 40 were screen failures (Fig. 1). The enrolled participants (N = 1002) were randomised to receive either the IPV-Al vaccine (n = 502) or the comparator IPV (n = 500) vaccine. Overall, 968 infants (96.6%) completed the trial visit one month after the primary vaccination series and 924 (92.2%) infants completed the last trial visit one month after the booster vaccination (Fig. 1). Two infants in the IPV-Al group and 3 in the IPV group were excluded from the PP analysis set due to major protocol deviations.
Fig. 1.
Trial profile. Visit 4 was one month after the primary vaccination series at 14 weeks. Visit 6 was one month after the booster vaccination at 9 months. The full analysis set (FAS) was defined as all randomised and vaccinated infants with a valid primary endpoint for at least one poliovirus type. The per-protocol analysis set was defined as all infants in the FAS who had no major deviations from the protocol. The safety analysis set was defined as all randomised infants who received at least one treatment dose. N = number of infants in the group.
Both vaccination groups were comparable in terms of demography and baseline characteristics (Table 1).
Table 1.
Baseline characteristics of the trial population.
| Characteristic | IPV-Al N = 502 |
IPV N = 500 |
|---|---|---|
| Sex, n (%) | ||
| Male | 255 (50.8) | 255 (51.0) |
| Female | 247 (49.2) | 245 (49.0) |
| Race Asian, n (%) | 502 (100) | 500 (100) |
| Age, days | 45.06 (4.3) | 45.06 (4.6) |
| Birth weight, kg | 3.05 (0.36) | 3.05 (0.35) |
Data are n (%) or mean (SD) for participants in the safety analysis set.
N = number of infants, SD = standard deviation.
3.2. Immunogenicity results
The seroconversion (primary endpoint) rates for poliovirus types 1, 2 and 3 following primary immunisation are presented in Table 2. Seroconversion rates after vaccination with three doses of IPV-Al compared to IPV were: type 1: 97.1% versus 99.0%; type 2: 94.2% versus 99.0%; and type 3: 98.3% versus 99.6%. Non-inferiority of IPV-Al to IPV with respect to the primary endpoint of seroconversion was demonstrated for each of the 3 poliovirus types, as indicated by the lower limit of the two-sided 95% CIs of the rate differences being above the predefined limit of −10%-points (Table 2).
Table 2.
Non-inferiority analysis of seroconversion (primary endpoint) and secondary endpoint seroprotection (titre ≥ 8) rates one month after the primary vaccination series.
| Poliovirus type | IPV-Al N = 483 % (95% CI) |
IPV N = 478 % (95% CI) |
Treatment difference (95% CI) |
|---|---|---|---|
| Seroconversion | |||
| Type 1 | 97.1 (95.2 to 98.4) | 99.0 (97.6 to 99.7) | −1.85 (-3.85 to −0.05) |
| Type 2 | 94.2 (91.7 to 96.1) | 99.0 (97.6 to 99.7) | −4.75 (-7.28 to −2.52) |
| Type 3 | 98.3 (96.8 to 99.3) | 99.6 (98.5 to 99.9) | −1.24 (-2.84 to 0.13) |
| Seroprotection | |||
| Type 1 | 97.9 (96.2 to 99.0) | 99.6 (98.5 to 99.9) | −1.65 (-3.38 to −0.21) |
| Type 2 | 100 (99.2 to 100) | 99.6 (98.5 to 99.9) | 0.42 (-0.43 to 1.51) |
| Type 3 | 99.0 (97.6 to 99.7) | 99.8 (98.8 to 100) | −0.83 (-2.20 to 0.31) |
Data are presented for the per-protocol analysis set. The primary endpoint was defined as (1) a type-specific post-vaccination titre ≥4-fold higher than the estimated maternal antibody titre, based on the pre-vaccination titre declining by a half-life of 28 days, and (2) a type-specific post-vaccination titre ≥8.
CI = confidence interval, N = number of infants in trial group.
In a sensitivity analysis of the primary seroconversion endpoint in the FAS, no major difference between the PP and the FAS population results was observed and non-inferiority of IPV-Al to IPV was also demonstrated in the FAS (treatment difference of −1.85%, −4.73% and −1.23% for type 1, 2 and 3 poliovirus types, respectively).
The two components of the primary endpoint were also analysed separately in the PP population. For IPV-Al compared with IPV, the rates for titres ≥4-fold the estimated maternal antibody titres were: type 1: 99.2% versus 99.2%; type 2: 94.2% versus 99.0%; and type 3: 99.2% versus 99.6%. In addition, between 97.9 and 100% of infants in the IPV-Al group and between 99.6 and 99.8% of those in the IPV group were seroprotected (antibody titres ≥8) after the primary vaccination series (Table 2), and non-inferiority (5%-margin) of the seroprotection of IPV-Al to IPV was confirmed across poliovirus types.
