Abstract
The translocator protein (TSPO) is an outer mitochondrial membrane protein that is widely used as a biomarker of neuroinflammation, being markedly upregulated in activated microglia in a range of brain pathologies. Despite its extensive use as a target in molecular imaging studies, the exact cellular functions of this protein remain in question. The long-held view that TSPO plays a fundamental role in the translocation of cholesterol through the mitochondrial membranes, and thus, steroidogenesis, has been disputed by several groups with the advent of TSPO knockout mouse models. Instead, much evidence is emerging that TSPO plays a fundamental role in cellular bioenergetics and associated mitochondrial functions, also part of a greater role in the innate immune processes of microglia. In this review, we examine the more direct experimental literature surrounding the immunomodulatory effects of TSPO. We also review studies which highlight a more central role for TSPO in mitochondrial processes, from energy metabolism, to the propagation of inflammatory responses through reactive oxygen species (ROS) modulation. In this way, we highlight a paradigm shift in approaches to TSPO functioning.
Keywords: neuroinflammation, translocator protein, microglia, reactive oxygen species, mitochondria
1. Introduction
The innate immune response is an emergent phenomenon arising from complex molecular and cellular signalling pathways. In the central nervous system (CNS), the innate immune response is orchestrated by microglial cells, capable of adopting differential functional states in response to stressors. The switch from homeostatic microglia to activated, potentially pro-inflammatory, microglia has become an important indicator of pathology in the CNS [1,2]. This switch is also known as M1/M2 polarization, where classically activated pro-inflammatory M1 microglia and alternatively activated M2 microglia lie on opposite ends of a continuum of functional states [3,4]. The pro-inflammatory M1 polarisation of resident microglia is often referred to as “neuroinflammation” to distinguish it from inflammatory tissue responses with recruitment of peripheral immunocytes. Neuroinflammation has been described across a wide spectrum of diseases, including psychiatric disorders, neurodegeneration and autoimmune diseases [5,6,7,8,9].
The strong metabolic demand of activated, proliferating microglia is reflected in the functional changes of mitochondria [10,11], and an intrinsic link exists between mitochondrial energetics and the mounting of an inflammatory response [12,13]. The pro-inflammatory M1 phenotype of microglia is underpinned by a switch from oxidative phosphorylation to glycolysis and involves shifts in mitochondrial fission and fusion [13,14]. Mitochondrial proteins are also involved in the signalling transduction pathways that activate inflammatory pathways to release pro-inflammatory factors, and also mediate apoptosis. Facilitating these immune responses is mitochondrial reactive oxygen species (ROS) release and oxidative stress signalling [15,16,17,18,19], as well as the NLRP3 inflammasome complex activation [20]. It is, therefore, important to understand the subcellular drivers of microglial reactivity, which will ultimately aid in the detection and targeting of key mediators of these immune processes.
One of the most widely studied biomarkers of microglial activation is the translocator protein 18 kDa (TSPO). TSPO is a transmembrane protein located primarily on the outer mitochondrial membrane [21,22], and was originally discovered as a peripheral binding site to diazepam [23], hence being long referred to as the peripheral benzodiazepine receptor (PBR). The marked upregulation of TSPO in activated microglia in a broad spectrum of neurobiological diseases has made TSPO a prominent target for positron emission tomography (PET) imaging studies [24]. Concomitantly, a large field of enquiry into TSPO binding agents for diagnostics and therapeutics has also emerged. Indeed, even the earliest description of TSPO upregulation in activated microglia was observed through the increased binding of prototypical TSPO ligands 1-(2-chlorophenyl)-N-methyl-N-(1-methylpropyl)-3-isoquinolinecarboxamide (PK11195) and 4’-Chlorodiazepam (Ro5-4864) in injury models [25,26]. Whilst these ligands are still widely used in studies probing TSPO functioning, newer classes of TSPO ligands have also emerged which will be mentioned throughout this review. Due to the prolific research into TSPO binding agents, several reviews have covered the many TSPO molecular imaging agents and their use in imaging studies in a spectrum of disorders [27,28,29], including neurodegenerative disorders [8,30,31,32,33], psychiatric disorders [34,35,36] and tumours [37].
Despite being widely utilised in imaging studies, the exact functions of TSPO are not well understood. It was long posited that TSPO was primarily involved in the translocation of cholesterol, and thus, steroidogenesis, supported by the strong abundance of TSPO expression in steroidogenic organs [38,39]. This led to the change in nomenclature from “peripheral benzodiazepine receptor” to “translocator protein” [40]. However, sparked by the creation of global TSPO knockout mouse models from independent groups [41,42,43,44], in which mice displayed normal pregnenolone levels, an overall shift in thinking about the functioning of TSPO emerged (several reviews exist which detail the history of TSPO research more comprehensively [45,46,47]). The field of TSPO has since expanded into several different pathways, with many of these lines of enquiry converging on the primary role of TSPO in immunomodulation, cellular bioenergetics, and associated mitochondrial processes. These lines of evidence have been achieved mainly through genetic deletion studies and studies using both older and novel TSPO binding agents. Along with this, several studies are now highlighting the potential neuroprotective properties of TSPO ligands in a broad range of disease or injury models.
In this review, we describe the more recent and growing body of literature surrounding the evolving knowledge of the functions of TSPO. Whilst TSPO has been studied in a broad spectrum of disease states in PET imaging studies, in this review we integrate more direct studies examining the role of TSPO in inflammatory responses, and its more central role in the modulation of mitochondrial energetic processes.
2. TSPO in Mitochondrial Processes
2.1. TSPO in Mitochondrial Bioenergetics
After a hypothesis first proposed by Anholt (1986), the earliest studies linking the function of TSPO to mitochondrial energy respiration used compounds targeting TSPO on isolated mitochondria from organs strongly expressing TSPO, such as the kidney, adrenals and liver [48,49]. This was followed by studies in a neuroblastoma cell line, where the high affinity ligands PK11195, and to a lesser extent, Ro5-4864, in co-culture resulted in dose-dependent increases in oxygen consumption compared to non-treated controls [50]. It was later found in a glioma cell line that these TSPO ligands can also increase mitochondrial numbers and mitochondrial division, further linking TSPO to mitochondrial dynamics [51]. However, from the earliest studies, the known strong presence of TSPO expression in steroidogenic organs and the ability of cholesterol to bind with high affinity to TSPO led to several years of study into the specific role of TSPO in cholesterol transport and steroidogenesis [39,52,53,54]. As this function continues to produce conflicting evidence, a role for TSPO in steroid synthesis cannot be ruled out, though further data in a range of experimental models is required.
In 2014, independent research groups created global and conditional TSPO knockout models which were found to be viable with no observable abnormalities, and importantly, no effect on steroidogenesis [41,43,55]. It was found, however, that microglia from TSPO knockout animals had lower ATP synthesis and oxygen consumption rates than their wildtype counterparts, suggesting that TSPO deficiency leads to alterations in microglial metabolic activity [41]. Extending on these findings, this group also demonstrated that TSPO overexpression in a human T-cell line increases mitochondrial ATP synthesis, compared to wildtype and empty-plasmid control cells, measured with the luciferin-luciferase bioluminescence assay in permeabilised Jurkat cells with intact mitochondria and cell structure. TSPO overexpressed cells also exhibited increased proliferation rates compared to wildtype and empty-plasmid control cells [56], thus establishing that a key role for TSPO may lie within cellular bioenergetics.
In more recent years, this path of inquiry has been pursued by multiple groups, using both rodent and human microglia. In the human microglia C20 cell line engineered for TSPO knockout, pregnenolone levels were unchanged in wildtype and knockout cells, including when exposed to TSPO ligands [57]. In agreement with Banati et al. (2014), basal and maximal respiration, as well as ATP-related oxygen consumption, was lower in TSPO knockout cells compared to wildtype cells. This was accompanied by reduced mitochondrial membrane potential and calcium retention [57]. In another recent study, using the rodent microglial cell line BV2, TSPO knockdown cells had altered mitochondrial membrane potential compared to scrambled controls. Furthermore, scramble BV2 cells treated with Ro5-4864 and PK11195 had increased basal respiration and ATP-related respiration [58], demonstrating the ability of TSPO-specific ligands to alter mitochondrial processes of microglia. A very recent and comprehensive study of the role of TSPO in several key mitochondrial functions has demonstrated similar results. TSPO knockout glioma cells were shown to have more mitochondrial fragmentation, increased levels of mitochondrial fission proteins such as FIS1, and decreased complex I activity compared to wildtype cells. TSPO knockout cells also had lower mitochondrial membrane potential, decreased global ATP production, reduced basal and maximal mitochondrial respiratory capacity and higher ROS levels compared to wildtype cells. These findings were also replicated in TSPO knockdown patient-derived stem-like GBM1B cells, demonstrating analogous effects in human cells [59]. Mechanistically, TSPO has been linked to the F1Fo-ATP synthase, the mitochondrial enzyme and protein complex responsible for synthesising cellular ATP. PK11195, Ro5-4864 and protoporphyrin IX (PPIX) have been found to modulate the phosphorylation of subunit c of the F1Fo-ATP synthase in isolated rat brain mitochondria [60]. PK11195 has also been found to inhibit mitophagy in Bcl-2 knockdown HeLa cells by inhibiting activity of the F1Fo-ATP synthase, in a similar way to oligomycin [61].
2.2. TSPO and Redox Mechanisms
An important by-product of the mitochondrial electron transport chain is the production of free radicals. Significant evidence has emerged linking TSPO to the production and modulation of ROS, important to the functioning of pro-inflammatory microglia [19]. In BV2 microglial cells, PK11195, Ro5-4864 and PPIX exposure in culture increased initial ROS production compared to non-exposed controls, and pre-treatment with an antioxidant blocked this effect [62]. In response to a stressor, TSPO transfected Jurkat cells were more resistant to UV-induced apoptosis, due to delayed membrane depolarisation, reduced caspase-3 activity and reduced superoxide generation compared to wildtype cells [63]. More recently, in a model of Alzheimer’s disease using amyloid precursor protein (APP) overexpressed neuroblastoma cells, newly synthesised imidazoquinazolinone TSPO ligands were able to reduce oxidative injury by decreasing ROS generation in response to H2O2 stimulation. These ligands could also stabilise mitochondrial respiration under stress conditions, and ultimately reduce levels of amyloid beta formation [64]. These novel ligands have also been found to increase levels of ATP production and stabilise mitochondrial membrane potential unrelated to any effects on steroidogenesis [65]. TSPO ligands have also demonstrated analogous effects in other immune cell types, as PK11195 was shown to reduce basal ROS generation in mouse primary peritoneal macrophages [66], and Ro5-4864 has been shown to preserve mitochondrial membrane potential and reduce ROS production after glucose deprivation stress in astrocytes, compared to controls [67].
