ABSTRACT
Objective
To investigate the impact of pharmaceutical care-based interventions on type 2 diabetes mellitus .
Methods
PubMed®, Cochrane and Web of Science data bases were searched for randomized controlled clinical trials. Studies evaluating pharmaceutical care-based interventions in type 2 diabetes mellitus published between 2012 and 2017 were included. Glycated hemoglobin was defined as the primary endpoint; blood pressure, triglycerides and cholesterol as secondary endpoints. The random effects model was used in meta-analysis.
Results
Fifteen trials involving 2,325 participants were included. Meta-analysis revealed considerable heterogeneity (I2>97%; p<0.001), reduction in glycated hemoglobin (-1.07%; 95%CI: -1.32; -0.83; p<0.001), glucose (-29.91mg/dL; 95%CI: -43.2; -16.6; p<0.001), triglyceride (19.8mg/dL; 95%CI: -36.6; -3.04; p=0.021), systolic blood pressure (-4.65mmHg; 95%CI: -8.9; -0.4; p=0.032) levels, and increased HDL levels (4.43mg/dL; 95%CI: 0.16; 8.70; p=0.042).
Conclusion
Pharmaceutical care-based clincal and education interventions have significant impact on type 2 diabetes mellitus . The tools Summary of Diabetes Self-Care Activities and the Morisky Medication Adherence Scale may be useful to monitor patients.
Keywords: Diabetes mellitus, type 2; Pharmaceutical services; Pharmacy service, hospital; Pharmacists
INTRODUCTION
Type 2 diabetes mellitus (T2DM) is characterized by pre- and postprandial hyperglycemia, combined with relative insulin insufficiency resulting from inadequate insulin secretion and low insulin sensitivity.1 Type 2 DM is a chronic disease with alarming growth rates in several countries, and is expected to become a serious health concern over the next decades.2 , 3 Type 2 is the most common form of diabetes and has been on the rise alongside cultural and social changes. Diabetes currently affects approximately 415 million people worldwide, with a global prevalence of 8.3% among adults; this number is expected to rise to 592 million, in 2035. Type 2 DM is thought to affect 14.3 million adult individuals in Brazil. Aside from individual costs associated with medical treatment of diabetes, the disease places a major economic burden on countries and respective health systems due to diabetes-related complications.4
Ongoing education is useful for patients,1 since diabetes management is complex and involves glucose monitoring, adherence to treatment, physical activity and dietary changes.5 Glycated hemoglobin (HbA1c) reflects blood glucose levels over the last 120 days and is the gold standard biomarker for diabetes control assessment and prediction of severe complications.6 According to current guidelines, blood glucose levels should be close to normal in order to prevent or delay complications.1 However, lack of adherence to treatment is common and may impact glycemic control, with increased mortality rates.7 Inadequate glycemic control is associated with increased risk of cardiovascular disease, neuropathy, retinopathy, nephropathy and hospitalization.6 , 8 Adherence to treatment is vital to fully benefit from therapeutic regimens. Approximately 20% to 50% of patients with chronic diseases report less than optimal adherence to drug therapy, which hinders effectiveness of treatment.9 , 10 Also, high glycemic indices have been reported in patients with poor adherence to treatment.11 , 12
Several factors have been associated with non-adherence to treatment, including social and economic aspects, pharmacotherapy complexity and patients’ beliefs regarding drugs.13 As pharmacotherapy specialists, clinical pharmacists contribute to patient care by providing individual guidance (alone or with other health professionals), assisting in planning and monitoring of therapeutic strategies aimed to improve the pathological conditions, treatment and adherence by a process entitled “pharmaceutical care”.14 , 15 This may be defined as “responsible provision of pharmacotherapy to achieve outcomes associated with improved quality of life for patients.”16
Identification of drug-related problems is another a vital aspect of pharmaceutical care aimed to prevent events that may impact on treatment outcomes, such as pharmacotherapy effectiveness, adverse reactions and polypharmacy, which are common among diabetic patients.17 - 21 Pharmaceutical care also provides drug-related information to help patients understand pharmacotherapy risks and benefits, so as to improve adherence to treatment and clinical outcomes.13
However, decision making in diabetic patient care has not yet been fully understood.22 There is a need to determine which pharmacist interventions are currently applicable in clinical practice. Also, only one meta-analysis of studies investigating pharmaceutical care in T2DM has been published to date.23 This study examined the hypothesis that pharmaceutical care would make significant contributions to T2DM control, particularly regarding HbA1c reduction in affected patients.
OBJECTIVE
To investigate the impact of pharmacist interventions on glycemic control in type 2 diabetes mellitus patients and other endpoints, such as blood pressure, triglycerides and cholesterol levels.
METHODS
Search strategy
A systematic review of randomized controlled clinical trials investigating the impact of pharmacist interventions in T2DM management was used as a reference for study selection and identification of new studies.24 The following databases were searched: PubMed®, Cochrane Central Register of Controlled Trials and Web of Science. Search strategies are detailed in appendix A.
Date of publication
Studies published between January 2012 and December 2014 were selected. Results of new searches were limited to articles published between January 2015 and October 2017.
Study selection
Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) recommendations were used for systematic review and meta-analysis.25 Studies with the following characteristics were selected: population comprising participants aged 18 years or older, with a diagnosis of T2DM; health team comprising one pharmacist capable of providing pharmaceutical care via clinical and/or educational interventions for management of participants with T2DM; comparing standard medical, nursing, and community pharmacy care, and defining HbA1c as the primary endpoint, and systolic (SBP) and diastolic blood pressure (DBP), triglycerides (TG) and cholesterol (low – LDL- and high density – HDL - lipoprotein) levels and adherence to treatment as secondary endpoints; conducted in outpatient clinics, hospitals and community pharmacies; prospective randomized controlled clinical trial design; published in English.
Studies conducted exclusively with participants suffering from type 1 diabetes mellitus , diabetes insipidus or gestational diabetes, involving interventions based exclusively on educational programs or leaflets, defining fasting blood glucose levels as primary endpoint, retrospective studies and non-randomized controlled clinical trials were excluded.
Risk of bias assessment
The Cochrane collaboration tool was used to assess selection, performance, detection, attrition, reporting and other biases. Selected studies were classified as having low, high or unclear risk of bias.
Data extraction
Selected studies were individually evaluated by a single author. Data were extracted in standard format using Microsoft Excel, and consisted of study characteristics, participant characteristics, pharmacist interventions carried out and outcome measures.
Statistical analysis
Statistical analyses were conducted using software (STATA 13; Statacorp, Texas, USA). The random effects model was selected to account for heterogeneity of studies included in the meta-analysis; I2 was calculated to assess the magnitude of heterogeneity between studies (I2 >50% and I2 >75% indicate substantial and considerable heterogeneity, respectively). The χ2 test was used to assess significance of heterogeneity (p<0.10).
Outcome measures
Outcome measures were defined as changes between the Intervention and the Control Group. Primary (HbA1c) and secondary (SBP, DBP, fasting glucose, TG, LDL and HDL cholesterol levels) endpoint measures were expressed as mean differences and 95% confidence intervals (95%CI). The findings were expressed using conventional measures: percentage for HbA1c; mmHg for SBP and DBP; and mg/dL for TG, LDL and HDL. The level of significance was set at 5%. Whenever results extracted from selected studies were expressed as mmol/L, these were converted to mg/dL.