The baseline GMTs at week 6 were similar in both vaccine groups (Table 3). The post-primary vaccination GMTs were high for all poliovirus types, regardless of treatment group, and were higher with IPV than with IPV-Al. A decline in GMTs from the post-primary vaccination series to the booster vaccination at 9 months was observed for all poliovirus types regardless of vaccine used. The decline appeared to be similar in both groups (supplementary figure), although the GMTs remained higher with IPV than IPV-Al.
Table 3.
Summary of seroprotection rates and serum neutralising antibody titres for poliovirus types 1, 2 and 3.
| Poliovirus type and endpoint |
Baseline (age 6 weeks) |
Post-primary vaccination (age 18 weeks) |
Pre-booster vaccination (age 9 months) |
Post-booster vaccination (age 10 months) |
||||
|---|---|---|---|---|---|---|---|---|
| IPV-Al n = 483 |
IPV n = 478 |
IPV-Al n = 483 |
IPV n = 478 |
IPV-Al n = 449 |
IPV n = 449 |
IPV-Al n = 441 |
IPV n = 442 |
|
| Type 1 | ||||||||
| Seroprotection (titre ≥ 8), % | 60.5 | 60.7 | 97.9 | 99.6 | 88.0 | 100.0 | 99.8 | 100.0 |
| GMT (95% CI) | 12.2 (10.6 to 14.1) | 12.2 (10.6 to 14.1) | 739.8 (635 to 862) | 3837 (3493 to 4216) | 132.3 (109 to 160) | 746.2 (666 to 836) | 8394 (7122 to 9894) | 31,558 (28798 to 34582) |
| Median titre | 11.3 | 11.3 | 1024 | 4096 | 181 | 724 | 11,585 | 32,768 |
| Type 2 | ||||||||
| Seroprotection (titre ≥ 8), % | 88.0 | 90.4 | 100.0 | 99.6 | 99.8 | 99.8 | 100.0 | 100.0 |
| GMT (95% CI) | 50.0 (43.4 to 57.6) | 49.8 (43.5 to 57.1) | 1272 (1135 to 1425) | 3611 (3279 to 3976) | 351.8 (314 to 395) | 748.5 (679 to 825) | 18,933 (17033 to 21045) | 35,164 (32239 to 38355) |
| Median titre | 64.0 | 45.3 | 1448 | 4096 | 362 | 724 | 16,384 | 32,768 |
| Type 3 | ||||||||
| Seroprotection (titre ≥ 8), % | 55.3 | 57.5 | 99.0 | 99.8 | 93.5 | 99.8 | 100.0 | 100.0 |
| GMT (95% CI) | 9.9 (8.7 to 11.2) | 11.6 (10.1 to 13.3) | 1110 (974 to 1265) | 4590 (4155 to 5071) | 142.9 (121 to 169) | 633.6 (559 to 718) | 15,691 (13767 to 17883) | 49,964 (45533 to 54826) |
| Median titre | 8.0 | 11.3 | 1448 | 4096 | 181 | 724 | 16,384 | 46,341 |
Data are presented for the per-protocol analysis set. CI = confidence interval, GMT = geometric mean titre, n = number of infants in trial group.
There was a sharp increase in antibody titres following the booster vaccination with both vaccines (Table 3). The post-booster GMTs were higher with IPV than IPV-Al for all poliovirus types. Regardless of vaccine, the GMTs were well in excess of the seroprotection threshold. The post-booster seroprotection rates for both vaccination groups were high, ranging from 99.8 to 100% of infants across poliovirus types (Table 3); only one infant (in the IPV-Al group) did not have seroprotection after the booster vaccination.
The booster effect (GMT post-booster/GMT pre-booster = GMTR) for the IPV-Al group compared with the IPV group was: 63 (95% CI 54; 73) vs 43 (37; 50) for type 1, 54 (48; 61) vs 47 (42; 53) for type 2 and 112 (95; 131) vs 80 (68; 93) for type 3. The booster effect ratios (GMTR IPV-Al/GMTR IPV) were 1.46 (1.18; 1.80) for type 1, 1.15 (0.97; 1.36) for type 2 and 1.40 (1.12; 1.75) for type 3.