Interestingly, TSPO and its involvement in ROS modulation has also been linked to mitophagy [17,68], a process which has been implicated in the innate immune response [69]. Through an interaction with voltage-dependent anion channel 1 (VDAC1), TSPO was able to inhibit mitophagy by increasing ROS production in mouse embryonic fibroblasts and canine mammary gland epithelial cells. TSPO was able to modulate levels of LC3B-II activity and the ubiquitination of key proteins involved in mitophagy. TSPO knockdown cells also displayed greater ATP production in response to challenge, and greater glutathione levels, compared to overexpressing cells and controls [68]. The production of ROS is important in the functioning of microglial responses, and in a recent hypothesis proposed by Guilarte et al. (2016), an interaction between TSPO and NOX2, producing ROS, may activate Nrf2 which is involved in redox homeostasis and antioxidant responses. This complex may work to regulate release of ROS in microglia, particularly in states of chronic neuroinflammation where there is prolonged activation causing oxidative damage to surrounding tissue [70].
TSPO functioning has also been linked to mitochondrial cell death processes and apoptosis through oxidative stress [71]. PK11195 pre-treatment in U118MG glioblastoma cells was able to prevent cell death induced by cobalt(II) chloride by inhibiting apoptosis, mitochondrial membrane potential collapse and cardiolipin oxidation. These effects were also observed after TSPO knockdown in U118MG cells [72]. TSPO has also been linked to nitric oxide (NO) in the induction of cell death. In U118MG cells, application of PK11195 with the NO donor sodium nitroprusside (SNP) attenuated cell death, counteracted decreases in metabolic activity, and reduced mitochondrial membrane potential collapse compared to SNP or vehicle controls. This effect was similar in TSPO knockdown cells, adding further evidence to the involvement of TSPO in cell death processes [73]. A similar phenomenon has also been demonstrated in a Drosophila model. TSPO knockout Drosophila had reduced gamma radiation-induced apoptosis, as well as increased lifespan compared to wildtype flies. TSPO knockout flies also had decreased oxidative phosphorylation enzymatic activity, increased oxidative stress, and reduced mitochondrial respiration after 1 week [74]. This was also confirmed later in a Drosophila model of alcohol dependence, where flies with conditional TSPO knockout in neurons had increased ROS production in the brain, although this was sex-dependent [75].
2.3. In Vivo Evidence for TSPO in Mitochondrial Processes
In concordance with this data, other studies using in vivo models have also demonstrated a key role for TSPO in mitochondrial processes, and also in neuroprotection. In a model of postischemia reperfusion in rats, Ro5-4864 pre-treatment reduced ROS levels, reduced the activity of NADPH oxidase, and increased activity of complex 1 and III of the electron transport chain in heart tissue, thereby improving functional recovery [76]. This ligand has also been shown to have mitochondrially-targeted protective properties in a rat model of myocardial ischemia-reperfusion, where Ro5-4864 pre-treatment in hypercholesterolemic rats inhibited cholesterol accumulation and restored oxidative phosphorylation compared to vehicle controls [77]. In an in vivo model of cortical trauma injury in rats, administration of Ro5-4864 after cortical contusion reduced the severity of brain mitochondrial damage as seen under transmission electron microscopy (TEM). This was accompanied by a reduced lactate/pyruvate ratio, indicating less metabolic damage in these animals compared to vehicle treated animals, ultimately leading to improved recovery [78]. Neuroprotective effects of newer TSPO ligands have also been reported. In a rat model of cortical infarction, 2-(2-chlorophenyl) quinazolin-4-yl dimethylcarbamate (2-Cl-MGV) administration after cerebral artery occlusion was found to prevent the collapse of mitochondrial membrane potential and reduce cytochrome c levels in the thalamus of injured rats. 2-Cl-MGV also rescued cognitive impairments and neuronal loss after injury compared to vehicle controls [79]. In a mouse model of spinal cord injury, administration of the TSPO ligand ZBD-2 following injury downregulated TSPO expression, reduced levels of inducible nitric oxide synthase (iNOS) and malondialdehyde (MDA), and increased levels of superoxide dismutase (SOD) in serum, whilst also reducing neuronal loss after injury [80], hence having antioxidative properties. It is therefore apparent that there is much emerging literature surrounding the role of TSPO in mitochondrial processes, including energy metabolism and ROS generation (Table 1). This is also important in the context of immune responses, as these mechanisms are intrinsically involved in the pro-inflammatory responses of microglia (Figure 1).
Table 1.
Summary of in vitro and in vivo experimental data describing the role of TSPO in mitochondrial processes.
| Model | Treatment/Ligands (Concentration) | Outcome | Reference |
|---|---|---|---|
| In vitro | |||
| Mouse GL261 glioma cells | TSPO KO | ↑ mitochondrial fragmentation, fission proteins, ROS, glycolysis ↓ Complex I activity, MMP, global ATP production, basal and maximal mitochondrial respiratory capacity | Fu et al. (2019) |
| Human C20 microglia | TSPO KO | ↓ MMP, basal and maximal respiration, ATP-related oxygen consumption | Milenkovic et al. (2019) |
| Mouse primary microglia | TSPO KO | ↓ mitochondrial ATP production, basal oxygen consumption rate | Banati et al. (2014) |
| Mouse BV2 microglia | TSPO KD and scramble control cells LPS + Ro5-4864 (100 nM), PK11195 (100 nM), XBD173 (1 or 10 μM) | TSPO KD ↓ MMP, proliferation ↑ non-mitochondrial respiration, proton leak Control cells, Ro5-4864 and PK11195 ↑ basal respiration, ATP-related oxygen consumption ↓ spare respiratory capacity TSPO KD, control cells, Ro5-4864, PK11195 ↑ MMP TSPO KD, Ro5-4864 ↑ maximal respiration and proton leak TSPO KD, PK11195, XBD173 ↑ coupling efficiency |
Bader et al. (2019) |
| Human U118MG cells | TSPO KD or Sodium nitroprusside + PK11195 (25 μM) | ↑ metabolic activity ↓ cell death, MMP collapse |
Shargorodsky et al. (2012) |
| Human U118MG cells | TSPO KD or CoCl2 + PK11195 (25 μM) | ↓ apoptosis, MMP collapse, ROS | Zeno et al. (2009) |
| Mouse embryonic fibroblasts, canine mammary gland epithelia | TSPO KD or overexpression | TSPO KD ↑ ATP production, GSH, LC3B-II ↓ ROS TSPO overexpression ↑ ROS ↓ GSH | Gatliff et al. (2014) |
| HeLa cells | Bcl-2 KD + PK11195 (100 μM) | ↓ mitophagy, F1Fo-ATPsynthase | Seneviratne et al. (2012) |
| Mouse peritoneal macrophages | PK11195, Ro5-4864 (1 μM) | PK11195 ↓ basal ROS Ro5-4864 ↑ basal ROS | Kupa et al. (2017) |
| Mouse BV2 microglia | PK11195, Ro5-4864, PPIX (10 nM) | ↑ ROS | Jayakumar et al. (2002) |
| Rat C6 and Human T98G cells | PK11195, Ro5-4864 (10 nM) | ↑ number of mitochondria, dividing mitochondria | Shirashi et al. (1991) |
| Mouse C1300 neuroblastoma cells | PK11195, Ro5-4864 (1 fm – 1 μM) | ↓ oxygen consumption | Larcher et al. (1989) |
| Rat isolated liver, kidney, adrenal mitochondria | PK11195, Ro5-4864 (1 μM) | ↓ mitochondrial respiratory control ratio | Hirsch et al. (1988) |
| Human T98G cells | Glucose deprivation + Ro5-4864 (10 nM-10 μm) | ↑ cell viability, MMP preservation ↓ ROS | Baez et al. (2017) |
| Human SH-SY5Y neuroblastoma cells | Mutant Tau cells + imidazoquinazolinones compounds 2a and 2b (10 nM) | ↑ ATP levels, MMP | Grimm et al. (2019) |
| Human SH-SY5Y neuroblastoma cells | APP overexpression + imidazoquinazolinones compounds 2a and 2b (10 nM) | ↑ mitochondrial respiration ↓ ROS, oxidative injury, cell death, Aβ levels | Lejri et al. (2019) |
| Human Jurkat cells | TSPO transfection | ↑ mitochondrial ATP production, cell proliferation | Liu et al. (2017) |
| Human Jurkat cells | TSPO transfection + UV exposure | ↓ superoxide, caspase 3 activity, MMP ↑ apoptosis resistance | Stoebner et al. (2001) |
| In vivo | |||
| Drosophila Aβ-42 induced neurodegeneration | TSPO KO | ↓ radiation-induced apoptosis, mitochondrial respiration, OXPHOS enzyme activity ↑ H2O2 resistance | Lin et al. (2014) |
| Drosophila model of alcohol dependence | Conditional TSPO KO in neurons | ↑ ROS (males only) ↓ caspase 3/7 activity | Lin et al. (2015) |
| Rat hypercholesterolemic rats | Myocardial ischemia-reperfusion + Ro5-4864 (10 mg/kg) | ↑ calcium retention, respiratory control ratio | Musman et al. (2017) |
| Rat cortical trauma injury | Ro5-4864, (5 mg/kg, repeat) | ↓ mitochondrial ultrastructural damage, metabolic damage ↑ neurological recovery | Soustiel et al. (2011) |
| Rat postischemia reperfusion, heart tissue | Ro5-4864 (16 μmol/L, 32 μmol/L, 64 μmol/L | ↓ ROS, NADPH oxidase ↑ functional recovery, complex I and III activity | Xiao et al. (2010) |
| Rat cortical infarction | 2-CI-MGV (7.5 mg/kg, repeat) | ↑ MMP, cognitive impairments, neuronal survival ↓ cytochrome c, Iba1+ microglia | Chen et al. (2017) |
| Mouse spinal cord injury | ZBD-2 (10 mg/kg, repeat) | ↓ serum MDA, iNOS ↑ SOD, neuronal survival | Cheng et al. (2016) |
Abbreviations: KO=knockout, ROS=reactive oxygen species, MMP=mitochondrial membrane potential, KD=knockdown, Aβ=amyloid beta, APP=amyloid precursor protein, GSH=glutathione, MDA=malondialdehyde, iNOS=inducible nitric oxide synthase, SOD=superoxide dismutase, OXPHOS=oxidative phosphorylation.