RESULTS
Study selection
The systematic used as reference for this study yielded 36 clinical trials.24 Of these, 25 were excluded due to non-conformity with selected time, and 11 were rated eligible. Four out of 11 eligible studies failed to define HbA1c as the primary endpoint. The final sample comprised seven studies.21 , 26 - 31
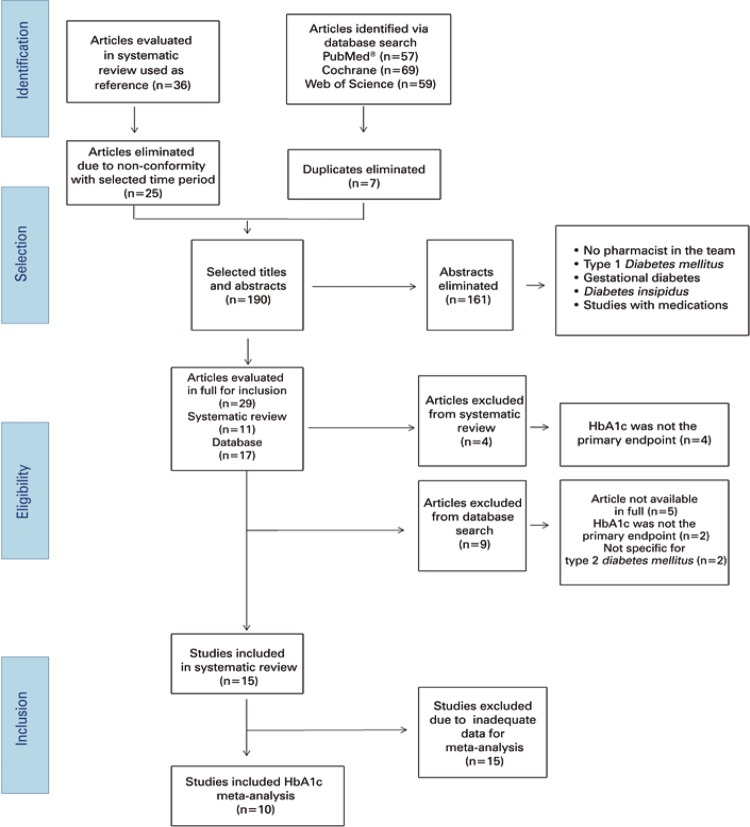
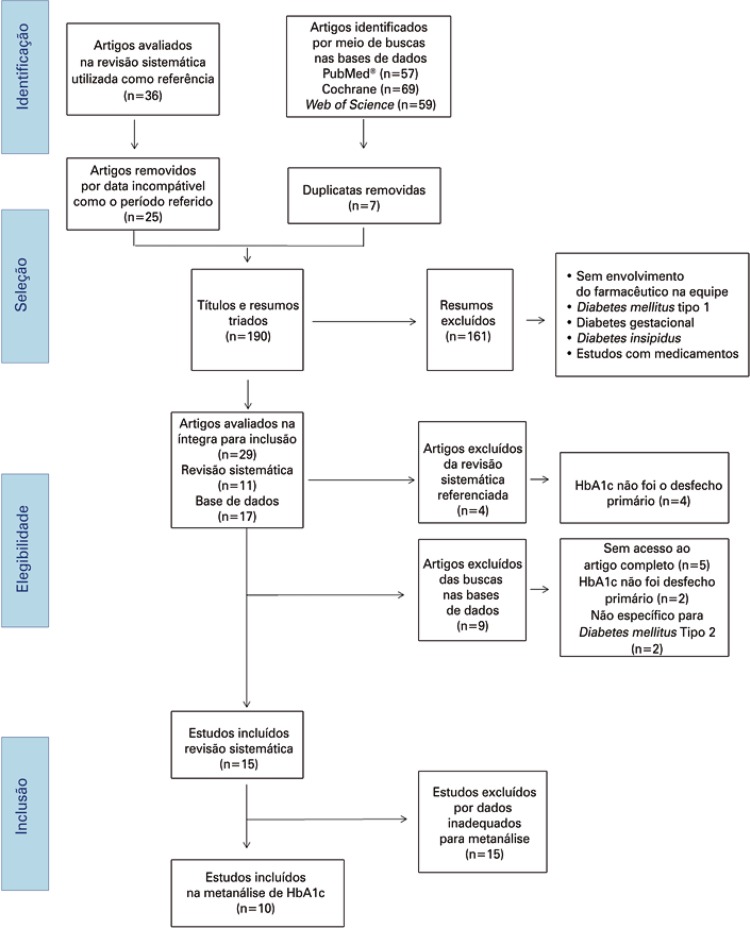
The database search strategy adopted yielded 185 results. Seven duplicates were eliminated in the screening process. Following analysis of title and abstract of 161 articles, 17 were selected. Of these, five were excluded since they were not available in full text; two for not defining HbA1c as the primary endpoint and two for not being specific for T2DM. The remaining eight articles were included in the analysis. Overall, 15 articles were included in the systematic review and 10 in the meta-analysis ( Figure 1 ).
Figure 1. Study selection flowchart.
HbA1c: Glycated hemoglobin.
Study characteristics
Studies included in the systematic review were conducted in outpatient clinics and community pharmacies of different countries, as follows: three in Brazil, three in China, one in Malaysia, one in the United Kingdom, one in Singapore, one in Taiwan, one in Iran, one in Iraq, two in Jordan, and one in the Turkish Republic of Northern Cyprus. Experimental design was randomized controlled in all cases and one study was multicenter. Follow-up ranged from 3 to 12 months (mean 7.9 months). Clinical trials included participants with HbA1c ranging from 6.5% to 9%. Detailed description of studies included is given in table 1 .
Table 1. Characteristics of studies included.
| Reference | Settings | Population | Characterization of the sample | Follow-up | Interval of intervention | Pharmacist interventions | Control | Clinical endpoint measures |
|---|---|---|---|---|---|---|---|---|
| Mahwi et al.(21) | Diabetes center in Iraq | Type 2 diabetics aged 30 to 80 years | n=65/65* Lost to follow-up: 3/4* Age: 52.0±7, 86/53.4±10.81*† Sex: 71.0%/67.2%* female | 3 months | Monthly | Adherence, drug-related problems | Standard care by medical team | HbA1c, fasting glucose and drug-related problems, adherence |
| Jarab et al.(26) | Diabetes outpatient service of a teaching hospital in Jordan | Type 2 diabetics aged ≥18 years, HbA1c ≥7.5% | n=85/86* Lost to follow-up: 8/7* Age: 63.4±10.1/65.3±9.2*† Sex: 42.4%/44.2%* female | 6 months | 8 weeks (follow-up telephone calls) | Patient education, drug-related problems, follow-up telephone calls, self-care | Standard care by medical and nursing teams | HbA1c, adherence, blood pressure, TC, HDL, LDL, TG, BMI, self-care (SDSCA) |
| Wishah et al.(27) | Diabetes outpatient service of a teaching hospital in Jordan | Type 2 diabetics aged ≥18 years, HbA1c ≥6.5%, use of oral hypoglycemic agent | n=52/54* Lost to follow-up: 2/3* Age: 52.9±9.6/53.2±11.2*† Sex: 61.5%/51.9%* female | 6 months | Not informed | Patient education, drug- related problems, self-care | Standard care by medical and nursing teams | HbA1c, blood pressure, TC, HDL, LDL, TG, BMI, fasting glucose, self-care (SDSCA) |
| Chung et al.(28) | Teaching hospital in Malaysia | Type 2 diabetics aged ≥21 and <75 years, HbA1c ≥8%, use of oral hypoglycemic agent | n=120/121* Lost to follow-up: NR Age: 59.7±9.5/58.5±8.3*† Sex: 58.3%/53.7%* female | 12 months | 3 to 4 months with monthly follow-up telephone calls | Medication review, diabetes education | Usual pharmacy services | HbA1c, fasting glucose, adherence |
| Ali et al.(29) | Community pharmacies in the United Kingdom | Type 2 diabetics aged ≥18 years, HbA1c ≥7%, use of oral hypoglycemic agent | n=25/23* Lost to follow-up: 2/0* Age: 66.4±12.7/66.8±10.2*† Sex: 43.5%/56.5%* male | 12 months | Monthly in the first 2 months, then every 3 months | Medication review, patient education, referral to other healthcare professionals | Standard care by medical and nursing teams and community pharmacies | HbA1c, fasting glucose, blood pressure, LDL, HDL, TG, BMI, DQoL, HRQoL, adherence, diabetes knowledge test (DKT), SIMS |
| Mourão et al.(30) | Primary Care Units in Brazil | Type 2 diabetics aged ≥18 years, HbA1c ≥7%, post-prandial glucose ≥180mg/dL, use of oral hypoglycemic agent | n=65/64* Lost to follow-up: 12/9* Age: 60.0±10.2/61.3±9.9*† Sex: 68.0%/66.0%* female | 12 months | Monthly | Drug-related problems, diabetes education | Standard care | HbA1c, blood pressure, LDL, HDL, TG, BMI, drug-related problems |
| Chan et al.(31) | Diabetes clinic of a public hospital in Hong Kong | Type 2 diabetics aged ≥18 years, HbA1c ≥8%, polypharmacy, use of oral hypoglycemic agent | n=51/54* Lost to follow-up: 0/0* Age: 63.2±9,5/61.74±11.2*† Gender: 58.8%/51.9%* male | 9 months | Not reported | Patient education, drug related problems | Standard care by medical team | HbA1c, blood pressure, LDL, HDL, TG, BMI, adherence, cardiovascular risk, cost-effectiveness |
| Korcegez et al.(32) | Diabetes outpatient service in a public hospital in Turkish Republic of Northern Cyprus | Type 2 diabetics diagnosed at least 6 months prior to the study, HbA1c >7% and use of oral hypoglycemic agent | n=75/77* Lost to follow-up: 4/3* Age: 61.80±10.38/62.22±9.54*† Sex: 77.3%/74.0%* female | 12 months | 2 months | Patient education, drug-related problems, self-care | Standard care by medical and nursing teams | HbA1c, blood pressure, TC, HDL, LDL, TG, BMI, fasting glucose, abdominal circumference, self-care (SDSCA) |
| Siaw et al.(33) | Four outpatient services in Singapore | Type 2 diabetics aged ≥21 years, HbA1c ≥7%, polypharmacy and multiple comorbidities | n=214/197* Lost to follow-up: 3/1* Age: 59.2±8.2/60.1±8.1*† Sex: 52.3%/60.9%* male | 6 months | 4 to 6 weeks | Patient education, drug-related problems, insulin dose adjustment based on symptoms (SIGN algorithm), follow-up telephone calls | Standard care by medical team | HbA1c, systolic blood pressure, LDL, TG, quality of life (PAID), satisfaction with treatment (DTSQ), use of health services, economic analysis |
| Cani et al.(34) | Diabetes outpatient service at a teaching hospital in São Paulo | Type 2 diabetics aged ≥45 years, HbA1c ≥ 8.0%, use of insulin | n=37/41* Lost to follow-up: 3/5* Age: 61.91±9.58/61.58±8.14*† Sex: 34.0%/36%* male | 6 months | Not informed | Patient education, drug-related problems, insulin administration technique | Standard care | HbA1c, knowledge about diabetes, knowledge about drugs, adherence, insulin administration technique, glucose monitoring, quality of life (QoL) |
| Aguiar et al.(35) | University secondary care hospital in São Paulo | Type 2 diabetics diagnosed at least 6 months prior to the study, HbA1c ≥7%, aged between 40 and 79 years, use of oral antidiabetic agent | n=36/37* Lost to follow-up: 0/0* Age: 61.1.6±7.9/62.4±8.2*† Sex: 69.4%/64,9%* female | 12 months | 2 to 6 months (depending on glucose levels) and follow-up telephone calls between visits | Patient education, drug- related problems, insulin administration technique, follow-up telephone calls | Standard care by medical and nursing teams | HbA1c, blood pressure, LDL, adherence |
| Chen et al.(36) | Nantou Hospital, in Taiwan | Type 2 diabetics aged ≥65 years, with HbA1c ≥9% | n=50/50* Lost to follow-up: NR Age: 72.16±6.6/72.76±5.9*† Sex: 50%/50%* male and female | 6 months | Monthly follow-up telephone calls | Patient education, drug-related problems, insulin administration technique, referral to other professionals, follow-up telephone calls | Standard care | HbA1c, fasting glucose, percentage of hospitalizations, economic analysis |
| Jahangard-Rafsanjani et al.(37) | Community pharmacy in Teheran, Iran | Type 2 diabetics with HbA1c >7% and use of oral hypoglycemic agent | n=51/50* Lost to follow-up: 6/10* Age: 57.6±8.3/55.9±8.7*† Sex: 25%/26% female | 5 months | Monthly | Patient education, drug- related problems, follow-up telephone calls, self-care | Standard care by medical team | HbA1c, BMI, blood pressure, adherence, self-care (SDSCA) |
| Xin et al.(38) | Tongde Hospital, Hangzhou province, China | Type 2 diabetics aged ≥18 years, no use of insulin over the last 18 months | n=120/120* Lost to follow-up: 6/7* Age: 58.8±14.4/59.2±14.2*† Sex: 51.8%/50.4%* male | 12 months | Not informed | Patient education, insulin administration technique, follow-up telephone calls | Standard care by medical team | HbA1c, adherence |
| Shao et al.(39) | University hospital in Nanjing province, China | Type 2 diabetics aged ≥18 years, HbA1c ≥7%, diagnosed 3 months before or earlier, and use of oral hypoglycemic agent | n=20/120* Lost to follow-up: 20/21* Age: 58.86±10.59/59.20±10.34*† Sex: 51%/475%* male | 6 months | 2 months (in-person) and monthly follow-up telephone calls | Patient education, follow-up telephone calls | Standard care by medical team | HbA1c, adherence, blood pressure, TC, HDL, LDL, TG, BMI, fasting glucose |
* relation between intervention and Control Group; † age in years (mean±standard deviation).