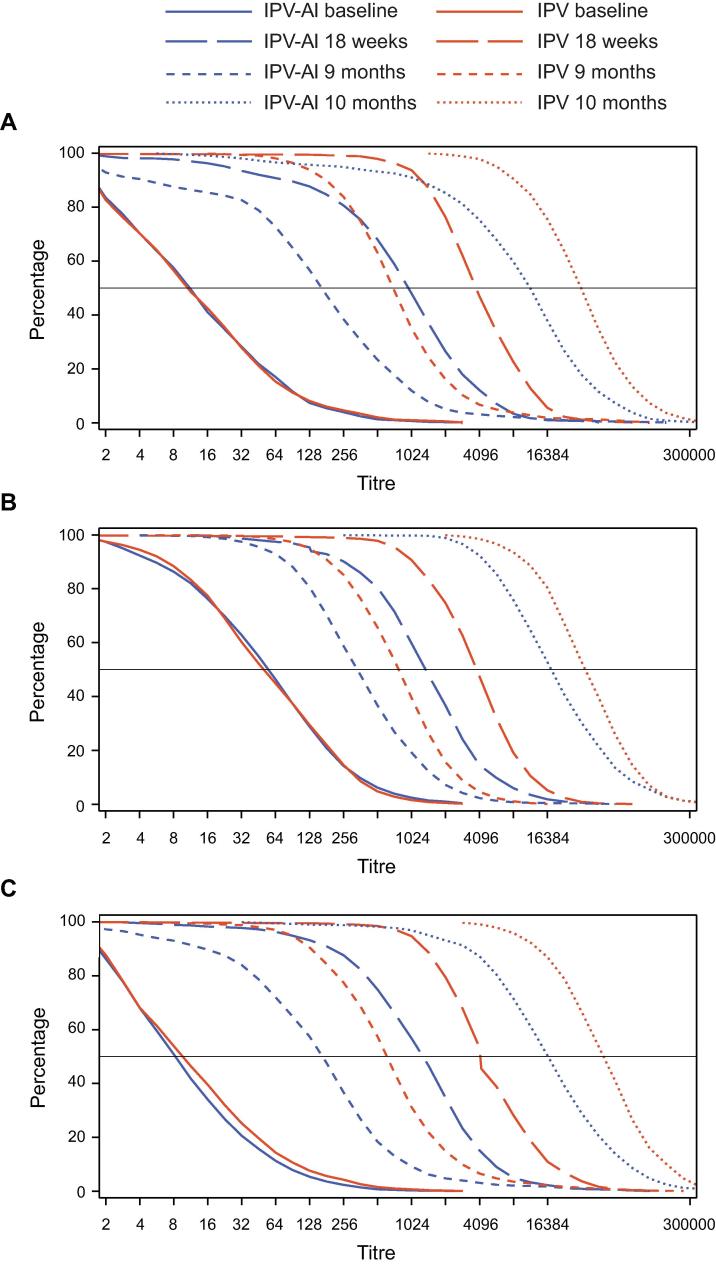
Reverse cumulative titre distribution curves (Fig. 2) illustrate the changes in antibody titre distributions before and after the primary and booster vaccinations. For each poliovirus type, the baseline curves are almost identical in the two groups. The post-primary vaccination curves illustrate that both vaccines were immunogenic with similar curve shapes for the two vaccines across poliovirus types. The pre-booster vaccination curves illustrate the decline in antibody levels from post- 3rd primary vaccination to pre-booster vaccination. The post-booster vaccination curves illustrate an increase in antibody titres for all poliovirus types in both vaccination groups. The shape of the post-primary and post-booster vaccination curves reflects the wider distribution of titres for type 1 and 3 serotypes than for type 2 in both IPV-Al and IPV vaccinated infants.
Fig. 2.
Reverse cumulative antibody titre distribution curves at baseline (6 weeks), post-primary vaccination (18 weeks), pre-booster (9 months) and post-booster vaccination (10 months) for poliovirus type 1 (A), type 2 (B) and type 3 (C).
In a subgroup analysis, more than 93.4% of infants in both treatment groups obtained seroconversion (primary endpoint) across all 3 poliovirus types following the primary vaccination series, irrespective of their seroprotection status at baseline (week 6). Similarly, more than 94.8% of infants in both treatment groups were seroprotected after the primary vaccination series across all 3 poliovirus types, irrespective of their seroprotection status at baseline, and all except for one infant in the IPV-Al group (titre of 5.7 for poliovirus type 1) were seroprotected after the booster vaccination.
3.3. Safety results
In total, 489 of 502 infants (97.4%) in the IPV-Al group and 492 of 500 infants (98.4%) in the IPV group had at least one AE reported by their parent/guardian over the course of the trial. The proportion of serious AEs was similar between groups: 29 infants (5.8%) in the IPV-Al group had 37 serious AEs recorded and 28 (5.6%) in the IPV group had 48 serious AEs recorded. All serious AEs were assessed as not related to the trial vaccine, except for one case of febrile seizure (IPV group) that was assessed as possibly related to treatment.
Five cases had a fatal outcome during the trial: two in the IPV-Al group due to pneumonia and sudden infant death syndrome and three in the IPV group due to gastroenteritis, parasitic gastroenteritis, pneumonia and febrile convulsion; hypovolemic shock and malnutrition; and pneumonia. None of the deaths were assessed as being related to the trial vaccines.