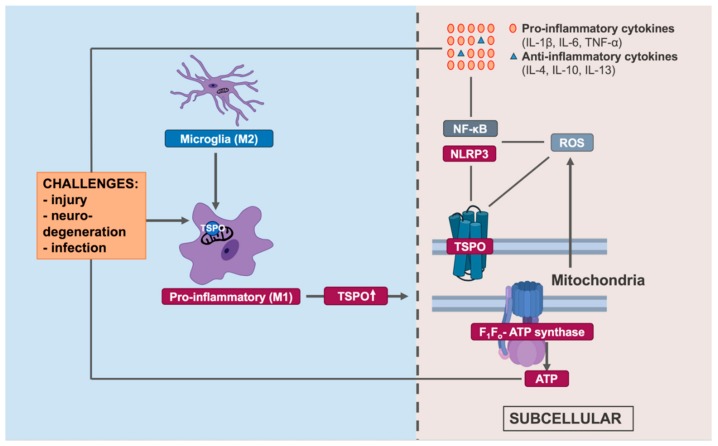
Figure 1.
Overview of the translocator protein (TSPO) in the inflammatory responses of microglia and its interaction with mitochondrial processes. Under stress conditions, TSPO is upregulated in activated, pro-inflammatory (M1) microglia. Located on the outer mitochondrial membrane, TSPO interacts with reactive oxygen species (ROS), a key part of the microglial inflammatory response. TSPO also interacts with inflammatory transcriptional pathways including MAPK and the NLRP3 inflammasome, resulting in the release of cytokines. These processes can be modulated by TSPO ligands, and by genetic deletion of TSPO, indicating a key role for TSPO in these processes.
3. TSPO in the Innate Immune Response
3.1. Microglial TSPO Expression and Modulation by TSPO Ligands
As a prominent molecular imaging biomarker of activated microglia in a range of pathologies, it is generally presumed that TSPO is an indicator of pro-inflammatory, aberrant microglial activation —hence “neuroinflammation”. However, the precise role of TSPO in the inflammatory processes of microglia during active disease states remains unclear. Furthermore, this is complicated by the known complexity of the functional states of microglia, most likely a spectrum from M1/M2 responses, depending on the stimulus [81]. The question of where on the spectrum TSPO is most prominently upregulated has been recently addressed by several studies. In a human microglial cell line, it was recently demonstrated that TSPO is directly involved in the modulation of pro- and anti-inflammatory phenotypes. TSPO mRNA expression was found to be greatest in cells after exposure to pro-inflammatory stimulation with IL-1β and IFN-γ. Differential secretion of pro- and anti-inflammatory cytokines could also be modulated by TSPO ligands and genetic knockdown. This was underpinned by mitochondrial ROS modulation, and NF-κB pathway expression, thereby underscoring TSPO in the mitochondrial processes of inflammatory responses [82]. Similarly, lipopolysaccharide (LPS) stimulation of mouse primary microglia resulted in increased TSPO expression in M1 microglia, though not in IL-4 treated M2 microglia. Thus, it was concluded that TSPO is specifically a biomarker of pro-inflammatory processes [83], a finding which has also been validated more recently in a similar experimental approach [84].
These conclusions have also been supported by studies using TSPO ligands. In primary human microglia, pre-treatment with PK11195 inhibited LPS-activation, reduced COX2 and TNF-α production, as well as calcium influx compared with vehicle treated controls [85]. Importantly, the morphology of microglia, which also reflects functional state, was similar to controls, thereby demonstrating the modulatory effect of PK11195 on microglial function and morphology [85]. In rat primary microglia, PK11195 has also been shown to inhibit increases in NO after LPS stimulation [86]. In primary mouse microglia, Etifoxine and PK11195 pre-treatment before toll-like receptor ligand activation were able to reduce microglial activation and production of TNF-α, CCL2 and IL-6 [87]. Vinpocetine, a specific TSPO ligand, was also shown to inhibit the activation and proliferation of LPS-stimulated or oxygen-glucose deprived BV2 cells compared to untreated controls. Furthermore, Vinpocetine was found to reduce the release of NO, IL-1β, IL-6 and TNF-α, whilst simultaneously suppressing NF-κB and AP-1 upregulation, which are important signalling transduction pathways in the inflammatory response [88].
Very recently, these findings were replicated in microglial cells using new generation TSPO binding agents. BV2 cells stimulated with LPS in the presence of TSPO ligands 2-Cl-MGV-1, MGV-1 and PK11195 all were able to mitigate COX2, iNOS and NO [89]. In a separate study using BV2 cells, assessing M1/M2 modulation, 2-Cl-MGV and MGV-1 suppressed LPS-induced cytokines IL-6, IL-1β, TNF-α and IFN-γ, though had no effect on IL-10 or IL-13 levels. These ligands also decreased NF-κB p65 activity and decreased ROS production as measured through cardiolipin content [90].
Not all studies have demonstrated the same immunomodulatory effect of TSPO ligands in pro-inflammatory suppression. PK11195 and Ro5-4864 treatment in rat primary microglia was found to increase the rate of phagocytosis, cell proliferation, ROS generation (also acting through NADPH oxidase), and IL-1β secretion, thereby increasing the pro-inflammatory capacity of microglia [91]. In TSPO knockdown BV2 cells challenged with LPS, increased ROS production, TNF-α expression and microglial proliferation rate has also been reported [92]. This same effect was also reported using the RAW 264.7 macrophage cell line, where TSPO knockdown cells exposed to Hemin activation increased TNF-α and IL-6 release compared to scramble controls [93]. In human cells, differential effects have also been reported. In human monocyte-derived macrophages, induced to an M1 state, TSPO mRNA expression was reduced compared to controls. There was also no difference in TSPO expression in M2 stimulated macrophages compared to control [94]. In human primary monocyte-derived macrophages, stimulated with LPS/IFN-γ, decreased TSPO gene expression and radioligand binding has also been reported in another study [95]. These results may reflect the known complexity of the functional and activation states of microglial cells, that may also be species dependent and dependent on the concentration of ligand applied.
3.2. Molecular Pathways of TSPO Immunomodulation
At the molecular level, the TSPO activation pathway interacts with downstream inflammatory effectors. Ro5-4864 application in THP-1 monocytes and bone marrow-derived macrophages has been shown to inhibit NLRP3 inflammasome complex activation and assembly after ATP stimulation, accompanied by reduced caspase-1 activation, IL-1β and IL-18 secretion [20]. TSPO transcription and expression is driven by c-Jun and STAT3 through the MAPK and PKCε signal transduction pathways, all of which are key to the induction of an inflammatory response [96,97,98]. ROS is also intrinsically linked to this pathway, activating PKCε-dependent pathways and c-Jun to control TSPO transcription [99]. PK11195 has also been shown to modulate genes and transcription factors in U118MG glioblastoma cells, particularly those related to cell viability, cell death, proliferation, and tumorigenesis, therefore showing that TSPO is involved in mitochondria-nuclear signalling and can modulate gene expression [22]. In the human macrophage cell line THP-1, exposure to Midazolam, a TSPO binding agent, suppressed LPS-induced inflammatory responses, including IL-6 expression, NO and NF-κB and MAPK activation. This was specific for TSPO, as TSPO knockout cells did not show this effect [100]. Hence, TSPO interacts with inflammation pathways at the transcriptional level, manifesting in the immunomodulatory effects described in this review.
3.3. In Vivo Immunomodulation of TSPO Ligands
Using in vivo models, TSPO ligands have been shown to modulate inflammation after injury or in certain disease states, thereby demonstrating neuroprotective properties (Table 2). In the earliest study examining this effect, Zavala et al. [101] demonstrated that administration of PK11195 and Ro5-4864 in mice impaired the release of IL-1β, TNF-α and IL-6 by peritoneal and spleen macrophages, accompanied by impaired oxidative respiratory burst of these macrophages. Since this finding, there have been several other studies using different disease and injury models demonstrating analogous effects. In an excitotoxic rat model of Huntington’s disease, PK11195 administration reduced the number of activated microglia after injury, and also reduced IL-1β, IL-6, TNF-α and iNOS mRNA expression after injury. This was also accompanied by a reduction in 4-HNE (lipid peroxidation) and 8-OHdG (oxidative DNA damage), alongside increased neuronal cell survival in the striatum near the site of injection, thereby conferring an anti-inflammatory and neuroprotective effect [102]. A similar phenomenon was also demonstrated with 3 novel pyrazolopyrimidine TSPO ligands; DPA-713, DPA-714 and propargyl-DPA in a quinolinic acid model of excitotoxic neurodegeneration. All pyrazolopyrimidine ligands decreased microglial activation and promoted neuronal survival in the injected striatum compared to vehicle controls [103].
Table 2.