HbA1c: glycated hemoglobin; TC: total cholesterol; HDL: high density lipoprotein; LDL: low density lipoprotein; TG: triglycerides; BMI: body mass index; SDSCA: Summary of Diabetes Self-Care Activities Questionnaire; NR: not reported; DQoL: Diabetes Quality of Life Brief Clinical Inventory; HRQoL: Health-Related Quality of Life; DKT: Diabetes Knowledge Test; SIMS: Satisfaction with Information Received About Medicines; PAID: Problem Areas in Diabetes Questionnaire; DTSQ: Diabetes Treatment Satisfaction Questionnaire; QoL: Quality of Life.
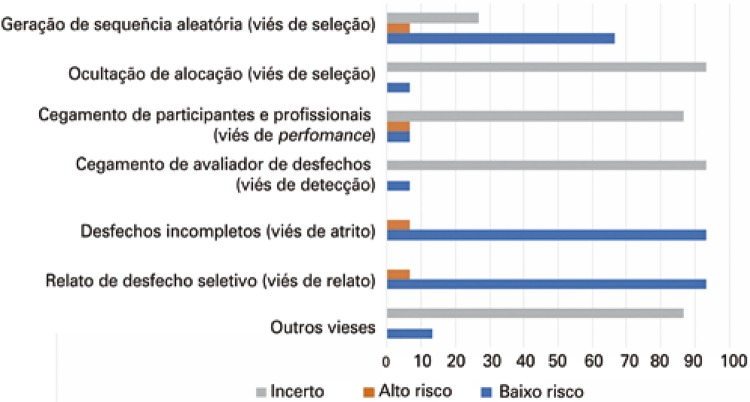
Risk of bias
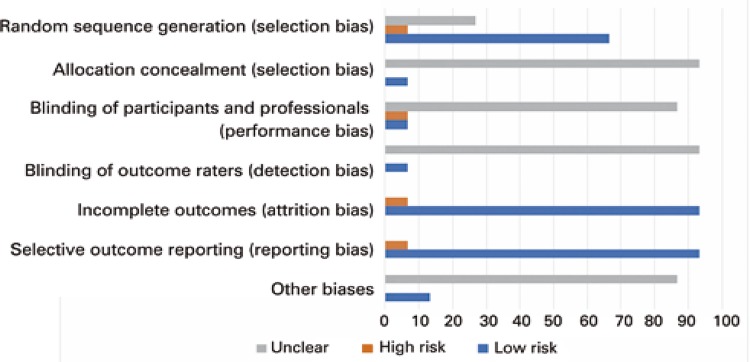
As regards selection bias, random sequence generation was thought to be adequate in most studies (10/15; 66.7%). Randomization strategy was not reported in four studies (4/15; 26.7%). High risk of bias was observed in one study (1/15; 6.7%) in which participants were randomized according to medical record number.32 Fourteen studies (14/15; 93.4%) failed to describe methods used to conceal random allocation sequences, and only one study reported auditing to ensure allocation concealment (multicenter study).33
As regards performance bias, no studies reported blinding to pharmacist’s activities, and exchange of information between participants may have occurred in 14 studies conducted in a single setting, except the multicenter study by Siaw et al . 33 That trial was thought to involve high risk of bias regarding blinding of participants and professionals, since participants in the Control Group were able to consult pharmacists, if required.34
As regards detection bias, only one study reported blinding of raters, who were therefore unaware of groups being evaluated.35 The remaining studies were thought to have unclear risk of bias, given measures employed to assess clinical outcomes were not described.
Attrition and reporting biases were limited to one study that retained high risk of bias due to lack of description of one of the secondary endpoints.27
As for other biases, only two studies were thought to be free from other sources of bias (2/15; 13.4%). Thirteen studies included in this systematic review and meta-analysis (13/15; 86.7%) were thought to have unclear risk of bias, given limitations presented by authors were deemed insufficient to estimate whether significant risk of bias might impact participant outcomes ( Figure 2 and Appendix B).
Figure 2. Risk of bias.
Population characteristics
Studies included in this systematic review involved 2,325 participants, with samples ranging from 36 to 214 participants. The proportion of male participants ranged from 22% to 75%. Mean age ranged from 52 to 72 years. Mean baseline HbA1c levels corresponded to 9.06% and 8,79% in the Intervention and Control Group, respectively. Aside from T2DM, most studies included emphasized multiple comorbidities related to secondary clinical endpoints, such as dyslipidemia, hypertension and obesity ( Table 1 ).
Pharmacist interventions
Interventions were conducted during in-person pharmaceutical visits or via follow-up telephone calls (7/15; 46.7%). However, details of interventions conducted via follow-up telephone calls were not provided in all studies. All clinical trials emphasized patient education activities (15/15; 100%) and collaboration with medical teams (14/15; 93.4%). However, when search terms “drug-related problems” (12/15; 80.0%) or “medication review” (2/15; 26.7%) were used, instruments applied failed to be described. Two studies21 , 31 defined frequency of drug-related problems as a clinical outcome of participants, and only two30 , 35 described the use of Pharmacotherapy WorkUp40 for the same purpose.
“Drug related problems” and “medication review ” tools were used to identify and solve drug-related problems during patient follow-up. These tools comprise key components of pharmacist interventions, such as: Feedback – recommendations regarding pharmacological treatment forwarded to medical teams in order to solve problems identified and optimize pharmacotherapy (adding, replacing or discontinuing medications, as well as dose adjustments). Follow-up telephone calls – pharmaceutical advice provided over the phone and assessment of adverse events. Patient education – educational interventions related to diabetes and its treatment for improved patient adherence, such as providing information about medications, adverse reactions, administration route and storage (particularly insulin), training aimed at recognition and correction of hypoglycemia, lifestyle changes (smoking cessation, alcoholism, proper diet and foot inspection), self-care promotion (glucose monitoring). All patients received verbal instructions; educational materials, such as leaflets, were also provided in some cases.
In one study, the clinical pharmacist was allowed to adjust insulin doses in naïve patients based on hypoglycemia signs/symptoms. An algorithm was validated for that purpose.33
In two studies29 , 36 (2/15, 26.7%) participants were referred to other professionals, such as dieticians and nurses.
The Control Group consisted of standard care provided in outpatient settings and community pharmacies, excluding interventions provided by clinical pharmacists, or diabetes education provided by other healthcare professionals, such as physicians and nurses ( Table 1 ).
Adherence
Adherence to treatment was a clinical endpoint in ten studies. The Morisky Medication Adherence Scale (MMAS-8 and MMAS-4) was used to assess participant adherence at baseline and at the end of the follow-up period. Significant improvement in adherence in the Intervention Group as compared to the Control Group was reported in all studies (p<0.05).
Meta-analysis
Heterogeneity analysis
Ten studies were included in the meta-analysis,21 , 27 - 29 , 32 , 34 , 36 - 39 all of them with high heterogeneity for all endpoints (I2 97% to 99%; p<0.001). The efficacy of pharmaceutical care to promote reduction of SBP, HbA1c, fasting glucose and TG levels and increase of HDL levels was demonstrated in all studies, in spite of significant heterogeneity. However, the outcomes LDL levels and DBP had no statistically significant differences.