Overall, the proportion of infants with at least one injection site reaction was similar between the IPV-Al (46.2%) and IPV (42.2%) treatment groups (Table 4). All injection site reactions were assessed as either mild or moderate in intensity. Almost all events were either erythema (40.4% of infants in the IPV-Al group and 38.4% in the IPV group) or swelling (34.9% and 29.6%, respectively). Most of the cases of erythema (94%) and swelling (85%) were <25 mm in diameter; less than 2% had a diameter ≥50 mm. The proportion of infants with at least one systemic AE was also similar between IPV-Al (97.2%) and IPV (98.0%) vaccines. The four most common systemic AEs were pyrexia, upper respiratory tract infection, irritability and somnolence. Almost all events (98%) were of mild intensity; 0.3% were severe, and most (62.9%) were considered related to treatment.
Table 4.
Summary of adverse injection site reactions and adverse events with a frequency of at least 5% of infants in any group.
| Adverse event type | IPV-Al N = 502 n (%) e |
IPV N = 500 n (%) e |
|---|---|---|
| Mild adverse injection site reactions | 230 (45.8) 848 | 208 (41.6) 715 |
| Injection site erythema | 202 (40.2) 488 | 191 (38.2) 407 |
| Injection site swelling | 171 (34.1) 356 | 144 (28.8) 304 |
| Injection site pain | 3 (0.6) 3 | 2 (0.4) 2 |
| Injection site bruising | 1 (0.2) 1 | 1 (0.2) 1 |
| Injection site dermatitis | – | 1 (0.2) 1 |
| Moderate adverse injection site reactions | 12 (2.4) 19 | 15 (3.0) 18 |
| Injection site swelling | 11 (2.2) 15 | 12 (2.4) 12 |
| Injection site erythema | 4 (0.8) 4 | 4 (0.8) 5 |
| Injection site pain | – | 1 (0.2) 1 |
| AEs with frequency ≥ 5% | 488 (97.2) 3139 | 490 (98.0) 3322 |
| Pyrexia | 425 (84.7) 838 | 448 (89.6) 980 |
| URTI | 284 (56.6) 503 | 279 (55.8) 469 |
| Irritability | 232 (46.2) 427 | 250 (50.0) 514 |
| Somnolence | 203 (40.4) 381 | 220 (44.0) 419 |
| Rhinitis | 99 (19.7) 127 | 67 (13.4) 84 |
| Decreased appetite | 77 (15.3) 119 | 88 (17.6)115 |
| Pneumonia | 74 (14.7) 94 | 72 (14.4) 85 |
| Systemic viral infection | 62 (12.4) 77 | 70 (14.0) 84 |
| Crying | 38 (7.6) 51 | 58 (11.6) 88 |
| Gastroenteritis | 51 (10.2) 57 | 43 (8.6) 49 |
| Nasopharyngitis | 51 (10.2) 55 | 34 (6.8) 35 |
| Vomiting | 43 (8.6) 52 | 36 (7.2) 47 |
| Viral rash | 27 (5.4) 28 | 23 (4.6) 24 |
| Bronchitis | 18 (3.6) 18 | 25 (5.0) 26 |
Data are for infants in the safety analysis set. AEs are presented by MedDRA (version 19.1) preferred term.
AE = adverse event, e = number of events, MedDRA = Medical Dictionary for Regulatory Activities, N = number of infants in group, n (%) = number (percentage) of infants with AE, URTI = upper respiratory tract infection.
4. Discussion
In the present phase 3 trial, the IPV-Al vaccine demonstrated high post-primary vaccination (WHO EPI schedule) seroconversion rates ranging from 94.2 to 98.3% across poliovirus types, comparable to those of IPV, which ranged from 99.0 to 99.6%. Non-inferiority of IPV-Al to IPV was confirmed with respect to the primary endpoint of seroconversion, using a non-inferiority margin of 10%, for each poliovirus type in the trial population of healthy infants from the Philippines. Following the primary vaccination series, seroprotection levels ranged from 97.9% to 100% for IPV-Al and from 99.6% to 99.8% for IPV, and non-inferiority of IPV-Al to IPV was confirmed. One month after the booster vaccination at 9 months, a clear immune response was demonstrated for both vaccines, with increases in both seroprotection rates and GMT levels. Antibody titre declines during the 6-month period from completed priming until the booster vaccination appeared to be similar in the IPV-Al and IPV groups. Overall, the results of the present trial support the applicability of the dose-sparing IPV-Al vaccine to help secure a stable supply of IPV for prevention of poliomyelitis.