Summary of in vitro and in vivo experimental data describing the role of TSPO in inflammatory processes.
| Model | Treatment/Ligands (Concentration) | Outcome | Reference |
|---|---|---|---|
| In vitro | |||
| Human C20 microglia | TSPO KD or IL-1β/IL-1β+IFN-γ + PK11195, Ro5-4864, Etifoxine, XBD173 (all 100 nM) | IL-1β/IL-1β+IFN-γ ↑ TSPO mRNA Etifoxine, XBD173 ↓ IL-8 Ro5-4864, PK11195, Etifoxine, XBD173 ↑ IL-4 ↓ ROS TSPO KD ↑ IL-8 ↓ IL-4 | Da Pozzo et al. (2019) |
| Mouse RAW 264.7 macrophages | TSPO KD or Hemin activation + Ro5-4864 (5 and 10 μM) | Ro5-4864 ↓ TNF-α, IL-6 TSPO KD ↑ IL-6, TNF-α | Bonsack et al. (2016) |
| Mouse BV2 microglia | LPS + TSPO KD | ↑ ROS, TNF-α, proliferation rate | Wang et al. (2014) |
| Mouse BV2 microglia | LPS + TSPO KD/overexpression, PK11195, Ro5-4864 (0.1 or 10 μM) | LPS + TSPO overexpression/ligands ↑ M2 related genes ↓ NF-κB activity, IL-6, TNF-α LPS +TSPO KD ↑ IL-6, TNF-α, NO | Bae et al. (2014) |
| Mouse primary microglia and bone-marrow derived macrophages | LPS/IL-4 polarisation | LPS ↑ TSPO expression | Pannell et al. (2019) |
| Human monocyte-derived macrophages and microglia | LPS/IL-4/IL-13 | LPS ↓ TSPO mRNA, TSPO radioligand binding | Owen et al. (2017) |
| Mouse primary microglia | LPS/IL-4 polarisation | LPS ↑ TSPO mRNA | Beckers et al. (2018) |
| Human monocyte-derived macrophages | LPS/IFN-γ stimulation | ↓ TSPO mRNA | Narayan et al. (2017) |
| Mouse BV2 microglia | LPS + 2-MGV-1, MGV-1, PK11195 (25 μM) | ↓ COX2, iNOS, NO | Azrad et al. (2019) |
| Mouse BV2 microglia | LPS + 2-MGV-1, MGV-1 (25 μM) | ↓ IL-6, IL-1β, TNF-α, IFN-γ, ROS, NF-κB p65 activity | Monga et al. (2019) |
| Human THP-1 monocytes/macrophages, mouse primary bone marrow-derived macrophages | LPS + ATP + Ro5-4864 (50 μM) | ↓ NLRP3 inflammasome activation/assembly, caspase-1, IL-1β, IL-18, ROS, MMP depolarization | Lee et al. (2016b) |
| Mouse BV2 microglia | LPS or oxygen-glucose deprivation + Vinpocetine (20 and 50 μM) | ↓ microglial activation and proliferation, NO, IL-6, IL-1β, TNF-α, NF-κB, AP-1 | Zhao et al. (2011) |
| Human THP-1 macrophages | LPS + Midazolam (15 μM) | ↓ IL-6, NO, NF-κB, MAPK | Horiguchi et al. (2019) |
| Rat primary microglia | LPS + PK11195 (100 μM) | ↓ NO | Wilms et al. (2003) |
| Human primary microglia | LPS + PK11195 (1 μM or 50 μM) | ↓ COX2, TNF-α, calcium influx, microglial activation | Choi et al. (2002) |
| Rat primary microglia | PK11195, Ro5-4864 (1nm-100 nM) | ↑ phagocytosis, cell proliferation, ROS, NADPH oxidase, IL-1β, microglial activation | Choi et al. (2011) |
| Mouse primary microglia | TLR ligand activation + PK11195, Etifoxine (50 μM) | ↓ TNF-α, IL-6, CCL2 | Lee et al. (2016) |
| In vivo | |||
| Mouse 3xTg-AD Alzheimer’s Disease | Ro5-4864 (3 mg/kg, repeat) | ↓ Aβ plaques, Iba1+ microglia ↑ behaviour and cognition | Barron et al. (2013) |
| Mouse primary peritoneal macrophages | LPS + Ro5-4864 (1 mg/kg) | ↓ IL-1β, TNF-α, IL-6, oxidative metabolism | Zavala et al. (1990) |
| Rat excitotoxic Huntington’s Disease | Quinolinic acid + PK11195 (5 nM) | ↓ Iba1+ microglia, IL-1β, IL-6, TNF-α, iNOS, 4-HNE, 8-OHdG ↑ neuronal survival | Ryu et al. (2005) |
| Rat excitotoxic neurodegeneration | Quinolinic acid + DPA-713, DPA-714 and propargyl-DPA (5 nM) | ↓ OX-42+ microglia ↑ neuronal survival | Leaver et al. (2012) |
| Mouse MPTP Parkinson’s Disease | XBD173 (50 mg/kg, repeat) | ↑ neuronal survival, dopamine, motor function, IL-10 ↓ Iba1+ microglia, COX2, CXCL10 | Gong et al. (2019) |
| Mouse EAE model | XBD173 (10, 20, 30 mg/kg, repeat) | ↓ IL-6, TNF-α and IL-17, clinical EAE score ↑ MBP expression, motor function | Leva et al. (2017) |
| Mouse retinal degeneration | XBD173 (10 mg/kg, repeat) | ↓ Iba1+ microglia, IL-6, CCL2, retinal degeneration | Scholz et al. (2015) |
| Rat traumatic brain injury | Etifoxine (50 mg/kg, repeat) | ↑ behaviour and sensorimotor function ↓ CD68+ microglia, neuronal degeneration, IL-1α, IL-1β, IL-6, TNF-α, CCL2 | Simon O’Brien et al. (2016) |
| Rat sciatic nerve crush injury | Etifoxine (50 mg/kg, repeat) | ↑ myelination, neuronal survival, sensory and motor function ↓ macrophage activation (OX-42+), IL-6, TNF-α, IL-1β | Girard et al. (2008) |
Abbreviations: KD=knockdown, NO=nitric oxide, LPS=lipopolysaccharide, MMP=mitochondrial membrane potential, ROS=reactive oxygen species, EAE=experimental autoimmune encephalomyelitis, MBP=myelin basic protein.
To emphasise the neuroprotective potential of a variety of TSPO ligands, several other studies have demonstrated improved progression, symptoms and functional recovery in various disease and injury models following ligand administration [104,105]. Etifoxine was found to promote greater regeneration of myelinated axons compared to vehicle controls 2 weeks after sciatic nerve crush injury. This was accompanied by increased neuronal survival, reduced activation of macrophages, and reduced pro-inflammatory cytokine secretion. Ultimately, this manifested in the recovery of sensory and motor functions [106]. Etifoxine administration has also been found to improve scores in behavioural testing and rescues from neuronal degeneration in a rat model of traumatic brain injury, accompanied by reduced microglial activation and reduced cortical concentrations of IL-1α, IL-1β, IL-6, CCL2 and TNF-α [107]. In an Alzheimer’s disease mouse model, application of Ro5-4864 attenuated the accumulation of amyloid beta plaques in the hippocampus and decreased microglial activation. Importantly, this was accompanied by improved behaviour and cognition [108]. In a study using a retinal degeneration mouse model, application of XBD173, another new generation TSPO ligand prevented microglial reactivity in the retina when exposed to injury and reduced both IL-6 and CCL2 gene expression. These findings were accompanied by prevention of retinal degeneration after injury, hence drastically inhibiting the progression of disease [109]. XBD173 has also been shown to decrease pro-inflammatory cytokines and delay Multiple Sclerosis progression and symptoms in an experimental autoimmune encephalomyelitis (EAE) mouse model [110], and also demonstrated efficacy in attenuating microglial activation and neuronal loss in an MPTP Parkinson’s disease model [111].
4. Future Directions
This review has presented the growing body of literature investigating the role of TSPO in inflammatory responses and in mitochondrial processes, where function has largely been explored through pharmacological studies. Whilst the diazepam derivative Ro5-4864 is regarded as selective for TSPO, careful reading of earlier studies reports the possibility of some remnant binding to GABA-ergic sites [112,113]. Hence, a degree of caution is necessary in the interpretation of in vitro observations where high concentrations of Ro5-4864 have been used. Whilst for PK11195 no other obvious binding site is known, the compound might insert itself into the lipid bilayers [114,115], an interaction that speculatively may contribute to the recent observation that the residence time of PK11195, rather than merely its binding affinity to TSPO, may determine its physiological activity [116]. Nonetheless, the continual study of novel TSPO binding agents will be important for the development of therapeutic compounds for a range of disorders. The therapeutic potential of TSPO ligands have already been demonstrated in combination with photodynamic [117] and sonodynamic therapy [118], where the ability of TSPO to modulate ROS and apoptosis mechanisms can be exploited. Whilst much has been learned through pharmacological targeting of TSPO, deletion studies of TSPO are comparatively lacking. Further studies using TSPO deficient cells and animal models under stress conditions, for example, after irradiation, are needed to clarify the exact role of TSPO in oxidative stress responses and microglial responses. Further studies using various experimental approaches are also required to address the discrepancies in data looking at ROS and energy metabolism, where pharmacological evidence and genetic deletion studies give sometimes inconsistent results. This may be owing to the differences between TSPO knockdown versus knockout, and the range of ligand concentrations used in studies. Studies using TSPO knockout material are also necessary in order to determine the specific effects or off-target effects of novel compounds.
The most widely studied context of TSPO has been centred around pro-inflammatory responses specifically. However, there are studies that demonstrated no difference or even decreases in TSPO expression after exposure to a pro-inflammatory stimulus in vitro [94,95]. It is also interesting that in a TSPO deficient mouse model, the ability to mount a local microglial response to nerve cell injury was not compromised [41], and in a more recent TSPO knockout model, TSPO deficiency did not affect microglial number or morphology in models of retinal degeneration [119]. The complex spectrum from pro- to anti-inflammatory processes in microglia has not yet been fully characterised, and the extent to which TSPO expression levels may provide an indication of the balance between pro- and anti-inflammatory tissue responses remains open. The terms “microglial activation” and “neuroinflammation” are perhaps too broad and require comprehensive assessment in response to specific stimuli, and may involve systems biological approaches going forward [120].
Even in vivo, PET studies have also reported a decrease in TSPO binding in certain disorders. For example, in a mouse schizophrenia model, TSPO radioligand binding was decreased in the prefrontal cortex, which did not match the concomitant increases in inflammatory cytokine levels [34]. In recent studies, evidence has confirmed that there is constitutive TSPO expression in cell types other than activated microglia in the brain. This includes, for example, neural stem cells, tanycytes, and most abundantly, vascular endothelial cells across the brain [26,121,122,123]. This has brought into question the approaches used for TSPO signal quantification in molecular imaging studies, and also raises questions as to the interpretation of imaging studies where a downregulation of TSPO is reported. Notably, when reductions below normal levels are observed, this may reflect a reduction in constitutively expressed TSPO which appears to be mainly located in the vasculature. Therefore, investigating other known cell types of TSPO expression over longer periods of time will be useful in order to ascertain whether the cumulative change in the regional expression levels of TSPO are due to a change in the number of cells expressing inducible TSPO, or whether indeed a downregulation of TSPO takes place in individual cells in which TSPO increases had been induced before. Furthermore, investigating other known cell types of TSPO expression will also be useful for future investigations into the functions of TSPO. This may be particularly pertinent given that the cell types of highest TSPO expression appear to be mitotically active, proliferative cells, further pointing to a fundamental role for TSPO in energy metabolism.