Glycated hemoglobin levels
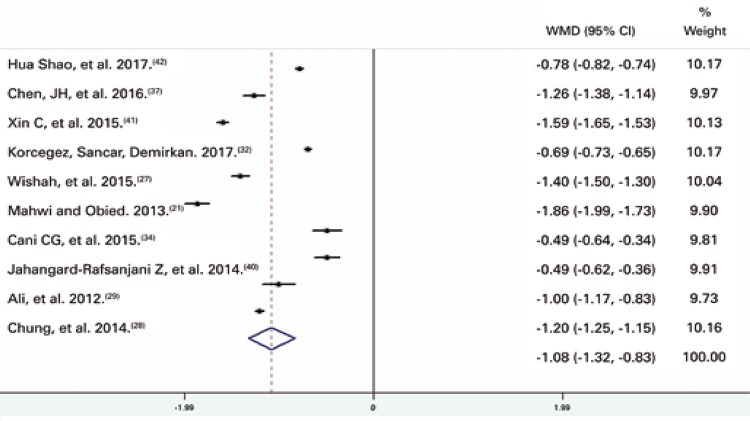
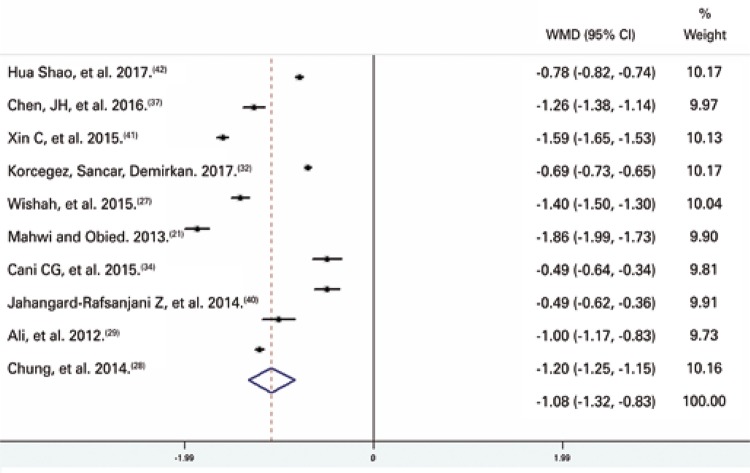
With respect to HbA1c, ten studies21 , 27 - 29 , 32 , 34 , 36 - 39 including 715 participants with mean baseline levels of 9.0% were selected. Meta-analysis revealed a mean difference of – 1.07% (95%CI: -1.32; -0.83; p<0.001). The impact of pharmacist interventions on HbA1c reduction in the Control Group is shown in the forest plot ( Figure 3 ).
Figure 3. Forest plot.
Fasting blood glucose levels
Six studies21 , 27 - 29 , 32 , 39 involving 457 participants revealed mean fasting blood glucose level reduction of – 29.91mg/dL (95%CI: -43.2; -16.6; p<0.001).
Triglycerides
Four studies27 , 29 , 32 , 39 involving 272 participants were included, with mean TG level reduction of – 19.8mg/dL (95%CI: -36.6; -3.04; p=0.021).
LDL and HDL
Variations in LDL and HDL levels were non-significant, with mean HDL level increase of 4.43mg/dL (95%CI: 0.16; 8.70; p=0.042), and mean LDL level reduction of – 5.263mg/dL (95%CI: -10.7; 0.18; p=0.058).27 , 29 , 32 , 39
Systolic and diastolic blood pressure
Only SBP differed significantly (mean reduction, - 4.65mmHg; 95%CI: -8.9; -0.4; p=0.032) across all four studies included. Mean reduction in DBP (–1.81mmHg; 95%CI: -3.7; 0.1; p=0.065) was non-significant.29 , 32 , 37 , 39
Frequency of interventions
Six studies involving frequent interventions (monthly or every two months) were included, with mean baseline HbA1c of 8.9%.21 , 29 , 32 , 36 , 37 , 39 Mean reduction of – 1.01% (p<0.001) was observed (95%CI: -1.2; -0.7). Mean reduction of – 1.17% (p<0.001; 95%CI: - 1.4; -0.8) was also observed in four studies that failed to report intervals between interventions or reporting intervention interval of three months.27 , 28 , 34 , 38 However, mean baseline HbA1c in this group was 9.48%.
DISCUSSION
According to meta-analysis results, all pharmacist interventions promoted significant reduction of SBP and HbA1c, fasting blood glucose, TG and HDL levels, with no impact on LDL levels or DBP. Santschi et al ., 41 conducted a meta-analysis of 39 randomized clinical trials with 14,224 participants with high cardiovascular risk (hypertension, dyslipidemia, diabetes, smoking and obesity) and observed SBP (− 7.6mmHg; 95%CI: -9.0; -6.3; I2 = 67%) and DBP (− 3.9mmHg; 95%CI: -5.1; 2.8; I2 = 83%) reduction in response to pharmacist interventions, such as patient education, feedback to medical teams, and identification of drug-related problems. Nonetheless, subgroup analysis to investigate differences between diabetic and non-diabetic participants in that study Santschi et al.,41 failed to reveal significant differences in SBP (– 6.4mmHg; 95%CI: -7.8; -5.1; p=0.37) and DBP (– 4.5mmHg; 95%CI: -6.3; -2.8; p=0.51). Results of this meta-analysis are in keeping with findings reported by Santschi et al.,41 with significant SBP reduction and no impact on DBP.
Deters et al.,42 included six studies in a meta-analysis of 640 participants in randomized clinical trials investigating the impact of pharmaceutical care on type 1 and type 2 diabetes. Mean HbA1c difference of – 0.66% (95%CI: - 0.86; -0.45) and non-significant heterogeneity (I2 =7.9%; p=0.3659) were reported. Deters et al.,42 also considered the meta-analytic effect of pharmacist interventions and evaluated mean HbA1c differences associated with drug-related problems/medication review (-0.79%) and feedback to medical team (-0.81%), and determined the impact of each intervention on the educational component: diabetes-related complications (-0.60%); knowledge about medications (-0.74%); diet, physical exercise and smoking cessation (-0.66%); self-monitoring of blood glucose analysis (-0.74%); definition of individual targets (-0.81%); adherence (-0.60%) and knowledge about diabetes (-0.54%). This study did not include meta-analysis per intervention, since not all clinical trials selected provided detailed description of components, such as number of patients submitted to a given intervention (educational interventions in particular). Only three of the studies included27 , 32 , 37 used the Summary of Diabetes Self-Care Activities (SDSCA) to measure the impact of pharmaceutical care in patient self-care components, such as diet, physical exercise practice, self-monitoring of blood glucose, foot care and smoking cessation.
A meta-analysis of 22 randomized clinical trials involving 1,382 participants with T2DM conducted by Aguiar et al ., 23 revealed a mean HbA1c reduction of – 0.85% (95%CI: -1.06; -0.65; p<0.0001) and significant (p<0.0001) and substantial (I2 =67.3%) heterogeneity. Subgroup analyses were conducted to investigate potential causes of heterogeneity, as follows: country where the study was conducted, type of contact with patients, studies using medication review and frequency of interventions, among others. Low (0% to 40%), non-significant (p>0.10) heterogeneity was observed in studies with the following characteristics: clinical trials conducted in the United States; participants with baseline HbA1c levels ≤9%; community pharmacy settings; lack of educational material provision by pharmacists; pharmacist authorized to alter drug prescriptions; more than one intervention per month and proper randomization. Aguiar et al ., 23 also observed higher mean HbA1c differences in patients with elevated baseline HbA1c levels. Findings of this study revealed greater HbA1c level reduction in trials with longer intervals between pharmacist interventions. However, those studies reported mean baseline HbA1c levels of 9.48%. Therefore, it can be argued that longer intervals between interventions are not associated with increased reduction of HbA1c levels. Likewise Aguiar et al ., 23 this study showed that patients with elevated baseline HbA1c levels may benefit more from pharmaceutical care, given the mean baseline HbA1c level of participants included in this meta-analysis was 9.0%.
This study reproduced the analysis conducted by Aguiar et al, . 23 to investigate potential causes of high heterogeneity between studies. Given the small number of studies (less than ten), meta-regression was not performed; rather, subgroup analysis was repeated using the random effect model according to trial characteristics (participants with baseline HbA1c levels <9%;27 , 32 , 34 , 36 , 37 interventions such as drug-related problems27 , 32 , 34 , 37 , 40 and medication review ; 28 , 29 frequent interventions -monthly or every 2 months;21 , 26 , 29 , 30 , 32 , 35 , 40 , 42 outpatient settings21 , 26 , 27 , 30 - 35 and community pharmacy;29 , 37 ) per sex ( i.e ., studies with larger proportion of males29 , 34 , 41 , 42 versus studies with larger proportion of females).21 , 27 , 28 , 32 , 37 , 39 All analyses revealed high and significant heterogeneity (I2 >98%; p<0.001). Analysis with study exclusion was also conducted. One trial included only elderly patients (≥65 years).38 This was thought to be potentially related to the high, significant heterogeneity observed; hence, sensitivity analysis excluding the aforementioned study was conducted, with similar results: I2 = 99.2% (p<0.001). Results were also similar following exclusion of studies with short follow-up21 , 37 and inadequate randomization.32 It was not possible to determine whether lack of specific tools such as Pharmacotherapy WorkUp for drug-related problems might have contributed to heterogeneity, because only two studies reported the use of this tool for that specific purpose.30 , 35 Even if all 15 studies selected for systematic review had been included in this meta-analysis, results would still probably be similar. Significant heterogeneity may have reflected differences in inclusion criteria between trials. HbA1c levels for inclusion of studies in this meta-analysis ranged from 6.5% to 9%, with mean variations in baseline HbA1c levels of 9.0% and 8.7%, in the Intervention and Control Groups, respectively. Insulin use34 , 36 , 38 is yet another potential cause of heterogeneity, as well as age and sex proportions, short follow-up21 , 37 and small number of participants.29 , 34
Given the multiculturalism of studies included in this systematic review and meta-analysis, cultural and ethnic differences may also have impacted on clinical outcomes, as may differences between health systems and educational and socioeconomic characteristics of participants. This analysis included studies conducted in different countries and regions around the world (South America, Europe, Eastern Mediterranean, Middle East and Asia), such as those of Chung et al ., 28 and Siaw et al . ,33 conducted in Malaysia and Singapore, respectively, enrolling participants of three different ethnic groups (Chinese, Malayans and Indians). Also worthy of notice are potential hurdles regarding intervention acceptance, which may vary in countries where pharmaceutical care is not well accepted. Aguiar et al ., 35 were the only authors to describe frequency of interventions and acceptance rates (96.9%) by medical teams.