The results of the present trial confirm those previously observed with the IPV-Al. In a phase 2 randomised, controlled trial [7], the IPV-Al vaccine was also non-inferior to IPV as regards seroconversion rates according to the same definition. In both trials, the post-primary vaccination GMTs for the three poliovirus types were lower in the IPV-Al group than the IPV group, most likely due to the lower antigen content of the IPV-Al vaccine. Regardless of vaccine, the GMTs were well in excess of the seroprotection threshold. After primary vaccination, the large majority of infants seroconverted (IPV-Al ≥94.2%; IPV ≥99.0% across poliovirus types) and were seroprotected (antibody titres ≥8) (IPV-Al ≥97.9%; IPV ≥99.6% across poliovirus types). Thus, in the present trial, it is considered unlikely that the lower GMTs in the IPV-Al group are clinically important. Irrespective of seroprotection status at baseline, high seroconversion and seroprotection rates were observed following primary vaccination. The booster vaccination administered approximately 6 months after completion of the primary vaccination series induced a clear immune response. Following the booster vaccination, there were no differences between the two vaccines in seroprotection rates across poliovirus types (99.8%-100% for IPV-Al and 100% for IPV), and seroprotection was obtained for all but one infant in the IPV-Al group. The pronounced booster effect indicates that although antibody titres had declined 6 months after the primary vaccination series, immunological priming ensured continued protection through an efficient booster response. Lasting immunity depends on adequate priming i.e. establishment of immune memory (generation of B memory cells). Immunological priming after vaccination with IPV-Al was demonstrated by robust booster effects and increase in post-booster GMTs compared to post-primary GMTs. The strong booster response after vaccination with IPV-Al indicates that immune memory has been established during the primary vaccination. Consequently, should titre levels fall below the protective threshold over time, following antigenic re-stimulation (from vaccine or poliovirus) antibody concentrations are expected to return to above the seroprotective threshold in virtually all of the population vaccinated with IPV-Al. A booster response was previously observed in a phase 1/2 trial, in which three reduced-dose vaccines, including the 1/10 IPV-Al used in the present trial, were administered as a booster dose to adolescents previously vaccinated with IPV at 3, 5 and 12 months and at 5 years [6]. Thus, IPV-Al does induce a booster effect in both IPV and IPV-Al primed individuals. The comparator used in this trial, IPV, was the same as that used in other trials investigating IPV-Al [17], [18].
In areas where poliovirus is endemic, early immunisation of infants is important and, according to the WHO EPI schedule [2], primary vaccination of infants at 6, 10 and 14 weeks of age is recommended, as used in the present trial. New-born infants are protected from polio by maternal antibodies transferred from the mother during the second trimester of pregnancy [19]. This passive immunity declines in a time-dependent manner as the maternal antibodies decay. Maternal antibodies have been shown to interfere with the infant serologic response to IPV vaccination [20]. Vaccinations given at 6, 10 and 14 weeks, the EPI schedule, is thus considered a more challenging schedule than the schedule at 2, 4 and 6 months due to the presence of more maternal antibodies.
Previous trials have also investigated the use of reduced doses of IPV compared to standard IPV, with the ultimate aim of obtaining a more affordable vaccine for infant vaccination programmes, especially in countries where low cost vaccines are urgently needed. Dose sparing by means of intradermal administration has demonstrated varying results in the EPI schedule [18], [21], [22], [23]. We have shown that dose sparing by means of intramuscular administration of a low-dose aluminium hydroxide adjuvanted IPV can be effective even when using the EPI schedule. In light of the insufficient global IPV supply to meet demand, new dose-sparing strategies have the potential not only to ameliorate supply availability issues but also to reduce immunisation costs [24].
The GMT levels following IPV-Al vaccination were lower than with IPV. Since the rate of decline in antibodies was similar for IPV-Al and IPV, the GMTs were also lower prior to the booster vaccination and there was no adjustment for pre-booster titre levels, which could be considered a limitation of the trial. A strength of the trial is the choice of primary endpoint, which combines measures of the infant’s own response to the vaccination (post-vaccination titre ≥4-fold higher than the estimated maternal antibody titre) and the immunological correlate for protection (post-vaccination titre ≥8), i.e. only infants that are both vaccine responders and have a titre above the limit of protection are considered to meet the primary endpoint. This is a stricter definition than the usual practice of defining seroconversion and seroprotection as separate endpoints.
The IPV-Al vaccine was well tolerated, with a safety profile comparable to that of standard IPV with respect to adverse events, including injection site reactions, as seen in previous trials with IPV-Al in adolescents and infants [6], [7]. Previous clinical trials and post-marketing experience with IPV and aluminium hydroxide adjuvanted IPV in different combinations have not revealed any safety concerns [17], [25], [26], [27], [28], [29]. Although there were five infant deaths in the trial, two in the IPV-Al group and three in the IPV group, none were assessed as being related to the trial vaccines. The rate of deaths in the trial was not higher than expected based on the infant mortality rate in the Philippines (in 2015, the mortality rates for age 0 to 1 year was 22 deaths per 1000 infants per year) [30].