Acknowledgments
CB is supported by an AINSE Postgraduate Award (AINSE PGRA).
Author Contributions
Conceptualization, C.B. and G.-J.L.; writing—original draft preparation, C.B.; writing—review and editing, G.-J.L., R.J.M., R.B. All authors have read and agreed to the published version of the manuscript
Funding
This research received no external funding.
Conflicts of Interest
The authors declare no conflict of interest.
References
- 1.Banati R.B. Visualising microglial activation in vivo. Glia. 2002;40:206–217. doi: 10.1002/glia.10144. [DOI] [PubMed] [Google Scholar]
- 2.Kreutzberg G.W. Microglia: A sensor for pathological events in the cns. Trends Neurosci. 1996;19:312–318. doi: 10.1016/0166-2236(96)10049-7. [DOI] [PubMed] [Google Scholar]
- 3.Ley K. M1 means kill; m2 means heal. J. Immunol. (Baltimore, Md.: 1950) 2017;199:2191–2193. doi: 10.4049/jimmunol.1701135. [DOI] [PubMed] [Google Scholar]
- 4.Akhmetzyanova E., Kletenkov K., Mukhamedshina Y., Rizvanov A. Different approaches to modulation of microglia phenotypes after spinal cord injury. Front. Syst. Neurosci. 2019;13:37. doi: 10.3389/fnsys.2019.00037. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Graeber M.B., Li W., Rodriguez M.L. Role of microglia in cns inflammation. FEBS Lett. 2011;585:3798–3805. doi: 10.1016/j.febslet.2011.08.033. [DOI] [PubMed] [Google Scholar]
- 6.Graeber M.B., Streit W.J. Microglia: Biology and pathology. Acta Neuropathol. 2010;119:89–105. doi: 10.1007/s00401-009-0622-0. [DOI] [PubMed] [Google Scholar]
- 7.Block M.L., Zecca L., Hong J.S. Microglia-mediated neurotoxicity: Uncovering the molecular mechanisms. Nat. Rev. Neurosci. 2007;8:57–69. doi: 10.1038/nrn2038. [DOI] [PubMed] [Google Scholar]
- 8.Banati R.B., Cagnin A., Myers R., Gunn R.N., Turkheimer F.E., Brooks D.J., Jones T. Microglial activation in neurodegenerative diseases: A pet study using [11c](r)-pk11195. NeuroImage. 2000:11. [Google Scholar]
- 9.Banati R.B., Newcombe J., Gunn R.N., Cagnin A., Turkheimer F., Heppner F., Price G., Wegner F., Giovannoni G., Miller D.H., et al. The peripheral benzodiazepine binding site in the brain in multiple sclerosis. Quantitative in vivo imaging of microglia as a measure of disease activity. Brain. 2000;123:2321–2337. doi: 10.1093/brain/123.11.2321. [DOI] [PubMed] [Google Scholar]
- 10.Banati R.B., Egensperger R., Maassen A., Hager G., Kreutzberg G.W., Graeber M.B. Mitochondria in activated microglia in vitro. J. Neurocytol. 2004;33:535–541. doi: 10.1007/s11068-004-0515-7. [DOI] [PubMed] [Google Scholar]
- 11.Weinberg S.E., Sena L.A., Chandel N.S. Mitochondria in the regulation of innate and adaptive immunity. Immunity. 2015;42:406–417. doi: 10.1016/j.immuni.2015.02.002. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Aldana B.I. Microglia-specific metabolic changes in neurodegeneration. J. Mol. Biol. 2019;431:1830–1842. doi: 10.1016/j.jmb.2019.03.006. [DOI] [PubMed] [Google Scholar]
- 13.Orihuela R., McPherson C.A., Harry G.J. Microglial m1/m2 polarization and metabolic states. Br. J. Pharm. 2016;173:649–665. doi: 10.1111/bph.13139. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Nair S., Sobotka K.S., Joshi P., Gressens P., Fleiss B., Thornton C., Mallard C., Hagberg H. Lipopolysaccharide-induced alteration of mitochondrial morphology induces a metabolic shift in microglia modulating the inflammatory response in vitro and in vivo. Glia. 2019;67:1047–1061. doi: 10.1002/glia.23587. [DOI] [PubMed] [Google Scholar]
- 15.Ghosh S., Castillo E., Frias E.S., Swanson R.A. Bioenergetic regulation of microglia. Glia. 2018;66:1200–1212. doi: 10.1002/glia.23271. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Angajala A., Lim S., Phillips J.B., Kim J.H., Yates C., You Z., Tan M. Diverse roles of mitochondria in immune responses: Novel insights into immuno-metabolism. Front. Immunol. 2018:9. doi: 10.3389/fimmu.2018.01605. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.Gatliff J., Campanella M. Tspo is a redox regulator of cell mitophagy. Biochem. Soc. Trans. 2015;43:543–552. doi: 10.1042/BST20150037. [DOI] [PubMed] [Google Scholar]
- 18.Banati R.B., Rothe G., Valet G., Kreutzberg G.W. Respiratory burst activity in brain macrophages: A flow cytometric study on cultured rat microglia. Neuropathol. Appl. Neurobiol. 1991;17:223–230. doi: 10.1111/j.1365-2990.1991.tb00718.x. [DOI] [PubMed] [Google Scholar]
- 19.Banati R.B., Gehrmann J., Schubert P., Kreutzberg G.W. Cytotoxicity of microglia. Glia. 1993;7:111–118. doi: 10.1002/glia.440070117. [DOI] [PubMed] [Google Scholar]
- 20.Lee J.W., Kim L.E., Shim H.J., Kim E.K., Hwang W.C., Min D.S., Yu S.W. A translocator protein 18 kda ligand, ro5-4864, inhibits atp-induced nlrp3 inflammasome activation. Biochem. Biophys. Res. Commun. 2016;474:587–593. doi: 10.1016/j.bbrc.2016.04.080. [DOI] [PubMed] [Google Scholar]
- 21.Anholt R.R., Pedersen P.L., De Souza E.B., Snyder S.H. The peripheral-type benzodiazepine receptor. Localization to the mitochondrial outer membrane. J. Biol. Chem. 1986;261:576–583. [PubMed] [Google Scholar]
- 22.Yasin N., Veenman L., Singh S., Azrad M., Bode J., Vainshtein A., Caballero B., Marek I., Gavish M. Classical and novel tspo ligands for the mitochondrial tspo can modulate nuclear gene expression: Implications for mitochondrial retrograde signaling. Int. J. Mol. Sci. 2017:18. doi: 10.3390/ijms18040786. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.Braestrup C., Squires R.F. Specific benzodiazepine receptors in rat brain characterized by high-affinity (3h)diazepam binding. Proc. Natl. Acad. Sci. United. States. Am. 1977;74:3805–3809. doi: 10.1073/pnas.74.9.3805. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.Chen M.K., Guilarte T.R. Translocator protein 18 kda (tspo): Molecular sensor of brain injury and repair. Pharm. Thera. 2008;118:1–17. doi: 10.1016/j.pharmthera.2007.12.004. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25.Gehlert D.R., Stephenson D.T., Schober D.A., Rash K., Clemens J.A. Increased expression of peripheral benzodiazepine receptors in the facial nucleus following motor neuron axotomy. Neurochem. Int. 1997;31:705–713. doi: 10.1016/S0197-0186(97)00007-7. [DOI] [PubMed] [Google Scholar]
- 26.Banati R.B., Myers R., Kreutzberg G.W. Pk (’peripheral benzodiazepine’)—Binding sites in the cns indicate early and discrete brain lesions: Microautoradiographic detection of [3h]pk 11195 binding to activated microglia. J. Neurocytol. 1997;26:77–82. doi: 10.1023/A:1018567510105. [DOI] [PubMed] [Google Scholar]
- 27.Ghadery C., Best L.A., Pavese N., Tai Y.F., Strafella A.P. Pet evaluation of microglial activation in non-neurodegenerative brain diseases. Curr. Neurol. Neurosci. Rep. 2019:19. doi: 10.1007/s11910-019-0951-x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 28.Best L., Ghadery C., Pavese N., Tai Y.F., Strafella A.P. New and old tspo pet radioligands for imaging brain microglial activation in neurodegenerative disease. Curr. Neurol. Neurosci. Rep. 2019:19. doi: 10.1007/s11910-019-0934-y. [DOI] [PubMed] [Google Scholar]
- 29.Cumming P., Burgher B., Patkar O., Breakspear M., Vasdev N., Thomas P., Liu G.J., Banati R. Sifting through the surfeit of neuroinflammation tracers. J. Cereb. Blood. Flow. Metab. 2018;38:204–224. doi: 10.1177/0271678X17748786. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 30.Mirzaei N., Tang S.P., Ashworth S., Coello C., Plisson C., Passchier J., Selvaraj V., Tyacke R.J., Nutt D.J., Sastre M. In vivo imaging of microglial activation by positron emission tomography with [(11)c]pbr28 in the 5xfad model of alzheimer's disease. Glia. 2016;64:993–1006. doi: 10.1002/glia.22978. [DOI] [PubMed] [Google Scholar]
- 31.Ji B., Maeda J., Sawada M., Ono M., Okauchi T., Inaji M., Zhang M.R., Suzuki K., Ando K., Staufenbiel M., et al. Imaging of peripheral benzodiazepine receptor expression as biomarkers of detrimental versus beneficial glial responses in mouse models of alzheimer's and other cns pathologies. J. Neurosci. 2008;28:12255–12267. doi: 10.1523/JNEUROSCI.2312-08.2008. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 32.Dupont A.C., Largeau B., Ribeiro M.J.S., Guilloteau D., Tronel C., Arlicot N. Translocator protein-18 kda (tspo) positron emission tomography (pet) imaging and its clinical impact in neurodegenerative diseases. Int. J. Mol. 2017:18. doi: 10.3390/ijms18040785. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 33.Cagnin A., Brooks D.J., Kennedy A.M., Gunn R.N., Myers R., Turkheimer F.E., Jones T., Banati R.B. In-vivo measurement of activated microglia in dementia. Lancet. 2001;358:461–467. doi: 10.1016/S0140-6736(01)05625-2. [DOI] [PubMed] [Google Scholar]