Methodological limitations of studies included in this meta-analysis must also be accounted for. The significance of pharmaceutical care in multiprofessional settings must be emphasized; however, several studies referred in this analysis described Control Group interventions as “standard care”, with no further specifications. The risk of bias in studies selected for this systematic review and meta-analysis was rated “unclear” regarding almost all aspects considered, as few authors reported allocation concealment methods and blinding of outcome raters. Settings where studies were conducted may have impacted results in some cases. Given the small size of the country in which one of the studies was conducted (Turkish Republic of Northern Cyprus), cross contamination between groups may have occurred.32 Therefore, the Control Group may have obtained data from the Intervention Group, even in studies conducted in a single outpatient setting (Hawthorne experience). In one of the studies, participants in the Control Group had access to baseline laboratory tests and may have mitigated the effects of pharmacist interventions by seeking greater medical attention.30 Also, selected studies did not involve blinding of clinical pharmacists’ activities, with potential increase in care provided by other healthcare professionals in the Control Group. For example, in one trial the clinical pharmacist was allowed to counsel patients in the Control Group, if required.34 Clear description of pharmaceutical care provided to participants in the Intervention Group was seldom given and few studies included SDSCA in the educational key component. Hence, statistical analysis per specific key component could not be performed, supporting results reported by Deters et al.,42 Overall, studies included in this meta-analysis reported that pharmacists involved in clinical trials were pharmacotherapy specialists and had been trained in diabetes education. However, data regarding training duration (hours) and healthcare professionals in charge were not always provided. Meta-analysis investigating participant adherence could not be conducted due to the wide variability of methods used to measure outcomes and the lack of standardized measures between studies. Standardization of instruments aimed to assess adherence and enable comparisons of findings across studies is therefore required. Frequency of intervention was not always clearly reported in studies in this analysis; conclusions regarding the ideal frequency of intervention could therefore not be drawn. Studies based on interventions performed every three months (or failing to report intervention intervals) reported greater reduction in HbA1c levels. However, mean baseline levels in this group of studies was greater than 9%, in contrast with less than 9% in studies involving monthly interventions. Hence, greater reduction in HbA1c levels may not be directly related to longer interval between interventions. As suggested by Aguiar et al . ,23 this analysis supports the hypothesis that patients with higher baseline HbA1c levels in may benefit more from pharmaceutical care.
According to the American Diabetes Association (ADA) and Sociedade Brasileira de Diabetes (SBD), treatment of diabetes mellitus must be determined by an active multiprofessional team, capable of providing continuing education and good quality of care.1 , 43 As regards the pharmaceutical profession, SBD refers the Collegiate Resolution (RDC 44/2009) of the National Health Surveillance Agency (ANVISA - Agência Nacional de Vigilância Sanitária ) for delivery of pharmaceutical services – including pharmaceutical care and capillary glucose test,43 while the ADA guidelines recommend assurance of rational use of insulin, and careful dosing supervision by pharmacists.1 Nevertheless, these guidelines fail to describe other components required for multiprofessional patient care.1 , 44 Results of this meta-analysis suggest key components such as drug-related problems/medication review (including feedback to medical teams) , patient education and follow-up telephone calls are associated with satisfactory clinical outcomes regarding reduction of HbA1c levels. Tools aimed to assess self-care ( e.g . SDSCA)45 and adherence ( e.g . MMAS-8),46 or to identify drug-related problems may be useful in patient follow-up.
This study has some limitations. Not all clinical trials selected for systematic review were included in the meta-analysis due to differences in outcome measure reporting (mean, standard deviation, median, IQR and 95%CI). Only studies expressing measures as mean and standard deviation were included. Also, the objective of this study was to identify recent evidence of pharmacist interventions in T2DM and evaluate related impacts. Studies published between 2012 and 2017 were therefore selected. Extension of this time frame would have allowed the inclusion of a greater number of randomized clinical trials. However, studies published before 2012 would likely not reflect current pharmaceutical practices. Data extraction, review and analysis in this study were performed by a single researcher. Still integrity of data presented in this systematic review with meta-analysis can be guaranteed.
CONCLUSION
This meta-analysis revealed high, significant heterogeneity between studies. Still, the findings suggest pharmaceutical care-related interventions have significant impacts on reduction of systolic blood pressure, glycated hemoglobin, fasting glucose and triglyceride levels, and on increase of HDL levels. The findings also suggest such interventions do not impact on diastolic blood pressure or LDL levels, and that patients with elevated baseline glycated hemoglobin levels may benefit more from pharmaceutical care. However, more randomized clinical trials with better methodological design are warranted for clearer reporting of pharmaceutical intervention outcomes.
Appendix.
Appendix A. . Search strategy.
| PubMed® |
|---|
| 1. Diabetes mellitus , type 2 [mh] (107.405) |
| 2. Type 2 diabetes (144.283) |
| 3. T2DM (13.054) |
| 4. Non insulin dependent diabetes mellitus (130.159) |
| 5. NIDDM (120.203) |
| 6. 1 OR 2 OR 3 OR 4 OR 5 (156.111) |
| 7. Pharmaceutical services [mh] (60.102) |
| 8. Pharmaceutical care (86.683) |
| 9. Clinical Pharmacy (71859) |
| 10. Community pharmacy (22.968) |
| 11. Pharmacist* (30.355) |
| 12. 7 OR 8 OR 9 OR 10 OR 11 (170.150) |
| 13. Randomized controlled trial [pt] (441.905) |
| 14. Random* AND Control* (797.089) |
| 15. 13 OR 14 (797.180) |
| 16. 6 AND 12 AND 15 (479) |
| 17. Cochrane Central Register of Controlled Trials filter according to date of publication (57) |
| Web of Science |
| 1. ts= Type 2 diabetes (153.853) |
| 2. ts = T2DM (13.045) |
| 3. ts = Non insulin dependent diabetes mellitus (10.421) |
| 4. ts = NIDDM (12.313) |
| 5. 1 OR 2 OR 3 OR 4 (168.261) |
| 6. ts = Pharmaceutical services (4.887) |
| 7. ts = Pharmaceutical care (13.954) |
| 8. ts = Clinical pharmacy (8.159) |
| 9. ts = Community pharmacy (6.730) |
| 10.ts = Pharmacist* (26.322) |
| 11.6 OR 7 OR 8 OR 9 OR 10 (47.569) |
| 12.ts = (Random* AND Control*) (586.584) |
| 13. 5 AND 11 AND 12 (211) |
| 14. Filter according to date of publication (59) |
| Cochrane Central Register of Controlled Trials |
| 1. [mh Diabetes mellitus , type 2] (11.714) |
| 2. Type 2 Diabetes (28.274) |
| 3. T2DM (2.910) |
| 4. Non insulin dependent diabetes mellitus (11.653) |
| 5. NIDDM (1.115) |
| 6. 1 OR 2 OR 3 OR 4 OR 5 (29.876) |
| 7. [mh “Pharmaceutical services”] (1.698) |
| 8. Pharmaceutical care (4.673) |
| 9. Clinical pharmacy (10.716) |
| 10. Community pharmacy (1.874) |
| 11. Pharmacist* (4.188) |
| 12. 7 OR 8 OR 9 OR 10 OR 11 (16.839) |
| 13. 6 AND 12 (1.941) |
| 14. Trials filtered according to date of publication (69) |
Appendix B. . Risk of bias.