5. Conclusions
The IPV-Al vaccine demonstrated high seroconversion and seroprotection rates one month after completion of the EPI vaccination schedule comparable to those of standard IPV. Non-inferiority of seroconversion (non-inferiority margin of 10%) and seroprotection rates (non-inferiority margin of 5%) was confirmed for all poliovirus types. IPV-Al induced a robust booster response in 9-month-old infants, and with seroprotection rates comparable to those achieved with IPV one month after the booster vaccination. While the post-vaccination GMTs were higher with IPV than with IPV-Al, they were well in excess of the seroprotection threshold for both vaccines. IPV-Al was well tolerated, with a safety profile comparable to that of standard IPV. IPV-Al has the promise to be a key tool in the final phases of the polio eradication endgame and is probably the most advanced among all the research and development initiatives targeted to mitigate the cost and supply constraints related to the use of inactivated polio vaccines [31]. The novel clinical evidence reported here supports the applicability of IPV-Al vaccine to help secure a stable supply of IPV and use of the vaccine in the target populations in the near future.
Declaration of Competing Interest
The authors declare the following financial interests/personal relationships which may be considered as potential competing interests: [Birgit Thierry-Carstensen and Pernille Nyholm Tingskov are employees of Statens Serum Institut, a governmental non-profit research organization, and Charlotte Sørensen, Pernille Ingemann Nielsen and Mie Vestergaard Kusk are employees of AJ Vaccines A/S. Both Statens Serum Institut and AJ Vaccines A/S were involved in developing the vaccine at the time the trial was conducted. May Emmeline B. Montellano received research grants from Sanofi Pasteur and SK Chemicals. Ananda S. Bandyopadhyay is a full-time employee at the Bill & Melinda Gates Foundation].
Acknowledgments
Acknowledgements
The authors thank the trial participants and their parents, the investigators and trial site staff who were involved in the conduct of the trial and the involved team at the Bill & Melinda Gates Foundation. We also thank Angela Stocks, PhD (Larix A/S, Copenhagen, Denmark) for editorial and medical writing services, which were funded by AJ Vaccines, Lina Saem Stoy, MPH (Statens Serum Institut), medical writer of the clinical trial report, and Klaus Juel Olsen, PhD and Britt Bech Andersen, Exam. Pharm. Cons. (Larix Data Science and Data Management departments, respectively) for their input to the design and conduct of the trial. The laboratory technicians in the Quality control department from AJ Vaccines, QC-VAC/IPV, determined the polio antibody titres.
Disclosures
LCB, JCC, SRG, CBT and HW have no conflicts of interest to disclose. BTC and PNT are employees of Statens Serum Institut, a governmental non-profit research organization, and CS, PIN and MVK are employees of AJ Vaccines A/S. Both Statens Serum Institut and AJ Vaccines A/S were involved in developing the vaccine at the time the trial was conducted. MBM received research grants from Sanofi Pasteur and SK Chemicals. ASB is a full-time employee at the Bill & Melinda Gates Foundation.
Author contributions
LCB and CBT made initial contributions to the conception and design of the trial and LCB, JCC, SRG, MBM and CBT contributed to the finalisation of study design, acquisition and analysis of data. ASB contributed to the conception and design of the trial. BTC, PNT, PIN and MVK made substantial contributions to the conception and design of the trial, contributed to the acquisition of data and made a substantial contribution to the analysis of data. CS was responsible for the antibody determinations. HW made substantial contributions to the conception and design of the trial as well as to the analysis of data. All authors contributed to the interpretation of the data. All authors were involved in the writing, reviewing and editing of the manuscript, gave final approval and agreed to be accountable for all aspects of the work.
Funding
This work was supported by the Bill & Melinda Gates Foundation, Seattle, WA, USA (grant number OPP1095741).
Footnotes
The development of IPV-Al was initiated by Statens Serum Institut (SSI) and was transferred to AJ Vaccines upon its establishment in January 2017.
Supplementary data to this article can be found online at https://doi.org/10.1016/j.vaccine.2019.10.064.
Contributor Information
Birgit Thierry-Carstensen, Email: BTC@ssi.dk.
Pernille Nyholm Tingskov, Email: PNT@ssi.dk.
Charlotte Sørensen, Email: CHS@ajvaccines.com.
Henrik Wachmann, Email: HEW@larixcro.com.
Ananda S. Bandyopadhyay, Email: Ananda.bandyopadhyay@gatesfoundation.org.
Pernille Ingemann Nielsen, Email: PXN@ajvaccines.com.
Mie Vestergaard Kusk, Email: MHK@ajvaccines.com.
Appendix A. Supplementary material
The following are the Supplementary data to this article:
References
- 1.World Health Organization (WHO). Poliomyelitis.. 2019. Accessed 27Mar2019. https://www.who.int/en/news-room/fact-sheets/detail/poliomyelitis.