- 34.Notter T., Coughlin J.M., Gschwind T., Weber-Stadlbauer U., Wang Y., Kassiou M., Vernon A.C., Benke D., Pomper M.G., Sawa A., et al. Translational evaluation of translocator protein as a marker of neuroinflammation in schizophrenia. Mol. Psychiatry. 2018;23:323–334. doi: 10.1038/mp.2016.248. [DOI] [PubMed] [Google Scholar]
- 35.Barichello T., Simões L.R., Collodel A., Giridharan V.V., Dal-Pizzol F., Macedo D., Quevedo J. The translocator protein (18 kda) and its role in neuropsychiatric disorders. Neurosci. Biobehav. Rev. 2017;83:183–199. doi: 10.1016/j.neubiorev.2017.10.010. [DOI] [PubMed] [Google Scholar]
- 36.Guilarte T.R. Tspo in diverse cns pathologies and psychiatric disease: A critical review and a way forward. Pharm. Thera. 2019;194:44–58. doi: 10.1016/j.pharmthera.2018.09.003. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 37.Roncaroli F., Su Z., Herholz K., Gerhard A., Turkheimer F.E. Tspo expression in brain tumours: Is tspo a target for brain tumour imaging? Clin. Transl. Imaging. 2016;4:145–156. doi: 10.1007/s40336-016-0168-9. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 38.Fan J., Campioli E., Midzak A., Culty M., Papadopoulos V. Conditional steroidogenic cell-targeted deletion of tspo unveils a crucial role in viability and hormone-dependent steroid formation. Proc. Natl. Acad. Sci. USA. 2015;112:7261–7266. doi: 10.1073/pnas.1502670112. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 39.Costa B., Pozzo E.D., Martini C. Translocator protein and steroidogenesis. Biochem. J. 2018;475:901–904. doi: 10.1042/BCJ20170766. [DOI] [PubMed] [Google Scholar]
- 40.Papadopoulos V., Baraldi M., Guilarte T.R., Knudsen T.B., Lacapere J.J., Lindemann P., Norenberg M.D., Nutt D., Weizman A., Zhang M.R., et al. Translocator protein (18kda): New nomenclature for the peripheral-type benzodiazepine receptor based on its structure and molecular function. Trends. Pharm. Sci. 2006;27:402–409. doi: 10.1016/j.tips.2006.06.005. [DOI] [PubMed] [Google Scholar]
- 41.Banati R.B., Middleton R.J., Chan R., Hatty C.R., Kam W.W., Quin C., Graeber M.B., Parmar A., Zahra D., Callaghan P., et al. Positron emission tomography and functional characterization of a complete pbr/tspo knockout. Nat. Commun. 2014;5:5452. doi: 10.1038/ncomms6452. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 42.Middleton R.J., Liu G.J., Banati R.B. Guwiyang wurra—’Fire mouse’: A global gene knockout model for tspo/pbr drug development, loss-of-function and mechanisms of compensation studies. Biochem. Soc. Trans. 2015;43:553–558. doi: 10.1042/BST20150039. [DOI] [PubMed] [Google Scholar]
- 43.Tu L.N., Morohaku K., Manna P.R., Pelton S.H., Butler W.R., Stocco D.M., Selvaraj V. Peripheral benzodiazepine receptor/translocator protein global knock-out mice are viable with no effects on steroid hormone biosynthesis. J. Biol. Chem. 2014;289:27444–27454. doi: 10.1074/jbc.M114.578286. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 44.Wang H., Zhai K., Xue Y., Yang J., Yang Q., Fu Y., Hu Y., Liu F., Wang W., Cui L., et al. Global deletion of tspo does not affect the viability and gene expression profile. PLoS ONE. 2016;11:e0167307. doi: 10.1371/journal.pone.0167307. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 45.Liu G.J., Middleton R.J., Hatty C.R., Kam W.W., Chan R., Pham T., Harrison-Brown M., Dodson E., Veale K., Banati R.B. The 18 kda translocator protein, microglia and neuroinflammation. Brain. Pathol. 2014;24:631–653. doi: 10.1111/bpa.12196. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 46.Beurdeley-Thomas A., Miccoli L., Oudard S., Dutrillaux B., Poupon M.F. The peripheral benzodiazepine receptors: A review. J. Neurooncol. 2000;46:45–56. doi: 10.1023/A:1006456715525. [DOI] [PubMed] [Google Scholar]
- 47.Gavish M., Bachman I., Shoukrun R., Katz Y., Veenman L., Weisinger G., Weizman A. Enigma of the peripheral benzodiazepine receptor. Pharm. Rev. 1999;51:629–650. [PubMed] [Google Scholar]
- 48.Anholt R.R.H. Mitochondrial benzodiazepine receptors as potential modulators of intermediary metabolism. Trends. Pharm. Sci. 1986;7:506–511. doi: 10.1016/0165-6147(86)90438-4. [DOI] [Google Scholar]
- 49.Hirsch J.D., Beyer C.F., Malkowitz L., Beer B., Blume A.J. Mitochondrial benzodiazepine receptors mediate inhibition of mitochondrial respiratory control. Mol. Pharm. 1989;35:157–163. [PubMed] [Google Scholar]
- 50.Larcher J.C., Vayssiere J.L., Le Marquer F.J., Cordeau L.R., Keane P.E., Bachy A., Gross F., Croizat B.P. Effects of peripheral benzodiazepines upon the o2 consumption of neuroblastoma cells. Eur. J. Pharm. 1989;161:197–202. doi: 10.1016/0014-2999(89)90843-1. [DOI] [PubMed] [Google Scholar]
- 51.Shiraishi T., Black K.L., Ikezaki K., Becker D.P. Peripheral benzodiazepine induces morphological changes and proliferation of mitochondria in glioma cells. J. Neurosci. Res. 1991;30:463–474. doi: 10.1002/jnr.490300303. [DOI] [PubMed] [Google Scholar]
- 52.Li H., Papadopoulos V. Peripheral-type benzodiazepine receptor function in cholesterol transport. Identification of a putative cholesterol recognition/interaction amino acid sequence and consensus pattern. Endocrinology. 1998;139:4991–4997. doi: 10.1210/endo.139.12.6390. [DOI] [PubMed] [Google Scholar]
- 53.Jaipuria G., Leonov A., Giller K., Vasa S.K., Jaremko Ł., Jaremko M., Linser R., Becker S., Zweckstetter M. Cholesterol-mediated allosteric regulation of the mitochondrial translocator protein structure. Nat. Commun. 2017;8:14893. doi: 10.1038/ncomms14893. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 54.Da Pozzo E., Giacomelli C., Costa B., Cavallini C., Taliani S., Barresi E., Da Settimo F., Martini C. Tspo piga ligands promote neurosteroidogenesis and human astrocyte well-being. Int. J. Mol. Sci. 2016;17:1028. doi: 10.3390/ijms17071028. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 55.Morohaku K., Pelton S.H., Daugherty D.J., Butler W.R., Deng W., Selvaraj V. Translocator protein/peripheral benzodiazepine receptor is not required for steroid hormone biosynthesis. Endocrinology. 2014;155:89–97. doi: 10.1210/en.2013-1556. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 56.Liu G.J., Middleton R.J., Kam W.W., Chin D.Y., Hatty C.R., Chan R.H., Banati R.B. Functional gains in energy and cell metabolism after tspo gene insertion. Cell. Cycle. 2017;16:436–447. doi: 10.1080/15384101.2017.1281477. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 57.Milenkovic V.M., Slim D., Bader S., Koch V., Heinl E.S., Alvarez-Carbonell D., Nothdurfter C., Rupprecht R., Wetzel C.H. Crispr-cas9 mediated tspo gene knockout alters respiration and cellular metabolism in human primary microglia cells. Int. J. Mol. 2019:20. doi: 10.3390/ijms20133359. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 58.Bader S., Wolf L., Milenkovic V.M., Gruber M., Nothdurfter C., Rupprecht R., Wetzel C.H. Differential effects of tspo ligands on mitochondrial function in mouse microglia cells. Psychoneuroendocrinology. 2019;106:65–76. doi: 10.1016/j.psyneuen.2019.03.029. [DOI] [PubMed] [Google Scholar]
- 59.Fu Y., Wang D., Wang H., Cai M., Li C., Zhang X., Chen H., Hu Y., Zhang X., Ying M., et al. Tspo deficiency induces mitochondrial dysfunction, leading to hypoxia, angiogenesis and a growth-promoting metabolic shift towards glycolysis in glioblastoma. Neuro. Oncol. 2019 doi: 10.1093/neuonc/noz183. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 60.Krestinina O.V., Grachev D.E., Odinokova I.V., Reiser G., Evtodienko Y.V., Azarashvili T.S. Effect of peripheral benzodiazepine receptor (pbr/tspo) ligands on opening of ca2+-induced pore and phosphorylation of 3.5-kda polypeptide in rat brain mitochondria. Biochem. (Mosc. ) 2009;74:421–429. doi: 10.1134/S0006297909040105. [DOI] [PubMed] [Google Scholar]
- 61.Seneviratne M.S., Faccenda D., De Biase V., Campanella M. Pk11195 inhibits mitophagy targeting the f1fo-atpsynthase in bcl-2 knock-down cells. Curr. Mol. Med. 2012;12:476–482. doi: 10.2174/156652412800163406. [DOI] [PubMed] [Google Scholar]
- 62.Jayakumar A.R., Panickar K.S., Norenberg M.D. Effects on free radical generation by ligands of the peripheral benzodiazepine receptor in cultured neural cells. J. Neurochem. 2002;83:1226–1234. doi: 10.1046/j.1471-4159.2002.01261.x. [DOI] [PubMed] [Google Scholar]
- 63.Stoebner P.E., Carayon P., Casellas P., Portier M., Lavabre-Bertrand T., Cuq P., Cano J.P., Meynadier J., Meunier L. Transient protection by peripheral benzodiazepine receptors during the early events of ultraviolet light-induced apoptosis. Cell. Death Differ. 2001;8:747–753. doi: 10.1038/sj.cdd.4400861. [DOI] [PubMed] [Google Scholar]