| Selection bias | Performance bias | Detection bias | Attrition bias | Reporting bias | Other biases | ||
|---|---|---|---|---|---|---|---|
|
|
|
|
|
|
|
||
| Reference | Random sequence generation | Allocation concealment | Blinding of participants and professionals | Blinding of outcome raters | Incomplete outcomes | Selective outcome reporting | Other sources of bias |
| Mahwi et al.(21) | Unclear risk of bias | Unclear risk of bias | Unclear risk of bias | Unclear risk of bias | Low risk | Low risk | Unclear risk of bias |
| Jarab et al.(26) | Low risk | Unclear risk of bias | Unclear risk of bias | Unclear risk of bias | Low risk | Low risk | Unclear risk of bias |
| Wishah et al. (27) | Low risk | Unclear risk of bias | Unclear risk of bias | Unclear risk of bias | High risk | High risk | Unclear risk of bias |
| Chung et al.(28) | Unclear risk of bias | Potential risk of bias | Unclear risk of bias | Unclear risk of bias | Low risk | Low risk | Unclear risk of bias |
| Ali et al.(29) | Low risk | Unclear risk of bias | Unclear risk of bias | Unclear risk of bias | Low risk | Low risk | Unclear risk of bias |
| Mourão et al.(30) | Low risk | Unclear risk of bias | Unclear risk of bias | Unclear risk of bias | Low risk | Low risk | Unclear risk of bias |
| Chan et al.(31) | Low risk | Unclear risk of bias | Unclear risk of bias | Unclear risk of bias | Low risk | Low risk | Unclear risk of bias |
| Korcegez et al.(32) | High risk | Unclear risk of bias | Unclear risk of bias | Unclear risk of bias | Low risk | Low risk | Unclear risk of bias |
| Siaw et al.(33) | Low risk | Low risk | Low risk | Unclear risk of bias | Low risk | Low risk | Low risk |
| Cani et al.(34) | Low risk | Unclear risk of bias | High risk | Unclear risk of bias | Low risk | Low risk | Unclear risk of bias |
| Aguiar et al.(35) | Low risk | Unclear risk of bias | Unclear risk of bias | Low risk | Low risk | Low risk | Low risk |
| Chen et al.(36) | Low risk | Unclear risk of bias | Unclear risk of bias | Unclear risk of bias | Low risk | Low risk | Unclear risk of bias |
| Jahangard-Rafsanjani et al.(37) | Low risk | Unclear risk of bias | Unclear risk of bias | Unclear risk of bias | Low risk | Low risk | Unclear risk of bias |
| Xin et al.(38) | Unclear risk of bias | Unclear risk of bias | Unclear risk of bias | Unclear risk of bias | Low risk | Low risk | Risco de viés incerto |
| Shao et al.(39) | Unclear risk of bias | Unclear risk of bias | Unclear risk of bias | Unclear risk of bias | Low risk | Low risk | Unclear risk of bias |
REFERENCES
- 1.1. American Diabetes Association. Standards of medical care in diabetes – 2017. Diabetes Care. 2017;40(Suppl1):S4-5.; American Diabetes Association Standards of medical care in diabetes – 2017. Diabetes Care. 2017;40(Suppl1):S4–S5. [PubMed] [Google Scholar]
- 2.2. Chen L, Magliano DJ, Zimmet PZ. The worldwide epidemiology of type 2 diabetes mellitus--present and future perspectives. Nat Rev Endocrinol. 2011;8(4):228-36. Review. [DOI] [PubMed]; Chen L, Magliano DJ, Zimmet PZ. The worldwide epidemiology of type 2 diabetes mellitus--present and future perspectives. Nat Rev Endocrinol. 2011;8(4):228–236. doi: 10.1038/nrendo.2011.183. Review. [DOI] [PubMed] [Google Scholar]
- 3.3. Smith KB, Smith MS. Obesity statistics. Prim Care. 2016;43(1):121-35. Review. [DOI] [PubMed]; Smith KB, Smith MS. Obesity statistics. Prim Care. 2016;43(1):121–135. doi: 10.1016/j.pop.2015.10.001. Review. [DOI] [PubMed] [Google Scholar]
- 4.4. International Diabetes Federation. IDF diabetes atlas. 7th ed. Brussels, Belgium: International Diabetes Federation; 2015.; International Diabetes Federation . IDF diabetes atlas. 7th. Brussels, Belgium: International Diabetes Federation; 2015. [Google Scholar]
- 5.5. Rubin RR, Peyrot M, Kruger DF, Travis LB. Barriers to insulin injection therapy: patient and health care provider perspectives. Diabetes Educ. 2009; 35(6):1014-22. [DOI] [PubMed]; Rubin RR, Peyrot M, Kruger DF, Travis LB. Barriers to insulin injection therapy: patient and health care provider perspectives. Diabetes Educ. 2009;35(6):1014–1022. doi: 10.1177/0145721709345773. [DOI] [PubMed] [Google Scholar]
- 6.6. Lai YR, Huang CC, Chiu WC, Liu RT, Tsai NW, Wang HC, et al. HbA1C Variability Is Strongly Associated With the Severity of Cardiovascular Autonomic Neuropathy in Patients With Type 2 Diabetes After Longer Diabetes Duration. Front Neurosci. 2019;13:458. [DOI] [PMC free article] [PubMed]; Lai YR, Huang CC, Chiu WC, Liu RT, Tsai NW, Wang HC, et al. HbA1C Variability Is Strongly Associated With the Severity of Cardiovascular Autonomic Neuropathy in Patients With Type 2 Diabetes After Longer Diabetes Duration. 458Front Neurosci. 2019;13 doi: 10.3389/fnins.2019.00458. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.7. Lee WC, Balu S, Cobden D, Joshi AV, Pashos CL. Medication adherence and the associated health-economic impact among patients with type 2 diabetes mellitus converting to insulin pen therapy: an analysis of third-party managed care claims data. Clin Ther. 2006;28(10):1712-25; discussion 1710-1. Erratum in: Clin Ther. 2006;28(11):1968-9. [DOI] [PubMed]; Lee WC, Balu S, Cobden D, Joshi AV, Pashos CL. Medication adherence and the associated health-economic impact among patients with type 2 diabetes mellitus converting to insulin pen therapy: an analysis of third-party managed care claims data. Clin Ther. 2006;28(10):1712–1725. doi: 10.1016/j.clinthera.2006.10.004. discussion 1710-1. Erratum in: Clin Ther. 2006;28(11):1968-9. [DOI] [PubMed] [Google Scholar]
- 8.8. ADVANCE Collaborative Group, Patel A, MacMahon S, Chalmers J, Neal B, Billot l, Woodward M, Marre M, Cooper M, Glasziou P, Grobbee D, Hamet P, Harrap S, Heller S, Liu L, Mancia G, Mogensen CE, Pan C, Poulter N, Rodgers A, Williams B, Bompoint S, de Galan BE, Joshi R, Travert F. Intensive blood glucose control and vascular outcomes in patients with type 2 diabetes. N Engl J Med. 2008;358(24):2560-72. [DOI] [PubMed]; ADVANCE Collaborative Group. Patel A, MacMahon S, Chalmers J, Neal B, l Billot, Woodward M, Marre M, Cooper M, Glasziou P, Grobbee D, Hamet P, Harrap S, Heller S, Liu L, Mancia G, Mogensen CE, Pan C, Poulter N, Rodgers A, Williams B, Bompoint S, Galan BE, Joshi R, Travert F. Intensive blood glucose control and vascular outcomes in patients with type 2 diabetes. N Engl J Med. 2008;358(24):2560–2572. doi: 10.1056/NEJMoa0802987. [DOI] [PubMed] [Google Scholar]
- 9.9. Butler RJ, Davis TK, Johnson WG, Gardner HH. Effects of nonadherence with prescription drugs among older adults. Am J Manag Care. 2011;17(2):153-60. [PubMed]; Butler RJ, Davis TK, Johnson WG, Gardner HH. Effects of nonadherence with prescription drugs among older adults. Am J Manag Care. 2011;17(2):153–160. [PubMed] [Google Scholar]
- 10.10. Foreman KF, Stockl KM, Le LB, Fisk E, Shah SM, Lew HC, et al. Impact of a text messaging pilot program on patient medication adherence. Clin Ther. 2012;34(5):1084-91. [DOI] [PubMed]; Foreman KF, Stockl KM, Le LB, Fisk E, Shah SM, Lew HC, et al. Impact of a text messaging pilot program on patient medication adherence. Clin Ther. 2012;34(5):1084–1091. doi: 10.1016/j.clinthera.2012.04.007. [DOI] [PubMed] [Google Scholar]
- 11.11. Tan MY, Magarey J. Self-care practices of Malaysian adults with diabetes and sub-optimal glycaemic control. Patient Educ Couns. 2008;72(2):252-67. [DOI] [PubMed]; Tan MY, Magarey J. Self-care practices of Malaysian adults with diabetes and sub-optimal glycaemic control. Patient Educ Couns. 2008;72(2):252–267. doi: 10.1016/j.pec.2008.03.017. [DOI] [PubMed] [Google Scholar]
- 12.12. Grant R, Adams AS, Trinacty CM, Zhang F, Kleinman K, Soumerai SB, et al. Relationship between patient medication adherence and subsequent clinical inertia in type 2 diabetes glycemic management. Diabetes Care. 2007;30(4):807-12. [DOI] [PubMed]; Grant R, Adams AS, Trinacty CM, Zhang F, Kleinman K, Soumerai SB, et al. Relationship between patient medication adherence and subsequent clinical inertia in type 2 diabetes glycemic management. Diabetes Care. 2007;30(4):807–812. doi: 10.2337/dc06-2170. [DOI] [PubMed] [Google Scholar]
- 13.13. Kooy MJ, van Geffen EC, Heerdink ER, van Dijk L, Bouvy ML. Effects of a Telephone Counselling Intervention by Pharmacist (TelCIP) on medication adherence, patient beliefs and satisfaction with information for patients starting treatment: study protocol for a cluster randomized controlled trial. BMC Health Serv Res. 2014;14:219. [DOI] [PMC free article] [PubMed]; Kooy MJ, van Geffen EC, Heerdink ER, van Dijk L, Bouvy ML. Effects of a Telephone Counselling Intervention by Pharmacist (TelCIP) on medication adherence, patient beliefs and satisfaction with information for patients starting treatment: study protocol for a cluster randomized controlled trial. 219BMC Health Serv Res. 2014;14 doi: 10.1186/1472-6963-14-219. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.14. Wubben DP, Vivian EM. Effects of pharmacist outpatient interventions on adults with diabetes mellitus: a systematic review. Pharmacotherapy. 2008; 28(4):421-36. Review. [DOI] [PubMed]; Wubben DP, Vivian EM. Effects of pharmacist outpatient interventions on adults with diabetes mellitus: a systematic review. Pharmacotherapy. 2008;28(4):421–436. doi: 10.1592/phco.28.4.421. Review. [DOI] [PubMed] [Google Scholar]