- 2.World Health Organization (WHO). Polio eradication & endgame strategic plan 2013-2018. Geneva, Switzerland. WHO Press World Health Organization; 2013. Accessed 27Mar2019. http://polioeradicationorg/who-we-are/strategy/.
- 3.Minor P. Vaccine-derived poliovirus (VDPV): Impact on poliomyelitis eradication. Vaccine. 2009;27:2649–2652. doi: 10.1016/j.vaccine.2009.02.071. [DOI] [PubMed] [Google Scholar]
- 4.Estivariz C.F., Pallansch M.A., Anand A., Wassilak S.G., Sutter R.W., Wenger J.D. Poliovirus vaccination options for achieving eradication and securing the endgame. Current Opin Virol. 2013;3:309–315. doi: 10.1016/j.coviro.2013.05.007. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Andreasen L.V., Hansen L.B., Andersen P., Agger E.M., Dietrich J. Aluminium hydroxide potentiates a protective Th1 biased immune response against polio virus that allows for dose sparing in mice and rats. Vaccine. 2015;33:1873–1879. doi: 10.1016/j.vaccine.2015.02.011. [DOI] [PubMed] [Google Scholar]
- 6.Lindgren L.M., Tingskov P.N., Justesen A.H., Nedergaard B.S., Olsen K.J., Andreasen L.V. First-in-human safety and immunogenicity investigations of three adjuvanted reduced dose inactivated poliovirus vaccines (IPV-Al SSI) compared to full dose IPV Vaccine SSI when given as a booster vaccination to adolescents with a history of IPV vaccination at 3, 5, 12months and 5years of age. Vaccine. 2017;35:596–604. doi: 10.1016/j.vaccine.2016.12.027. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Rivera L., Pedersen R.S., Pena L., Olsen K.J., Andreasen L.V., Kromann I. Immunogenicity and safety of three aluminium hydroxide adjuvanted vaccines with reduced doses of inactivated polio vaccine (IPV-Al) compared with standard IPV in young infants in the Dominican Republic: a phase 2, non-inferiority, observer-blinded, randomised, and controlled dose investigation trial. Lancet Infect Dis. 2017;17:745–753. doi: 10.1016/S1473-3099(17)30177-9. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Robertson S. Module 6: Poliomyelitis. In: The Immunological Basis for Immunization Series, WHO. 1993. Accessed 27Mar2019. http://www.who.int/ihr/polio1993en.pdf.
- 9.Brown G.C., Rabson A.S., Schieble J.H. II Serological Studies and Virus Isolations from Pharyngeal Secretions. 1955. The effect of gamma globulin on subclinical infection in familial associates of poliomyelitis cases; pp. 71–80. [PubMed] [Google Scholar]
- 10.Plotkin S.A. Correlates of protection induced by vaccination. Clin Vaccine Immunol. 2010;17:1055–1065. doi: 10.1128/CVI.00131-10. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.World Medical Association Declaration of Helsinki: ethical principles for medical research involving human subjects. JAMA. 2000;284:3043-45. [PubMed]
- 12.International Conference on Harmonisation. ICH Harmonised guideline. Integrated addendum to ICH E6(1): guideline for good clinical practice E6(R2). 2016. Accessed 27Mar2019. https://www.ich.org/fileadmin/Public_Web_Site/ICH_Products/Guidelines/Efficacy/E6/E6_R2__Step_4_2016_1109.pdf.
- 13.Melnick JL. Enteroviruses. In: AS E, editor. Viral infections of humans: Epidemiology and control. Switzerland: Springer Nature; 1984. p. 187-251.