- 64.Lejri I., Grimm A., Halle F., Abarghaz M., Klein C., Maitre M., Schmitt M., Bourguignon J.J., Mensah-Nyagan A.G., Bihel F., et al. Tspo ligands boost mitochondrial function and pregnenolone synthesis. J. Alzheimer’s Dis. Jad. 2019 doi: 10.3233/JAD-190127. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 65.Grimm A., Lejri I., Halle F., Schmitt M., Gotz J., Bihel F., Eckert A. Mitochondria modulatory effects of new tspo ligands in a cellular model of tauopathies. J. Neuroendocr. 2019:e12796. doi: 10.1111/jne.12796. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 66.Kupa L.V.K., Drewes C.C., Barioni E.D., Neves C.L., Sampaio S.C., Farsky S.H.P. Role of translocator 18 kda ligands in the activation of leukotriene b4 activated g-protein coupled receptor and toll like receptor-4 pathways in neutrophils. Front. Pharm. 2017;8:766. doi: 10.3389/fphar.2017.00766. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 67.Baez E., Guio-Vega G.P., Echeverria V., Sandoval-Rueda D.A., Barreto G.E. 4′-chlorodiazepam protects mitochondria in t98g astrocyte cell line from glucose deprivation. Neurotox. Res. 2017;32:163–171. doi: 10.1007/s12640-017-9733-x. [DOI] [PubMed] [Google Scholar]
- 68.Gatliff J., East D., Crosby J., Abeti R., Harvey R., Craigen W., Parker P., Campanella M. Tspo interacts with vdac1 and triggers a ros-mediated inhibition of mitochondrial quality control. Autophagy. 2014;10:2279–2296. doi: 10.4161/15548627.2014.991665. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 69.Sliter D.A., Martinez J., Hao L., Chen X., Sun N., Fischer T.D., Burman J.L., Li Y., Zhang Z., Narendra D.P., et al. Parkin and pink1 mitigate sting-induced inflammation. Nature. 2018;561:258–262. doi: 10.1038/s41586-018-0448-9. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 70.Guilarte T.R., Loth M.K., Guariglia S.R. Tspo finds nox2 in microglia for redox homeostasis. Trends. Pharm. Sci. 2016;37:334–343. doi: 10.1016/j.tips.2016.02.008. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 71.Zeineh N., Nagler R., Gabay M., Weizman A., Gavish M. Effects of cigarette smoke on tspo-related mitochondrial processes. Cells. 2019:8. doi: 10.3390/cells8070694. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 72.Zeno S., Zaaroor M., Leschiner S., Veenman L., Gavish M. Cocl(2) induces apoptosis via the 18 kda translocator protein in u118mg human glioblastoma cells. Biochemistry. 2009;48:4652–4661. doi: 10.1021/bi900064t. [DOI] [PubMed] [Google Scholar]
- 73.Shargorodsky L., Veenman L., Caballero B., Pe'er Y., Leschiner S., Bode J., Gavish M. The nitric oxide donor sodium nitroprusside requires the 18 kda translocator protein to induce cell death. Apoptosis. 2012;17:647–665. doi: 10.1007/s10495-012-0725-2. [DOI] [PubMed] [Google Scholar]
- 74.Lin R., Angelin A., Da Settimo F., Martini C., Taliani S., Zhu S., Wallace D.C. Genetic analysis of dtspo, an outer mitochondrial membrane protein, reveals its functions in apoptosis, longevity, and ab42-induced neurodegeneration. Aging Cell. 2014;13:507–518. doi: 10.1111/acel.12200. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 75.Lin R., Rittenhouse D., Sweeney K., Potluri P., Wallace D.C. Tspo, a mitochondrial outer membrane protein, controls ethanol-related behaviors in drosophila. PloS Genet. 2015;11:e1005366. doi: 10.1371/journal.pgen.1005366. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 76.Xiao J., Liang D., Zhang H., Liu Y., Li F., Chen Y.H. 4′-chlorodiazepam, a translocator protein (18 kda) antagonist, improves cardiac functional recovery during postischemia reperfusion in rats. Exp. Biol. Med. (Maywood.) 2010;235:478–486. doi: 10.1258/ebm.2009.009291. [DOI] [PubMed] [Google Scholar]
- 77.Musman J., Paradis S., Panel M., Pons S., Barau C., Caccia C., Leoni V., Ghaleh B., Morin D. A tspo ligand prevents mitochondrial sterol accumulation and dysfunction during myocardial ischemia-reperfusion in hypercholesterolemic rats. Biochem. Pharm. 2017;142:87–95. doi: 10.1016/j.bcp.2017.06.125. [DOI] [PubMed] [Google Scholar]
- 78.Soustiel J.F., Vlodavsky E., Milman F., Gavish M., Zaaroor M. Improvement of cerebral metabolism mediated by ro5-4864 is associated with relief of intracranial pressure and mitochondrial protective effect in experimental brain injury. Pharm. Res. 2011;28:2945–2953. doi: 10.1007/s11095-011-0463-0. [DOI] [PubMed] [Google Scholar]
- 79.Chen Y., Veenman L., Singh S., Ouyang F., Liang J., Huang W., Marek I., Zeng J., Gavish M. 2-cl-mgv-1 ameliorates apoptosis in the thalamus and hippocampus and cognitive deficits after cortical infarct in rats. Stroke. 2017;48:3366–3374. doi: 10.1161/STROKEAHA.117.019439. [DOI] [PubMed] [Google Scholar]
- 80.Cheng Q., Sun G.J., Liu S.B., Yang Q., Li X.M., Li X.B., Liu G., Zhao J.N., Zhao M.G. A novel translocator protein 18 kda ligand, zbd-2, exerts neuroprotective effects against acute spinal cord injury. Clin. Exp. Pharm. Physiol. 2016;43:930–938. doi: 10.1111/1440-1681.12606. [DOI] [PubMed] [Google Scholar]
- 81.Boche D., Perry V.H., Nicoll J.A.R. Review: Activation patterns of microglia and their identification in the human brain. Neuropathol. Appl. Neurobiol. 2013;39:3–18. doi: 10.1111/nan.12011. [DOI] [PubMed] [Google Scholar]
- 82.Pozzo E.D., Tremolanti C., Costa B., Giacomelli C., Milenkovic V.M., Bader S., Wetzel C.H., Rupprecht R., Taliani S., Settimo F.D., et al. Microglial pro-inflammatory and anti-inflammatory phenotypes are modulated by translocator protein activation. Int. J. Mol. Sci. 2019;20:4467. doi: 10.3390/ijms20184467. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 83.Beckers L., Ory D., Geric I., Declercq L., Koole M., Kassiou M., Bormans G., Baes M. Increased expression of translocator protein (tspo) marks pro-inflammatory microglia but does not predict neurodegeneration. Mol. Imaging. Biol. 2018;20:94–102. doi: 10.1007/s11307-017-1099-1. [DOI] [PubMed] [Google Scholar]
- 84.Pannell M., Economopoulos V., Wilson T.C., Kersemans V., Isenegger P.G., Larkin J.R., Smart S., Gilchrist S., Gouverneur V., Sibson N.R. Imaging of translocator protein upregulation is selective for pro-inflammatory polarized astrocytes and microglia. Glia. 2019 doi: 10.1002/glia.23716. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 85.Choi H.B., Khoo C., Ryu J.K., van Breemen E., Kim S.U., McLarnon J.G. Inhibition of lipopolysaccharide-induced cyclooxygenase-2, tumor necrosis factor-alpha and [ca2+]i responses in human microglia by the peripheral benzodiazepine receptor ligand pk11195. J. Neurochem. 2002;83:546–555. doi: 10.1046/j.1471-4159.2002.01122.x. [DOI] [PubMed] [Google Scholar]
- 86.Wilms H., Claasen J., Rohl C., Sievers J., Deuschl G., Lucius R. Involvement of benzodiazepine receptors in neuroinflammatory and neurodegenerative diseases: Evidence from activated microglial cells in vitro. Neurobiol. Dis. 2003;14:417–424. doi: 10.1016/j.nbd.2003.07.002. [DOI] [PubMed] [Google Scholar]
- 87.Lee J.W., Nam H., Yu S.W. Systematic analysis of translocator protein 18 kda (tspo) ligands on toll-like receptors-mediated pro-inflammatory responses in microglia and astrocytes. Exp. Neurobiol. 2016;25:262–268. doi: 10.5607/en.2016.25.5.262. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 88.Zhao Y.Y., Yu J.Z., Li Q.Y., Ma C.G., Lu C.Z., Xiao B.G. Tspo-specific ligand vinpocetine exerts a neuroprotective effect by suppressing microglial inflammation. Neuron. Glia. Biol. 2011;7:187–197. doi: 10.1017/S1740925X12000129. [DOI] [PubMed] [Google Scholar]
- 89.Azrad M., Zeineh N., Weizman A., Veenman L., Gavish M. The tspo ligands 2-cl-mgv-1, mgv-1, and pk11195 differentially suppress the inflammatory response of bv-2 microglial cell to lps. Int. J. Mol. Sci. 2019:20. doi: 10.3390/ijms20030594. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 90.Monga S., Nagler R., Amara R., Weizman A., Gavish M. Inhibitory effects of the two novel tspo ligands 2-cl-mgv-1 and mgv-1 on lps-induced microglial activation. Cells. 2019:8. doi: 10.3390/cells8050486. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 91.Choi J., Ifuku M., Noda M., Guilarte T.R. Translocator protein (18 kda)/peripheral benzodiazepine receptor specific ligands induce microglia functions consistent with an activated state. Glia. 2011;59:219–230. doi: 10.1002/glia.21091. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 92.Wang M., Wang X., Zhao L., Ma W., Rodriguez I.R., Fariss R.N., Wong W.T. Macroglia-microglia interactions via tspo signaling regulates microglial activation in the mouse retina. J. Neurosci. 2014;34:3793–3806. doi: 10.1523/JNEUROSCI.3153-13.2014. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 93.Bonsack F.t., Alleyne C.H., Jr., Sukumari-Ramesh S. Augmented expression of tspo after intracerebral hemorrhage: A role in inflammation? J. Neuroinflammation. 2016;13:151. doi: 10.1186/s12974-016-0619-2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 94.Narayan N., Mandhair H., Smyth E., Dakin S.G., Kiriakidis S., Wells L., Owen D., Sabokbar A., Taylor P. The macrophage marker translocator protein (tspo) is down-regulated on pro-inflammatory ’m1’ human macrophages. PLoS ONE. 2017;12:e0185767. doi: 10.1371/journal.pone.0185767. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 95.Owen D.R., Narayan N., Wells L., Healy L., Smyth E., Rabiner E.A., Galloway D., Williams J.B., Lehr J., Mandhair H., et al. Pro-inflammatory activation of primary microglia and macrophages increases 18 kda translocator protein expression in rodents but not humans. J. Cereb. Blood. Flow. Metab. 2017;37:2679–2690. doi: 10.1177/0271678X17710182. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 96.Batarseh A., Li J., Papadopoulos V. Protein kinase c epsilon regulation of translocator protein (18 kda) tspo gene expression is mediated through a mapk pathway targeting stat3 and c-jun transcription factors. Biochemistry. 2010;49:4766–4778. doi: 10.1021/bi100020e. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 97.Kim H., Zamel R., Bai X.H., Liu M. Pkc activation induces inflammatory response and cell death in human bronchial epithelial cells. PLoS ONE. 2013;8:e64182. doi: 10.1371/journal.pone.0064182. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 98.Kaminska B. Mapk signalling pathways as molecular targets for anti-inflammatory therapy--from molecular mechanisms to therapeutic benefits. Biochim. Biophys. Acta. 2005;1754:253–262. doi: 10.1016/j.bbapap.2005.08.017. [DOI] [PubMed] [Google Scholar]
- 99.Gatliff J., Campanella M. Tspo: Kaleidoscopic 18-kda amid biochemical pharmacology, control and targeting of mitochondria. Biochem. J. 2016;473:107–121. doi: 10.1042/BJ20150899. [DOI] [PubMed] [Google Scholar]
- 100.Horiguchi Y., Ohta N., Yamamoto S., Koide M., Fujino Y. Midazolam suppresses the lipopolysaccharide-stimulated immune responses of human macrophages via translocator protein signaling. Int. Immunopharmacol. 2019;66:373–382. doi: 10.1016/j.intimp.2018.11.050. [DOI] [PubMed] [Google Scholar]
- 101.Zavala F., Taupin V., Descamps-Latscha B. In vivo treatment with benzodiazepines inhibits murine phagocyte oxidative metabolism and production of interleukin 1, tumor necrosis factor and interleukin-6. J. Pharm. Exp. 1990;255:442–450. [PubMed] [Google Scholar]
- 102.Ryu J.K., Choi H.B., McLarnon J.G. Peripheral benzodiazepine receptor ligand pk11195 reduces microglial activation and neuronal death in quinolinic acid-injected rat striatum. Neurobiol. Dis. 2005;20:550–561. doi: 10.1016/j.nbd.2005.04.010. [DOI] [PubMed] [Google Scholar]
- 103.Leaver K.R., Reynolds A., Bodard S., Guilloteau D., Chalon S., Kassiou M. Effects of translocator protein (18 kda) ligands on microglial activation and neuronal death in the quinolinic-acid-injected rat striatum. ACS Chem. Neurosci. 2012;3:114–119. doi: 10.1021/cn200099e. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 104.Ma B., Liu X., Huang X., Ji Y., Jin T., Ma K. Translocator protein agonist ro5-4864 alleviates neuropathic pain and promotes remyelination in the sciatic nerve. Mol. Pain. 2018;14:1744806917748019. doi: 10.1177/1744806917748019. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 105.Mills C., Makwana M., Wallace A., Benn S., Schmidt H., Tegeder I., Costigan M., Brown R.H., Jr., Raivich G., Woolf C.J. Ro5-4864 promotes neonatal motor neuron survival and nerve regeneration in adult rats. Eur. J. Neurosci. 2008;27:937–946. doi: 10.1111/j.1460-9568.2008.06065.x. [DOI] [PubMed] [Google Scholar]
- 106.Girard C., Liu S., Cadepond F., Adams D., Lacroix C., Verleye M., Gillardin J.M., Baulieu E.E., Schumacher M., Schweizer-Groyer G. Etifoxine improves peripheral nerve regeneration and functional recovery. Proc. Natl. Acad. Sci. USA. 2008;105:20505–20510. doi: 10.1073/pnas.0811201106. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 107.Simon-O'Brien E., Gauthier D., Riban V., Verleye M. Etifoxine improves sensorimotor deficits and reduces glial activation, neuronal degeneration, and neuroinflammation in a rat model of traumatic brain injury. J. Neuroinflammation. 2016;13:203. doi: 10.1186/s12974-016-0687-3. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 108.Barron A.M., Garcia-Segura L.M., Caruso D., Jayaraman A., Lee J.W., Melcangi R.C., Pike C.J. Ligand for translocator protein reverses pathology in a mouse model of alzheimer's disease. J. Neurosci. 2013;33:8891–8897. doi: 10.1523/JNEUROSCI.1350-13.2013. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 109.Scholz R., Caramoy A., Bhuckory M.B., Rashid K., Chen M., Xu H., Grimm C., Langmann T. Targeting translocator protein (18 kda) (tspo) dampens pro-inflammatory microglia reactivity in the retina and protects from degeneration. J. Neuroinflammation. 2015;12:201. doi: 10.1186/s12974-015-0422-5. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 110.Leva G., Klein C., Benyounes J., Halle F., Bihel F., Collongues N., De Seze J., Mensah-Nyagan A.G., Patte-Mensah C. The translocator protein ligand xbd173 improves clinical symptoms and neuropathological markers in the sjl/j mouse model of multiple sclerosis. Biochim. Biophys. Acta Mol. Basis. Dis. 2017;1863:3016–3027. doi: 10.1016/j.bbadis.2017.09.007. [DOI] [PubMed] [Google Scholar]
- 111.Gong J., Szego E.M., Leonov A., Benito E., Becker S., Fischer A., Zweckstetter M., Outeiro T., Schneider A. Translocator protein ligand protects against neurodegeneration in the mptp mouse model of parkinsonism. J. Neurosci. 2019;39:3752–3769. doi: 10.1523/JNEUROSCI.2070-18.2019. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 112.Snell C.R., Snell P.H. Benzodiazepines modulate the a2 adenosine binding sites on 108cc15 neuroblastoma x glioma hybrid cells. Br. J. Pharm. 1984;83:791–798. doi: 10.1111/j.1476-5381.1984.tb16234.x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 113.File S.E., Pellow S. Ro5-4864, a ligand for benzodiazepine micromolar and peripheral binding sites: Antagonism and enhancement of behavioural effects. Psychopharmacol. (Berl.) 1983;80:166–170. doi: 10.1007/BF00427962. [DOI] [PubMed] [Google Scholar]
- 114.Hatty C.R., Le Brun A.P., Lake V., Clifton L.A., Liu G.J., James M., Banati R.B. Investigating the interactions of the 18kda translocator protein and its ligand pk11195 in planar lipid bilayers. Biochim. Biophys. Acta. 2014;1838:1019–1030. doi: 10.1016/j.bbamem.2013.12.013. [DOI] [PubMed] [Google Scholar]
- 115.Hatty C.R., Banati R.B. Protein-ligand and membrane-ligand interactions in pharmacology: The case of the translocator protein (tspo) Pharmacol. Res. 2015;100:58–63. doi: 10.1016/j.phrs.2015.07.029. [DOI] [PubMed] [Google Scholar]
- 116.Costa B., Cavallini C., Da Pozzo E., Taliani S., Da Settimo F., Martini C. The anxiolytic etifoxine binds to tspo ro5-4864 binding site with long residence time showing a high neurosteroidogenic activity. ACS Chem. Neurosci. 2017;8:1448–1454. doi: 10.1021/acschemneuro.7b00027. [DOI] [PubMed] [Google Scholar]
- 117.Yang L., Zhang S., Ling X., Shao P., Jia N., Bai M. Multilayer photodynamic therapy for highly effective and safe cancer treatment. Acta Biomater. 2017;54:271–280. doi: 10.1016/j.actbio.2017.03.012. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 118.Sun X., Guo S., Wang W., Cao Z., Dan J., Cheng J., Cao W., Tian F., Cao W., Tian Y. Potential involvement of the 18 kda translocator protein and reactive oxygen species in apoptosis of thp-1 macrophages induced by sonodynamic therapy. PLoS ONE. 2018;13:e0196541. doi: 10.1371/journal.pone.0196541. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 119.Klee K., Storti F., Barben M., Samardzija M., Langmann T., Dunaief J., Grimm C. Systemic knockout of tspo in mice does not affect retinal morphology, function and susceptibility to degeneration. Exp. Eye. Res. 2019:188. doi: 10.1016/j.exer.2019.107816. [DOI] [PubMed] [Google Scholar]
- 120.Svahn A.J., Becker T.S., Graeber M.B. Emergent properties of microglia. Brain Pathol. 2014;24:665–670. doi: 10.1111/bpa.12195. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 121.Notter T., Coughlin J.M., Sawa A., Meyer U. Reconceptualization of translocator protein as a biomarker of neuroinflammation in psychiatry. Mol. Psychiatry. 2018;23:36–47. doi: 10.1038/mp.2017.232. [DOI] [PubMed] [Google Scholar]
- 122.Betlazar C., Harrison-Brown M., Middleton R.J., Banati R., Liu G.J. Cellular sources and regional variations in the expression of the neuroinflammatory marker translocator protein (tspo) in the normal brain. Int. J. Mol. 2018:19. doi: 10.3390/ijms19092707. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 123.Kim S., Kim N., Park S., Jeon Y., Lee J., Yoo S.J., Lee J.W., Moon C., Yu S.W., Kim E.K. Tanycytic tspo inhibition induces lipophagy to regulate lipid metabolism and improve energy balance. Autophagy. 2019:1–21. doi: 10.1080/15548627.2019.1659616. [DOI] [PMC free article] [PubMed] [Google Scholar]