- 15.15. Toklu HZ, Hussain A. The changing face of pharmacy practice and the need for a new model of pharmacy education. J Young Pharm. 2013;5(2):38-40. Review. [DOI] [PMC free article] [PubMed]; Toklu HZ, Hussain A. The changing face of pharmacy practice and the need for a new model of pharmacy education. J Young Pharm. 2013;5(2):38–40. doi: 10.1016/j.jyp.2012.09.001. Review. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.16. Hepler CD, Strand LM. Opportunities and responsibilities in pharmaceutical care. Am J Hosp Pharm. 1990;47(3):533-43. [PubMed]; Hepler CD, Strand LM. Opportunities and responsibilities in pharmaceutical care. Am J Hosp Pharm. 1990;47(3):533–543. [PubMed] [Google Scholar]
- 17.17. Zaman Huri H, Fun Wee H. Drug related problems in type 2 diabetes patients with hypertension: a cross-sectional retrospective study. BMC Endocr Disord. 2013;13:2. [DOI] [PMC free article] [PubMed]; Zaman Huri H, Fun Wee H. Drug related problems in type 2 diabetes patients with hypertension: a cross-sectional retrospective study. 2BMC Endocr Disord. 2013;13 doi: 10.1186/1472-6823-13-2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.18. Kaufmann CP, Stämpfli D, Hersberger KE, Lampert ML. Determination of risk factors for drug-related problems: a multidisciplinary triangulation process. BMJ Open. 2015;5(3):e006376. [DOI] [PMC free article] [PubMed]; Kaufmann CP, Stämpfli D, Hersberger KE, Lampert ML. Determination of risk factors for drug-related problems: a multidisciplinary triangulation process. BMJ Open. 2015;5(3):e006376. doi: 10.1136/bmjopen-2014-006376. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.19. Zaman Huri H, Chai Ling L. Drug-related problems in type 2 diabetes mellitus patients with dyslipidemia. BMC Public Health. 2013;13:1192. [DOI] [PMC free article] [PubMed]; Zaman Huri H, Chai Ling L. Drug-related problems in type 2 diabetes mellitus patients with dyslipidemia. 1192BMC Public Health. 2013;13 doi: 10.1186/1471-2458-13-1192. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.20. Al-Taani GM, Al-Azzam SI, Alzoubi KH, Darwish Elhajji FW, Scott MG, Alfahel H, et al. Prediction of drug-related problems in diabetic outpatients in a number of hospitals, using a modeling approach. Drug Healthc Patient Saf. 2017;9:65-70. [DOI] [PMC free article] [PubMed]; Al-Taani GM, Al-Azzam SI, Alzoubi KH, Darwish Elhajji FW, Scott MG, Alfahel H, et al. Prediction of drug-related problems in diabetic outpatients in a number of hospitals, using a modeling approach. Drug Healthc Patient Saf. 2017;9:65–70. doi: 10.2147/DHPS.S125114. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.21. Mahwi TO, Obied KA. Role of the pharmaceutical care in the management of patients with type 2 diabetes mellitus. Int J Pharm Sci Res. 2013;4(4):1363-69.; Mahwi TO, Obied KA. Role of the pharmaceutical care in the management of patients with type 2 diabetes mellitus. Int J Pharm Sci Res. 2013;4(4):1363–1369. [Google Scholar]
- 22.22. Elissen AM, Steuten LM, Lemmens LC, Drewes HW, Lemmens KM, Meeuwissen JA, et al. Meta-analysis of the effectiveness of chronic care management for diabetes: investigating heterogeneity in outcomes. J Eval Clin Pract. 2013;19(5):753-62. [DOI] [PubMed]; Elissen AM, Steuten LM, Lemmens LC, Drewes HW, Lemmens KM, Meeuwissen JA, et al. Meta-analysis of the effectiveness of chronic care management for diabetes: investigating heterogeneity in outcomes. J Eval Clin Pract. 2013;19(5):753–762. doi: 10.1111/j.1365-2753.2012.01817.x. [DOI] [PubMed] [Google Scholar]
- 23.23. Aguiar PM, Brito Gde C, Lima Tde M, Santos AP, Lyra DP Jr, Storpirtis S. Investigating Sources of Heterogeneity in Randomized Controlled Trials of the Effects of Pharmacist Interventions on Glycemic Control in Type 2 Diabetic Patients: A Systematic Review and Meta-Analysis. PLoS One. 2016;11(3):e0150999. Review. [DOI] [PMC free article] [PubMed]; Aguiar PM, Brito Gde C, Lima Tde M, Santos AP, Lyra DP, Jr, Storpirtis S. Investigating Sources of Heterogeneity in Randomized Controlled Trials of the Effects of Pharmacist Interventions on Glycemic Control in Type 2 Diabetic Patients: A Systematic Review and Meta-Analysis. PLoS One. 2016;11(3):e0150999. doi: 10.1371/journal.pone.0150999. Review. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.24. Pousinho S, Morgado M, Falcão A, Alves G. Pharmacist interventions in the management of type 2 diabetes mellitus: a systematic review of randomized controlled trials. J Manag Care Spec Pharm. 2016;22(5):493-515. [DOI] [PMC free article] [PubMed]; Pousinho S, Morgado M, Falcão A, Alves G. Pharmacist interventions in the management of type 2 diabetes mellitus: a systematic review of randomized controlled trials. J Manag Care Spec Pharm. 2016;22(5):493–515. doi: 10.18553/jmcp.2016.22.5.493. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25.25. Liberati A, Altman DG, Tetzlaff J, Mulrow C, Gøtzsche PC, Ioannidis JP, et al. The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate healthcare interventions: explanation and elaboration. BMJ. 2009;339:b2700. [DOI] [PMC free article] [PubMed]; Liberati A, Altman DG, Tetzlaff J, Mulrow C, Gøtzsche PC, Ioannidis JP, et al. The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate healthcare interventions: explanation and elaboration. b2700BMJ. 2009;339 doi: 10.1136/bmj.b2700. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26.26. Jarab AS, Alqudah SG, Mukattash TL, Shattat G, Al-Qirim T. Randomized controlled trial of clinical pharmacy management of patients with type 2 diabetes in an outpatient diabetes clinic in Jordan. J Manag Care Pharm. 2012;18(7):516-26. [DOI] [PMC free article] [PubMed]; Jarab AS, Alqudah SG, Mukattash TL, Shattat G, Al-Qirim T. Randomized controlled trial of clinical pharmacy management of patients with type 2 diabetes in an outpatient diabetes clinic in Jordan. J Manag Care Pharm. 2012;18(7):516–526. doi: 10.18553/jmcp.2012.18.7.516. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 27.27. Wishah RA, Al-Khawaldeh OA, Albsoul AM. Impact of pharmaceutical care interventions on glycemic control and other health-related clinical outcomes in patients with type 2 diabetes: Randomized controlled trial. Diabetes Metab Syndr. 2015;9(4):271-6. [DOI] [PubMed]; Wishah RA, Al-Khawaldeh OA, Albsoul AM. Impact of pharmaceutical care interventions on glycemic control and other health-related clinical outcomes in patients with type 2 diabetes: Randomized controlled trial. Diabetes Metab Syndr. 2015;9(4):271–276. doi: 10.1016/j.dsx.2014.09.001. [DOI] [PubMed] [Google Scholar]
- 28.28. Chung WW, Chua SS, Lai PS, Chan SP. Effects of a pharmaceutical care model on medication adherence and glycemic control of people with type 2 diabetes. Patient Prefer Adherence. 2014;8:1185-94. [DOI] [PMC free article] [PubMed]; Chung WW, Chua SS, Lai PS, Chan SP. Effects of a pharmaceutical care model on medication adherence and glycemic control of people with type 2 diabetes. Patient Prefer Adherence. 2014;8:1185–1194. doi: 10.2147/PPA.S66619. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 29.29. Ali M, Schifano F, Robinson P, Phillips G, Doherty L, Melnick P, et al. Impact of community pharmacy diabetes monitoring and education programme on diabetes management: a randomized controlled study. Diabet Med. 2012; 29(9):e326-33. [DOI] [PubMed]; Ali M, Schifano F, Robinson P, Phillips G, Doherty L, Melnick P, et al. Impact of community pharmacy diabetes monitoring and education programme on diabetes management: a randomized controlled study. Diabet Med. 2012;29(9):e326–e333. doi: 10.1111/j.1464-5491.2012.03725.x. [DOI] [PubMed] [Google Scholar]
- 30.30. Mourão AO, Ferreira WR, Martins MA, Reis AM, Carrillo MR, Guimarães AG, et al. Pharmaceutical care program for type 2 diabetes patients in Brazil: a randomised controlled trial. Int J Clin Pharm. 2013;35(1):79-86. [DOI] [PubMed]; Mourão AO, Ferreira WR, Martins MA, Reis AM, Carrillo MR, Guimarães AG, et al. Pharmaceutical care program for type 2 diabetes patients in Brazil: a randomised controlled trial. Int J Clin Pharm. 2013;35(1):79–86. doi: 10.1007/s11096-012-9710-7. [DOI] [PubMed] [Google Scholar]
- 31.31. Chan CW, Siu SC, Wong CK, Lee VW. A pharmacist care program: positive impact on cardiac risk in patients with type 2 diabetes. J Cardiovasc Pharmacol Ther. 2012;17(1):57-64. [DOI] [PubMed]; Chan CW, Siu SC, Wong CK, Lee VW. A pharmacist care program: positive impact on cardiac risk in patients with type 2 diabetes. J Cardiovasc Pharmacol Ther. 2012;17(1):57–64. doi: 10.1177/1074248410396216. [DOI] [PubMed] [Google Scholar]