- 14.Donken R., de Melker H.E., Rots N.Y., Berbers G., Knol M.J. Comparing vaccines: a systematic review of the use of the non-inferiority margin in vaccine trials. Vaccine. 2015;33:1426–1432. doi: 10.1016/j.vaccine.2015.01.072. [DOI] [PubMed] [Google Scholar]
- 15.El-Sayed N., El-Gamal Y., Abbassy A.A., Seoud I., Salama M., Kandeel A. Monovalent type 1 oral poliovirus vaccine in newborns. New England J Med. 2008;359:1655–1665. doi: 10.1056/NEJMoa0800390. [DOI] [PubMed] [Google Scholar]
- 16.Newcombe R.G. Interval estimation for the difference between independent proportions: comparison of eleven methods. Stat Med. 1998;17:873–890. doi: 10.1002/(sici)1097-0258(19980430)17:8<873::aid-sim779>3.0.co;2-i. [DOI] [PubMed] [Google Scholar]
- 17.Pietrzyk J.J., Wysocki J., Pejcz J., Galaj A., Majda-Stanislawska E., Kayhty H. Safety and immunogenicity of a DTaP-IPV(Vero) (serum-free) combination vaccine in comparison to DTaP-IPV(Mkc) when administered simultaneously with Haemophilus influenzae type B conjugate vaccine (PRP-T) in children at 2, 3.5, 5 and 16 months of age. Vaccine. 2008;26:5296–5303. doi: 10.1016/j.vaccine.2008.07.033. [DOI] [PubMed] [Google Scholar]
- 18.Resik S., Tejeda A., Lago P.M., Diaz M., Carmenates A., Sarmiento L. Randomized controlled clinical trial of fractional doses of inactivated poliovirus vaccine administered intradermally by needle-free device in Cuba. J Infect Dis. 2010;201:1344–1352. doi: 10.1086/651611. [DOI] [PubMed] [Google Scholar]
- 19.Edwards K.M. Maternal antibodies and infant immune responses to vaccines. Vaccine. 2015;33:6469–6472. doi: 10.1016/j.vaccine.2015.07.085. [DOI] [PubMed] [Google Scholar]
- 20.Voysey M., Kelly D.F., Fanshawe T.R., Sadarangani M., O'Brien K.L., Perera R. The influence of maternally derived antibody and infant age at vaccination on infant vaccine responses : an individual participant meta-analysis. JAMA Pediatrics. 2017;171:637–646. doi: 10.1001/jamapediatrics.2017.0638. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.Cadorna-Carlos J., Vidor E., Bonnet M.C. Randomized controlled study of fractional doses of inactivated poliovirus vaccine administered intradermally with a needle in the Philippines. Int J Infect Dis Off Publicat Int Soc Infect Dis. 2012;16:e110–e116. doi: 10.1016/j.ijid.2011.10.002. [DOI] [PubMed] [Google Scholar]
- 22.Okayasu H., Sein C., Chang Blanc D., Gonzalez A.R., Zehrung D., Jarrahian C. Intradermal administration of fractional doses of inactivated poliovirus vaccine: a dose-sparing option for polio immunization. J Infect Dis. 2017;216:S161–S167. doi: 10.1093/infdis/jix038. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.Vidor E. Poliovirus vaccine - inactivated. Vaccines. 7th ed: Elsevier; 2018. p. 841-65.
- 24.Hickling J, Jones R, Nundy N. Improving the affordability of inactivated poliovirus vaccines (IPV) for use in low- and middle-income countries: An economic analysis of strategies to reduce the cost of routine IPV immunization 2010. Report. Accessed 27Mar2019. https://path.azureedge.net/media/documents/TS_IPV_econ_analysis.pdf.
- 25.Plotkin S.A., Liese J., Madhi S.A., Ortiz E. A DTaP-IPV//PRP approximately T vaccine (Pentaxim): a review of 16 years' clinical experience. Expert Rev Vacc. 2011;10:981–1005. doi: 10.1586/erv.11.72. [DOI] [PubMed] [Google Scholar]
- 26.Haastrup E., Thierry-Carstensen B., Jensen A.M., Stellfeld M., Heilmann C. Safety and immunogenicity of a booster dose of inactivated poliovirus vaccine produced in vero-cells. Vaccine. 2004;22:958–962. doi: 10.1016/j.vaccine.2003.09.011. [DOI] [PubMed] [Google Scholar]
- 27.Thierry-Carstensen B., Dalby T., Stevner M.A., Robbins J.B., Schneerson R., Trollfors B. Experience with monocomponent acellular pertussis combination vaccines for infants, children, adolescents and adults–a review of safety, immunogenicity, efficacy and effectiveness studies and 15 years of field experience. Vaccine. 2013;31:5178–5191. doi: 10.1016/j.vaccine.2013.08.034. [DOI] [PubMed] [Google Scholar]
- 28.Thierry-Carstensen B., Jordan K., Uhlving H.H., Dalby T., Sorensen C., Jensen A.M. A randomised, double-blind, non-inferiority clinical trial on the safety and immunogenicity of a tetanus, diphtheria and monocomponent acellular pertussis (TdaP) vaccine in comparison to a tetanus and diphtheria (Td) vaccine when given as booster vaccinations to healthy adults. Vaccine. 2012;30:5464–5471. doi: 10.1016/j.vaccine.2012.06.073. [DOI] [PubMed] [Google Scholar]
- 29.Hawken J., Troy S.B. Adjuvants and inactivated polio vaccine: a systematic review. Vaccine. 2012;30:6971–6979. doi: 10.1016/j.vaccine.2012.09.059. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 30.Global, regional, national, and selected subnational levels of stillbirths, neonatal, infant, and under-5 mortality, 1980-2015: a systematic analysis for the Global Burden of Disease Study 2015. Lancet (London, England). 2016;388:1725-74. [DOI] [PMC free article] [PubMed]
- 31.Bandyopadhyay A.S., Garon J., Seib K., Orenstein W.A. Polio vaccination: past, present and future. Future Microbiol. 2015;10:791–808. doi: 10.2217/fmb.15.19. [DOI] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.