- 32.32. Korcegez EI, Sancar M, Demirkan K. Effect of a pharmacist-led program on improving outcomes in patients with type 2 diabetes mellitus from northern cyprus: a randomized controlled trial. J Manag Care Spec Pharm. 2017;23(5):573-82. [DOI] [PMC free article] [PubMed]; Korcegez EI, Sancar M, Demirkan K. Effect of a pharmacist-led program on improving outcomes in patients with type 2 diabetes mellitus from northern cyprus: a randomized controlled trial. J Manag Care Spec Pharm. 2017;23(5):573–582. doi: 10.18553/jmcp.2017.23.5.573. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 33.33. Siaw MY, Ko Y, Malone DC, Tsou KY, Lew YJ, Foo D, et al. Impact of pharmacist-involved collaborative care on the clinical, humanistic and cost outcomes of high-risk patients with type 2 diabetes (IMPACT): a randomized controlled trial. J Clin Pharm Ther. 2017;42(4):475-82. [DOI] [PubMed]; Siaw MY, Ko Y, Malone DC, Tsou KY, Lew YJ, Foo D, et al. Impact of pharmacist-involved collaborative care on the clinical, humanistic and cost outcomes of high-risk patients with type 2 diabetes (IMPACT): a randomized controlled trial. J Clin Pharm Ther. 2017;42(4):475–482. doi: 10.1111/jcpt.12536. [DOI] [PubMed] [Google Scholar]
- 34.34. Cani CG, Lopes Lda S, Queiroz M, Nery M. Improvement in medication adherence and self-management of diabetes with a clinical pharmacy program: a randomized controlled trial in patients with type 2 diabetes undergoing insulin therapy at a teaching hospital. Clinics (Sao Paulo). 2015; 70(2):102-6. [DOI] [PMC free article] [PubMed]; Cani CG, Lopes Lda S, Queiroz M, Nery M. Clinics. 2. Vol. 70. Sao Paulo: 2015. Improvement in medication adherence and self-management of diabetes with a clinical pharmacy program: a randomized controlled trial in patients with type 2 diabetes undergoing insulin therapy at a teaching hospital; pp. 102–106. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 35.35. Aguiar PM, da Silva CH, Chiann C, Dórea EL, Lyra DP Jr, Storpirtis S. Pharmacist-physician collaborative care model for patients with uncontrolled type 2 diabetes in Brazil: results from a randomized controlled trial. J Eval Clin Pract. 2018;24(1):22-30. [DOI] [PubMed]; Aguiar PM, Silva CH, Chiann C, Dórea EL, Lyra DP, Jr, Storpirtis S. Pharmacist-physician collaborative care model for patients with uncontrolled type 2 diabetes in Brazil: results from a randomized controlled trial. J Eval Clin Pract. 2018;24(1):22–30. doi: 10.1111/jep.12606. [DOI] [PubMed] [Google Scholar]
- 36.36. Chen JH, Ou HT, Lin TC, Lai EC, Kao YH. Pharmaceutical care of elderly patients with poorly controlled type 2 diabetes mellitus: a randomized controlled trial. Int J Clin Pharm. 2016;38(1):88-95. [DOI] [PubMed]; Chen JH, Ou HT, Lin TC, Lai EC, Kao YH. Pharmaceutical care of elderly patients with poorly controlled type 2 diabetes mellitus: a randomized controlled trial. Int J Clin Pharm. 2016;38(1):88–95. doi: 10.1007/s11096-015-0210-4. [DOI] [PubMed] [Google Scholar]
- 37.37. Jahangard-Rafsanjani Z, Sarayani A, Nosrati M, Saadat N, Rashidian A, Hadjibabaie M, et al. Effect of a community pharmacist-delivered diabetes support program for patients receiving specialty medical care: a randomized controlled trial. Diabetes Educ. 2015;41(1):127-35. [DOI] [PubMed]; Jahangard-Rafsanjani Z, Sarayani A, Nosrati M, Saadat N, Rashidian A, Hadjibabaie M, et al. Effect of a community pharmacist-delivered diabetes support program for patients receiving specialty medical care: a randomized controlled trial. Diabetes Educ. 2015;41(1):127–135. doi: 10.1177/0145721714559132. [DOI] [PubMed] [Google Scholar]
- 38.38. Xin C, Xia Z, Jiang C, Lin M, Li G. Effect of pharmaceutical care on medication adherence of patients newly prescribed insulin therapy: a randomized controlled study. Patient Prefer Adherence. 2015;9:797-802. [DOI] [PMC free article] [PubMed]; Xin C, Xia Z, Jiang C, Lin M, Li G. Effect of pharmaceutical care on medication adherence of patients newly prescribed insulin therapy: a randomized controlled study. Patient Prefer Adherence. 2015;9:797–802. doi: 10.2147/PPA.S84411. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 39.39. Shao H, Chen G, Zhu C, Chen Y, Liu Y, He Y, et al. Effect of pharmaceutical care on clinical outcomes of outpatients with type 2 diabetes mellitus. Patient Prefer Adherence. 2017;11:897-903. [DOI] [PMC free article] [PubMed]; Shao H, Chen G, Zhu C, Chen Y, Liu Y, He Y, et al. Effect of pharmaceutical care on clinical outcomes of outpatients with type 2 diabetes mellitus. Patient Prefer Adherence. 2017;11:897–903. doi: 10.2147/PPA.S92533. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 40.40. Cipolle R, Strand L, Morley P. Pharmaceutical Care Practice:The Clinician’s Guide. 2nd ed. New York: McGraw-Hill; 2004.; Cipolle R, Strand L, Morley P. Pharmaceutical Care Practice:The Clinician’s Guide. 2nd. New York: McGraw-Hill; 2004. [Google Scholar]
- 41.41. Santschi V, Chiolero A, Colosimo AL, Platt RW, Taffé P, Burnier M, et al. Improving blood pressure control through pharmacist interventions: a meta-analysis of randomized controlled trials. J Am Heart Assoc. 2014;3(2): e000718. Review. [DOI] [PMC free article] [PubMed]; Santschi V, Chiolero A, Colosimo AL, Platt RW, Taffé P, Burnier M, et al. Improving blood pressure control through pharmacist interventions: a meta-analysis of randomized controlled trials. J Am Heart Assoc. 2014;3(2):e000718. doi: 10.1161/JAHA.113.000718. Review. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 42.42. Deters MA, Laven A, Castejon A, Doucette WR, Ev LS, Krass I, et al. Effective Interventions for Diabetes Patients by Community Pharmacists: A Meta-analysis of Pharmaceutical Care Components. Ann Pharmacother. 2018; 52(2):198-211. [DOI] [PubMed]; Deters MA, Laven A, Castejon A, Doucette WR, Ev LS, Krass I, et al. Effective Interventions for Diabetes Patients by Community Pharmacists: A Meta-analysis of Pharmaceutical Care Components. Ann Pharmacother. 2018;52(2):198–211. doi: 10.1177/1060028017733272. [DOI] [PubMed] [Google Scholar]
- 43.43. Sociedade Brasileira de Diabetes (SBD). Diretrizes da Sociedade Brasileira de Diabetes 2015-2016 [Internet]. São Paulo: A.C. Farmacêutica, 2016 [citado 2019 Abr 2]. Disponível em: https://www.diabetes.org.br/profissionais/images/docs/DIRETRIZES-SBD-2015-2016.pdf ; Sociedade Brasileira de Diabetes (SBD) Diretrizes da Sociedade Brasileira de Diabetes 2015-2016. São Paulo: A.C. Farmacêutica; 2016. [citado 2019 Abr 2]. Internet. https://www.diabetes.org.br/profissionais/images/docs/DIRETRIZES-SBD-2015-2016.pdf. [Google Scholar]
- 44.44. Handelsman Y, Mechanick JI, Blonde L, Grunberger G, Bloomgarden ZT, Bray GA, Dagogo- Jack S, Davidson JA, Einhorn D, Ganda O, Garber AJ, Hirsch IB, Horton ES, Ismail-Beigi F, Jellinger PS, Jones KL, Jovanovič L, Lebovitz H, Levy P, Moghissi ES, Orzeck EA, Vinik AI, Wyne KL; AACE Task Force for Developing Diabetes Comprehensive Care Plan. American Association of Clinical Endocrinologists. Medical guideline for clinical practices for developing diabetes mellitus comprehensive care plan. Endocr Pract. 2011;17(Suppl 2):1-53. [DOI] [PubMed]; Handelsman Y, Mechanick JI, Blonde L, Grunberger G, Bloomgarden ZT, Bray GA, Dagogo- Jack S, Davidson JA, Einhorn D, Ganda O, Garber AJ, Hirsch IB, Horton ES, Ismail-Beigi F, Jellinger PS, Jones KL, Jovanovič L, Lebovitz H, Levy P, Moghissi ES, Orzeck EA, Vinik AI, Wyne KL, AACE Task Force for Developing Diabetes Comprehensive Care Plan American Association of Clinical Endocrinologists. Medical guideline for clinical practices for developing diabetes mellitus comprehensive care plan. Endocr Pract. 2011;17(Suppl 2):1–53. doi: 10.4158/ep.17.s2.1. [DOI] [PubMed] [Google Scholar]
- 45.45. Toobert DJ, Hampson SE, Glasgow RE. The summary of diabetes self-care activities measure: results from 7 studies and a revised scale. Diabetes Care. 2000;23(7):943-50. [DOI] [PubMed]; Toobert DJ, Hampson SE, Glasgow RE. The summary of diabetes self-care activities measure: results from 7 studies and a revised scale. Diabetes Care. 2000;23(7):943–950. doi: 10.2337/diacare.23.7.943. [DOI] [PubMed] [Google Scholar]
- 46.46. Moon SJ, Lee WY, Hwang JS, Hong YP, Morisky DE. Accuracy of a screening tool for medication adherence: a systematic review and meta-analysis of the Morisky Medication Adherence Scale-8. PLoS One. 2017;12(11):e0187139. Review. Erratum in: PLoS One. 2018;13(4):e0196138. [DOI] [PMC free article] [PubMed]; Moon SJ, Lee WY, Hwang JS, Hong YP, Morisky DE. Accuracy of a screening tool for medication adherence: a systematic review and meta-analysis of the Morisky Medication Adherence Scale-8. PLoS One. 2017;12(11):e0187139. doi: 10.1371/journal.pone.0187139. Review. Erratum in: PLoS One. 2018;13(4):e0196138. [DOI] [PMC free article] [PubMed] [Google Scholar]